41c173be93a97c47c56df99ff6eae537.ppt
- Количество слайдов: 36
 Diagnosing and Managing Asthma in Children LARRY S. POSNER M. D. Associate Clinical Professor of Pediatrics, UCSF Principal, North Bay Allergy and Asthma Associates
Diagnosing and Managing Asthma in Children LARRY S. POSNER M. D. Associate Clinical Professor of Pediatrics, UCSF Principal, North Bay Allergy and Asthma Associates
 Asthma Is Prevalent: Significant Morbidity and Mortality 32. 6 Million People Have Had an Asthma Diagnosis in Their Lifetime 22. 2 Million People Are Currently Diagnosed With Asthma 12. 2 Million People Suffer From Asthma Attacks Annually Approximately 4000 Asthma. Related Deaths Occur Annually Approximately 11 People Die From Asthma Each Day Available at: http: //www. cdc. gov/nchs/products/pubd/hestats/asthma. htm. Accessed March 12, 2007.
Asthma Is Prevalent: Significant Morbidity and Mortality 32. 6 Million People Have Had an Asthma Diagnosis in Their Lifetime 22. 2 Million People Are Currently Diagnosed With Asthma 12. 2 Million People Suffer From Asthma Attacks Annually Approximately 4000 Asthma. Related Deaths Occur Annually Approximately 11 People Die From Asthma Each Day Available at: http: //www. cdc. gov/nchs/products/pubd/hestats/asthma. htm. Accessed March 12, 2007.
 Pediatric Asthma: Facts and Figures • Asthma is the most common chronic disorder in children and adolescents 1 • Asthma is a leading cause of school absences, resulting in 14 million missed school days a year 2 1. American Academy of Allergy, Asthma, and Immunology, Inc. , 1999. 2. Mannino DM, et al. MMWR Morb Mortal Wkly Rep. March 29, 2002; 51(SS 01); 1 -13.
Pediatric Asthma: Facts and Figures • Asthma is the most common chronic disorder in children and adolescents 1 • Asthma is a leading cause of school absences, resulting in 14 million missed school days a year 2 1. American Academy of Allergy, Asthma, and Immunology, Inc. , 1999. 2. Mannino DM, et al. MMWR Morb Mortal Wkly Rep. March 29, 2002; 51(SS 01); 1 -13.
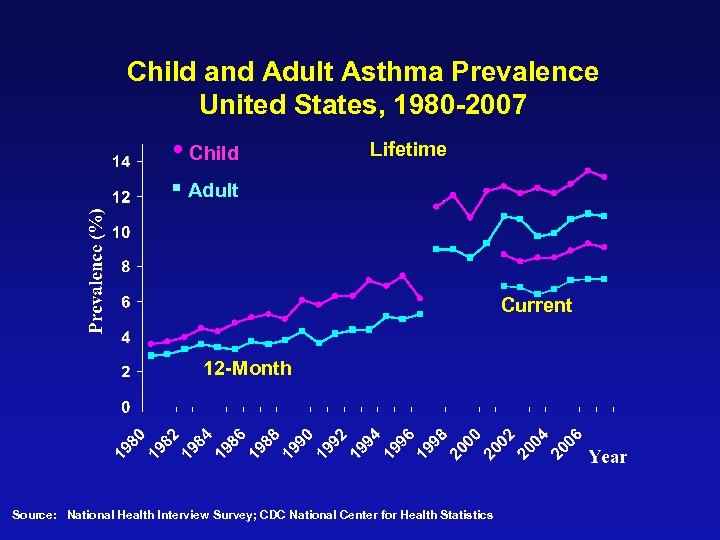 Child and Adult Asthma Prevalence United States, 1980 -2007 • Child Lifetime § Adult Current 12 -Month Source: National Health Interview Survey; CDC National Center for Health Statistics
Child and Adult Asthma Prevalence United States, 1980 -2007 • Child Lifetime § Adult Current 12 -Month Source: National Health Interview Survey; CDC National Center for Health Statistics
 Asthma Trends A child born a generation from now is twice as likely to develop asthma as one born today
Asthma Trends A child born a generation from now is twice as likely to develop asthma as one born today
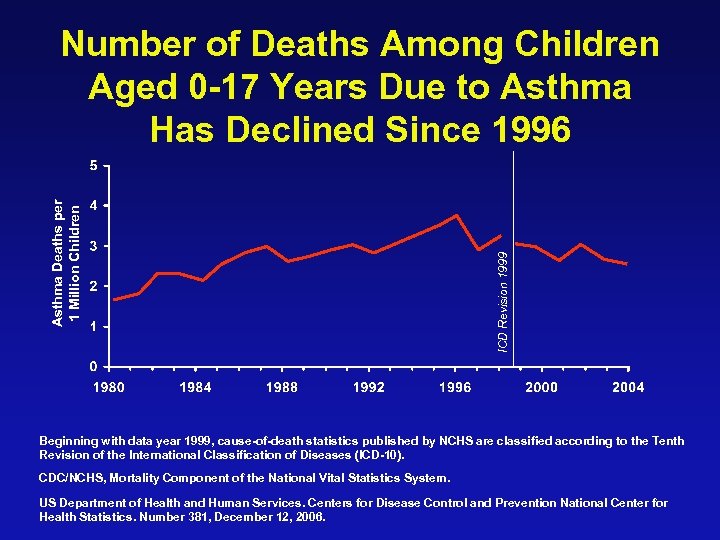 ICD Revision 1999 Asthma Deaths per 1 Million Children Number of Deaths Among Children Aged 0 -17 Years Due to Asthma Has Declined Since 1996 Beginning with data year 1999, cause-of-death statistics published by NCHS are classified according to the Tenth Revision of the International Classification of Diseases (ICD-10). CDC/NCHS, Mortality Component of the National Vital Statistics System. US Department of Health and Human Services. Centers for Disease Control and Prevention National Center for Health Statistics. Number 381, December 12, 2006.
ICD Revision 1999 Asthma Deaths per 1 Million Children Number of Deaths Among Children Aged 0 -17 Years Due to Asthma Has Declined Since 1996 Beginning with data year 1999, cause-of-death statistics published by NCHS are classified according to the Tenth Revision of the International Classification of Diseases (ICD-10). CDC/NCHS, Mortality Component of the National Vital Statistics System. US Department of Health and Human Services. Centers for Disease Control and Prevention National Center for Health Statistics. Number 381, December 12, 2006.
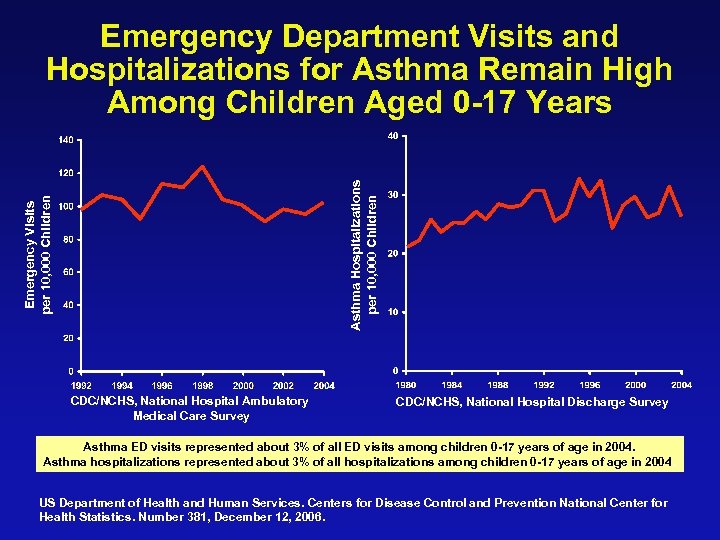 Emergency Visits per 10, 000 Children Asthma Hospitalizations per 10, 000 Children Emergency Department Visits and Hospitalizations for Asthma Remain High Among Children Aged 0 -17 Years CDC/NCHS, National Hospital Ambulatory Medical Care Survey CDC/NCHS, National Hospital Discharge Survey Asthma ED visits represented about 3% of all ED visits among children 0 -17 years of age in 2004. Asthma hospitalizations represented about 3% of all hospitalizations among children 0 -17 years of age in 2004. US Department of Health and Human Services. Centers for Disease Control and Prevention National Center for Health Statistics. Number 381, December 12, 2006.
Emergency Visits per 10, 000 Children Asthma Hospitalizations per 10, 000 Children Emergency Department Visits and Hospitalizations for Asthma Remain High Among Children Aged 0 -17 Years CDC/NCHS, National Hospital Ambulatory Medical Care Survey CDC/NCHS, National Hospital Discharge Survey Asthma ED visits represented about 3% of all ED visits among children 0 -17 years of age in 2004. Asthma hospitalizations represented about 3% of all hospitalizations among children 0 -17 years of age in 2004. US Department of Health and Human Services. Centers for Disease Control and Prevention National Center for Health Statistics. Number 381, December 12, 2006.
 Are Children With Asthma Achieving the NIH Goals of Therapy?
Are Children With Asthma Achieving the NIH Goals of Therapy?
 Where Should We Start NIH Goals of Asthma Therapy • Minimal or no chronic symptoms day or night • Minimal or no exacerbations • No limitations on activities; no missed school/work • Maintain (near) normal pulmonary function • Minimal use of inhaled short-acting beta 2 - agonists • Minimal or no adverse effects from medications Guidelines for the Diagnosis and Management of Asthma—Update on Selected Topics 2002. NIH, NHLBI. May 2003 (reprint). NIH publication 02 -5075.
Where Should We Start NIH Goals of Asthma Therapy • Minimal or no chronic symptoms day or night • Minimal or no exacerbations • No limitations on activities; no missed school/work • Maintain (near) normal pulmonary function • Minimal use of inhaled short-acting beta 2 - agonists • Minimal or no adverse effects from medications Guidelines for the Diagnosis and Management of Asthma—Update on Selected Topics 2002. NIH, NHLBI. May 2003 (reprint). NIH publication 02 -5075.
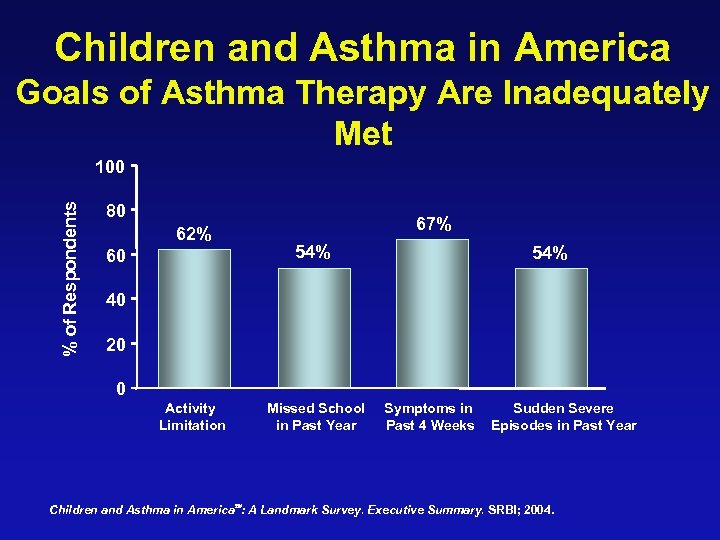 Children and Asthma in America Goals of Asthma Therapy Are Inadequately Met % of Respondents 100 80 62% 60 67% 54% 40 20 0 Activity Limitation Missed School in Past Year Symptoms in Past 4 Weeks Sudden Severe Episodes in Past Year Children and Asthma in America : A Landmark Survey. Executive Summary. SRBI; 2004.
Children and Asthma in America Goals of Asthma Therapy Are Inadequately Met % of Respondents 100 80 62% 60 67% 54% 40 20 0 Activity Limitation Missed School in Past Year Symptoms in Past 4 Weeks Sudden Severe Episodes in Past Year Children and Asthma in America : A Landmark Survey. Executive Summary. SRBI; 2004.
 Children and Asthma in America Parent-Child Gap in Perception of Asthma Symptoms in the Past 4 Weeks 68% 70% 60% % of Respondents 60% 50% Parents Children (10 -15) 50% 44% 40% 27% 26% 30% 20% 10% 0% During Day During Exercise During Night Children and Asthma in America : A Landmark Survey. Executive Summary. SRBI; 2004.
Children and Asthma in America Parent-Child Gap in Perception of Asthma Symptoms in the Past 4 Weeks 68% 70% 60% % of Respondents 60% 50% Parents Children (10 -15) 50% 44% 40% 27% 26% 30% 20% 10% 0% During Day During Exercise During Night Children and Asthma in America : A Landmark Survey. Executive Summary. SRBI; 2004.
 Children and Asthma in America • Many children with asthma are not achieving the NIH goals of therapy • Poorly controlled asthma has a significant impact on daily lives of children and their families • The survey highlights the need for improved asthma management Better assessment and treatment • Proper patient and family education • Improved dialogue between the child, parents, and their clinician •
Children and Asthma in America • Many children with asthma are not achieving the NIH goals of therapy • Poorly controlled asthma has a significant impact on daily lives of children and their families • The survey highlights the need for improved asthma management Better assessment and treatment • Proper patient and family education • Improved dialogue between the child, parents, and their clinician •
 Diagnosing Asthma: Spirometry Testing of lung function is one means of diagnosing asthma.
Diagnosing Asthma: Spirometry Testing of lung function is one means of diagnosing asthma.
 Challenges in Treating Childhood Asthma n May be difficult to make a “definitive” diagnosis in very young children l Lack of objective measurement l Lack of subjective awareness of symptoms n Underdiagnosis in children of asthma is a frequent problem
Challenges in Treating Childhood Asthma n May be difficult to make a “definitive” diagnosis in very young children l Lack of objective measurement l Lack of subjective awareness of symptoms n Underdiagnosis in children of asthma is a frequent problem
 Diagnosing Asthma: Medical History • Symptoms • Coughing • Wheezing • Shortness of breath • Chest tightness • Patterns to Symptoms • Family History • Response to medication
Diagnosing Asthma: Medical History • Symptoms • Coughing • Wheezing • Shortness of breath • Chest tightness • Patterns to Symptoms • Family History • Response to medication
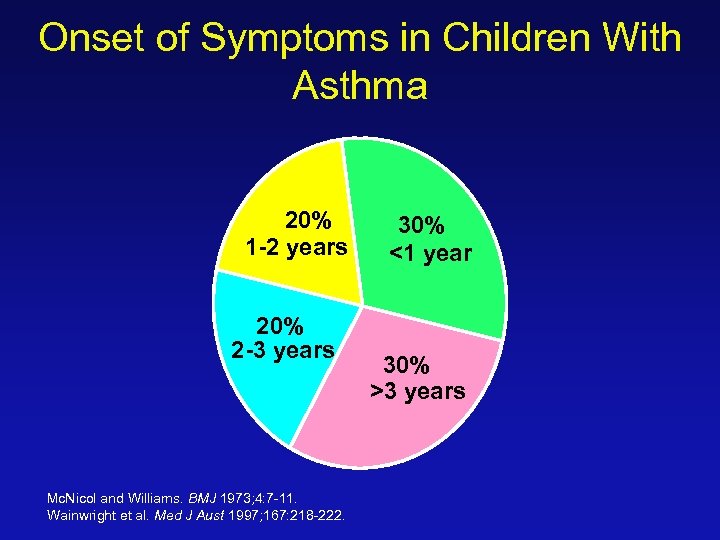 Onset of Symptoms in Children With Asthma 20% 1 -2 years 20% 2 -3 years Mc. Nicol and Williams. BMJ 1973; 4: 7 -11. Wainwright et al. Med J Aust 1997; 167: 218 -222. 30% <1 year 30% >3 years
Onset of Symptoms in Children With Asthma 20% 1 -2 years 20% 2 -3 years Mc. Nicol and Williams. BMJ 1973; 4: 7 -11. Wainwright et al. Med J Aust 1997; 167: 218 -222. 30% <1 year 30% >3 years
 Asthma is a Spectrum of Disease Mild intermittent asthma Cough/wheeze only with colds or exercise Severe persistent asthma Daily symptoms at rest
Asthma is a Spectrum of Disease Mild intermittent asthma Cough/wheeze only with colds or exercise Severe persistent asthma Daily symptoms at rest
 Precipitating / Aggravating Factors “Asthma triggers” Viral upper respiratory infections n Allergen exposure n n Exercise n Irritants (especially smoke) Weather n Strong emotion n Gastroesophageal reflux n
Precipitating / Aggravating Factors “Asthma triggers” Viral upper respiratory infections n Allergen exposure n n Exercise n Irritants (especially smoke) Weather n Strong emotion n Gastroesophageal reflux n
 Approaches to Treatment • AVOIDANCE - Environmental control • PHARMACOLOGIC THERAPY - Step therapy per NHLBI guidelines • ALLERGY IMMUNOTHERAPY
Approaches to Treatment • AVOIDANCE - Environmental control • PHARMACOLOGIC THERAPY - Step therapy per NHLBI guidelines • ALLERGY IMMUNOTHERAPY
 Avoidance • Influenza vaccination • Tobacco smoke • Fireplace smoke • Air “fresheners” • Allergens
Avoidance • Influenza vaccination • Tobacco smoke • Fireplace smoke • Air “fresheners” • Allergens
 Reducing Indoor Allergens House-Dust Mites • Essential: • • • Encase mattress/box-spring in an allergenimpermeable cover Encase pillow in an allergen-impermeable cover or wash weekly Wash sheets and blankets in hot water weekly (>130 o F is necessary for killing mites) Remove other reservoirs from the bedroom Carpet treatments unclear
Reducing Indoor Allergens House-Dust Mites • Essential: • • • Encase mattress/box-spring in an allergenimpermeable cover Encase pillow in an allergen-impermeable cover or wash weekly Wash sheets and blankets in hot water weekly (>130 o F is necessary for killing mites) Remove other reservoirs from the bedroom Carpet treatments unclear
 Cat Allergen • Major cat allergen Fel d 1 found in saliva and dander • In homes with indoor cats, 35% of allergen reservoir is continually airborne. • Dander accumulates in carpet upholstered furniture and bedding • Cat dander is an almost ubiquitous indoor allergen
Cat Allergen • Major cat allergen Fel d 1 found in saliva and dander • In homes with indoor cats, 35% of allergen reservoir is continually airborne. • Dander accumulates in carpet upholstered furniture and bedding • Cat dander is an almost ubiquitous indoor allergen
 Teach Patients To Reduce Exposure to Inhalant Allergens ANIMAL DANDER • Remove pet from house (ideal) • Keep animal out of patient’s bedroom (at a minimum) • Mattress/pillow encasements • Wipe down surfaces with a damp cloth • Portable HEPA air filtration • Keep window closed • Seal or put a filter on air ducts that lead to bedroom
Teach Patients To Reduce Exposure to Inhalant Allergens ANIMAL DANDER • Remove pet from house (ideal) • Keep animal out of patient’s bedroom (at a minimum) • Mattress/pillow encasements • Wipe down surfaces with a damp cloth • Portable HEPA air filtration • Keep window closed • Seal or put a filter on air ducts that lead to bedroom
 Pharmacotherapy
Pharmacotherapy
 Stepwise Approach to Therapy for Adults and Children: Maintaining Control STEP 4 Multiple longterm-control medications, including prednisone STEP 4 Severe Persistent STEP 3 Moderate Persistent STEP 2 Mild Persistent STEP 1 Mild Intermittent Step Down STEP 3 > 1 Long-term-control meds (Preferred low dose ICS+LABA) STEP 2 1 Long-term-control medication: anti-inflammatory (Preferred low-dose ICS) STEP 1 Quick-relief medication: PRN Step Up
Stepwise Approach to Therapy for Adults and Children: Maintaining Control STEP 4 Multiple longterm-control medications, including prednisone STEP 4 Severe Persistent STEP 3 Moderate Persistent STEP 2 Mild Persistent STEP 1 Mild Intermittent Step Down STEP 3 > 1 Long-term-control meds (Preferred low dose ICS+LABA) STEP 2 1 Long-term-control medication: anti-inflammatory (Preferred low-dose ICS) STEP 1 Quick-relief medication: PRN Step Up
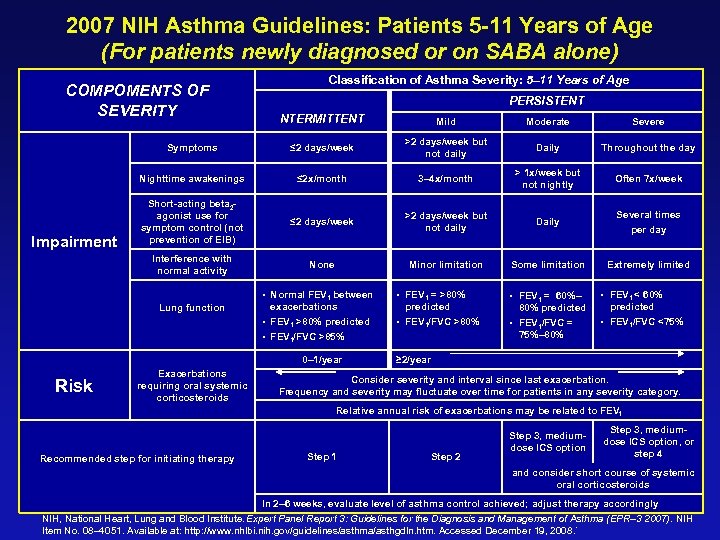 2007 NIH Asthma Guidelines: Patients 5 -11 Years of Age (For patients newly diagnosed or on SABA alone) COMPOMENTS OF SEVERITY Classification of Asthma Severity: 5– 11 Years of Age PERSISTENT Mild Moderate Severe Symptoms ≤ 2 days/week >2 days/week but not daily Daily Throughout the day Nighttime awakenings ≤ 2 x/month 3– 4 x/month > 1 x/week but not nightly Often 7 x/week Short-acting beta 2 agonist use for symptom control (not prevention of EIB) ≤ 2 days/week >2 days/week but not daily Daily Several times per day Interference with normal activity Impairment NTERMITTENT None Minor limitation Some limitation Extremely limited • Normal FEV 1 between Lung function exacerbations • FEV 1 >80% predicted • FEV 1 = >80% predicted • FEV 1/FVC >80% Risk Exacerbations requiring oral systemic corticosteroids • FEV 1 < 60% • FEV 1/FVC = • FEV 1/FVC <75% 80% predicted 75%– 80% • FEV 1/FVC >85% 0– 1/year • FEV 1 = 60%– ≥ 2/year Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time for patients in any severity category. Relative annual risk of exacerbations may be related to FEV 1 Recommended step for initiating therapy Step 1 Step 2 Step 3, mediumdose ICS option, or step 4 and consider short course of systemic oral corticosteroids In 2– 6 weeks, evaluate level of asthma control achieved; adjust therapy accordingly NIH, National Heart, Lung and Blood Institute. Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma (EPR– 3 2007). NIH Item No. 08– 4051. Available at: http: //www. nhlbi. nih. gov/guidelines/asthma/asthgdln. htm. Accessed December 19, 2008. `
2007 NIH Asthma Guidelines: Patients 5 -11 Years of Age (For patients newly diagnosed or on SABA alone) COMPOMENTS OF SEVERITY Classification of Asthma Severity: 5– 11 Years of Age PERSISTENT Mild Moderate Severe Symptoms ≤ 2 days/week >2 days/week but not daily Daily Throughout the day Nighttime awakenings ≤ 2 x/month 3– 4 x/month > 1 x/week but not nightly Often 7 x/week Short-acting beta 2 agonist use for symptom control (not prevention of EIB) ≤ 2 days/week >2 days/week but not daily Daily Several times per day Interference with normal activity Impairment NTERMITTENT None Minor limitation Some limitation Extremely limited • Normal FEV 1 between Lung function exacerbations • FEV 1 >80% predicted • FEV 1 = >80% predicted • FEV 1/FVC >80% Risk Exacerbations requiring oral systemic corticosteroids • FEV 1 < 60% • FEV 1/FVC = • FEV 1/FVC <75% 80% predicted 75%– 80% • FEV 1/FVC >85% 0– 1/year • FEV 1 = 60%– ≥ 2/year Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time for patients in any severity category. Relative annual risk of exacerbations may be related to FEV 1 Recommended step for initiating therapy Step 1 Step 2 Step 3, mediumdose ICS option, or step 4 and consider short course of systemic oral corticosteroids In 2– 6 weeks, evaluate level of asthma control achieved; adjust therapy accordingly NIH, National Heart, Lung and Blood Institute. Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma (EPR– 3 2007). NIH Item No. 08– 4051. Available at: http: //www. nhlbi. nih. gov/guidelines/asthma/asthgdln. htm. Accessed December 19, 2008. `
 Goal of Asthma Therapy: ACHIEVE CONTROL Reduce Impairment • Prevent chronic and troublesome symptoms • Require infrequent use of inhaled SABA (≤ 2 days/week) • Maintain (near) “normal” pulmonary function • Maintain normal activity levels • Meet patients’ expectations of, and satisfaction with, asthma care Reduce Risk • Prevent recurrent exacerbations • Minimize need for emergency department visits or hospitalizations • Prevent progressive loss of lung function • Provide optimal pharmacotherapy, with minimal or no adverse effects NAEPP = National Asthma Education and Prevention Program; SABA = short-acting β 2 -agonists.
Goal of Asthma Therapy: ACHIEVE CONTROL Reduce Impairment • Prevent chronic and troublesome symptoms • Require infrequent use of inhaled SABA (≤ 2 days/week) • Maintain (near) “normal” pulmonary function • Maintain normal activity levels • Meet patients’ expectations of, and satisfaction with, asthma care Reduce Risk • Prevent recurrent exacerbations • Minimize need for emergency department visits or hospitalizations • Prevent progressive loss of lung function • Provide optimal pharmacotherapy, with minimal or no adverse effects NAEPP = National Asthma Education and Prevention Program; SABA = short-acting β 2 -agonists.

 Stepwise Approach for Managing Asthma in Children Aged 5 to 11 Years: NAEPP Guidelines Step 6 Step 1 Preferred: SABA prn Step 2 Step 3 Preferred: Medium-Dose Preferred: Low-Dose ICS (A) ICS (B) Alternative: LTRA or (B), Low-Dose ICS Cromolyn (B), and either Nedocromil (B), LABA (B), or LTRA (B), Theophylline (B) or Theophylline (B) LTRA = leukotriene receptor antagonist. Step 4 Preferred: Medium-Dose ICS + LABA (B) Alternative: Medium-Dose ICS and either LTRA (B) or Theophylline (B) Step 5 Preferred: High-Dose ICS + Preferred: LABA + Oral High-Dose ICS Corticosteroid (D) + LABA (B) Alternative: High-Dose ICS and either LTRA or LTRA (B) Theophylline or and Oral Theophylline (B) Corticosteroid (D) --------------
Stepwise Approach for Managing Asthma in Children Aged 5 to 11 Years: NAEPP Guidelines Step 6 Step 1 Preferred: SABA prn Step 2 Step 3 Preferred: Medium-Dose Preferred: Low-Dose ICS (A) ICS (B) Alternative: LTRA or (B), Low-Dose ICS Cromolyn (B), and either Nedocromil (B), LABA (B), or LTRA (B), Theophylline (B) or Theophylline (B) LTRA = leukotriene receptor antagonist. Step 4 Preferred: Medium-Dose ICS + LABA (B) Alternative: Medium-Dose ICS and either LTRA (B) or Theophylline (B) Step 5 Preferred: High-Dose ICS + Preferred: LABA + Oral High-Dose ICS Corticosteroid (D) + LABA (B) Alternative: High-Dose ICS and either LTRA or LTRA (B) Theophylline or and Oral Theophylline (B) Corticosteroid (D) --------------
 Stepwise Approach for Managing Asthma in Children Aged 0 to 4 Years: NAEPP Guidelines Intermittent Step 1 Preferred: SABA prn Moderate to Severe Persistent Mild Persistent Step 2 Preferred: Low-Dose ICS (A) Alternative: Montelukast (A) or Cromolyn (B) Step 3 Preferred: Medium-Dose ICS (D) Step 4 Preferred: Medium-Dose ICS and either Montelukast or LABA (D) ICS = inhaled corticosteroid; LABA = long-acting β 2 -agonist; SABA = short-acting β 2 -agonist. Step 5 Preferred: High-Dose ICS and either Montelukast or LABA (D) Step 6 Preferred: High-Dose ICS and either Montelukast or LABA and Oral Corticosteroids (D)
Stepwise Approach for Managing Asthma in Children Aged 0 to 4 Years: NAEPP Guidelines Intermittent Step 1 Preferred: SABA prn Moderate to Severe Persistent Mild Persistent Step 2 Preferred: Low-Dose ICS (A) Alternative: Montelukast (A) or Cromolyn (B) Step 3 Preferred: Medium-Dose ICS (D) Step 4 Preferred: Medium-Dose ICS and either Montelukast or LABA (D) ICS = inhaled corticosteroid; LABA = long-acting β 2 -agonist; SABA = short-acting β 2 -agonist. Step 5 Preferred: High-Dose ICS and either Montelukast or LABA (D) Step 6 Preferred: High-Dose ICS and either Montelukast or LABA and Oral Corticosteroids (D)
 Immunotherapy for Asthma Meta-analyses: • Abramson et al • • • AJRCCM 1995; 151: 969 -974 Allergy 1999; 54: 1022 -41 Ross et al • Clinical Therapeutics 2000; 22: 329 -341
Immunotherapy for Asthma Meta-analyses: • Abramson et al • • • AJRCCM 1995; 151: 969 -974 Allergy 1999; 54: 1022 -41 Ross et al • Clinical Therapeutics 2000; 22: 329 -341
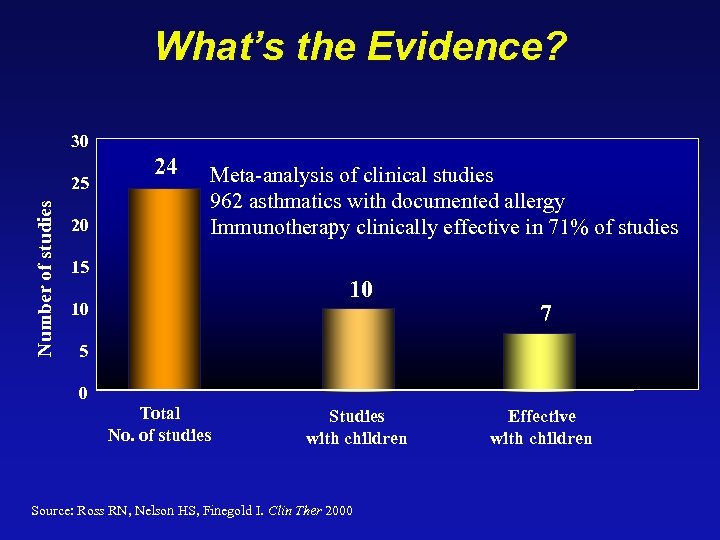 What’s the Evidence? 30 Number of studies 25 20 24 Meta-analysis of clinical studies 962 asthmatics with documented allergy Immunotherapy clinically effective in 71% of studies 15 10 10 7 5 0 Total No. of studies Studies with children Source: Ross RN, Nelson HS, Finegold I. Clin Ther 2000 Effective with children
What’s the Evidence? 30 Number of studies 25 20 24 Meta-analysis of clinical studies 962 asthmatics with documented allergy Immunotherapy clinically effective in 71% of studies 15 10 10 7 5 0 Total No. of studies Studies with children Source: Ross RN, Nelson HS, Finegold I. Clin Ther 2000 Effective with children
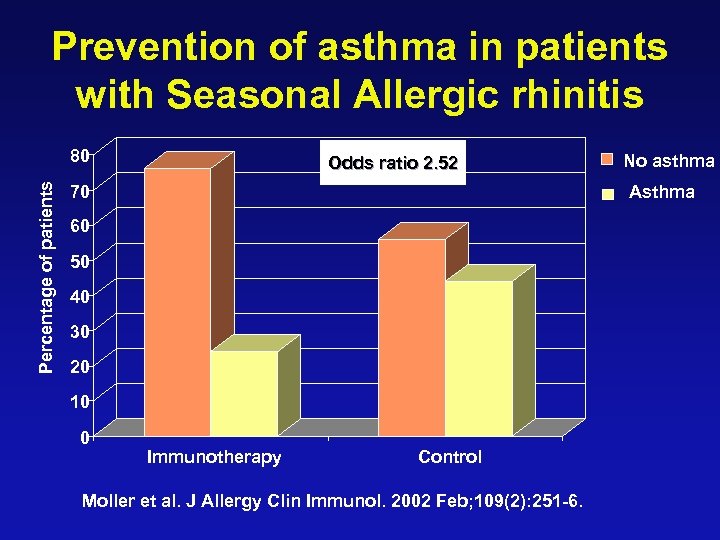 Prevention of asthma in patients with Seasonal Allergic rhinitis Percentage of patients 80 Odds ratio 2. 52 70 Asthma 60 50 40 30 20 10 0 No asthma Immunotherapy Control Moller et al. J Allergy Clin Immunol. 2002 Feb; 109(2): 251 -6.
Prevention of asthma in patients with Seasonal Allergic rhinitis Percentage of patients 80 Odds ratio 2. 52 70 Asthma 60 50 40 30 20 10 0 No asthma Immunotherapy Control Moller et al. J Allergy Clin Immunol. 2002 Feb; 109(2): 251 -6.
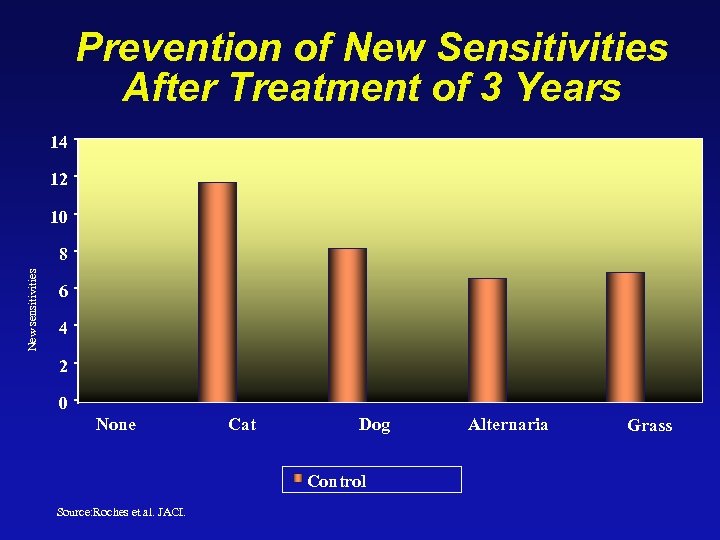 Prevention of New Sensitivities After Treatment of 3 Years 14 12 10 New sensitivities 8 6 4 2 0 None Cat Dog Control Source: Roches et al. JACI. Alternaria Grass
Prevention of New Sensitivities After Treatment of 3 Years 14 12 10 New sensitivities 8 6 4 2 0 None Cat Dog Control Source: Roches et al. JACI. Alternaria Grass
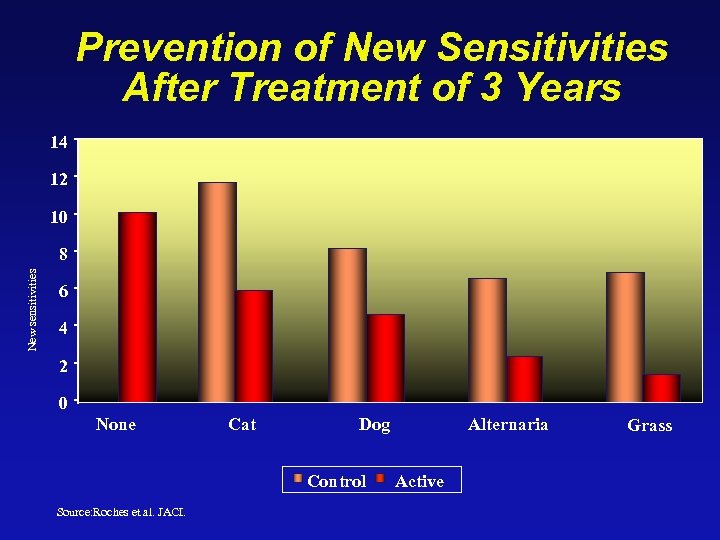 Prevention of New Sensitivities After Treatment of 3 Years 14 12 10 New sensitivities 8 6 4 2 0 None Cat Dog Control Source: Roches et al. JACI. Alternaria Active Grass
Prevention of New Sensitivities After Treatment of 3 Years 14 12 10 New sensitivities 8 6 4 2 0 None Cat Dog Control Source: Roches et al. JACI. Alternaria Active Grass
 Summary • Asthma in children is increasing in prevalence • While mortality from asthma has improved in recent years, morbidity has not • The diagnosis of asthma in young children is challenging • Asthma is children is generally not adequately controlled. • Management of asthma includes reduction of triggers, pharmacotherapy and immunotherapy • NHLBI guidelines for asthma management emphasizes: • assessing control at each visit • Stepping up or down therapy
Summary • Asthma in children is increasing in prevalence • While mortality from asthma has improved in recent years, morbidity has not • The diagnosis of asthma in young children is challenging • Asthma is children is generally not adequately controlled. • Management of asthma includes reduction of triggers, pharmacotherapy and immunotherapy • NHLBI guidelines for asthma management emphasizes: • assessing control at each visit • Stepping up or down therapy


