d7bf5414eb416d66b52248a3e890e37f.ppt
- Количество слайдов: 32

Commercial Best Practices in Revenue Cycle Management 17 November 2015 @ 0800 – 0900 19 November 2015 @ 1400 – 1500 For entry into the webinar, log into: http: //altarum. adobeconnect. com/ubo. Enter as a guest with your full name and Service or NCR MD affiliation for attendance verification. Instructions for CEU credit are at the end of this presentation. View and listen to the webinar through your computer or Web–enabled mobile device. Note: The DHA UBO Program Office is not responsible for and does not reimburse any airtime, data, roaming or other charges for mobile, wireless and any other internet connections and use. If you need technical assistance with this webinar, contact us at webmeeting@altarum. org. You may submit a question or request technical assistance at any time during a live broadcast by entering it into the “Question” field of Adobe Connect.

Learning Objectives 1. Understand the purpose of the UBO Third Party Collections Program 2. Understand the importance of revenue cycle management in the MHS 3. Understand examples of RCM best practices, including using a revenue dashboard to effectively track metrics and manage revenue operations 4. Understand the requirements of the 2014 National Defense Authorization Act Section 712 and how DHA UBO is utilizing a dashboard to comply with the law 5. Understand the industry changes ahead and the impacts to UBO 2

UBO Third Party Collections Program • The purpose of the Third Party Collections Program (TPCP) is to: – Bill insurers for care provided to eligible Do. D beneficiaries (excludes Active Duty) with other health insurance (excluding Medicare & TRICARE) – Eligible Do. D beneficiaries include: Active Duty Family Members, Former Spouses and Retirees • Money collected from third party payers serves a critical purpose for Military Treatment Facilities (MTFs): – All funds collected are retained by your MTF – Third party collections (TPC) are in addition to each MTF’s Operations & Maintenance (O&M) budget – Adhering to key federal regulations, UBO policies and procedures and your local MTF guidance will minimize funds that are lost to fraud, waste and abuse 3

Federal Regulations to Collect 32 CFR § 220. 2 Statutory Obligation of Third Party Payer to Pay (a) Basic rule. Pursuant to 10 U. S. C. 1095(a)(1), a third party payer has an obligation to pay the United States the reasonable charges for healthcare services provided in or through any facility of the Uniformed Services to a covered beneficiary who is also a beneficiary under the third party payer's plan. The obligation to pay is to the extent that the beneficiary would be eligible to receive reimbursement or indemnification from the third party payer if the beneficiary were to incur the costs on the beneficiary's own behalf. (b) Application of cost shares. If the third party payer's plan includes a requirement for a deductible or copayment by the beneficiary of the plan, then the amount the United States may collect from the third party payer is the reasonable charge for the care provided less the appropriate deductible or copayment amount. (c) Claim from United States exclusive. The only way for a third party payer to satisfy its obligation under 10 U. S. C. 1095 is to pay the facility of the uniformed service or other authorized representative of the United States. Payment by a third party payer to the beneficiary does not satisfy 10 U. S. C. 1095. 4
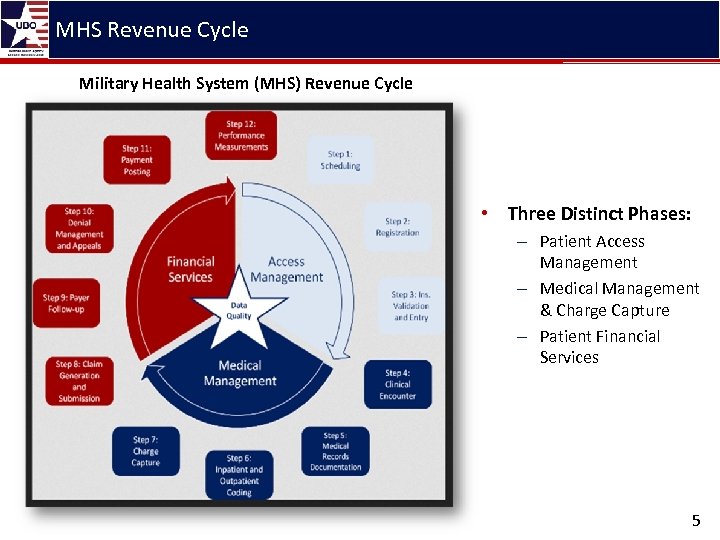
MHS Revenue Cycle Military Health System (MHS) Revenue Cycle • Three Distinct Phases: – Patient Access Management – Medical Management & Charge Capture – Patient Financial Services 5

Overview of Revenue Cycle Management What is Revenue Cycle Management? • The role of revenue cycle management (RCM) is to improve the efficiency and quality of revenue cycle operations in order to maximize the recovery of reasonable charges for health services provided to non-uniformed service beneficiaries. No Margin, No Mission • Hospital operating profit margins in the commercial sector have remained relatively steady at 3% in recent years, which indicates they are controlling expenses to meet fluctuations in revenues – the bottom line is that providers in both the civilian and military sectors are being asked to do more with less. • All revenue collected by the TPCP is returned directly to the O&M budget of the MTF where the care was delivered and is used to improve the quality of health care. Often the funds allow the continuation of programs or purchasing of equipment at the MTFs for which there would otherwise not be funding. • RCM is at the forefront of DHA UBO’s mission to optimize allowable health care cost recovery within compliance guidelines to support MHS’s operational and readiness missions. 6
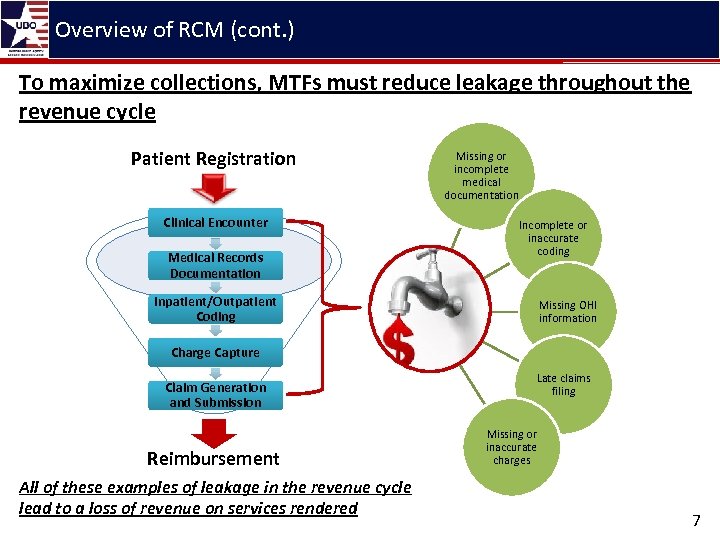
Overview of RCM (cont. ) To maximize collections, MTFs must reduce leakage throughout the revenue cycle Patient Registration Clinical Encounter Medical Records Documentation Inpatient/Outpatient Coding Missing or incomplete medical documentation Incomplete or inaccurate coding Missing OHI information Charge Capture Claim Generation and Submission Reimbursement All of these examples of leakage in the revenue cycle lead to a loss of revenue on services rendered Late claims filing Missing or inaccurate charges 7
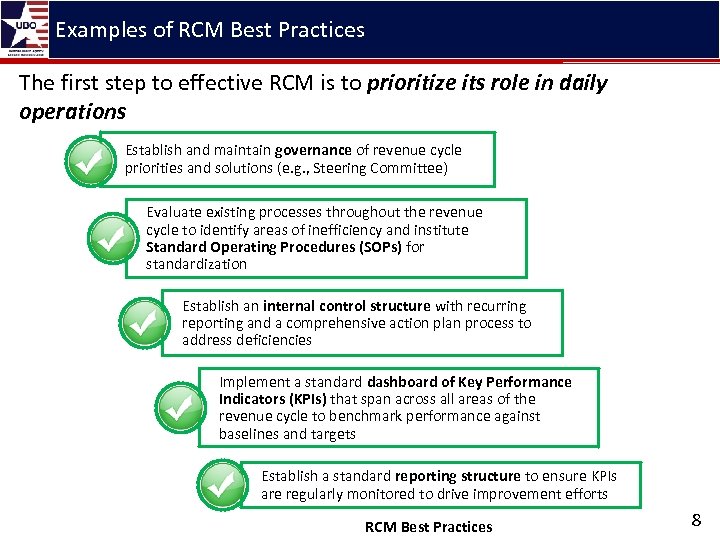
Examples of RCM Best Practices The first step to effective RCM is to prioritize its role in daily operations Establish and maintain governance of revenue cycle priorities and solutions (e. g. , Steering Committee) Evaluate existing processes throughout the revenue cycle to identify areas of inefficiency and institute Standard Operating Procedures (SOPs) for standardization Establish an internal control structure with recurring reporting and a comprehensive action plan process to address deficiencies Implement a standard dashboard of Key Performance Indicators (KPIs) that span across all areas of the revenue cycle to benchmark performance against baselines and targets Establish a standard reporting structure to ensure KPIs are regularly monitored to drive improvement efforts RCM Best Practices 8

RCM Best Practice: Performance Dashboard • A dashboard is a performance management tool that uses organized data, actionable metrics and clear targets to measure performance against desired goals – The data depicted should be timely (daily, weekly and monthly) • Dashboards are used at the top level to measure performance against organizational strategy and at lower levels to measure performance against departmental goals and objectives • Powerful dashboards drill into dynamic reports that depict KPIs in a graphical format to analyze trends and determine root causes Proactive performance management is simple! Track KPIs daily, weekly and monthly against targets Display KPIs graphically to determine trends Drill-down into data to identify root causes Adjust targets, refine processes, institute corrective action plans Primary Purposes of a Dashboard 9

2014 National Defense Authorization Act Section 712 • Section 712 of the 2014 National Defense Authorization Act (NDAA) requires DHA to execute a three-year pilot program to test and evaluate commercial revenue best practices to increase third party collections – The pilot program must compare third party collections performance of MTFs that use specific revenue best practices (pilot sites) against MTFs that do not use the best practices (peer sites) • The pilot program commenced in August 2014 • At the conclusion of the pilot program (March 2018), DHA must submit a final report to Congress including an analysis of data and pilot results, a financial cost/benefit analysis and recommendations for potential national deployment 10

Pilot Program Objectives Objective 1: • Evaluate the differences in TPC performance of MTFs that: 1) Contract all TPCP operations and staff to an external vendor (pilot sites) 2) Employ MTF workforce for TPCP operations (peer sites) Objective 2: • Evaluate the differences in TPC performance of MTFs that: 1) At the start of the pilot, used the ARMSPro© billing solution prior to migrating to the Armed Forces Billing and Collections Solution (ABACUS) (pilot sites) 2) At the start of the pilot, used TPOCS and CHCS prior to migrating to ABACUS (peer sites) Objective 3: • • Implement a revenue dashboard tool to track financial and operational performance of pilot and peer MTFs on a monthly basis – The dashboard tool is comprised of new industry-standard KPIs not previously reported to DHA UBO – Establish KPI baselines and targets Integrate the dashboard into daily operations at pilot MTFs to ensure KPIs are regularly monitored and utilized to drive improvement efforts 11

Pilot Program Criteria used to select pilot sites: • MTF provides inpatient and outpatient services • Mix of 1 small, medium and large hospital • Mix of 1 MTF from each Service and the NCR MD Criteria used to select peer sites: • Same peer group in MHS Data Repository (small, medium, large hospital) as the pilot site • Same geographic region (West, Mid-South, Mid-Atlantic, Pacific regions) as the pilot site 12
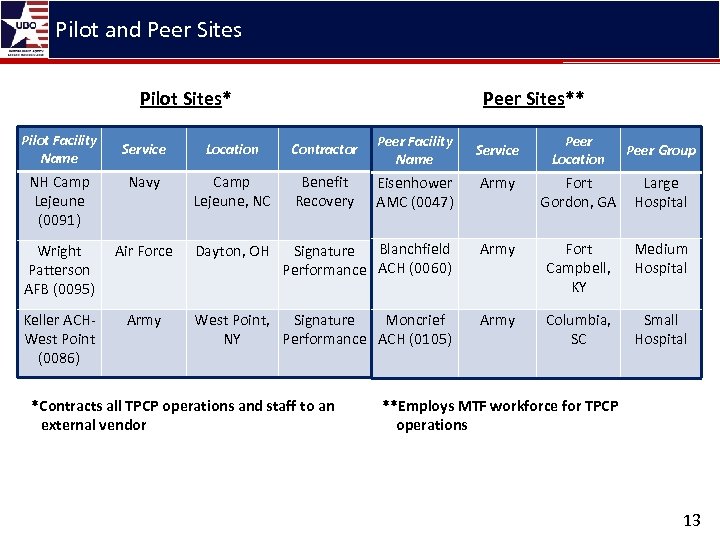
Pilot and Peer Sites Pilot Sites* Pilot Facility Name Peer Sites** Service Location Contractor Peer Facility Name Peer Location Peer Group NH Camp Lejeune (0091) Navy Camp Lejeune, NC Benefit Recovery Eisenhower AMC (0047) Army Fort Gordon, GA Large Hospital Wright Patterson AFB (0095) Air Force Dayton, OH Signature Blanchfield Performance ACH (0060) Army Fort Campbell, KY Medium Hospital Keller ACHWest Point (0086) Army West Point, Signature Moncrief NY Performance ACH (0105) Army Columbia, SC Small Hospital *Contracts all TPCP operations and staff to an external vendor Service **Employs MTF workforce for TPCP operations 13
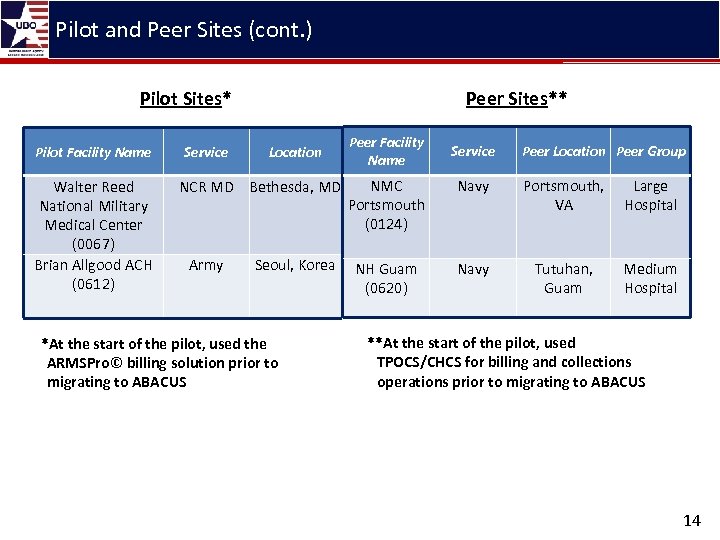
Pilot and Peer Sites (cont. ) Pilot Sites* Pilot Facility Name Walter Reed National Military Medical Center (0067) Brian Allgood ACH (0612) Service Peer Sites** Location NCR MD Bethesda, MD Army Seoul, Korea *At the start of the pilot, used the ARMSPro© billing solution prior to migrating to ABACUS Peer Facility Name Service Peer Location Peer Group NMC Portsmouth (0124) Navy Portsmouth, VA Large Hospital NH Guam (0620) Navy Tutuhan, Guam Medium Hospital **At the start of the pilot, used TPOCS/CHCS for billing and collections operations prior to migrating to ABACUS 14

Pilot Dashboard Overarching Features and Benefits • Introduces more granular KPIs measured at a monthly frequency: Provides a month-to-month look at performance trends across three important domains: – Total Billings and Collections: Tracks total monthly billings and collections used to gauge facility performance against established goals – Accounts Receivables (A/R) Management: Measures the timeliness of resolving outstanding A/R before hitting the 90+ day aging point – Claims Adjudication: Trends $ amounts of lost reimbursement for valid reasons; indicates MTF compliance with payer requirements and the payer’s ability to accurately reimburse • Provides monthly baseline data for the start of the pilot: Establishes baseline data for each metric which can be used to determine monthly, quarterly, and yearly goals at the MTF level • Creates a graphical representation of performance trends: Provides a visual depiction of revenue performance at contracted and non-contracted sites • Introduces a commercial best practice tool for RCM: Enables MTFs to view their data in different ways to better inform decision-making 15
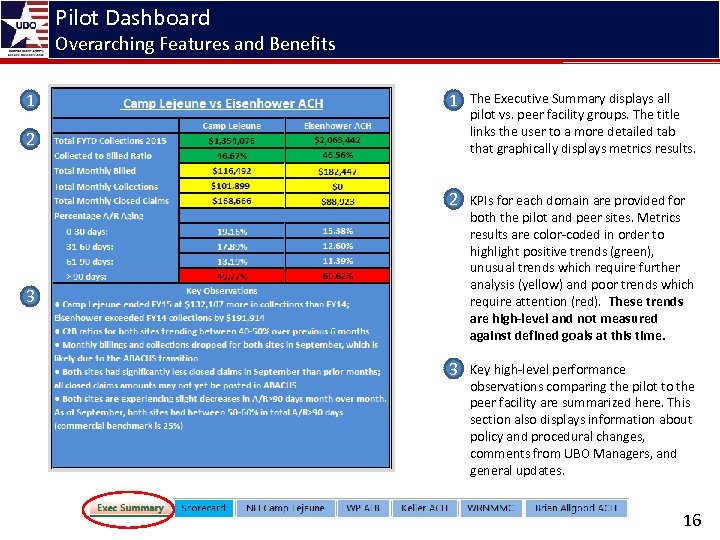

Pilot Dashboard Overarching Features and Benefits 1 1 The Executive Summary displays all pilot vs. peer facility groups. The title links the user to a more detailed tab that graphically displays metrics results. 2 KPIs for each domain are provided for both the pilot and peer sites. Metrics results are color-coded in order to highlight positive trends (green), unusual trends which require further analysis (yellow) and poor trends which require attention (red). These trends are high-level and not measured against defined goals at this time. 3 Key high-level performance observations comparing the pilot to the peer facility are summarized here. This section also displays information about policy and procedural changes, comments from UBO Managers, and general updates. 2 3 16
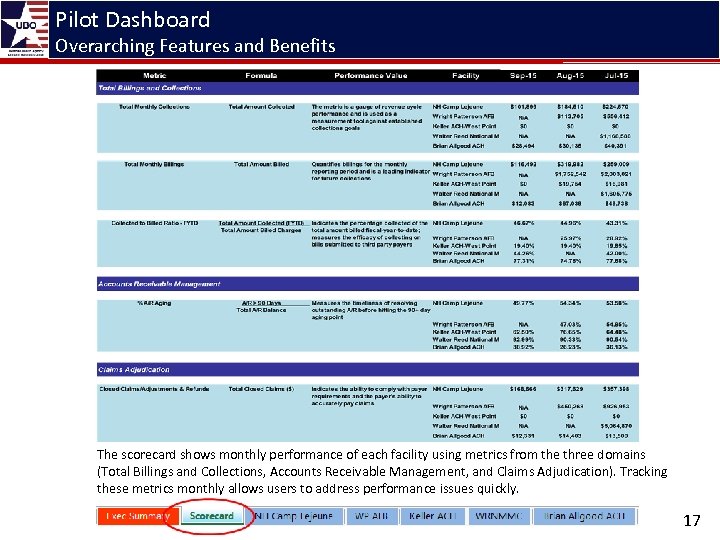
Pilot Dashboard Overarching Features and Benefits The scorecard shows monthly performance of each facility using metrics from the three domains (Total Billings and Collections, Accounts Receivable Management, and Claims Adjudication). Tracking these metrics monthly allows users to address performance issues quickly. 17

Pilot Dashboard Overarching Features and Benefits • Each pilot and peer facility group has a designated tab that displays monthly metrics graphically to determine trends. • The site tab contains the following information for each pilot and peer MTF: – – – Total Monthly Collections Total Fiscal Year to Date (FYTD) Collections Total Monthly Closed Claims Top Closed claims Reason Codes by Dollar Amount Percent of Accounts Receivable Aging • As previously discussed, the user is taken to the site tab by clicking on the title links on the executive summary tab. • The following slides provide an example of the data displayed on the site tab for “NH Camp Lejeune and Eisenhower ACH. ” 18
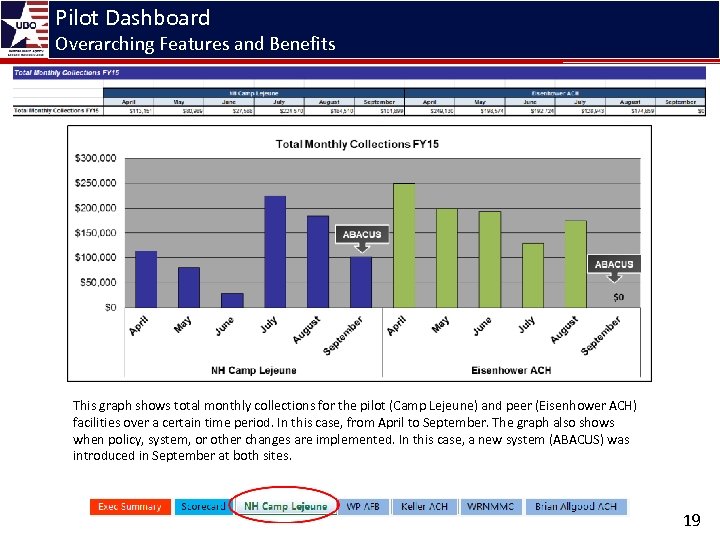
Pilot Dashboard Overarching Features and Benefits This graph shows total monthly collections for the pilot (Camp Lejeune) and peer (Eisenhower ACH) facilities over a certain time period. In this case, from April to September. The graph also shows when policy, system, or other changes are implemented. In this case, a new system (ABACUS) was introduced in September at both sites. 19
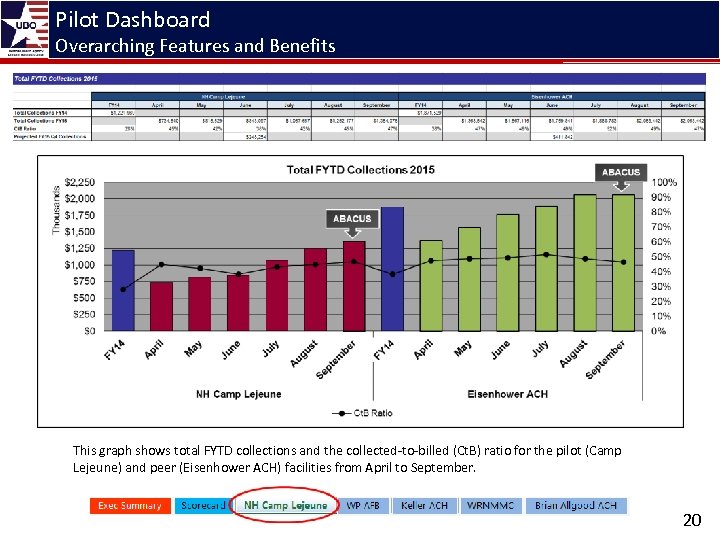
Pilot Dashboard Overarching Features and Benefits This graph shows total FYTD collections and the collected-to-billed (Ct. B) ratio for the pilot (Camp Lejeune) and peer (Eisenhower ACH) facilities from April to September. 20
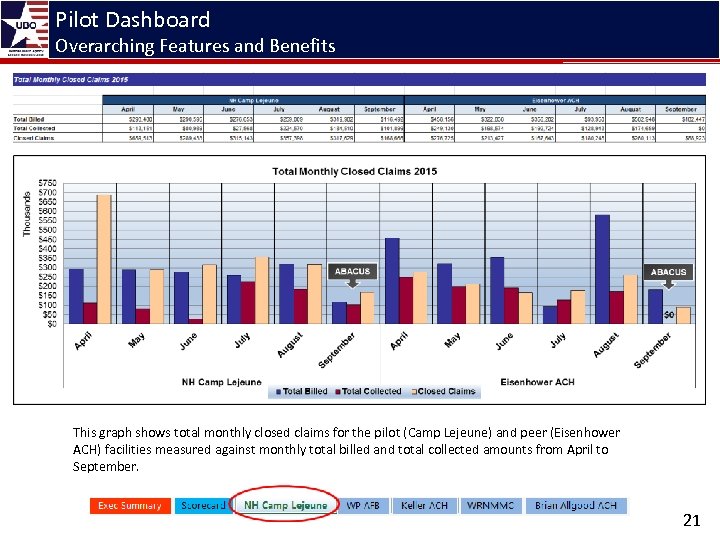
Pilot Dashboard Overarching Features and Benefits This graph shows total monthly closed claims for the pilot (Camp Lejeune) and peer (Eisenhower ACH) facilities measured against monthly total billed and total collected amounts from April to September. 21
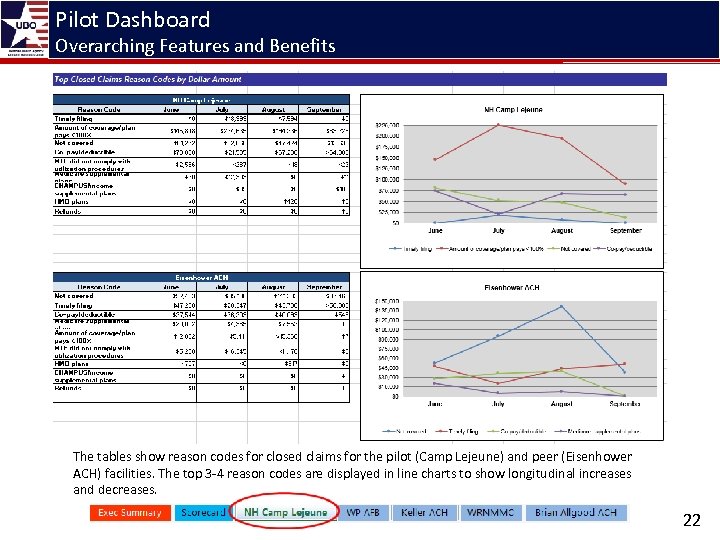
Pilot Dashboard Overarching Features and Benefits The tables show reason codes for closed claims for the pilot (Camp Lejeune) and peer (Eisenhower ACH) facilities. The top 3 -4 reason codes are displayed in line charts to show longitudinal increases and decreases. 22
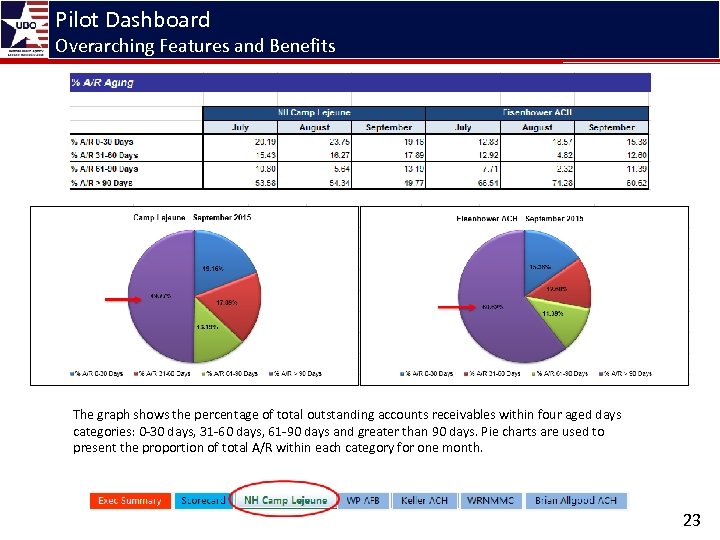
Pilot Dashboard Overarching Features and Benefits The graph shows the percentage of total outstanding accounts receivables within four aged days categories: 0 -30 days, 31 -60 days, 61 -90 days and greater than 90 days. Pie charts are used to present the proportion of total A/R within each category for one month. 23

Pilot Progress to Date • DHA UBO designed and developed a revenue dashboard tool to track monthly operational performance of pilot and peer sites which supplements quarterly TPCP metrics reporting. – The dashboard incorporates new industry-standard KPIs not previously reported to DHA UBO • DHA UBO collected DD 2570 and DD 2571 (A/R Aging) reports monthly from each facility to populate KPIs in the dashboard tool (data collection began in March 2015). • DHA UBO conducted month-over-month high-level trend analyses of metrics performance to understand differences in performance between pilot and peer sites. 24
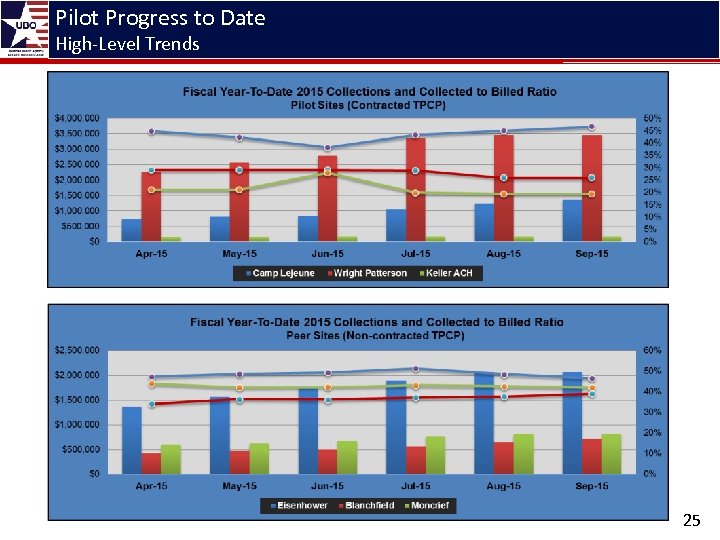
Pilot Progress to Date High-Level Trends 25
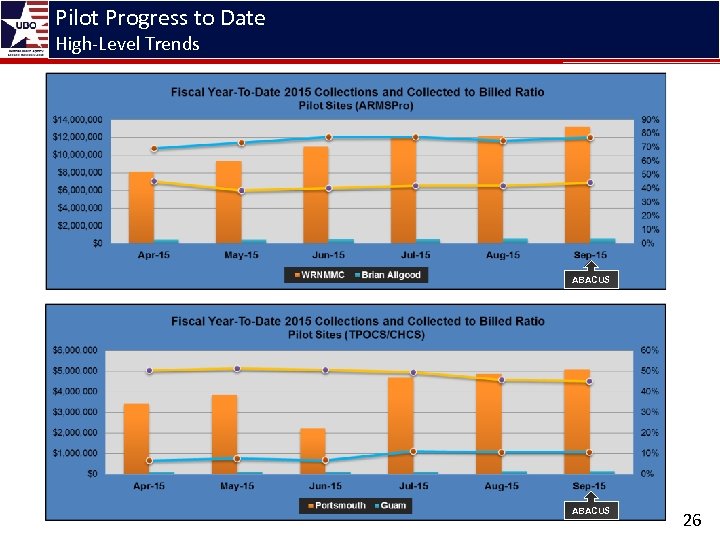
Pilot Progress to Date High-Level Trends ABACUS 26

Pilot Next Steps Incorporating New Best Practice RCM Metrics • High-level trends for FYTD collections and Ct. B ratios for pilot and peer sites are identified, but further analysis is required to understand the WHYs: – Why are there variances in total collections amounts between pilot sites and pilot and peer sites? – Why are there variances in Ct. B ratios between pilot sites and pilot and peer sites? Let’s Dive a Little Deeper… What do we need to know (site by site) to evaluate these trends? • What is the service mix for Non-Active Duty patients? • What proportion of Non-Active Duty patients have Other Health Insurance? • What percentage of gross A/R dollars are unbilled? What percentage was billed, but not sent to the payer? • What percentage of billed claims is paid correctly? What percentage received zero pay? Partial pay? By which payers? For what reasons? • What follow-up activity occurs for denied claims? What is the frequency of follow-up? • What is the net days in A/R (average # days revenue outstanding)? 27
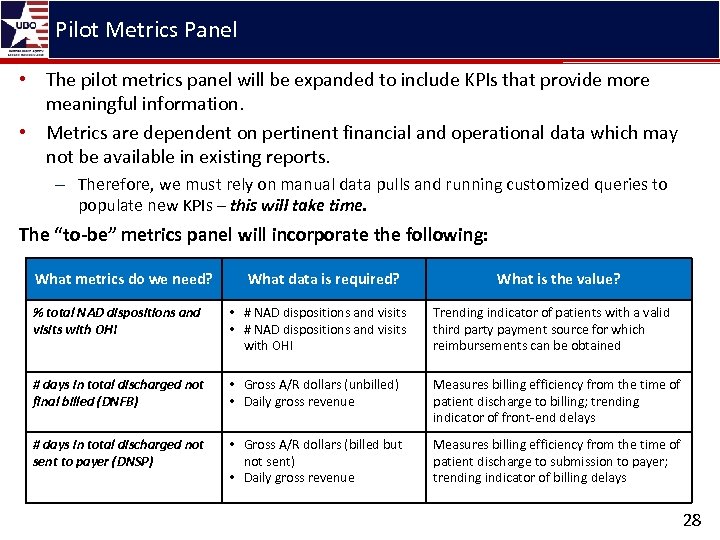
Pilot Metrics Panel • The pilot metrics panel will be expanded to include KPIs that provide more meaningful information. • Metrics are dependent on pertinent financial and operational data which may not be available in existing reports. – Therefore, we must rely on manual data pulls and running customized queries to populate new KPIs – this will take time. The “to-be” metrics panel will incorporate the following: What metrics do we need? What data is required? What is the value? % total NAD dispositions and visits with OHI • # NAD dispositions and visits with OHI Trending indicator of patients with a valid third party payment source for which reimbursements can be obtained # days in total discharged not final billed (DNFB) • Gross A/R dollars (unbilled) • Daily gross revenue Measures billing efficiency from the time of patient discharge to billing; trending indicator of front-end delays # days in total discharged not sent to payer (DNSP) • Gross A/R dollars (billed but not sent) • Daily gross revenue Measures billing efficiency from the time of patient discharge to submission to payer; trending indicator of billing delays 28
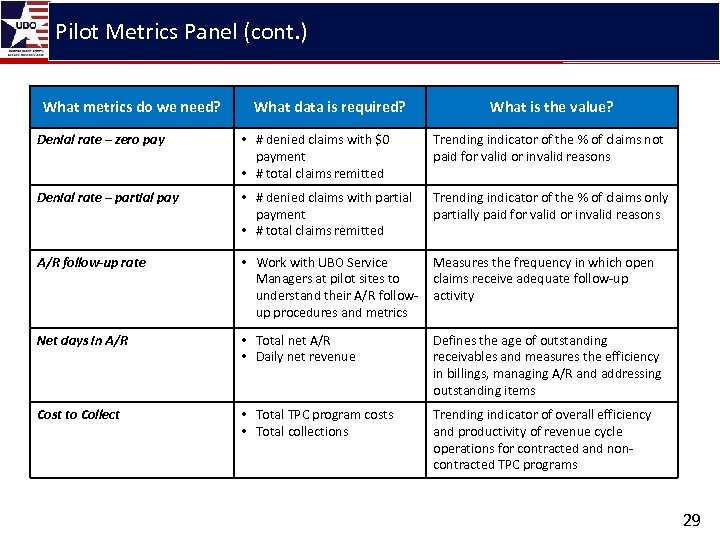
Pilot Metrics Panel (cont. ) What metrics do we need? What data is required? What is the value? Denial rate – zero pay • # denied claims with $0 payment • # total claims remitted Trending indicator of the % of claims not paid for valid or invalid reasons Denial rate – partial pay • # denied claims with partial payment • # total claims remitted Trending indicator of the % of claims only partially paid for valid or invalid reasons A/R follow-up rate • Work with UBO Service Managers at pilot sites to understand their A/R followup procedures and metrics Measures the frequency in which open claims receive adequate follow-up activity Net days in A/R • Total net A/R • Daily net revenue Defines the age of outstanding receivables and measures the efficiency in billings, managing A/R and addressing outstanding items Cost to Collect • Total TPC program costs • Total collections Trending indicator of overall efficiency and productivity of revenue cycle operations for contracted and noncontracted TPC programs 29

Industry Changes Ahead • • Evidence-Based Medicine (EBM): EBM aims to address the clinical practice variations with the help of things like standardized guidelines to achieve consistency, quality, and safety (e. g. payer reimbursements based on adherence to evidence-based standards, such as acceptable # cases of pneumonia). Bundled Payments: Bundled payments are a single payment to providers for all services to treat a given condition or provide a given treatment. – MHS currently uses a form of bundled charges for inpatient services (MS-DRG based), but outpatient services are still billed on a fee-for-service basis. – As the industry moves towards bundled payments, MHS has an opportunity to explore the potential to improve or develop their own outpatient bundled payment initiatives. • Accountable Care Organizations (ACOs): ACOs comprise a group of health care providers who give coordinated care and chronic disease management. ACO’s payment is tied to achieving specific health care quality and outcomes. – ACOs may begin instituting new reporting requirements or lower reimbursement rates for providers outside of their network. As a result, the MHS could potentially see lower third-party payer reimbursements. • High Deductible Health Plans (HDHP): MTFs may be billing OHI carriers more frequently, but receiving lower reimbursements because patients who have not met their high deductibles must pay out-of-pocket. More regulation and less reimbursement – improving the quality of patient care and the accuracy and efficiency of billing and collections operations is critical now more than ever! 30
Thank You Questions? 31

Instructions for CEU Credit This in-service webinar has been approved by the American Academy of Professional Coders (AAPC) for 1. 0 Continuing Education Unit (CEU) credit for Do. D personnel (. mil address required). Granting of this approval in no way constitutes endorsement by the AAPC of the program, content or the program sponsor. There is no charge for this credit. • Live broadcast webinar (post-test not required) – Login prior to the broadcast with your: 1) full name; 2) Service affiliation; and 3) e-mail address – View the entire broadcast – After completion of both of the live broadcasts and after attendance records have been verified, a Certificate of Approval including an AAPC Index Number will be sent via e-mail to participants who logged in or e-mailed as required. This may take several business days. • Archived webinar (post-test required) – View the entire archived webinar (free and available on demand at: http: //health. mil/Military-Health. Topics/Business-Support/Uniform-Business-Office/UBO-Learning-Center/Archived-Webinars ) – Complete a post-test available within the archived webinar – E-mail answers to UBO. Learning. Center@altarum. org – If you receive a passing score of at least 70%, we will e-mail MHS personnel with a. mil email address a Certificate of Approval including an AAPC Index Number • The original Certificate of Approval may not be altered except to add the participant ’s name and webinar date or the date the archived Webinar was viewed. Certificates should be maintained on file for at least six months beyond your renewal date in the event you are selected for CEU verification by AAPC • For additional information or questions regarding AAPC CEUs, please contact the AAPC. • Other organizations, such as American Health Information Management Association (AHIMA), American College of Healthcare Executives (ACHE), and American Association of Healthcare Administrative Managers (AAHAM), may also grant credit for DHA UBO Webinars. Check with the organization directly for qualification and reporting guidance. 32
d7bf5414eb416d66b52248a3e890e37f.ppt