10cfe160ebd6896d30870cf805770a92.ppt
- Количество слайдов: 45

CONCUSSIONS & THEIR IMPACT By: John D. Anderson, PT, DPT, LAT, ATC Credit to Tim Rylander, PT, MPT, OCS



Concussions/m. TBI • Increased awareness and attention • 3. 8 million incidents/year • 15% minority (false)
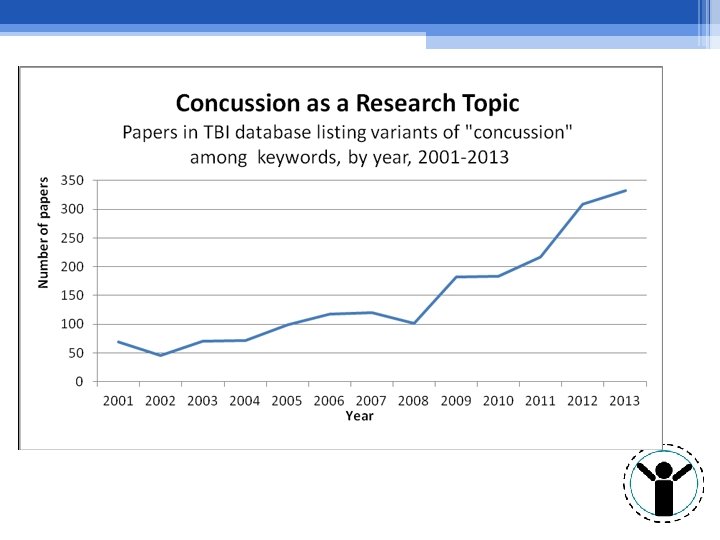

Concussion in the Workplace Per “SFM: The Work Comp Experts” 48% increase in concussions that caused injured employees to lose time from work from 2012 -2014 79% of reported concussions related to slips, trips and falls, strikes to the head, or MVAs $33, 000 = average lost-time concussion claim https: //simplyworkcomp. com/work-related-concussions-on-the-rise-use-these-tips-to-prevent-them/

WHAT IS A CONCUSSION?

A Concussion (m. TBI) is a complex pathophysiological process afecting the brain, induced by traumatic biomechanical forces secondary to direct or indirect forces to the head. Disturbance of brain function is related to neurometabolic dysfunction, rather than structural brain injury, and is typically asociated wih normal structural imaging findings (CT Scan, MRI). Concussion may or may not involve a loss of consciousness. Concussion results in a constellation of physical, cognitive, emotional, and sleep-related symptoms. Recovery is a sequential process and symptoms may last from several minutes to days, weeks, months, or even longer in some cases. -CDC Physicians Toolkit; Collins, Gioia et al 2006

Key Points • • • m. TBI Normal Images Impact & Non-Impact Loss of Consciousness Constellation of Symptoms
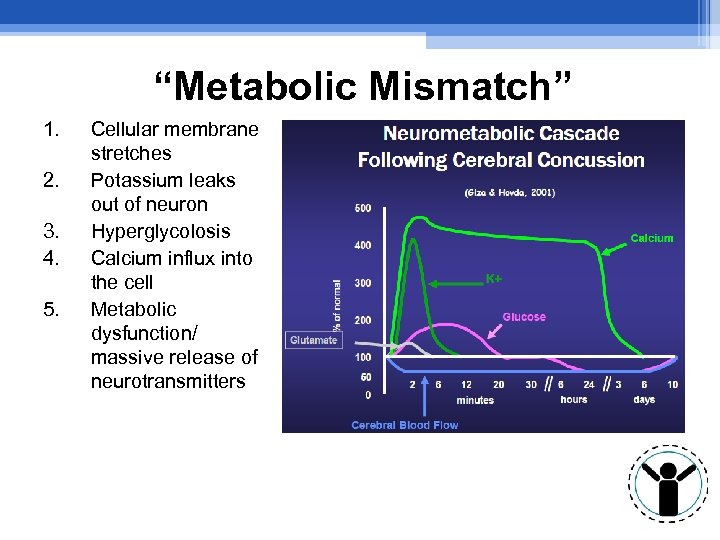
“Metabolic Mismatch” 1. 2. 3. 4. 5. Cellular membrane stretches Potassium leaks out of neuron Hyperglycolosis Calcium influx into the cell Metabolic dysfunction/ massive release of neurotransmitters

Common Symptoms • • • Headache (71%) Lethargy (58%) Difficulty concentrating (57%) Dizziness (55%) Fogginess (53%) Visual disturbance (49%) Visual sensitivity (47%) Memory deficits (43%) Balance problems (43%)

Recovery Time At 2 weeks post event, 80% are recovered At 3 weeks that increases to 90% However, 20% of athletes take OVER 3 weeks to recover

Risk Factors Effecting Recovery Primary Existing risk factors which existed prior to the concussion. (Premorbid) Secondary Factors which occur post injury (Prognostic)

Primary Previous concussion Prior history of migraines Diagnosis of learning disability or ADHD Sex Females are 1. 7 times more likely to have concussion Age Younger more inclined and longer healing

Secondary Post traumatic migraine syndrome (Headache with photo/ phonosensativity Immediate dizziness Sub-Acute Fogginess (3 -7 days) Vomiting Dizziness Numbness


When to Refer Research is varied some here although trend is toward sooner the better ARC guideline is that if patient is symptomatic at 2 weeks, need PT referral If more symptomatic or with many risk factors than earlier referral may be warranted

Vestibular Rehabilitation • A sub-specialty of the physical therapy profession focusing on balance, gaze stability, gait stability, and vestibular function.

Balance • Ability to control one’s COG over a selective BOS within a given sensory environment. • Reflex vs Systems models

Dynamic Postural Control • Postural Orientation ▫ Ability to maintain proper relationship of body segments within the environment for a specific task • Postural Stability ▫ Ability to control one’s center of mass in relation to a given base of support

Derivation of Balance • Somatosensory ▫ First line of defense • Visual ▫ Second line of defense • Vestibular ▫ Provides conflict resolution between systems

Somatosensory Specifics • Special attention given to the craniocervical complex • Rarely does concussion occur without neck trauma • Cervical impairments may impact postural disturbances and contribute towards symptoms
Anatomy: Musculoskeletal • Upper cervical vertebrae • Suboccipitals • Deep intervertebral muscles

Vestibular • Measures gravitational and accelerational forces • Consists of both central and peripheral circuitry • Common manifestations include dizziness, motion sensitivity, and limited positional tolerance

Functional Vision • • • Gaze Stabilization? Normal vs abnormal Tracking Saccades Vergence
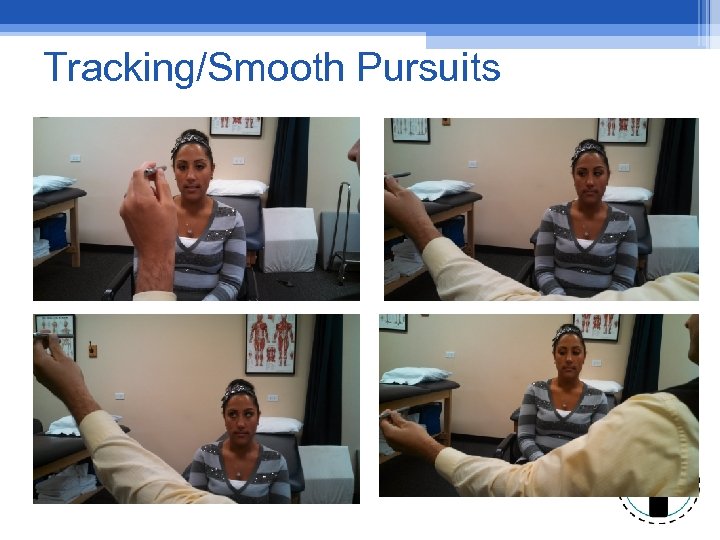
Tracking/Smooth Pursuits

Saccades

Convergence
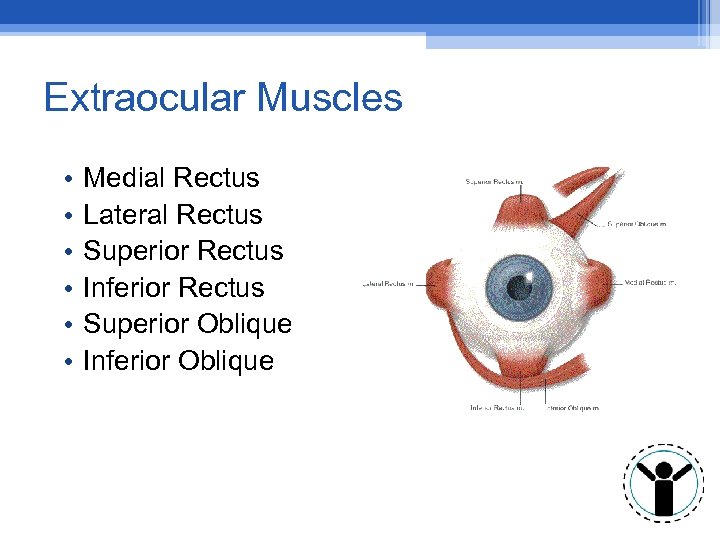
Extraocular Muscles • • • Medial Rectus Lateral Rectus Superior Rectus Inferior Rectus Superior Oblique Inferior Oblique

Examination • History • Objective Data • Self-Efficacy Questionnaires

History • • DOI Impact/non-impact LOC Amnesia Symptoms Hx of concussions Management thus far

Objective Measures • • Musculoskeletal Oculomotor Exam Vestibular Function Balance

Oculomotor Exam • • • ROM (physiological “H”) Tracking Saccades Optokinetic Reflex Convergence Cover Test

Vestibular Function • • Dix-Hallpike Supine Lateral Head Turn Test VOR Head Thrust Test

Balance • • BESS DGI TUG Romberg (sharpened) • SLS (EO/EC)

Self-Efficacy Questionnaires • • Activities-specific Balance Confidence Scale Dizziness Handicap Inventory UCLA Dizziness Questionnaire Rivermead Post Concussion Questionare

Treatment • Improve vestibular and oculomotor function • Address musculoskeletal impairments • Slowly increase both cardiovascular and cognitive load

Case 1 Tammy • 46 y/o female struck by a van of federal marshals while crossing the street at the local court house. • Impact was hard enough to where she left an imprint on the vehicle. She flew 56 feet in the air landing on her back and hitting her head.

• She was initially diagnosed with a pelvic fracture and a severe tibial contusion. She was subsequently treated for a year (at a different company) for her musculoskeletal injuries. • The entire time, she was complaining of headaches, and feeling off balance. • It wasn’t until she was referred to pain management that it was thought that she may of sustained a concussion during the initial incident.

• Upon initial evaluation she presented with c/o dizziness specifically when exposed to busy visual environments or following increased computer work. • She had consistent c/o HA, specifically headaches that originated at the base of her head/ neck and wrapped around to her temples. • She felt as though she had poor balance stating that she felt unsteady with ambulation.

• Ocular Examination revealed a convergence insufficiency, along with poor saccadic function. Her VOR was impaired, and her dynamic visual acuity was positive for oscillopsia. • Musculoskeletal Evaluation- Upper cervical spine was locked up at the AO junction, and her cervical extrinsics were very tight. • Following treatment, she was able to return to work full-time at her regular responsibilities

Case 2 • The patient was a 48 y/o male who worked as a tree service foreman. • There was an incident where semi-truck was lodged underneath a tree limb and his crew was called to the scene. • So the patient took it upon himself to climb onto the truck and attempt to cut the branch away.

• Unfortunately, the patient ended up falling between the cab of the truck and the trailer, bounced, and then landed on his head on the street. • His hardhat cracked in half. • Upon evaluation, his primary complaints was that of dizziness described as a spinning sensation when he looked up, or when he rolled left in bed. He denies any headache, or any other symptoms.

• Examination revealed oculomotor function WNL, and normal cervical ROM and mobility. His only impairments were vestibular orientated which included slow VOR function, and a positive Dix. Hallpike indicative of a benign paroxysmal positional vertigo. • The patient was seen for three visits, prior to a complete resolution of symptoms and a full return to work.

Thank you for your time. John D. Anderson, PT, DPT, LAT, ATC Clinic Director/ Owner Team Rehabilitation Fishers, IN (317) 813 -4770 (317) 691 -4144 (Cell) John. anderson@team-rehab. com
10cfe160ebd6896d30870cf805770a92.ppt