8265611dc00c3fa4fc07eec314151337.ppt
- Количество слайдов: 48
 Cervical Cancer Screening 2010 and PID in pregnancy Delese La. Cour M. D. Pediatric and Adolescent Gynecology Johns Hopkins Community Physicians January 29, 2010
Cervical Cancer Screening 2010 and PID in pregnancy Delese La. Cour M. D. Pediatric and Adolescent Gynecology Johns Hopkins Community Physicians January 29, 2010

 Cervical Cancer Screening 1943 Papanicolaou and Trout published their monograph on the use of vaginal and cervical cytology as a screening tool for cervical neoplasm The incidence of cervical cancer has been reduced by 50% Cervical cancer has dropped from the #2 female cancer deaths to the 13 th
Cervical Cancer Screening 1943 Papanicolaou and Trout published their monograph on the use of vaginal and cervical cytology as a screening tool for cervical neoplasm The incidence of cervical cancer has been reduced by 50% Cervical cancer has dropped from the #2 female cancer deaths to the 13 th
 Types of Cervical Cancer Squamous cell Approximately 80 -90% of cervical cancers Adenocarcinoma 10% Clear cell cervical cancer Mucinous adenocarcinoma Adenosquamous Glassy cell carcinoma Stromal sarcoma Sarcoma botryoides Leiomyosarcoma Lymphoma Small cervical cancer Adenoid cystic carcinoma of the cervix
Types of Cervical Cancer Squamous cell Approximately 80 -90% of cervical cancers Adenocarcinoma 10% Clear cell cervical cancer Mucinous adenocarcinoma Adenosquamous Glassy cell carcinoma Stromal sarcoma Sarcoma botryoides Leiomyosarcoma Lymphoma Small cervical cancer Adenoid cystic carcinoma of the cervix
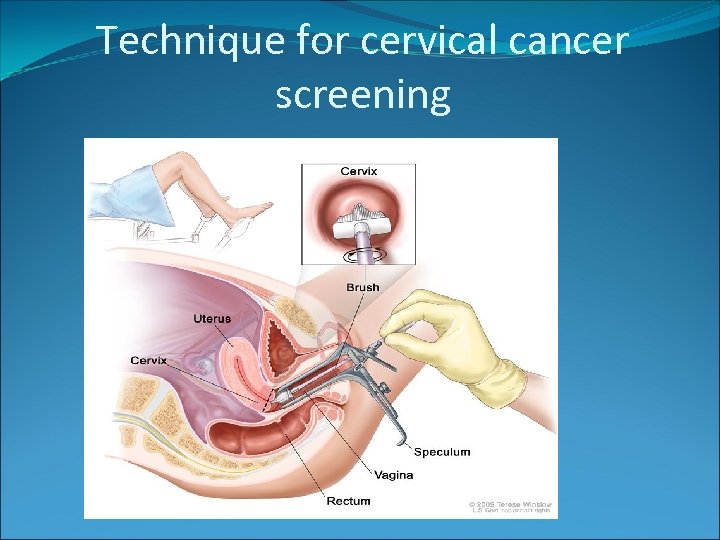 Technique for cervical cancer screening
Technique for cervical cancer screening
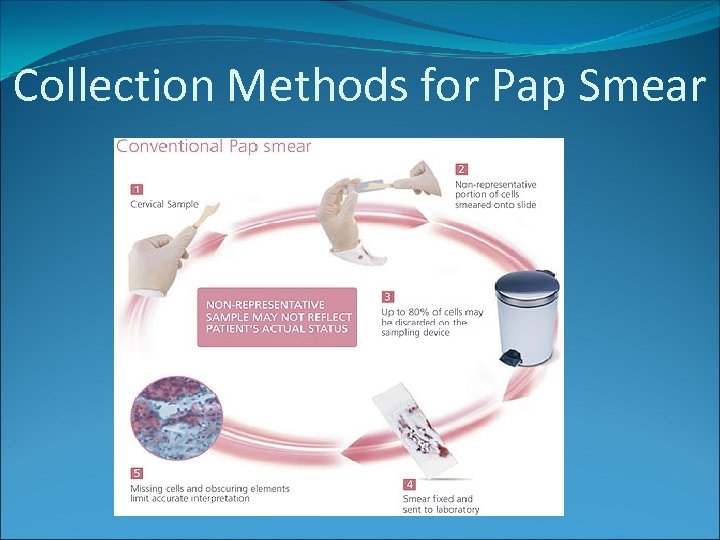 Collection Methods for Pap Smear
Collection Methods for Pap Smear
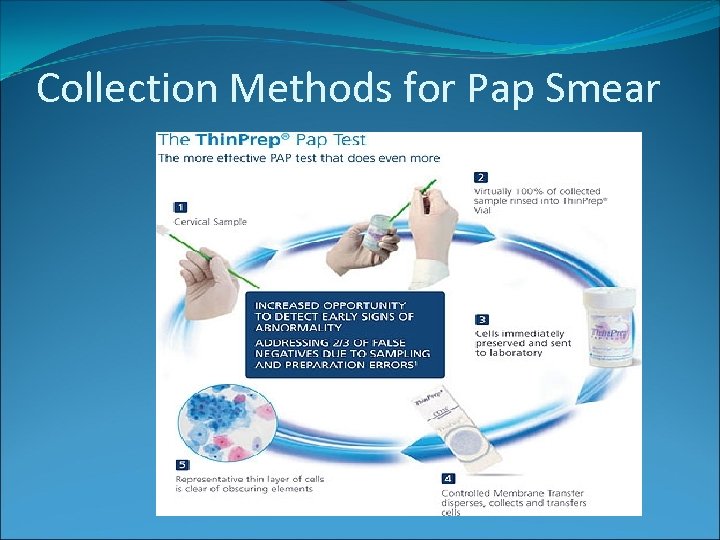 Collection Methods for Pap Smear
Collection Methods for Pap Smear
 Bethesda System 2001 SPECIMEN ADEQUACY Satisfactory for evaluation (note presence/absence of endocervical/ transformation zone component) Unsatisfactory for evaluation. . . Specimen rejected/not processed Specimen processed and examined, but unsatisfactory for evaluation of epithelial abnormality because GENERAL CATEGORIZATION (Optional) Negative for intraepithelial lesion or malignancy Epithelial cell abnormality INTERPRETATION/RESULT Negative for Intraepithelial Lesion or Malignancy Organisms Trichomonas vaginalis , Fungal oganisms consistent with Candida species Shift in flora suggestive of bacterial vaginosis Bacteria consistent with Actinomyces species Cellular changes consistent with herpes simplex virus Other non-neoplastic findings Reactive cellular changes associated with inflammation radiation intrauterine contraceptive device Glandular cells status posthysterectomy Atrophy
Bethesda System 2001 SPECIMEN ADEQUACY Satisfactory for evaluation (note presence/absence of endocervical/ transformation zone component) Unsatisfactory for evaluation. . . Specimen rejected/not processed Specimen processed and examined, but unsatisfactory for evaluation of epithelial abnormality because GENERAL CATEGORIZATION (Optional) Negative for intraepithelial lesion or malignancy Epithelial cell abnormality INTERPRETATION/RESULT Negative for Intraepithelial Lesion or Malignancy Organisms Trichomonas vaginalis , Fungal oganisms consistent with Candida species Shift in flora suggestive of bacterial vaginosis Bacteria consistent with Actinomyces species Cellular changes consistent with herpes simplex virus Other non-neoplastic findings Reactive cellular changes associated with inflammation radiation intrauterine contraceptive device Glandular cells status posthysterectomy Atrophy
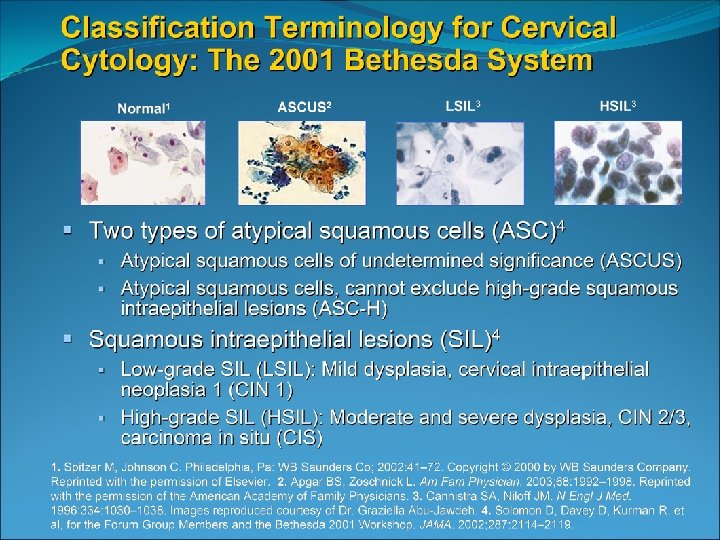
 Bethesda System 2001 Epithelial Cell Abnormalities Squamous cell Atypical squamous cells (ASC) of undetermined significance (ASC-US) cannot exclude HSIL (ASC-H) Low-grade squamous intraepithelial lesion (LSIL) encompassing: human papillomavirus/mild dysplasia/cervical intraepithelial neoplasia (CIN) 1 High-grade squamous intraepithelial lesion (HSIL) moderate and severe dysplasia, carcinoma in situ; CIN 2 and CIN 3 Squamous cell carcinoma Glandular cell Atypical glandular cells (AGC) Atypical glandular cells, favor neoplastic Endocervical adenocarcinoma in situ (AIS) Adenocarcinoma
Bethesda System 2001 Epithelial Cell Abnormalities Squamous cell Atypical squamous cells (ASC) of undetermined significance (ASC-US) cannot exclude HSIL (ASC-H) Low-grade squamous intraepithelial lesion (LSIL) encompassing: human papillomavirus/mild dysplasia/cervical intraepithelial neoplasia (CIN) 1 High-grade squamous intraepithelial lesion (HSIL) moderate and severe dysplasia, carcinoma in situ; CIN 2 and CIN 3 Squamous cell carcinoma Glandular cell Atypical glandular cells (AGC) Atypical glandular cells, favor neoplastic Endocervical adenocarcinoma in situ (AIS) Adenocarcinoma
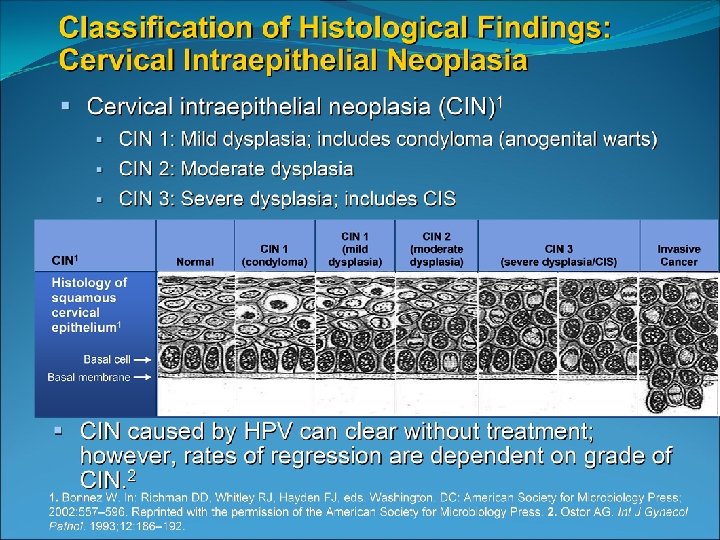
 Cervical cancer screening should begin at age 21 A) High prevalence of HPV infection in teenagers B) Most dysplasia regresses spontaneously in adolescents C) Invasive cervical cancer is rare in those younger than 21 D) Potential for adverse effects of side effects American College of Obstetrics and Gynecology Practice Bulletin No 109, Dec 2009
Cervical cancer screening should begin at age 21 A) High prevalence of HPV infection in teenagers B) Most dysplasia regresses spontaneously in adolescents C) Invasive cervical cancer is rare in those younger than 21 D) Potential for adverse effects of side effects American College of Obstetrics and Gynecology Practice Bulletin No 109, Dec 2009
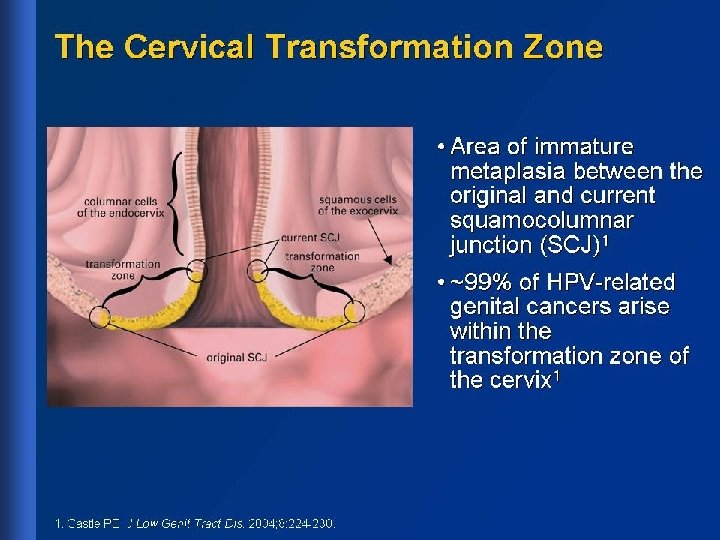
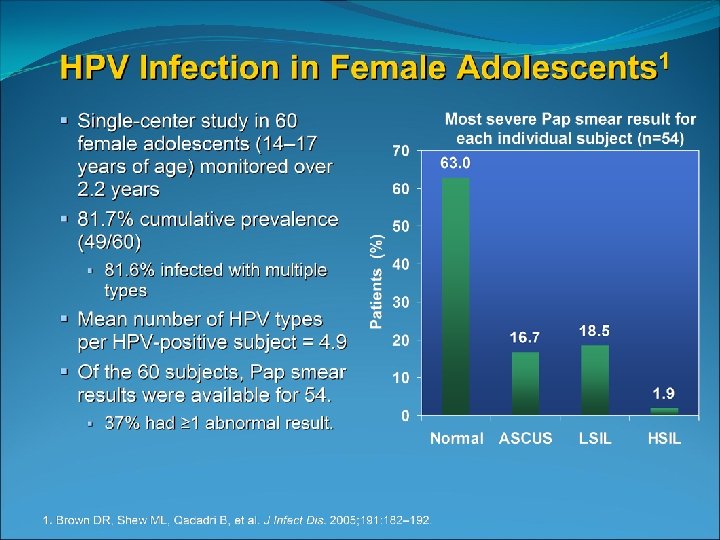
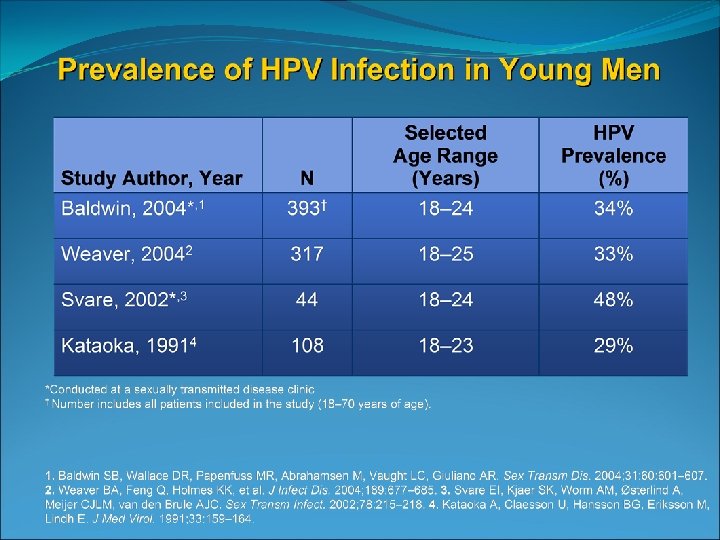
 High prevalence of HPV infection in teenagers
High prevalence of HPV infection in teenagers
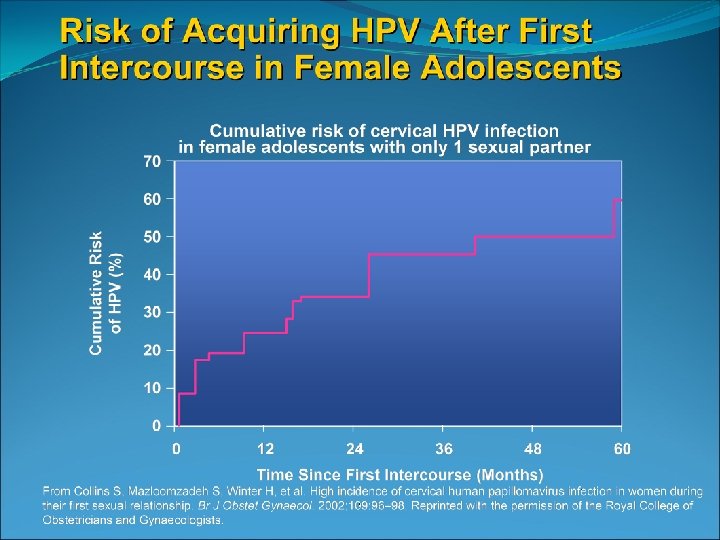
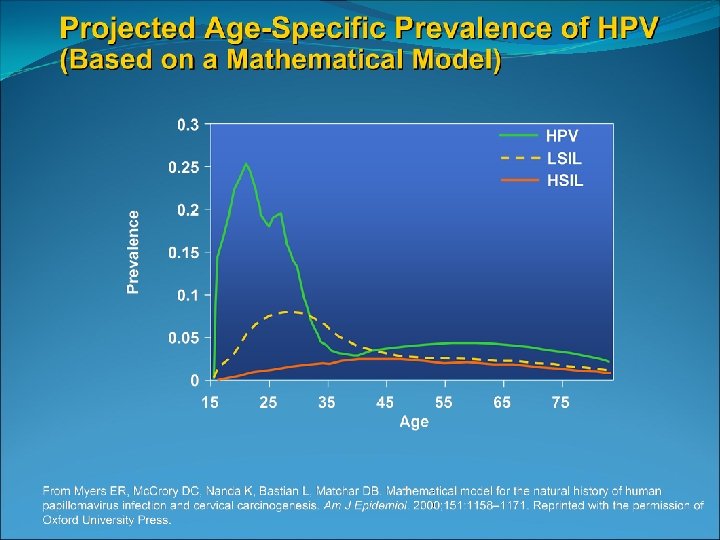
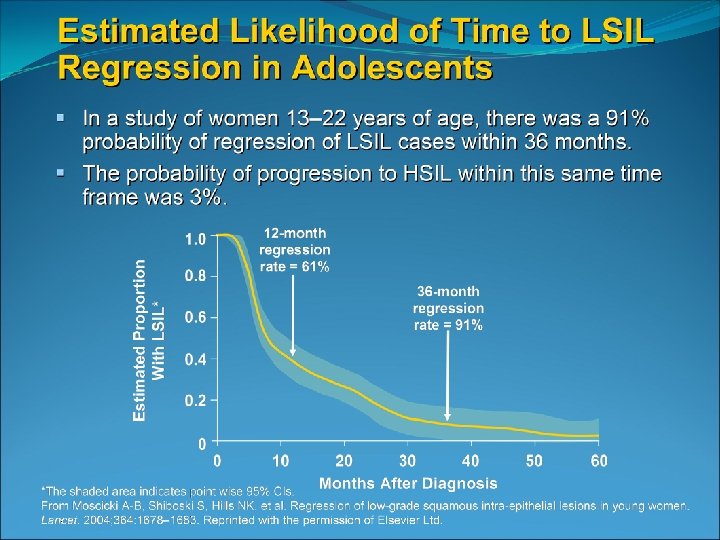
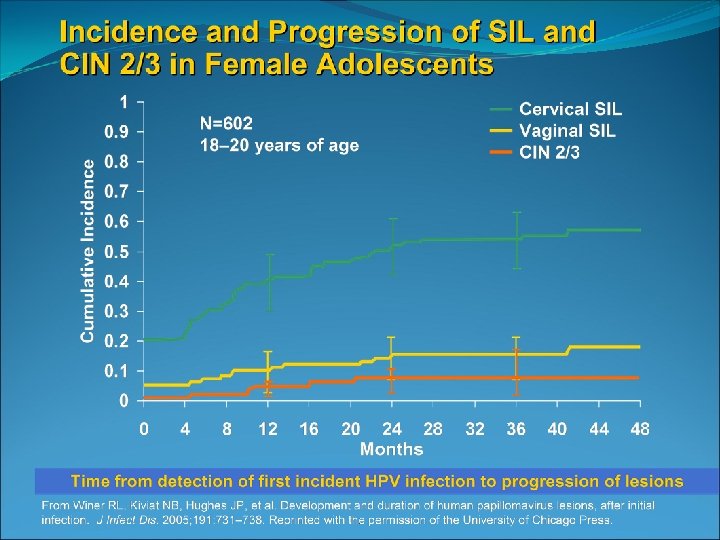
 Most dysplasia regresses spontaneously in adolescents A prospective study of 187 women aged 18 -22 years old found that LSIL had reverted to negative in 61% after 1 year and 91% after 3 years Only 3% progressed to CIN 3 Two smaller studies of adolescent females with biopsy confirmed CIN 2 showed 65 -75% regression after 18 months and 36 months ACOG practice bulletin 2009
Most dysplasia regresses spontaneously in adolescents A prospective study of 187 women aged 18 -22 years old found that LSIL had reverted to negative in 61% after 1 year and 91% after 3 years Only 3% progressed to CIN 3 Two smaller studies of adolescent females with biopsy confirmed CIN 2 showed 65 -75% regression after 18 months and 36 months ACOG practice bulletin 2009
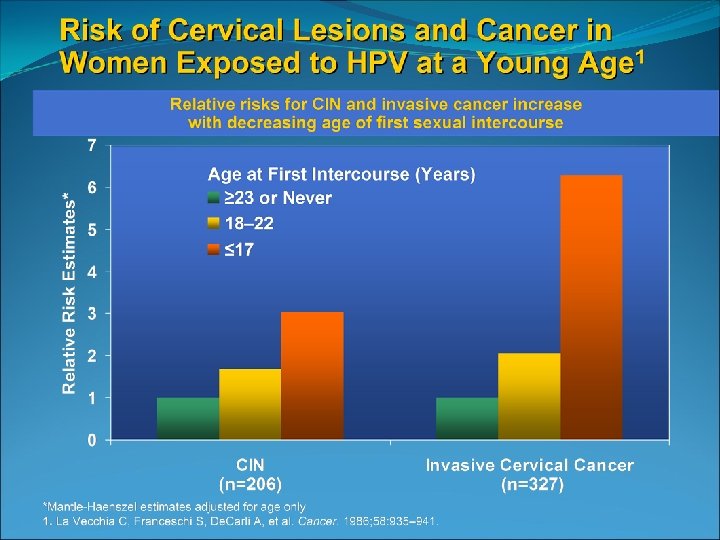
 Invasive cervical cancer is rare in those younger than 21 Only 0. 1 % of cervical cancers occur before age 21 National data from 1998 through 2003 identified 14 cases of invasive cancer /year in those ages 15 -19 SEER 2002 -2006 incidence rate of 1 -2 cases per 1, 000 females aged 15 -19 (Surveillance Epidemiology and End Results)
Invasive cervical cancer is rare in those younger than 21 Only 0. 1 % of cervical cancers occur before age 21 National data from 1998 through 2003 identified 14 cases of invasive cancer /year in those ages 15 -19 SEER 2002 -2006 incidence rate of 1 -2 cases per 1, 000 females aged 15 -19 (Surveillance Epidemiology and End Results)
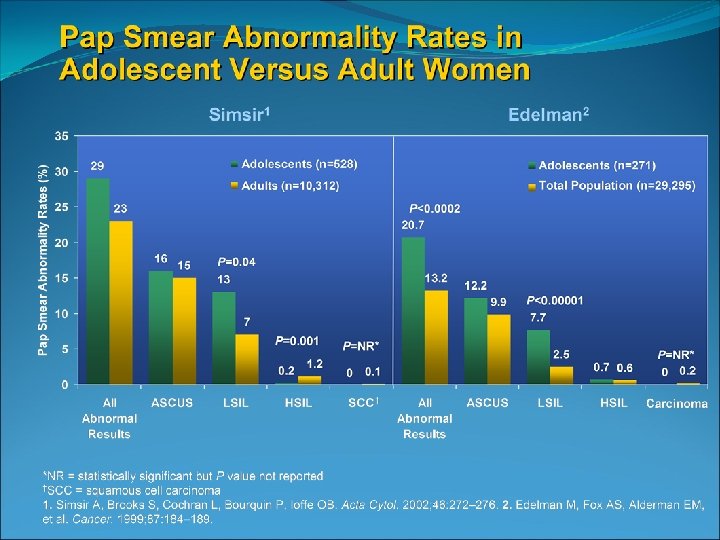
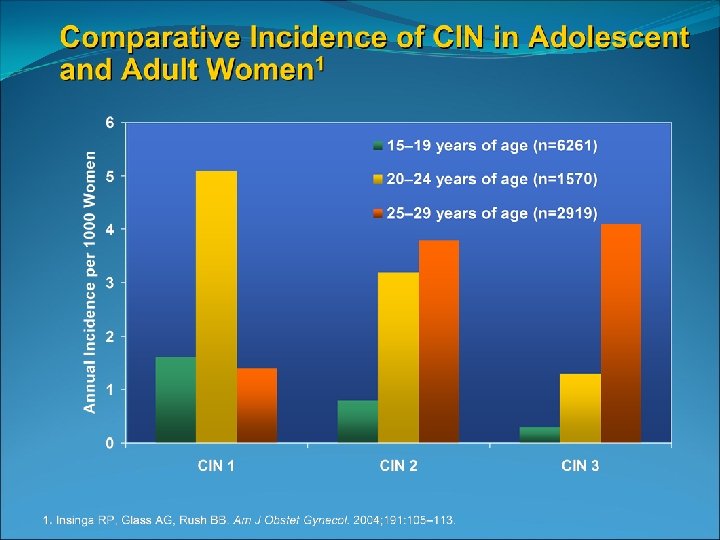
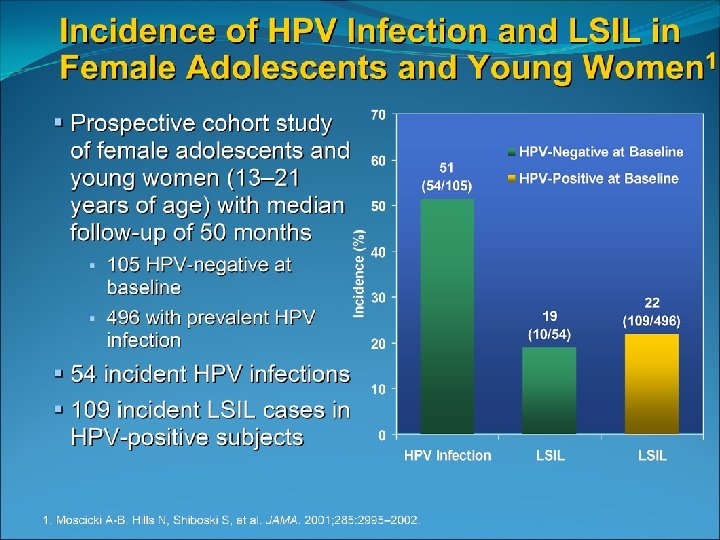
 Potential for adverse effects of side effects Significantly increased risk of : Preterm birth Low birth weight Neonatal intensive care admissions For every 18 LEEPs preformed there will be an additional preterm birth Suh-Burgmann B and Kinney W 2006 ASCCP Vol 10 , Issue 2, 2006
Potential for adverse effects of side effects Significantly increased risk of : Preterm birth Low birth weight Neonatal intensive care admissions For every 18 LEEPs preformed there will be an additional preterm birth Suh-Burgmann B and Kinney W 2006 ASCCP Vol 10 , Issue 2, 2006
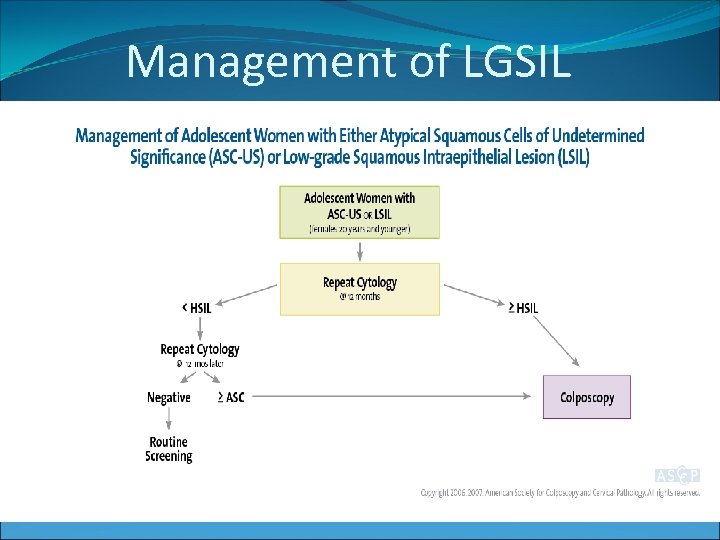 Management of LGSIL
Management of LGSIL
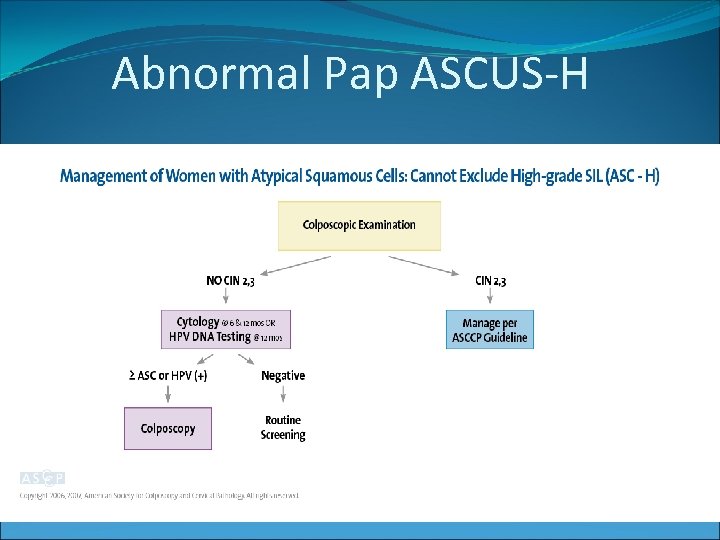 Abnormal Pap ASCUS-H
Abnormal Pap ASCUS-H
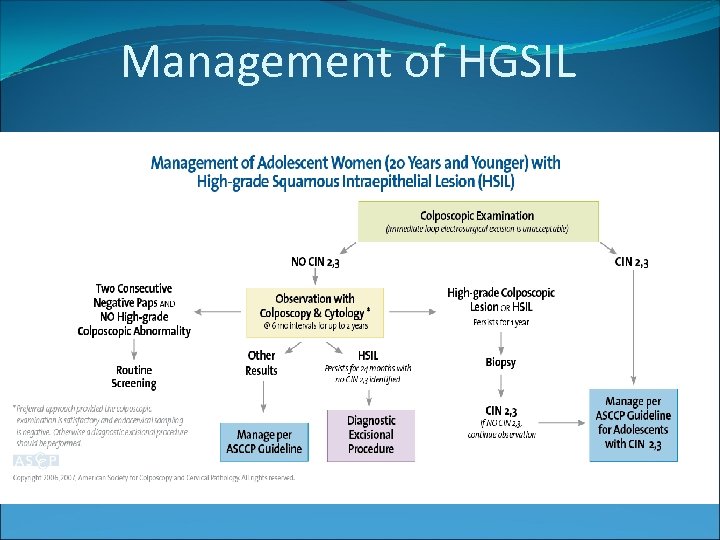 Management of HGSIL
Management of HGSIL
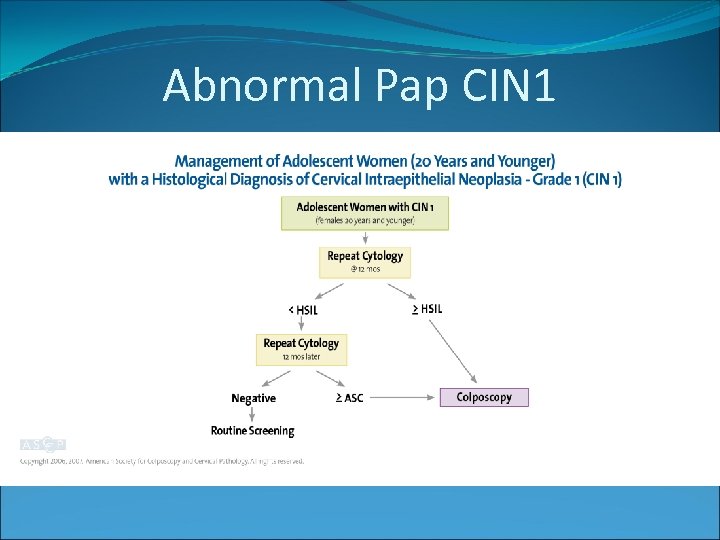 Abnormal Pap CIN 1
Abnormal Pap CIN 1
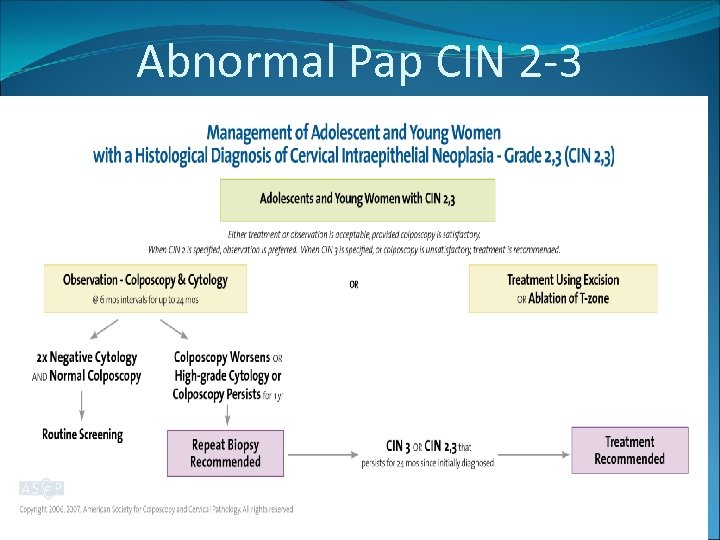 Abnormal Pap CIN 2 -3
Abnormal Pap CIN 2 -3
 How often to screen Frequency of cervical cytology screening Every 2 years for women aged 21 -29 Women aged 30 or older with three consecutive negative pap smears can be followed every three years More frequent screening for HIV infected women Immunosuppressed women Women exposed to DES Women with previously treated CIN 2, CIN 3 , or cancer
How often to screen Frequency of cervical cytology screening Every 2 years for women aged 21 -29 Women aged 30 or older with three consecutive negative pap smears can be followed every three years More frequent screening for HIV infected women Immunosuppressed women Women exposed to DES Women with previously treated CIN 2, CIN 3 , or cancer
 How often to screen Frequency Women with HIV should be screened every 6 months in the first year of diagnosis, then every year Women treated in the past for CIN 2, CIN 3, or cancer are at risk for 20 years for recurrence or persistence, annual screening
How often to screen Frequency Women with HIV should be screened every 6 months in the first year of diagnosis, then every year Women treated in the past for CIN 2, CIN 3, or cancer are at risk for 20 years for recurrence or persistence, annual screening
 Special Notes The frequency of those with same sex partners Penetrative sex at an early age Same screening in those who have been vaccinated against HPV ( ACOG press release 11/09)
Special Notes The frequency of those with same sex partners Penetrative sex at an early age Same screening in those who have been vaccinated against HPV ( ACOG press release 11/09)

 Pelvic Inflammatory disease in pregnancy A 23 year old P 2032 at 8 weeks and 6 /7 days presents to ER with complaint of nausea, vomiting, and abdominal pain Past Medical history : NC Past Surgical history : TAB x 3 Social history : positive marijuana use Gyn/OB history: new partner, history of Chlamydia, Trich, PID in past, SVD times two Vitals 37. 0 , RR 20, P 65, BP 97/59 PE: moderate distress Abdomen soft, no rebound or guarding, Pelvic: Yellow vaginal discharge, cervical motion tenderness Sonogram: 8 week fetus with fetal HMS
Pelvic Inflammatory disease in pregnancy A 23 year old P 2032 at 8 weeks and 6 /7 days presents to ER with complaint of nausea, vomiting, and abdominal pain Past Medical history : NC Past Surgical history : TAB x 3 Social history : positive marijuana use Gyn/OB history: new partner, history of Chlamydia, Trich, PID in past, SVD times two Vitals 37. 0 , RR 20, P 65, BP 97/59 PE: moderate distress Abdomen soft, no rebound or guarding, Pelvic: Yellow vaginal discharge, cervical motion tenderness Sonogram: 8 week fetus with fetal HMS
 Pelvic Inflammatory disease in pregnancy Labs: WBC 4. 9, Hct 39. 9, Positive culture for chlamydia, Trich on wet prep Hospital course: pt was admitted with diagnosis of PID in pregnancy, Treated 48 hours with IV Gentamycin and Clindamycin , po Azithomycin Discharge Home with Clindamycin for ten days
Pelvic Inflammatory disease in pregnancy Labs: WBC 4. 9, Hct 39. 9, Positive culture for chlamydia, Trich on wet prep Hospital course: pt was admitted with diagnosis of PID in pregnancy, Treated 48 hours with IV Gentamycin and Clindamycin , po Azithomycin Discharge Home with Clindamycin for ten days
 Pelvic Inflammatory Disease Most of the times multi-organism Can range from endometritis to pelvic abcesses 300, 000 cases per year 16 -20% in Adolescents Clinical diagnosis overestimated and difficult
Pelvic Inflammatory Disease Most of the times multi-organism Can range from endometritis to pelvic abcesses 300, 000 cases per year 16 -20% in Adolescents Clinical diagnosis overestimated and difficult
 Pelvic Inflammatory Disease • Empiric treatment warranted if suspected because of long term effects if untreated • Begin treatment if sexually active and – Uterine tenderness –Adnexal tenderness – Cervical motion tenderness (CMT)
Pelvic Inflammatory Disease • Empiric treatment warranted if suspected because of long term effects if untreated • Begin treatment if sexually active and – Uterine tenderness –Adnexal tenderness – Cervical motion tenderness (CMT)
 Pelvic Inflammatory Disease Additional Criteria: Temp > 101 F (38. 3 C) Mucopurulent cervical discharge WBC on microscopy Increased erythrocyte sedimentation rate Increased C-reactive protein Positive culture for N. gonorrhea or Chlamydia
Pelvic Inflammatory Disease Additional Criteria: Temp > 101 F (38. 3 C) Mucopurulent cervical discharge WBC on microscopy Increased erythrocyte sedimentation rate Increased C-reactive protein Positive culture for N. gonorrhea or Chlamydia
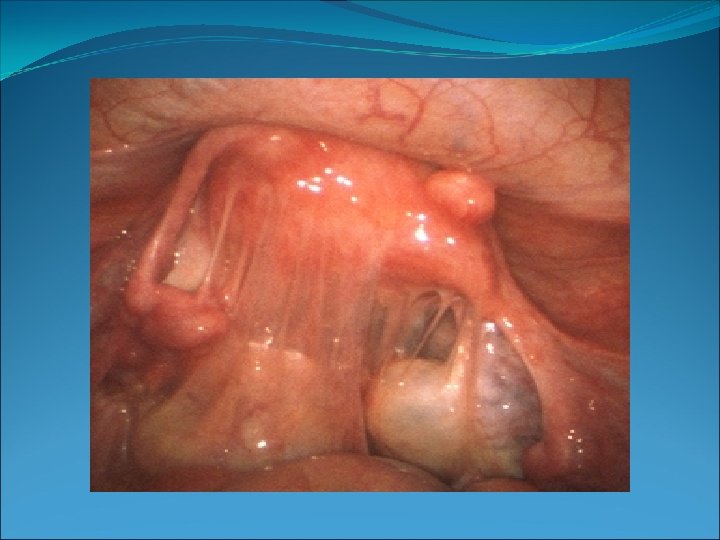
 Pelvic Inflammatory Disease Treat in hospital if: Surgical emergency cannot be excluded Pregnancy (rare 1: 1000 to 1: 25000) No initial clinical response Does not tolerate PO Severe illness Tubo-Ovarian abscess
Pelvic Inflammatory Disease Treat in hospital if: Surgical emergency cannot be excluded Pregnancy (rare 1: 1000 to 1: 25000) No initial clinical response Does not tolerate PO Severe illness Tubo-Ovarian abscess
 Pelvic Inflammatory Disease Rx. Outpatient: A: Ofloxacin 400 mg PO BID X 14 days OR Levofloxacin 500 mg PO QD X 14 days +/- Metronidazole 500 mg PO BID X 14 days B: Ceftriaxone 250 mg IM X 1 dose OR Cefoxitin 2 g IM X 1 dose + Probenecid 1 g PO OR Other third generation cephalosporin Plus Doxycycline 100 mg PO BID X 14 days +/- Metronidazole 500 mg PO BID X 14 days CDC STD treatment guidelines 2006 1 -94
Pelvic Inflammatory Disease Rx. Outpatient: A: Ofloxacin 400 mg PO BID X 14 days OR Levofloxacin 500 mg PO QD X 14 days +/- Metronidazole 500 mg PO BID X 14 days B: Ceftriaxone 250 mg IM X 1 dose OR Cefoxitin 2 g IM X 1 dose + Probenecid 1 g PO OR Other third generation cephalosporin Plus Doxycycline 100 mg PO BID X 14 days +/- Metronidazole 500 mg PO BID X 14 days CDC STD treatment guidelines 2006 1 -94
 Pelvic Inflammatory Disease In House A: Cefotetan 2 g IV Q 12 OR Cefoxitin 2 g IV Q 6 H Plus Doxycycline 100 mg IV or PO Q 12 H B: Clindamycin 900 mg IV q 8 h Plus Gentamicin 2 mg/kg loading f/u 1. 5 mg/kg Q 8 H C: Ofloxacin 400 mg IV Q 6 h or Levofloxacin 500 mg QD +/- Metronidazole 500 mg IV Q 8 H or Unasyn 3 g IV Q 6 H Plus Doxycycline 100 mg PO IV Q 12 H CDC STD treatment guidelines 2006 1 -94
Pelvic Inflammatory Disease In House A: Cefotetan 2 g IV Q 12 OR Cefoxitin 2 g IV Q 6 H Plus Doxycycline 100 mg IV or PO Q 12 H B: Clindamycin 900 mg IV q 8 h Plus Gentamicin 2 mg/kg loading f/u 1. 5 mg/kg Q 8 H C: Ofloxacin 400 mg IV Q 6 h or Levofloxacin 500 mg QD +/- Metronidazole 500 mg IV Q 8 H or Unasyn 3 g IV Q 6 H Plus Doxycycline 100 mg PO IV Q 12 H CDC STD treatment guidelines 2006 1 -94
 Pelvic Inflammatory Disease Pregnancy: Multiple reports in the literature (1: 1000 -1: 25000) Easily confused with ectopic pregnancy Associated with fetal wastage and poor outcomes Etiology confusing: Sperm carrying bacteria? Infection prior to 12 weeks and membrane apposition? Reactivation of latent disease? Hematogenous or Lymphatic spread? Lara-Torre E et al JRM 2002; 47: 959 -61
Pelvic Inflammatory Disease Pregnancy: Multiple reports in the literature (1: 1000 -1: 25000) Easily confused with ectopic pregnancy Associated with fetal wastage and poor outcomes Etiology confusing: Sperm carrying bacteria? Infection prior to 12 weeks and membrane apposition? Reactivation of latent disease? Hematogenous or Lymphatic spread? Lara-Torre E et al JRM 2002; 47: 959 -61
 Pelvic Inflammatory Disease Pregnancy (cont): Aggressive antibiotic treatment warranted prior to uterine evacuation Conservative treatment may maintain pregnancy to term Delay in diagnosis because of pregnancy may worsen outcomes Decrease immune response in pregnancy may worsen presentation and progression
Pelvic Inflammatory Disease Pregnancy (cont): Aggressive antibiotic treatment warranted prior to uterine evacuation Conservative treatment may maintain pregnancy to term Delay in diagnosis because of pregnancy may worsen outcomes Decrease immune response in pregnancy may worsen presentation and progression



