0f7ff323905fd7ebc8db944ecafe1805.ppt
- Количество слайдов: 77

Disease Management Megatrends: State-of-the-Industry 2008 and Beyond Delivering on promises. . . January 2008 Vince Kuraitis JD, MBA Better Health Technologies, LLC www. e-Care. Management. com blog (208) 395 -1197 1

9 Chronic Disease Management Megatrends ü MAGNITUDE: We are just scratching the surface of chronic disease challenges. ü INTEGRATION: The 50 year tide is shifting toward integration, away from specialization. ü MEDICARE: While Medicare has endorsed the need for chronic disease management, disappointing results from recent demo projects make future direction unclear. ü PROVIDERS: Care providers have woken up to DM opportunities and threats; they are promoting the Chronic Care Model and the medical home. ü MAKE, ASSEMBLE, BUY? Fewer are buying as health management becomes increasingly strategic. ü TECHNOLOGY: DM in your home and your pocket. ü BEHAVIOR CHANGE: DM is moving from a medical to a social model; behavior change has become the Holy Grail. ü CLINICAL AND ECONOMIC ROI: Round one is over, DM wins; Round 2 has just begun. ü WILDCARDS! 2 © www. bhtinfo. com

This presentation. . . • . . . is a synthesis of major trends affecting disease/care management • . . . is continually updated. Look for in the upper left corner as a guide to significant changes since the January 2007 version. • . . . reflects the evolution of trends. Since early 2007 the wording of the megatrends relating to Medicare and Providers has changed significantly • Note: items with blue outlining are hyperlinked to original sources, e. g. , 3 © www. bhtinfo. com

MAGNITUDE: We are just scratching the surface of chronic disease challenges. 4 © www. bhtinfo. com

The Big Picture 5 © www. bhtinfo. com

Despite Efforts to Date, the Chronic Care Challenge is Growing • Over the next 10 years, the global incidence of chronic disease is predicted to increase by 17%, further fueling the global burden of disease. Several factors account for this driving force: – The success of modern healthcare in transforming formerly lethal diseases, injuries, and conditions (e. g. , HIV, spinal cord injuries, diabetes, tuberculosis, and multiple sclerosis) into chronic conditions that require continuous treatment; – Reductions in premature mortality and increasing longevity resulting in longer-lived chronic conditions and health-related dependencies; and – Increases in the behaviors (e. g. , unhealthy diet, physical inactivity, and tobacco use) that significantly contribute to many prevalent chronic diseases. 6 © www. bhtinfo. com

Chronic disease is gaining increasing global attention. . 7
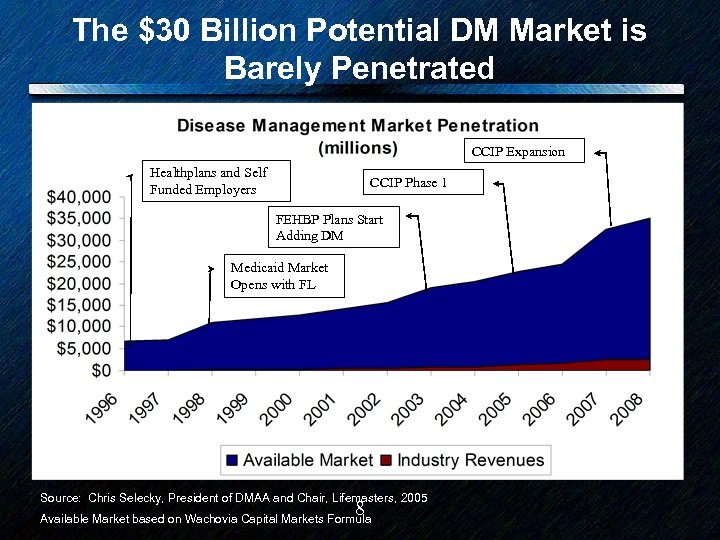
The $30 Billion Potential DM Market is Barely Penetrated CCIP Expansion Healthplans and Self Funded Employers CCIP Phase 1 FEHBP Plans Start Adding DM Medicaid Market Opens with FL Source: Chris Selecky, President of DMAA and Chair, Lifemasters, 2005 8 Available Market based on Wachovia Capital Markets Formula

• Is a $30+ Billion DM market projection realistic? ? ? • DM’s primary economic value proposition comes from avoiding hospital and ER costs. – CMS projects that U. S. hospital costs in 2015 will be $1. 1 Trillion (not a typo). – Q. What’s $30 B as a percentage of $1. 1 T? – A. 2. 7% • You decide. 9 © www. bhtinfo. com

INTEGRATION: The 50 year tide is shifting toward integration, away from specialization. 10 © www. bhtinfo. com

There are Multiple Dimensions to “Integration” • Information and communication technologies (ICT) – Interoperability – Transportability – Convergence of devices • Local care provider integration (especially physicians) • Physical health and mental health • Etc. 11 © www. bhtinfo. com

To Date DM Clinical/Business Models Have Emphasized Specialization • Specialized companies providing services • Specialized contracting/financing model -- guaranteed savings • Specialized focus on individual diseases (migrating toward multiple comorbid conditions) • Specialized technologies: predictive modeling, call centers, medical management workflow software, etc. • Specialized delivery models are developing for unique customers – Managed Care Organizations • • • – Special Needs Plans – Specialty pharma – State high-risk pools – Multiple diseases – Comorbid patients – Highest cost/risk patients – etc. , etc. HMOs PPOs other – Medicaid (in various flavors) – Medicare – Employers 12 © www. bhtinfo. com
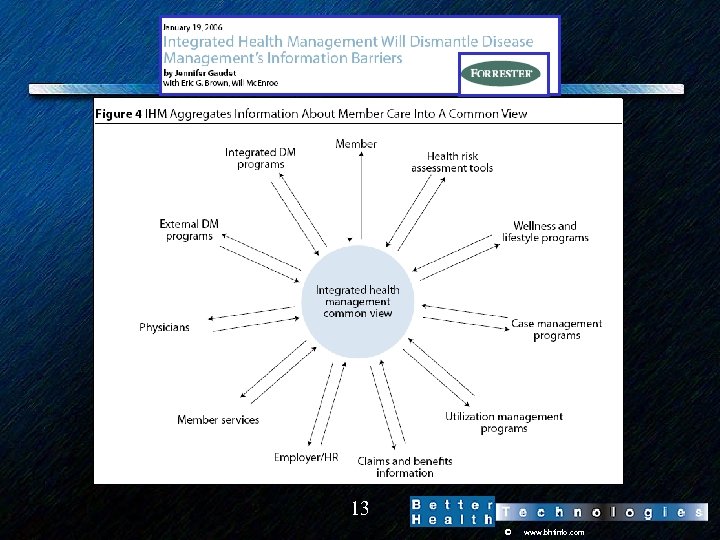
13 © www. bhtinfo. com
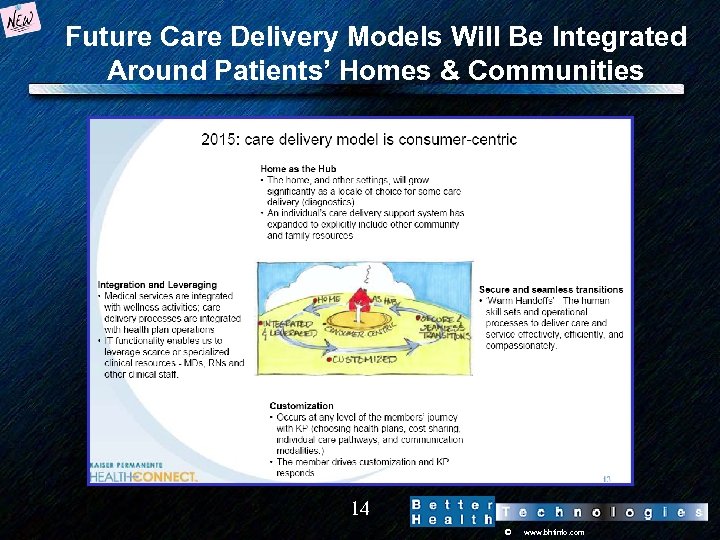
Future Care Delivery Models Will Be Integrated Around Patients’ Homes & Communities 14 © www. bhtinfo. com

MEDICARE: While Medicare has endorsed the need for chronic disease management, disappointing results from recent demo projects make future direction unclear. The Event-of-the-Decade for DM 15 © www. bhtinfo. com
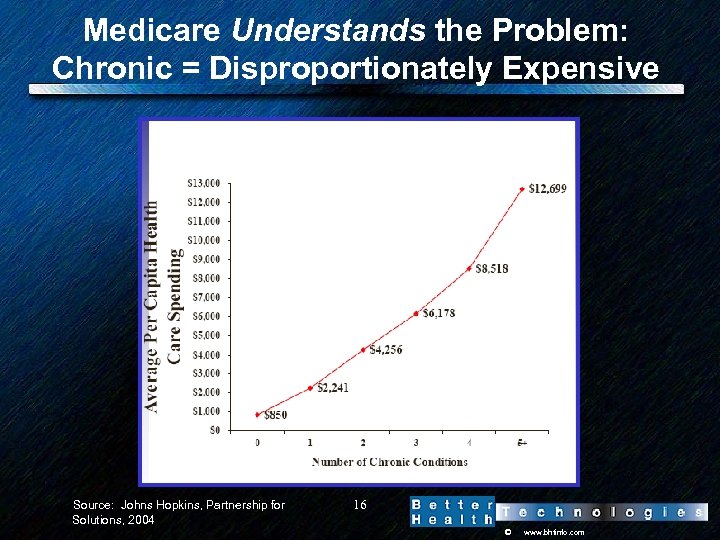
Medicare Understands the Problem: Chronic = Disproportionately Expensive Source: Johns Hopkins, Partnership for 16 Solutions, 2004 © www. bhtinfo. com

Medicare DM Demos: Little Evidence of Success • Medicare Health Support (MHS) appeared to be the favorite son demo to expand DM into Medicare – MHS has attracted worldwide attention – Legislation requires roll out if successful • Elements of MHS model • – Focus on highest cost/risk population (frail elderly) – Disease management -- carve out to private companies & health plans ( vs. CCM) – Guaranteed 5% savings business model – Short term ROI – Randomized control trial Results to-date: little evidence of success. See First “Official” Report on Medicare Health Support DM Pilot Finds Virtually No Evidence of Success, Disease Management and the Medicare Health Support (MHS) Project: “Houston, we have a problem. ” 17 © www. bhtinfo. com

Early MHS Results Are Not Encouraging • • • First, although the intervention and comparison groups are similar at randomization, our analyses reveal that an unexpected pattern in PBPM differences between intervention and comparison groups emerges between the time of randomization and the start of the MHS pilots. Second, participating beneficiaries tend to be a healthier and less costly subset of the intervention group. Thus, high participation rates will likely be a factor in the ability of the MHSOs to impact their assigned intervention populations. And, Third, fees paid to date far exceed any savings produced. The negotiated MHSO monthly fees are a much higher percentage of the comparison groups’ PBPMs than the percentage savings on payments through the first 6 -month pilot period. Fees negotiated by the MHSOs with CMS have not been covered by reductions in Medicare expenditures, let alone an additional 5% savings in Medicare payments. Without a substantial reduction in each MHSO’s monthly fee, budget neutrality after the first year is questionable. Source: RTI International Report to Congress: Evaluation of Phase I of Medicare Health Support (Formerly Voluntary Chronic Care Improvement) Pilot Program Under Traditional Fee-for-Service Medicare, June 2007 18 © www. bhtinfo. com

Findings from Four Demonstrations • No effects on adherence or self-care • Only 3 of the 20 programs reduced hospitalizations or gross costs (4. 5% reduction in MCC admissions) – Another had effects for CHF subgroup in urban counties • No effects on mortality • Scattered modest effects on quality indicators: – CHF: MCC reduced preventable hospitalizations – Diabetes: Telemedicine improved Hb. A 1 c, cholesterol, blood pressure; MCC reduced preventable hospitalizations • Patients love the programs 19 © www. bhtinfo. com

Why Doesn’t DM Work Better? • Changing patient and provider behavior is HARD: – Limited use of behavior change models – No incentive for physicians to communicate • Some patients too ill, others not at short-run risk: – But targeting is not the major problem • Programs don’t collect timely hospitalization and Rx info • Usual care providers are minimally engaged 20 © www. bhtinfo. com

Why Doesn’t DM Work Better? • Programs led by marketers, not clinical experts: – Ineffective use of available data – Unfamiliar with unique needs of the elderly • Contact info poor in population-based models • Improvements in quality of care don’t guarantee better patient outcomes in short run 21 © www. bhtinfo. com

CMS’ Take on Medicare DM Demos Source: Linda Magno, CMS, presenting at the Patient Centered Primary Care Collaborative Summit, November 2007 22 © www. bhtinfo. com

Many Other CMS Demo/Pilot Projects Involve Patients With Chronic Diseases • Medicare is undertaking a wide range of demonstration/pilot projects • Many directly involve patients with chronic conditions – – – Physician Group Practice (PGP) Care Management for High Cost Beneficiaries (CMHCB) Special Needs Plans (SNP) Medicare Medical Home demonstration (discussed later) and others 23 © www. bhtinfo. com

What are some of Medicare’s other options toward an optimal chronic care management program? • • From: a guaranteed 5% savings business model To: considering many alternative payment mechanisms: capitation, shared savings, payfor-performance, and/or fee-for-service DM. • • From: focusing on short-term ROI To: focusing on medium-long term ROI, quality improvement & compression of morbidity • • From: DM carve outs to private companies & health plans To: exploring options to re-integrate care providers into care management processes, e. g. , the Chronic Care Model, the Medical Home model or a managed care model (e. g. utilization review, case management, pre-certification, etc. ). • • From: focusing on high-risk, chronic, co-morbid patients To: including programs to address mainstream Medicare patients with prevention and population health approaches • • From: rigid implementation of inflexible program structures To: Rapid Learning Models. Open up the data, while protecting for personal identification, to all “qualified” people to learn what can be learned in a timely fashion. The process should be transparent and open and available to the taxpayers who have funded these demonstrations. • • From: is MHS working as originally designed? To: what’s the optimal chronic care management program, financing structure, and evaluation model for Medicare? 24

PROVIDERS: Care providers have woken up to DM opportunities and threats; they are promoting the Chronic Care Model and the medical home. 25 © www. bhtinfo. com

Model #1: Disease Management Model • • Medium sized, privately & publicly held companies $2 billion revenues in 2007 (Source: DMPC) Payers are increasingly assembling DM components Key elements – Telephonic services, centralized call centers • Support patient life style change • Promote evidence based practice – Started as carve-out model – Guaranteed savings promoted by DMPC – Focusing on highest cost, highest risk patients • Challenges: physician buy-in, proprietary IT • Major players: 26 © www. bhtinfo. com

Model #2: Chronic Care Model • Pioneered at Group Health Cooperative • Key elements – Community based – Transformation of health care – Restructuring of physician practice • Challenges: no reimbursement, academic/research focus • Protagonists: 27
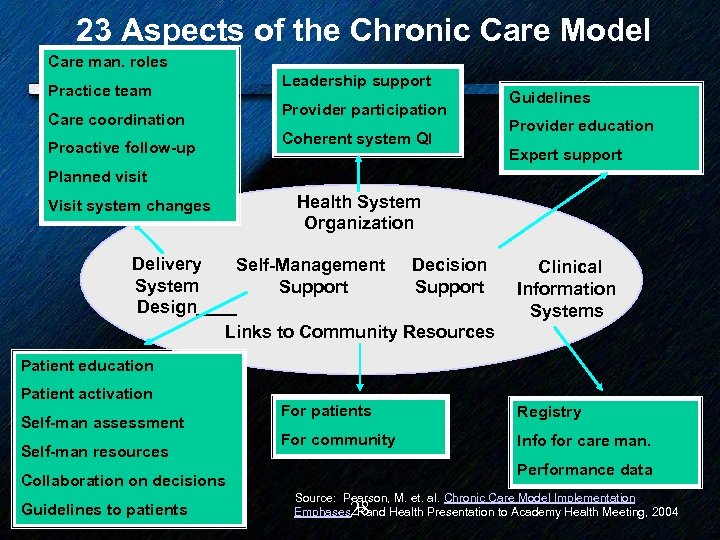
23 Aspects of the Chronic Care Model Care man. roles Practice team Care coordination Proactive follow-up Leadership support Provider participation Coherent system QI Guidelines Provider education Expert support Planned visit Visit system changes Health System Organization Delivery Self-Management Decision System Support Design Links to Community Resources Clinical Information Systems Patient education Patient activation Self-man assessment Self-man resources For patients Registry For community Info for care man. Performance data Collaboration on decisions Guidelines to patients Source: Pearson, M. et. al. Chronic Care Model Implementation Emphases, Rand Health Presentation to Academy Health Meeting, 2004 28

Who Wrote This Statement? “The literature has correctly indicated that the term ‘care coordination’, which is often used interchangeably with the term ‘care management, ’ refers to a variety of activities. – managing the transition of care across settings – use of patient registries to allow for population-based care protocols, the – use of frequent follow-up with patients to promote treatment plan compliance and to obtain healthcare data – use of clinical practice guidelines, including feedback to the physician regarding their degree of compliance with the guidelines – teaching of disease self-management skills to patients. . ” 29 © www. bhtinfo. com

• Was it written by a DM company? a home health agency? a health plan? • No, it was written by. . . doctors! – Source: American College of Physicians Position Paper, Reform of the Dysfunctional Healthcare Payment and Delivery System, April 2006 • . . . and here's the punch line: “These care coordination activities are at the core of what defines a primary care physician. ” 30 © www. bhtinfo. com

The Cats are Herding: the Medical Home Model is Gaining Momentum With Physicians. . . 31 © www. bhtinfo. com

. . . and Congress. . . • December 2006 – Congresses passed the Medicare Medical Home Demonstration (MMHD) • MMHD similarity to MHS: high cost, chronic patients; multiple comorbidities • MMHD differences from MHS – No requirement of 5% guaranteed savings – Physicians can keep 80% of savings • An RFP for the MMHD will be issued early in 2008 32 © www. bhtinfo. com

. . . and payers. . 33 © www. bhtinfo. com

. . . but there are many details to work out and questions to address. • How will a MH be defined, recognized (e. g. , see NCQA’s program), and measured? • What should payment levels be for the MH? • Will physicians invest time and $$ to participate? • Will physicians change behavior and workflow? • Will physicians want to collaborate with payers? • Will the Medicare Medical Home Demo be successful? • Will other pilot projects prove successful? 34 © www. bhtinfo. com

The Medical Home Model – Paying for Technology and Process Improvement • Proposed payment framework for the medical home model includes $$ for: – – coordination of care health information technology secure e-mail and telephone consultation; remote monitoring of clinical data using technology. 35 © www. bhtinfo. com

MAKE, ASSEMBLE, BUY? Fewer are buying as health management becomes increasingly strategic. 36 © www. bhtinfo. com

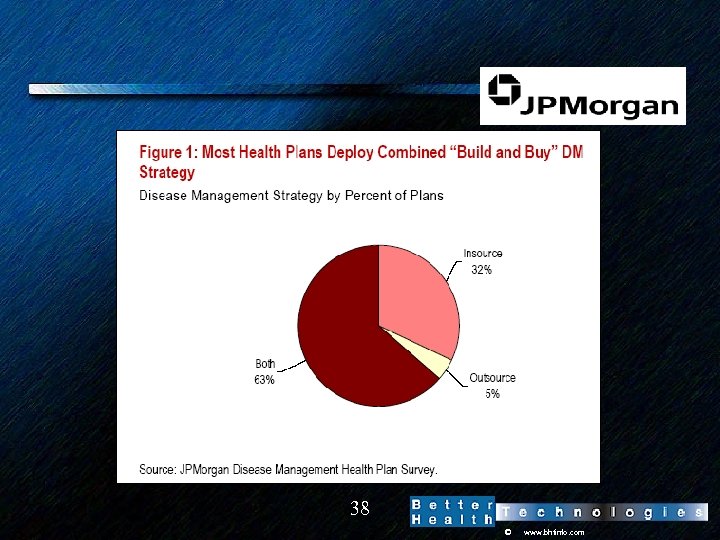
Health Plan Views Of the DM Make/Buy/Assemble Decision Have Evolved • 7 years ago – – "DM is really complicated" "It will take us 18 months to get started" "Start up cost are significant“ “Let’s buy” • Today – "DM isn't rocket science; we've learned from the vendors" – "Care management is increasingly strategic; it is a core competency that we need to do ourselves" – "We'll get better integration if we do it ourselves; medical management workflow software is key” – “We need to assemble DM components and make sure that we keep control over key leverage points” 37 © www. bhtinfo. com
38 © www. bhtinfo. com

Health Plans Moving From ‘Buy’ to ‘Build’ DM Model Disease Management News, September 25, 2006 39 © www. bhtinfo. com

Is the Trend Toward “Assembling” a Major Threat to DM Companies? • Not really. • Remember. . . the market potential for DM is $30+ Billion. There’s a lot of growth to go around. 40 © www. bhtinfo. com

TECHNOLOGY: DM in your home and your pocket. Health care anywhere. 41 © www. bhtinfo. com

Tech Megatrends A. B. C. D. E. The Full Rollout of DM Technology Will Take Time Technologies are Converging The Healthcare Unbound Market Opportunity Is Huge (Forrester) 2008 Could Be A Breakout Year for Remote Patient Monitoring Watch for New Platforms Facilitating Interoperability & Transportability • • Personal Health Records (PHRs) Corporate efforts – Microsoft Health. Vault, Google Health, Dossia Mobile/wireless apps Hospital At Home F. Next Generation Technology – “You Ain’t Seen Nothing Yet” G. Will The DM Community Be Leaders Or Laggards In the March toward Interoperability? 42 © www. bhtinfo. com

A) The Full Rollout of DM Technology Will Take Time Do the Math. Diseases/conditions x Value propositions x Technologies x User environments = Thousands of Potential Applications 43 © www. bhtinfo. com
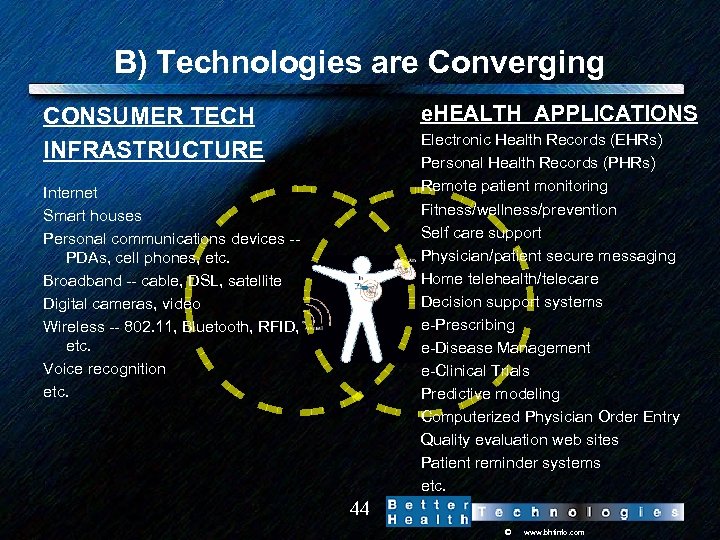
B) Technologies are Converging e. HEALTH APPLICATIONS CONSUMER TECH INFRASTRUCTURE Electronic Health Records (EHRs) Personal Health Records (PHRs) Remote patient monitoring Fitness/wellness/prevention Self care support Physician/patient secure messaging Home telehealth/telecare Decision support systems e-Prescribing e-Disease Management e-Clinical Trials Predictive modeling Computerized Physician Order Entry Quality evaluation web sites Patient reminder systems etc. Internet Smart houses Personal communications devices -- PDAs, cell phones, etc. Broadband -- cable, DSL, satellite Digital cameras, video Wireless -- 802. 11, Bluetooth, RFID, etc. Voice recognition etc. 44 © www. bhtinfo. com

Focal Points for Convergence Home Networks, Smart Phones, EHRs CONSUMER e. HEALTH Home Network PHR/ EHR Smart Phone 45 © www. bhtinfo. com
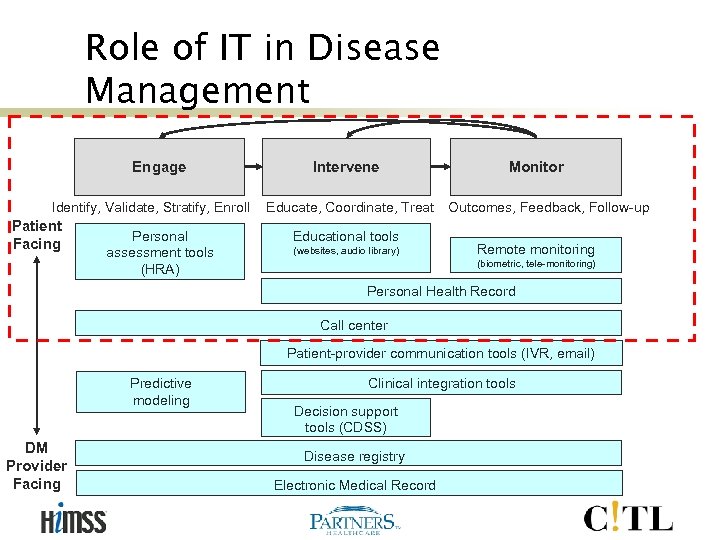
Role of IT in Disease Management Engage Intervene Identify, Validate, Stratify, Enroll Educate, Coordinate, Treat Patient Facing Personal assessment tools (HRA) Educational tools (websites, audio library) Monitor Outcomes, Feedback, Follow-up Remote monitoring (biometric, tele-monitoring) Personal Health Record Call center Patient-provider communication tools (IVR, email) Predictive modeling DM Provider Facing Clinical integration tools Decision support tools (CDSS) Disease registry Electronic Medical Record
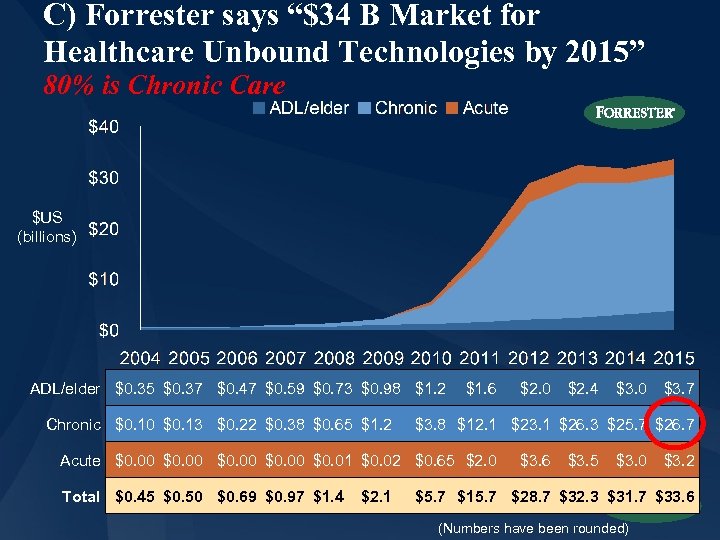
C) Forrester says “$34 B Market for Healthcare Unbound Technologies by 2015” 80% is Chronic Care $US (billions) ADL/elder $0. 35 $0. 37 $0. 47 $0. 59 $0. 73 $0. 98 $1. 2 Chronic $0. 10 $0. 13 $0. 22 $0. 38 $0. 65 $1. 2 $1. 6 $2. 1 $2. 4 $3. 0 $3. 7 $3. 8 $12. 1 $23. 1 $26. 3 $25. 7 $26. 7 Acute $0. 00 $0. 01 $0. 02 $0. 65 $2. 0 Total $0. 45 $0. 50 $0. 69 $0. 97 $1. 4 $2. 0 $3. 6 $3. 5 $3. 0 $3. 2 $5. 7 $15. 7 $28. 7 $32. 3 $31. 7 $33. 6 (Numbers have been rounded)

D) 2008 Could Be A Breakthrough Year For RPM • Continua begins to address major challenges – Interoperability of devices – Pricing (indirectly) • But other challenges remain – IT/integration – Reimbursement/business model – Licensure/regulatory issues 48 © www. bhtinfo. com

Promoters 49

The Multiparameter Remote Patient Monitoring (RPM) Market is Migrating. . . • From – High unit prices rooted in the industry's early focus on medical device markets and business models – Proprietary devices, proprietary IT, non-interoperable data – Low unit volume, moderate margins per unit – Competition based on vendor lock-in through high switching costs • To: – Low unit prices as the technology evolves toward consumer markets and consumer business models – Intereroperable devices, common IT platforms, and interoperable data – High unit volume, low margins per unit – Competition based on value-adds and service 50 © www. bhtinfo. com

. . . but Consider the Systemic Barriers • • Reimbursement HIPAA: Privacy/confidentiality issues Physician workflow Technology maturity – – Infrastructure Bandwidth Interoperability/Standards Friendly user interfaces 51 © www. bhtinfo. com

E) Watch for New Platforms and Networks Facilitating Interoperability & Transportability of Personal Health Information “The sine qua non is sharing data” Adam Bosworth, former director of Google Health • Personal Health Records • Corporate efforts – Microsoft Health Vault, Google Health, Dossia • Mobile/Wireless Applications • Hospital at Home 52 © www. bhtinfo. com

PHR Background • 2 models of PHRs – Stand alone – Tethered: typically to a health plan, provider, employer • • Each has challenges The “populating the PHR with data” problem 200 PHRs on the market Generations of PHRs – 1 st generation: PHR as “APPLICATION” -- an online repository of personal health information (PHI) – Next generation – PHR as PLATFORM 53 © www. bhtinfo. com
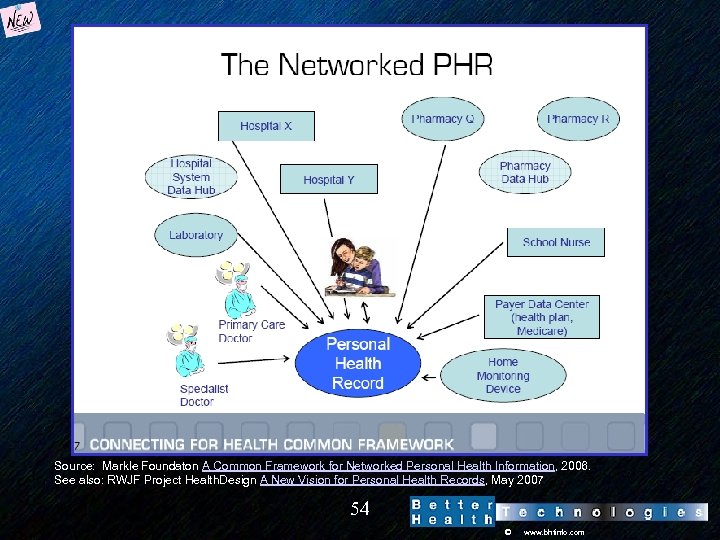
Source: Markle Foundaton A Common Framework for Networked Personal Health Information, 2006. See also: RWJF Project Health. Design A New Vision for Personal Health Records, May 2007 54 © www. bhtinfo. com
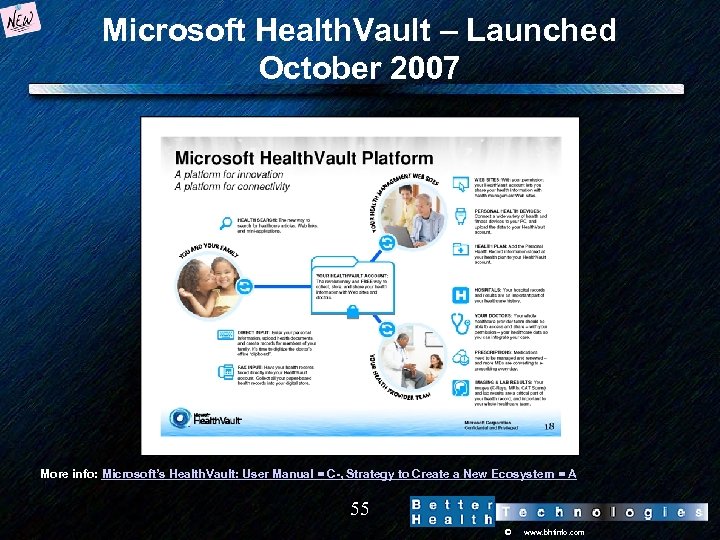
Microsoft Health. Vault – Launched October 2007 More info: Microsoft’s Health. Vault: User Manual = C-, Strategy to Create a New Ecosystem = A 55 © www. bhtinfo. com
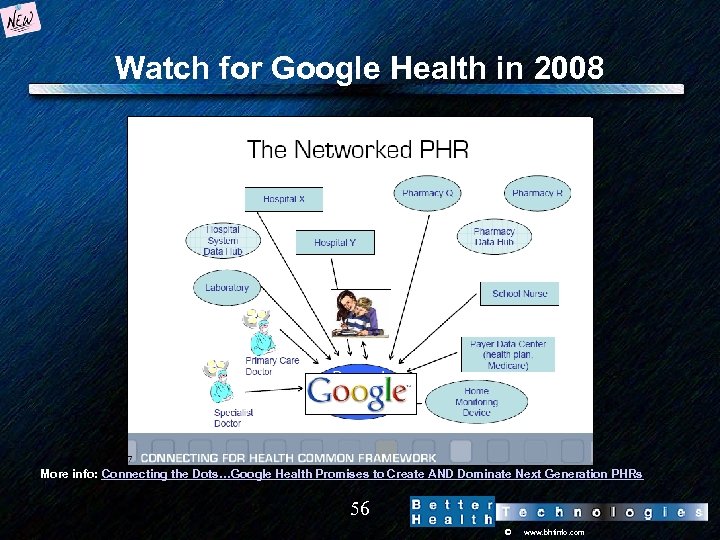
Watch for Google Health in 2008 More info: Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs 56 © www. bhtinfo. com

Watch for QUALCOMM’s Mobile Platform (Life. Comm) in 2008 More info: Disease Management Going Mobile & Retail: QUALCOMM’s Health Care MVNO 57 © www. bhtinfo. com

The Value Proposition of Mobile Technology for DM is Huge! Chronic Disease/Condition Management is migrating – From a clinical based model – Toward a behavior change model How can you optimize behavior change without 24 x 7 x 365 connectivity to the patient? 58 © www. bhtinfo. com

Hospital at Home (HAH) Dates Back to the 1960 s – Almost Completely Outside the U. S. 59

The Most Significant U. S. HAH Initiative is at Johns Hopkins 60 © www. bhtinfo. com

Current Tech & Apps are a Collective Platform to Support HAH Hospital At Home • • • EHRs Telemedicine Niche apps Remote Patient Monitoring Disease Management Personal Health Records Mobile telehealth Health 2. 0 Etc 61 © www. bhtinfo. com

F) The Next Generation of DM Technology When the Technology is Just “There” “Ubiquitous Health” “Sense and Simplicity” “Pervasive Computing” 62 © www. bhtinfo. com

G) Will the DM community be leaders or laggards in the movement for health information technology interoperability? 63 © www. bhtinfo. com

BEHAVIOR CHANGE: DM is moving from a medical to a social model; behavior change has become the Holy Grail. 64 © www. bhtinfo. com
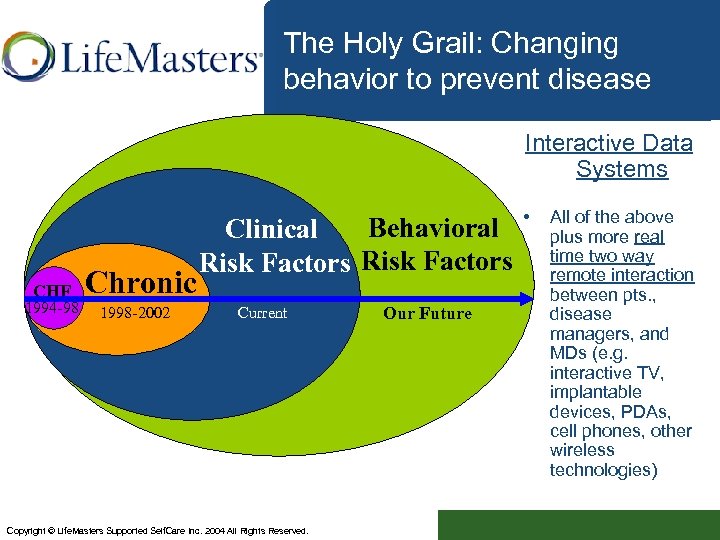
The Holy Grail: Changing behavior to prevent disease Interactive Data Systems CHF 1994 -98 Chronic 1998 -2002 Behavioral Clinical Risk Factors Current Copyright © Life. Masters Supported Self. Care Inc. 2004 All Rights Reserved. Our Future • All of the above plus more real time two way remote interaction between pts. , disease managers, and MDs (e. g. interactive TV, implantable devices, PDAs, cell phones, other wireless technologies)

Behavior Change in a Nutshell • More than 50 years of research on health behavior change has not provided us with easy answers in understanding patient nonadherence. • Despite the renewed interest in adherence research, we have a long road ahead in translating behavior change principles into practical application. • Actionable messages are critical to success. – When physicians and other health care professionals use their referent power they can be influential in patient adherence. . higher patient adherence is associated with physicians who create warm personal relationships with their patients, and work with them to address adherence and lifestyle issues. – Expanding referent power beyond physicians to patientaffiliated reference groups may be challenging to DM, but it may increase the influence of adherence messages exponentially. Source: Turpin, R. et. al. “Patient Adherence: Present State and Future Directions” Disease Management, December 2007 66 © www. bhtinfo. com

CLINICAL AND ECONOMIC ROI: Round one is over, DM wins; Round 2 has just begun. 67 © www. bhtinfo. com

The DM/ROI Debate Of the Past 10 Years Has Not Always Been Framed Constructively “DM has ROI” “No it doesn’t” “Yes it does” “No it doesn’t” “Jane, you ignorant slut” 68 © www. bhtinfo. com

Reframing the DM/ROI Debate: 2 Seemingly Contradictory Statements #1: Whether DM provides ROI has become irrelevant #2: The DM/ROI debate will continue to be scientifically evaluated for the next decade 69 © www. bhtinfo. com
#1: The DM/ROI Debate Has Become Irrelevant DM Has Gone Mainstream 70 © www. bhtinfo. com

#2: The DM/ROI Debate Will Continue To Be Scientifically Evaluated For The Next Decade Level of Proof 0 #1 No evidence #2 100 Preponderance Clear and of Convincing Evidence Beyond A Reasonable Doubt • #1 = DM today • #2 = Continuing DM ROI and outcome measurement for the future • Source: With attribution to Gordon Norman, MD, MBA, Chief Medical Officer of Alere 71 © www. bhtinfo. com Absolute Certainty

Will We Ever “Get Along” and Measure Outcomes and ROI Consistently? • In 2006, DMAA released the first volume of its long-awaited Outcomes Guidelines Report, which described industry consensus approaches to measuring financial outcomes in disease management. • In 2007, a follow-up document, the Outcomes Guidelines Report Volume II, added clinical measures. • In 2008, a third volume of the report is planned for publication. • These are significant steps. . . but don’t expect the debate AND controversy about ROI to end soon. 72 © www. bhtinfo. com

WILDCARDS! 73 © www. bhtinfo. com

Watchful Waiting. . • Will employers stay the course in supporting DM? • Can pay-for-performance P 4 P initiatives align incentives? • Will retail clinics start doing DM in a big way? • Can U. S. style DM be exported to international markets? • Will Consumer Driven Health Plans (CDHPs) be the spark to ignite a consumer model of chronic disease management? • How will the 2008 elections affect health policy? While DM has received bi-partisan support, dramatic system reforms (e. g. physician reimbursement) are possible. 74 © www. bhtinfo. com

APPENDIX A Better Health Technologies, LLC 75 © www. bhtinfo. com

Better Health Technologies, LLC • Technology and health care delivery are shifting: – From: Acute and episodic care delivered in hospitals and doctors’ offices – To: Chronic disease and condition management delivered in homes, workplaces, and communities • BHT provides consulting, business development, and speaking services to assist companies in: 1) Understanding the shift 2) Positioning – what’s the right strategy, tactics, and business model? 3) Integrating your offering into the value chain – what are the right partnerships? 76 © www. bhtinfo. com

BHT Clients Pre-IPO Companies Established organizations Pharos Innovations Health. Post Cardiobeat EZWeb Sensitron Life Navigator Medical Peace Stress Less Diabetes. Manager. com Cogni. Med Caresoft Benchmark Oncology SOS Wireless Click 4 Care e. Care Technologies The Healan Group Fitsense Elite Care Technologies Intel Digital Health Group Samsung Electronics, South Korea -- Global Research Group -- Samsung Advanced Institute of Technology -- Digital Solution Center Amedisys Medtronic -- Neurological Disease Management -- Cardiac Rhythm Patient Management Siemens Medical Solutions Philips Electronics Joslin Diabetes Center GSK Disease Management Association of America PCS Health Systems Varian Medical Systems VRI Washoe Health System S 2 Systems Corp. Health Physician IPA Centocor 77 © www. bhtinfo. com
0f7ff323905fd7ebc8db944ecafe1805.ppt