89b7aad1c4462c2f41e82e5aa7940be3.ppt
- Количество слайдов: 75
 Disparities in Mental Health Care of Diverse Populations: The Process of Elimination University of Texas Health Sciences Center Committee of Advancement of Women and Minorities Distinguished Speakers Series San Antonio, Texas March 27, 2009 Annelle B. Primm, MD, MPH Director, Minority and National Affairs American Psychiatric Association
Disparities in Mental Health Care of Diverse Populations: The Process of Elimination University of Texas Health Sciences Center Committee of Advancement of Women and Minorities Distinguished Speakers Series San Antonio, Texas March 27, 2009 Annelle B. Primm, MD, MPH Director, Minority and National Affairs American Psychiatric Association
 Public Health Model n n Population perspective – tip of the iceberg, the evidence of [people] not seen Case finding Risk factors and protective factors Prevention: n Primary (prophylaxis) n Secondary (early intervention) n Tertiary (chronic care, maintenance)
Public Health Model n n Population perspective – tip of the iceberg, the evidence of [people] not seen Case finding Risk factors and protective factors Prevention: n Primary (prophylaxis) n Secondary (early intervention) n Tertiary (chronic care, maintenance)
 Determinants of Mental Health Individual Biology n Individual Behavior n Social Environment n Physical Environment n Access to Quality Care n Policies & Interventions n
Determinants of Mental Health Individual Biology n Individual Behavior n Social Environment n Physical Environment n Access to Quality Care n Policies & Interventions n
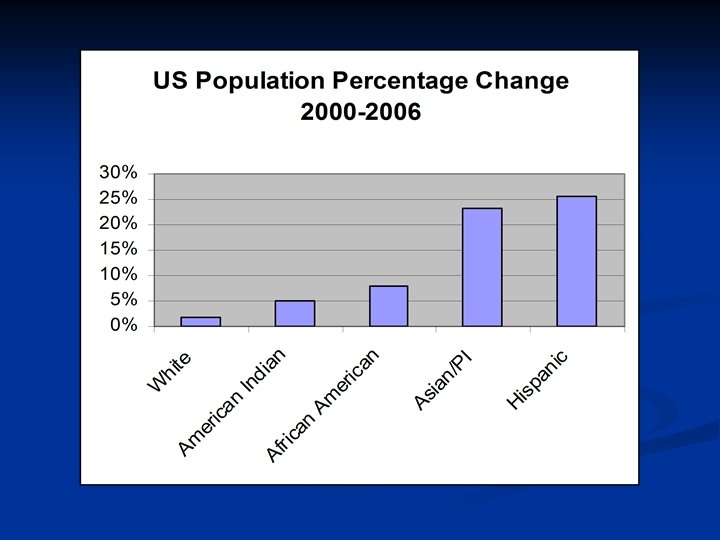
 Major Racial Ethnic Groups in U. S. n Latinos/Hispanics - 15% n African Americans - 13% n Asian American/Pacific Islanders - 5% n American Indians/Alaska Natives - 1% U. S. Census 2007
Major Racial Ethnic Groups in U. S. n Latinos/Hispanics - 15% n African Americans - 13% n Asian American/Pacific Islanders - 5% n American Indians/Alaska Natives - 1% U. S. Census 2007
 Surgeon General’s Report on Mental Health: Race, Culture, and Ethnicity Striking disparities in mental health care for people of color n Less likely to receive services n Poorer quality of care n Underrepresented in mental health research n Disparities impose great disability burden on people of color n Culture counts n
Surgeon General’s Report on Mental Health: Race, Culture, and Ethnicity Striking disparities in mental health care for people of color n Less likely to receive services n Poorer quality of care n Underrepresented in mental health research n Disparities impose great disability burden on people of color n Culture counts n
 Influence of Culture on Mental Illness and Mental Health How patients communicate n How patients manifest symptoms n How patients cope n Range of family and community support n Willingness to seek treatment n U. S. Dept. of Health and Human Services Office of the Surgeon General, SAMHSA Au
Influence of Culture on Mental Illness and Mental Health How patients communicate n How patients manifest symptoms n How patients cope n Range of family and community support n Willingness to seek treatment n U. S. Dept. of Health and Human Services Office of the Surgeon General, SAMHSA Au
 Factors in Mental Health, Mental Illness and Service Use n Racism n Discrimination n Economic impoverishment n Mistrust n Fear n Cultural and social influences n Biological, psychological and environmental factors U. S. Dept. of Health and Human Services Office of the Surgeon General,
Factors in Mental Health, Mental Illness and Service Use n Racism n Discrimination n Economic impoverishment n Mistrust n Fear n Cultural and social influences n Biological, psychological and environmental factors U. S. Dept. of Health and Human Services Office of the Surgeon General,
 High Need Populations n Overrepresentation of ethnically diverse populations n Homeless n Chronic Disease and Disability n Correctional facilities n Victims of violence n Child welfare n Immigrants and refugees U. S. DHHS, Office of the Surgeon General, SAMHSA August 2001
High Need Populations n Overrepresentation of ethnically diverse populations n Homeless n Chronic Disease and Disability n Correctional facilities n Victims of violence n Child welfare n Immigrants and refugees U. S. DHHS, Office of the Surgeon General, SAMHSA August 2001
 What Are Racial and Ethnic Health Disparities? n Differences and inequalities among racial, ethnic, linguistic, and cultural groups in n Risk and predisposition n Disease prevalence, health status, and diagnosis n Health care quality not due to access-related factors or clinical needs, preferences, and appropriateness of intervention n Health outcomes and mortality
What Are Racial and Ethnic Health Disparities? n Differences and inequalities among racial, ethnic, linguistic, and cultural groups in n Risk and predisposition n Disease prevalence, health status, and diagnosis n Health care quality not due to access-related factors or clinical needs, preferences, and appropriateness of intervention n Health outcomes and mortality
 IOM Report: Unequal Treatment n Racial and ethnic disparities exist regardless of SES n n Poorer quality of care n n Higher morbidity and mortality from the leading causes of death Worse outcomes Racial and ethnic minorities tend to receive a lower quality of healthcare than non-minorities, even when access-related factors, such as patients’ insurance status and income, are controlled. Smedley et al 2003; IOM 2002
IOM Report: Unequal Treatment n Racial and ethnic disparities exist regardless of SES n n Poorer quality of care n n Higher morbidity and mortality from the leading causes of death Worse outcomes Racial and ethnic minorities tend to receive a lower quality of healthcare than non-minorities, even when access-related factors, such as patients’ insurance status and income, are controlled. Smedley et al 2003; IOM 2002
 Outcomes: Higher Mortality n African-Americans n n American Indians and Alaska Natives n n Diabetes, infant mortality Asian Americans and Pacific Islanders n n Heart disease and stroke, cancer (breast, lung, and prostate), diabetes, infant mortality, HIV/AIDS Tuberculosis, stroke, cervical cancer Hispanics n Diabetes, uncontrolled hypertension, HIV/AIDS
Outcomes: Higher Mortality n African-Americans n n American Indians and Alaska Natives n n Diabetes, infant mortality Asian Americans and Pacific Islanders n n Heart disease and stroke, cancer (breast, lung, and prostate), diabetes, infant mortality, HIV/AIDS Tuberculosis, stroke, cervical cancer Hispanics n Diabetes, uncontrolled hypertension, HIV/AIDS
 Disparities in Seeking Mental Health Care African Americans: more likely to use emergency services or primary care providers than mental health specialists. (Surgeon General, 2001) Asian Americans: Only 4% would seek help from mental health specialist vs. 26 percent of whites. (Zhang et al. , 1998) Latinos: < 1 in 11 with mental disorders contact mental health specialists, & < 1 in 5 contact primary care providers. (Surgeon General, 2001) Native Americans: 44% with a mental health problem sought any kind of help--and only 28% of those contacted a mental health agency. (King, 1999)
Disparities in Seeking Mental Health Care African Americans: more likely to use emergency services or primary care providers than mental health specialists. (Surgeon General, 2001) Asian Americans: Only 4% would seek help from mental health specialist vs. 26 percent of whites. (Zhang et al. , 1998) Latinos: < 1 in 11 with mental disorders contact mental health specialists, & < 1 in 5 contact primary care providers. (Surgeon General, 2001) Native Americans: 44% with a mental health problem sought any kind of help--and only 28% of those contacted a mental health agency. (King, 1999)
 Unmet Need n Levels of unmet need (not receiving specialist or generalist care in past 12 months, with identified diagnosis in same period) African Americans – 72% n Asian Americans – 78% n Hispanics – 70% n Non-Hispanic Whites – 61% n Alegria et al 2006
Unmet Need n Levels of unmet need (not receiving specialist or generalist care in past 12 months, with identified diagnosis in same period) African Americans – 72% n Asian Americans – 78% n Hispanics – 70% n Non-Hispanic Whites – 61% n Alegria et al 2006
 Mental Health Disparities n n n Underuse of community outpatient care Use of alternative sources of help (faith, family, folk) primary care and alternative medicine Later entry into treatment, especially at the crisis or emergency stage High drop-out rate and fewer treatment sessions High rates of inpatient care, especially involuntary Cultural Competence Standards, 1997
Mental Health Disparities n n n Underuse of community outpatient care Use of alternative sources of help (faith, family, folk) primary care and alternative medicine Later entry into treatment, especially at the crisis or emergency stage High drop-out rate and fewer treatment sessions High rates of inpatient care, especially involuntary Cultural Competence Standards, 1997
 Mental Health Disparities Less access to bi-lingual services n More likely to be misdiagnosed n Less evidence based care n More inpatient hospitalizations n Less follow up after psychiatric hospitalization n
Mental Health Disparities Less access to bi-lingual services n More likely to be misdiagnosed n Less evidence based care n More inpatient hospitalizations n Less follow up after psychiatric hospitalization n
 Mental Health Disparities Underdiagnosis and undertreatment of anxiety and mood disorders n Differential prescribing patterns n Lower metabolism of certain psychotropic medications n More side effects and less adherence n More seclusion and restraint n
Mental Health Disparities Underdiagnosis and undertreatment of anxiety and mood disorders n Differential prescribing patterns n Lower metabolism of certain psychotropic medications n More side effects and less adherence n More seclusion and restraint n
 Ethnocultural Influences on Mental Health Care Outcomes Direct: n Cultural beliefs and preferences n Pathoplasticity n Ethnopsychopharmacology
Ethnocultural Influences on Mental Health Care Outcomes Direct: n Cultural beliefs and preferences n Pathoplasticity n Ethnopsychopharmacology
 Ethnocultural Influences on Mental Health Care Outcomes Indirect: n Bias and stereotyping n Misinterpretation of behavior and belief n Lack of symptom recognition n Misdiagnosis and inappropriate treatment n Ignorance of ethnocultural issues
Ethnocultural Influences on Mental Health Care Outcomes Indirect: n Bias and stereotyping n Misinterpretation of behavior and belief n Lack of symptom recognition n Misdiagnosis and inappropriate treatment n Ignorance of ethnocultural issues
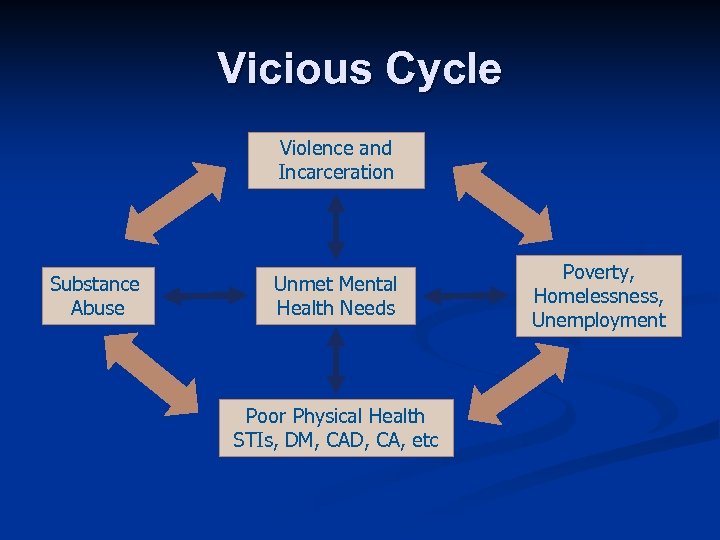 Vicious Cycle Violence and Incarceration Substance Abuse Unmet Mental Health Needs Poor Physical Health STIs, DM, CAD, CA, etc Poverty, Homelessness, Unemployment
Vicious Cycle Violence and Incarceration Substance Abuse Unmet Mental Health Needs Poor Physical Health STIs, DM, CAD, CA, etc Poverty, Homelessness, Unemployment
 Barriers and Mediators to Equitable Mental Health Care for Diverse Racial and Ethnic Groups Barriers Personal/Family n Acceptability n Cultural beliefs n Language/literacy Use of Services Visits n Primary care n Specialty n Emergency n Attitudes, beliefs n Preferences n Involvement in care n Health behavior n Education/income Structural n Availability n Appointments n How organized n Transportation Financial n Insurance coverage n Reimbursement levels n Public support Procedures n Preventive n Diagnostic n Therapeutic Mediators Quality of providers n Cultural competence n Communication skills n Medical knowledge n Technical skills n Bias/stereotyping n Appropriateness of care n Efficacy of treatment n Patient adherence Outcomes Health Status n Mortality n Morbidity n Well-being n Functioning Equity of Services Patient Views of Care n Experiences n Satisfaction n Effective partnership Modified from Institute of Medicine. Access to Health Care in America: A Model for Monitoring Access. Washington, DC: National Academy Press; 1993. Cooper LA, Hill MN, Powe NR. J Gen Internal Med. 2002; 477 -486.
Barriers and Mediators to Equitable Mental Health Care for Diverse Racial and Ethnic Groups Barriers Personal/Family n Acceptability n Cultural beliefs n Language/literacy Use of Services Visits n Primary care n Specialty n Emergency n Attitudes, beliefs n Preferences n Involvement in care n Health behavior n Education/income Structural n Availability n Appointments n How organized n Transportation Financial n Insurance coverage n Reimbursement levels n Public support Procedures n Preventive n Diagnostic n Therapeutic Mediators Quality of providers n Cultural competence n Communication skills n Medical knowledge n Technical skills n Bias/stereotyping n Appropriateness of care n Efficacy of treatment n Patient adherence Outcomes Health Status n Mortality n Morbidity n Well-being n Functioning Equity of Services Patient Views of Care n Experiences n Satisfaction n Effective partnership Modified from Institute of Medicine. Access to Health Care in America: A Model for Monitoring Access. Washington, DC: National Academy Press; 1993. Cooper LA, Hill MN, Powe NR. J Gen Internal Med. 2002; 477 -486.
 Barriers: Attitudes and Language n n Immigrant populations (Asian Americans and Hispanics) with limited English proficiency report communication a major obstacle in addressing MH concerns Cultural perception of mental illness affects: n likelihood of seeking care n support n feelings of shame, stigma, weakness n help seeking at crisis stage rather than earlier Alegria et al 2006; Minski S 2003; Cooper et al 2001; Yeh & Inose 2002
Barriers: Attitudes and Language n n Immigrant populations (Asian Americans and Hispanics) with limited English proficiency report communication a major obstacle in addressing MH concerns Cultural perception of mental illness affects: n likelihood of seeking care n support n feelings of shame, stigma, weakness n help seeking at crisis stage rather than earlier Alegria et al 2006; Minski S 2003; Cooper et al 2001; Yeh & Inose 2002
 Barriers: Language 18 % of the U. S. population (nearly 47 million people) speak a language other than English at home n 28% of all Spanish speakers, 22. 5% of Asian and Pacific Islander speakers and 13% of Indo-European language speakers speak English either not well or not at all n Limited English Proficiency (LEP) affects a person’s ability to access and receive health and mental health care n National Health Law Program NHe. LP, 2006
Barriers: Language 18 % of the U. S. population (nearly 47 million people) speak a language other than English at home n 28% of all Spanish speakers, 22. 5% of Asian and Pacific Islander speakers and 13% of Indo-European language speakers speak English either not well or not at all n Limited English Proficiency (LEP) affects a person’s ability to access and receive health and mental health care n National Health Law Program NHe. LP, 2006
 Barriers: Attitudes and Beliefs African Americans and Hispanics had lower odds than non-Hispanic whites of finding antidepressant medications acceptable n African Americans had lower odds and Hispanics had higher odds than non. Hispanic whites of finding counseling acceptable. n Cooper et al 2003
Barriers: Attitudes and Beliefs African Americans and Hispanics had lower odds than non-Hispanic whites of finding antidepressant medications acceptable n African Americans had lower odds and Hispanics had higher odds than non. Hispanic whites of finding counseling acceptable. n Cooper et al 2003
 Barriers: Health Behavior n Physicians were less patient-centered with African American than non-Hispanic white patients n Less patient input is associated with less information recall, treatment adherence, satisfaction with care, return visits, and suboptimal health outcomes Roter et al 1997
Barriers: Health Behavior n Physicians were less patient-centered with African American than non-Hispanic white patients n Less patient input is associated with less information recall, treatment adherence, satisfaction with care, return visits, and suboptimal health outcomes Roter et al 1997
 Availability of Mental Health Services by Race, Ethnicity n n African Americans account for 2% psychologists, 4% social workers in U. S. In 2005, 16. 7% of psychiatrists were from the 4 major racial/ethnic groups: (Black 2. 6%; Asian 9. 6%, Hispanic 4. 4%, Native American 0. 07%) Percentage of Spanish-speaking healthcare professionals unknown In 1996, only 29 psychiatrists identified as AIAN heritage U. S. Dept. of Health and Human Services Office of the Surgeon General, SAMH
Availability of Mental Health Services by Race, Ethnicity n n African Americans account for 2% psychologists, 4% social workers in U. S. In 2005, 16. 7% of psychiatrists were from the 4 major racial/ethnic groups: (Black 2. 6%; Asian 9. 6%, Hispanic 4. 4%, Native American 0. 07%) Percentage of Spanish-speaking healthcare professionals unknown In 1996, only 29 psychiatrists identified as AIAN heritage U. S. Dept. of Health and Human Services Office of the Surgeon General, SAMH
 Mediators: Cultural Competence n n Limited racial/ethnic diversity of MH providers Greater cultural difference may result in higher likelihood of misdiagnosis Cultural incompetence, including language barriers, increase likelihood of misdiagnosis When needed, less than 20% of patients seeking MH services, had interpreter services available Alegria et al 2006; Minski S et al 2003
Mediators: Cultural Competence n n Limited racial/ethnic diversity of MH providers Greater cultural difference may result in higher likelihood of misdiagnosis Cultural incompetence, including language barriers, increase likelihood of misdiagnosis When needed, less than 20% of patients seeking MH services, had interpreter services available Alegria et al 2006; Minski S et al 2003
 Culturally Competent Care Health and human services are offered and delivered in a way that are sensitive to the language, culture and traditions of nonnative immigrants, migrants and ethnic minorities with the goal of minimizing or eliminating long standing disparities in the health status of people with diverse racial, ethnic or cultural backgrounds. (www. icfdn. org)
Culturally Competent Care Health and human services are offered and delivered in a way that are sensitive to the language, culture and traditions of nonnative immigrants, migrants and ethnic minorities with the goal of minimizing or eliminating long standing disparities in the health status of people with diverse racial, ethnic or cultural backgrounds. (www. icfdn. org)
 Culturally Competent Care The ability of any health care provider of any cultural background in one’s organization to effectively treat any patient of any cultural background. (Matus, JC 2004, Health Care Manag)
Culturally Competent Care The ability of any health care provider of any cultural background in one’s organization to effectively treat any patient of any cultural background. (Matus, JC 2004, Health Care Manag)
 Cultural Competence A set of congruent behaviors, attitudes and policies that come together as a system, agency or among professionals and enable that system, agency or those professionals to work effectively in crosscultural situations. (AAFP, 2001)
Cultural Competence A set of congruent behaviors, attitudes and policies that come together as a system, agency or among professionals and enable that system, agency or those professionals to work effectively in crosscultural situations. (AAFP, 2001)
 Cultural Competence Acceptance and respect for differences n Continuing self assessment regarding culture n Attention to the dynamics of difference n Ongoing development of cultural knowledge and resources n Dynamic and flexible application of service models to meet the needs of diverse populations n SAMHSA, CMHS, 1998
Cultural Competence Acceptance and respect for differences n Continuing self assessment regarding culture n Attention to the dynamics of difference n Ongoing development of cultural knowledge and resources n Dynamic and flexible application of service models to meet the needs of diverse populations n SAMHSA, CMHS, 1998
 Outline for Cultural Formulation DSM IV-TR cultural identity of the individual n cultural explanations of the individual’s illness n cultural factors related to psychosocial environment and levels of functioning n cultural elements of the relationship between the individual and the clinician n overall cultural assessment for diagnosis and care n
Outline for Cultural Formulation DSM IV-TR cultural identity of the individual n cultural explanations of the individual’s illness n cultural factors related to psychosocial environment and levels of functioning n cultural elements of the relationship between the individual and the clinician n overall cultural assessment for diagnosis and care n
 Mediators: Cultural Competence n n At least 1 in 5 resident physicians surveyed (from seven specialties) reported not being prepared to deal with cross-cultural issues Approximately half of residents reported receiving little or no training in understanding how to address patients from different cultures (50%), or how to identify patient mistrust (56%), relevant religious beliefs (50%), and relevant cultural customs (48%) Weisman et al 2005
Mediators: Cultural Competence n n At least 1 in 5 resident physicians surveyed (from seven specialties) reported not being prepared to deal with cross-cultural issues Approximately half of residents reported receiving little or no training in understanding how to address patients from different cultures (50%), or how to identify patient mistrust (56%), relevant religious beliefs (50%), and relevant cultural customs (48%) Weisman et al 2005
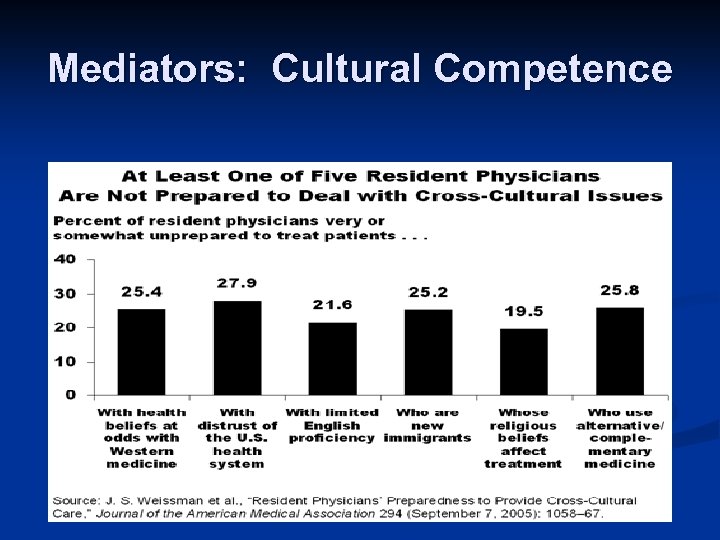 Mediators: Cultural Competence
Mediators: Cultural Competence
 Mediators: Bias and Stereotyping n Un-structured interviews lead to greater variability in diagnosis, greater reliance on bias/stereotypes n Psychometric validation is needed to determine whether disparities in diagnoses reflect differences in detection (clinical uncertainty, biases) Strakowski SM et al 2003; West et al 2006
Mediators: Bias and Stereotyping n Un-structured interviews lead to greater variability in diagnosis, greater reliance on bias/stereotypes n Psychometric validation is needed to determine whether disparities in diagnoses reflect differences in detection (clinical uncertainty, biases) Strakowski SM et al 2003; West et al 2006
 The Ethnopsychopharmacological Approach n Assessment n n Choice of medication n Cultural formulation for diagnosis Use medical history, concurrent medications, diet, food supplements, and herbals combined with knowledge of enzyme activity in certain ethnic groups. Start at lower doses. Monitor patient n n n Proceed slowly - involve family If side effects are intolerable - lower dosage or choose drug metabolized through different route If no response - check adherence, raise dose and monitor levels; add inhibitors; switch drug (Henderson, 2007)
The Ethnopsychopharmacological Approach n Assessment n n Choice of medication n Cultural formulation for diagnosis Use medical history, concurrent medications, diet, food supplements, and herbals combined with knowledge of enzyme activity in certain ethnic groups. Start at lower doses. Monitor patient n n n Proceed slowly - involve family If side effects are intolerable - lower dosage or choose drug metabolized through different route If no response - check adherence, raise dose and monitor levels; add inhibitors; switch drug (Henderson, 2007)
 Outcomes: Patient Views of Care n n n Reported spending enough time with providers n 50% of Asian Americans n 57% of Hispanics n 70% of non-Hispanic Whites Reported having negative experience with service providers n 20% of Asian Americans and Hispanics (NLAAS) Reported being treated with disrespect or looked down on in their patient/provider relationship n 14% of African Americans n 20% of Asian Americans n 19% of Hispanics n 9% of non-Hispanic Whites Alegria et al 2006; Blanchard & Lurie, 2004; Collins et al 2002
Outcomes: Patient Views of Care n n n Reported spending enough time with providers n 50% of Asian Americans n 57% of Hispanics n 70% of non-Hispanic Whites Reported having negative experience with service providers n 20% of Asian Americans and Hispanics (NLAAS) Reported being treated with disrespect or looked down on in their patient/provider relationship n 14% of African Americans n 20% of Asian Americans n 19% of Hispanics n 9% of non-Hispanic Whites Alegria et al 2006; Blanchard & Lurie, 2004; Collins et al 2002
 Outcomes: Patient Satisfaction Patients feel more involved with their care when their physician is of the same race n Greater involvement with care translates into higher patient satisfaction and better medical care n Cooper-Patrick et al 1999
Outcomes: Patient Satisfaction Patients feel more involved with their care when their physician is of the same race n Greater involvement with care translates into higher patient satisfaction and better medical care n Cooper-Patrick et al 1999
 Outcomes: Effective Partnership n Racial/ethnic minorities rate the quality of interpersonal care by physicians and within the health care system in general more negatively than non-Hispanic whites. Collins et al 2002
Outcomes: Effective Partnership n Racial/ethnic minorities rate the quality of interpersonal care by physicians and within the health care system in general more negatively than non-Hispanic whites. Collins et al 2002
 Landmark Reports & National Initiatives 1997 Cultural Competence Standards n 1998 President Clinton’s Presidential Initiative on Healthcare Disparities n 2000 IOM Crossing the Quality Chasm n 2001 SG Report on MH: Culture, Race, & Ethnicity n 2002 IOM Unequal Treatment: Confronting Racial & Ethnic Disparities in Health Care n
Landmark Reports & National Initiatives 1997 Cultural Competence Standards n 1998 President Clinton’s Presidential Initiative on Healthcare Disparities n 2000 IOM Crossing the Quality Chasm n 2001 SG Report on MH: Culture, Race, & Ethnicity n 2002 IOM Unequal Treatment: Confronting Racial & Ethnic Disparities in Health Care n
 Landmark Reports & Initiatives n n n 2003 President Bush’s New Freedom Commission on Mental Health 2004 IOM In the Nation’s Compelling Interest: Ensuring Diversity in the Health Care Workforce 2005 Commission to End Health Care Disparities (AMA, NHMA) 2005 Sullivan Report, Missing Persons AAMC Health Professionals for Diversity 2005 IOM Health Care for Mental and Substance Use Conditions
Landmark Reports & Initiatives n n n 2003 President Bush’s New Freedom Commission on Mental Health 2004 IOM In the Nation’s Compelling Interest: Ensuring Diversity in the Health Care Workforce 2005 Commission to End Health Care Disparities (AMA, NHMA) 2005 Sullivan Report, Missing Persons AAMC Health Professionals for Diversity 2005 IOM Health Care for Mental and Substance Use Conditions
 Synopsis of Culturally and Linguistically Appropriate Services (CLAS) Standards n n n Quality care Diverse staff Ongoing education and training Free and competent language assistance services Patient-related materials and signage Strategic plan Organizational self-assessment Collect data Profile and needs assessment Collaborative partnerships Conflict and grievance process Publicize successes
Synopsis of Culturally and Linguistically Appropriate Services (CLAS) Standards n n n Quality care Diverse staff Ongoing education and training Free and competent language assistance services Patient-related materials and signage Strategic plan Organizational self-assessment Collect data Profile and needs assessment Collaborative partnerships Conflict and grievance process Publicize successes
 Health Disparities Collaboratives n n n Community of Learners HRSA support of strategic state and national partnerships Improving systems of health care Planned care model Model for improvement in the context of community-oriented primary care Improve health outcomes (diabetes, asthma, depression) and organizational sustainability
Health Disparities Collaboratives n n n Community of Learners HRSA support of strategic state and national partnerships Improving systems of health care Planned care model Model for improvement in the context of community-oriented primary care Improve health outcomes (diabetes, asthma, depression) and organizational sustainability
 Nat’l Network to Eliminate Disparities in Behavioral Health - NNED n n SAMHSA in partnership with the National Alliance of Multi-ethnic Behavioral Health Associations Vision: diverse families thrive, participate and contribute to healthy communities Community and ethnic-based organizations and networks, knowledge discovery centers, and a national facilitation center Equity in care is an inadequate outcome, rather transformation is needed for behavioral health focused on culturally and linguistically competent interventions
Nat’l Network to Eliminate Disparities in Behavioral Health - NNED n n SAMHSA in partnership with the National Alliance of Multi-ethnic Behavioral Health Associations Vision: diverse families thrive, participate and contribute to healthy communities Community and ethnic-based organizations and networks, knowledge discovery centers, and a national facilitation center Equity in care is an inadequate outcome, rather transformation is needed for behavioral health focused on culturally and linguistically competent interventions
 IOM Unequal Treatment: Recommendations Increase public and provider awareness of disparities n Change financial incentives to improve quality, decrease fragmentation of care n Ensure provider supply, reduce barriers and promote quality evidence-based practice n Promote civil rights enforcement n Institute of Medicine, 2003
IOM Unequal Treatment: Recommendations Increase public and provider awareness of disparities n Change financial incentives to improve quality, decrease fragmentation of care n Ensure provider supply, reduce barriers and promote quality evidence-based practice n Promote civil rights enforcement n Institute of Medicine, 2003
 IOM Unequal Treatment: Recommendations n n Promote provider training, cultural competence, translation services, community health workers and multidisciplinary teams Promote patient education to enhance access and participation in treatment decisions Collect data on access, utilization and quality including race/ethnicity/language and monitor progress Conduct more research on sources of disparities and interventions to eliminate them Institute of Medicine, 2003
IOM Unequal Treatment: Recommendations n n Promote provider training, cultural competence, translation services, community health workers and multidisciplinary teams Promote patient education to enhance access and participation in treatment decisions Collect data on access, utilization and quality including race/ethnicity/language and monitor progress Conduct more research on sources of disparities and interventions to eliminate them Institute of Medicine, 2003
 Rationale for Culturally Competent Health Care • Responding to demographic changes • Eliminating disparities in the health status of people of diverse racial, ethnic, & cultural backgrounds • Improving the quality of services & outcomes • Meeting legislative, regulatory, & accreditation mandates • Gaining a competitive edge in the marketplace • Decreasing the likelihood of liability/malpractice claims Cohen E, Goode T. Policy Brief 1: Rationale for cultural competence in primary health care. Georgetown University Child Development Center, The National Center for Cultural Competence. Washington, D. C. , 1999.
Rationale for Culturally Competent Health Care • Responding to demographic changes • Eliminating disparities in the health status of people of diverse racial, ethnic, & cultural backgrounds • Improving the quality of services & outcomes • Meeting legislative, regulatory, & accreditation mandates • Gaining a competitive edge in the marketplace • Decreasing the likelihood of liability/malpractice claims Cohen E, Goode T. Policy Brief 1: Rationale for cultural competence in primary health care. Georgetown University Child Development Center, The National Center for Cultural Competence. Washington, D. C. , 1999.
 Cultural Competence Guiding Principles n Quality n Data Driven Systems n Outcomes n Prevention
Cultural Competence Guiding Principles n Quality n Data Driven Systems n Outcomes n Prevention
 Cultural Competence Techniques n n n n Interpreter Services Written Translations Concordant Clinicians and Staff Education and Training Community Health Workers Health Promotion Organizational Supports Brach and Fraser, Quality Management in Health Care, 2002, 10(4), 15 -28
Cultural Competence Techniques n n n n Interpreter Services Written Translations Concordant Clinicians and Staff Education and Training Community Health Workers Health Promotion Organizational Supports Brach and Fraser, Quality Management in Health Care, 2002, 10(4), 15 -28
 Clinician Patient Behavioral Change n n Improved Communication Increased Trust Improved Epidemiologic and Treatment Efficacy Knowledge Expanded Cultural and Environmental Understanding Brach and Fraser, Quality Management in Health Care, 2002, 10(4), 15 -28
Clinician Patient Behavioral Change n n Improved Communication Increased Trust Improved Epidemiologic and Treatment Efficacy Knowledge Expanded Cultural and Environmental Understanding Brach and Fraser, Quality Management in Health Care, 2002, 10(4), 15 -28
 Reducing Health Disparities Through the Implementation of Cultural Competency Diverse Populations Cultural Competency • linguistically • ethnically • culturally • effective techniques • sound implementation + Appropriate Services for Diverse Groups Improved Outcomes for Diverse Groups • preventive • screening • diagnostic • treatment • health status • functioning • satisfaction Reduction of Health Disparities Source: Brach and Fraser, Cultural Competency; 2000
Reducing Health Disparities Through the Implementation of Cultural Competency Diverse Populations Cultural Competency • linguistically • ethnically • culturally • effective techniques • sound implementation + Appropriate Services for Diverse Groups Improved Outcomes for Diverse Groups • preventive • screening • diagnostic • treatment • health status • functioning • satisfaction Reduction of Health Disparities Source: Brach and Fraser, Cultural Competency; 2000
 General Strategies to Address Disparities Must address all potential factors affecting disparities n May need to address subpopulations of diverse ethnic and racial groups differently, dependent on how various factors affect them n Include diverse communities at all levels of research, policy, planning, programs, evaluation n
General Strategies to Address Disparities Must address all potential factors affecting disparities n May need to address subpopulations of diverse ethnic and racial groups differently, dependent on how various factors affect them n Include diverse communities at all levels of research, policy, planning, programs, evaluation n
 Strategies to Increase Use of Services n n Integration of Mental Health in Primary care settings Increase screening and focus on prevention Increase knowledge of ethnic and racial differences for effective diagnosis and treatment (address at level of training, medical school, residency, and CME) Standards for screening, referral, diagnosis, and treatment
Strategies to Increase Use of Services n n Integration of Mental Health in Primary care settings Increase screening and focus on prevention Increase knowledge of ethnic and racial differences for effective diagnosis and treatment (address at level of training, medical school, residency, and CME) Standards for screening, referral, diagnosis, and treatment
 Strategies to Reduce Barriers n n n Policy and funding to improve/increase (structural and personnel) MH services in human services, and other public sectors where populations are affected (correctional, child welfare, school, community health) Universal health insurance to assure coverage Mental health parity Public marketing to increase population knowledge, change health behavior Patient activation
Strategies to Reduce Barriers n n n Policy and funding to improve/increase (structural and personnel) MH services in human services, and other public sectors where populations are affected (correctional, child welfare, school, community health) Universal health insurance to assure coverage Mental health parity Public marketing to increase population knowledge, change health behavior Patient activation
 Strategies to Enhance Mediating Factors n n n Provider education on cultural competence Clinicians should consider patients’ cultural and social context when negotiating treatment decisions Provider incentives (career, financial) for successful referral and engagement Increase ethnic and racial minority representation in all clinical trials (better understand environmental and biological interactions and effect on symptomatology/drug interaction) Language competency in assessment/diagnostic instruments
Strategies to Enhance Mediating Factors n n n Provider education on cultural competence Clinicians should consider patients’ cultural and social context when negotiating treatment decisions Provider incentives (career, financial) for successful referral and engagement Increase ethnic and racial minority representation in all clinical trials (better understand environmental and biological interactions and effect on symptomatology/drug interaction) Language competency in assessment/diagnostic instruments
 Strategies to Improve Outcomes n n Greater public health interventions as basis for correctional, child welfare, human services systems Collecting data and reporting on race and ethnic groups’ health status (mental health, functioning, co-morbidities) Clinicians to screen for suicide risk and monitor carefully consumers with anxiety and mood disorders Longitudinal studies to evaluate equity of services, patient experiences
Strategies to Improve Outcomes n n Greater public health interventions as basis for correctional, child welfare, human services systems Collecting data and reporting on race and ethnic groups’ health status (mental health, functioning, co-morbidities) Clinicians to screen for suicide risk and monitor carefully consumers with anxiety and mood disorders Longitudinal studies to evaluate equity of services, patient experiences
 Office of Minority and National Affairs (OMNA) APA’s nerve center for the mental health of diverse and underserved populations
Office of Minority and National Affairs (OMNA) APA’s nerve center for the mental health of diverse and underserved populations
 Our Mission To contribute to the improvement of the quality of care for diverse and underserved populations n To meet the professional needs of psychiatrists from under-represented (MUR) groups n
Our Mission To contribute to the improvement of the quality of care for diverse and underserved populations n To meet the professional needs of psychiatrists from under-represented (MUR) groups n
 Our Main Issues & Constituencies People of African, Asian, Hispanic, Native American descent n Women n Gay, Lesbian and Bisexual Issues n International Medical Graduates n Religious and Spiritual Issues n
Our Main Issues & Constituencies People of African, Asian, Hispanic, Native American descent n Women n Gay, Lesbian and Bisexual Issues n International Medical Graduates n Religious and Spiritual Issues n
 Our Priorities Increase diversity in psychiatry n Foster the professional well-being of psychiatrists from underrepresented groups n Increase knowledge of the mental health needs of underserved populations n Educate communities about mental health disparities n Forge alliances to prevent and eliminate disparities n
Our Priorities Increase diversity in psychiatry n Foster the professional well-being of psychiatrists from underrepresented groups n Increase knowledge of the mental health needs of underserved populations n Educate communities about mental health disparities n Forge alliances to prevent and eliminate disparities n
 American Psychiatric Association Disparities Elimination Efforts n n n Buy-in at the top: elected leaders, Board of Trustees, executive staff Support of the Office of Minority and National Affairs (OMNA) Recommendations stemming from SGR Supplement passed by board of trustees: n n n Increase access to quality care Support capacity development, education and training Expand the science base Promote collaboration and advocacy Eliminating Mental Health Disparities Roundtable .
American Psychiatric Association Disparities Elimination Efforts n n n Buy-in at the top: elected leaders, Board of Trustees, executive staff Support of the Office of Minority and National Affairs (OMNA) Recommendations stemming from SGR Supplement passed by board of trustees: n n n Increase access to quality care Support capacity development, education and training Expand the science base Promote collaboration and advocacy Eliminating Mental Health Disparities Roundtable .
 Fellowship Programs Minority Fellowships Program n SAMHSA, Astra. Zeneca n Program for Minority Research Training in Psychiatry (in collaboration with APIRE) n Spurlock Congressional Fellowship n Medical student programs n Mentoring, travel scholarships, addiction and HIV psychiatry summer externships n
Fellowship Programs Minority Fellowships Program n SAMHSA, Astra. Zeneca n Program for Minority Research Training in Psychiatry (in collaboration with APIRE) n Spurlock Congressional Fellowship n Medical student programs n Mentoring, travel scholarships, addiction and HIV psychiatry summer externships n
 Recognition Awards n n n n Simon Bolivar Award (Hispanic leaders) Solomon Carter Fuller Award (pioneering African-Americans) John Fryer Award (GLBT health) Oskar Pfister Award (religion, spirituality, and psychiatry) Kun-Po Soo Award (Asian cultural heritage) George Tarjan Award (IMG advocacy) Jeanne Spurlock Achievement Award (MFP graduate)
Recognition Awards n n n n Simon Bolivar Award (Hispanic leaders) Solomon Carter Fuller Award (pioneering African-Americans) John Fryer Award (GLBT health) Oskar Pfister Award (religion, spirituality, and psychiatry) Kun-Po Soo Award (Asian cultural heritage) George Tarjan Award (IMG advocacy) Jeanne Spurlock Achievement Award (MFP graduate)
 OMNA Products n CME curriculum, NAMI-APA effort n n Let’s Talk Facts series on Mental Health of Diverse Populations available at healthyminds. org n n People of African, Asian, American Indian, Hispanic descent Book n n In Living Color: Treating Depression in Diverse Populations for primary care Disparities in Psychiatric Care: Clinical and Cross. Cultural Perspectives DVDs n n Latino Mental Health DVD and Guidebook Real Psychiatry: Doctors in Action
OMNA Products n CME curriculum, NAMI-APA effort n n Let’s Talk Facts series on Mental Health of Diverse Populations available at healthyminds. org n n People of African, Asian, American Indian, Hispanic descent Book n n In Living Color: Treating Depression in Diverse Populations for primary care Disparities in Psychiatric Care: Clinical and Cross. Cultural Perspectives DVDs n n Latino Mental Health DVD and Guidebook Real Psychiatry: Doctors in Action

 OMNA Special Projects n n n n Women’s Mental Health Roundtable All Healers Mental Health Alliance OMNA on Tour Community Connections Doctors Back to School Transformational Leadership in Psychiatry Academy National Minority Mentors Network n Collaboration with Texas Regional Psychiatry Minority Mentorship Network (TRMMN)
OMNA Special Projects n n n n Women’s Mental Health Roundtable All Healers Mental Health Alliance OMNA on Tour Community Connections Doctors Back to School Transformational Leadership in Psychiatry Academy National Minority Mentors Network n Collaboration with Texas Regional Psychiatry Minority Mentorship Network (TRMMN)
 Diversity-Related Outcomes n n n TRPMMN illustrates: Increased medical school diversity is associated with white students feeling better prepared to care for diverse patients. * Compositional Diversity: proportions of URM students and non-white, non-URM students Interactional Diversity: climate for interracial interaction, individual exposure to diverse perspectives *Saha et al, Student Body Racial and Ethnic Composition and Diversity-Related Outcomes in US Medical Schools, JAMA, Sept. 10, 2008, 300(10): 1135 -1145
Diversity-Related Outcomes n n n TRPMMN illustrates: Increased medical school diversity is associated with white students feeling better prepared to care for diverse patients. * Compositional Diversity: proportions of URM students and non-white, non-URM students Interactional Diversity: climate for interracial interaction, individual exposure to diverse perspectives *Saha et al, Student Body Racial and Ethnic Composition and Diversity-Related Outcomes in US Medical Schools, JAMA, Sept. 10, 2008, 300(10): 1135 -1145
 OMNA Future Priorities Support TRPMMN and other regional mentorship networks n Psychiatrists Back To School n Aspiring Psychiatrists n Community of Scholars, national network of minority psychiatry faculty and mentors n Collaborate with APA district branches and a variety of educational and ethnic medical and psychiatric associations to foster diversity, recruitment, retention, advancement and leadership n
OMNA Future Priorities Support TRPMMN and other regional mentorship networks n Psychiatrists Back To School n Aspiring Psychiatrists n Community of Scholars, national network of minority psychiatry faculty and mentors n Collaborate with APA district branches and a variety of educational and ethnic medical and psychiatric associations to foster diversity, recruitment, retention, advancement and leadership n
 What can you do to eliminate disparities? n Know your population Demographics n Socio-environmental conditions n Epidemiologic vulnerabilities n Know yourself (challenge your biases) n Listen to your patients and make a concerted effort to understand cultural context and belief system n
What can you do to eliminate disparities? n Know your population Demographics n Socio-environmental conditions n Epidemiologic vulnerabilities n Know yourself (challenge your biases) n Listen to your patients and make a concerted effort to understand cultural context and belief system n
 What can you do to eliminate disparities? Notice patterns of health care delivery and question differences in quality by race, ethnicity and linguistic background n Collect data by race and ethnicity (or encourage your institution to) in order to uncover disparities in care n Educate your patients about what their illness is, what to do to manage it, and why it is important (health literacy) n
What can you do to eliminate disparities? Notice patterns of health care delivery and question differences in quality by race, ethnicity and linguistic background n Collect data by race and ethnicity (or encourage your institution to) in order to uncover disparities in care n Educate your patients about what their illness is, what to do to manage it, and why it is important (health literacy) n
 What can you do to eliminate disparities? Treat your patients like they want to be treated. Look for the commonalities that arise from sheer humanity n Encourage patients to ask questions and be active participants in their health care n Showing patients you care engenders trust, regardless of differences n Trust is key to establishing an effective patient–health professional partnership n
What can you do to eliminate disparities? Treat your patients like they want to be treated. Look for the commonalities that arise from sheer humanity n Encourage patients to ask questions and be active participants in their health care n Showing patients you care engenders trust, regardless of differences n Trust is key to establishing an effective patient–health professional partnership n
 Crossing the Quality Chasm: A New Health System for the 21 st Century Six Aims for Improvement Safe n Effective n Patient-centered n Timely n Efficient n Equitable n IOM, 2001
Crossing the Quality Chasm: A New Health System for the 21 st Century Six Aims for Improvement Safe n Effective n Patient-centered n Timely n Efficient n Equitable n IOM, 2001
 Patient-centered Care Providing care that is respectful of and responsive to individual patient preferences, needs, and values, and ensuring that patient values guide all clinical decisions.
Patient-centered Care Providing care that is respectful of and responsive to individual patient preferences, needs, and values, and ensuring that patient values guide all clinical decisions.
 Person-centered Care Healthcare partnership among practitioners, patients, and their families to ensure that decisions respond to and respect patients' wants, needs, and preferences and solicit patients' input on the education and support they need to make decisions and participate in their own care. (Adapted from Agency for Healthcare Research and Quality, 2002) Six dimensions of person-centered care: 1. Respect for patient’s values, preferences, and expressed needs 2. Coordination and integration of care 3. Information, communication, and education 4. Physical comfort 5. Emotional support 6. Involvement of family and friends (Gerteis et al, 1993)
Person-centered Care Healthcare partnership among practitioners, patients, and their families to ensure that decisions respond to and respect patients' wants, needs, and preferences and solicit patients' input on the education and support they need to make decisions and participate in their own care. (Adapted from Agency for Healthcare Research and Quality, 2002) Six dimensions of person-centered care: 1. Respect for patient’s values, preferences, and expressed needs 2. Coordination and integration of care 3. Information, communication, and education 4. Physical comfort 5. Emotional support 6. Involvement of family and friends (Gerteis et al, 1993)
 Recovery-oriented Care “Mental health recovery is a journey of healing and transformation enabling a person with a mental health problem to live a meaningful life in a community of his or her choice while striving to achieve his or her full potential. ” (SAMHSA Consensus Statement, 2006) It is important to convey a sense of hope that this is achievable for all Americans with mental health needs.
Recovery-oriented Care “Mental health recovery is a journey of healing and transformation enabling a person with a mental health problem to live a meaningful life in a community of his or her choice while striving to achieve his or her full potential. ” (SAMHSA Consensus Statement, 2006) It is important to convey a sense of hope that this is achievable for all Americans with mental health needs.


