9774ace1d54e17903c87e2e7e81f7812.ppt
- Количество слайдов: 41
 Challenges in Addressing the Needs of Toronto’s Homeless in Death and Dying: A Qualitative Study Yonah Krakowsky MD University of Toronto, Canada Working Group on Homelessness and Palliative Care Supervisor: Dr. Holly Knowles
Challenges in Addressing the Needs of Toronto’s Homeless in Death and Dying: A Qualitative Study Yonah Krakowsky MD University of Toronto, Canada Working Group on Homelessness and Palliative Care Supervisor: Dr. Holly Knowles
 Overview • • • Cases Background Agency Experience Research Question Methodology Results Conclusions Recommendations Acknowledgements
Overview • • • Cases Background Agency Experience Research Question Methodology Results Conclusions Recommendations Acknowledgements
 “There is Such Thing as a Good Death”
“There is Such Thing as a Good Death”
 Todd • 54 year old male • 14 years on street, frequented Scott Mission and various shelters • Alcoholic with Liver Disease • Found unconscious on Street December 8 • Picked up, admitted to SMH, died alone December 10
Todd • 54 year old male • 14 years on street, frequented Scott Mission and various shelters • Alcoholic with Liver Disease • Found unconscious on Street December 8 • Picked up, admitted to SMH, died alone December 10
 Paul • 66 year old male, Hep C, IDU user, • 19 years on the street • Followed by nurse he was familiar with • Developed Pneumonia in November, admitted to SMH transferred to palliative care service with the help of nurse • Died in December surrounded by friends, possessions and minister
Paul • 66 year old male, Hep C, IDU user, • 19 years on the street • Followed by nurse he was familiar with • Developed Pneumonia in November, admitted to SMH transferred to palliative care service with the help of nurse • Died in December surrounded by friends, possessions and minister
 Population • 5, 052 Homeless People in Toronto • 29 times more like to have Hep C • 5 times more like to have Heart Disease • 30% suffer from serious depression Homeless people have significantly less interaction with the health care community and therefore a greatly restricted window in which to attain palliative services
Population • 5, 052 Homeless People in Toronto • 29 times more like to have Hep C • 5 times more like to have Heart Disease • 30% suffer from serious depression Homeless people have significantly less interaction with the health care community and therefore a greatly restricted window in which to attain palliative services
 Population • Many homeless people are found dead on the street • Many are rushed to emergency and die soon after • Both cases exclude possibility of meaningful palliative care
Population • Many homeless people are found dead on the street • Many are rushed to emergency and die soon after • Both cases exclude possibility of meaningful palliative care
 Medical Issue: Palliative Care Palliative care is a specialized form of health care directed at maximizing quality of life in the terminally ill and helping patients and their families and friends deal with death.
Medical Issue: Palliative Care Palliative care is a specialized form of health care directed at maximizing quality of life in the terminally ill and helping patients and their families and friends deal with death.
 Palliative Care. Physical Emotional Social Spiritual Psychological
Palliative Care. Physical Emotional Social Spiritual Psychological
 Palliative Resources Available to Toronto’s Homeless • St. Michael’s Hospital • Perram House and other Palliative Care Homes in the community • Seaton House and other Toronto Shelters
Palliative Resources Available to Toronto’s Homeless • St. Michael’s Hospital • Perram House and other Palliative Care Homes in the community • Seaton House and other Toronto Shelters
 Agency: Working Group on Homelessness and Palliative Care • Mission is to improve the provision of palliative care services to homeless individuals, through advocacy, education/research and advancing services. • Collection of nurses, physicians, social workers, administrators from different shelters/programs • Meet monthly to discuss issues, initiate change and follow progress in achieving goals • Support Network: St. Felix, 410 Sherborne, Street Health
Agency: Working Group on Homelessness and Palliative Care • Mission is to improve the provision of palliative care services to homeless individuals, through advocacy, education/research and advancing services. • Collection of nurses, physicians, social workers, administrators from different shelters/programs • Meet monthly to discuss issues, initiate change and follow progress in achieving goals • Support Network: St. Felix, 410 Sherborne, Street Health
 Experience • Spent Tuesdays at Seaton House, Scott Mission, PARC and Street Health. • Spent time volunteering in clinics with medical residents (Seaton House), interacting with street nurses, and participating in shelter-based programs • Held informal and formal (for the study) interviews with support staff and clients.
Experience • Spent Tuesdays at Seaton House, Scott Mission, PARC and Street Health. • Spent time volunteering in clinics with medical residents (Seaton House), interacting with street nurses, and participating in shelter-based programs • Held informal and formal (for the study) interviews with support staff and clients.
 Research Question How can Toronto’s palliative care resources be improved to increase access and better serve the city’s homeless?
Research Question How can Toronto’s palliative care resources be improved to increase access and better serve the city’s homeless?
 Determinant of Heath Access to Palliative Care
Determinant of Heath Access to Palliative Care
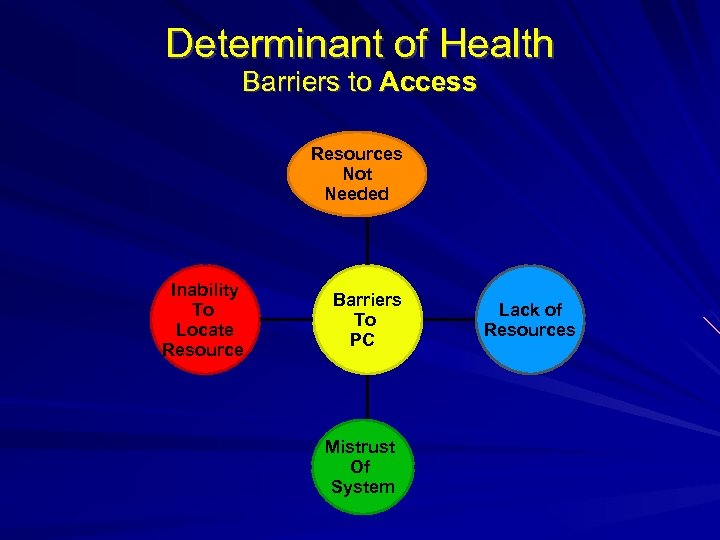 Determinant of Health Barriers to Access Resources Not Needed Inability To Locate Resource Barriers To PC Mistrust Of System Lack of Resources
Determinant of Health Barriers to Access Resources Not Needed Inability To Locate Resource Barriers To PC Mistrust Of System Lack of Resources
 Methodology • 6 semi-structured qualitative interviews • Homeless care providers from Toronto • • Shelters All had at least 8 years experience All had some homeless palliative experience 45 min- 1 hour interview Audio recorded, transcribed analyzed using thematic analysis
Methodology • 6 semi-structured qualitative interviews • Homeless care providers from Toronto • • Shelters All had at least 8 years experience All had some homeless palliative experience 45 min- 1 hour interview Audio recorded, transcribed analyzed using thematic analysis
 Interview Structure • Individual’s experiences • Successes in providing palliative care • Barriers to access • Ways of improving access and services
Interview Structure • Individual’s experiences • Successes in providing palliative care • Barriers to access • Ways of improving access and services
 Thematic Analysis 5. Produce Report 4. Define Themes 1. Review Data 2. Search for Themes 3. Review Themes
Thematic Analysis 5. Produce Report 4. Define Themes 1. Review Data 2. Search for Themes 3. Review Themes
 Results Emergence of Themes 1. Negative Experiences with the Health Care System 2. Training of Palliative Care Staff 3. Dying the Way One Lives 4. Diversity in Delivery 5. Role of the City
Results Emergence of Themes 1. Negative Experiences with the Health Care System 2. Training of Palliative Care Staff 3. Dying the Way One Lives 4. Diversity in Delivery 5. Role of the City
 1. Negative Experiences with Health Care “Access is useless if homeless people don’t feel respected…I’ve spent years maintaining relationships with my clients and they are all strongly based on trust and respect and I always hear complaints about the way doctors, nurses and even medical students treat the homeless ”
1. Negative Experiences with Health Care “Access is useless if homeless people don’t feel respected…I’ve spent years maintaining relationships with my clients and they are all strongly based on trust and respect and I always hear complaints about the way doctors, nurses and even medical students treat the homeless ”
 1. Negative Experiences with Health Care Harm Reduction “If doctors and nurses don’t appreciate or even know the value of harm reduction in dealing with the homeless why should we be sending our clients to see them, it’s so counterproductive, we want them to be embraced and helped not lectured and alienated…” Trust “You toss everything else out the window, without trust there’s going to be no connection. People would rather die on the streets in filth that be confined in a space with people they don’t trust. That’s the reality with all of us”
1. Negative Experiences with Health Care Harm Reduction “If doctors and nurses don’t appreciate or even know the value of harm reduction in dealing with the homeless why should we be sending our clients to see them, it’s so counterproductive, we want them to be embraced and helped not lectured and alienated…” Trust “You toss everything else out the window, without trust there’s going to be no connection. People would rather die on the streets in filth that be confined in a space with people they don’t trust. That’s the reality with all of us”
 1. Negative Experiences with the Health Care Advocacy “ Navigating the health care system is difficult for anyone, having an advocate is important. There is definitely a role for advocacy in the hospital. Having a point person available to help the homeless person navigate the hospital, the administration, arrange visitors, all of that, that would really ease the experience and warm the idea of being part of the system which can help”
1. Negative Experiences with the Health Care Advocacy “ Navigating the health care system is difficult for anyone, having an advocate is important. There is definitely a role for advocacy in the hospital. Having a point person available to help the homeless person navigate the hospital, the administration, arrange visitors, all of that, that would really ease the experience and warm the idea of being part of the system which can help”
 Negative Experiences with the Health Care System Negative Experiences with Health Care Harm Reduction Trust Advocacy
Negative Experiences with the Health Care System Negative Experiences with Health Care Harm Reduction Trust Advocacy
 2. Training of Staff Talking About Death “Comfort in talking about death, that’s really essential. It’s not natural, by any means. If people can they avoid it. My friends, family, everyone, it’s a hard subject, the hardest probably. Staff can’t be expected to deal with such a heavy issue without training. …”
2. Training of Staff Talking About Death “Comfort in talking about death, that’s really essential. It’s not natural, by any means. If people can they avoid it. My friends, family, everyone, it’s a hard subject, the hardest probably. Staff can’t be expected to deal with such a heavy issue without training. …”
 2. Training of Staff Unique Street Issues “I used to think that in order to do this thing, we’d need to make institutions dedicated to serving the dying homeless, over the years however I’ve come to realize that the best, or at least most practical way to deal with this issues is through better training staff to be more sensitive to street issues, talk about death and respect harm reduction strategies. How can we evaluate this though? I’m really not sure. ”
2. Training of Staff Unique Street Issues “I used to think that in order to do this thing, we’d need to make institutions dedicated to serving the dying homeless, over the years however I’ve come to realize that the best, or at least most practical way to deal with this issues is through better training staff to be more sensitive to street issues, talk about death and respect harm reduction strategies. How can we evaluate this though? I’m really not sure. ”
 2. Training of Staff Street Issues Death and Dying
2. Training of Staff Street Issues Death and Dying
 3. “People want to die the way they lived” “There was this one man who was brought to a palliative care home and they insisted on him watching these movies that they “knew” he would like. In the end, after much negotiating it was arranged that his favorite wrestling show, or movie, or whatever, was put on TV because that’s what he liked and that’s what he wanted to die watching. That’s a real success story”
3. “People want to die the way they lived” “There was this one man who was brought to a palliative care home and they insisted on him watching these movies that they “knew” he would like. In the end, after much negotiating it was arranged that his favorite wrestling show, or movie, or whatever, was put on TV because that’s what he liked and that’s what he wanted to die watching. That’s a real success story”
 3. People want to die the way they lived “Institutions that cater to the dying homeless have to tolerate their visitors. I’ve heard from people great stories of homes that all of a sudden were having heavy drug users, sex trade workers, a whole mix of interesting people visit one of their palliative patients. We all want to be surrounded by our friends when we go. ”
3. People want to die the way they lived “Institutions that cater to the dying homeless have to tolerate their visitors. I’ve heard from people great stories of homes that all of a sudden were having heavy drug users, sex trade workers, a whole mix of interesting people visit one of their palliative patients. We all want to be surrounded by our friends when we go. ”

 4. Variety of Delivery • “I know people want to die in shelters but some want to die on the street, with their friends like they’ve lived. Everyone has a different idea. If we’re actually talking about palliative care we want to make sure people die in the way they want to. If we’re accepting that than it seems clear there can’t be a one idea that satisfies everyone. There isn't one resource that will serve everyone” • “I don’t see any success in forcing dying people into a home dedicated to that. We need to give choices and options. That’s extremely important. If for majority of one’s life they felt out of control, shouldn’t we let them have control as they die- wouldn’t that be wonderful? ”
4. Variety of Delivery • “I know people want to die in shelters but some want to die on the street, with their friends like they’ve lived. Everyone has a different idea. If we’re actually talking about palliative care we want to make sure people die in the way they want to. If we’re accepting that than it seems clear there can’t be a one idea that satisfies everyone. There isn't one resource that will serve everyone” • “I don’t see any success in forcing dying people into a home dedicated to that. We need to give choices and options. That’s extremely important. If for majority of one’s life they felt out of control, shouldn’t we let them have control as they die- wouldn’t that be wonderful? ”
 4. Variety of Delivery Shelter Based Street Based Mobile Units Hospital Based
4. Variety of Delivery Shelter Based Street Based Mobile Units Hospital Based
 5. Role of The City “The city has changed it’s policies with the emphasis on streets to homes. Unfortunately we are not allowed to provide blankets and what are considered “survival” materials to the homeless. Offering comfort to people dying on the street becomes difficult”
5. Role of The City “The city has changed it’s policies with the emphasis on streets to homes. Unfortunately we are not allowed to provide blankets and what are considered “survival” materials to the homeless. Offering comfort to people dying on the street becomes difficult”
 5. Role of the City “At the very least we’d appreciate having the city stay out of our way, at this point any sort of mobile care to those dying on the streets is pretty much impossible. We have to get them inside if we want to treat them. The city seems intent on continuing their streets to home program”
5. Role of the City “At the very least we’d appreciate having the city stay out of our way, at this point any sort of mobile care to those dying on the streets is pretty much impossible. We have to get them inside if we want to treat them. The city seems intent on continuing their streets to home program”
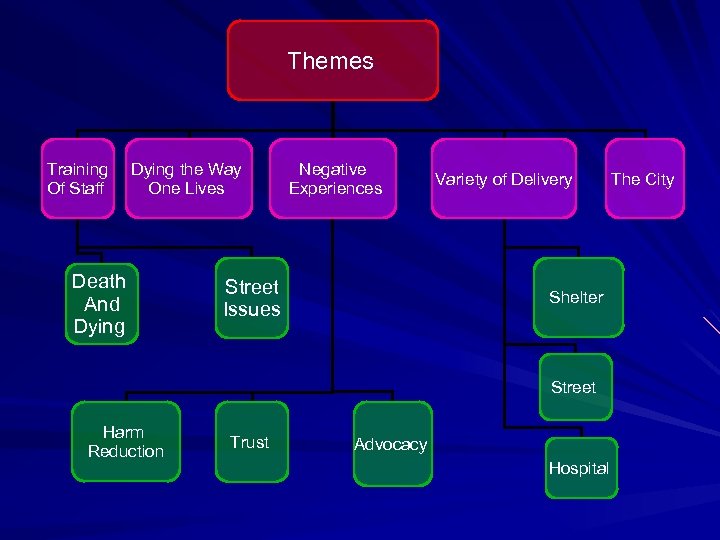 Themes Training Of Staff Dying the Way One Lives Death And Dying Negative Experiences Street Issues Variety of Delivery Shelter Street Harm Reduction Trust Advocacy Hospital The City
Themes Training Of Staff Dying the Way One Lives Death And Dying Negative Experiences Street Issues Variety of Delivery Shelter Street Harm Reduction Trust Advocacy Hospital The City
 Conclusions 1. Strengthening the relationship between the homeless and the Health Care system 2. Training of palliative care staff and homeless care providers 3. Respecting the unique experience and needs of the homeless
Conclusions 1. Strengthening the relationship between the homeless and the Health Care system 2. Training of palliative care staff and homeless care providers 3. Respecting the unique experience and needs of the homeless
 Conclusions 4. Providing multiple forms of palliative care 5. Encouraging the city to facilitate the distribution of palliative care material to those wishing to remain on the street
Conclusions 4. Providing multiple forms of palliative care 5. Encouraging the city to facilitate the distribution of palliative care material to those wishing to remain on the street
 Recommendations • A more global effort should be made to make the homeless more comfortable with the health care system • A role for a homeless advocate in hospital to help navigate the system • Palliative staff must be trained to address the unique issues facing the homeless (harm reduction) • Homeless care providers must be trained to address the unique issues facing the dying
Recommendations • A more global effort should be made to make the homeless more comfortable with the health care system • A role for a homeless advocate in hospital to help navigate the system • Palliative staff must be trained to address the unique issues facing the homeless (harm reduction) • Homeless care providers must be trained to address the unique issues facing the dying
 Recommendations • A three-pronged approach including: • Hospital based • Shelter based • Mobile units • The city should either serve no role or a supportive one • Next Project: Sample homeless population
Recommendations • A three-pronged approach including: • Hospital based • Shelter based • Mobile units • The city should either serve no role or a supportive one • Next Project: Sample homeless population
 Thank you • Dr. Holly Knowles • Dragana and Sonya • Beth Pelton • Paddy Bowen • Cathy Crowe
Thank you • Dr. Holly Knowles • Dragana and Sonya • Beth Pelton • Paddy Bowen • Cathy Crowe
 References City of Toronto. Shelter, Support and Housing Administration 2006. Quicks Facts. Toronto: City of Toronto. Available at www. toronto. ca/housing City of Toronto. Staff report street needs assessment 2006. Toronto: City of Toronto. Available at www. toronto. ca/housing/pdf/streetneedsassessment Street Health. 2007. The Street Health Report 2007. Toronto: Street Heath. Available at: steethealth. ca Hwang, SW. , O'Connell JJ. , Lebow, JM. , Bierer MF. , Orav, EJ. , Brennan TA. (2001). Health care utilization among homeless adults prior to death. J Health Care Poor Undeserved, 12(1), 50 -8. Gelberg L, Thompson L. (1997) Competing priorities as a barrier to medical care among homeless adults in Los Angeles. American Journal of Public Health. 87: 217220. Kushel MB, Vittingholff E. , Haas J. (2000). Factors associated with the health care utilization of homeless persons. JAMA, 285: 200 -206. Hwang, SW. (2002). Is homelessness hazardous to your health? Obstacles to the demonstration of a casual relationship. Canadian Journal of Public Health, 93, 407410. Andrulis, D. (1998). Access to care is the centerpiece in the elimination of socioeconomic disparities in health. Annals of Internal Medicine, 129, 412 -416. Sepulvda, C. , Marlin A. , Yoshida, T. , Ullrich A. (2002). Palliative care: the World Health Organization's global perspective. Journal of Pain and Symptom Management, 24, 91 -6. Kellehar, A. (2000). Spirituality and palliative care: a model of needs. Palliative Medicine, 14(2), 149 -155.
References City of Toronto. Shelter, Support and Housing Administration 2006. Quicks Facts. Toronto: City of Toronto. Available at www. toronto. ca/housing City of Toronto. Staff report street needs assessment 2006. Toronto: City of Toronto. Available at www. toronto. ca/housing/pdf/streetneedsassessment Street Health. 2007. The Street Health Report 2007. Toronto: Street Heath. Available at: steethealth. ca Hwang, SW. , O'Connell JJ. , Lebow, JM. , Bierer MF. , Orav, EJ. , Brennan TA. (2001). Health care utilization among homeless adults prior to death. J Health Care Poor Undeserved, 12(1), 50 -8. Gelberg L, Thompson L. (1997) Competing priorities as a barrier to medical care among homeless adults in Los Angeles. American Journal of Public Health. 87: 217220. Kushel MB, Vittingholff E. , Haas J. (2000). Factors associated with the health care utilization of homeless persons. JAMA, 285: 200 -206. Hwang, SW. (2002). Is homelessness hazardous to your health? Obstacles to the demonstration of a casual relationship. Canadian Journal of Public Health, 93, 407410. Andrulis, D. (1998). Access to care is the centerpiece in the elimination of socioeconomic disparities in health. Annals of Internal Medicine, 129, 412 -416. Sepulvda, C. , Marlin A. , Yoshida, T. , Ullrich A. (2002). Palliative care: the World Health Organization's global perspective. Journal of Pain and Symptom Management, 24, 91 -6. Kellehar, A. (2000). Spirituality and palliative care: a model of needs. Palliative Medicine, 14(2), 149 -155.
 Questions?
Questions?


