54205d21bcc461b19ba11a0c1d4f780a.ppt
- Количество слайдов: 43

Cancer Survivor Health and Productivity Beyond the Disease: The Impact of Cancer Survivorship on employers, benefit managers, health & disability insurers

Section Header Goes Here Subhead Goes Here

3

Victim……Patient……Survivor: Lost in Transition? • The learning objectives of the proposed CE Program: – Present the key clinical, financial, vocational and emotional milestones from Cancer diagnosis through a resumption of work – Illustrate the internal and external factors that influence lost time during cancer treatment and a successful resumption of work following cancer treatment – Describe the effective application of a disease/disability management products and services that promote the health, productivity and employability of the cancer survivor. • The expected outcomes of the proposed CE Program: – Improve the understanding by health & disability insurance and benefit specialists, as well as employers of the cancer survivor’s employment options, family dynamics, work motivation and work disruptions due to cancer treatment. – Profile the high risk factors leading to excessive lost time, reduced employment opportunities and the cost of cancer care for survivors – Illustrate a program model that enhances productivity and employment strategies in connection with a supportive benefit design, claims, disability/disease management process and a measurable ROI. 4

CE program: Rationale • Epidemiology: Cancer is one of the leading causes of death and disability in the American work force. The incidence of cancer in the 40 to 65 year age cohort is on the increase. Correspondingly, this age cohort constitutes the largest growth group in the American work force, as well as the largest percentage of LTD claims in the Unum book of business. • Survivorship: Recent studies demonstrate that a measurable increase in the 5 year survivorship of individuals with Breast, Prostate, and Colorectal cancers are at levels more characteristic of a serious chronic disease than of a terminal illness. • Transition: The American Cancer Society recognizes the transition from cancer patient to cancer survivor is the next critical area of attention. Promoting the individual’s emotional and family adjustment, long term independence, as well as protecting the productivity and employability of the cancer survivor have become a priority. • Work Outcomes: While a large percentage (estimated 60% to 85%) of cancer survivors ultimately return to work, the overall quality of health, productivity and employability, as well as costs have not been well documented. Correspondingly, little is known as to what differentiates between a successful and unsuccessful employability post cancer treatment. 5

Program Outline: CE Course Outline • Section 1 Context of Survivorship (2 hour program) (15 minutes) – Patterns of Incidence, Rates of Survivorship, • Section 2 Framework of Survivorship (30 minutes) – Dealing with the acute stages of diagnosis & treatment – Friends, families, co-workers and care givers – Coping, emotional resilience & post traumatic stress disorder (PTSD) – Fatigue - Neurocognitive changes (Chemobrain) - Pain – Realignments & Adjustments • Section 3 Employer Productivity & Benefits Prescription (30 Minutes – Work place – Benefits – Economics coverage and gaps • Section 4 Quality of Work Life Study (30 minutes) – Study Methodology – Outcomes – Implications for insurers, benefit managers & Employers • Section 5 Cancer Survivor Resources & Studies (Handouts) 6

Section 1 Context of Survivorship Patterns of Incidence Rates of Survivorship 7

Cancer Survivorship: Beyond the Disease • Increased Incidence with Increased Survivorship – Screening, Early Diagnosis, Improved Treatment, Reduced Toxicity of Treatment • Definitions of Survivorship – Expected vs. Observed: Differences of opinion – Six months post diagnosis – 2 year – 5 year post diagnosis survivor rates – Alive one day post treatment – Winners or Losers…never a tie • Survivorship Issues: – The Journey – Impact on Well Being: The cost of survivorship – Independence: Not being a hostage to the disease – Impact on Productivity – Impact on Employers “I don’t want to live forever… I just want to live as long as I am alive” Anonymous Cancer Survivor, Summer, 2006 8
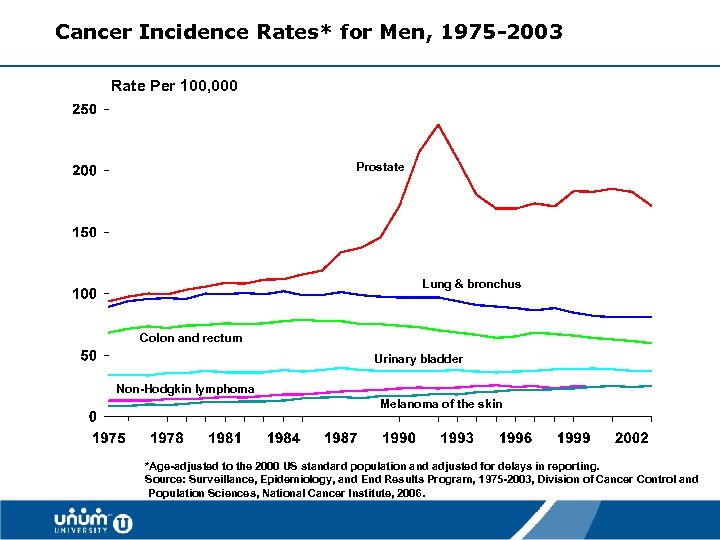
Cancer Incidence Rates* for Men, 1975 -2003 Rate Per 100, 000 Prostate Lung & bronchus Colon and rectum Urinary bladder Non-Hodgkin lymphoma Melanoma of the skin *Age-adjusted to the 2000 US standard population and adjusted for delays in reporting. Source: Surveillance, Epidemiology, and End Results Program, 1975 -2003, Division of Cancer Control and Population Sciences, National Cancer Institute, 2006. 9
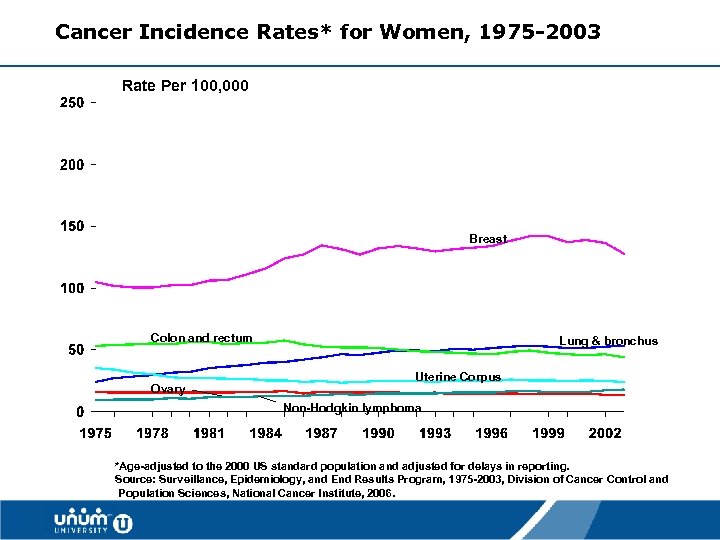
Cancer Incidence Rates* for Women, 1975 -2003 Rate Per 100, 000 Breast Colon and rectum Ovary Lung & bronchus Uterine Corpus Non-Hodgkin lymphoma *Age-adjusted to the 2000 US standard population and adjusted for delays in reporting. Source: Surveillance, Epidemiology, and End Results Program, 1975 -2003, Division of Cancer Control and Population Sciences, National Cancer Institute, 2006. 10
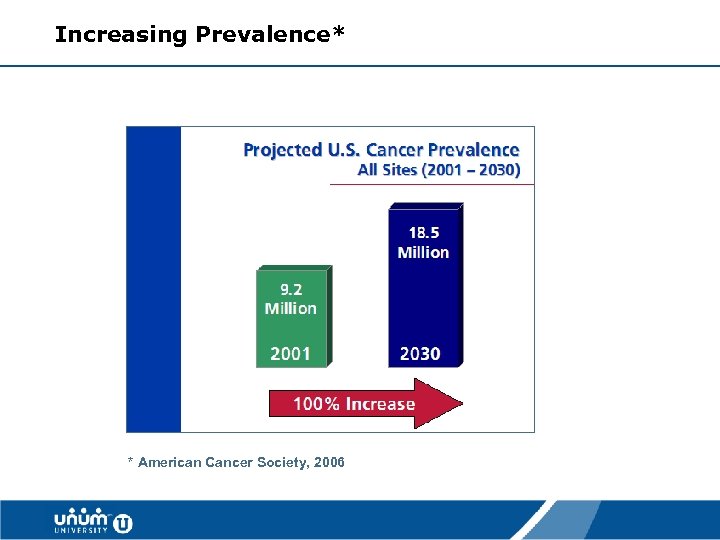
Increasing Prevalence* * American Cancer Society, 2006 11
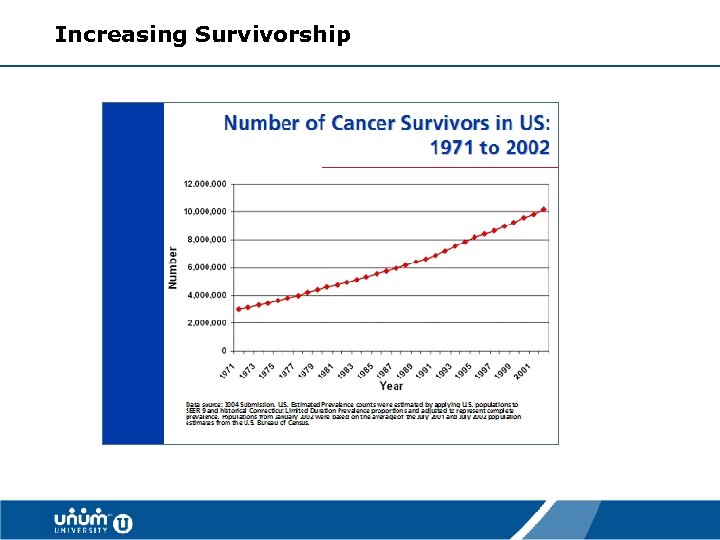
Increasing Survivorship 12
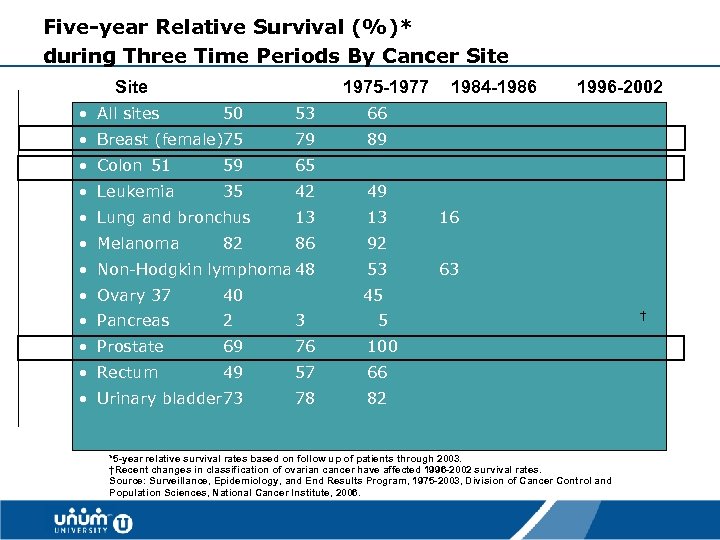
Five-year Relative Survival (%)* during Three Time Periods By Cancer Site • All sites 1975 -1977 50 53 79 89 • Colon 51 59 65 • Leukemia 35 42 49 13 13 86 92 • Non-Hodgkin lymphoma 48 53 1996 -2002 66 • Breast (female)75 1984 -1986 • Lung and bronchus • Melanoma 82 • Ovary 37 40 2 3 5 • Prostate 69 76 100 • Rectum 49 57 66 • Urinary bladder 73 78 63 45 • Pancreas 16 82 † *5 -year relative survival rates based on follow up of patients through 2003. †Recent changes in classification of ovarian cancer have affected 1996 -2002 survival rates. Source: Surveillance, Epidemiology, and End Results Program, 1975 -2003, Division of Cancer Control and Population Sciences, National Cancer Institute, 2006. 13

Section 2 Framework of Survivorship Dealing with the acute stages of diagnosis & treatment Friends, families, co-workers and care givers Coping, emotional resilience & PTSD Fatigue - Neurocognitive changes (Chemobrain) - Pain Realignments & Adjustments 14

A Conceptual Framework: A Quality of Work Life * Physical Functional Ability Strength/Fatigue Sleep & Rest Nausea Appetite Constipation Pain Vocational/Social Independence Financial Burden Caregiver Burden Roles and Relationships Roles & Relationships Intimacy Sexual Function Appearance Quality of Work Life Psychological Anxiety Depression Enjoyment/Leisure Pain Distress Happiness/Fear Cognition/Attention Spiritual Hope Suffering Meaning of Pain Religiosity Transcendence Adopted from presentation by Mary Scherbring, CNS, MS, OCN® Clinical Nurse Specialist, Mayo Clinic, 2006 & Ferrell, et al. 1991 Clinic 15

Treatment: Its Killing Me!!! – Emotionally • Depression • Anxiety • Acute Stress Response/ Post Traumatic Stress • Drug Reactions or Side Effects • Grief & Loss – Physically • Side Effects of Treatment – Economically • Concerns about insurance coverage • “Lifetime Limits” • Transportation • Medication Reimbursement • “Experimental Treatments” 16
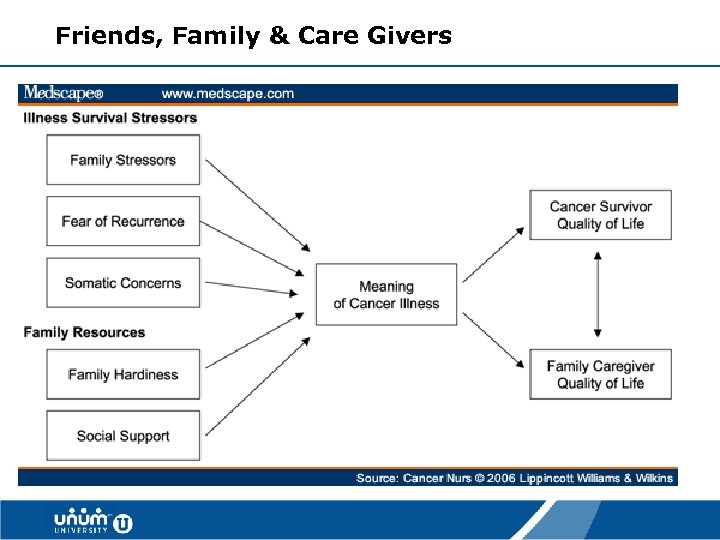
Friends, Family & Care Givers 17

Physical & Emotional Resilience • Coping Mechanisms: What works? What is predictable? • Types of Coping found in Cancer Patients/Survivors – Seek and Use Social Support – Cognitive Escape-Avoidance – Distancing – Focus on the Positive – Behavioral Escape and Avoidance • Mediated by Personal, Situational, and Cancer Characteristics • Dependent on an Appraisal Process – Impact of Events Scale – Acute and Post Traumatic Stress 18

Silent Saboteurs: Fatigue • Physical Fatigue – Fatigue is the most common unmanaged symptom in patients with cancer. – A review of the literature indicates that fatigue affects between 70 -100% of individuals diagnosed and being treated for various cancers. – The NIH State-of-the-Science Conference Statement identified fatigue as one of three “emphasized” symptoms. – The National Comprehensive Cancer Network Fatigue Practice Guidelines Panel defines fatigue as § “an unusual, persistent, subjective sense of tiredness related to cancer or cancer treatment that interferes with usual functioning”. § “pervasive, unusual, excessive tiredness which involves the whole body, is disproportionate to or unrelated to activity level or exertion and is usually not relieved by rest or sleep”. 19

Silent Saboteurs : “Chemo Brain” aka Neurocognitive Changes • It has been suggested, both anecdotally and in the literature, that a perceived or actual decline in cognitive functioning can have a negative impact on not only quality of life, but on adjustment following Cancer Treatments • What do we know? • Slowed reaction time • Reduced attention and concentration • Difficulties in reasoning and problem-solving • Memory impairment • Higher cognitive functioning impairment • Subtle reduction of memory performance • No deterioration of cognitive function after a median follow-up of 27 months posthyperfractionated TBI • Mild to moderate cognitive impairment in 60%. Selective attention and executive function Information processing speed • Verbal learning Verbal and visual memory 20

Silent Saboteur: Pain • Pain is poorly studied in cancer survivors • The existing data look only at certain post-treatment pain syndromes such as post surgical (post-thoracotomy or postmastectomy pain) • Our pilot work suggested pain is a problem for up to 40% of survivors • Mainly mild to moderate in intensity – unclear how well it is treated • We are studying its impact on 600 survivors – Examining pain prevalence – Characteristics and impact on quality of life – Treatment issues • Pain can be a constant reminder of the disease and “patient-ness” 21

Silent Saboteurs: Doing it All Over Again • Post Traumatic Stress Disorder - PTSD – Incidence – Identification – Triggers – Coping Styles & Strategies – Employer Resources – Survivor as a hostage to the disease – Emotional Resilience 22

Survival: Realignments & Adjustments Changing priorities as a cancer survivor • Personal – Meaning Making – What is important? – Personal/ Cancer Milestones • Work – Wanting to vs. Having to – Fears about return to work – Adjusting to changes (fatigue, “Chemobrain”) that may effect ability to transition back to work. • Family – Transition from Caretaker/Care Giver to “Normal Roles” in the family – Return to Work 23

Section 3 Employer Productivity & Benefits Prescription Work place consideration Health & Disability Benefits Economics coverage and gaps Critical Illness and LTC Implications 24

Employer Guidelines: A Productivity Rx • Managing the productivity impact @ Diagnosis: – Timing & context – Avoid premature work decisions – Appropriate communication with co-workers – During treatment: Protect future productivity – Give “permission” to engage in treatment • Employee Presenteeism & Care Givers • Understand expect to have intermittent lost time • Transitions out and back: Work site accommodations and adjustments • Expect financial gaps created by non treatment costs • Explore employer, disability & healthcare insurer partnerships • Accessibility to new therapies • Performance Management: The good employee who becomes a “bad” employee 25

Benefits & Productivity • Employment provides security on many fronts for the cancer survivor: – Intrinsic • Feeling needed and valued as contributing member of a team or organization • Sense or normalcy and order after a period of relative chaos – Financial • Salary to meet obligations – Ongoing – Resulting from treatment – Rebuilding • Security in having benefits (insurance, PTO, EAP, etc) to help offset possible future costs of illness • Cancer survivors may value all of these more than coworkers who have not been diagnosed with cancer 26

Covering Financial Gaps • Opportunities for employers – PTO or vacation donation – Flexible schedules – Setting expectations – Communication to other employees – Workplace accommodations • Offer employees: – Access to a comprehensive health plan (employer and/or employee paid) – Access to disability plans through work – Option to buy additional coverage (cancer, critical illness) through the worksite. • Education regarding the value of benefits and different options available to them – Include case studies if possible • Establish and clearly document programs that can be applied broadly to the employee base 27

Other Considerations • Caregivers face stresses as well – many are similar to those faced by the cancer patient him / herself – Can programs be developed to support these individuals? • Flexible schedules • PTO donation (? ) • Access to EAP programs 28

Section 4 Quality of Work Life Study • Study Methodology • Outcomes • Implications for insurers, benefit managers & employers 29

Methodology • Phase I Health & Productivity Profiles: Define cancer patterns, trends & relationships within Unum. Provident’s enterprise wide book of business (Oct. 2006 – June. 2007) Primary activities: Determine the demographic, employment and productivity trends, patterns for the FML/STD/LTD cancer survivors. • Phase II Health & Productivity Connections Determine the relative impact of various independent variables on post treatment work status, cancer related absenteeism, presenteeism and employability (June 2007 – January. 2008). Primary activities: Determine the degree of impact certain internal and external independent variables have on the cancer survivors' employment, productivity, benefit utilization and medical costs (dependent variables). • Phase III Health & Productivity Model Demonstrate the impact of a model health & productivity program for cancer survivors (January 2008 – January , 2009) Primary activities: Design, develop and evaluate the impact of a clinical and corporate based model health & productivity program for cancer survivors. • Research Partners – Unum UK – James Cancer Center, The Ohio State University – Memorial Sloan Kettering Cancer Center 30
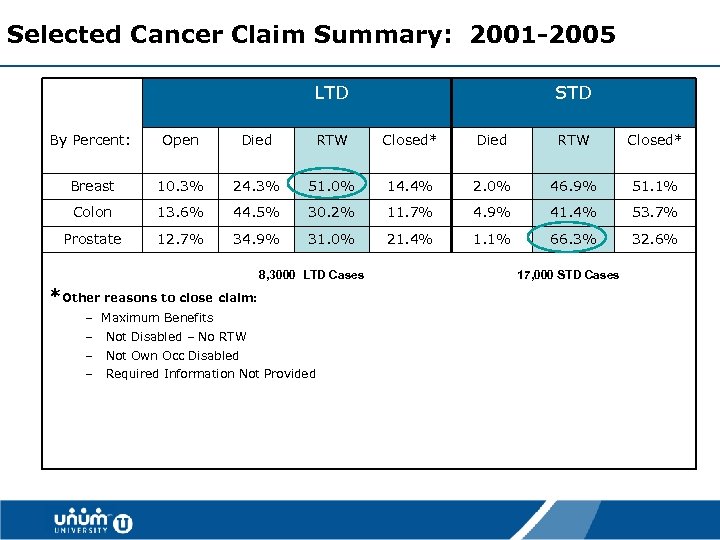
Selected Cancer Claim Summary: 2001 -2005 LTD STD By Percent: Open Died RTW Closed* Breast 10. 3% 24. 3% 51. 0% 14. 4% 2. 0% 46. 9% 51. 1% Colon 13. 6% 44. 5% 30. 2% 11. 7% 4. 9% 41. 4% 53. 7% Prostate 12. 7% 34. 9% 31. 0% 21. 4% 1. 1% 66. 3% 32. 6% 8, 3000 LTD Cases 17, 000 STD Cases *Other reasons to close claim: – Maximum Benefits – Not Disabled – No RTW – Not Own Occ Disabled – Required Information Not Provided 31
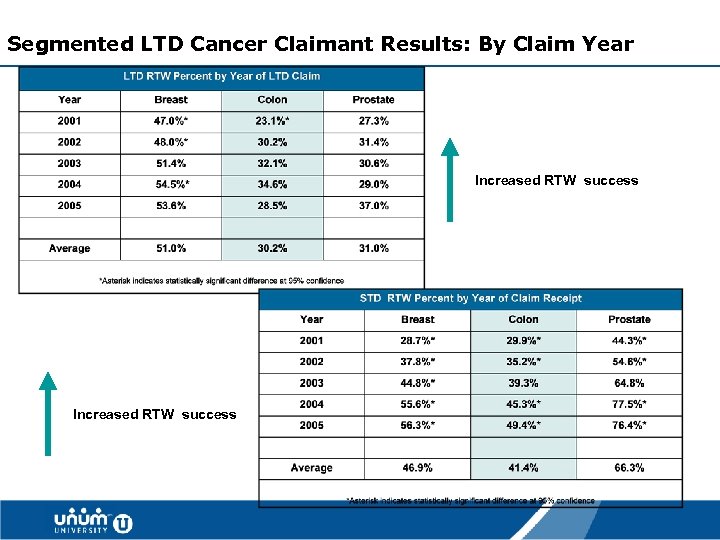
Segmented LTD Cancer Claimant Results: By Claim Year Increased RTW success 32
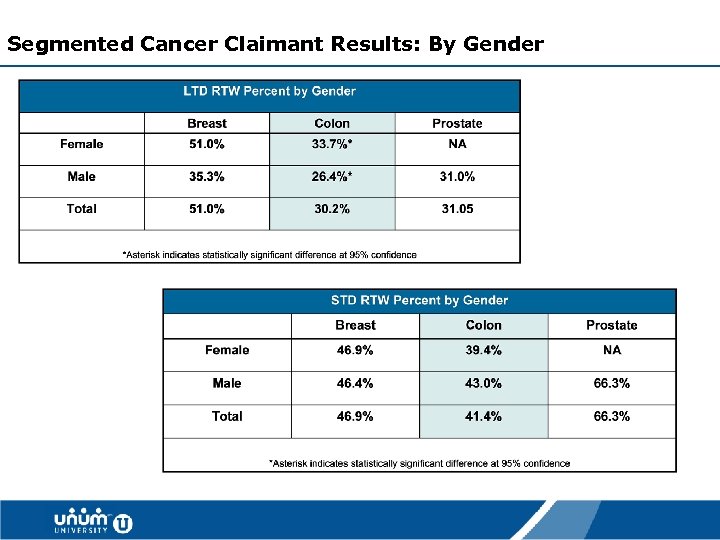
Segmented Cancer Claimant Results: By Gender 33
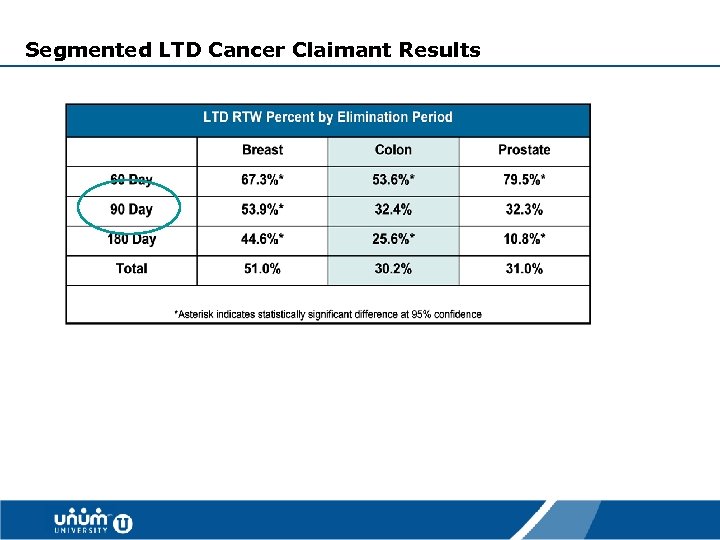
Segmented LTD Cancer Claimant Results 34
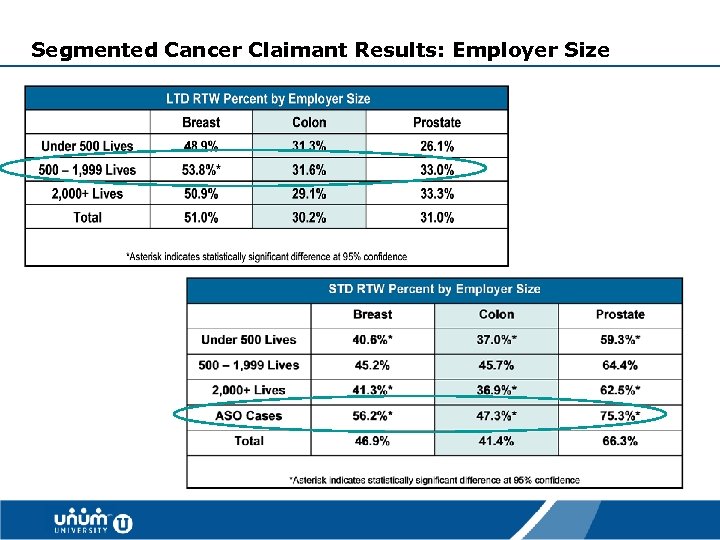
Segmented Cancer Claimant Results: Employer Size 35
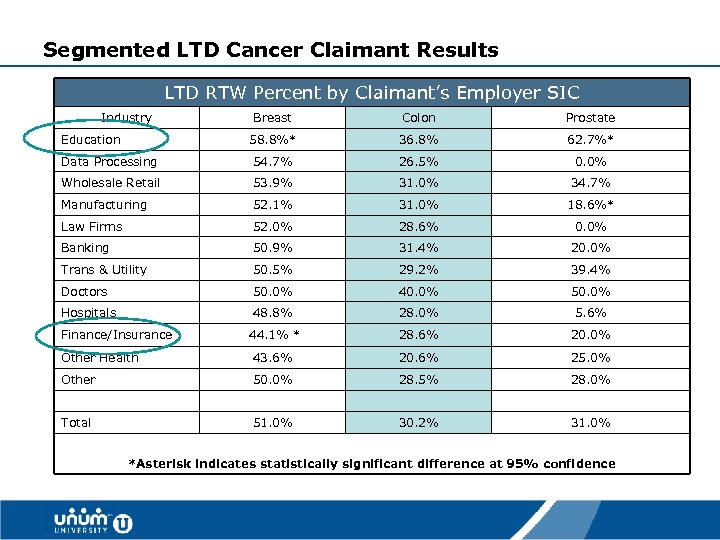
Segmented LTD Cancer Claimant Results LTD RTW Percent by Claimant’s Employer SIC Industry Breast Colon Prostate 58. 8%* 36. 8% 62. 7%* Data Processing 54. 7% 26. 5% 0. 0% Wholesale Retail 53. 9% 31. 0% 34. 7% Manufacturing 52. 1% 31. 0% 18. 6%* Law Firms 52. 0% 28. 6% 0. 0% Banking 50. 9% 31. 4% 20. 0% Trans & Utility 50. 5% 29. 2% 39. 4% Doctors 50. 0% 40. 0% 50. 0% Hospitals 48. 8% 28. 0% 5. 6% 44. 1% * 28. 6% 20. 0% Other Health 43. 6% 20. 6% 25. 0% Other 50. 0% 28. 5% 28. 0% Total 51. 0% 30. 2% 31. 0% Education Finance/Insurance *Asterisk indicates statistically significant difference at 95% confidence 36
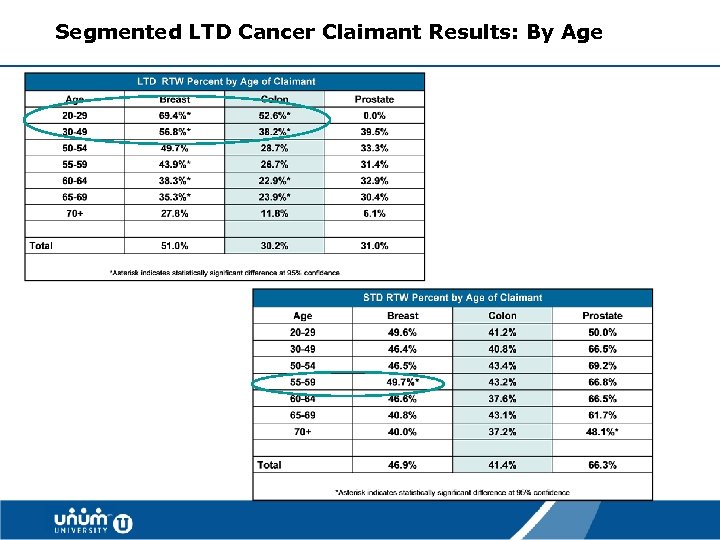
Segmented LTD Cancer Claimant Results: By Age 37
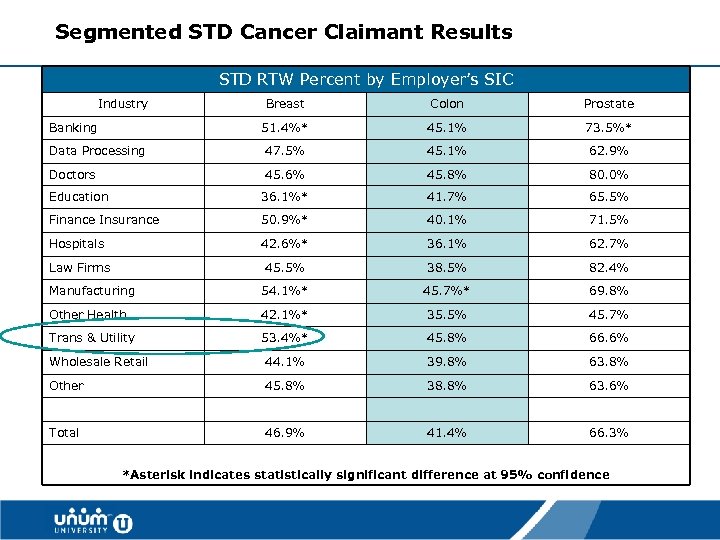
Segmented STD Cancer Claimant Results STD RTW Percent by Employer’s SIC Industry Breast Colon Prostate 51. 4%* 45. 1% 73. 5%* Data Processing 47. 5% 45. 1% 62. 9% Doctors 45. 6% 45. 8% 80. 0% Education 36. 1%* 41. 7% 65. 5% Finance Insurance 50. 9%* 40. 1% 71. 5% Hospitals 42. 6%* 36. 1% 62. 7% Law Firms 45. 5% 38. 5% 82. 4% Manufacturing 54. 1%* 45. 7%* 69. 8% Other Health 42. 1%* 35. 5% 45. 7% Trans & Utility 53. 4%* 45. 8% 66. 6% Wholesale Retail 44. 1% 39. 8% 63. 8% Other 45. 8% 38. 8% 63. 6% Total 46. 9% 41. 4% 66. 3% Banking *Asterisk indicates statistically significant difference at 95% confidence 38

Section 5 Cancer Survivor Resources & Studies 39

Selected Resources • Hewitt, M, Herdman, R. Holland, J Editors, Meeting Psychosocial Needs of Women with Breast Cancer Institute of Medicine and the National Research Council of the National Academies, 2004, Washington DC • From Cancer Patient to Cancer Survivor: Lost in Transition, National Academy of Science 2005 • Healthy People 2010 Cancer: Centers for Disease Control and Prevention, National Institutes of Health • Bednarek HL, Bradley CJ. Work and retirement after cancer diagnosis. Research in Nursing & Health. 2005 Apr; 28(2): pp 126 -35. • Drolet M, Maunsell E, Mondor M, Brisson C, Brisson J, Masse B, Deschenes L. Work absence after breast cancer diagnosis: a population-based study. Canadian Medical • Association Journal. 2005 Sep 27; 173(7): pp 765 -71. • Fairey AS, Courneya KS, Field CJ, Mackey JR. Physical exercise and immune system function in cancer survivors: a comprehensive review and future directions. Cancer. 2002 Jan 15; 94(2): pp 539 -51. • Main DS, Nowels CT, Cavender TA, Etschmaier M, Steiner JF. A qualitative study of work and work return in cancer survivors. Psychooncology. 2005 Nov; 14(11). pp 992 -1004. • Maunsell E, Brisson C, Dubois L, Lauzier S, Fraser A. Work problems after breast cancer: an exploratory qualitative study. Psychooncology. 1999 Nov-Dec; 8(6): pp 467 -73. • Short PF, Vasey JJ, Tunceli K. Employment pathways in a large cohort of adult cancer survivors. Cancer. 2005 Mar 15; 103(6): pp 1292 -301. • Spelten ER, Sprangers MA, Verbeek JH. Factors reported to influence the return to work of cancer survivors: a literature review. Psychooncology. 2002, Mar-Apr: 11(2): pp 124 -31. • Thewes B, Burtow P, Girgis A, Pendlebury S. The psychosocial needs of breast cancer survivors; a qualitative study of the shared and unique needs of younger versus older survivors. Psychooncology. 2004 Mar; 13(3): pp 177 -89. • Wold KS, Byers T, Crane LA, Ahnen D. What do cancer survivors believe causes cancer? Cancer causes & control : CCC. 2005 Mar: 16(2): pp 115 -23. 40

Selected Resources • Edwards, Brenda K. ; et al. Annual Report to the Nation on the Status of Cancer, 1975 -2002, Featuring Population-Based Trends in Cancer Treatment, Journal of the National Cancer Institute, Vol. 97, No. 19, Oct. 5, 2005 • Fairey, Adrian S. , B. A. ; Courneya, Kerry S. , Ph. D. ; Field, Catherine J. , Ph. D. , R. D. ; Mackey, John R. , M. D. Physical Exercise and Immune System Function In Cancer Survivors, Cancer, January 15, 2002, Vol. 94, No. 2 • Langeveld, N. E. ; Stam, H. ; Grootenhuis, M. A. ; Last, B. F. Quality of Life in Young Adult Survivors of Childhood Cancer, Support Care Center (2002) 10: 579 -600 • Schroevers, Maya J. ; Ranchor, Adelita V. ; and Sanderman, Robert. The Role of Age at the Onset of Cancer in Relation to Survivors’ Long-Term Adjustment: A Controlled Comparison Over an Eight-Year Period, Psycho-Oncology 13: 740 -752 (2004) • Schou, Inger; et al. Multiple Predictors of Health-Related Quality of Life in Early Stage Breast Cancer. Data From Year Follow-Up Study Compared with the General Population, Quality of Life Research (2005) 14: 1813 -1823 • Coreil, Jeannine; Wilke, Jaime; Pintado, Irene. Cultural Models of Illness and Recovery in Breast Cancer Support Groups, Qualitative Health Research, Vol. 14, No. 7, September 2004, 905 -923 • Gotay, Carolyn Cook; Isaacs, Patti; Pagano, Ian. Quality of Life in Patients Who Survive a Dire Prognosis Compared to Control Cancer Survivors, Psycho-Oncology, 13: 882 -892 (2004) • Knight, Sara J. , Ph. D. ; et al. Ethnic Variation in Localized Prostate Cancer: A Pilot Study of Preferences, Optimism, and Quality of Life Among Black and White Veterans, Clinical Prostate Cancer, Vol. 3, No. 1, 31 -37, 2004 • Schou, Inger; Ekeberg, Ǿ. ; and Ruland, C. M. The Mediating Role of Appraisal and Coping in the Relationship Between Optimism-Pessimism and Quality of Life, Psycho-Oncology 14: 718 -727 (2005) • Carver, Charles S. ; Smith, Roselyn G. ; Petronis, Vida M. ; and Antoni, Michael H. Quality of Life Among Long-Term Survivors of Breast Cancer: Different Types of Antecedents Predict Different Classes of Outcomes, Psycho-Oncology 15: 749 -758 (2006) 41

Ready to learn more? • Web sites – http: //ons. org/clinical/Treatment/Surgery. shtml – http: //nci. nih. gov/ – http: //www. cancer. org/docroot/home/index. asp • Many specific cancer advocacy groups have their own web site – http: //www. curekidneycancer. org/ (kidney) – http: //www. ustoo. org (prostate) – http: //www. alcase. org/ (lung) – http: //www. pancan. org (pancreatic) • What about the caregivers? – http: //www. nfcacares. org • Cancer Survivorship – Cancer survivors bill of rights http: //www. cancer. gov/cancertopics/life-after-treatment/page 12 42

Presenter’s Biographies: • Heidi Bimrose, MA, CRC, CEBS, Director, Health & Productivity Development: Heidi received her Bachelor's Degree in Communicative Disorders and Master's Degree in Rehabilitation Counseling from Northern Illinois University. She is a Certified Rehabilitation Counselor (CRC), a certified Employee Benefit Specialist (CEBS), and an Associate, Life and Health Claims (ALHC). She is a member of the International Association of Rehabilitation Professionals. • J. Philip Bruen, CEBS, Vice President and Practice Leader, Large Employer Market: Phil is a Certified Employee Benefit Specialist (CEBS) with 25 years of insurance sales experience. • Carol Davis, CEBS, Senior Director, Health & Productivity Development: Carol received her Bachelor’s Degree from the University of North Carolina at Chapel Hill. She is a Certified Employee Benefit Specialist (CEBS), Fellow Life Management Institute (FMLI) and a registered cytotechnologist with the American Society of Clinical Pathology, CT(ASCP). She is a member of the Society of Human Resource Management. • Robert Jacob, FMLI, Director, Health & Productivity Development: Jake received his Bachelor’s Degree in Business Economics from Ithaca College and an M. B. A. from New Hampshire University. • Kenneth Mitchell, Ph. D. , Vice President, Health & Productivity Development Kenneth Mitchell received his Ph. D. from the Pennsylvania State University and served as an assistant and tenured associate professor in the School of Medicine, University of North Carolina - Chapel Hill. He also serves as the principle investigator on Unum's study of the Health, Productivity and Employability of Cancer Survivors. • Blake Strack, Ph. D. , Director, Health & Productivity Development: Dr. Strack received his B. A. in Human Resources Management from Syracuse University and his Ph. D. in Public Policy Analysis from the State University of New York at Buffalo. • Kristin Tugman, MS, CRC, LPC, Director, Health & Productivity Development Kristin has been working in the field of vocational rehabilitation since 1997 when she graduated from Georgia State University with a Master of Rehabilitation Counseling degree. Kristin is a Certified Rehabilitation Counselor and a Licensed Professional Counselor. • Tim Ward, Regional Sales Manager, National Accounts Tim received his Bachelor’s Degree from the University of Denver and has 30 years of insurance sales experience. Lydia Griffith Jilek BA - Bates College - English – 1992 MBA - University of MN - 1997 MAHR/IR (Masters of Arts in Human Resources & Industrial Relations - University of MN - 1997 Unum - 2006 - Present - Director of Product Development Medica Health Plans - 1997 - 2006 - roles in Broker Compensation & Licensing, Sales Reporting, Market Research and Product Management and Development with a focus on Consumer Directed Health Plan development (HRA, HSA, FSA). • FX-3053 43
54205d21bcc461b19ba11a0c1d4f780a.ppt