a3dad01358a70bdde5a2600ea9ed4cad.ppt
- Количество слайдов: 53

Cystic Fibrosis Microbiology: Away Day October 2017 Dr David Garner Consultant Microbiologist Frimley Park Hospital www. microbiologynutsandbolts. co. uk

Aims & Objectives • Discuss current issues in CF microbiology • To understand how a sputum sample is processed • To know how to interpret a sputum result • To understand why antibiotic sensitivities are of limited use in CF • To know the problem microorganisms in CF • To be aware of the infection control issues in CF • To make microbiology “interesting” for all of you! www. microbiologynutsandbolts. co. uk

Mark • 27 years old with cystic fibrosis • Initial problems as a child with bacteria such as: – Streptococcus pneumoniae – Haemophilus influenzae – Staphylococcus aureus • More recent problems with: – Pseudomonas aeruginosa • Admitted with an exacerbation of his cystic fibrosis • What are you going to do? www. microbiologynutsandbolts. co. uk

Mark • • • Check what he has grown before Admit him to a side room on the CF unit Send a sputum sample to Microbiology Intensify physiotherapy Start antibiotics Review compliance with other medications www. microbiologynutsandbolts. co. uk

Requesting sputum cultures? • In ICE select “Respiratory and AAFB Acute www. microbiologynutsandbolts. co. uk
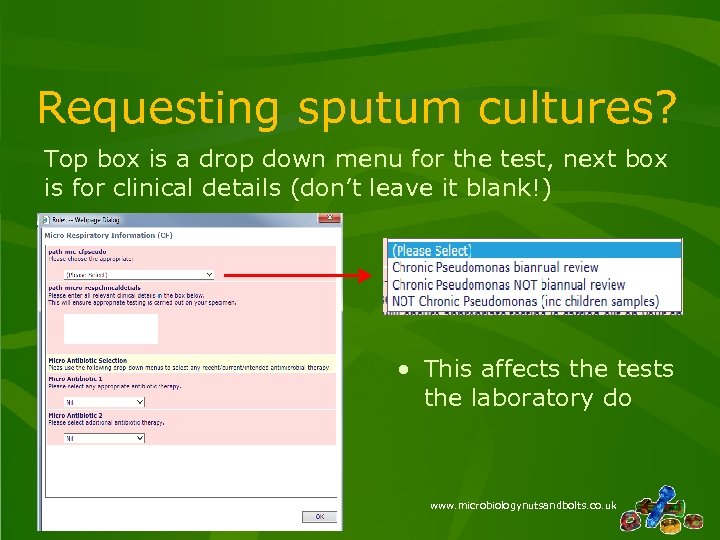
Requesting sputum cultures? Top box is a drop down menu for the test, next box is for clinical details (don’t leave it blank!) • This affects the tests the laboratory do www. microbiologynutsandbolts. co. uk
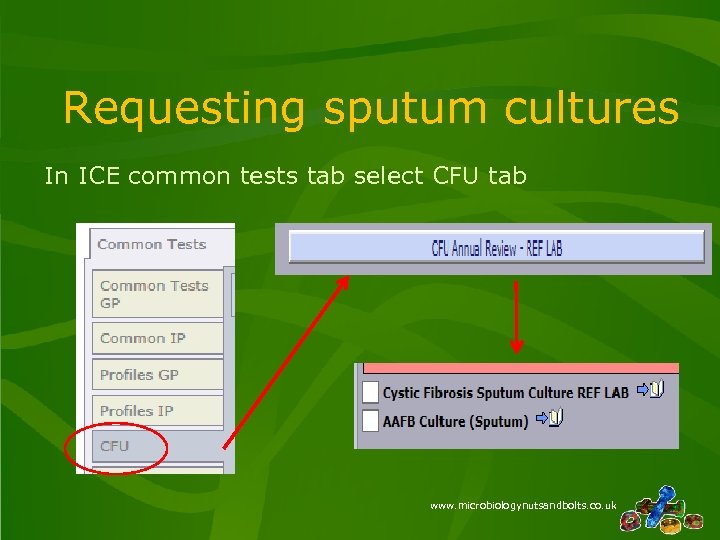
Requesting sputum cultures In ICE common tests tab select CFU tab www. microbiologynutsandbolts. co. uk

What tests does the lab do? • Chronic Pseudomonas Biannual review – sent to Ref. Lab for Typing and MIC testing – Only select twice yearly (the reference laboratory will not test samples which are sent more frequently) • Chronic pseudomonas NOT annual review – Identification of Pseudomonas, no sensitivities • NOT chronic pseudomonas – Full identification and sensitivities of microorganisms www. microbiologynutsandbolts. co. uk

What does a lab look like? www. microbiologynutsandbolts. co. uk

What does a lab look like? www. microbiologynutsandbolts. co. uk

What does a lab look like? www. microbiologynutsandbolts. co. uk

Respiratory laboratory www. microbiologynutsandbolts. co. uk

Respiratory laboratory www. microbiologynutsandbolts. co. uk

Culture: how is sputum processed? • Plated to mixture of selective and non-selective agar depending on clinical details – E. g. Cystic Fibrosis = B. cepacia agar • Incubated for 48 hours before reporting • Sensitivities take a further 24 -48 hours • Total time 48 -96 hours after receipt. www. microbiologynutsandbolts. co. uk

How to interpret a sputum result? • Appearance – Mucoid, Salivary, Purulent, Blood Stained… • Microscopy – Gram’s stain, Ziehl Neelsen (ZN) stain… • Culture – Is the organism consistent with the clinical picture? www. microbiologynutsandbolts. co. uk

Appearance of sputum • Salivary – Spit not phlegm, risk of contamination • Mucoid – Upper respiratory tract specimen, no evidence of inflammation • Purulent – Pus, indicates inflammation • Blood stained – May indicate infection www. microbiologynutsandbolts. co. uk
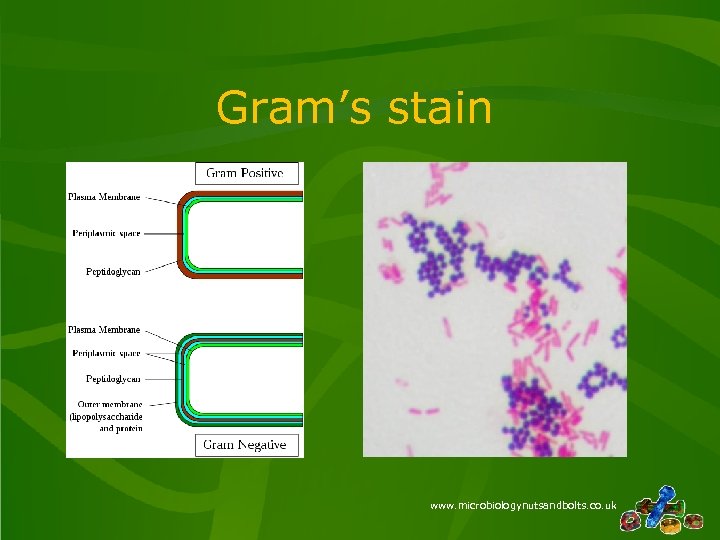
Gram’s stain www. microbiologynutsandbolts. co. uk
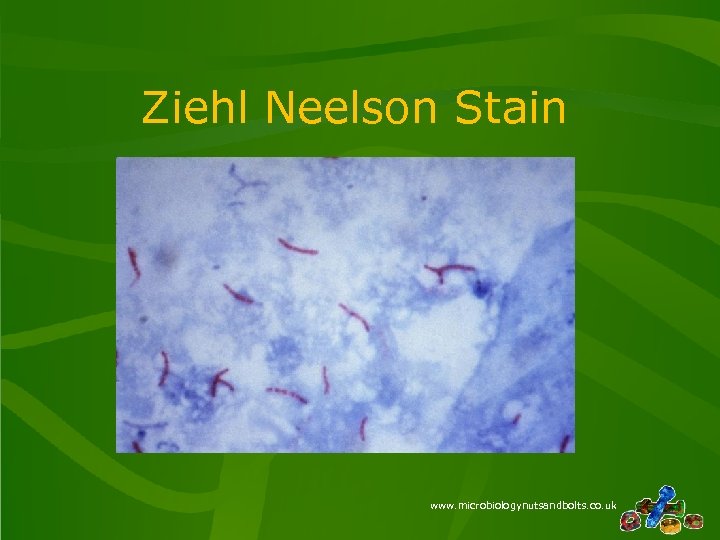
Ziehl Neelson Stain www. microbiologynutsandbolts. co. uk
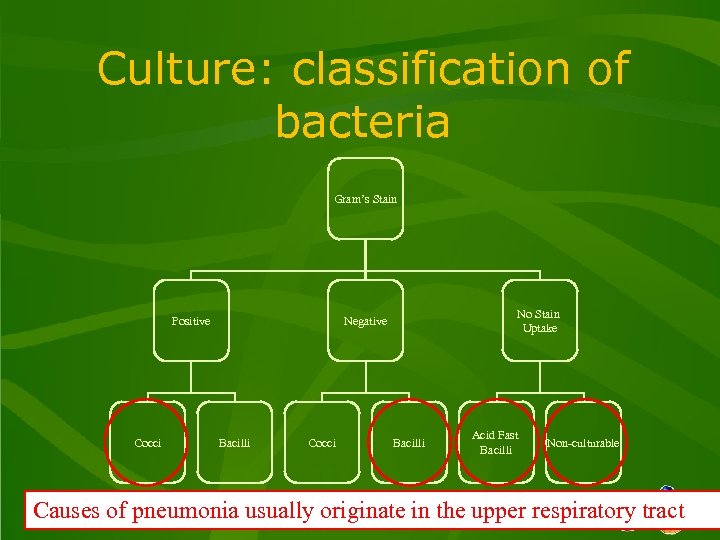
Culture: classification of bacteria Gram’s Stain Positive Cocci No Stain Uptake Negative Bacilli Cocci Bacilli Acid Fast Bacilli Non-culturable Causes of pneumonia usually originate inwww. microbiologynutsandbolts. co. uk tract the upper respiratory

Classification of Grampositive cocci www. microbiologynutsandbolts. co. uk
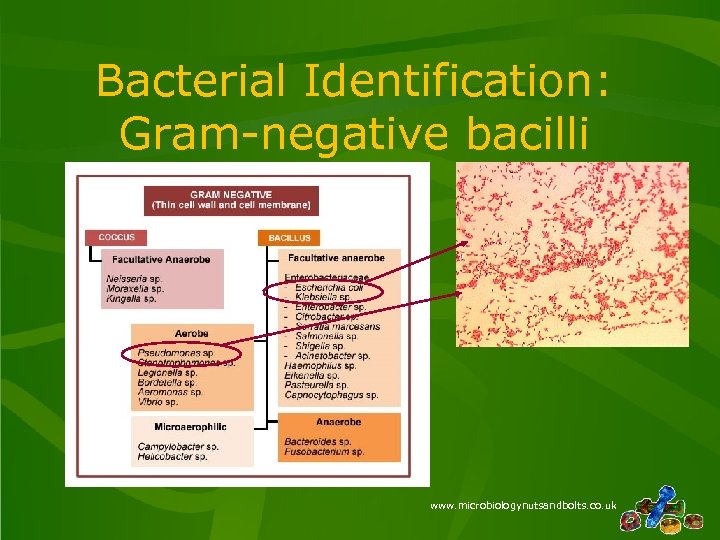
Bacterial Identification: Gram-negative bacilli www. microbiologynutsandbolts. co. uk

Normal Flora www. microbiologynutsandbolts. co. uk

CF “Normal” Flora Eventually also: MDR P. aeruginosa, Burkholderia spp. , Stenotrophomas maltophilia, Achromobacter spp. , Non-tuberculous mycobacteria…! www. microbiologynutsandbolts. co. uk

Factors Affecting Normal Flora • Exposure to antibiotics provides a selective pressure – e. g. previous antibiotics for CAP • Increased antimicrobial resistant organisms in the environment – e. g. Pseudomonas in critical care units • Easily transmissible organisms – e. g. Staphylococcus aureus • Failure to clear colonising bacteria – E. g. Pseudomonas aeruginosa • Immunosuppressants – e. g. steroids www. microbiologynutsandbolts. co. uk

Do patients need antibiotics? • CF patients can get the same types of infection everyone gets e. g. UTI, tonsillitis, cellulitis • Viruses do not respond to antibacterials! – However there antivirals e. g. aciclovir, oseltamivir • The presence of bacteria does not necessarily mean there is an infection! – Bacteria colonise, such as upper respiratory tract, surgical wounds, ulcers www. microbiologynutsandbolts. co. uk

How do you choose an antibiotic? • What are the common micro-organisms causing the infection? • Is the antibiotic active against the common micro-organisms? • Do I need a bactericidal antibiotic rather than bacteriostatic? • Does the antibiotic get into the site of infection in adequate amounts? • How much antibiotic do I need to give? • What route do I need to use to give the antibiotic? www. microbiologynutsandbolts. co. uk

In reality… …you choose what worked before… www. microbiologynutsandbolts. co. uk
Why do exacerbations of cystic fibrosis occur? www. microbiologynutsandbolts. co. uk

Exacerbation of CF • Caused by: – New bacteria – New strain of bacteria or change in phenotype – Non-cultured bacteria or viruses • Increased exacerbations decreased survival • Decreased symptoms increased FEV 1 • Risk factors for treatment failure: – – Female Low BMI Cepacia Time delay to starting treatment www. microbiologynutsandbolts. co. uk

Treatment of Exacerbation • High doses of Beta-lactam PLUS aminoglycoside – Choice of antibiotic • Identification of organism • Previous successful therapy • Allergies – Susceptibility testing not helpful • Too variable • Not predictive of clinical response • No value in synergy testing – Duration • Good lung function = 7 -14 days • Poor lung function = longer (guided by response) www. microbiologynutsandbolts. co. uk

Why sensitivities don’t help At least 4 different appearances of P. aeruginosa www. microbiologynutsandbolts. co. uk

Why sensitivities don’t help At least 3 different sensitivity patterns for each appearance of P. aeruginosa Is this 12 different bacteria? www. microbiologynutsandbolts. co. uk

Why sensitivities don’t help Genetic finger printing shows only 1 P. aeruginosa = clever bug!!!! www. microbiologynutsandbolts. co. uk

Problem microorganisms www. microbiologynutsandbolts. co. uk

Mycobacterium abscessus www. microbiologynutsandbolts. co. uk

Who gets M. abscessus? • Rates are increasing: highest in 11 -20 year olds • Transmission – Indirect patient to patient – Surface contamination – Airborne? Pseudomonas detectable in air 3 hours after room vacated Vitamin B 12 deficiency Azithromycin Decreased autophagy Decreased macrophage activity Increased M. abscessus www. microbiologynutsandbolts. co. uk

Why does it matter? • Faster rate of decline in lung function (FEV 1) – 2. 5% vs. 1. 6% per year • Absolute contraindication to transplant (unless able to eradicate? ) • Infection control restrictions • Stigmatisation? • Difficult to diagnose in patients on antibiotics that interfere with culture e. g. macrolides, aminoglycosides www. microbiologynutsandbolts. co. uk

Combination therapy • Approx. 20% response (off Abx and culture negative) • Intensive phase (1 -3 months) – Clarithromycin (if sensitive) – PLUS IV Amikacin – PLUS Tigecycline AND Imipenem • Continuation phase (until culture negative for 12 months on therapy!) – Clarithromycin (if sensitive) – PLUS nebulised Amikacin – PLUS 1 -3 of Minocycline OR Clofazamine OR Linezolid OR Moxifloxacin OR Cotrimoxazole www. microbiologynutsandbolts. co. uk

Rhinovirus www. microbiologynutsandbolts. co. uk

Rhinovirus • 1 in 3 patients have a virus in an exacerbation • Two fold increased risk of exacerbation – Less effect on FEV 1 than other causes • • Associated with increased Abx use Mainly found in summer and autumn Increase bacterial release from biofilms Individual response to Rhinovirus – Immune mediated? – Worse with type A than B or C • Persists for ≥ 2 months in some patients www. microbiologynutsandbolts. co. uk

Burkholderia cepacia complex www. microbiologynutsandbolts. co. uk

B. cepacia complex • • 2010 = 17 species 2014 = 18 species (B. pseudomultivorans) Previous Genomovars now have distinct names Most important – B. cepacia – B. multivorans – B. cenocepacia (contraindication to transplant) • Mortality – 2003 >50% at 5 years (Manchester, Vancouver) – 2010 <10% at 5 years (Prague) – Why? • Not part of the normal human flora www. microbiologynutsandbolts. co. uk

Epidemiology • Infection control precautions work – Prevent spread from patient-to-patient • Global epidemic B. cepacia strains – How do they spread internationally? • B. multivorans – Increasingly common – Rare patient-to-patient transmission – Can be replaced by B. cepacia (but not the reverse) www. microbiologynutsandbolts. co. uk

Non B. cepacia complex strains • B. gladioli – 3 rd most common strain in USA – Clinical significance unclear www. microbiologynutsandbolts. co. uk

Infection Control www. microbiologynutsandbolts. co. uk

Transmission • Main problems P. aeruginosa and B. cepacia complex • Routes – Environment-to-patient – Patient-to-patient • Mainly droplet spread – Within few metres • Potential droplet nuclei spread – Remain suspended in air up to 3 hours after patient leaves www. microbiologynutsandbolts. co. uk

Recommendations • Surveillance – Identify organisms – Refer for PFGE • Standard precautions – For patients as well as staff – Consider H 2 O 2 but no evidence • Segregate ALL patients – No common areas – Only patients from same household can share • No B. cepacia complex or M. abscessus patients in CF wards or outpatient clinics www. microbiologynutsandbolts. co. uk

M. abscessus • CF Trust UK and American CF Guidelines • Separate clinic in different building • No shared equipment AT ALL! • No admission to CF unit – Negative pressure side-room – Sporicidal cleaning then leave room empty for 24 hours www. microbiologynutsandbolts. co. uk

Recommendations • Gloves and aprons for contact with patient and their environment (UK CF Trust) – 20% of HCW contamination from environment • No routine use of masks for inpatients • Ventilation – Wait 60 minutes before final disinfection of room after patient discharged – Negative pressure room www. microbiologynutsandbolts. co. uk

After all that… Mark • Previous results checked – No epidemic P. aeruginosa, B. cepacia complex, M. abscessus • Admitted to CF unit • Sputum sample sent (requested as exacerbation of CF not chronic Pseud) • Started on Meropenem PLUS Tobramycin • Sputum result confirmed P. aeruginosa sensitive to Meropenem and Tobramycin • Mark improved quickly and went home after a week in hospital www. microbiologynutsandbolts. co. uk

www. microbiologynutsandbolts. co. uk

Conclusion • Infections in cystic fibrosis are very difficult to manage • Multiple factors cause problems: – – – Patient factors Allergies Antibiotic resistance Laboratory issues Odd bacteria! • Successful management requires team work! www. microbiologynutsandbolts. co. uk

Any Questions? Available to buy on www. microbiologynutsandbolts. co. uk
a3dad01358a70bdde5a2600ea9ed4cad.ppt