abc4c9144c6c276f98e0c998130a4af1.ppt
- Количество слайдов: 76
 Cardio-Pulmonary Resuscitation Piotr Krupa I Oddział Kliniczny Anestezjologii i Intensywnej Terapii z Pododdziałem 1 Kardioanestezjologii
Cardio-Pulmonary Resuscitation Piotr Krupa I Oddział Kliniczny Anestezjologii i Intensywnej Terapii z Pododdziałem 1 Kardioanestezjologii
 Where can I find guiedlines? n AHA – American Heart Association n ERC – European Resuscitation Council n ILCOR – International Liaison Committee on Resuscitation 81 (2010) 1219– 1276 (https: //www. erc. edu/index. php/doc. Library/en/view. Doc/1195/3/) 2
Where can I find guiedlines? n AHA – American Heart Association n ERC – European Resuscitation Council n ILCOR – International Liaison Committee on Resuscitation 81 (2010) 1219– 1276 (https: //www. erc. edu/index. php/doc. Library/en/view. Doc/1195/3/) 2
 Definitions BLS : Basic Life Support Provided by bystanders with no professional equipment ALS : Advanced Life Support Provided by healthcare professionals with specialist equipment CPR : Cardio-Pulmonary Resuscitation All actions which are maintained to restore breath and circulation 3
Definitions BLS : Basic Life Support Provided by bystanders with no professional equipment ALS : Advanced Life Support Provided by healthcare professionals with specialist equipment CPR : Cardio-Pulmonary Resuscitation All actions which are maintained to restore breath and circulation 3
 Definitions Resusitation (lat. resuscitare) All actions which are maintained to restore basic life signs like breath and circulation. Reanimation (lat. reanimatio)–„the action of restoring to life” All actions which are maintained to restore not only basic life signs like breath and circulation but also action of central nervous system. 4
Definitions Resusitation (lat. resuscitare) All actions which are maintained to restore basic life signs like breath and circulation. Reanimation (lat. reanimatio)–„the action of restoring to life” All actions which are maintained to restore not only basic life signs like breath and circulation but also action of central nervous system. 4
 Figure 1. Figure from publication by Safar and Mc. Mahon 16 illustrating the need for neck extension and jaw thrust to maintain a patent airway during mouth-to-mouth artificial ventilation. Cooper J A et al. Circulation 2006; 114: 2839 -2849 5 Copyright © American Heart Association
Figure 1. Figure from publication by Safar and Mc. Mahon 16 illustrating the need for neck extension and jaw thrust to maintain a patent airway during mouth-to-mouth artificial ventilation. Cooper J A et al. Circulation 2006; 114: 2839 -2849 5 Copyright © American Heart Association
 History 1874 r. Moritz Schiff “cardiac massage” (compression of the dog’s chest)) 1892 r. Friedrich Maass, first male cardiac massage CLOSED-CHEST CARDIAC MASSAGE Kouwenhoven; Jude; Knickerbocker – JAMA 1960; 173: 1064 – 1067 6
History 1874 r. Moritz Schiff “cardiac massage” (compression of the dog’s chest)) 1892 r. Friedrich Maass, first male cardiac massage CLOSED-CHEST CARDIAC MASSAGE Kouwenhoven; Jude; Knickerbocker – JAMA 1960; 173: 1064 – 1067 6
 History 1948 r. – first defibrillation (open chest) – Claud Beck 1955 – Paul Zoll – first successful defibrillation (closed chest) 7
History 1948 r. – first defibrillation (open chest) – Claud Beck 1955 – Paul Zoll – first successful defibrillation (closed chest) 7
 Introduction • Europe – sudden cardiac arrest (SCA) 350 000 – 700 000 /rok • VF – ok. 25 – 30 % • AED is available – VF – 59 – 65% 8
Introduction • Europe – sudden cardiac arrest (SCA) 350 000 – 700 000 /rok • VF – ok. 25 – 30 % • AED is available – VF – 59 – 65% 8
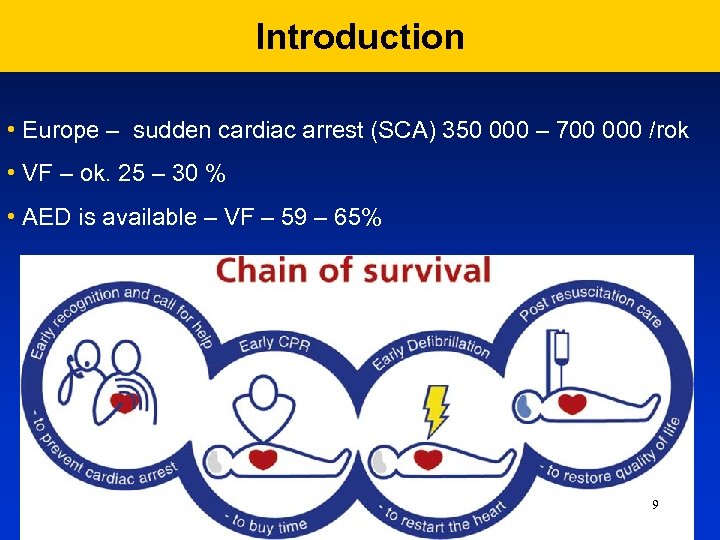 Introduction • Europe – sudden cardiac arrest (SCA) 350 000 – 700 000 /rok • VF – ok. 25 – 30 % • AED is available – VF – 59 – 65% 9
Introduction • Europe – sudden cardiac arrest (SCA) 350 000 – 700 000 /rok • VF – ok. 25 – 30 % • AED is available – VF – 59 – 65% 9
 Introduction Following VF OHCA, cardiopulmonary resuscitation plus defibrillation within 3– 5 min of collapse can produce survival rates as high as 49– 75%. Each minute of delay before defibrillation reduces the probability of survival to discharge by 10– 12%. 10
Introduction Following VF OHCA, cardiopulmonary resuscitation plus defibrillation within 3– 5 min of collapse can produce survival rates as high as 49– 75%. Each minute of delay before defibrillation reduces the probability of survival to discharge by 10– 12%. 10
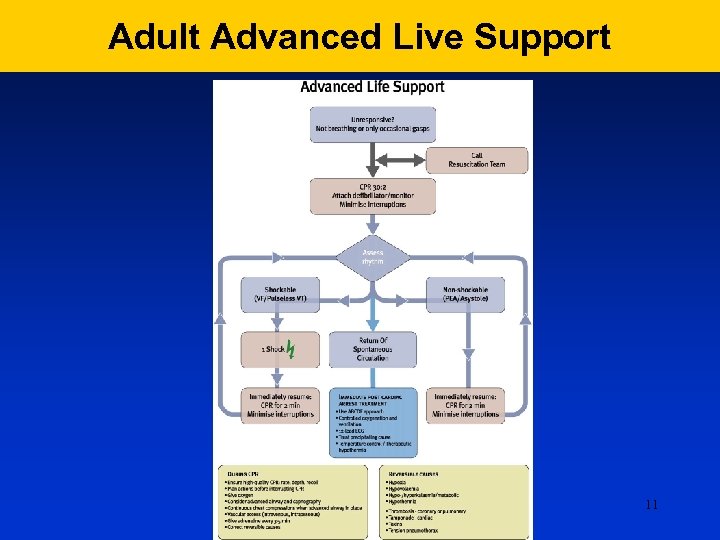 Adult Advanced Live Support 11
Adult Advanced Live Support 11
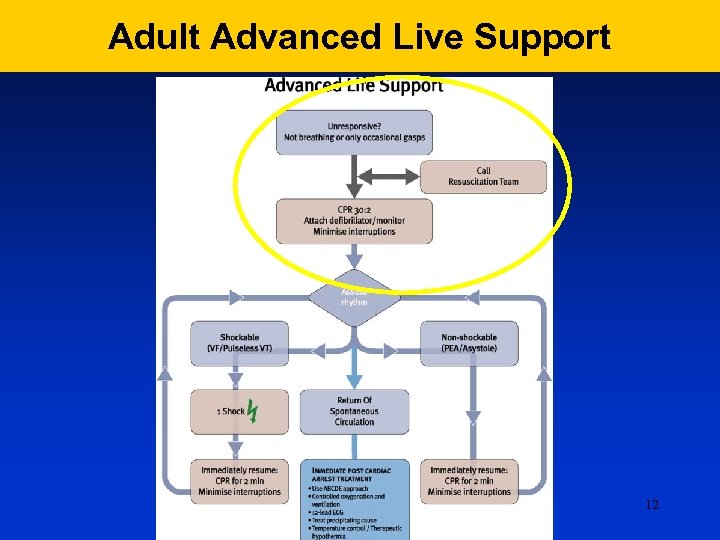 Adult Advanced Live Support 12
Adult Advanced Live Support 12
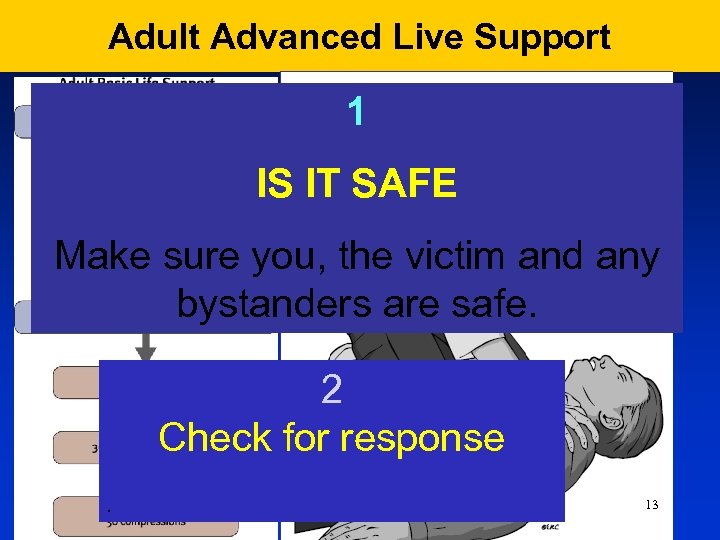 Adult Advanced Live Support 1 IS IT SAFE Make sure you, the victim and any bystanders are safe. 2 Check for response. 13
Adult Advanced Live Support 1 IS IT SAFE Make sure you, the victim and any bystanders are safe. 2 Check for response. 13
 Adult Advanced Live Support 3 Shout for help 14
Adult Advanced Live Support 3 Shout for help 14
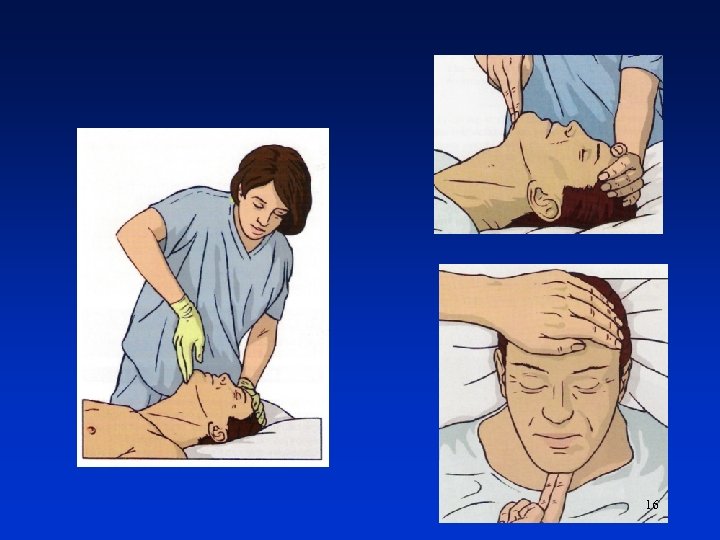
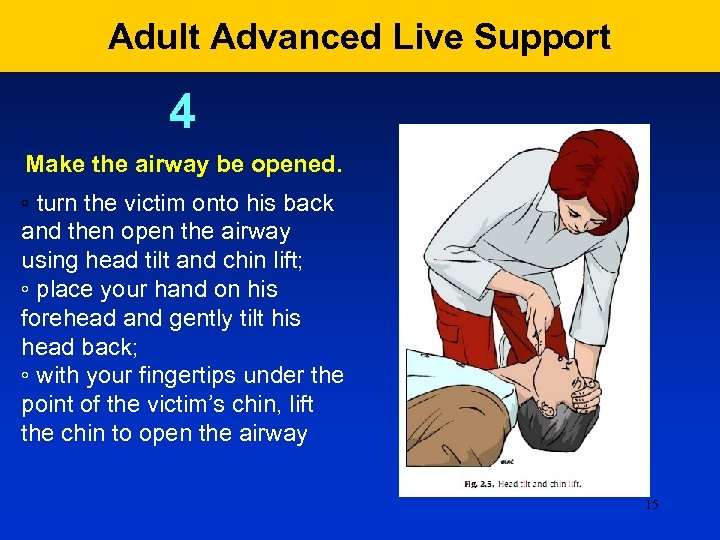 Adult Advanced Live Support 4 Make the airway be opened. ◦ turn the victim onto his back and then open the airway using head tilt and chin lift; ◦ place your hand on his forehead and gently tilt his head back; ◦ with your fingertips under the point of the victim’s chin, lift the chin to open the airway 15
Adult Advanced Live Support 4 Make the airway be opened. ◦ turn the victim onto his back and then open the airway using head tilt and chin lift; ◦ place your hand on his forehead and gently tilt his head back; ◦ with your fingertips under the point of the victim’s chin, lift the chin to open the airway 15
 16
16
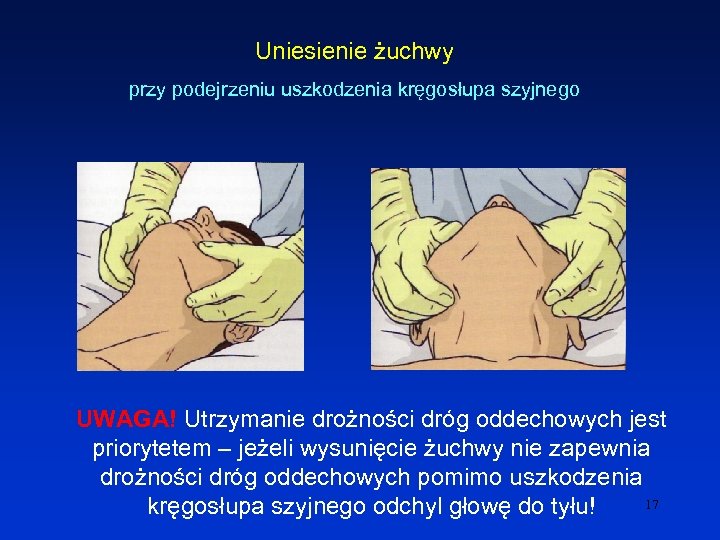 Uniesienie żuchwy przy podejrzeniu uszkodzenia kręgosłupa szyjnego UWAGA! Utrzymanie drożności dróg oddechowych jest priorytetem – jeżeli wysunięcie żuchwy nie zapewnia drożności dróg oddechowych pomimo uszkodzenia 17 kręgosłupa szyjnego odchyl głowę do tyłu!
Uniesienie żuchwy przy podejrzeniu uszkodzenia kręgosłupa szyjnego UWAGA! Utrzymanie drożności dróg oddechowych jest priorytetem – jeżeli wysunięcie żuchwy nie zapewnia drożności dróg oddechowych pomimo uszkodzenia 17 kręgosłupa szyjnego odchyl głowę do tyłu!
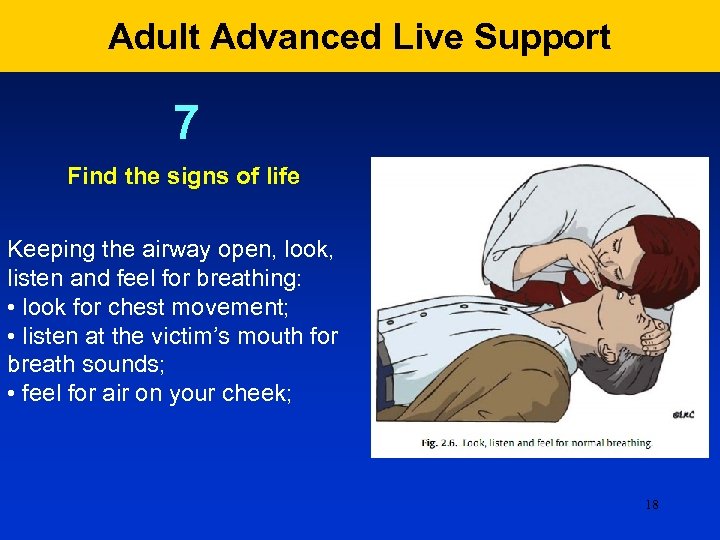 Adult Advanced Live Support 7 Find the signs of life Keeping the airway open, look, listen and feel for breathing: • look for chest movement; • listen at the victim’s mouth for breath sounds; • feel for air on your cheek; 18
Adult Advanced Live Support 7 Find the signs of life Keeping the airway open, look, listen and feel for breathing: • look for chest movement; • listen at the victim’s mouth for breath sounds; • feel for air on your cheek; 18
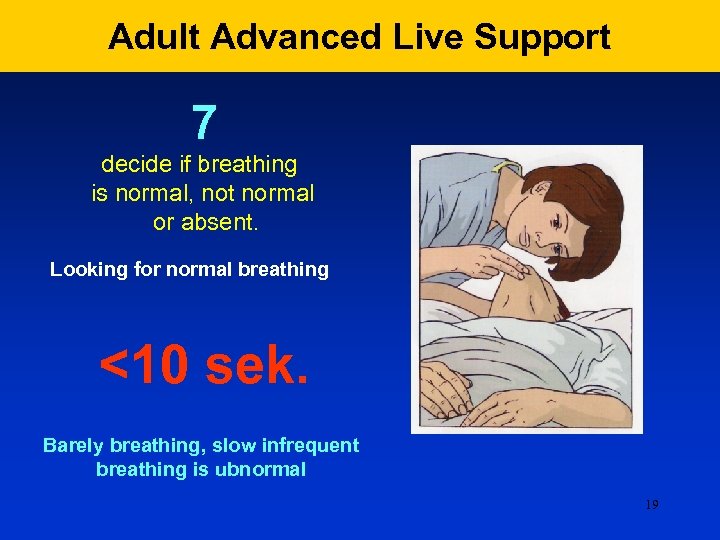 Adult Advanced Live Support 7 decide if breathing is normal, not normal or absent. Looking for normal breathing <10 sek. Barely breathing, slow infrequent breathing is ubnormal 19
Adult Advanced Live Support 7 decide if breathing is normal, not normal or absent. Looking for normal breathing <10 sek. Barely breathing, slow infrequent breathing is ubnormal 19
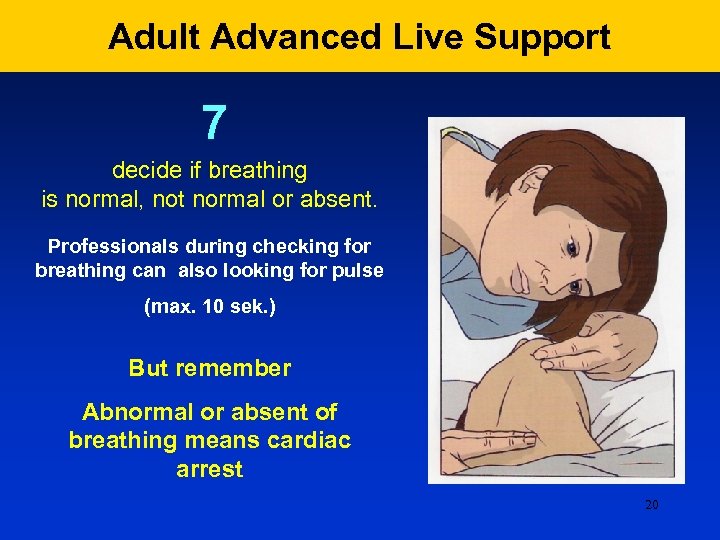 Adult Advanced Live Support 7 decide if breathing is normal, not normal or absent. Professionals during checking for breathing can also looking for pulse (max. 10 sek. ) But remember Abnormal or absent of breathing means cardiac arrest 20
Adult Advanced Live Support 7 decide if breathing is normal, not normal or absent. Professionals during checking for breathing can also looking for pulse (max. 10 sek. ) But remember Abnormal or absent of breathing means cardiac arrest 20
 Adult Advanced Live Support If there are no signs of life: send someone for help and to find and bring an AED if available; or if you are on your own, use your mobile phone to alert the ambulance service leave the victim only when there is no other option v 21
Adult Advanced Live Support If there are no signs of life: send someone for help and to find and bring an AED if available; or if you are on your own, use your mobile phone to alert the ambulance service leave the victim only when there is no other option v 21
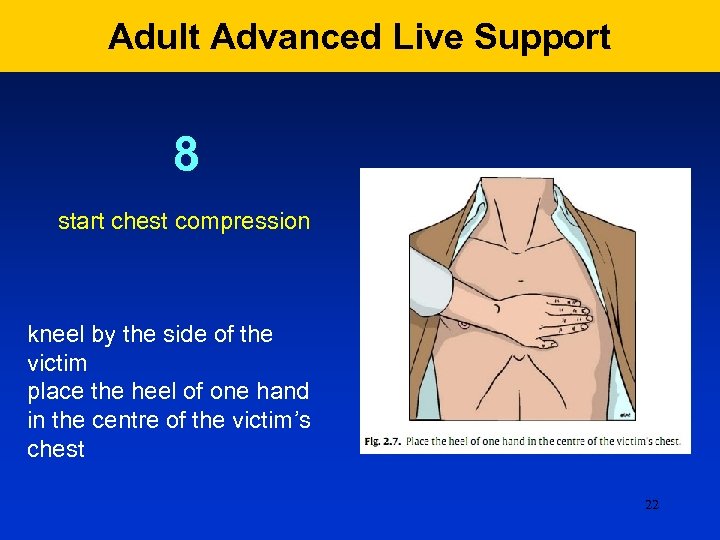 Adult Advanced Live Support 8 start chest compression kneel by the side of the victim place the heel of one hand in the centre of the victim’s chest 22
Adult Advanced Live Support 8 start chest compression kneel by the side of the victim place the heel of one hand in the centre of the victim’s chest 22
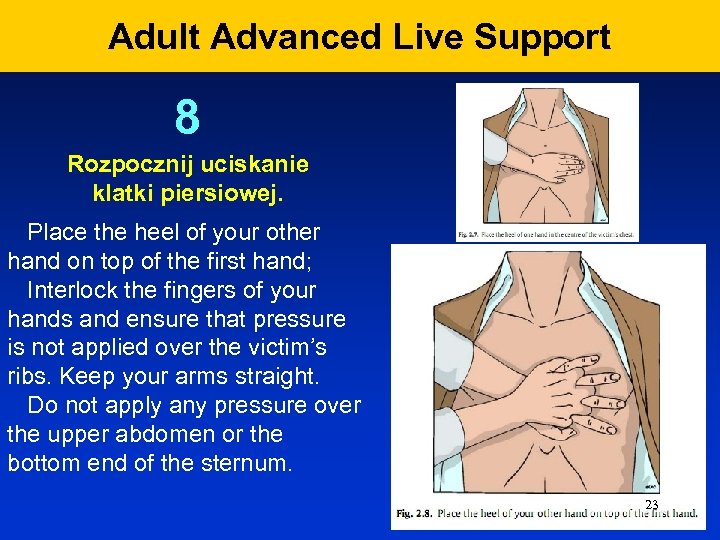 Adult Advanced Live Support 8 Rozpocznij uciskanie klatki piersiowej. Place the heel of your other hand on top of the first hand; Interlock the fingers of your hands and ensure that pressure is not applied over the victim’s ribs. Keep your arms straight. Do not apply any pressure over the upper abdomen or the bottom end of the sternum. 23
Adult Advanced Live Support 8 Rozpocznij uciskanie klatki piersiowej. Place the heel of your other hand on top of the first hand; Interlock the fingers of your hands and ensure that pressure is not applied over the victim’s ribs. Keep your arms straight. Do not apply any pressure over the upper abdomen or the bottom end of the sternum. 23
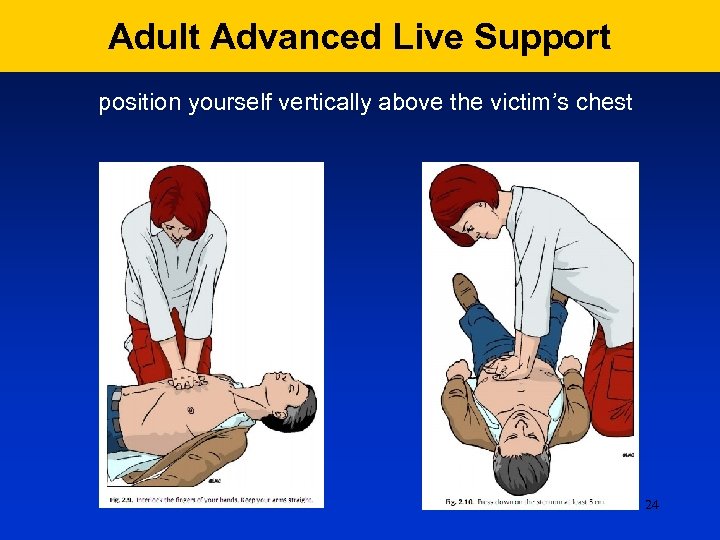 Adult Advanced Live Support position yourself vertically above the victim’s chest 24
Adult Advanced Live Support position yourself vertically above the victim’s chest 24
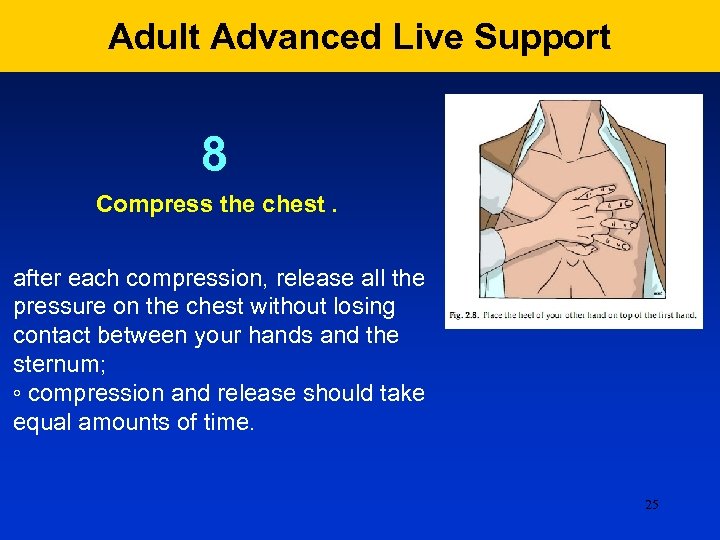 Adult Advanced Live Support 8 Compress the chest. after each compression, release all the pressure on the chest without losing contact between your hands and the sternum; ◦ compression and release should take equal amounts of time. 25
Adult Advanced Live Support 8 Compress the chest. after each compression, release all the pressure on the chest without losing contact between your hands and the sternum; ◦ compression and release should take equal amounts of time. 25
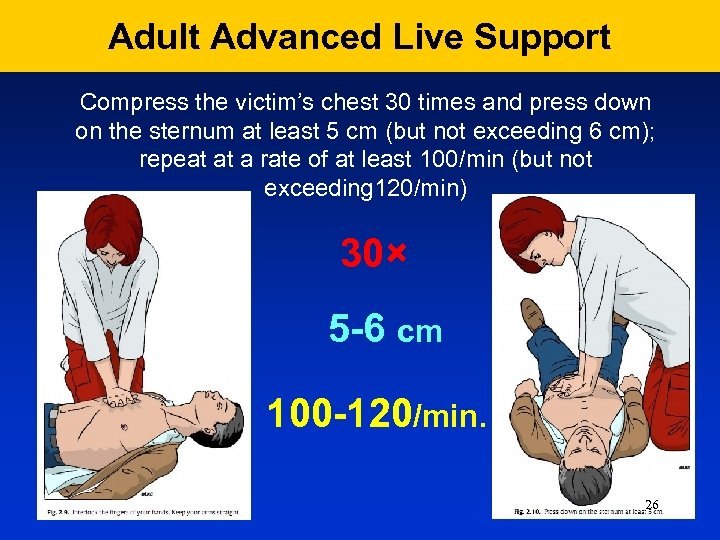 Adult Advanced Live Support Compress the victim’s chest 30 times and press down on the sternum at least 5 cm (but not exceeding 6 cm); repeat at a rate of at least 100/min (but not exceeding 120/min) 30× 5 -6 cm 100 -120/min. 26
Adult Advanced Live Support Compress the victim’s chest 30 times and press down on the sternum at least 5 cm (but not exceeding 6 cm); repeat at a rate of at least 100/min (but not exceeding 120/min) 30× 5 -6 cm 100 -120/min. 26
 Adult Advanced Live Support Przybliżone wartości głębokości ucisków klatki piersiowej: Adults: at least 5 cm (but not exceeding 6 cm) Niemowlęta: 1/3 wymiaru poprzecznego klatki piersiowej (ok. 4 cm) Chiildren>1 r. ż. : 1/3 wymiaru poprzecznego klatki piersiowej (ok. 5 cm) 30: 2 27
Adult Advanced Live Support Przybliżone wartości głębokości ucisków klatki piersiowej: Adults: at least 5 cm (but not exceeding 6 cm) Niemowlęta: 1/3 wymiaru poprzecznego klatki piersiowej (ok. 4 cm) Chiildren>1 r. ż. : 1/3 wymiaru poprzecznego klatki piersiowej (ok. 5 cm) 30: 2 27
 Adult Advanced Live Support Przybliżone wartości głębokości ucisków klatki piersiowej: 30: 2 Dorośli: przynajmniej 5 cm (ale nie przekraczać 6 cm) Niemowlęta: 1/3 wymiaru poprzecznego klatki piersiowej (ok. 4 cm) Dzieci >1 r. ż. : 1/3 wymiaru poprzecznego klatki piersiowej (ok. 5 cm) 15: 2 28
Adult Advanced Live Support Przybliżone wartości głębokości ucisków klatki piersiowej: 30: 2 Dorośli: przynajmniej 5 cm (ale nie przekraczać 6 cm) Niemowlęta: 1/3 wymiaru poprzecznego klatki piersiowej (ok. 4 cm) Dzieci >1 r. ż. : 1/3 wymiaru poprzecznego klatki piersiowej (ok. 5 cm) 15: 2 28
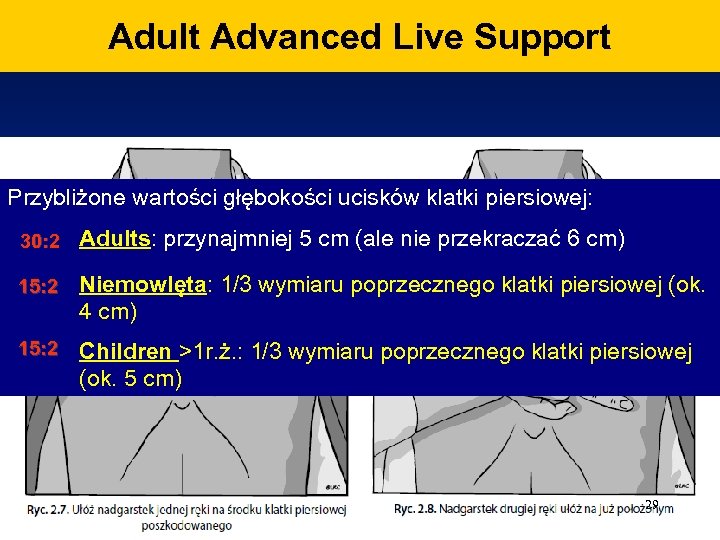 Adult Advanced Live Support Przybliżone wartości głębokości ucisków klatki piersiowej: 30: 2 Adults: przynajmniej 5 cm (ale nie przekraczać 6 cm) 15: 2 Niemowlęta: 1/3 wymiaru poprzecznego klatki piersiowej (ok. 4 cm) 15: 2 Children >1 r. ż. : 1/3 wymiaru poprzecznego klatki piersiowej (ok. 5 cm) 29
Adult Advanced Live Support Przybliżone wartości głębokości ucisków klatki piersiowej: 30: 2 Adults: przynajmniej 5 cm (ale nie przekraczać 6 cm) 15: 2 Niemowlęta: 1/3 wymiaru poprzecznego klatki piersiowej (ok. 4 cm) 15: 2 Children >1 r. ż. : 1/3 wymiaru poprzecznego klatki piersiowej (ok. 5 cm) 29
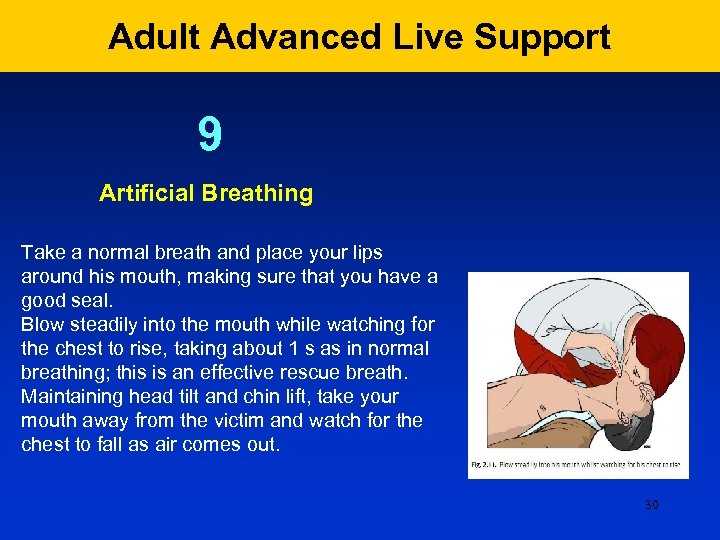 Adult Advanced Live Support 9 Artificial Breathing Take a normal breath and place your lips around his mouth, making sure that you have a good seal. Blow steadily into the mouth while watching for the chest to rise, taking about 1 s as in normal breathing; this is an effective rescue breath. Maintaining head tilt and chin lift, take your mouth away from the victim and watch for the chest to fall as air comes out. 30
Adult Advanced Live Support 9 Artificial Breathing Take a normal breath and place your lips around his mouth, making sure that you have a good seal. Blow steadily into the mouth while watching for the chest to rise, taking about 1 s as in normal breathing; this is an effective rescue breath. Maintaining head tilt and chin lift, take your mouth away from the victim and watch for the chest to fall as air comes out. 30
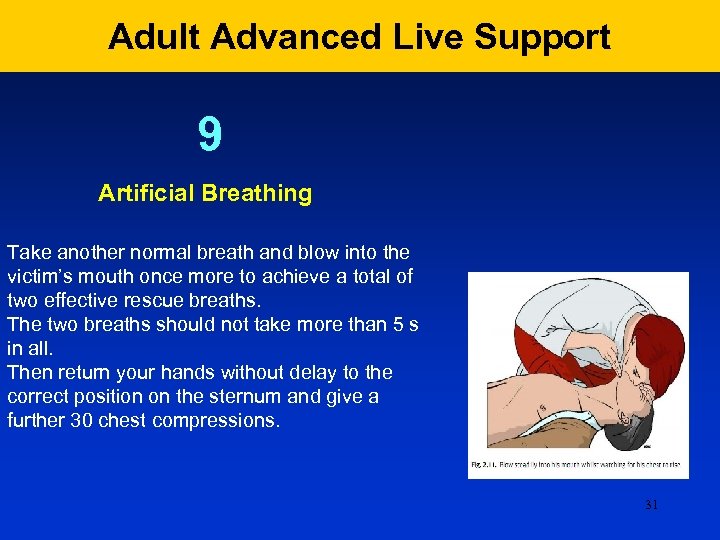 Adult Advanced Live Support 9 Artificial Breathing Take another normal breath and blow into the victim’s mouth once more to achieve a total of two effective rescue breaths. The two breaths should not take more than 5 s in all. Then return your hands without delay to the correct position on the sternum and give a further 30 chest compressions. 31
Adult Advanced Live Support 9 Artificial Breathing Take another normal breath and blow into the victim’s mouth once more to achieve a total of two effective rescue breaths. The two breaths should not take more than 5 s in all. Then return your hands without delay to the correct position on the sternum and give a further 30 chest compressions. 31
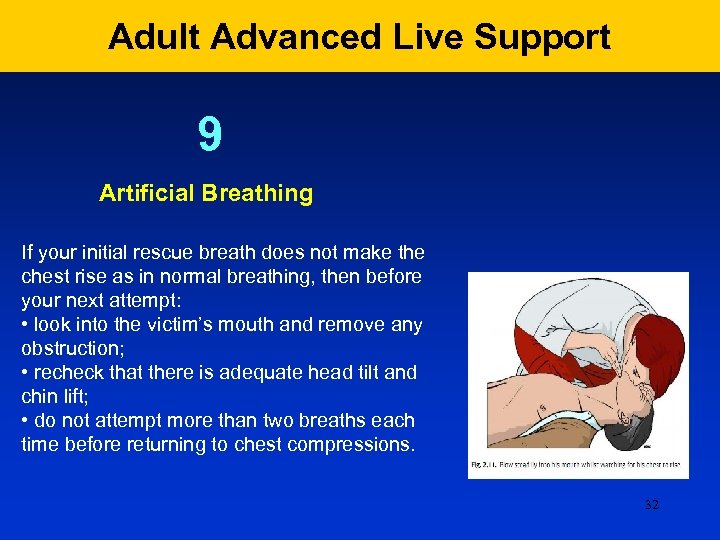 Adult Advanced Live Support 9 Artificial Breathing If your initial rescue breath does not make the chest rise as in normal breathing, then before your next attempt: • look into the victim’s mouth and remove any obstruction; • recheck that there is adequate head tilt and chin lift; • do not attempt more than two breaths each time before returning to chest compressions. 32
Adult Advanced Live Support 9 Artificial Breathing If your initial rescue breath does not make the chest rise as in normal breathing, then before your next attempt: • look into the victim’s mouth and remove any obstruction; • recheck that there is adequate head tilt and chin lift; • do not attempt more than two breaths each time before returning to chest compressions. 32
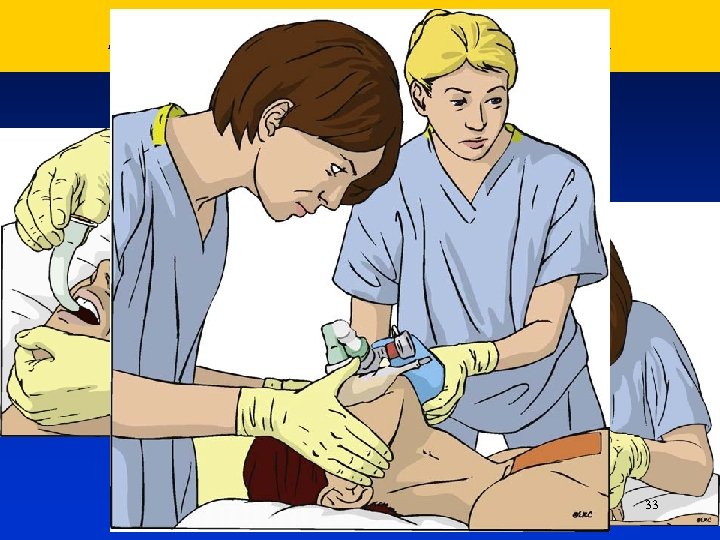 Adult Advanced Live Support 33
Adult Advanced Live Support 33
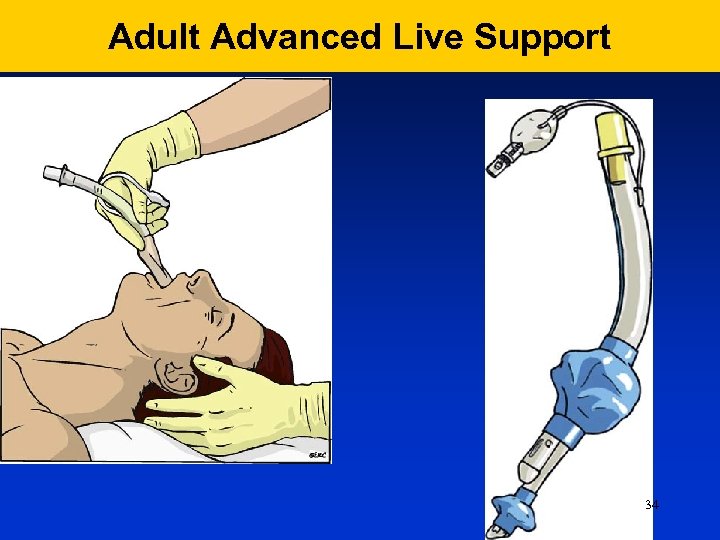 Adult Advanced Live Support 34
Adult Advanced Live Support 34
 Adult Advanced Live Support 9 Artificial Breathing if you are not trained, or are unwilling to give rescue breaths, give chest compressions only; • if only chest compressions are given, these should be continuous, at a rate of at least 100/min (but not exceeding 120/min). ? 35
Adult Advanced Live Support 9 Artificial Breathing if you are not trained, or are unwilling to give rescue breaths, give chest compressions only; • if only chest compressions are given, these should be continuous, at a rate of at least 100/min (but not exceeding 120/min). ? 35
 Adult Advanced Live Support • compression of the chest = release • Minimize the break between compressions • Speed 100/min (120) • Only chest compression…. ? (Animal studies have shown that chest-compression-only CPR may be as effective as combined ventilation and compression in the first few minutes after non-asphyxial arrest) (chest compression- only CPR have shown that arterial oxygen stores deplete in 2– 4 min) 36
Adult Advanced Live Support • compression of the chest = release • Minimize the break between compressions • Speed 100/min (120) • Only chest compression…. ? (Animal studies have shown that chest-compression-only CPR may be as effective as combined ventilation and compression in the first few minutes after non-asphyxial arrest) (chest compression- only CPR have shown that arterial oxygen stores deplete in 2– 4 min) 36
 Adult Basic Live Support Chest compression-only may be sufficient only in the first few minutes after collapse. Chest-compression-only CPR is not as effective as conventional CPR for cardiac arrests of non-cardiac origin (e. g. , drowning or suffocation) in adults and children. Chest compression combined with rescue breaths is, therefore, the method of choice for CPR delivered by both trained lay rescuers and professionals. 37
Adult Basic Live Support Chest compression-only may be sufficient only in the first few minutes after collapse. Chest-compression-only CPR is not as effective as conventional CPR for cardiac arrests of non-cardiac origin (e. g. , drowning or suffocation) in adults and children. Chest compression combined with rescue breaths is, therefore, the method of choice for CPR delivered by both trained lay rescuers and professionals. 37
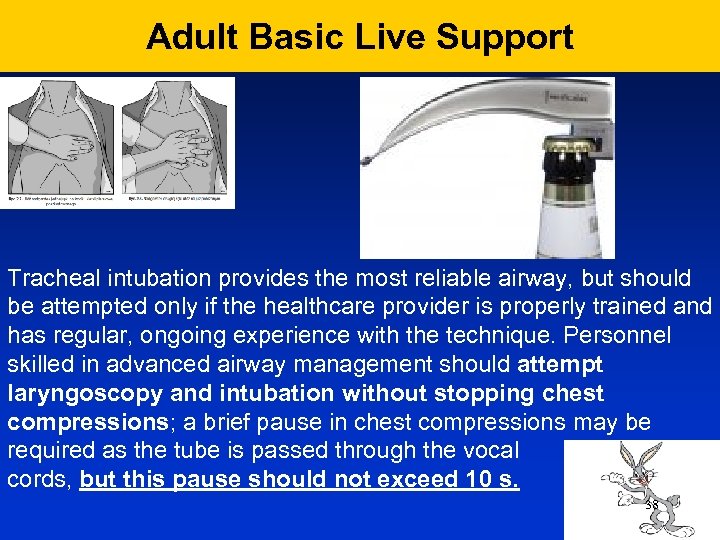 Adult Basic Live Support Tracheal intubation provides the most reliable airway, but should be attempted only if the healthcare provider is properly trained and has regular, ongoing experience with the technique. Personnel skilled in advanced airway management should attempt laryngoscopy and intubation without stopping chest compressions; a brief pause in chest compressions may be required as the tube is passed through the vocal cords, but this pause should not exceed 10 s. 38
Adult Basic Live Support Tracheal intubation provides the most reliable airway, but should be attempted only if the healthcare provider is properly trained and has regular, ongoing experience with the technique. Personnel skilled in advanced airway management should attempt laryngoscopy and intubation without stopping chest compressions; a brief pause in chest compressions may be required as the tube is passed through the vocal cords, but this pause should not exceed 10 s. 38
 Adult Basic Live Support 10 Continuation • Continue with chest compressions and rescue breaths in a ratio of 30: 2. • Stop to recheck the victim only if he starts to wake up: to move, opens eyes and to breathe normally. Otherwise, do not interrupt resuscitation. 39
Adult Basic Live Support 10 Continuation • Continue with chest compressions and rescue breaths in a ratio of 30: 2. • Stop to recheck the victim only if he starts to wake up: to move, opens eyes and to breathe normally. Otherwise, do not interrupt resuscitation. 39
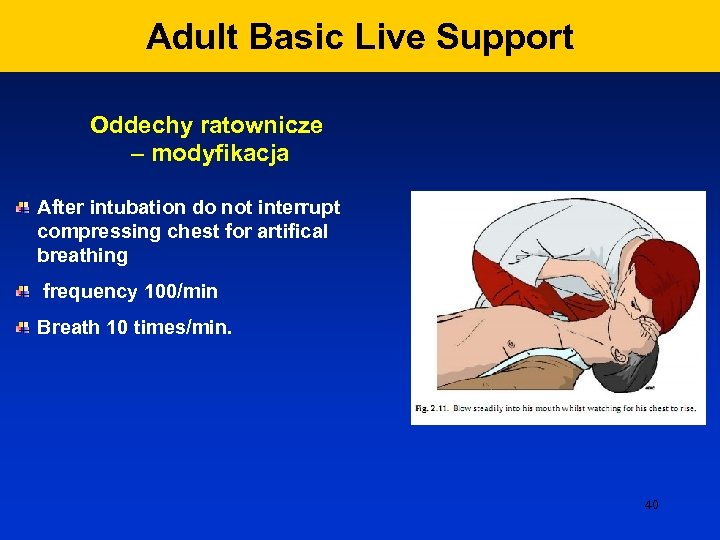 Adult Basic Live Support Oddechy ratownicze – modyfikacja After intubation do not interrupt compressing chest for artifical breathing frequency 100/min Breath 10 times/min. 40
Adult Basic Live Support Oddechy ratownicze – modyfikacja After intubation do not interrupt compressing chest for artifical breathing frequency 100/min Breath 10 times/min. 40
 Adult Advanced Live Support When the cardio-monitor will be available assess the rhythm 41
Adult Advanced Live Support When the cardio-monitor will be available assess the rhythm 41
 Adult Advanced Live Support When the cardio-monitor will be available assess the rhythm When the defibrillator arrives, apply the paddles to the patient and analyse the rhythm. If self-adhesive defibrillation pads are available, apply these without interrupting chest compressions. The use of adhesive electrode pads or a ‘quick-look’ paddles technique will enable rapid assessment of heart rhythm compared with attaching ECG electrodes. Pause briefly to assess the heart rhythm. With a manual defibrillator, if the rhythm is VF/VT charge the defibrillator while another rescuer continues chest 42 compressions.
Adult Advanced Live Support When the cardio-monitor will be available assess the rhythm When the defibrillator arrives, apply the paddles to the patient and analyse the rhythm. If self-adhesive defibrillation pads are available, apply these without interrupting chest compressions. The use of adhesive electrode pads or a ‘quick-look’ paddles technique will enable rapid assessment of heart rhythm compared with attaching ECG electrodes. Pause briefly to assess the heart rhythm. With a manual defibrillator, if the rhythm is VF/VT charge the defibrillator while another rescuer continues chest 42 compressions.
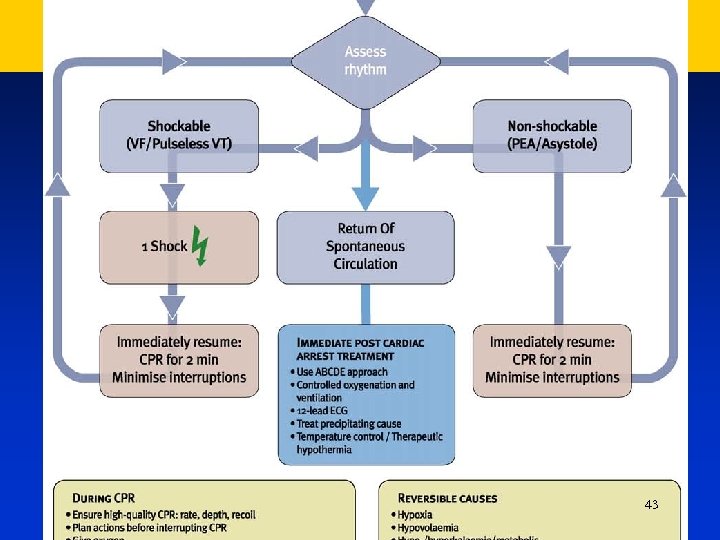 Adult Advanced Live Support When the cardio-monitor will be available check the rhythm 43
Adult Advanced Live Support When the cardio-monitor will be available check the rhythm 43
 Adult Advanced Live Support With a manual defibrillator, if the rhythm is VF/VT charge the defibrillator while another rescuer continues chest compressions. Once the defibrillator is charged, pause the chest compressions, ensure that all rescuers are clear of the patient and give one shock (360 J monophasic or 150– 200 J biphasic) Minimise the delay between stopping chest compressions and delivery of the shock (the preshock pause) 44
Adult Advanced Live Support With a manual defibrillator, if the rhythm is VF/VT charge the defibrillator while another rescuer continues chest compressions. Once the defibrillator is charged, pause the chest compressions, ensure that all rescuers are clear of the patient and give one shock (360 J monophasic or 150– 200 J biphasic) Minimise the delay between stopping chest compressions and delivery of the shock (the preshock pause) 44
 Adult Advanced Live Support Without reassessing the rhythm or feeling for a pulse, resume CPR (CV ratio 30: 2) immediately after the shock, starting with chest compressions. Even if the defibrillation attempt is successful inrestoring a perfusing rhythm, it takes time until the post-shock circulation is established and it is very rare for a pulse to be palpable immediately after defibrillation. 45
Adult Advanced Live Support Without reassessing the rhythm or feeling for a pulse, resume CPR (CV ratio 30: 2) immediately after the shock, starting with chest compressions. Even if the defibrillation attempt is successful inrestoring a perfusing rhythm, it takes time until the post-shock circulation is established and it is very rare for a pulse to be palpable immediately after defibrillation. 45
 Adult Advanced Live Support Continue CPR for 2 min, then pause briefly to assess the rhythm; if still VF/VT, give a second shock (360 -J monophasic or 150– 360 -J biphasic). Without reassessing the rhythm or feeling for a pulse, resume CPR (CV ratio 30: 2) immediately after the shock, starting with chest compressions. 46
Adult Advanced Live Support Continue CPR for 2 min, then pause briefly to assess the rhythm; if still VF/VT, give a second shock (360 -J monophasic or 150– 360 -J biphasic). Without reassessing the rhythm or feeling for a pulse, resume CPR (CV ratio 30: 2) immediately after the shock, starting with chest compressions. 46
 Adult Advanced Live Support Continue CPR for 2 min, then pause briefly to assess the rhythm; if still VF/VT, give a third shock (360 J monophasic or 150– 360 J biphasic). Without reassessing the rhythm or feeling for a pulse, resume CPR (CV ratio 30: 2) immediately after the shock, starting with chest compressions. If IV/IO access has been obtained, give adrenaline 1 mg and amiodarone 300 mg once compressions have resumed. 47
Adult Advanced Live Support Continue CPR for 2 min, then pause briefly to assess the rhythm; if still VF/VT, give a third shock (360 J monophasic or 150– 360 J biphasic). Without reassessing the rhythm or feeling for a pulse, resume CPR (CV ratio 30: 2) immediately after the shock, starting with chest compressions. If IV/IO access has been obtained, give adrenaline 1 mg and amiodarone 300 mg once compressions have resumed. 47
 Adult Advanced Live Support If signs of life return during CPR (purposeful movement, normal breathing, or coughing), check the monitor; if an organised rhythm is present, check for a pulse. If a pulse is palpable, continue post-resuscitation care and/or treatment of peri-arrest arrhythmia ROSC Post resuciation care 48
Adult Advanced Live Support If signs of life return during CPR (purposeful movement, normal breathing, or coughing), check the monitor; if an organised rhythm is present, check for a pulse. If a pulse is palpable, continue post-resuscitation care and/or treatment of peri-arrest arrhythmia ROSC Post resuciation care 48
 Adult Advanced Live Support 3 shocks (one by one) If a patient has a monitored and witnessed cardiac arrest in the catheter laboratory or early after cardiac surgery Confirm cardiac arrest and shout for help. • If the initial rhythm is VF/VT, give up to three quick successive (stacked) shocks. Start chest compressions immediately after the third shock and continue CPR for 2 min. 49
Adult Advanced Live Support 3 shocks (one by one) If a patient has a monitored and witnessed cardiac arrest in the catheter laboratory or early after cardiac surgery Confirm cardiac arrest and shout for help. • If the initial rhythm is VF/VT, give up to three quick successive (stacked) shocks. Start chest compressions immediately after the third shock and continue CPR for 2 min. 49
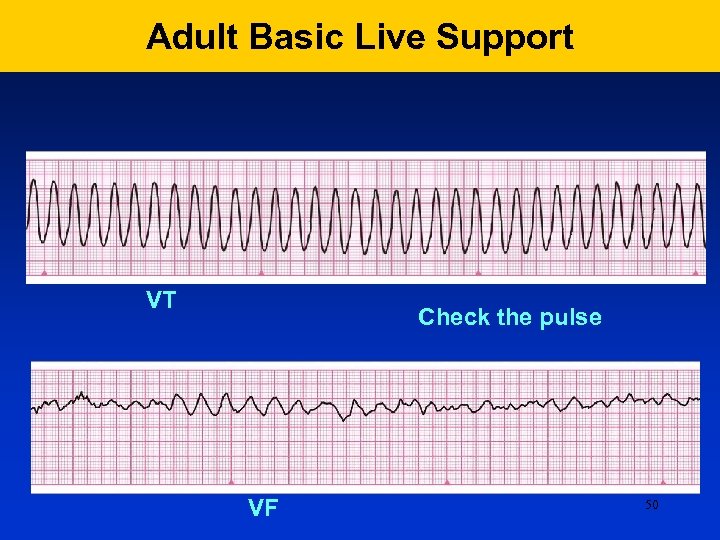 Adult Basic Live Support VT Check the pulse VF 50
Adult Basic Live Support VT Check the pulse VF 50
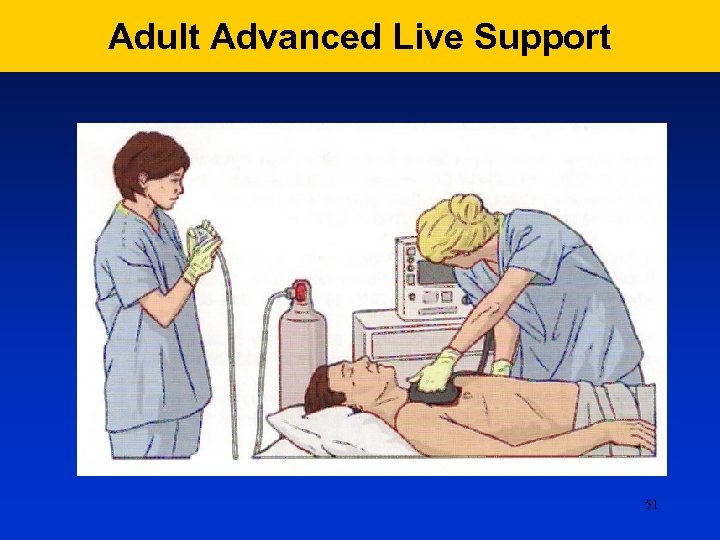 Adult Advanced Live Support 51
Adult Advanced Live Support 51
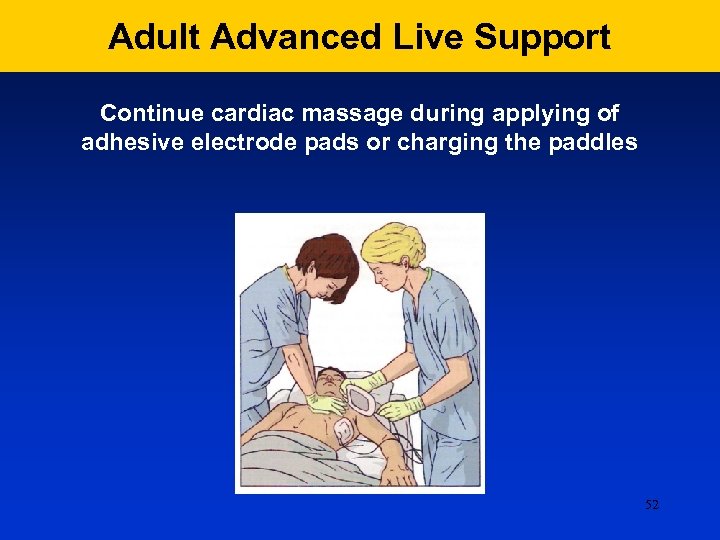 Adult Advanced Live Support Continue cardiac massage during applying of adhesive electrode pads or charging the paddles 52
Adult Advanced Live Support Continue cardiac massage during applying of adhesive electrode pads or charging the paddles 52
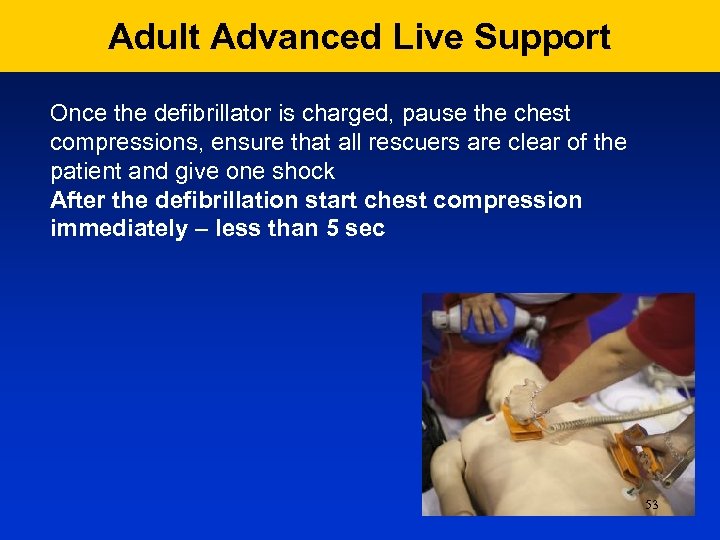 Adult Advanced Live Support Once the defibrillator is charged, pause the chest compressions, ensure that all rescuers are clear of the patient and give one shock After the defibrillation start chest compression immediately – less than 5 sec 53
Adult Advanced Live Support Once the defibrillator is charged, pause the chest compressions, ensure that all rescuers are clear of the patient and give one shock After the defibrillation start chest compression immediately – less than 5 sec 53
 Zmiany w wytycznych ALS Drugs to the tracheal tube ? If intravenous access is unavaiable give the drugs by Intraosseous route 54
Zmiany w wytycznych ALS Drugs to the tracheal tube ? If intravenous access is unavaiable give the drugs by Intraosseous route 54
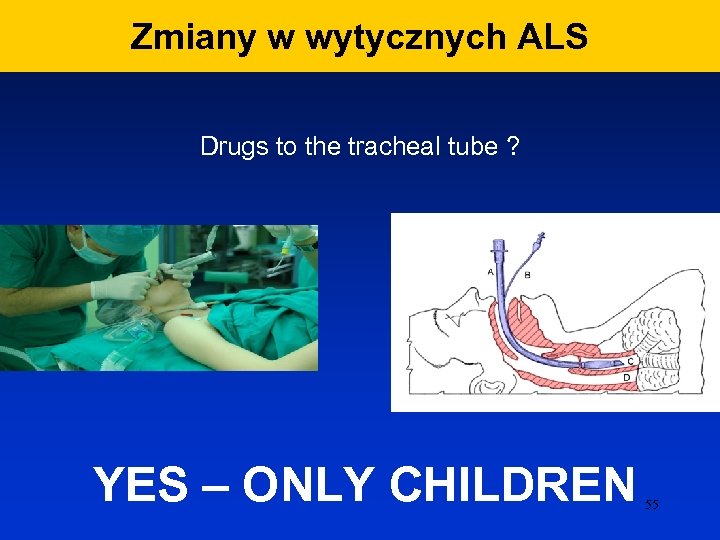 Zmiany w wytycznych ALS Drugs to the tracheal tube ? YES – ONLY CHILDREN 55
Zmiany w wytycznych ALS Drugs to the tracheal tube ? YES – ONLY CHILDREN 55
 Adult Advanced Live Support REVERSIBLE CAUSES OF SCA FOUR „Hs” FOUR„Ts” • hypoxia • tension pneumothorax • hypovolemia • Trombosis - coronary or pulmonary • hypo-/hyperkalemia/ metabolic • hypothermia • tamponade cardiac • toxins/leki/trucizny 56
Adult Advanced Live Support REVERSIBLE CAUSES OF SCA FOUR „Hs” FOUR„Ts” • hypoxia • tension pneumothorax • hypovolemia • Trombosis - coronary or pulmonary • hypo-/hyperkalemia/ metabolic • hypothermia • tamponade cardiac • toxins/leki/trucizny 56
 Adult Advanced Live Support Epinephrine The alpha adrenergic actions of adrenaline cause vasoconstriction, which increases myocardial and cerebral perfusion pressure. The higher coronary blood flow increases the frequency and amplitude ofther VF waveform and should improve the chance of restoring a circulation when defibrillation is attempted every 3–– 5 min of CPR (alternate cycles). Dose 1 mg Do not interrupt CPR to give drugs. 57
Adult Advanced Live Support Epinephrine The alpha adrenergic actions of adrenaline cause vasoconstriction, which increases myocardial and cerebral perfusion pressure. The higher coronary blood flow increases the frequency and amplitude ofther VF waveform and should improve the chance of restoring a circulation when defibrillation is attempted every 3–– 5 min of CPR (alternate cycles). Dose 1 mg Do not interrupt CPR to give drugs. 57
 Adult Advanced Live Support Epinephrine In a patient, who is asystolic or PEA give a dose of epinephrine as soon as possible (as soon as you will get an access to the vein) Dose 1 mg every 3–– 5 min of CPR (alternate cycles). Do not interrupt CPR to give drugs. 58
Adult Advanced Live Support Epinephrine In a patient, who is asystolic or PEA give a dose of epinephrine as soon as possible (as soon as you will get an access to the vein) Dose 1 mg every 3–– 5 min of CPR (alternate cycles). Do not interrupt CPR to give drugs. 58
 Adult Advanced Live Support Amiodaron EBM - improves the short-term outcome of survival to hospital admission Działanie membrane-stabilising anti-arrhythmic drug that increases the duration of the action potential and refractory period in atrial and ventricular myocardium Wskazania: refractory VF/VT; haemodynamically stable ventricular tachycardia (VT) and other resistant tachyarrhythmias Dose: • 300 mg iv diluted in 5% dextrose to the volume 59 of 20 ml
Adult Advanced Live Support Amiodaron EBM - improves the short-term outcome of survival to hospital admission Działanie membrane-stabilising anti-arrhythmic drug that increases the duration of the action potential and refractory period in atrial and ventricular myocardium Wskazania: refractory VF/VT; haemodynamically stable ventricular tachycardia (VT) and other resistant tachyarrhythmias Dose: • 300 mg iv diluted in 5% dextrose to the volume 59 of 20 ml
 Adult Advanced Live Support Lidokaina Lidocaine is indicated in refractory VF/VT (when amiodarone is unavailable). Dose: consider an initial dose of 100 mg (1– 1. 5 mg/kg) of lidocaine for VF/pulseless VT refractory to three shocks. Give an additional bolus of 50 mg if necessary. The total dose should not exceed 3 mg/kg during the first hour. 60
Adult Advanced Live Support Lidokaina Lidocaine is indicated in refractory VF/VT (when amiodarone is unavailable). Dose: consider an initial dose of 100 mg (1– 1. 5 mg/kg) of lidocaine for VF/pulseless VT refractory to three shocks. Give an additional bolus of 50 mg if necessary. The total dose should not exceed 3 mg/kg during the first hour. 60
 Adult Advanced Live Support Magnez Drug acting: improves the contractile response of the stunned myocardium, and limits infarct size by a mechanism that has yet to be fully elucidated Indications: • ventricular or supraventricular tachycardia associated with hypomagnesaemia; • torsades de pointes; • digoxin toxicity. Dose 2 g (8 mmol) peripherally over 1– 2 min; it may be repeated after 10 61 – 15 min
Adult Advanced Live Support Magnez Drug acting: improves the contractile response of the stunned myocardium, and limits infarct size by a mechanism that has yet to be fully elucidated Indications: • ventricular or supraventricular tachycardia associated with hypomagnesaemia; • torsades de pointes; • digoxin toxicity. Dose 2 g (8 mmol) peripherally over 1– 2 min; it may be repeated after 10 61 – 15 min
 Adult Advanced Live Support Calcium may be harmful to the ischaemic myocardium and may impair cerebral recovery. Give calcium during resuscitation only when indicated specifically, hyperkalaemia; hypocalcaemia; overdose of calcium channel-blocking drugs. Dose: 10 ml 10% Calcium chloratum 62
Adult Advanced Live Support Calcium may be harmful to the ischaemic myocardium and may impair cerebral recovery. Give calcium during resuscitation only when indicated specifically, hyperkalaemia; hypocalcaemia; overdose of calcium channel-blocking drugs. Dose: 10 ml 10% Calcium chloratum 62
 Adult Advanced Live Support Natrium bicarbonicum Consider sodium bicarbonate for: • life-threatening hyperkalaemia; • cardiac arrest associated with hyperkalaemia; • tricyclic overdose. Dose: 50 ml 8, 4% Natrium bicarbonicum 63
Adult Advanced Live Support Natrium bicarbonicum Consider sodium bicarbonate for: • life-threatening hyperkalaemia; • cardiac arrest associated with hyperkalaemia; • tricyclic overdose. Dose: 50 ml 8, 4% Natrium bicarbonicum 63
 Adult Advanced Live Support Remember!!! NATRIUM BICARBONICUM CALCIUM CHLORATUM 64
Adult Advanced Live Support Remember!!! NATRIUM BICARBONICUM CALCIUM CHLORATUM 64
 Adult Advanced Live Support Atropine antagonises the action of the parasympathetic neurotransmitter acetylcholine at muscarinic receptors (blocking of n. X). Asystole during cardiac arrest is usually due to primary myocardial pathology rather than excessive vagal tone that’s why routine use for asystole or PEA is no longer recommended. 65
Adult Advanced Live Support Atropine antagonises the action of the parasympathetic neurotransmitter acetylcholine at muscarinic receptors (blocking of n. X). Asystole during cardiac arrest is usually due to primary myocardial pathology rather than excessive vagal tone that’s why routine use for asystole or PEA is no longer recommended. 65
 Pediatric Basic/Advanced Live Support 66
Pediatric Basic/Advanced Live Support 66
 Pediatric Basic/Advanced Live Support neonate < 4 tygodnia życia Newborn 1 – 12 miesięcy child 1 rż do okresu pokwitania 67
Pediatric Basic/Advanced Live Support neonate < 4 tygodnia życia Newborn 1 – 12 miesięcy child 1 rż do okresu pokwitania 67
 er cu y t fe sa he t e d. ur hil ns c E d an s re of 1 68
er cu y t fe sa he t e d. ur hil ns c E d an s re of 1 68
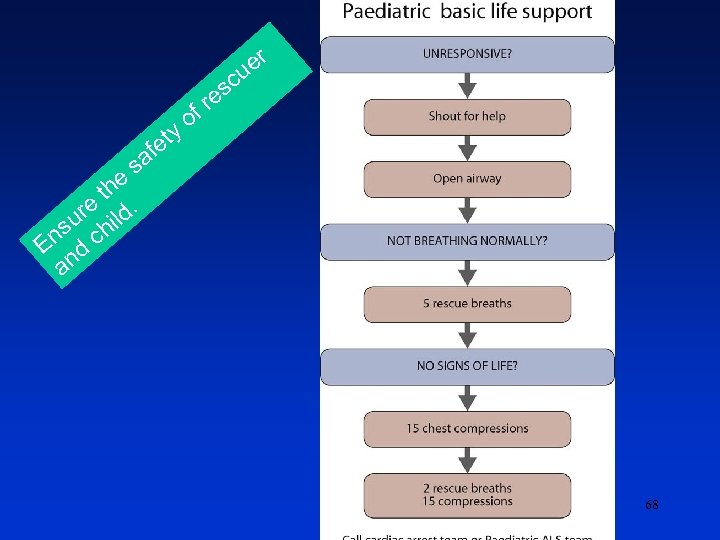
 Pediatric Basic/Advanced Live Support For both infants and children, if you have difficulty achieving an effective breath, the airway may be obstructed: • Open the child’s mouth and remove any visible obstruction. Do not perform a blind finger sweep. Ensure that there is adequate head tilt and chin lift but also that the neck is not over extended. • If head tilt and chin lift has not opened the airway, try the jaw thrust method. • Make up to five attempts to achieve effective breaths, if still unsuccessful, move on to chest compressions. 69
Pediatric Basic/Advanced Live Support For both infants and children, if you have difficulty achieving an effective breath, the airway may be obstructed: • Open the child’s mouth and remove any visible obstruction. Do not perform a blind finger sweep. Ensure that there is adequate head tilt and chin lift but also that the neck is not over extended. • If head tilt and chin lift has not opened the airway, try the jaw thrust method. • Make up to five attempts to achieve effective breaths, if still unsuccessful, move on to chest compressions. 69
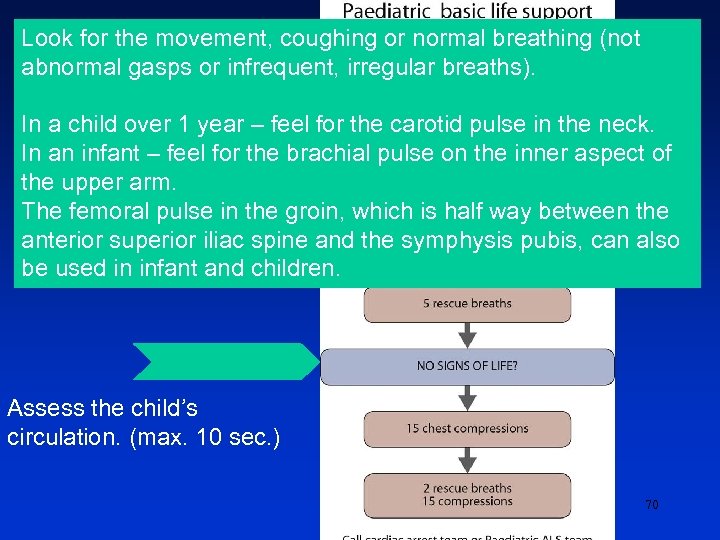 Look for the movement, coughing or normal breathing (not abnormal gasps or infrequent, irregular breaths). In a child over 1 year – feel for the carotid pulse in the neck. In an infant – feel for the brachial pulse on the inner aspect of the upper arm. The femoral pulse in the groin, which is half way between the anterior superior iliac spine and the symphysis pubis, can also be used in infant and children. 1 Assess the child’s circulation. (max. 10 sec. ) 70
Look for the movement, coughing or normal breathing (not abnormal gasps or infrequent, irregular breaths). In a child over 1 year – feel for the carotid pulse in the neck. In an infant – feel for the brachial pulse on the inner aspect of the upper arm. The femoral pulse in the groin, which is half way between the anterior superior iliac spine and the symphysis pubis, can also be used in infant and children. 1 Assess the child’s circulation. (max. 10 sec. ) 70
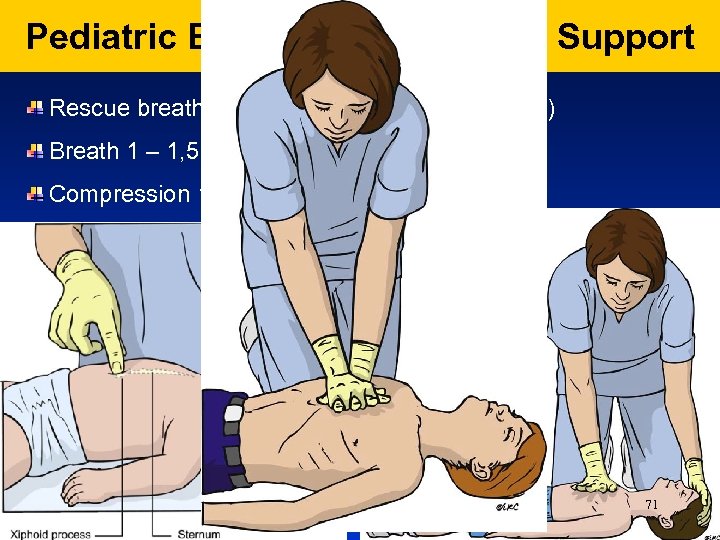 Pediatric Basic/Advanced Live Support Rescue breath (5 breaths, następnie CPR 15: 2) Breath 1 – 1, 5 sek. Compression 100 – 120/min 71
Pediatric Basic/Advanced Live Support Rescue breath (5 breaths, następnie CPR 15: 2) Breath 1 – 1, 5 sek. Compression 100 – 120/min 71
 Pediatric Basic/Advanced Live Support When do you need to call first for assistance, before rescue breaths and 1 min of cpr? witnessed, sudden collapse of the child when the rescuer is alone. cardiac arrest is likely to be caused by an arrhythmia and the child will need defibrillation 72
Pediatric Basic/Advanced Live Support When do you need to call first for assistance, before rescue breaths and 1 min of cpr? witnessed, sudden collapse of the child when the rescuer is alone. cardiac arrest is likely to be caused by an arrhythmia and the child will need defibrillation 72
 Pediatric Basic/Advanced Live Support Epinephrine dose: iv, io 10 mcg/kgmc tracheal tube: 100 mcg/kg Admiodaroe dose 5 mg/kg Defibrillation 4 J/kg 73
Pediatric Basic/Advanced Live Support Epinephrine dose: iv, io 10 mcg/kgmc tracheal tube: 100 mcg/kg Admiodaroe dose 5 mg/kg Defibrillation 4 J/kg 73
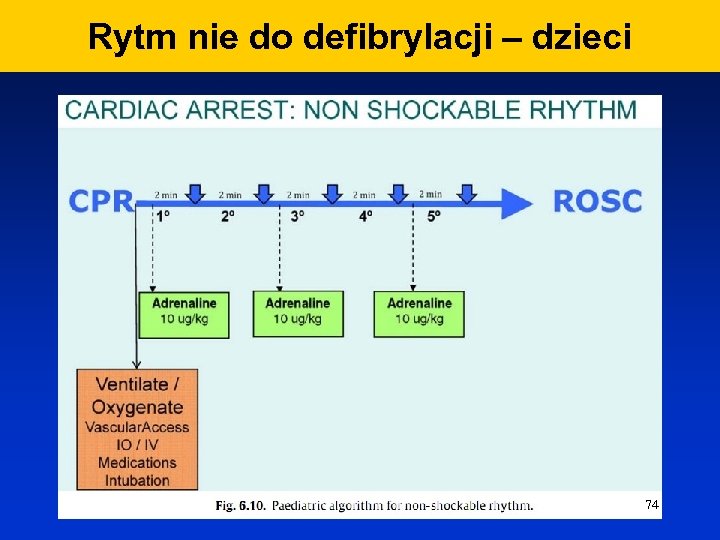 Rytm nie do defibrylacji – dzieci 74
Rytm nie do defibrylacji – dzieci 74
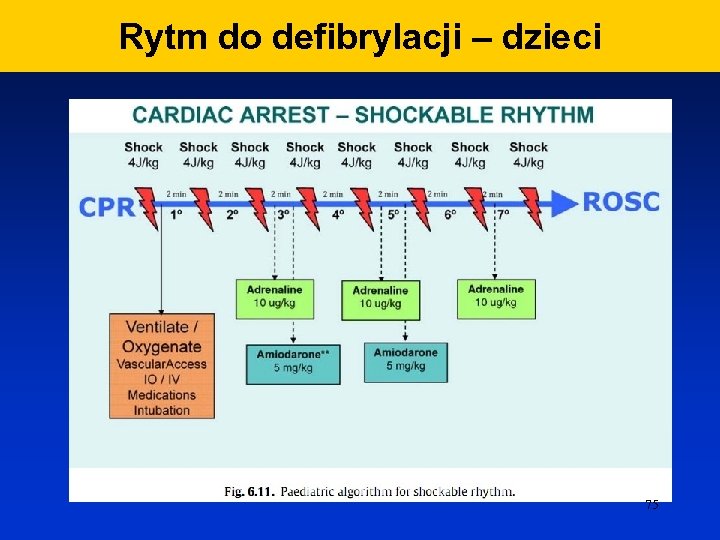 Rytm do defibrylacji – dzieci 75
Rytm do defibrylacji – dzieci 75
 KONIEC 76
KONIEC 76


