4d70d8d8e835d3b91ae55e675893dbee.ppt
- Количество слайдов: 23
 Assessment of Sleep Disorders Cynthia M. Dorsey, Ph. D. Director, Sleep Research Program Mc. Lean Hospital, Belmont, MA Assistant Professor of Psychology (Dept. of Psychiatry) Harvard Medical School, Boston, MA
Assessment of Sleep Disorders Cynthia M. Dorsey, Ph. D. Director, Sleep Research Program Mc. Lean Hospital, Belmont, MA Assistant Professor of Psychology (Dept. of Psychiatry) Harvard Medical School, Boston, MA
 Prevalence of sleep disorders • 40 million Americans have sleep disorders; 95% are undiagnosed. • Americans are chronically sleep deprived; 63 million suffer from EDS • 100, 000 drowsy driving crashes per year • Sleep deprivation and sleepiness from -insufficient sleep -1° sleep disorders
Prevalence of sleep disorders • 40 million Americans have sleep disorders; 95% are undiagnosed. • Americans are chronically sleep deprived; 63 million suffer from EDS • 100, 000 drowsy driving crashes per year • Sleep deprivation and sleepiness from -insufficient sleep -1° sleep disorders
 Prevalence of Insomnia • Insomnia is the most common sleep complaint in the industrialized world • Complaints in 30% to 40% • Complaint with distress or impairment: 8% to 19% Sateia MJ et al. SLEEP 2000; 23.
Prevalence of Insomnia • Insomnia is the most common sleep complaint in the industrialized world • Complaints in 30% to 40% • Complaint with distress or impairment: 8% to 19% Sateia MJ et al. SLEEP 2000; 23.
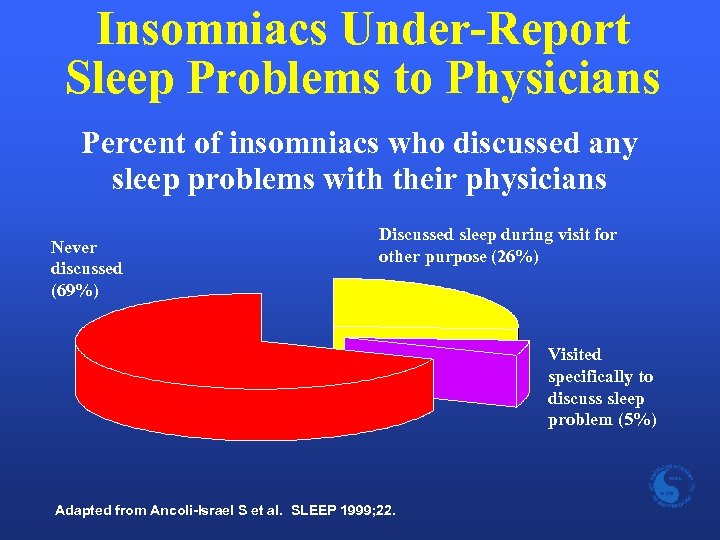 Insomniacs Under-Report Sleep Problems to Physicians Percent of insomniacs who discussed any sleep problems with their physicians Never discussed (69%) Discussed sleep during visit for other purpose (26%) Visited specifically to discuss sleep problem (5%) Adapted from Ancoli-Israel S et al. SLEEP 1999; 22.
Insomniacs Under-Report Sleep Problems to Physicians Percent of insomniacs who discussed any sleep problems with their physicians Never discussed (69%) Discussed sleep during visit for other purpose (26%) Visited specifically to discuss sleep problem (5%) Adapted from Ancoli-Israel S et al. SLEEP 1999; 22.
 Assessment: Patient History • • • History of sleep complaint Daytime symptoms Sleep habits (24 -hour sleep / wake cycle) Risks / Precipitating Factors Medical, neurological & psychiatric history • Medications • Health habits
Assessment: Patient History • • • History of sleep complaint Daytime symptoms Sleep habits (24 -hour sleep / wake cycle) Risks / Precipitating Factors Medical, neurological & psychiatric history • Medications • Health habits
 Assessment: Patient Questionnaires • • • Standard sleep history and symptoms Pittsburgh Sleep Quality Index (PSQI) Post Sleep Inventory Insomnia Interview Schedule Sleep Impairment Index
Assessment: Patient Questionnaires • • • Standard sleep history and symptoms Pittsburgh Sleep Quality Index (PSQI) Post Sleep Inventory Insomnia Interview Schedule Sleep Impairment Index
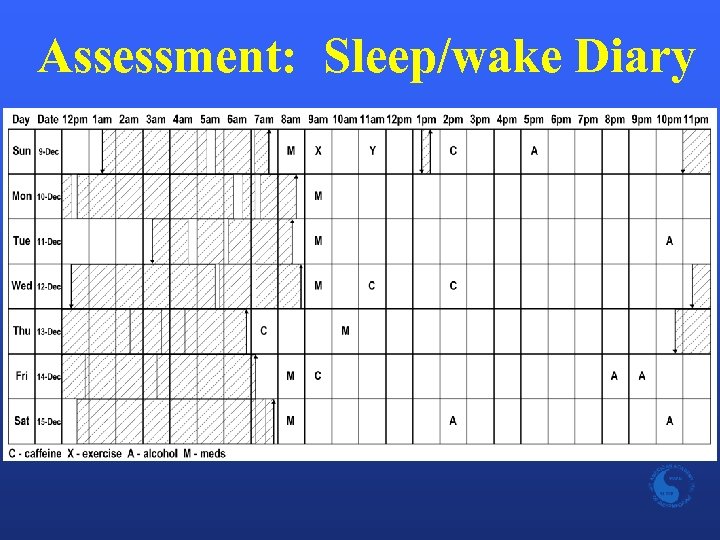 Assessment: Sleep/wake Diary
Assessment: Sleep/wake Diary
 Assessment: Epworth Sleepiness Scale “how likely to dose off or fall asleep” 0= not likely at all; 3= very likely (range of scale 0 -24, with abnormal > 10 -12) • sitting and reading • watching TV • sitting inactive in public place • passenger in a car for an hour • Lying down to rest in afternoon • sitting and talking to someone • sitting quietly after lunch • in a car stopped in traffic for a few minutes
Assessment: Epworth Sleepiness Scale “how likely to dose off or fall asleep” 0= not likely at all; 3= very likely (range of scale 0 -24, with abnormal > 10 -12) • sitting and reading • watching TV • sitting inactive in public place • passenger in a car for an hour • Lying down to rest in afternoon • sitting and talking to someone • sitting quietly after lunch • in a car stopped in traffic for a few minutes
 Assessment: Polysomnography • Indications – Suspect other sleep disorder – Poor treatment response • Not routinely indicated for the evaluation of insomnia Practice parameters for the evaluation of chronic insomnia. SLEEP 2000; 23.
Assessment: Polysomnography • Indications – Suspect other sleep disorder – Poor treatment response • Not routinely indicated for the evaluation of insomnia Practice parameters for the evaluation of chronic insomnia. SLEEP 2000; 23.
 Obstructive Sleep Apnea Repetitive upper airway obstruction during sleep: Symptoms: snoring, sleepiness, witnessed pauses in breathing, increased BMI/neck size Results: oxygen desaturation, arousal from sleep, increased risk for HTN, arrhythmia.
Obstructive Sleep Apnea Repetitive upper airway obstruction during sleep: Symptoms: snoring, sleepiness, witnessed pauses in breathing, increased BMI/neck size Results: oxygen desaturation, arousal from sleep, increased risk for HTN, arrhythmia.
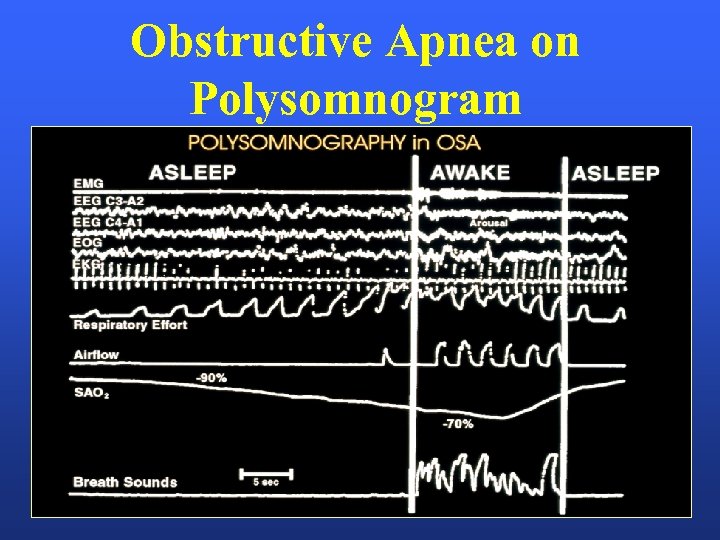 Obstructive Apnea on Polysomnogram
Obstructive Apnea on Polysomnogram
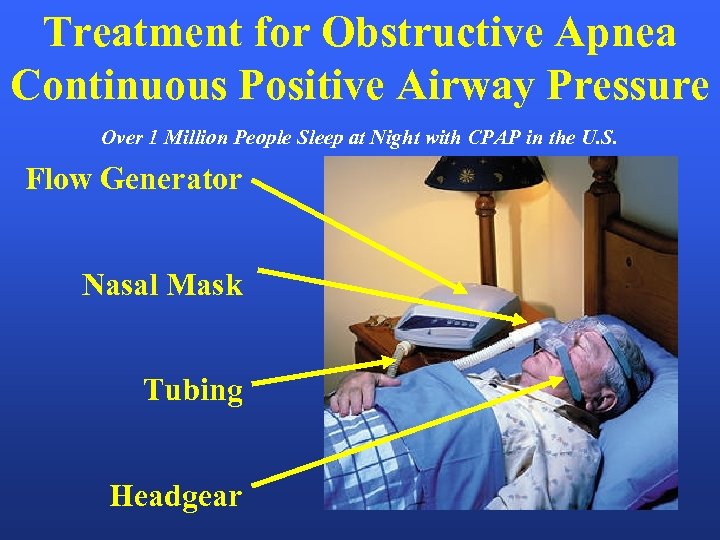 Treatment for Obstructive Apnea Continuous Positive Airway Pressure Over 1 Million People Sleep at Night with CPAP in the U. S. Flow Generator Nasal Mask Tubing Headgear
Treatment for Obstructive Apnea Continuous Positive Airway Pressure Over 1 Million People Sleep at Night with CPAP in the U. S. Flow Generator Nasal Mask Tubing Headgear

 Oximetry Many studies. Many methods of analysis. Most suggest this is neither sensitive nor specific for the diagnosis of sleep apnea. Not currently recommended as a standard diagnostic approach.
Oximetry Many studies. Many methods of analysis. Most suggest this is neither sensitive nor specific for the diagnosis of sleep apnea. Not currently recommended as a standard diagnostic approach.
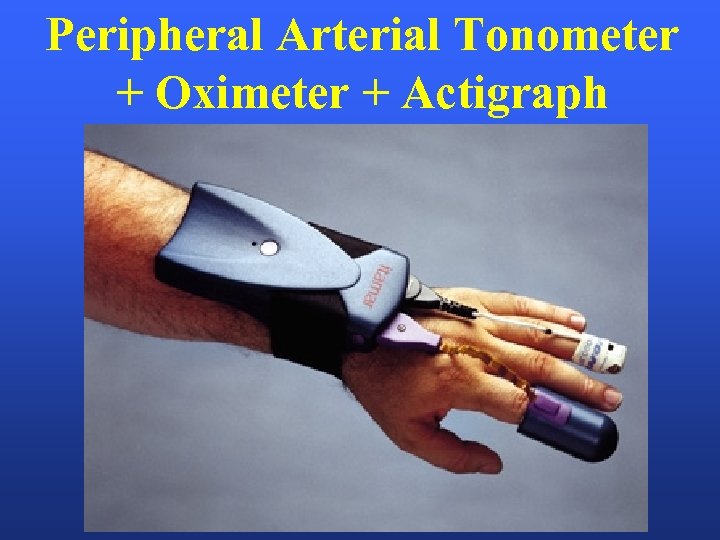 Peripheral Arterial Tonometer + Oximeter + Actigraph
Peripheral Arterial Tonometer + Oximeter + Actigraph
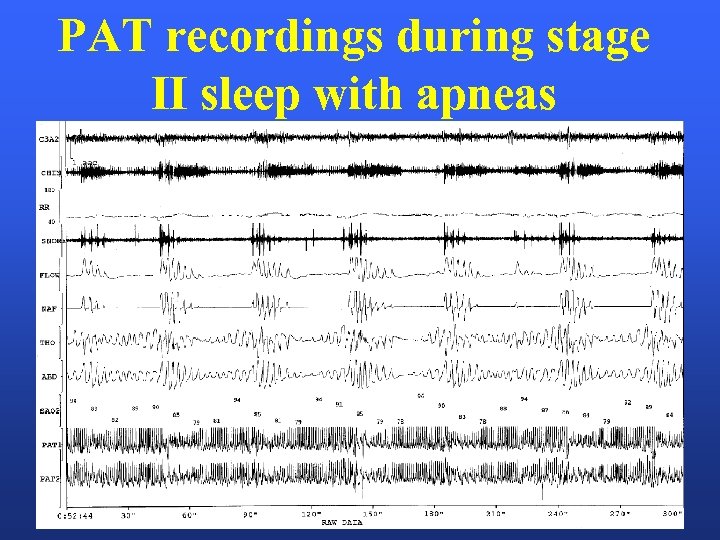 PAT recordings during stage II sleep with apneas
PAT recordings during stage II sleep with apneas
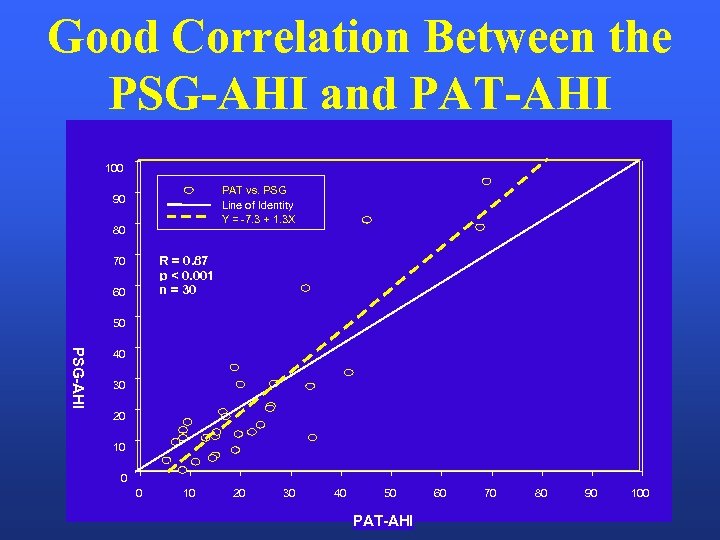 Good Correlation Between the PSG-AHI and PAT-AHI 100 PAT vs. PSG Line of Identity Y = -7. 3 + 1. 3 X 90 80 R = 0. 87 p < 0. 001 n = 30 70 60 50 PSG-AHI 40 30 20 10 0 0 10 20 30 40 50 PAT-AHI 60 70 80 90 100
Good Correlation Between the PSG-AHI and PAT-AHI 100 PAT vs. PSG Line of Identity Y = -7. 3 + 1. 3 X 90 80 R = 0. 87 p < 0. 001 n = 30 70 60 50 PSG-AHI 40 30 20 10 0 0 10 20 30 40 50 PAT-AHI 60 70 80 90 100
 Apnea Diagnostics If strong suspicion of sleep apnea, split night study is most cost-effective approach if CPAP is therapy of choice. If oral appliance is the treatment under consideration, a variety of home diagnostic approaches are reasonable. Follow-up evaluation (also possibly a home study) is mandatory if more than mild apnea is being treated with the appliance.
Apnea Diagnostics If strong suspicion of sleep apnea, split night study is most cost-effective approach if CPAP is therapy of choice. If oral appliance is the treatment under consideration, a variety of home diagnostic approaches are reasonable. Follow-up evaluation (also possibly a home study) is mandatory if more than mild apnea is being treated with the appliance.
 Core symptoms of Restless Legs Syndrome (RLS) Sensory: “achy”, “crawly” or “painful” Motor: restlessness, usually in distribution of sensory events, if present Diurnal variation: worse in evening Worse with immobility/relief with activity Walters, 1995
Core symptoms of Restless Legs Syndrome (RLS) Sensory: “achy”, “crawly” or “painful” Motor: restlessness, usually in distribution of sensory events, if present Diurnal variation: worse in evening Worse with immobility/relief with activity Walters, 1995
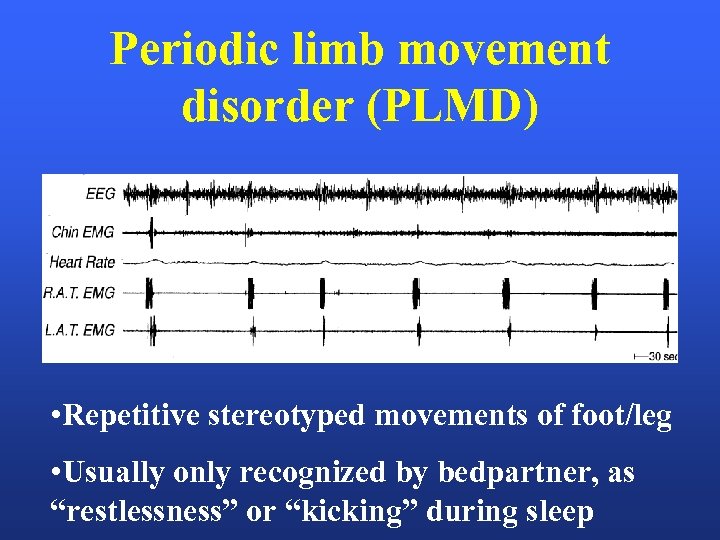 Periodic limb movement disorder (PLMD) • Repetitive stereotyped movements of foot/leg • Usually only recognized by bedpartner, as “restlessness” or “kicking” during sleep
Periodic limb movement disorder (PLMD) • Repetitive stereotyped movements of foot/leg • Usually only recognized by bedpartner, as “restlessness” or “kicking” during sleep
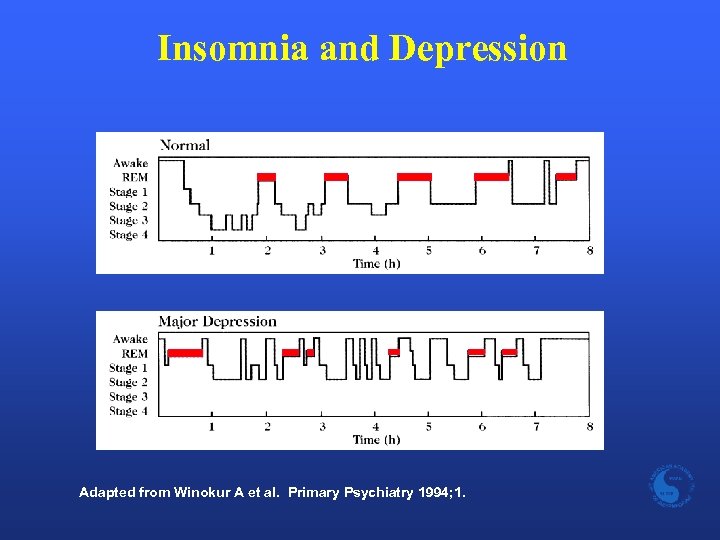 Insomnia and Depression Adapted from Winokur A et al. Primary Psychiatry 1994; 1.
Insomnia and Depression Adapted from Winokur A et al. Primary Psychiatry 1994; 1.
 Diagnosis of Narcolepsy Overnight polysomnography – Comorbid OSA or PLMD are not uncommon Multiple Sleep Latency Test (MSLT) – Mean sleep onset latency < 5 -7 minutes – 2 Sleep-onset REM naps Negative toxic screen Discontinue REM-suppressing and stimulant medications at least 2 wks before testing
Diagnosis of Narcolepsy Overnight polysomnography – Comorbid OSA or PLMD are not uncommon Multiple Sleep Latency Test (MSLT) – Mean sleep onset latency < 5 -7 minutes – 2 Sleep-onset REM naps Negative toxic screen Discontinue REM-suppressing and stimulant medications at least 2 wks before testing
 Conclusions • Initial interview is essential • Polysomnography remains the gold standard for assessing disorders of sleep fragmentation (e. g. OSA, PLMD) • If polysomnography is unavailable, home monitoring is reasonable Follow-up evaluation is mandatory
Conclusions • Initial interview is essential • Polysomnography remains the gold standard for assessing disorders of sleep fragmentation (e. g. OSA, PLMD) • If polysomnography is unavailable, home monitoring is reasonable Follow-up evaluation is mandatory


