b5895a1d58864d85fb8b5baa054e27f0.ppt
- Количество слайдов: 40
 Comprehensive Acute Stroke Care in the United States - organization and current trends RADOSLAV RAYCHEV, MD DEPARTMENTS OF NEUROLOGICAL SURGERY AND NEUROLOGY UNIVERSITY OF CALIFORNIA IRVINE SCHOOL OF MEDICINE
Comprehensive Acute Stroke Care in the United States - organization and current trends RADOSLAV RAYCHEV, MD DEPARTMENTS OF NEUROLOGICAL SURGERY AND NEUROLOGY UNIVERSITY OF CALIFORNIA IRVINE SCHOOL OF MEDICINE
 Acute Stroke Facts Leading cause of disability worldwide 2 nd leading cause of death worldwide >5 million stroke survivors $40 to $50 billion per year in the US 90% of those who survive will have deficits 80 % of strokes can be prevented
Acute Stroke Facts Leading cause of disability worldwide 2 nd leading cause of death worldwide >5 million stroke survivors $40 to $50 billion per year in the US 90% of those who survive will have deficits 80 % of strokes can be prevented
 In a typical acute ischemic stroke, every minute the brain loses 1. 9 million neurons 14 billion synapses 7. 5 miles myelinated fibers -- Saver, Stroke 2006
In a typical acute ischemic stroke, every minute the brain loses 1. 9 million neurons 14 billion synapses 7. 5 miles myelinated fibers -- Saver, Stroke 2006
 Emergent Stroke Care and the Chain of Survival Patient Knowledge Calling 911 EMS ED Staff Stroke Team Stroke Unit
Emergent Stroke Care and the Chain of Survival Patient Knowledge Calling 911 EMS ED Staff Stroke Team Stroke Unit
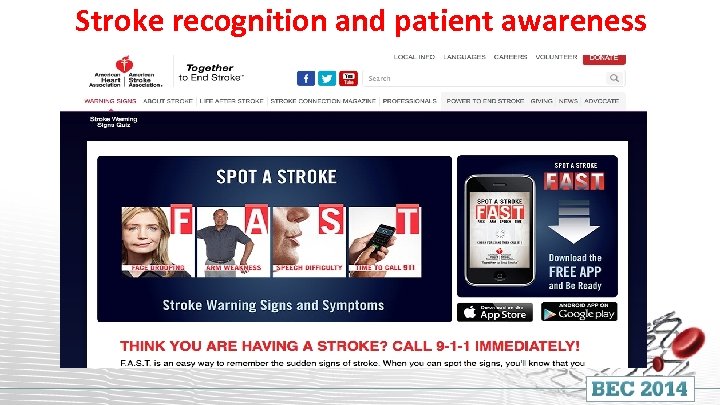 Stroke recognition and patient awareness
Stroke recognition and patient awareness
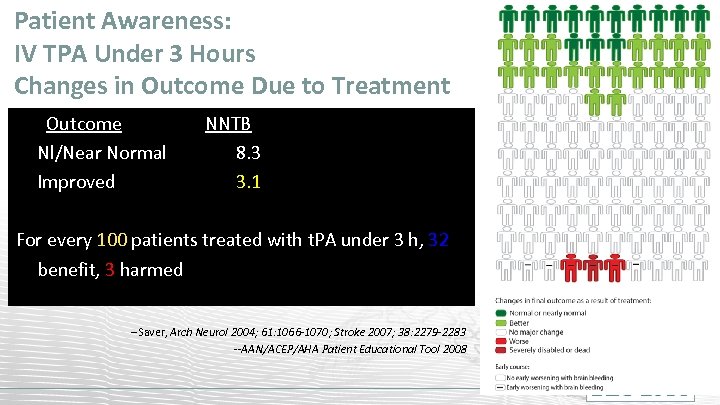 Patient Awareness: IV TPA Under 3 Hours Changes in Outcome Due to Treatment Outcome Nl/Near Normal Improved NNTB 8. 3 3. 1 For every 100 patients treated with t. PA under 3 h, 32 benefit, 3 harmed --Saver, Arch Neurol 2004; 61: 1066 -1070; Stroke 2007; 38: 2279 -2283 --AAN/ACEP/AHA Patient Educational Tool 2008
Patient Awareness: IV TPA Under 3 Hours Changes in Outcome Due to Treatment Outcome Nl/Near Normal Improved NNTB 8. 3 3. 1 For every 100 patients treated with t. PA under 3 h, 32 benefit, 3 harmed --Saver, Arch Neurol 2004; 61: 1066 -1070; Stroke 2007; 38: 2279 -2283 --AAN/ACEP/AHA Patient Educational Tool 2008
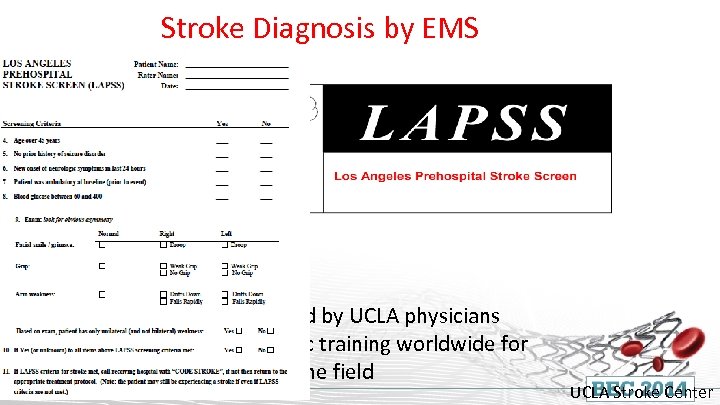 Stroke Diagnosis by EMS • Designed and validated by UCLA physicians • Now part of paramedic training worldwide for recognizing stroke in the field UCLA Stroke Center
Stroke Diagnosis by EMS • Designed and validated by UCLA physicians • Now part of paramedic training worldwide for recognizing stroke in the field UCLA Stroke Center
 Currently Available Recanalization Therapies in Acute Cerebral Ischemia Intravenous IV TPA under 3 hours FDA approved, guideline endorsed, RCT supported IV TPA 3 -. 4. 5 hours RCT supported, guideline endorsed, under FDA review Catheter Mechanical embolectomy ≤ 8 h (Stentrievers) Mechanical aspiration ≤ 8 h (Penumbra device) FDA approved for clot clearance, no RCTs Mechanical angioplasty/stenting FDA approved for clot clearance, no RCTs FDA approved for failed medical therapy IA fibrinolytics ≤ 6 h Off label, 1. 5 positive RCTs, weakly guideline endorsed
Currently Available Recanalization Therapies in Acute Cerebral Ischemia Intravenous IV TPA under 3 hours FDA approved, guideline endorsed, RCT supported IV TPA 3 -. 4. 5 hours RCT supported, guideline endorsed, under FDA review Catheter Mechanical embolectomy ≤ 8 h (Stentrievers) Mechanical aspiration ≤ 8 h (Penumbra device) FDA approved for clot clearance, no RCTs Mechanical angioplasty/stenting FDA approved for clot clearance, no RCTs FDA approved for failed medical therapy IA fibrinolytics ≤ 6 h Off label, 1. 5 positive RCTs, weakly guideline endorsed
 Catheter Intervention - For Large Vessel Occlusion Good outcome for patients with NIHSS > 20 in IMS III Trial: 23. 8% with Endovascular treatment 16. 8% with IV TPA
Catheter Intervention - For Large Vessel Occlusion Good outcome for patients with NIHSS > 20 in IMS III Trial: 23. 8% with Endovascular treatment 16. 8% with IV TPA
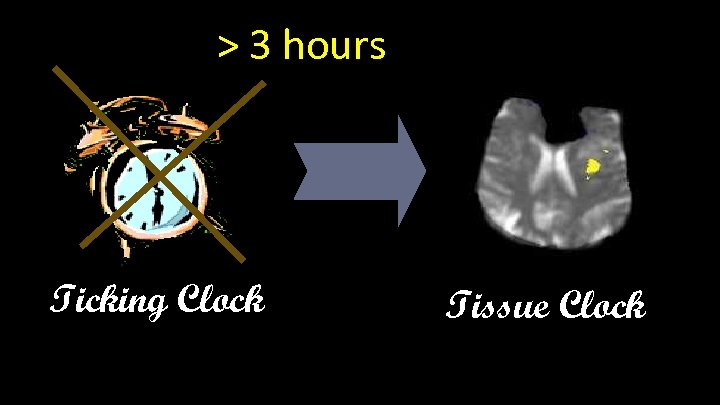 > 3 hours Ticking Clock Tissue Clock
> 3 hours Ticking Clock Tissue Clock
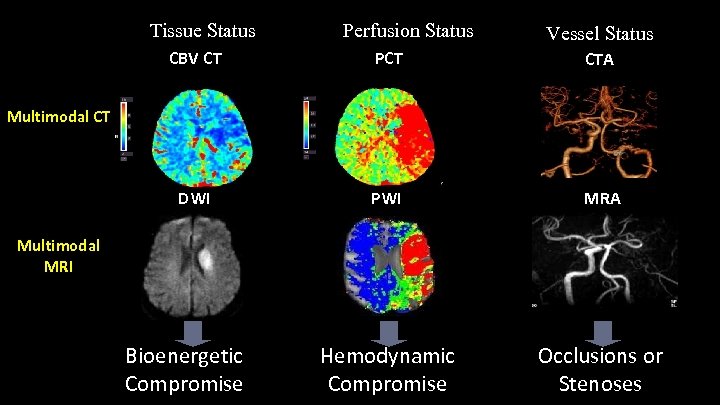 Tissue Status Perfusion Status Vessel Status CBV CT PCT CTA DWI PWI MRA Hemodynamic Compromise Occlusions or Stenoses Multimodal CT Multimodal MRI Bioenergetic Compromise
Tissue Status Perfusion Status Vessel Status CBV CT PCT CTA DWI PWI MRA Hemodynamic Compromise Occlusions or Stenoses Multimodal CT Multimodal MRI Bioenergetic Compromise
 Stroke Systems: Two Tier US Model EMS --Trained dispatchers, high priority triage --Paramedics trained in stroke recognition (e. g. LAPSS) --Deliver patients to nearest stroke capable hospital --Pre-arrival notification Primary Stroke Centers - Spokes --Able to provide initial, acute care --Able to use rt-PA and other acute therapies in a safe and efficient manner --Can admit patients if they have a Stroke Unit Comprehensive Stroke Centers - Hubs --Able to care for complex patients --Advanced treatments (i. e. coils, stents, etc) --Trained specialists in key areas (Vascular neurology, Neurointerventional procedures, Neurocritical Care, Vascular Neurosurgery)
Stroke Systems: Two Tier US Model EMS --Trained dispatchers, high priority triage --Paramedics trained in stroke recognition (e. g. LAPSS) --Deliver patients to nearest stroke capable hospital --Pre-arrival notification Primary Stroke Centers - Spokes --Able to provide initial, acute care --Able to use rt-PA and other acute therapies in a safe and efficient manner --Can admit patients if they have a Stroke Unit Comprehensive Stroke Centers - Hubs --Able to care for complex patients --Advanced treatments (i. e. coils, stents, etc) --Trained specialists in key areas (Vascular neurology, Neurointerventional procedures, Neurocritical Care, Vascular Neurosurgery)
 Brain Attack Coalition American Academy of Neurology American Association of Neurological Surgeons American Association of Neurosciences Nurses American College of Emergency Physicians American Heart Association American Society of Neuroradiology National Institute of Neurologic Disorders and Stroke National Stroke Association Neurocritical Care Society Stroke Belt Consortium Society of Neuro. Interventional Surgery Veterans Administration
Brain Attack Coalition American Academy of Neurology American Association of Neurological Surgeons American Association of Neurosciences Nurses American College of Emergency Physicians American Heart Association American Society of Neuroradiology National Institute of Neurologic Disorders and Stroke National Stroke Association Neurocritical Care Society Stroke Belt Consortium Society of Neuro. Interventional Surgery Veterans Administration
 Supportive Data – Efficacy of Stroke Systems Stroke units (↓ LOS, ↓ complications) Stroke teams (more rapid responses) Neurological expertise (↓ mortality) Use of rt-PA Utility of QI/QA programs Care-Maps
Supportive Data – Efficacy of Stroke Systems Stroke units (↓ LOS, ↓ complications) Stroke teams (more rapid responses) Neurological expertise (↓ mortality) Use of rt-PA Utility of QI/QA programs Care-Maps
 • Circulation (2009) • 790 US hospitals, 2003 -2007 • 322, 847 consecutive ischemic stroke and TIA patients
• Circulation (2009) • 790 US hospitals, 2003 -2007 • 322, 847 consecutive ischemic stroke and TIA patients
 EMS Stroke Center Diversion to primary stroke center: New York Experience Door to stroke team (mins) Door to CT Door to TPA IV TPA rate in TPA eligible Pre 35 161 114 29% 6 wks 17 86 78 50%
EMS Stroke Center Diversion to primary stroke center: New York Experience Door to stroke team (mins) Door to CT Door to TPA IV TPA rate in TPA eligible Pre 35 161 114 29% 6 wks 17 86 78 50%
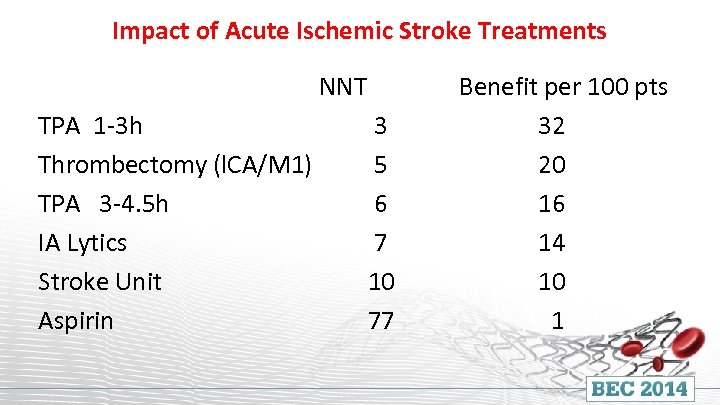 Impact of Acute Ischemic Stroke Treatments NNT TPA 1 -3 h Thrombectomy (l. CA/M 1) TPA 3 -4. 5 h IA Lytics Stroke Unit Aspirin 3 5 6 7 10 77 Benefit per 100 pts 32 20 16 14 10 1
Impact of Acute Ischemic Stroke Treatments NNT TPA 1 -3 h Thrombectomy (l. CA/M 1) TPA 3 -4. 5 h IA Lytics Stroke Unit Aspirin 3 5 6 7 10 77 Benefit per 100 pts 32 20 16 14 10 1
 PRIMARY STROKE CENTER MAP
PRIMARY STROKE CENTER MAP
 BAC Recommendations—Comprehensive Stroke Centers Multidisciplinary group; AAN, ACEP, AANS, AHA, NSA AANN, NIH, ASNR, SBC – Stroke 2005
BAC Recommendations—Comprehensive Stroke Centers Multidisciplinary group; AAN, ACEP, AANS, AHA, NSA AANN, NIH, ASNR, SBC – Stroke 2005
 Comprehensive Stroke Centers: Key Components Neurologists, neurosurgeons, ED personnel, and experts in neuroendovascular procedures Full intensive care unit Neuroimaging interpreted within 20 minutes of acquisition Neurosurgical personnel within 30 minutes Door-to-needle time 60 minutes for IV t. PA Door-to-groin puncture time 90 minutes for IA Availability of rehabilitation services
Comprehensive Stroke Centers: Key Components Neurologists, neurosurgeons, ED personnel, and experts in neuroendovascular procedures Full intensive care unit Neuroimaging interpreted within 20 minutes of acquisition Neurosurgical personnel within 30 minutes Door-to-needle time 60 minutes for IV t. PA Door-to-groin puncture time 90 minutes for IA Availability of rehabilitation services
 Pre Hospital Diversion to Comprehensive Stroke Centers: Endorsed by AHA/ASA
Pre Hospital Diversion to Comprehensive Stroke Centers: Endorsed by AHA/ASA
 UCI Stroke Center
UCI Stroke Center
 Pre Hospital Acute Stroke Treatment The Field Administration of Stroke Therapy – Magnesium (FAST-MAG) Phase III Trial
Pre Hospital Acute Stroke Treatment The Field Administration of Stroke Therapy – Magnesium (FAST-MAG) Phase III Trial
 NIH FAST-MAG Trial throughout LA and Orange County Los Angeles and Orange Counties Ethnically diverse population 13. 3 million Prehospital 2298 paramedics 40 EMS Provider Agencies 315 ambulances Hospital 60 receiving hospitals 952 Physicians Sample 1700 Patients enrolled Jan 2005 – March 2013 Saver et al, International Stroke Conference 2014, San Diego, CA
NIH FAST-MAG Trial throughout LA and Orange County Los Angeles and Orange Counties Ethnically diverse population 13. 3 million Prehospital 2298 paramedics 40 EMS Provider Agencies 315 ambulances Hospital 60 receiving hospitals 952 Physicians Sample 1700 Patients enrolled Jan 2005 – March 2013 Saver et al, International Stroke Conference 2014, San Diego, CA
 FAST-MAG: Novel Aspects Diagnosis of Stroke in the field/ambulance LAPSS Physician Cellphone interview Rating Pretreatments Stroke Severity LAMS Consent Physician cell phone elicitation Randomization Pre-encounter randomization Saver et al, International Stroke Conference 2014, San Diego, CA
FAST-MAG: Novel Aspects Diagnosis of Stroke in the field/ambulance LAPSS Physician Cellphone interview Rating Pretreatments Stroke Severity LAMS Consent Physician cell phone elicitation Randomization Pre-encounter randomization Saver et al, International Stroke Conference 2014, San Diego, CA
 FAST-MAG: Results Specific Aim - Unsuccessful No benefit of Magnesium Field enrollment in phase 3 clinical trial is practical and feasible 74. 3% of stroke patients treated in the first “golden hour” 75% of stroke patients treated in the first 20 min of ambulance arrival LAPSS – 97% accuracy System Aim – Successful Fastest Delivery of Stroke Treatment in a Clinical Trial Pre-hospital EMS assessment with physician by cell phone Saver et al, International Stroke Conference 2014, San Diego, CA
FAST-MAG: Results Specific Aim - Unsuccessful No benefit of Magnesium Field enrollment in phase 3 clinical trial is practical and feasible 74. 3% of stroke patients treated in the first “golden hour” 75% of stroke patients treated in the first 20 min of ambulance arrival LAPSS – 97% accuracy System Aim – Successful Fastest Delivery of Stroke Treatment in a Clinical Trial Pre-hospital EMS assessment with physician by cell phone Saver et al, International Stroke Conference 2014, San Diego, CA
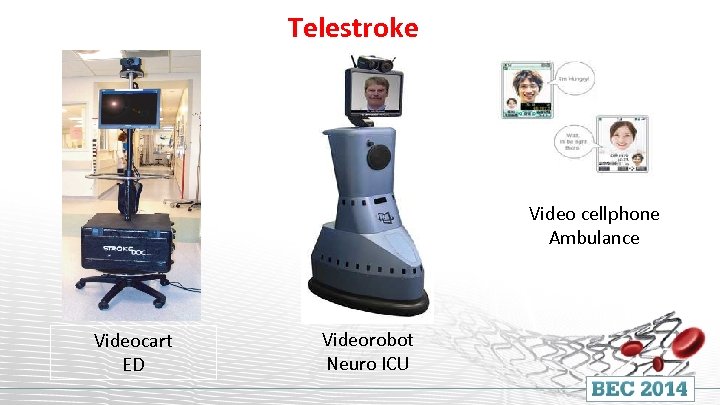 Telestroke Video cellphone Ambulance Videocart ED Videorobot Neuro ICU
Telestroke Video cellphone Ambulance Videocart ED Videorobot Neuro ICU
 Mobile Stroke Units – Future of AIS treatment Prehospital Thrombolysis: A Manual from Berlin STEMO - A specialized ambulance equipped with: Mobile CT scanner Point of care laboratory Telemedicine Ebinger et al, J Vis Exp 2013
Mobile Stroke Units – Future of AIS treatment Prehospital Thrombolysis: A Manual from Berlin STEMO - A specialized ambulance equipped with: Mobile CT scanner Point of care laboratory Telemedicine Ebinger et al, J Vis Exp 2013
 Case Example 60 y/o male with acute aphasia and R hemiplegia (NIHSS 22) Witnessed onset at work 911 called EMS transported the patient to a primary stroke center within 15 min (Riverside county) UCI Stroke Center
Case Example 60 y/o male with acute aphasia and R hemiplegia (NIHSS 22) Witnessed onset at work 911 called EMS transported the patient to a primary stroke center within 15 min (Riverside county) UCI Stroke Center
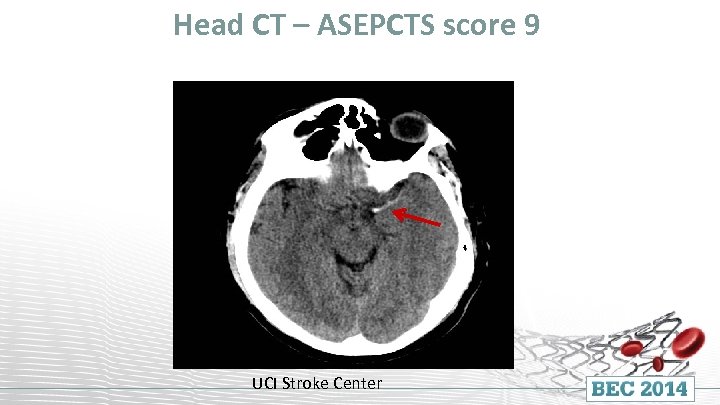 Head CT – ASEPCTS score 9 UCI Stroke Center
Head CT – ASEPCTS score 9 UCI Stroke Center
 Primary Stroke Center Patient was evaluated by teleneurology NIHSS 22 (global aphasia and R hemiplegia) Received IV TPA No improvement noted
Primary Stroke Center Patient was evaluated by teleneurology NIHSS 22 (global aphasia and R hemiplegia) Received IV TPA No improvement noted
 Comprehensive Stroke Center Transferred to UCI Stroke Center via ambulance Arrived at UCI within 3. 5 hours after onset Repeat exam showed persistent global aphasia and R sided hemiplegia – NIHSS 22 UCI Stroke Center
Comprehensive Stroke Center Transferred to UCI Stroke Center via ambulance Arrived at UCI within 3. 5 hours after onset Repeat exam showed persistent global aphasia and R sided hemiplegia – NIHSS 22 UCI Stroke Center
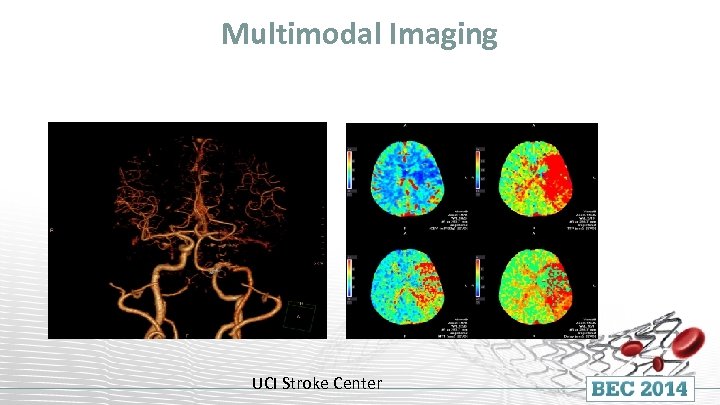 Multimodal Imaging UCI Stroke Center
Multimodal Imaging UCI Stroke Center
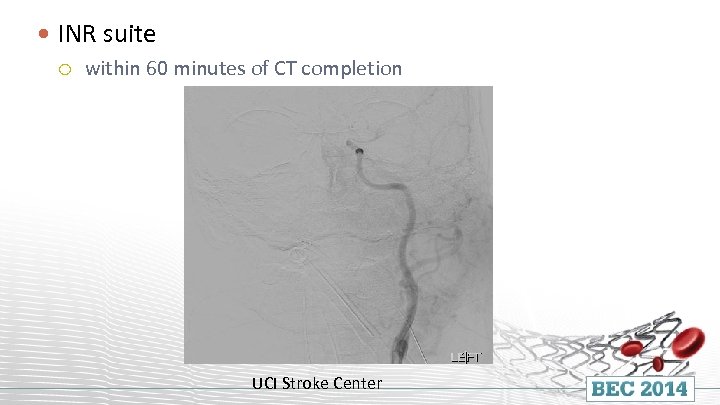 INR suite within 60 minutes of CT completion UCI Stroke Center
INR suite within 60 minutes of CT completion UCI Stroke Center
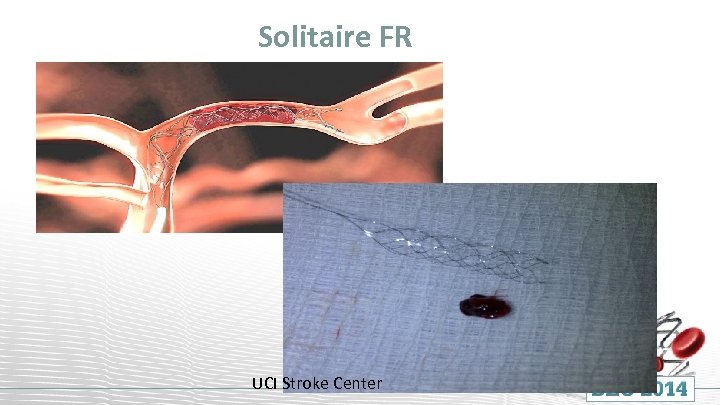 Solitaire FR UCI Stroke Center
Solitaire FR UCI Stroke Center
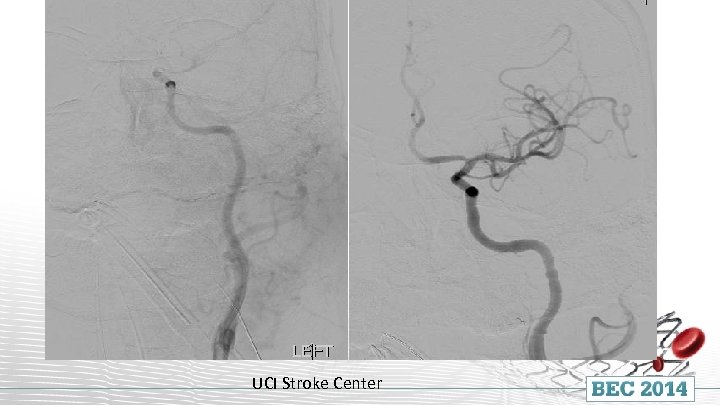 UCI Stroke Center
UCI Stroke Center
 Follow up Substantial improvement within 24 hours: Patient is moving the right side against gravity, comprehends and utters simple words = NIHSS 10 UCI Stroke Center
Follow up Substantial improvement within 24 hours: Patient is moving the right side against gravity, comprehends and utters simple words = NIHSS 10 UCI Stroke Center
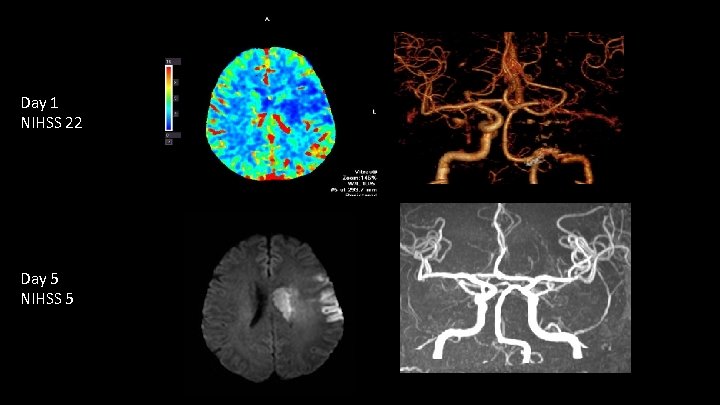 Day 1 NIHSS 22 Day 5 NIHSS 5 UCI Stroke Center
Day 1 NIHSS 22 Day 5 NIHSS 5 UCI Stroke Center
 60 y/o male with acute right sided weakness and inability to speak Last known well 911 call Primary Stroke Center arrival Teleneurology consult IV TPA Comprehensive Stroke Center arrival Multimodal Imaging IA Recanalization @ 7: 00 AM @ 10 min @ 30 min @ 1 hr 05 min @ 2 hr @ 3 hr 30 min @ 3 hr 50 min @ 5 hr 10 min
60 y/o male with acute right sided weakness and inability to speak Last known well 911 call Primary Stroke Center arrival Teleneurology consult IV TPA Comprehensive Stroke Center arrival Multimodal Imaging IA Recanalization @ 7: 00 AM @ 10 min @ 30 min @ 1 hr 05 min @ 2 hr @ 3 hr 30 min @ 3 hr 50 min @ 5 hr 10 min
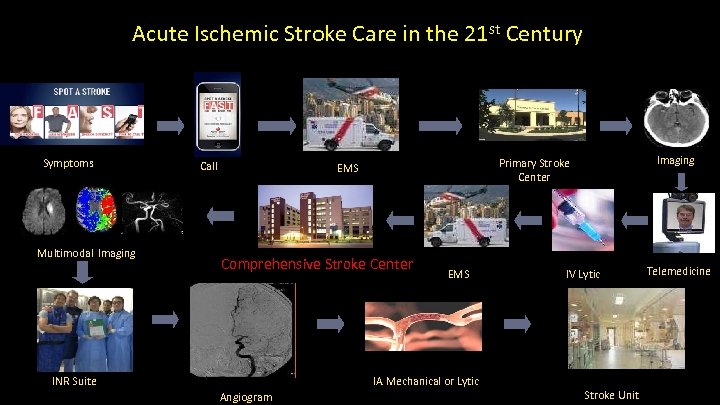 Acute Ischemic Stroke Care in the 21 st Century UCI Stroke Center Symptoms Multimodal Imaging Call Comprehensive Stroke Center INR Suite EMS IA Mechanical or Lytic Angiogram Imaging Primary Stroke Center EMS IV Lytic Stroke Unit Telemedicine
Acute Ischemic Stroke Care in the 21 st Century UCI Stroke Center Symptoms Multimodal Imaging Call Comprehensive Stroke Center INR Suite EMS IA Mechanical or Lytic Angiogram Imaging Primary Stroke Center EMS IV Lytic Stroke Unit Telemedicine


