db2e83a482818ef9c69222531c55e42f.ppt
- Количество слайдов: 24

BHAMASHAH SWASTHYA BIMA YOJANA RAJASTHAN An overview of the scheme…….

BUDGET DECLARATION BY HON’BLE CHIEF MINISTER Hon’ble Chief Minister has announced “. . . ; g vko'; d g. S fd insurance ds ek/; e ls jk. T; dh xjhc vk. Sj oafpr turk dks futh v. Lirkyksa esa Hkh mipkj dh lqfo/kk miy. C/k djokb. Z tk; s. A vr% e. Sa jk. T; esa [kk| lqj{kk vf/kfu; e ds varx. Zr ik= l. Hkh ifjokjksa ds fy, Lok. LF; chek ; kstuk ykxw djus dh ? kks"k. kk djrh gw¡A bl ; kstuk dk yk. Hk Hkkek'kkg dk. MZ feyus ds lk. Fk feyus yxsxk. A bl ; kstuk ds varx. Zr jk. T; ds yx. Hkx 67 izfr'kr ifjokj yk. Hkkf. Uor gks ldsaxs vk. Sj ; s jktdh; vk. Sj accredited futh v. Lirkyksa esa Indoor patient ds : i esa Hkh viuk mipkj djk ldsaxs. A lkek. U; chekfj; ksa ds fy, izfr ifjokj 30 gtkj #i; s r. Fkk fpf. Ugr xa. Hkhj chekfj; ksa ds fy, 3 yk[k #i; s rd dk insurance coverage gksxk. A , sls ifjokjksa dks OPD jksxh ds : i esa fu%'kq. Yd 2

WHAT IS BHAMASHAH SWASTHYA BIMA YOJANA? It is a scheme to provide cashless facility to the IPD patients. For the identified families covered under National Food Security Act (NFSA) and Rashtriya Swasthya Bima Yojana (RSBY). By the Government (Medical and Health Department) Through an Insurance Company “New India Assurance Company” On a fixed premium per family per year on floater basis

AIMS OF THE SCHEME To Hedge Govt. moneys To provide quality health care that avoids large out of pocket expenditure To provide financial security against illness To Improve health status of the State. To create a data base which could be used to make policy level changes in Healthcare. To bring a revolution in healthcare in rural area – by providing stimulus to Private Sector to open hospitals in rural areas and reducing the increasing burden on Government facilities.

SALIENT FEATURES OF BSBY o Cashless for beneficiary o Only for IPD procedures. o 1715 disease packages are covered under the scheme which includes 1045 packages for Secondary illness, 500 for Tertiary illnesses. o 170 disease packages are reserved for Govt. Institutions. (these includes 65) o For the families covered under NFSA or RSBY. o To be coupled with Bhamashah Scheme. Treatment through Govt. and accredited private hospitals. Coverage of Rs. 30, 000 for general illnesses and Rs. 3 lakh for serious ailments. Provision for fund enhancement. MNDY , MNJY and MMBPLJRK to continue as usual. 5

SALIENT FEATURES OF BSBY Beneficiaries will be covered for secondary and tertiary illness according to the pre decided package rates. Pre-existing conditions or diseases will be covered from beginning of the scheme. Transportation allowance of INR 100 in cash to be given during discharge of the beneficiary with an annual ceiling of INR 500 and shall be a given only for Cardiac & Polytrauma cases. Transportation allowance is included in the package cost. Pre hospitalization of 7 days and post hospitalization of 15 days to be covered under the scheme.

THE PACKAGE COST INCLUDES…. . ü Bed charges ü Nursing and boarding charges ü Surgeons, Anaesthetists and other Consultants fees ü Aanaesthesia, Blood, oxygen, implants, medicines, consumables etc. ü Cost of radiological and pathological diagnostic Tests like blood, urine, x-ray etc. ü Transportation allowance for poly-trauma and cardiac cases ü Food for beneficiary during hospital admission

ADVANTAGES TO THE HEALTH INSTITUTION Direct Benefits: --Financial Strengthening of RMRS of the institution. As private hospitals are also empanelled , this scheme will result in lessened workload on Govt. Institution. Indirect Benefits: Increased satisfaction level of patient. (as it is complete package, patient doesn’t have to go for any extra medicines or investigations) Lesser incidents of bribing/overbilling etc as all activities will be monitored through IT portal.

ADVANTAGES TO THE BENEFICIARY Direct Benefits: --Cashless, hassel free. Low OOP expenditure. Opportunity to get treatment in private hospitals. All pre-existing diseases covered. 7 days pre and 15 days post hospitalization expenses covered. Indirect Benefits: Improved Health status Improved Economic Status Improved satisfaction level
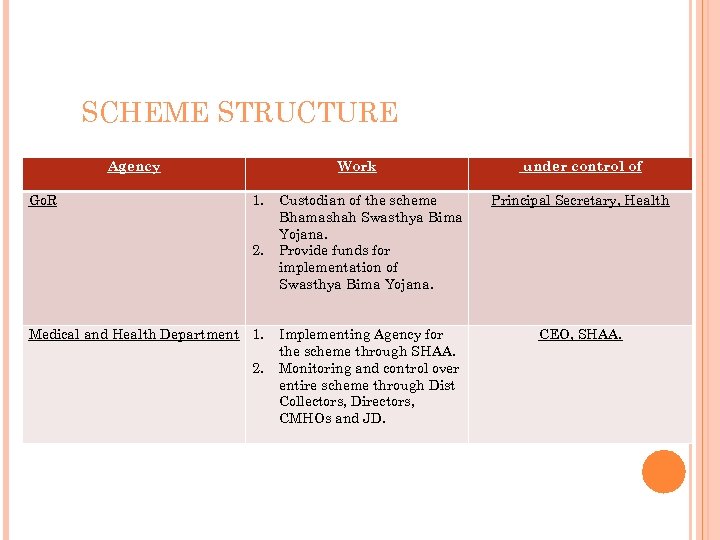
SCHEME STRUCTURE Agency Go. R Work 1. 2. Medical and Health Department 1. 2. under control of Custodian of the scheme Bhamashah Swasthya Bima Yojana. Provide funds for implementation of Swasthya Bima Yojana. Principal Secretary, Health Implementing Agency for the scheme through SHAA. Monitoring and control over entire scheme through Dist Collectors, Directors, CMHOs and JD. CEO, SHAA.

SCHEME STRUCTURE Agency Rajasthan State Health Assurance Agency Work 1. 2. 3. 4. 5. 6. 7. 8. Undertake all activities related to implementation of Bhamashah Swasthya Bima Yojana. Fixing accreditation criteria and accreditation of private hospitals in association with Insurance Company. Price setting of packages and finalization of packages through committee of technical experts. Preparation of Medical Protocols for identified packages. Medical Audit of Claims. Grievance Redressal. IEC plan for the scheme to be followed by Insurance Company. Monitoring and check that clauses of all RFPs/agreements are being complied. under control of CEO, SHAA
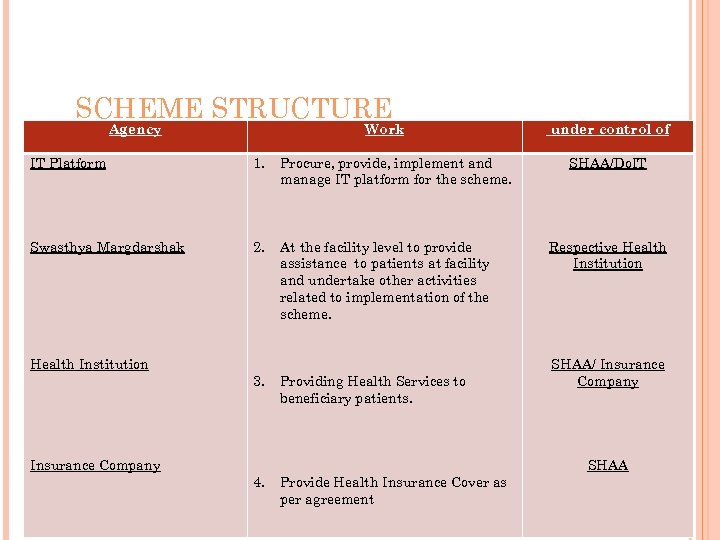

SCHEME STRUCTURE Agency Work IT Platform 1. Procure, provide, implement and manage IT platform for the scheme. Swasthya Margdarshak 2. At the facility level to provide assistance to patients at facility and undertake other activities related to implementation of the scheme. Health Institution Insurance Company 3. 4. Providing Health Services to beneficiary patients. Provide Health Insurance Cover as per agreement under control of SHAA/Do. IT Respective Health Institution SHAA/ Insurance Company SHAA
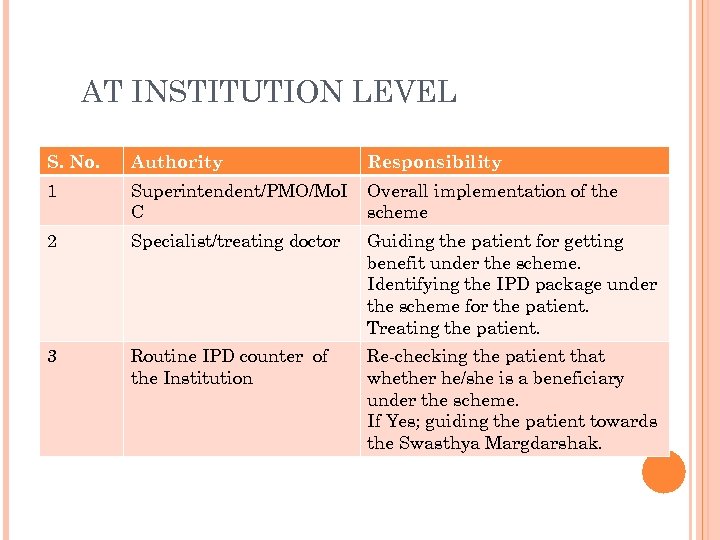
AT INSTITUTION LEVEL S. No. Authority Responsibility 1 Superintendent/PMO/Mo. I C Overall implementation of the scheme 2 Specialist/treating doctor Guiding the patient for getting benefit under the scheme. Identifying the IPD package under the scheme for the patient. Treating the patient. 3 Routine IPD counter of the Institution Re-checking the patient that whether he/she is a beneficiary under the scheme. If Yes; guiding the patient towards the Swasthya Margdarshak.
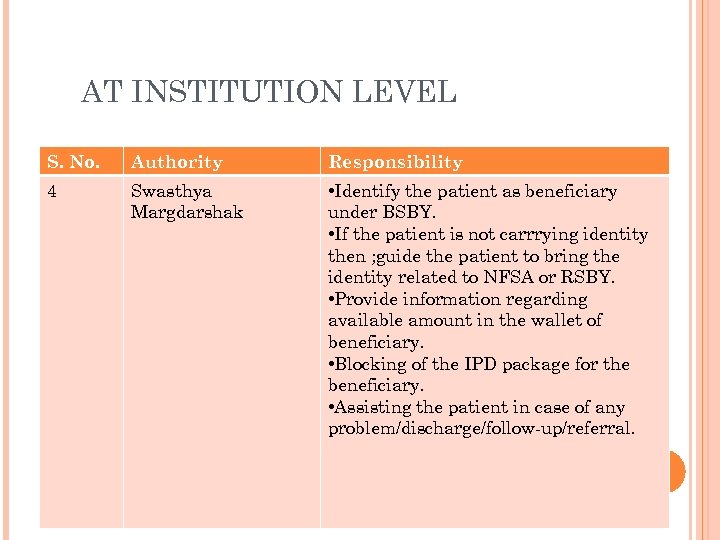
AT INSTITUTION LEVEL S. No. Authority Responsibility 4 Swasthya Margdarshak • Identify the patient as beneficiary under BSBY. • If the patient is not carrrying identity then ; guide the patient to bring the identity related to NFSA or RSBY. • Provide information regarding available amount in the wallet of beneficiary. • Blocking of the IPD package for the beneficiary. • Assisting the patient in case of any problem/discharge/follow-up/referral.

SERVICE PROVIDERS UNDER THE SCHEME Government Hospitals CHC and above level upto Medical College Hospitals shall stand empanelled. All private hospitals empanelled under RSBY shall also be stand empanelled. Other private hospitals fulfilling the empanelment criteria, shall be empanelled by Insurer after approval of Government. EMPANELMENT PROCESS The Insurance Company will empanel the hospitals on set parameters for quality after approval of Government. The geographical spread of the hospitals to be considered to prevent any disparity in the access to health facilities. Empanelment would require approval of SHAA.

HOSPITAL EMPANELMENT Minimum criteria for hospital empanelment – • It should have at least 30 inpatient beds. • It should be equipped in providing medical and surgical and diagnostic facilities. • General Ward: Should have separate wards for Males and Females • A well-equipped operation theatre • It should have qualified doctor(s) and nurse(s) and paramedic staff • Round the clock in house/tied up blood bank facility

HOSPITAL EMPANELMENT Obligations towards beneficiaries - • Shall not offer discriminatory treatment of patients on the basis of status/caste/money etc. • In case the hospital does not have the facilities required to provide treatment to the patients it shall refer the patient to a suitable health facility after providing of first aid/ services. • The hospital shall arrange for transport of the patient to the referred health facility. • Shall not deny treatment to any beneficiary

GRIEVANCE REDRESSAL Call centre/software would receive grievances from the beneficiaries/empanelled hospitals/Insurer. It would be under direct control of the Government A strong grievance Redressal mechanism for quick and appropriate grievance disposal The Grievance committee would be pro beneficiary Grievance reported at the call centre would be presented to the District Grievance Committee. Either of the parties if not satisfied may make an appeal to state Grievance Committee. Any grievances and appeal against the decision of the State Grievance Committee may be referred to the Appellate Authority for arbitration

GRIEVANCE REDRESSAL District Monitoring & Grievance Committee: The committee to be chaired by District Collector and will have Chief Medical and Health Officer, District level representative of the Insurer and a nominated member by Insurance Company State Monitoring & Grievance Committee: The committee will be chaired by CEO, SHAA and will have Additional Mission Director, NHM, Rajasthan State Health Society, Director- Public Health, Dean. Government Medical College, Insurance Company Representative, GM/CMD from a Public Sector Insurance Company, representative of the Risk Management Organization. Appellate Authority: The appellate authority will comprise of four members, and they shall include, Principal Secretary (Health), Secretary/Joint Secretary (Medical Education), Secretary/ Joint Secretary (health) and an officer nominated by PSF not below the rank of Joint Secretary.

IT ENABLED MONITORING MECHANISM Information technology would facilitate implementation of the scheme by Department of Medical, Health and Family Welfare under the broad framework / umbrella of Bhamashah Yojana. The IT department is undertaking following responsibilities To design a web-based application for implementation of SBY. To link the web-based application for SBY with following important applications: Bhamashah Database Hub UIDAI Database Hub Arogya Online e-Aushadhi e-Mitra

URGENT TO DO FOR DISTRICTS……. Procurement of Hardware as indicated in letter dated 31. 10. 15. Engagement of Swasthya Margdarshaks on these institutions as directed vide letter dated 5. 11. 15 and 17. 11. 15. Swasthya Margdarshaks are to be appointed on an IPD of 50 patients daily and 24 X 7 for one counter. However; Institution may appoint higher/lesser number of Swasthya Mardarshaks as per requirement. Inputs/suggestions on Disease packages latest by 20. 11. 15 as directed by Hon’ble MH in VC dated 17. 11. 15.

URGENT TO DO FOR DISTRICTS……. Dry Run has to start in all District Hospitals from 30. 11. 15. Therefore all necessary activities vis procurement of hardware and engagement of Swasthya Margdarshks etc. is to be completed by 25. 11. 15. Information to state latest by 26. 11. 15 with details of the trainee’s name, designation, place of posting.

PACKAGE LIST

THANK YOU!
db2e83a482818ef9c69222531c55e42f.ppt