27ea93e1c70831c1cf4b036712ea071a.ppt
- Количество слайдов: 134
 Clinical Management of the Common Opportunistic Infections HIV Care and ART: A Course for Physicians
Clinical Management of the Common Opportunistic Infections HIV Care and ART: A Course for Physicians
 Learning Objectives • Identify when HIV-related opportunistic infections (OIs) occur in relation to CD 4 cell count • Describe the syndromic diagnosis and treatment of common OIs • Describe the primary and secondary prophylaxis for common OIs
Learning Objectives • Identify when HIV-related opportunistic infections (OIs) occur in relation to CD 4 cell count • Describe the syndromic diagnosis and treatment of common OIs • Describe the primary and secondary prophylaxis for common OIs
 Syndromes Considered in This Unit • • • Fever Cough Headache w/ and w/o neurological findings Gastrointestinal disease Rash
Syndromes Considered in This Unit • • • Fever Cough Headache w/ and w/o neurological findings Gastrointestinal disease Rash
 Opportunistic Infection: Definition • Infections that develop as a result of damage to the immune system are called opportunistic infections or OIs • These infections take advantage of the opportunity provided by a weakened immune system • Infections tend to appear at predictable stages of immune deterioration
Opportunistic Infection: Definition • Infections that develop as a result of damage to the immune system are called opportunistic infections or OIs • These infections take advantage of the opportunity provided by a weakened immune system • Infections tend to appear at predictable stages of immune deterioration
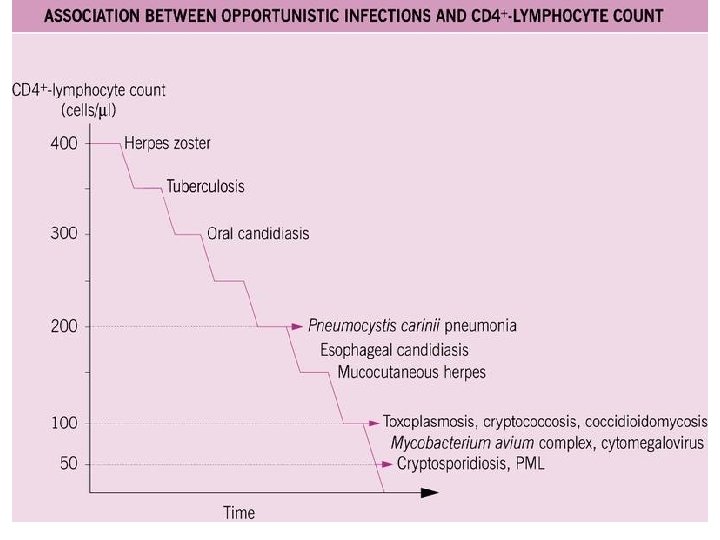
 Principles of OIs with HIV • Caused by defect in cell-mediated immunity, so common viral and bacterial infections are not increased – Exceptions: S. pneumoniae and Salmonella • Nearly all OIs respond to HAART – Exception: PML (progressive multifocal leukoencephalopathy) • Immune Reconstitution Inflammatory Syndrome (IRIS) – Paradoxical illness associated with improving immunity – Most common with CD 4 <50, following initiation of effective HAART – Treatment: continue ART and OI treatment +/- steroids
Principles of OIs with HIV • Caused by defect in cell-mediated immunity, so common viral and bacterial infections are not increased – Exceptions: S. pneumoniae and Salmonella • Nearly all OIs respond to HAART – Exception: PML (progressive multifocal leukoencephalopathy) • Immune Reconstitution Inflammatory Syndrome (IRIS) – Paradoxical illness associated with improving immunity – Most common with CD 4 <50, following initiation of effective HAART – Treatment: continue ART and OI treatment +/- steroids
 Case 1 • Sisay, a 42 year-old merchant, presented to the OPD complaining of two weeks high grade and intermittent fever that usually comes in the afternoon • He has no complaints except fever. Specifically, he denies: – – – Cough or shortness of breath Abdominal pain, diarrhea or vomiting Loss of appetite or weight loss Urinary complaints Headache or neck pain Travel to malaria endemic area
Case 1 • Sisay, a 42 year-old merchant, presented to the OPD complaining of two weeks high grade and intermittent fever that usually comes in the afternoon • He has no complaints except fever. Specifically, he denies: – – – Cough or shortness of breath Abdominal pain, diarrhea or vomiting Loss of appetite or weight loss Urinary complaints Headache or neck pain Travel to malaria endemic area
 Discussion • What would you include in your initial differential diagnosis?
Discussion • What would you include in your initial differential diagnosis?
 • Definition: 38°C • Pattern: > Diurnal variation – Highest at night, low in AM • Fever patterns: Picket fence, sustained intermittent • Pattern is usually not helpful except Malaria – diurnal Lymphoma – Pel Epstein
• Definition: 38°C • Pattern: > Diurnal variation – Highest at night, low in AM • Fever patterns: Picket fence, sustained intermittent • Pattern is usually not helpful except Malaria – diurnal Lymphoma – Pel Epstein
 Fever of unknown origin (FUO) • Classic definition - Temp > 38. 3°C - Three wks - No dx with 1 wk workup • Causes - ID: TB, endocarditis, IAS - CVD: Still dis, RA, SLE • Granulomas: Temp. arteritis, sarcoid, Crohn dis, etc. • Tumors: Lymphoma, leukemia, “omas”, hepatic mets • Other: Drugs, factitious
Fever of unknown origin (FUO) • Classic definition - Temp > 38. 3°C - Three wks - No dx with 1 wk workup • Causes - ID: TB, endocarditis, IAS - CVD: Still dis, RA, SLE • Granulomas: Temp. arteritis, sarcoid, Crohn dis, etc. • Tumors: Lymphoma, leukemia, “omas”, hepatic mets • Other: Drugs, factitious
 FUO by category Young Old Travelers AIDS Viral Temp. art Salmonella Enigmatic Polyalgia Malaria Tumors TB TB MAC Lymphoma PCP
FUO by category Young Old Travelers AIDS Viral Temp. art Salmonella Enigmatic Polyalgia Malaria Tumors TB TB MAC Lymphoma PCP
 Ethiopia + HIV 2 -3 wks CD 4 >200 <200 Main causes TB, Malaria Adverse drug reaction Above plus Lymphoma, M. avium, Toxoplasmosis, Cryptococcosis, Leishmaniasis
Ethiopia + HIV 2 -3 wks CD 4 >200 <200 Main causes TB, Malaria Adverse drug reaction Above plus Lymphoma, M. avium, Toxoplasmosis, Cryptococcosis, Leishmaniasis
 Additional Information • Sisay had been seen in the local health center where blood film (BF) was done. He was treated with antibiotics after the BF turned out to be negative but showed no improvement • He was screened for HIV five years back and was seropositive. He has never been ill and has received no treatment
Additional Information • Sisay had been seen in the local health center where blood film (BF) was done. He was treated with antibiotics after the BF turned out to be negative but showed no improvement • He was screened for HIV five years back and was seropositive. He has never been ill and has received no treatment
 Discussion • How does this additional information affect your differential diagnosis? • What might you expect to find on physical examination?
Discussion • How does this additional information affect your differential diagnosis? • What might you expect to find on physical examination?
 Physical Examination • • Vital signs Head and neck – Thrush, fundoscopy Lungs – Rales, consolidation Cor Abdomen – Liver and spleen, tenderness Skin – Rash, nodules Neuro – localizing findings strength, DTRs; cranial nerves, Rhomberg
Physical Examination • • Vital signs Head and neck – Thrush, fundoscopy Lungs – Rales, consolidation Cor Abdomen – Liver and spleen, tenderness Skin – Rash, nodules Neuro – localizing findings strength, DTRs; cranial nerves, Rhomberg
 Discussion • How does this additional information affect your differential diagnosis? • How do you investigate this patient?
Discussion • How does this additional information affect your differential diagnosis? • How do you investigate this patient?
 Differential Diagnosis: Infections • Protozoal: malaria, toxoplasma, leishmania, others • Bacterial – Local pyogenic infection of the chest, urinary tract, the CNS, sinuses, etc – Bacteremia/septicemia due to Salmonella, Streptococcus, Staphylococcus, H. influenza, meningococcus, etc – Mycobacterial infection – M. tuberculosis, M. avium, M. kansasii – Viral infections: HSV, VZV, CMV – Fungal infections: PCP, Cryptococcosis, Candidiasis
Differential Diagnosis: Infections • Protozoal: malaria, toxoplasma, leishmania, others • Bacterial – Local pyogenic infection of the chest, urinary tract, the CNS, sinuses, etc – Bacteremia/septicemia due to Salmonella, Streptococcus, Staphylococcus, H. influenza, meningococcus, etc – Mycobacterial infection – M. tuberculosis, M. avium, M. kansasii – Viral infections: HSV, VZV, CMV – Fungal infections: PCP, Cryptococcosis, Candidiasis
 Differential Diagnosis (2) • Neoplasms – Lymphoma (NHL) – Kaposi's sarcoma • Others – Drug reaction
Differential Diagnosis (2) • Neoplasms – Lymphoma (NHL) – Kaposi's sarcoma • Others – Drug reaction
 Drug Fever • Symptoms: Usually none • Fever pattern: Picket fence or sustained • Usual causes in Ethiopia: sulfa, Dapsone, Clindamycin, Phenytoin, Betalactams Serious causes: NVP, ABC • Diagnosis: Discontinue drug → fever resolves in 24 -48 hours
Drug Fever • Symptoms: Usually none • Fever pattern: Picket fence or sustained • Usual causes in Ethiopia: sulfa, Dapsone, Clindamycin, Phenytoin, Betalactams Serious causes: NVP, ABC • Diagnosis: Discontinue drug → fever resolves in 24 -48 hours
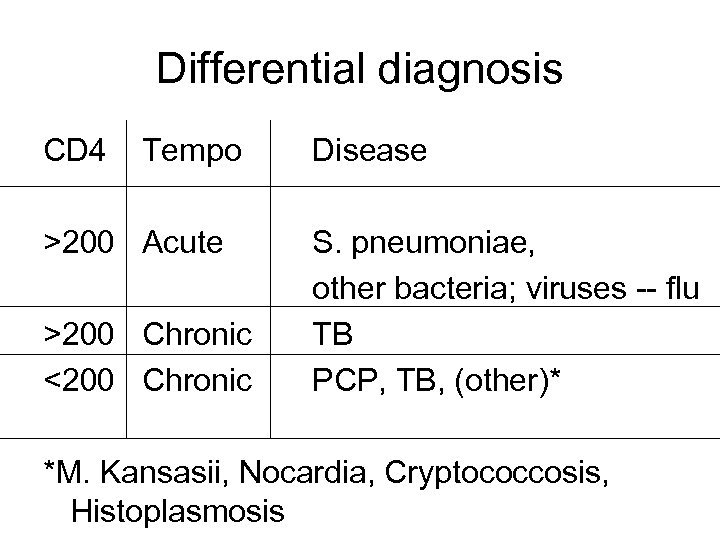 Differential diagnosis CD 4 Tempo Disease >200 Acute S. pneumoniae, other bacteria; viruses -- flu >200 Chronic TB <200 Chronic PCP, TB, (other)* *M. Kansasii, Nocardia, Cryptococcosis, Histoplasmosis
Differential diagnosis CD 4 Tempo Disease >200 Acute S. pneumoniae, other bacteria; viruses -- flu >200 Chronic TB <200 Chronic PCP, TB, (other)* *M. Kansasii, Nocardia, Cryptococcosis, Histoplasmosis
 Approach to Fever in HIV Patients Meticulous Physical Exam • HEENT, including sinuses and ears • Lymphoglandular system • Chest, including intercostal tenderness and cardiac evaluation • Abdominal exam including PR • Genitourinary system, including gynecological evaluation • Musculoskeletal • Integumentary • CNS, including meningeal signs and fundoscopy
Approach to Fever in HIV Patients Meticulous Physical Exam • HEENT, including sinuses and ears • Lymphoglandular system • Chest, including intercostal tenderness and cardiac evaluation • Abdominal exam including PR • Genitourinary system, including gynecological evaluation • Musculoskeletal • Integumentary • CNS, including meningeal signs and fundoscopy
 Discussion • How would you approach the laboratory evaluation of a patient with fever of undetermined origin? • What tests would you include in your initial evaluation? • If these were non-diagnostic, what additional tests would you consider?
Discussion • How would you approach the laboratory evaluation of a patient with fever of undetermined origin? • What tests would you include in your initial evaluation? • If these were non-diagnostic, what additional tests would you consider?
 Laboratory Investigation • • CBC Malaria smear (if likely) Blood culture (? ) AFB stain + culture Serologic studies Blood chemistry – LFT Chest x-ray
Laboratory Investigation • • CBC Malaria smear (if likely) Blood culture (? ) AFB stain + culture Serologic studies Blood chemistry – LFT Chest x-ray
 Additional Tests • • • Ultrasound, CT scan, MRI Lumbar puncture (CSF analysis) FNA of lymph nodes, biopsy skin lesions CD 4 count, viral load (if not recently done) Bone marrow
Additional Tests • • • Ultrasound, CT scan, MRI Lumbar puncture (CSF analysis) FNA of lymph nodes, biopsy skin lesions CD 4 count, viral load (if not recently done) Bone marrow
 Case Study Discussion • How would you manage Sisay?
Case Study Discussion • How would you manage Sisay?
 Fever Management • Definitive management of the causative agent – Therapeutic trial may be considered if tests are nondiagnostic • Supportive – catabolic febrile state may require various supportive measures. Based on the patient, consider: – – – Rehydration Electrolyte replacement Calorie replacement Respiratory support Palliative control of fever, e. g. , with antipyretic, sponging
Fever Management • Definitive management of the causative agent – Therapeutic trial may be considered if tests are nondiagnostic • Supportive – catabolic febrile state may require various supportive measures. Based on the patient, consider: – – – Rehydration Electrolyte replacement Calorie replacement Respiratory support Palliative control of fever, e. g. , with antipyretic, sponging
 Examples of Fever-causing Agents without localizing signs • • • Leishmaniasis Mycobacterium avium complex Tuberculosis Lymphoma Drug fever
Examples of Fever-causing Agents without localizing signs • • • Leishmaniasis Mycobacterium avium complex Tuberculosis Lymphoma Drug fever
 Visceral Leishmaniasis and HIV Co-infection • Caused by L. donovanii, an important OI among persons infected with HIV-1 • Reports mainly from S. Europe, E. Africa, N. and S. America and Asia • Most co-infected patients with clinically evident leishmaniasis have CD 4 cell less than 200/µl • HIV and L. donovanii affect the same cell lines, causing cumulative deficiency of the immune response • Leishmania parasites suppress Th 1 activity
Visceral Leishmaniasis and HIV Co-infection • Caused by L. donovanii, an important OI among persons infected with HIV-1 • Reports mainly from S. Europe, E. Africa, N. and S. America and Asia • Most co-infected patients with clinically evident leishmaniasis have CD 4 cell less than 200/µl • HIV and L. donovanii affect the same cell lines, causing cumulative deficiency of the immune response • Leishmania parasites suppress Th 1 activity
 Visceral Leishmaniasis Clinical Manifestations • Patients present with fever, organomegaly, anemia or pancytopenia • Presentation could be atypical, but VL should be suspected in those with travel history to endemic areas
Visceral Leishmaniasis Clinical Manifestations • Patients present with fever, organomegaly, anemia or pancytopenia • Presentation could be atypical, but VL should be suspected in those with travel history to endemic areas
 Visceral Leishmaniasis Diagnosis and Treatment • Diagnosis – Serology less sensitive in immunocompromised hosts. – Parasite could be detected in peripheral blood of immunocompromised patients. – Bone marrow aspirate more sensitive, and splenic aspirate most sensitive. • Treatment – First line – Pentavalent antimonials (Sb) – Alternatives – Pentamidine, Amphotericin B – Relapse and toxicity are common in patients coinfected with HIV.
Visceral Leishmaniasis Diagnosis and Treatment • Diagnosis – Serology less sensitive in immunocompromised hosts. – Parasite could be detected in peripheral blood of immunocompromised patients. – Bone marrow aspirate more sensitive, and splenic aspirate most sensitive. • Treatment – First line – Pentavalent antimonials (Sb) – Alternatives – Pentamidine, Amphotericin B – Relapse and toxicity are common in patients coinfected with HIV.
 Mycobacterium Avium Complex (MAC) Overview • Ubiquitous in the environment: soil, water, food, house dust, domestic and wild animals • Low CD 4 (<50) is required • Diagnosis requires AFB stain and culture. Usual is blood in special media held 3 weeks • Pre-HAART, MAC was the most common OI, affecting up to 43% of AIDS patients in America • Not seen in Ethiopia, but his may reflect lack of diagnostic resources • Dramatic ART treatment impact
Mycobacterium Avium Complex (MAC) Overview • Ubiquitous in the environment: soil, water, food, house dust, domestic and wild animals • Low CD 4 (<50) is required • Diagnosis requires AFB stain and culture. Usual is blood in special media held 3 weeks • Pre-HAART, MAC was the most common OI, affecting up to 43% of AIDS patients in America • Not seen in Ethiopia, but his may reflect lack of diagnostic resources • Dramatic ART treatment impact
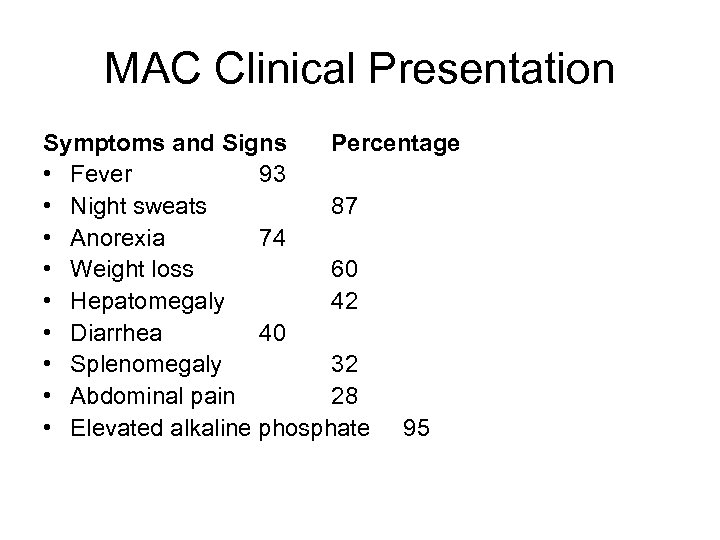 MAC Clinical Presentation Symptoms and Signs Percentage • Fever 93 • Night sweats 87 • Anorexia 74 • Weight loss 60 • Hepatomegaly 42 • Diarrhea 40 • Splenomegaly 32 • Abdominal pain 28 • Elevated alkaline phosphate 95
MAC Clinical Presentation Symptoms and Signs Percentage • Fever 93 • Night sweats 87 • Anorexia 74 • Weight loss 60 • Hepatomegaly 42 • Diarrhea 40 • Splenomegaly 32 • Abdominal pain 28 • Elevated alkaline phosphate 95
 MAC Treatment • At least two medications – Clarithromycin 500 mg bid po (or Azithromycin 500 -600 mg qd po) AND – Ethambutol 15 mg/kg qd po • Add 3 rd or 4 th drug if: CD 4 count <50; high mycobacterial loads; or absence of effective ART – Ciprofloxacin 500 -750 mg bid po – Levofloxacin 500 mg qd po – Amikacin IV 10 -15 mg/kg qd
MAC Treatment • At least two medications – Clarithromycin 500 mg bid po (or Azithromycin 500 -600 mg qd po) AND – Ethambutol 15 mg/kg qd po • Add 3 rd or 4 th drug if: CD 4 count <50; high mycobacterial loads; or absence of effective ART – Ciprofloxacin 500 -750 mg bid po – Levofloxacin 500 mg qd po – Amikacin IV 10 -15 mg/kg qd
 Case Two • Belaynesh is a 34 year-old woman presenting with two months history of non productive cough, and two weeks of fever with progressively worse shortness of breath • Also notes three months of generalized body weakness, loss of appetite and 8 kg. weight loss • Her husband died two years ago of “bird” (pulmonary disease) leaving her with two children who are now 12 and 14
Case Two • Belaynesh is a 34 year-old woman presenting with two months history of non productive cough, and two weeks of fever with progressively worse shortness of breath • Also notes three months of generalized body weakness, loss of appetite and 8 kg. weight loss • Her husband died two years ago of “bird” (pulmonary disease) leaving her with two children who are now 12 and 14
 Discussion • What would you include in your initial differential diagnosis?
Discussion • What would you include in your initial differential diagnosis?
 On examination. . . • • She was in respiratory distress Mild cyanosis of the finger tips Bilateral fine diffuse rales Vital signs – – – BP Temp Pulse Resp WT 110/70 mm Hg 38 o. C 112/m 36/m 48 Kgs • What tests would you like to order?
On examination. . . • • She was in respiratory distress Mild cyanosis of the finger tips Bilateral fine diffuse rales Vital signs – – – BP Temp Pulse Resp WT 110/70 mm Hg 38 o. C 112/m 36/m 48 Kgs • What tests would you like to order?
 Potential Diagnostic Tests • CBC • Sputum culture & stain for AFB, bacteria, fungal • CXR • HIV serology • LFT, RFT, etc • CD 4
Potential Diagnostic Tests • CBC • Sputum culture & stain for AFB, bacteria, fungal • CXR • HIV serology • LFT, RFT, etc • CD 4
 Belaynesh’s Laboratory Results • • WBC TLC Hgb Gram stain AFB HIV serology CD 4 CXR 2500/mm 3 750/mm 3 12 g/dl negative 3 x positive pending as follows
Belaynesh’s Laboratory Results • • WBC TLC Hgb Gram stain AFB HIV serology CD 4 CXR 2500/mm 3 750/mm 3 12 g/dl negative 3 x positive pending as follows
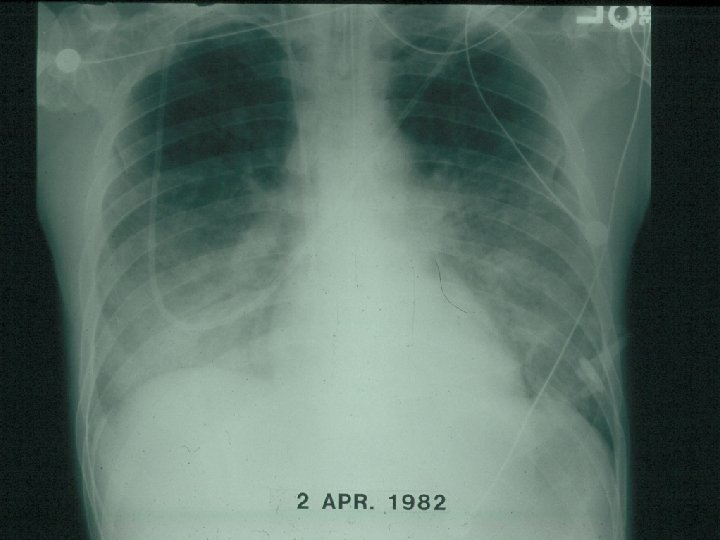 PCP Chest Radiograph
PCP Chest Radiograph
 Discussion • How do these results change your differential diagnosis? • How would you manage this patient?
Discussion • How do these results change your differential diagnosis? • How would you manage this patient?
 Focused Differential Diagnosis • PCP • Pulmonary tuberculosis (atypical appearance) in late stage HIV disease
Focused Differential Diagnosis • PCP • Pulmonary tuberculosis (atypical appearance) in late stage HIV disease
 Pneumocystis Jiroveci Pneumonia • Most humans infected early in life • Diagnosis via induced sputum or bronchoalveolar lavage (bronchoscopy) – Stains with Wright-Giemsa, methenamine silver, and direct immunofluorescence • Typical presentation – Non-productive cough – Exertional dyspnea – Gradual fever
Pneumocystis Jiroveci Pneumonia • Most humans infected early in life • Diagnosis via induced sputum or bronchoalveolar lavage (bronchoscopy) – Stains with Wright-Giemsa, methenamine silver, and direct immunofluorescence • Typical presentation – Non-productive cough – Exertional dyspnea – Gradual fever
 Pneumocystis Treatment • Standard regimen: – Cotrimoxazole (15 -20 mg TMP + 75 -100 mg SMX)/kg/day in 3 doses IV or PO for 3 weeks • Alternative treatments: – Dapsone 100 mg qd + Trimethoprim 15 mg/kg/day PO divided tid x 3 wks – Primaquine 15 -30 mg qd + Clindamycin 450 mg po q 8 h x 3 wks
Pneumocystis Treatment • Standard regimen: – Cotrimoxazole (15 -20 mg TMP + 75 -100 mg SMX)/kg/day in 3 doses IV or PO for 3 weeks • Alternative treatments: – Dapsone 100 mg qd + Trimethoprim 15 mg/kg/day PO divided tid x 3 wks – Primaquine 15 -30 mg qd + Clindamycin 450 mg po q 8 h x 3 wks
 Adjunctive Corticosteroids in Pneumocystis Therapy • Adjunctive corticosteroids are indicated for severe hypoxemia (p. O 2<70, Aa. DO 2>35) • Reduces mortality by 50% • Start within 72 hours of presentation • Regimen – Prednisone 40 mg po bid x 5 days, followed by – 40 mg qd x 5 days, followed by – 20 mg qd x 11 days • No benefit for mild episodes • Use cautiously if diagnosis is not confirmed, and watch for other OIs
Adjunctive Corticosteroids in Pneumocystis Therapy • Adjunctive corticosteroids are indicated for severe hypoxemia (p. O 2<70, Aa. DO 2>35) • Reduces mortality by 50% • Start within 72 hours of presentation • Regimen – Prednisone 40 mg po bid x 5 days, followed by – 40 mg qd x 5 days, followed by – 20 mg qd x 11 days • No benefit for mild episodes • Use cautiously if diagnosis is not confirmed, and watch for other OIs
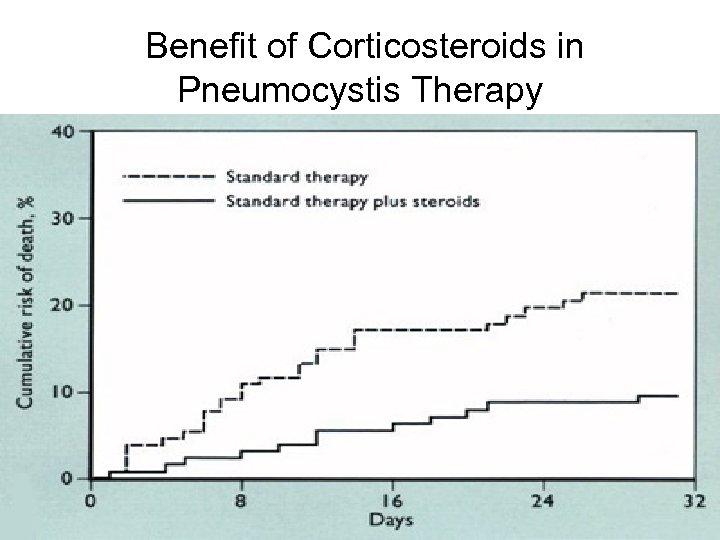 Benefit of Corticosteroids in Pneumocystis Therapy
Benefit of Corticosteroids in Pneumocystis Therapy
 Pneumocystis Prophylaxis Indications • Primary prophylaxis (to prevent disease) – CD 4 < 350/mm 3 – WHO Stage II, IV – HIV-associated oral candidiasis – Unexplained fever • Secondary prophylaxis (after pneumonia, to prevent recurrence) – Prior episode of PCP
Pneumocystis Prophylaxis Indications • Primary prophylaxis (to prevent disease) – CD 4 < 350/mm 3 – WHO Stage II, IV – HIV-associated oral candidiasis – Unexplained fever • Secondary prophylaxis (after pneumonia, to prevent recurrence) – Prior episode of PCP
 Pneumocystis Prophylaxis Agents • Standard regimen – Cotrimoxazole (TMP/SMX) 1 tab daily* • Alternate regimens – Dapsone 100 mg daily • Duration of treatment: lifelong, but • May safely discontinue if immune system restored from ART – Must have CD 4 > 250 for 3 months *TMP-SMX is no more effective than dapsone for preventing PCP, but also prevents toxo, Listeria, S. pneumo, S. aureus, Legionella etc.
Pneumocystis Prophylaxis Agents • Standard regimen – Cotrimoxazole (TMP/SMX) 1 tab daily* • Alternate regimens – Dapsone 100 mg daily • Duration of treatment: lifelong, but • May safely discontinue if immune system restored from ART – Must have CD 4 > 250 for 3 months *TMP-SMX is no more effective than dapsone for preventing PCP, but also prevents toxo, Listeria, S. pneumo, S. aureus, Legionella etc.
 Resolution • Belaynesh was started with Bactrim and steroids • After seven days of treatment she started to show marked clinical improvement but also developed a rash. This was uncomplicated (no fever, blistering, mucous membrane lesions) so she was”treated through”. • She was discharged with: 1) oral Bactrim, 2) appointment for the OPD, and 3) instructions to return if she worsened
Resolution • Belaynesh was started with Bactrim and steroids • After seven days of treatment she started to show marked clinical improvement but also developed a rash. This was uncomplicated (no fever, blistering, mucous membrane lesions) so she was”treated through”. • She was discharged with: 1) oral Bactrim, 2) appointment for the OPD, and 3) instructions to return if she worsened
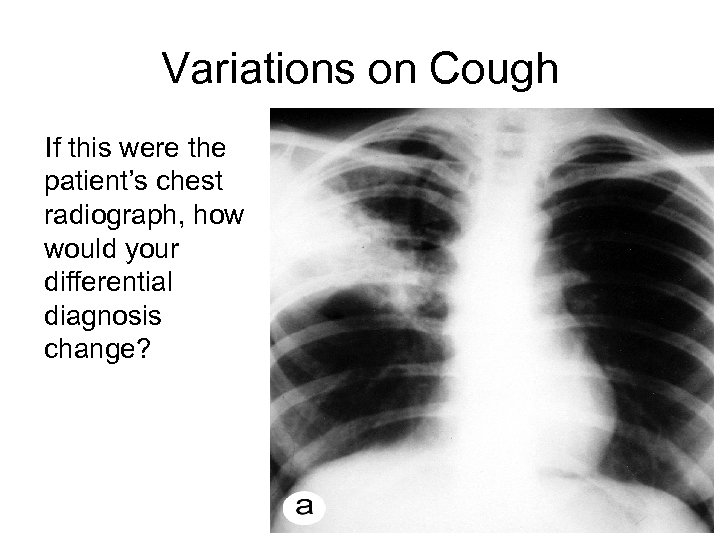 4 What is the diagnosis if this is were his x-ray ? Variations on Cough If this were the patient’s chest radiograph, how would your differential diagnosis change?
4 What is the diagnosis if this is were his x-ray ? Variations on Cough If this were the patient’s chest radiograph, how would your differential diagnosis change?
 Differential Diagnosis • CXR demonstrates lobar pneumonia – Finding is consistent with Pneumococcal pneumonia – HIV also affects the humoral immunity. Thus, HIV patients also develop recurrent bacterial infection – Tb pneumonitis should also be considered
Differential Diagnosis • CXR demonstrates lobar pneumonia – Finding is consistent with Pneumococcal pneumonia – HIV also affects the humoral immunity. Thus, HIV patients also develop recurrent bacterial infection – Tb pneumonitis should also be considered
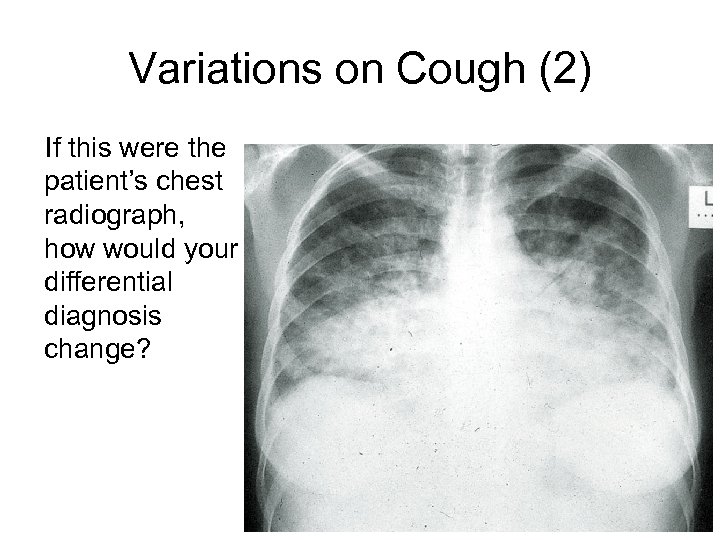 Variations on Cough (2) If this were the patient’s chest radiograph, how would your differential diagnosis change?
Variations on Cough (2) If this were the patient’s chest radiograph, how would your differential diagnosis change?
 Differential Diagnosis • Pulmonary tuberculosis • Fungal pneumonia • Neoplastic – Kaposi sarcoma – Non-Hodgkin's lymphoma
Differential Diagnosis • Pulmonary tuberculosis • Fungal pneumonia • Neoplastic – Kaposi sarcoma – Non-Hodgkin's lymphoma
 Pulmonary Kaposi Sarcoma • Diagnosis – Presence of skin KS would support the X-ray diagnosis, though other pulmonary diseases may occur in setting of cutaneous KS – CT scan may help elucidate • What treatment, if any, would you recommend?
Pulmonary Kaposi Sarcoma • Diagnosis – Presence of skin KS would support the X-ray diagnosis, though other pulmonary diseases may occur in setting of cutaneous KS – CT scan may help elucidate • What treatment, if any, would you recommend?
 Kaposi Sarcoma Treatment Immune Strengthening • HAART – Regression of KS with HAART – Should be first line treatment • Immunotherapy
Kaposi Sarcoma Treatment Immune Strengthening • HAART – Regression of KS with HAART – Should be first line treatment • Immunotherapy
 Kaposi Sarcoma Treatment Chemotherapy • Indicated for rapidly progressive oral, pulmonary or visceral disease – Low dose ABV or BV every 2 weeks – 25 -88% response rate – Myelotoxicity common • Liposomal doxorubicin/daunorubicin – Superior to conventional chemo with less toxicity – Toxicities • Bone marrow • Hand-foot syndrome
Kaposi Sarcoma Treatment Chemotherapy • Indicated for rapidly progressive oral, pulmonary or visceral disease – Low dose ABV or BV every 2 weeks – 25 -88% response rate – Myelotoxicity common • Liposomal doxorubicin/daunorubicin – Superior to conventional chemo with less toxicity – Toxicities • Bone marrow • Hand-foot syndrome
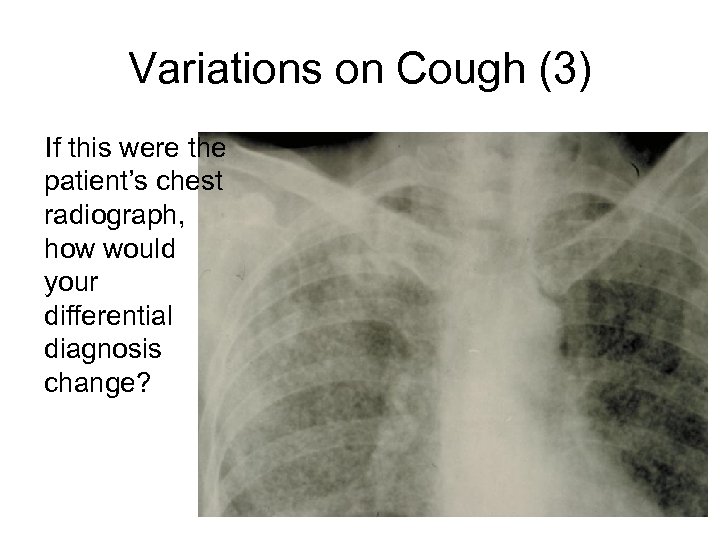 Variations on Cough (3) If this were the patient’s chest radiograph, how would your differential diagnosis change?
Variations on Cough (3) If this were the patient’s chest radiograph, how would your differential diagnosis change?
 Differential Diagnosis • • • Milliary tuberculosis PCP Viral and fungal pneumonia LIP (Lymphoid interstitial pneumonitis) Others
Differential Diagnosis • • • Milliary tuberculosis PCP Viral and fungal pneumonia LIP (Lymphoid interstitial pneumonitis) Others
 Case Three • Amare, a 38 year-old English teacher from Bahir Dar, presents to the general OPD with 10 days history of fever and headache • For the past two days he has vomited any ingested matter • Today he had one seizure with inability to communicate
Case Three • Amare, a 38 year-old English teacher from Bahir Dar, presents to the general OPD with 10 days history of fever and headache • For the past two days he has vomited any ingested matter • Today he had one seizure with inability to communicate
 Additional Information Amare’s sister also reports: • Amare has had slight right-side body weakness and 2 days difficulty with speech • He had pulmonary tuberculosis 2 years ago • He received an HIV positive test result 6 months ago, after he lost considerable weight for no apparent reason. He shared this information with her, but was afraid to seek medical care
Additional Information Amare’s sister also reports: • Amare has had slight right-side body weakness and 2 days difficulty with speech • He had pulmonary tuberculosis 2 years ago • He received an HIV positive test result 6 months ago, after he lost considerable weight for no apparent reason. He shared this information with her, but was afraid to seek medical care
 Discussion • What would you include in your initial differential diagnosis? • Should you do an LP?
Discussion • What would you include in your initial differential diagnosis? • Should you do an LP?
 Additional Findings • Chronically ill appearing • Vital signs – Temp. 38. 8° C – Wt 52 Kg • Facial seborrhoeic dermatitis • Fundoscopy – bilateral papilledema • Right extremity power 3/5, brisk DTR
Additional Findings • Chronically ill appearing • Vital signs – Temp. 38. 8° C – Wt 52 Kg • Facial seborrhoeic dermatitis • Fundoscopy – bilateral papilledema • Right extremity power 3/5, brisk DTR
 Discussion • How does this additional information change your initial differential diagnosis? • What tests would you like to order? • Should you do a LP?
Discussion • How does this additional information change your initial differential diagnosis? • What tests would you like to order? • Should you do a LP?
 Test Results • • WBC 3500/mm 3 TLC 800/mm 3 Hgb 10 g/dl Blood Film negative VDRL non-reactive CXR normal Node FNA pending Serology for toxoplasma and CT of the brain could not be done as these investigations are not available.
Test Results • • WBC 3500/mm 3 TLC 800/mm 3 Hgb 10 g/dl Blood Film negative VDRL non-reactive CXR normal Node FNA pending Serology for toxoplasma and CT of the brain could not be done as these investigations are not available.
 Discussion • How does this additional information change your thinking? • How would your thinking change if you knew the brain CT showed 2 ringenhancing lesions? • How would your thinking change if the toxoplasma serology were negative? • How would your thinking change if the CT scan was negative?
Discussion • How does this additional information change your thinking? • How would your thinking change if you knew the brain CT showed 2 ringenhancing lesions? • How would your thinking change if the toxoplasma serology were negative? • How would your thinking change if the CT scan was negative?
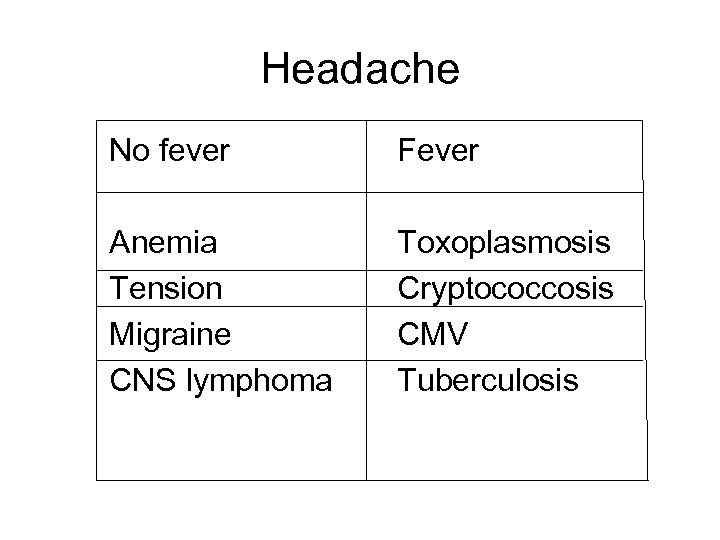 Headache No fever Fever Anemia Tension Migraine CNS lymphoma Toxoplasmosis Cryptococcosis CMV Tuberculosis
Headache No fever Fever Anemia Tension Migraine CNS lymphoma Toxoplasmosis Cryptococcosis CMV Tuberculosis
 (Partial) Differential Diagnosis • • Cerebral toxoplasmosis Cerebral or meningeal TB CNS lymphoma Cryptococcosis
(Partial) Differential Diagnosis • • Cerebral toxoplasmosis Cerebral or meningeal TB CNS lymphoma Cryptococcosis
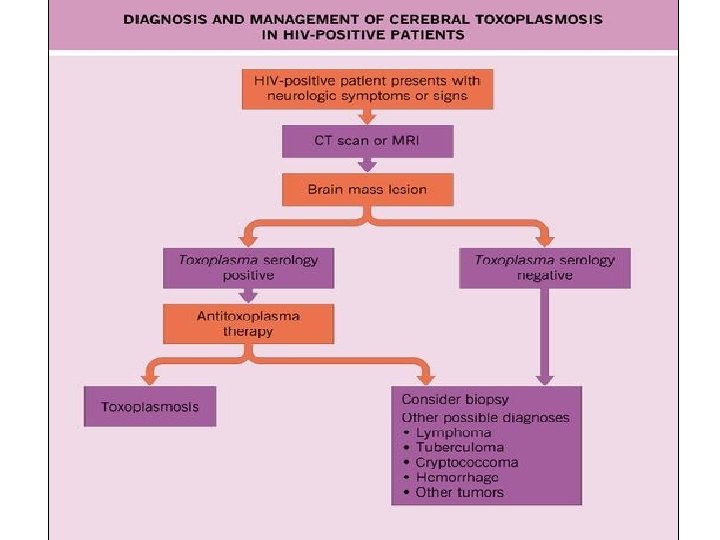
 Toxoplasmosis Facts • Is caused by Toxoplasma gondii • Usual source is inadequately cooked meat and cats • Infection is usually acquired with no symptoms, it stays dormant and it grows when there is loss of cell mediated immune protection. • Seropositivity in Ethiopia reaches 80% • For a AIDS patient with CD 4 <100 mm 3 focal neurologic signs, cerebral toxoplasmosis is the most likely diagnosis
Toxoplasmosis Facts • Is caused by Toxoplasma gondii • Usual source is inadequately cooked meat and cats • Infection is usually acquired with no symptoms, it stays dormant and it grows when there is loss of cell mediated immune protection. • Seropositivity in Ethiopia reaches 80% • For a AIDS patient with CD 4 <100 mm 3 focal neurologic signs, cerebral toxoplasmosis is the most likely diagnosis
 Treatment Considerations • The presentation is so characteristic that many guidelines suggest routine treatment for toxoplasmosis • A lack of response to such therapy (symptoms and MRI changes) within 1 -2 weeks indicates other possible conditions: – Central nervous system lymphoma – Tuberculoma – Cryptococcoma
Treatment Considerations • The presentation is so characteristic that many guidelines suggest routine treatment for toxoplasmosis • A lack of response to such therapy (symptoms and MRI changes) within 1 -2 weeks indicates other possible conditions: – Central nervous system lymphoma – Tuberculoma – Cryptococcoma
 Treatment Response • With empiric treatment for Toxoplasmosis, what should we expect? – Nearly 90% of patients will respond clinically within days of starting therapy – CT and MRI scans show improvement by 14 days following treatment initiation
Treatment Response • With empiric treatment for Toxoplasmosis, what should we expect? – Nearly 90% of patients will respond clinically within days of starting therapy – CT and MRI scans show improvement by 14 days following treatment initiation
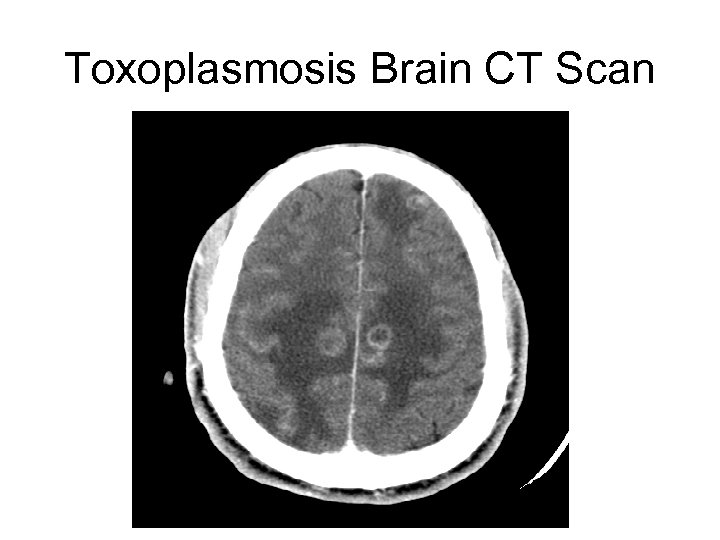 Toxoplasmosis Brain CT Scan
Toxoplasmosis Brain CT Scan
 Toxoplasmosis Treatment • Fansidar: 2 tabs bid x 2 days, then 1 tab qd (Ethiopia) • Alternative: Pyrimethamine 200 mg once, followed by • Pyrimethamine 50 -75 mg/day, plus • Sulfadiazine 1. 0 -1. 5 gm q 6 hrs, plus • Folinic acid 10 -20 mg/d* x 6 wks then half dose v Corticosteroids (dexamethasone 4 mg PO or IV q 6 hrs) used if cerebral edema present, and discontinued as soon as clinically feasible *Folinic acid needed with pyrimethamine, but expense limits use in Ethiopia
Toxoplasmosis Treatment • Fansidar: 2 tabs bid x 2 days, then 1 tab qd (Ethiopia) • Alternative: Pyrimethamine 200 mg once, followed by • Pyrimethamine 50 -75 mg/day, plus • Sulfadiazine 1. 0 -1. 5 gm q 6 hrs, plus • Folinic acid 10 -20 mg/d* x 6 wks then half dose v Corticosteroids (dexamethasone 4 mg PO or IV q 6 hrs) used if cerebral edema present, and discontinued as soon as clinically feasible *Folinic acid needed with pyrimethamine, but expense limits use in Ethiopia
 Additional Treatment Questions • How long will you continue the primary treatment for toxoplasmosis? • Could alternatives to the standard regimens be used? • Which drugs do we commonly use to treat toxoplasmosis in the Ethiopian context? • What about suppressive therapy in this patient?
Additional Treatment Questions • How long will you continue the primary treatment for toxoplasmosis? • Could alternatives to the standard regimens be used? • Which drugs do we commonly use to treat toxoplasmosis in the Ethiopian context? • What about suppressive therapy in this patient?
 Primary Treatment Duration • Duration of Rx is 6 weeks, or 3 weeks after complete resolution of lesions on CT (if repeat CT is available)
Primary Treatment Duration • Duration of Rx is 6 weeks, or 3 weeks after complete resolution of lesions on CT (if repeat CT is available)
 Alternative Regimens • Pyrimethamine and Folinic acid (standard dose) PLUS • Clindamycin 600 mg q 6 hrs, or • Cotrimoxazole (TMP 5 mg + SMX 25 mg)/kg IV or PO bid, or • Atovaquone 1. 5 gm PO bid, or • Pyrimethamine and Leucovorin (standard dose) PLUS Azithromycin 900 -1200 mg PO qd
Alternative Regimens • Pyrimethamine and Folinic acid (standard dose) PLUS • Clindamycin 600 mg q 6 hrs, or • Cotrimoxazole (TMP 5 mg + SMX 25 mg)/kg IV or PO bid, or • Atovaquone 1. 5 gm PO bid, or • Pyrimethamine and Leucovorin (standard dose) PLUS Azithromycin 900 -1200 mg PO qd
 Suppressive Therapy • Fansidar 1 po qd • Pyrimethamine 25 mg + sulfadiazine 500 mg + folinic acid 10 -25 mg PO qd • Cotrimoxazole DS tablet daily – Can be stopped when the CD 4 count remains ≥ 200 for 6 months
Suppressive Therapy • Fansidar 1 po qd • Pyrimethamine 25 mg + sulfadiazine 500 mg + folinic acid 10 -25 mg PO qd • Cotrimoxazole DS tablet daily – Can be stopped when the CD 4 count remains ≥ 200 for 6 months
 Are Therapies Potentially Toxic? YES
Are Therapies Potentially Toxic? YES
 Common Toxicities • Bone marrow suppression, including: – Thrombocytopenia – Leucopenia – Anemia • If signs of folate deficiency develop, reduce the dosage or discontinue the drug • Folinic acid (Leucovorin) 5 to 15 mg daily should be administered with pyrimethamine
Common Toxicities • Bone marrow suppression, including: – Thrombocytopenia – Leucopenia – Anemia • If signs of folate deficiency develop, reduce the dosage or discontinue the drug • Folinic acid (Leucovorin) 5 to 15 mg daily should be administered with pyrimethamine
 Primary Prophylaxis for Toxoplasmosis • When is it indicated? • Positive serology + CD 4 <100 • What is used? TMP-SMX: IDS covers PCP also
Primary Prophylaxis for Toxoplasmosis • When is it indicated? • Positive serology + CD 4 <100 • What is used? TMP-SMX: IDS covers PCP also
 Toxoplasmosis Primary Prophylaxis (2) • Alternative regimen – Dapsone 50 mg/day, plus pyrimethamine 50 mg weekly, plus folinic acid 25 mg weekly (if available) • Primary prophylaxis can be stopped if CD 4 count >200 cells/mm 3 for more than three months following HAART
Toxoplasmosis Primary Prophylaxis (2) • Alternative regimen – Dapsone 50 mg/day, plus pyrimethamine 50 mg weekly, plus folinic acid 25 mg weekly (if available) • Primary prophylaxis can be stopped if CD 4 count >200 cells/mm 3 for more than three months following HAART
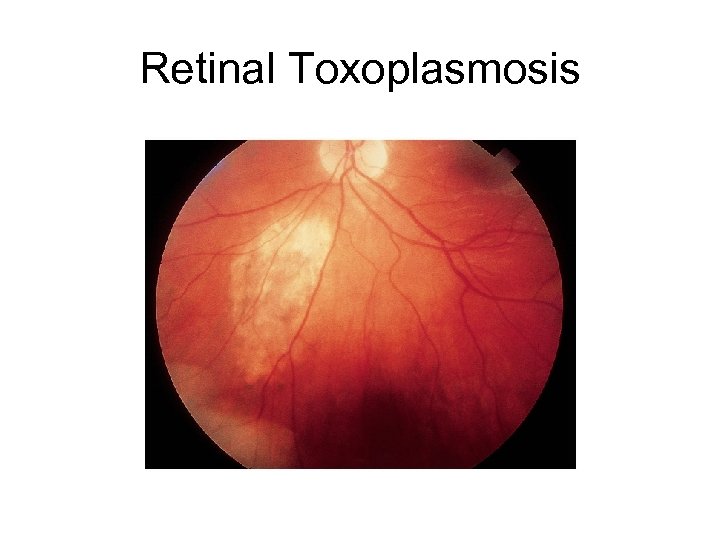 Retinal Toxoplasmosis
Retinal Toxoplasmosis
 Variation on Headache • What if the patient did not have a seizure or focal neurological findings, but still had persistent fever and severe headache? How would this change your thinking and/or your management?
Variation on Headache • What if the patient did not have a seizure or focal neurological findings, but still had persistent fever and severe headache? How would this change your thinking and/or your management?
 Additional Information • No neck stiffness • LP was done: – Opening pressure = 300 mm H 2 O – 30 WBC/mm 3 – Protein 35 gm% – Glucose: normal – India ink stain: pending
Additional Information • No neck stiffness • LP was done: – Opening pressure = 300 mm H 2 O – 30 WBC/mm 3 – Protein 35 gm% – Glucose: normal – India ink stain: pending
 Discussion • How do you interpret these findings? • What is normal OP? • What additional tests will you do?
Discussion • How do you interpret these findings? • What is normal OP? • What additional tests will you do?
 Additional Information • Results from additional tests: – India ink was positive for Cryptococcus – CSF Cryptococcal culture: Positive – Other tests in the CSF: Negative
Additional Information • Results from additional tests: – India ink was positive for Cryptococcus – CSF Cryptococcal culture: Positive – Other tests in the CSF: Negative
 Cryptococcal Meningitis • • Caused by C. neoformans Infection acquired through inhalation Occurs in advanced disease (CD 4<100) Rarely, presents as pneumonitis, or as disseminated disease that includes skin (umbilicated vesicles, like molluscum) • Clinical manifestations may be subtle
Cryptococcal Meningitis • • Caused by C. neoformans Infection acquired through inhalation Occurs in advanced disease (CD 4<100) Rarely, presents as pneumonitis, or as disseminated disease that includes skin (umbilicated vesicles, like molluscum) • Clinical manifestations may be subtle
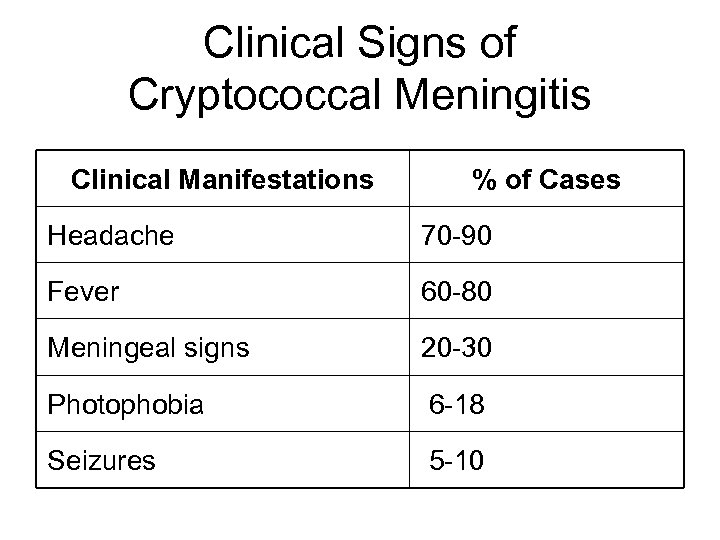 Clinical Signs of Cryptococcal Meningitis Clinical Manifestations % of Cases Headache 70 -90 Fever 60 -80 Meningeal signs 20 -30 Photophobia 6 -18 Seizures 5 -10
Clinical Signs of Cryptococcal Meningitis Clinical Manifestations % of Cases Headache 70 -90 Fever 60 -80 Meningeal signs 20 -30 Photophobia 6 -18 Seizures 5 -10
 Cryptococcal Meningitis Treatment • Fluconazole: 800 mg/d x 2 wks, then 400 mg/d x 8 wks, then 200 mg/d • Amphotericin 0. 7 mg/kg/day IV plus flucytosine 25 mg PO qid for 2 weeks followed by Fluconazole then 400 mg/d x 8 wks then 200 mg/d • Treat until CD 4 >200 x > 3 mo
Cryptococcal Meningitis Treatment • Fluconazole: 800 mg/d x 2 wks, then 400 mg/d x 8 wks, then 200 mg/d • Amphotericin 0. 7 mg/kg/day IV plus flucytosine 25 mg PO qid for 2 weeks followed by Fluconazole then 400 mg/d x 8 wks then 200 mg/d • Treat until CD 4 >200 x > 3 mo
 Case Four • Sara, a 32 year-old accountant, presented with retrosternal pain associated with swallowing of both solid and liquid foods of two weeks duration • She also reports generalized body weakness and weight loss • One month back she developed whitish oral lesions, treated with topical antifungals
Case Four • Sara, a 32 year-old accountant, presented with retrosternal pain associated with swallowing of both solid and liquid foods of two weeks duration • She also reports generalized body weakness and weight loss • One month back she developed whitish oral lesions, treated with topical antifungals
 Discussion • What would you include in your initial differential diagnosis? • What would you expect to find on physical examination?
Discussion • What would you include in your initial differential diagnosis? • What would you expect to find on physical examination?
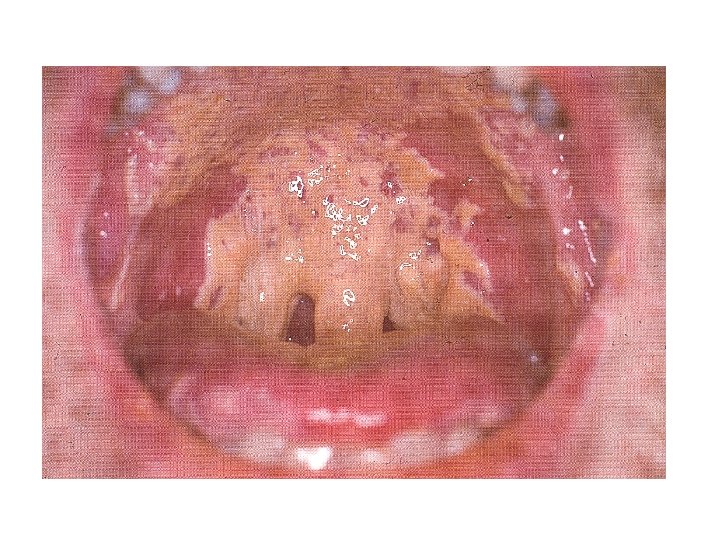
 Physical Examination • She was chronically sick looking • Vital signs were all in normal range • Small, unremarkable posterior cervical lymph nodes • Extensive oral candidiasis • Chest clear • No other pertinent findings
Physical Examination • She was chronically sick looking • Vital signs were all in normal range • Small, unremarkable posterior cervical lymph nodes • Extensive oral candidiasis • Chest clear • No other pertinent findings
 Discussion • How does this additional information affect your differential diagnosis? • How do you investigate this patient?
Discussion • How does this additional information affect your differential diagnosis? • How do you investigate this patient?
 Differential Diagnosis • • Esophageal candidiasis CMV esophagitis HSV esophagitis Kaposi's sarcoma or lymphoma Idiopathic ulcers (aphthous ulcers) Gastroesophageal reflux disease Combination of 2 or more
Differential Diagnosis • • Esophageal candidiasis CMV esophagitis HSV esophagitis Kaposi's sarcoma or lymphoma Idiopathic ulcers (aphthous ulcers) Gastroesophageal reflux disease Combination of 2 or more
 Diagnostic Interventions • KOH from oral lesion • Barium swallow • Endoscopy and tissue biopsy – – – Tissue staining for CMV Fluorescent antibody tests Antigen detection tests (CMV & HSV) Polymerase chain reaction (PCR) Viral culture • None of these are necessary if typical presentation and response to empiric treatment using fluconazole, 100 -200 mg/d
Diagnostic Interventions • KOH from oral lesion • Barium swallow • Endoscopy and tissue biopsy – – – Tissue staining for CMV Fluorescent antibody tests Antigen detection tests (CMV & HSV) Polymerase chain reaction (PCR) Viral culture • None of these are necessary if typical presentation and response to empiric treatment using fluconazole, 100 -200 mg/d
 Therapy • Esophageal candidiasis would be the most likely diagnosis in this patient – Fluconazole 200 mg/day PO (up to 400 mg/day) for 14 -21 days – Alternative treatments • Ketoconazole 200 -400 mg PO qd for 14 -21 days • Itraconazole 200 mg PO qd for 14 -21 days
Therapy • Esophageal candidiasis would be the most likely diagnosis in this patient – Fluconazole 200 mg/day PO (up to 400 mg/day) for 14 -21 days – Alternative treatments • Ketoconazole 200 -400 mg PO qd for 14 -21 days • Itraconazole 200 mg PO qd for 14 -21 days
 Therapy (2) • CMV esophagitis requires systemic ganciclovir – Oral ganciclovir has poor oral absorption so IV treatment is preferred • HSV esophagitis may be treated with acyclovir • Kaposi sarcoma should be treated with HAART and/or otherapies as described previously • Idiopathic ulcers may respond to oral steroids • Reflux is treated as for non-HIV patients
Therapy (2) • CMV esophagitis requires systemic ganciclovir – Oral ganciclovir has poor oral absorption so IV treatment is preferred • HSV esophagitis may be treated with acyclovir • Kaposi sarcoma should be treated with HAART and/or otherapies as described previously • Idiopathic ulcers may respond to oral steroids • Reflux is treated as for non-HIV patients
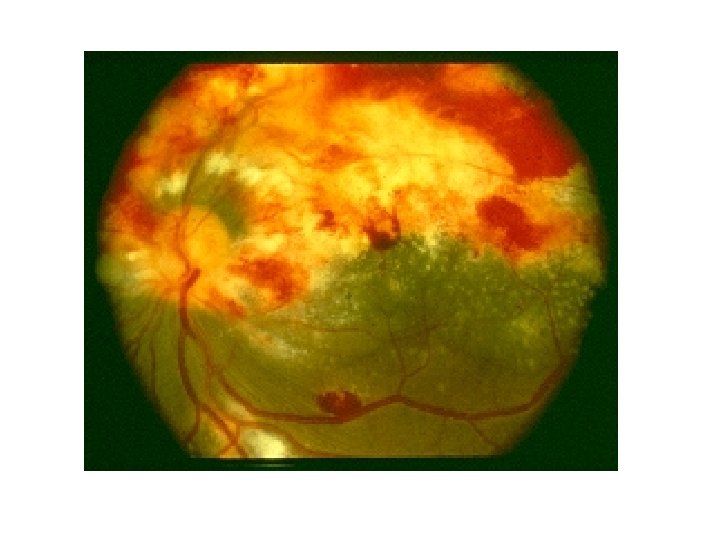
 CMV • Typically does not cause disease until CD 4 <50 • Manifestations in HIV patients: – Retinitis • Unilateral or bilateral visual disturbance • Confirmed by retina exam showing “scrambled eggs & ketchup” (exudates & hemorrhages) – GI disease • Esophagitis • Colitis with watery diarrhea, abdominal pain • Neurologic disorders
CMV • Typically does not cause disease until CD 4 <50 • Manifestations in HIV patients: – Retinitis • Unilateral or bilateral visual disturbance • Confirmed by retina exam showing “scrambled eggs & ketchup” (exudates & hemorrhages) – GI disease • Esophagitis • Colitis with watery diarrhea, abdominal pain • Neurologic disorders
 Case Five • Solomon, a 42 year-old farmer, presents to the OPD with a one month history of watery diarrhea • He reports minimal abdominal pain and bloating, with no tenesmus • He also reports generalized body weakness and significant weight loss
Case Five • Solomon, a 42 year-old farmer, presents to the OPD with a one month history of watery diarrhea • He reports minimal abdominal pain and bloating, with no tenesmus • He also reports generalized body weakness and significant weight loss
 Discussion • What would you include in your initial differential diagnosis?
Discussion • What would you include in your initial differential diagnosis?
 Additional Information • He was recently admitted for this problem and treated with IV fluids and oral antibiotics • Treatment helped a little but the problem recurred • He was screened for HIV and was found positive but he was not started with ARV • Other diagnostic tests were negative • He was treated for tuberculosis five years back
Additional Information • He was recently admitted for this problem and treated with IV fluids and oral antibiotics • Treatment helped a little but the problem recurred • He was screened for HIV and was found positive but he was not started with ARV • Other diagnostic tests were negative • He was treated for tuberculosis five years back
 Physical Examination • He is chronically ill appearing and emaciated • Vital signs – – – PB 90/60 mm Hg PR 110/m RR 18/m T 36 o. C Wt 46 kg • Oral candidiasis • No lymphadenopathy • Normal chest, cardiovascular • Soft abdomen, no masses or organomegaly • Old herpes zoster scar on the trunk • No other abnormal findings in the other systems
Physical Examination • He is chronically ill appearing and emaciated • Vital signs – – – PB 90/60 mm Hg PR 110/m RR 18/m T 36 o. C Wt 46 kg • Oral candidiasis • No lymphadenopathy • Normal chest, cardiovascular • Soft abdomen, no masses or organomegaly • Old herpes zoster scar on the trunk • No other abnormal findings in the other systems
 Discussion • How does this additional information change your initial differential diagnosis? • What laboratory tests would you perform?
Discussion • How does this additional information change your initial differential diagnosis? • What laboratory tests would you perform?
 Differential Diagnosis • Enteropathogenic bacteria – Shigella – Salmonella – E. coli • CMV • Mycobacteria – M. tuberculosis – M. bovis • Parasites – E. histolytica – G. lamblia – Cryptosporidium parvum – Isospora belli – Strongyloides stercoralis, others
Differential Diagnosis • Enteropathogenic bacteria – Shigella – Salmonella – E. coli • CMV • Mycobacteria – M. tuberculosis – M. bovis • Parasites – E. histolytica – G. lamblia – Cryptosporidium parvum – Isospora belli – Strongyloides stercoralis, others
 Laboratory Diagnosis • Direct microscopy of stool, including leukocyte stain • Stool culture • AFB stain • Modified AFB stain • Endoscopy and colon biopsy • Assessment of related effects (CBC, LFT, RFT, electrolytes, blood sugar, U/A, VDRL, CD 4, viral load)
Laboratory Diagnosis • Direct microscopy of stool, including leukocyte stain • Stool culture • AFB stain • Modified AFB stain • Endoscopy and colon biopsy • Assessment of related effects (CBC, LFT, RFT, electrolytes, blood sugar, U/A, VDRL, CD 4, viral load)
 Diagnosis and Treatment of Common Causes of Diarrhea in AIDS Patients
Diagnosis and Treatment of Common Causes of Diarrhea in AIDS Patients
 Case Six • Your colleague working in a nearby health center calls you to ask for advice in managing an HIV patient • The patient has been well, without illness, but now presents concerned about a new skin lesion
Case Six • Your colleague working in a nearby health center calls you to ask for advice in managing an HIV patient • The patient has been well, without illness, but now presents concerned about a new skin lesion
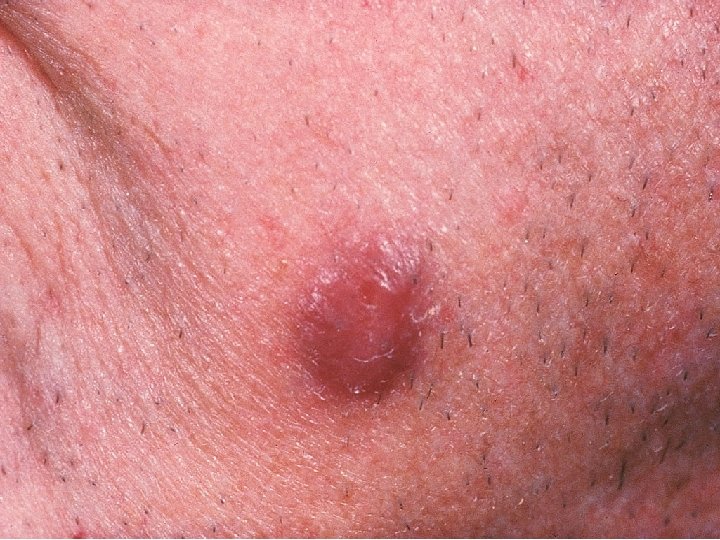 Skin Kaposi
Skin Kaposi
 Additional Information • On physical examination, you also note a lesion in the eye
Additional Information • On physical examination, you also note a lesion in the eye
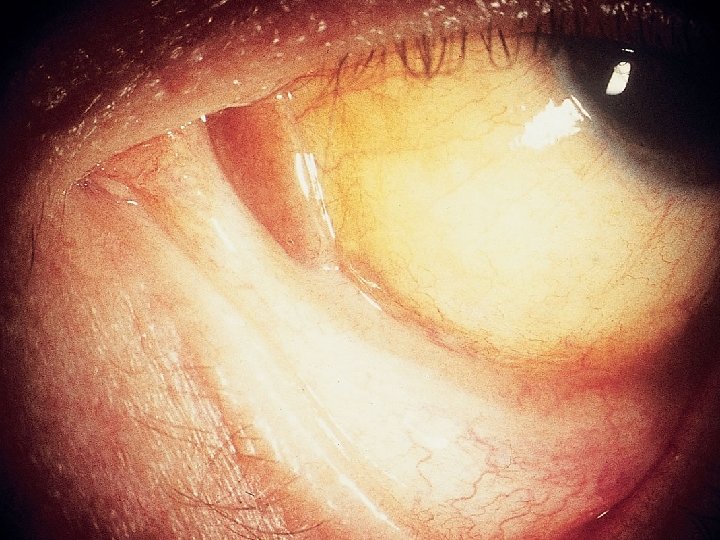 Conjunctival Kaposi
Conjunctival Kaposi
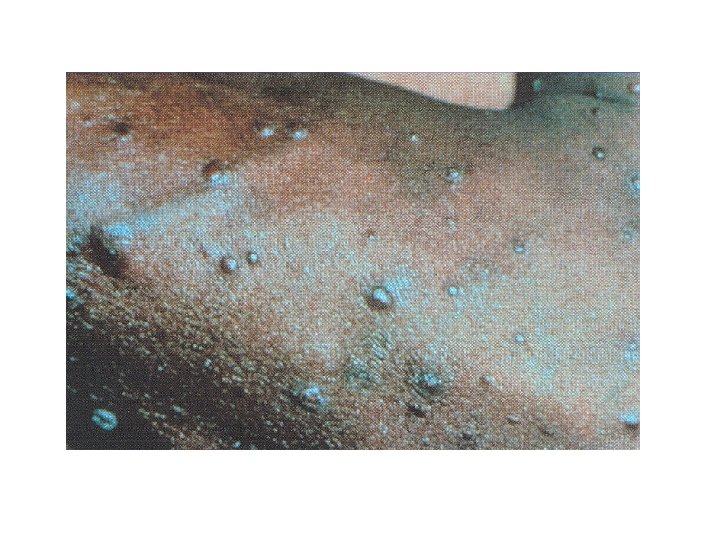
 Kaposi Sarcoma Epidemiology • Was most common cancer at beginning of AIDS epidemic • With use of HAART, KS incidence has declined by 66% between 1989 and 1997, and has likely declined further • Decline in KS may be due to: – HAART-induced HIV down-regulation with immune recovery – Change in sexual practice may have decreased transmission
Kaposi Sarcoma Epidemiology • Was most common cancer at beginning of AIDS epidemic • With use of HAART, KS incidence has declined by 66% between 1989 and 1997, and has likely declined further • Decline in KS may be due to: – HAART-induced HIV down-regulation with immune recovery – Change in sexual practice may have decreased transmission
 KS Etiology and Pathogenesis • Cause is Human Herpes Virus 8 (HHV 8), but treating HHV 8 doesn’t seem to work • Multiple heterosexual contacts is a risk factor for HHV-8 in Africa • Main mechanism of transmission appears to be saliva
KS Etiology and Pathogenesis • Cause is Human Herpes Virus 8 (HHV 8), but treating HHV 8 doesn’t seem to work • Multiple heterosexual contacts is a risk factor for HHV-8 in Africa • Main mechanism of transmission appears to be saliva
 KS Clinical Manifestations • Can affect almost any organ system • Most common sites include: – Skin: Nodular lesions purple or black; can progress to multiple lesions – Oral cavity: flat to nodular lesions – Edema of legs and/or face due to lymphatic obstruction – GI tract: can have KS anywhere in GI tract, which can cause intestinal blockage and bleeding; usually asymptomatic – Pulmonary: can spread along bronchi and vessels; usually asymptomatic – Diagnosis is usually by observing typical lesions
KS Clinical Manifestations • Can affect almost any organ system • Most common sites include: – Skin: Nodular lesions purple or black; can progress to multiple lesions – Oral cavity: flat to nodular lesions – Edema of legs and/or face due to lymphatic obstruction – GI tract: can have KS anywhere in GI tract, which can cause intestinal blockage and bleeding; usually asymptomatic – Pulmonary: can spread along bronchi and vessels; usually asymptomatic – Diagnosis is usually by observing typical lesions
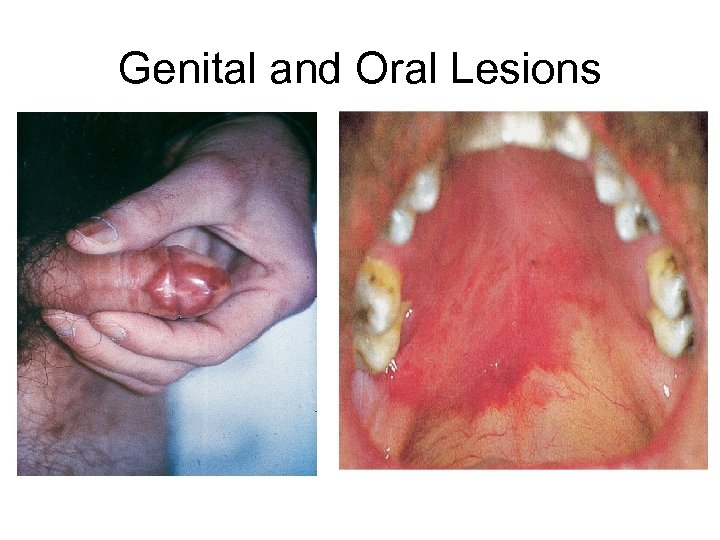 Genital and Oral Lesions
Genital and Oral Lesions
 Kaposi Sarcoma Diagnosis • Skin and oral lesions are typically diagnosed by visual exam • May present with multiple lesions (>25) and • Lung and GI-tract lesions need endoscopy to visualize typical nodular purple lesions on bronchi and gut mucosa; biopsy often falsely negative Resolution of skin lesions with HAART supports a presumptive diagnosis
Kaposi Sarcoma Diagnosis • Skin and oral lesions are typically diagnosed by visual exam • May present with multiple lesions (>25) and • Lung and GI-tract lesions need endoscopy to visualize typical nodular purple lesions on bronchi and gut mucosa; biopsy often falsely negative Resolution of skin lesions with HAART supports a presumptive diagnosis
 Kaposi Sarcoma Treatment • HAART • Local therapy for skin lesions – – – Alitretinoin gel (35 -50% response) Local radiation (20 -70% response) Intralesional vinblastine/vincristine (70 -90% response) Cryotherapy (85% response) Photodynamic therapy Surgical excision • Systemic therapy failure of local therapy or extensive disease
Kaposi Sarcoma Treatment • HAART • Local therapy for skin lesions – – – Alitretinoin gel (35 -50% response) Local radiation (20 -70% response) Intralesional vinblastine/vincristine (70 -90% response) Cryotherapy (85% response) Photodynamic therapy Surgical excision • Systemic therapy failure of local therapy or extensive disease
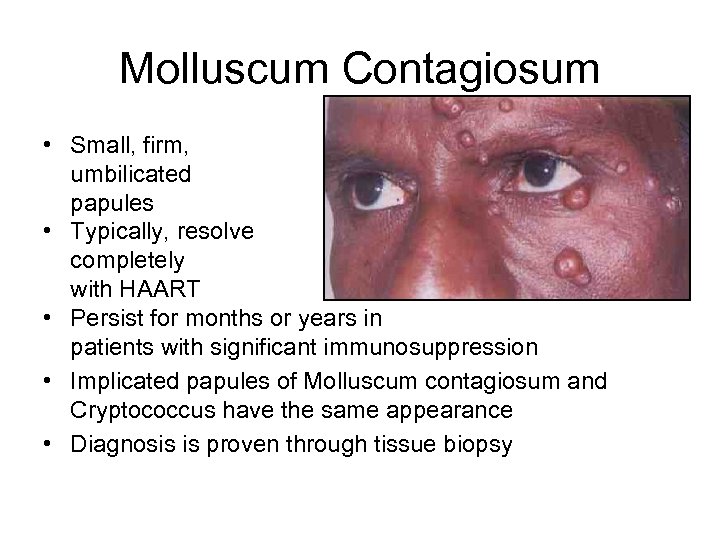 Molluscum Contagiosum • Small, firm, umbilicated papules • Typically, resolve completely with HAART • Persist for months or years in patients with significant immunosuppression • Implicated papules of Molluscum contagiosum and Cryptococcus have the same appearance • Diagnosis is proven through tissue biopsy
Molluscum Contagiosum • Small, firm, umbilicated papules • Typically, resolve completely with HAART • Persist for months or years in patients with significant immunosuppression • Implicated papules of Molluscum contagiosum and Cryptococcus have the same appearance • Diagnosis is proven through tissue biopsy
 Molluscum Contagiosum Treatment • The goal of treatment is to remove the soft center from each lesion. • Various methods are available, including: – Curettage – Chemical destruction with concentrated phenol – Cryotherapy – Electrocautery • Generally lesions disappear with HAART.
Molluscum Contagiosum Treatment • The goal of treatment is to remove the soft center from each lesion. • Various methods are available, including: – Curettage – Chemical destruction with concentrated phenol – Cryotherapy – Electrocautery • Generally lesions disappear with HAART.
 Pruritic Papular Eruption (PPE ) • Multiple, chronic, pruritic, hyperpigmented papules distributed symmetrically on the trunk and extremities • May be one of the earliest clinical manifestations of HIV, despite being a marker of advanced disease • Etiology unclear • Primarily a clinical diagnosis • Eosinophilia and elevated Ig. E are usual findings • Success has been reported with UVB light, with or without oral antipruritics, as well as pentoxifylline
Pruritic Papular Eruption (PPE ) • Multiple, chronic, pruritic, hyperpigmented papules distributed symmetrically on the trunk and extremities • May be one of the earliest clinical manifestations of HIV, despite being a marker of advanced disease • Etiology unclear • Primarily a clinical diagnosis • Eosinophilia and elevated Ig. E are usual findings • Success has been reported with UVB light, with or without oral antipruritics, as well as pentoxifylline
 Pruritic Papular Eruption (PPE )
Pruritic Papular Eruption (PPE )
 Seborrheic Dermatitis • Characterized by reddish scaling eruption that favors the scalp, ears, sternum, face, axillae and crural folds • Occasionally the scales can be yellowish or greasy appearing • Topical treatment with corticosteroid creams are helpful • Systemic steroids are seldom needed • Medicated shampoos can help the dandruff associated with scalp involvement
Seborrheic Dermatitis • Characterized by reddish scaling eruption that favors the scalp, ears, sternum, face, axillae and crural folds • Occasionally the scales can be yellowish or greasy appearing • Topical treatment with corticosteroid creams are helpful • Systemic steroids are seldom needed • Medicated shampoos can help the dandruff associated with scalp involvement
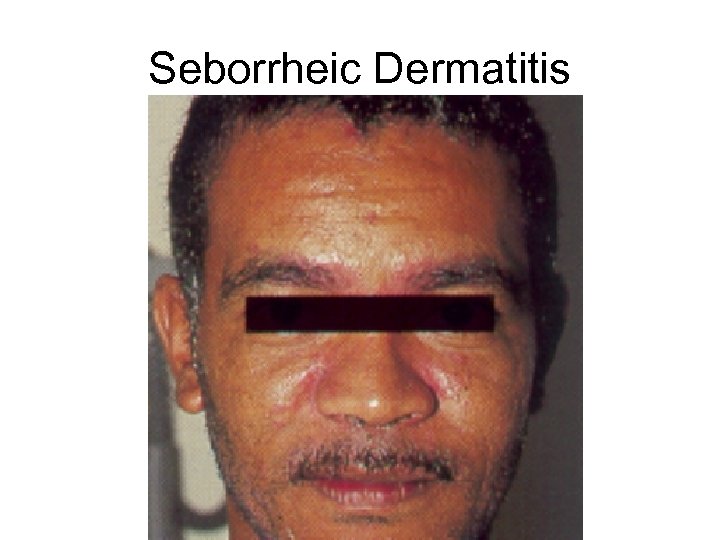 Seborrheic Dermatitis
Seborrheic Dermatitis
 Eosinophilic folliculitis • Characterized by multiple sterile follicular pustules and urticarial papules on the face, trunk, and extremities • Often confused with bacterial folliculitis • Involved follicles show spongiotic changes with eosinophilic and lymphocyte infiltration of the epidermis • Eosinophilia, leukocytosis, and elevated Ig. E levels are often present • Topical steroids are the mainstay of treatment
Eosinophilic folliculitis • Characterized by multiple sterile follicular pustules and urticarial papules on the face, trunk, and extremities • Often confused with bacterial folliculitis • Involved follicles show spongiotic changes with eosinophilic and lymphocyte infiltration of the epidermis • Eosinophilia, leukocytosis, and elevated Ig. E levels are often present • Topical steroids are the mainstay of treatment
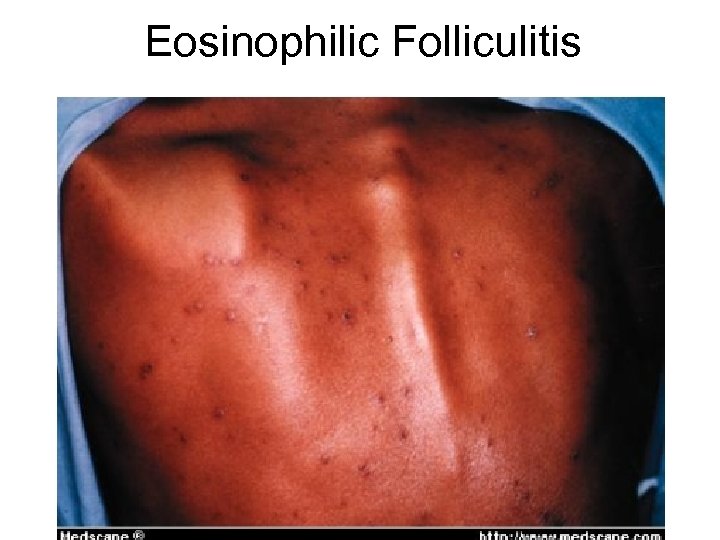 Eosinophilic Folliculitis
Eosinophilic Folliculitis
 Herpes (Varicella) Zoster • Occurs due to reactivation of varicella zoster • In HIV: – Often multi-dermatomal – May be recurrent – Occurs early in disease; first episode usually in patients with CD 4 count>350 cells /mm 3 • If treated with acyclovir within 72 hrs of the first appearance of symptoms (pain, redness, papular rash) the progress/appearance of vesicular lesions may be arrested
Herpes (Varicella) Zoster • Occurs due to reactivation of varicella zoster • In HIV: – Often multi-dermatomal – May be recurrent – Occurs early in disease; first episode usually in patients with CD 4 count>350 cells /mm 3 • If treated with acyclovir within 72 hrs of the first appearance of symptoms (pain, redness, papular rash) the progress/appearance of vesicular lesions may be arrested
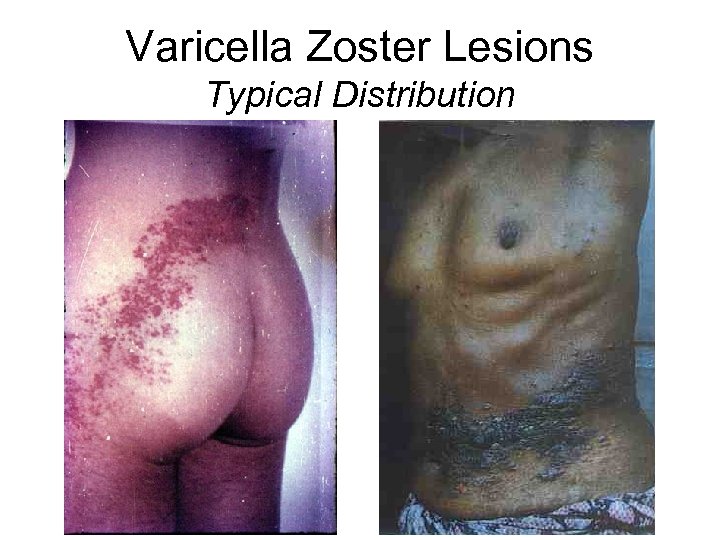 Varicella Zoster Lesions Typical Distribution
Varicella Zoster Lesions Typical Distribution
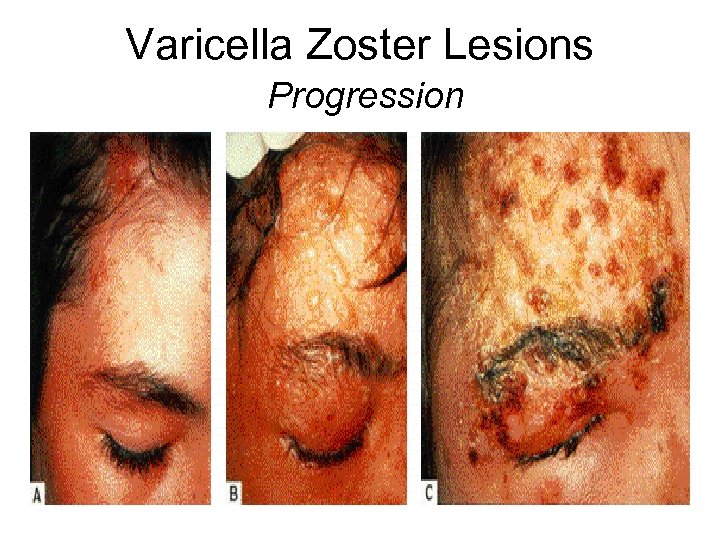 Varicella Zoster Lesions Zoster Sequence Progression
Varicella Zoster Lesions Zoster Sequence Progression
 Varicella Zoster Treatment • Famciclovir 500 mg po tid for 7 -10 days • Valacyclovir 1 gm po tid for 7 -10 days • Acyclovir 800 mg po 5 x/day for 7 -10 days – Superimposed bacterial infection should be treated with antibiotics. • Zoster Ophthalmicus can cause blindness – Treatment - Acyclovir 800 mg po 5 x daily, plus – Topical acyclovir ointment applied 5 x daily with topical midriatics to prevent synechae formation and corneal opacity
Varicella Zoster Treatment • Famciclovir 500 mg po tid for 7 -10 days • Valacyclovir 1 gm po tid for 7 -10 days • Acyclovir 800 mg po 5 x/day for 7 -10 days – Superimposed bacterial infection should be treated with antibiotics. • Zoster Ophthalmicus can cause blindness – Treatment - Acyclovir 800 mg po 5 x daily, plus – Topical acyclovir ointment applied 5 x daily with topical midriatics to prevent synechae formation and corneal opacity
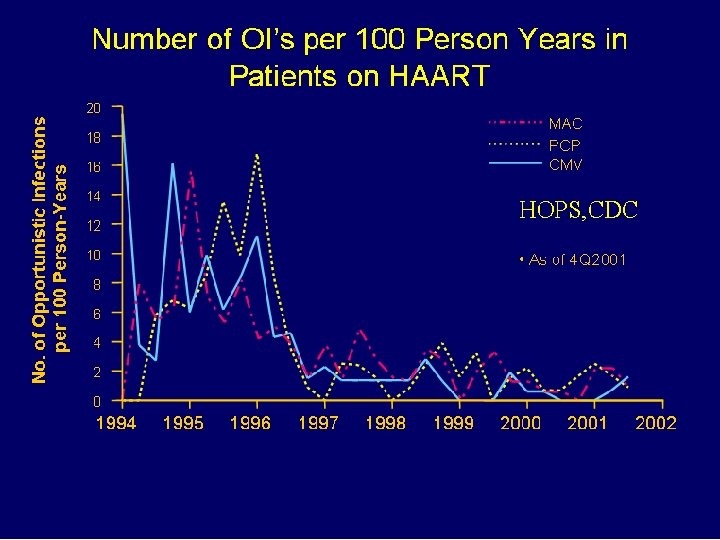 No. OI’s following HAART introduction
No. OI’s following HAART introduction
 Key Points • Infections that develop as a result of damage to the immune system are called opportunistic infections or OIs • Most OIs and complications of HIV develop when the CD 4 count drops below 200/mm 3 • OIs are leading causes of morbidity and mortality in HIV-infected persons
Key Points • Infections that develop as a result of damage to the immune system are called opportunistic infections or OIs • Most OIs and complications of HIV develop when the CD 4 count drops below 200/mm 3 • OIs are leading causes of morbidity and mortality in HIV-infected persons
 Key Points • Common OIs in Ethiopia include TB, PCP, Toxoplasmosis, and Cryptococcus • Many OIs are both preventable and treatable • Standards exist for diagnosing and treating common HIV-related OIs • After appropriate OI treatment, assessment for ART therapy is needed
Key Points • Common OIs in Ethiopia include TB, PCP, Toxoplasmosis, and Cryptococcus • Many OIs are both preventable and treatable • Standards exist for diagnosing and treating common HIV-related OIs • After appropriate OI treatment, assessment for ART therapy is needed


