7919a5f1fb4a7e88015a1ab4492aa943.ppt
- Количество слайдов: 52

Biology of Ticks and Mites L. Hannah Gould, MS, Ph. D Bacterial Diseases Branch Division of Vector-Borne Infectious Diseases Centers for Disease Control and Prevention Fort Collins, CO

Overview • Ticks, mites, and their identification • Tick-borne diseases in the United States – – – Lyme disease Rocky Mountain Spotted Fever Ehrlichiosis Babesiosis Tularemia Tick-borne relapsing fever • Mites

Ticks, mites, and their identification

Ticks and Mites • Not insects • Four life stages – – Egg Larva (6 legs) Nymph (8 legs) Adult (8 legs) • Ticks: ≈ 80 species in US, 12 of public health/veterinary importance • Mites: 45, 000 described species!

Ixodes scapularis • Blacklegged tick, deer tick • Transmits Lyme disease, babesiosis, ehrlichiosis • Found on eastern and north central United States • Feed on wide variety of mammals and birds

Dermacentor variabilis and D. andersoni • Dog tick, wood tick • Vector of Rocky mountain spotted fever, tularemia • Widely distributed, common • Adults feed on dogs, other medium to large mammals; larvae/nymphs feed on small rodents

Amblyomma americanum • Lone star tick • Vector of human monocytic ehrlichiosis, STARI • Widely distributed in southeastern US, Atlantic Coast • Wide host range

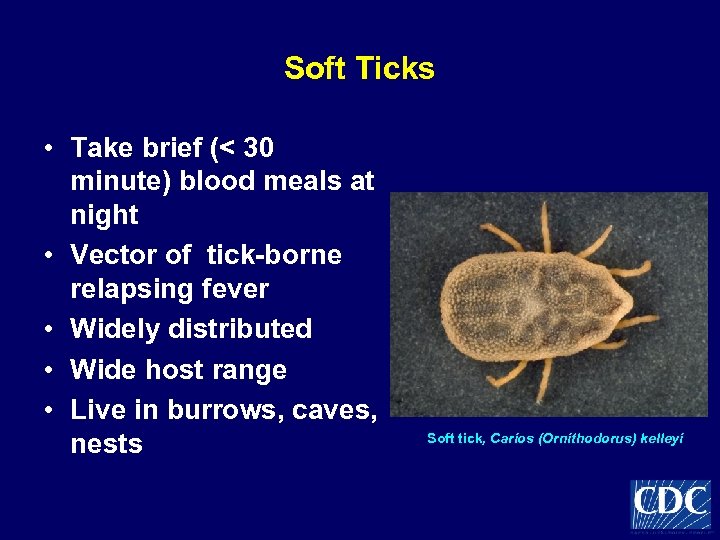
Soft Ticks • Take brief (< 30 minute) blood meals at night • Vector of tick-borne relapsing fever • Widely distributed • Wide host range • Live in burrows, caves, nests Soft tick, Carios (Ornithodorus) kelleyi

Other ticks of public health importance Scientific Name Ixodes pacificus Common Name Western blacklegged tick Notes Lyme disease Ixodes cookei Woodchuck tick Powassan virus Rhipicephalus sanguineus Dermacentor albipictus Brown dog tick Tick infestations Winter tick Large animals; hunters

Tick-borne Diseases in the US
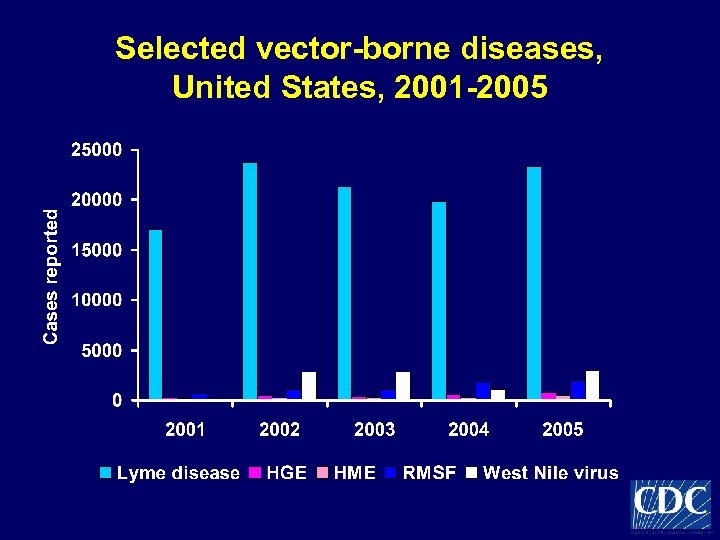
Selected vector-borne diseases, United States, 2001 -2005

Lyme Disease • Identified in 1976 • Caused by Borrelia burgdorferi • Transmitted by Ixodes scapularis and I. pacificus ticks • Reservoirs include small mammals and birds • Deer enhance tick populations, not a reservoir
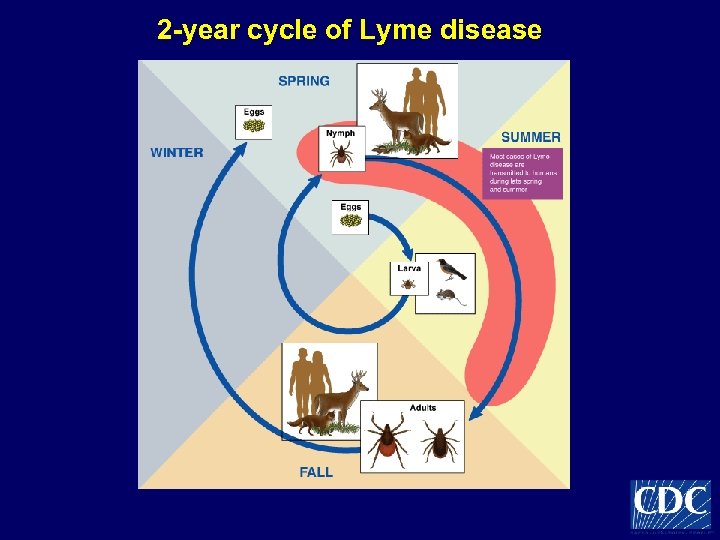
2 -year cycle of Lyme disease
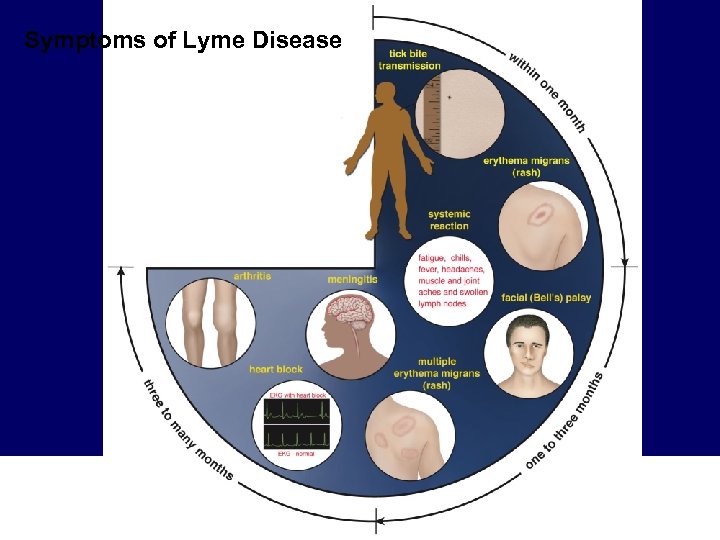
Symptoms of Lyme Disease
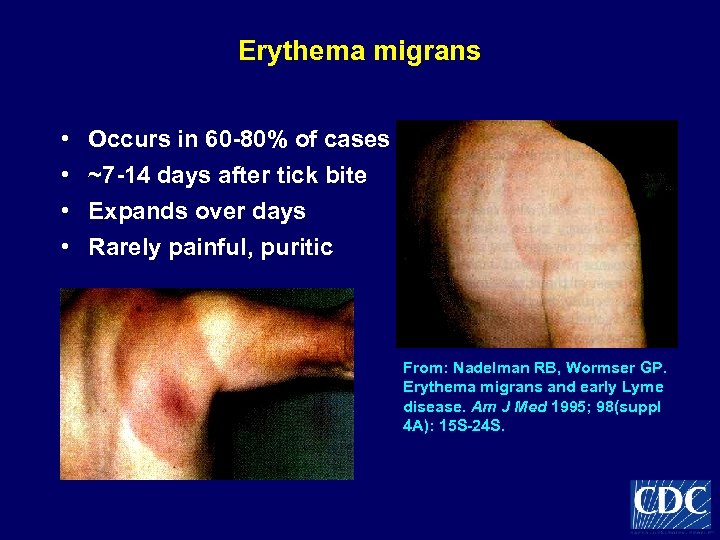
Erythema migrans • • Occurs in 60 -80% of cases ~7 -14 days after tick bite Expands over days Rarely painful, puritic From: Nadelman RB, Wormser GP. Erythema migrans and early Lyme disease. Am J Med 1995; 98(suppl 4 A): 15 S-24 S.
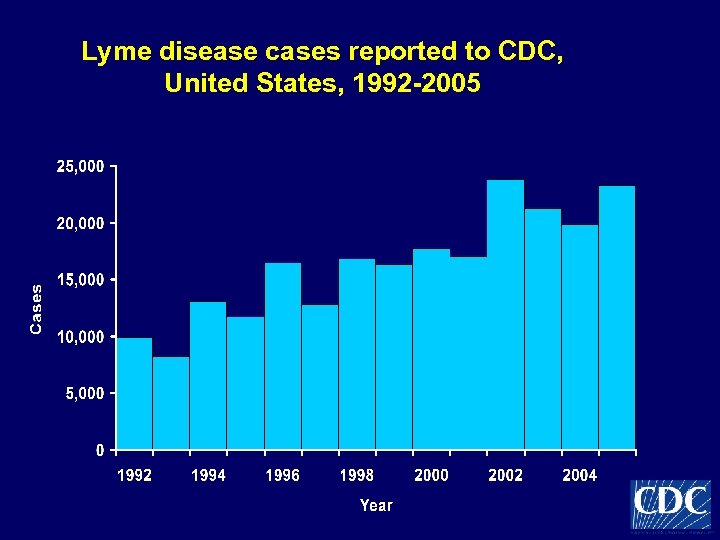
Lyme disease cases reported to CDC, United States, 1992 -2005
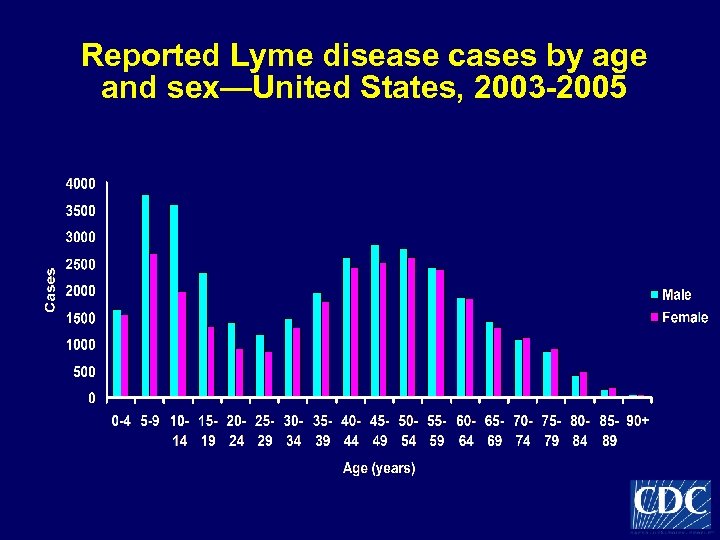
Reported Lyme disease cases by age and sex—United States, 2003 -2005
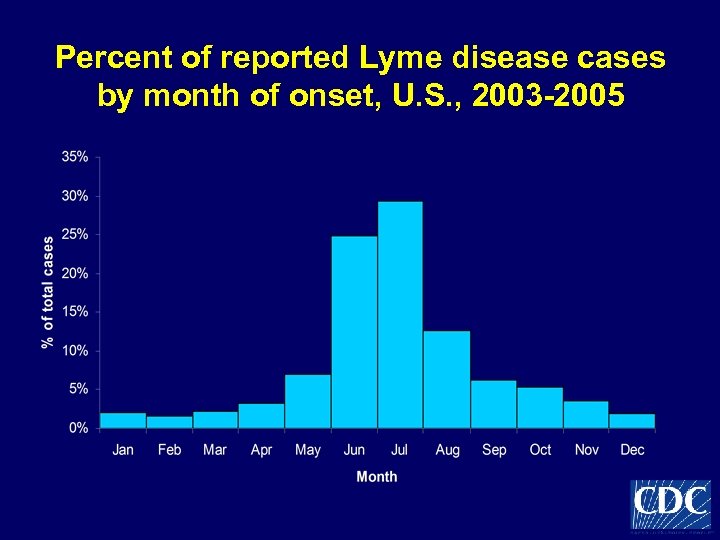
Percent of reported Lyme disease cases by month of onset, U. S. , 2003 -2005
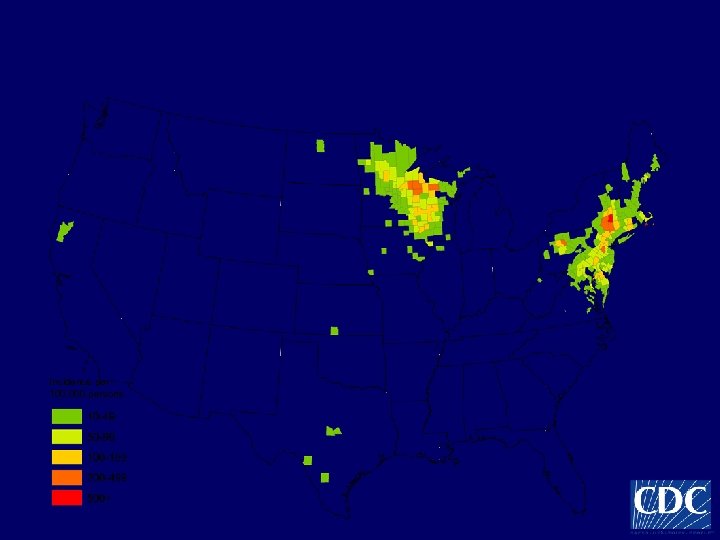
Reported Lyme disease incidence by county of residence—United States, 2005 Incidence per 100, 000 persons
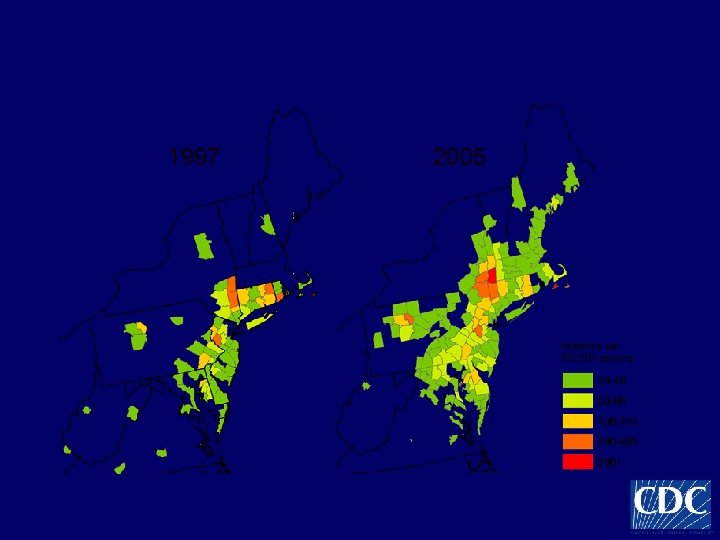
Lyme disease high incidence counties, Northeastern United States 1997 2005 Incidence per 100, 000 persons
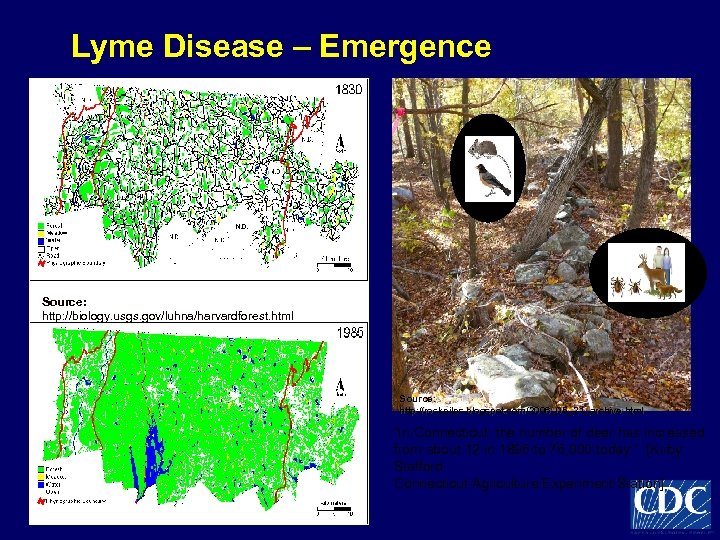
Lyme Disease – Emergence Source: http: //biology. usgs. gov/luhna/harvardforest. html Source: http: //rockpiles. blogspot. com/2006_05_21_archive. html “In Connecticut, the number of deer has increased from about 12 in 1896 to 76, 000 today. ” [Kirby Stafford Connecticut Agriculture Experiment Station]
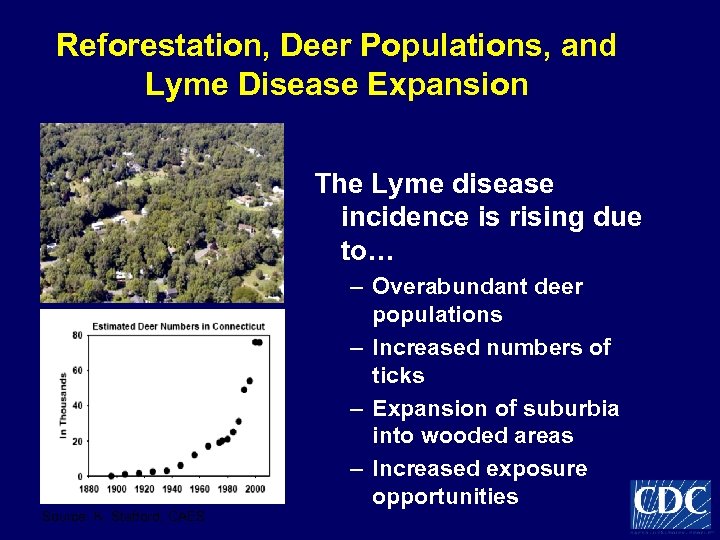
Reforestation, Deer Populations, and Lyme Disease Expansion The Lyme disease incidence is rising due to… Source: K. Stafford, CAES – Overabundant deer populations – Increased numbers of ticks – Expansion of suburbia into wooded areas – Increased exposure opportunities

Southern Tick-associated Rash Illness (STARI) • Causes rash similar to that of Lyme disease • Transmitted by Amblyomma americanum • Southeastern and south-central United States Photo: Wormser et al CID 2005

Rocky Mountain Spotted Fever (RMSF) • Caused by Rickettsia rickettsii • Transmitted most commonly by Dermacentor variabilis and D. andersoni • 250 -1200 cases/year in United States
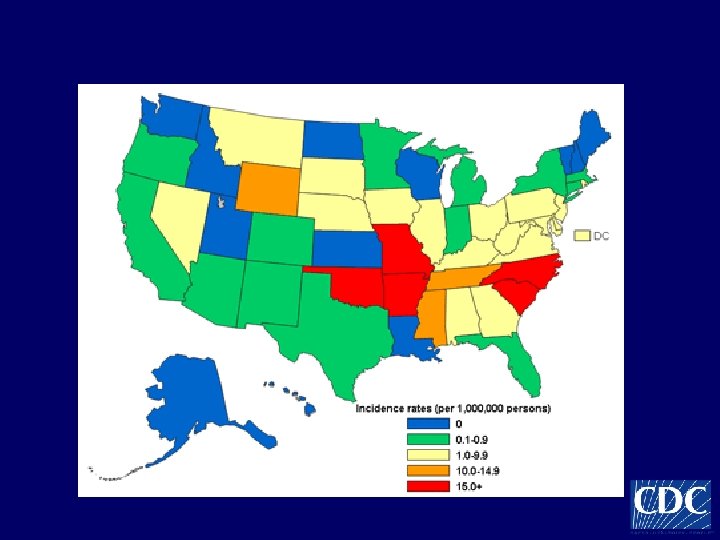
Incidence of RMSF in the United States
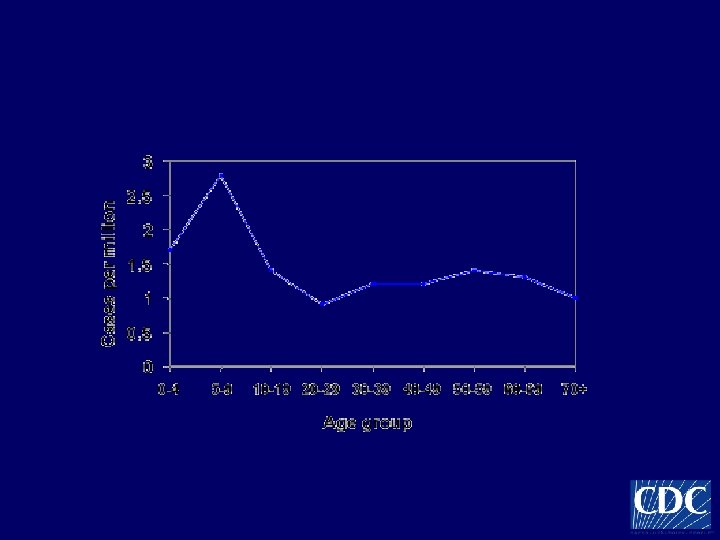
Age distribution of RMSF in the United States
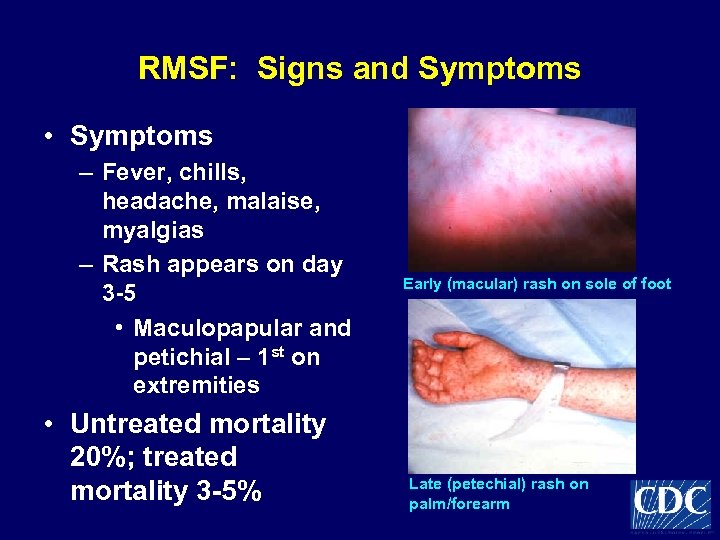
RMSF: Signs and Symptoms • Symptoms – Fever, chills, headache, malaise, myalgias – Rash appears on day 3 -5 • Maculopapular and petichial – 1 st on extremities • Untreated mortality 20%; treated mortality 3 -5% Early (macular) rash on sole of foot Late (petechial) rash on palm/forearm

Ehrlichiosis (Anaplasmosis) Ehrlichia chaffeensis (Human Monocytic Ehrlichiosis) – Transmitted by Amblyomma americanum – Southeastern and south central United States E. ewingii – Rare, immunosuppressed patients – Few cases in central United States E. phagocytophila (Human Granulocytic Ehrlichiosis) – Approximately 1200 cases per year in United States – Northeast, upper mid-Western United States – Transmitted by Ixodes scapularis and I. pacificus

Ehrlichiosis (Anaplasmosis) • Ehrlichia chaffeensis (Human Monocytic Ehrlichiosis, HME) – Transmitted by Amblyomma americanum – Southeastern and south central United States • E. phagocytophila (Human Granulocytic Ehrlichiosis, HGE) – Approximately 1200 cases per year in United States – Northeast, upper mid-Western United States – Transmitted by Ixodes scapularis and I. pacificus • E. ewingii – Rare, immunosuppressed patients – Few cases in central United States
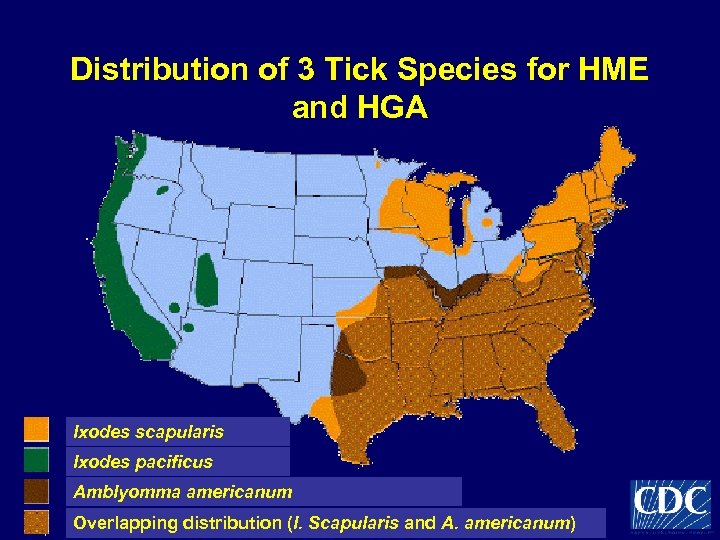
Distribution of 3 Tick Species for HME and HGA Ixodes scapularis Ixodes pacificus Amblyomma americanum Overlapping distribution (I. Scapularis and A. americanum)
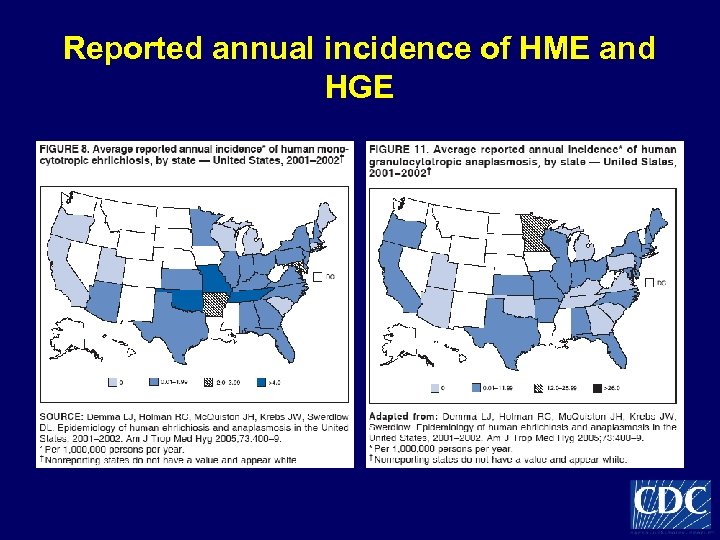
Reported annual incidence of HME and HGE

Clinical Presentation of Human Ehrlichioses Signs and symptoms Severe clinical spectrum • • • Disseminated intravascular coagulation • Pancytopenia • Encephalitis • Meningitis • Pulmonary Infiltrates • Gastrointestinal bleeding • Respiratory failure • Renal failure • Fatalities Fever Malaise Headache Myalgia/Arthralgia Anorexia Chills/Sweating Nausea/Vomiting Rash Cough Diarrhea Abdominal pain

Babesiosis • • • Caused by Babesia microti Transmitted by Ixodes scapularis Reservoir in white-footed mice Northeastern and mid-Western US Rare, few cases each year Clinically more severe in immunocompromised and elderly

Tularemia • Caused by bacterium, Franciscella tularensis • Transmitted by: – Tick (Dermacentor variabils, D. andersoni, Ambloymma americanum) or deerfly bite – handling infected sick or dead animals – eating or drinking contaminated food or water – inhaling airborne bacteria • 200 cases per year in United States • Most cases in south-central and western United States • Symptoms dependent on the route of infection

Tick-borne Relapsing Fever (TBRF) • Caused by Borrelia hermsii, B. parkeri, B. turicatae • Transmitted by Ornithodoros spp. soft ticks • Ticks feed quickly and painlessly at night • Rodents are primary reservoirs • Sporadic cases in the western U. S. (~25/year) • Associated with rustic cabins, high altitude • Recurrent fevers
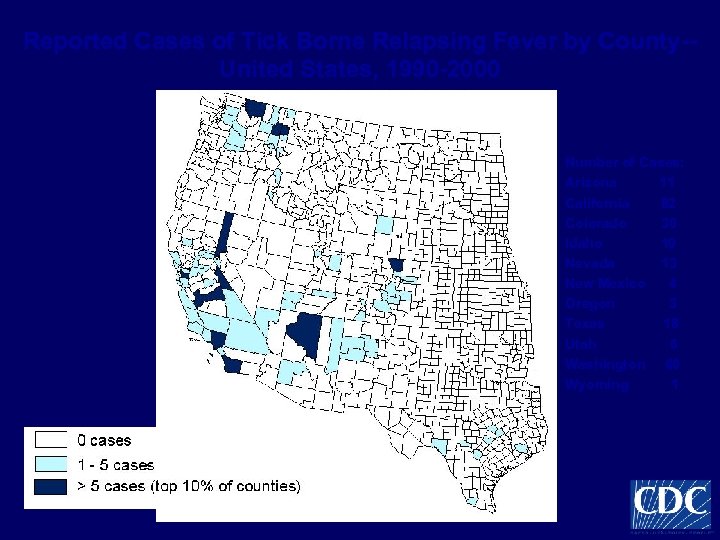
Reported Cases of Tick Borne Relapsing Fever by County-United States, 1990 -2000 Number of Cases: Arizona 11 California 82 Colorado 30 Idaho 19 Nevada 13 New Mexico 4 Oregon 3 Texas 18 Utah 6 Washington 60 Wyoming 1

Tick Paralysis • Caused by toxin produced by Dermacentor ticks • Acute, ascending, flaccid paralysis • Reversed upon removal of tick • May result in death if tick is not removed • More frequent in young girls
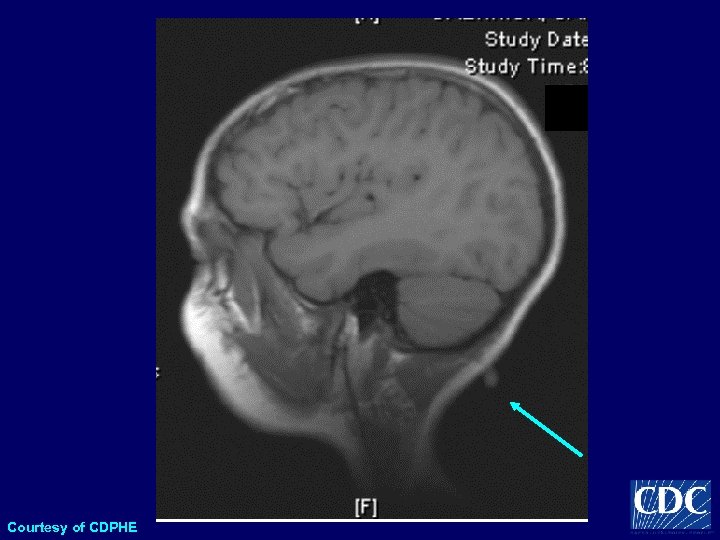
Courtesy of CDPHE

Treatment of tick-borne diseases Disease Antibiotic Lyme disease STARI Rocky Mountain Spotted Fever Babesiosis Tetracyclines, penicillins Ehrlichiosis Tularemia Tick-borne Relapsing Fever Doxycycline several Tetracyclines, erythromycin Doxycycline Clindamycin + quinine sulfate /azithromycin + atovaquone

Tick Testing and Tick Bite Prophylaxis • Neither generally recommended following tick bites • For Lyme disease, tick bite prophylaxis (single 200 mg dose doxycycline) recommended only when: – – Tick reliably identified and attached for ≥ 36 hours Can be started w/in 24 hours Infection rate ≥ 20% Doxycycline not contraindicated • Always monitor site of tick bite and health closely following a tick bite
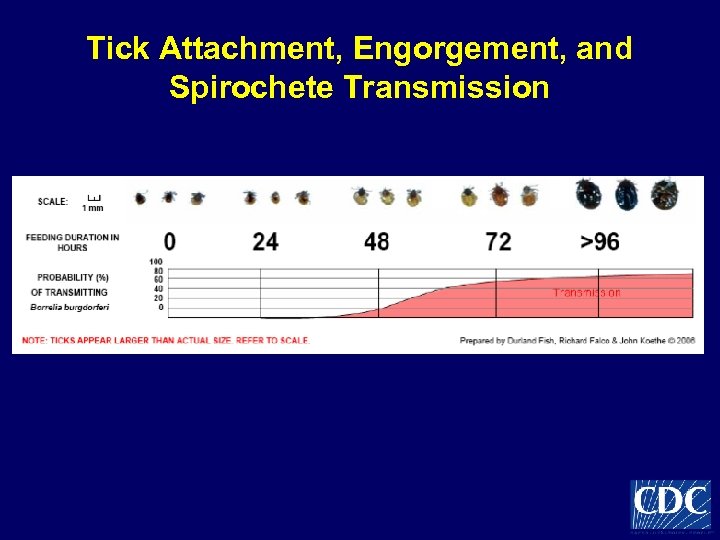
Tick Attachment, Engorgement, and Spirochete Transmission

Vaccination against tick-borne diseases • Vaccine for Lyme disease removed from market in 2002 • Vaccines not available for other tick-borne diseases

Proper Tick Removal • Use fine-tipped tweezers to grasp tick close to skin • Pull tick’s body away from skin (avoid crushing head) • Clean skin with soap and water • Properly dispose of tick DON’T: use petroleum jelly, a hot match, nail polish, or other products to remove a tick.

Mites

Family Trombiculidae: Chiggers • Eastern US; most common in southern states • Larvae attach to skin for 4 -6 days • Cause intense itching and dermatitis • Chigger mites can vector scrub typhus http: //mdc. mo. gov/nathis/arthopo/chiggers/
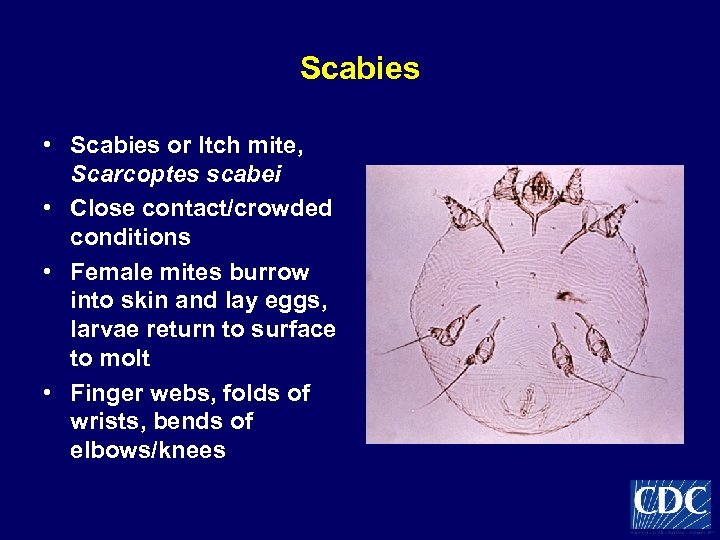
Scabies • Scabies or Itch mite, Scarcoptes scabei • Close contact/crowded conditions • Female mites burrow into skin and lay eggs, larvae return to surface to molt • Finger webs, folds of wrists, bends of elbows/knees

Other Mites Causing Dermatitis • Many species cause dermatitis: – – – Chicken Mite Northern fowl mite Tropical rat mite House mite Grain mite Straw itch mite • Cause intense itching and irritation • Infestations common after floods, rat/bird control Ornithonyssus bacoti Tropical Rat Mite
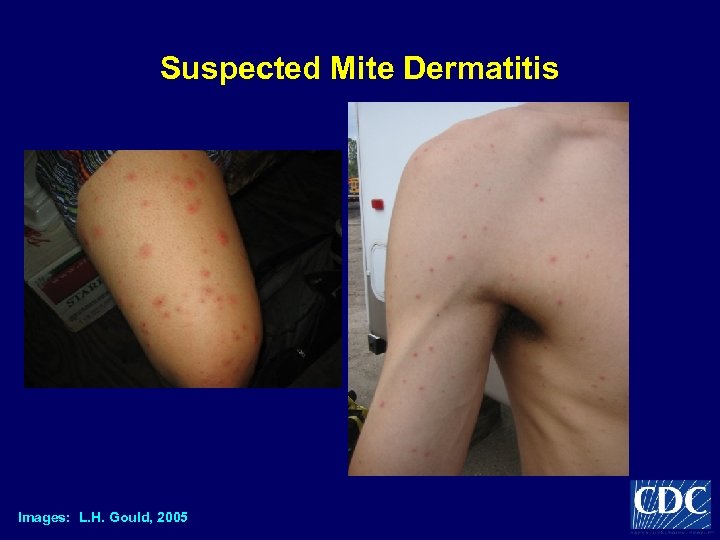
Suspected Mite Dermatitis Images: L. H. Gould, 2005

House Dust Mites • Allergen-symptoms include sneezing, itchy, watery eyes, runny nose, respiratory problems, eczema and asthma • Require damp environment • Feed on dander • “Dust control” http: //creatures. ifas. ufl. edu/urban/house_dust_mite_ fig 1. htm

Useful Resources • http: //www. cdc. gov/ncid od/diseases/submenus/ sub_lyme. htm • http: //www. cdc. gov/ncid od/dvbid/lyme/ld_resou rces. htm – Tick Management Handbook – IDSA Guidelines for Lyme Disease treatment

Additional information Division of Vector-Borne Infectious Diseases National Center for Zoonotic, Vector-Borne, and Enteric Diseases Centers for Disease Control and Prevention 3150 Rampart Road Fort Collins, Colorado, 80522 Telephone: (970) 221 -6400 Fax: (970) 221 -6476 Email: dvbid@cdc. gov Images (if noted): http: //phil. cdc. gov/phil/home. asp The findings and conclusions in this presentation are those of the authors and do not necessarily represent the views of the Centers for Disease Control and Prevention.
7919a5f1fb4a7e88015a1ab4492aa943.ppt