94aded9fc5f58d797723162b5129155b.ppt
- Количество слайдов: 70


Clozapine Underutilization: Addressing the Barriers Deanna L. Kelly, Pharm. D. , BCPP Professor of Psychiatry Director, Treatment Research Program Maryland Psychiatric Research Center (MPRC) University of Maryland School of Medicine Raymond C. Love, Pharm. D. , FASHP Professor of Pharmacy Practice and Science Director, Mental Health Pharmacy Program University of Maryland School of Pharmacy

Overview: Summary of Project Purpose • Clozapine is a medication that exhibits unique efficacy and effectiveness for those with serious mental illness, despite side effects that present challenges to its use • These challenges have evolved into a set of barriers that discourage the use of clozapine • Proven approaches using interprofessional models of care can help meet the needs of patients receiving clozapine • State and local government, federal agencies, academic medical centers, prescribers and others all have vital roles to play in increasing access to clozapine • NASHMPD has commissioned a White Paper to help rectify the clozapine situation nationally

NASMHPD Workgroup • • • Raymond C. Love, Pharm. D, BCPP, FASHP Deanna Kelly, Pharm. D, BCPP Oliver Freudenreich, MD, FAPM Mac. Kenzie A. Sayer, BS Kathy Sanders, MD Andrew J. Mc. Lean MD, MPH Dale K. Adair, MD Brian Hepburn, MD Aaron J. Walker, MPA Stuart Yael Gordon, JD

CLOZAPINE EFFICACY, EFFECTIVENESS AND RISK TO BENEFIT PROFILE
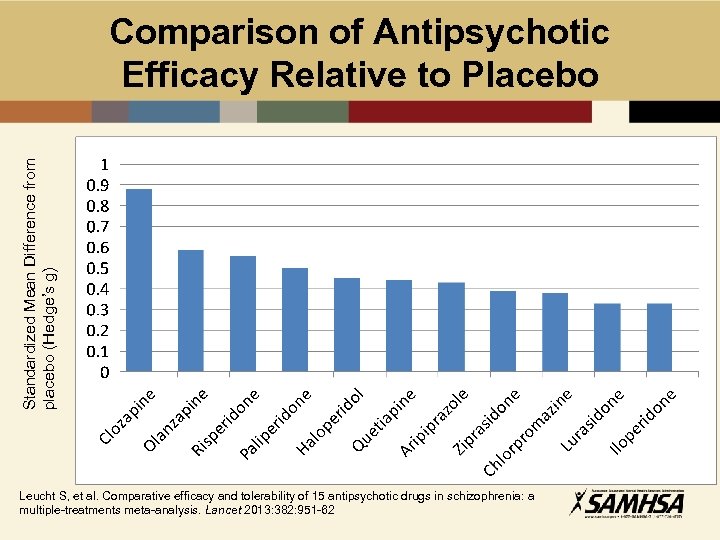
Standardized Mean Difference from placebo (Hedge’s g) Comparison of Antipsychotic Efficacy Relative to Placebo Leucht S, et al. Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis. Lancet 2013: 382: 951 -62

Clozapine Superiority Effectiveness Studies • Several large effectiveness studies suggest that clozapine: • averages significantly greater time to treatment discontinuation • is associated with significantly greater patient perceived ratings • is associated with significantly greater clinician ratings Lieberman JA, et al. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med. 2005; 353: 1209– 23; Lewis SW, et al. Randomized controlled trial of effect of prescription of clozapine versus other second-generation antipsychotic drugs in resistant schizophrenia. Schizophr Bull. 2006; 32(4): 715– 23.

Importance of Clozapine • The Schizophrenia Patient Outcomes Research Team (PORT) recommends that patients with persistent positive symptoms of schizophrenia receive an adequate trial of clozapine • More recent guidelines recommend clozapine after two failed antipsychotic trials • Harvard South Shore Program Algorithm • British Association for Psychopharmacology Guidelines • The National Institute for Health and Care Excellence (NICE) Clinical Guideline for Schizophrenia” • Early use is critical for young patients with schizophrenia who are treatment-refractory and in whom only clozapine offers a chance for improvement and course stabilization as the basis for recovery Buchanan, R. W. , et al. , Schizophr Bull, 2010; Osser, D. N. , M. J. Roudsari, and T. Manschreck, Harv Rev Psychiatry; Barnes, T. R. , J Psychopharmacol, 2011. National Institute for Health and Care Excellence, 2014; Agid, O. , et al. , J Clin Psychiatry, 2011.

Broad Range of Effectiveness • Clozapine may have utility for a variety of other disorders and conditions • treatment of hostility and aggression • treatment-resistant bipolar disorder • psychogenic polydipsia/hyponatremia • Parkinson Disease Psychosis and psychosis in Lewy-Body dementia • Borderline Personality Disorder • tardive dyskinesia (TD) • Growing evidence also suggests clozapine may be an option in youth with early onset schizophrenia • Clozapine is the only antipsychotic with a Food and Drug Administration approval for suicidality and it has the lowest mortality rate among all antipsychotic treatments

Risk to Benefit Profile • Clozapine use is associated with a variety of side effects, some of which are potentially serious • Common side effects include: hypersalivation, tachycardia, enuresis, sweating, eosinophilia, metabolic syndrome and constipation • Serious but rare side effects include: myocarditis (3% risk), cardiomyopathy (0. 02 -0. 1% risk), seizures (1 -3% risk), and severe neutropenia (0. 05 -0. 86%) • Severe neutropenia risk has led the FDA to mandate regular blood draws to monitor the absolute neutrophil count (ANC) Sagy, R. , A. Weizman, and N. Katz, Int Clin Psychopharmacol, 2014. Mitchell, A. J. , et al. Schizophr Bull, 2013. Raja, M. , . Curr Drug Saf, 2011. Ronaldson, K. J. , P. B. Fitzgerald, and J. J. Mc. Neil, Acta Psychiatr Scand, 2015. . Layland, J. J. , D. Liew, and D. L. Prior, . Med J Aust, 2009; Williams, A. M. and S. H. Park, CNS Drugs, 2015. . Honigfeld, G. , et al. , . J Clin Psychiatry, 1998. Munro, J. , et al. , Br J Psychiatry, 1999. Lahdelma, L. and B. Appelberg, J Clin Psychiatry, 2012. . Drew, L. , Psychiatry, 2013. Balda, M. V. , et al. , Int Clin Psychopharmacol, 2015

Risk to Benefit Profile (cont. ) • The decision to use clozapine requires a thorough consideration of both its risks and benefits, a thoughtful patient centered approach and a system that facilitates safe and appropriate use • Often ignored in risk-benefit discussions are the medical risks of not using clozapine • Other antipsychotics and polypharmacy have medical risks • Poorly treated psychiatric illness can complicate medical treatment Hill, M. and O. Freudenreich, Clozapine: key discussion points for prescribers. Clin Schizophr Relat Psychoses, 2013. 6(4): p. 177 -85; Misawa, F. , et al. , Is antipsychotic polypharmacy associated with metabolic syndrome even after adjustment for lifestyle effects? : a cross-sectional study. BMC Psychiatry, 2011. 11: p. 118.

Clozapine Cost-Effectiveness • N=479 clozapine starts compared to N=2240 polypharmacy starts • Continuously enrolled Medicaid patients, 6 months prior and 12 months post • Significantly fewer emergency department visits • Significantly lower overall costs • $21, 315 all cause lower • $17, 457 mental illness related • $10, 582 lower for schizophrenia Velligan, et al. Psychiatric Services 2015; 66(2): 127 -33

CLOZAPINE UNDERUTILIZATION
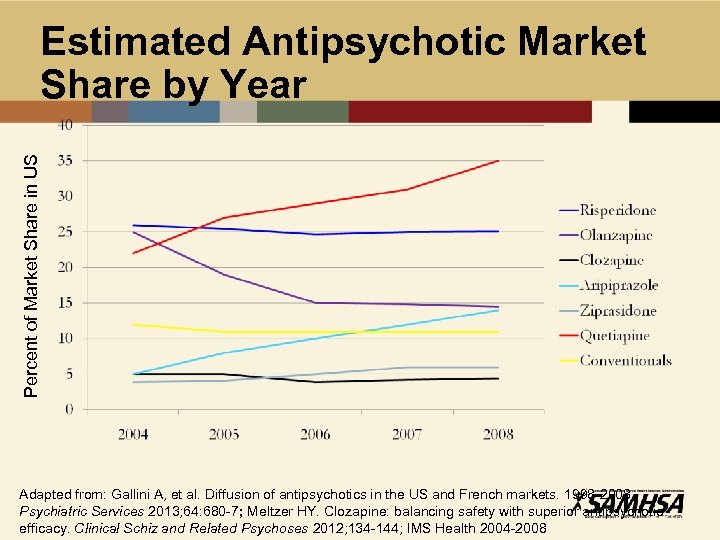
Percent of Market Share in US Estimated Antipsychotic Market Share by Year Adapted from: Gallini A, et al. Diffusion of antipsychotics in the US and French markets. 1998 -2008. Psychiatric Services 2013; 64: 680 -7; Meltzer HY. Clozapine: balancing safety with superior antipsychotic efficacy. Clinical Schiz and Related Psychoses 2012; 134 -144; IMS Health 2004 -2008
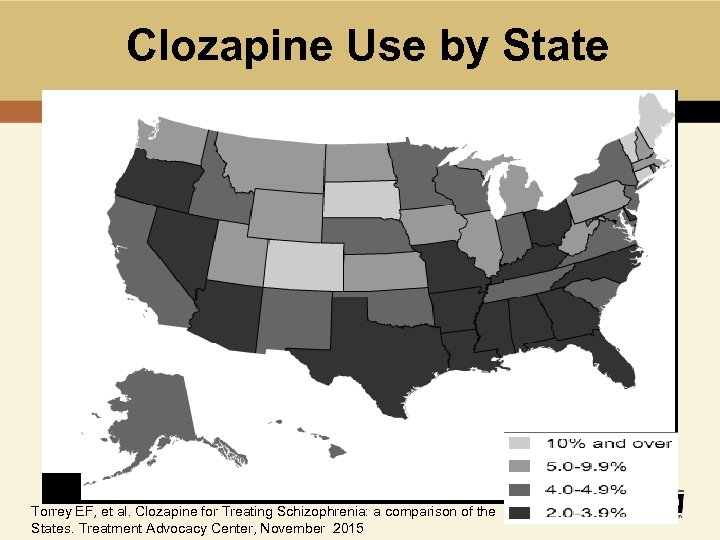
Clozapine Use by State Torrey EF, et al. Clozapine for Treating Schizophrenia: a comparison of the States. Treatment Advocacy Center, November 2015
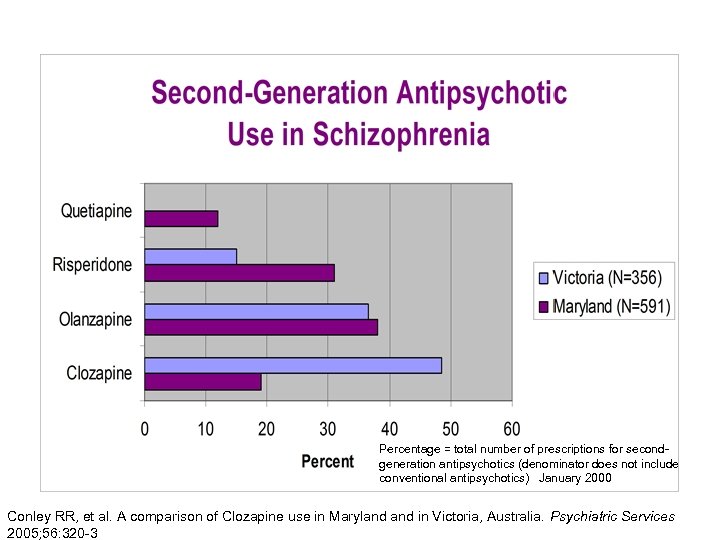
Percentage = total number of prescriptions for secondgeneration antipsychotics (denominator does not include conventional antipsychotics) January 2000 Conley RR, et al. A comparison of Clozapine use in Maryland in Victoria, Australia. Psychiatric Services 2005; 56: 320 -3

Clozapine Underutilization • In patients with two adequate failed antipsychotic trials the mean time to clozapine initiation was 47. 7 months (range 0 -219) with 5 trials prior • 68% of patients had 3 or more trials before clozapine initiation (mean prior therapy was ~ 8 yrs) • Time from diagnosis to clozapine initiation increased from 1996 to 2003 • Polypharmacy is higher than clozapine use with little evidence based guidance (approximately 20%) • Why the delay and underuse of clozapine? Howes OD, et al. Adherence to treatment guidelines in clinical practice: study of antipsychotic treatment prior to clozapine initiation. Br J of Psychiatry 2012; 201: 481 -5; Alessi-Severini S, et al. Clozapine prescribing in a Canadian outpatient population. PLo. S ONE 2013 epub ahead of print; Nielsen J, et al. Geographical and temporal variations in clozapine prescription for schizophrenia. European Neuropsychopharmacology 2012; 22: 818 -824; Gören JL, et al. Antipsychotic prescribing pathways, polypharmacy, and clozapine use in treatment of schizophrenia. Psychiatric Services 2013; 64: 527 -33; Gallego JA, et al. Prevalence and correlates of antipsychotic


Mortality Risk is Not Greater • Mortality with clozapine lower compared to other antipsychotic medications (HR = 0. 74) (N=66, 881 patients Finland) • Mortality is lower with clozapine compared to other antipsychotic medications (OR = 0. 23) (N=6, 987 patients Denmark) • Our group- finds mortality risk is same with clozapine compared to other antipsychotics both on survival analysis and autopsy findings Tiihonen J, et al. 11 -year follow-up of mortality in patients with schizophrenia: a population-based cohort study. Lancet 2009; 374: 620 -7; Kiviniemi M, et al. Antipsychotics and mortality in first onset schizophrenia: prospective Finnish register study with 5 year follow-up. Schizophr Res 2013; 150: 274 -280; Kelly DL, et al. Cardiac-Related Abnormalities at Autopsy in People with severe mental illness treated with clozapine or risperidone. Schizophr Res 2009; 107: 134 -8

BARRIERS TO CLOZAPINE

Overcoming Barriers to Use • Prescriber knowledge and comfort • Patient and family knowledge and comfort • Clozapine clinics • Hospitals and formularies • Registration in Clozapine. REMS • Point of care monitoring • Pharmacogenetic testing Sections we review in White Paper

Overcoming Barriers to Use • Assistance in clozapine initiation • Use in correctional systems and forensic settings • Managing side effects • Improving transitions of care • Suicide and emergency hotlines • Working with Medicaid and managed care companies • Blood draw ease and monitoring Sections we review in White Paper
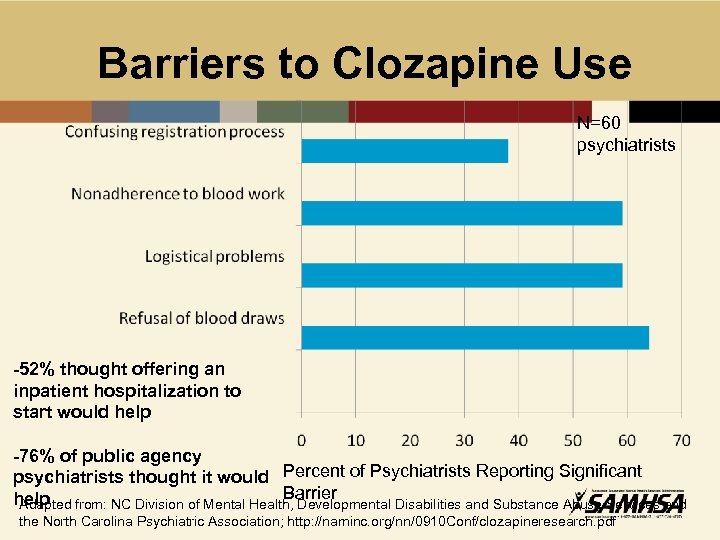
Barriers to Clozapine Use N=60 psychiatrists -52% thought offering an inpatient hospitalization to start would help -76% of public agency psychiatrists thought it would Percent of Psychiatrists Reporting Significant Barrier help Adapted from: NC Division of Mental Health, Developmental Disabilities and Substance Abuse Services and the North Carolina Psychiatric Association; http: //naminc. org/nn/0910 Conf/clozapineresearch. pdf
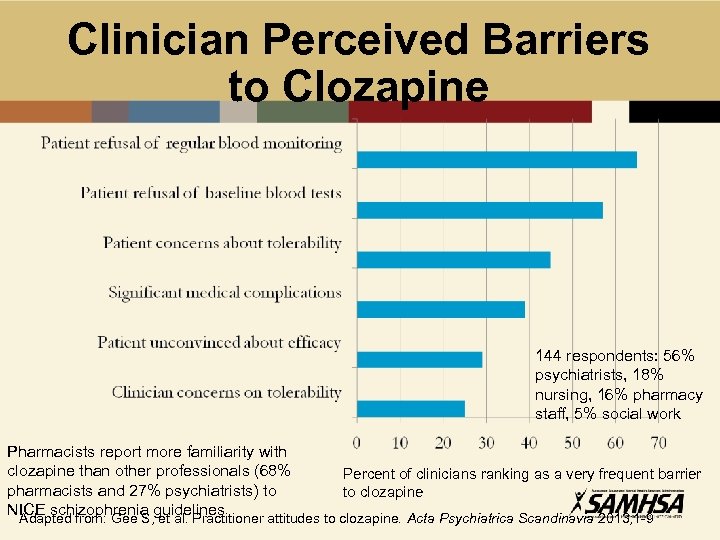
Clinician Perceived Barriers to Clozapine 144 respondents: 56% psychiatrists, 18% nursing, 16% pharmacy staff, 5% social work Pharmacists report more familiarity with clozapine than other professionals (68% pharmacists and 27% psychiatrists) to NICE schizophrenia guidelines Percent of clinicians ranking as a very frequent barrier to clozapine Adapted from: Gee S, et al. Practitioner attitudes to clozapine. Acta Psychiatrica Scandinavia 2013; 1 -9
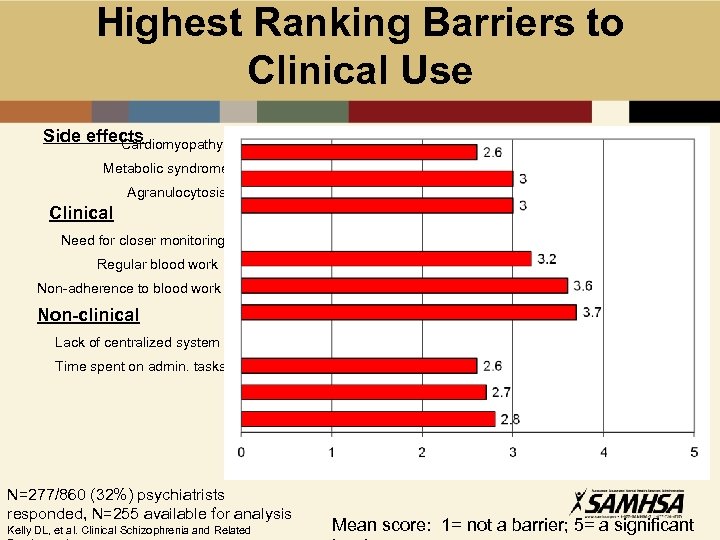
Highest Ranking Barriers to Clinical Use Side effects Cardiomyopathy Metabolic syndrome Agranulocytosis Clinical Need for closer monitoring Regular blood work Non-adherence to blood work Non-clinical Lack of centralized system Time spent on admin. tasks N=277/860 (32%) psychiatrists responded, N=255 available for analysis Kelly DL, et al. Clinical Schizophrenia and Related Mean score: 1= not a barrier; 5= a significant
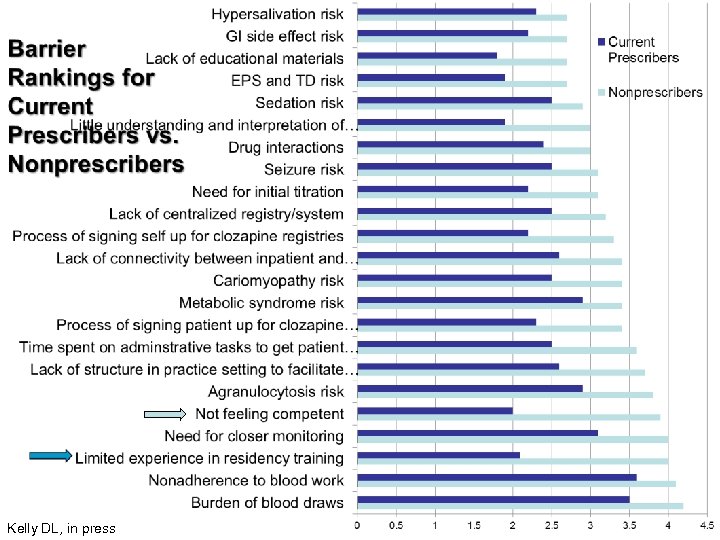
Kelly DL, in press

Patient’s Attitudes to Clozapine • N=1284, 27 clozapine clinics in UK • 86% feel better on clozapine • 89% prefer clozapine to other antipsychotics • 87% think advantages outweigh disadvantages • 28% rank frequent blood work as biggest disadvantage Taylor et al. Clozapine- a survey of patient perspectives. Psychiatr Bull 2000; 24: 450 -2.
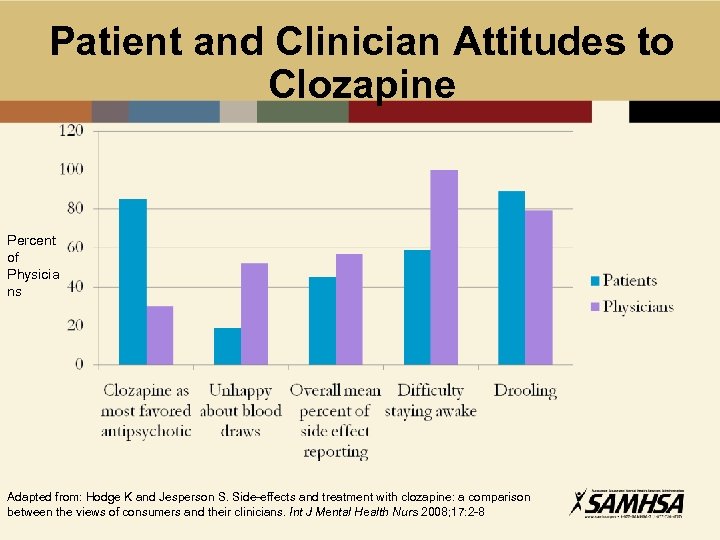
Patient and Clinician Attitudes to Clozapine Percent of Physicia ns Adapted from: Hodge K and Jesperson S. Side-effects and treatment with clozapine: a comparison between the views of consumers and their clinicians. Int J Mental Health Nurs 2008; 17: 2 -8

Psychiatrists and Severe Neutropenia • Psychiatrists overestimate real risk of severe neutropenia (agranulocytosis) • 23% think risk is >1% • 67% don’t know risk is greatest in first 6 months • Psychiatrists are 5 X more likely than patients to rate severe neutropenia risk as most problematic issue with clozapine Nielsen J, et al. Psychiatrist’s attitude towards and knowledge of clozapine treatment. J Psychopharmacol 2010; 24: 965 -71.

STRATEGIES FOR IMPROVED USE
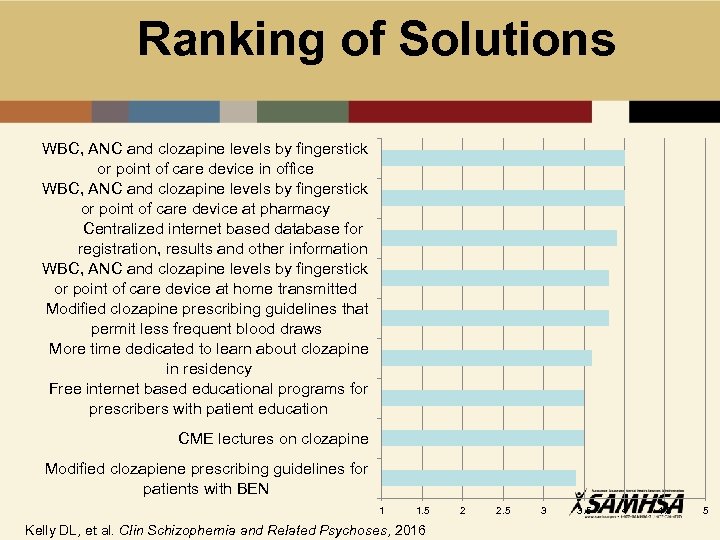
Ranking of Solutions WBC, ANC and clozapine levels by fingerstick or point of care device in office WBC, ANC and clozapine levels by fingerstick or point of care device at pharmacy Centralized internet based database for registration, results and other information WBC, ANC and clozapine levels by fingerstick or point of care device at home transmitted Modified clozapine prescribing guidelines that permit less frequent blood draws More time dedicated to learn about clozapine in residency Free internet based educational programs for prescribers with patient education CME lectures on clozapine Modified clozapiene prescribing guidelines for patients with BEN 1 1. 5 Kelly DL, et al. Clin Schizophernia and Related Psychoses, 2016 2 2. 5 3 3. 5 4 4. 5 5

Solutions Survey • Second survey sent to top clozapine prescribers in medicaid • 94 sent; 21 returned (22. 3%) • Top ranked solutions: 1. POC fingerstick (3. 75) 2. BEN support (3. 63) 3. Education program for families (3. 50) 4. Centralized Clozapine Clinic (3. 40) 5. Education program for physicians (3. 35) Kelly, et al. unpublished

Solutions Survey • Physicians that have <15 years experience: 1. Centralized Clinic (5. 0) 2. POC fingerstick (4. 67) 3. Backup prescriber (4. 33) 4. Inpatient referral (4. 0) 5. Education program for families and transportation for patients (3. 67) Kelly, et al. unpublished data

NEW GUIDELINES FOR CLOZAPINE MONITORING

Summary of Changes • Clozapine now managed through one entity - The Risk Evaluation and Mitigation Strategy (REMS) • Certification of prescribers, designees, and pharmacies • New thresholds for clozapine discontinuation - Provisions for BEN patients - Only ANC levels reported - Prescribers can continue treatment with rationale • Non-Rechallenge Master File discontinued - Agranulocytosis no longer in terminology

Summary of Unchanged • No change in frequency of blood draws • With exception that three times weekly instead of twice weekly at lower cut off values • No point of care monitoring approvals • No hematology consults required - Recommended under certain conditions • No changes in labeling other than around neutropenia

What happened to “agranulocytosis”? • No mention of agranulocytosis in new FDA guidelines; now defined as severe neutropenia • Mild Neutropenia - ANC 1, 000 -1, 499/mm 3 • Moderate Neutropenia - ANC 500 -999/mm 3 • Severe Neutropenia - ANC <500/mm 3

New thresholds for monitoring (general) ANC Treatment Recommendations** ANC Monitoring New patient initiation ANC ≥ 1500/mm 3 Initiate treatment Weekly x 6 months Every 2 weeks 6 -12 months Monthly after 12 months Mild Neutropenia ANC 10001499/mm 3 Continue treatment Redraw to confirm 3 X weekly until ANC ≥ 1500 Then return to patient’s last normal range monitoring interval Moderate Neutropenia ANC 500 -999/mm 3 Recommend hematology consult Interrupt treatment Resume once ANC normalizes to at least 1000 Redraw to confirm Daily ANC until at least 1000 Then three times weekly until at least 1500 Once ANC at least 1500, check weekly for 4 weeks then return to normal interval Severe Neutropenia Recommend heme consult ANC <500/mm 3 Interrupt treatment Do not rechallenge unless benefits outweigh risks Redraw to confirm Daily ANC until at least 1000 Then three times weekly until at least 1500 If rechallenged, resume as a new patient **Providers may continue treatment outside these ranges with rationale

Neutropenia in People of African Descent • Normative WBC ranges established in Caucasians • Lower WBC and ANC in African vs. European descent • Benign Ethnic Neutropenia • The occurrence of neutropenia (<1500 cells/mm 3), defined by normative data in white populations, in individuals of other ethnic groups who are otherwise healthy and who do not have repeated or severe infections • Linked to allelic variant of Duffy (FY) Antigen for Receptor Chemokine (DARC) Gene • ANC difference related to this factor is sufficient to explain the observed racial difference Haddy TB, e tal. Benign ethnic neutropenia: what is a normal absolute neutrophil count? J Lab Clin Med, 1999; 133: 15 -22. Shoenfeld Y, et al. Benign familial leukopenia and neutropenia in different ethnic groups. Eur J Haematol, 1988; 41: 273 -7. Reich D, et al. Reduced neutrophil count in people of African descent is due to a regulatory variant in the Duffy antigen receptor for chemokines gene. PLo. S Genet, 2009; 5: e 1000360.
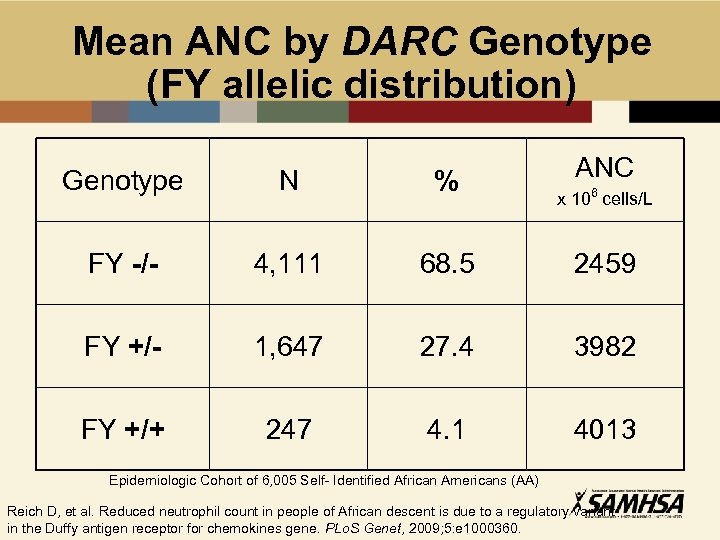
Mean ANC by DARC Genotype (FY allelic distribution) ANC Genotype N % FY -/- 4, 111 68. 5 2459 FY +/- 1, 647 27. 4 3982 FY +/+ 247 4. 1 4013 x 106 cells/L Epidemiologic Cohort of 6, 005 Self- Identified African Americans (AA) Reich D, et al. Reduced neutrophil count in people of African descent is due to a regulatory variant in the Duffy antigen receptor for chemokines gene. PLo. S Genet, 2009; 5: e 1000360.
Reich D, Nalls MA, Kao WHL, Akylbekova EL, et al. (2009) Reduced Neutrophil Count in People of African Descent Is Due To a Regulatory Variant in the Duffy Antigen Receptor for Chemokines Gene. PLo. S Genet 5(1): e 1000360. doi: 10. 1371/journal. pgen. 1000360 http: //www. plosgenetics. org/article/info: doi/10. 1371/journal. pgen. 1000360
Clozapine in African American Patients • Less likely to be initiated on clozapine -10. 3% vs. 15. 3% of 2911 inpatients in Maryland • More likely to be dc’s from clozapine - 42% vs. 23% after two years • More likely to be dc’s for neutropenia (5. 3% vs. 2. 4%) • Less likely to develop severe neutropenia (0. 62% vs. 0%) Kelly DL, et al. Clozapine Utilization and Outcomes by Race in a Public Mental Health System: 1994 -2000. J Clin Psychiatry, 2006; 67: 1404 -11; Kelly DL, et al. Clozapine Underutilization and discontinuation in African-Americans Due to Leucopenia. Schizophrenia Bulletin, 2007; 33: 1221 -4.

Largest Agranulocytois Cohort to Date • The NIMH funded Clozapine Induced Agranulocytosis Consortium (CIAC), collected data on an international sample of 482 CLZ-treated patients, including 161 agranulocytosis cases and 321 CLZ treated patients without agranulocytosis. • Of the 161 agranulocytosis cases, most were EA and only 5 worldwide in the consortium were AA, again suggesting rare occurrence of severe neutropenia and agranulocytosis risk in AA • Results: • HLA-DQB 1 (OR=0. 19, 95 CI: 0. 12 -0. 29) • HLA-B (OR=3. 3, 95% CI: 2. 3 -4. 9) Goldstein, J. I. , et al. , Clozapine-induced Agranulocytosis/granulocytopenia Is Associated with Rare HLA-DQB 1 and HLA_B Alleles. Nature Communications 2014; 5: 4757

Clozapine Treatment in Patients with Benign Neutropenia • Retrospective single site study • Data collection of patients with benign neutropenia who received clozapine with modified individual monitoring parameters • Primary outcome: difference in ANC values after initiation of clozapine compared to before clozapine • Secondary outcomes: • Within-participant fluctuations in ANC • Patient outcome on clozapine • Excluded patients receiving lithium Davis, Kelly et al, J Clin Psych, manuscript in press.

Demographic Characteristics Characteristic Number of patients 26 Age at clozapine initiation, mean (range) 34 years (20 – 56 years) Gender Male, n (%) 19 (73. 1%) Female, n (%) 7 (26. 9%) Race/Ethnicity African-American, n (%) 19 (73. 1%) Caucasian, n (%) 7 (26. 9%) Stabilized clozapine dose, mean (range) Davis, Kelly et al, J Clin Psych, manuscript in press. 456 mg (50 – 900 mg)
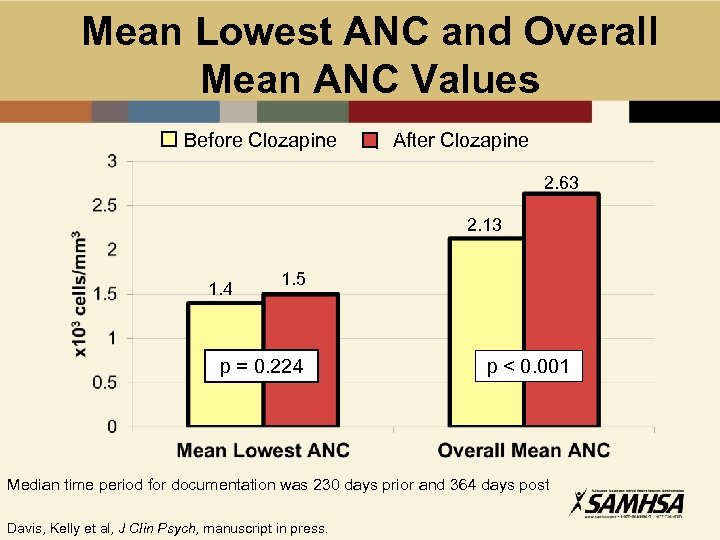
Mean Lowest ANC and Overall Mean ANC Values Before Clozapine After Clozapine 2. 63 2. 13 1. 4 1. 5 p = 0. 224 p < 0. 001 Median time period for documentation was 230 days prior and 364 days post Davis, Kelly et al, J Clin Psych, manuscript in press.

Results • No cases of severe neutropenia (ANC < 500 cells/mm 3) • ANC < 1000 cells/mm 3: • 1/271 (0. 4%) prior and 3/1096 (0. 3%) after (p=0. 795) • No patients were discontinued for falling below their modified guideline parameters • 5 patients had modified guidelines discontinued and successfully remain on manufacturer guidelines to date • 2 patients discontinued due to thrombocytopenia: • 1)Thrombocytopenia at baseline, no change with clozapine • 2) Normal platelets at baseline. With clozapine, steady decline to minimum of 93 x 103/μL. Improved, but not recovered to baseline 4 months after clozapine discontinuation. Davis, Kelly et al, J Clin Psych, manuscript in press.
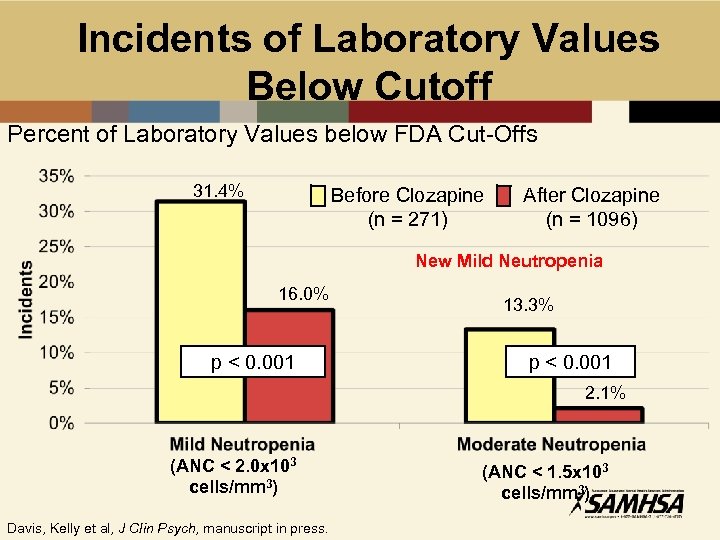
Incidents of Laboratory Values Below Cutoff Percent of Laboratory Values below FDA Cut-Offs 31. 4% Before Clozapine (n = 271) After Clozapine (n = 1096) New Mild Neutropenia 16. 0% p < 0. 001 13. 3% p < 0. 001 2. 1% (ANC < 2. 0 x 103 cells/mm 3) Davis, Kelly et al, J Clin Psych, manuscript in press. (ANC < 1. 5 x 103 cells/mm 3)
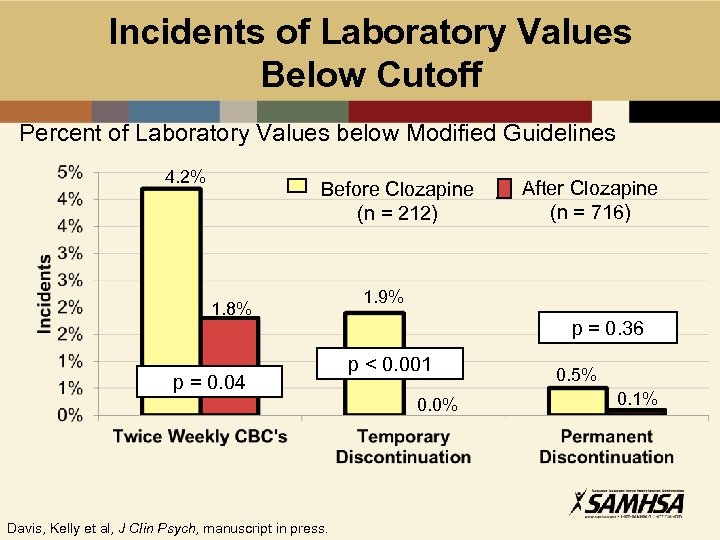
Incidents of Laboratory Values Below Cutoff Percent of Laboratory Values below Modified Guidelines 4. 2% Before Clozapine (n = 212) 1. 8% p = 0. 04 1. 9% p = 0. 36 p < 0. 001 0. 0% Davis, Kelly et al, J Clin Psych, manuscript in press. After Clozapine (n = 716) 0. 5% 0. 1%

New provisions for BEN patients ANC Treatment Recommendations** New patient initiation ANC ≥ 1000/mm 3 Obtain at least two baseline Weekly x 6 months ANC before initiation Every 2 weeks 6 -12 months Initiate treatment Monthly after 12 months Mild Neutropenia ANC 10001499/mm 3 Continue treatment Mild neutropenia normal range for BEN Weekly x 6 months Every 2 weeks from 6 -12 months Monthly after 12 months Moderate Neutropenia ANC 500 -999/mm 3 Recommend hematology consult Continue treatment Redraw to confirm ANC three times weekly until at least 1000 or pt’s known baseline Then check weekly for 4 weeks then return to patient’s normal range interval Severe Neutropenia Recommend heme consult ANC <500/mm 3 Interrupt treatment Do not rechallenge unless benefits outweigh risks ANC Monitoring Redraw to confirm Daily ANC until at least 500 Then three times weekly until at least to pt’s normal baseline If rechallenged, resume as a new patient **Providers may continue treatment outside these ranges with rationale

Biomarker and Safety Study of Clozapine in Patients with BEN • Aim to study and understand the safety and normal pattern of ANC fluctuations in BEN patients. - N=250, mostly African ancestry patients - 6 week observation, followed by 6 month open label treatment - FDA IND with special monitoring parameter - 3 sites, MPRC, Howard University and Federal Neuropsychiatric Hospital Yaba, Lagos, Nigeria • Aim to test to see if people with BEN have a genetic variant that may put them at risk of having a naturally lower ANC count than people who are White. - DARC allele relationship to ANC and treatment Kelly, PI. NIMH R 01 ongoing

Clozapine Clinics • VA study finds physicians would want to prescribe if more administrative and clinical support available through a clinic. - Clinical pharmacist assigned to oversee clinical and administrative tasks or outpatient clinic - 1 hour consultation with patient - Pharmacist responsible for: registration, assessment, dosage adjustment, monitoring, prescription processing • • • Cost savings Better discontinuation rates Early intervention into suicidality Good patient response Caregiver and family comfort level increased Williams T and Purvis TL. Development of an outpatient pharmacist-managed clozapine clinic. Am J Health-Syst Pharm 2012; 69: 1192 -5

Provider Education • Clozapine clinic at Massachusetts General Hospital (MGH) was incorporated into the Adult Psychiatric Residency • Weekly clinic plus education for 6 weeks - Positive feedback from residents - Resident’s knowledge about clozapine increased • Psychiatric trainees examined case vignettes with clinical and patient perspective information - The decision to follow guidelines and recommend clozapine was influenced principally by the importance of the patient’s positive symptoms - Authors recommend practice based learning education with residents - Clozapine optimization requires skills in advanced decision making including prioritizing patient’s perspective Freudenrich et al. Training in a clozapine clinic for psychiatry residents: a plea and suggestions for implementation. Acad Psychiatry 2013; 37: 27 -30. Falzer PR, et al. Optimizing clozapine through clinical decision making, Acta Psychiatr Scand 2012; 126: 47 -58.

Patient Education • Pharmacist created patient information leaflet compared to company produced educational leaflet for readability using REALM screening tool • Readability increased from 72. 5% to 95% and reading level scores decreased from 10. 3 to 8 on REALM with pharmacist created leaflet • No assessment of improved clozapine outcomes or utilization REALM= Rapid Estimate of Adult Literacy in Medicine Health Literacy Brosnan S, et al. Health literacy and the clozapine patient. Perspectives in Public Health 2012; 132: 39 -42

What is being done with Point of Care? • White blood cell technology developed, not accepted into the Clozapine. REMS • Monitoring for blood levels for maximizing, response, minimizing toxicity and monitoring adherence in development
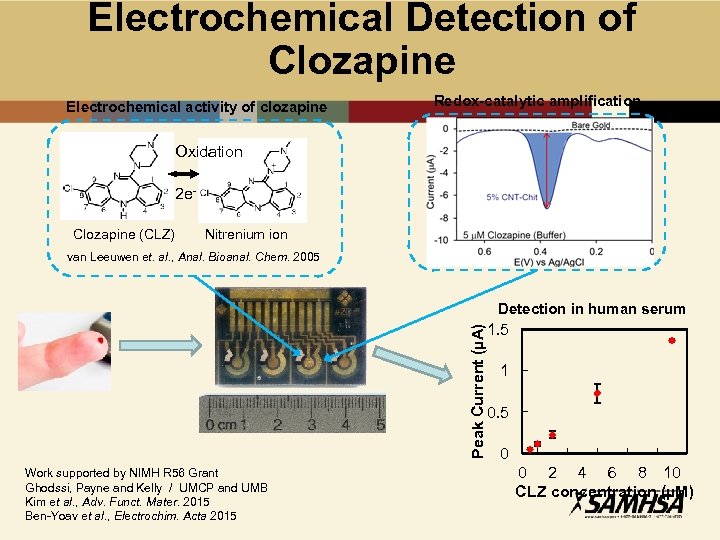
Electrochemical Detection of Clozapine Electrochemical activity of clozapine Redox-catalytic amplification Oxidation 2 e. Clozapine (CLZ) Nitrenium ion van Leeuwen et. al. , Anal. Bioanal. Chem. 2005 Peak Current (µA) Detection in human serum Work supported by NIMH R 56 Grant Ghodssi, Payne and Kelly / UMCP and UMB Kim et al. , Adv. Funct. Mater. 2015 Ben-Yoav et al. , Electrochim. Acta 2015 1. 5 1 0. 5 0 0 2 4 6 8 10 CLZ concentration (µM)

Clozapine Recommendations RESULTS OF THE NASMHPD WORKGROUP

Prescribers • Prescribers of clozapine should establish links with primary care practices to assist in the management of side effects that may emerge during treatment with clozapine • Prescribers should continually seek to improve knowledge base with lifelong learning on clozapine treatment • Less experienced prescribers should establish links with more experienced prescribers who can assist them in addressing issues that arise during clozapine treatment

Acute Care and Psychiatric Hospitals • All acute care and psychiatric hospitals should have clozapine on their formulary as an essential medication • All acute care and psychiatric hospitals should have policies and procedures to facilitate the safe and appropriate use of clozapine • All acute care hospitals should have access to appropriate staff or resources that allow continuation of clozapine on an inpatient basis when appropriate • All acute care hospitals should establish a policy that discharges patients on clozapine if: • they were taking clozapine prior to admission, • they were exhibiting a therapeutic response to clozapine, and • there is no contraindication to the use of clozapine upon discharge.

Academic Scientists and Pharmaceutical Research Programs • • • Neuroscience and pharmacologic research should focus on the molecular underpinnings of clozapine’s actions in order to facilitate the development of agents which share clozapine’s efficacy while eliminating its worse side effects Research should also focus on improving the understanding of clozapine induced blood dyscrasias, eliciting factors associated with a positive response to clozapine and discovering biomarkers that could improve the risk-to-benefit ratio for treatment with clozapine Systems research should focus on demonstrating clozapine’s cost effectiveness in various systems of care including forensics, best practices for interdisciplinary teams managing patients receiving clozapine, developing novel practice and service models and establishing the effectiveness of prevention strategies for clozapine-associated weight gain and metabolic effects Technological support should include the development of point-of-care testing devices to perform hematologic monitoring for those receiving clozapine Research should be focused to aid the FDA in modifying prescribing and monitoring guidelines for those receiving clozapine

Local and State Health Authorities • Every public health system of care should have a system that provides ready access to clozapine, provides appropriate safety monitoring of patients receiving it and encourages prescribers to consider its use when appropriate • Mental health authorities should consider establishing model programs for the initiation and monitoring of clozapine patients and consider offering evidence-based recommendations for addressing metabolic side effects and other emergent side effects • Mental health authorities should establish mechanisms for the initiation of clozapine in outpatients such as designated beds in respite care or sites offering 24 hour supervision or clozapine clinics with this capacity and expertise.

Local and State Health Authorities • • • Academic centers in consultation with state or local mental health authorities should establish interdisciplinary consultation centers for community providers involved in the management of patients receiving clozapine Mental health authorities should develop community specific systems for laboratory monitoring of patients receiving clozapine that may include the use of Assertive Community Treament (ACT) teams, transportation systems, visiting phlebotomists, pharmacy based phlebotomy or other solutions Mental health authorities should develop population management tools to facilitate and monitor transitions of care, help assure continuation of treatment and reduce interruptions in the treatment of patients receiving clozapine.

Payers • • • Payers should develop payment mechanisms that recognize the complexity of managing patients receiving clozapine including: - enhanced payment mechanisms for prescribers; - payment mechanisms for nurses, pharmacists and social workers participating in interdisciplinary clozapine teams; - payment for telemedicine systems to provide consultation for community health professionals managing clozapine patients - payment for transportation for patients for laboratory monitoring and/or payments for home visits for phlebotomy Clozapine should be a Tier 1 preferred medication (or its equivalent) on the formularies of all state Medicaid programs, Medicare prescription drug programs, pharmacy benefit/managed care programs contracting with state Medicaid programs and other payers of pharmacy benefits Payers should encourage the development, adoption of and reimburse for Medication Therapy Management (MTM) services for patients receiving clozapine.

Correctional Systems • Every correctional health care system should have a system that provides ready access to clozapine or establishes mechanisms for referral of inmates who are appropriate for treatment with clozapine • Every correctional health care system should have policies and procedures to facilitate the safe and appropriate use of clozapine • Every correctional health care system should provide appropriate safety monitoring of patients receiving clozapine

Providers of Continuing Education for Health Professionals • Health professional organizations and continuing education providers should develop and offer interdisciplinary continuing education programs on the use of clozapine that include physicians, pharmacists, nurses, social workers and other health care providers

National Efforts • National efforts should focus on the development and dissemination of the following types of toolkits and information related to clozapine: - Sample informed consent form for clozapine; - Discussion paper on shared decision making; - Forms for monitoring specific side effects; - Patient and family education materials; - Checklists for establishing a clozapine clinic including: • materials on interdisciplinary roles in the management of patients receiving • • • clozapine establishing pharmacy linkages for patients receiving clozapine options for hematologic testing potential funding mechanisms or models for clozapine programs and models for a clozapine consultation service including interdisciplinary telehealth models; - Reference clozapine. links to educational programs regarding the use of

National Efforts • • National efforts should continually evaluate the Clozapine. REMS Program in order to assure that it facilitates clozapine use and does not present unintended barriers to use - This evaluation should consider scientific evidence and analyze data trends that might inform changes in clozapine monitoring guidelines such as less frequent ANC monitoring, genetic testing that dictates less stringent hematologic monitoring, or elimination of ANC monitoring in patient groups who have minimal risk of severe neutropenia (ie. , African descent) National efforts should focus on work with relevant stakeholders to explore the use of the Clozapine. REMS Program as a population management tool that could be used by state systems to facilitate and monitor transitions of care, help assure continuation of treatment and reduce interruptions in treatment in patients receiving clozapine.

National Efforts • • • Telehealth and call center technology should be used to provide access to professionals who can provide consultation on the complexities of clozapine use The technology of the Clozapine. REMS registry should be harnessed to improved facilitate and monitor transitions of care and reduce interruptions in treatment for those receiving clozapine Establishment of a dynamic, web-based source of information educational programs providing information on delivery models, patient monitoring, patient and family education and provider education would assist all who might serve potential recipients of clozapine Point-of-care testing should be developed to assist in monitoring of those receiving clozapine Biomarker testing to improve the predictability of response to clozapine and the risk for specific adverse effects should be developed

Conclusions • Clozapine is a superior medication for the treatment of refractory schizophrenia and may be effective for a wide spectrum of other indications • Clozapine is underused due to a variety of barriers related to the drug and its properties, the health care system, regulatory requirements and reimbursement issues • This white paper provides the framework for addressing these barriers and recommending strategies for the entire health care system to consider • If access to clozapine is improved, millions of patients could benefit. In turn their improved care could substantial cost savings to the entire health care system

94aded9fc5f58d797723162b5129155b.ppt