7501988ce8da78d2dd30b31967cdd405.ppt
- Количество слайдов: 117

Biomedical Informatics 2011 Year in Review Notable publications and events in Informatics since the 2010 AMIA Symposium Daniel R. Masys, MD Affiliate Professor Biomedical and Health Informatics University of Washington, Seattle
Content for this session is at: http: //faculty. washington. edu/dmasys/Year. In. Review including citation lists and links and this Power. Point
Index to all Years in Review http: //faculty. washington. edu/dmasys/Year. In. Review

Design for this Session l l l Modeled on American College of Physician “Update” sessions Emphasis on ‘what it is’ and ‘why it is important’ Audience interaction for each category of item discussed

Source of Content for Session l l Literature review of RCTs indexed by Me. SH term “Medical Informatics”, “Telemedicine” & descendents or main Me. SH term “Bioinformatics”, and Entrez date between November 2010 and October 2011 further qualified by involvement of >100 providers or patients Poll of American College of Medical Informatics fellows list

Thanks to: l l l l Russ Altman David Bates Bruce Buchanan George Hripcsak Ken Goodman Christoph Lehmann Harold Lehmann Nancy Lorenzi l l l l Betsy Humphreys Don Detmer Blackford Middleton Joyce Mitchell Morris Collen Bill Stead Dean Sittig Bill Tierney

Session components Representative New Literature l Notable Events – the ‘Top Five’ list l

New Literature Highlights: Clinical Informatics Clinical Decision Support l Telemedicine l The practice of informatics l

New Literature Highlights: Bioinformatics and Computational Biology Human Health and Disease l The practice of bioinformatics l

Clinical Decision Support 51 new RCTs published meeting search criteria November 2010 – October 2011

Clinical Decision Support for Providers: cardiovascular diseases l l Reference l Magid DJ, et. al, A multimodal blood pressure control intervention in 3 healthcare systems. Am J Manag Care. 2011 Apr; 17(4): e 96 -103 Source l Institute for Health Research, Kaiser Permanente Colorado, Denver. Aim l To determine if a multimodal intervention composed of patient education, home blood pressure (BP) monitoring, BP measurement reporting to an interactive voice response (IVR) phone system, and clinical pharmacist follow-up improves BP control compared with usual care. Methods l RCT conducted at 3 healthcare systems in Denver, Colorado, including a large health maintenance organization, a Veterans Affairs medical center, and a county hospital. l Prospective study with patient enrollment, medication consultation and adjustment, remote BP monitoring, and follow-up at 6 months.

Clinical Decision Support for Providers: cardiovascular diseases l l l Reference l Magid DJ, et. al, A multimodal blood pressure control intervention in 3 healthcare systems. Am J Manag Care. 2011 Apr; 17(4): e 96 -103. . Methods, cont’d l At each site, patients with uncontrolled BP were randomized to the multimodal intervention vs usual care for 6 months, with the primary end point of BP reduction. Results l 338 patients randomized, 283 (84%) completed the study, including 138 intervention patients and 145 usual care patients. l BP was higher in the intervention group vs the usual care group (150. 5/89. 4 vs 143. 8/85. 3 mm Hg). l At 6 months, BPs were similar in the intervention group vs the usual care group (137. 4 vs 136. 7 mm Hg, P =. 85 for systolic; 82. 9 vs 81. 1 mm Hg, P =. 14 for diastolic).

Clinical Decision Support for Providers: cardiovascular diseases l l l Reference l Magid DJ, et. al, A multimodal blood pressure control intervention in 3 healthcare systems. Am J Manag Care. 2011 Apr; 17(4): e 96 -103. Results, cont’d l BP reductions were greater in the intervention group vs the usual care group (− 13. 1 vs − 7. 1 mm Hg, P =. 006 for systolic; − 6. 5 vs − 4. 2 mm Hg, P =. 07 for diastolic). l Adherence to medications was similar between the 2 groups, but intervention patients had a greater increase in medication regimen intensity. Conclusions l A multimodal intervention of patient education, home BP monitoring, BP measurement reporting to an IVR system, and clinical pharmacist follow-up achieved greater reductions in BP compared with usual care.

Clinical Decision Support for Providers: cardiovascular diseases l l Reference l Magid DJ, et. al, A multimodal blood pressure control intervention in 3 healthcare systems. Am J Manag Care. 2011 Apr; 17(4): e 96 -103. Importance l Hybrid decision support systems such as automated phone response systems, combined with self-generated physiologic monitoring observations, and a human effector arm (clinical pharmacist followup), can provide effective sociotechnical approaches to decision support.

Clinical Decision Support for Providers: cardiovascular diseases l l Reference l Bosworth HB, et. al, Home blood pressure management and improved blood pressure control: results from a randomized controlled trial. Arch Intern Med. 2011 Jul 11; 171(13): 1173 -80. Source l Health Services Research and Development, Durham Veterans Affairs Medical Center, Durham, NC Aim l To determine which of 3 interventions was most effective in improving blood pressure (BP) control Methods l 4 -arm randomized trial with 18 -month follow-up at the primary care clinics at a Veterans Affairs Medical Center. l Pts randomized to either usual care or 1 of 3 telephone-based intervention groups: l l l (1) nurse-administered behavioral management, (2) nurse- and physician-administered medication management, or (3) a combination of both.

Clinical Decision Support for Providers: cardiovascular diseases l l l Reference l Bosworth HB, et. al, Home blood pressure management and improved blood pressure control: results from a randomized controlled trial. Arch Intern Med. 2011 Jul 11; 171(13): 1173 -80. Methods, cont’d l Intervention telephone calls were triggered based on home BP values transmitted via telemonitoring devices. l Behavioral management involved promotion of health behaviors. Medication management involved adjustment of medications by a study physician and nurse based on hypertension treatment guidelines. l Primary outcome was change in BP control measured at 6 -month intervals over 18 months Results l 593 individuals enrolled; 48% were African American. l Both behavioral management and medication management alone showed significant improvements at 12 months-12. 8% (95% confidence interval [CI], 1. 6%-24. 1%) and 12. 5% (95% CI, 1. 3%23. 6%), respectively-but not at 18 months.

Clinical Decision Support for Providers: cardiovascular diseases l l l Reference l Bosworth HB, et. al, Home blood pressure management and improved blood pressure control: results from a randomized controlled trial. Arch Intern Med. 2011 Jul 11; 171(13): 1173 -80. Results, cont’d l In subgroup analyses, among those with poor baseline BP control, systolic BP decreased in the combined intervention group by 14. 8 mm Hg (95% CI, -21. 8 to -7. 8 mm Hg) at 12 months and 8. 0 mm Hg (95% CI, -15. 5 to -0. 5 mm Hg) at 18 months, relative to usual care. Conclusions l Overall intervention effects were moderate, but among individuals with poor BP control at baseline, the effects were larger. l Study indicates the importance of identifying individuals most likely to benefit from potentially resource intensive programs

Clinical Decision Support for Providers: cardiovascular diseases l l Reference l Bosworth HB, et. al, Home blood pressure management and improved blood pressure control: results from a randomized controlled trial. Arch Intern Med. 2011 Jul 11; 171(13): 1173 -80. Importance l Example of automated physiologic home monitoring alerting clinic personnel to intervene in a chronic condition with an effector mechanism involving interpersonal communications. l Similar interventions will be increasingly enabled by wireless communications and low cost/high reliability solid state monitors.

Clinical Decision Support for Providers: cardiovascular diseases l l Reference l Schnipper JL, et. al, Effects of documentation-based decision support on chronic disease management. A m J Manag Care. 2010 Dec; 16(12 Suppl HIT): SP 72 -81. Source l Division of General Medicine and Primary Care, Brigham and Women's Hospital, Boston, MA Aim l To evaluate whether a new documentation-based clinical decision support system (CDSS) is effective in addressing deficiencies in the care of patients with coronary artery disease (CAD) and diabetes mellitus (DM). Methods l Controlled trial randomized by physician. l Primary care physicians (PCPs) in 10 ambulatory practices assigned to usual care or a CAD/DM Smart Form for 9 months. l Primary outcome was the proportion of deficiencies in care that were addressed within 30 days after a patient visit
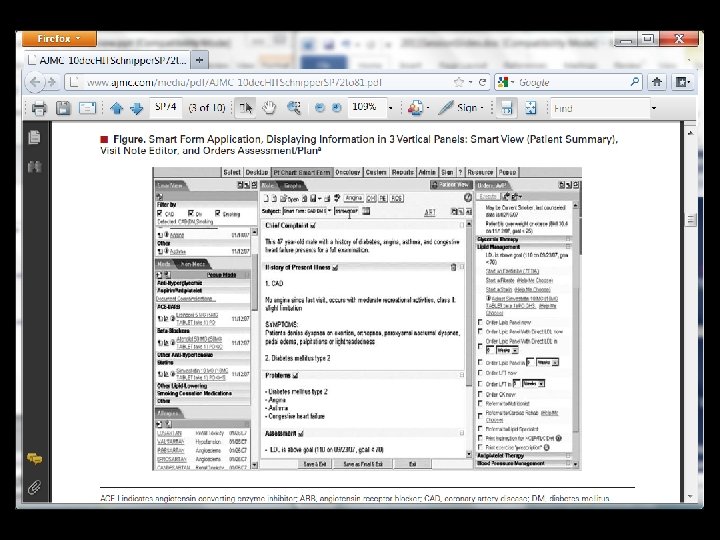

Clinical Decision Support for Providers: cardiovascular diseases l l Reference l Schnipper JL, et. al, Effects of documentation-based decision support on chronic disease management. A m J Manag Care. 2010 Dec; 16(12 Suppl HIT): SP 72 -81. Results l Smart Form was used for 5. 6% of eligible patients. l In the intention-to-treat analysis, patients of intervention PCPs had a greater proportion of deficiencies addressed within 30 days of a visit compared with controls (11. 4% vs 10. 1%, adjusted and clustered odds ratio =1. 14; 95% confidence interval, 1. 02 -1. 28; P =. 02). l Differences were more pronounced in the "on-treatment" analysis: 17. 0% of deficiencies were addressed after visits in which the Smart Form was used compared with 10. 6% of deficiencies after visits in which it was not used (P <. 001). l Measures that improved included documentation of smoking status and prescription of antiplatelet agents when appropriate. .

Clinical Decision Support for Providers: cardiovascular diseases l l l Reference l Schnipper JL, et. al, Effects of documentation-based decision support on chronic disease management. A m J Manag Care. 2010 Dec; 16(12 Suppl HIT): SP 72 -81. Conclusions l Overall use of the CAD/DM Smart Form was low, and improvements in management were modest. l When used, documentation-based decision support shows promise. Importance l Systems have to be used in order to have any effects on care

Clinical Decision Support for Providers: cardiovascular diseases l l l Reference l Fitzgerald M, et. al, Trauma resuscitation errors and computerassisted decision support. Arch Surg. 2011 Feb; 146(2): 218 -25. Source l The Alfred Hospital, Melbourne, Victoria, Australia. Aim l To determine whether computer-aided decision support during the first 30 minutes of trauma resuscitation reduces management. Methods l Prospective, open, randomized, controlled interventional study that evaluated the effect of real-time, computer-prompted, evidence-based decision and action algorithms on error occurrence during initial resuscitation between January 24, 2006, and February 25, 2008. l Enrolled severely injured adults at a level I trauma center Results l 1171 patients were recruited into 3 groups: 300 into a baseline control group, 436 into a concurrent control group, and 435 into the study group.

Clinical Decision Support for Providers: cardiovascular diseases l l l Reference l Fitzgerald M, et. al, Trauma resuscitation errors and computerassisted decision support. Arch Surg. 2011 Feb; 146(2): 218 -25. Results, cont’d l There was a reduction in error rate per patient from the baseline control group to the study group (2. 53 to 2. 13, P =. 004) and from the control group to the study group (2. 30 to 2. 13, P =. 04). l A critical decision was required every 72 seconds, and error-free resuscitations were increased from 16. 0% to 21. 8% (P =. 049) during the first 30 minutes of resuscitation. l Morbidity from shock management (P =. 03), blood use (P <. 001), and aspiration pneumonia (P =. 046) were decreased. . Conclusions l Computer-aided, real-time decision support resulted in improved protocol compliance and reduced errors and morbidity.

Clinical Decision Support for Providers: cardiovascular diseases l Reference l Fitzgerald M, et. al, Trauma resuscitation errors and computerassisted decision support. Arch Surg. 2011 Feb; 146(2): 218 -25. l Importance l Effective real time decision support can be designed for timepressured, high intensity clinical interactions such as trauma resuscitation. l Substantial additional opportunity for improvement. l Stay healthy, my friends…

Clinical Decision Support for Providers: cancer detection and treatment l l Reference l Imperiale TF et. al, Provider acceptance, safety, and effectiveness of a computer-based decision tool for colonoscopy preparation. Int J Med Inform. 2011 Oct; 80(10): 726 -33. Source l Indianapolis VA Medical Center, Indiana University Medical Center and Regenstrief Institute, Indianapolis, IN. Aims l To assess provider acceptance of recommendations by a decision tool that scans the electronic medical record and determines whether sodium phosphate may be taken. l To determine decision tool effects on a composite outcome of colonoscopies canceled, rescheduled, aborted, or repeated sooner than recommended due to preparation (prep) quality; prep quality; colonoscopy duration; and patient satisfaction with and tolerance of the preparation. . Methods l Four alternating four-week periods to compare the decision tool with usual care for outpatient colonoscopy.

Clinical Decision Support for Providers: cancer detection and treatment l l l Reference l Imperiale TF et. al, Provider acceptance, safety, and effectiveness of a computer-based decision tool for colonoscopy preparation. Int J Med Inform. 2011 Oct; 80(10): 726 -33. Methods, cont’d l All decision tool decisions were reviewed in real-time by gastroenterology nurses and/or physicians. l Patients completed a survey about the prep process. l Endoscopists blindly rated prep quality. l Colonoscopy duration and findings were recorded. Results l Of 354 persons in the decision tool group, 4 prep decisions were overridden because of patient preference or prior prep failure, but none for medical reasons. l Sodium phosphate was used more frequently in the decision tool group (73% vs. 41%; P<0. 01).

Clinical Decision Support for Providers: cancer detection and treatment l l l Reference l Imperiale TF et. al, Provider acceptance, safety, and effectiveness of a computer-based decision tool for colonoscopy preparation. Int J Med Inform. 2011 Oct; 80(10): 726 -33. Results, cont’d l No difference between the decision tool and usual care groups in the composite outcome (26% vs. 30%, respectively; P=0. 29), acceptable prep quality (62% vs. 56%; P=0. 22), colonoscopy duration (28 vs. 30 min; P=0. 17), patient satisfaction (P=0. 38), or preparation tolerance (P=0. 37) Conclusions l An electronic medical record-based decision tool can safely and effectively tailor the prep for colonoscopy and may improve colonoscopy efficiency and patient satisfaction

Clinical Decision Support for Providers: cancer detection and treatment l l Reference l Imperiale TF et. al, Provider acceptance, safety, and effectiveness of a computer-based decision tool for colonoscopy preparation. Int J Med Inform. 2011 Oct; 80(10): 726 -33. Importance l CDSS systems can be effectively applied to low intensity settings where elective choices about outpatient procedures may have large multiplier effects based on the frequency and cost of the procedures planned.

Clinical Decision Support for Providers: cancer detection and treatment l l Reference l Cleeland CS, et. al, Automated symptom alerts reduce postoperative symptom severity after cancer surgery: a randomized controlled clinical trial. J Clin Oncol. 2011 Mar 10; 29(8): 994 -1000. Source l MD Anderson Cancer Center, Houston, TX. Aim l To determine whether at-home symptom monitoring plus feedback to clinicians about severe symptoms contributes to more effective postoperative symptom control after cancer-related thoracotomy. Methods l A two arm RCT for patients receiving thoracotomy for lung cancer or lung metastasis. l After hospital discharge, patients rated symptoms twice weekly for 4 weeks via automated telephone calls. l For intervention group patients, an e-mail alert was forwarded to the patient's clinical team for response if any of a subset of symptoms (pain, disturbed sleep, distress, shortness of breath, or constipation) reached a predetermined severity threshold.

Clinical Decision Support for Providers: cancer detection and treatment l l l Reference l Cleeland CS, et. al, Automated symptom alerts reduce postoperative symptom severity after cancer surgery: a randomized controlled clinical trial. J Clin Oncol. 2011 Mar 10; 29(8): 994 -1000. Methods, cont’d l No alerts were generated for controls. l Group differences in symptom threshold events were examined by generalized estimating equation modeling. Results l 100 patients enrolled; 79 patients completed the study. l Intervention group experienced greater reduction in symptom threshold events than did controls (19% v 8%, respectively) and a more rapid decline in symptom threshold events. l Difference in average reduction in symptom interference between groups was -0. 36 (SE, 0. 078; P =. 02). l Clinicians responded to 84% of e-mail alerts.

Clinical Decision Support for Providers: cancer detection and treatment l l Reference l Cleeland CS, et. al, Automated symptom alerts reduce postoperative symptom severity after cancer surgery: a randomized controlled clinical trial. J Clin Oncol. 2011 Mar 10; 29(8): 994 -1000. . Results, cont’d l Both groups reported equally high satisfaction with the automated system and with postoperative symptom control. Conclusions l Frequent symptom monitoring with alerts to clinicians when symptoms became moderate or severe reduced symptom severity during the 4 weeks after thoracic surgery. l Methods of automated symptom monitoring and triage may improve symptom control after major cancer surgery. Importance l Example of systems approach to acquiring symptom data, automated filtering and clinician alerting

Clinical Decision Support for Providers: cancer detection and treatment l l Reference l Berry DL, et. al, Enhancing patient-provider communication with the electronic self-report assessment for cancer: a randomized trial. J Clin Oncol. 2011 Mar 10; 29(8): 1029 -35. Epub 2011 Jan 31. Source l Harvard Medical School, Boston, MA. Aim l T determine the effect of the Electronic Self-Report Assessment. Cancer (ESRA-C) on the likelihood of Symptoms and Quality of Life Issues (SQLIs) being discussed between clinicians and patients with cancer in ambulatory clinic visits. l Secondary objectives included comparison of visit duration between groups and usefulness of the ESRA-C as reported by clinicians. . Methods l RCT in Pts with various cancer diagnoses and stages at two institutions of a comprehensive cancer center. l Patient-reported SQLIs were automatically displayed on a graphical summary and provided to the clinical team before an on-treatment visit. l In control group, no summary was provided.

Clinical Decision Support for Providers: cancer detection and treatment l l l Reference l Berry DL, et. al, Enhancing patient-provider communication with the electronic self-report assessment for cancer: a randomized trial. J Clin Oncol. 2011 Mar 10; 29(8): 1029 -35. Epub 2011 Jan 31. Methods, cont’d l SQLIs were scored for level of severity or distress. l One on-treatment clinic visit was audio recorded for each participant and then scored for discussion of each SQLI. l Authors hypothesized that problematic SQLIs would be discussed more often when the intervention was delivered to the clinicians. Results l The likelihood of SQLIs being discussed differed by randomized group and depended on whether an SQLI was first reported as problematic (P =. 032). l Clinic visits were similar with regard to duration between groups, and clinicians reported the summary as useful

Clinical Decision Support for Providers: cancer detection and treatment l l l Reference l Berry DL, et. al, Enhancing patient-provider communication with the electronic self-report assessment for cancer: a randomized trial. J Clin Oncol. 2011 Mar 10; 29(8): 1029 -35. Epub 2011 Jan 31. Conclusion l The ESRA-C is the first electronic self-report application to increase discussion of SQLIs in a US randomized clinical trial. Importance l Contributes to the emerging trend of capturing data from patients, formatting it and presenting it to clinicians to encourage clinical management behaviors that represent best practice.

Clinical Decision Support for Providers: diabetes l l Reference l Cebul RD et. al, Electronic health records and quality of diabetes care. N Engl J Med. 2011 Sep 1; 365(9): 825 -33. Source l Department of Medicine, Case Western Reserve University at Metro. Health Medical Center, Cleveland, OH. Aim l To compare achievement of and improvement in quality standards for diabetes at practices using EHRs with CDSS with those at practices using paper records. Methods l All practices, including many safety-net primary care practices, belonged to a regional quality collaborative and publicly reported performance. l Authors used generalized estimating equations to calculate the percentage-point difference between EHR-based and paper-based practices with respect to achievement of composite standards for diabetes care (including four component standards) and outcomes (five standards), after adjusting for covariates and accounting for clustering.

Clinical Decision Support for Providers: diabetes l l l Reference l Cebul RD et. al, Electronic health records and quality of diabetes care. N Engl J Med. 2011 Sep 1; 365(9): 825 -33 Methods, cont’d l Covariates included insurance type (Medicare, commercial, Medicaid, or uninsured), race or ethnic group (white, black, Hispanic, or other), age, sex, estimated household income, and level of education. l Analyses were conducted separately for the overall sample and for safety-net practices. Results l From July 2009 through June 2010, data were reported for 27, 207 adults with diabetes seen at 46 practices; safety-net practices accounted for 38% of patients. l After adjustment for covariates, achievement of composite standards for diabetes care was 35. 1 percentage points higher at EHR sites than at paper-based sites (P<0. 001), and achievement of composite standards for outcomes was 15. 2 percentage points higher (P=0. 005).

Clinical Decision Support for Providers: diabetes l l Reference l Cebul RD et. al, Electronic health records and quality of diabetes care. N Engl J Med. 2011 Sep 1; 365(9): 825 -33 Results, cont’d l EHR sites were associated with higher achievement on eight of nine component standards. l Such sites were also associated with greater improvement in care (a difference of 10. 2 percentage points in annual improvement, P<0. 001) and outcomes (a difference of 4. 1 percentage points in annual improvement, P=0. 02). l Across all insurance types, EHR sites were associated with significantly higher achievement of care and outcome standards and greater improvement in diabetes care. l Results confined to safety-net practices were similar.

Clinical Decision Support for Providers: diabetes l l l Reference l Cebul RD et. al, Electronic health records and quality of diabetes care. N Engl J Med. 2011 Sep 1; 365(9): 825 -33 Conclusions l Findings support the premise that federal policies encouraging the meaningful use of EHRs may improve the quality of care across insurance types. Importance l Regional-scale assessment for a common chronic condition reports a beneficial effect of EHRs with CDSS.

Clinical Decision Support for Providers: diabetes l l Reference l O'Connor PJ, et. al, Impact of electronic health record clinical decision support on diabetes care: a randomized trial. Ann Fam Med. 2011 Jan -Feb; 9(1): 12 -21. Source l Health Partners Medical Group, Minneapolis, MN. Aim l To assess the impact of an electronic health record-based diabetes clinical decision support system on control of hemoglobin A(1 c) (glycated hemoglobin), blood pressure, and low-density lipoprotein (LDL) cholesterol levels in adults with diabetes. Methods l Clinic-randomized trial conducted from October 2006 to May 2007 in Minnesota. l Patients were randomized either to receive or not to receive an electronic health record (EHR)-based clinical decision support system designed to improve care for those patients whose hemoglobin A(1 c), blood pressure, or LDL cholesterol levels were higher than goal at any office visit.

Clinical Decision Support for Providers: diabetes l l l Reference l O'Connor PJ, et. al, Impact of electronic health record clinical decision support on diabetes care: a randomized trial. Ann Fam Med. 2011 Jan -Feb; 9(1): 12 -21. Methods, cont’d l Analysis used general and generalized linear mixed models with repeated time measurements to accommodate the nested data structure. Results l 11 clinics with 41 consenting primary care physicians and the physicians' 2, 556 patients with diabetes enrolled. l The intervention group physicians used the EHR-based decision support system at 62. 6% of all office visits made by adults with diabetes. l Intervention group diabetes patients had significantly better hemoglobin A(1 c) (intervention effect -0. 26%; 95% confidence interval, -0. 06% to -0. 47%; P=. 01), and better maintenance of systolic blood pressure control (80. 2% vs 75. 1%, P=. 03).

Clinical Decision Support for Providers: diabetes l l l Reference l O'Connor PJ, et. al, Impact of electronic health record clinical decision support on diabetes care: a randomized trial. Ann Fam Med. 2011 Jan -Feb; 9(1): 12 -21. Methods, cont’d l Analysis used general and generalized linear mixed models with repeated time measurements to accommodate the nested data structure. Results, cont’d l Intervention group had borderline better maintenance of diastolic blood pressure control (85. 6% vs 81. 7%, P =. 07), but not improved lowdensity lipoprotein cholesterol levels (P =. 62) than patients of physicians randomized to the control arm of the study. l Among intervention group physicians, 94% were satisfied or very satisfied with the intervention, and moderate use of the support system persisted for more than 1 year after feedback and incentives to encourage its use were discontinued.

Clinical Decision Support for Providers: diabetes l l l Reference l O'Connor PJ, et. al, Impact of electronic health record clinical decision support on diabetes care: a randomized trial. Ann Fam Med. 2011 Jan -Feb; 9(1): 12 -21. Conclusions l EHR-based diabetes clinical decision support significantly improved glucose control and some aspects of blood pressure control in adults with type 2 diabetes. Importance l Adds to literature on utility of outpatient CDSS systems for high prevalence chronic conditions. l CDSS studies that use objective physiologic data (BP, Hb. A 1 C) have an advantage in presentation and interpretation of results

Clinical Decision Support for Providers: infectious diseases l l Reference l Humiston SG, et. al, Increasing inner-city adult influenza vaccination rates: a randomized controlled trial. Public Health Rep. 2011 Jul. Aug; 126 Suppl 2: 39 -47. Source l Department of Pediatrics, University of Rochester School of Medicine and Dentistry, Rochester, NY. Aim l To evaluate the effect of the practice-based intervention on influenza immunization rates and disparities in vaccination rates by race/ethnicity and insurance status. Methods l RCTl during 2003 -2004 testing patient tracking/recall/outreach and provider prompts on improving influenza immunization rates. l Patients aged > or = 65 years in six large inner-city primary care practices were randomly allocated to study or control group. l Influenza immunization coverage was measured prior to enrollment and on the end date. .

Clinical Decision Support for Providers: infectious diseases l l Reference l Humiston SG, et. al, Increasing inner-city adult influenza vaccination rates: a randomized controlled trial. Public Health Rep. 2011 Jul. Aug; 126 Suppl 2: 39 -47. Results l At study end, immunization rates were greater for the intervention group than for the control group (64% vs. 22%, p < 0. 0001). l When controlling for other factors, the intervention group was more than six times as likely to receive influenza vaccine. l The intervention was effective across gender, race/ ethnicity, age, and insurance subgroups. l Among the intervention group, 3. 5% of African Americans and 3. 2% of white people refused influenza immunization. .

Clinical Decision Support for Providers: infectious diseases l l l Reference l Humiston SG, et. al, Increasing inner-city adult influenza vaccination rates: a randomized controlled trial. Public Health Rep. 2011 Jul. Aug; 126 Suppl 2: 39 -47. Conclusions l Patient tracking/recall/outreach and provider prompts were intensive but successful approaches to increasing seasonal influenza immunization rates among inner-city seniors Importance l Few CDSS studies show 300% improvement over baseline (and 2/3 of all events in compliance) with preventive medicine best practices

Clinical Decision Support for Providers: infectious diseases l l Reference l Szilagyi PG, et. al, Effectiveness of a citywide patient immunization navigator program on improving adolescent immunizations and preventive care visit rates. Arch Pediatr Adolesc Med. 2011 Jun; 165(6): 547 -53. Source l Department of Pediatrics, University of Rochester School of Medicine and Dentistry, Rochester, NY. Aim l To assess the impact of a tiered patient immunization navigator intervention (immunization tracking, reminder/recall, and outreach) on improving immunization and preventive care visit rates in urban adolescents. Methods l Same informatics infrastructure as that used for inner city adults, applied to urban adolescents. l Immunization ‘navigators’ at each practice implemented a tiered protocol: immunization tracking, telephone or mail reminder/recall, and home visits if participants remained unimmunized or behind on preventive care visits

Clinical Decision Support for Providers: infectious diseases l l Reference l Szilagyi PG, et. al, Effectiveness of a citywide patient immunization navigator program on improving adolescent immunizations and preventive care visit rates. Arch Pediatr Adolesc Med. 2011 Jun; 165(6): 547 -53. Results l Intervention and control groups were similar at baseline for demographics (mean age, 13. 5 years; 63% black, 14% white, and 23% Hispanic adolescents; and 74% receiving Medicaid) l Immunization rates at the end of the study were 44. 7% for the intervention group and 32. 4% for the control group (adjusted risk ratio, 1. 4; 95% confidence interval, 1. 3 -1. 5) l Preventive care visit rates were 68. 0% for the intervention group and 55. 2% for the control group (1. 2; 1. 2 -1. 3). l Findings were similar across practices, sexes, ages, and insurance providers.

Clinical Decision Support for Providers: infectious diseases l l Reference l Szilagyi PG, et. al, Effectiveness of a citywide patient immunization navigator program on improving adolescent immunizations and preventive care visit rates. Arch Pediatr Adolesc Med. 2011 Jun; 165(6): 547 -53. Results, cont’d l The intervention cost was $3. 81 per adolescent per month l The cost per additional adolescent fully vaccinated was $465, and the cost per additional adolescent receiving a preventive care visit was $417.

Clinical Decision Support for Providers: infectious diseases l l l Reference l Szilagyi PG, et. al, Effectiveness of a citywide patient immunization navigator program on improving adolescent immunizations and preventive care visit rates. Arch Pediatr Adolesc Med. 2011 Jun; 165(6): 547 -53. Conclusions l A tiered tracking, reminder/recall, and outreach intervention improved immunization and preventive care visit rates in urban adolescents. Importance l Study presents cost-effectiveness data which relatively few CDSS studies do (but probably all should in the current healthcare environment)

Clinical Decision Support for Providers: infectious diseases l l Reference l Were MC, et. Al (including Tierney), Evaluation of computer-generated reminders to improve CD 4 laboratory monitoring in sub-Saharan Africa: a prospective comparative study. J Am Med Inform Assoc. 2011 Mar-Apr; 18(2): 150 -5. Epub 2011 Jan 20. Source l Indiana University School of Medicine, Indianapolis, IN. Aim l To test the hypothesis that clinical summaries with computergenerated reminders could improve clinicians' compliance with CD 4 testing guidelines in the resource-limited setting of sub-Saharan Africa. . Methods l A prospective comparative study of two randomly selected outpatient adult HIV clinics in western Kenya. l Printed summaries with reminders for overdue CD 4 tests were made available to clinicians in the intervention clinic but not in the control clinic.

Clinical Decision Support for Providers: infectious diseases l l l Reference l Were MC, et. al, Evaluation of computer-generated reminders to improve CD 4 laboratory monitoring in sub-Saharan Africa: a prospective comparative study. J Am Med Inform Assoc. 2011 Mar. Apr; 18(2): 150 -5. Epub 2011 Jan 20. Methods, cont’d l Changes in order rates for overdue CD 4 tests were compared between and within the two clinics. Results l The computerized reminder system identified 717 encounters (21%) with overdue CD 4 tests. l Analysis by study assignment (regardless of summaries being printed or not) revealed that with computer-generated reminders, CD 4 order rates were significantly higher in the intervention clinic compared to the control clinic (53% vs 38%, OR = 1. 80, CI 1. 34 to 2. 42, p < 0. 0001).

Clinical Decision Support for Providers: infectious diseases l l l Reference l Were MC, et. al, Evaluation of computer-generated reminders to improve CD 4 laboratory monitoring in sub-Saharan Africa: a prospective comparative study. J Am Med Inform Assoc. 2011 Mar. Apr; 18(2): 150 -5. Epub 2011 Jan 20. Methods, cont’d l Changes in order rates for overdue CD 4 tests were compared between and within the two clinics. Results l When comparison was restricted to encounters where summaries with reminders were printed, order rates in intervention clinic were even higher (63%). l The intervention clinic increased CD 4 ordering from 42% before reminders to 63% with reminders (50% increase, OR = 2. 32, CI 1. 67 to 3. 22, p < 0. 0001), compared to control clinic with only 8% increase from prestudy baseline (CI 0. 83 to 1. 46, p = 0. 51).

Clinical Decision Support for Providers: infectious diseases l l l Reference l Were MC, et. al, Evaluation of computer-generated reminders to improve CD 4 laboratory monitoring in sub-Saharan Africa: a prospective comparative study. J Am Med Inform Assoc. 2011 Mar. Apr; 18(2): 150 -5. Epub 2011 Jan 20. Conclusions l Clinical summaries with computer-generated reminders significantly improved clinician compliance with CD 4 testing guidelines in the resource-limited setting of sub-Saharan Africa. l This technology can have broad applicability to improve quality of HIV care in these settings. Importance l CDSS’s are not just for high tech healthcare settings

Clinical Decision Support for Providers: medication management l l Reference l Lapane KL, et. al, Effect of a pharmacist-led multicomponent intervention focusing on the medication monitoring phase to prevent potential adverse drug events in nursing homes. J Am Geriatr Soc. 2011 Jul; 59(7): 1238 -45. Source l Department of Epidemiology and Community Health, Virginia Commonwealth University, Richmond, VA. Aim l To determine the extent to which the use of a clinical informatics tool that implements prospective monitoring plans reduces the incidence of potential delirium, falls, hospitalizations potentially due to adverse drug events, and mortality. Methods l Randomized cluster trial in twenty-five nursing homes serviced by two long-term care pharmacies l Pharmacy automatically generated Geriatric Risk Assessment Med. Guide (GRAM) reports and automated monitoring plans for falls and delirium within 24 hours of admission or as part of the normal time frame of federally mandated drug regimen review.

Clinical Decision Support for Providers: medication management l l l Reference l Lapane KL, et. al, Effect of a pharmacist-led multicomponent intervention focusing on the medication monitoring phase to prevent potential adverse drug events in nursing homes. J Am Geriatr Soc. 2011 Jul; 59(7): 1238 -45. Methods, cont’d l Measured incidence of potential delirium, falls, hospitalizations potentially due to adverse drug events, and mortality. Results l Study included residents living in nursing homes during 2003 (1, 711 in 12 intervention; 1, 491 in 13 usual care) and 2004 (1, 769 in 12 intervention; 1, 552 in 13 usual care). l GRAM triggered monitoring plans for 491 residents. l Newly admitted residents in the intervention homes experienced a lower rate of potential delirium onset than those in usual care homes (adjusted hazard ratio (HR)=0. 42, overall hospitalization (adjusted HR=0. 89), and mortality (adjusted HR=0. 88).

Clinical Decision Support for Providers: medication management l l Reference l Lapane KL, et. al, Effect of a pharmacist-led multicomponent intervention focusing on the medication monitoring phase to prevent potential adverse drug events in nursing homes. J Am Geriatr Soc. 2011 Jul; 59(7): 1238 -45. Results, cont’d l In longer stay residents, the effects of the intervention were attenuated, and all estimates included unity. Conclusions l Using CDSS technology in long-term care pharmacies may reduce adverse effects associated with medication use. Importance l Systems approaches to care help in nursing homes also

Clinical Decision Support for Providers: medication management l l Reference l Bhardwaja B, et. al, Improving prescribing safety in patients with renal insufficiency in the ambulatory setting: the Drug Renal Alert Pharmacy (DRAP) program. Pharmacotherapy. 2011 Apr; 31(4): 346 -56. . Source l Pharmacy Department, Kaiser Permanente Colorado, Denver, CO. Aim l To determine whether a computerized Drug Renal Alert Pharmacy (DRAP) program could decrease the rate of medication errors in drug selection or dosing for 15 target drugs in patients with renal insufficiency. Methods l RCT involving a computerized too to alert pharmacists at the time of dispensing to possible errors in target drug selection and dosing for patients with renal insufficiency. l 15 target drugs identified based on frequency of use and risk of serious adverse events

Clinical Decision Support for Providers: medication management l l l Reference l Bhardwaja B, et. al, Improving prescribing safety in patients with renal insufficiency in the ambulatory setting: the Drug Renal Alert Pharmacy (DRAP) program. Pharmacotherapy. 2011 Apr; 31(4): 346 -56. Methods, cont’d l Primary outcome was the proportion of medication errors, defined as target drugs that should be avoided or were dosed inappropriately, in the intervention and usual care groups. . Results l Of eligibile 32, 917 patients, 6125 patients (3025 in the intervention group and 3100 in the usual care group) were prescribed at least one target drug and were included in the analysis. l No significant differences in baseline characteristics between groups. l Over the 15 -month intervention period, the proportion of medication errors was significantly lower in the intervention group than the usual care group (33% vs 49%, p<0. 001).

Clinical Decision Support for Providers: medication management l l Reference l Bhardwaja B, et. al, Improving prescribing safety in patients with renal insufficiency in the ambulatory setting: the Drug Renal Alert Pharmacy (DRAP) program. Pharmacotherapy. 2011 Apr; 31(4): 346 -56. Results, cont’d l After the study period, when the intervention was expanded to both groups, a 20% reduction in errors was sustained in the combined groups over the subsequent 7 months. Conclusions l The DRAP program was successful in reducing medication errors for patients with renal insufficiency in an ambulatory setting and was demonstrated to have sustainability after study completion. Importance l Good news: medication errors dropped from roughly half of patients to a third of patients l Bad news: a third of patients still had medication errors

Clinical Decision Support for Providers: nursing care l l Reference l Dykes PC, et. al, Fall prevention in acute care hospitals: a randomized trial. JAMA. 2010 Nov 3; 304(17): 1912 -8. . . Source l Brigham and Women's Hospital/Partners Health. Care System, Harvard Medical School, Boston, MA. Aim l To investigate whether a fall prevention tool kit (FPTK) using health information technology (HIT) decreases patient falls in hospitals. Methods l Cluster randomized study comparing patient fall rates in 4 urban US hospitals in units that received usual care (4 units and 5104 patients) or the intervention (4 units and 5160 patients) l The FPTK integrated existing communication and workflow patterns into the HIT application. l Based on a valid fall risk assessment scale completed by a nurse, the FPTK software tailored fall prevention interventions to address patients' specific determinants of fall risk. l FPTK produced bed posters composed of brief text with an accompanying icon, patient education handouts, and plans of care

Clinical Decision Support for Providers: nursing care l l l Reference l Dykes PC, et. al, Fall prevention in acute care hospitals: a randomized trial. JAMA. 2010 Nov 3; 304(17): 1912 -8. Methods, cont’d l The primary outcome was patient falls per 1000 patient-days adjusted for site and patient care unit. A secondary outcome was fall-related injuries. Results l During the 6 -month intervention period, the number of patients with falls differed between control (n = 87) and intervention (n = 67) units (P=. 02). l Site-adjusted fall rates were significantly higher in control units (4. 18 [95% confidence interval {CI}, 3. 45 -5. 06] per 1000 patient-days) than in intervention units (3. 15 [95% CI, 2. 54 -3. 90] per 1000 patient-days; P =. 04). .

Clinical Decision Support for Providers: nursing care l l Reference l Dykes PC, et. al, Fall prevention in acute care hospitals: a randomized trial. JAMA. 2010 Nov 3; 304(17): 1912 -8. Results, cont’d l FPTK was found to be particularly effective with patients aged 65 years or older (adjusted rate difference, 2. 08 [95% CI, 0. 61 -3. 56] per 1000 patient-days; P =. 003). l No significant effect was noted in fall-related injuries. Conclusions l The use of a fall prevention tool kit in hospital units compared with usual care significantly reduced rate of falls. Importance l Hybrid outputs from CDSS applications (e. g. , bed posters, Pt handouts, care plans) can be effective for common inpatient risks

Clinical Decision Support for Patients: cancer detection (4 RCTs) l References l Miller DP Jr, et. al, Effectiveness of a web-based colorectal cancer screening patient decision aid: a randomized controlled trial in a mixed-literacy population. Am J Prev Med. 2011 Jun; 40(6): 608 -15. [Wake Forest, Salem NC] l Hoffman RM, et. al, A system-based intervention to improve colorectal cancer screening uptake. Am J Manag Care. 2011 Jan; 17(1): 49 -55. [New Mexico VA] l Leffler DA, et. al, An alerting system improves adherence to follow -up recommendations from colonoscopy examinations. Gastroenterology. 2011 Apr; 140(4): 1166 -1173. e 1 -3. [Beth Israel Deaconess, Boston] l Cameron KA, et. al, Patient outreach to promote colorectal cancer screening among patients with an expired order for colonoscopy: a randomized controlled trial. Arch Intern Med. 2011 Apr 11; 171(7): 642 -6. [Northwestern U. , Chicago]. .

Clinical Decision Support for Patients: cancer detection (4 RCTs) l l Interventions l Wake Forest: web-based CRC educational tool viewed just before appointment. l New Mexico VA: mail fecal occult blood tests directly to patients based on EHR-derived criteria l Beth Israel Deaconess: use prior colonoscopy records to send reminder letters to PCPs and to patients, plus telephone call to Pts l Northwestern: EHR-derived cohort sent letter from PCP, brochure, colon cancer DVD, and follow-up phone call. Results l All interventions statistically significantly improved rates of colon cancer screening.

Clinical Decision Support for Patients: diabetes l l Reference l Lim S, et. al, Improved glycemic control without hypoglycemia in elderly diabetic patients using the ubiquitous healthcare service, a new medical information system. Diabetes Care. 2011 Feb; 34(2): 30813. . Source l Department of Medical Informatics, Seoul National University Bundang Hospital, Seongnam, Korea. Aim l To assess the effect of patient self monitoring and CDSS on quality and efficiency of care for elderly patients with type 2 diabetes. Methods l 6 -month randomized, controlled clinical trial involving 144 patients aged >60 years. l Participants were randomly assigned to receive routine care (control, n = 48), to the self-monitored blood glucose (SMBG, n = 47) group, or to the u-healthcare group (n = 49).

Clinical Decision Support for Patients: diabetes l l Reference l Lim S, et. al, Improved glycemic control without hypoglycemia in elderly diabetic patients using the ubiquitous healthcare service, a new medical information system. Diabetes Care. 2011 Feb; 34(2): 30813. . Methods, cont’d l U-healthcare system = medical instructions given through the patient's mobile phone. l Patients receive a glucometer with a public switched telephone network-connected cradle that automatically transfers test results to a hospital-based server. l Once the data are transferred to the server, an automated system, the CDSS rule engine, generates and sends patient-specific messages by mobile phone l The primary end point was the proportion of patients achieving A 1 C <7% without hypoglycemia at 6 months.

Clinical Decision Support for Patients: diabetes l l l Reference l Lim S, et. al, Improved glycemic control without hypoglycemia in elderly diabetic patients using the ubiquitous healthcare service, a new medical information system. Diabetes Care. 2011 Feb; 34(2): 30813. Results l After 6 months, mean A 1 C level was significantly decreased from 7. 8 ± 1. 3% to 7. 4 ± 1. 0% (P < 0. 001) in the u-healthcare group and from 7. 9 ± 1. 0% to 7. 7 ± 1. 0% (P = 0. 020) in the SMBG group, compared with 7. 9 ± 0. 8% to 7. 8 ± 1. 0% (P = 0. 274) in the control group. l The proportion of patients with A 1 C <7% without hypoglycemia was 30. 6% in the u-healthcare group, 23. 4% in the SMBG group (23. 4%), and 14. 0% in the control group (P < 0. 05). ). Conclusions l The CDSS-based u-healthcare service achieved better glycemic control with less hypoglycemia than SMBG and routine care and may provide effective and safe diabetes management in the elderly diabetic patients.

Clinical Decision Support for Patients: diabetes l l Reference l Lim S, et. al, Improved glycemic control without hypoglycemia in elderly diabetic patients using the ubiquitous healthcare service, a new medical information system. Diabetes Care. 2011 Feb; 34(2): 30813. Importance l Harbinger of a coming wave of intelligent cell phone apps for self care, enabled by physiologic monitors

Clinical Decision Support for Patients: Other conditions (4 RCTs) l References l Montori VM, et. al, Use of a decision aid to improve treatment decisions in osteoporosis: the osteoporosis choice randomized trial. Am J Med. 2011 Jun; 124(6): 549 -56. [Mayo Clinic] l Mouttapa M, et. al, The Personal Nutrition Planner: a 5 -week, computer-tailored intervention for women. J Nutr Educ Behav. 2011 May-Jun; 43(3): 165 -72. [Cal State, Fullerton] l Kelders SM, et. al, Effectiveness of a Web-based intervention aimed at healthy dietary and physical activity behavior: a randomized controlled trial about users and usage. J Med Internet Res. 2011 Apr 14; 13(2): e 32. [University of Twente, Netherlands] l Wright A, et al, Randomized Controlled Trial of Health Maintenance Reminders Provided Directly to Patients Through an Electronic PHR. J Gen Intern Med. 2011 Sep 9. [Brigham & Womens]

Clinical Decision Support for Patients: other (4 RCTs) l l Interventions l Mayo Clinic: Tailored pictographic 10 -year fracture risk estimate, absolute risk reduction with bisphonates, side effects, and out-ofpocket cost; control patients received a standard brochure. l Cal State Fullerton: web app producing individualized nutrition feedback based on initial on-line assessment. l Twente Univ: Healthy Weight Assistant (HWA), a Web-based intervention aimed at healthy dietary and physical activity behavior. l Brigham & Womens: Tethered PHR with ‘e-Journal’ providing health maintenance reminders Results l All interventions showed statistically significantly improved rates of desired outcomes

CDSS Unintended Consequences l l Reference l Nanji KC et. al, Errors associated with outpatient computerized prescribing systems. J Am Med Inform. Assoc. 2001 Jun 29. Source l Department of Anesthesia, Critical Care and Pain Medicine, Massachusetts General Hospital, Boston, MA Aims l To report the frequency, types, and causes of errors associated with outpatient computer-generated prescriptions l To develop a framework to classify these errors to determine which strategies have greatest potential for preventing them. Methods l Retrospective cohort study of 3850 computer-generated prescriptions received by a commercial outpatient pharmacy chain across three states over 4 weeks in 2008. l Clinician panel reviewed the prescriptions to identify and classify medication errors.

CDSS Unintended Consequences l l l Reference l Nanji KC et. al, Errors associated with outpatient computerized prescribing systems. J Am Med Inform. Assoc. 2001 Jun 29. Methods, cont’d l Primary outcomes were the incidence of medication errors; potential adverse drug events, defined as errors with potential for harm; and rate of prescribing errors by error type and by prescribing system. Results l Of 3850 prescriptions, 452 (11. 7%) contained 466 total errors, of which 163 (35. 0%) were considered potential adverse drug events. l Error rates varied by computerized prescribing system, from 5. 1% to 37. 5%. The most common error was omitted information (60. 7% of all errors). l Results consistent with literature on manual handwritten prescription error rates. The number, type, and severity of errors varied by computerized prescribing system, suggesting that some systems may be better at preventing errors than others.

CDSS Unintended Consequences l l l Reference l Nanji KC et. al, Errors associated with outpatient computerized prescribing systems. J Am Med Inform. Assoc. 2001 Jun 29. Conclusions l Implementing a computerized prescribing system without comprehensive functionality and processes in place to ensure meaningful system use does not decrease medication errors. l The authors offer targeted recommendations on improving computerized prescribing systems to prevent errors Importance l Technology must be well designed and thoughtfully implemented to get intended effects l The persistent tendency of media and opponents of technology to draw conclusions that technology is not as good as manual alternatives is a continuing challenge for those who design and implement such systems

6 New CDSS RCTs showing no difference for intervention vs. control 1. 2. 3. 4. 5. 6. Linder JA, et. al, Electronic health record feedback to improve antibiotic prescribing for acute respiratory infections. Am J Manag Care. 2010 Dec; 16(12 Suppl HIT): e 311 -9. [Brigham & Womens, Boston] Sequist TD, et. al, Electronic patient messages to promote colorectal cancer screening: a randomized controlled trial. Arch Intern Med. 2011 Apr 11; 171(7): 636 -41. Epub 2010 Dec 13. . [Brigham & Womens, Boston] Eisenstein EL, et. al, Clinical and economic results from a randomized trial of clinical decision support in a rural health network. Stud Health Technol Inform. 2011; 164: 77 -81. [Univ. Washington, Seattle] Chung MH, et. al, A randomized controlled trial comparing the effects of counseling and alarm device on HAART adherence and virologic outcomes. P Lo. S Med. 2011 Mar; 8. [Univ. Washington, Seattle] Gill JM, et. al, Impact of EHR-based clinical decision support on adherence to guidelines for patients on NSAIDs: a randomized controlled trial. Ann Fam Med. 2011 Jan-Feb; 9(1): 22 -30. [Delaware Valley] Pellegrino VA, et. al, Computer based haemodynamic guidance system is effective and safe in management of postoperative cardiac surgery patients. Anaesth Intensive Care. 2011 Mar; 39(2): 191 -201. [Alfred Hospital, Melbourne]

Clinical Decision Support for Providers and Patients Questions and Comments

Telemedicine 14 new RCTs published November 2010 – October 2011 • 6 cardiovascular diseases • 3 diabetes • 2 infectious diseases • 1 each: depression, multiple sclerosis, cancer care

Telemedicine – cardiovascular diseases 3 RCTs l References l Crossley GH, et. al, The CONNECT (Clinical Evaluation of Remote Notification to Reduce Time to Clinical Decision) trial: the value of wireless remote monitoring with automatic clinician alerts. J Am Coll Cardiol. 2011 Mar 8; 57(10): 1181 -9. [Univ Tennessee Coll Med] l Christensen H, et. al, Home management of oral anticoagulation via telemedicine versus conventional hospital-based treatment. Telemed J E Health. 2011 Apr; 17(3): 169 -76. Epub 2011 Jan 23. [Univ Health Network, Toronto] l Nolan RP, et. al, Therapeutic benefit of preventive telehealth counseling in the Community Outreach Heart Health and Risk Reduction Trial. Am J Cardiol. 2011 Mar 1; 107(5): 690 -6. Epub 2011 Jan 6.

Telemedicine – cardiovascular diseases l Interventions l Univ Tenn: Implantable cardioverter-defibrillators with wireless remote monitoring connect to automated clinician alerts. l l l Denmark: Home INR monitoring of oral anticoagulant therapy combined with web-based expert system dose advisor Toronto: Telehealth lifestyle counseling via online group videoconferencing Results l All interventions yielded statistically significant increases in desired outcome variables relative to control groups.

Telemedicine – diabetes (3 RCTs) l References 1. Wakefield BJ, et. al, Effectiveness of home telehealth in comorbid diabetes and hypertension: a randomized, controlled trial. Telemed J E Health. 2011 May; 17(4): 254 -61. [Univ Iowa] 2. Weinstock RS, et. al, Glycemic control and health disparities in older ethnically diverse underserved adults with diabetes: five -year results from the Informatics for Diabetes Education and Telemedicine (IDEATel) study. Diabetes Care. 2011 Feb; 34(2): 274 -9. [SUNY upstate] 3. van Bastelaar KM, et. al, Web-based depression treatment for type 1 and type 2 diabetic patients: a randomized, controlled trial. Diabetes Care. 2011 Feb; 34(2): 320 -5. Epub 2011 Jan 7. 4. [VU Univ Med Ctr, Netherlands]

Telemedicine - diabetes l Interventions l l Univ Iowa: nurse-managed home telehealth device w/ standard telephone line for BP and BG data transmission between the patient’s home and the study center. SUNY/IDEATel: upload BG data and receive ‘home visits’ via video Netherlands: Internet-delivered Cognitive Behavioral Therapy for diabetics with depression. Results l l Statistically significant decreases in Hb. A 1 C levels for studies focused on blood glucose control Reduction in depressive symptoms in the CBT trials

Telemedicine – infectious diseases l References l Pop-Eleches C, et. al, Mobile phone technologies improve adherence to antiretroviral treatment in a resource-limited setting: a randomized controlled trial of text message reminders. AIDS. 2011 Mar 27; 25(6): 825 -34. [Columbia Univ] l Yardley L, et. al, Evaluation of a Web-based intervention providing tailored advice for self-management of minor respiratory symptoms: exploratory randomized controlled trial. J Med Internet Res. 2010 Dec 15; 12(4): e 66. [Univ. Southhampton, UK]

Telemedicine – infectious diseases l Interventions l l l Columbia Univ: SMS text messages to cell phones of HIV patients in sub-Saharan Africa reminding them to take ARV meds. Univ Southampton: “Internet Doctor” providing tailored advice on self management of minor URIs. Results l SMS weekly text messages improved ARV compliance l Improved understanding of illness and decreased clinic visits among persons with URIs.

4 New Telemedicine RCTs showing no difference for intervention vs. control 1. Koehler F, et. al, Impact of remote telemedical management on mortality and hospitalizations in ambulatory patients with chronic heart failure: the telemedical interventional monitoring in heart failure study. Circulation. 2011 May 3; 123(17): 1873 -80. [Cardiovascular Center, Berlin] 2. Konstam V, et. al, Health-related quality of life in a multicenter randomized controlled comparison of telephonic disease management and automated home monitoring in patients recently hospitalized with heart failure: SPAN-CHF II trial. J Card Fail. 2011 Feb; 17(2): 151 -7. [Univ. Massachusetts] 3. Madsen LB, et. al, Economic evaluation of home blood pressure telemonitoring: a randomized controlled trial. Blood Press. 2011 Apr; 20(2): 117 -25. Epub 2010 Nov 24. [Aarhus Univ. , Denmark]

4 New Telemedicine RCTs showing no difference for intervention vs. control 4. Miller DM, et. al, Web-based self-management for patients with multiple sclerosis: a practical, randomized trial. Telemed J E Health. 2011 Jan. Feb; 17(1): 5 -13. [Cleveland Clinic]

Telemedicine Questions and Comments

Practice of Informatics

Practice of Informatics: issues related to EHR adoption (5 articles) l References 1. Linder JA et. al, Clinician characteristics and use of novel electronic health record functionality in primary care. J Am Med Inform Assoc. 2011 Sep 7. [Brigham & Womens] Key finding: contrary to conventional wisdom, busy clinicians with complex patients are more likely to use new EHR functionality than peers who are less busy 2. Wilcox AB, Chen YH, Hripcsak G. Minimizing electronic health record patient-note mismatches. J Am Med Inform Assoc. 2011 Jul-Aug; 18(4): 511 -4. [Columbia Univ. ] Key finding: wrong patient notes in EHRs occur at frequency of about 0. 5% (1 in 200) but can be reduced to 1: 300 by pop-up alerting.

Practice of Informatics: issues related to EHR adoption (5 articles) l References 3. Adler-Milstein J, Bates DW, Jha AK. A survey of health information exchange organizations in the United States: implications for meaningful use. Ann Intern Med 2011; 154(10): 666 -671. [Brigham & Womens] Key findings: Only 13 of 75 operational RHIOs supported stage 1 meaningful use (covering 3% of hospitals and 0. 9% of practices), and none met an expert-derived definition of a comprehensive RHIO. Overall, 50 of 75 RHIOs (67%) did not meet the criteria for financial viability. 4. Sittig DF, Singh H. Defining health information technologyrelated errors: new developments since to err is human. Arch Intern Med. 2011 Jul 25; 171(14): 1281 -4. [Univ Texas Houston] Key findings: definitions of types of HIT-related errors and a sociotechnical approach to understand causes of errors

Practice of Informatics: issues related to EHR adoption (5 articles) l References 5. Goodman KW et. al, Challenges in ethics, safety, best practices, and oversight regarding HIT vendors, their customers, and patients: a report of an AMIA special task force. Journal of the American Medical Informatics Association 2011; 18(1): 77 -81. [Univ. Miami] Key findings: patient safety trumps corporate liability and IP concerns. Transparency and standards of corporate conduct needed. Institutions should provide ethics education to purchasers and users.

Practice of Informatics: clinical data mining l References l Tatonetti, NP et. al, Detecting drug interactions from adverseevent reports: interaction between paroxetine and pravastatin increases blood glucose levels. Clinical Pharmacology & Therapeutics, 90(1), 133– 142. doi: 10. 1038/clpt. 2011. 83 [Stanford, Harvard, Vanderbilt] l Holmes AB, et. al, Discovering disease associations by integrating electronic clinical data and medical literature. PLo. S One. 2011; 6(6): e 21132. Epub 2011 Jun 23. [Columbia Univ]

Practice of Informatics l l Methods l Stanford: Look for glycemic effects in FDA Adverse Event database, find higher than expected BG with co-administration of two drugs, then verified observed associations by data mining 3 institution-wide EMR data warehouses. l Columbia: NLP + statistical approach to finding co-morbidities of rare diseases (Kaposi sarcoma, toxoplasmosis, Kawasaki disease) from data mining of literature (Pub. Med + Wikipedia) combined with local EHR data. Results l Stanford-Harvard-Vanderbilt consortium found unique paroxetine + pravastatin induced hyperglycemia not associated with either drug administered alone. l Columbia found new association between Kawasaki disease and autism. l Approaches published and available for use by others.

Practice of Informatics l l l References l Jameson E, et. al, Electronic gaming as pain distraction. Pain Res Manag. 2011 Jan-Feb; 16(1): 27 -32. Source l Department of Psychological Medicine, Dunedin School of Medicine, Dunedin, New Zealand. Methods l 60 participants were asked to submerge their hand in cold (2°C) water for as long as they could tolerate. l They did this with no distraction, and then with active (electronic gaming system) and passive (television) distraction, in randomly assigned order. l Tolerance time, pain intensity ratings and task absorption ratings were measured for each condition. .

Practice of Informatics l l l References l Jameson E, et. al, Electronic gaming as pain distraction. Pain Res Manag. 2011 Jan-Feb; 16(1): 27 -32. Results l Participants in both experiments had a significantly higher pain tolerance and reported less pain with the active distraction compared with passive or no distraction. l They also had more enjoyment, less anxiety and greater reduction in pain with active distraction. l These experiments offer further support for the use of electronic games as a method of pain control. . Importance l More evidence explaining why your kids ignore you while playing video games

Practice of Informatics l l Reference l Müller BH, et. al, One-session computer-based exposure treatment for spider-fearful individuals--efficacy of a minimal self-help intervention in a randomised controlled trial. J Behav Ther Exp Psychiatry. 2011 Jun; 42(2): 179 -84. Source l Department of Clinical Psychology and Psychotherapy, University of Basel, Missionsstrasse 60/62, CH-4055 Basel, Switzerland. Aim l To investigate the efficacy of one-session computer-based exposure (CBE) as a self-help treatment for spider-fearful individuals. . Methods l Spider-fearful participants in a CBE group underwent one 27 -min session of standardised exposure to nine fear-eliciting spider pictures l Treatment outcome was compared to spider-fearful control participants exposed to nine neutral pictures. l Fear reduction was quantified on a subjective level by the Fear of Spiders Questionnaire (FSQ) and complemented with a behavioural approach test (BAT). .

Practice of Informatics l l l Reference l Müller BH, et. al, One-session computer-based exposure treatment for spider-fearful individuals --efficacy of a minimal self-help intervention in a randomised controlled trial. J Behav Ther Exp Psychiatry. 2011 Jun; 42(2): 179 -84. Epub 2010 Dec 14. Results l Compared to control participants, CBE participants showed greater fear reduction from pre- to posttreatment on both the subjective level (FSQ) and the behavioural level (BAT). l Moreover, in contrast to the control group, the obtained subjective fear reduction effect remained stable in the CBE group at 1 -month followup. l These findings highlight the role of computer-based self-help as a minimal but effective intervention to reduce fear of spiders. . Importance l Self evident ; -).

Practice of Informatics Questions and Comments

New Literature Highlights: Bioinformatics and Computational Biology Human Health and Disease l The practice of bioinformatics l

Bioinformatics: Human Health & Disease – cancer l References l Tiacci E, et. al, BRAF mutations in hairy-cell leukemia. N Engl J Med. 2011 Jun 16; 364(24): 2305 -15. Epub 2011 Jun 11. [Univ. Perugia, Italy] Key findings: Whole exome sequencing of 47 patients found a specific mutation (BRAF V 600 E) that is pathognomonic and causal for the disease. l Pasqualucci L et al. Analysis of the coding genome of diffuse large B-cell lymphoma. Nat Genet. 2011 Jul 31; 43(9): 830 -7. doi: 10. 1038/ng. 892. [Columbia Univ. ] Key findings: Average non. Hodgkins lymphoma case has 30 expressed clonal gene alterations, few in common across cases.

Bioinformatics: Human Health & Disease – cancer l References l Chang HH, et. al, A transcriptional network signature characterizes lung cancer subtypes. Cancer. 2011 Jan 15; 117(2): 353 -60. doi: 10. 1002/cncr. 25592. [Harvard-MIT informatics] Key findings: developed a classifier based on gene expression profiles of 111 lung cancer specimens that distinguishes Adenocarcinoma from Squamous Cell Carcinoma and points to 3 genes that are responsible. (Last work of Marco Ramoni) l Kamper P, et. al, Proteomic analysis identifies galectin-1 as a predictive biomarker for relapsed/refractory disease in classical Hodgkin lymphoma. Blood. 2011 Jun 16; 117(24): 663849. Epub 2011 Apr 19. Key findings: Proteomic analysis of 14 Hodgkins lymphoma found a common protein biomarker that predicts treatment response and survival

Bioinformatics: Human Health & Disease – cancer l References l Stein RA, et. al, Epigenetics--the link between infectious diseases and cancer. JAMA. 2011 Apr 13; 305(14): 1484 -5. A good review of the relationship of the microbiome and cancer in humans.

Bioinformatics: Human Health & Disease – CNS l References l Gilman SR et. al, Rare de novo variants associated wih autism implicate a large functional network of genes involved in formation and function of synapses. Neuron. 2011 Jun 9; 70(5): 898 -907. [Columbia Univ. ] Key findings: Used analysis of rare genetic variants to show autism linked to synapse development, and explain why autism is more common in males than females. l Föcking M, et. al, Common proteomic changes in the hippocampus in schizophrenia and bipolar disorder and particular evidence for involvement of cornu ammonis regions 2 and 3. Arch Gen Psychiatry. 2011 May; 68(5): 477 -88. [Royal College of Surgeons, Dublin Ireland] Key findings: Used proteomics to find distinctive abnormal proteins in the hippocampus in schizophrenia and bipolar disorder.

The Practice of Bioinformatics l Reference l Altman RB, et. al, Pharmacogenomics: "noninferiority" is sufficient for initial implementation. Clin Pharmacol Ther. 2011 Mar; 89(3): 348 -50. [Stanford Univ. ] Key findings: because of the combinatorics of rare variants predict that conclusive evidence of gene-drug effects will often not be found with the certainty levels used in clinical trials, standard for using pharmacogenetic data should be whether it is no worse than standard prescribing.

Computational Biology and Bioinformatics Questions and Comments

Top Five List of Notable Events in the Past 12 months

“Top Five” Events 5. Total population of planet earth passes 7 billion

“Top Five” Events 5. Total population of planet earth passes 7 billion 4. December 10, 2010. Release of PCAST Health Information Technology Report


“Top Five” Events 5. Total population of planet earth passes 7 billion 4. December 10, 2010. Release of PCAST Health Information Technology Report 3. National Library of Medicine 175 th Anniversary

“Top Five” Events 5. Total population of planet earth passes 7 billion 4. December 10, 2010. Release of PCAST Health Information Technology Report 3. National Library of Medicine 175 th Anniversary 2. May 2011. First payments for EHR Meaningful Use


And the #1 top event of 2010 is…

“Top Five” Events 5. Total population of planet earth passes 7 billion 4. December 10, 2010. Release of PCAST Health Information Technology Report 3. National Library of Medicine 175 th Anniversary 2. May 2011. First payments for EHR Meaningful Use 1. September 2011. American Board of Medical Specialties approves Certification in Clinical Informatics
Content for this session is at: http: //faculty. washington. edu/dmasys/Year. In. Review including citation lists and links and this Power. Point
7501988ce8da78d2dd30b31967cdd405.ppt