46b795fbfb7d852f6d546fd5b5dcb139.ppt
- Количество слайдов: 23
 Child Health Evaluation and Research Unit Division of General Pediatrics, University of Michigan Factors Related to the Formation of Smallpox Response Teams in US Hospitals UM Research Team: Alex R. Kemper, MD, MS; Anne E. Cowan, MPH; Matthew M. Davis, MD, MAPP; Emily J. Kennedy, MPH; Sarah J. Clark, MPH; and Gary L. Freed, MD, MPH CDC Collaborator: Pamela L. Y. H. Ching, MS, SD, RD, LD National Immunization Conference May 13, 2004
Child Health Evaluation and Research Unit Division of General Pediatrics, University of Michigan Factors Related to the Formation of Smallpox Response Teams in US Hospitals UM Research Team: Alex R. Kemper, MD, MS; Anne E. Cowan, MPH; Matthew M. Davis, MD, MAPP; Emily J. Kennedy, MPH; Sarah J. Clark, MPH; and Gary L. Freed, MD, MPH CDC Collaborator: Pamela L. Y. H. Ching, MS, SD, RD, LD National Immunization Conference May 13, 2004
 Background • October 2002: ACIP/HICPAC recommended that hospitals vaccinate teams of healthcare workers to prepare for a potential smallpox outbreak • January 2003: Smallpox Pre-Event Vaccination Program (SPVP) implemented at state and local levels with CDC assistance • Hospital participation lower than expected
Background • October 2002: ACIP/HICPAC recommended that hospitals vaccinate teams of healthcare workers to prepare for a potential smallpox outbreak • January 2003: Smallpox Pre-Event Vaccination Program (SPVP) implemented at state and local levels with CDC assistance • Hospital participation lower than expected
 Objectives • Understand factors influencing hospitals’ decisions to participate in the SPVP • Identify factors that would lead nonparticipants to change their decision • Describe policies developed by participating hospitals to implement vaccination program
Objectives • Understand factors influencing hospitals’ decisions to participate in the SPVP • Identify factors that would lead nonparticipants to change their decision • Describe policies developed by participating hospitals to implement vaccination program
 Methods: Hospital Selection • Smallpox preparedness coordinators from 24 states with estimated hospital participation of 25 -75% were contacted by CDC • 9 states provided hospital contact information: CA, KY, ME, MI, MS, MN, UT, VA, and WY • Acute care hospitals chosen to represent variation in size, county, affiliation, and decision to participate in SPVP • 148 hospitals in final sample – Ranged from 5 in MS to 21 in UT
Methods: Hospital Selection • Smallpox preparedness coordinators from 24 states with estimated hospital participation of 25 -75% were contacted by CDC • 9 states provided hospital contact information: CA, KY, ME, MI, MS, MN, UT, VA, and WY • Acute care hospitals chosen to represent variation in size, county, affiliation, and decision to participate in SPVP • 148 hospitals in final sample – Ranged from 5 in MS to 21 in UT
 Methods: Interview Process • Semi-structured telephone interviews were conducted with hospital decision-makers between June-November 2003 • Interview protocol (~20 minutes): – – – Individuals involved in decision Hospital’s ultimate decision Whether specific factors considered Key factor(s) in decision SPVP participants: program implementation SPVP non-participants: factors that would change decision
Methods: Interview Process • Semi-structured telephone interviews were conducted with hospital decision-makers between June-November 2003 • Interview protocol (~20 minutes): – – – Individuals involved in decision Hospital’s ultimate decision Whether specific factors considered Key factor(s) in decision SPVP participants: program implementation SPVP non-participants: factors that would change decision
 Specific Factors Addressed in Interview • Perceived risk of smallpox outbreak • Risks of vaccination – Safety for vaccinees – Exposure of patients/close contacts of employees – Policies for vaccinated employees • Costs to hospital – Compensation for adverse events – Liability – Other costs • Stakeholder influences – Employees – General public – Other outside parties
Specific Factors Addressed in Interview • Perceived risk of smallpox outbreak • Risks of vaccination – Safety for vaccinees – Exposure of patients/close contacts of employees – Policies for vaccinated employees • Costs to hospital – Compensation for adverse events – Liability – Other costs • Stakeholder influences – Employees – General public – Other outside parties
 Results • Decision-makers at 123 of 148 hospitals (83%) were interviewed – Response rates ranged from 60 -94% across states • 88 of 123 hospitals (72%) decided to participate in SPVP – No staff were vaccinated at 22 of these 88 hospitals
Results • Decision-makers at 123 of 148 hospitals (83%) were interviewed – Response rates ranged from 60 -94% across states • 88 of 123 hospitals (72%) decided to participate in SPVP – No staff were vaccinated at 22 of these 88 hospitals
 Factors Considered in Decision Chose to Participate in SPVP (n=88) Chose Not to Participate in SPVP (n=35) Risk of a Smallpox Outbreak 88% (77) 91% (32) Risks of Vaccination 90% (79) 100% (35) Potential for adverse events in vaccinees 82% (72) 97% (34) Exposure of close contacts of vaccinees 63% (55) 80% (28) Need for policies for vaccinated employees 57% (50) 60% (21) Costs to the Hospital 91% (80) 94% (33) Compensation for adverse events 78% (69) 89% (31) Liability 77% (68) 83% (29) Other financial or opportunity costs 28% (25) 26% (10) Stakeholder Influences 72% (63) 74% (26) Employees 38% (33) 37% (13) General public 34% (30) 26% (9) Other outside parties 44% (39) 49% (17) Factor
Factors Considered in Decision Chose to Participate in SPVP (n=88) Chose Not to Participate in SPVP (n=35) Risk of a Smallpox Outbreak 88% (77) 91% (32) Risks of Vaccination 90% (79) 100% (35) Potential for adverse events in vaccinees 82% (72) 97% (34) Exposure of close contacts of vaccinees 63% (55) 80% (28) Need for policies for vaccinated employees 57% (50) 60% (21) Costs to the Hospital 91% (80) 94% (33) Compensation for adverse events 78% (69) 89% (31) Liability 77% (68) 83% (29) Other financial or opportunity costs 28% (25) 26% (10) Stakeholder Influences 72% (63) 74% (26) Employees 38% (33) 37% (13) General public 34% (30) 26% (9) Other outside parties 44% (39) 49% (17) Factor
 Factors Considered in Decision (continued) Risk of Smallpox Outbreak • Hospitals made own assessment of risk of a smallpox outbreak • Many also assessed their perceived risk of exposure – e. g. , proximity to urban areas, likelihood of receiving case as transfer patient • Almost all felt the risk of outbreak was low – “The risk of an outbreak didn’t seem likely, but if it were to happen, it would be devastating and we felt we needed to be prepared ahead of time. ”
Factors Considered in Decision (continued) Risk of Smallpox Outbreak • Hospitals made own assessment of risk of a smallpox outbreak • Many also assessed their perceived risk of exposure – e. g. , proximity to urban areas, likelihood of receiving case as transfer patient • Almost all felt the risk of outbreak was low – “The risk of an outbreak didn’t seem likely, but if it were to happen, it would be devastating and we felt we needed to be prepared ahead of time. ”
 Factors Considered in Decision (continued) Risks of Vaccination • Participating hospitals found ways to address safety concerns – e. g. , employee education, screening protocols • Those that decided not to participate had unresolved concerns about vaccine safety or determined that risks too great • Many hospitals struggled over need to develop employee policies to protect contacts of vaccinees
Factors Considered in Decision (continued) Risks of Vaccination • Participating hospitals found ways to address safety concerns – e. g. , employee education, screening protocols • Those that decided not to participate had unresolved concerns about vaccine safety or determined that risks too great • Many hospitals struggled over need to develop employee policies to protect contacts of vaccinees
 Factors Considered in Decision (continued) Costs to Hospital • Regardless of decision, liability and workers’ compensation major concerns – federal legislation did not necessarily alleviate concerns • Workers’ compensation addressed in varying ways • A few smaller hospitals concerned with cost of lost work time (e. g. , nursing shortages)
Factors Considered in Decision (continued) Costs to Hospital • Regardless of decision, liability and workers’ compensation major concerns – federal legislation did not necessarily alleviate concerns • Workers’ compensation addressed in varying ways • A few smaller hospitals concerned with cost of lost work time (e. g. , nursing shortages)
 Factors Considered in Decision (continued) Stakeholder Influences • Employees not a significant influence – though unions very influential in some cases • Public opinion not a major consideration – balance between positive view of being prepared with stigma of “smallpox hospital” label • Main outside stakeholders: local and state health departments, federal government, and other hospitals within community or corporate network
Factors Considered in Decision (continued) Stakeholder Influences • Employees not a significant influence – though unions very influential in some cases • Public opinion not a major consideration – balance between positive view of being prepared with stigma of “smallpox hospital” label • Main outside stakeholders: local and state health departments, federal government, and other hospitals within community or corporate network
 Factors Considered in Decision (continued) Stakeholder Influences (continued) • Influence of state and local public health officials overwhelmingly positive – “Local public health officials worked along side us and we developed a better relationship regarding the entire disaster planning program” • In a few cases, influence of public health officials was negative – “The main reason we ended up not participating was due to the lack of preparedness and technical support from the local health department. ”
Factors Considered in Decision (continued) Stakeholder Influences (continued) • Influence of state and local public health officials overwhelmingly positive – “Local public health officials worked along side us and we developed a better relationship regarding the entire disaster planning program” • In a few cases, influence of public health officials was negative – “The main reason we ended up not participating was due to the lack of preparedness and technical support from the local health department. ”
 Key Factors
Key Factors
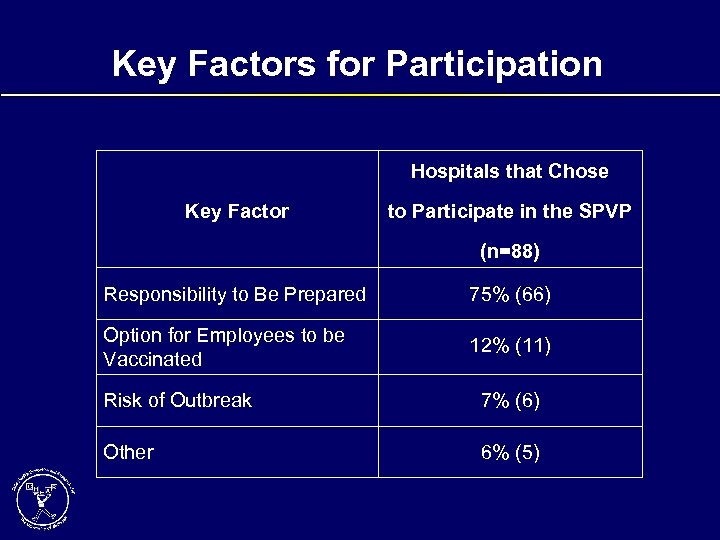 Key Factors for Participation Hospitals that Chose Key Factor to Participate in the SPVP (n=88) Responsibility to Be Prepared 75% (66) Option for Employees to be Vaccinated 12% (11) Risk of Outbreak 7% (6) Other 6% (5)
Key Factors for Participation Hospitals that Chose Key Factor to Participate in the SPVP (n=88) Responsibility to Be Prepared 75% (66) Option for Employees to be Vaccinated 12% (11) Risk of Outbreak 7% (6) Other 6% (5)
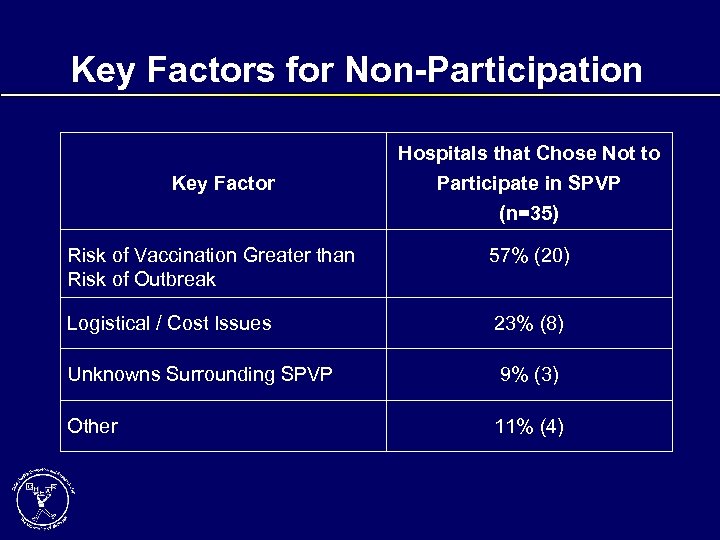 Key Factors for Non-Participation Key Factor Hospitals that Chose Not to Participate in SPVP (n=35) Risk of Vaccination Greater than Risk of Outbreak 57% (20) Logistical / Cost Issues 23% (8) Unknowns Surrounding SPVP 9% (3) Other 11% (4)
Key Factors for Non-Participation Key Factor Hospitals that Chose Not to Participate in SPVP (n=35) Risk of Vaccination Greater than Risk of Outbreak 57% (20) Logistical / Cost Issues 23% (8) Unknowns Surrounding SPVP 9% (3) Other 11% (4)
 Factors That Would Change Non-Participants’ Decision • Outbreak of smallpox somewhere in world most commonly cited • Other factors included: – more adequate compensation – comprehensive information on safety of vaccine – more/better information risk of outbreak
Factors That Would Change Non-Participants’ Decision • Outbreak of smallpox somewhere in world most commonly cited • Other factors included: – more adequate compensation – comprehensive information on safety of vaccine – more/better information risk of outbreak
 Program Participants: Recruitment Strategies • Healthcare worker participation voluntary in all cases • About 50% of hospitals offered vaccination to all employees • Others offered vaccination only to certain personnel, with wide variability across hospitals: – “We concentrated on ED staff due to their high skill level. We also tried to get volunteers from Infectious Disease, Dermatology, and Psychiatry. ” – “Vaccine was offered only to patient care providers (RNs, MDs, ED staff), security officers, and infection control. ” – “Vaccine was offered to everyone except personnel in obstetrics and oncology. ”
Program Participants: Recruitment Strategies • Healthcare worker participation voluntary in all cases • About 50% of hospitals offered vaccination to all employees • Others offered vaccination only to certain personnel, with wide variability across hospitals: – “We concentrated on ED staff due to their high skill level. We also tried to get volunteers from Infectious Disease, Dermatology, and Psychiatry. ” – “Vaccine was offered only to patient care providers (RNs, MDs, ED staff), security officers, and infection control. ” – “Vaccine was offered to everyone except personnel in obstetrics and oncology. ”
 Program Participants: Recruitment Strategies (continued) • Given occupational mix of vaccinees, few hospitals developed specific smallpox response teams – At the vast majority of hospitals, only nurses or physicians were vaccinated – Ancillary staff (e. g. , housekeeping, security), laboratory personnel, respiratory therapists, and radiology technicians were rarely vaccinated
Program Participants: Recruitment Strategies (continued) • Given occupational mix of vaccinees, few hospitals developed specific smallpox response teams – At the vast majority of hospitals, only nurses or physicians were vaccinated – Ancillary staff (e. g. , housekeeping, security), laboratory personnel, respiratory therapists, and radiology technicians were rarely vaccinated
 Program Participants: Site Care • Almost all hospitals developed a policy for care of the vaccination site – Most designated staff to perform site checks, usually an employee health or infection control nurse – Several hospitals allowed vaccinated staff to check their sites themselves • Most adhered to recommendation that site checks be conducted daily
Program Participants: Site Care • Almost all hospitals developed a policy for care of the vaccination site – Most designated staff to perform site checks, usually an employee health or infection control nurse – Several hospitals allowed vaccinated staff to check their sites themselves • Most adhered to recommendation that site checks be conducted daily
 Program Participants: Policies for Vaccinated Staff • Some hospitals went above and beyond guidelines with respect to employee leave / reassignment policies – One hospital furloughed vaccinees (3 -day, paid) – Several hospitals reassigned employees, though specific policies varied • Some hospitals offered paid leave in the event of an adverse reaction to vaccination
Program Participants: Policies for Vaccinated Staff • Some hospitals went above and beyond guidelines with respect to employee leave / reassignment policies – One hospital furloughed vaccinees (3 -day, paid) – Several hospitals reassigned employees, though specific policies varied • Some hospitals offered paid leave in the event of an adverse reaction to vaccination
 Discussion • Hospitals considered many complex issues in (1) deciding whether to participate in SPVP and (2) implementing vaccination program – available information not always complete/consistent – variation across hospitals even within same community • State/local public health played key role in addressing–or failing to address–uncertainty
Discussion • Hospitals considered many complex issues in (1) deciding whether to participate in SPVP and (2) implementing vaccination program – available information not always complete/consistent – variation across hospitals even within same community • State/local public health played key role in addressing–or failing to address–uncertainty
 Discussion (continued) • Future smallpox preparedness efforts can benefit from: – consistent messages conveyed across all levels of public health – a more collaborative approach between local public health officials and individual hospitals – buy-in from national level stakeholders (e. g. , American Hospital Association)
Discussion (continued) • Future smallpox preparedness efforts can benefit from: – consistent messages conveyed across all levels of public health – a more collaborative approach between local public health officials and individual hospitals – buy-in from national level stakeholders (e. g. , American Hospital Association)


