8845c0b4f6acd1f12ab6e69e71ea2bbe.ppt
- Количество слайдов: 47
 Corneal Transplantation PHRM-520, L. S. No-5. 1 1
Corneal Transplantation PHRM-520, L. S. No-5. 1 1
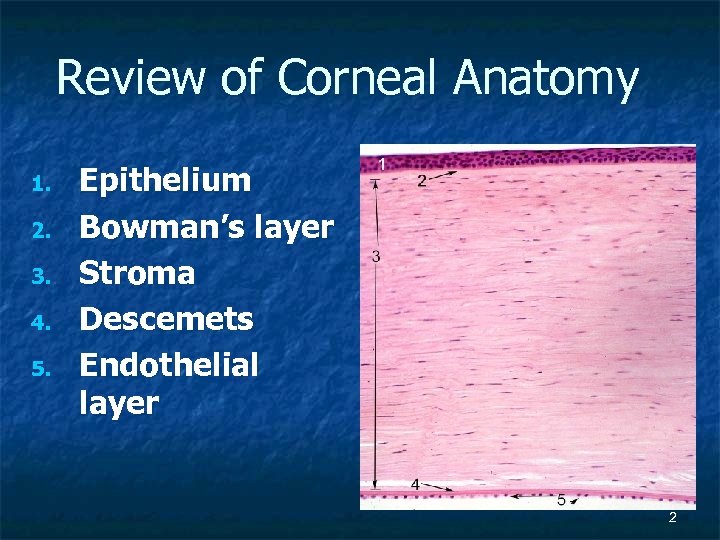 Review of Corneal Anatomy 1. 2. 3. 4. 5. Epithelium Bowman’s layer Stroma Descemets Endothelial layer 2
Review of Corneal Anatomy 1. 2. 3. 4. 5. Epithelium Bowman’s layer Stroma Descemets Endothelial layer 2
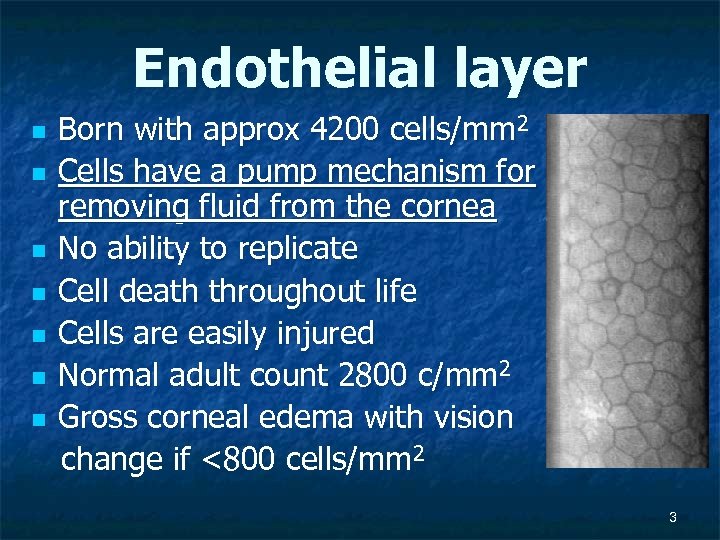 Endothelial layer n n n n Born with approx 4200 cells/mm 2 Cells have a pump mechanism for removing fluid from the cornea No ability to replicate Cell death throughout life Cells are easily injured Normal adult count 2800 c/mm 2 Gross corneal edema with vision change if <800 cells/mm 2 3
Endothelial layer n n n n Born with approx 4200 cells/mm 2 Cells have a pump mechanism for removing fluid from the cornea No ability to replicate Cell death throughout life Cells are easily injured Normal adult count 2800 c/mm 2 Gross corneal edema with vision change if <800 cells/mm 2 3
 Indications for Corneal Transplantation n n Lack of corneal clarity (scar) Corneal curvature abnormalities (ectasia) Corneal edema Lack of corneal integrity 4
Indications for Corneal Transplantation n n Lack of corneal clarity (scar) Corneal curvature abnormalities (ectasia) Corneal edema Lack of corneal integrity 4
 Why Corneal Grafting? n n n Corneal Opacity Corneal Clouding Corneal Ectasias Corneal Edema Fuchs Endothelial Dystrophy 5
Why Corneal Grafting? n n n Corneal Opacity Corneal Clouding Corneal Ectasias Corneal Edema Fuchs Endothelial Dystrophy 5
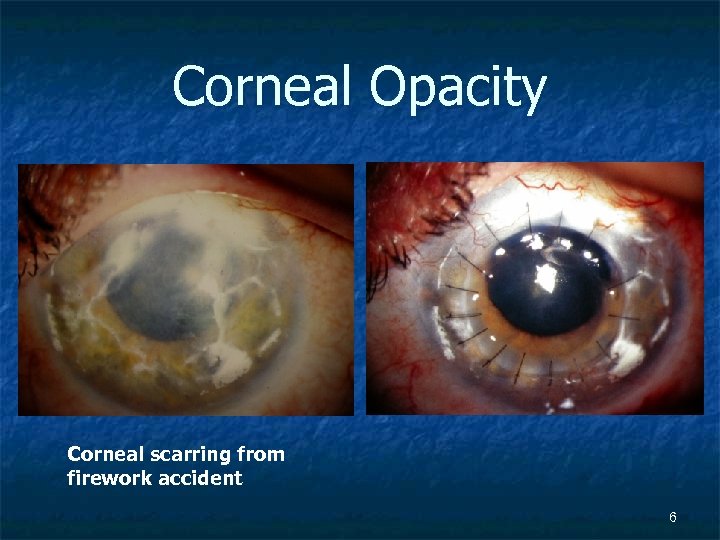 Corneal Opacity Corneal scarring from firework accident 6
Corneal Opacity Corneal scarring from firework accident 6
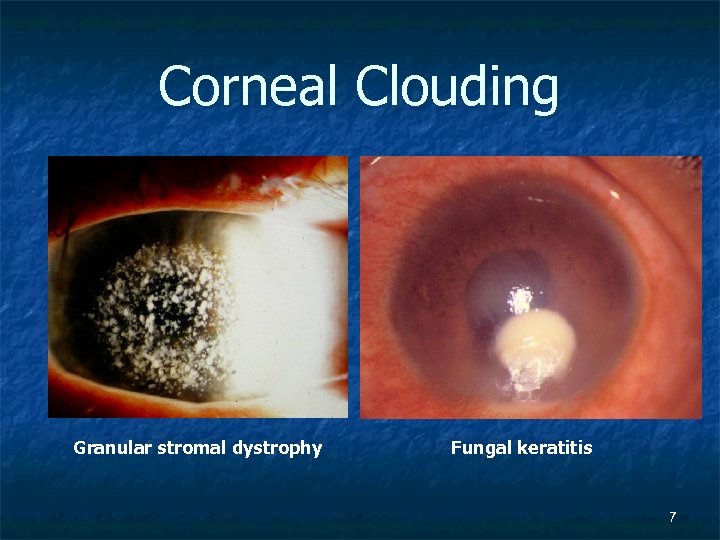 Corneal Clouding Granular stromal dystrophy Fungal keratitis 7
Corneal Clouding Granular stromal dystrophy Fungal keratitis 7
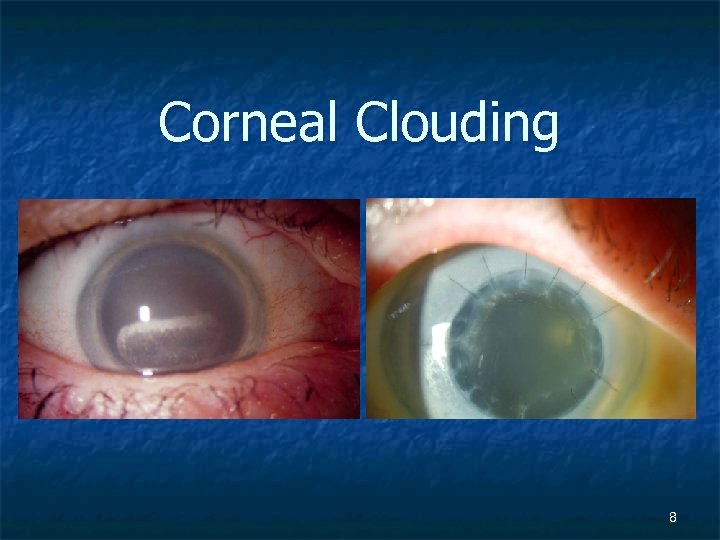 Corneal Clouding 8
Corneal Clouding 8
 Corneal Ectasias n n Keratoconus- progressive corneal thinning and steepening. Presents in late teens and causes astigmatism that may not be correctable with glasses or rigid contact lenses Pellucid marginal degeneration 9
Corneal Ectasias n n Keratoconus- progressive corneal thinning and steepening. Presents in late teens and causes astigmatism that may not be correctable with glasses or rigid contact lenses Pellucid marginal degeneration 9
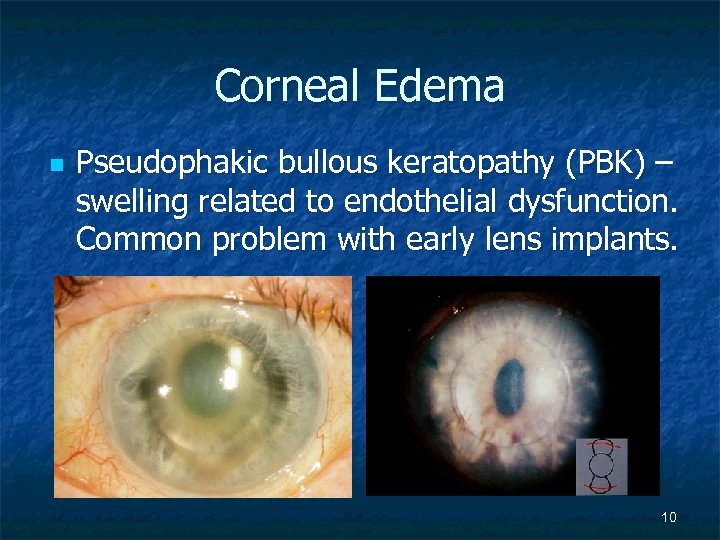 Corneal Edema n Pseudophakic bullous keratopathy (PBK) – swelling related to endothelial dysfunction. Common problem with early lens implants. 10
Corneal Edema n Pseudophakic bullous keratopathy (PBK) – swelling related to endothelial dysfunction. Common problem with early lens implants. 10
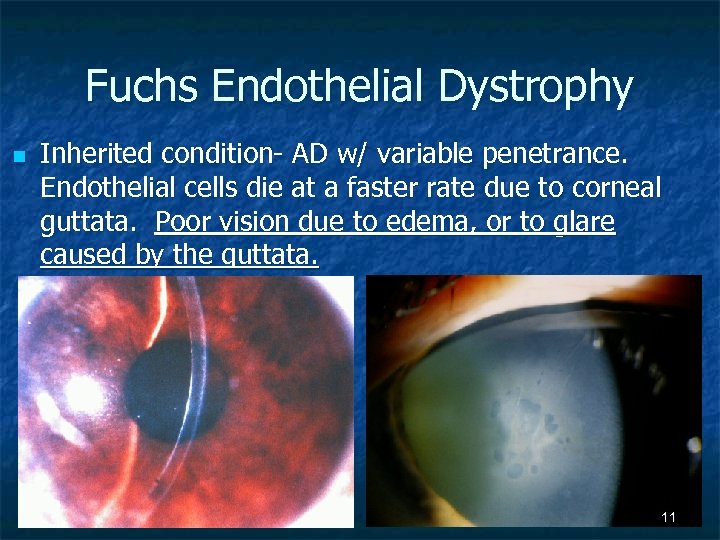 Fuchs Endothelial Dystrophy n Inherited condition- AD w/ variable penetrance. Endothelial cells die at a faster rate due to corneal guttata. Poor vision due to edema, or to glare caused by the guttata. 11
Fuchs Endothelial Dystrophy n Inherited condition- AD w/ variable penetrance. Endothelial cells die at a faster rate due to corneal guttata. Poor vision due to edema, or to glare caused by the guttata. 11
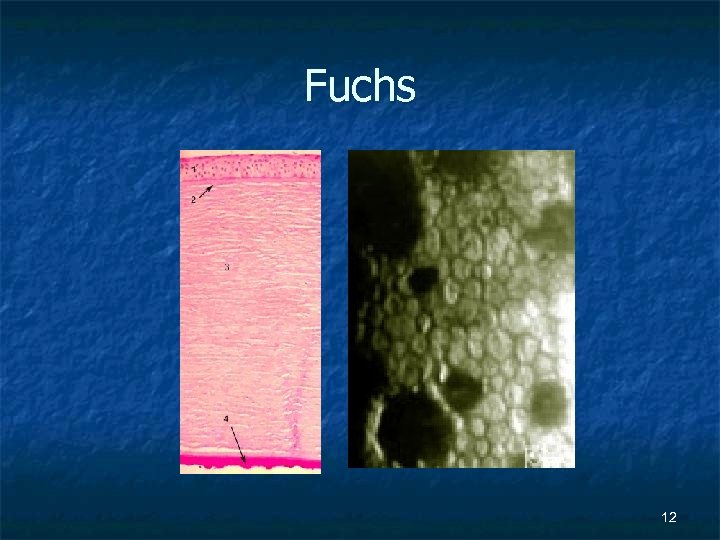 Fuchs 12
Fuchs 12
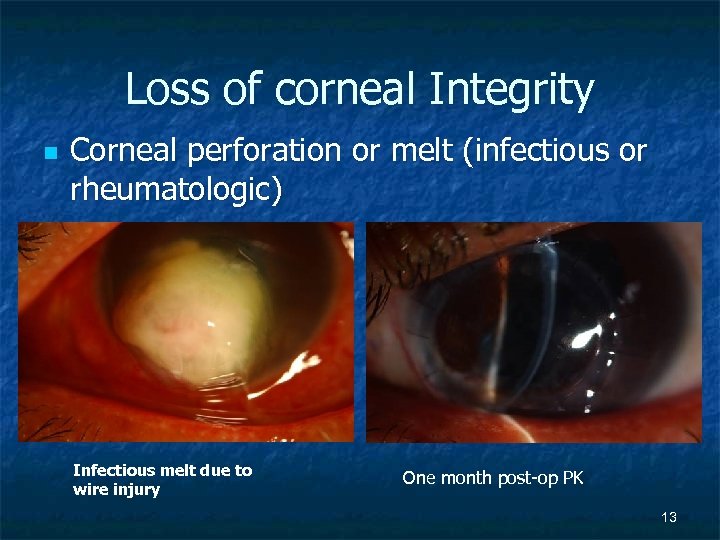 Loss of corneal Integrity n Corneal perforation or melt (infectious or rheumatologic) Infectious melt due to wire injury One month post-op PK 13
Loss of corneal Integrity n Corneal perforation or melt (infectious or rheumatologic) Infectious melt due to wire injury One month post-op PK 13
 History n 1906 – Dr. Eduard Konrad Zirm in Moravia performed the first successful penetrating keratoplasty (PK) on a farmer in Prague who sustained bilateral alkali burns after cleaning his chicken coop with lime. Bilateral 5 mm grafts from a single donor (11 yo boy who required enucleation) 14
History n 1906 – Dr. Eduard Konrad Zirm in Moravia performed the first successful penetrating keratoplasty (PK) on a farmer in Prague who sustained bilateral alkali burns after cleaning his chicken coop with lime. Bilateral 5 mm grafts from a single donor (11 yo boy who required enucleation) 14
 History n Essential Principles (still in use) 1. 2. 3. 4. Donor must be human Aseptic technique No antiseptic agents should go on cornea Protect graft w/ saline moistened gauze 15
History n Essential Principles (still in use) 1. 2. 3. 4. Donor must be human Aseptic technique No antiseptic agents should go on cornea Protect graft w/ saline moistened gauze 15
 Limitations n n n good understanding of corneal physiology or immunology fine sutures or operating microscope pharmacologic ability to treat or prevent rejection 16
Limitations n n n good understanding of corneal physiology or immunology fine sutures or operating microscope pharmacologic ability to treat or prevent rejection 16
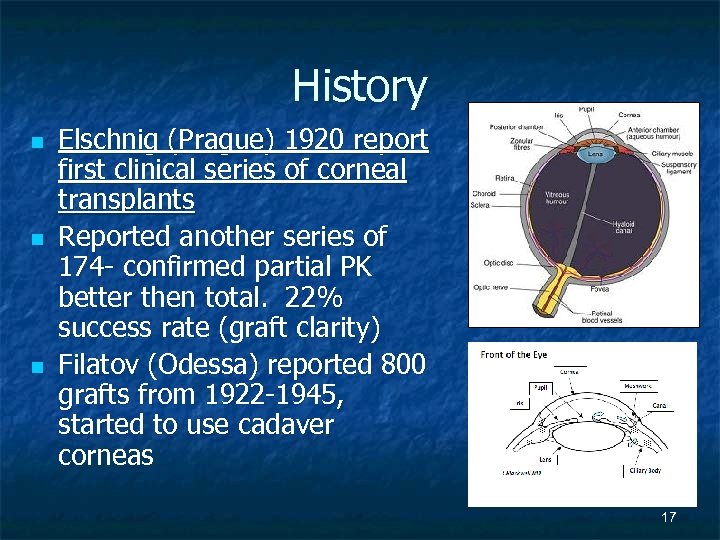 History n n n Elschnig (Prague) 1920 report first clinical series of corneal transplants Reported another series of 174 - confirmed partial PK better then total. 22% success rate (graft clarity) Filatov (Odessa) reported 800 grafts from 1922 -1945, started to use cadaver corneas 17
History n n n Elschnig (Prague) 1920 report first clinical series of corneal transplants Reported another series of 174 - confirmed partial PK better then total. 22% success rate (graft clarity) Filatov (Odessa) reported 800 grafts from 1922 -1945, started to use cadaver corneas 17
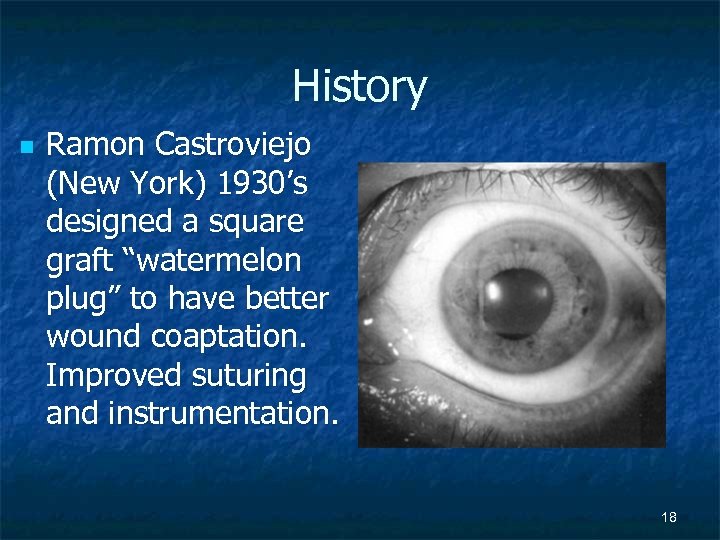 History n Ramon Castroviejo (New York) 1930’s designed a square graft “watermelon plug” to have better wound coaptation. Improved suturing and instrumentation. 18
History n Ramon Castroviejo (New York) 1930’s designed a square graft “watermelon plug” to have better wound coaptation. Improved suturing and instrumentation. 18
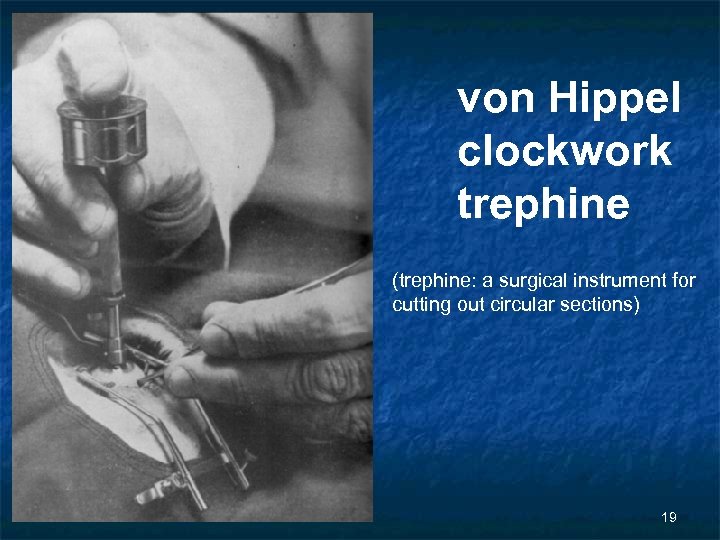 von Hippel clockwork trephine (trephine: a surgical instrument for cutting out circular sections) 19
von Hippel clockwork trephine (trephine: a surgical instrument for cutting out circular sections) 19
 History n n 1945 R. Townley Paton started the first Eye Bank in NYC. Early tissue was acquired from prisoners executed at Sing-Sing prison A. Edward Maumenee at Wilmer Eye Hospital advanced the field with his work in corneal physiology and immunology. Coincided w/ the advent of topical corticosteroids which had a profound effect on modern corneal transplantation Surgical success was followed by optical success 20
History n n 1945 R. Townley Paton started the first Eye Bank in NYC. Early tissue was acquired from prisoners executed at Sing-Sing prison A. Edward Maumenee at Wilmer Eye Hospital advanced the field with his work in corneal physiology and immunology. Coincided w/ the advent of topical corticosteroids which had a profound effect on modern corneal transplantation Surgical success was followed by optical success 20
 1950 to present n n n n Operating microscope New trephines and laser trephination New suture needles Viscoelastics Steroids and other immunomodulators Better antibiotics Eye Bank Association of America (1961) Improved storage medium for donor corneas 21
1950 to present n n n n Operating microscope New trephines and laser trephination New suture needles Viscoelastics Steroids and other immunomodulators Better antibiotics Eye Bank Association of America (1961) Improved storage medium for donor corneas 21
 Eye Bank Association of America contraindications for donor corneas n n n n Death of unknown cause Unknown central nervous system disease Infections including HIV or hepatitis Active ocular inflammation Leukemia or lymphoma Cancer in the eye Congenital corneal dystrophies or ectasias (e. g. keratoconus) Prior refractive surgery (e. g. LASIK) 22
Eye Bank Association of America contraindications for donor corneas n n n n Death of unknown cause Unknown central nervous system disease Infections including HIV or hepatitis Active ocular inflammation Leukemia or lymphoma Cancer in the eye Congenital corneal dystrophies or ectasias (e. g. keratoconus) Prior refractive surgery (e. g. LASIK) 22
 Storage Media n n Optisol GS allows for storage up to 10 days. Allows surgery to be scheduled electively D to P (death to preservation) preferably less than 12 hours 23
Storage Media n n Optisol GS allows for storage up to 10 days. Allows surgery to be scheduled electively D to P (death to preservation) preferably less than 12 hours 23
 Types of Corneal Transplants n n Penetrating keratoplasty (PK) Lamellar keratoplasty (LK) n Anterior lamellar keratoplasty (ALK) n Deep anterior lamellar keratoplasty (DALK) n Posterior lamellar keratoplasty (PLK) n Endothelial keratoplasty (EK) n Deep lamellar endothelial keratoplasty (DLEK) n Descemet’s stripping endothelial keratoplasty (DSEK) 24
Types of Corneal Transplants n n Penetrating keratoplasty (PK) Lamellar keratoplasty (LK) n Anterior lamellar keratoplasty (ALK) n Deep anterior lamellar keratoplasty (DALK) n Posterior lamellar keratoplasty (PLK) n Endothelial keratoplasty (EK) n Deep lamellar endothelial keratoplasty (DLEK) n Descemet’s stripping endothelial keratoplasty (DSEK) 24
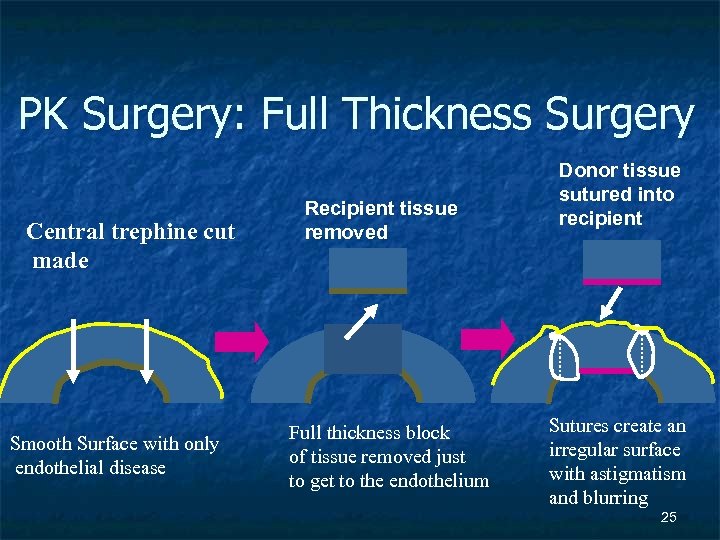 PK Surgery: Full Thickness Surgery Central trephine cut made Smooth Surface with only endothelial disease Recipient tissue removed Full thickness block of tissue removed just to get to the endothelium Donor tissue sutured into recipient Sutures create an irregular surface with astigmatism and blurring 25
PK Surgery: Full Thickness Surgery Central trephine cut made Smooth Surface with only endothelial disease Recipient tissue removed Full thickness block of tissue removed just to get to the endothelium Donor tissue sutured into recipient Sutures create an irregular surface with astigmatism and blurring 25
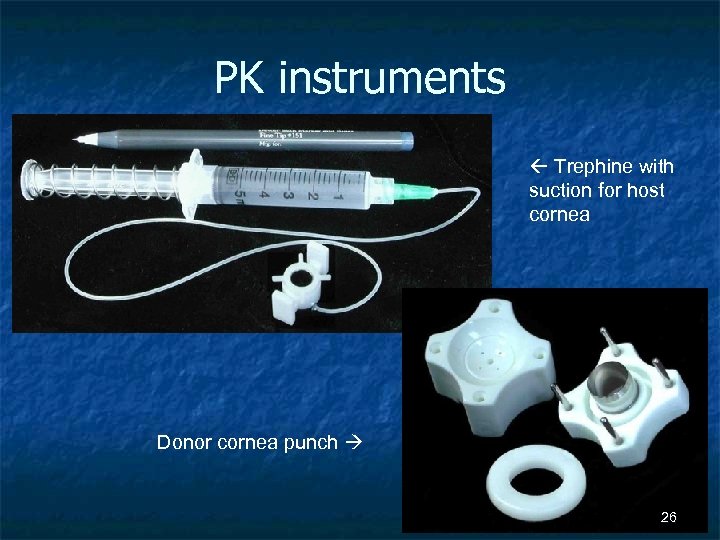 PK instruments Trephine with suction for host cornea Donor cornea punch 26
PK instruments Trephine with suction for host cornea Donor cornea punch 26
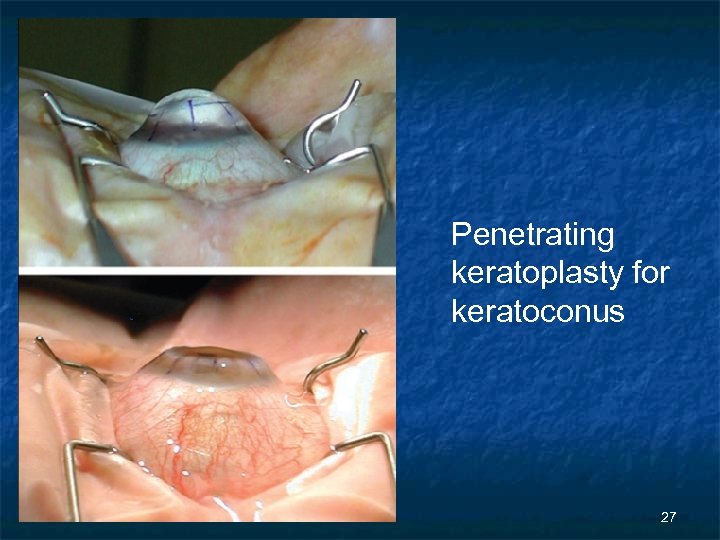 Penetrating keratoplasty for keratoconus 27
Penetrating keratoplasty for keratoconus 27
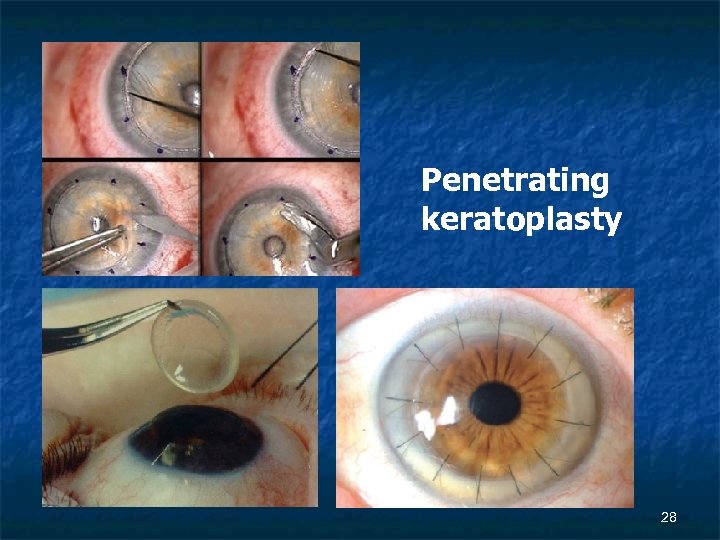 Penetrating keratoplasty 28
Penetrating keratoplasty 28
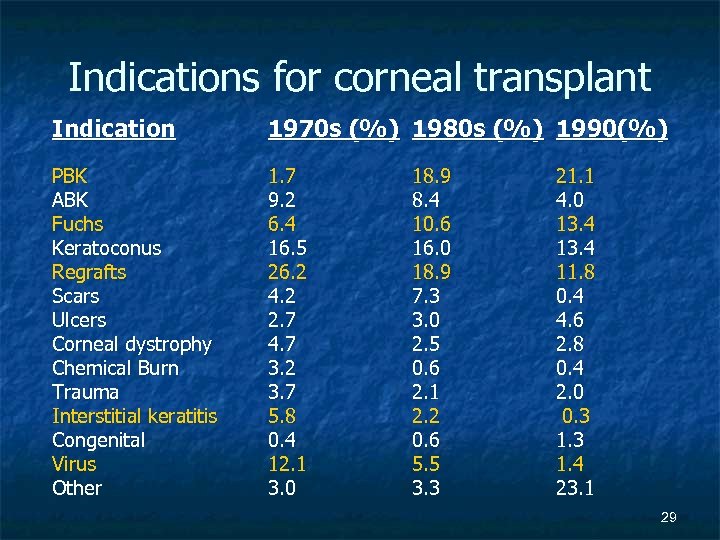 Indications for corneal transplant Indication 1970 s (%) 1980 s (%) 1990(%) PBK ABK Fuchs Keratoconus Regrafts Scars Ulcers Corneal dystrophy Chemical Burn Trauma Interstitial keratitis Congenital Virus Other 1. 7 9. 2 6. 4 16. 5 26. 2 4. 2 2. 7 4. 7 3. 2 3. 7 5. 8 0. 4 12. 1 3. 0 18. 9 8. 4 10. 6 16. 0 18. 9 7. 3 3. 0 2. 5 0. 6 2. 1 2. 2 0. 6 5. 5 3. 3 21. 1 4. 0 13. 4 11. 8 0. 4 4. 6 2. 8 0. 4 2. 0 0. 3 1. 4 23. 1 29
Indications for corneal transplant Indication 1970 s (%) 1980 s (%) 1990(%) PBK ABK Fuchs Keratoconus Regrafts Scars Ulcers Corneal dystrophy Chemical Burn Trauma Interstitial keratitis Congenital Virus Other 1. 7 9. 2 6. 4 16. 5 26. 2 4. 2 2. 7 4. 7 3. 2 3. 7 5. 8 0. 4 12. 1 3. 0 18. 9 8. 4 10. 6 16. 0 18. 9 7. 3 3. 0 2. 5 0. 6 2. 1 2. 2 0. 6 5. 5 3. 3 21. 1 4. 0 13. 4 11. 8 0. 4 4. 6 2. 8 0. 4 2. 0 0. 3 1. 4 23. 1 29
 Problems with PK: n n n Unpredictable astigmatism and corneal power Infection Ulceration Vascularization Rejection Poor Wound Healing: Risk of Rupture 30
Problems with PK: n n n Unpredictable astigmatism and corneal power Infection Ulceration Vascularization Rejection Poor Wound Healing: Risk of Rupture 30
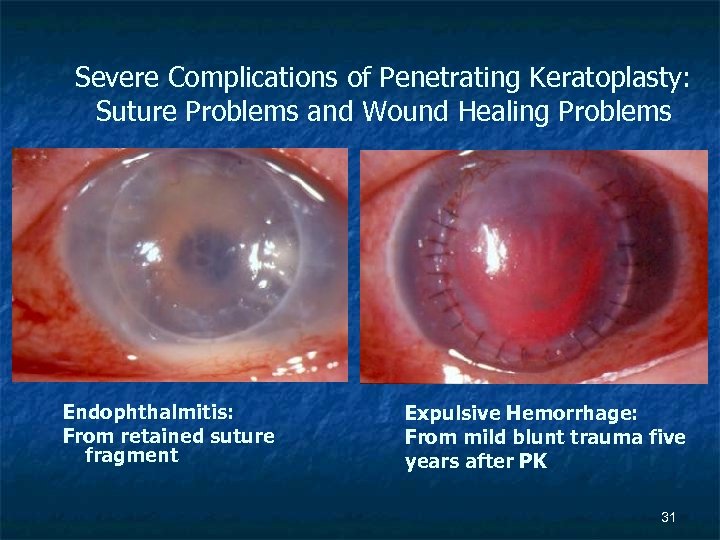 Severe Complications of Penetrating Keratoplasty: Suture Problems and Wound Healing Problems Endophthalmitis: From retained suture fragment Expulsive Hemorrhage: From mild blunt trauma five years after PK 31
Severe Complications of Penetrating Keratoplasty: Suture Problems and Wound Healing Problems Endophthalmitis: From retained suture fragment Expulsive Hemorrhage: From mild blunt trauma five years after PK 31
 Deep Lamellar Endothelial Keratoplasty n n n First described by Dr. Gerrit Melles- 1998 First done in the US by Mark Terry, M. D. Terry has done> 250 between 2000 -05 Terry has trained> 100 cornea specialists to perform DLEK, and formed EKG (Endothelial Keratoplasty Group) Initially all procedures done under IRB 32
Deep Lamellar Endothelial Keratoplasty n n n First described by Dr. Gerrit Melles- 1998 First done in the US by Mark Terry, M. D. Terry has done> 250 between 2000 -05 Terry has trained> 100 cornea specialists to perform DLEK, and formed EKG (Endothelial Keratoplasty Group) Initially all procedures done under IRB 32
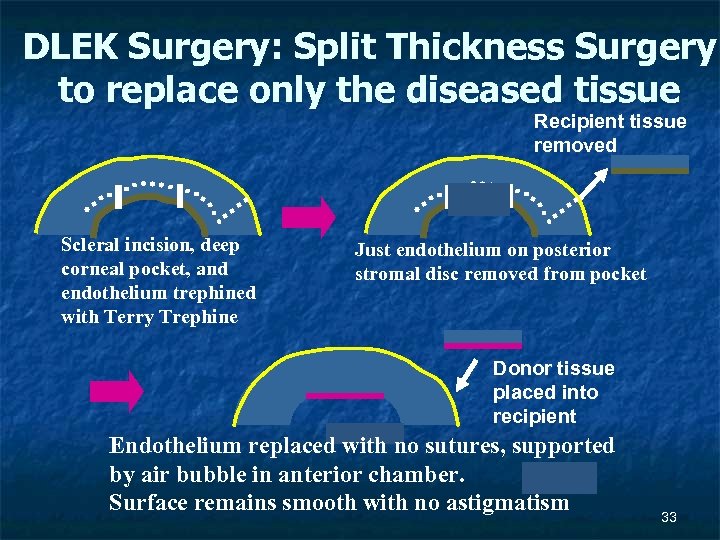 DLEK Surgery: Split Thickness Surgery to replace only the diseased tissue Recipient tissue removed Scleral incision, deep corneal pocket, and endothelium trephined with Terry Trephine Just endothelium on posterior stromal disc removed from pocket Donor tissue placed into recipient Endothelium replaced with no sutures, supported by air bubble in anterior chamber. Surface remains smooth with no astigmatism 33
DLEK Surgery: Split Thickness Surgery to replace only the diseased tissue Recipient tissue removed Scleral incision, deep corneal pocket, and endothelium trephined with Terry Trephine Just endothelium on posterior stromal disc removed from pocket Donor tissue placed into recipient Endothelium replaced with no sutures, supported by air bubble in anterior chamber. Surface remains smooth with no astigmatism 33
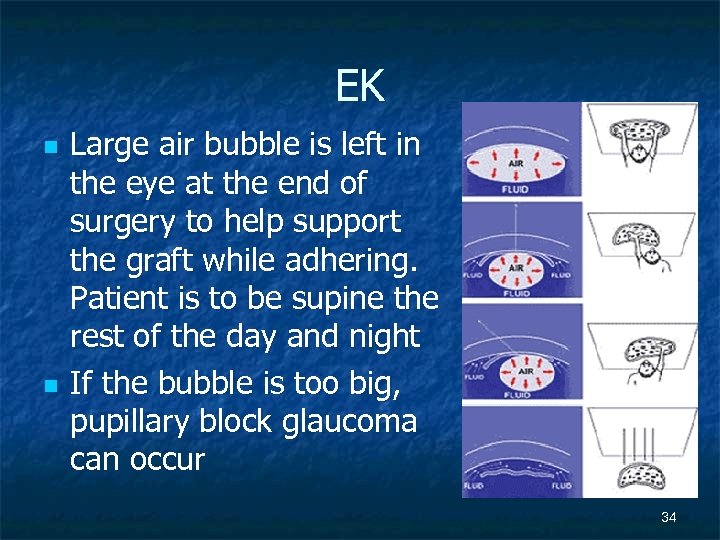 EK n n Large air bubble is left in the eye at the end of surgery to help support the graft while adhering. Patient is to be supine the rest of the day and night If the bubble is too big, pupillary block glaucoma can occur 34
EK n n Large air bubble is left in the eye at the end of surgery to help support the graft while adhering. Patient is to be supine the rest of the day and night If the bubble is too big, pupillary block glaucoma can occur 34
 Advantages of EK over PK n n Faster visual recovery Less postoperative astigmatism (confirmed by corneal topography) Stronger globe integrity due to lack of fullthickness corneal incision No suture related infections 35
Advantages of EK over PK n n Faster visual recovery Less postoperative astigmatism (confirmed by corneal topography) Stronger globe integrity due to lack of fullthickness corneal incision No suture related infections 35
 Disadvantages of DLEK n n n More time consuming and difficult procedure due to lamellar dissection Graft dislocation- 5 -20% on post-op day 1 Not as many patients get to 20/20 as with PK; may be interface problem 36
Disadvantages of DLEK n n n More time consuming and difficult procedure due to lamellar dissection Graft dislocation- 5 -20% on post-op day 1 Not as many patients get to 20/20 as with PK; may be interface problem 36
 DSEK- Descemets Stripping Endothelial Keratoplasty n n 2005 Price, Gorovoy- eliminated the recipient dissection by just removing descemets membrane and the endothelium Surgeon still had to perform the lamellar dissection on the donor. If it went badly, the tissue wasted. 37
DSEK- Descemets Stripping Endothelial Keratoplasty n n 2005 Price, Gorovoy- eliminated the recipient dissection by just removing descemets membrane and the endothelium Surgeon still had to perform the lamellar dissection on the donor. If it went badly, the tissue wasted. 37
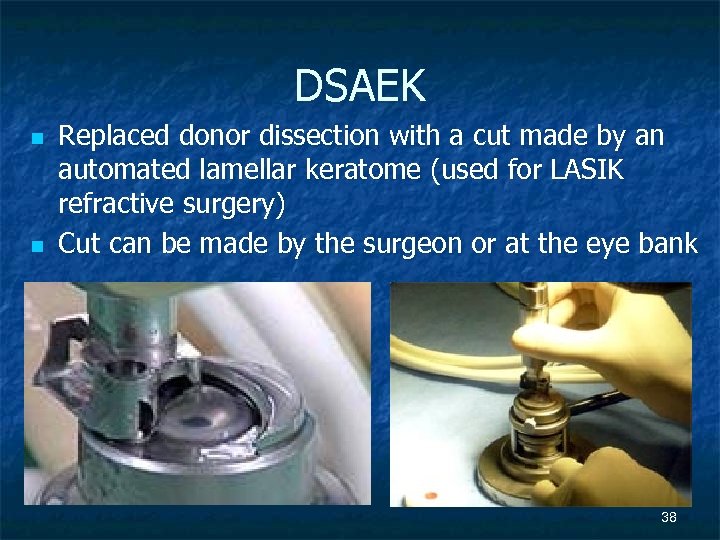 DSAEK n n Replaced donor dissection with a cut made by an automated lamellar keratome (used for LASIK refractive surgery) Cut can be made by the surgeon or at the eye bank 38
DSAEK n n Replaced donor dissection with a cut made by an automated lamellar keratome (used for LASIK refractive surgery) Cut can be made by the surgeon or at the eye bank 38
 DSAEK at UVA n n n We undertook an IRB approved prospective study to look at the DSAEK procedure as described by Terry (Ophthalmology 2008; 115: 1179 -1186) Dr. Paul Phillips (previous resident at UVA and Terry fellow 2007 -2008) performed initial procedures and taught LAO Strictly followed the procedure First case performed 9/16/09 All tissue was pre-cut at Portland Eye Bank 39
DSAEK at UVA n n n We undertook an IRB approved prospective study to look at the DSAEK procedure as described by Terry (Ophthalmology 2008; 115: 1179 -1186) Dr. Paul Phillips (previous resident at UVA and Terry fellow 2007 -2008) performed initial procedures and taught LAO Strictly followed the procedure First case performed 9/16/09 All tissue was pre-cut at Portland Eye Bank 39
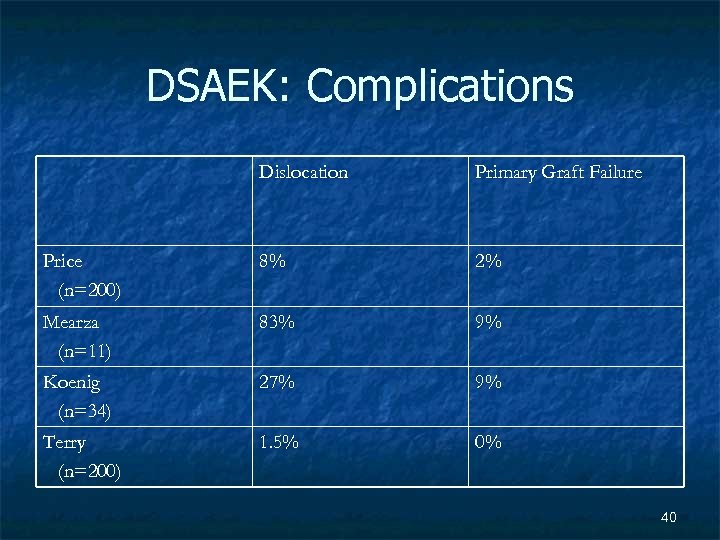 DSAEK: Complications Dislocation Primary Graft Failure Price (n=200) 8% 2% Mearza (n=11) 83% 9% Koenig (n=34) 27% 9% Terry (n=200) 1. 5% 0% 40
DSAEK: Complications Dislocation Primary Graft Failure Price (n=200) 8% 2% Mearza (n=11) 83% 9% Koenig (n=34) 27% 9% Terry (n=200) 1. 5% 0% 40
 Cases – J. S n n n 62 yo F w/ Fuchs LAO did PK OD 8/03 – did “well” 20/40 -3. 25+4. 75 x 025 (unable to tolerate RGP) 9/16/09 TCC Phaco/IOL and 8. 0 mm DSAEK – PP 20/25 Va unaided at 1 month post-op VERY HAPPY patient 41
Cases – J. S n n n 62 yo F w/ Fuchs LAO did PK OD 8/03 – did “well” 20/40 -3. 25+4. 75 x 025 (unable to tolerate RGP) 9/16/09 TCC Phaco/IOL and 8. 0 mm DSAEK – PP 20/25 Va unaided at 1 month post-op VERY HAPPY patient 41
 P. R. n n n 58 yo F w/ Fuchs LAO did PK OS 5/05 – did “well” 20/30 +4. 50+1. 25 x 055 5/19/09 TCC Phaco/IOL and 8. 0 mm DSAEK – LAO 20/20 -1 unaided 1 month post-op VERY HAPPY patient 42
P. R. n n n 58 yo F w/ Fuchs LAO did PK OS 5/05 – did “well” 20/30 +4. 50+1. 25 x 055 5/19/09 TCC Phaco/IOL and 8. 0 mm DSAEK – LAO 20/20 -1 unaided 1 month post-op VERY HAPPY patient 42
 43
43
 44
44
 45
45
 Summary n n Corneal transplantation has evolved dramatically over the past century. The most recent advances have allowed the procedure to become less invasive and more optically successful for the recipient, but more challenging for the surgeon. 46
Summary n n Corneal transplantation has evolved dramatically over the past century. The most recent advances have allowed the procedure to become less invasive and more optically successful for the recipient, but more challenging for the surgeon. 46
 Thank You 47
Thank You 47


