98dda151ffe19b2ee1c86d1f1e76b12a.ppt
- Количество слайдов: 73

Dementia/Delirium 2017 Denise Kresevic RN Ph. D, APN-BC FAAN Louis Stokes Cleveland VAMC University Hospitals Case Medical Center

Am I mostly normal ? • • Grocery list- left at home Enter a room and cant remember Just cant remember names Cant remember NPI #, OAARS # and all computer passwords • »

Normal/ Abnormal Normal Abnormal Occasional bad decision Loss of ability to do $ Miss date/day Occasional problem with words • Lose things occasionally • • Consistent bad choices Occasional missed payment Miss season/year Much difficulty with conversation • Often loses things cant retrace steps, blames others

What does dementia look like in everyday life? • • Can’t remember familiar recipes Lose things around the house Get lost in or going to familiar places Forget to pay bills or forget to mail bills Difficulty balancing checkbook Miss appointments / forget to take medication Usually don’t recognize there’s a problem May become paranoid, people taking things

What does dementia look like in everyday life? • • Decreased interest in activity or life – Apathy Increasingly confused as it becomes dark Hygiene / grooming may become worse Irritable, with reminders from family • • • Sleep disturbance Forget to eat or drink adequately Language problems (ex: Not native English) Cooking accidents / inability to fix things Personality Changes / Behavioral Changes

Dementia • - a syndrome characterized by progressive decline in multiple areas of cognitive function, which eventually produces significant deficits in ability selfcare and social and occupational performance.

Consequences Patients with dementia have difficulty: –identifying changes in health status –describing symptoms of comorbid conditions –asking clearly for pain relief –comprehending instructions –following directions for self care and safety They are more vulnerable to stress when making transitions in care Payments for care for 2012 are estimated to be: $200 Billion 7

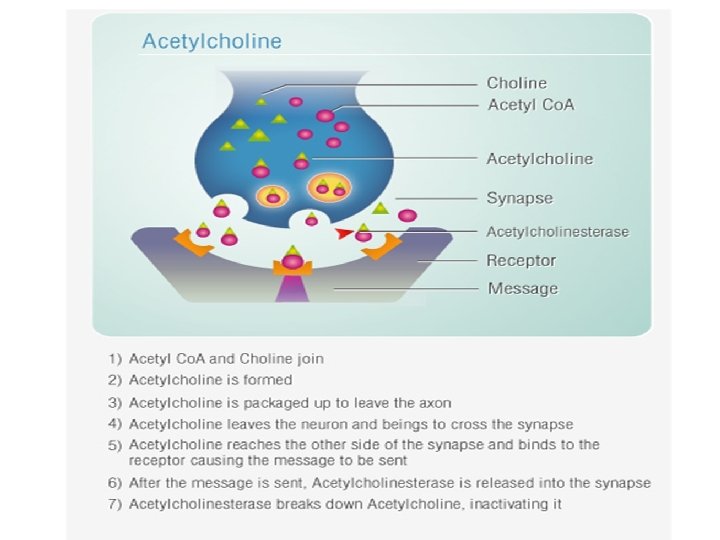
Theories of Etiology Amyloid Cascade Hypothesis • Amyloid Precursor Protein Error – produces plaques (genetic abnormality on Chromosome 21) –Studies suggest that about 25 percent of adults with Down syndrome over age 35 have symptoms of Alzheimer’s disease ; most over age 50 will develop AD 1. Plaques – toxic peptides Amyloid Beta – 40, 42, 43 (Aβ) extracellular 2. Aβ - 42 oligomers form / interfere with synaptic functioning 3. Plaques cause inflammation (microglia, astrocytes cytokines / free radicals 4. Plaques induce tangles causes Abnormal Tau Phosphorylation Microtubles convert to tangles within the neuron - intracellular 5. Cholinergic Neuronal dysfunction / loss spreads Apo-E – defect in the protein that binds to amyloid to remove it Dysfunction of Glutamate –Excitotoxicity –Follows in the later stages
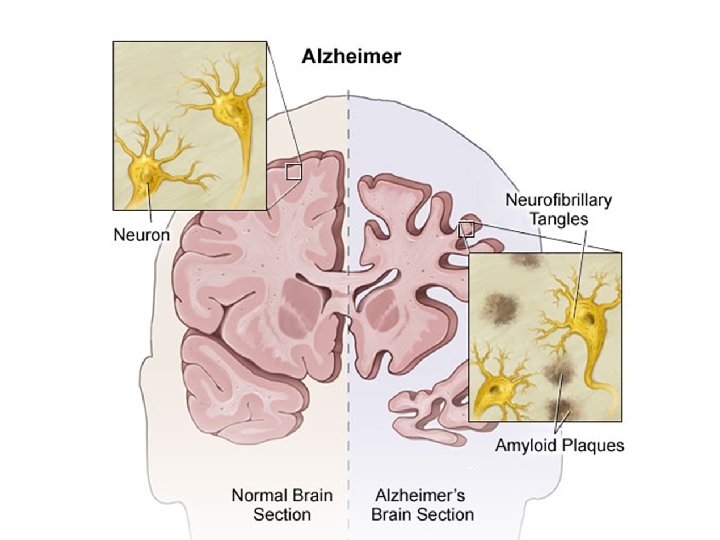

Dementia Characteristics • Impairs cognition -- primarily memory – but also language, insight, judgment, ability to plan • Affects ability to care for self, including managing own care • Causes behavioral and psychological problems • Creates strain for family caregivers 3

Medical History: Risk Factors • Cardiac / Vascular HTN (what’s bad for the heart is bad for the brain) • • Cerebrovascular, TBI falls Diabetes Parkinson’s, Multiple Sclerosis (neurodegenerative) Family History of Dementia (AD, ) Alcohol / Substance Abuse – Chronic Smoking / Obesity Low Folate / High Homocysteine

Dementia in DSM-V • Memory Impairment (ability to learn new or recall previously learned info is impaired) • Cognitive Disturbance a) Aphasia (language disturbance) b) Apraxia (impaired ability to carry out motor activities despite intact motor function) c) Agnosia (failure to recognize or identify objects despite intact sensory function) d) Disturbance in Executive Functioning: Driving • Both cause significant impairment in social or occupational functioning

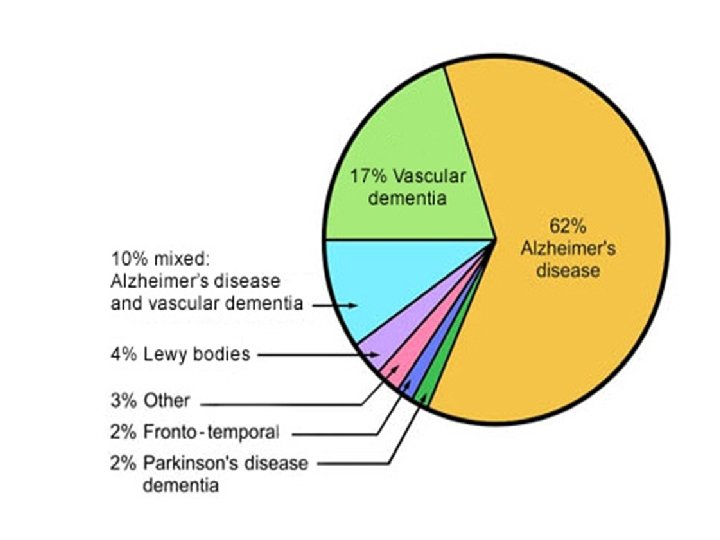
Types of Dementia • • • Alzheimer’s Type Vascular Dementia Lewy Body Dementia Frontotemporal Dementia Alcohol/Substance-Induced Dementia Parkinson’s Dementia Huntington’s Dementia HIV induced Dementia due to Creutzfeldt-Jakob Disease Dementia due to Head Trauma Dr. Alois Alzheimer
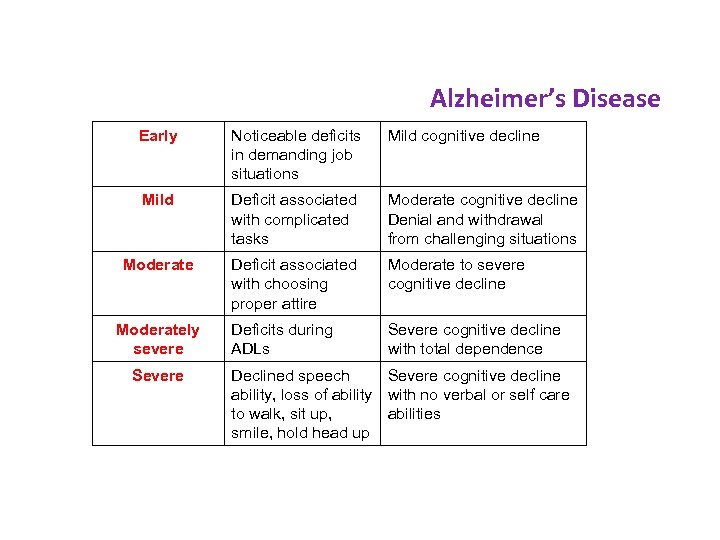
Alzheimer’s Disease Early Noticeable deficits in demanding job situations Mild cognitive decline Mild Deficit associated with complicated tasks Moderate cognitive decline Denial and withdrawal from challenging situations Moderate Deficit associated with choosing proper attire Moderate to severe cognitive decline Deficits during ADLs Severe cognitive decline with total dependence Moderately severe Severe Declined speech Severe cognitive decline ability, loss of ability with no verbal or self care to walk, sit up, abilities smile, hold head up 16

The Real World • Miss S. 72 years old has been followed for primary care HTN OA for several years • Retired teacher (was forced to retire) ex-nun • Vague history of anxiety • Lives with her sister for last 30 years • Comes to the office today at the insistence of her sister who is “very concerned” about her memory

Subjective Data • Forgets names, words, appointments, looses keys • HTN –Lisinopril 20 mg daily HCTZ BP 140/90 • Multi vitamin, Vitamin D 2000 U daily • No alcohol or tobacco • Negative CP DOE dizziness edema • OA Tylenal 650 mg 1 -2 times a day • Weight stable • Watches salt

More history for Miss S. • How long (several months maybe longer) • No urinary symptoms • Still driving – no tickets accidents – a few weeks ago took a “wrong turn” coming home from the movies • Able to balance check book ok • No other over the counter meds • No recent falls/trauma

Dementia History/Work-Up • • Medical History Family History Onset / Progression of Symptoms Areas of Dysfunction Behavioral Manifestations Affect or Personality Changes Medication Review / Reconciliation, Consider other causes for the patient’s symptoms before making conclusions

Medication Reconciliation • Anti-Cholinergic Load – Bladder Agents – TCA (pain, mood, sleep) – SSRI’s, Antipsychotics • Sleep Aids – Anti-histamines, hypnotics – Old supply Ativan • Benzodiazepines – May have been on for 20 years • Pain Medications – Narcotics

Cognitive Screening ? • • MMSE (Folstein) – no longer public domain Mo. CA (adjusts for education) Clock Drawing Test Trails Test A & B Verbal Fluency Geriatric Depression Scale Mini-Cog
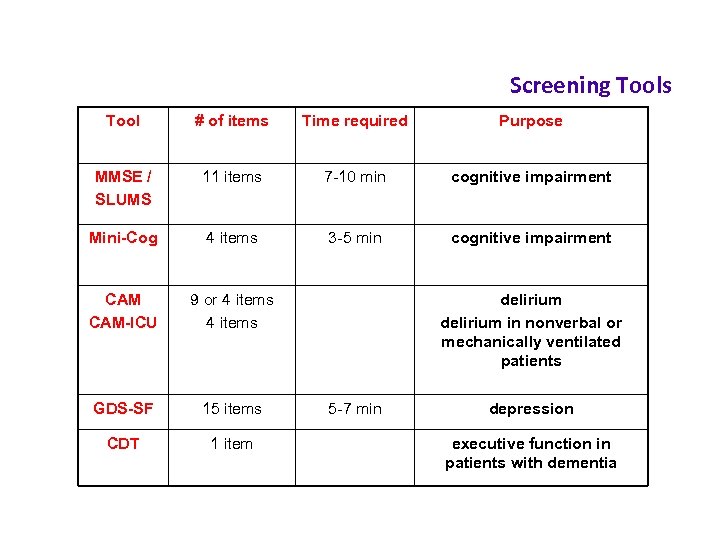
Screening Tools Tool # of items Time required Purpose MMSE / SLUMS 11 items 7 -10 min cognitive impairment Mini-Cog 4 items 3 -5 min cognitive impairment CAM-ICU 9 or 4 items GDS-SF 15 items CDT 1 item delirium in nonverbal or mechanically ventilated patients 5 -7 min depression executive function in patients with dementia 23

Cognitive Screening • • MMSE (Folstein) – no longer public domain Mo. CA (adjusts for education) Clock Drawing Test Trails Test A & B Verbal Fluency Geriatric Depression Scale Mini-Cog

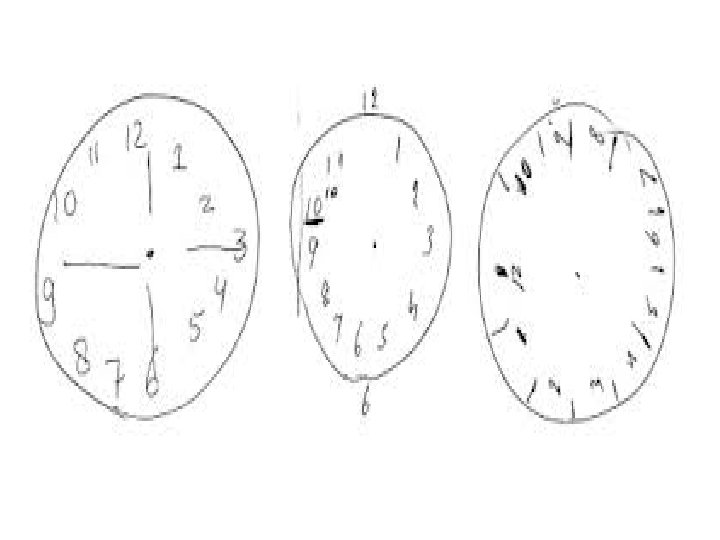
Clock Drawing Test (part of Mini Coag) • CDT – draw the face of a clock, put all the numbers in, then make it read 11: 10 – 4 point scoring method • • Circle All 12 numbers present Numbers in correct position Hands in correct position – 10 point scoring method
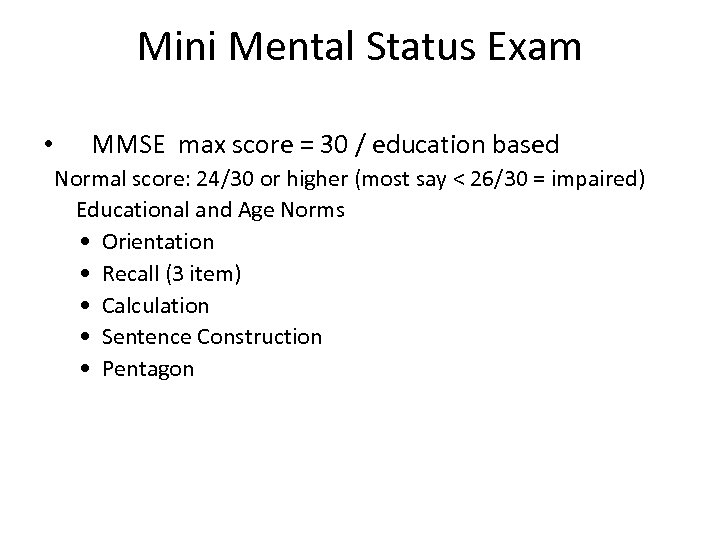

Mini Mental Status Exam • MMSE max score = 30 / education based Normal score: 24/30 or higher (most say < 26/30 = impaired) Educational and Age Norms • Orientation • Recall (3 item) • Calculation • Sentence Construction • Pentagon

Montreal Cognitive Assessment • Mo. CA < 26/30 = Mild Cognitive Impairment • 5 item recall • Sentence recall – Found to be more sensitive in detecting mild impairment in general population and in those with Parkinson’s Disease (NIH study) – Journal of the American Geriatric Society (2009), Feb (2), 304 -308 • www. mocatest. org


Depression • Single question-no • Geriatric Depression scale < 5 ( 2/15 wnl) • Likes to stay home, worries about bad things

Miss S. Physical Assessment • • Apical, postural BP slight elevation Hearing/vision ok Motor, ok gait, Romberg, no drift Minicog, abnormal clock/recall 1/3

Dementia Work-Up • Labwork: CBC, CMP, TSH, B-12, Folate, RPR, Homocysteine, drug levels /VDRL • Neuro-Imaging: CT of Head, MRI of Brain, PET scan • Cognitive Testing – per Psychologist, Neuropsychologist, Occupational Therapist / Speech Therapist • Cognitive Screening

Dementia Work-Up • Labwork: CBC, CMP, TSH, B-12, Folate, RPR, Homocysteine, drug levels • Neuro-Imaging: CT of Head, MRI of Brain, PET scan • Cognitive Testing – per Psychologist, Neuropsychologist, Occupational Therapist / Speech Therapist • Cognitive Screening/depresson screen

Vascular Dementia Diagnosis • No widely accepted neuropathological criteria established • Onset of cognitive decline may be sudden or progressive • Found in Pt’s with Stroke, Chronic HTN, Micro-Vascular Disease, Arteriosclerosis, amputations, CABG, other bypass procedures, DVT’s, SDH, Emboli, coag problems • May be Focal Deficits: based on location of lesion • Presents of abnormal vascular anatomy on CT of Head or MRI • Occupational Exposure: Repeated TBI (new concern) • Vascular Depression: Common – Sertraline most researched for treatment

Vascular Dementia • May result from genetic diseases, endocarditis (infection of a heart valve). • Or due to amyloid angiopathy (a process in which amyloid protein builds up in the brain's blood vessels, sometimes causing hemorrhagic or "bleeding" strokes) Adapted from slideshow found at: http: //www. emedicinehealth. com/slideshow_dementia/article_em. htm University Hospitals Harrington Heart and Vascular Institute
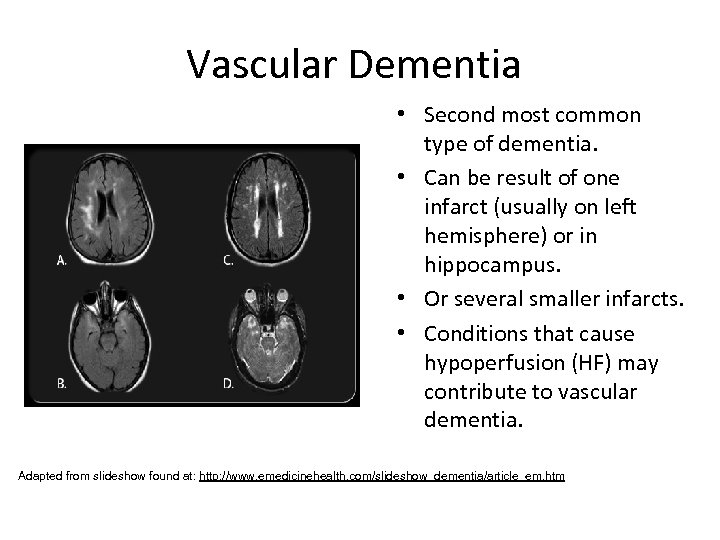
Vascular Dementia • Second most common type of dementia. • Can be result of one infarct (usually on left hemisphere) or in hippocampus. • Or several smaller infarcts. • Conditions that cause hypoperfusion (HF) may contribute to vascular dementia. Adapted from slideshow found at: http: //www. emedicinehealth. com/slideshow_dementia/article_em. htm
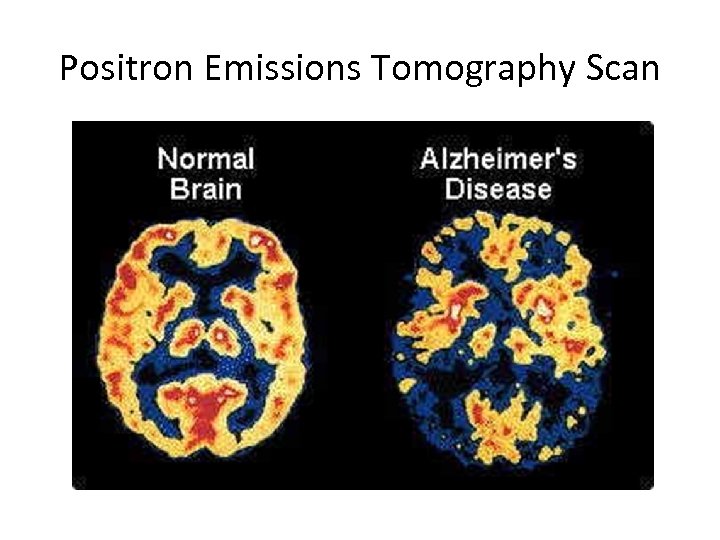
Positron Emissions Tomography Scan

Imaging Discussion/rationale for patient/family $ MRI-non contrast no gadolinium No contra indications r/o mass, hydrocephalus, old stokes, small vessel disease • Pet (research)? • • •

Plan for Miss. S. • • Labs (no VDRL) Stop Ativan (was taking 1 -2 week) Continue BP Tylenol current meds Sleep hygiene Education overview of MCI Dementia Wants to think about MRI, RTC 1 month

Dementia with Lewy Bodies Diagnosis • Cognitive changes with Parkinson features • Other signs of Autonomic Dysfunction – Syncope / falls – Unexplained loss of consciousness – Other psychotic symptoms – delusions/non-visual hallucinations

Dementia with Lewy Bodies Diagnosis • Core Features (2 are needed for dx) – Fluctuating cognition – Recurrent Visual Hallucinations – people/animals – Spontaneous signs of Parkinsonism • Suggestive Features – REM sleep behavior disorder – SEVERE NEUROLEPTIC SENSITIVITY – PET imaging decreased metabolism

Parkinson’s Dementia • ETIOLOGY • Abnormal protein: • Accumulates inside neurons of the substantia nigra. • This accumulation is called "alpha-synuclein" first described by a Professor Lewy • Lewy Body: Proteins are also found in the brain's neurons outside the deep brain structures, in the "thinking" parts of the brain in Parkinson's Disease Dementia and in Lewy body dementia.

Frontotemporal Dementia Diagnosis • Strong evidence of familial link – 5 genes identified • Effect younger population – Onset b/ 51 -63 yr – Can be Rapid Progression • Does not effect Cholinergic system, has effect on serotonergic system • Tau - toxic protein pathology
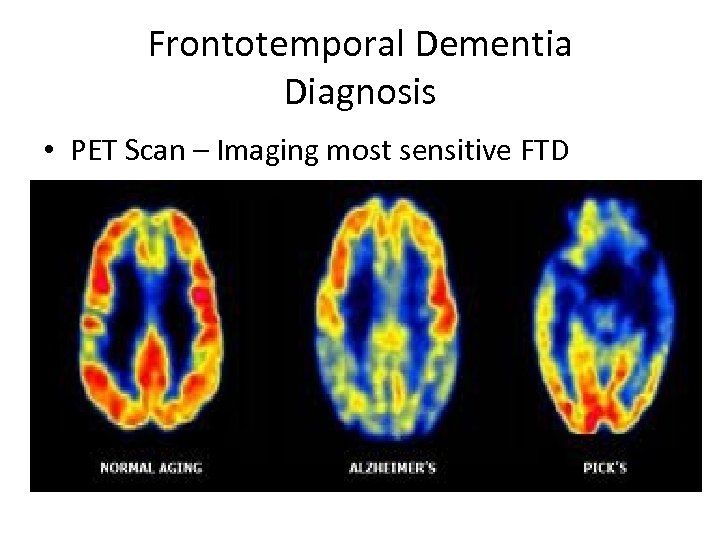
Frontotemporal Dementia Diagnosis • PET Scan – Imaging most sensitive FTD
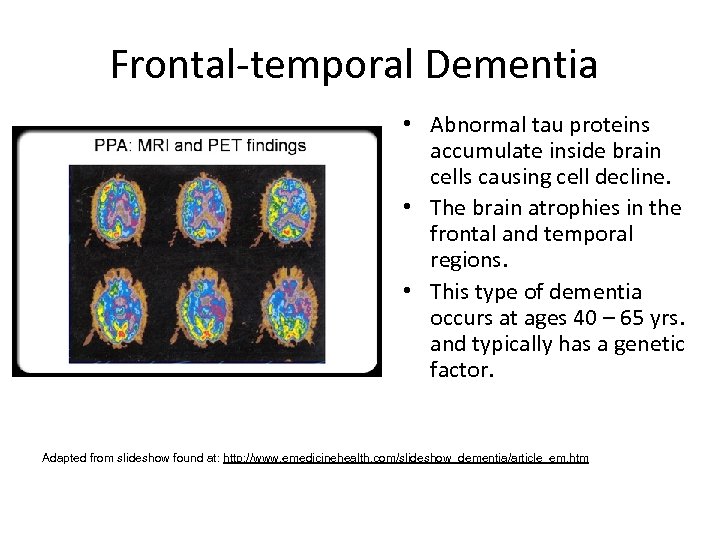
Frontal-temporal Dementia • Abnormal tau proteins accumulate inside brain cells causing cell decline. • The brain atrophies in the frontal and temporal regions. • This type of dementia occurs at ages 40 – 65 yrs. and typically has a genetic factor. Adapted from slideshow found at: http: //www. emedicinehealth. com/slideshow_dementia/article_em. htm

Frontotemporal Dementia Diagnosis • Insidious onset / gradual progression • May present with depression, apathy, aggression, personality changes, language deficits and disinhibition • Decline in social inter-personal conduct • Impairment in regulation of personal conduct (sexual inappropriateness) • Progressive Language Impairment • Emotional blunting • Loss of insight

Frontotemporal Lobe Dementia Treatment MOST DIFFICULT TO TREAT No FDA approved medications Target symptom management Trazadone/Nefazadone – some evidence of improved behaviors (start Trazadone 25 TID) • SSRI’s – some efficacy with irritability, anxiety, disinhibition • Mood Stabilizers – can be helpful • •

Medications for Alzheimer’s Type Dementia • Acetylcholinesterase Inhibitors (Ach. I’s) Donepezil (Aricept) all stages Indicated: All stages of Alzheimer’s Dementia • Initiate 5 mg daily x 4 wk; then increase 10 mg • Renal impairment leave at 5 mg daily • New Dose = 23 mg daily (sustained release) for Mod. Sev Stages (should be on 10 mg daily for at least 3 months first) • ½ life 70 hr; steady state in 15 days • Wt loss , night mares, bradycardia

Medications for Alzheimer’s Type Dementia Acetylcholinesterase Inhibitors • Rivastigmine (Exelon) –mild mod • Indicated for Parkinson’s Dementia • Indicate mod-sev Alzheimer’s Dementia • 1. 5 mg BID x 1 mo; 3 mg BID x 1 mo; 4. 5 mg BID x 1 mo; 6 mg BID (with largest meals of the day) • Patch 4. 6 mg/24 hr & 9. 5 mg/24 hr ( less GI) • No known CYP 450 enzyme interactions • No recommended hepatic / renal dosing

Medications for Alzheimer’s Type Dementia • Acetylcholinesterase Inhibitors • Galantamine (Razadyne) (formally Reminyl) (mild mod) • Indicated: mod-sev Alzheimer’s Dementia • 4 mg BID x 1 mo; 8 mg BID x 1 mo; 12 mg BID ER formulation – 8, 16, 24 mg daily ( q 4 wk) • Do not exceed 16 mg/day with hepatic/renal impairment • Metabolized by CYP 450 enzymes 2 D 6, 3 A 4 • Caution: Tagamet, Nizoral, EES, Paxil, NSAID’s, Anti. Cholinergic agents

Medications for Alzheimer’s Type Dementia N-methyl D-aspartate receptor antagonist • Memantine (Namenda) – 2004 • Indicated for Mod – Severe Alzheimer’s Dem. • Thought to interfere with Glutaminergic overstimulation (exitotoxicity) • Dosing: 5 mg daily x 1 wk; 5 mg BID x 1 wk; 5 mg qam & 10 mg qhs x 1 wk; target dose 10 mg BID • Severe Renal Impairment: Max dose 5 mg BID – EGFR < 60

Treatment all dementias Optimize function and quality of life and capitalize on remaining strengths. – Consider using complementary and alternative therapies – Don’t forget the obvious pain, discomfort, constipation, stimulation – Prevent excess disability – Support caregivers

Non-Pharm. Treatments • • • Non-Toxic Environment - calm / accepting / unclutter Daily Routine – structure is a good thing Locks on Doors / Prevent wandering Register with Alzheimer’s Association & local police Medic Alert ID Bracelet: “Memory Impaired” Put Contact Information in Wallet / Purse Driving: Assessment / hide keys / hide car Take over IADL’s / DPOA-HC Don’t argue with incorrect / paranoid statements Remind, Reassure, Redirect Not always necessary to Re-Orient distressing Encourage socialization

Miss S returns BP 130/80 apical Wt. down 2# Still anxious no ativan MRI vascular changes Labs unremarkable Dx mixed dementia mild Alzheimers ICD 331. 0 without behavior, vascular • ? Meds • • •

Mixed Dementia (AD & Vascular) • • No FDA approved Treatments Ach. I’s can be helpful Mementine found to be helpful Prevention of further vascular deterioration important

Meds • ACI not helpful in vascular dementia • ACI may be helpful in mixed will try for Miss S • Currently Miss S. behavior ok • Continue to monitor Depression

A sudden behavioral change • Sister leaves a phone message • “You have to help, she is terrible, screaming, crying wants to go home” • What is going on ? ? ?

Delirium • From the Greek word • “To be off the path” • Changes at the cellular level- neurotransmitter sites, anti cholinergic intoxication • Preventable • Difficult to detect • Superimposed on dementia

Delirium (Pathophysiology) Proposed Theories • Neurotransmitters (dopamine; gammaaminobutyric acid; acetylcholine) • Alteration in synthesis, release, inactivation resulting in excess dopamine, acetylcholine depletion • Additional Neurotransmitter imbalances: serotonin imbalance, endorphin hyperfunction, increased noradrenergic 59 activity

Delirium: DSM 5 Disturbance of attention, develops over short time, change from baseline, accompanied by changes in cognitive domain, such as memory, disorientation, language, perception, that cannot be accounted for by pre -existing or other neurocognitive disorders; • occurs in context of severely reduced level of arousal • • APA, 2013
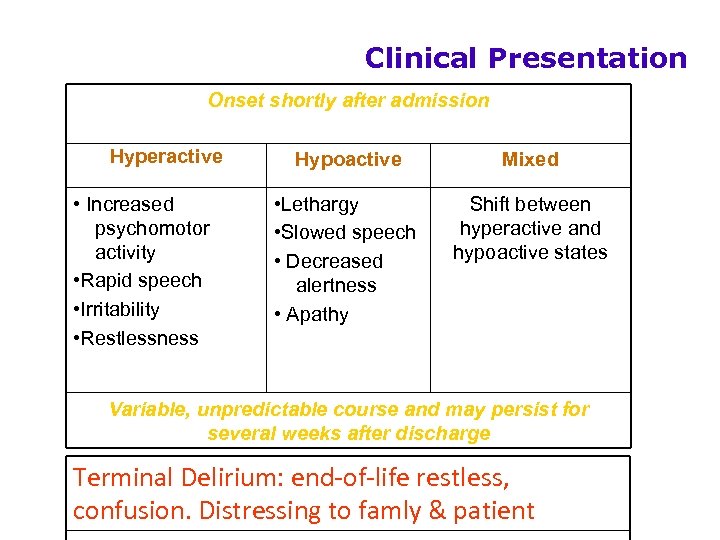

Clinical Presentation Onset shortly after admission Hyperactive • Increased psychomotor activity • Rapid speech • Irritability • Restlessness Hypoactive Mixed • Lethargy • Slowed speech • Decreased alertness • Apathy Shift between hyperactive and hypoactive states Variable, unpredictable course and may persist for several weeks after discharge Terminal Delirium: end-of-life restless, confusion. Distressing to famly & patient 61

Long-term outcomes • One year mortality rates: 35 -40% (Moran et al. Aust J Hosp Pharm. 2001; 31: 35 -40) • Functional decline • Long term cognitive decline* • New nursing home placement *Many patients never return to baseline Witlox et al. JAMA 2010; 304; 443 -451 62

CONFUSION ASSESSMENT METHOD • CAM originally developed by Inouye and Foreman • Refined by Ely for ICU (CAM-ICU) Brief CAM • • • Can maintain eye contact Inattention-SAVE A HAART Months of year -6 forward/back Follow commands Hold up 2 fingers Questions

Delirium Management D – DRUGS! medications E – Environmental changes L – Lack of drugs (withdrawal: ETOH, benzos, SSRI/SNRI) I – Infection, immobility, iatrogenic events R – Restraints, reduced sensory input I – Intracranial (CVA, bleed/SDH, meningitis, post-ictal) U – Urinary and fecal retention, urinary catheter M – Metabolic (dehydration, hypoxia, electrolytes, uremia, ammonia, thyroid, MALNUTRITION) PAIN SLEEP DEPRIVATION SURGERY 1. Avoid anticholinergics, bzns, most sleep aides and antipsychotics 2. Tempered reorientation, daytime stimulation, avoid unnecessary room changes and nighttime interruptions, encourage visits 3. Limit Foley catheters, avoid restraints, early PT/OT 4. Encourage eyeglasses and hearing aides 5. Bowel regimen (especially if pt is on narcotics) 6. Hydration 7. Nutrition 8. Treat pain

Dementia, Delirium • • • Low grade fever + urine culture Treat Bactrim Things get a little better Then 6 months later- has stopped driving, now losing weight, not sleeping, crying

Impact on Family Caregiver • Negatively affects family caregivers due to: – – Intensity of needed care Emotional upset, isolation, neglect of own needs Changes in the relationship with the person with dementia Lengthy and progressive course of the disease • Results in: – Caregiver stress and strain – Depression – Poor medical health 4

Treatment Address ethical issues – Ethical issues relevant to patients with dementia include: • Defining decision-making capacity and identifying situations that require substitute decision-making, • Addressing situations related to everyday life (e. g. , patient preferences, and socially questionable behaviors), and • Discussing possible limitations on medical interventions such as hospitalization and CPR

Artificial Nutrition and Hydration • It is a common ethical issue in patients with dementia • Opinions vary as whether an extraordinary measure or routine care • Short-term use of enteral nutrition may help to show if artificial nutrition and hydration will prevent further decline • Not a “one time” decision

Miss S. • “ No aggressive treatments” • But willing to try anti depressant (Mirtazapine)

Miss S. 2 years later • • Progressed to severe behavior Referred to Psychiatry, admitted Started on anti psychotics (EKG QT ok) Developed bowel obstruction Admitted to a nursing home Aspirated Died with hospice a few weeks later

Recent Dementia Research Evidenced. Based Treatment • Mental Exercise • Physical Exercise • Socialization PROTECTIVE FACTORS • Don’t Smoke • Education / Higher Socioeconomic levels • Little Alcohol daily (1 -2 / day)

Evidenced Based Interventions AHRQ (Alzheimer’s) • • + cognitive training, exercise + - B 12 - omega 3 - Vitamin D (low strength) - Vitamin E (women) - BP Rx , statin (low strength) - ASA

Goals of Care • People with dementia are individuals with same needs values as other adults • Small changes can make big differences • Treat the disease • Treat the symptoms Be alert for delirium • Support the patient • Support the caregiver • Something can always be done
98dda151ffe19b2ee1c86d1f1e76b12a.ppt