ec542be86d451392b13055f2c71c4b8a.ppt
- Количество слайдов: 43
 Chronic Disease Management @ Duke Family Medicine Woody Warburton, MD Professor and Division Chief Conference on Practice Improvement: Health Information and Patient Education November 10, 2006 Denver , CO 1
Chronic Disease Management @ Duke Family Medicine Woody Warburton, MD Professor and Division Chief Conference on Practice Improvement: Health Information and Patient Education November 10, 2006 Denver , CO 1
 Outline 1. The Clinical Practice 2. Chronic Disease Management l What are we doing in diabetes? l Group visits – a 15 month analysis 3. Diabetes metrics – how are we doing? 4. Obstacles 5. Conclusions & Next Steps 2
Outline 1. The Clinical Practice 2. Chronic Disease Management l What are we doing in diabetes? l Group visits – a 15 month analysis 3. Diabetes metrics – how are we doing? 4. Obstacles 5. Conclusions & Next Steps 2
 Clinical Practice Profile § § § Family physician faculty (. 2→. 6 FTE) Physician assistants & nurse practitioner (. 2→. 8 FTE) Established patients (3 visits in 3 years) Diabetic patients Hypertension patients Medicare Medicaid Managed Care (Duke Select) Other (Aetna, Cigna, BCBS etc) Provider office visits/year 14 6 13, 400 1, 400 4, 200 12% 15% 42% 31% 38, 000 3
Clinical Practice Profile § § § Family physician faculty (. 2→. 6 FTE) Physician assistants & nurse practitioner (. 2→. 8 FTE) Established patients (3 visits in 3 years) Diabetic patients Hypertension patients Medicare Medicaid Managed Care (Duke Select) Other (Aetna, Cigna, BCBS etc) Provider office visits/year 14 6 13, 400 1, 400 4, 200 12% 15% 42% 31% 38, 000 3
 Learners & Staff l l l l 10 - 15 FM Residents 2 - 4 Medical students/month 2 Pharm D students/mo 1 - 2 PA students/mo 5 RN/ 3 LPN/ 10 MA 1. 2 MSW 1 Pharm D 0. 3 Registered Dietician 4
Learners & Staff l l l l 10 - 15 FM Residents 2 - 4 Medical students/month 2 Pharm D students/mo 1 - 2 PA students/mo 5 RN/ 3 LPN/ 10 MA 1. 2 MSW 1 Pharm D 0. 3 Registered Dietician 4
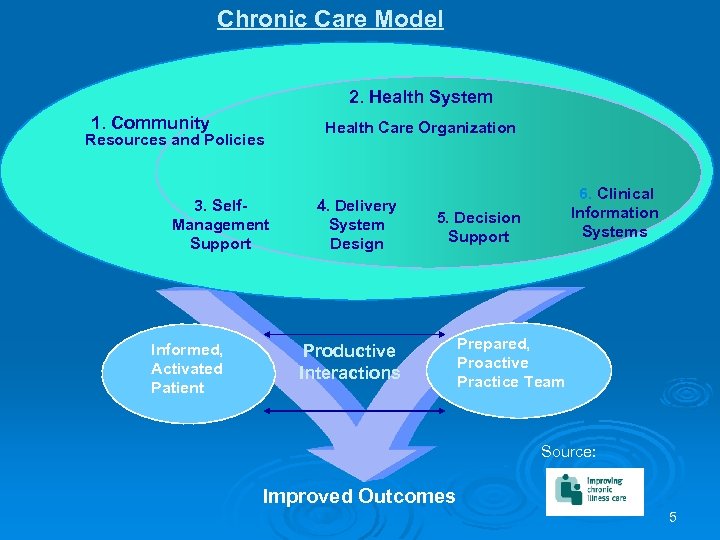 Chronic Care Model 2. Health System 1. Community Resources and Policies 3. Self. Management Support Informed, Activated Patient Health Care Organization 4. Delivery System Design 6. Clinical Information Systems 5. Decision Support Productive Interactions Prepared, Proactive Practice Team Source: Improved Outcomes 5
Chronic Care Model 2. Health System 1. Community Resources and Policies 3. Self. Management Support Informed, Activated Patient Health Care Organization 4. Delivery System Design 6. Clinical Information Systems 5. Decision Support Productive Interactions Prepared, Proactive Practice Team Source: Improved Outcomes 5
 So What Are We Doing? Clinical Information System I. l Registry l DM Reminder Tab l Transcription Template • - CDEMS (Poor Man’s Reminder System) 6
So What Are We Doing? Clinical Information System I. l Registry l DM Reminder Tab l Transcription Template • - CDEMS (Poor Man’s Reminder System) 6
 Diabetic Template 7
Diabetic Template 7
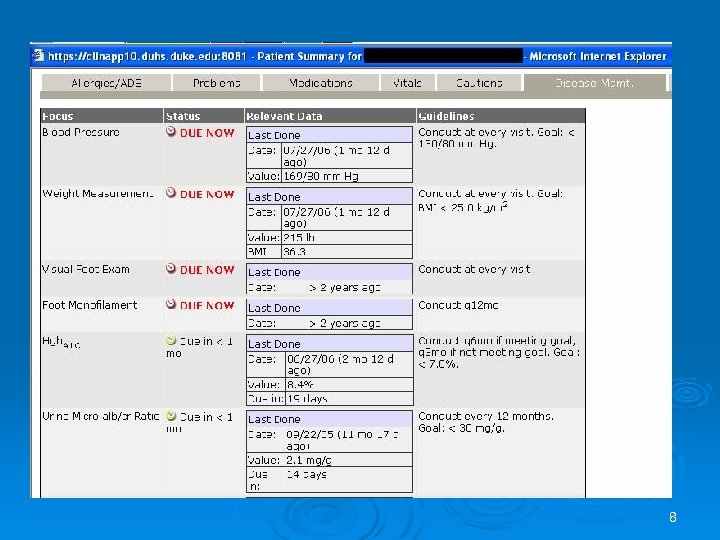 8
8
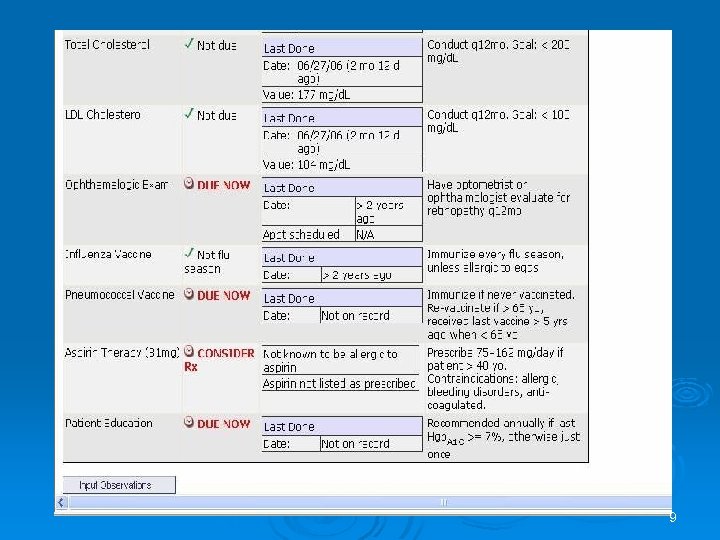 9
9
 II. Delivery System Design v Multidisciplinary Team - Weekly v v v v MD RN Front desk/Call center PA Pharm D MSWCD MSW – Medicaid Case manager – Duke Select (HMO) Work with Community Partners!!!!! 10
II. Delivery System Design v Multidisciplinary Team - Weekly v v v v MD RN Front desk/Call center PA Pharm D MSWCD MSW – Medicaid Case manager – Duke Select (HMO) Work with Community Partners!!!!! 10
 Case Management Conferences Ø MSW / Pharm D/ Clinician (s) Ø Move to continuity teams Ø Use registry to define candidates 11
Case Management Conferences Ø MSW / Pharm D/ Clinician (s) Ø Move to continuity teams Ø Use registry to define candidates 11
 Foot Care Ø PA Trained at (Diabetic) Wound Clinic & Podiatrist Office Ø Acquire equipment – nail cutters & dremel Ø Readily available monofilament for testing Ø Internal marketing 12
Foot Care Ø PA Trained at (Diabetic) Wound Clinic & Podiatrist Office Ø Acquire equipment – nail cutters & dremel Ø Readily available monofilament for testing Ø Internal marketing 12
 Nutrition Ø Popular topic with group visits Ø 1 + year battle to get RD onto staff Ø Billing headaches Ø Still struggle for patient self management 13
Nutrition Ø Popular topic with group visits Ø 1 + year battle to get RD onto staff Ø Billing headaches Ø Still struggle for patient self management 13
 Home Visits Ø Students / Residents Ø 1° with Medicaid population Ø Excellent learning Ø No show problem 14
Home Visits Ø Students / Residents Ø 1° with Medicaid population Ø Excellent learning Ø No show problem 14
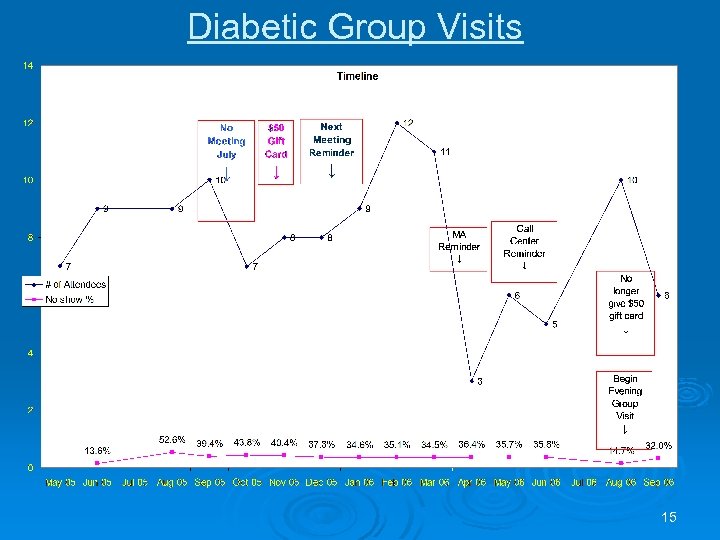 Diabetic Group Visits 15
Diabetic Group Visits 15
 Attendance (July ’ 05 → Sept ’ 06) l 50% arrival rate l 13. 5% cancellation rate l 34. 9% no show rate 16
Attendance (July ’ 05 → Sept ’ 06) l 50% arrival rate l 13. 5% cancellation rate l 34. 9% no show rate 16
 Participants Clinical Metrics 1 group visit only – 48 participants l A 1 c<7% = 27% (13/48) l LDL<100 = 29% (14/48) l BP<130/80 = 33% (16/48) Repeat Group Visits – 25 participants l A 1 c<7% = 48% (12/25) l LDL<100 = 56% (14/25) l BP<130/80 = 48% (12/25) 17
Participants Clinical Metrics 1 group visit only – 48 participants l A 1 c<7% = 27% (13/48) l LDL<100 = 29% (14/48) l BP<130/80 = 33% (16/48) Repeat Group Visits – 25 participants l A 1 c<7% = 48% (12/25) l LDL<100 = 56% (14/25) l BP<130/80 = 48% (12/25) 17
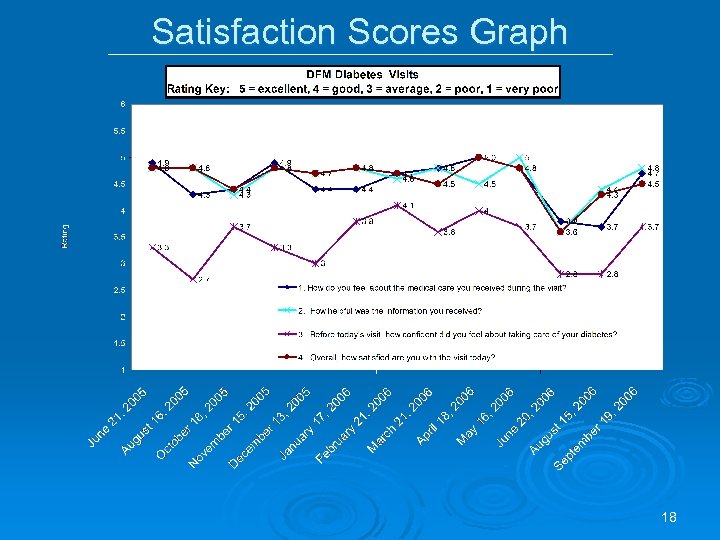 Satisfaction Scores Graph 18
Satisfaction Scores Graph 18
 Time/Energy Analysis l Quality coordinator - 5 hrs/mo l Call Center reminders - 2 hrs/mo l Physician Assistants (2) – 4 hrs/mo l Pharm D – 2 hrs/mo 19
Time/Energy Analysis l Quality coordinator - 5 hrs/mo l Call Center reminders - 2 hrs/mo l Physician Assistants (2) – 4 hrs/mo l Pharm D – 2 hrs/mo 19
 Group Visit: Cost Analysis Cost Per Group Visit Personnel $ 382 Direct cost – Refreshments $ 20 Gift card $ 50 TOTAL $452 Revenue Total charges (99213 & 99214) Total adjustments (per contracts) Total payments Average revenue per Group Visit $9, 557 <$5, 927> $3, 507 $319 20
Group Visit: Cost Analysis Cost Per Group Visit Personnel $ 382 Direct cost – Refreshments $ 20 Gift card $ 50 TOTAL $452 Revenue Total charges (99213 & 99214) Total adjustments (per contracts) Total payments Average revenue per Group Visit $9, 557 <$5, 927> $3, 507 $319 20
 Group Visit: Conclusions 1. Group visits meet patient satisfaction & improve care. 2. Patients feel more comfortable with their disease. 3. May need >1 yr to see clinical benefits. 4. Not cost effective with current model. 5. Unclear if this is a “stepping stone” to new chronic disease care. 6. One of many tools to improve chronic disease management. 21
Group Visit: Conclusions 1. Group visits meet patient satisfaction & improve care. 2. Patients feel more comfortable with their disease. 3. May need >1 yr to see clinical benefits. 4. Not cost effective with current model. 5. Unclear if this is a “stepping stone” to new chronic disease care. 6. One of many tools to improve chronic disease management. 21
 III. Decision Support Ø DM tab – long time coming!!! Ø Endocrinologist on DM team – key buy-in 22
III. Decision Support Ø DM tab – long time coming!!! Ø Endocrinologist on DM team – key buy-in 22
 IV. Self-Management Ø Patient Self Management Support Ø Residents teach faculty about Self Management Ø Staff (RN, MSW, & Pharm D) provide follow-up support 23
IV. Self-Management Ø Patient Self Management Support Ø Residents teach faculty about Self Management Ø Staff (RN, MSW, & Pharm D) provide follow-up support 23
 24
24
 V. Organization of Health Care Ø Mission to” improve health of the community” Ø Focus - 1° on chronic disease – less on preventive & acute care Ø Department chair & division chief leadership Ø QI program metrics 25
V. Organization of Health Care Ø Mission to” improve health of the community” Ø Focus - 1° on chronic disease – less on preventive & acute care Ø Department chair & division chief leadership Ø QI program metrics 25
 Quality Measurement Without an EMR Ø Random sample ~ 100 charts – every 3 - 6 months Ø Resident & student (MS, PA, Pharm D) work force Ø QI masters trained analyst Ø HEDIS/State/ACCC/CMS - standard audit 26
Quality Measurement Without an EMR Ø Random sample ~ 100 charts – every 3 - 6 months Ø Resident & student (MS, PA, Pharm D) work force Ø QI masters trained analyst Ø HEDIS/State/ACCC/CMS - standard audit 26
 Results So Far Ø HEDIS Metrics Ø State Metrics Ø ACCC Metrics Ø Healthy People (2010) 27
Results So Far Ø HEDIS Metrics Ø State Metrics Ø ACCC Metrics Ø Healthy People (2010) 27
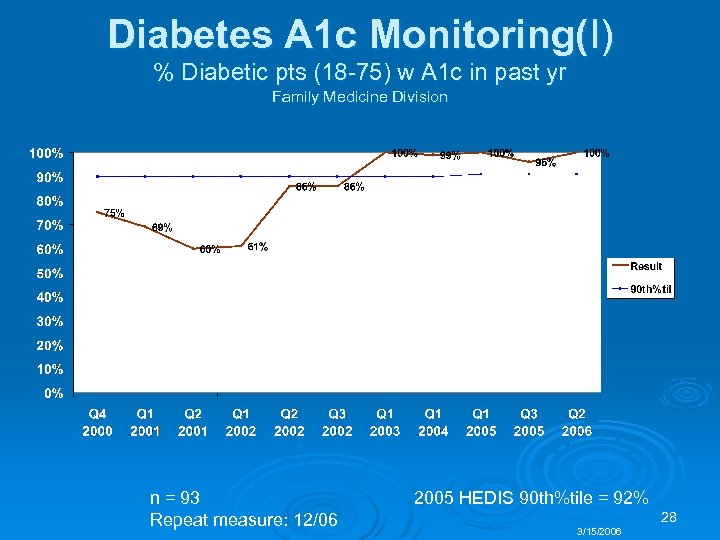 Diabetes A 1 c Monitoring(I) % Diabetic pts (18 -75) w A 1 c in past yr Family Medicine Division n = 93 Repeat measure: 12/06 2005 HEDIS 90 th%tile = 92% 28 3/15/2006
Diabetes A 1 c Monitoring(I) % Diabetic pts (18 -75) w A 1 c in past yr Family Medicine Division n = 93 Repeat measure: 12/06 2005 HEDIS 90 th%tile = 92% 28 3/15/2006
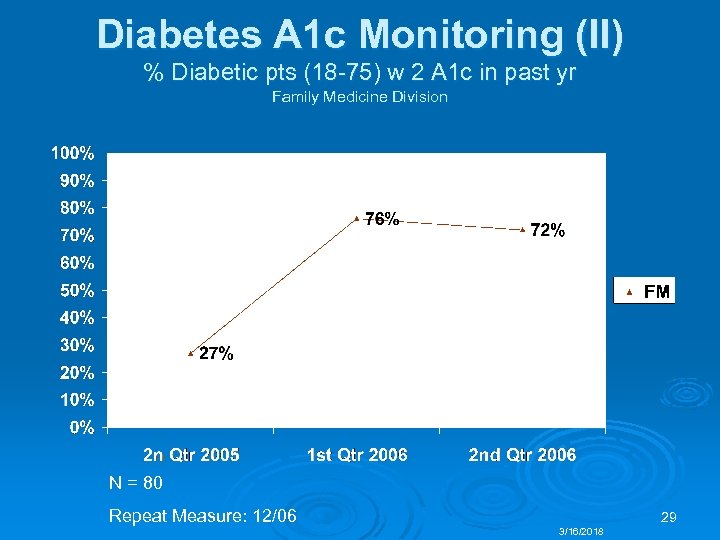 Diabetes A 1 c Monitoring (II) % Diabetic pts (18 -75) w 2 A 1 c in past yr Family Medicine Division N = 80 Repeat Measure: 12/06 29 3/16/2018
Diabetes A 1 c Monitoring (II) % Diabetic pts (18 -75) w 2 A 1 c in past yr Family Medicine Division N = 80 Repeat Measure: 12/06 29 3/16/2018
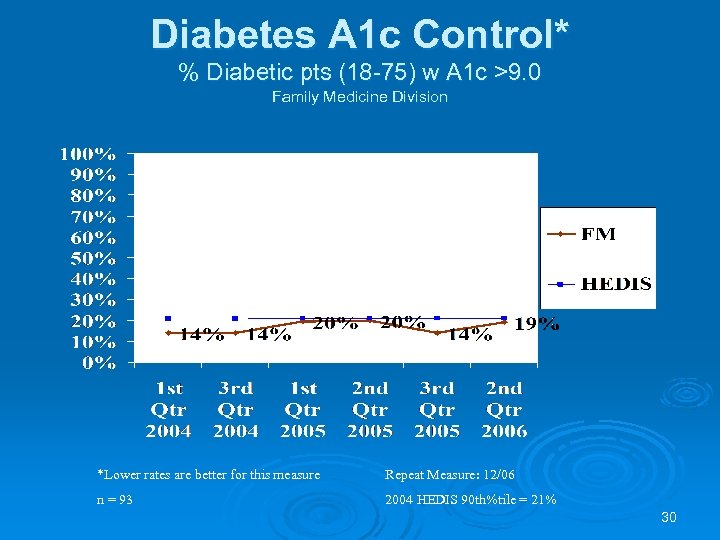 Diabetes A 1 c Control* % Diabetic pts (18 -75) w A 1 c >9. 0 Family Medicine Division *Lower rates are better for this measure Repeat Measure: 12/06 n = 93 2004 HEDIS 90 th%tile = 21% 30
Diabetes A 1 c Control* % Diabetic pts (18 -75) w A 1 c >9. 0 Family Medicine Division *Lower rates are better for this measure Repeat Measure: 12/06 n = 93 2004 HEDIS 90 th%tile = 21% 30
 Diabetes A 1 c Control (II) % Diabetic pts (18 -75) w A 1 c< 7. 0 Department of Community and Family Medicine n = 80 Repeat Measure: 12/07 6/06 31
Diabetes A 1 c Control (II) % Diabetic pts (18 -75) w A 1 c< 7. 0 Department of Community and Family Medicine n = 80 Repeat Measure: 12/07 6/06 31
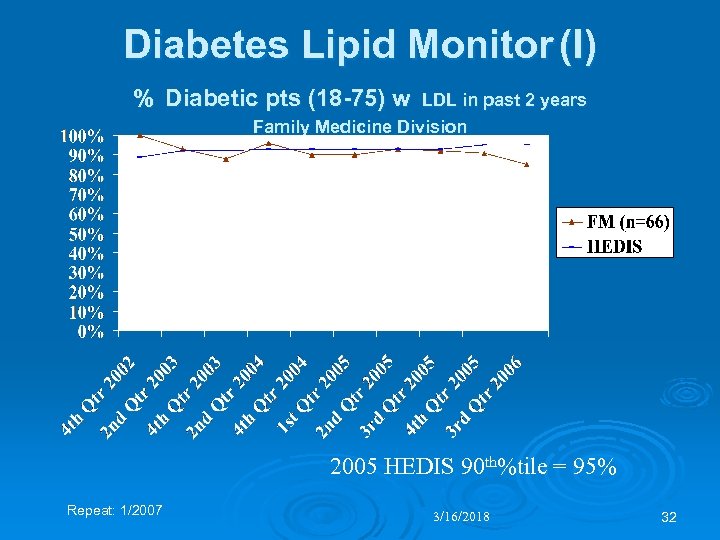 Diabetes Lipid Monitor (I) % Diabetic pts (18 -75) w LDL in past 2 years Family Medicine Division 2005 HEDIS 90 th%tile = 95% Repeat: 1/2007 3/16/2018 32
Diabetes Lipid Monitor (I) % Diabetic pts (18 -75) w LDL in past 2 years Family Medicine Division 2005 HEDIS 90 th%tile = 95% Repeat: 1/2007 3/16/2018 32
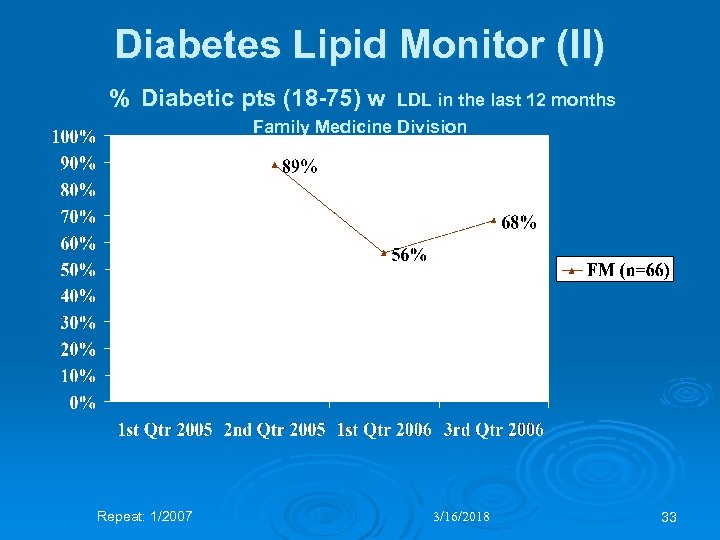 Diabetes Lipid Monitor (II) % Diabetic pts (18 -75) w LDL in the last 12 months Family Medicine Division Repeat: 1/2007 3/16/2018 33
Diabetes Lipid Monitor (II) % Diabetic pts (18 -75) w LDL in the last 12 months Family Medicine Division Repeat: 1/2007 3/16/2018 33
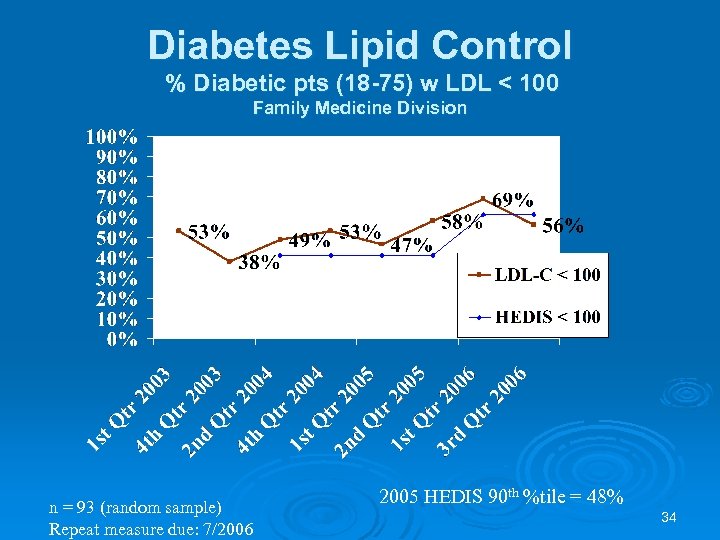 Diabetes Lipid Control % Diabetic pts (18 -75) w LDL < 100 Family Medicine Division n = 93 (random sample) Repeat measure due: 7/2006 2005 HEDIS 90 th %tile = 48% 34
Diabetes Lipid Control % Diabetic pts (18 -75) w LDL < 100 Family Medicine Division n = 93 (random sample) Repeat measure due: 7/2006 2005 HEDIS 90 th %tile = 48% 34
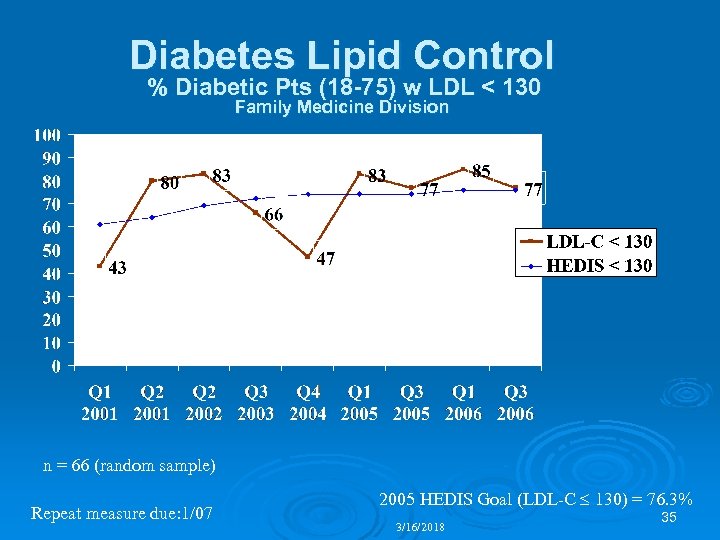 Diabetes Lipid Control % Diabetic Pts (18 -75) w LDL < 130 Family Medicine Division n = 66 (random sample) Repeat measure due: 1/07 2005 HEDIS Goal (LDL-C 130) = 76. 3% 3/16/2018 35
Diabetes Lipid Control % Diabetic Pts (18 -75) w LDL < 130 Family Medicine Division n = 66 (random sample) Repeat measure due: 1/07 2005 HEDIS Goal (LDL-C 130) = 76. 3% 3/16/2018 35
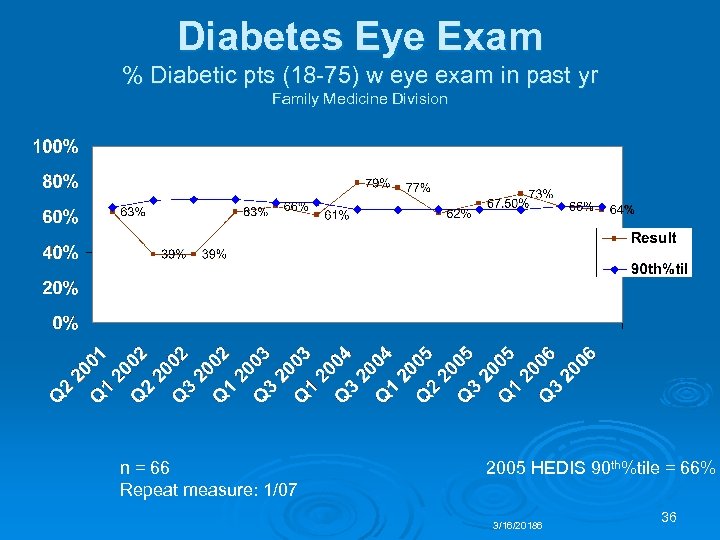 Diabetes Eye Exam % Diabetic pts (18 -75) w eye exam in past yr Family Medicine Division n = 66 Repeat measure: 1/07 2005 HEDIS 90 th%tile = 66% 3/16/20186 36
Diabetes Eye Exam % Diabetic pts (18 -75) w eye exam in past yr Family Medicine Division n = 66 Repeat measure: 1/07 2005 HEDIS 90 th%tile = 66% 3/16/20186 36
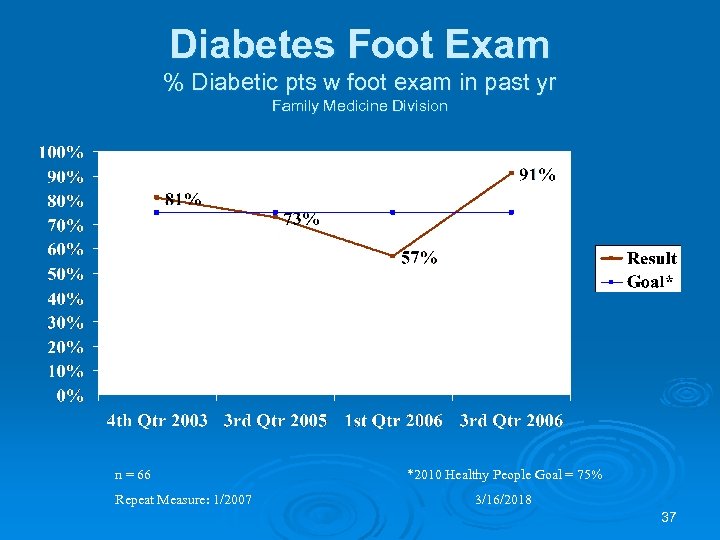 Diabetes Foot Exam % Diabetic pts w foot exam in past yr Family Medicine Division n = 66 Repeat Measure: 1/2007 *2010 Healthy People Goal = 75% 3/16/2018 37
Diabetes Foot Exam % Diabetic pts w foot exam in past yr Family Medicine Division n = 66 Repeat Measure: 1/2007 *2010 Healthy People Goal = 75% 3/16/2018 37
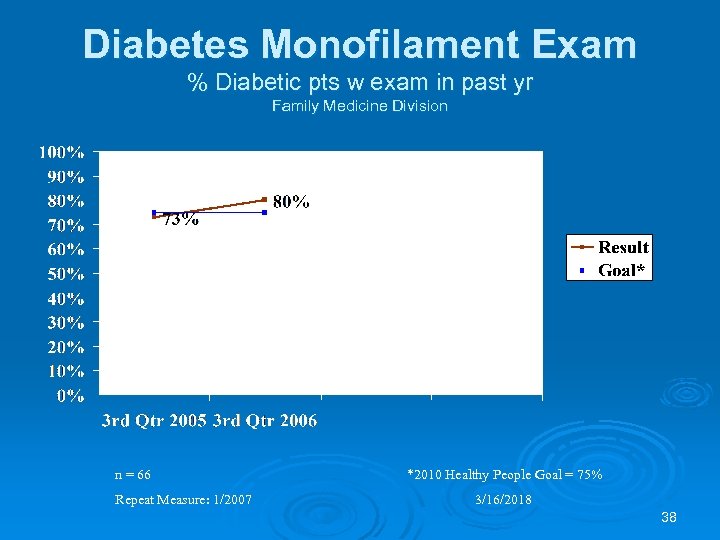 Diabetes Monofilament Exam % Diabetic pts w exam in past yr Family Medicine Division n = 66 Repeat Measure: 1/2007 *2010 Healthy People Goal = 75% 3/16/2018 38
Diabetes Monofilament Exam % Diabetic pts w exam in past yr Family Medicine Division n = 66 Repeat Measure: 1/2007 *2010 Healthy People Goal = 75% 3/16/2018 38
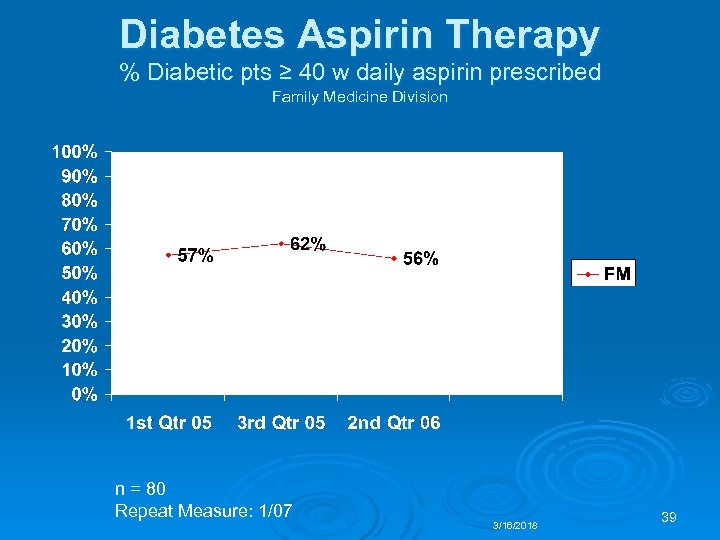 Diabetes Aspirin Therapy % Diabetic pts ≥ 40 w daily aspirin prescribed Family Medicine Division n = 80 Repeat Measure: 1/07 3/16/2018 39
Diabetes Aspirin Therapy % Diabetic pts ≥ 40 w daily aspirin prescribed Family Medicine Division n = 80 Repeat Measure: 1/07 3/16/2018 39
 Learners Integrated Into Model l Clinical Practice Guidelines l QI Audit l Initial meaningful changes in practice to improve care l Attend monthly QI meeting l Resident taught faculty about self-management 40
Learners Integrated Into Model l Clinical Practice Guidelines l QI Audit l Initial meaningful changes in practice to improve care l Attend monthly QI meeting l Resident taught faculty about self-management 40
 Obstacles Ø No extra $ but department priority Ø E-browser/data repository is specialty driven & not CDM focused Ø No true EMR Ø Faculty Ø No shared residency clinical practice data Ø Nursing – old / new school -agree on CPG for the practice -group not solo practice faculty believe in & model different behavior -older MD have problems 41
Obstacles Ø No extra $ but department priority Ø E-browser/data repository is specialty driven & not CDM focused Ø No true EMR Ø Faculty Ø No shared residency clinical practice data Ø Nursing – old / new school -agree on CPG for the practice -group not solo practice faculty believe in & model different behavior -older MD have problems 41
 Obstacles (con’t) Resident issues Ø CDM not sexy Ø CDM not easy -- takes time & energy Ø Not recognize importance of team function & QI work Ø Rotation schedule – difficult to be part of the development 42
Obstacles (con’t) Resident issues Ø CDM not sexy Ø CDM not easy -- takes time & energy Ø Not recognize importance of team function & QI work Ø Rotation schedule – difficult to be part of the development 42
 Conclusions & Next Steps Ø Diabetes is great model to learn elements of CDM Ø QI metrics feed improvements in Diabetes care Ø Behavior change is hard – staff & faculty – patients Ø Focus & spotlight improves care Ø Hypertension & COPD are next!!! 43
Conclusions & Next Steps Ø Diabetes is great model to learn elements of CDM Ø QI metrics feed improvements in Diabetes care Ø Behavior change is hard – staff & faculty – patients Ø Focus & spotlight improves care Ø Hypertension & COPD are next!!! 43


