ea3b1d611937944b35bfe5c00db0bdb8.ppt
- Количество слайдов: 55
 Critical Challenges in Osteoporosis— From Patient Presentation To Therapeutic Decision Points: An Overview of Issues, Concepts, and Clinical Strategies SCREEN AND INTERVENE Evidence-Basis for Patient Screening and Risk Stratification: Principles for Approaching a Broad Population of Patients at Risk for Osteoporosis
Critical Challenges in Osteoporosis— From Patient Presentation To Therapeutic Decision Points: An Overview of Issues, Concepts, and Clinical Strategies SCREEN AND INTERVENE Evidence-Basis for Patient Screening and Risk Stratification: Principles for Approaching a Broad Population of Patients at Risk for Osteoporosis
 Program Contents Definitions ► Epidemiology ► Pathophysiology ► Clinical Features ► Diagnosis ► Therapy ►
Program Contents Definitions ► Epidemiology ► Pathophysiology ► Clinical Features ► Diagnosis ► Therapy ►
 Definition Osteoporosis is defined as a skeletal disorder characterized by compromised bone strength predisposing a person to increased risk of fracture 1 1. NIH Consensus Development Panel on Osteoporosis Prevention, Diagnosis, and Therapy. JAMA. 2001; 285: 785 -795.
Definition Osteoporosis is defined as a skeletal disorder characterized by compromised bone strength predisposing a person to increased risk of fracture 1 1. NIH Consensus Development Panel on Osteoporosis Prevention, Diagnosis, and Therapy. JAMA. 2001; 285: 785 -795.
 Key Features of Osteoporosis ► Bone involution in both sexes with aging and a superimposed acceleration of bone loss in women after the menopause ► Low bone mass coupled with micro-architectural deterioration leading to enhanced bone fragility and ultimately fracture
Key Features of Osteoporosis ► Bone involution in both sexes with aging and a superimposed acceleration of bone loss in women after the menopause ► Low bone mass coupled with micro-architectural deterioration leading to enhanced bone fragility and ultimately fracture
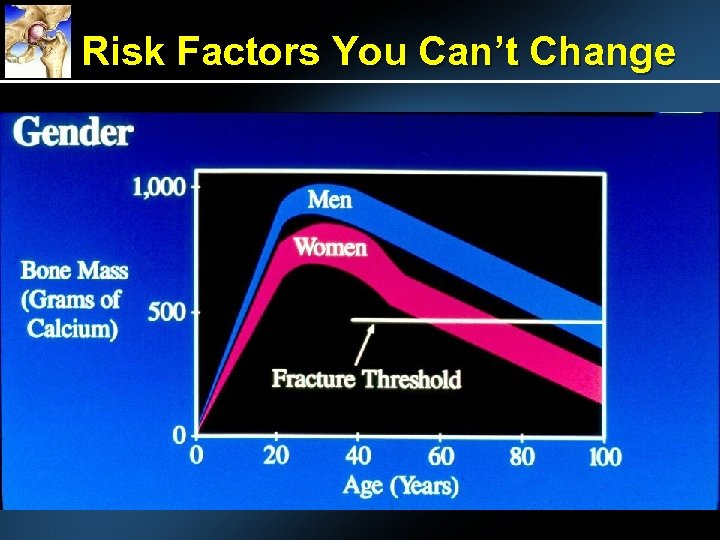 Risk Factors You Can’t Change
Risk Factors You Can’t Change
 Contents ► Epidemiology Prevalence Incidence Sites Cost Status of care
Contents ► Epidemiology Prevalence Incidence Sites Cost Status of care
 Prevalence ► 44 million Americans have or are at risk of osteoporosis 55% of all people ages 50 years 10 million have osteoporosis 34 million more have low bone mass 50% of women aged 50 years will experience a fracture in their lifetime ► Prevalence is expected to increase with the growth of the elderly population ►
Prevalence ► 44 million Americans have or are at risk of osteoporosis 55% of all people ages 50 years 10 million have osteoporosis 34 million more have low bone mass 50% of women aged 50 years will experience a fracture in their lifetime ► Prevalence is expected to increase with the growth of the elderly population ►
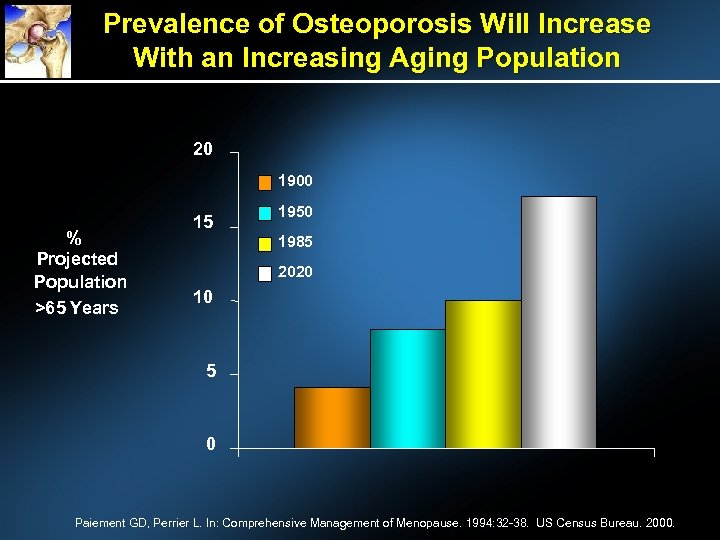 Prevalence of Osteoporosis Will Increase With an Increasing Aging Population 20 1900 % Projected Population >65 Years 15 1950 1985 2020 10 5 0 Paiement GD, Perrier L. In: Comprehensive Management of Menopause. 1994: 32 -38. US Census Bureau. 2000.
Prevalence of Osteoporosis Will Increase With an Increasing Aging Population 20 1900 % Projected Population >65 Years 15 1950 1985 2020 10 5 0 Paiement GD, Perrier L. In: Comprehensive Management of Menopause. 1994: 32 -38. US Census Bureau. 2000.
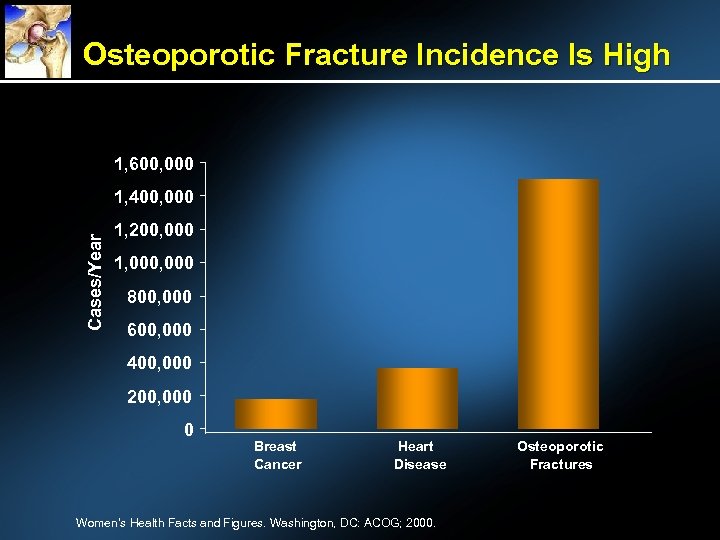 Osteoporotic Fracture Incidence Is High 1, 600, 000 Cases/Year 1, 400, 000 1, 200, 000 1, 000 800, 000 600, 000 400, 000 200, 000 0 Breast Cancer Heart Disease Women’s Health Facts and Figures. Washington, DC: ACOG; 2000. Osteoporotic Fractures
Osteoporotic Fracture Incidence Is High 1, 600, 000 Cases/Year 1, 400, 000 1, 200, 000 1, 000 800, 000 600, 000 400, 000 200, 000 0 Breast Cancer Heart Disease Women’s Health Facts and Figures. Washington, DC: ACOG; 2000. Osteoporotic Fractures
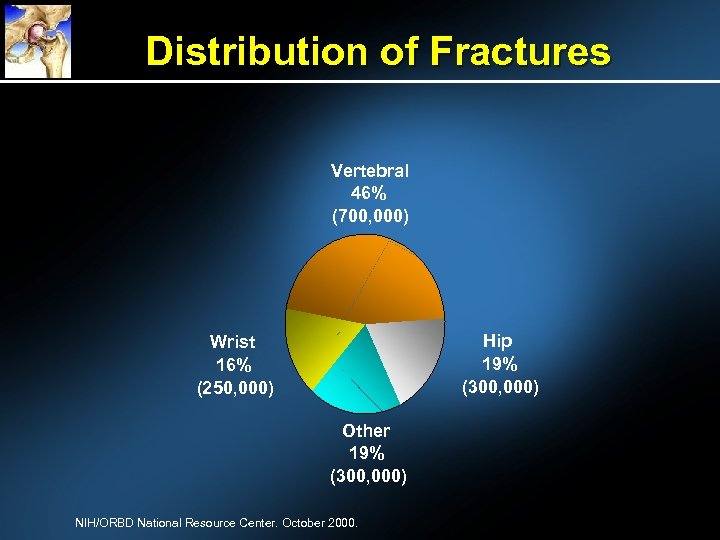 Distribution of Fractures Vertebral 46% (700, 000) Hip 19% (300, 000) Wrist 16% (250, 000) Other 19% (300, 000) NIH/ORBD National Resource Center. October 2000.
Distribution of Fractures Vertebral 46% (700, 000) Hip 19% (300, 000) Wrist 16% (250, 000) Other 19% (300, 000) NIH/ORBD National Resource Center. October 2000.
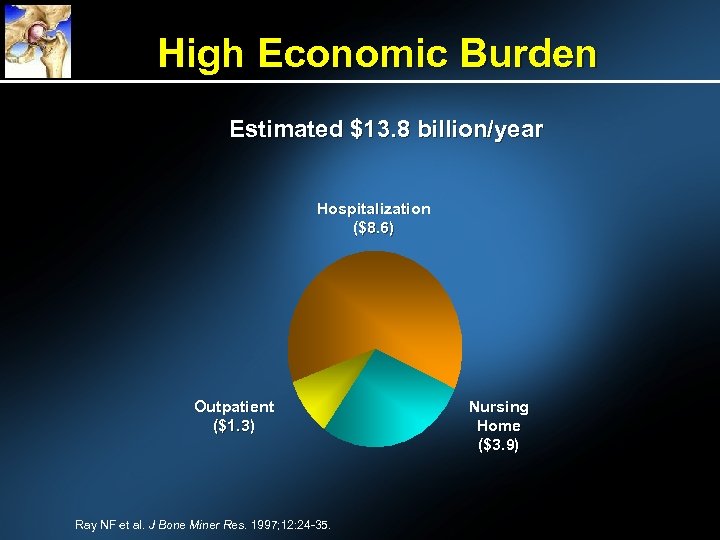 High Economic Burden Estimated $13. 8 billion/year Hospitalization ($8. 6) Outpatient ($1. 3) Ray NF et al. J Bone Miner Res. 1997; 12: 24 -35. Nursing Home ($3. 9)
High Economic Burden Estimated $13. 8 billion/year Hospitalization ($8. 6) Outpatient ($1. 3) Ray NF et al. J Bone Miner Res. 1997; 12: 24 -35. Nursing Home ($3. 9)
 Current Status of Care ► 3% to 5% of hip fracture patients are diagnosed for osteoporosis and treated ► 3% of wrist fracture patients receive BMD testing ► Only 12% of vertebral fractures are diagnosed and 2% are treated Freedman KB et al. J Bone Joint Surg Am. 2000; 82: 1063 -1070. Gehlbach SH et al. Osteoporosis Int. 2000; 11: 577 -582. Wiktorowicz ME. J Bone Miner Res. 1997; 12: S 252.
Current Status of Care ► 3% to 5% of hip fracture patients are diagnosed for osteoporosis and treated ► 3% of wrist fracture patients receive BMD testing ► Only 12% of vertebral fractures are diagnosed and 2% are treated Freedman KB et al. J Bone Joint Surg Am. 2000; 82: 1063 -1070. Gehlbach SH et al. Osteoporosis Int. 2000; 11: 577 -582. Wiktorowicz ME. J Bone Miner Res. 1997; 12: S 252.
 Content ► Pathophysiology Bone Remodeling Types of Osteoporosis
Content ► Pathophysiology Bone Remodeling Types of Osteoporosis
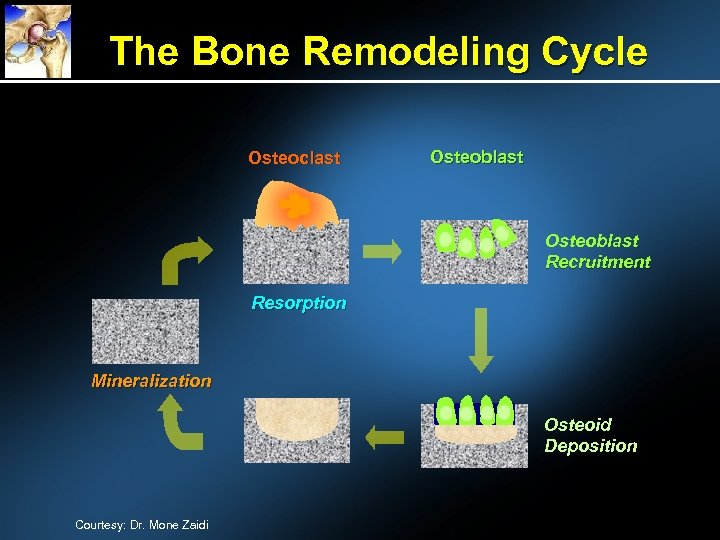 The Bone Remodeling Cycle Osteoclast Osteoblast Recruitment Resorption Mineralization Osteoid Deposition Courtesy: Dr. Mone Zaidi
The Bone Remodeling Cycle Osteoclast Osteoblast Recruitment Resorption Mineralization Osteoid Deposition Courtesy: Dr. Mone Zaidi
 Disordered Bone Remodeling as the Cause of Osteoporosis ► High Remodeling Hypogonadal (including post-menopausal) Hyperparathyroidism Hyperthyroidism Others ► Low Remodeling Involutional (Aging) Glucocorticoids (high dose) HIV
Disordered Bone Remodeling as the Cause of Osteoporosis ► High Remodeling Hypogonadal (including post-menopausal) Hyperparathyroidism Hyperthyroidism Others ► Low Remodeling Involutional (Aging) Glucocorticoids (high dose) HIV
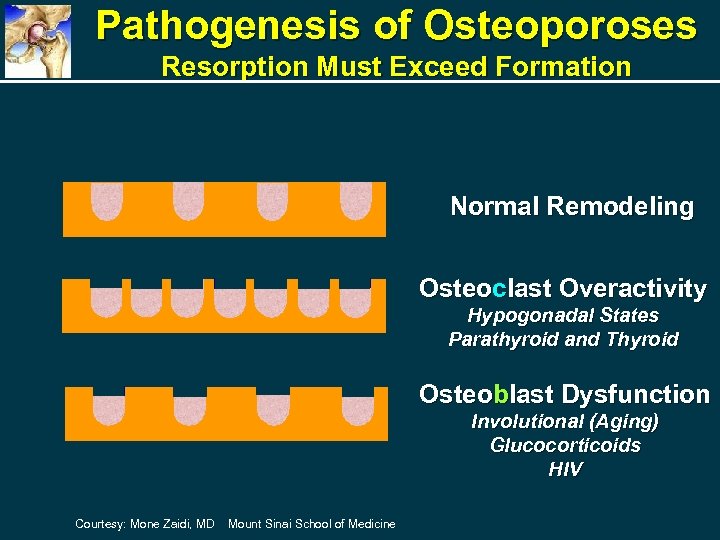 Pathogenesis of Osteoporoses Resorption Must Exceed Formation Normal Remodeling Osteoclast Overactivity Hypogonadal States Parathyroid and Thyroid Osteoblast Dysfunction Involutional (Aging) Glucocorticoids HIV Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
Pathogenesis of Osteoporoses Resorption Must Exceed Formation Normal Remodeling Osteoclast Overactivity Hypogonadal States Parathyroid and Thyroid Osteoblast Dysfunction Involutional (Aging) Glucocorticoids HIV Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
 Content ► Clinical Features Vertebral Fractures Non-Vertebral Fractures Risk Stratification
Content ► Clinical Features Vertebral Fractures Non-Vertebral Fractures Risk Stratification
 Vertebral Fractures ► Most common fractures (46%) ► Insidious ► Progressive ► Often unrecognized ► Associated with – Deformity, height loss, back pain – Morbidity and mortality ► Predict future vertebral and non- vertebral fractures
Vertebral Fractures ► Most common fractures (46%) ► Insidious ► Progressive ► Often unrecognized ► Associated with – Deformity, height loss, back pain – Morbidity and mortality ► Predict future vertebral and non- vertebral fractures
 Non. Vertebral Fractures ► Entire skeleton can be involved – Wrist – Ankle – Pelvis – Humerus – Rib – Others ► Associated with significant disability
Non. Vertebral Fractures ► Entire skeleton can be involved – Wrist – Ankle – Pelvis – Humerus – Rib – Others ► Associated with significant disability
 Hip Fracture ► Most serious clinical event ► Morbidity is high – 50% do not regain independence – 50% do not regain previous mobility ► Mortality is high – 1 in 5 patients die within 1 year ► Patients not treated for osteoporosis NIH Consensus Development Panel. JAMA. 2001; 285: 785 -795.
Hip Fracture ► Most serious clinical event ► Morbidity is high – 50% do not regain independence – 50% do not regain previous mobility ► Mortality is high – 1 in 5 patients die within 1 year ► Patients not treated for osteoporosis NIH Consensus Development Panel. JAMA. 2001; 285: 785 -795.
 Risk of Fracture All postmenopausal women with the following: Low BMD ► Fracture after 50 years ► Age 65 years ► Maternal history of fracture after 50 years ► Low body weight ( 125 lb) ► Smoking ► Corticosteroid use ► Other secondary causes ► Black DM et al. Osteoporosis Int. 2001; 12: 519 -528.
Risk of Fracture All postmenopausal women with the following: Low BMD ► Fracture after 50 years ► Age 65 years ► Maternal history of fracture after 50 years ► Low body weight ( 125 lb) ► Smoking ► Corticosteroid use ► Other secondary causes ► Black DM et al. Osteoporosis Int. 2001; 12: 519 -528.
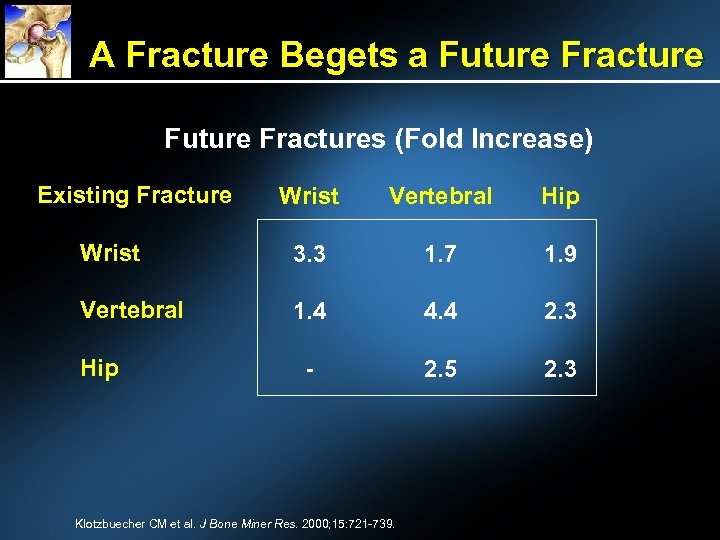 A Fracture Begets a Future Fractures (Fold Increase) Existing Fracture Wrist Vertebral Hip Wrist 3. 3 1. 7 1. 9 Vertebral 1. 4 4. 4 2. 3 - 2. 5 2. 3 Hip Klotzbuecher CM et al. J Bone Miner Res. 2000; 15: 721 -739.
A Fracture Begets a Future Fractures (Fold Increase) Existing Fracture Wrist Vertebral Hip Wrist 3. 3 1. 7 1. 9 Vertebral 1. 4 4. 4 2. 3 - 2. 5 2. 3 Hip Klotzbuecher CM et al. J Bone Miner Res. 2000; 15: 721 -739.
 Fracture Stratification Key Points ► Main risk factors – Low BMD – Presence of a fracture after 50 years ► Risk for fracture increases – With number of risk factors – With each subsequent fracture
Fracture Stratification Key Points ► Main risk factors – Low BMD – Presence of a fracture after 50 years ► Risk for fracture increases – With number of risk factors – With each subsequent fracture
 Content ► Diagnosis Clinical Assessment Diagnostic Criteria Bone Densitometry
Content ► Diagnosis Clinical Assessment Diagnostic Criteria Bone Densitometry
 Clinical Evaluation ► History – Risk factor assessment – Medical history – Family history – Social history (smoking, alcohol) – Evaluation of fall risk ► Physical – Height loss >1. 5 inches – Kyphosis ► Tests – BMD – X-ray of thoracic/lumbar spine – Bone turnover markers – Laboratory tests as necessary AACE Guidelines. Endocr Pract. 2001; 7: 293 -312.
Clinical Evaluation ► History – Risk factor assessment – Medical history – Family history – Social history (smoking, alcohol) – Evaluation of fall risk ► Physical – Height loss >1. 5 inches – Kyphosis ► Tests – BMD – X-ray of thoracic/lumbar spine – Bone turnover markers – Laboratory tests as necessary AACE Guidelines. Endocr Pract. 2001; 7: 293 -312.
 Kyphotic vs. Non-Kyphotic The Kyphotic Woman ► Likely has osteoporosis and vertebral fractures ► Confirmatory spinal x-ray for diagnosis ► Baseline BMD The Non-Kyphotic Woman ► Spinal x-ray or DXA if height loss >1. 5 inches ► Atraumatic vertebral fractures = osteoporosis a
Kyphotic vs. Non-Kyphotic The Kyphotic Woman ► Likely has osteoporosis and vertebral fractures ► Confirmatory spinal x-ray for diagnosis ► Baseline BMD The Non-Kyphotic Woman ► Spinal x-ray or DXA if height loss >1. 5 inches ► Atraumatic vertebral fractures = osteoporosis a
 Diagnosis BMD Criteria: Low T-Score Non-BMD Criteria: Fragility Fracture
Diagnosis BMD Criteria: Low T-Score Non-BMD Criteria: Fragility Fracture
 WHO Diagnostic Criteria The WHO Study Group. Geneva, 1994 T-Score* Classification > -1. 0 Normal -1. 0 to -2. 5 Osteopenia < -2. 5 or lower Osteoporosis < -2. 5 + fracture Severe osteoporosis *T-score = number of standard deviations (SDs) below or above the peak bone mass in young adults.
WHO Diagnostic Criteria The WHO Study Group. Geneva, 1994 T-Score* Classification > -1. 0 Normal -1. 0 to -2. 5 Osteopenia < -2. 5 or lower Osteoporosis < -2. 5 + fracture Severe osteoporosis *T-score = number of standard deviations (SDs) below or above the peak bone mass in young adults.
 Techniques Diagnosis Risk Assessment/ Research Central dual energy xray absorptiometry (DXA) ► Gold standard ► WHO criteria applied ►Peripheral DXA (p. DXA) National Osteoporosis Foundation. Washington, DC; 1999. ►Ultrasound ►Quantitative computed tomography (QCT)
Techniques Diagnosis Risk Assessment/ Research Central dual energy xray absorptiometry (DXA) ► Gold standard ► WHO criteria applied ►Peripheral DXA (p. DXA) National Osteoporosis Foundation. Washington, DC; 1999. ►Ultrasound ►Quantitative computed tomography (QCT)
 Central vs Peripheral DXA Central DXA Peripheral DXA Establish or confirm diagnosis ► Assess fracture risk ► Follow up ► Enhance patient compliance ► Different from WHO ► T-score criteria ► Fracture risk assessment in elderly with low T-scores
Central vs Peripheral DXA Central DXA Peripheral DXA Establish or confirm diagnosis ► Assess fracture risk ► Follow up ► Enhance patient compliance ► Different from WHO ► T-score criteria ► Fracture risk assessment in elderly with low T-scores
 Content ► Therapeutic Considerations Mode of Action Anti-resorptive Agents Anabolic Agents Bisphonate Failure Efficacy Testing
Content ► Therapeutic Considerations Mode of Action Anti-resorptive Agents Anabolic Agents Bisphonate Failure Efficacy Testing
 Goals for Therapy ► Fracture prevention ► Stabilize or increase bone mass ► Provide tolerability and longterm safety ► Ensure compliance and adherence
Goals for Therapy ► Fracture prevention ► Stabilize or increase bone mass ► Provide tolerability and longterm safety ► Ensure compliance and adherence
 Nonpharmacologic Approaches ► Calcium intake – Diet and/or supplementation: 1200 mg/day ► Vitamin D supplementation – Diagnose and treat deficiency/insufficiency – Supplement: 400 -800 IU/day ► Regular load-bearing and muscle- strengthening exercise (no weight lifting if BMD in spine is low) ► Fall prevention advice ► Home safety evaluation
Nonpharmacologic Approaches ► Calcium intake – Diet and/or supplementation: 1200 mg/day ► Vitamin D supplementation – Diagnose and treat deficiency/insufficiency – Supplement: 400 -800 IU/day ► Regular load-bearing and muscle- strengthening exercise (no weight lifting if BMD in spine is low) ► Fall prevention advice ► Home safety evaluation
 Medications FDA-Approved Prevention Treatment Hormone replacement Yes No Calcitonin (Miacalcin®) Raloxifene (Evista®) No Yes Yes Alendronate (Fosamax®) Risedronate (Actonel®) Yes Yes Ibandronate (Boniva®) Ibandronate Injection (Boniva®) Parathyroid hormone (Forteo®) Yes Yes *Not considered.
Medications FDA-Approved Prevention Treatment Hormone replacement Yes No Calcitonin (Miacalcin®) Raloxifene (Evista®) No Yes Yes Alendronate (Fosamax®) Risedronate (Actonel®) Yes Yes Ibandronate (Boniva®) Ibandronate Injection (Boniva®) Parathyroid hormone (Forteo®) Yes Yes *Not considered.
 Osteoporosis Therapeutics Decrease Resorption ► Bisphonates ► Estrogen ► Raloxifene ► Calcitonin Enhance Formation ► Parathyroid Hormone
Osteoporosis Therapeutics Decrease Resorption ► Bisphonates ► Estrogen ► Raloxifene ► Calcitonin Enhance Formation ► Parathyroid Hormone
 Anti-Resorptive Versus Anabolic Anti-Resorptive High Turnover Bone Loss Low Turnover Bone Loss PTH - Anabolic Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
Anti-Resorptive Versus Anabolic Anti-Resorptive High Turnover Bone Loss Low Turnover Bone Loss PTH - Anabolic Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
 PTH Mode of Delivery = Bone Activity Intermittent versus Continuous = Osteoblastic versus Osteoclastic = Formation versus Resorption = Bone Gain versus Bone Loss Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
PTH Mode of Delivery = Bone Activity Intermittent versus Continuous = Osteoblastic versus Osteoclastic = Formation versus Resorption = Bone Gain versus Bone Loss Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
 PTH – Anabolic Action Receptor Binding and Signal Transduction Increased Osteoblast Survival Enhanced Osteoblast Differentiation Net Increase in Number and Activity of Bone-Forming Osteoblasts
PTH – Anabolic Action Receptor Binding and Signal Transduction Increased Osteoblast Survival Enhanced Osteoblast Differentiation Net Increase in Number and Activity of Bone-Forming Osteoblasts
 Calcitonin Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
Calcitonin Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
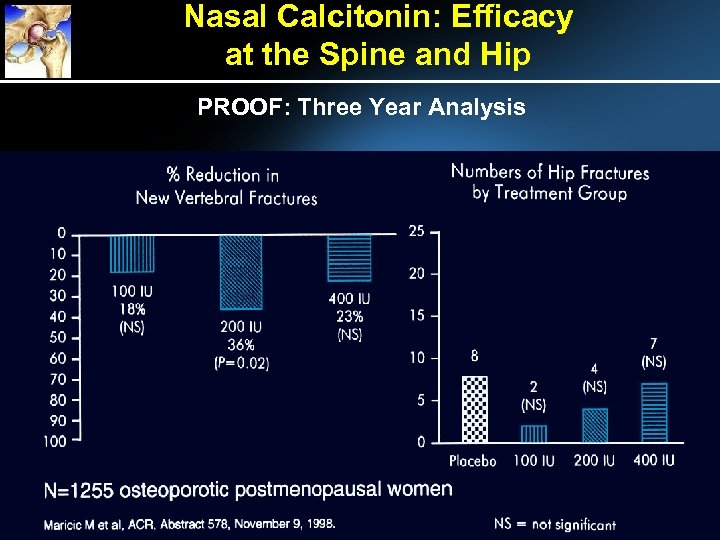 Nasal Calcitonin: Efficacy at the Spine and Hip PROOF: Three Year Analysis
Nasal Calcitonin: Efficacy at the Spine and Hip PROOF: Three Year Analysis
 Estrogen and Raloxifene ► ► Reduce the birth (genesis) of new osteoclasts from bone marrow Does not inhibit the activity of mature resorbing osteoclasts Osteoclast birth increases exponentially to a peak within the first few years of the menopausal transition Maximum bio-efficacy in early menopause and declines with age and disease severity/fractures Zaidi, M. , et. al. (2001) Journal of Bone and Mineral Research.
Estrogen and Raloxifene ► ► Reduce the birth (genesis) of new osteoclasts from bone marrow Does not inhibit the activity of mature resorbing osteoclasts Osteoclast birth increases exponentially to a peak within the first few years of the menopausal transition Maximum bio-efficacy in early menopause and declines with age and disease severity/fractures Zaidi, M. , et. al. (2001) Journal of Bone and Mineral Research.
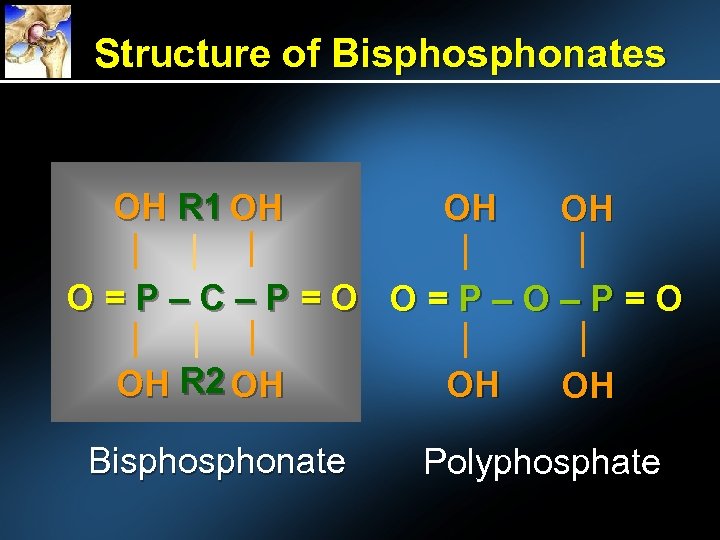 Structure of Bisphonates OH R 1 OH OH OH O=P–C–P=O O=P–O–P=O OH R 2 OH Bisphonate OH OH Polyphosphate
Structure of Bisphonates OH R 1 OH OH OH O=P–C–P=O O=P–O–P=O OH R 2 OH Bisphonate OH OH Polyphosphate
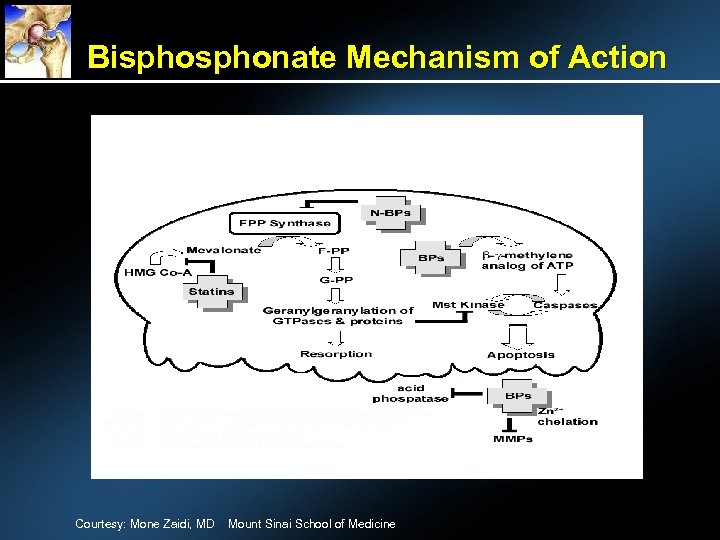 Bisphonate Mechanism of Action Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
Bisphonate Mechanism of Action Courtesy: Mone Zaidi, MD Mount Sinai School of Medicine
 Possible Causes of Poor Adherence? Lack of positive reinforcement? Osteoporosis eclipsed by other chronic conditions? Poor patient education? POOR ADHERENCE Concern about side effects? Complex dosing guidelines? Disruption to daily routine? (less frequent dosing)
Possible Causes of Poor Adherence? Lack of positive reinforcement? Osteoporosis eclipsed by other chronic conditions? Poor patient education? POOR ADHERENCE Concern about side effects? Complex dosing guidelines? Disruption to daily routine? (less frequent dosing)
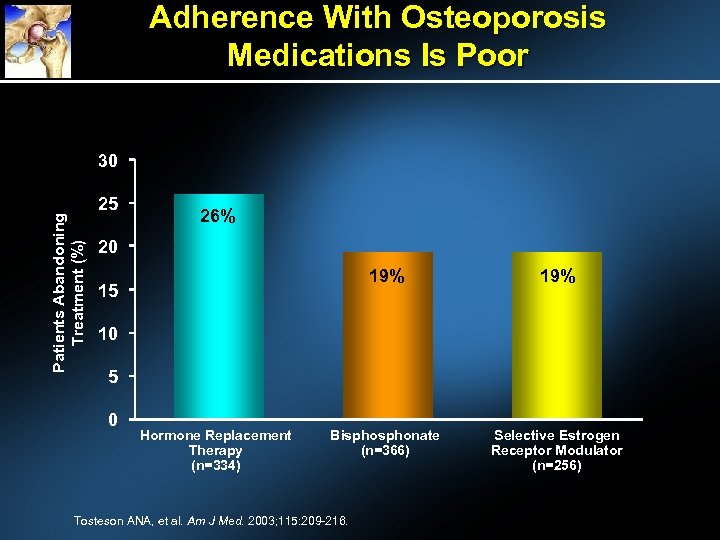 Adherence With Osteoporosis Medications Is Poor Patients Abandoning Treatment (%) 30 25 26% 20 19% Bisphonate (n=366) Selective Estrogen Receptor Modulator (n=256) 15 10 5 0 Hormone Replacement Therapy (n=334) Tosteson ANA, et al. Am J Med. 2003; 115: 209 -216.
Adherence With Osteoporosis Medications Is Poor Patients Abandoning Treatment (%) 30 25 26% 20 19% Bisphonate (n=366) Selective Estrogen Receptor Modulator (n=256) 15 10 5 0 Hormone Replacement Therapy (n=334) Tosteson ANA, et al. Am J Med. 2003; 115: 209 -216.
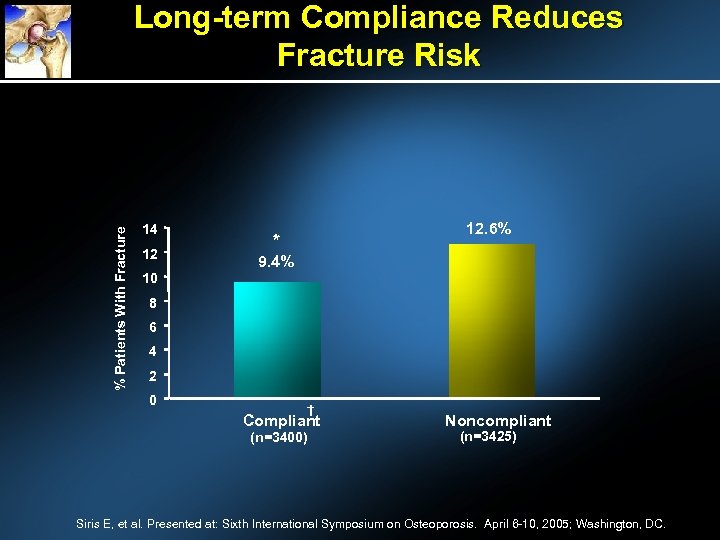 % Patients With Fracture Long-term Compliance Reduces Fracture Risk 14 12 12. 6% * 9. 4% 10 8 6 4 2 0 † Compliant (n=3400) Noncompliant (n=3425) Siris E, et al. Presented at: Sixth International Symposium on Osteoporosis. April 6 -10, 2005; Washington, DC.
% Patients With Fracture Long-term Compliance Reduces Fracture Risk 14 12 12. 6% * 9. 4% 10 8 6 4 2 0 † Compliant (n=3400) Noncompliant (n=3425) Siris E, et al. Presented at: Sixth International Symposium on Osteoporosis. April 6 -10, 2005; Washington, DC.
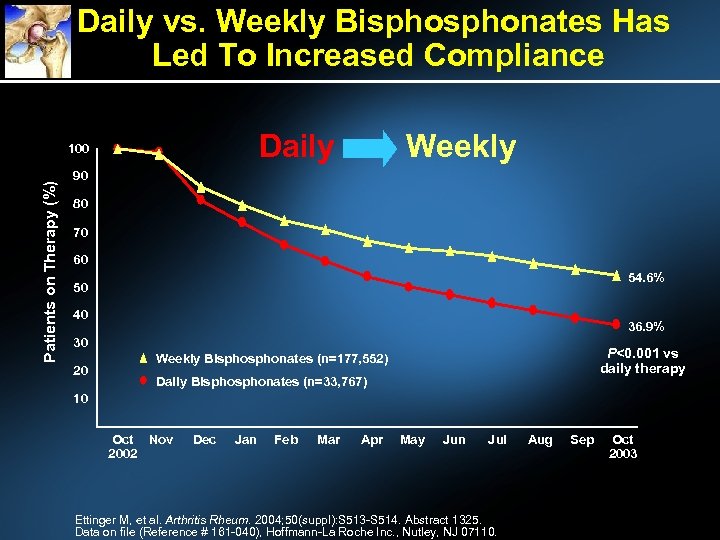 Daily vs. Weekly Bisphonates Has Led To Increased Compliance Daily Patients on Therapy (%) 100 Weekly 90 80 70 60 54. 6% 50 40 36. 9% 30 20 P<0. 001 vs daily therapy Weekly Bisphonates (n=177, 552) Daily Bisphonates (n=33, 767) 10 Oct Nov 2002 Dec Jan Feb Mar Apr May Jun Jul Ettinger M, et al. Arthritis Rheum. 2004; 50(suppl): S 513 -S 514. Abstract 1325. Data on file (Reference # 161 -040), Hoffmann-La Roche Inc. , Nutley, NJ 07110. Aug Sep Oct 2003
Daily vs. Weekly Bisphonates Has Led To Increased Compliance Daily Patients on Therapy (%) 100 Weekly 90 80 70 60 54. 6% 50 40 36. 9% 30 20 P<0. 001 vs daily therapy Weekly Bisphonates (n=177, 552) Daily Bisphonates (n=33, 767) 10 Oct Nov 2002 Dec Jan Feb Mar Apr May Jun Jul Ettinger M, et al. Arthritis Rheum. 2004; 50(suppl): S 513 -S 514. Abstract 1325. Data on file (Reference # 161 -040), Hoffmann-La Roche Inc. , Nutley, NJ 07110. Aug Sep Oct 2003
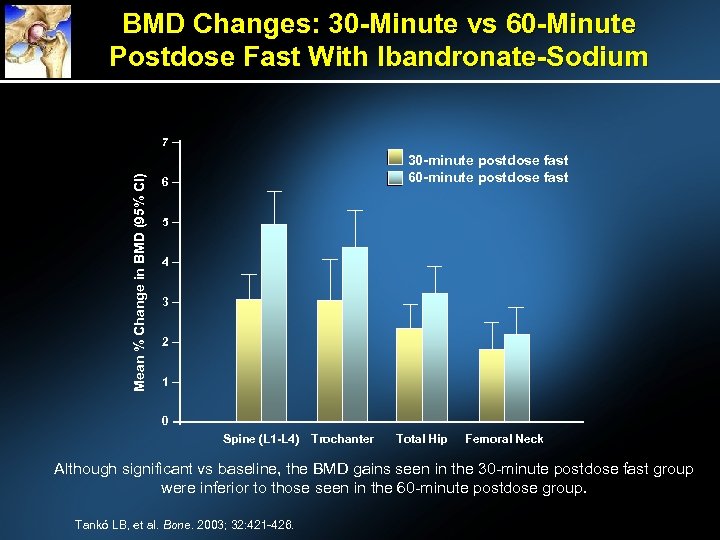 BMD Changes: 30 -Minute vs 60 -Minute Postdose Fast With Ibandronate-Sodium Mean % Change in BMD (95% Cl) 7 30 -minute postdose fast 6 5 4 3 2 1 0 Spine (L 1 -L 4) Trochanter Total Hip Femoral Neck Although significant vs baseline, the BMD gains seen in the 30 -minute postdose fast group were inferior to those seen in the 60 -minute postdose group. Tankó LB, et al. Bone. 2003; 32: 421 -426.
BMD Changes: 30 -Minute vs 60 -Minute Postdose Fast With Ibandronate-Sodium Mean % Change in BMD (95% Cl) 7 30 -minute postdose fast 6 5 4 3 2 1 0 Spine (L 1 -L 4) Trochanter Total Hip Femoral Neck Although significant vs baseline, the BMD gains seen in the 30 -minute postdose fast group were inferior to those seen in the 60 -minute postdose group. Tankó LB, et al. Bone. 2003; 32: 421 -426.
 Efficacy Testing Of Anti-osteoporosis Drugs The FDA-mandated primary outcome measures (end point) for all pivotal trials is the demonstration of efficacy in reducing vertebral fracture Non-vertebral fractures, BMD and bone remodeling markers are secondary end points Secondary end points are never statistically powered in terms of patient numbers to detect differences between placebo and drug
Efficacy Testing Of Anti-osteoporosis Drugs The FDA-mandated primary outcome measures (end point) for all pivotal trials is the demonstration of efficacy in reducing vertebral fracture Non-vertebral fractures, BMD and bone remodeling markers are secondary end points Secondary end points are never statistically powered in terms of patient numbers to detect differences between placebo and drug
 Non-Vertebral Fractures ► Multiple non-vertebral sites, the definition of which varies across clinical trials Heterogenous group of bones, with different proportions of cortical and cancellous bone ► Differences in non-vertebral fracture incidence and disease severity in placebo groups ►
Non-Vertebral Fractures ► Multiple non-vertebral sites, the definition of which varies across clinical trials Heterogenous group of bones, with different proportions of cortical and cancellous bone ► Differences in non-vertebral fracture incidence and disease severity in placebo groups ►
 Conclusions ► Characterized by a loss of bone mass and architecture ► Inevitable consequence of aging in both sexes ► Accelerated following menopause, disease and drugs ► Early detection and intervention is mandatory ► Fracture stratification allows identification beyond BMD ► Bisphonates are the mainstay of therapy ► Ensuring compliance through less complex dosing should lead to greater therapeutic benefit
Conclusions ► Characterized by a loss of bone mass and architecture ► Inevitable consequence of aging in both sexes ► Accelerated following menopause, disease and drugs ► Early detection and intervention is mandatory ► Fracture stratification allows identification beyond BMD ► Bisphonates are the mainstay of therapy ► Ensuring compliance through less complex dosing should lead to greater therapeutic benefit
 Fracture Risk Reporting ► Since the goal of osteoporosis therapy is fracture prevention, patient selection is best based on fracture risk ► T-score alone does not provide a complete assessment of fracture risk ► Combination of clinical risk factors with BMD may provide a better way of identifying patients for treatment
Fracture Risk Reporting ► Since the goal of osteoporosis therapy is fracture prevention, patient selection is best based on fracture risk ► T-score alone does not provide a complete assessment of fracture risk ► Combination of clinical risk factors with BMD may provide a better way of identifying patients for treatment
 Selection of Clinical Risk Factors ► Independent of BMD (if BMD is known) ► Validated in multiple populations (sex, ethnicity, country) ► Easily obtainable ► Amenable to intended treatment ► Intuitive Adapted from Kanis JA et al. Osteoporos Int. 2005; 16: 581 -589.
Selection of Clinical Risk Factors ► Independent of BMD (if BMD is known) ► Validated in multiple populations (sex, ethnicity, country) ► Easily obtainable ► Amenable to intended treatment ► Intuitive Adapted from Kanis JA et al. Osteoporos Int. 2005; 16: 581 -589.
 Clinical Risk Factors Femoral neck T-score + ► Age ► Previous low trauma fracture ► Current cigarette smoking ► Rheumatoid arthritis ► High alcohol intake (> 2 units/day) ► Parental history of hip fracture ► Prior or current glucocorticoid use Adapted from Kanis JA et al. Osteoporos Int. 2005; 16: 581 -589.
Clinical Risk Factors Femoral neck T-score + ► Age ► Previous low trauma fracture ► Current cigarette smoking ► Rheumatoid arthritis ► High alcohol intake (> 2 units/day) ► Parental history of hip fracture ► Prior or current glucocorticoid use Adapted from Kanis JA et al. Osteoporos Int. 2005; 16: 581 -589.
 Intervention Threshold ► A fracture probability above which it is cost-effective to treat with pharmacological agents ► Based on statistical modeling using many medical, social, and economic assumptions
Intervention Threshold ► A fracture probability above which it is cost-effective to treat with pharmacological agents ► Based on statistical modeling using many medical, social, and economic assumptions


