9b7912fefd9813995f10f1772d075368.ppt
- Количество слайдов: 64

BRIEFING TO SELECT COMMITTEE ON APPROPRIATIONS Expenditure on National Health Insurance Grant and NHI Pilot sites 2014 /2015 9 JUNE 2015 1

Outline • Focus areas for the National Health Insurance Conditional Grant (NHI-CG) in 2014/15 • GP Contracting • Expenditure on Schedule 5 and Schedule 6 CG 2014/15 FY • Expenditure and activities (Donor funding and Global Fund) • 2014 / 2015 NHI Rapid Appraisal 2
NHI Pilot Districts

GP Contracting • The following two slides show the number of GPs by NHI Pilot District as well as NHI pilot district doctor coverage. • Three options were being tested: – Direct contracting through NDOH – Service Provider – Western Cape option
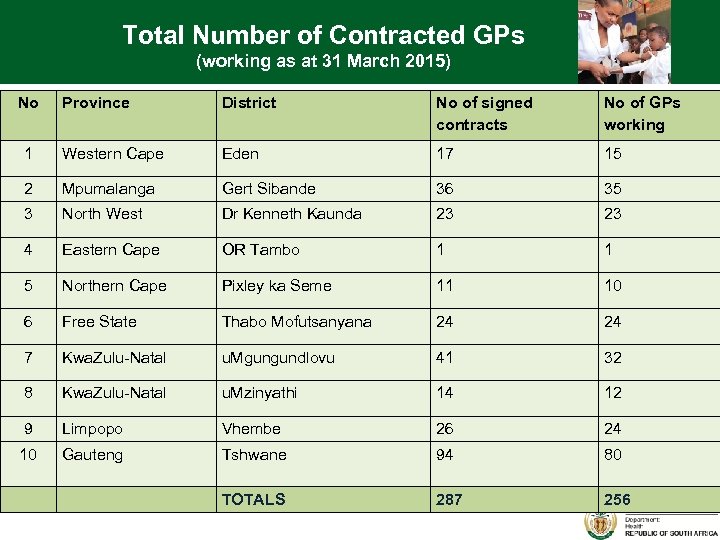
Total Number of Contracted GPs (working as at 31 March 2015) No Province District No of signed contracts No of GPs working 1 Western Cape Eden 17 15 2 Mpumalanga Gert Sibande 36 35 3 North West Dr Kenneth Kaunda 23 23 4 Eastern Cape OR Tambo 1 1 5 Northern Cape Pixley ka Seme 11 10 6 Free State Thabo Mofutsanyana 24 24 7 Kwa. Zulu-Natal u. Mgungundlovu 41 32 8 Kwa. Zulu-Natal u. Mzinyathi 14 12 9 Limpopo Vhembe 26 24 10 Gauteng Tshwane 94 80 TOTALS 287 256
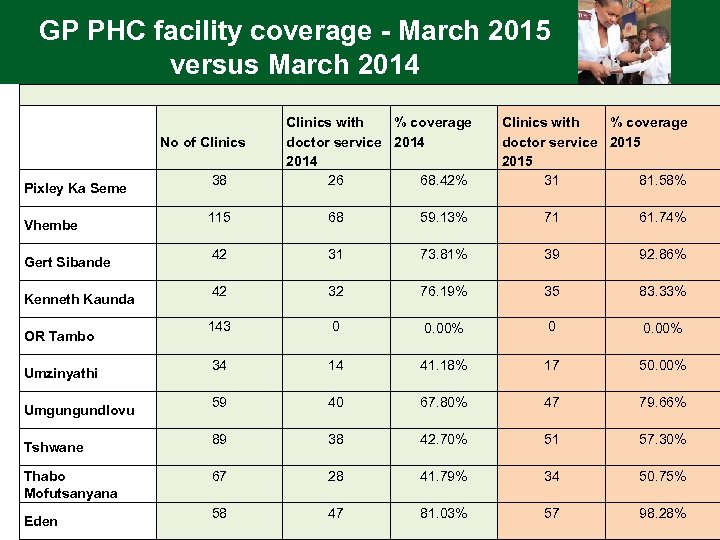
GP PHC facility coverage - March 2015 versus March 2014 No of Clinics Pixley Ka Seme Vhembe Gert Sibande Kenneth Kaunda OR Tambo Umzinyathi Umgungundlovu Tshwane Thabo Mofutsanyana Eden 38 115 42 143 34 59 89 67 58 Clinics with % coverage doctor service 2014 26 68. 42% 68 59. 13% 31 73. 81% 32 76. 19% 0 0. 00% 14 41. 18% 40 67. 80% 38 42. 70% 28 41. 79% 47 81. 03% % coverage Clinics with doctor service 2015 31 81. 58% 71 61. 74% 39 92. 86% 35 83. 33% 0 0. 00% 17 50. 00% 47 79. 66% 51 57. 30% 34 50. 75% 57 98. 28%
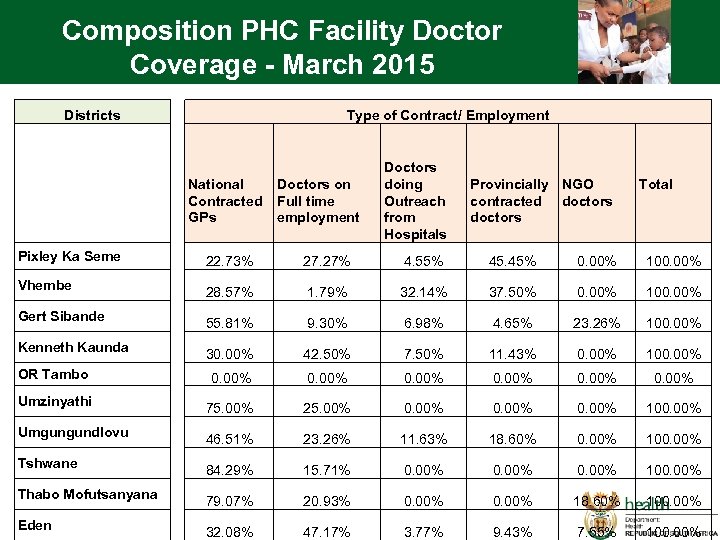
Composition PHC Facility Doctor Coverage - March 2015 Districts Type of Contract/ Employment National Doctors on Contracted Full time GPs employment Pixley Ka Seme Vhembe Gert Sibande Kenneth Kaunda OR Tambo Umzinyathi Umgungundlovu Tshwane Thabo Mofutsanyana Eden Doctors doing Outreach from Hospitals Provincially NGO contracted doctors Total 22. 73% 27. 27% 4. 55% 45. 45% 0. 00% 100. 00% 28. 57% 1. 79% 32. 14% 37. 50% 0. 00% 100. 00% 55. 81% 9. 30% 6. 98% 4. 65% 23. 26% 100. 00% 30. 00% 42. 50% 7. 50% 11. 43% 0. 00% 100. 00% 0. 00% 75. 00% 25. 00% 0. 00% 100. 00% 46. 51% 23. 26% 11. 63% 18. 60% 0. 00% 100. 00% 84. 29% 15. 71% 0. 00% 100. 00% 79. 07% 20. 93% 0. 00% 18. 60% 100. 00% 32. 08% 47. 17% 3. 77% 9. 43% 7. 55% 100. 00%

GP/Doctor Contracting • The introduction of an independent service provider to recruit and place GPs in facilities has increased the number of GPs contracted. • The contract only came into effect in November 2014, • Prior to the introduction of the independent service provider, just over 150 doctors were recruited during the 21 months of the project. • Since November 2014, a further 150 doctors have been recruited increasing the number of doctors to 256. • The service provider has a further 300 doctors in the recruitment pipeline however this is contingent on funding • During 2015/16 the intention is to supply a minimum of 180, 000 hours to clinics in 9 pilot districts.
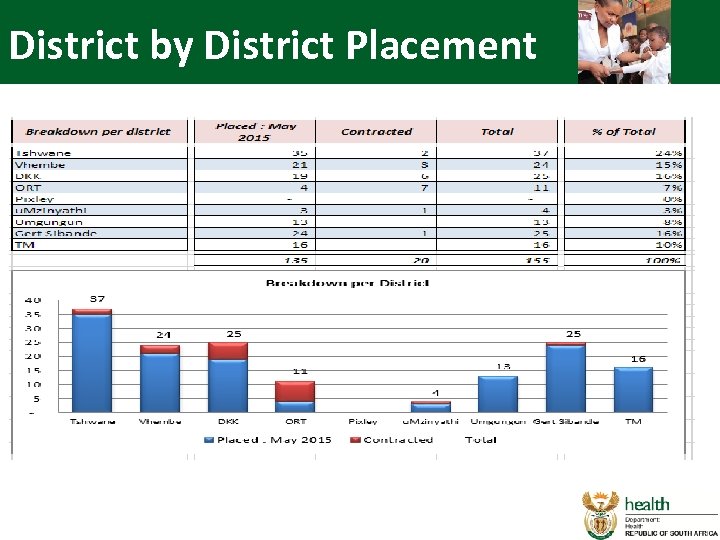
District by District Placement
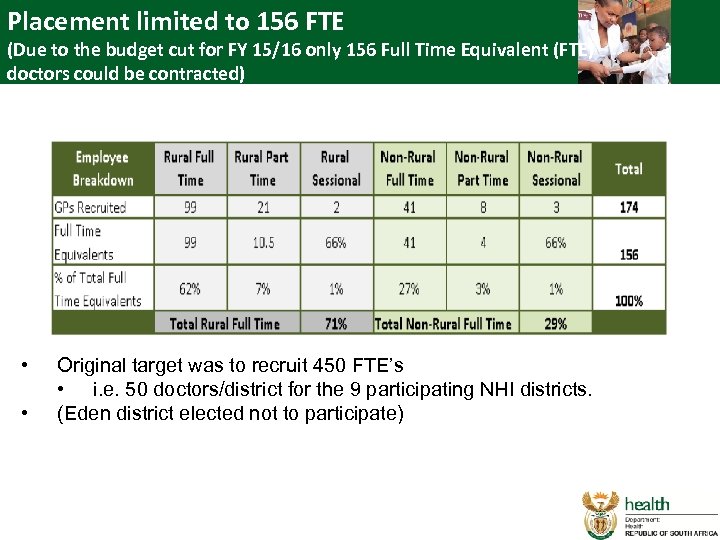
Placement limited to 156 FTE (Due to the budget cut for FY 15/16 only 156 Full Time Equivalent (FTE) doctors could be contracted) • • Original target was to recruit 450 FTE’s • i. e. 50 doctors/district for the 9 participating NHI districts. (Eden district elected not to participate)

Western Cape approach • The Western Cape DOH is excluded as they are implementing a different framework. • The WCDOH is using a principle of deploying existing medical officers employed by the WCDOH to clinics in the Eden district, and using the grant funding, they are employing doctors on sessional basis in hospitals to cover the gap left by the medical officers deployed to clinics. • According to the WCDOH, this has proved to be highly effective strategy as attracting private GPs to hospitals is easier than to clinics. • The team is assessing the impact of this model against the NDOH and the service provider model. 11

NHI-CG Schedule 6 Focus Area GP Contracting • GPs were slow in signing up for the GP contracting initiative because of concerns that the state of our health facilities will hamper their quality of work • Their concerns about the state of our PHC facilities are being addressed through the Ideal Clinic programme and while the working environment in many of our clinics is still being attended to, the GPs who have signed on have reported that they have been pleasantly surprised by the good working conditions in some of clinics. As result many have since increased the working hours they spend working in public health facilities • Contracting numbers improved with the appointment of an external service provider

NHI-CG Schedule 6 Focus Area • • GP Contracting This feedback is gathered through interactions with the GPs during orientation sessions and during support visits to the health facilities where they are providing services This positive trend has also been demonstrated by the constantly increasing number of GPs who have signed on At the end of March 2014 we had 119 GPs working to complement permanent staff in public health facilities. This number increased to 256 at the end of March 2015 The number of GPs on contract now will expend 100% of the budget for 2015/16
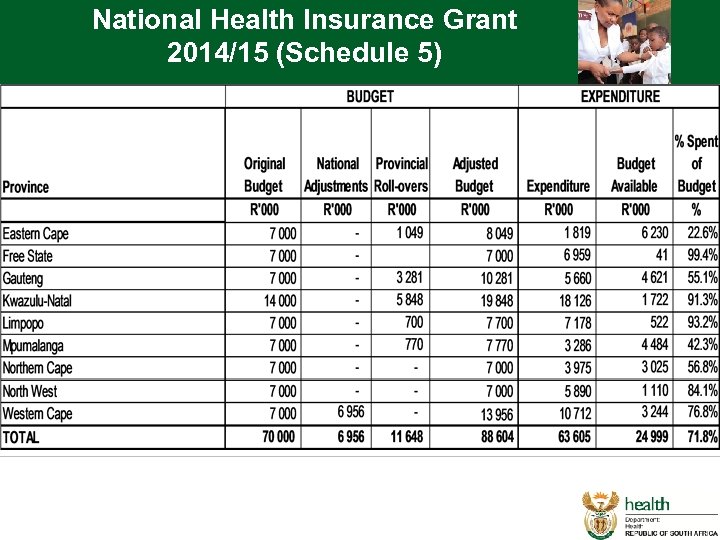
National Health Insurance Grant 2014/15 (Schedule 5)
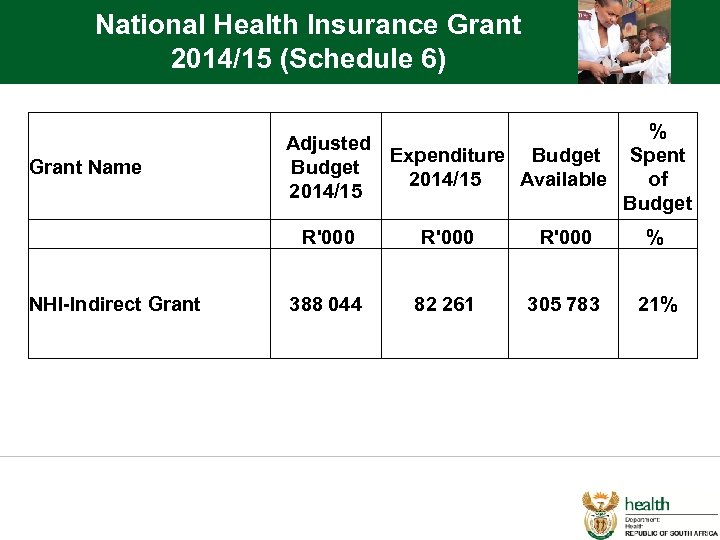
National Health Insurance Grant 2014/15 (Schedule 6) % Adjusted Expenditure Budget Spent Budget 2014/15 Available of 2014/15 Budget Grant Name NHI-Indirect Grant R'000 % 388 044 82 261 305 783 21%

Project Deliverables in NHI Pilot Districts using donor funds during 2014 -15

NHI Green Paper Phase 1: Focus Areas • • NHI White Paper and Legislative Process Management reforms and designation of Hospitals Establishment Office of Health Standard Compliance Public Health facility audit, Quality Improvement and Certification Building capacity to manage NHI Through the strengthening of District Management Costing Model Establishment of NHI Fund Accreditation and contracting of private providers by NHI Fund

NHI Green Paper Phase 1: Focus Areas Hospital Reimbursement reform Appointment of District Clinical Specialists Support Municipal Ward-based Primary Health Care Outreach Teams School -Based PHC services Public Hospital Infrastructure and Equipment Human resources for health Information management and systems support NHI Conditional Grant to support piloting of initial work in 10 Districts • Population Registration • ICT • Accreditation and contracting of private providers by NHI Fund • • 18

Hospital Reimbursement reform

Hospital Reimbursement reform • Fist phase for developing and testing of a Diagnosis Related Grouper (DRG) as an alternative reimbursement tool for hospitals was completed • This involved developing a base DRG tool for the 10 central hospitals across the country. • As at March 2015, the Department had managed to extract clinical and financial data from central hospitals. • The data has been categorised into 25 Major Diseases as part of the preliminary technical work to develop and apply a disease algorithm. • Technical work on case mix and actuarial analyses has been undertaken on the data that has been aggregated and a triangulation process has been undertaken with regards to data from other third party sources.

Hospital Reimbursement reform • A group of 10 professional nurses with extensive clinical (diagnostic and procedural) coding experience were employed to collect the data. • The coding team was deployed to 8 of the 10 central hospitals in South Africa. – The team was supported onsite by a team supervisor, project management assistant and project management team. • The clinical data collection tool was developed, tested and approved for use. • From 17 June 2014 until 6 March 2015, a total of more than 24 000 files were coded (final total in verification process). This exceeded the target of 22 500 files expected. • All data is maintained in the secured database

Appointment of District Clinical Specialists Support
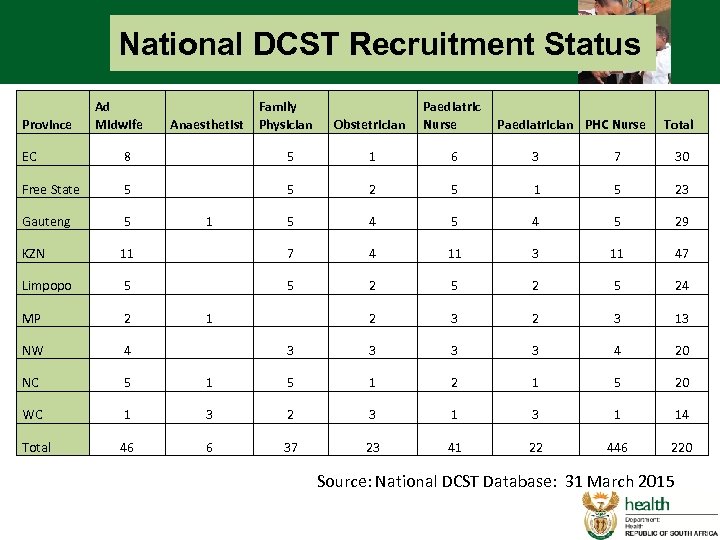
National DCST Recruitment Status Province Ad Midwife Anaesthetist Family Physician Obstetrician Paediatric Nurse Paediatrician PHC Nurse Total EC 8 5 1 6 3 7 30 Free State 5 5 2 5 1 5 23 Gauteng 5 1 5 4 5 29 KZN 11 7 4 11 3 11 47 Limpopo 5 5 2 5 24 MP 2 1 2 3 13 NW 4 3 3 4 20 NC 5 1 2 1 5 20 WC 1 3 2 3 1 14 Total 46 6 37 23 41 22 446 220 Source: National DCST Database: 31 March 2015

Municipal Ward-based Primary Health Care Outreach Teams
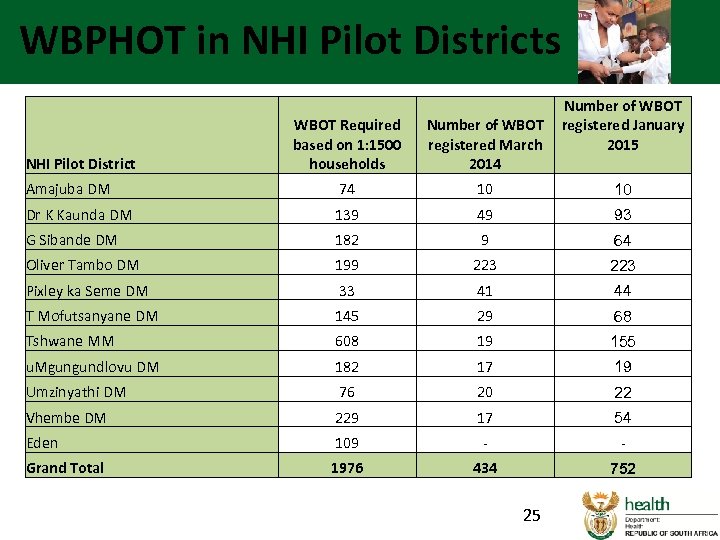
WBPHOT in NHI Pilot Districts Number of WBOT registered January 2015 WBOT Required based on 1: 1500 households Number of WBOT registered March 2014 Amajuba DM 74 10 10 Dr K Kaunda DM 139 49 93 G Sibande DM 182 9 64 Oliver Tambo DM 199 223 Pixley ka Seme DM 33 41 44 T Mofutsanyane DM 145 29 68 Tshwane MM 608 19 155 u. Mgungundlovu DM 182 17 19 Umzinyathi DM 76 20 22 Vhembe DM 229 17 54 Eden 109 - - Grand Total 1976 434 752 NHI Pilot District 25
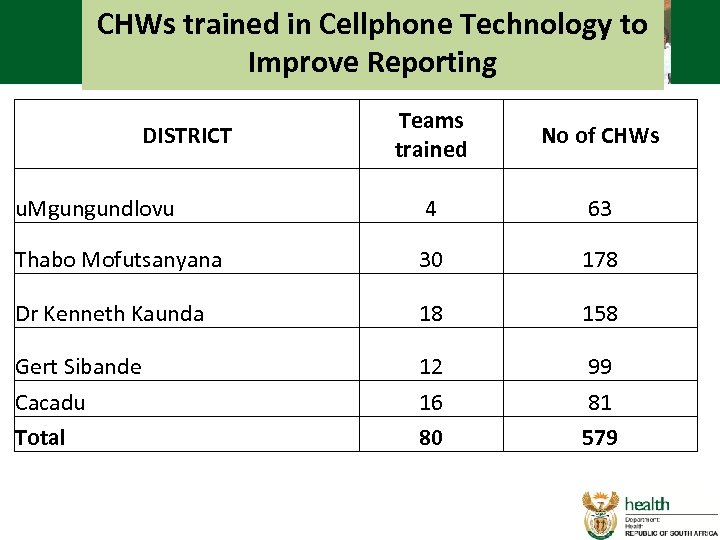
CHWs trained in Cellphone Technology to Improve Reporting Teams trained No of CHWs u. Mgungundlovu 4 63 Thabo Mofutsanyana 30 178 Dr Kenneth Kaunda 18 158 Gert Sibande Cacadu Total 12 16 80 99 81 579 DISTRICT

WBOT being trained on the m. Health: • Those teams reporting to DHIS have received basic orientation to use of cell phones • Scheduled training on the full m. Health manual 27

School -Based PHC services

School Health Services • To improve access to school health services additional School Health Mobile Vehicles were purchased and distributed in the NHI Pilot Districts – 27 Mobile PHC Trucks – 17 Oral Health Mobiles – 3 Eye Care Mobiles
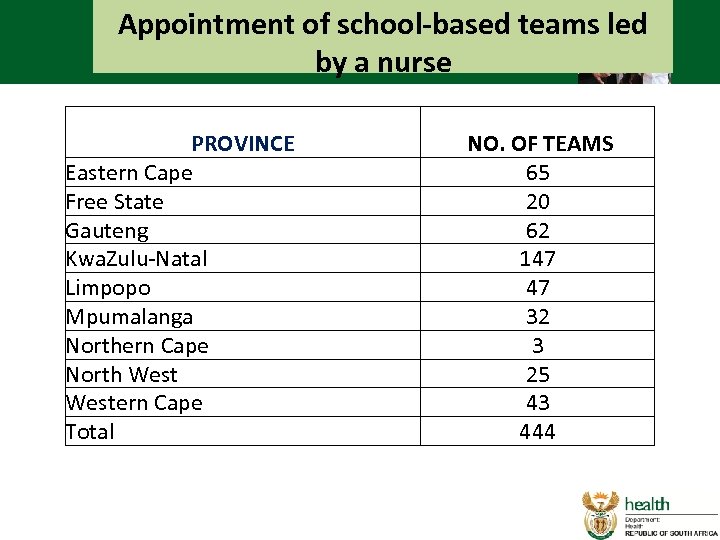
Appointment of school-based teams led by a nurse PROVINCE Eastern Cape Free State Gauteng Kwa. Zulu-Natal Limpopo Mpumalanga Northern Cape North Western Cape Total NO. OF TEAMS 65 20 62 147 47 32 3 25 43 444

PHC Facility Renovations
PHC Facility - Renovations
PHC Facility - Renovations

Photo’s of Dr Consulting Rooms Boiketlo Clinic (FS) 34

Photo’s of Dr Consulting Rooms Delekile Khoza clinic (NW) 35

Human resources for health

Information management and systems support Patient Administration Rationalisation of Registers Assesment of PHC Patient Information systems
PHC Facilities Patient Administration

Rationalisation of Registers

Background • The Health Systems Trust (HST) has been commissioned to coordinate and manage the national roll-out of the rationalised set of registers in all PHC facilities and provide technical support to provinces during this process. – Reducing the 56 Registers used in PHC facilities to 6 Registers • The set of rationalised registers that was implemented is as follows: – PHC comprehensive daily tick register + reception daily headcount register – TIER. net: ART for all HIV positive patients (including TB, Pregnant women, HIV+e babies) – TB registers (case identification and treatment registers) – Theatre register ( for facilities performing MMC and TOPs) – Delivery register – Midnight census for PHC facilities providing inpatient services


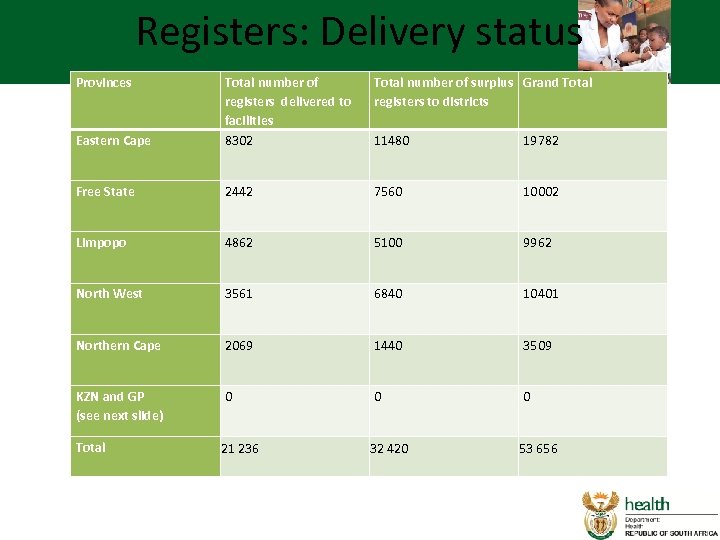
Registers: Delivery status Provinces Total number of surplus Grand Total registers to districts Eastern Cape Total number of registers delivered to facilities 8302 11480 19782 Free State 2442 7560 10002 Limpopo 4862 5100 9962 North West 3561 6840 10401 Northern Cape 2069 1440 3509 KZN and GP (see next slide) 0 0 0 Total 21 236 32 420 53 656

New set of Registers

Findings: positive perceptions • Waiting time reduced. • Reporting on fewer elements and workload is less • Uniformity of data collection tools leading to less administration and more better recording • More time spent with patients • Removal of duplications • Easy to collet correct data elements as layout on one page • Better reporting

Health Patient Registration

Primary Health Care Patient Information System • In preparation of the development of an automated patient based information system the HNSF work was extended to include the assessment of patient-centric primary healthcare (PHC) systems currently in use in the country, inlcuding systems used in the private sector and aimed at primary healthcare. Open Expression of Interest yielded 37 responses; • 23 systems were shortlisted based on eligibility criteria; • 1 Vendor retracted their submission; • Rigorous evaluation process including: – Definition of PHC system requirements; – Collection of detailed information from system vendors; – Representations from each system vendor; – Site visits where each of the systems were deployed;

Primary Health Care Patient Information System • This assessment culminated in recommendations on the most appropriate PHC Patient based information system to be deployed in PHC facilities • The outcome of this assessment is Automated PHC Patient Information systems - implemented in the NHI pilot districts ( 700 facilities) and be linked to the second phase of the scale up (1400 facilities)

Health Patient Registration System (HPRS) • Secure central database on a web based platform available to public health facilities to capture and verify beneficiary identification via bar coded identity documents and biometric methods. It also records patient visits to facilities. • Patient registry – a critical component to implement electronic health records nationally. • Planning tool because beneficiaries are linked to facilities based on their demographic details. • • Currently implemented at PHC facilities in NHI Pilot Districts. Auto-generates a unique Health Patient Registration Number (HPRN) and assigns to registered and successfully verified beneficiary. – HPRN is an internal system number that could be able to uniquely identify health beneficiaries for all other patients (including Foreign nationals). – South African National ID Number remains the primary identification for South African citizens.

KZN Beta Implementation September 2014 Focus on Patient Registration Reception Desk Support Integrated Team Approach RIPDA HPRS Certification of Competency Daily Data Capture Onsite Training
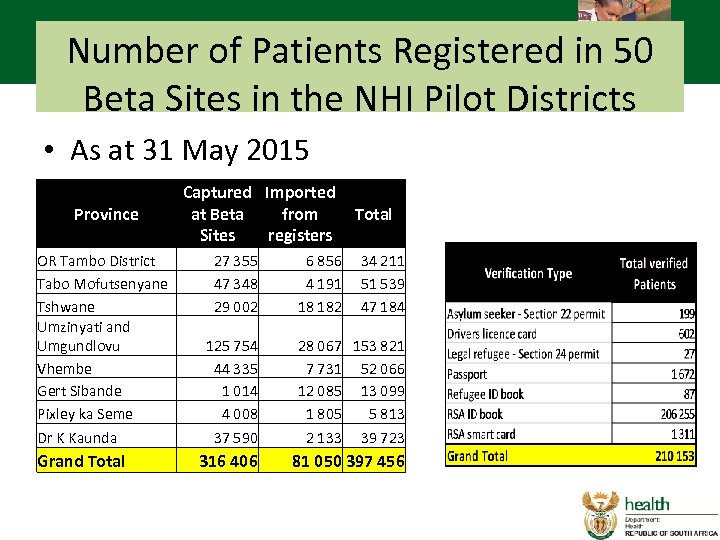
Number of Patients Registered in 50 Beta Sites in the NHI Pilot Districts • As at 31 May 2015 Province OR Tambo District Tabo Mofutsenyane Tshwane Umzinyati and Umgundlovu Vhembe Gert Sibande Pixley ka Seme Dr K Kaunda Grand Total Captured Imported at Beta from Sites registers 27 355 47 348 29 002 6 856 4 191 18 182 Total 34 211 51 539 47 184 125 754 44 335 1 014 4 008 37 590 28 067 153 821 7 731 52 066 12 085 13 099 1 805 5 813 2 133 39 723 316 406 81 050 397 456
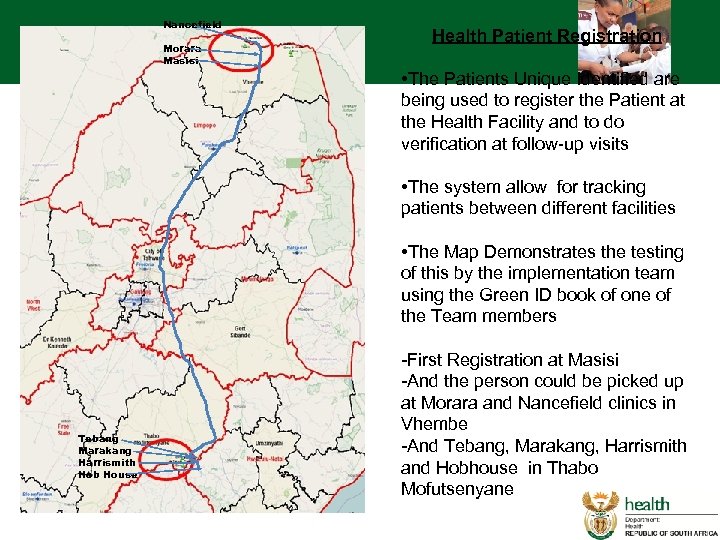
Nancefield Morara Masisi Health Patient Registration • The Patients Unique Identified are being used to register the Patient at the Health Facility and to do verification at follow-up visits • The system allow for tracking patients between different facilities • The Map Demonstrates the testing of this by the implementation team using the Green ID book of one of the Team members Tebang Marakang Harrismith Hob House -First Registration at Masisi -And the person could be picked up at Morara and Nancefield clinics in Vhembe -And Tebang, Marakang, Harrismith and Hobhouse in Thabo Mofutsenyane

Health Provider Registry • Software development completed • Infrastructure hardware established • Next step is to develop an implementation plan in consultation with health professional organisations

Accreditation and contracting of private providers
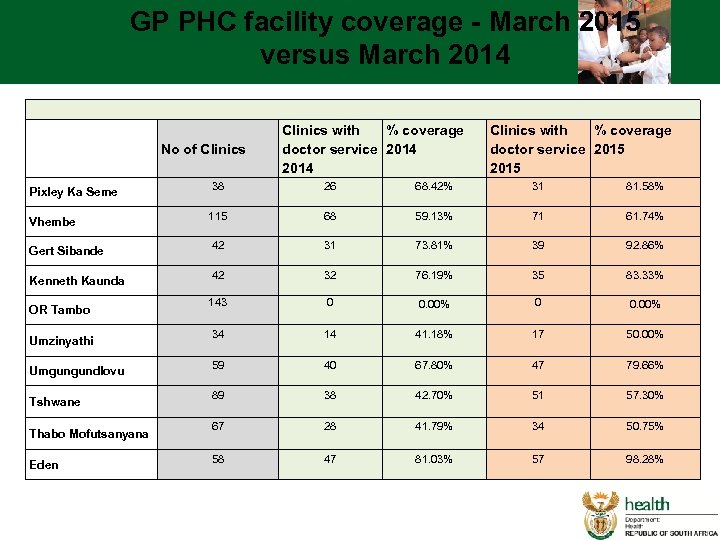
GP PHC facility coverage - March 2015 versus March 2014 No of Clinics Pixley Ka Seme Vhembe Gert Sibande Kenneth Kaunda OR Tambo Umzinyathi Umgungundlovu Tshwane Thabo Mofutsanyana Eden Clinics with % coverage doctor service 2014 % coverage Clinics with doctor service 2015 38 115 42 143 34 59 89 67 26 68 31 32 0 14 40 38 28 68. 42% 59. 13% 73. 81% 76. 19% 0. 00% 41. 18% 67. 80% 42. 70% 41. 79% 31 71 39 35 0 17 47 51 34 81. 58% 61. 74% 92. 86% 83. 33% 0. 00% 50. 00% 79. 66% 57. 30% 50. 75% 58 47 81. 03% 57 98. 28%

Central Chronic Medicines Dispensing and Distribution Program

Central Chronic Medicines Dispensing and Distribution Program • • • CCMDD aims to decongest public healthcare facilities and improve access to chronic medicines in South Africa. The program contracts the dispensing and distribution of repeat prescriptions for stable chronic patients to private sector service providers. The program of two program components, Central Chronic Medicines Dispensing and Distribution (CCMDD) and Pick-up Points (Pu. Ps). The first relates to individual patients’ medicines being centrally dispensed and distributed to the point of service delivery. The second relates to the provision of pre-dispensed medicines at private sector pharmacies, or ‘Pick-Up-Points’ (PUP), that is conveniently located for patients. Ø CCMDD is currently being rolled out in 10 districts, as well as in 2 hospitals that are not in the NHI districts. Ø Combined both models have in excess of 380, 000 patients; with current enrolments in the private distribution model half at around 190, 000.

Project Specific Expenditure 2014 -15
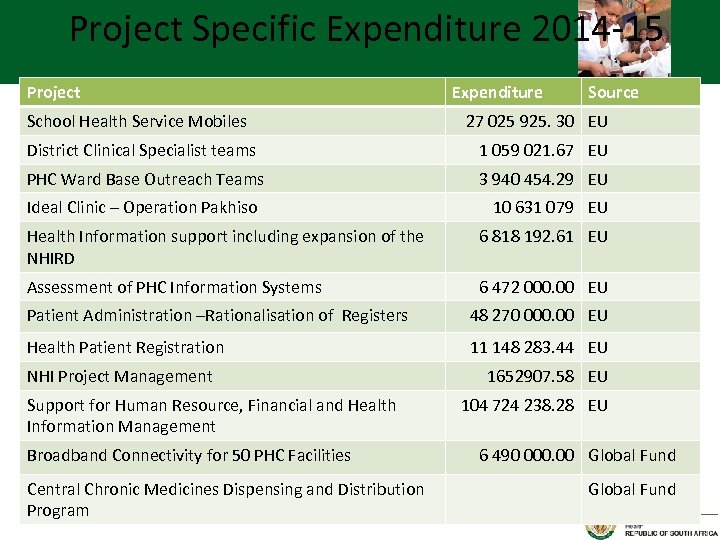
Project Specific Expenditure 2014 -15 Project School Health Service Mobiles Expenditure Source 27 025 925. 30 EU District Clinical Specialist teams 1 059 021. 67 EU PHC Ward Base Outreach Teams 3 940 454. 29 EU Ideal Clinic – Operation Pakhiso 10 631 079 EU Health Information support including expansion of the NHIRD 6 818 192. 61 EU Assessment of PHC Information Systems 6 472 000. 00 EU Patient Administration –Rationalisation of Registers 48 270 000. 00 EU Health Patient Registration 11 148 283. 44 EU NHI Project Management Support for Human Resource, Financial and Health Information Management Broadband Connectivity for 50 PHC Facilities Central Chronic Medicines Dispensing and Distribution Program 1652907. 58 EU 104 724 238. 28 EU 6 490 000. 00 Global Fund

NHI Pilot Sites Appraisal
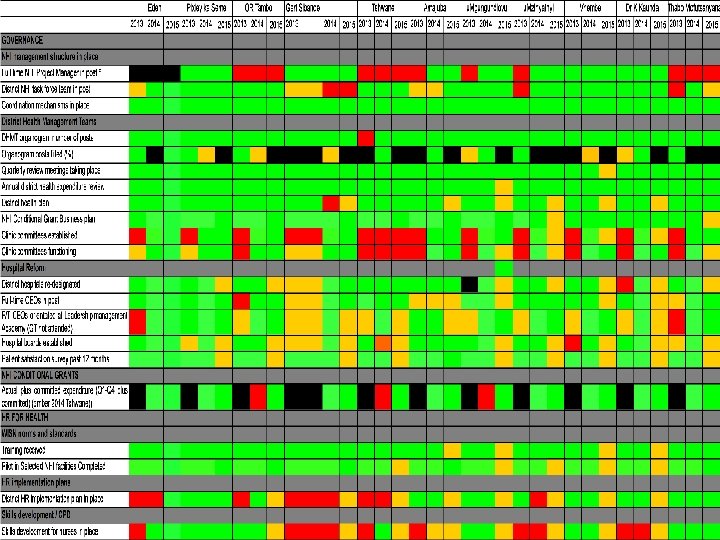
62
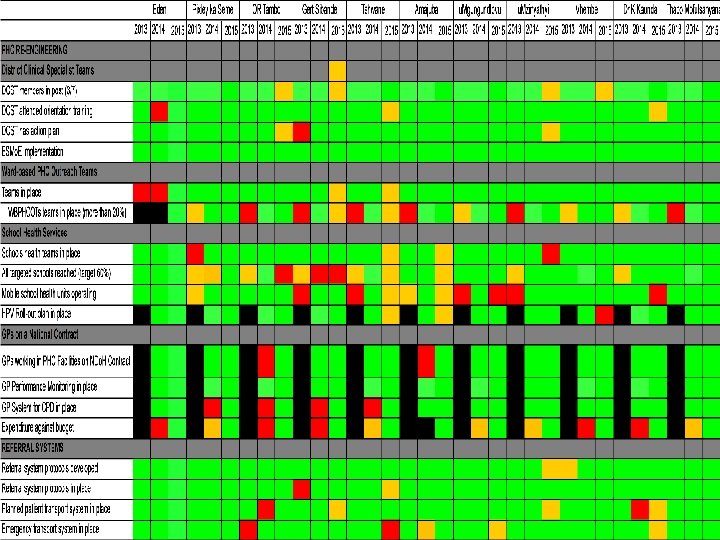
63
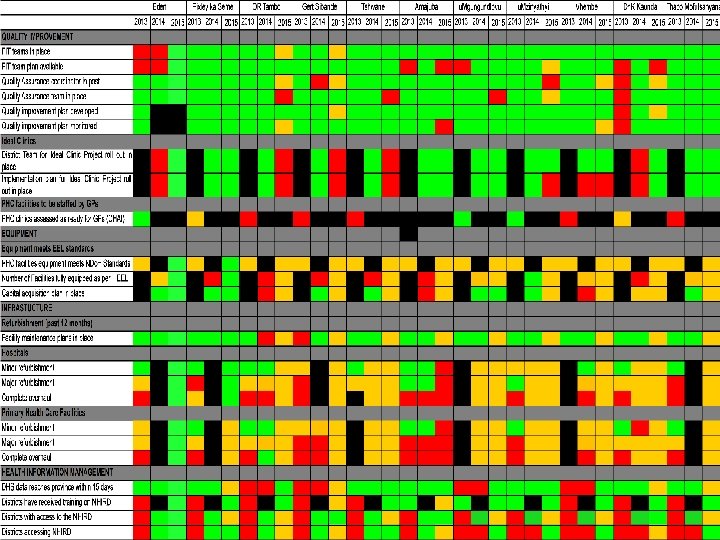
64
9b7912fefd9813995f10f1772d075368.ppt