fb39e1b0770a002a22f780ef82802120.ppt
- Количество слайдов: 44

Case persentation R 1 王振憲

General Data n n n n Chart No. : 20412591 Name: 王XX Birth Date: 2000/5/11 Age: 6 y/o Gender: female ED: 2006. 10. 12 18: 48 BT: 37. 2 C, P 121, R 23, BP 102/58, Sp. O 2 96%

Chief complaint nausea/vomitting since yesterday n vomitting for 5 -6 times n fever up to 37. 8 C since yesterday n

Present Illness Non-bilious vomiting 5 -6 time since last night about 22: 00. n Intermittent headache over Lt frontal area. n No aggravating factor, but alleviated after vomiting n No similar complaint had happened previously n Fever ( BT max 37. 8℃), Cough(-), Rhinorrhea(-), Abdominal pain(-), Diarrhea(-) n

Present Illness No preceding history of trauma, seizures, diaphoresis, palpitations or blurring of vision n Activity: decreased n Appetite: poor n LMD r/o acute gastroenteritis, r/o meningitis --> refer to CGMH ER n

Past History Drug Allergy: nil n Admission history: nil n Birth history: G 2 P 2 GA 38 wk BBW 3040 g n Newborn screen: normal n Vaccination: as schedule n Development: as milestone n Non-contributory family history n

Physical exam General Appearance: ill-looking n Consciousness: lethargy, E 4 V 5 M 6 n HEENT: no icterus sclera, pink conjunctiva n Neck: supple, no stiffness n Chest: clear BS, RHB without murmur n Abdomen: soft and flat, normoactive bowel sound n Extremities: free movable, no edema n

More about headache n n n n Family Hx Pattern: acute, acute and recurrent, chronic and nonprogressive, chronic and progressive Age at onset Presence or absence of aura and prodrome Frequency, severity, and duration of attack Time and mode of onset Quality, site, and radiation of pain Associated symptoms and abnormalities

More about headache n n n n n Precipitating and relieving factors Relationship with food/alcohol Response to any previous treatment Any recent change in weight or vision Association with recent trauma Any recent changes in sleep, exercise, or diet State of general health Change in school or home environment Possible association with environmental factors

More about headache Growth abnormalities n Nocturnal awakening from headache n Nuchal rigidity n Transient or persistent focal neurologic deficit n Persistent vomiting n Known risk factor for intracranial pathology n Lethargy n Personality change n Pulsatile tinnitus n

Lab exam 20: 18 CBC-DC, sugar, CRP, BUN, Cr, Na, K, ALT n KUB n
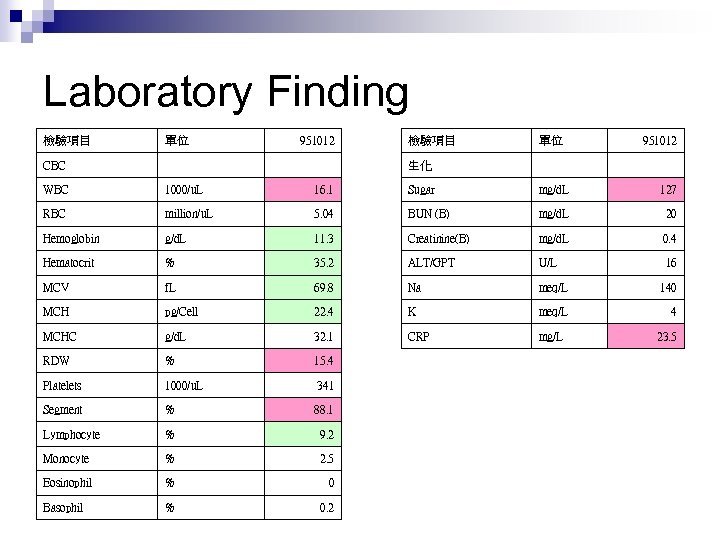
Laboratory Finding 檢驗項目 單位 CBC WBC 1000/u. L RBC 951012 檢驗項目 單位 生化 16. 1 Sugar mg/d. L 127 million/u. L 5. 04 BUN (B) mg/d. L 20 Hemoglobin g/d. L 11. 3 Creatinine(B) mg/d. L 0. 4 Hematocrit % 35. 2 ALT/GPT U/L 16 MCV f. L 69. 8 Na meq/L 140 MCH pg/Cell 22. 4 K meq/L 4 MCHC g/d. L 32. 1 CRP mg/L RDW % 15. 4 Platelets 1000/u. L 341 Segment % 88. 1 Lymphocyte % 9. 2 Monocyte % 2. 5 Eosinophil % 0 Basophil % 0. 2 951012 23. 5

Initial Impression + Plan Vomiting n R/O Aseptic meningits n R/O acute gastritis n ¨ Glycerol 5 ml/hr ¨ IV Metoclopramide ¨ Admission

Hospital Course n n n 10/12 22: 10 BP: 136/78, HR: 86 RR: 20 10/12 23: 38 Seizure attack, decorticate rigidity with pupil dilation, GCS: E 1 V 1 M 3, pupil size: 7 -/7 -, HR: 93次/分 BP: 153/106 mm. Hg ¨ Give O 2 flow -> seizure subsided 5 min later ¨ VBG: p. H 7. 251, Pa. CO 2 39. 0, Pa. O 2 42. 4, HCO 3 16. 8, BE -10. 5, Sa. O 2(%) 70. 7, Sp. O 2(%) 10/12 23: 43 BP 154/93, HR 93

Hospital Course 10/13 00: 35 BP 146/86 HR 62 n Seizure attack again, anisocoria, pupil size: 5+/8¨IV Valium ¨Transfer to PICU ¨Brain CT n 10/13 01: 00 BP 167/114, HR 131 n
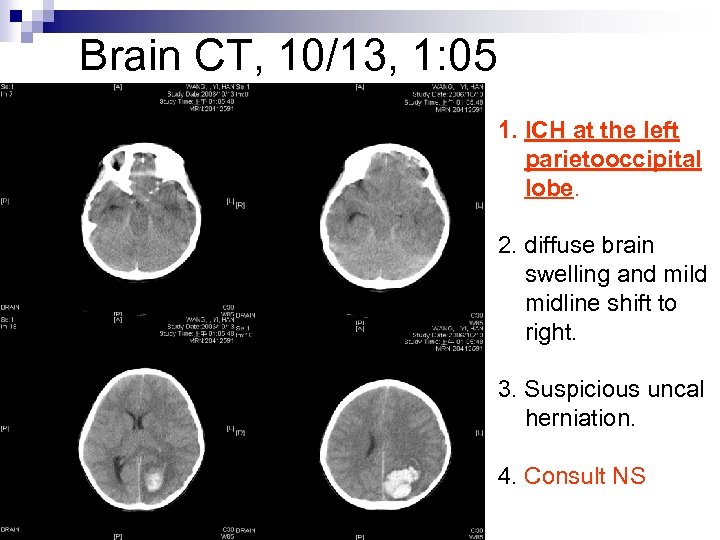
Brain CT, 10/13, 1: 05 1. ICH at the left parietooccipital lobe. 2. diffuse brain swelling and mild midline shift to right. 3. Suspicious uncal herniation. 4. Consult NS
Craniotomy, 10/13, 2: 35 n n n CRANIOTOMY FOR VASCULAR LESIONS, AVM ICP MONITORING 1. Supine position 2. Left occipital craniotomy. 3. Very severe brain swelling. 4. Left occipital corticotomy and removed 20 -30 ml of hematoma. 5. AVM nidus at the inner side of the hematoma near falx. 6. Feeding artery from medial-inferior (R/O branch of PCA) 7. The AVM nidus was removed smoothly. Right frontal burr hole and EVD for ICP monitoring. Cefazolin 200 mg Q 6 H
Hospital Course n n n n 10/13 07: 07 GCS: E 1 VEM 4 ICP: 8 cm. H 2 O HR 118 /min R: 20 /min BP: 167/114 mm. Hg ABG: p. H 7. 448 PCO 2 24. 0 PO 2 182. 2 HCO 3 16. 3 SBE -7. 8 SAT 99. 3% 10/13 08: 45 Hb 15. 5 PLT 186 K PT/PTT 11. 9/31. 0 GCS E 1 V E M 4 ICP 16 cm. H 2 O Morphine 1. 5 mg Q 4 H PRN Valproate 100 mg Q 8 H

Hospital Course 10/13 9: 30 n consicous change after operation n E 2 VEM 3 n Arrange brain CT n
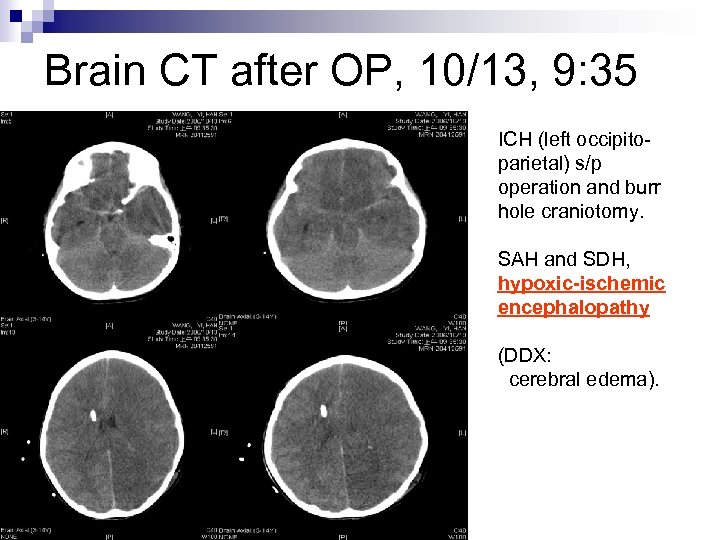
Brain CT after OP, 10/13, 9: 35 ICH (left occipitoparietal) s/p operation and burr hole craniotomy. SAH and SDH, hypoxic-ischemic encephalopathy (DDX: cerebral edema).

Hospital Course 10/13 9: 50 n Rx: Mannitol, Dexan, Depakin n NS suggest craniectomy for decompression n ¨ Family refused for operation ¨ Sign DNR Hypotension Fluid challenge, Add Dopamin and Epinephrine to maintain CPP > 60 n Diabetes insipidus DDAVP, replace free water deficit n

Hospital Course n n n 10/15 Cerebral salt wasting correction of intravascular volume depletion, hyponatremia, replace ongoing urinary sodium loss GCS: E 1 Ve. M 1, Pupil 6 -/6 -

Hospital Course 10/16 n Na: 126, K: 3. 3 n Hyponatremia -> change IVF: D 0. 45 S n Hypokalemia -> add KCL in IVF n

Hospital Course n n n n n 10/18 Na: 139, K: 3. 6 DC depakin EEG: Abnormal record showed diffuse cortical dysfunction, r/o electrocortical silence 10/19 BP stable, taper epinephrine to 0. 08 ug/kg/min DC Cefazolin Taper Dexan

Hospital Course 10/20 n BP stable, taper bosmin to 0. 06 ug/kg/min n Hyponatremia -> 3% Na. Cl infusion n Hypo. Mg -> supplement Mg. SO 4 n

Hospital Course n n n 10/25 hypotension, leukocytosis -> r/o sepsis -> septic workup, then give Tazocin and Vancomycin Sepsis, pneumonia, UTI sp/c: ORSA u/c: Enterococcus >100000 Change to unasyn 0. 7 PC q 6 h, baktar 1 PC po BID

Hospital Course n n n 10/27 bulging mass over the preveious craniotomy wound, r/o CSF collection, r/o pus, r/o brain tissue 10/30 tapping of the scalp bulging mass some pus like semi-fluid was expelled out. brain echo showed no brain blood flow, great ICP, the bulging mass was deemed to be brain necrotic tissue.

Hospital Course n n 11/4 Hypotension noted after bosmin taper to 0. 06 mcg/kg/min, and recovered after bosmin 0. 1 mcg/kg/min, and dopamin 10 mcg/kg/min 11/5 hypotension improved

Hospital Course 11/7 n Hypotension, dopamine to 12 mcg/kg/min n 11/11 n Hypotension, Dopamine 16 mcg/kg/min Epinephrine 0. 1 mcg/kg/min n
Hospital Course 11/21 n Bradycardia to 20/bpm, desaturation, lip cyanosis--> Ambu bagging return to 91/bpm, Sa. O 2: 98% n 11/25 n Stable condition n

Final diagnosis n n n AVM ruptured with ICH at the left parietooccipital lobe, with IICP s/p craniotomy Hypoxic ischemic encephalopathy Subdural hemorrhage at the left side superior falx Cerebral salt wasting syndrome Electrocotical silence, Brain death Sepsis, pneumonia, UTI

Arteriovenous malformations of the brain

Ø Ø Kondziolka D, Humphreys RP, Hoffman HJ, Hendrick EB, Drake JM. Arteriovenous malformations of the brain in children: a forty year experience. Can J Neurol Sci. 1992 Feb; 19(1): 40 -5. Paul W Brazis, MD, Andrew G Lee, MD Approach to the child with headache, 2006 Up. To. Date Hladky JP, Lejeune JP, Blond S, Pruvo JP, Dhellemmes P. Cerebral arteriovenous malformations in children: report on 62 cases. Childs Nerv Syst. 1994 Jul; 10(5): 328 -33 Stapf C, Mast H, Sciacca RR, Choi JH, Khaw AV, Connolly ES, Pile-Spellman J, Mohr JP. Predictors of hemorrhage in patients with untreated brain arteriovenous malformation. Neurology. 2006 May 9; 66(9): 1350 -5.

Definition n n Lesions of the cerebral vasculature develop such that blood flows directly from the arterial system to the venous system without passing through a capillary system. The arteriovenous (AV) shunt is the definitive characteristic of these lesions.

Pathophysiology The direct connection between the arterial and venous systems supplies a lowresistance shunt for arterial blood and exposes the venous system to abnormally high pressures. n This results in a system of enlarged feeding vessels, the tangled nidus of the AVM itself, and enlarged draining venous structures n

Etiology n AVMs are considered congenital lesions and are characterized by a failure of the embryonic vascular plexus to fully differentiate and develop a mature capillary bed in the affected area.

Clinical presentation n n n Hemorrhage (53%) ¨ Acute onset of severe headache ¨ May be described as the worst headache of the patient's life Seizure (46%) Headache (34%) Progressive neurologic deficit (21%) Hemorrhage is more likely to be caused by small lesions, while seizures are more likely to be caused by large lesions Pediatric patients ¨ Heart failure ¨ Macrocephaly ¨ Prominent scalp veins

Clinical presentation n n The annual risk of intracranial hemorrhages associated with AVMs is 2 -3%. The mortality rate associated with the initial bleed is 10%. The mortality rate associated with the second bleed is 13%, and the rate increases to 20% for each subsequent bleed. The incidence of new neurologic deficit occurring with each bleed is 50%.

Clinical presentation Approximately 7. 6% of patients with an AVM develop an aneurysm. n Alternatively, 1. 1% of patients with an aneurysm are found to have an AVM. n

Risk of hemorrhagic AVM Hemorrhage before n Increasing age n Deep brain location n Exclusive deep venous drainage n

Imaging studies n n n CT scan is the first imaging choice in an emergent setting MRI is the first imaging choice in a nonemergency setting (eg, workup of seizure, headache, or neurologic deficit). Magnetic resonance angiograms (MRAs) can reveal the anatomy of the AVM noninvasively but have lower resolution than conventional angiography. Cerebral angiography provides definitive diagnosis. CT angiography has improved dramatically and, in some cases, provides a less invasive alternative to catheter angiography

Treatment Endovascular neurosurgery n Surgery (craniotomy) n Stereotactic radiosurgery n Combination therapy n

Thanks for your attention
fb39e1b0770a002a22f780ef82802120.ppt