59577579a36b91c9a177cd2f6df49274.ppt
- Количество слайдов: 22

Beyond e. Prescribing Factors Influencing Patient Safety in Medical Group Practices - September 26 th, 2007 AHRQ 2007: Improving Healthcare, Improving Live Larry Garber, M. D. – Medical Director for Informatics


Overview • Sources of Adverse Drug Events (ADE’s) in the ambulatory setting • Reducing anticoagulant-related ADE’s • Future plans and barriers to reducing ADE’s 3
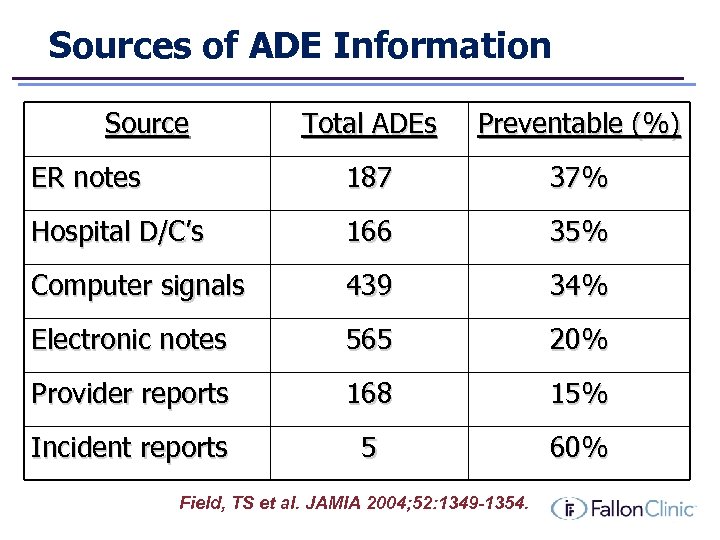
Sources of ADE Information Source Total ADEs Preventable (%) ER notes 187 37% Hospital D/C’s 166 35% Computer signals 439 34% Electronic notes 565 20% Provider reports 168 15% Incident reports 5 60% Field, TS et al. JAMIA 2004; 52: 1349 -1354.

ADE Rates in the Ambulatory Setting • • ADEs: 50 per 1000 person-years Preventable ADEs: 14 per 1000 person-years (28%) Extrapolated to total Medicare 65+: 1, 446, 949 ADEs per year 438, 046 preventable ADEs/year This is likely to be an underestimate Gurwitz JH et al JAMA 2003; 289: 1107 -1116
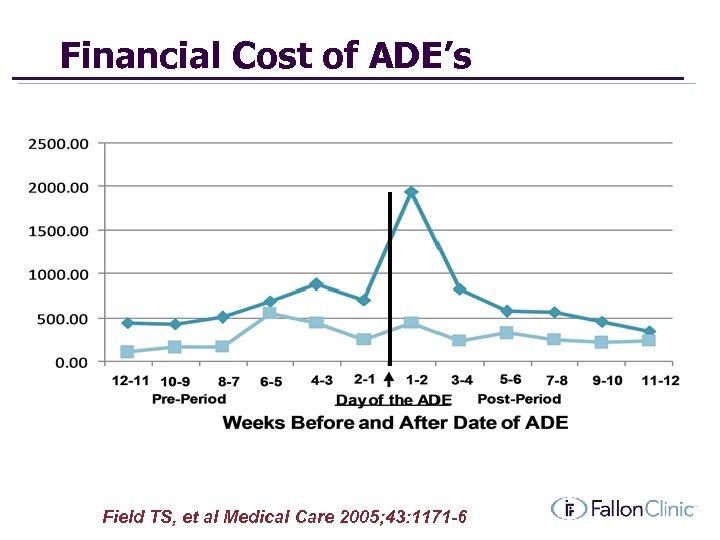
Financial Cost of ADE’s Field TS, et al Medical Care 2005; 43: 1171 -6

Financial Cost of ADE’s • • Increase in costs after an ADE: $1310 Increase after a preventable ADE: $1983 Extrapolated to 1000 adults age 65+ Costs per year to treat preventable ADEs: $27, 365
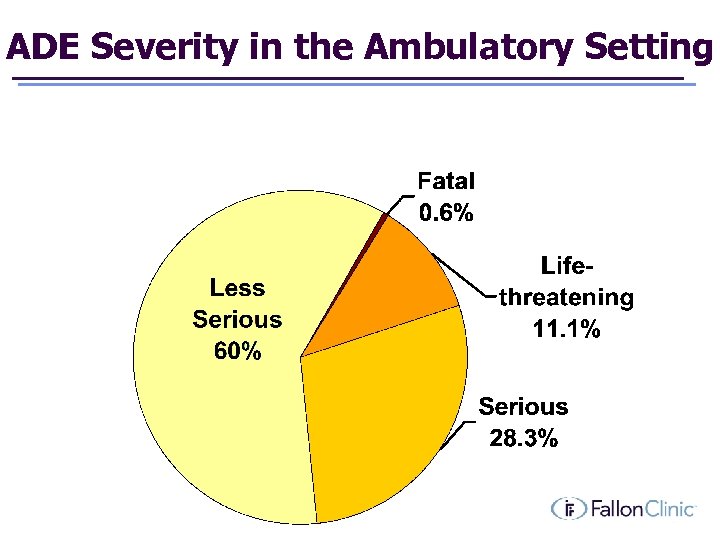
ADE Severity in the Ambulatory Setting

Severity & Preventability Of fatal & life-threatening events Preventable 52% Of less serious events Preventable 20%
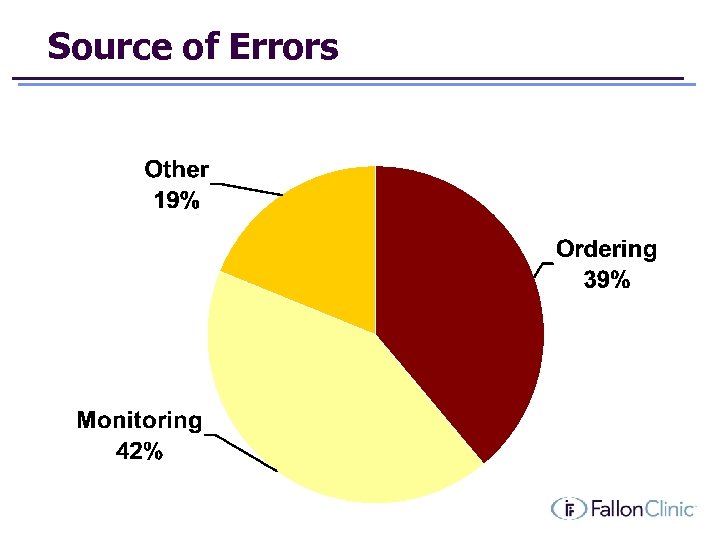
Source of Errors

So where do you start? 11
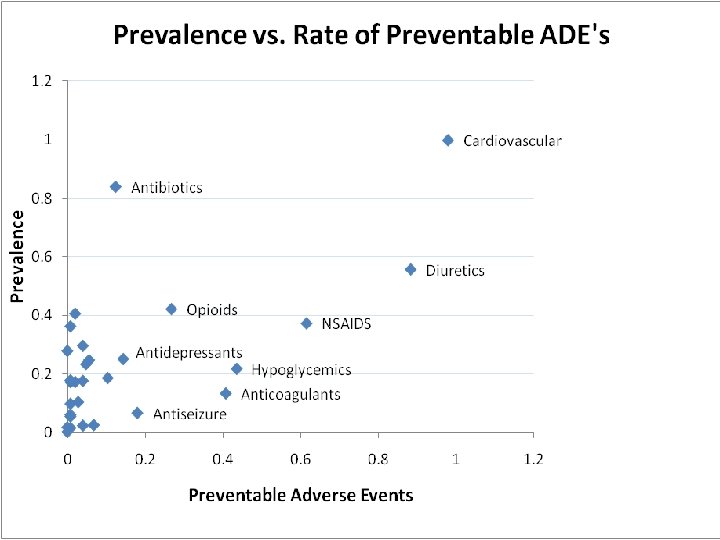
12
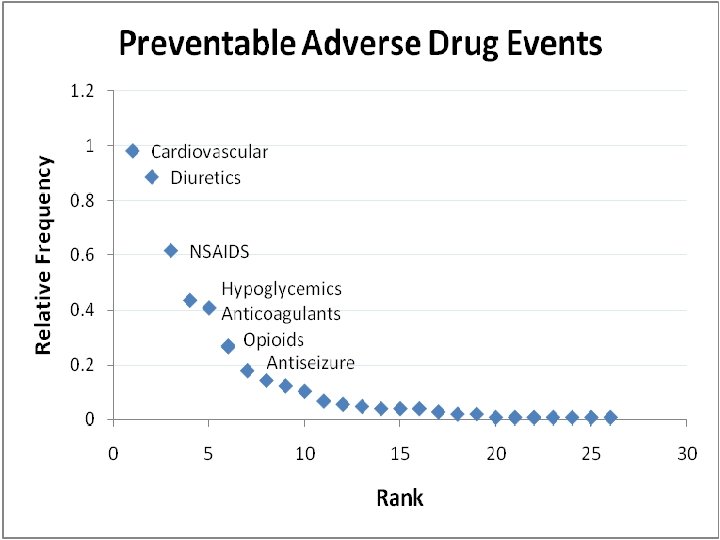
13
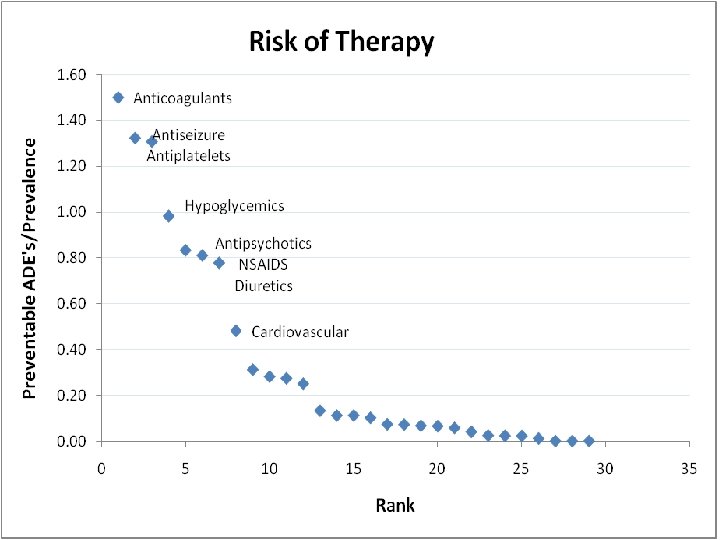
14

Fallon Approach to Preventing ADE’s • First target the Fatal & Life-Threatening preventable ADE’s è Warfarin • Then do a system-wide solution for the others 15

Preventing Warfarin ADE’s • Ordering/Prescribing è e. Prescribing with drug interaction checking è Simplified referrals to Anticoagulation Clinic • Monitoring è Converted Anticoagulation Clinic to Epic’s EHR è Simplified tracking of lab no-shows 16
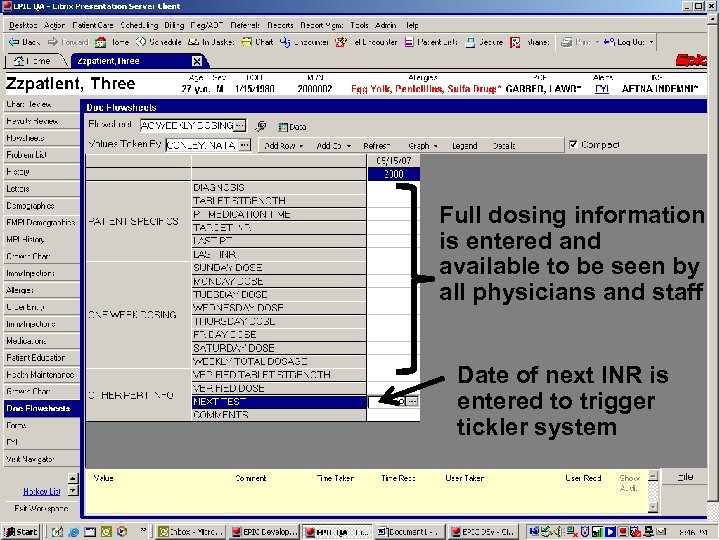
Full dosing information is entered and available to be seen by all physicians and staff Date of next INR is entered to trigger tickler system 17
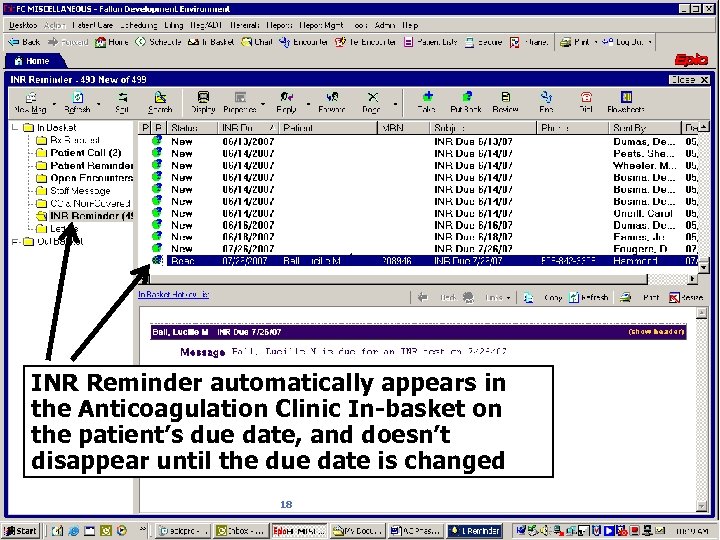
INR Reminder automatically appears in the Anticoagulation Clinic In-basket on the patient’s due date, and doesn’t disappear until the due date is changed 18

Preventing Other ADE’s • Use probabilistic risk assessment to: è characterize systemic and behavioral elements that increase of ADE’s during ordering/monitoring è identify potentially high-yield and likely-to-besuccessful interventions • Estimate likelihood that interventions at any given step would be successful in reducing errors at that step • Select interventions for implementation Field TS et al AHRQ Grant # 1 P 20 HS 017109 -01 19

Barriers to preventing ADE’s • Most organizations don’t have EHR’s • e. Prescribing doesn’t solve the monitoring problem • Many EHR’s don’t currently have the functionality to provide alerts for missing events without being in the context of a patient encounter • MD compliance • Time and money required to build interventions 20

Summary: • • ADEs are common and often preventable Types of errors suggest focus on prescribing and monitoring è Provision of information to physicians and assistants at right time, right place… è Use of automated tickler systems • Costs are high and savings from preventing ADEs could partially offset costs of interventions

Questions? Larry Garber, M. D. Lawrence. Garber@Fallon. Clinic. org Special thanks to Terry Field, Ph. D and Jerry Gurwitz, M. D. for their assistance on this presentation and never-ending work to study and prevent ADE’s 22
59577579a36b91c9a177cd2f6df49274.ppt