761e68a15348fe80c9be913d23c2d279.ppt
- Количество слайдов: 21
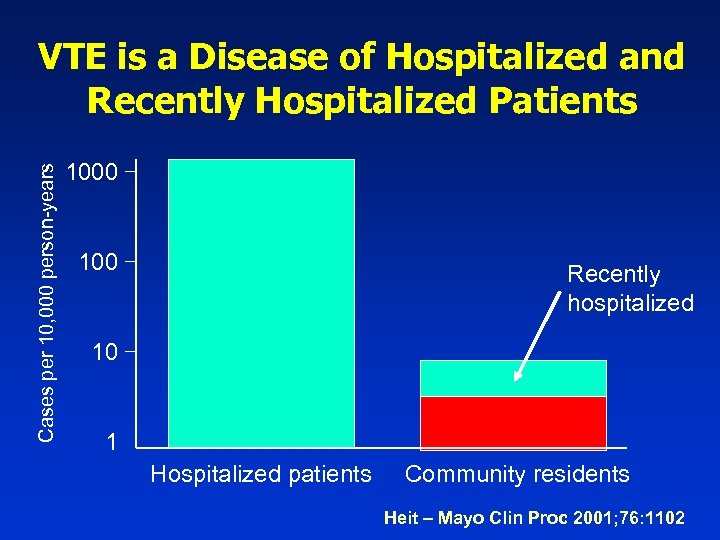 Cases per 10, 000 person-years VTE is a Disease of Hospitalized and Recently Hospitalized Patients 1000 100 Recently hospitalized 10 1 Hospitalized patients Community residents Heit – Mayo Clin Proc 2001; 76: 1102
Cases per 10, 000 person-years VTE is a Disease of Hospitalized and Recently Hospitalized Patients 1000 100 Recently hospitalized 10 1 Hospitalized patients Community residents Heit – Mayo Clin Proc 2001; 76: 1102
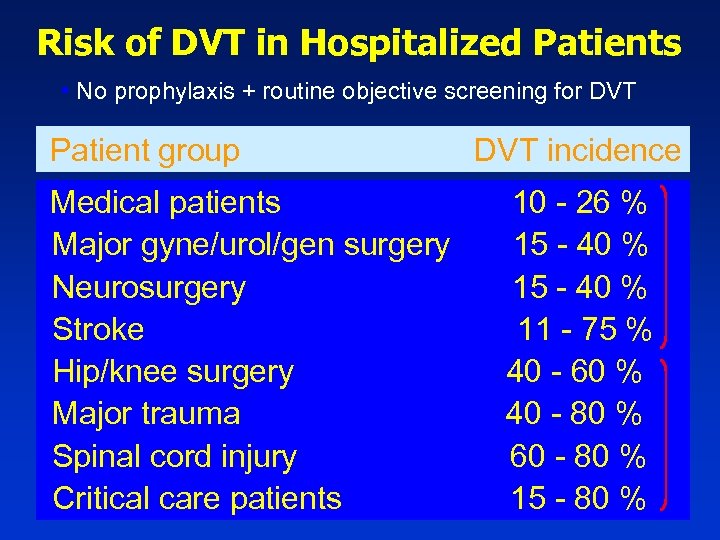 Risk of DVT in Hospitalized Patients • No prophylaxis + routine objective screening for DVT Patient group Medical patients Major gyne/urol/gen surgery Neurosurgery Stroke Hip/knee surgery Major trauma Spinal cord injury Critical care patients DVT incidence 10 - 26 % 15 - 40 % 11 - 75 % 40 - 60 % 40 - 80 % 60 - 80 % 15 - 80 %
Risk of DVT in Hospitalized Patients • No prophylaxis + routine objective screening for DVT Patient group Medical patients Major gyne/urol/gen surgery Neurosurgery Stroke Hip/knee surgery Major trauma Spinal cord injury Critical care patients DVT incidence 10 - 26 % 15 - 40 % 11 - 75 % 40 - 60 % 40 - 80 % 60 - 80 % 15 - 80 %
 Risk Factors for VTE Stasis Hypercoagulability Age > 40 Immobility CHF Stroke Paralysis Spinal Cord injury Hyperviscosity Polycythemia Severe COPD Anesthesia Obesity Varicose Veins Cancer High estrogen states Inflammatory Bowel Nephrotic Syndrome Sepsis Smoking Pregnancy Thrombophilia Anderson FA Jr. & Wheeler HB. Clin Chest Med 1995; 16: 235. Endothelial Damage Surgery Prior VTE Central lines Trauma
Risk Factors for VTE Stasis Hypercoagulability Age > 40 Immobility CHF Stroke Paralysis Spinal Cord injury Hyperviscosity Polycythemia Severe COPD Anesthesia Obesity Varicose Veins Cancer High estrogen states Inflammatory Bowel Nephrotic Syndrome Sepsis Smoking Pregnancy Thrombophilia Anderson FA Jr. & Wheeler HB. Clin Chest Med 1995; 16: 235. Endothelial Damage Surgery Prior VTE Central lines Trauma
 Risk Factors for VTE ve ha E ts Endothelial T Stasis Hypercoagulability ien r VDamage Age > 40 Cancer at fo p Immobility High estrogen states or Surgery ed. Bowelct CHF Inflammatory Prior VTE liz. Syndrome fa a Stroke Nephrotic it isk Central lines p Paralysis Sepsis Trauma os ne r Spinal Cord injuryh Smoking st s. Pregnancy o a to Hyperviscosity M le Thrombophilia Polycythemia at Severe COPD Anesthesia Obesity Varicose Veins Anderson FA Jr. & Wheeler HB. Clin Chest Med 1995; 16: 235. Bick RL & Kaplan H. Med Clin North Am 1998; 82: 409.
Risk Factors for VTE ve ha E ts Endothelial T Stasis Hypercoagulability ien r VDamage Age > 40 Cancer at fo p Immobility High estrogen states or Surgery ed. Bowelct CHF Inflammatory Prior VTE liz. Syndrome fa a Stroke Nephrotic it isk Central lines p Paralysis Sepsis Trauma os ne r Spinal Cord injuryh Smoking st s. Pregnancy o a to Hyperviscosity M le Thrombophilia Polycythemia at Severe COPD Anesthesia Obesity Varicose Veins Anderson FA Jr. & Wheeler HB. Clin Chest Med 1995; 16: 235. Bick RL & Kaplan H. Med Clin North Am 1998; 82: 409.
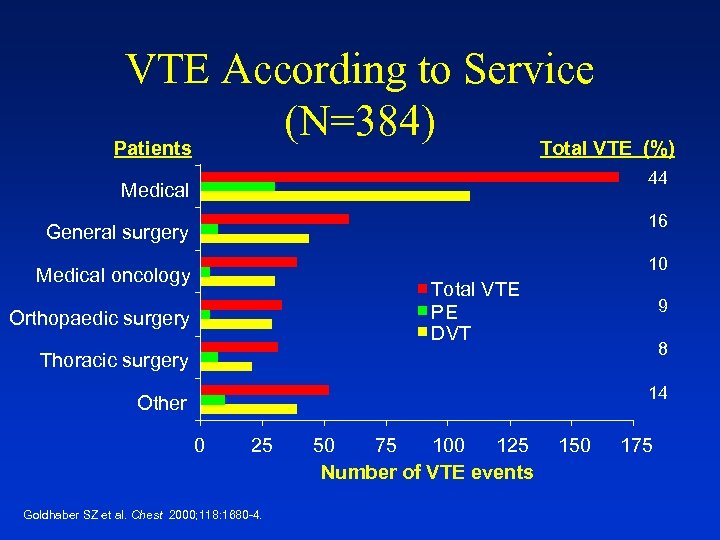 VTE According to Service (N=384) Patients Total VTE (%) 44 Medical 16 General surgery 10 Medical oncology Total VTE PE DVT Orthopaedic surgery 9 8 Thoracic surgery 14 Other 0 25 Goldhaber SZ et al. Chest 2000; 118: 1680 -4. 50 75 100 125 Number of VTE events 150 175
VTE According to Service (N=384) Patients Total VTE (%) 44 Medical 16 General surgery 10 Medical oncology Total VTE PE DVT Orthopaedic surgery 9 8 Thoracic surgery 14 Other 0 25 Goldhaber SZ et al. Chest 2000; 118: 1680 -4. 50 75 100 125 Number of VTE events 150 175
 VTE: A Major Source of Mortality and Morbidity • 200, 000 VTE deaths per year (half primary) – More than HIV, MVAs, Breast Cancer combined • 80, 000 preventable deaths in hospital • 10% of hospital deaths, most common cause of preventable hospital death • Huge costs and morbidity • Recurrence of DVT, post-thrombotic syndrome and chronic PE / PAH are long term sequelae
VTE: A Major Source of Mortality and Morbidity • 200, 000 VTE deaths per year (half primary) – More than HIV, MVAs, Breast Cancer combined • 80, 000 preventable deaths in hospital • 10% of hospital deaths, most common cause of preventable hospital death • Huge costs and morbidity • Recurrence of DVT, post-thrombotic syndrome and chronic PE / PAH are long term sequelae
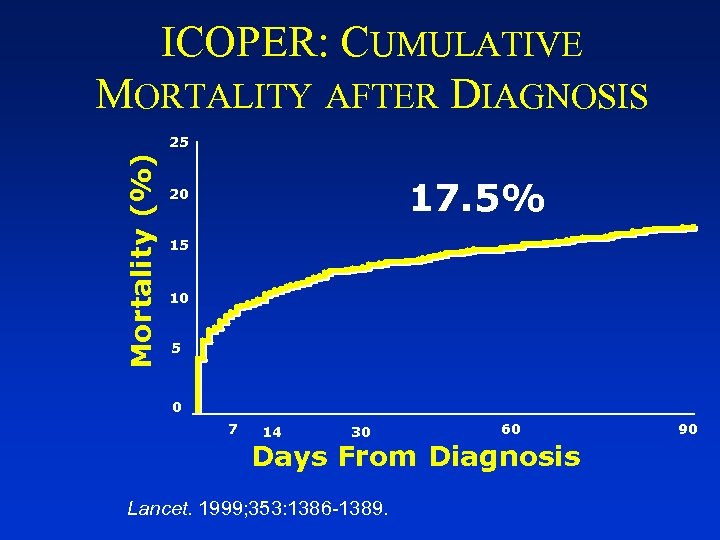 ICOPER: CUMULATIVE MORTALITY AFTER DIAGNOSIS Mortality (%) 25 17. 5% 20 15 10 5 0 7 14 30 60 Days From Diagnosis Lancet. 1999; 353: 1386 -1389. 90
ICOPER: CUMULATIVE MORTALITY AFTER DIAGNOSIS Mortality (%) 25 17. 5% 20 15 10 5 0 7 14 30 60 Days From Diagnosis Lancet. 1999; 353: 1386 -1389. 90
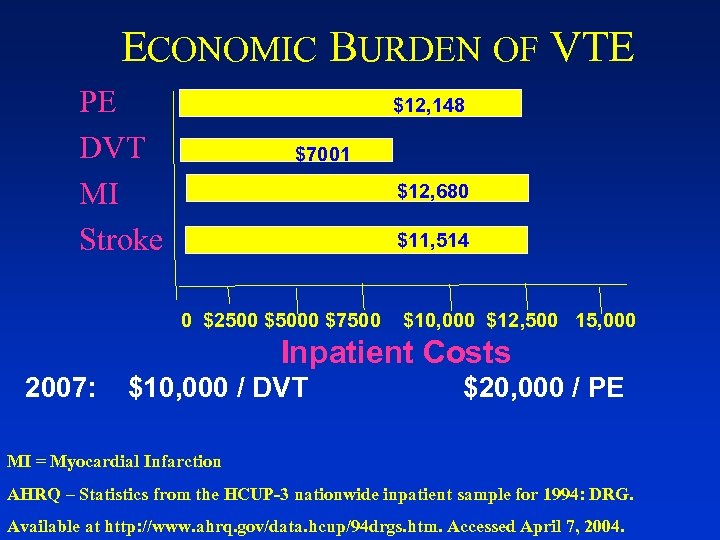 ECONOMIC BURDEN OF VTE PE DVT MI Stroke $12, 148 $7001 $12, 680 $11, 514 0 $2500 $5000 $7500 $10, 000 $12, 500 15, 000 Inpatient Costs 2007: $10, 000 / DVT $20, 000 / PE MI = Myocardial Infarction AHRQ – Statistics from the HCUP-3 nationwide inpatient sample for 1994: DRG. Available at http: //www. ahrq. gov/data. hcup/94 drgs. htm. Accessed April 7, 2004.
ECONOMIC BURDEN OF VTE PE DVT MI Stroke $12, 148 $7001 $12, 680 $11, 514 0 $2500 $5000 $7500 $10, 000 $12, 500 15, 000 Inpatient Costs 2007: $10, 000 / DVT $20, 000 / PE MI = Myocardial Infarction AHRQ – Statistics from the HCUP-3 nationwide inpatient sample for 1994: DRG. Available at http: //www. ahrq. gov/data. hcup/94 drgs. htm. Accessed April 7, 2004.
 Good News! Effective, safe, and cost-effective VTE prophylaxis is available! • Pharmacologic Prophylaxis reduces DVT and PE by 50 -65% • Symptomatic and Asymptomatic VTE reduced. • Bleeding risk due to prophylaxis is rare. • HIT – 2. 37% with UFH (occasionally very serious) –. 06% with LMWH Cost effectiveness of VTE prophylaxis has been repeatedly demonstrated. Geerts et al. Chest. 2004 Sep; 126(3 Suppl): 338 S-400 S. Shojania KG et al. Making health care safer…. www. ahrq. gov/clinic/ptsafety/. Martel – Blood 2005; 106: 2710
Good News! Effective, safe, and cost-effective VTE prophylaxis is available! • Pharmacologic Prophylaxis reduces DVT and PE by 50 -65% • Symptomatic and Asymptomatic VTE reduced. • Bleeding risk due to prophylaxis is rare. • HIT – 2. 37% with UFH (occasionally very serious) –. 06% with LMWH Cost effectiveness of VTE prophylaxis has been repeatedly demonstrated. Geerts et al. Chest. 2004 Sep; 126(3 Suppl): 338 S-400 S. Shojania KG et al. Making health care safer…. www. ahrq. gov/clinic/ptsafety/. Martel – Blood 2005; 106: 2710
 Registry Data Highlight the Underuse of Thromboprophylaxis DVT-FREE RIETE IMPROVE BAD NEWS! Only a minority of hospitalized medical patients receive thromboprophylaxis Goldhaber SZ, Tapson VF. Am J Cardiol 2004; 93: 259 -62. Monreal M, et al. J Thromb Haemost 2004; 2: 1892 -8. Tapson V, et al. Blood 2004; 104: 11. Abstract #1762.
Registry Data Highlight the Underuse of Thromboprophylaxis DVT-FREE RIETE IMPROVE BAD NEWS! Only a minority of hospitalized medical patients receive thromboprophylaxis Goldhaber SZ, Tapson VF. Am J Cardiol 2004; 93: 259 -62. Monreal M, et al. J Thromb Haemost 2004; 2: 1892 -8. Tapson V, et al. Blood 2004; 104: 11. Abstract #1762.
 National Position Statements • Leapfrog 1: PE is “the most common preventable cause of hospital death in the United States” • Agency for Healthcare Research and Quality (AHRQ)2: Thromboprophylaxis is the number 1 patient safety practice • American Public Health Association (APHA)3: “The disconnect between evidence and execution as it relates to DVT prevention amounts to a public health crisis. ” 1. 2. 3. The Leapfrog Group Hospital Quality and Safety Survey. Available at: www. leapfrog. medstat. com/pdf/Final/doc Shojania KG, et al. Making Healthcare Safer: A Critical Analysis of Patient Safety Practices. AHRQ, 2001. Available at: www. ahrq. gov/clinic/ptsafety/ White Paper. Deep-vein thrombosis: Advancing awareness to protect patient lives. 2003. Available at: www. alpha. org/ppp/DVT_White_Paper. pdf
National Position Statements • Leapfrog 1: PE is “the most common preventable cause of hospital death in the United States” • Agency for Healthcare Research and Quality (AHRQ)2: Thromboprophylaxis is the number 1 patient safety practice • American Public Health Association (APHA)3: “The disconnect between evidence and execution as it relates to DVT prevention amounts to a public health crisis. ” 1. 2. 3. The Leapfrog Group Hospital Quality and Safety Survey. Available at: www. leapfrog. medstat. com/pdf/Final/doc Shojania KG, et al. Making Healthcare Safer: A Critical Analysis of Patient Safety Practices. AHRQ, 2001. Available at: www. ahrq. gov/clinic/ptsafety/ White Paper. Deep-vein thrombosis: Advancing awareness to protect patient lives. 2003. Available at: www. alpha. org/ppp/DVT_White_Paper. pdf
 VTE Prevention on the Radar • • SCIP NQF JCAHO AHRQ APHA CMS Leap Frog
VTE Prevention on the Radar • • SCIP NQF JCAHO AHRQ APHA CMS Leap Frog
 VTE Candidate Performance Measures Selected Measures for Alpha Testing: April 2006 Risk Assessment/ Prophylaxis 1. Documentation of VTE risk assessment (RA)/prophylaxis within 24 hours of hospital admission 2. Documentation of VTE RA/prophylaxis within 24 hrs of transfer to ICU Treatment 3. Documentation of inferior vena cava filter insertion 4. VTE patients with overlap of parenteral and wafarin anticoagulation therapy 5. VTE patients receiving UFH with platelet monitoring 6. VTE patients with renal insufficiency that received reduced/discontinued anticoagulation therapy 7. VTE patients receiving UFH management by nomogram/protocol 8. VTE discharge instructions Outcomes 9. VTE patients with INR > 6 after initiation of warfarin therapy 10. Incidence of potentially preventable hospital-acquired VTE http: //www. jointcommission. org/Performance. Measurement
VTE Candidate Performance Measures Selected Measures for Alpha Testing: April 2006 Risk Assessment/ Prophylaxis 1. Documentation of VTE risk assessment (RA)/prophylaxis within 24 hours of hospital admission 2. Documentation of VTE RA/prophylaxis within 24 hrs of transfer to ICU Treatment 3. Documentation of inferior vena cava filter insertion 4. VTE patients with overlap of parenteral and wafarin anticoagulation therapy 5. VTE patients receiving UFH with platelet monitoring 6. VTE patients with renal insufficiency that received reduced/discontinued anticoagulation therapy 7. VTE patients receiving UFH management by nomogram/protocol 8. VTE discharge instructions Outcomes 9. VTE patients with INR > 6 after initiation of warfarin therapy 10. Incidence of potentially preventable hospital-acquired VTE http: //www. jointcommission. org/Performance. Measurement
 Patient admitted to hospital Flow Diagram: Delivering Appropriate VTE Prophylaxis 35% of failures MD orders appropriate VTE prophylaxis at admission Nurse ensures VTE prophylaxis administered MD links patient’s VTE risk to level to menu of appropriate VTE prophylaxis options 30% of failures MD performs VTE risk assessment Pharmacy dispenses and delivers drug Central Supply delivers SCDs or GCS Support staff ambulates patient TID Change in patient’s VTE risk level, contraindications, or site/unit of care Patient discharged 15% of failures 20% of failures Mean Baseline Performance: 50% (% of patients on appropriate VTE prophylaxis in the hospital) VTE Prophylaxis can be complicated!
Patient admitted to hospital Flow Diagram: Delivering Appropriate VTE Prophylaxis 35% of failures MD orders appropriate VTE prophylaxis at admission Nurse ensures VTE prophylaxis administered MD links patient’s VTE risk to level to menu of appropriate VTE prophylaxis options 30% of failures MD performs VTE risk assessment Pharmacy dispenses and delivers drug Central Supply delivers SCDs or GCS Support staff ambulates patient TID Change in patient’s VTE risk level, contraindications, or site/unit of care Patient discharged 15% of failures 20% of failures Mean Baseline Performance: 50% (% of patients on appropriate VTE prophylaxis in the hospital) VTE Prophylaxis can be complicated!
 A lot of things can go wrong…. . Education alone won’t get it done • • • Risk assessments for VTE and bleeding not standardized Risk assessment fails to occur Definitions of appropriate prophylaxis variable Conflicting order sets and protocols Contributing risks (lines, sedation, restraints) Prophylaxis fails to shift with changes in patient status Platelet monitoring does not occur When to stop prophy uncertain, not standardized. Medication changes, weight, age, renal function, recent or impending procedures can alter optimal approach. • Transitions across providers and locations leads to inconsistent approach.
A lot of things can go wrong…. . Education alone won’t get it done • • • Risk assessments for VTE and bleeding not standardized Risk assessment fails to occur Definitions of appropriate prophylaxis variable Conflicting order sets and protocols Contributing risks (lines, sedation, restraints) Prophylaxis fails to shift with changes in patient status Platelet monitoring does not occur When to stop prophy uncertain, not standardized. Medication changes, weight, age, renal function, recent or impending procedures can alter optimal approach. • Transitions across providers and locations leads to inconsistent approach.
 National Recommendations • American College of Chest Physicians (ACCP)1: “We recommend that every hospital develop a formal strategy that addresses the prevention of thromboembolic complications. ” • National Quality Forum (NQF)2: “Evaluate each patient upon admission, and periodically thereafter, for the risk of DVT/PE. Utilize clinically appropriate methods to prevent DVT/VTE. ” (Safe Practice 17) • Joint Commission on Accreditation of Healthcare Organizations (JCAHO)3: “Contraindications to DVT prophylaxis must be documented” 1. 2. 3. Geerts WH, et al. Chest 2004; 126: 338 S National Consensus Standards for the Prevention and Care of Deep Vein Thrombosis, 2004. Available at: www. qualityforum. org Available at: www. jcaho. org/pms/core+measures/2 adicu 3 dvt. pdf
National Recommendations • American College of Chest Physicians (ACCP)1: “We recommend that every hospital develop a formal strategy that addresses the prevention of thromboembolic complications. ” • National Quality Forum (NQF)2: “Evaluate each patient upon admission, and periodically thereafter, for the risk of DVT/PE. Utilize clinically appropriate methods to prevent DVT/VTE. ” (Safe Practice 17) • Joint Commission on Accreditation of Healthcare Organizations (JCAHO)3: “Contraindications to DVT prophylaxis must be documented” 1. 2. 3. Geerts WH, et al. Chest 2004; 126: 338 S National Consensus Standards for the Prevention and Care of Deep Vein Thrombosis, 2004. Available at: www. qualityforum. org Available at: www. jcaho. org/pms/core+measures/2 adicu 3 dvt. pdf
 Seventh ACCP Consensus “All institutions should have a program in place that allows for the evaluation of a patient’s risk of developing VTE. If patients are found to be at risk of VTE, appropriate prophylaxis should be implemented (Grade 1 A). ” Geerts WH, et al. Chest 2004; 126: 338 S-400 S.
Seventh ACCP Consensus “All institutions should have a program in place that allows for the evaluation of a patient’s risk of developing VTE. If patients are found to be at risk of VTE, appropriate prophylaxis should be implemented (Grade 1 A). ” Geerts WH, et al. Chest 2004; 126: 338 S-400 S.
 Strategies to Improve Thromboprophylaxis Success • • • Excellent quality guidelines National body endorsement Hospital accreditation (JCAHO) Pay for performance (CMS) Local written policy (care pathway) for the hospital / program / patient care unit • Multidisciplinary team • Goals and Measures • Standardized risk assessment and order sets
Strategies to Improve Thromboprophylaxis Success • • • Excellent quality guidelines National body endorsement Hospital accreditation (JCAHO) Pay for performance (CMS) Local written policy (care pathway) for the hospital / program / patient care unit • Multidisciplinary team • Goals and Measures • Standardized risk assessment and order sets

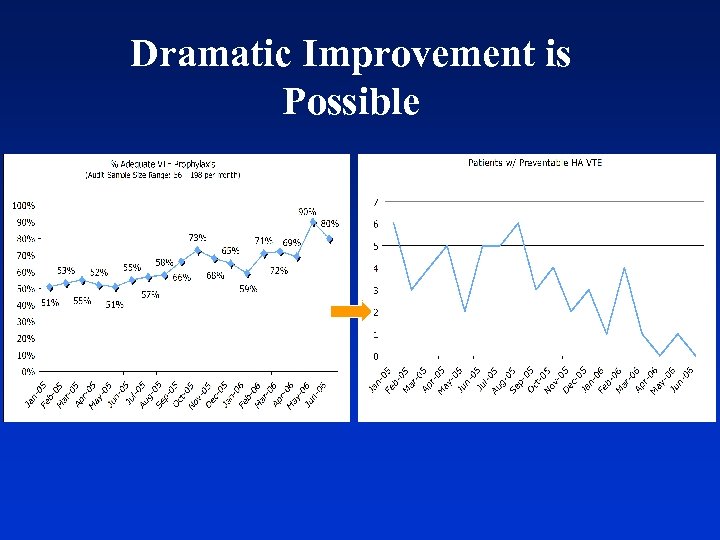 Dramatic Improvement is Possible
Dramatic Improvement is Possible
 Summary • VTE is a very important source of hospital acquired cost, mortality, and morbidity. • Effective, safe, and cost-effective are available, but underutilized in our institution. • Increasing scrutiny from multiple agencies • Institutional prioritization and support needed. • A roadmap enhancing our chances of success is available.
Summary • VTE is a very important source of hospital acquired cost, mortality, and morbidity. • Effective, safe, and cost-effective are available, but underutilized in our institution. • Increasing scrutiny from multiple agencies • Institutional prioritization and support needed. • A roadmap enhancing our chances of success is available.


