f5c7cdd24cc959f677e097ca5c2f9f31.ppt
- Количество слайдов: 174

Diabetes Self Management Education Course Amy Bouthillette Clinical Dietitian, Certified Diabetes Educator Carrie Palmer Adult Nurse Practitioner, Certified Diabetes Educator

What Is Diabetes?

Learning Points • Know the difference between Type 1 and Type 2 diabetes • Know the job of glucose • Know the job of insulin • List some health factors related to getting Type 2 diabetes

Type 1 Diabetes • Body does not make insulin • Usually develops in children or young adults • Normal Weight • Must take insulin daily to live

Type 2 Diabetes • Cells do not use insulin properly • Not enough insulin being produced • Generally develops in adulthood – Becoming more common in children due to obesity • Common in persons who are overweight • Many different ways to treat, including diet and exercise, pills, or insulin

Type 2 Diabetes, Key Concepts • • Obesity Insulin Resistance Elevated Insulin Levels Reduced ability to make insulin

Insulin Resistance • Common in persons who are overweight • Insulin not as effective, and does not allow glucose into cells efficiently, causing blood sugar levels to rise • There is enough insulin activity to prevent diabetic coma
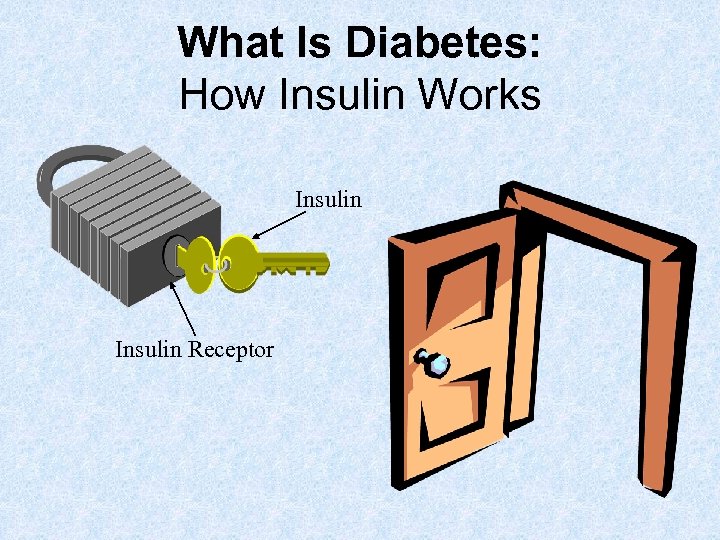
What Is Diabetes: How Insulin Works Insulin Receptor
How Insulin Works • Insulin is a hormone made in your pancrease • It works like a key to unlock cells so that blood sugar (glucose) can enter • Glucose is then used by the body as fuel
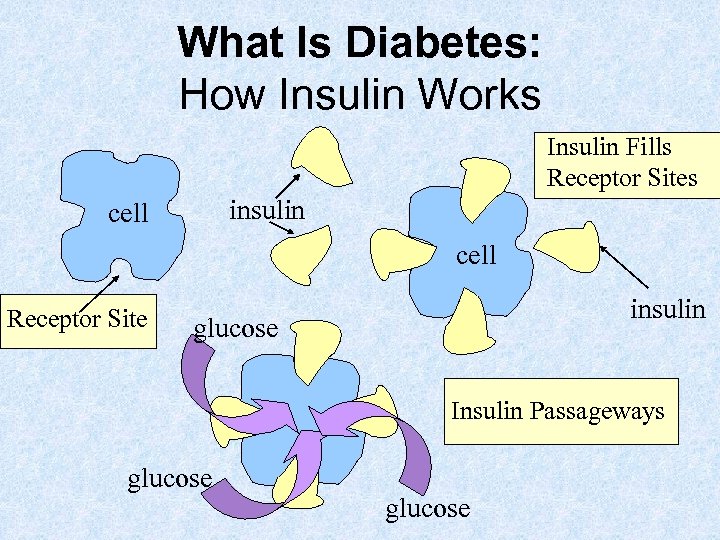
What Is Diabetes: How Insulin Works Insulin Fills Receptor Sites insulin cell Receptor Site insulin glucose Insulin Passageways glucose
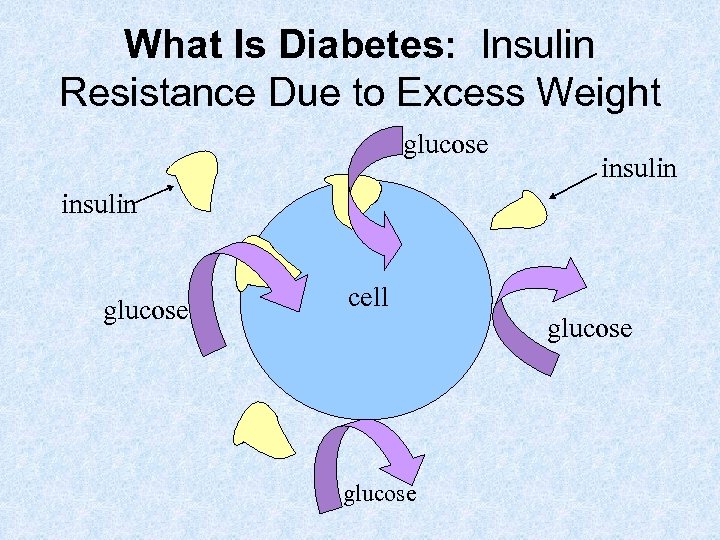
What Is Diabetes: Insulin Resistance Due to Excess Weight glucose insulin glucose cell glucose
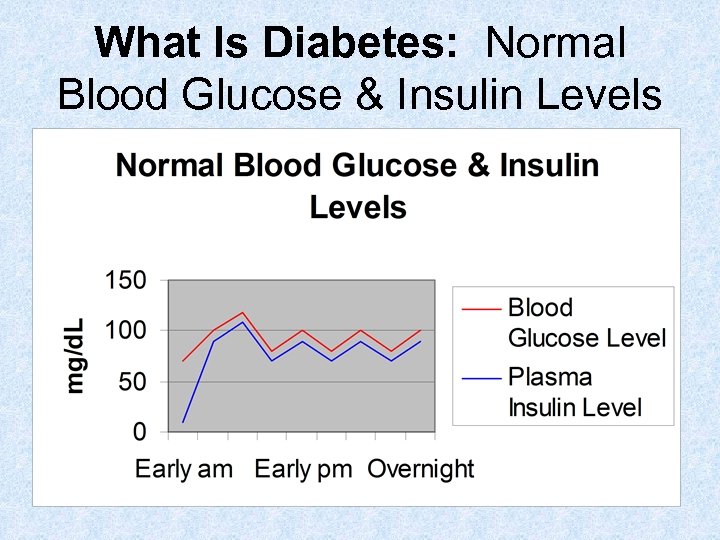
What Is Diabetes: Normal Blood Glucose & Insulin Levels

Monitoring Your Diabetes: Important Tests and Goals

Learning Points • Know why it is important to check glucoses • Be able to describe a range for normal glucoses before food • Be able to describe what A 1 c test measures and what the goal is for A 1 c • Know when you need to test your glucose more often
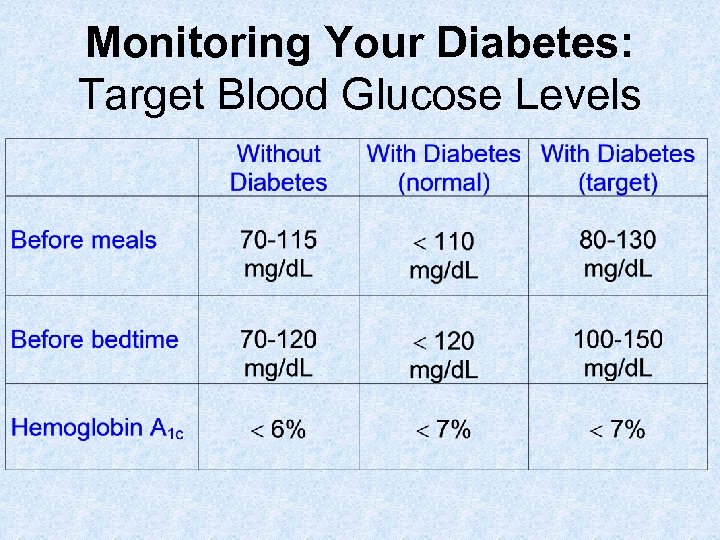

Monitoring Your Diabetes: Target Blood Glucose Levels

Know Your Number 14 10 240 210 8 180 150 6 120 5 Monitoring Your Diabetes: What does an A 1 c mean 270 7 Good Control 300 9 Pretty Good 330 11 Not Good 13 12 Poor Control 360 90 A 1 c Blood Sugar An A 1 c measures how much sugar has been sticking to red blood cells over a 3 month period of time. An A 1 c is a measure of long-term diabetes control. Goal is A 1 c <7
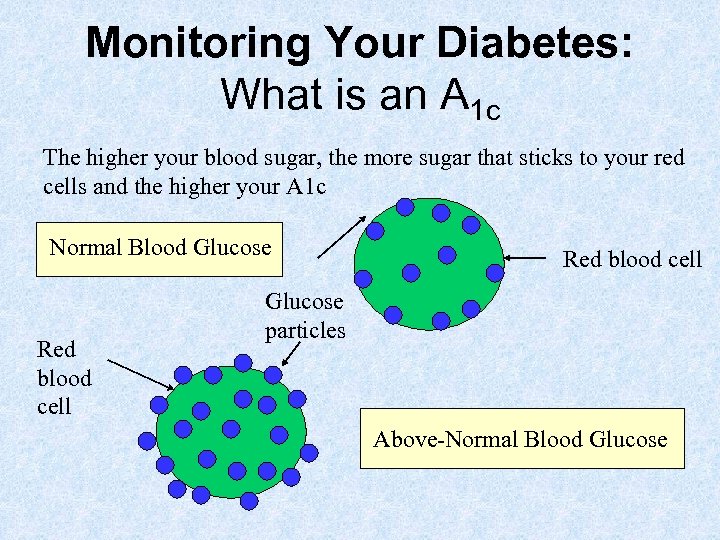
Monitoring Your Diabetes: What is an A 1 c The higher your blood sugar, the more sugar that sticks to your red cells and the higher your A 1 c Normal Blood Glucose Red blood cell Glucose particles Above-Normal Blood Glucose

Monitoring Your Diabetes: Testing your A 1 c • Your doctor will check your A 1 cevery 3 to 6 months • Your doctor may check your A 1 c more often if: – You have blood sugars above goal – Your last A 1 c was high – You have had symptoms of low blood sugar

Monitoring Your Diabetes: Controlled blood sugars and A 1 c • Blood sugars and an A 1 c at or below goal (7% or less) can protect your: – Heart, brain, blood vessels – Eyes – Kidneys – Nerves – Feet

Monitoring Your Diabetes: Testing Your Sugars at Home

Testing Sugars- How often? • Depends what kinds of medicine you take: – Most patients taking pills test once a day – Patients taking insulin may need to test between 1 and 4 times a day • Determined by the type of insulin and its action • Test more often if: – You have had low blood sugars (BG<70) – Sugars have been unusually high (over 200) – You are sick – You are starting a new exercise program

Monitoring Your Diabetes: Sample Diabetes Record- Fasting
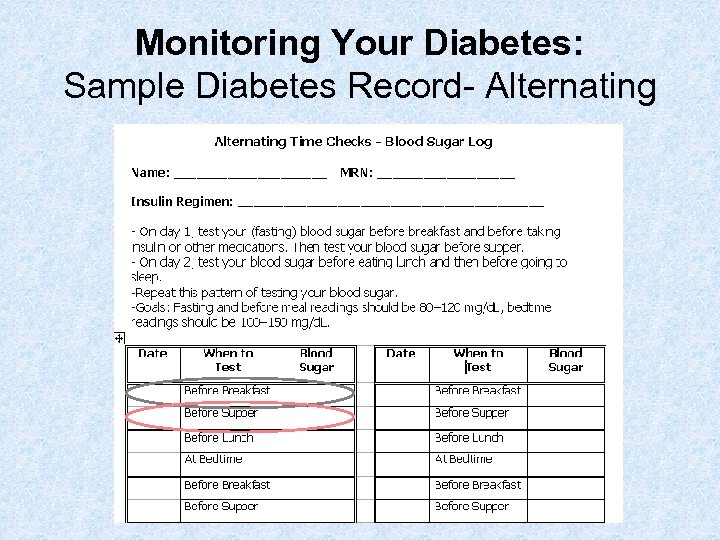

Monitoring Your Diabetes: Sample Diabetes Record- Alternating
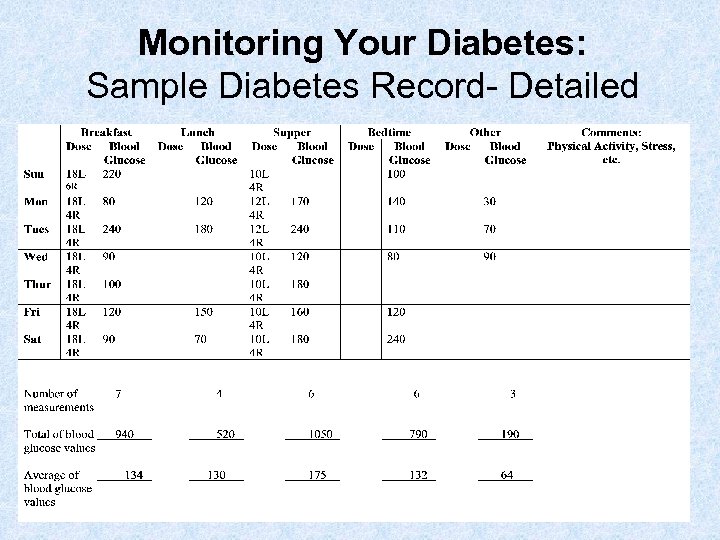
Monitoring Your Diabetes: Sample Diabetes Record- Detailed
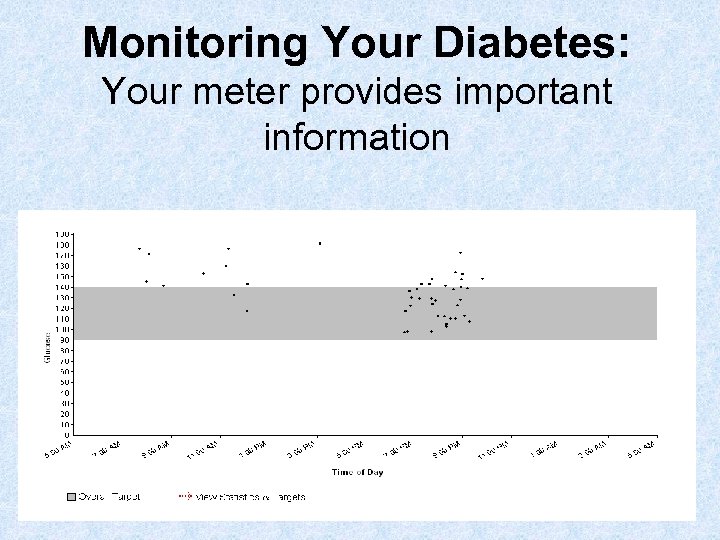
Monitoring Your Diabetes: Your meter provides important information

Other Points to Remember • Make sure you know how to correctly use your meter • Don’t share meters • Always bring meter to doctor’s visits

What Affects Your Blood Sugar? What is hypoglycemia & hyperglycemia?

Learning Points • Know signs of high blood sugar (hyperglycemia) • Know the signs of low blood sugar (hypoglycemia) • Know what to do when sugars are too high or too low

Your Blood Sugar: Hyperglycemia or High Blood Sugar • Symptoms – Extreme thirst – Frequent urination – Dry skin – Hunger – Blurred vision – Drowsiness – Decreased healing

Your Blood Sugar: Hyperglycemia or High Blood Sugar • Causes – Too much food – Too little insulin or diabetes medicine – Illness – Stress • Onset – Gradual – If extremely high or you have type 1 diabetes it may progress to diabetic coma – Damage to your eyes, kidneys, and nerves happens over time

Your Blood Sugar: Hyperglycemia or High Blood Sugar • What can you do when you have symptoms? – Test blood glucose more often – Don’t wait, call your doctor if your blood sugar is over 200 mg/d. L for several tests or for 2 days

Your Blood Sugar: Symptoms of Hypoglycemia • Shaking • Fast heartbeat • Sweating • Dizziness • Anxiety • • • Hunger Impaired vision Weakness/fatigue Headache Irritability

Your Blood Sugar: Hypoglycemia or Low Blood Sugar • Causes – Too little food – Too much insulin or diabetes medicine – Extra activity or exercise • Onset – Sudden • May progress to unconsciousness, confusion, or insulin shock

Your Blood Sugar: Treatment of Hypoglycemia 4 Steps to treating your blood sugar: Quick sugar, 10 to 15 grams carbohydrate Recheck blood glucose in 15 to 20 minutes and repeat treatment if necessary 3. If your glucose is normal, eat a protein meal or snack 4. If you have symptoms, but BG is over 70, have snack *Treat all sugars under 70 mg/dl (with or without symptoms) 1. 2. *If you have symptoms, but no meter, treat and try to be prepared and have meter with you the next time.

Hypoglycemia or Low Sugar: Step 1 - 10 to 15 Grams of Carbs Pick One of these 5 to 8 Life Savers® 1/4 to 1/3 cup raisins 4 oz. orange juice 8 oz. milk 2 to 3 Glucose Tablets ½ can of regular soda 3 to 5 peppermint candies
Hypoglycemia or Low Sugar: Step 2 - Recheck Blood Sugar
Hypoglycemia or Low Sugar: Step 3 - Eat a protein snack Pick One ½ meat sandwich peanut butter sandwich or crackers & cheese

Hypoglycemia or Low Sugar: Foods to avoid for lows Potato Chips Doughnuts Chocolate Pizza Nuts Ice Cream Cake Cookies

Monitoring Your Diabetes: Your blood pressure, cholesterol, and key medications

Your Heart: Controlling diabetes is more than just sugar • The number one killer of Americans is heart disease: – Heart attacks – Strokes • If you have diabetes, your have 4 X the risk of a heart attack • You must control your blood pressure, cholesterol, and take key medications

Your Heart: Blood Pressure • What used to be considered a “normal” blood pressure may in fact be abnormal – Goals change • If your blood pressure is significantly elevated, it may be more important for your doctor to improve than your sugar • Goal – If you have diabetes your pressure should be lower than someone who does not have diabetes – Systolic less than 130 mm. Hg (top number) – Diastolic less than 80 mm. Hg (bottom number)

Your Heart: Cholesterol • What used to be considered a “normal” cholesterol may in fact be abnormal – Goals change • Goal – If you have diabetes your cholesterol should be lower than someone who does not have diabetes – Total cholesterol under 200 mg/dl – LDL (bad cholesterol) less than 100 mg/dl – HDL (good cholesterol) over 40 mg/dl – Triglycerides (blood fat) less than 150 mg/dl • You need a cholesterol medicine if you are not at goal, you have had heart surgery or a heart attack/stroke, or your total cholesterol is over 135 mg/dl and you are older than 35
Your Heart: Key Medicines • Most patients over 35 years old who have diabetes could benefit from key medications: – Cholesterol medications- Statins – Blood pressure medications- ACE-I or ARB – Blood thinners- A daily baby aspirin

Monitoring Your Diabetes: Summary
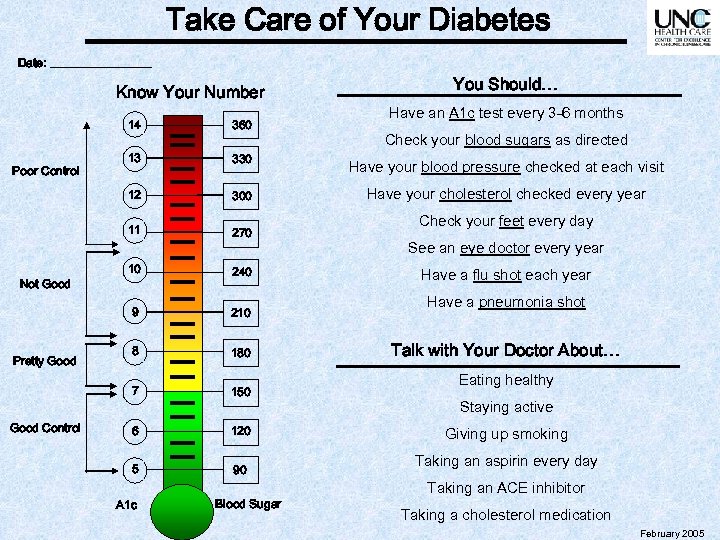
Take Care of Your Diabetes Date: _________ Know Your Number You Should… Have an A 1 c test every 3 -6 months 14 300 Have your cholesterol checked every year 270 10 240 210 8 180 7 Good Control Have your blood pressure checked at each visit 9 Pretty Good 330 11 Not Good 13 12 Poor Control 360 150 6 120 5 90 A 1 c Blood Sugar Check your blood sugars as directed Check your feet every day See an eye doctor every year Have a flu shot each year Have a pneumonia shot Talk with Your Doctor About… Eating healthy Staying active Giving up smoking Taking an aspirin every day Taking an ACE inhibitor Taking a cholesterol medication February 2005
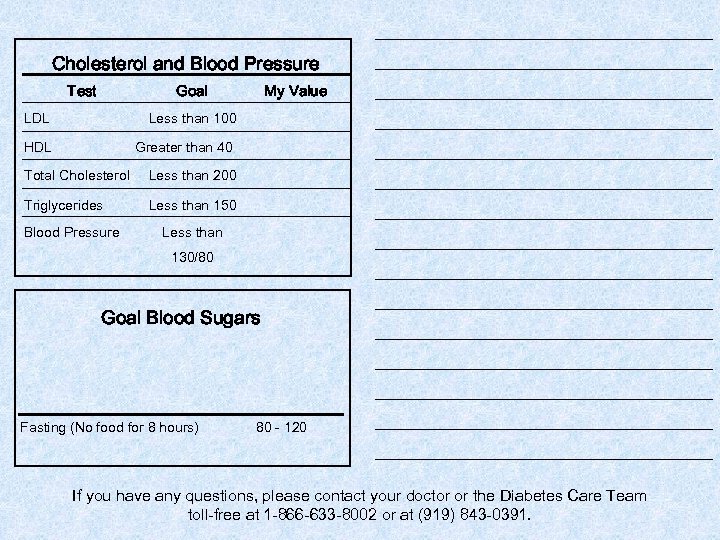

Cholesterol and Blood Pressure Test Goal LDL Less than 100 HDL My Value Greater than 40 Total Cholesterol Less than 200 Triglycerides Less than 150 Blood Pressure Less than 130/80 Goal Blood Sugars Fasting (No food for 8 hours) 80 - 120 ___________________________ ___________________________ ___________________________ ___________________________ If you have any questions, please contact your doctor or the Diabetes Care Team toll-free at 1 -866 -633 -8002 or at (919) 843 -0391.

Long Term Considerations with Diabetes Preventative Efforts Complications

Learning Points • List some complications of uncontrolled diabetes • Describe some preventive screenings for your eyes, feet • Know how often you should check your feet • Describe some behaviors to prevent developing complications from diabetes

Preventing Complications • Diabetes can cause other problems if not well controlled • Be sure to monitor: Feet Eyes Heart Kidneys

Screenings Your Doctor Can Do • • • Check cholesterol every year Dental exam and cleaning twice a year Foot check every visit with your doctor Thorough foot exam every year Urine check for kidney damage (microalbumin) every year
Behaviors to Prevent Complications • Pneumonia vaccination at least once • Flu shot every year • Dilated eye exam by an ophthalmologist every year

Personal Habits You Can Do • • Check your blood sugar Maintain a healthy weight Stop smoking Exercise Eat a healthy diet Check your feet every day Brush and Floss your teeth every day

Foot Care • Keep your blood sugars in good control • Check your feet every day – Look for cuts, blisters, red spots, swelling – Use a mirror to check the bottoms of your feet or ask someone to help • Wash your feet every day in warm (not hot) water – Dry well, especially between the toes

Foot Care • Keep your feet soft and smooth – Use thin coat of lotion on the tops and bottoms of feet – Do not use lotion between your toes • Trim toenails weekly if you can reach them – Trim straight across – File edges with an emery board

Foot Care • Protect your feet from hot and cold by avoiding contact with hot water or surfaces and wearing socks to keep feet warm • Elevate feet when you are sitting and avoid crossing legs • Stop smoking to improve blood flow to your feet

Foot Care • Wear Shoes and Socks at All times – Never walk barefoot – Wear comfortable shoes that protect feet – Feel inside of your shoes before putting them on to make sure lining is smooth and no objects are inside

When to see the Podiatrist • If you cannot reach or see well enough to cut your own nails • If your toenails are too thick for you to cut • If you have thick callouses • If you have now or have ever had a foot ulcer • If you have numbness in your feet
Long Term Complications Cardiovascular disease Retinopathy (eye damage) Nephropathy (kidney damage) Neuropathy (nerve damage)

Cardiovascular Disease • Diseases of the heart and large blood vessels • 65% of people with diabetes die from heart attack or stroke • People with diabetes often have heart attacks earlier in life • 1 out of 3 people with diabetes have peripheral arterial disease, which reduces blood flow to your feet

ABC’s to Protect Your Heart and Blood Vessels • A is for A 1 c: less than 7% • B is for Blood Pressure: 130/80 or less • C is for Cholesterol: – LDL (bad) cholesterol less than 100 – HDL (good) cholesterol greater than 40 in men and 50 in women – Triglycerides less than 150

What YOU can do to Protect Your Heart • • • Take your medicines! Take an aspirin every day Exercise Eat a healthy diet Quit Smoking Reduce stress

Retinopathy (eye damage) • Leading cause of blindness in US is diabetes • Risk is increased each year you have diabetes • Can be prevented by excellent control of blood sugar • Can be prevented with routine eye exams and early detection • Can be treated with laser surgery by an ophthalmologist

Nephropathy (kidney damage) • Leading cause of kidney failure and need for dialysis in US • First sign is protein spilling into urine, tested with urine Microalbumin. • Advanced kidney damage later evident on bloodwork • Kidney damage or worsening kidney damage can be prevented by excellent blood sugar and blood pressure control, and by certain blood pressure medications

Neuropathy (nerve damage) • Diabetes is the leading cause of leg amputation in the US • Numbness, tingling, burning, or other painful sensations in hands and feet • Slowed digestion of food in stomach causing nausea, vomiting, or diarrhea • Carpal tunnel syndrome causing pain in hands and wrists • Other nerve problems-sexual dysfunction

Neuropathy (nerve damage) • Increased risk with each year of diabetes, high blood sugar, and smoking • Can lead to foot ulcers and foot deformities • Prevent and improve symptoms with excellent blood sugars • Must practice good foot care • Some medications can improve painful symptoms, but not numbness.

Hour 2 Medicines for Diabetes • Diabetes pills • Insulins • New diabetes medicines

Learning Points Know why it is important to take your medicines as prescribed Know the medications you are on for diabetes Know the possible side effects of your meds
Diabetes Pills: Oral Medications
Diabetes Pills: Sulfonylureas • These tell the pancreas to make more insulin
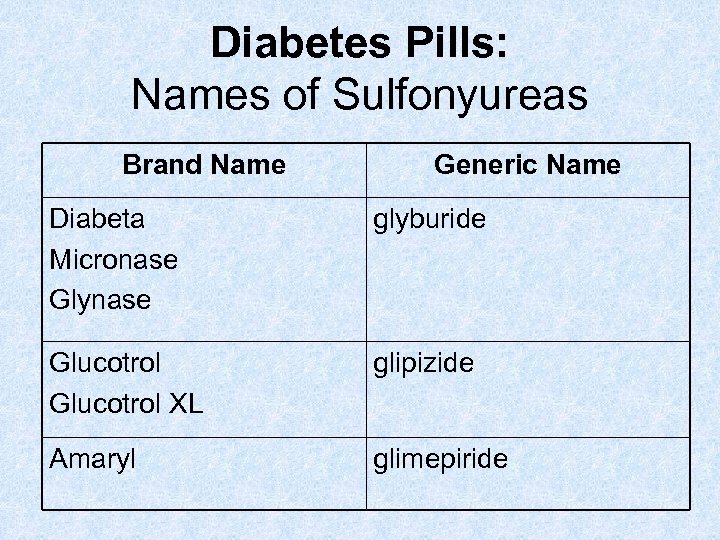
Diabetes Pills: Names of Sulfonyureas Brand Name Generic Name Diabeta Micronase Glynase glyburide Glucotrol XL glipizide Amaryl glimepiride

Diabetes Pills: Things to know about sulfonylureas • Main thing to watch out for is having too many low blood sugars. If this happens, your doctor will give you a lower dose. • Take the same way everyday • Glucotrol XL cannot be crushed or cut in half; might see its empty shell in toilet
Diabetes Pills: Metformin • Tells the liver to stop sending out sugar

Diabetes Pills: Metformin • Comes as generic metformin or brand name Glucophage • Also comes in a long-acting form

Diabetes Pills: Things to know about metformin • Can help people lose some weight • Main side effects are upset stomach and diarrhea – These usually get better after about 1 week – Taking with food can help • Does not cause blood sugar to go too low • Cannot be used in kidney disease or certain kinds of heart failure. Talk with doctor if you have these. • Contact doctor if you notice new fatigue, nausea, muscle pain/weakness, or fast breathing because these could be signs of a serious side effect

Diabetes Pills: Glitazones • These help insulin in your body work better

Diabetes Pills: Names of Glitazones • Avandia and Actos • Only come as brand name pills

Diabetes Pills: Things to know about glitazones • The more common side effects of these are weight gain and swelling • People with heart failure should discuss this with their doctor before taking • Occasional blood work to test the liver is recommended, although liver problems on this medicine are very rare • These pills usually take 6 to 12 weeks before you can see their full benefit on blood sugar • These are expensive

Diabetes Pills: Meglitinides • These tell the pancreas to make more insulin • These are taken with meals, so you skip a dose if you skip a meal

Diabetes Pills: Names of Meglitinides • Prandin® and Starlix® • Only come as brand name pills

Diabetes Pills: Meglitinides • Things to know – Main side effect to watch out for is low sugars • Might have a lower chance of having lows compared with sulfonylureas – These are expensive

Diabetes Pills: Alpha-glucosidase inhibitors • These pills slow down the absorption of carbohydrates (carbs) from the gut after you eat

Diabetes Pills: Names of Alpha-glucosidase inhibitors • Precose® • Glyset™ • Only come as brand name pills

Diabetes Pills: Things to know about alpha-glucosidase inhibitors • Biggest problem with these pills is that they can cause a lot of stomach upset and gas (70%) • This gets better over time, but for some people it stays a problem with these pills • Have to take it with every meal, since it works on food directly. Skip taking if you skip a meal

Combination Diabetes Pills Available • Glucovance® – Metformin + glyburide • Metaglip® – Metformin + glipizide • Avandamet® – Avandia® + metformin • Avandaryl® – Avandia® + Amaryl®
All About Insulin

Insulin • Used in patients with type 1 and type 2 diabetes • Used to replace the insulin your body is no longer able to make – You need insulin to move glucose into cells after eating. This lowers blood sugar and provides fuel to your body. • Available in different formulations – Short-acting insulin to take with meals – Long-acting insulin to provide baseline insulin – Insulin mixes
Types of Insulin • • “Meal” Insulin Long-Acting Insulin Mixes Come in vials or pens
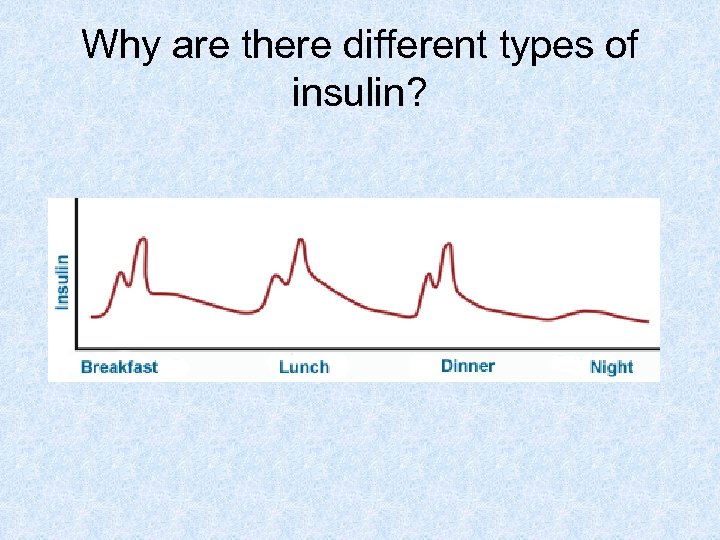
Why are there different types of insulin?

“Meal” Insulins • Humulin R®, Novolin R® – “Regular” insulin – Clear – Short-acting – Inject these 30 minutes before meals – For some people, these last a couple of hours too long, so that blood sugar is too low after effect of meal wears off

“Meal” Insulins • Novolog®, Humalog®, Apidra® – Clear – Rapid-Acting – Inject these 15 minutes before meals – Can inject right before meal or immediately after finishing meal – These last for a shorter time in body, so they wears off faster and are less likely to cause low blood sugar between meals

Intermediate-acting insulins • Novolin N®, Humulin N® – Cloudy – Lasts about 12 -18 hours – Inject these at consistent times, as prescribed – Usually taken twice a day

Long-acting Insulins • Lantus® – Clear – Longer acting, usually taken once a day at same times • Levemir® – Clear – Long acting, taken once or twice a day

Insulin “Mixes” • Humulin 70/30, Novolin 70/30 – Mixtures of 70% NPH and 30% regular insulin • Humalog Mix 75/25 – Mixture of 75% longer-acting and 25% fastacting insulin • Novolog Mix 70/30 – Mixture of 70% longer-acting and 30% fastacting insulin

Insulin “Mixes” • Cloudy • Usually taken twice a day with meals. • Longer-acting part tends to work better when taken later at night (8 -10 pm) than when taken with supper • Difficult to obtain good control with mixes due to low blood sugar risks • Depend on very consistent meal patterns!
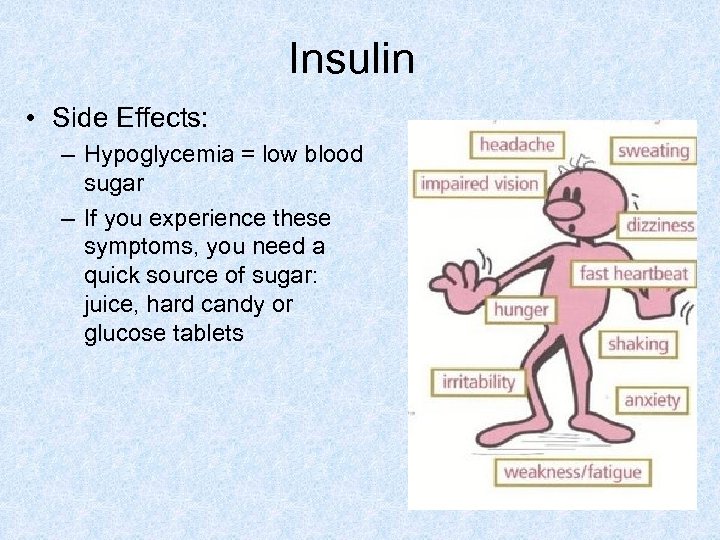
Insulin • Side Effects: – Hypoglycemia = low blood sugar – If you experience these symptoms, you need a quick source of sugar: juice, hard candy or glucose tablets

Insulin • Side Effects (continued): – Soreness or redness at injection site • You can minimize this by rotating the injection site each time you administer insulin – Feeling nervous or agitated – Increased thirst or appetite • Your dose may need to be changed to help with these symptoms
Insulin – Drawing up doses 1. 2. 3. 4. 5. 6. 7. Wash your hands Inspect insulin for particles before using – replace if necessary If using a cloudy insulin (like Humulin N, Novolin N, or a “mixed” insulin) – gently roll vial between hands Check how many units you need to inject. Then pull back the syringe plunger to draw that amount of air into the syringe Push the needle into the top of the insulin bottle. Push the plunger to put air into the bottle. Keep the needle in the bottle Holding the needle in the bottle, turn the bottle upsidedown. Then pull out the plunger to measure the units of insulin you need. Take the needle out of the bottle
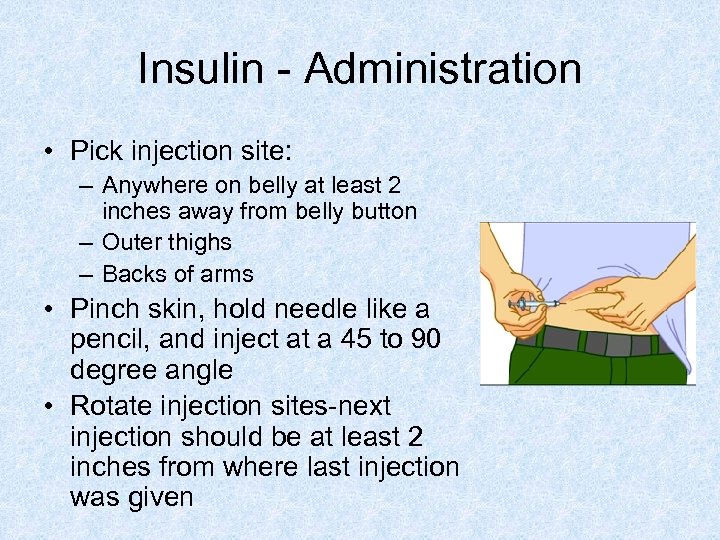
Insulin - Administration • Pick injection site: – Anywhere on belly at least 2 inches away from belly button – Outer thighs – Backs of arms • Pinch skin, hold needle like a pencil, and inject at a 45 to 90 degree angle • Rotate injection sites-next injection should be at least 2 inches from where last injection was given
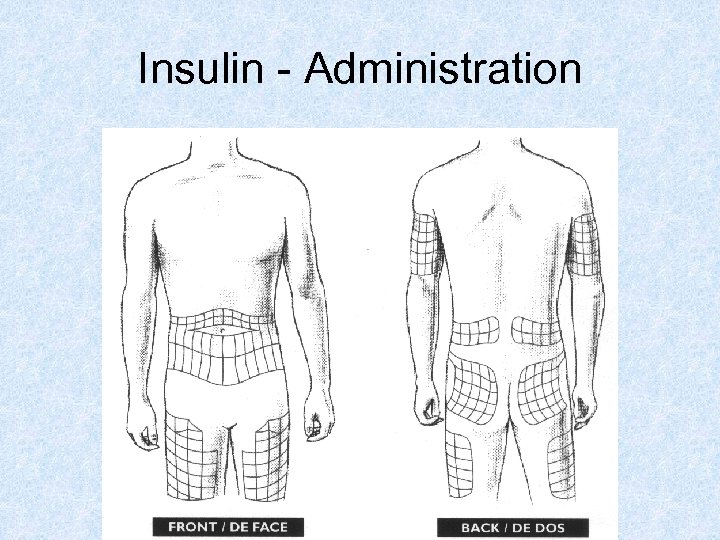
Insulin - Administration

Insulin – Storage • Refrigerate all insulin vials while not inuse • May keep individual insulin vial at room temperature once in-use – Just avoid exposing vials to high temperatures (over 85 degrees F) for extended periods • Never freeze insulin – do not use after it has been frozen

Insulin – Storage • Whether kept in refrigerator or at room temperature, most insulin vials should be discarded 4 weeks after first dose was drawn from it – Exception: Levemir is good until 42 days after first use • Insulin pens – vary widely in expiration dating once in-use– always check with pharmacist for your individual product

New Medicines • Byetta • Symlin • Januvia

New Medicines - Byetta® • Injections: 5 - and 10 -mcg prefilled pens • Can be used in people who are not on insulin but are taking diabetes pills • Given twice a day with meals • Cannot be mixed with any insulins

New Medicines - Byetta® • Generally only small decreases in blood sugar – A 1 c goes down about ½ % • Lowers blood sugars that are high within a few hours after meals • Side effect of nausea – May cause some people to lose some weight

New Medicines - Symlin® • Injection: comes in vial or pen • Can be used in people on insulin, in both type 1 and type 2 diabetes • Given 3 times a day with meals

New Medicines - Symlin® • Generally only small decreases in blood sugar – A 1 c goes down about ½ % • Your doctor will cut down doses of your insulins, since there can be a risk of dropping your blood sugar too low • Lowers blood sugars that are high within a few hours after meals • Side effect of nausea – May cause some people to lose some weight

New Medicines – Januvia® • Oral tablets • Usually given once a day and can be taken with or without food • Used for patients with Type 2 Diabetes • Can be used in patients also taking metformin or a glitazone

New Medicines – Januvia® • Works in 2 ways: – Tells your body to make more insulin – Tells your body to make less sugar • Generally only small decreases in blood sugar – A 1 c goes down ½ % • You may need a lower dose if you have kidney disease • Side effects: headache, respiratory infections and low sugars

Physical Activity

Learning Points • Describe how exercise affects blood glucose levels • Describe how regular exercise affects the body • Know how much exercise a person should get each week

Physical Activity: How Does Exercise Help? • Improves cholesterol and other lipids • If hypertensive, helps to control high blood pressure • Improves cardiovascular function • Diminishes potential for weight gain

Physical Activity: How Does Exercise Help? • Improves insulin sensitivity • Increases sense of well-being • Increases flexibility and muscle strength

Physical Activity: Before You Begin an Exercise Program. . . • Consult your doctor • Adjust insulin and carbohydrate, if necessary • Check your blood sugar before and after exercising • Carry fast-acting sugar • Wear ID • Use stomach area for shots

Physical Activity: Things to Keep in Mind • Exercise should be appropriate for your lifestyle and general condition • Wear proper shoes & inspect your feet daily • Use protective equipment as necessary

Physical Activity: Getting Started • Start your exercise program slowly • Be sure it is enjoyable • At first, exercise may be limited to 5 -10 minute periods on 3 -4 days a week • When you are ready, gradually increase the length of time you exercise and the number of days of exercise each week

Physical Activity: Types of Exercise • Aerobic exercise (with oxygen) – Includes endurance exercise • Walking, riding bikes, swimming – Improves heart fitness • Anaerobic exercise (without oxygen) – Lasts for short durations • Resistance training (lifting weights) • Flexibility training (stretching) – Improves muscle strength

Exercise Recommendations for Diabetes Aerobic activity • At least 150 minutes per week (moderate) • And/Or 90 minutes per week (vigorous) • Spread over at least 3 days, not skipping more than 2 days in a row Strength or resistance training • 3 x a week • Work up to 3 sets of 8 -10 repetitions To keep lost weight off (over 30 pounds)- maintain 60 minutes a day of moderate to vigorous activity

Physical Activity: Planning Your Exercise Program • What exercise programs or activities are safe & practical for you to do regularly? • Where will you do these activities? • What time of day will you do your program? • How often will you exercise? • How long will you exercise each time?
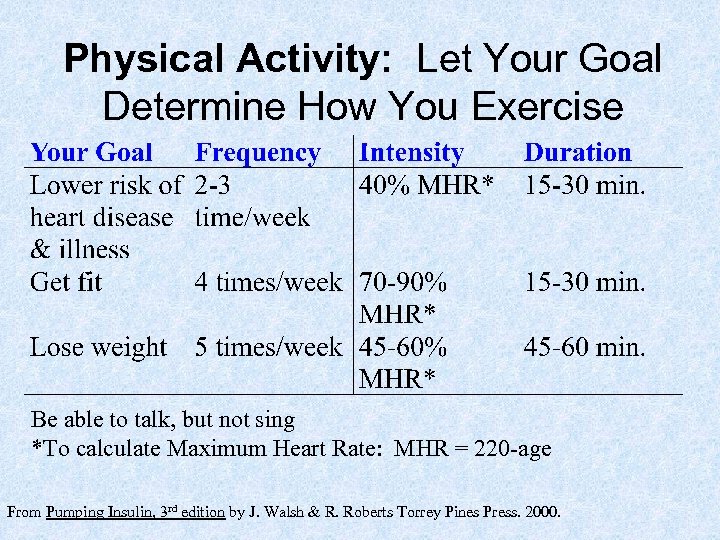
Physical Activity: Let Your Goal Determine How You Exercise Be able to talk, but not sing *To calculate Maximum Heart Rate: MHR = 220 -age From Pumping Insulin, 3 rd edition by J. Walsh & R. Roberts Torrey Pines Press. 2000.

Physical Activity: Precautions • Avoid exercising in extreme heat or cold • Maintain adequate hydration before, during, and after exercise • Self-monitor blood glucose • When during exercise is your risk for hypoglycemia the greatest?

Planning Your Exercise Program • Include a mix of stretching, aerobic, and weight-bearing activities • Know your target heart rate • Plan activities in your calendar • Track your exercise progress in a notebook • Plan a reward for sticking to your program

Eating Basics- Hour 3

Learning Points • Know which foods contain carbohydrates • Describe appropriate portion sizes • List some items to look for on the food label • Describe a healthy snack or meal

Overview of Topics • • Food and Blood Glucose Meal Planning Carbohydrate Counting Food Labels Heart Healthy Eating Goal Setting Food Log/Diary

Food Types and Examples • “Fat” Foods: butter, oils, fatback, mayonnaise, cream, margarine • “Protein” Foods: chicken, fish, meat, eggs • “Carbohydrate” Foods: bread, rice, crackers, cereal, fruit
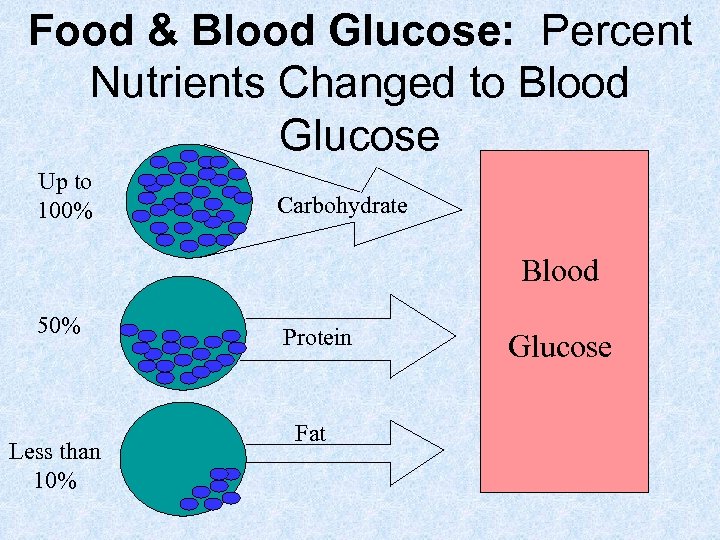
Food & Blood Glucose: Percent Nutrients Changed to Blood Glucose Up to 100% Carbohydrate Blood 50% Less than 10% Protein Fat Glucose
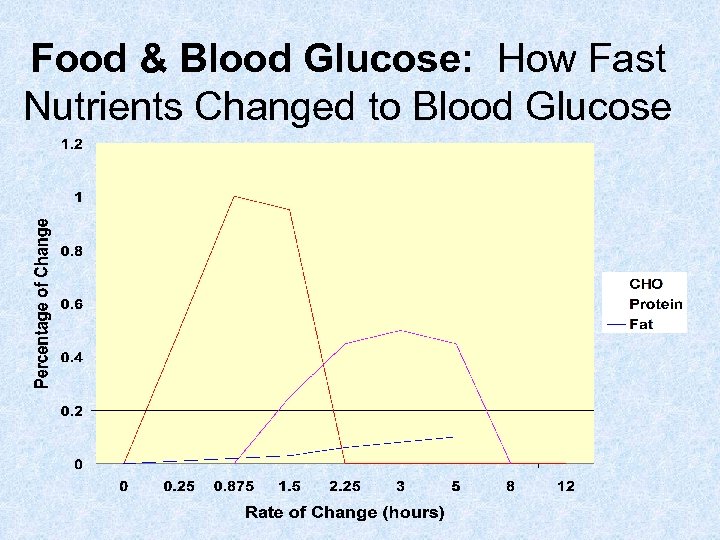
Food & Blood Glucose: How Fast Nutrients Changed to Blood Glucose

Meal Planning

Why Do I Need to Plan Meals? • Helps maintain normal blood glucose • Helps maintain normal cholesterol (blood fats) • Provide right amount of calories • Prevent, delay, or treat diabetes-related complications • Improve health through optimal nutrition
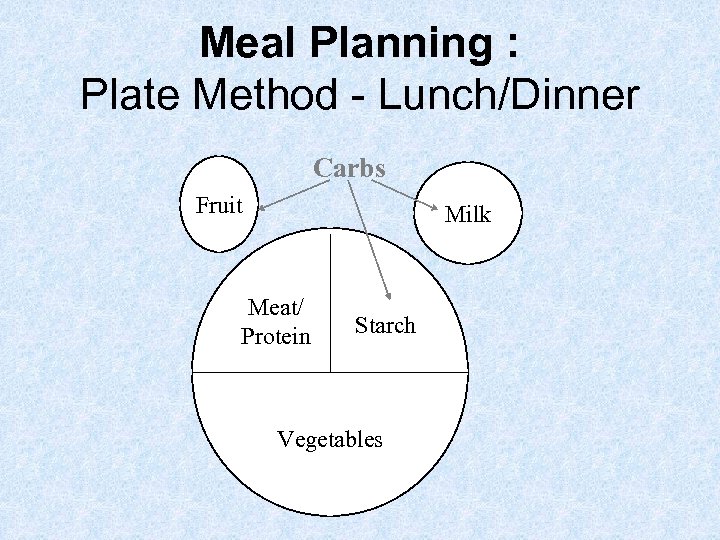
Meal Planning : Plate Method - Lunch/Dinner Carbs Fruit Milk Meat/ Protein Starch Vegetables

Carbohydrate Counting • Try to eat the same amount at each meal • Swap one “exchange” or another in list • 1 exchange = 15 g carbohydrate • Match carb intake to insulin • Use the food label to figure out grams or other carbohydrate counting book

Examples of Exchanges • • 1 cup milk 6 saltine crackers 1/3 cup rice ½ cup of canned fruit ½ cup pinto beans 1 slice bread 1 small apple 5 pieces hard candy
How Many Exchanges? • Many people can start with 3 exchanges per meal • Snacks can be 1 or 2 exchanges • Individualized for each person • Check glucoses 2 hours after eating • (150 -180= carbohydrate intake is ok)
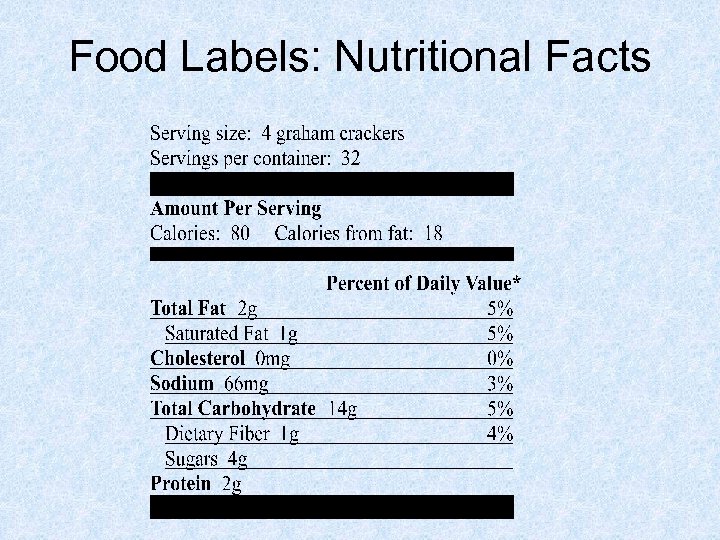
Food Labels: Nutritional Facts

Looking at Labels Exercise • • Look at your food product How many calories? Carbs? Sodium? How many servings in the package? If you ate the whole package, how many servings did you eat? How many carbs?

Heart Healthy Eating • Eat Less Unhealthy Fat (cholesterol, saturated, trans fat) • Replace with Healthy fats (oils, margarine) • More Fiber • Less Salt or Sodium
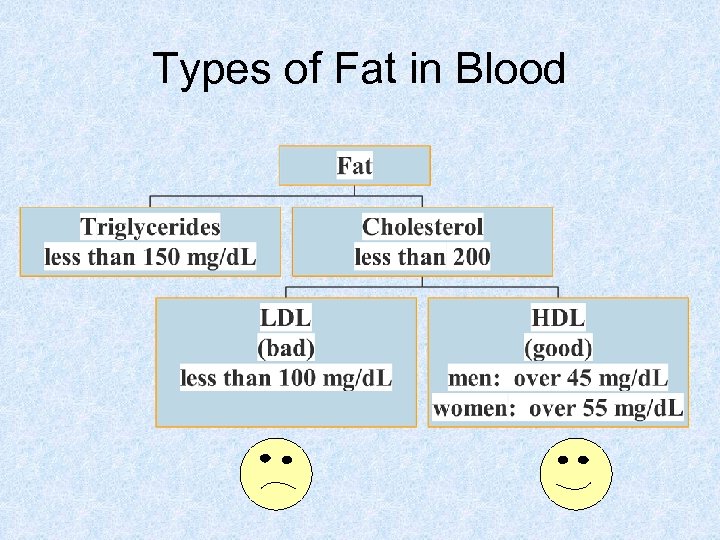
Types of Fat in Blood

Types of Fat in Diet Unhealthy Fats Healthy Fats Limit total intake Use these in place of the unhealthy fats Cholesterol Unsaturated Fats: Saturated Fat Monounsaturated Trans fat Polyunsaturated Omegas 3 s

Eating for a Healthy Heart: Sources of Cholesterol & Fat Trans Fat Fried Foods Donuts Chips Packaged cookies, crackers, cakes Margarine Small amounts in animal products Polyunsaturated (ok in small amounts) Monounsaturated (choose more often)

Eating for a Healthy Heart • • Eat More Fiber Two types, two jobs Soluble fiber- helps to lower cholesterol Insoluble fiber-helps prevent constipation

Sources of Fiber: Soluble • Soluble Fiber (helps lower blood fats) – – – – Raw vegetables Fresh fruits Barley Dried peas Brown rice Okra Kidney beans Lentils – Pinto beans – Black-eyed peas – Whole-grain products • oat, oat bran, and rice bran cereals • soy pasta • oat bran, rye, and pumpernickel breads • oat and rye crackers

Sources of Fiber: Insoluble • Insoluble Fiber (helps prevent constipation) – Some raw vegetables – Wheat bran products: • • cereal (100% bran, Allbran, Fiber One) Pasta (whole wheat) Bread (whole wheat, white wheat) crackers

Grocery Shopping Tips • Read all Food Labels • Stick to the outside aisles of the store • Focus on lean meats, fruits and vegetables, low fat dairy and whole grain products • Always shop with a grocery list • Don’t shop while hungry

Will it be more expensive? • Reduce food costs: – Canned/frozen or seasonal fruits and veggies – More meatless meals – Purchasing less junk foods, sodas, “extras” – Preparing more meals at home – Special “diabetic foods” are not necessary – Shop store sales and use coupons – Avoid food waste & spoilage, use up leftovers Tips on Cutting Cost

Breakfast Ideas • Breakfast One: – toasted low fat cheese sandwich – 8 oz. skim milk • Breakfast Two: – oatmeal-1 c. after cooking-(1/2 c. Dry) – tangerine (1 small) – boiled egg (1)

More Breakfast Ideas • Breakfast Three: – apple, 1 small – low fat cottage cheese, ½ cup – english muffin- 1 whole – margarine, 1 -2 tsp. • Breakfast Four: – – Cheerios ( 1 cup) ½ cup 1% milk Wheat toast- 1 slice 1 Tbsp. peanut butter

Snack Ideas • Snack One: – peanut butter (1 -2 T. ) – graham crackers (3 squares, 2 1/2” square) unsweetened tea • Snack Two: – turkey roll-up (1 -2 oz. ) – 4 or 5 olives – popcorn (3 c. , reduced fat microwave) – diet soft drink

More Snack Ideas • Snack Three: – 8 oz. artificially sweetened yogurt – handful of nuts (1/4 c. ) – Water with lemon • Snack Four: – hummus (1/3 c. ) – carrots (1/2 c. ) – herbal tea

Food Log • Write down what you eat • Write the date, time, amounts of food, mood, blood sugars, medicine • Try for a week • Look for patterns • Bring to your nutrition appointment • Recommend all patients meet with RD at least once
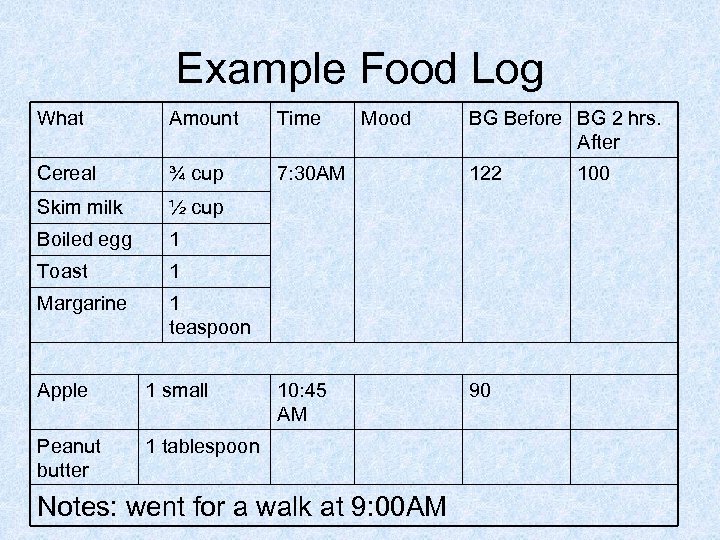
Example Food Log What Amount Time Cereal ¾ cup 7: 30 AM 122 Skim milk ½ cup Boiled egg 1 Toast 1 Margarine 1 teaspoon 10: 45 AM 90 Apple 1 small Peanut butter Mood 1 tablespoon Notes: went for a walk at 9: 00 AM BG Before BG 2 hrs. After 100

Stress and Coping

Learning Points • Know how stress or depression can affect blood glucose • Be able to identify/anticipate stressful situations • Be able to provide a solution for a stressful situation or change in routine

Stress and Coping • Social pressure from friends, family, church, work • What are some examples of situations where you are pressured to not take care of your diabetes?

What Stress Can Do • Too much stress can keep you from taking good care of yourself and your diabetes • Make other problems worse (blood sugars, blood pressure) • Lead to poor choices, poor planning • Keeps you in the “stress cycle”

Putting the Pieces Together: Social Situation You are attending a family birthday dinner at your sister’s house. Your sister, who takes pride in her cooking, has prepared a special meal with several courses. Most of the foods are combination dishes with sauces and gravies. After dinner, your sister personally hands you the dessert tray, insisting that you take some. She says, “I know several people with diabetes, and they eat anything. ”

Putting the Pieces Together: Social Situation 1. What are some ways to handle this situation? 2. What are some ways you can plan ahead for these special events? 3. What are other strategies for dealing with this type of situation?

Putting the Pieces Together: Social Situation You feel good about the way you have been following your diabetes care plan. You want to keep doing well, but the holidays are coming. You know that both your schedule and usual meal plan will be different. 1. What are strategies you can use so that you stay on track?

Putting the Pieces Together: Social Situation You usually take your evening insulin at about 5: 30 pm, eat dinner at 6: 00 pm, and have a snack before bedtime at about 10: 00 pm. Today you have been invited to a holiday dinner at a friend’s home at 8: 00 pm. *How might you handle this change in your schedule?

Putting the Pieces Together: Family Situation (con’t) 1. What problems might happen when you get home? 2. What are some ways to handle this situation?

Putting the Pieces Together: Family Situation You are a 50 -year old woman with newly diagnosed type 2 diabetes. You’ve decided to follow a meal plan because you want to lose one pound a week. You take insulin, but your doctor says if you can lose weight, there’s a chance you may not need to stay on it. Since you’ve always cooked all the meals for the family, your husband & sons expect you to keep doing so. Your sons have already told you they do not want to eat “rabbit food. ” Your husband has kept on eating his snack foods in front of you. He makes a point of telling you that you shouldn’t have “even a taste. ”

Changing Behavior

Setting Goals
Learning Point s • Be able to identify a personal goal for your diabetes care • Name key steps to help reach your goal

Goal Setting • S. M. A. R. T. Goals • Specific (what exactly are you going to do? ) • Measurable • Achievable • Realistic • Time-line

Goal Setting I want to eat more vegetables. SMART Goal: I will eat more vegetables at lunch. I will eat 1 extra serving a day. I will pack carrot sticks in my lunch.

Stress and Coping: Ten Commandments for Managing Stress • Thou shalt organize thyself – take better control of how you spend time & energy to better handle stress • Thou shalt control thy environment – get rid of stress or get help by controlling who & what you’re around

Stress and Coping: Ten Commandments for Managing Stress • Thou shalt love thyself – give yourself positive feedback – you’re a unique person doing the best you can • Thou shalt reward thyself – put leisure activities into your life – doing this will give you something to look forward to

Stress and Coping: Ten Commandments for Managing Stress • Thou shalt exercise – exercise at least 3 days per week for 15 -30 minutes – health & productivity depend on your body’s ability to bring oxygen & food into its cells • Thou shalt relax – get away from stress by focusing on – breathing & positive thoughts – ways to relax include dreaming, prayer & meditation, progressive relaxation, listening to music, & talking with friends & loved ones

Stress and Coping: Ten Commandments for Managing Stress • Thou shalt rest as regularly as possible – take breaks and sleep 7 -8 hours a night – there is only so much your mind can absorb at once • Thou shalt be aware of thyself – watch for stress signs like insomnia, headaches, anxiety, upset stomach, & cold/flu

Stress and Coping: Ten Commandments for Managing Stress • Thou shalt feed, thy body healthy food – eat a balanced diet so your body is well fueled – avoid foods high in calories, fat, & sugar – avoid using drugs or alcohol to deal with stress • Thou shalt Enjoy thyself! – happier people tend to live longer & have fewer health problems – look for the humor in life when times are tough

Resources Books: Diabetes Burnout Caring for the Diabetic Soul Diabetic Meals for $7 a day or Less Diabetic Cooking for One Websites: www. diabetes. org www. ncdiabetes. org www. americanheart. org www. mypyramid. gov Organizations: American Diabetes Association (1 -800 -DIABETES) North Carolina Diabetes Association (1 -877 -362 -2678)

Diabetes and Pregnancy Planning • Higher rates of miscarriage and birth defects with high blood sugars in mom • If not planning pregnancy, must use method of birth control • If planning pregnancy, get sugar under control first • Get weight under control with diet and exercise

Diabetes and Pregnancy Planning • Before getting pregnant – Get blood pressure checked – Get eyes checked – Exam of heart and blood vessels by your doctor – Have kidneys and thyroid checked by blood work

Gestational Diabetes • High blood sugar during pregnancy in otherwise non-diabetic person • Can cause large birthweight babies • Must tightly control sugar during pregnancy • Goes away after pregnancy, but likely occur in future pregnancies; many women go on to develop type 2 diabetes
f5c7cdd24cc959f677e097ca5c2f9f31.ppt