495ad06effe108f6e5f0f639093a0141.ppt
- Количество слайдов: 28

Board Certification in Family Medicine Obstetrics—An Opportunity for Good Wm. Mac. Millan Rodney MD, FAAFP, FACEP Professor and Chair, Medicos para la Familia Memphis, Nashville, and International Editor, American Journal of Clinical Medicine American Board of Family Medicine Obstetrics WONCA 2010; Cancun, Mexico; Presenting The Family Medicine Obstetrics Curriculum and Data Medicos: A Success in Expanding Services at a Lower Cost. Eliminating Barriers to Family Planning: Hysteroscopic Tubal Occlusion without Anesthesia

Why Certification in Family Medicine Obstetrics? The American Model of highly specialized services is untenable wherever per capita income is less than $25, 000 per year. This is most of the planet. Childbirth has become a treacherous technical adventure with over 30% of women receiving a Cesarean birth. A start up OB service in a Florida Hospital requested and received over $12 million to deliver 300 babies per year. [$40, 000 each] In the USA, OB-Gyn has subspecialized to the point that many OB’s no longer deliver babies. Unfortunately hospitals and many international medical schools are following this model Africa, the UK, and USA are now developing 4 year options with one of these options to include surgical OB. Australians broke away from General Practice and created a specialty for rural and frontier medicine A new model is needed and available. Although , dwarfed by traditional academic medical centers, there are 30+ viable Family Medicine Obstetrics programs currently in operation. Africa has several others.

Multiple locations suggest Validity; See www. aafp. org fellowships Terminology Varies: Maternal Child Health is a thesis requiring 2 year program at Brown. The others are one year programs with most using the title Family Medicine Obstetrics Tacoma, Wa. Calls itself a rural fellowship 30 current MCH/OB fellowships programs offering 48 positions – – 3 Maternal Child Health fellowships 15 programs established since 2000 10 programs established 1990 -2000 5 programs established in 1980’s The unifying feature is training in surgical obstetrics. For example ETSU has a rural fellowship without obstetrics.

Pecci C, Leeman L, Wilkinson J. Family Medicine Obstetrics Fellowship Graduates: Training and Post-fellowship Experience. Fam Med 2008; 40(5): 326 -32. A Ten year Sample 32 fellowship programs identified; 26 programs represented 254 fellowship graduates identified graduating between 1992 -2002 166 surveys returned (65. 4%) 123 completed OB Fellowships; 43 completed MCH Fellowships 10 received a Masters of Public Health degree during fellowship
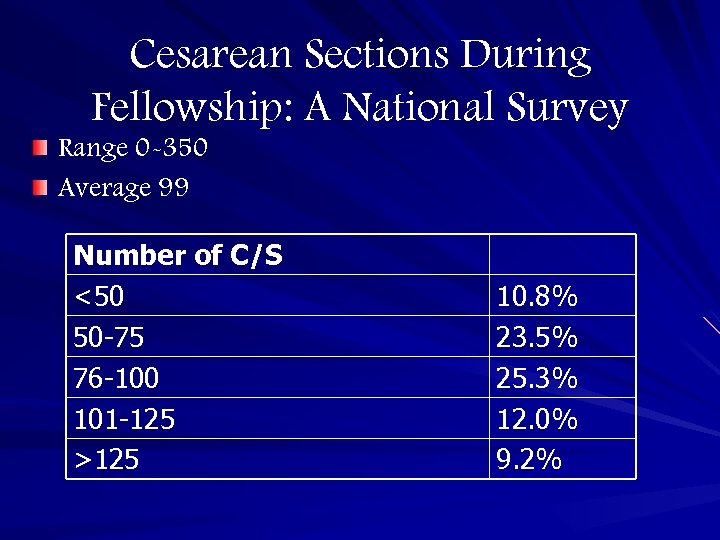
Cesarean Sections During Fellowship: A National Survey Range 0 -350 Average 99 Number of C/S <50 50 -75 76 -100 101 -125 >125 10. 8% 23. 5% 25. 3% 12. 0% 9. 2%
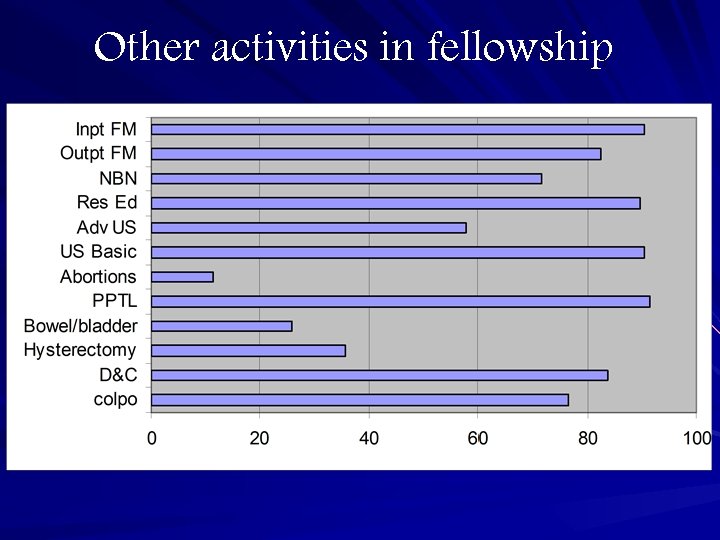
Other activities in fellowship

Family Medicine Obstetrics-Method. Wm. Mac. MIllan Rodney MD Career Statistics Fellowship Group 19922010; 100% sample response TOTAL Entered – Female 30 80 38% Completed Obtained Cesarean Privileges Spent ≥ 2 years Rural At Least 1 year as Faculty 74 71 47 36 93% 96% 64% 49%

Fellowship Training Goals – Maintain an identity in and a role for Family Medicine. – Provide continuing comprehensive health care unrestricted by age, organ system, and location of service. – Develop credentialed physicians similar to the African model of a district hospital physician combining public health, family medicine obstetrics with the ability to function in a mission hospital[some ortho, ER, +] Operative vaginal delivery and Cesarean sections Newborn resuscitation and stabilization Obstetrical, gyn, and emergency ultrasound Colposcopy , gyn, and office surgeries Care of complicated obstetric patients Evidence-based, family-centered maternal-child care

Fellowship Certification Advantages and Disadvantages Creates clear advantage for family physicians in communities where some surgical skills are necessary. The GP is elevated to OB with additional skills in general Med-Peds-Office Surgery. Creates an academic credential for hospitals unlikely to accept generic primary care physicians. Difficult process of training, written examination, and oral examination which needs to be expanded for international physicians. Need USA or Canadian medical license. Fellowships pay $50, 000 -90, 000 per year in US.

Am Board of Family Medicine Obstetrics— To Apply for Written Exam http: //www. abpsga. org/certification/family_ medicine_obstetric/application. html Be a graduate of a recognized college of medicine confirmed by a copy of an allopathic/osteopathic degree or a letter of verification from the institution where the degree was earned. In the case of foreign medical schools, an English translation of the document is also required. Graduates of foreign medical schools must also include a copy of their Education Commission for Foreign Medical Graduates (ECFMG) Certificate. Canadian medical schools and medical training programs are considered equivalent to U. S. medical schools and medical training programs. Hold a valid and unrestricted license to practice medicine in the United States, or its territories, or in Canada and submit copies of all licenses. License(s) must include date of expiration.

Am Board of Family Medicine Obstetrics-Requirements Verify staff privileges by means of an original signed letter from the administrator of each hospital, or facility, at which privileges are held confirming good standing at that facility. The letter(s) must be current, dated no more than one year prior to the date the application is received by ABPS. Be certified on the "Provider" level in the Advanced Life Support in Obstetrics (ALSO) program, and Neonatal Resuscitation Provider (NRP) program. ALSO and NRP do not have to be current at the time of submitting the application, but must be current and on file 30 days prior to taking the examination. Be board certified in Family Medicine by the ABMS, ABPS or AOA or be eligible to be certified by the Canadian Council of Family Practice (CCFP), or the Royal College of Physicians and Surgeons (RCPSC). Other Board Certifications may be considered on an individual basis.

Am Board Family Medicine Obstetrics-Requirements Be qualified under one of the following: – Have completed residency training in a program approved by the Accreditation Council of Graduate Medical Education or the American Osteopathic Association, Canadian Council of Family Practice (CCFP), or the Royal College of Physicians and surgeons (RCPSC) and deemed acceptable to the American Board of Family Medicine Obstetrics. Such training must include identifiable training and experience in Family Medicine Obstetrics as determined by the American Board of Family Medicine Obstetrics and approved by the ABPS. The ABPS now accepts all residencies accepted by the Royal College of Physicians and Surgeons of Canada (RCPSC). ABPS therefore now accepts all residencies approved by ACGME, AOA, or RCPSC. It should be noted that the ABPS accepts ALL medical residencies approved by the RCPSC, including approved residencies outside Canada.

Am Board Family Medicine Obstetrics--Requirements Osteopathic physicians who have successfully completed an AOAapproved internship, plus an AOA-approved General Medicine residency and have a minimum of two (2) years full-time experience in Family Medicine and 300 hours of CME acceptable to the BCFM. Submit three (3) letters of recommendation from active Diplomates of an ABPS, ABMS, or AOA-recognized board of certification. Letters of recommendation must be current (dated no more than one year prior to the date the application is received by the ABPS) and on letterhead stationery. The ABFMO requires original letters; copies are not acceptable. The ABFMO recommends that the letters be sent to the applicant for inclusion with other application documents.

Clinical Practice Track - This Track Will Be Available Until 2018. The applicant must have been actively engaged in the practice of Family Medicine with care of obstetric patients on an ongoing basis for five (5) years. This care should include the practice of surgical obstetrics. Documentation of training in obstetrics should include a case log listing all obstetrical cases completed in the previous two years. Applicants should demonstrate that their volume of obstetrical medicine is sufficient to maintain competence. . Applicants should have performed a minimum of 100 vaginal deliveries within the last 5 years. Applicants should have performed a minimum of 50 cesarean sections within the last 5 years.

Fellowship Track to ABFMOB Applicants who have satisfactorily completed a 12 -month, full-time fellowship that is recognized by the ABFMO will be considered eligible to sit for the written exam. The applicant should have completed their fellowship training within the last five years (8/2002). A list of fellowship programs that are currently recognized by the ABFMO is attached. Applicants who have completed a fellowship program that has not been recognized by the ABFMO may ask their program to submit materials for consideration. For Fellows who have completed a recognized fellowship, the fellowship director must submit an original signed letter of verification attesting to the applicant’s satisfactory completion of the program. The requirements for Fellowship training are outlined in the document “Guidelines for Recognition of Fellowship Programs by the ABFMO” and include the following minimum numbers of procedures. – A minimum of 100 vaginal deliveries. – A minimum of 50 cesarean sections, with a case log that is externally validated by one of the following: Medical Records, Medical Staff Office, Medical Director or Department Chair.

ABFMOB Oral Examination After successful completion of the written examination, applicants are also required to submit verification of competency in operative obstetrics and complete an oral examination. This portion of the examination will have an additional fee. The process is as follows: – The applicant must submit the names of three active Diplomates of an ABPS, ABMS, or AOA-recognized board of certification who will observe, or who have observed, the applicant during the care of Obstetrical patients, including at least 5 cesarean sections, and who will be willing to attest to the applicant’s surgical skills. – The Board will ask one or more of these physicians to complete and sign a notarized Statement of Evaluation regarding the applicant’s level of independence and surgical skill, to view click here. – Those applicants who successfully complete the attestation process will be eligible to sit for the oral examination.

OB FELLOWSHIP OUTCOMES 1992 -2010: WHERE DO THEY GO, WHO STOPS DELIVERING AND WHY? Wm. Mac. Millan Rodney MD, Conchita Martinez MD, Millard Collins MD, Greg Laurence MD, Carl Pean MD, Joe Stallings MD – Acknowledgments: Charles E. Couch, M. D. , ACOG[deceased], James Weber MD[deceased]; Eugene Felmar MD[deceased] Address Correspondence to: Wm. Mac. Millan Rodney, M. D. , 6575 Black Thorn Cove Memphis , Tn. 38119 e-mail: Wmrodney@aol. com Procedural Skills and Office Technology; www. psot. com

The Fellowship Solved Other Problems Regained financial control and ability to self fund a model office with open access appointments, EMR, all procedural equipment. The university “dumbs down” family medicine by forcing it to abandon skills. Retained alliances with ALSO statewide coalition, surgery lab, ultrasound course, and AAFP. Established osteopathic and allopathic alliances with Oklahoma State, the University of Arkansas, Louisiana, and rural locations in. Funded Developed alliance with previous faculty who had left academia for private practice. They provide selectives in GI endoscopy and Derm. Established 501 c 3 and began endowment. Implemented global outreach with fellowship rotations in Kenya, Ghana, Ecuador, Guatemala, and others. Trained leadership capable physicians who went on to colonize previously hostile environments. One hospital system welcomed fellowship trained family physicians into the department of Obstetrics.

Health Services Research The electronic medical record and a digital xray system created efficiencies and improved care. The OB call group 24/7 365 staffed an open access appointment system leading to improved service and 63, 000 visits in 2009. Gross revenue topped $ 5 Million. Published over 10 Studies and funded other research. See bibliography www. psot. com Developed an internet based and PDA available prenataldelivery database for the management of risk. >4, 000 deliver Developed a curriculum in Office and Obstetrical surgery. – Cognitive preloading for psychomotor skills: – The role of the live animal laboratory as simulator for repair of complex lacerations and inadvertent bladder entry. – Ultrasound assessment as a means of avoiding Cesarean Hysterectomy.

Transfer of Technology Projects Medicos-- A Mission Hospital Simulation in Tennessee Minor Surgery, Urgent Care, and some ER reengineered in the office Diagnostic services: ECG, CXR, and basic lab reengineered for the Office Colposcopy 1984 - established – Electrosurgery and cryosurgery came with this procedure OB-Gyn Ultrasound 1984 -established GI/ENT endoscopy 1979 -established American Board of Family Medicine Obstetrics

Board Certification in Family Medicine Obstetrics—An Opportunity for Good Wm. Mac. Millan Rodney MD, FAAFP, FACEP Professor and Chair, Medicos para la Familia Memphis, Nashville, and International Editor, American Journal of Clinical Medicine American Board of Family Medicine Obstetrics WONCA 2010; Cancun, Mexico; Presenting The Family Medicine Obstetrics Curriculum and Data Medicos: A Success in Expanding Services at a Lower Cost. Eliminating Barriers to Family Planning: Hysteroscopic Tubal Occlusion without Anesthesia

References Supporting Cesarean Training in Family Medicine Nothnagle, M; Sicilia, J; Forman, S, et al, Rodney WM. Required Procedural Training in Fammily Medicine Residency: A Consensus Statement. Fam Med 2008; 40(4): 248 -52. 24)Kelly B, Sicilia J, Forman S. Advanced Procedural Training in Family Medicine: A Consensus Statement Fam Med 2009; 41(6): 398 -404. 25)Norris T, Reese, J, Pirani M, et al. Are Rural Family Physicians Comfortable Performing Cesarean Sections? J Fam Pract 1996; 43: 455 -460. 26)Deutchman M, Connor P, Gobbo R, Fitz. Simmons R. Outcomes Of Cesarean Sections Performed By Family Physicians And The Training They Received: A 15 -Year Retrospective Study. J Am Board Fam Pract 1995; 8: 81 -90. 27)Eidson-Ton WS, Nuovo J, Solis B, et al; An Enhanced Obstetrics Track for a Family Practice Residency Program: Results from the First 6 Years. J Am Board Fam Pract 2005; 18: 223 -8. 28)Pecci C, Leeman L, Wilkinson J, Family Medicine obstyetrics Fellowship Graduates: Training and Post-fellowship Experience. Fam Med 2008; 40(5): 326 -32. 29)Heider A, Neely B, Bell L. Cesarean Delivery Results in a Family Medicine Resedency Using a Specific Training Model. Fam Med 2006; 38(2): 103 -9.

Bibliography 1. Morgan WC, Rodney WM, Hahn RG, Garr DA, O'Brien J. Echografie bij Verloskunden en gynaecologie in de praktijruiute: Een ondersteuning voor Luisartsenverloskunde (Office-based ultrasound as a support for family centered obstetrics), Huissarts Nu (HANU) 1987; 16: 277 -280. 2. Morgan WC, Rodney WM, Garr DA, Hahn RG. Ultrasound for the primary care physician: Applications in family-centered obstetrics. Postgrad Med 1988; 83(2): 103 -107 3. Hahn R, Ornstein S, Davies TC, Rodney WM, et al. Obstetric ultrasound training for family physicians: results from a multi-site study. J Fam Pract 1988; 26: 553 -558. 4. Hahn RG, Davies TC, Rodney WM. Diagnostic ultrasound in general practice. Fam Pract--An International Journal 1988; 5(2): 129 -135. 5. Rodney WM, Prislin MD, Hahn RG. Family practice obstetrical ultrasound in an urban community health center: Birth outcomes and examination accuracy of the initial 227 cases. J Fam Pract 1990; 30: 163 -168. 6. Rodney WM, Hahn RG, Hartman KJ, Deutchman ME. Obstetric ultrasound by family physicians. J Fam Pract 1992; 34: 186 -200. 7. Deutchman ME, Hahn RG, Rodney WM. Maternal gallbladder assessment during obstetric ultrasound: results and technique. J Fam Pract 1994; 39: 33 -37. 8. Euans DW, Hahn RG, Rodney WM. A comparison of manual and ultrasound measurements of fundal height. J Fam Pract 1995; 40: 233 -236. 9. Rodney WM. Historical observations from the RRC 1994 -2000: Maternity care[OB] training in FP. J Am Board Fam Pract 2002; 15: 255 -56. 10. Dresang LT. Rodney WM, Dees J. Teaching OB ultrasound to family practice residents. Fam Med 2004; 36: 98 -107. 11. Dresang LT, Rodney WM, Leeman L, Dees J, Koch, P, Palencio M. ALSO in Ecuador: Teaching the Teachers. J Am Board Fam Practice. 2004; 17(4): 276 -282. http: //www. jabfp. org/cgi/content/full/17/4/276 12. Dresang LT, Rodney WM, Rodney KMM. Prenatal Ultrasound: A tale of two cities. J Nat Med Association Feb 2006; 98: 167 -171.

Challenges—Civil Rights Political stability and the threat of mandatory consultation for things like labor at 36 weeks The threat of a “bad case”. Medicos para la Familia example: – No maternal deaths or morbidity, n=3000 + deliveries – 14 newborn deaths, shoulder dystocias, brachial plexus injury; retained placentas, over 1000 Cesareans, abruptio; HELLP; American nursing politics, staff squabbles – One lawsuit, and medical malpractice insurance has doubled to $30, 000/year since 1999. Year one cost is $12, 000.




International Medicine vs. USA Twice the service at a tenth of the cost 50 bed hospital Destin Fla Comprehensive women’s health program to cost $ 12 million for start up. Currently 500 women in the county deliver each year. Start up $24, 000 per delivery. Hospital charges $4 -5 k/delivery “We’re not-forprofit. ” Reference The Destin Log. May 7, 2005. p. A 14
495ad06effe108f6e5f0f639093a0141.ppt