Celiac_Disease.pptx
- Количество слайдов: 31
 Celiac Disease. It’s Influence on the Children’s Health and Function of Digestive System. by K. Yakovlev group 244, O. Shik, group 228
Celiac Disease. It’s Influence on the Children’s Health and Function of Digestive System. by K. Yakovlev group 244, O. Shik, group 228
 The Plan 1. Definition 2. Historical background 3. Causes of the disease 4. Epidemiology 5. Pathogenesis 6. Clinical presentation 7. Associated diseases 8. Therapy
The Plan 1. Definition 2. Historical background 3. Causes of the disease 4. Epidemiology 5. Pathogenesis 6. Clinical presentation 7. Associated diseases 8. Therapy
 The Definintion Celiac disease is an immune-mediated systemic disorder which is caused by the reaction to gliadin and characterized by the presence of anti-tissue transglutaminase antibodies or glutendepending manifestations incl. enteropathy.
The Definintion Celiac disease is an immune-mediated systemic disorder which is caused by the reaction to gliadin and characterized by the presence of anti-tissue transglutaminase antibodies or glutendepending manifestations incl. enteropathy.
 Historical background CD was first accurately described by Samuel J. Gee in 1888. In early 1950 the role of wheat and rye in the pathogenesis of the disease was established.
Historical background CD was first accurately described by Samuel J. Gee in 1888. In early 1950 the role of wheat and rye in the pathogenesis of the disease was established.
 Causes of the Disease Cereal Proteins Other Environmental factors Inherited factors
Causes of the Disease Cereal Proteins Other Environmental factors Inherited factors
 Cereal Proteins The cereals that are toxic for patients with CD are wheat, rye and barley. However rice and maize are nontoxic and are being used as the wheat substitute in the diet of CD patients
Cereal Proteins The cereals that are toxic for patients with CD are wheat, rye and barley. However rice and maize are nontoxic and are being used as the wheat substitute in the diet of CD patients
 Environmental Factors CD is suggested to be more dangerous in very young infants so that the age plays a great role Also the presentation of the gluten in the diet increases the risk of CD So CD may be prevented by avoiding gluten in the first two eyars
Environmental Factors CD is suggested to be more dangerous in very young infants so that the age plays a great role Also the presentation of the gluten in the diet increases the risk of CD So CD may be prevented by avoiding gluten in the first two eyars
 Other factors which may cause CD are: Viral infections Bacterial invasion Decreased immunity
Other factors which may cause CD are: Viral infections Bacterial invasion Decreased immunity
 Genetic Markers The strongest association of CD is with HLA (Human Leukocyte Antigens) markers HLA class II markers are responsible in presentation of antigen to T-cells
Genetic Markers The strongest association of CD is with HLA (Human Leukocyte Antigens) markers HLA class II markers are responsible in presentation of antigen to T-cells
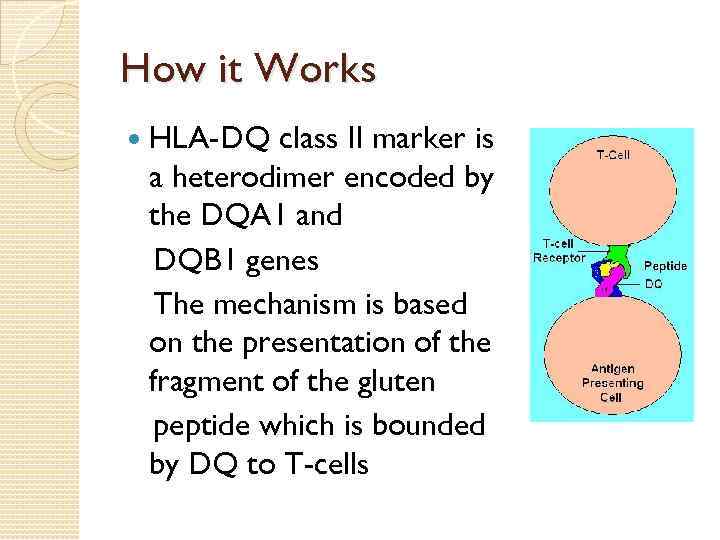 How it Works HLA-DQ class II marker is a heterodimer encoded by the DQA 1 and DQB 1 genes The mechanism is based on the presentation of the fragment of the gluten peptide which is bounded by DQ to T-cells
How it Works HLA-DQ class II marker is a heterodimer encoded by the DQA 1 and DQB 1 genes The mechanism is based on the presentation of the fragment of the gluten peptide which is bounded by DQ to T-cells
 Epidemiology The reported prevalence of symptomatic CD is 1 in 1000 live births The prevalence in woman appears to be greater than in men The clinical prevalence of CD is just the top of the iceberg as the biopsy studies reveal CD in 1: 99 children
Epidemiology The reported prevalence of symptomatic CD is 1 in 1000 live births The prevalence in woman appears to be greater than in men The clinical prevalence of CD is just the top of the iceberg as the biopsy studies reveal CD in 1: 99 children
 Several prevalence have been indicated in most European countries, in North and South America, in USA To a greater extend the most CD cases are undetected Susceptible group: Children under 2 years, genetically predisposed persons, persons who live in poor districts of the world
Several prevalence have been indicated in most European countries, in North and South America, in USA To a greater extend the most CD cases are undetected Susceptible group: Children under 2 years, genetically predisposed persons, persons who live in poor districts of the world
 Pathogenesis Celiac disease is a T-cell – mediated, chronic inflammatory disorder with an autoimmune component Altered processing of gliadin provides the production of the antibodies to gliadin (which are the special Ig A, Ig. G)
Pathogenesis Celiac disease is a T-cell – mediated, chronic inflammatory disorder with an autoimmune component Altered processing of gliadin provides the production of the antibodies to gliadin (which are the special Ig A, Ig. G)
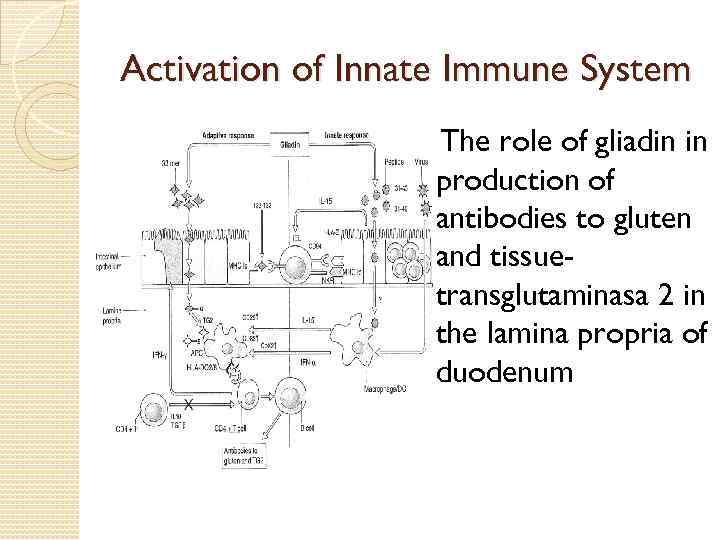 Activation of Innate Immune System The role of gliadin in production of antibodies to gluten and tissuetransglutaminasa 2 in the lamina propria of duodenum
Activation of Innate Immune System The role of gliadin in production of antibodies to gluten and tissuetransglutaminasa 2 in the lamina propria of duodenum
 Processing of Gliadin, Adaptive Response First stage is the proteolysis of gliadin which results in a number of deamidated peptides (Transglutaminasa 2) Second stage is binding the proteins into the peptide pocket of HLA-DQ 2/8 molecules of APC allowing their presentation to CD 4+ T cells
Processing of Gliadin, Adaptive Response First stage is the proteolysis of gliadin which results in a number of deamidated peptides (Transglutaminasa 2) Second stage is binding the proteins into the peptide pocket of HLA-DQ 2/8 molecules of APC allowing their presentation to CD 4+ T cells
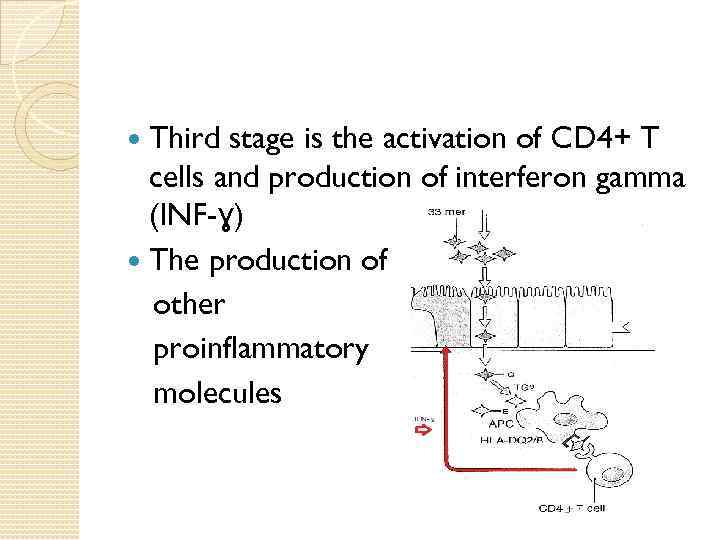 Third stage is the activation of CD 4+ T cells and production of interferon gamma (INF-ɣ) The production of other proinflammatory molecules
Third stage is the activation of CD 4+ T cells and production of interferon gamma (INF-ɣ) The production of other proinflammatory molecules
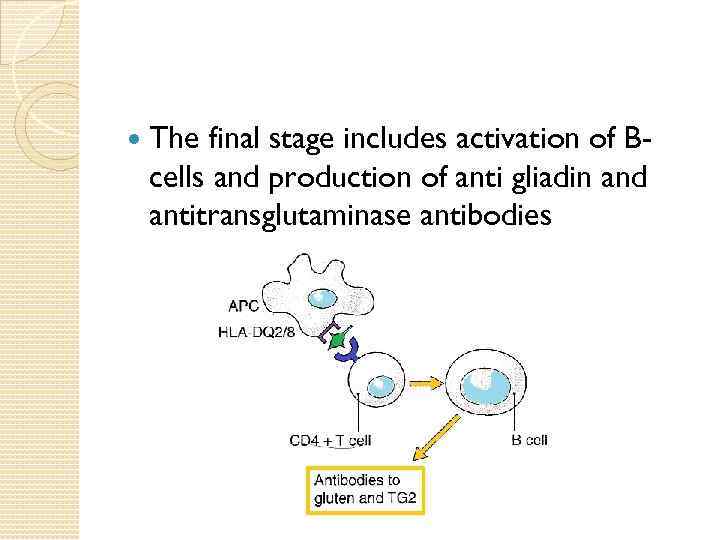 The final stage includes activation of Bcells and production of anti gliadin and antitransglutaminase antibodies
The final stage includes activation of Bcells and production of anti gliadin and antitransglutaminase antibodies
 The Role of Innate Immunity The Innate Immunity is activated by specific “A” gliadin sequences and focused on production of Il 15 and subsequent reaction with CD 25 and CD 83 markers of APC and affecting IEL (Intraepithelial Lymphocytes)
The Role of Innate Immunity The Innate Immunity is activated by specific “A” gliadin sequences and focused on production of Il 15 and subsequent reaction with CD 25 and CD 83 markers of APC and affecting IEL (Intraepithelial Lymphocytes)
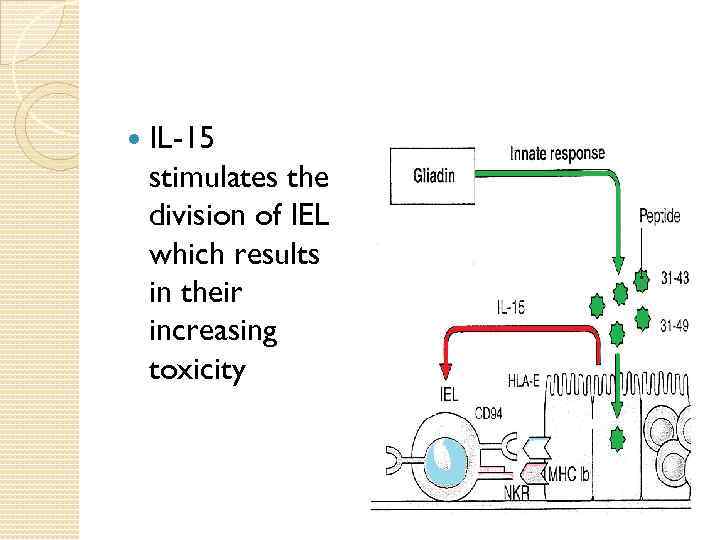 IL-15 stimulates the division of IEL which results in their increasing toxicity
IL-15 stimulates the division of IEL which results in their increasing toxicity
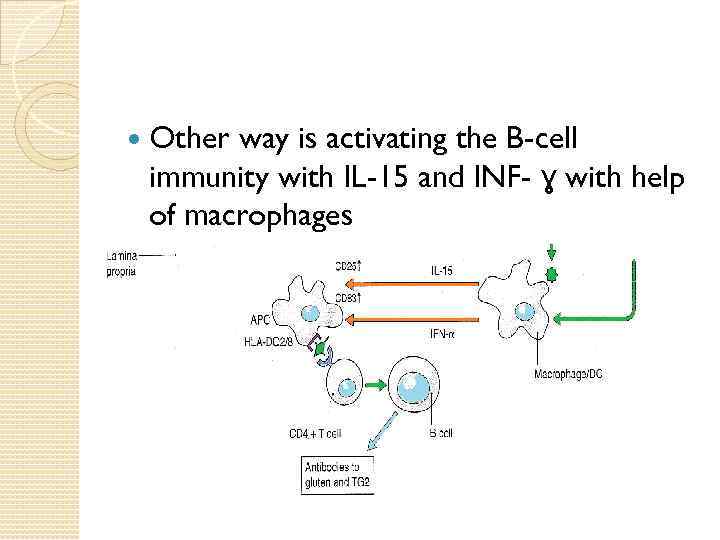 Other way is activating the B-cell immunity with IL-15 and INF- ɣ with help of macrophages
Other way is activating the B-cell immunity with IL-15 and INF- ɣ with help of macrophages
 Autoimmune Phenomena in CD The most characteristic expression of CD id the presence of TG 2 antibodies in patients sera. TG 2 antibodies inhibit the fermental activity of transglutaminase 2 and disturbs crosstalk between epithelial cells and fibroblasts beneath and supports their proliferation
Autoimmune Phenomena in CD The most characteristic expression of CD id the presence of TG 2 antibodies in patients sera. TG 2 antibodies inhibit the fermental activity of transglutaminase 2 and disturbs crosstalk between epithelial cells and fibroblasts beneath and supports their proliferation
 TG 2 antibodies are produced in mucosa and can be detected before appearing in circulation. But TG 2 antibodies (Ig. A) may be present in liver, nervous system and in the heart muscle which may lead to autoimmune disorders of corresponding systems
TG 2 antibodies are produced in mucosa and can be detected before appearing in circulation. But TG 2 antibodies (Ig. A) may be present in liver, nervous system and in the heart muscle which may lead to autoimmune disorders of corresponding systems
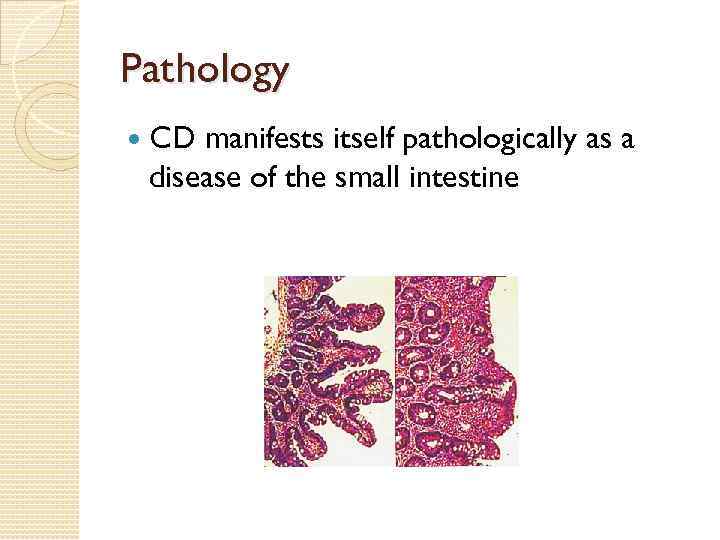 Pathology CD manifests itself pathologically as a disease of the small intestine
Pathology CD manifests itself pathologically as a disease of the small intestine
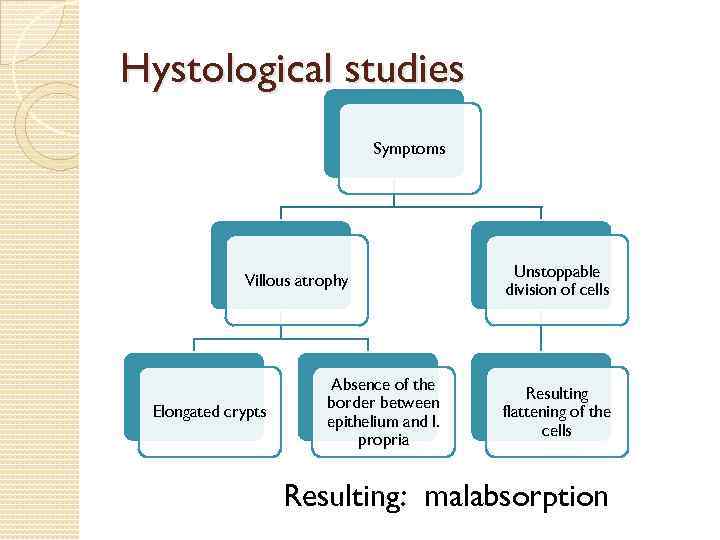 Hystological studies Symptoms Villous atrophy Elongated crypts Absence of the border between epithelium and l. propria Unstoppable division of cells Resulting flattening of the cells Resulting: malabsorption
Hystological studies Symptoms Villous atrophy Elongated crypts Absence of the border between epithelium and l. propria Unstoppable division of cells Resulting flattening of the cells Resulting: malabsorption
 External factors Diarrhea Paleness of skin Reduced appetite Dystrophy Swelling of the lower limbs Inflammation of mucose membranes Vomiting Abdominal distention Hidden disease curse
External factors Diarrhea Paleness of skin Reduced appetite Dystrophy Swelling of the lower limbs Inflammation of mucose membranes Vomiting Abdominal distention Hidden disease curse
 Clinical Presentation Hepatic failure Dental abnormalities (enamel hypoplasia) Dermatitis Herpetiformis which is the gluten dependent eruption disease with the skin blisters full of Ig. A and indistinguisheble duodenum histology from CD Latent low TG 2 ab titers patients
Clinical Presentation Hepatic failure Dental abnormalities (enamel hypoplasia) Dermatitis Herpetiformis which is the gluten dependent eruption disease with the skin blisters full of Ig. A and indistinguisheble duodenum histology from CD Latent low TG 2 ab titers patients
 Associated Diseases Pernicious anemia Autoimmune thrombocytopenia Sarcoidosis Diabetes Allopecia Cardiomyopathies
Associated Diseases Pernicious anemia Autoimmune thrombocytopenia Sarcoidosis Diabetes Allopecia Cardiomyopathies
 Diagnosis and Therapy Serological tests to Ig. A to TG 2 antibodies to endomysial cells HLA-DQ 2/8 presence test Biopsy which should be performed while upper endoscopy is beeing made
Diagnosis and Therapy Serological tests to Ig. A to TG 2 antibodies to endomysial cells HLA-DQ 2/8 presence test Biopsy which should be performed while upper endoscopy is beeing made
 Two mandatory are required for the diagnosis of CD those are the duodenum biopsy (establishes the villous pathology) and finding Ig. A a/b in circulation Also the clinical remission after withdraw of gluten-free diet is a major clinical sign
Two mandatory are required for the diagnosis of CD those are the duodenum biopsy (establishes the villous pathology) and finding Ig. A a/b in circulation Also the clinical remission after withdraw of gluten-free diet is a major clinical sign
 Therapy includes two postulates 1. Gluten free diet (life long) Taking care about associated diseases
Therapy includes two postulates 1. Gluten free diet (life long) Taking care about associated diseases
 Thanks you dear colleges!
Thanks you dear colleges!


