383c6258885f99d89836dd27b80540cc.ppt
- Количество слайдов: 149

 Cervical Cancer Screening… An Overview AMR NADIM, MD Professor of Obstetrics & Gynecology Ain Shams Faculty Of Medicine
Cervical Cancer Screening… An Overview AMR NADIM, MD Professor of Obstetrics & Gynecology Ain Shams Faculty Of Medicine
 Cervical Carcinoma Second in frequency among women cancers. It is still the most frequent cancer in the developing countries. 400, 000 new cases identified each year 80% of new cases in developing countries At least 200, 000 women die each year Screening programs reduced the mortality from cancer cervix in developed countries by 70%.
Cervical Carcinoma Second in frequency among women cancers. It is still the most frequent cancer in the developing countries. 400, 000 new cases identified each year 80% of new cases in developing countries At least 200, 000 women die each year Screening programs reduced the mortality from cancer cervix in developed countries by 70%.
![Incidence And Mortality For Cervical Cancer Vs Breast Cancer, [United States, 2000] Source: American Incidence And Mortality For Cervical Cancer Vs Breast Cancer, [United States, 2000] Source: American](https://present5.com/presentation/383c6258885f99d89836dd27b80540cc/image-4.jpg) Incidence And Mortality For Cervical Cancer Vs Breast Cancer, [United States, 2000] Source: American Cancer Society, 2000
Incidence And Mortality For Cervical Cancer Vs Breast Cancer, [United States, 2000] Source: American Cancer Society, 2000
 HPV infection Condyloma Accuminata Exophytic Frond like surface Lesion may be single or multiple Located within or outside the transformation zone
HPV infection Condyloma Accuminata Exophytic Frond like surface Lesion may be single or multiple Located within or outside the transformation zone
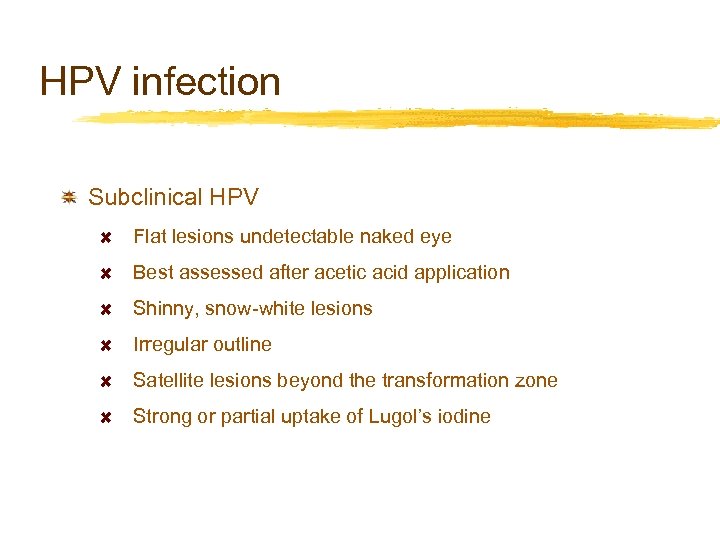 HPV infection Subclinical HPV Flat lesions undetectable naked eye Best assessed after acetic acid application Shinny, snow-white lesions Irregular outline Satellite lesions beyond the transformation zone Strong or partial uptake of Lugol’s iodine
HPV infection Subclinical HPV Flat lesions undetectable naked eye Best assessed after acetic acid application Shinny, snow-white lesions Irregular outline Satellite lesions beyond the transformation zone Strong or partial uptake of Lugol’s iodine
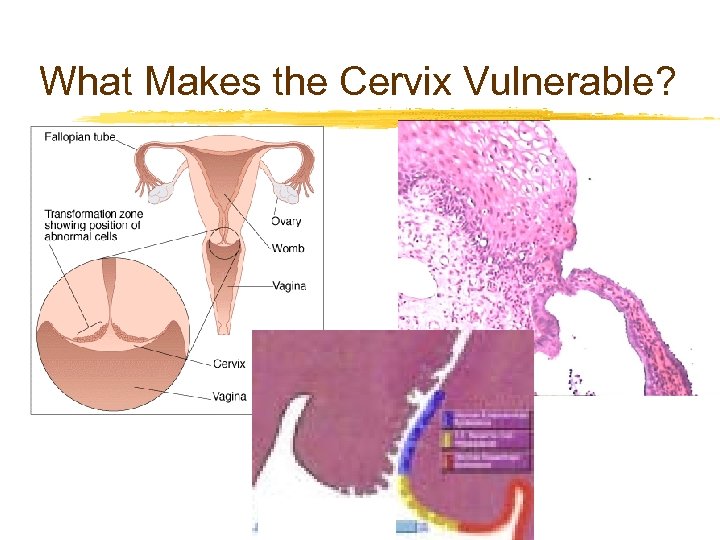 What Makes the Cervix Vulnerable?
What Makes the Cervix Vulnerable?
 The HPV-cervical cancer link Human papillomavirus (HPV) is a very common infection (more than 50% of adults get it, in most it is a transitory infection). 99. 7% of cervical cancer cases are associated with HPV. Progression from HPV infection to cancer usually takes 20 -30 years.
The HPV-cervical cancer link Human papillomavirus (HPV) is a very common infection (more than 50% of adults get it, in most it is a transitory infection). 99. 7% of cervical cancer cases are associated with HPV. Progression from HPV infection to cancer usually takes 20 -30 years.
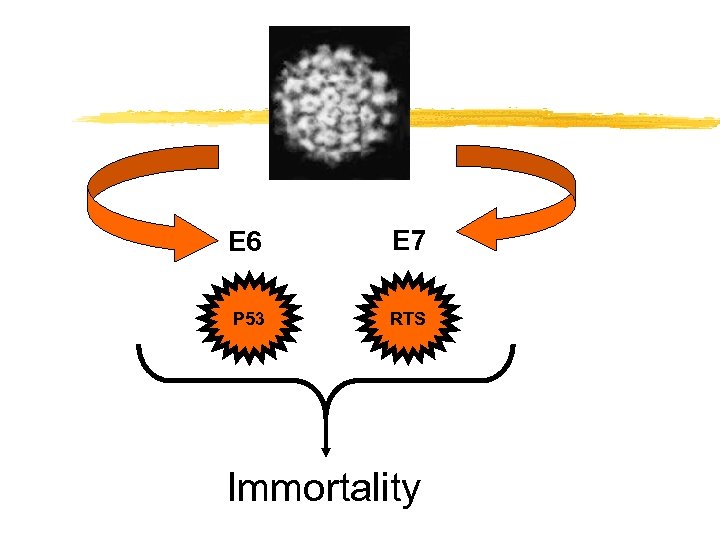 E 6 E 7 P 53 RTS Immortality
E 6 E 7 P 53 RTS Immortality
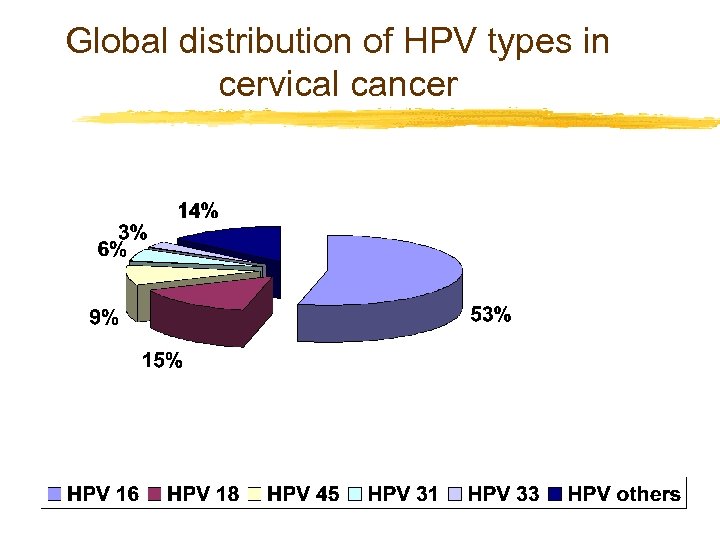 Global distribution of HPV types in cervical cancer
Global distribution of HPV types in cervical cancer
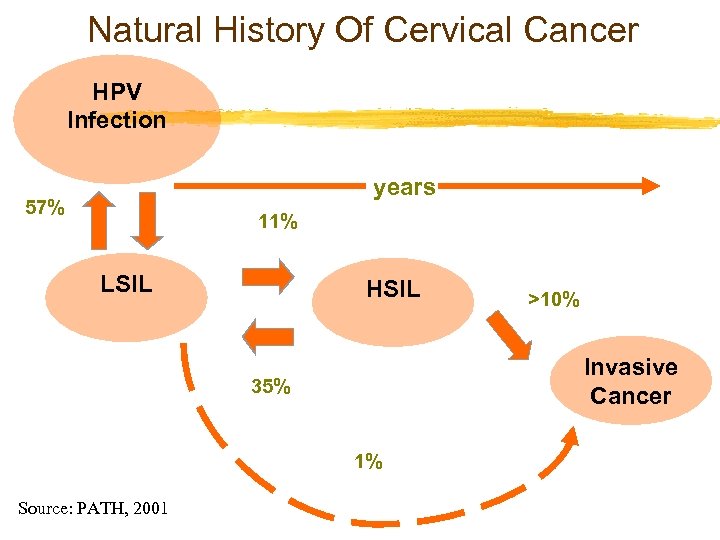 Natural History Of Cervical Cancer HPV Infection years 57% 11% LSIL HSIL Invasive Cancer 35% 1% Source: PATH, 2001 >10%
Natural History Of Cervical Cancer HPV Infection years 57% 11% LSIL HSIL Invasive Cancer 35% 1% Source: PATH, 2001 >10%
 Screening…? Organized identification High coverage of a target population Continuous quality assessment. Feasibility of treatment & follow up Of a pre - clinical disease state by a test that is repeated at a given interval
Screening…? Organized identification High coverage of a target population Continuous quality assessment. Feasibility of treatment & follow up Of a pre - clinical disease state by a test that is repeated at a given interval
 To screen or To screen not ? Recommended Screening Cervical Carcinoma Breast Carcinoma Colorectal Carcinoma Not yet , for… Ovarian Cancer Bronchogenic Carcinoma Skin cancer Oral Cancer Prostate Cancer Cervical Cancer Screening by The Pap Smear Is one of the very few cost effective interventions to prevent cancer.
To screen or To screen not ? Recommended Screening Cervical Carcinoma Breast Carcinoma Colorectal Carcinoma Not yet , for… Ovarian Cancer Bronchogenic Carcinoma Skin cancer Oral Cancer Prostate Cancer Cervical Cancer Screening by The Pap Smear Is one of the very few cost effective interventions to prevent cancer.
 Pre - requisites For Successful Screening After Wilson and Jugner (1968): The condition should be an important health problem. There should be an accepted treatment. Facilities for treatment and diagnosis should be available. There should be a recognizable latent or early symptomatic stage. There should be a suitable method of examination. The test should be acceptable to the population. The natural history of the disease should be adequately understood
Pre - requisites For Successful Screening After Wilson and Jugner (1968): The condition should be an important health problem. There should be an accepted treatment. Facilities for treatment and diagnosis should be available. There should be a recognizable latent or early symptomatic stage. There should be a suitable method of examination. The test should be acceptable to the population. The natural history of the disease should be adequately understood
 Pre - requisites, cont. . There should be an agreed policy on whom to treat as patients. The cost should be economically balanced with the expenditure of medical care as a whole. Case finding should be a continuing process. They apply reasonably well for screening of Cervical Carcinoma
Pre - requisites, cont. . There should be an agreed policy on whom to treat as patients. The cost should be economically balanced with the expenditure of medical care as a whole. Case finding should be a continuing process. They apply reasonably well for screening of Cervical Carcinoma
 Effective Screening Program Should be tailored to suit the principles for national cancer control programs. We Should NOT copy other’s programs. . . Otherwise Too much money & effort will be spent with minimal impact on the incidence & mortality from the disease.
Effective Screening Program Should be tailored to suit the principles for national cancer control programs. We Should NOT copy other’s programs. . . Otherwise Too much money & effort will be spent with minimal impact on the incidence & mortality from the disease.
 Cancer Cervix : A Screenable Preventable Disease Cancer cervix still represents a problem in the developing counties: Less than 5% of the population is screened. Its natural history is well-known. Definitive pre-cancerous lesions are identified and treatment will eradicate the disease. Screening tools available for more than 60 years and are subjected to continuous innovations to increase specificity and sensitivity
Cancer Cervix : A Screenable Preventable Disease Cancer cervix still represents a problem in the developing counties: Less than 5% of the population is screened. Its natural history is well-known. Definitive pre-cancerous lesions are identified and treatment will eradicate the disease. Screening tools available for more than 60 years and are subjected to continuous innovations to increase specificity and sensitivity
 Cervical Cancer Is Preventable Primary prevention Education to reduce high-risk sexual behavior Risk assessment Secondary prevention Identify and treat precancerous lesions before they progress to cervical cancer
Cervical Cancer Is Preventable Primary prevention Education to reduce high-risk sexual behavior Risk assessment Secondary prevention Identify and treat precancerous lesions before they progress to cervical cancer
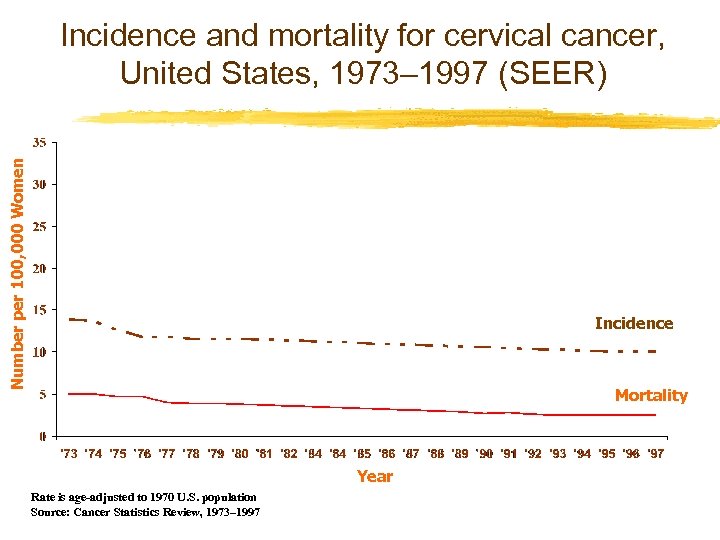 Number per 100, 000 Women Incidence and mortality for cervical cancer, United States, 1973– 1997 (SEER) Incidence Mortality Year Rate is age-adjusted to 1970 U. S. population Source: Cancer Statistics Review, 1973– 1997
Number per 100, 000 Women Incidence and mortality for cervical cancer, United States, 1973– 1997 (SEER) Incidence Mortality Year Rate is age-adjusted to 1970 U. S. population Source: Cancer Statistics Review, 1973– 1997
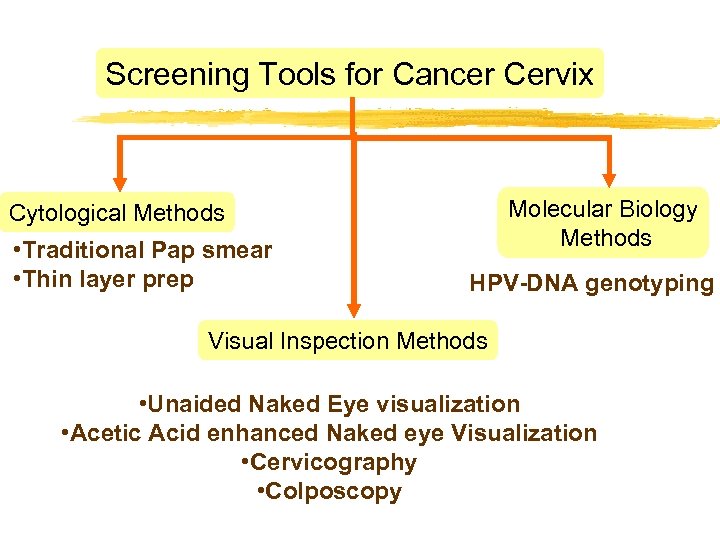 Screening Tools for Cancer Cervix Molecular Biology Methods Cytological Methods • Traditional Pap smear • Thin layer prep HPV-DNA genotyping Visual Inspection Methods • Unaided Naked Eye visualization • Acetic Acid enhanced Naked eye Visualization • Cervicography • Colposcopy
Screening Tools for Cancer Cervix Molecular Biology Methods Cytological Methods • Traditional Pap smear • Thin layer prep HPV-DNA genotyping Visual Inspection Methods • Unaided Naked Eye visualization • Acetic Acid enhanced Naked eye Visualization • Cervicography • Colposcopy
 The Papanicolaou Test Nicknamed … Pap Smear
The Papanicolaou Test Nicknamed … Pap Smear
 Cytopathology: Cytopathology is diagnosis of disease in cells. Exfoliative & Non-Exfoliative - cytology. Exfoliative: Cell samples are collected from normally shedding tissues like epithelium. spatula or brush to enhances collection. Non-Exfoliative: Cells samples collected by needles with suction pressure. (FNAC) Cytology specimen is fixed, stained and studied under microscope.
Cytopathology: Cytopathology is diagnosis of disease in cells. Exfoliative & Non-Exfoliative - cytology. Exfoliative: Cell samples are collected from normally shedding tissues like epithelium. spatula or brush to enhances collection. Non-Exfoliative: Cells samples collected by needles with suction pressure. (FNAC) Cytology specimen is fixed, stained and studied under microscope.
 What is a Pap Smear? Screening test for cervical cancer. It is a type of exfoliative cytology test. Simple, safe, non-invasive method Developed by “George Papanicolaou” Exfoliated cells from cervix are collected usually enhanced by using a variety of spatulas or brushes. The specimen is processed and studied for morphology.
What is a Pap Smear? Screening test for cervical cancer. It is a type of exfoliative cytology test. Simple, safe, non-invasive method Developed by “George Papanicolaou” Exfoliated cells from cervix are collected usually enhanced by using a variety of spatulas or brushes. The specimen is processed and studied for morphology.
 Who should have PAP test. . Every woman should have an annual Pap examination when she becomes sexually active or turns 18 years old [ whichever comes first]. Defining the target population is important in any screening program.
Who should have PAP test. . Every woman should have an annual Pap examination when she becomes sexually active or turns 18 years old [ whichever comes first]. Defining the target population is important in any screening program.
 What is the best time for PAP: The best time for a Pap examination is during the two weeks following the end of menstrual flow. (Proliferative phase). Why…? If menopause, Pap examination can be scheduled anytime
What is the best time for PAP: The best time for a Pap examination is during the two weeks following the end of menstrual flow. (Proliferative phase). Why…? If menopause, Pap examination can be scheduled anytime
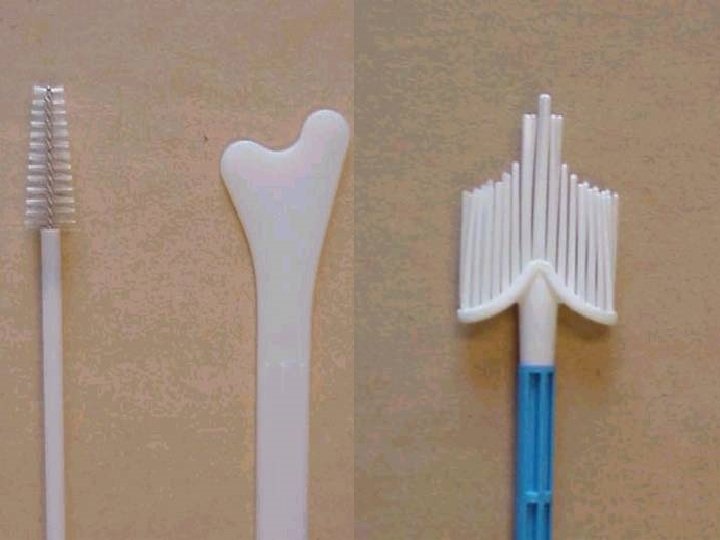
 Take Care. . . Use a good sampling device Do Not use Lubricants while taking the smear. Do Not be too slow in plating the slide Sample the endocervical canal and the whole transformation zone. Do Not insert the sampling device too deep in the endocervical canal: This invites bleeding It might draw cells different to interpret.
Take Care. . . Use a good sampling device Do Not use Lubricants while taking the smear. Do Not be too slow in plating the slide Sample the endocervical canal and the whole transformation zone. Do Not insert the sampling device too deep in the endocervical canal: This invites bleeding It might draw cells different to interpret.
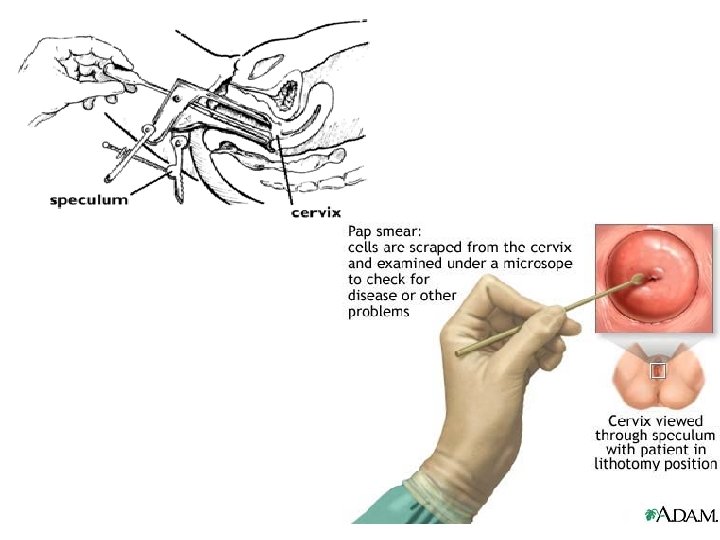
 Who are at increased risk of Cervical Cancer? · Any woman can develop cancer cervix. · Multiple sex partners or a partner who has had multiple female partners. · Have had genital warts. · Sexual relations before the age of 18. · Previous abnormal pap examination. · Rare in virgins and with use of condoms.
Who are at increased risk of Cervical Cancer? · Any woman can develop cancer cervix. · Multiple sex partners or a partner who has had multiple female partners. · Have had genital warts. · Sexual relations before the age of 18. · Previous abnormal pap examination. · Rare in virgins and with use of condoms.
 The Target Population What should happen… From onset of sexual activity and throughout life. Covering all social classes. Covering urban and rural sectors. What should be avoided … Limiting screening to the CBP Limiting screening to a particular social class or a particular sector. It is estimated that less than 5 % of women in the developing countries are screened. These are essentially women under 35.
The Target Population What should happen… From onset of sexual activity and throughout life. Covering all social classes. Covering urban and rural sectors. What should be avoided … Limiting screening to the CBP Limiting screening to a particular social class or a particular sector. It is estimated that less than 5 % of women in the developing countries are screened. These are essentially women under 35.
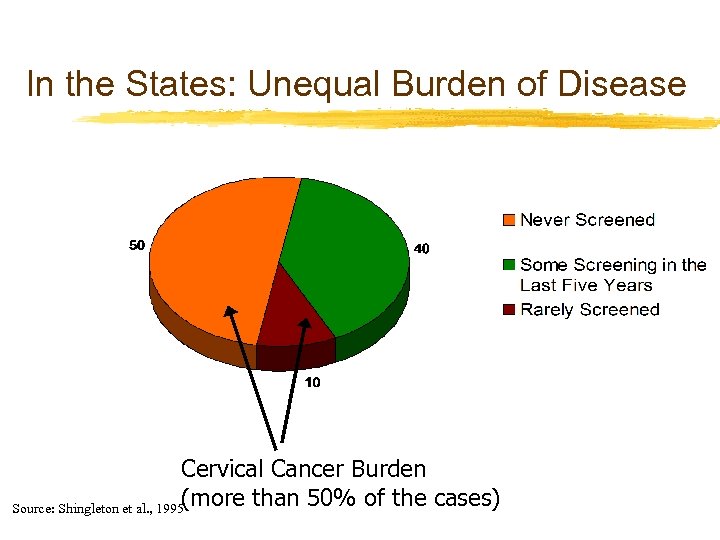 In the States: Unequal Burden of Disease Cervical Cancer Burden (more than 50% of the cases) Source: Shingleton et al. , 1995
In the States: Unequal Burden of Disease Cervical Cancer Burden (more than 50% of the cases) Source: Shingleton et al. , 1995
 IN EGYPT. . . Only sporadic attempts of screening. No nation-wide program Primary health care providers…? Lack of screening of the older women : the priority target group. Lack of appreciation by the women of the relevance of the disease Lack of availability of health care in the rural areas. Fatalism ﺍﻟﺨـــﻮﻑ ﻣﻦ ﺍﻟﻤﺠـــــﻬــــﻮﻝ
IN EGYPT. . . Only sporadic attempts of screening. No nation-wide program Primary health care providers…? Lack of screening of the older women : the priority target group. Lack of appreciation by the women of the relevance of the disease Lack of availability of health care in the rural areas. Fatalism ﺍﻟﺨـــﻮﻑ ﻣﻦ ﺍﻟﻤﺠـــــﻬــــﻮﻝ
 Characteristics of women never or rarely screened for cervical cancer Older Low SES and/or lack of insurance or ability to pay for screening Less educated No regular health care provider Live in culturally-isolated urban neighborhoods or hard-to-reach rural areas
Characteristics of women never or rarely screened for cervical cancer Older Low SES and/or lack of insurance or ability to pay for screening Less educated No regular health care provider Live in culturally-isolated urban neighborhoods or hard-to-reach rural areas
 Pathology of Cervix: the uterine cervix is continually being bombarded by a variety of stress including mechanical, microbiologic, chemical, and hormonal insults. The cervix responds by Acute or chronic inflammatory reactions Adaptive proliferative responses like Hyperplasia, Metaplasia & Dysplasia. Anaplasia - Benign & Malignant tumors.
Pathology of Cervix: the uterine cervix is continually being bombarded by a variety of stress including mechanical, microbiologic, chemical, and hormonal insults. The cervix responds by Acute or chronic inflammatory reactions Adaptive proliferative responses like Hyperplasia, Metaplasia & Dysplasia. Anaplasia - Benign & Malignant tumors.
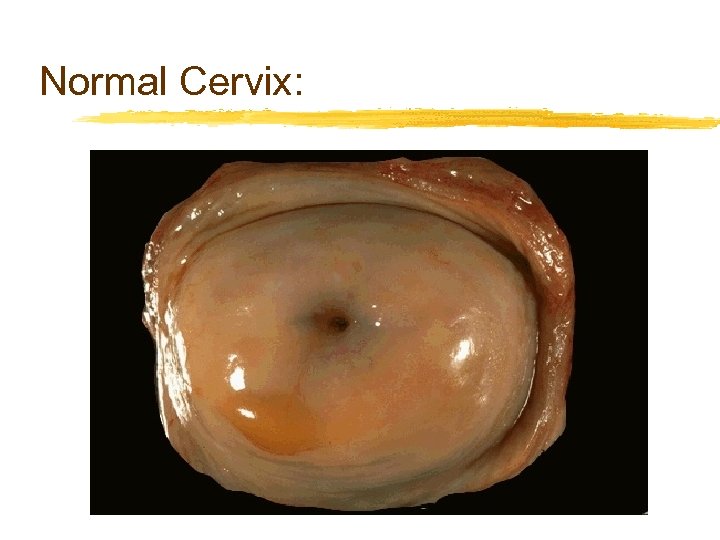 Normal Cervix:
Normal Cervix:
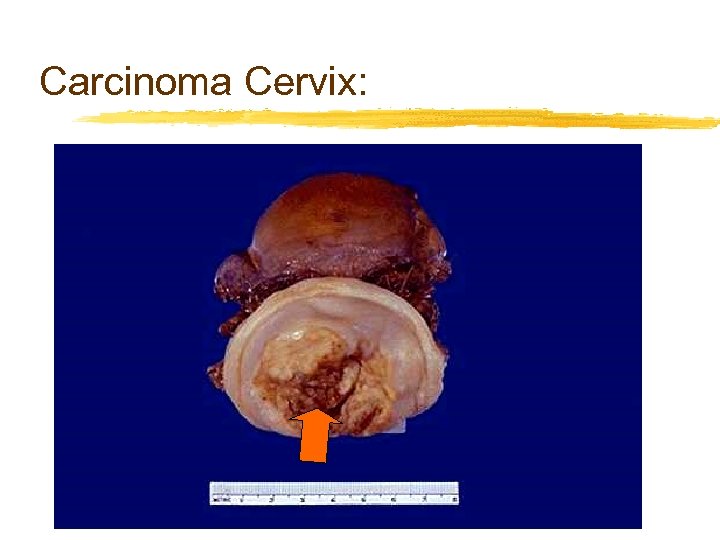 Carcinoma Cervix:
Carcinoma Cervix:
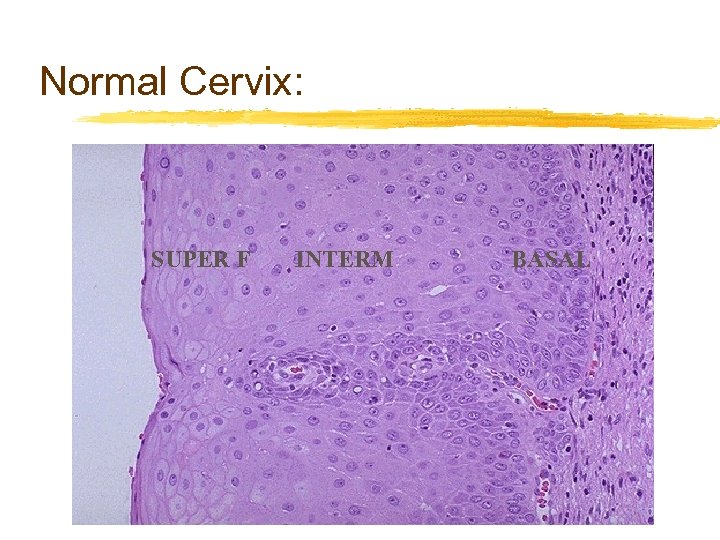 Normal Cervix: SUPER F INTERM BASAL
Normal Cervix: SUPER F INTERM BASAL
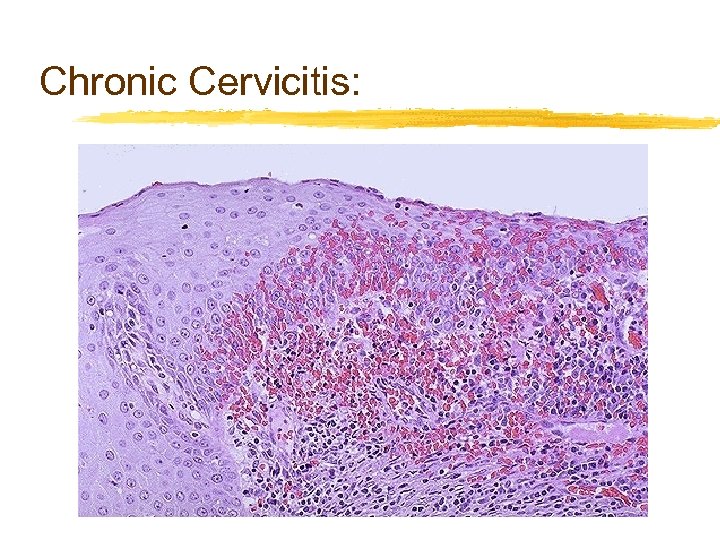 Chronic Cervicitis:
Chronic Cervicitis:
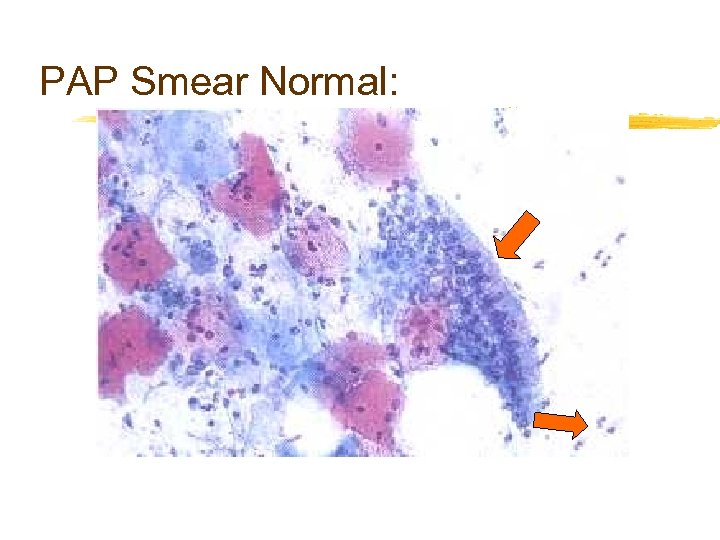 PAP Smear Normal:
PAP Smear Normal:
 Pathogenesis: (non-neoplastic) 1. 2. 3. 4. Chronic cervicitis Hyperplasia – Number Metaplasia – Change to squamous Dysplasia – no-maturation, disorder (CIN 1 -3, CIS)
Pathogenesis: (non-neoplastic) 1. 2. 3. 4. Chronic cervicitis Hyperplasia – Number Metaplasia – Change to squamous Dysplasia – no-maturation, disorder (CIN 1 -3, CIS)
 Pathogenesis: (Neoplastic( Malignant (Cervical Cancer) Invasion & Spreading.
Pathogenesis: (Neoplastic( Malignant (Cervical Cancer) Invasion & Spreading.
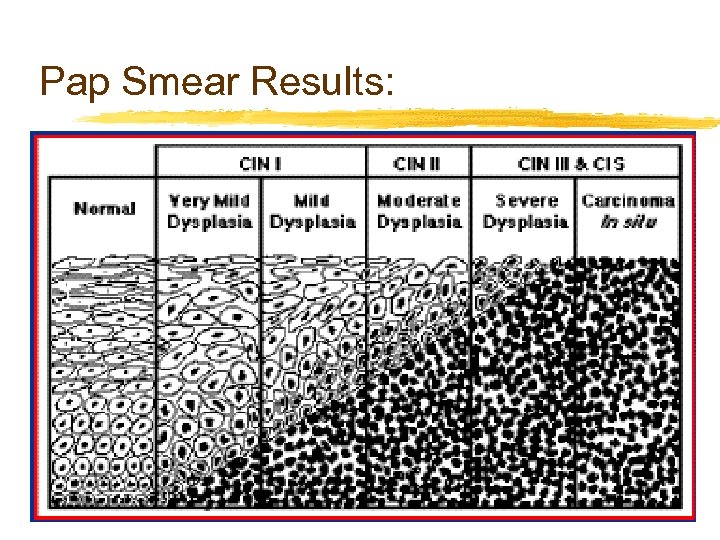 Pap Smear Results:
Pap Smear Results:
 Existing Screening Guidelines WHO (1992): Annual Pap tests are often unnecessary—“it is clear that it is more costeffective to recruit a high proportion of the population and screen them infrequently, than to recruit a low proportion and screen them often. ”
Existing Screening Guidelines WHO (1992): Annual Pap tests are often unnecessary—“it is clear that it is more costeffective to recruit a high proportion of the population and screen them infrequently, than to recruit a low proportion and screen them often. ”
 Existing Screening Guidelines (continued( USPSTF (1996): “There is little evidence that women who receive annual screening are at significantly lower risk for invasive cervical cancer than are women who are tested every 3– 5 years. ”
Existing Screening Guidelines (continued( USPSTF (1996): “There is little evidence that women who receive annual screening are at significantly lower risk for invasive cervical cancer than are women who are tested every 3– 5 years. ”
 Existing Screening Guidelines (continued( ACPM (1996): “Estimates from mathematical models indicate that regular triennial screening would achieve 91 -96% of the benefit of annual screening, while greatly reducing the cost, potential harms, and inconvenience. ”
Existing Screening Guidelines (continued( ACPM (1996): “Estimates from mathematical models indicate that regular triennial screening would achieve 91 -96% of the benefit of annual screening, while greatly reducing the cost, potential harms, and inconvenience. ”
 Existing Screening Guidelines (continued( ACOG (2000): “After a woman has had three or more consecutive, satisfactory, annual cytological examinations with normal findings, the Pap test may be performed less frequently on a low-risk woman at the discretion of her physician. ” ACS (2001): “After three or more consecutive annual exams with normal findings, the Pap test may be performed less frequently at the discretion of the physician. ”
Existing Screening Guidelines (continued( ACOG (2000): “After a woman has had three or more consecutive, satisfactory, annual cytological examinations with normal findings, the Pap test may be performed less frequently on a low-risk woman at the discretion of her physician. ” ACS (2001): “After three or more consecutive annual exams with normal findings, the Pap test may be performed less frequently at the discretion of the physician. ”
 The Screening Interval…A Controversy A negative smear ensures a protective effect of 93% if repeated yearly and 91 % if repeated at 3 years interval. At 10 years interval the protective effect drops to 64 % …still a 2/3 reduction of the risk.
The Screening Interval…A Controversy A negative smear ensures a protective effect of 93% if repeated yearly and 91 % if repeated at 3 years interval. At 10 years interval the protective effect drops to 64 % …still a 2/3 reduction of the risk.
 Screening Interval…Our Policy Annual Screening of ladies is advocated, we think it is a way of establishing a multiplicative correction effect by which the 20% false negative screening results may be reduced down to 1 %. “Unsatisfactory smears” are repeated the following cycle. “Satisfactory smears but limited by…. ” are repeated as soon as the condition is corrected. If laser or conization were made, the smear is repeated after 3 months.
Screening Interval…Our Policy Annual Screening of ladies is advocated, we think it is a way of establishing a multiplicative correction effect by which the 20% false negative screening results may be reduced down to 1 %. “Unsatisfactory smears” are repeated the following cycle. “Satisfactory smears but limited by…. ” are repeated as soon as the condition is corrected. If laser or conization were made, the smear is repeated after 3 months.
 Pap Test as a Screening Tool Sensitivity Moderate: 51– 88% Specificity High: 95– 98% Source: Meyers et al. , 2000 Brown and Garber, 1999 Given the sensitivity and specificity of the Pap test, “. . . the major barrier to prevention of cervical cancer is not the accuracy of the Pap test, but the failure to be screened at all. ”
Pap Test as a Screening Tool Sensitivity Moderate: 51– 88% Specificity High: 95– 98% Source: Meyers et al. , 2000 Brown and Garber, 1999 Given the sensitivity and specificity of the Pap test, “. . . the major barrier to prevention of cervical cancer is not the accuracy of the Pap test, but the failure to be screened at all. ”
 The Fluid - Based Technology The Thin - Prep The sample is put into a liquid medium “collection vial” which is sent to the lab where it is processed as a thin layer slide. There is no more: Air drying artifacts. Dirty backgrounds. Spreading errors Cells left entangled in the sampling device.
The Fluid - Based Technology The Thin - Prep The sample is put into a liquid medium “collection vial” which is sent to the lab where it is processed as a thin layer slide. There is no more: Air drying artifacts. Dirty backgrounds. Spreading errors Cells left entangled in the sampling device.
 The Thin - Prep, cont. . . All the cells are examined Cells are more evenly distributed. HPV typing & semi quantitative assays. The Sensitivity & Specificity are increased: - More detection of SIL, less incidence of “satisfactory but limited. ” - Eliminating many ASCUS
The Thin - Prep, cont. . . All the cells are examined Cells are more evenly distributed. HPV typing & semi quantitative assays. The Sensitivity & Specificity are increased: - More detection of SIL, less incidence of “satisfactory but limited. ” - Eliminating many ASCUS
 What We Know About Liquidbased Testing Technologies More sensitive, but not more specific, than conventional Pap tests (Austin, 1998) ACOG did not recommend routine use in 1998: Cost too high Insufficient data demonstrating reduction of disease incidence or cancer survival Currently silent on the issue
What We Know About Liquidbased Testing Technologies More sensitive, but not more specific, than conventional Pap tests (Austin, 1998) ACOG did not recommend routine use in 1998: Cost too high Insufficient data demonstrating reduction of disease incidence or cancer survival Currently silent on the issue
 The French Society of Clinical Cytology Study Group recently compared the sensitivity, specificity, and interobserver reliability of conventional Pap tests, monolayer cytology, and HPV testing in a setting with "complete independence from the suppliers. " What the researchers discovered was that results with the conventional Pap smear were more often satisfactory according to the Bethesda system, more reliable, and had consistently better sensitivity and specificity than monolayer cytology. Coste J, et al; French Society of Clinical Cytology Study Group. 2003
The French Society of Clinical Cytology Study Group recently compared the sensitivity, specificity, and interobserver reliability of conventional Pap tests, monolayer cytology, and HPV testing in a setting with "complete independence from the suppliers. " What the researchers discovered was that results with the conventional Pap smear were more often satisfactory according to the Bethesda system, more reliable, and had consistently better sensitivity and specificity than monolayer cytology. Coste J, et al; French Society of Clinical Cytology Study Group. 2003
 HPV/DNA Testing Atypical LSIL Triage Study Trials No benefit for women with LSIL results Probable benefit for women with ASCUS results
HPV/DNA Testing Atypical LSIL Triage Study Trials No benefit for women with LSIL results Probable benefit for women with ASCUS results
 An Ideal Reporting System… High degree of sensitivity and specificity. Reproducible. Uniformat and standardized nomenclature. Therapeutic implications are drawn from diagnostic nomenclature. Emphasizes that the pap test is a a request for a medical consultation between the gynecologist and the cytopathologist.
An Ideal Reporting System… High degree of sensitivity and specificity. Reproducible. Uniformat and standardized nomenclature. Therapeutic implications are drawn from diagnostic nomenclature. Emphasizes that the pap test is a a request for a medical consultation between the gynecologist and the cytopathologist.
 And So Was Introduced The Bethesda System… First issued following a NCI workshop in 1989. Revised in 1991 and 1993. Latest revision in October 2001.
And So Was Introduced The Bethesda System… First issued following a NCI workshop in 1989. Revised in 1991 and 1993. Latest revision in October 2001.
 The Bethesda System Confounding terminologies were omitted, e. g. Smears with evidence of repair or inflammations are reported as being “within normal limits. ” The Pap smear is redefined as a medical consultation The physician provides the history The cytologist provides the diagnosis And make recommendations regarding follow up
The Bethesda System Confounding terminologies were omitted, e. g. Smears with evidence of repair or inflammations are reported as being “within normal limits. ” The Pap smear is redefined as a medical consultation The physician provides the history The cytologist provides the diagnosis And make recommendations regarding follow up
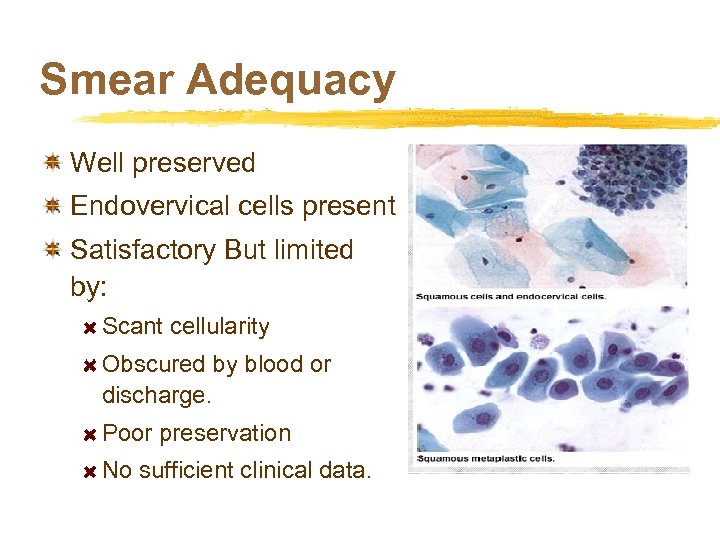 Smear Adequacy Well preserved Endovervical cells present Satisfactory But limited by: Scant cellularity Obscured by blood or discharge. Poor preservation No sufficient clinical data.
Smear Adequacy Well preserved Endovervical cells present Satisfactory But limited by: Scant cellularity Obscured by blood or discharge. Poor preservation No sufficient clinical data.
 Unsatisfactory for Diagnosis Poor preparation. Obscured by blood or inflammation or discharge. Scanty cellularity. Unlabeled slides
Unsatisfactory for Diagnosis Poor preparation. Obscured by blood or inflammation or discharge. Scanty cellularity. Unlabeled slides
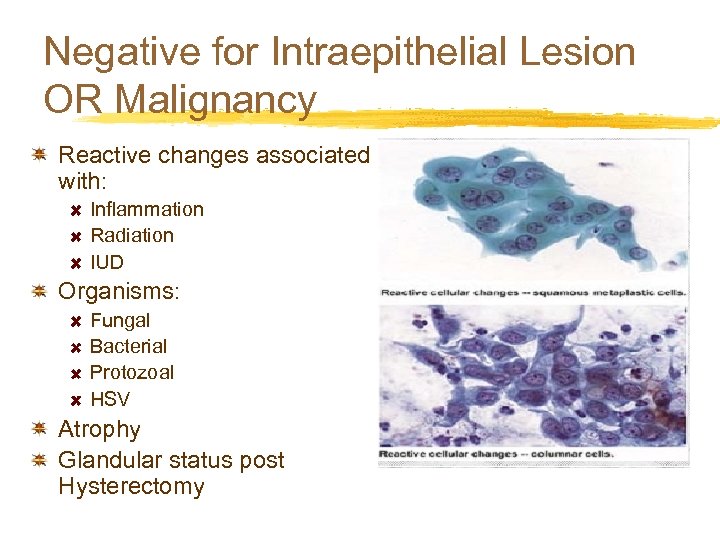 Negative for Intraepithelial Lesion OR Malignancy Reactive changes associated with: Inflammation Radiation IUD Organisms: Fungal Bacterial Protozoal HSV Atrophy Glandular status post Hysterectomy
Negative for Intraepithelial Lesion OR Malignancy Reactive changes associated with: Inflammation Radiation IUD Organisms: Fungal Bacterial Protozoal HSV Atrophy Glandular status post Hysterectomy
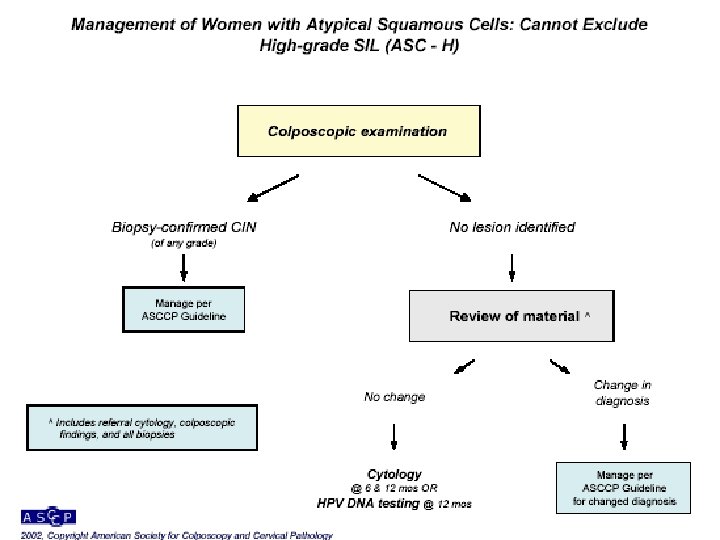
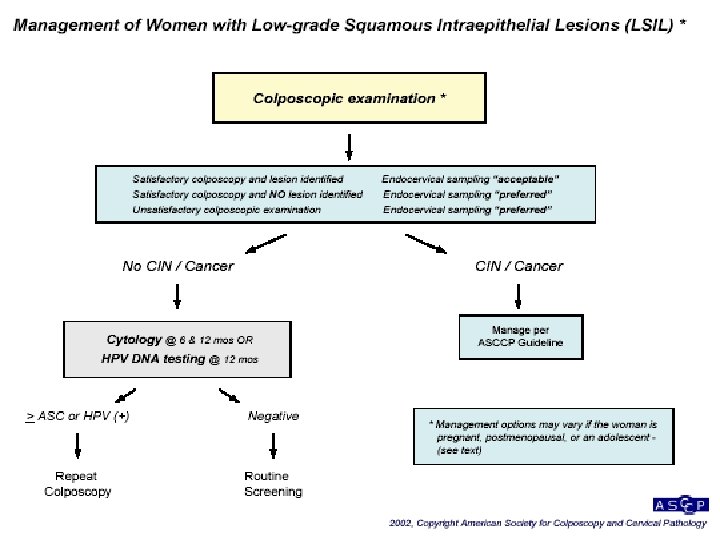
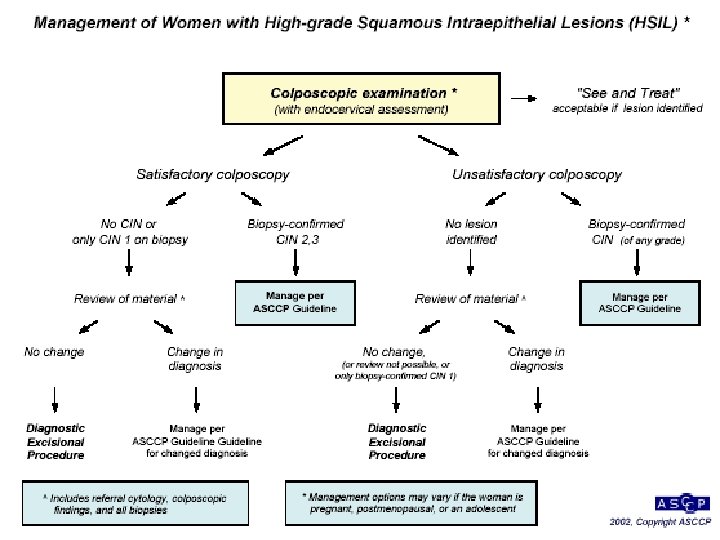
 Epithelial Cell Abnormalities Squamous cells Atypical squamous cells Of undetermined significance: ASC-US Can not exclude HSIL: ASC-H LSIL HSIL Squamous cell carcinoma Glandular cells Atypical GUS Endocervical Endometrial Other Atypical Endocervical cells, favor neoplastic Glandular cells, favor neoplastic Endocervical Adenocarc. In situ Adenocarcinoma
Epithelial Cell Abnormalities Squamous cells Atypical squamous cells Of undetermined significance: ASC-US Can not exclude HSIL: ASC-H LSIL HSIL Squamous cell carcinoma Glandular cells Atypical GUS Endocervical Endometrial Other Atypical Endocervical cells, favor neoplastic Glandular cells, favor neoplastic Endocervical Adenocarc. In situ Adenocarcinoma
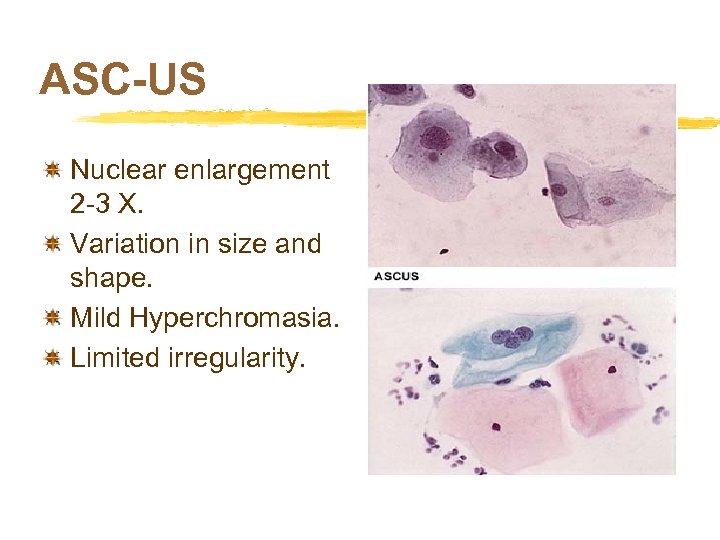 ASC-US Nuclear enlargement 2 -3 X. Variation in size and shape. Mild Hyperchromasia. Limited irregularity.
ASC-US Nuclear enlargement 2 -3 X. Variation in size and shape. Mild Hyperchromasia. Limited irregularity.
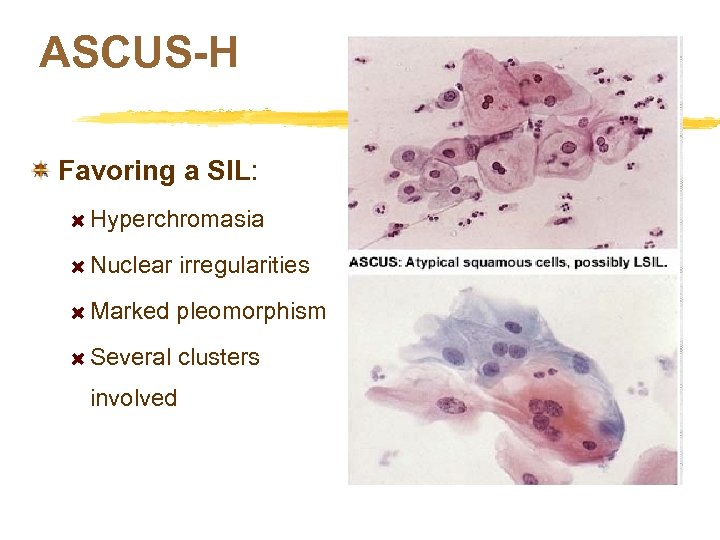 ASCUS-H Favoring a SIL: Hyperchromasia Nuclear irregularities Marked pleomorphism Several clusters involved
ASCUS-H Favoring a SIL: Hyperchromasia Nuclear irregularities Marked pleomorphism Several clusters involved
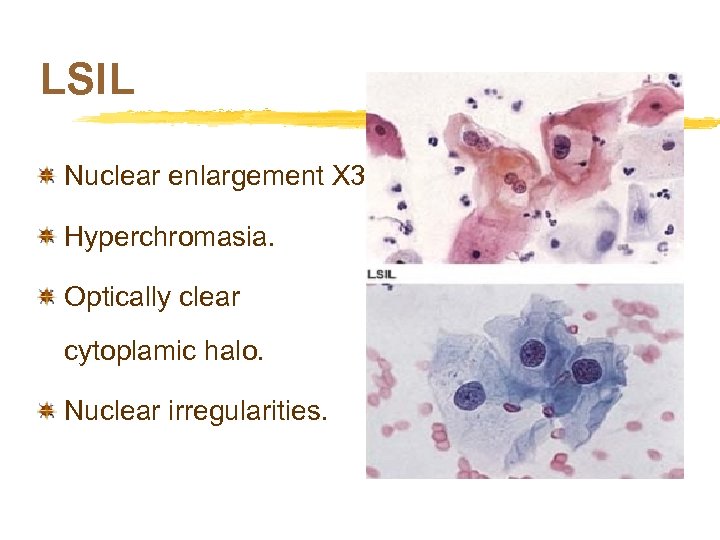 LSIL Nuclear enlargement X 3. Hyperchromasia. Optically clear cytoplamic halo. Nuclear irregularities.
LSIL Nuclear enlargement X 3. Hyperchromasia. Optically clear cytoplamic halo. Nuclear irregularities.
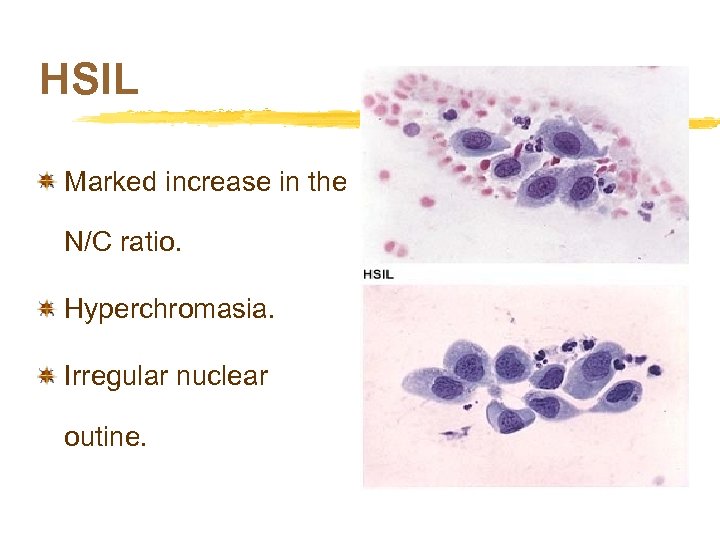 HSIL Marked increase in the N/C ratio. Hyperchromasia. Irregular nuclear outine.
HSIL Marked increase in the N/C ratio. Hyperchromasia. Irregular nuclear outine.
 The Bethesda System, TBS Making a uniform Terminology. Eliminating the Papanicolaou classes. Including statement on the adequacy of the specimen. To highlight that cytological examination is a medical consultation between clinician and cytologist To provide a frame work dealing with reparative atypia
The Bethesda System, TBS Making a uniform Terminology. Eliminating the Papanicolaou classes. Including statement on the adequacy of the specimen. To highlight that cytological examination is a medical consultation between clinician and cytologist To provide a frame work dealing with reparative atypia
 “Satisfactory for Evaluation , But Limited By…” Lack of clinical Information. Lack of endocervical component. Partially obscured by blood or inflammatory background : 50 -75% of the slide.
“Satisfactory for Evaluation , But Limited By…” Lack of clinical Information. Lack of endocervical component. Partially obscured by blood or inflammatory background : 50 -75% of the slide.
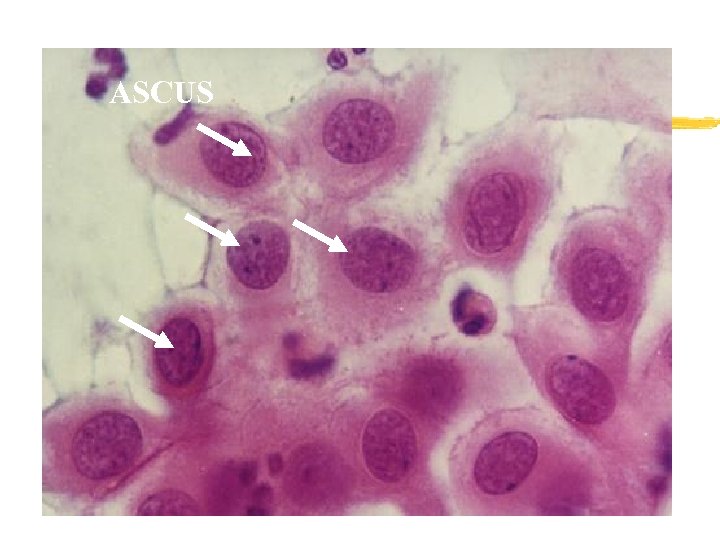 ASCUS
ASCUS
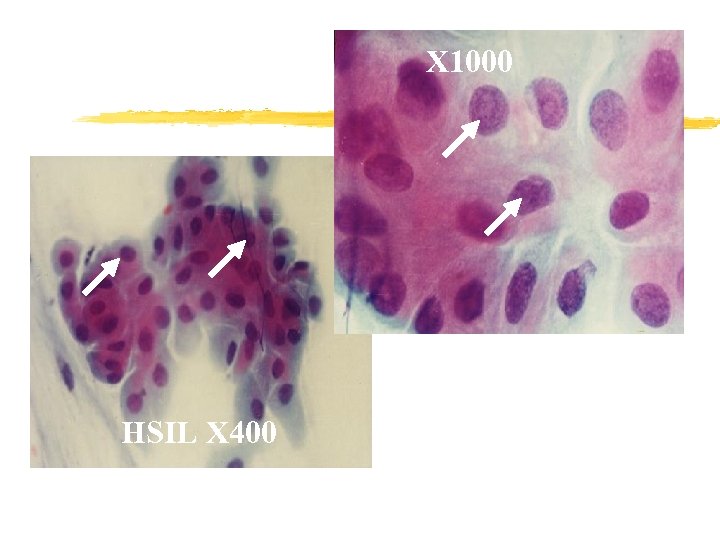 X 1000 HSIL X 400
X 1000 HSIL X 400
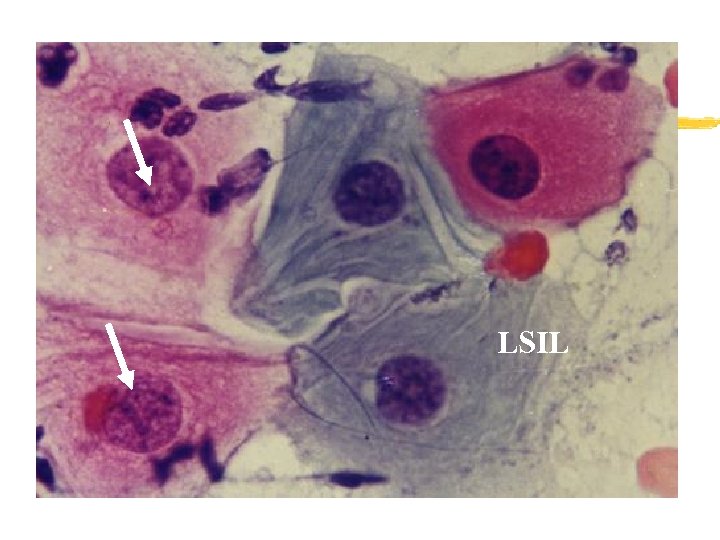 LSIL
LSIL
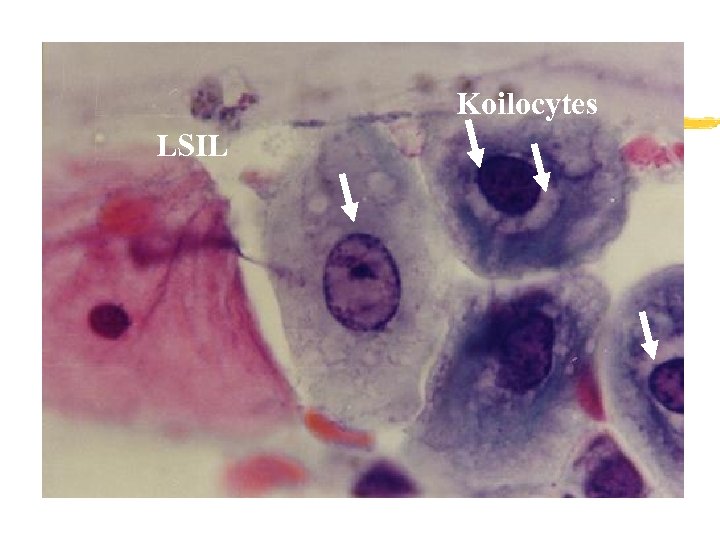 Koilocytes LSIL
Koilocytes LSIL
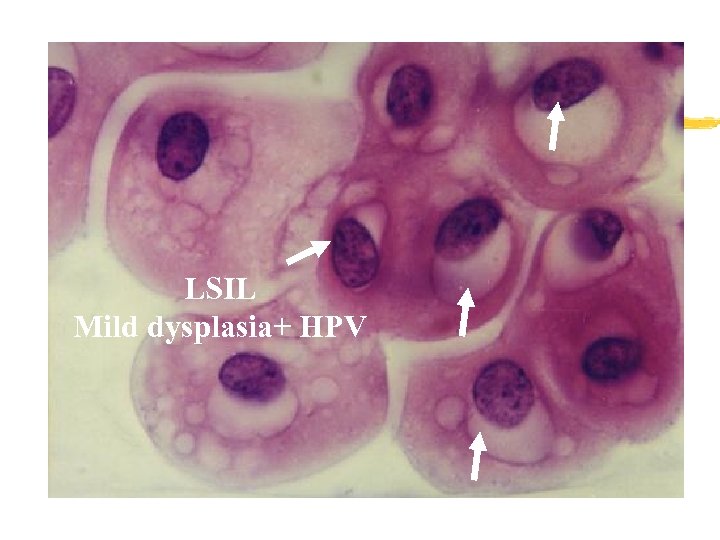 LSIL Mild dysplasia+ HPV
LSIL Mild dysplasia+ HPV
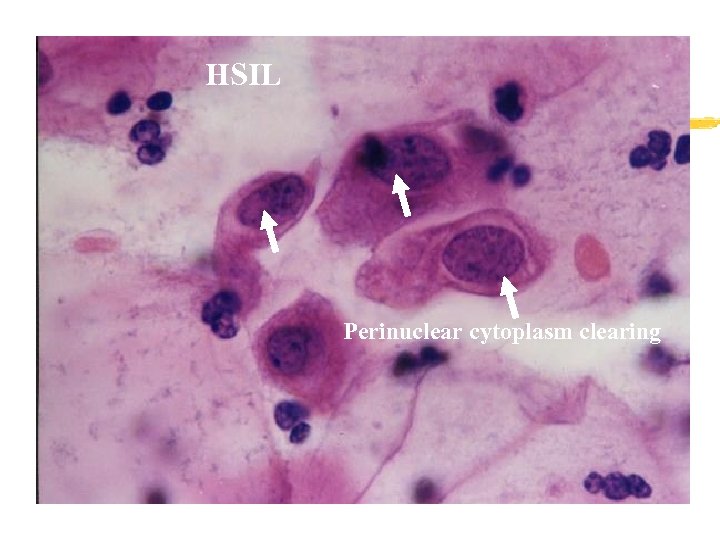 HSIL Perinuclear cytoplasm clearing
HSIL Perinuclear cytoplasm clearing
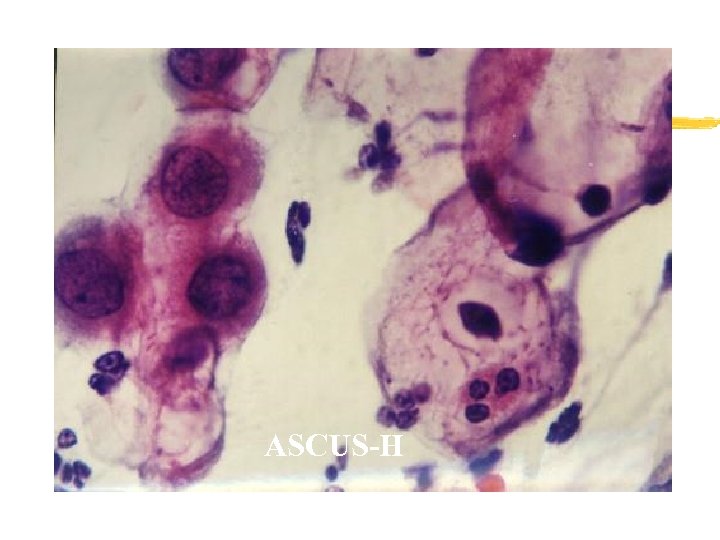 ASCUS-H
ASCUS-H
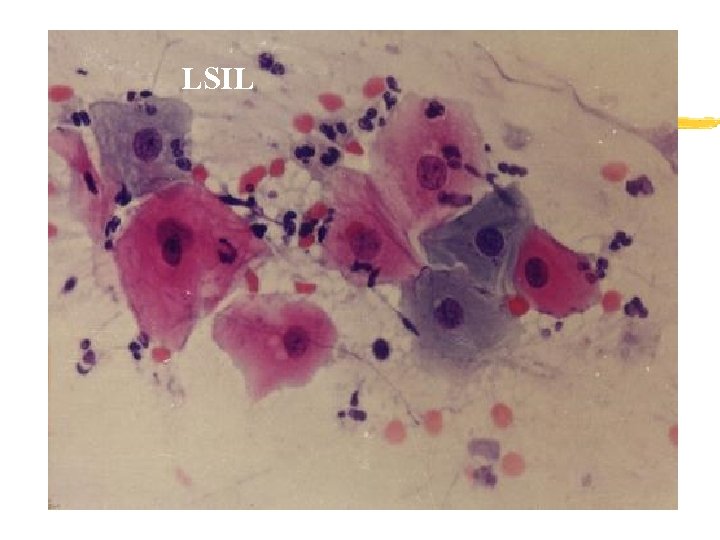 LSIL
LSIL
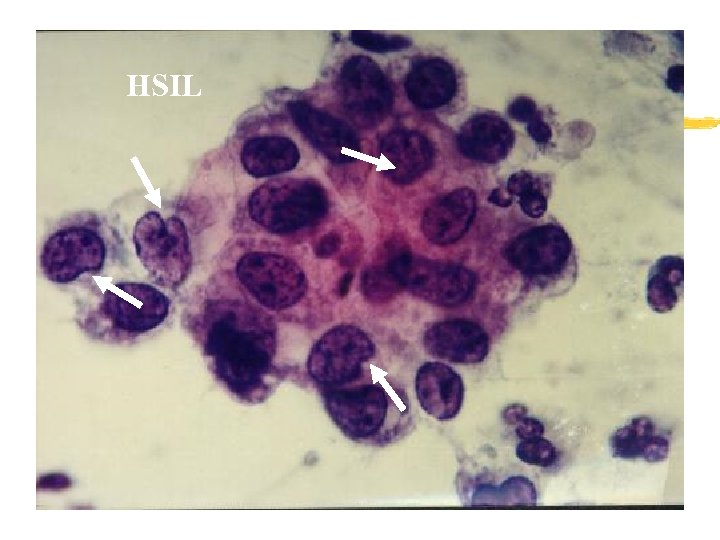 HSIL
HSIL
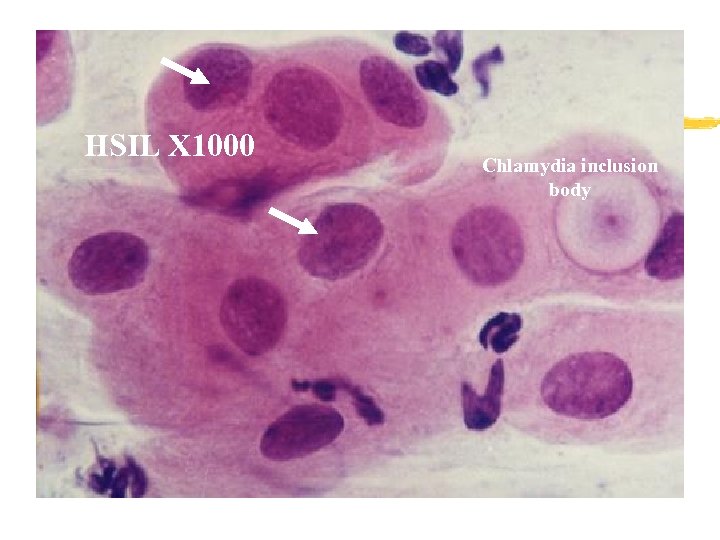 HSIL X 1000 Chlamydia inclusion body
HSIL X 1000 Chlamydia inclusion body
 Quality Control & Computer Assisted Rescreening Strategies Random rescreening by senior cytologists of slides that were originally classified as negative. Directed rescreening for slides of known patients at risk. The auto Pap 300 QC system The Pap Net system
Quality Control & Computer Assisted Rescreening Strategies Random rescreening by senior cytologists of slides that were originally classified as negative. Directed rescreening for slides of known patients at risk. The auto Pap 300 QC system The Pap Net system
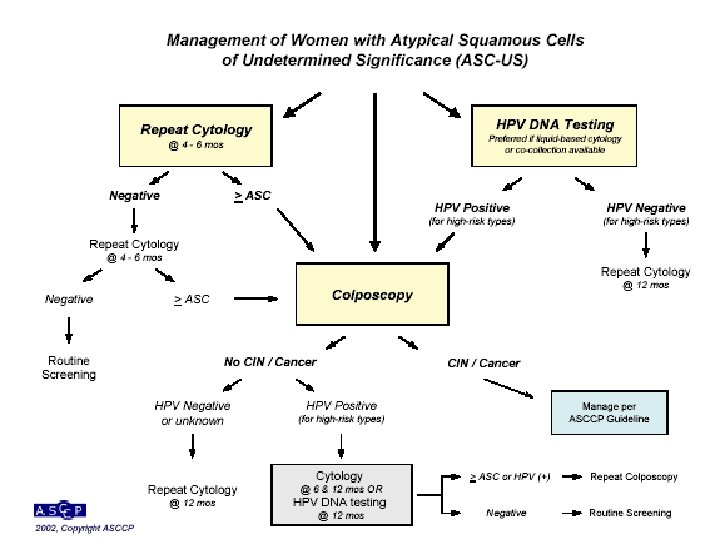
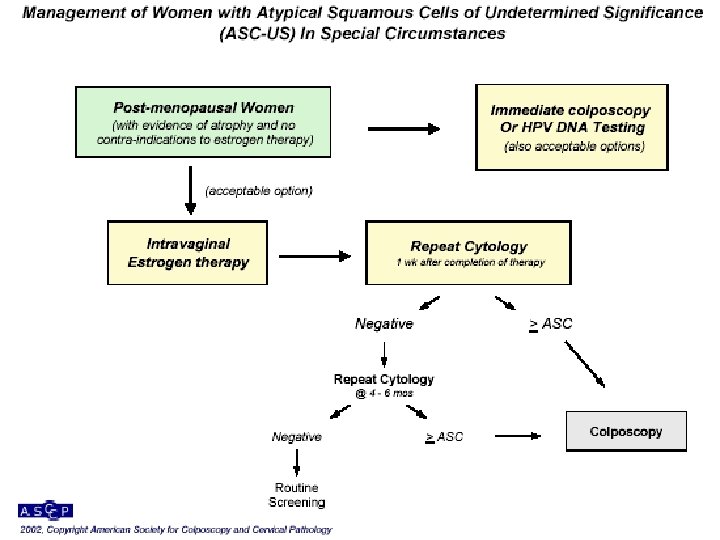
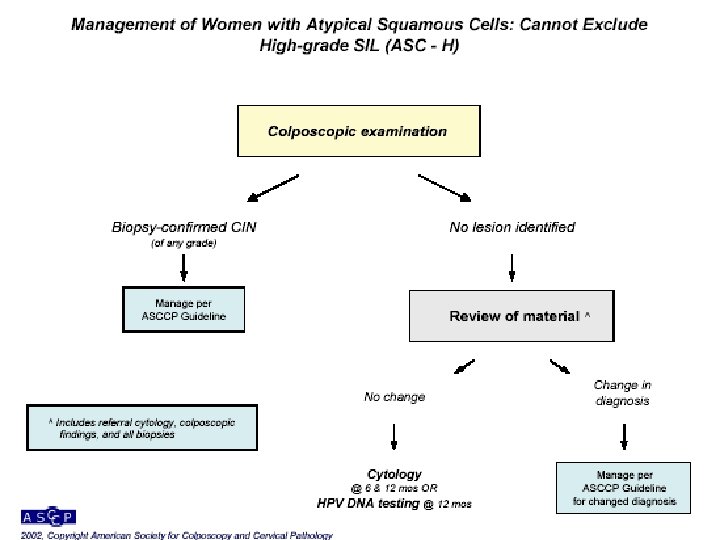
 End Of The First Part
End Of The First Part
 Visualizing the Cervix z. Unaided Naked eye examination z. Acetic acid-enhanced Naked eye examination (VIA) z. Cervicography z. Colposcopy
Visualizing the Cervix z. Unaided Naked eye examination z. Acetic acid-enhanced Naked eye examination (VIA) z. Cervicography z. Colposcopy
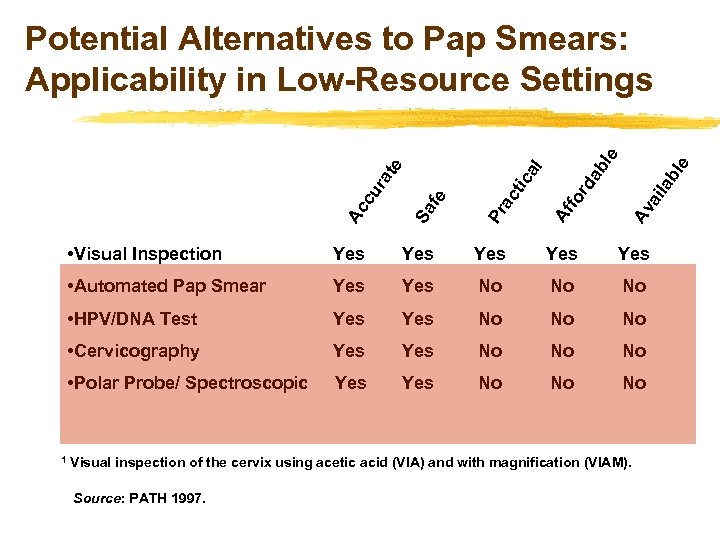 bl e ab l Av ai la rd Af fo tic ac Pr • Visual Inspection Yes Yes Yes • Automated Pap Smear Yes No No No • HPV/DNA Test Yes No No No • Cervicography Yes No No No • Polar Probe/ Spectroscopic 1 Sa fe Ac cu r at al e e Potential Alternatives to Pap Smears: Applicability in Low-Resource Settings Yes No No No Visual inspection of the cervix using acetic acid (VIA) and with magnification (VIAM). Source: PATH 1997.
bl e ab l Av ai la rd Af fo tic ac Pr • Visual Inspection Yes Yes Yes • Automated Pap Smear Yes No No No • HPV/DNA Test Yes No No No • Cervicography Yes No No No • Polar Probe/ Spectroscopic 1 Sa fe Ac cu r at al e e Potential Alternatives to Pap Smears: Applicability in Low-Resource Settings Yes No No No Visual inspection of the cervix using acetic acid (VIA) and with magnification (VIAM). Source: PATH 1997.
 Acetic Acid –enhanced Visual Inspection of the Cervix “VIA” 1. Acetic acid coagulates mucus, which becomes easier to remove. -allows a better view of the cervix 2. Acetic acid constricts the superficial vessels and blows up the columnar papillae so that they become pale. allows a better view of the squamocolumnar junction 3. Acetic acid causes dehydration of the cells and coagulation of cellular proteins, thereby reducing the transparency of the epithelium allows a better recognition of dysplastic epithelium
Acetic Acid –enhanced Visual Inspection of the Cervix “VIA” 1. Acetic acid coagulates mucus, which becomes easier to remove. -allows a better view of the cervix 2. Acetic acid constricts the superficial vessels and blows up the columnar papillae so that they become pale. allows a better view of the squamocolumnar junction 3. Acetic acid causes dehydration of the cells and coagulation of cellular proteins, thereby reducing the transparency of the epithelium allows a better recognition of dysplastic epithelium
 Abnormalities Seen After Acetic Acid Aceto-white Margins and surface White gland openings Mosaic & punctation Abnormal vessels
Abnormalities Seen After Acetic Acid Aceto-white Margins and surface White gland openings Mosaic & punctation Abnormal vessels
 What May Be Acetowhite NOT All acetowhite lesions are cancer Any of these epithelial changes can become acetowhite Healing or regenerating epithelium Congenital transformation zone Inflammation Immature squamous metaplasia HPV infection SIL Adenocarcinoma Invasive squamous cell carcinoma
What May Be Acetowhite NOT All acetowhite lesions are cancer Any of these epithelial changes can become acetowhite Healing or regenerating epithelium Congenital transformation zone Inflammation Immature squamous metaplasia HPV infection SIL Adenocarcinoma Invasive squamous cell carcinoma
 VIA: Conclusions Alternative to cytology or HPV testing Effective in identifying precancerous disease Identify cancers Effective in ruling out disease Specificity of VIA is likely to depend on: training intervention presence of STDs in population screened importance placed on picking up diseased cases Positive predictive value of VIA can be increased through sequential or risk-based triage screening
VIA: Conclusions Alternative to cytology or HPV testing Effective in identifying precancerous disease Identify cancers Effective in ruling out disease Specificity of VIA is likely to depend on: training intervention presence of STDs in population screened importance placed on picking up diseased cases Positive predictive value of VIA can be increased through sequential or risk-based triage screening
 The Alternative…Downstaging !!! The detection of the disease at an earlier stage when still curable… Just Insert a speculum and look at the cervix
The Alternative…Downstaging !!! The detection of the disease at an earlier stage when still curable… Just Insert a speculum and look at the cervix
 Warning signs of early cervical cancer 1. Yellowish and friable epithelium 2. Abnormal contour 3. Ulceration 4. Atypical vessels 5. Very severe colposcopic atypia 6. Large, significant lesion 7. Canal lesion, going out of range 8. Perimenopausal and post radiation
Warning signs of early cervical cancer 1. Yellowish and friable epithelium 2. Abnormal contour 3. Ulceration 4. Atypical vessels 5. Very severe colposcopic atypia 6. Large, significant lesion 7. Canal lesion, going out of range 8. Perimenopausal and post radiation
 Mimics of cervical cancer 1. Severe cervicitis e. g. , herpes, syphilis 2. Benign ulceration e. g. , trauma 3. Foreign body reaction 4. Granulomatous cervical conditions 5. Granuloma inguinale 6. Lymphogranuloma venereum 7. Schistosomiasis 8. Cervical condylomata Cololposcopy aids differentiation. Histology is the gold standard
Mimics of cervical cancer 1. Severe cervicitis e. g. , herpes, syphilis 2. Benign ulceration e. g. , trauma 3. Foreign body reaction 4. Granulomatous cervical conditions 5. Granuloma inguinale 6. Lymphogranuloma venereum 7. Schistosomiasis 8. Cervical condylomata Cololposcopy aids differentiation. Histology is the gold standard
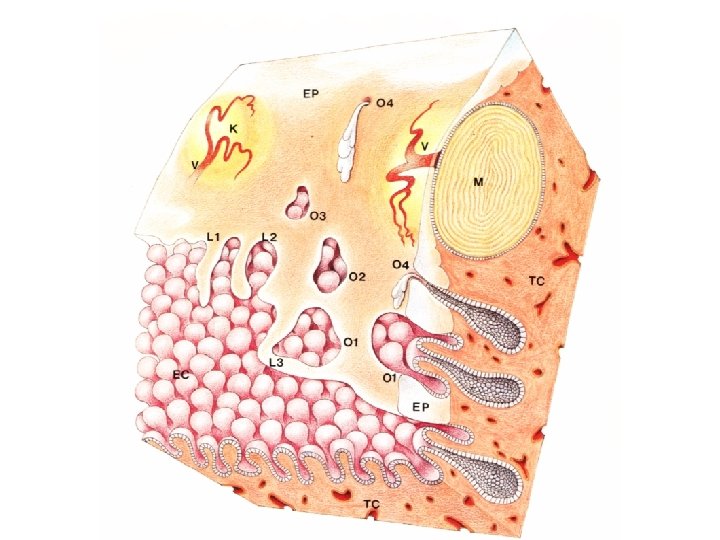
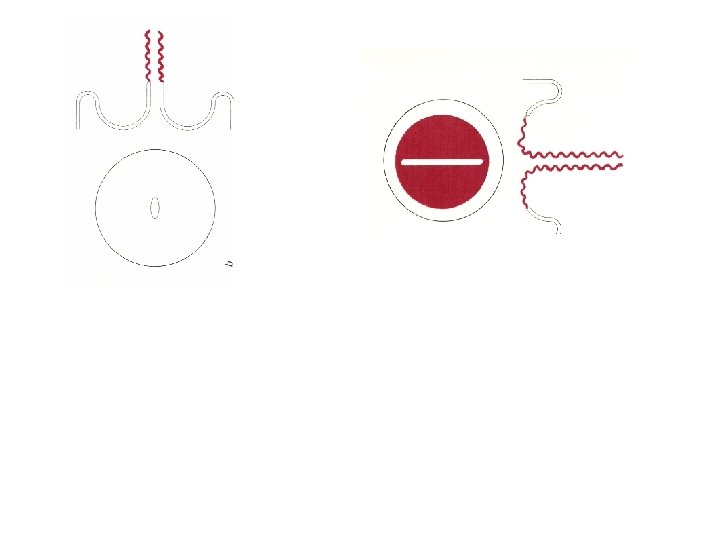
 What May Be Acetowhite NOT All acetowhite lesions are cancer Any of these epithelial changes can become acetowhite Healing or regenerating epithelium Congenital transformation zone Inflammation Immature squamous metaplasia HPV infection SIL Adenocarcinoma Invasive squamous cell carcinoma
What May Be Acetowhite NOT All acetowhite lesions are cancer Any of these epithelial changes can become acetowhite Healing or regenerating epithelium Congenital transformation zone Inflammation Immature squamous metaplasia HPV infection SIL Adenocarcinoma Invasive squamous cell carcinoma
 Visualizing the Cervix z. Unaided Naked eye examination z. Acetic acid-enhanced Naked eye examination (VIA) z. Visual Inspection with Lugol’s Iodine (VILI) z. Cervicography z. Colposcopy
Visualizing the Cervix z. Unaided Naked eye examination z. Acetic acid-enhanced Naked eye examination (VIA) z. Visual Inspection with Lugol’s Iodine (VILI) z. Cervicography z. Colposcopy
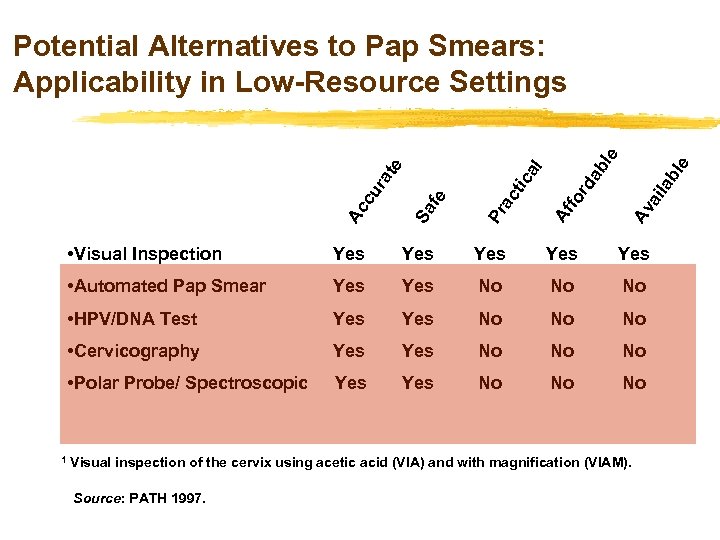 bl e ab l Av ai la rd Af fo tic ac Pr • Visual Inspection Yes Yes Yes • Automated Pap Smear Yes No No No • HPV/DNA Test Yes No No No • Cervicography Yes No No No • Polar Probe/ Spectroscopic 1 Sa fe Ac cu r at al e e Potential Alternatives to Pap Smears: Applicability in Low-Resource Settings Yes No No No Visual inspection of the cervix using acetic acid (VIA) and with magnification (VIAM). Source: PATH 1997.
bl e ab l Av ai la rd Af fo tic ac Pr • Visual Inspection Yes Yes Yes • Automated Pap Smear Yes No No No • HPV/DNA Test Yes No No No • Cervicography Yes No No No • Polar Probe/ Spectroscopic 1 Sa fe Ac cu r at al e e Potential Alternatives to Pap Smears: Applicability in Low-Resource Settings Yes No No No Visual inspection of the cervix using acetic acid (VIA) and with magnification (VIAM). Source: PATH 1997.
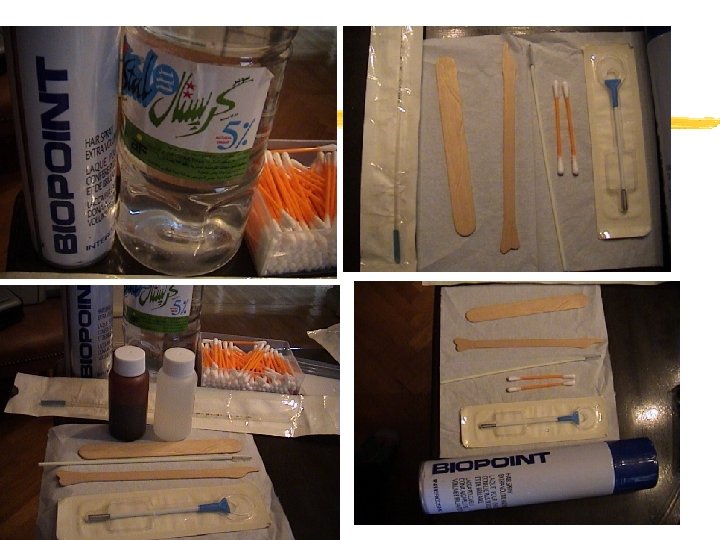
 Acetic Acid –enhanced Visual Inspection of the Cervix “VIA” 1. Acetic acid coagulates mucus, which becomes easier to remove. -allows a better view of the cervix 2. Acetic acid constricts the superficial vessels and blows up the columnar papillae so that they become pale. allows a better view of the squamocolumnar junction 3. Acetic acid causes dehydration of the cells and coagulation of cellular proteins, thereby reducing the transparency of the epithelium allows a better recognition of dysplastic epithelium
Acetic Acid –enhanced Visual Inspection of the Cervix “VIA” 1. Acetic acid coagulates mucus, which becomes easier to remove. -allows a better view of the cervix 2. Acetic acid constricts the superficial vessels and blows up the columnar papillae so that they become pale. allows a better view of the squamocolumnar junction 3. Acetic acid causes dehydration of the cells and coagulation of cellular proteins, thereby reducing the transparency of the epithelium allows a better recognition of dysplastic epithelium
 Abnormalities Seen After Acetic Acid Aceto-white Margins and surface White gland openings Mosaic & punctation Abnormal vessels
Abnormalities Seen After Acetic Acid Aceto-white Margins and surface White gland openings Mosaic & punctation Abnormal vessels
 What May Be Acetowhite NOT All acetowhite lesions are cancer Any of these epithelial changes can become acetowhite Healing or regenerating epithelium Congenital transformation zone Inflammation Immature squamous metaplasia HPV infection SIL Adenocarcinoma Invasive squamous cell carcinoma
What May Be Acetowhite NOT All acetowhite lesions are cancer Any of these epithelial changes can become acetowhite Healing or regenerating epithelium Congenital transformation zone Inflammation Immature squamous metaplasia HPV infection SIL Adenocarcinoma Invasive squamous cell carcinoma
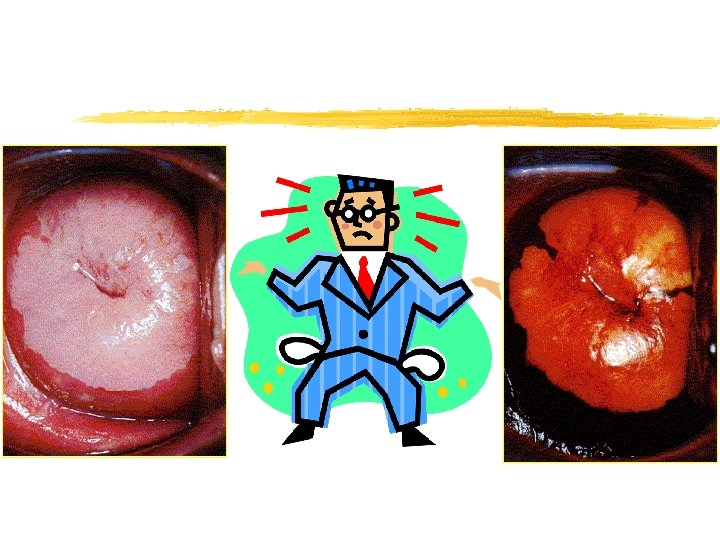

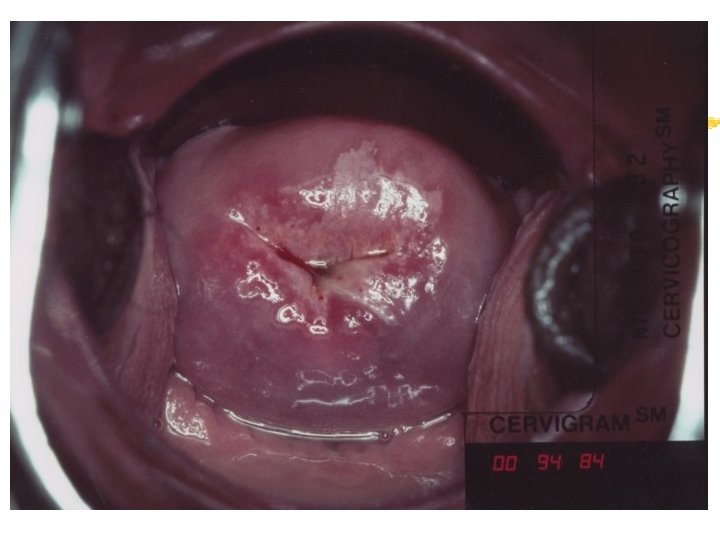
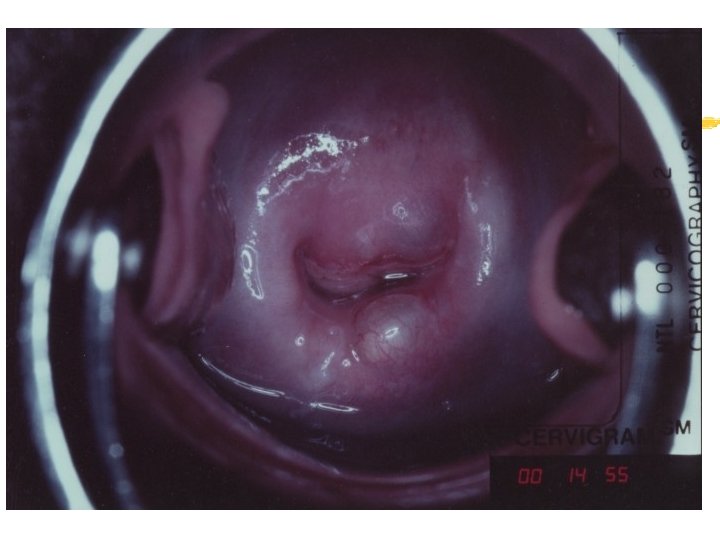
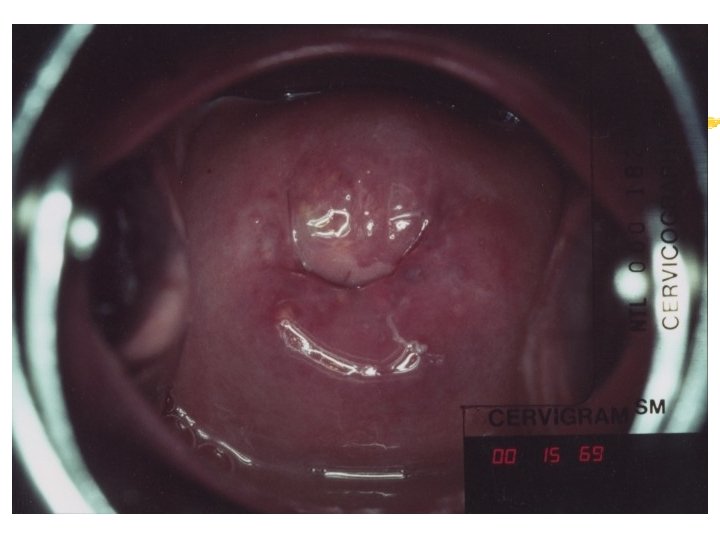
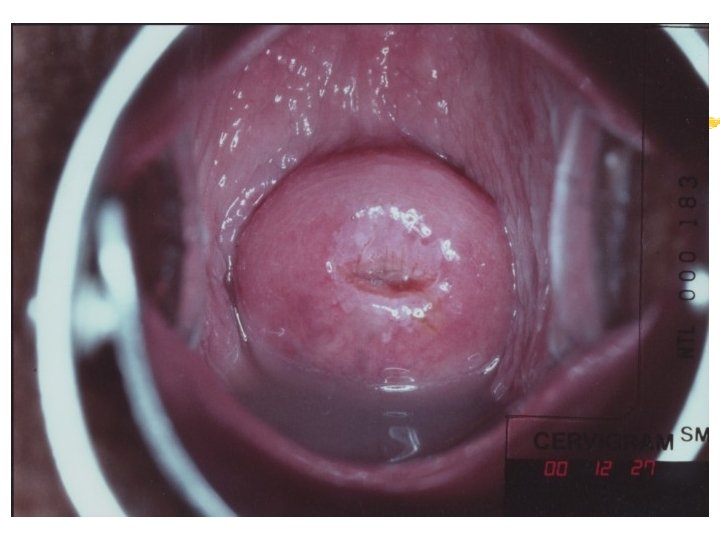
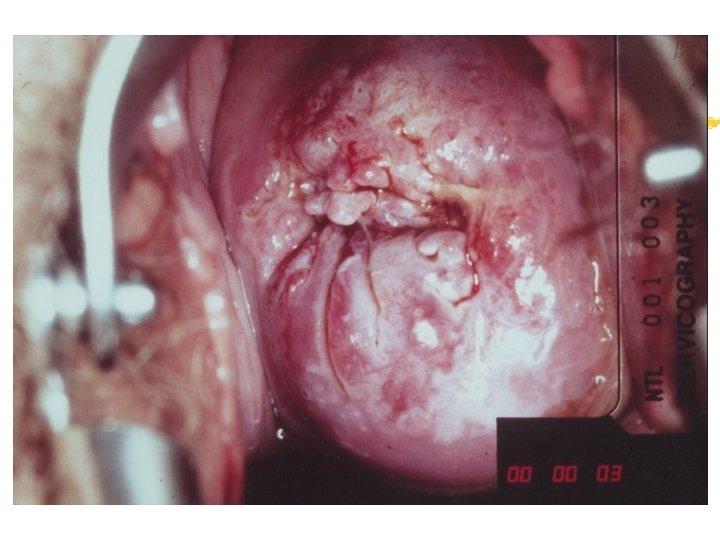
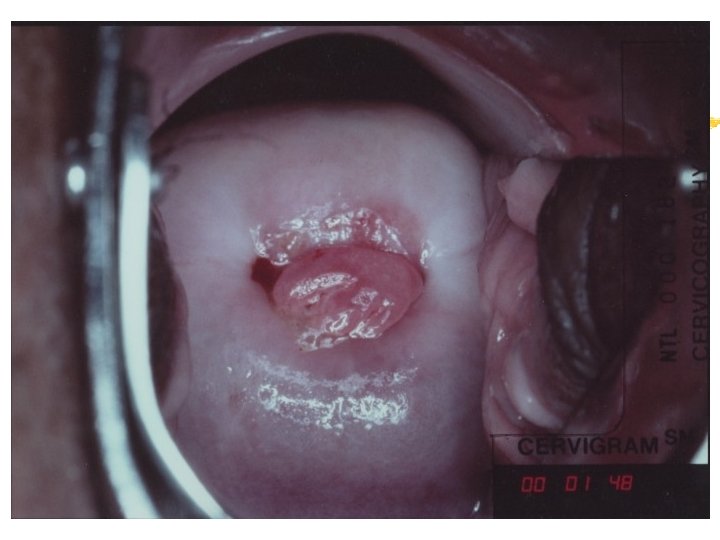
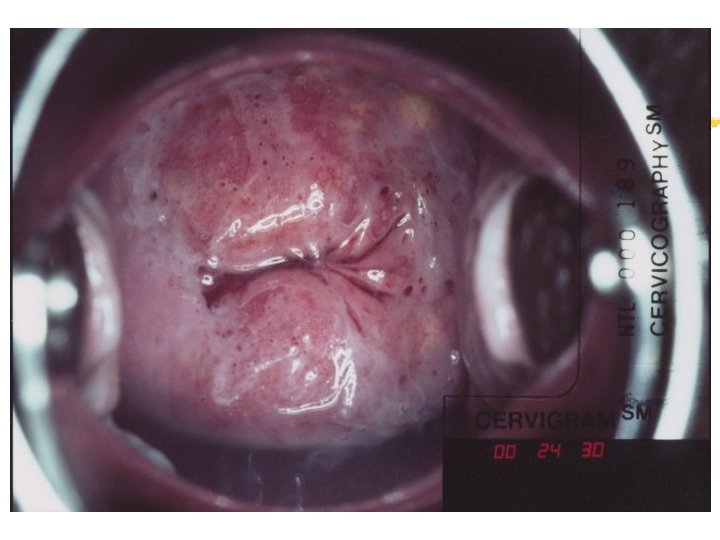
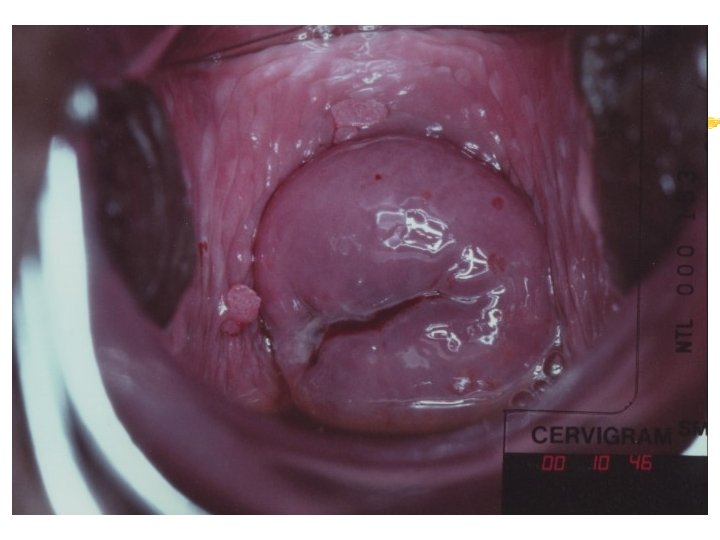
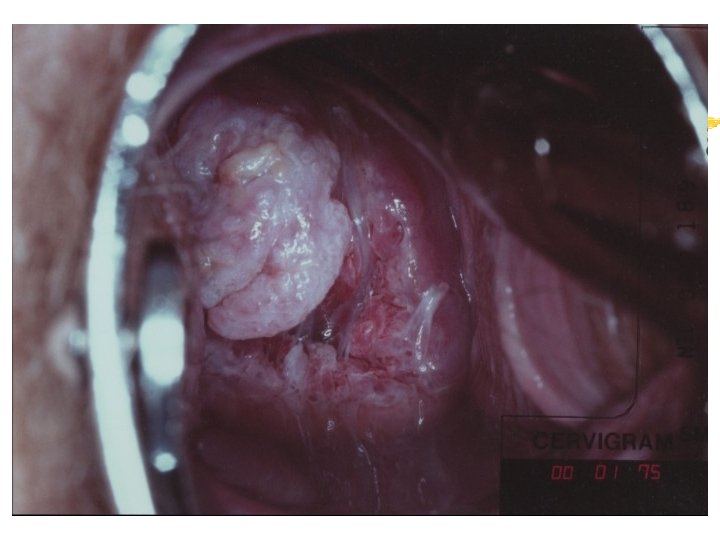
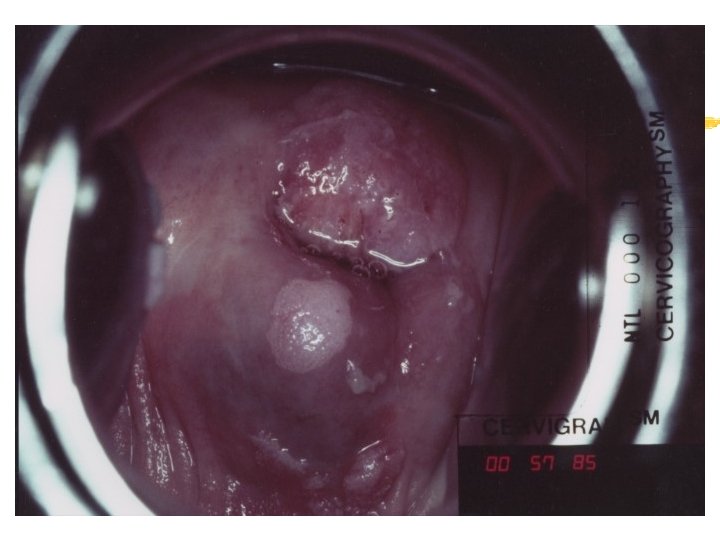
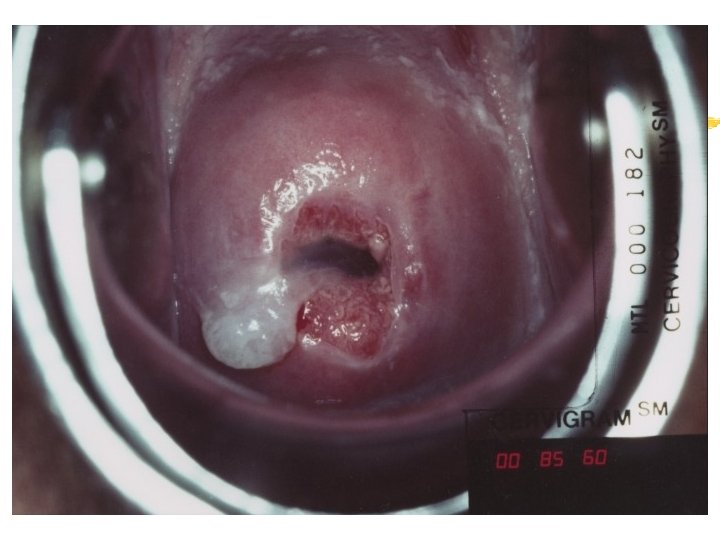
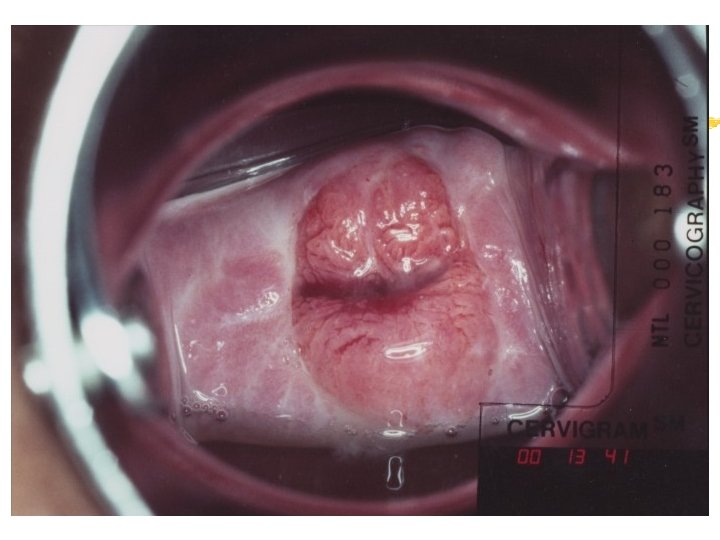
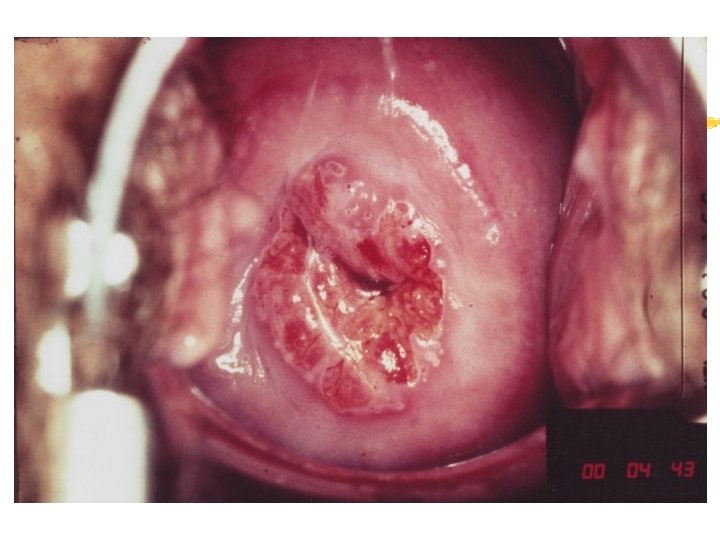
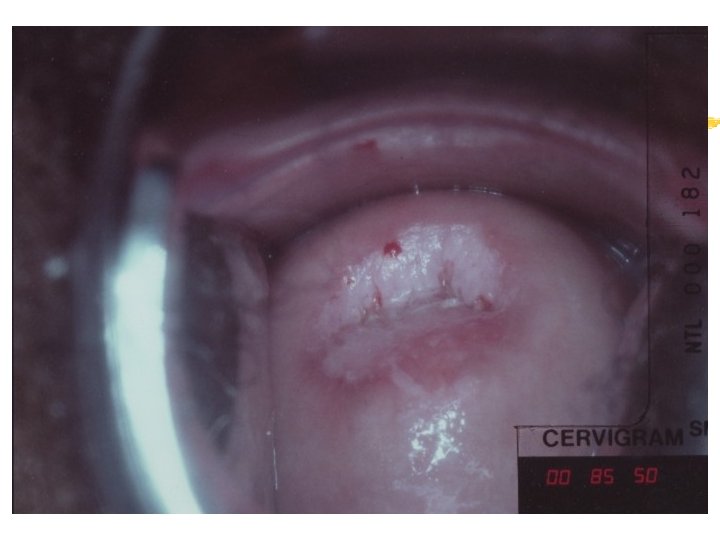
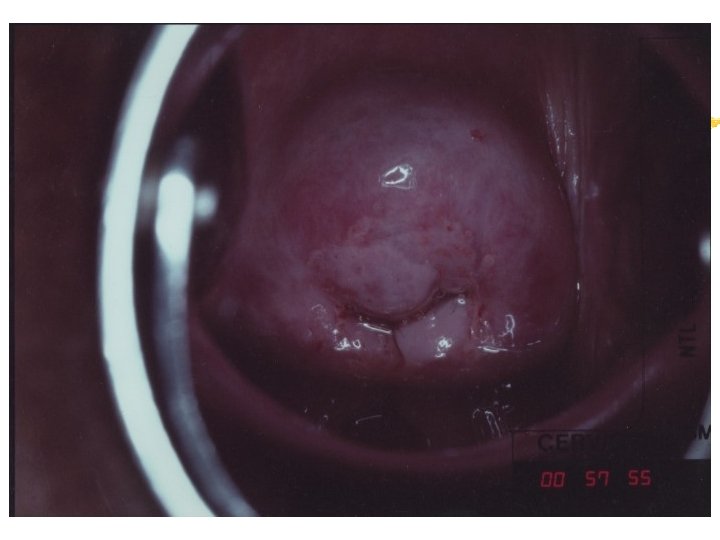
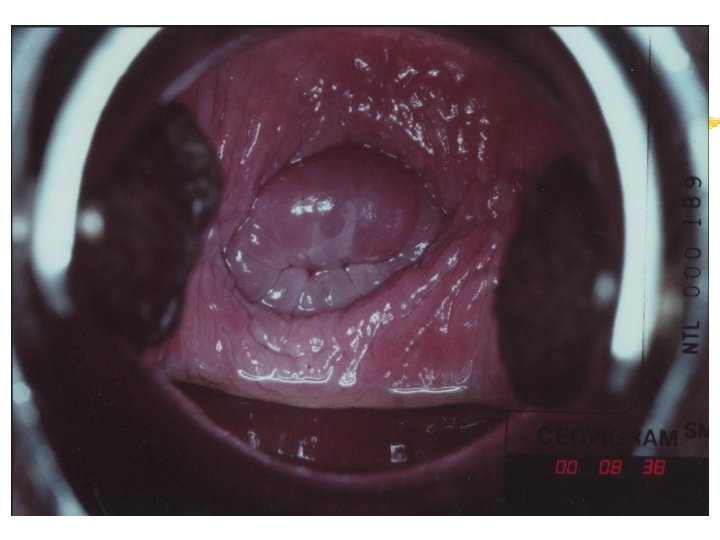
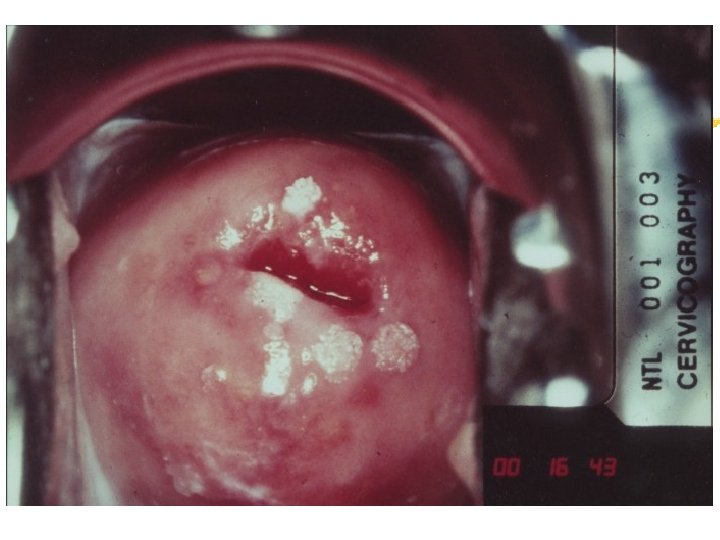
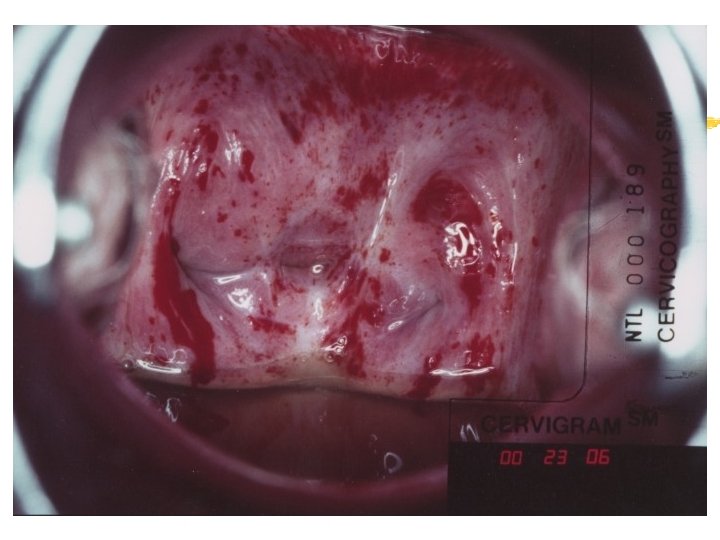
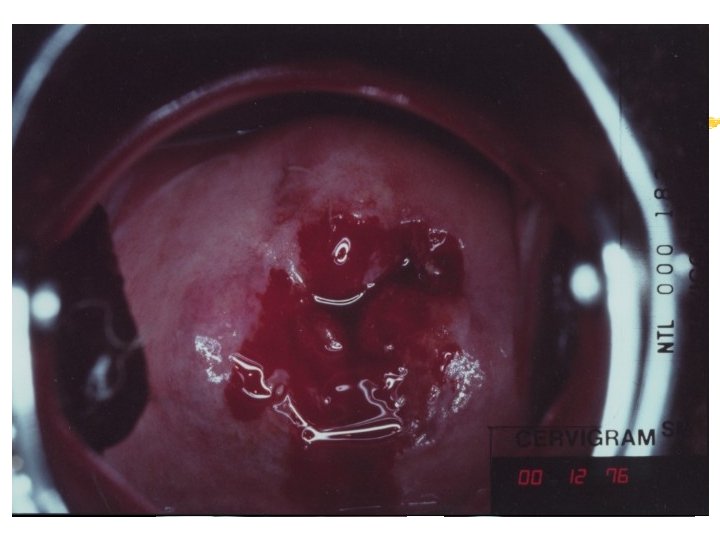
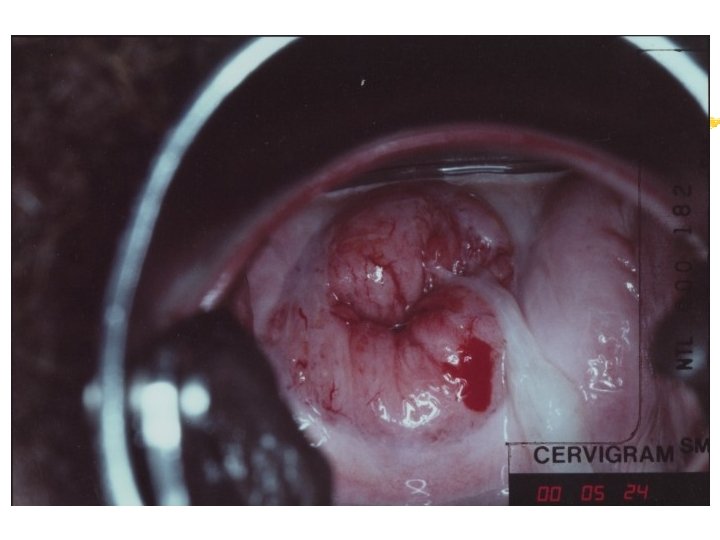
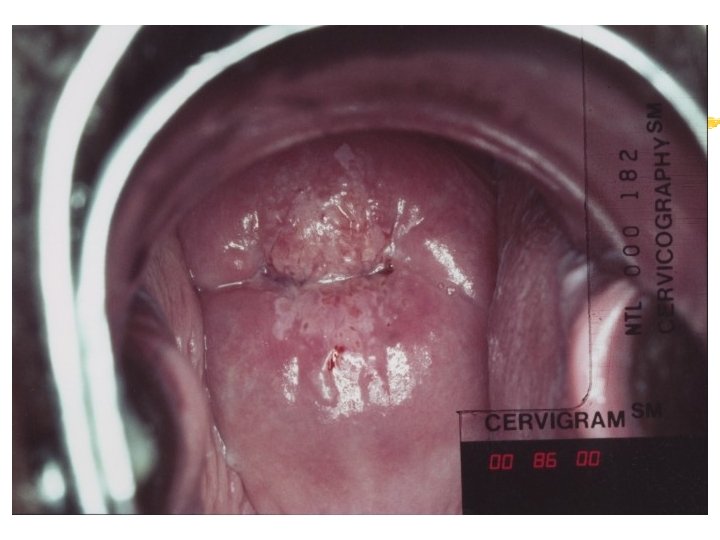
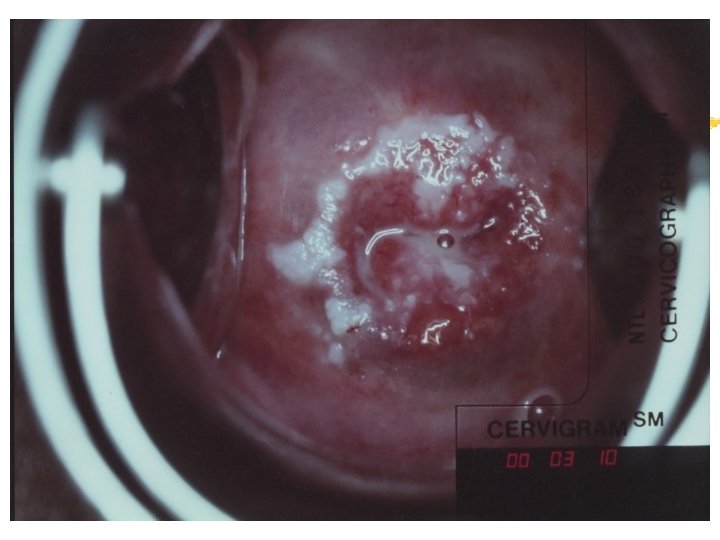
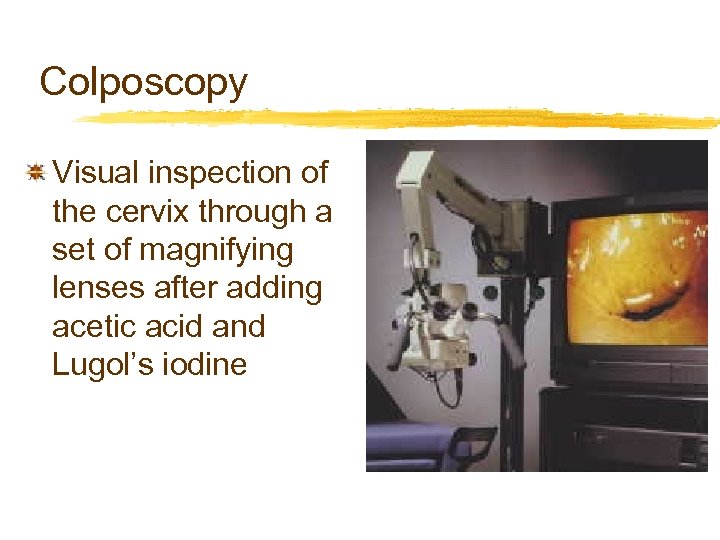 Colposcopy Visual inspection of the cervix through a set of magnifying lenses after adding acetic acid and Lugol’s iodine
Colposcopy Visual inspection of the cervix through a set of magnifying lenses after adding acetic acid and Lugol’s iodine
 Indications Grossly visible or palpable abnormality of the cervix ? ? Abnormal cervical cytology Positive screening test for cervical neoplasia such as spectroscopy, cervicography, speculoscopy Cervical cytology unsatisfactory due to unexplained inflammation History of in-utero diethylstilbestrol (DES) exposure Unexplained cervico-vaginal discharge Unexplained abnormal lower genital tract bleeding History of lower genital tract neoplasia (cervical, vaginal, vulvar) Post-treatment surveillance
Indications Grossly visible or palpable abnormality of the cervix ? ? Abnormal cervical cytology Positive screening test for cervical neoplasia such as spectroscopy, cervicography, speculoscopy Cervical cytology unsatisfactory due to unexplained inflammation History of in-utero diethylstilbestrol (DES) exposure Unexplained cervico-vaginal discharge Unexplained abnormal lower genital tract bleeding History of lower genital tract neoplasia (cervical, vaginal, vulvar) Post-treatment surveillance
 Colposcopic signs. Diagnostic between non significant TZ(NS) and highly significant (HS) NS -Acetic acid -Limits -Perilesional reaction -Situation -Surface -Epithelial trauma -Visual density -Vascularization -Glandular openings not visible precise absent generally near ectopy HS visible imprecise present rarely associated to ectopy flat coarse no ulcerations erosions, ulcerations stronger in periphery stronger near SCJ normal vessels atypical vessels absent present and often Keratinized
Colposcopic signs. Diagnostic between non significant TZ(NS) and highly significant (HS) NS -Acetic acid -Limits -Perilesional reaction -Situation -Surface -Epithelial trauma -Visual density -Vascularization -Glandular openings not visible precise absent generally near ectopy HS visible imprecise present rarely associated to ectopy flat coarse no ulcerations erosions, ulcerations stronger in periphery stronger near SCJ normal vessels atypical vessels absent present and often Keratinized
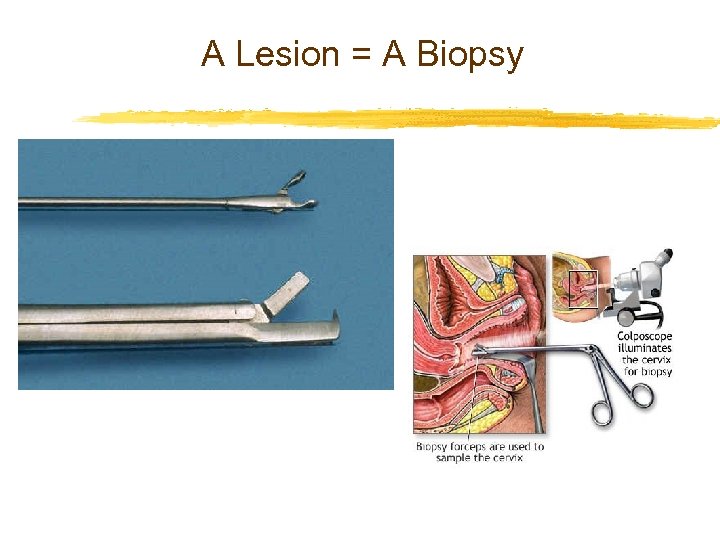 A Lesion = A Biopsy
A Lesion = A Biopsy
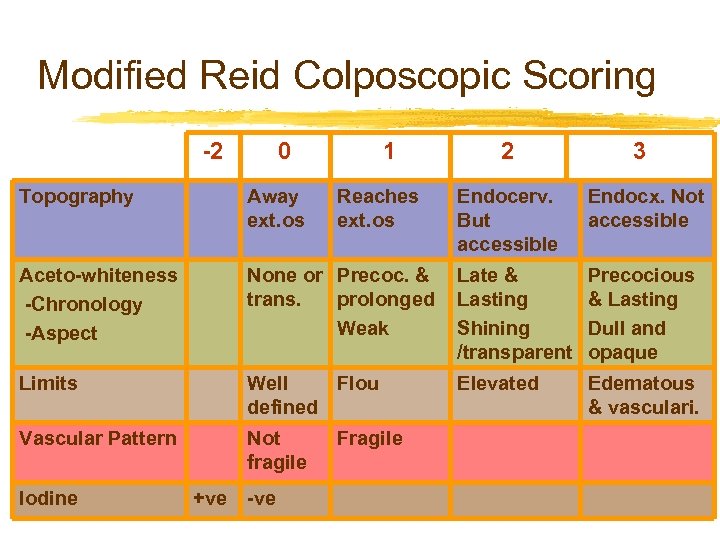 Modified Reid Colposcopic Scoring -2 0 1 3 Endocerv. But accessible Endocx. Not accessible Topography Away ext. os Aceto-whiteness -Chronology -Aspect None or Precoc. & trans. prolonged Weak Late & Lasting Shining /transparent Precocious & Lasting Dull and opaque Limits Well Flou defined Elevated Edematous & vasculari. Vascular Pattern Not fragile Iodine +ve -ve Reaches ext. os 2 Fragile
Modified Reid Colposcopic Scoring -2 0 1 3 Endocerv. But accessible Endocx. Not accessible Topography Away ext. os Aceto-whiteness -Chronology -Aspect None or Precoc. & trans. prolonged Weak Late & Lasting Shining /transparent Precocious & Lasting Dull and opaque Limits Well Flou defined Elevated Edematous & vasculari. Vascular Pattern Not fragile Iodine +ve -ve Reaches ext. os 2 Fragile
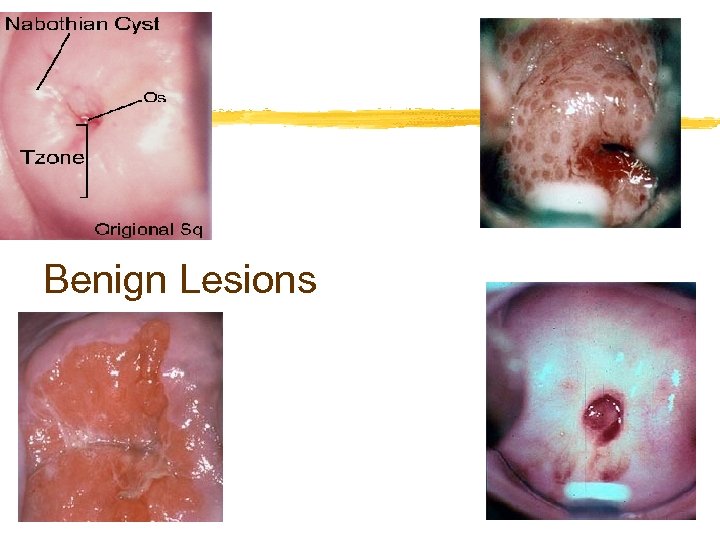 Benign Lesions
Benign Lesions
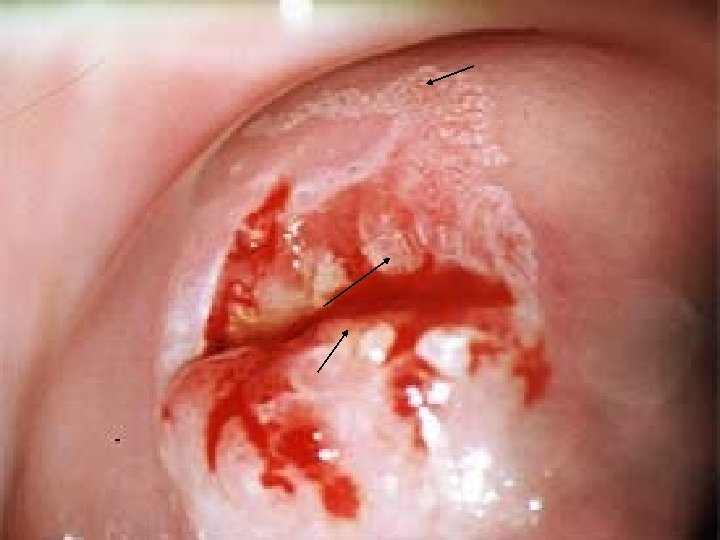
 Pitfalls of Colposcopy False SCJ caused by abrasion. The SCJ is identified by being the lower limit of the columnar epithelium and not the upper limit of the squamous epithelium. The SCJ up in the canal. The Previously Treated Cervix. Glandular Lesions. Missing Vaginal lesions.
Pitfalls of Colposcopy False SCJ caused by abrasion. The SCJ is identified by being the lower limit of the columnar epithelium and not the upper limit of the squamous epithelium. The SCJ up in the canal. The Previously Treated Cervix. Glandular Lesions. Missing Vaginal lesions.
 Atypical transformation zone 1. Acetowhite epithelium 2. Vascular structure a. Mosaic pattern b. Punctation c. Abnormal vessels 3. Leukoplakia
Atypical transformation zone 1. Acetowhite epithelium 2. Vascular structure a. Mosaic pattern b. Punctation c. Abnormal vessels 3. Leukoplakia
 Acetowhiteness 1. SIL …dehydration of nuclear dense lesion 2. HPV …keratin swelling in HPV infected cells 3. Immature squamous metaplasia 4. Healing/regenerating epithelium 5. Congenital transformation zone 6. Inflammation 7. Adednocarcinomas Invasive squamous carcinoma
Acetowhiteness 1. SIL …dehydration of nuclear dense lesion 2. HPV …keratin swelling in HPV infected cells 3. Immature squamous metaplasia 4. Healing/regenerating epithelium 5. Congenital transformation zone 6. Inflammation 7. Adednocarcinomas Invasive squamous carcinoma
 Vascular structure Mosaic pattern (cobblestone-like appearance). thick whitish areas of small fields polygonal or oval in shape surrounded by reddish borders (fine blood vessels) iodine negative
Vascular structure Mosaic pattern (cobblestone-like appearance). thick whitish areas of small fields polygonal or oval in shape surrounded by reddish borders (fine blood vessels) iodine negative
 Vascular structure Punctation … a series of fine red dots on a whitish background. Punctate vessels … dilated, elongated, often slightly twisted and irregular terminal vessels of the hairpin type.
Vascular structure Punctation … a series of fine red dots on a whitish background. Punctate vessels … dilated, elongated, often slightly twisted and irregular terminal vessels of the hairpin type.
 Cervicography: This is NOT Colposcopy High-quality colposcopic-type photography of the cervix Cervicoscope - Hand-held camera with a macrolens and a ring-flash Cervicogram - 35 -mm photo slide is taken Principles Recognition of lesions by means suitable magnification and illumination Fix up the problems of colposcopy 1. a less expensive form 2. noninvasive method 3. do not require expert skill
Cervicography: This is NOT Colposcopy High-quality colposcopic-type photography of the cervix Cervicoscope - Hand-held camera with a macrolens and a ring-flash Cervicogram - 35 -mm photo slide is taken Principles Recognition of lesions by means suitable magnification and illumination Fix up the problems of colposcopy 1. a less expensive form 2. noninvasive method 3. do not require expert skill
 Procedures of cervicography A) Taking a 35 -mm cervicogram (1) Insert speculum and open as wide as possible … expose an entire cervix and upper vagina (2) Apply first application of 5% acetic acid by dabbing … cleanse the cervix of blood and mucus (3) View the cervix through the cervicoscope … allows time to begin taking epithelial change (4) Apply second application of acetic acid. (5) Take two cervicogram pictures B) Developing the images C) Interpreting a magnified image that was projected on the screen (1) Negative if no definitive lesions are visible (2) Atypical if there was evidence of acetowhite lesion of doubtful significance (3) Positive if there was evidence of a minor or major-grade lesion or cancer
Procedures of cervicography A) Taking a 35 -mm cervicogram (1) Insert speculum and open as wide as possible … expose an entire cervix and upper vagina (2) Apply first application of 5% acetic acid by dabbing … cleanse the cervix of blood and mucus (3) View the cervix through the cervicoscope … allows time to begin taking epithelial change (4) Apply second application of acetic acid. (5) Take two cervicogram pictures B) Developing the images C) Interpreting a magnified image that was projected on the screen (1) Negative if no definitive lesions are visible (2) Atypical if there was evidence of acetowhite lesion of doubtful significance (3) Positive if there was evidence of a minor or major-grade lesion or cancer
 Why is cervicography needed? 1. Screening - the pap smear alone is not sensitive enough - broadened cytology criteria decreases specificity - triage of increased numbers of atypical smears 2. Documentation - Evaluation and follow-up - Research - Teaching
Why is cervicography needed? 1. Screening - the pap smear alone is not sensitive enough - broadened cytology criteria decreases specificity - triage of increased numbers of atypical smears 2. Documentation - Evaluation and follow-up - Research - Teaching
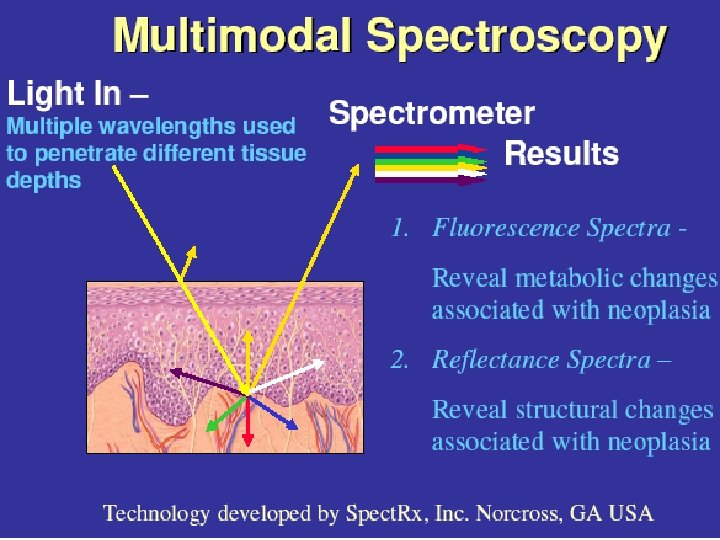
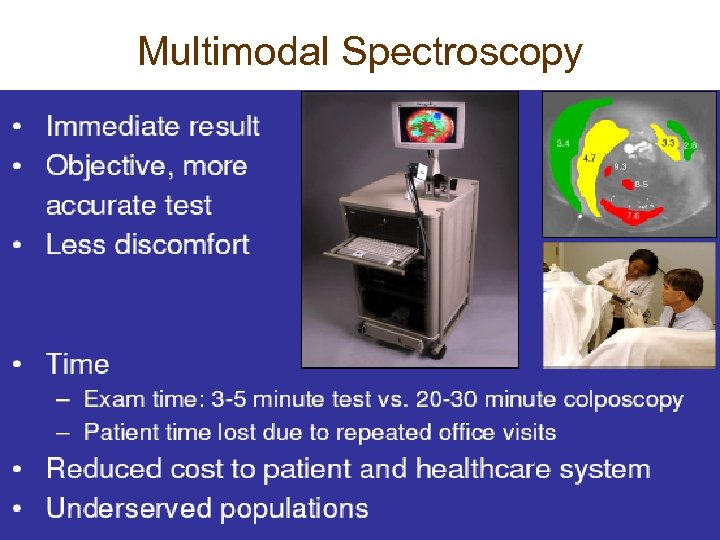 Multimodal Spectroscopy
Multimodal Spectroscopy
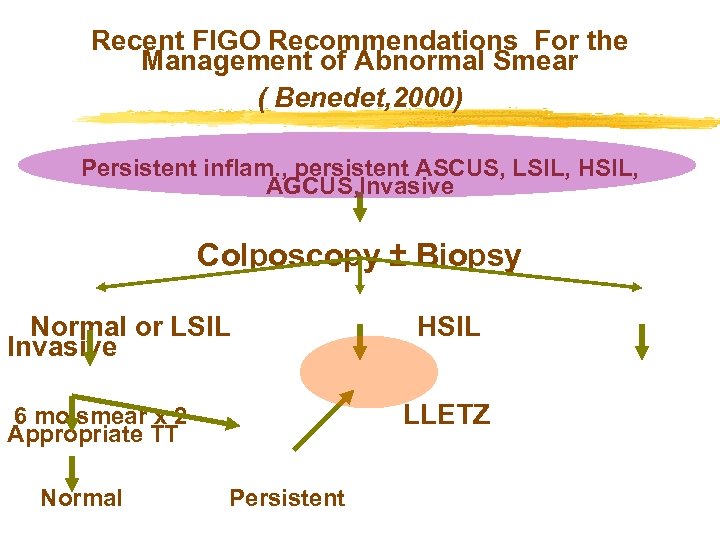 Recent FIGO Recommendations For the Management of Abnormal Smear ( Benedet, 2000) Persistent inflam. , persistent ASCUS, LSIL, HSIL, AGCUS, Invasive Colposcopy ± Biopsy Normal or LSIL Invasive LLETZ 6 mo smear x 2 Appropriate TT Normal HSIL Persistent
Recent FIGO Recommendations For the Management of Abnormal Smear ( Benedet, 2000) Persistent inflam. , persistent ASCUS, LSIL, HSIL, AGCUS, Invasive Colposcopy ± Biopsy Normal or LSIL Invasive LLETZ 6 mo smear x 2 Appropriate TT Normal HSIL Persistent
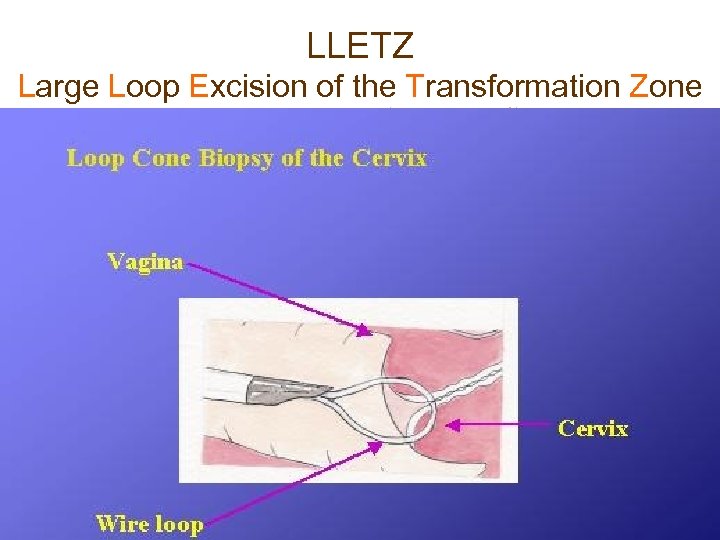 LLETZ Large Loop Excision of the Transformation Zone
LLETZ Large Loop Excision of the Transformation Zone
 Coming to an end… Cervical cancer is a preventable disease. It is even curable if caught at an early stage. Cervical screening is one of the most successful public health measures ever introduced for the prevention of cancer. Successful screening strategy should be coupled with an effective treating policy to eradicate pre-malignant lesions
Coming to an end… Cervical cancer is a preventable disease. It is even curable if caught at an early stage. Cervical screening is one of the most successful public health measures ever introduced for the prevention of cancer. Successful screening strategy should be coupled with an effective treating policy to eradicate pre-malignant lesions
 Still, many of the world's, most vulnerable women are not being screened. It is the implementation of comprehensive, organized, and quality cervical screening programs that demand our energies and attention as health professionals, policymakers, governments, and citizens.
Still, many of the world's, most vulnerable women are not being screened. It is the implementation of comprehensive, organized, and quality cervical screening programs that demand our energies and attention as health professionals, policymakers, governments, and citizens.


