e0b0730f4e4f69c752d426e81a641530.ppt
- Количество слайдов: 108
 Community Acquired Methicillin- Resistant Staphylococcus aureus Mohamad Mooty, M. D. Infectious Diseases Eastern Maine Medical Center
Community Acquired Methicillin- Resistant Staphylococcus aureus Mohamad Mooty, M. D. Infectious Diseases Eastern Maine Medical Center
 MRSA Historical Aspects 1959 First clinical use of methicillin 1961 First description of MRSA 1967 First report of nosocomial infection in the US (2 cases) 1968 Increase in MRSA in the UK 1968 -1979 Rise and subsequent wane of prevalence of MRSA (especially nosocomial infections) in Europe, Australia, and elsewhere (except US) 1975 -1980 First reports of problems with MRSA in the US; most occurred in large tertiary care hospitals (especially burn units and ICUs) 1980 MRSA increase in prevalence in US nursing homes; CA-MRSA infections in the US 1998 Emergence of CA-MRSA
MRSA Historical Aspects 1959 First clinical use of methicillin 1961 First description of MRSA 1967 First report of nosocomial infection in the US (2 cases) 1968 Increase in MRSA in the UK 1968 -1979 Rise and subsequent wane of prevalence of MRSA (especially nosocomial infections) in Europe, Australia, and elsewhere (except US) 1975 -1980 First reports of problems with MRSA in the US; most occurred in large tertiary care hospitals (especially burn units and ICUs) 1980 MRSA increase in prevalence in US nursing homes; CA-MRSA infections in the US 1998 Emergence of CA-MRSA
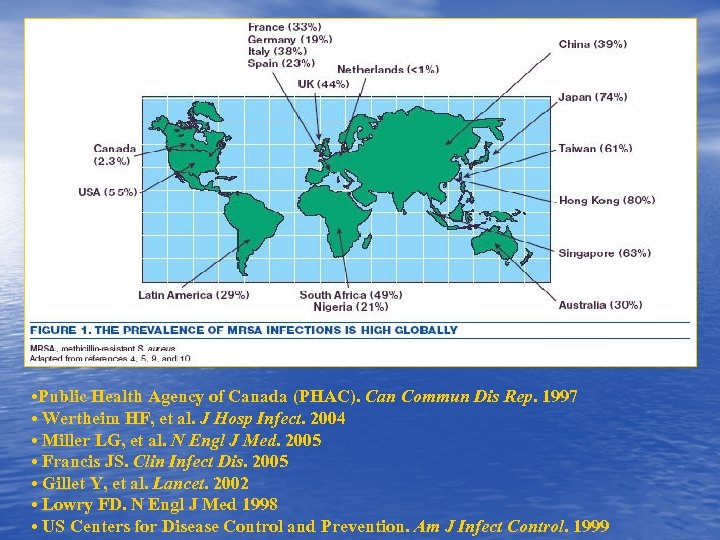 • Public Health Agency of Canada (PHAC). Can Commun Dis Rep. 1997 • Wertheim HF, et al. J Hosp Infect. 2004 • Miller LG, et al. N Engl J Med. 2005 • Francis JS. Clin Infect Dis. 2005 • Gillet Y, et al. Lancet. 2002 • Lowry FD. N Engl J Med 1998 • US Centers for Disease Control and Prevention. Am J Infect Control. 1999
• Public Health Agency of Canada (PHAC). Can Commun Dis Rep. 1997 • Wertheim HF, et al. J Hosp Infect. 2004 • Miller LG, et al. N Engl J Med. 2005 • Francis JS. Clin Infect Dis. 2005 • Gillet Y, et al. Lancet. 2002 • Lowry FD. N Engl J Med 1998 • US Centers for Disease Control and Prevention. Am J Infect Control. 1999
 MRSA Historical Aspects • USA Prevalence in ICU: 60 percent • More than 90, 000 invasive infections due to MRSA occurred in the United States in 2005
MRSA Historical Aspects • USA Prevalence in ICU: 60 percent • More than 90, 000 invasive infections due to MRSA occurred in the United States in 2005
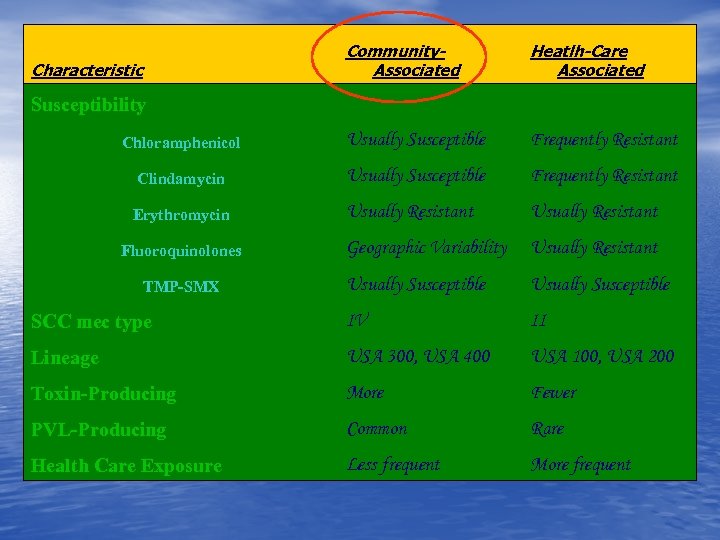 Characteristic Community. Associated Heatlh-Care Associated Susceptibility Chloramphenicol Usually Susceptible Frequently Resistant Clindamycin Usually Susceptible Frequently Resistant Erythromycin Usually Resistant Geographic Variability Usually Resistant Usually Susceptible SCC mec type IV II Lineage USA 300, USA 400 USA 100, USA 200 Toxin-Producing More Fewer PVL-Producing Common Rare Health Care Exposure Less frequent More frequent Fluoroquinolones TMP-SMX
Characteristic Community. Associated Heatlh-Care Associated Susceptibility Chloramphenicol Usually Susceptible Frequently Resistant Clindamycin Usually Susceptible Frequently Resistant Erythromycin Usually Resistant Geographic Variability Usually Resistant Usually Susceptible SCC mec type IV II Lineage USA 300, USA 400 USA 100, USA 200 Toxin-Producing More Fewer PVL-Producing Common Rare Health Care Exposure Less frequent More frequent Fluoroquinolones TMP-SMX
 v. Definition v. History v. Epidemiology v. Clinical Features v. Virulence Factors v. Risk Factors v. Clinical Management “Outpatient” v Prevention “Decolonization”
v. Definition v. History v. Epidemiology v. Clinical Features v. Virulence Factors v. Risk Factors v. Clinical Management “Outpatient” v Prevention “Decolonization”
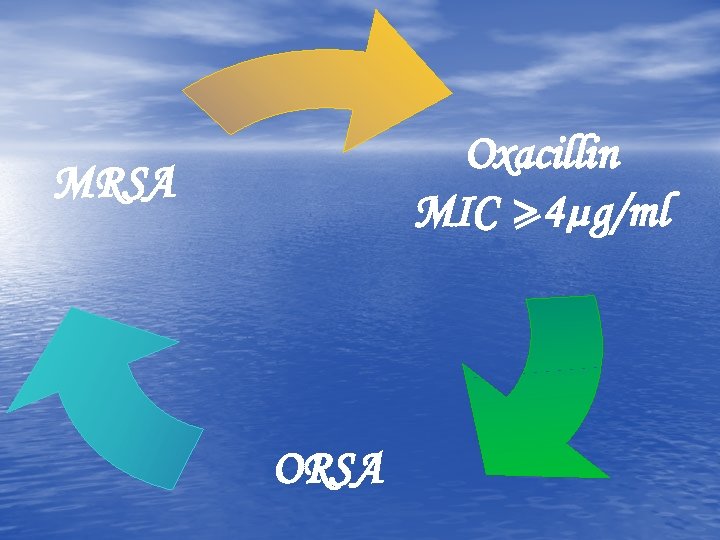 Oxacillin MIC > 4µg/ml MRSA ORSA
Oxacillin MIC > 4µg/ml MRSA ORSA
 • CDC: Defining c-MRSA Illness Compatible with Staphylococcal Disease MRSA Cultured from site Outpatient Setting Hospital admission: < 48 hours No Admission within the past year: ❁Health Care Facility ❁Surgery ❁Dialysis ❁Permanent Indwelling Catheter ❁Percutaneous Medical Device MMWR 2004; 53: 767 -70
• CDC: Defining c-MRSA Illness Compatible with Staphylococcal Disease MRSA Cultured from site Outpatient Setting Hospital admission: < 48 hours No Admission within the past year: ❁Health Care Facility ❁Surgery ❁Dialysis ❁Permanent Indwelling Catheter ❁Percutaneous Medical Device MMWR 2004; 53: 767 -70
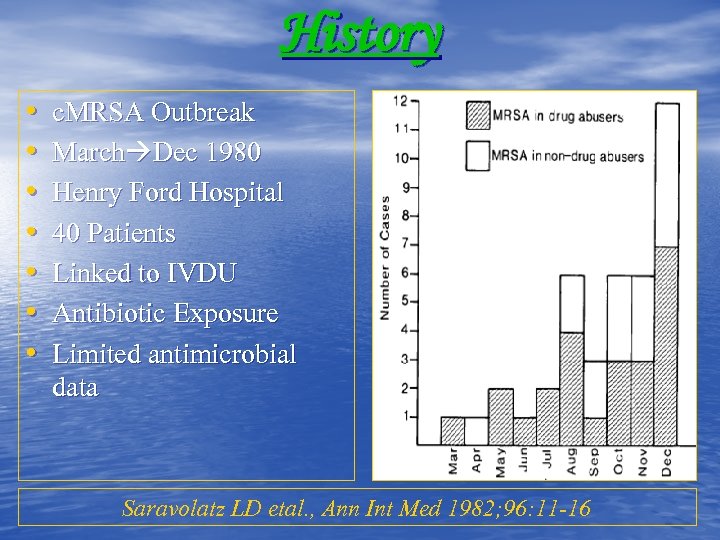 History • • c. MRSA Outbreak March Dec 1980 Henry Ford Hospital 40 Patients Linked to IVDU Antibiotic Exposure Limited antimicrobial data Saravolatz LD etal. , Ann Int Med 1982; 96: 11 -16
History • • c. MRSA Outbreak March Dec 1980 Henry Ford Hospital 40 Patients Linked to IVDU Antibiotic Exposure Limited antimicrobial data Saravolatz LD etal. , Ann Int Med 1982; 96: 11 -16
 History • Brian MJ, Ped Infect Dis J 1989 • Taylor G etal. , Can J Infect Dis 1990 • Udo EE etal. , J Hosp Infect 1993 • Pate KR etal. , Lancet 1995 • Maguire GP etal. , Med J Aust 1996 • Heffernan H etal. , Lab. Link 1997 • Durmaz B, J Hosp Infect 1997 • Collignon P etal. , Lancet 1998 • Herolds BC etal. , JAMA 1998
History • Brian MJ, Ped Infect Dis J 1989 • Taylor G etal. , Can J Infect Dis 1990 • Udo EE etal. , J Hosp Infect 1993 • Pate KR etal. , Lancet 1995 • Maguire GP etal. , Med J Aust 1996 • Heffernan H etal. , Lab. Link 1997 • Durmaz B, J Hosp Infect 1997 • Collignon P etal. , Lancet 1998 • Herolds BC etal. , JAMA 1998
 History Mississippi Chicago Australia c. MRSA Turkey New Guinea New Zealand Canada
History Mississippi Chicago Australia c. MRSA Turkey New Guinea New Zealand Canada
 History C-MRSA Epidemic Potential SSTI Non β-Lactam Susceptible Poor Hygiene
History C-MRSA Epidemic Potential SSTI Non β-Lactam Susceptible Poor Hygiene
 History • 4 Fatal Pediatric c. MRSA infections • Bacteremia Sepsis • Non-multiresistant Strains • Distinct: Nosocomial • Typing: Related MMWR 1999
History • 4 Fatal Pediatric c. MRSA infections • Bacteremia Sepsis • Non-multiresistant Strains • Distinct: Nosocomial • Typing: Related MMWR 1999
 v. Specialized MRSA surveillance project in 2001 v. Active Bacterial Core Surveillance program: ❁Population-based ❁Epidemiologic Features ❁Invasive Bacterial Diseases
v. Specialized MRSA surveillance project in 2001 v. Active Bacterial Core Surveillance program: ❁Population-based ❁Epidemiologic Features ❁Invasive Bacterial Diseases
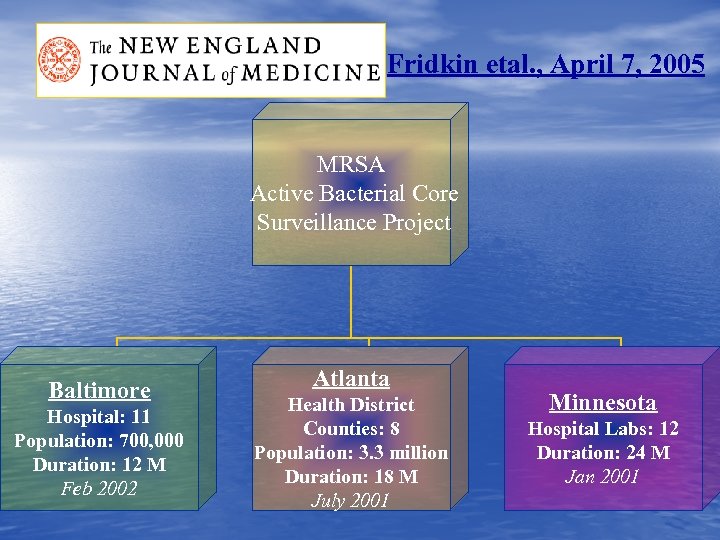 Fridkin etal. , April 7, 2005 MRSA Active Bacterial Core Surveillance Project Baltimore Hospital: 11 Population: 700, 000 Duration: 12 M Feb 2002 Atlanta Health District Counties: 8 Population: 3. 3 million Duration: 18 M July 2001 Minnesota Hospital Labs: 12 Duration: 24 M Jan 2001
Fridkin etal. , April 7, 2005 MRSA Active Bacterial Core Surveillance Project Baltimore Hospital: 11 Population: 700, 000 Duration: 12 M Feb 2002 Atlanta Health District Counties: 8 Population: 3. 3 million Duration: 18 M July 2001 Minnesota Hospital Labs: 12 Duration: 24 M Jan 2001
 20% 12% 8%
20% 12% 8%
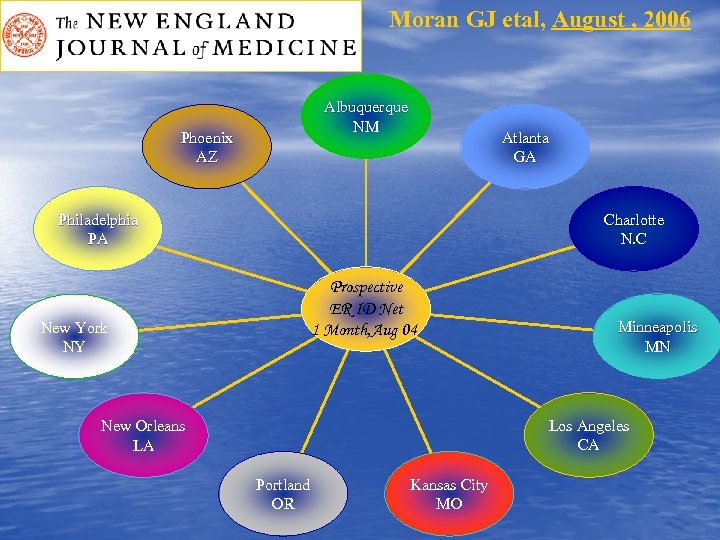 Moran GJ etal, August , 2006 Albuquerque NM Phoenix AZ Atlanta GA Philadelphia PA Charlotte N. C Prospective ER ID Net 1 Month, Aug 04 New York NY Minneapolis MN Los Angeles CA New Orleans LA Portland OR Kansas City MO
Moran GJ etal, August , 2006 Albuquerque NM Phoenix AZ Atlanta GA Philadelphia PA Charlotte N. C Prospective ER ID Net 1 Month, Aug 04 New York NY Minneapolis MN Los Angeles CA New Orleans LA Portland OR Kansas City MO
 Moran GJ etal, August , 2006 v SSTI: 422 patients S. aureus: 320 patients (76%) v MRSA: 249 Patients (78%) v OVERALL Prevalence: 59 % (15 74%). v Pulsed-field type USA 300: 97 % v SCCmec type IV & Panton–Valentine leukocidin toxin gene: 98 % v Susceptibility: ❁ Clindamycin: 95 % ❁ Erythromycin: 6 % ❁ Fluoroquinolones: 60% ❁ Rifampin: 100% ❁ TMP-SMX: 100% ❁ Tetracyclin: 92% ❁ Discordant Antibiotic Therapy: 100/175 patients (57 percent).
Moran GJ etal, August , 2006 v SSTI: 422 patients S. aureus: 320 patients (76%) v MRSA: 249 Patients (78%) v OVERALL Prevalence: 59 % (15 74%). v Pulsed-field type USA 300: 97 % v SCCmec type IV & Panton–Valentine leukocidin toxin gene: 98 % v Susceptibility: ❁ Clindamycin: 95 % ❁ Erythromycin: 6 % ❁ Fluoroquinolones: 60% ❁ Rifampin: 100% ❁ TMP-SMX: 100% ❁ Tetracyclin: 92% ❁ Discordant Antibiotic Therapy: 100/175 patients (57 percent).
 Prepared by Anne R. Sites, MPH www. mainpublichealth. gov
Prepared by Anne R. Sites, MPH www. mainpublichealth. gov
 Infectious Disease Epidemiology Report 2004 -05 • Annual Average: 111 Cases • Incidence Rate: 8. 6 cases/100, 000 Population • Gender: Male (57 %) • Race: 94% White “Information available for 68 cases”
Infectious Disease Epidemiology Report 2004 -05 • Annual Average: 111 Cases • Incidence Rate: 8. 6 cases/100, 000 Population • Gender: Male (57 %) • Race: 94% White “Information available for 68 cases”
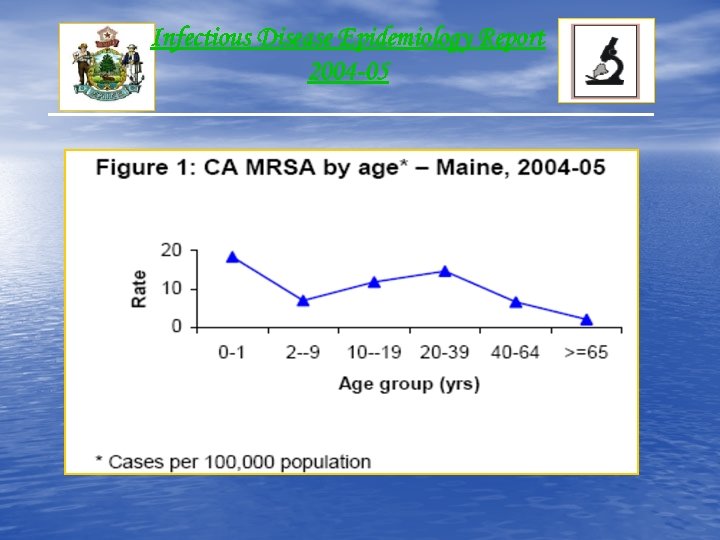 Infectious Disease Epidemiology Report 2004 -05
Infectious Disease Epidemiology Report 2004 -05
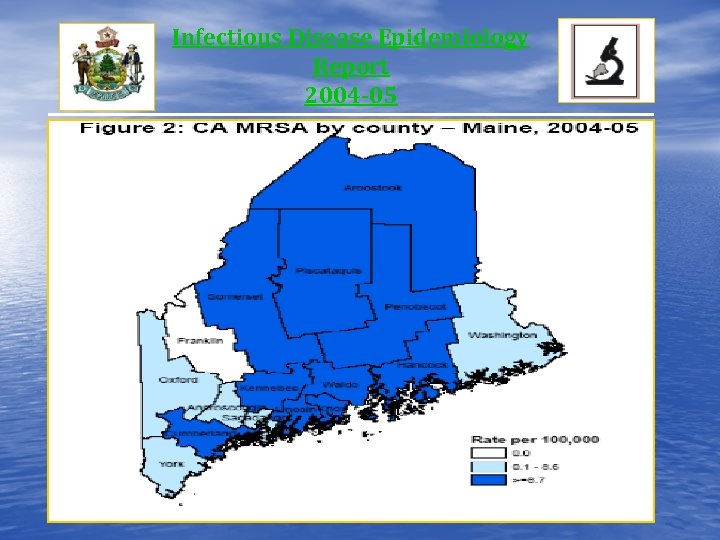 Infectious Disease Epidemiology Report 2004 -05
Infectious Disease Epidemiology Report 2004 -05
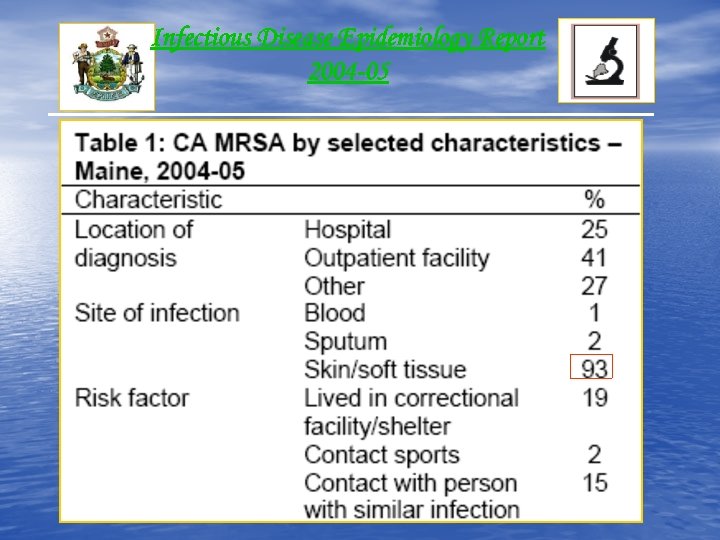 Infectious Disease Epidemiology Report 2004 -05
Infectious Disease Epidemiology Report 2004 -05
 Infectious Disease Epidemiology Report 2004 -05 v. Four clusters v 26 MRSA skin infections v. The final sources of infection were not determined v. Risks factors: ● Sharing of personal items ● Assisting in changing of wound dressings ● Tattooing
Infectious Disease Epidemiology Report 2004 -05 v. Four clusters v 26 MRSA skin infections v. The final sources of infection were not determined v. Risks factors: ● Sharing of personal items ● Assisting in changing of wound dressings ● Tattooing

 Common Presentation v. Younger Patients v No risk Factors v Boils/ Abscesses
Common Presentation v. Younger Patients v No risk Factors v Boils/ Abscesses
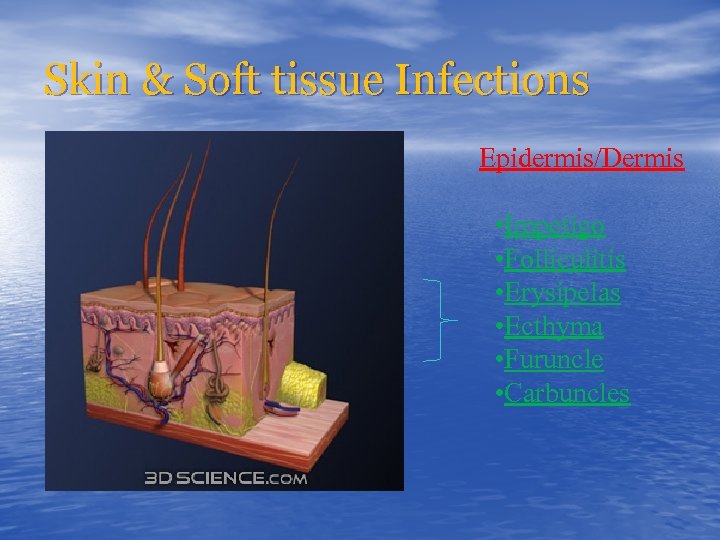 Skin & Soft tissue Infections Epidermis/Dermis • Impetigo • Folliculitis • Erysipelas • Ecthyma • Furuncle • Carbuncles
Skin & Soft tissue Infections Epidermis/Dermis • Impetigo • Folliculitis • Erysipelas • Ecthyma • Furuncle • Carbuncles
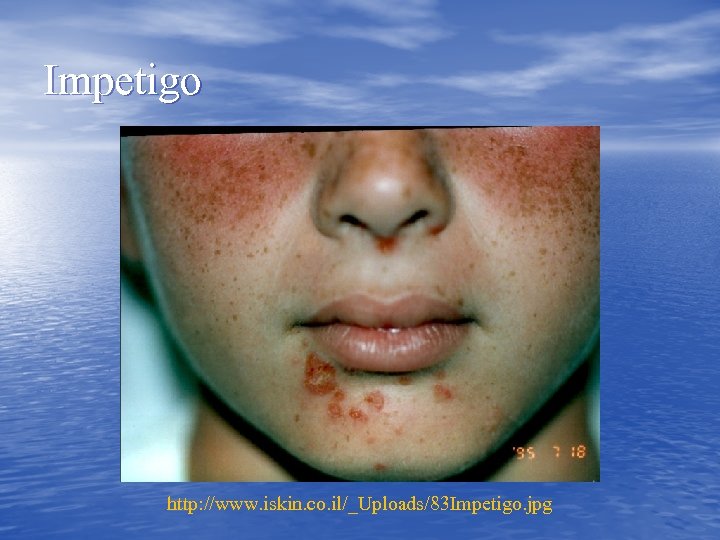 Impetigo http: //www. iskin. co. il/_Uploads/83 Impetigo. jpg
Impetigo http: //www. iskin. co. il/_Uploads/83 Impetigo. jpg
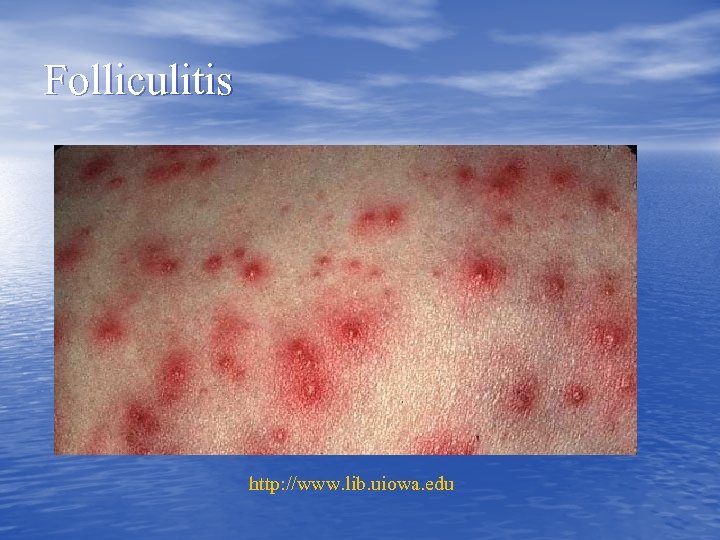 Folliculitis http: //www. lib. uiowa. edu
Folliculitis http: //www. lib. uiowa. edu
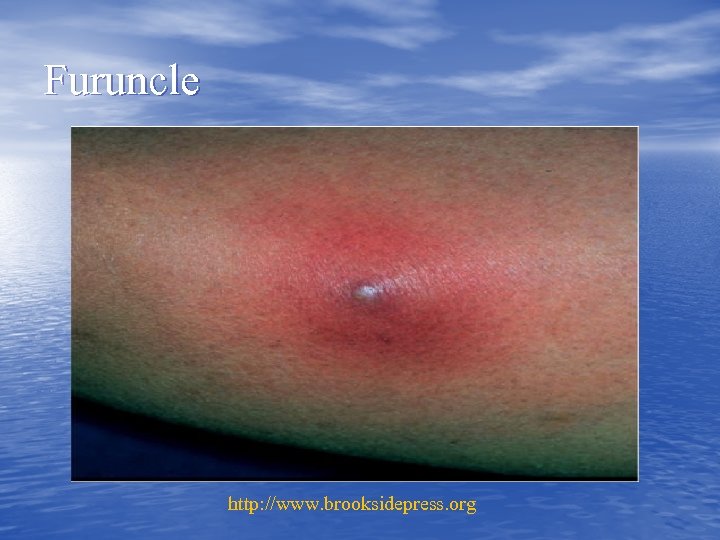 Furuncle http: //www. brooksidepress. org
Furuncle http: //www. brooksidepress. org
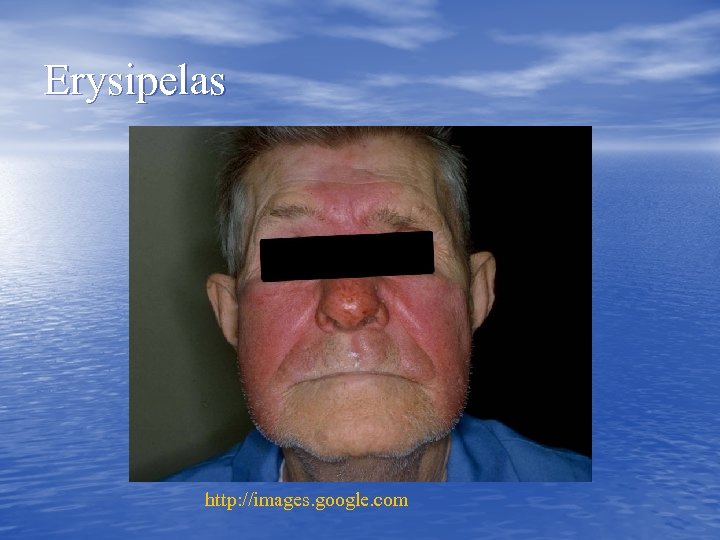 Erysipelas http: //images. google. com
Erysipelas http: //images. google. com
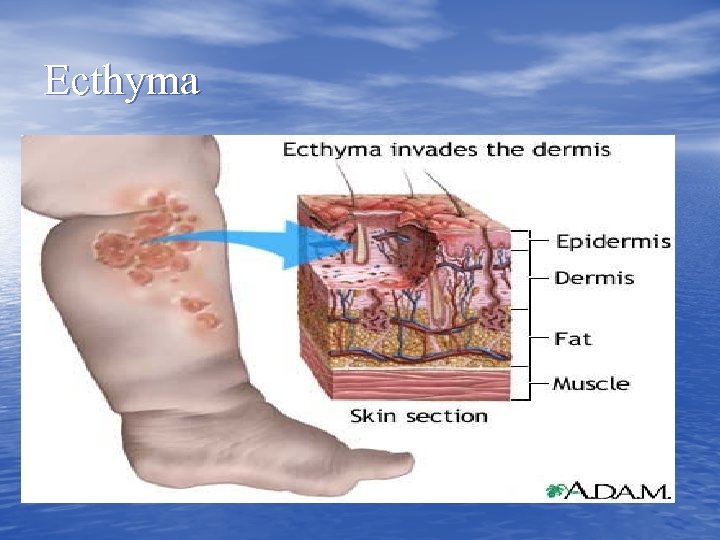 Ecthyma
Ecthyma
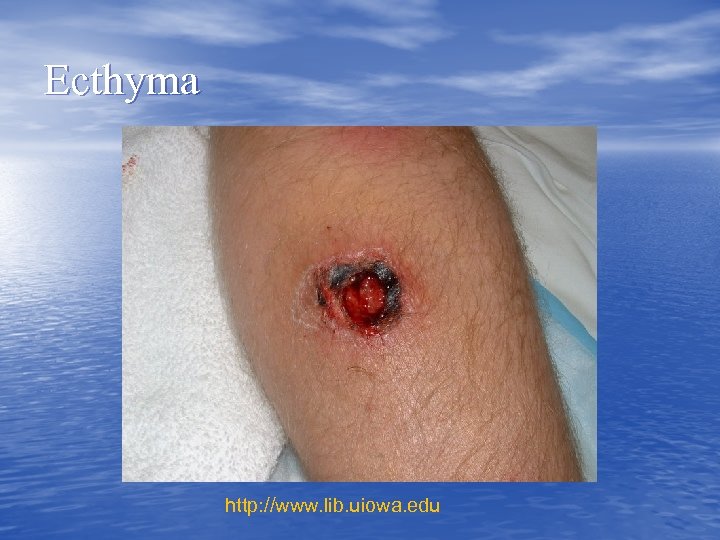 Ecthyma http: //www. lib. uiowa. edu
Ecthyma http: //www. lib. uiowa. edu
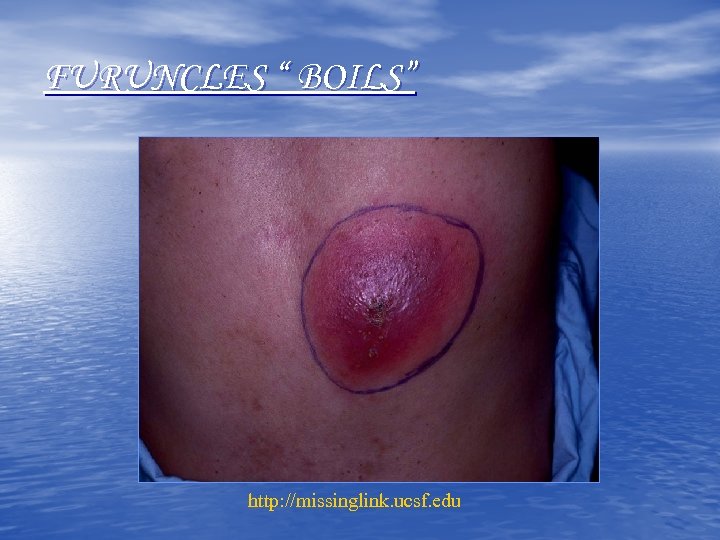 FURUNCLES “ BOILS” http: //missinglink. ucsf. edu
FURUNCLES “ BOILS” http: //missinglink. ucsf. edu
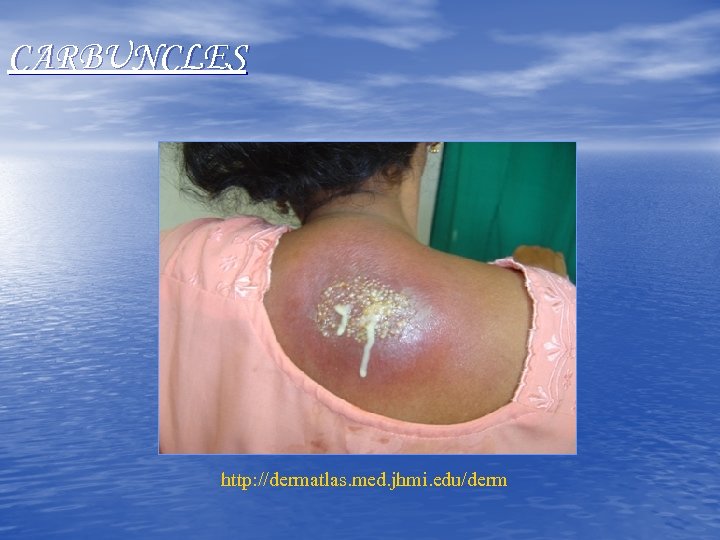 CARBUNCLES http: //dermatlas. med. jhmi. edu/derm
CARBUNCLES http: //dermatlas. med. jhmi. edu/derm
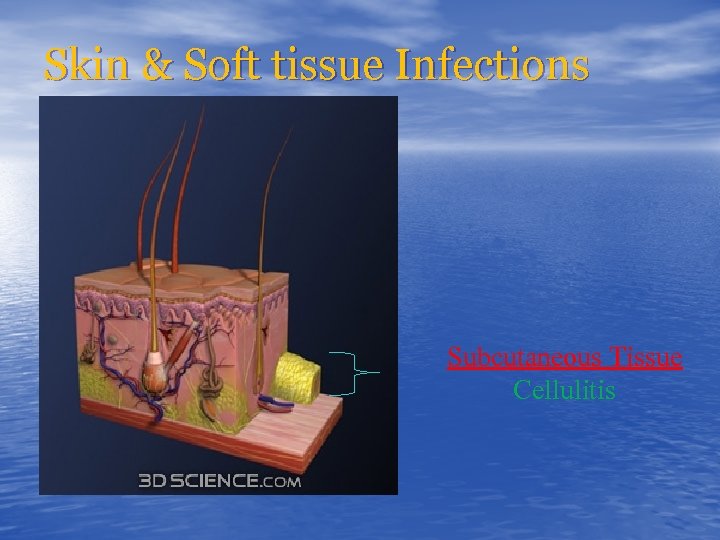 Skin & Soft tissue Infections Subcutaneous Tissue Cellulitis
Skin & Soft tissue Infections Subcutaneous Tissue Cellulitis
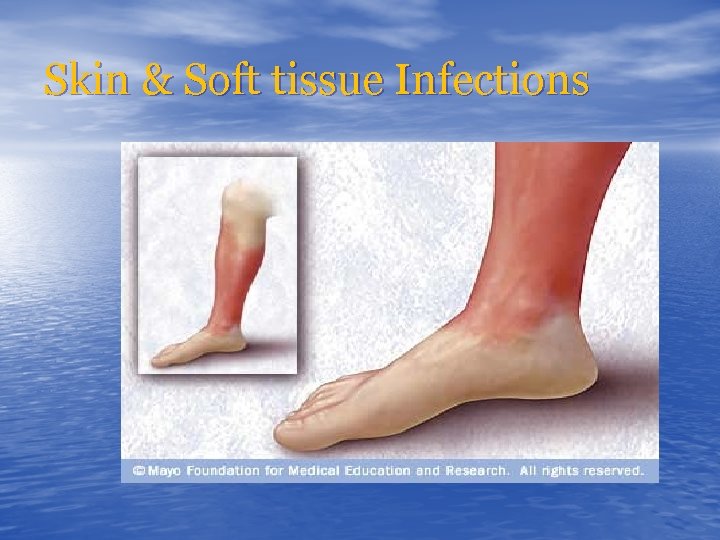 Skin & Soft tissue Infections
Skin & Soft tissue Infections
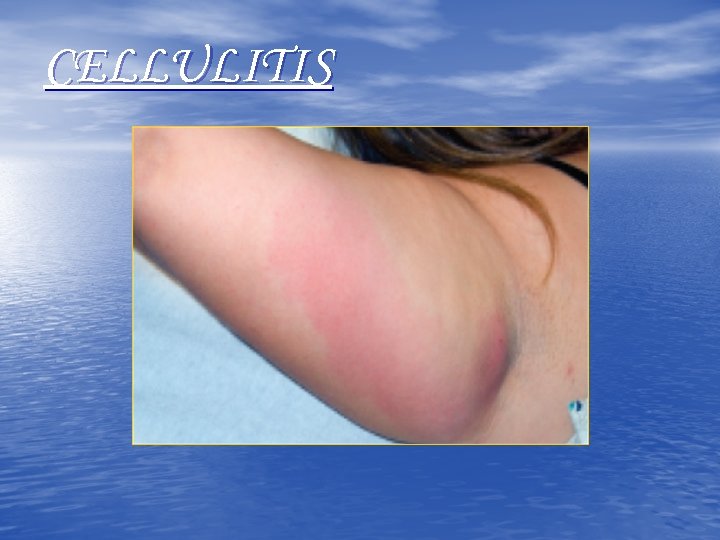 CELLULITIS
CELLULITIS
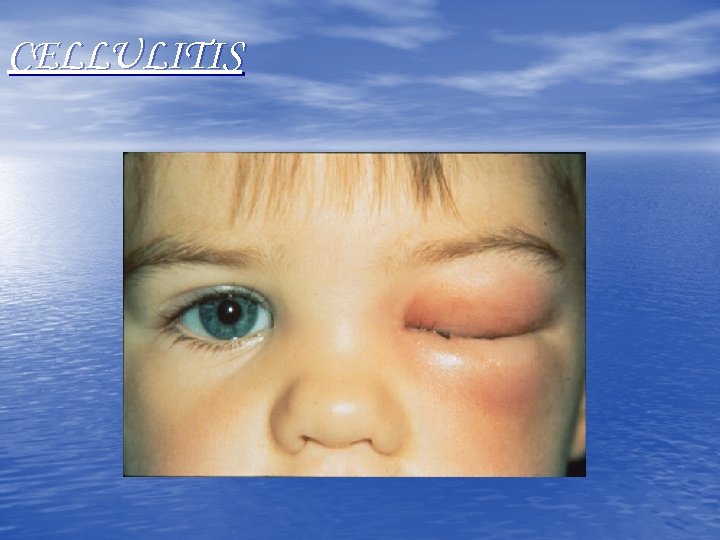 CELLULITIS
CELLULITIS
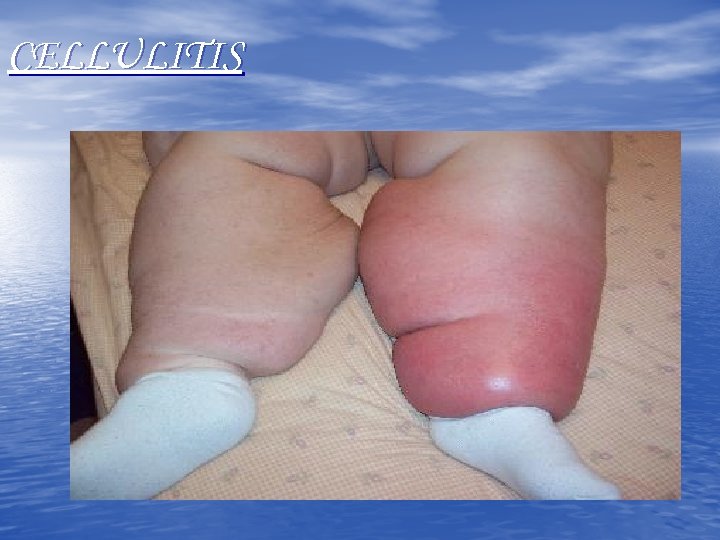 CELLULITIS
CELLULITIS
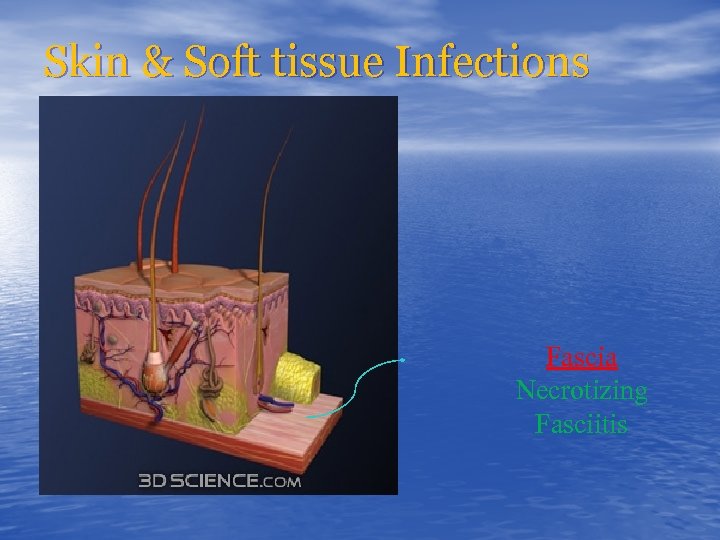 Skin & Soft tissue Infections Fascia Necrotizing Fasciitis
Skin & Soft tissue Infections Fascia Necrotizing Fasciitis
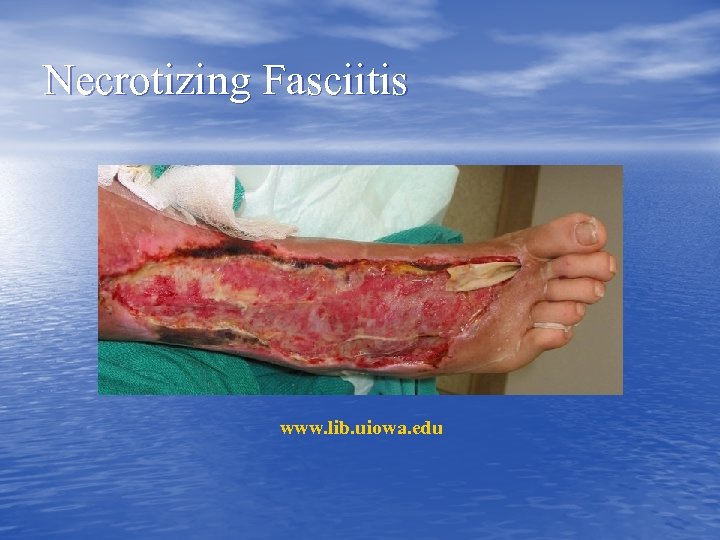 Necrotizing Fasciitis www. lib. uiowa. edu
Necrotizing Fasciitis www. lib. uiowa. edu
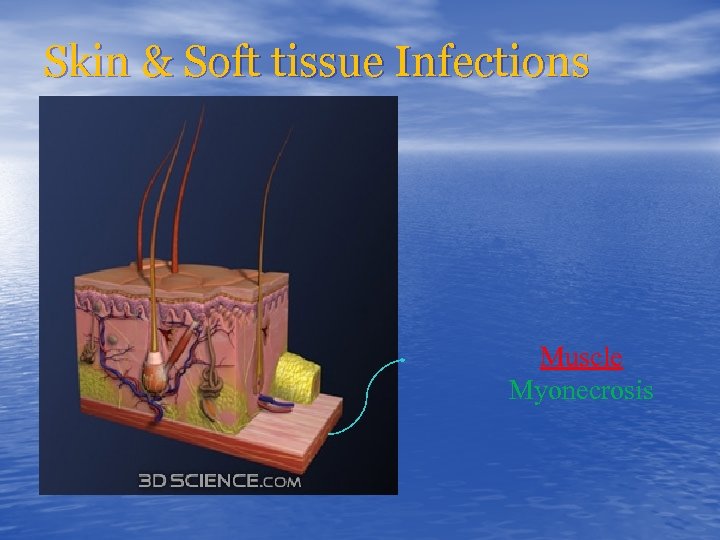 Skin & Soft tissue Infections Muscle Myonecrosis
Skin & Soft tissue Infections Muscle Myonecrosis
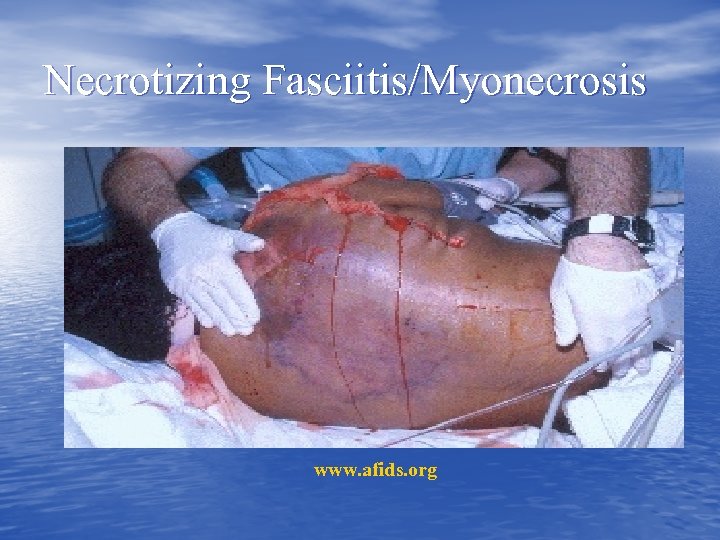 Necrotizing Fasciitis/Myonecrosis www. afids. org
Necrotizing Fasciitis/Myonecrosis www. afids. org
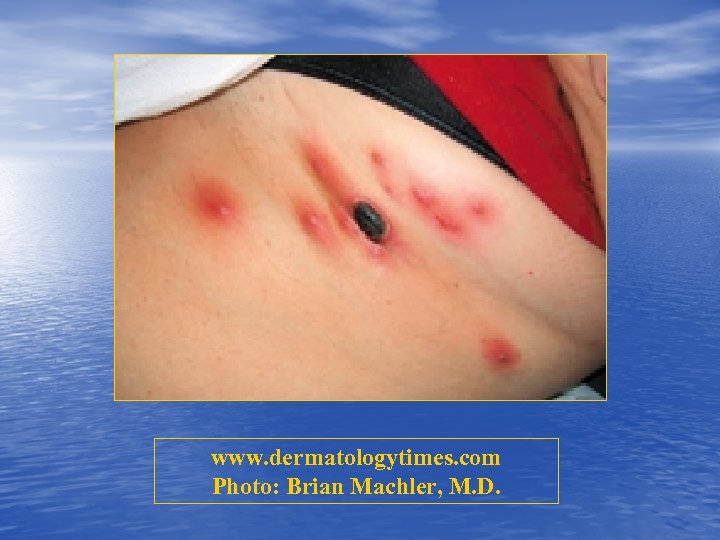 www. dermatologytimes. com Photo: Brian Machler, M. D.
www. dermatologytimes. com Photo: Brian Machler, M. D.
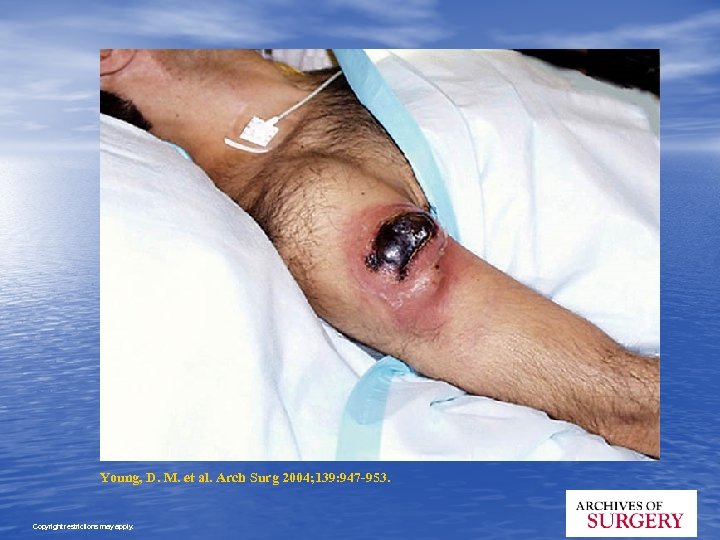 Young, D. M. et al. Arch Surg 2004; 139: 947 -953. Copyright restrictions may apply.
Young, D. M. et al. Arch Surg 2004; 139: 947 -953. Copyright restrictions may apply.
 Serious Infections Case Reports v Bacteremia “MMWR 1999” v Osteomyelitis/ Pyomyositis “ Pate et al. , Lancet 1995” v Sepsis Syndrome “Mongkolrattanothai K etal, CID , 2003”
Serious Infections Case Reports v Bacteremia “MMWR 1999” v Osteomyelitis/ Pyomyositis “ Pate et al. , Lancet 1995” v Sepsis Syndrome “Mongkolrattanothai K etal, CID , 2003”
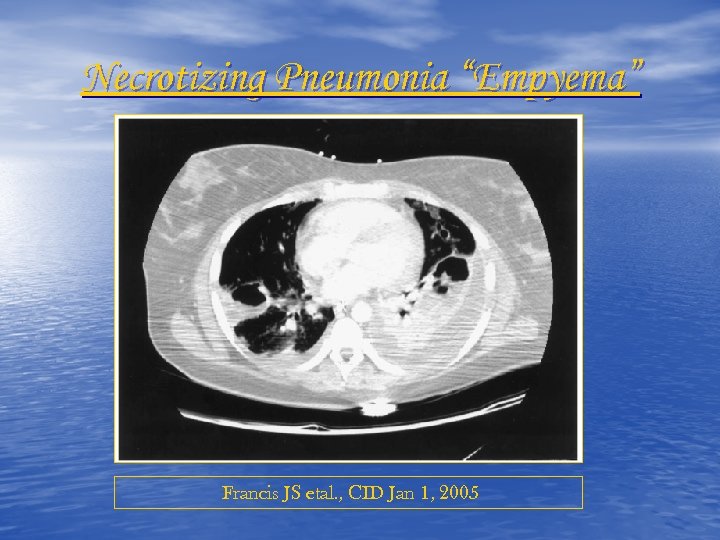 Necrotizing Pneumonia “Empyema” Francis JS etal. , CID Jan 1, 2005
Necrotizing Pneumonia “Empyema” Francis JS etal. , CID Jan 1, 2005
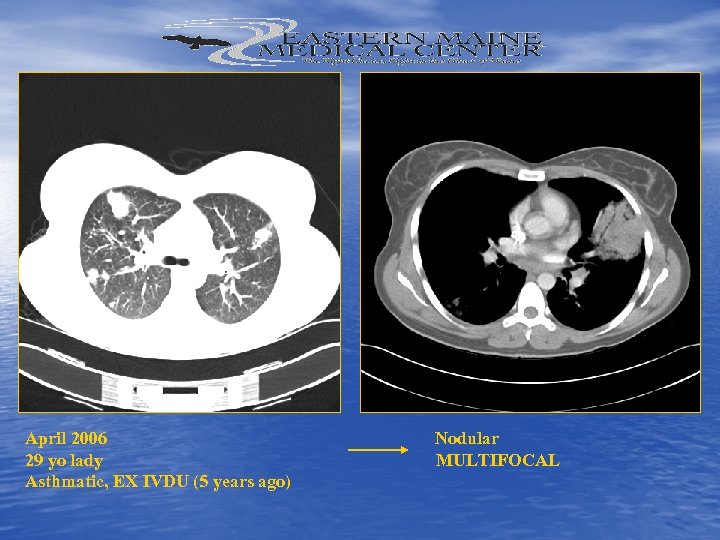 April 2006 Nodular 29 yo lady MULTIFOCAL Asthmatic, EX IVDU (5 years ago)
April 2006 Nodular 29 yo lady MULTIFOCAL Asthmatic, EX IVDU (5 years ago)
 Endocarditis v. Johns Hopkins University Hospital, Baltimore, MD. v. Retrospective chart review: 12 months v. Positive blood cultures v. No risk factors for MRSA acquisition v. Modified Duke's criteria: Five / 193 patients. v. Isolates: PVL gene positive Type IV SCCmec element. v PFGE: Skin isolate identical to blood isolate Bahrain M. et al, Scand J Infect Dis. 2006; 38(8): 702 -7.
Endocarditis v. Johns Hopkins University Hospital, Baltimore, MD. v. Retrospective chart review: 12 months v. Positive blood cultures v. No risk factors for MRSA acquisition v. Modified Duke's criteria: Five / 193 patients. v. Isolates: PVL gene positive Type IV SCCmec element. v PFGE: Skin isolate identical to blood isolate Bahrain M. et al, Scand J Infect Dis. 2006; 38(8): 702 -7.
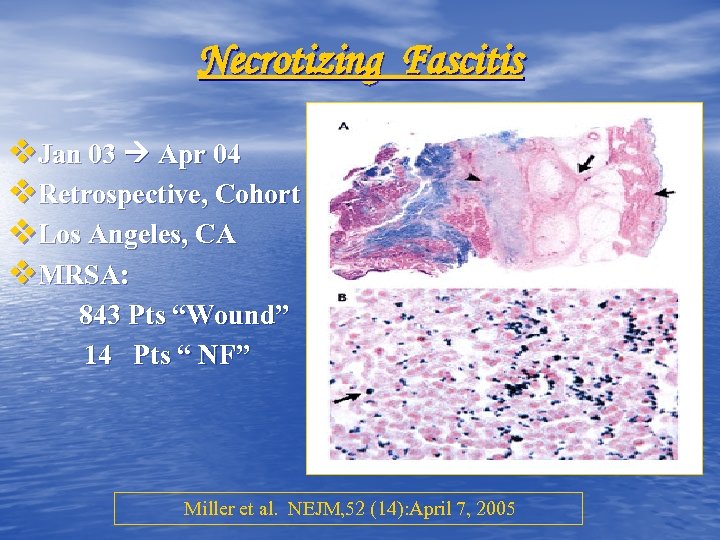 Necrotizing Fascitis v. Jan 03 Apr 04 v. Retrospective, Cohort v. Los Angeles, CA v. MRSA: 843 Pts “Wound” 14 Pts “ NF” Miller et al. NEJM, 52 (14): April 7, 2005
Necrotizing Fascitis v. Jan 03 Apr 04 v. Retrospective, Cohort v. Los Angeles, CA v. MRSA: 843 Pts “Wound” 14 Pts “ NF” Miller et al. NEJM, 52 (14): April 7, 2005
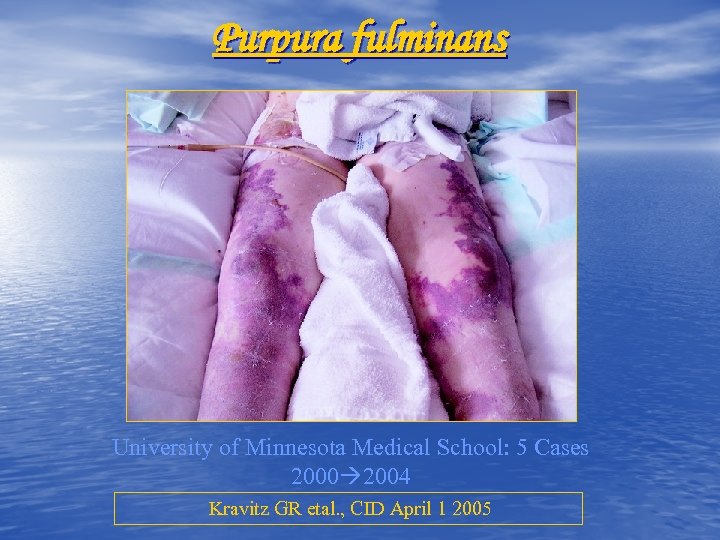 Purpura fulminans University of Minnesota Medical School: 5 Cases 2000 2004 Kravitz GR etal. , CID April 1 2005
Purpura fulminans University of Minnesota Medical School: 5 Cases 2000 2004 Kravitz GR etal. , CID April 1 2005
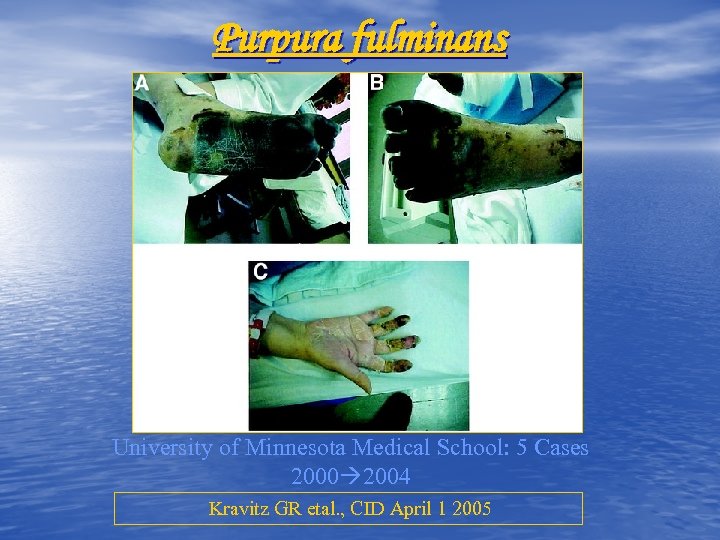 Purpura fulminans University of Minnesota Medical School: 5 Cases 2000 2004 Kravitz GR etal. , CID April 1 2005
Purpura fulminans University of Minnesota Medical School: 5 Cases 2000 2004 Kravitz GR etal. , CID April 1 2005
 Virulence of c-MRSA
Virulence of c-MRSA
 Virulence of c-MRSA Doubling Times 28. 79 +/- 7. 09 min Community 38. 81 +/- 7. 01 min Nosocomial Okuma K etal, J Clin Microbiol 2002
Virulence of c-MRSA Doubling Times 28. 79 +/- 7. 09 min Community 38. 81 +/- 7. 01 min Nosocomial Okuma K etal, J Clin Microbiol 2002

 Virulence of c-MRSA • • • Discovered in 1894 “van de Velde” Distinguished in 1932 “ Panton & Valentine” Genes enters via a bacteriophage Gamma Haemolysins PVL Van de Velde, Cellule 1894 Panton PN, Valentine FCO, Lancet 1932
Virulence of c-MRSA • • • Discovered in 1894 “van de Velde” Distinguished in 1932 “ Panton & Valentine” Genes enters via a bacteriophage Gamma Haemolysins PVL Van de Velde, Cellule 1894 Panton PN, Valentine FCO, Lancet 1932
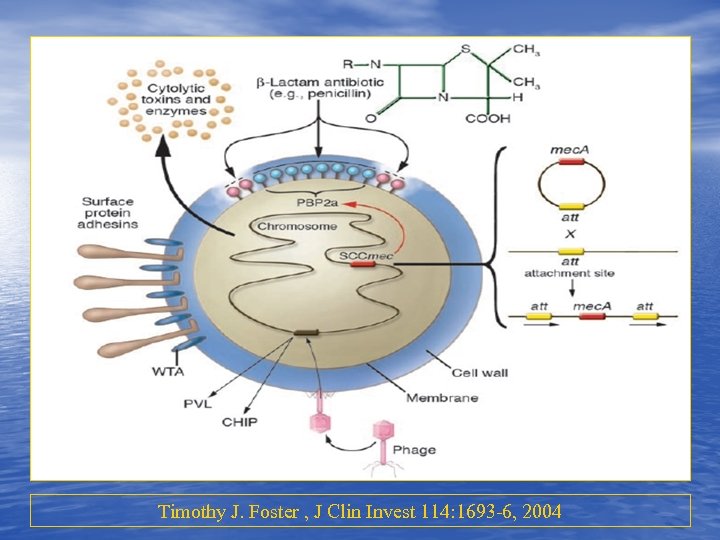 Timothy J. Foster , J Clin Invest 114: 1693 -6, 2004
Timothy J. Foster , J Clin Invest 114: 1693 -6, 2004
 Virulence of c-MRSA PVL Dermonecrotic Toxin Affinity Collagen & Laminin SSTI “Boils/ Impetigo” Necrotizing Pneumonia Mortality
Virulence of c-MRSA PVL Dermonecrotic Toxin Affinity Collagen & Laminin SSTI “Boils/ Impetigo” Necrotizing Pneumonia Mortality
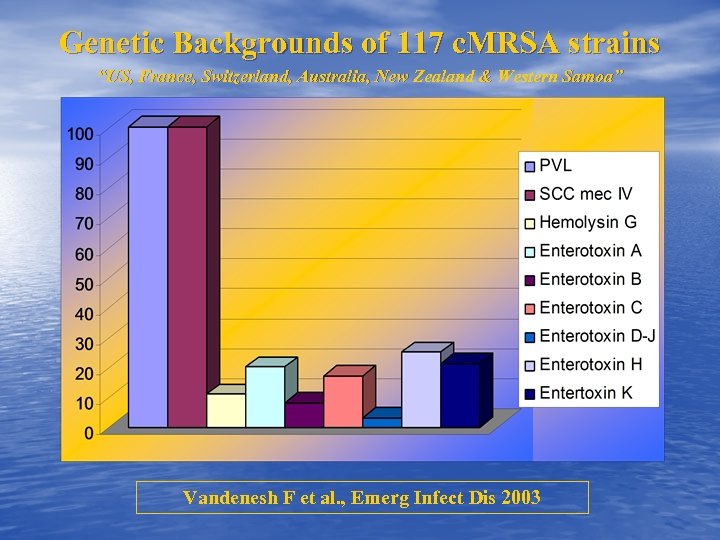 Genetic Backgrounds of 117 c. MRSA strains “US, France, Switzerland, Australia, New Zealand & Western Samoa” Vandenesh F et al. , Emerg Infect Dis 2003
Genetic Backgrounds of 117 c. MRSA strains “US, France, Switzerland, Australia, New Zealand & Western Samoa” Vandenesh F et al. , Emerg Infect Dis 2003
 • Is NOT a Universal Marker of c. MRSA • At least 4 epidemics “Australia”: No PVL Gene New South Wales 100 Islates 68% PVL 4% Toxic Shock-Syndrome Toxin-1 25 % Enterotoxin Genes Barbagiannakos T etal, Int. Symposium Staph. & Strep. Infection, Oct 2004 O’Brien FG atal. , J Clin Microbiol 2004
• Is NOT a Universal Marker of c. MRSA • At least 4 epidemics “Australia”: No PVL Gene New South Wales 100 Islates 68% PVL 4% Toxic Shock-Syndrome Toxin-1 25 % Enterotoxin Genes Barbagiannakos T etal, Int. Symposium Staph. & Strep. Infection, Oct 2004 O’Brien FG atal. , J Clin Microbiol 2004
 • Is it the Major Virulence Determinant in C-MRSA Disease? • Mouse infection models: PVL-positive versus PVLnegative • Strains lacking PVL were as virulent in mouse sepsis and abscess models as those containing the leukotoxin. Voyich JM etal. , JID 194, 2006
• Is it the Major Virulence Determinant in C-MRSA Disease? • Mouse infection models: PVL-positive versus PVLnegative • Strains lacking PVL were as virulent in mouse sepsis and abscess models as those containing the leukotoxin. Voyich JM etal. , JID 194, 2006
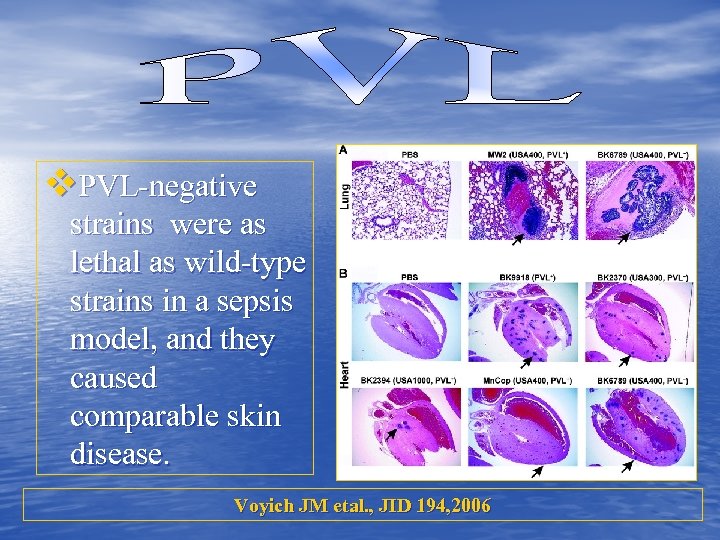 v. PVL-negative strains were as lethal as wild-type strains in a sepsis model, and they caused comparable skin disease. Voyich JM etal. , JID 194, 2006
v. PVL-negative strains were as lethal as wild-type strains in a sepsis model, and they caused comparable skin disease. Voyich JM etal. , JID 194, 2006

 IVDU Playing Contact Sports Previous Antimicrobials Man Who has sex With men Steam Baths Clients Community MRSA Resident of Developmental Disabled Institutions Incarceration In Goal Being a Military Recruit
IVDU Playing Contact Sports Previous Antimicrobials Man Who has sex With men Steam Baths Clients Community MRSA Resident of Developmental Disabled Institutions Incarceration In Goal Being a Military Recruit
 IVDU • First reports in Detroit • Subsequently many report “San Francisco” • Not Universal “ Not shown in Australian studies” ♦ Saravolatz LD etal. , Ann Intern Med 1982 ♦ Charlebois ED etal. , Clin Infect Dis 2002 ♦ Young DM etal. , Arch Surg 2004
IVDU • First reports in Detroit • Subsequently many report “San Francisco” • Not Universal “ Not shown in Australian studies” ♦ Saravolatz LD etal. , Ann Intern Med 1982 ♦ Charlebois ED etal. , Clin Infect Dis 2002 ♦ Young DM etal. , Arch Surg 2004
 Contact Sports ♦ Stacey AR etal. , Br J Sports med 1998 ♦ Lindenmayer JM etal. , Arch Intern Med 1998 ♦ MMWR 2003
Contact Sports ♦ Stacey AR etal. , Br J Sports med 1998 ♦ Lindenmayer JM etal. , Arch Intern Med 1998 ♦ MMWR 2003
 Kazakova et al. February 3, 2005 Epidemic-Curve Graph (Top) & Field Position Diagram (Bottom): MRSA cases among St. Louis Rams Professional Football Players “ 2003” Box on graph & field diagram= MRSA infection Different colors= different players Boxes of same color= recurrent infections. X = Defensive-player position O= Offensive-player position.
Kazakova et al. February 3, 2005 Epidemic-Curve Graph (Top) & Field Position Diagram (Bottom): MRSA cases among St. Louis Rams Professional Football Players “ 2003” Box on graph & field diagram= MRSA infection Different colors= different players Boxes of same color= recurrent infections. X = Defensive-player position O= Offensive-player position.
 Kazakova et al. February 3, 2005 • • • Retrospective cohort study Nasal Swab Survey 84 St. Louis Rams football players & staff members. S. aureus analyzed by PFGE & Gene typing During the 2003 football season: ● 8 MRSA infections: 5/58 Rams players (9 %) ●All infections developed at turf-abrasion sites ●Infection was significantly associated with the lineman or linebacker position & higher BMI. ●MRSA : whirlpools and taping gel ●MRSA : 35/ 84 nasal swabs from players and staff members (42%). ●MRSA : competing football team had PFGE patterns that were indistinguishable from those of the Rams' ●MRSA: All positive PVL & SCC mec type IVa resistance
Kazakova et al. February 3, 2005 • • • Retrospective cohort study Nasal Swab Survey 84 St. Louis Rams football players & staff members. S. aureus analyzed by PFGE & Gene typing During the 2003 football season: ● 8 MRSA infections: 5/58 Rams players (9 %) ●All infections developed at turf-abrasion sites ●Infection was significantly associated with the lineman or linebacker position & higher BMI. ●MRSA : whirlpools and taping gel ●MRSA : 35/ 84 nasal swabs from players and staff members (42%). ●MRSA : competing football team had PFGE patterns that were indistinguishable from those of the Rams' ●MRSA: All positive PVL & SCC mec type IVa resistance
 August 22, 2003 / 52(33); 793 -795 Methicillin-Resistant Staphylococcus aureus Infections Among Competitive Sports Participants Colorado, Indiana, Pennsylvania, and Los Angeles 2000 2003
August 22, 2003 / 52(33); 793 -795 Methicillin-Resistant Staphylococcus aureus Infections Among Competitive Sports Participants Colorado, Indiana, Pennsylvania, and Los Angeles 2000 2003
 Prison Incarceration • • • Several Epidemic reports Boils/Abscesses/Invasive disease Strain: USA 300 Carriage: Inmates & Goalers Factors: ♦ Hygiene ♦ Poor access to health care ♦ Lack of MRSA recognition CDC: MMWR Rep 2003; 52: 992 -6 Georgia, California & Texas
Prison Incarceration • • • Several Epidemic reports Boils/Abscesses/Invasive disease Strain: USA 300 Carriage: Inmates & Goalers Factors: ♦ Hygiene ♦ Poor access to health care ♦ Lack of MRSA recognition CDC: MMWR Rep 2003; 52: 992 -6 Georgia, California & Texas
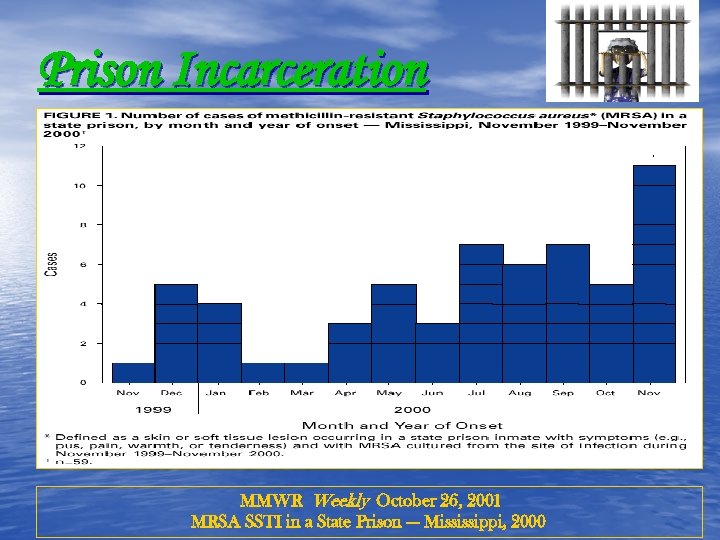 Prison Incarceration MMWR Weekly October 26, 2001 MRSA SSTI in a State Prison --- Mississippi, 2000
Prison Incarceration MMWR Weekly October 26, 2001 MRSA SSTI in a State Prison --- Mississippi, 2000
 Prison Incarceration v. May 30 th, 2005: One week v. Two Maine Correctional Facilities v. SSTI: 11 Inmates v. No evidence of direct connection v. None among correctional officers or other staff
Prison Incarceration v. May 30 th, 2005: One week v. Two Maine Correctional Facilities v. SSTI: 11 Inmates v. No evidence of direct connection v. None among correctional officers or other staff
 Military Service Brooke Army Medical Center Fort Sam Houston, TX 1994 -1997 67 Cases SSTI 24 (36%) C-MRSA Baum SE Mil Med 2003
Military Service Brooke Army Medical Center Fort Sam Houston, TX 1994 -1997 67 Cases SSTI 24 (36%) C-MRSA Baum SE Mil Med 2003
 Military Service Military Medical Facilities, San Diego 1990 2004 1888 MRSA Cases “ 1227” 65 % C-MRSA Incidence 155/100 K person-year “ 2004” Type IV Crum N etal. , Am J Med Oct 2005 (43 rd IDSA Abstract)
Military Service Military Medical Facilities, San Diego 1990 2004 1888 MRSA Cases “ 1227” 65 % C-MRSA Incidence 155/100 K person-year “ 2004” Type IV Crum N etal. , Am J Med Oct 2005 (43 rd IDSA Abstract)
 Homosexuality • Outbreaks reported • Boils • Investigation in process • Sexual behavior & Drug use Garthwaite T: http: //www. lapublichealth. org/std/MRSAproviders. pdf MMWR Reb 2003; 52: 88
Homosexuality • Outbreaks reported • Boils • Investigation in process • Sexual behavior & Drug use Garthwaite T: http: //www. lapublichealth. org/std/MRSAproviders. pdf MMWR Reb 2003; 52: 88
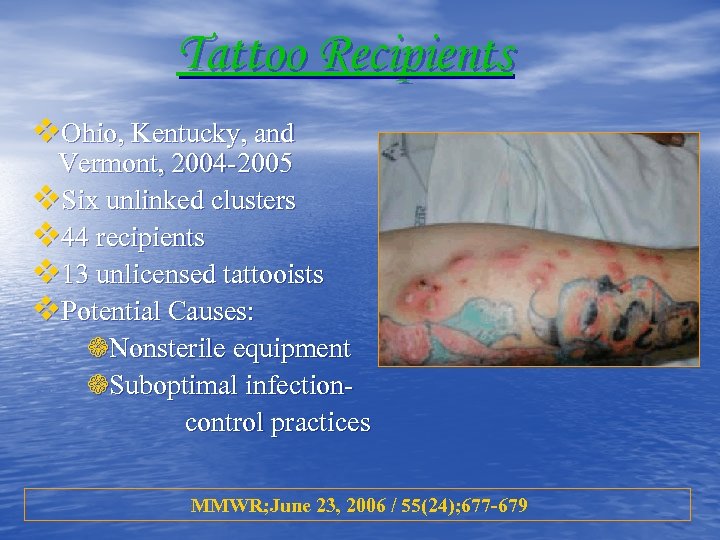 Tattoo Recipients v. Ohio, Kentucky, and Vermont, 2004 -2005 v. Six unlinked clusters v 44 recipients v 13 unlicensed tattooists v. Potential Causes: ❁Nonsterile equipment ❁Suboptimal infectioncontrol practices MMWR; June 23, 2006 / 55(24); 677 -679
Tattoo Recipients v. Ohio, Kentucky, and Vermont, 2004 -2005 v. Six unlinked clusters v 44 recipients v 13 unlicensed tattooists v. Potential Causes: ❁Nonsterile equipment ❁Suboptimal infectioncontrol practices MMWR; June 23, 2006 / 55(24); 677 -679
 Other Reported Risk Factors Alaskan Sauna Use Landen MG, West J Med 2000 Day Care Center Toronto Canada Huang YC, Pediatr Infect Dis J 2004
Other Reported Risk Factors Alaskan Sauna Use Landen MG, West J Med 2000 Day Care Center Toronto Canada Huang YC, Pediatr Infect Dis J 2004
 Strategies for Clinical Management “ 1” Skin Abscess “Spider Bite” Purpura FUlminans Sepsis Syndrome Necrotizing Fascitis Endocarditis Pneumonia Osteomyelitis Septic Arthritis
Strategies for Clinical Management “ 1” Skin Abscess “Spider Bite” Purpura FUlminans Sepsis Syndrome Necrotizing Fascitis Endocarditis Pneumonia Osteomyelitis Septic Arthritis
 Strategies for Clinical Management “ 2” Fluid “Purtulent lesions Abscess Cavity” Bone Respiratory “Sputum DTA BAL Pleural Fluid” Specimen “Cutlure & Susceptibility” Joint Blood
Strategies for Clinical Management “ 2” Fluid “Purtulent lesions Abscess Cavity” Bone Respiratory “Sputum DTA BAL Pleural Fluid” Specimen “Cutlure & Susceptibility” Joint Blood
 Strategies for Clinical Management “ 3” v. Routine Nasal Cultures: Not necessary v. Molecular typing: No information v. Incision and drainage: ✾ Routinely ✾ Fine Needle Aspirate
Strategies for Clinical Management “ 3” v. Routine Nasal Cultures: Not necessary v. Molecular typing: No information v. Incision and drainage: ✾ Routinely ✾ Fine Needle Aspirate
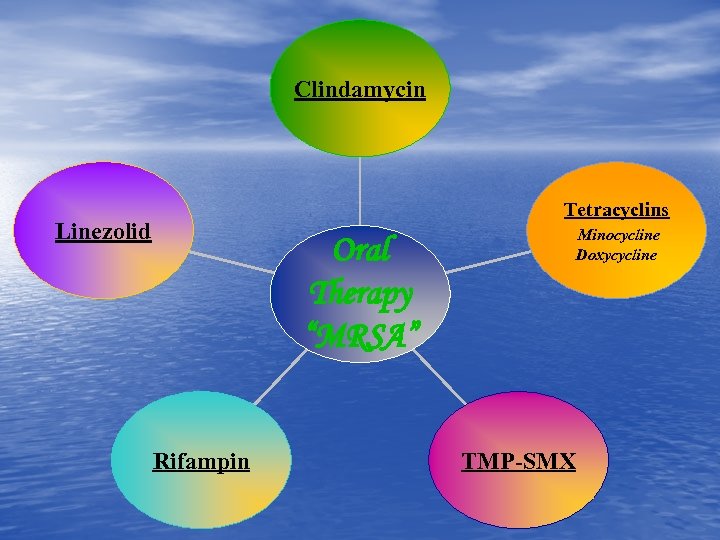 Clindamycin Linezolid Oral Therapy “MRSA” Rifampin Tetracyclins Minocycline Doxycycline TMP-SMX
Clindamycin Linezolid Oral Therapy “MRSA” Rifampin Tetracyclins Minocycline Doxycycline TMP-SMX
 CLINDAMYCIN • • Advantages FDA Approved “S. aureus” Widely Used Reports of Success Prevent Toxin Production • Disadvantages Not FDA approved MRSA • Clostridium difficile • Children ? ! Faden H, etal, Pediatr Infect Dis J, May 2001 Frank AL etal. , Pediatr Infect Dis J, June 2002 Marcinak JF etal. , Curr Opin Infect Dis , June 2003
CLINDAMYCIN • • Advantages FDA Approved “S. aureus” Widely Used Reports of Success Prevent Toxin Production • Disadvantages Not FDA approved MRSA • Clostridium difficile • Children ? ! Faden H, etal, Pediatr Infect Dis J, May 2001 Frank AL etal. , Pediatr Infect Dis J, June 2002 Marcinak JF etal. , Curr Opin Infect Dis , June 2003
 CLINDAMYCIN Inducible MLSB Phenotype Efflux to Macrolides Fully Susceptible D-Zone Test
CLINDAMYCIN Inducible MLSB Phenotype Efflux to Macrolides Fully Susceptible D-Zone Test
 Tetracyclines • • Advantages Doxycyline: FDA Approved “S. aureus” Small Case Series: SSTI ? Minocycline ? Doxycycline Ruhe JJ etal. , CID May 2005 • • • Disadvantages Not FDA approved MRSA Little Information Not for Invasive Pregnancy Children
Tetracyclines • • Advantages Doxycyline: FDA Approved “S. aureus” Small Case Series: SSTI ? Minocycline ? Doxycycline Ruhe JJ etal. , CID May 2005 • • • Disadvantages Not FDA approved MRSA Little Information Not for Invasive Pregnancy Children
 Tmp-Smx Disadvantages Advantages • Several Successful • Case Reports Small Case Series: SSTI • • Ardati KO etal. , J Pediatr 1979 Jemni L etal. , CID 1994 Seligman SJ etal. , J Infect Dis 1973 Stein A etal. , Antimicro Agents Chemo 1998 ♦Markowitz N, Ann Intern Med 1992 Not FDA approved MRSA Not for Invasive♦ 3 rd trimester Pregnancy Infants < 2 Months”
Tmp-Smx Disadvantages Advantages • Several Successful • Case Reports Small Case Series: SSTI • • Ardati KO etal. , J Pediatr 1979 Jemni L etal. , CID 1994 Seligman SJ etal. , J Infect Dis 1973 Stein A etal. , Antimicro Agents Chemo 1998 ♦Markowitz N, Ann Intern Med 1992 Not FDA approved MRSA Not for Invasive♦ 3 rd trimester Pregnancy Infants < 2 Months”
 Rifampin • Should not be used as a single agent • Used in combination • Achieves high concentration in Mucosal surfaces ? • • promote eradication of MRSA coverage ? Benefit Drug-Drug interactions Yu VL etal, NEJM Jul 10, 1986
Rifampin • Should not be used as a single agent • Used in combination • Achieves high concentration in Mucosal surfaces ? • • promote eradication of MRSA coverage ? Benefit Drug-Drug interactions Yu VL etal, NEJM Jul 10, 1986
 Linezolid • • • FDA approved: Complicated SSTI & HAP “adults” Myelosuppression “Dose & Duration dependent” Case reports: . Peripheral neuropathy. Optic Neuropathy. Lactic acidosis Cost Resistance Apodaca AA, NEJM Jan 2003 Bressler AM, Lancet Infect Dis August 2004 Lee E etal. , CLin Infect Dis Nov 2003 Tsiodras S etal. , Lancet July 2001
Linezolid • • • FDA approved: Complicated SSTI & HAP “adults” Myelosuppression “Dose & Duration dependent” Case reports: . Peripheral neuropathy. Optic Neuropathy. Lactic acidosis Cost Resistance Apodaca AA, NEJM Jan 2003 Bressler AM, Lancet Infect Dis August 2004 Lee E etal. , CLin Infect Dis Nov 2003 Tsiodras S etal. , Lancet July 2001
 Not Optimal Fluoroquinolone Macrolides
Not Optimal Fluoroquinolone Macrolides
 Fluoroquinoloes • Ciprofloxacin & Levofloxacin: Complicated SSTI • Moxifloxacin & Gatifloxacin: Uncomplicated SSTI • None: MRSA infections Resistant mutants Replase & Rx Failure • Blumberg HM etal. , J Infect Dis June 1991 • Piercy EA etal. , Antimicrob Agents Chemother , Jan 1989 • Jones ME etal, Antimicrob Agents Chemother, June 2002
Fluoroquinoloes • Ciprofloxacin & Levofloxacin: Complicated SSTI • Moxifloxacin & Gatifloxacin: Uncomplicated SSTI • None: MRSA infections Resistant mutants Replase & Rx Failure • Blumberg HM etal. , J Infect Dis June 1991 • Piercy EA etal. , Antimicrob Agents Chemother , Jan 1989 • Jones ME etal, Antimicrob Agents Chemother, June 2002
 Macrolides/Azalides • Erythromycin/ Clarithromycin & Azithromycin: Uncomplicated SSTI • MRSA: No data • Resistance: Common “ MRSA” Fridkin SK etal, N Engl J Med, April 2005
Macrolides/Azalides • Erythromycin/ Clarithromycin & Azithromycin: Uncomplicated SSTI • MRSA: No data • Resistance: Common “ MRSA” Fridkin SK etal, N Engl J Med, April 2005
 Vancomycin Quinpristin / Tigecyclin Dalfopristin Ceftaroline Parentral Agents Telavancin Teicoplanin Daptomycin Linezolid
Vancomycin Quinpristin / Tigecyclin Dalfopristin Ceftaroline Parentral Agents Telavancin Teicoplanin Daptomycin Linezolid
 Dalbavancin More… Oritavancin Investigational Agents Tedozolid Ceftobiprole
Dalbavancin More… Oritavancin Investigational Agents Tedozolid Ceftobiprole
 I. Keep draining wound covered : dry clean bandages II. Regular hand cleaning: Soap and water or alcohol based hand gel III. Maintain good general hygiene “regular bathing” IV. No items sharing: Towels, clothing, bedding, bar soap, razors, and athletic equipment that touches the skin V. Launder clothing that has come in contact with draining wound after each use and dry thoroughly VI. If not able to cover wound, do not participate in athletic activities until your wound is completely healed VII. Clean equipment and other environmental surfaces with OTC disinfectants/detergents.
I. Keep draining wound covered : dry clean bandages II. Regular hand cleaning: Soap and water or alcohol based hand gel III. Maintain good general hygiene “regular bathing” IV. No items sharing: Towels, clothing, bedding, bar soap, razors, and athletic equipment that touches the skin V. Launder clothing that has come in contact with draining wound after each use and dry thoroughly VI. If not able to cover wound, do not participate in athletic activities until your wound is completely healed VII. Clean equipment and other environmental surfaces with OTC disinfectants/detergents.

 Decolonization Strategies • • • 2005: EIN 471 Respondents 6800 Patients 86%: Nasal Decolonization “ 4200 patients” 57%: Family Decolonization “ 1800 patients” Steven C. Buckingham October , 2006
Decolonization Strategies • • • 2005: EIN 471 Respondents 6800 Patients 86%: Nasal Decolonization “ 4200 patients” 57%: Family Decolonization “ 1800 patients” Steven C. Buckingham October , 2006
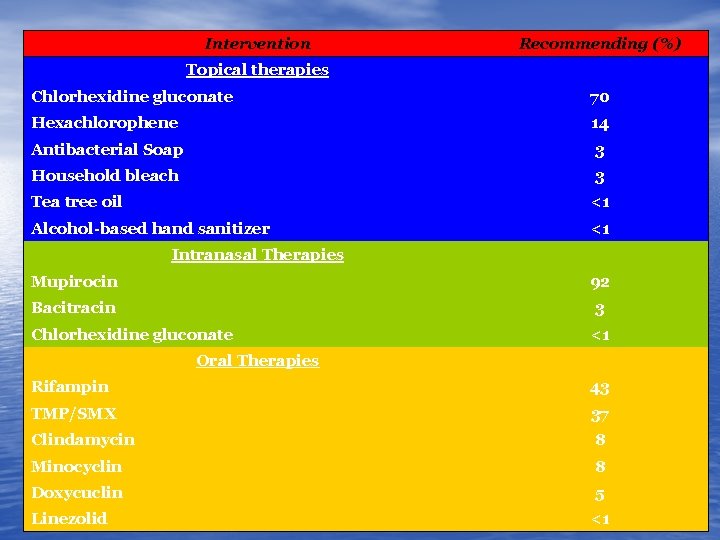 Intervention Topical therapies Recommending (%) Chlorhexidine gluconate 70 Hexachlorophene 14 Antibacterial Soap 3 Household bleach 3 Tea tree oil <1 Alcohol-based hand sanitizer <1 Intranasal Therapies Mupirocin 92 Bacitracin 3 Chlorhexidine gluconate <1 Oral Therapies Rifampin 43 TMP/SMX 37 Clindamycin 8 Minocyclin 8 Doxycuclin 5 Linezolid <1
Intervention Topical therapies Recommending (%) Chlorhexidine gluconate 70 Hexachlorophene 14 Antibacterial Soap 3 Household bleach 3 Tea tree oil <1 Alcohol-based hand sanitizer <1 Intranasal Therapies Mupirocin 92 Bacitracin 3 Chlorhexidine gluconate <1 Oral Therapies Rifampin 43 TMP/SMX 37 Clindamycin 8 Minocyclin 8 Doxycuclin 5 Linezolid <1
 Alcohol-based Hand Sanitizers v 60 -95% Alcohol v. Broad range of pathogens v. Versus Standard hand washing: ●More effective among health care workers v. Versus Plain/Antimicrobial Soap: ●Less Skin irritation & dryness MMWR 2002; 51: 1 -45
Alcohol-based Hand Sanitizers v 60 -95% Alcohol v. Broad range of pathogens v. Versus Standard hand washing: ●More effective among health care workers v. Versus Plain/Antimicrobial Soap: ●Less Skin irritation & dryness MMWR 2002; 51: 1 -45
 Antimicrobial Soap v. Active ingredients: Triclocarban or Triclosan v. No evidence of superiority over plain soap Larson EL etal, Amm Intern Med 2004; 140: 321 -9
Antimicrobial Soap v. Active ingredients: Triclocarban or Triclosan v. No evidence of superiority over plain soap Larson EL etal, Amm Intern Med 2004; 140: 321 -9
 Hexachlorophene v. Bisphenol: 1950’s v. Neurological toxcitiy “ infants” v. FDA: not safe & effective
Hexachlorophene v. Bisphenol: 1950’s v. Neurological toxcitiy “ infants” v. FDA: not safe & effective
 Chlorhexidine Gluconate v. Cationic bisbiguanide v. USA: 1970 s v. Antimicrobial Activity: ● Broad: Gram-positives ● Modest: MRSA “ Comparable to plain soap” v Dermatitis v Cost Hunag Y etal. , Am J Infect Control 1994 Guilhermetti M etal. , Infect Control Hosp Epidemiol 2001
Chlorhexidine Gluconate v. Cationic bisbiguanide v. USA: 1970 s v. Antimicrobial Activity: ● Broad: Gram-positives ● Modest: MRSA “ Comparable to plain soap” v Dermatitis v Cost Hunag Y etal. , Am J Infect Control 1994 Guilhermetti M etal. , Infect Control Hosp Epidemiol 2001
 Povidone/Iodine v. More active against MRSA v. More Skin irritation v. Systemic absorption can occur Block SH, Cutis 1980
Povidone/Iodine v. More active against MRSA v. More Skin irritation v. Systemic absorption can occur Block SH, Cutis 1980
 Household Bleach v. Active Ingredient: Sodium Hypochlorite v 1847: Semmelweis v. Not intended: Personal use v. Safety & Efficacy: Not established v. Skin Irritation & Odor
Household Bleach v. Active Ingredient: Sodium Hypochlorite v 1847: Semmelweis v. Not intended: Personal use v. Safety & Efficacy: Not established v. Skin Irritation & Odor
 Systemic Antimicrobials v. Insufficient Evidence v. Antimicrobial Resistance
Systemic Antimicrobials v. Insufficient Evidence v. Antimicrobial Resistance
 Intranasal Mupirocin v. Can eradicate Nasal Carriage v. Reestablishment: 6 -12 months v. Efficacy: MRSA < MSSA v. Resistance: Emerging Doebbeling BN etal. , CID 1993 Doebbeling BN etal. , Arch Intern Med 1994
Intranasal Mupirocin v. Can eradicate Nasal Carriage v. Reestablishment: 6 -12 months v. Efficacy: MRSA < MSSA v. Resistance: Emerging Doebbeling BN etal. , CID 1993 Doebbeling BN etal. , Arch Intern Med 1994
 Tea Tree Oil v. Volatile essential oil v Melaleuca alternifolia v. Variety products: Soaps, shampoo, creams… v. Nasal eradication: Less effective than mupirocin v. Safety profile: Not established Dryden MS etal. , J Hosp Infect 2004
Tea Tree Oil v. Volatile essential oil v Melaleuca alternifolia v. Variety products: Soaps, shampoo, creams… v. Nasal eradication: Less effective than mupirocin v. Safety profile: Not established Dryden MS etal. , J Hosp Infect 2004
 • Randomized Controlled trial • 87 Rxed Patients vs 25 Placebo; 7 Days Course of: – 2% chlorhexidine gluconate washes – 2% mupirocin ointment intranasally – Oral rifampin – Oral doxycycline • At 3 months F/U: – 74% of Rxed Pts. had Cx Negative vs 32% of those not treated (P=. 0001) Simor AE etal. , CID, Jan 15 th 2007, 178 85
• Randomized Controlled trial • 87 Rxed Patients vs 25 Placebo; 7 Days Course of: – 2% chlorhexidine gluconate washes – 2% mupirocin ointment intranasally – Oral rifampin – Oral doxycycline • At 3 months F/U: – 74% of Rxed Pts. had Cx Negative vs 32% of those not treated (P=. 0001) Simor AE etal. , CID, Jan 15 th 2007, 178 85