c7cccf8010ffabd6321a782da4de7f27.ppt
- Количество слайдов: 34

Beating Joe Camel: The American Society of Anesthesiologists Smoking Cessation Initiative 1

Beating Joe Camel… • Why bother? • Barriers • The ASA Smoking Cessation Initiative • How to help in three minutes or less • How to get paid for helping (under some circumstances)
Why bother? Quitting Smoking Improves Surgical Outcomes 3 Surgery May Promote Quitting Smoking

Tobacco Cessation Improves Surgical Outcomes • Cardiovascular complications • Respiratory complications • Wound related complications 4

Short Term Cardiovascular Benefits of Smoking Cessation • Nicotine Half life of ~1 -2 h Decreases in heart rate and systolic blood pressure in 24 hrs • Carbon Monoxide Half life of ~4 hours Level near normal at 12 hrs • Preoperative abstinence decreases the frequency of intraoperative ischemia* 5 *Woehlck et al, Anesth Analg 89: 856, 1999
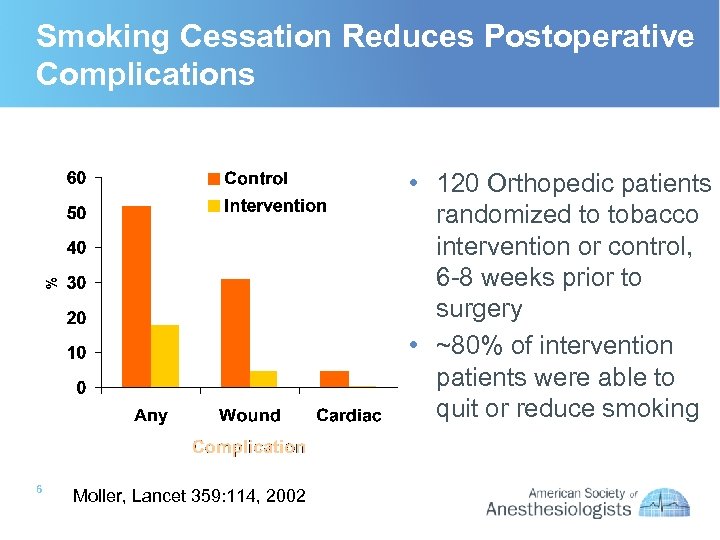
Smoking Cessation Reduces Postoperative Complications • 120 Orthopedic patients randomized to tobacco intervention or control, 6 -8 weeks prior to surgery • ~80% of intervention patients were able to quit or reduce smoking 6 Moller, Lancet 359: 114, 2002
Why bother? Quitting Smoking Improves Surgical Outcomes 7 Surgery May Promote Quitting Smoking

Surgery Promotes Tobacco Cessation • Opportunity to intervene – Contact with healthcare system – Forced abstinence • Major medical interventions improve quit rates – Occurs even in the absence of tobacco interventions – May also improve the effectiveness of tobacco interventions 8
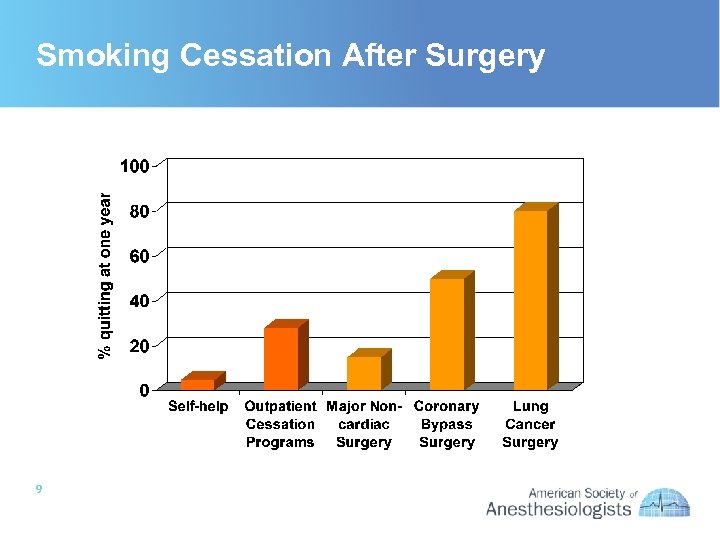
Smoking Cessation After Surgery 9

Perioperative Smoking Cessation Barriers • Quitting just before surgery increases pulmonary complications • Nicotine replacement therapy is dangerous • Surgical patients are already too stressed • Patients don’t want to hear about their smoking – they have enough to worry about 10
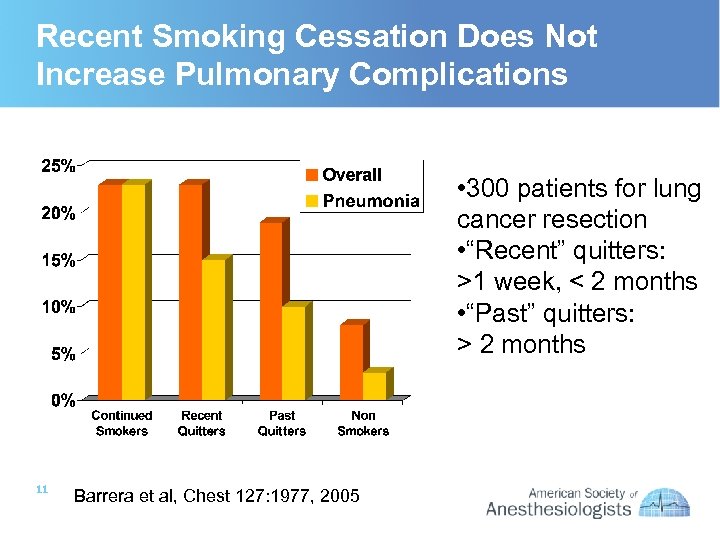
Recent Smoking Cessation Does Not Increase Pulmonary Complications • 300 patients for lung cancer resection • “Recent” quitters: >1 week, < 2 months • “Past” quitters: > 2 months 11 Barrera et al, Chest 127: 1977, 2005
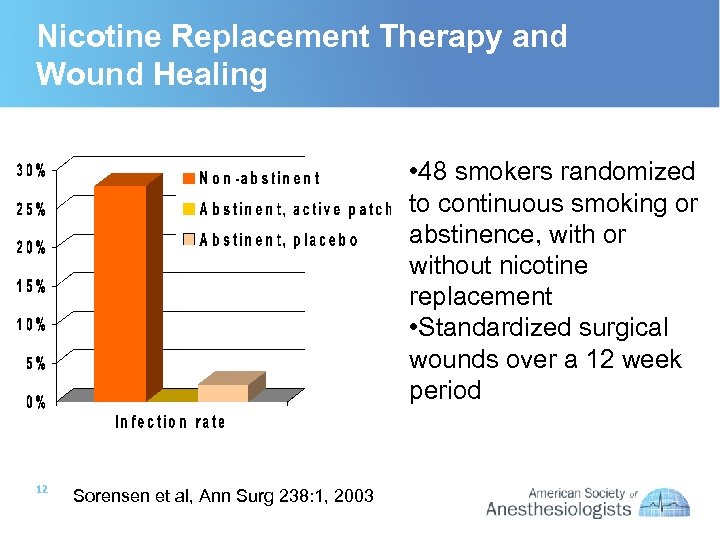
Nicotine Replacement Therapy and Wound Healing • 48 smokers randomized to continuous smoking or abstinence, with or without nicotine replacement • Standardized surgical wounds over a 12 week period 12 Sorensen et al, Ann Surg 238: 1, 2003
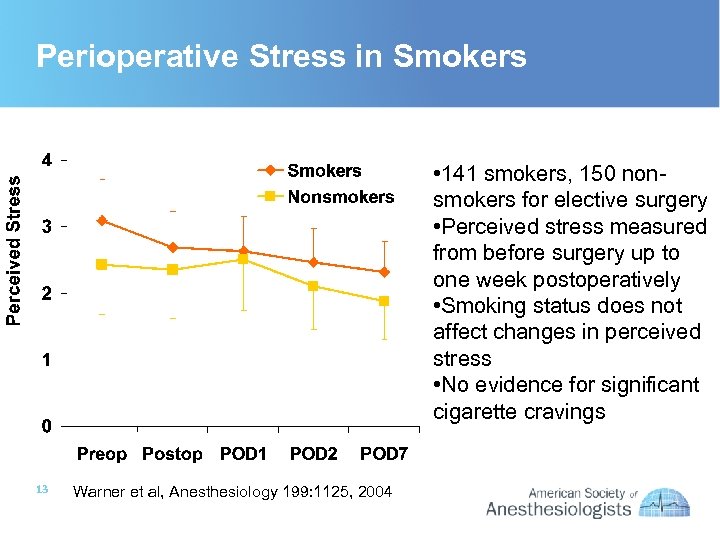
Perioperative Stress in Smokers • 141 smokers, 150 nonsmokers for elective surgery • Perceived stress measured from before surgery up to one week postoperatively • Smoking status does not affect changes in perceived stress • No evidence for significant cigarette cravings 13 Warner et al, Anesthesiology 199: 1125, 2004

What do smokers expect? • Essentially all smokers are aware of general health hazards – Most are not aware of how it might affect their surgery – and want to know! • They want information and options • Almost all will not be offended if you discuss their smoking… • But they do not want a sermon 14 Warner et al, Am J Prev Med 35: S 486, 2008

The Real Barriers to Intervention “I don’t know how” “I don’t have time” “It’s not my job” 15
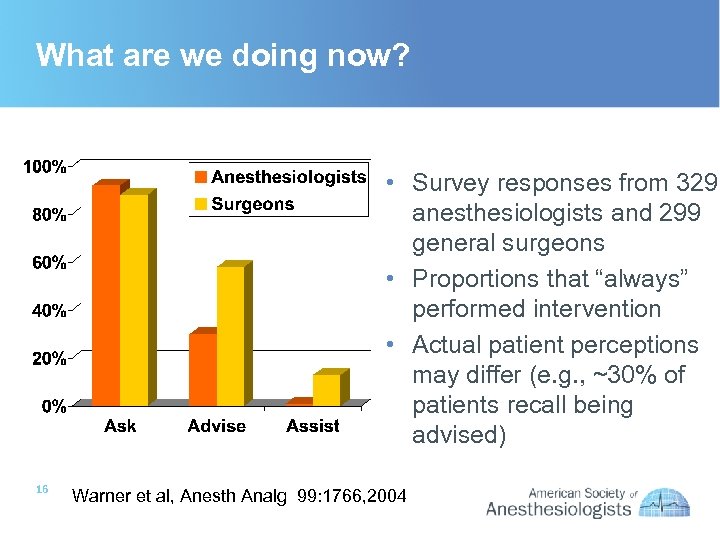
What are we doing now? • Survey responses from 329 anesthesiologists and 299 general surgeons • Proportions that “always” performed intervention • Actual patient perceptions may differ (e. g. , ~30% of patients recall being advised) 16 Warner et al, Anesth Analg 99: 1766, 2004

ASA Smoking Cessation Initiative: Rationale • Smoking cessation improves perioperative outcomes • Sustained abstinence produced by this teachable moment produces an average 6 -8 years of life gained • Demonstrate to the public that anesthesiologists are perioperative physicians who care about patient health • Recent CMS changes make it possible to bill for tobacco interventions lasting three or more minutes 17

ASA Smoking Cessation Initiative Vision and Goals • Vision – Every smoker cared for by an anesthesiologist will receive assistance in quitting as an integral part of care • Goal – Increase the involvement of ASA members in smoking cessation efforts, thus increasing abstinence rates for their patients who smoke 18

ASA Smoking Cessation Initiative Strategies • Encourage all anesthesiologists to consistently apply the ASK, ADVISE, and REFER technique • Develop anesthesiologists who can serve as leaders for local efforts to provide tobacco intervention services in perioperative practice • Educate the public regarding the importance of perioperative smoking cessation • Create partnerships with other healthcare professionals to promote a comprehensive perioperative strategy for patients who smoke 19

What should we do for smokers who need surgery? • ASK Assess tobacco use at every visit • ADVISE Strongly urge all tobacco users to quit • REFER To a tobacco quitline or other resources 20

What are Quitlines? • • Free via telephone to all Americans Staffed by trained specialists Up to 4 -6 personalized sessions Some offer free nicotine replacement therapy • Up to 30% success rates for patients who complete sessions Most providers and patients know nothing about quitlines…. 21

ASK every patient about tobacco use • Ask even if you already know the answer – Reinforces the message that as a physician you think their tobacco use is significant 22

ADVISE all smokers to quit • Why quit for surgery? – Talking Points – Quit for as long as possible before and after surgery • Day of surgery especially important – “fast” from both food and cigarettes – Benefits of quitting to wound healing, heart and lungs – Great opportunity to quit for good • Many people don’t have cravings • Need to be smoke free in the hospital anyway 23

REFER smokers to quitlines or other resources • What are quitlines? – Talking Points – – – Quitlines are free Talk with a specialist, not a recording Free stop smoking medications may be available Can call anytime, even after surgery Can help you stay off cigarettes even if you have already quit • Can also use proactive fax referral • 1 -800 -QUIT-NOW 24

ASA Quitline Card 25

ASA Patient and Provider Brochures 26

Other Patient Resources • Tobacco treatment specialists – Available in many practice settings – Often hospital-based • Web sites – www. smokefree. gov – www. asahq. org/stopsmoking • Insurers – E. g. , Blue Cross/Shield, Blue. Print for Health stop smoking program 27

Tobacco Intervention CMS Reimbursement • Who is covered? – Patients who use tobacco and have a disease or adverse health effect found by the US Surgeon General to be linked to tobacco use – Patients who take certain therapeutic agents whose metabolism or dosage is affected by tobacco use as based on FDA-approved information • CPT® Codes – 99406 Smoking and tobacco-use cessation counseling visit; intermediate, greater than 3 minutes up to 10 minutes – 99407 Smoking and tobacco-use cessation counseling visit; intensive, greater than 10 minutes 28

Tobacco Intervention CMS Reimbursement • Cessation counseling attempt occurs when a qualified physician or other Medicare recognized practitioner determines that a beneficiary meets the eligibility requirements and initiates treatment • Two attempts, up to 4 sessions, allowed every 12 months • No credentialing requirements 29

ASA Smoking Cessation Initiative Task Force Pilot Program • Identified 14 practices nationally, both private practices and academic • Implemented Ask-Advise-Refer strategy from Oct. – Dec. 2007 • Practices surveyed after this period to determine feasibility and gather feedback 30

Pilot Project Highlights (n=94 responses) • ~50% expressed increased self-efficacy • ~75% agree that they would incorporate AAR in their practice • High acceptance of materials • ~80% agree that the ASA should encourage 31
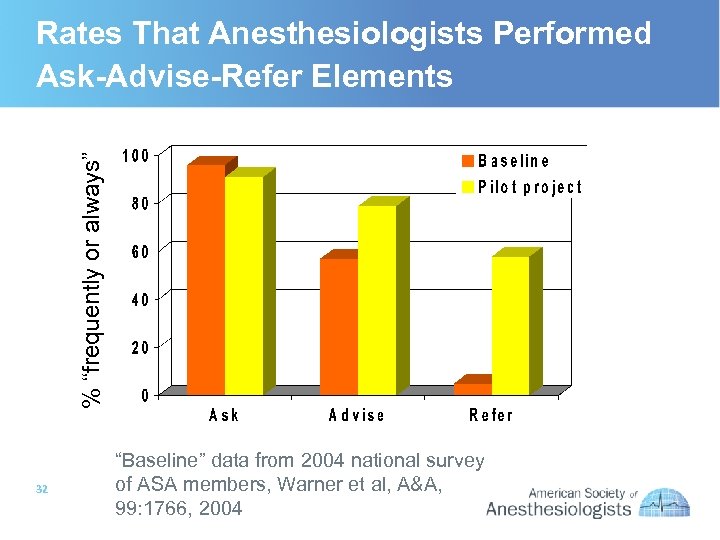
% “frequently or always” Rates That Anesthesiologists Performed Ask-Advise-Refer Elements 32 “Baseline” data from 2004 national survey of ASA members, Warner et al, A&A, 99: 1766, 2004

Bottom Line… • You can make a difference in the lives of your patients who smoke • You can help without being an expert in tobacco control – and get paid for doing it • The ASA is working to provide you with the tools needed to do this effectively 33

What about Joe Camel? 34
c7cccf8010ffabd6321a782da4de7f27.ppt