POSTER_A1.ppt
- Количество слайдов: 1
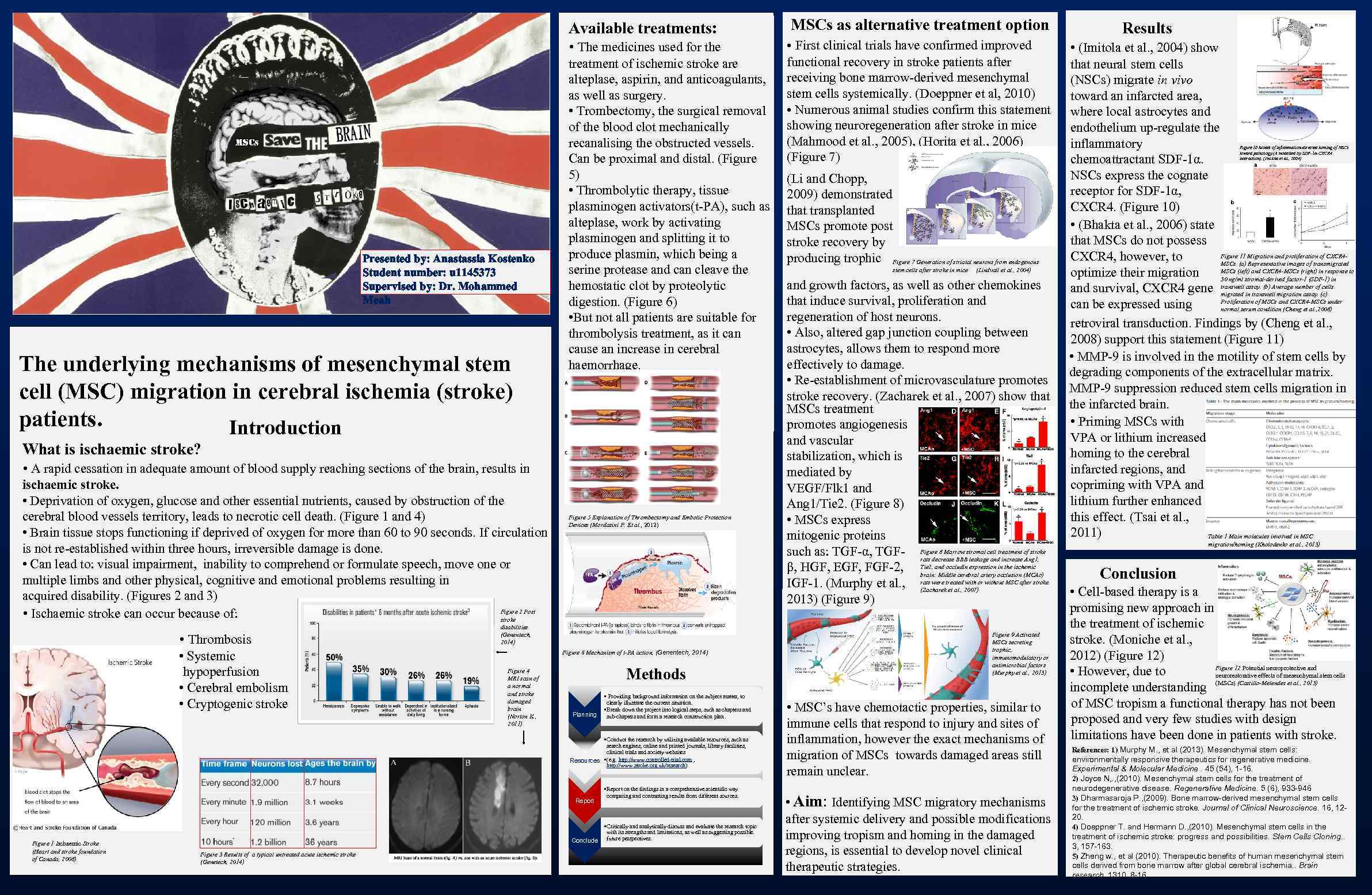
Available treatments: • The medicines used for the Presented by: Anastassia Kostenko Student number: u 1145373 Supervised by: Dr. Mohammed Meah The underlying mechanisms of mesenchymal stem cell (MSC) migration in cerebral ischemia (stroke) patients. Introduction MSCs as alternative treatment option • First clinical trials have confirmed improved functional recovery in stroke patients after receiving bone marrow-derived mesenchymal stem cells systemically. (Doeppner et al, 2010) • Numerous animal studies confirm this statement showing neuroregeneration after stroke in mice (Mahmood et al. , 2005), (Horita et al. , 2006) (Figure 7) treatment of ischemic stroke are alteplase, aspirin, and anticoagulants, as well as surgery. • Trombectomy, the surgical removal of the blood clot mechanically recanalising the obstructed vessels. Can be proximal and distal. (Figure 5) • Thrombolytic therapy, tissue plasminogen activators(t-PA), such as alteplase, work by activating plasminogen and splitting it to produce plasmin, which being a serine protease and can cleave the hemostatic clot by proteolytic digestion. (Figure 6) • But not all patients are suitable for thrombolysis treatment, as it can cause an increase in cerebral haemorrhage. What is ischaemic stroke? • A rapid cessation in adequate amount of blood supply reaching sections of the brain, results in ischaemic stroke. • Deprivation of oxygen, glucose and other essential nutrients, caused by obstruction of the cerebral blood vessels territory, leads to necrotic cell death. (Figure 1 and 4) • Brain tissue stops functioning if deprived of oxygen for more than 60 to 90 seconds. If circulation is not re-established within three hours, irreversible damage is done. • Can lead to: visual impairment, inability to comprehend or formulate speech, move one or multiple limbs and other physical, cognitive and emotional problems resulting in acquired disability. (Figures 2 and 3) Figure 2 Post • Ischaemic stroke can occur because of: stroke • Thrombosis • Systemic lhypoperfusion • Cerebral embolism • Cryptogenic stroke Figure 5 Explanation of Thrombectomy and Embolic Protection Devices (Mordasini P. Et al. , 2012) disabilities (Genentech, 2014) Figure 6 Mechanism of t-PA action, (Genentech, 2014) Figure 4 MRI scan of a normal and stroke damaged brain (Norton K. , 2011) Methods Planning • Providing background information on the subject matter, to clearly illustrate the current situation. • Break down the project into logical steps, such as chapters and sub-chapters and form a research construction plan. • Conduct the research by utilizing available resources, such as search engines, online and printed journals, library facilities, clinical trials and society websites Resources • (e. g. http: //www. controlled-trial. com , http: //www. stroke. org. uk/research) Report Figure 1 Ischaemic Stroke (Heart and stroke foundation of Canada, 2008) • Report on the findings in a comprehensive scientific way comparing and contrasting results from different sources. • Critically and analytically discuss and evaluate the research topic with its strengths and limitations, as well as suggesting possible Conclude future perspectives. Figure 3 Results of a typical untreated acute ischemic stroke (Genetech, 2014) (Li and Chopp, 2009) demonstrated that transplanted MSCs promote post stroke recovery by producing trophic Figure 7 Generation of striatal neurons from endogenous stem cells after stroke in mice (Lindvall et al. , 2004) and growth factors, as well as other chemokines that induce survival, proliferation and regeneration of host neurons. • Also, altered gap junction coupling between astrocytes, allows them to respond more effectively to damage. • Re-establishment of microvasculature promotes stroke recovery. (Zacharek et al. , 2007) show that MSCs treatment promotes angiogenesis and vascular stabilization, which is mediated by VEGF/Flk 1 and Ang 1/Tie 2. (Figure 8) • MSCs express mitogenic proteins such as: TGF-α, TGF- Figure 8 Marrow stromal cell treatment of stroke rats decrease BBB leakage and increase Ang 1, in the ischemic β, HGF, EGF, FGF-2, Tie 2, and occludin expression occlusion (MCAo) brain: Middle cerebral artery with IGF-1. (Murphy et al. , rats were treated 2007)or without MSC after stroke. (Zacharek et al. , 2013) (Figure 9) Figure 9 Activated MSCs secreting trophic, immunomodulatory or antimicrobial factors (Murphy et al. , 2013) • MSC’s have chemotactic properties, similar to immune cells that respond to injury and sites of inflammation, however the exact mechanisms of migration of MSCs towards damaged areas still remain unclear. • Aim: Identifying MSC migratory mechanisms after systemic delivery and possible modifications improving tropism and homing in the damaged regions, is essential to develop novel clinical therapeutic strategies. Results • (Imitola et al. , 2004) show that neural stem cells (NSCs) migrate in vivo toward an infarcted area, where local astrocytes and endothelium up-regulate the inflammatory chemoattractant SDF-1α. NSCs express the cognate receptor for SDF-1α, CXCR 4. (Figure 10) • (Bhakta et al. , 2006) state that MSCs do not possess Figure 11 Migration and proliferation of CXCR 4, however, to MSCs. (a) Representative images of transmigrated optimize their migration MSCs (left) and CXCR 4 -MSCs (right) in response to 30 ng/ml stromal-derived factor-1 (SDF-1) in assay. (b) Average number of cells and survival, CXCR 4 gene transwell in transwell migration assay. (c) migrated Proliferation of MSCs and CXCR 4 -MSCs under can be expressed using normal serum condition (Cheng et al. , 2008) retroviral transduction. Findings by (Cheng et al. , 2008) support this statement (Figure 11) • MMP-9 is involved in the motility of stem cells by degrading components of the extracellular matrix. MMP-9 suppression reduced stem cells migration in the infarcted brain. • Priming MSCs with VPA or lithium increased homing to the cerebral infarcted regions, and copriming with VPA and lithium further enhanced this effect. (Tsai et al. , 2011) Table 1 Main molecules involved in MSC Figure 10 Model of inflammation-directed homing of NSCs toward pathology (A modelled by SDF-1α-CXCR 4 interaction). (Imitola et al. , 2004) migration/homing (Kholodenko et al. , 2013) Conclusion • Cell-based therapy is a promising new approach in the treatment of ischemic stroke. (Moniche et al. , 2012) (Figure 12) Figure 12 Potential neuroprotective and • However, due to neurorestorative effects of mesenchymal stem cells incomplete understanding (MSCs) (Castillo-Melendez et al. , 2013) of MSC tropism a functional therapy has not been proposed and very few studies with design limitations have been done in patients with stroke. References: 1) Murphy M. , et al (2013). Mesenchymal stem cells: environmentally responsive therapeutics for regenerative medicine. Experimental & Molecular Medicine. 45 (54), 1 -16. 2) Joyce N, . , (2010). Mesenchymal stem cells for the treatment of neurodegenerative disease. Regenerative Medicine. 5 (6), 933 -946 3) Dharmasaroja P. , (2009). Bone marrow-derived mesenchymal stem cells for the treatment of ischemic stroke. Journal of Clinical Neuroscience. 16, 1220. 4) Doeppner T. and Hermann D. , (2010). Mesenchymal stem cells in the treatment of ischemic stroke: progress and possibilities. Stem Cells Cloning. . 3, 157 -163. 5) Zheng w. , et al (2010). Therapeutic benefits of human mesenchymal stem cells derived from bone marrow after global cerebral ischemia. . Brain research. 1310, 8 -16.
POSTER_A1.ppt