 ARKIV NATIONAL V. N. KARAZIN KH. N. UNIVERSITY OF PEDIATRICS THE DEPARTMENT ALERGOSIS. RESPIRATORY IAL ASTHMA IN BRONCH CHILDREN AS. L. RAKOVSKA
ARKIV NATIONAL V. N. KARAZIN KH. N. UNIVERSITY OF PEDIATRICS THE DEPARTMENT ALERGOSIS. RESPIRATORY IAL ASTHMA IN BRONCH CHILDREN AS. L. RAKOVSKA
 ALLERGIC DISEASE MAY INVOLVE ONLY THE SKIN OR THE NOSE, EYES, LUNGS, AND GASTROINTESTINAL TRACT ALONE OR IN COMBINATION. MANY PATIENTS HAVE MORE THAN ONE ALLERGIC SYMPTOM.
ALLERGIC DISEASE MAY INVOLVE ONLY THE SKIN OR THE NOSE, EYES, LUNGS, AND GASTROINTESTINAL TRACT ALONE OR IN COMBINATION. MANY PATIENTS HAVE MORE THAN ONE ALLERGIC SYMPTOM.
 MOST COMMON ALLERGIC DISEASES IN CHILDREN • ATOPIC DERMATITIS (ECZEMA) • ALLERGIC RHINITIS • ASTHMA
MOST COMMON ALLERGIC DISEASES IN CHILDREN • ATOPIC DERMATITIS (ECZEMA) • ALLERGIC RHINITIS • ASTHMA
 ATOPIC DERMATITIS «ATOPIC MARСH» • INFANTS WITH ATOPIC DERMATITIS ARE PREDISPOSED TO DEVELOPING ALLERGIC RHINITIS AND/OR ASTHMA LATER IN CHILDHOOD, THE SOCALLED “ATOPIC MARCH”. ALLERGIC RHINITIS ASTHMA
ATOPIC DERMATITIS «ATOPIC MARСH» • INFANTS WITH ATOPIC DERMATITIS ARE PREDISPOSED TO DEVELOPING ALLERGIC RHINITIS AND/OR ASTHMA LATER IN CHILDHOOD, THE SOCALLED “ATOPIC MARCH”. ALLERGIC RHINITIS ASTHMA
 MAIN CAUSING FACTORS OF ALLERGIC DISEASES • 1. HEREDITARY • 2. ENVIRONMENTAL
MAIN CAUSING FACTORS OF ALLERGIC DISEASES • 1. HEREDITARY • 2. ENVIRONMENTAL
 ETIOLOGY • A FAMILY HISTORY OF ALLERGIC DISEASE IS OFTEN • PRESENT IN AFFECTED PATIENTS. MULTIPLE GENES PREDISPOSE TO ATOPY, INCLUDING THE LINKAGE OF ATOPY WITH CHROMOSOME 5. IF ONE PARENT HAS ALLERGIES, THE RISK IS 25% THAT A CHILD WILL DEVELOP ALLERGIC DISEASE. IF BOTH PARENTS HAVE ALLERGIES, THE RISK INCREASES TO 50% TO 70%. SIMILAR ALLERGIC DISEASES TEND TO OCCUR IN FAMILIES; IF BOTH PARENTS HAVE ALLERGIC RHINITIS, THEIR CHILDREN ALSO WILL HAVE ALLERGIC RHINITIS.
ETIOLOGY • A FAMILY HISTORY OF ALLERGIC DISEASE IS OFTEN • PRESENT IN AFFECTED PATIENTS. MULTIPLE GENES PREDISPOSE TO ATOPY, INCLUDING THE LINKAGE OF ATOPY WITH CHROMOSOME 5. IF ONE PARENT HAS ALLERGIES, THE RISK IS 25% THAT A CHILD WILL DEVELOP ALLERGIC DISEASE. IF BOTH PARENTS HAVE ALLERGIES, THE RISK INCREASES TO 50% TO 70%. SIMILAR ALLERGIC DISEASES TEND TO OCCUR IN FAMILIES; IF BOTH PARENTS HAVE ALLERGIC RHINITIS, THEIR CHILDREN ALSO WILL HAVE ALLERGIC RHINITIS.
 • ATOPY IS A RESULT OF A COMPLEX INTERACTION BETWEEN MULTIPLE GENES AND ENVIRONMENTAL FACTORS. • ATOPY IMPLIES SPECIFIC IG E-MEDIATED DISEASES, INCLUDING ALLERGIC RHINITIS, ASTHMA, AND ATOPIC DERMATITIS.
• ATOPY IS A RESULT OF A COMPLEX INTERACTION BETWEEN MULTIPLE GENES AND ENVIRONMENTAL FACTORS. • ATOPY IMPLIES SPECIFIC IG E-MEDIATED DISEASES, INCLUDING ALLERGIC RHINITIS, ASTHMA, AND ATOPIC DERMATITIS.
 PATHOPHYSIOLOGY OF ATOPY • ATOPY IS CHARACTERIZED BY ELEVATED LEVELS OF IG E AND EOSINOPHILIA WITH A PREDOMINANCE OF TH 2 CYTOKINES, INCLUDING INTERLEUKIN (IL)-4, IL-5, AND IL-13.
PATHOPHYSIOLOGY OF ATOPY • ATOPY IS CHARACTERIZED BY ELEVATED LEVELS OF IG E AND EOSINOPHILIA WITH A PREDOMINANCE OF TH 2 CYTOKINES, INCLUDING INTERLEUKIN (IL)-4, IL-5, AND IL-13.
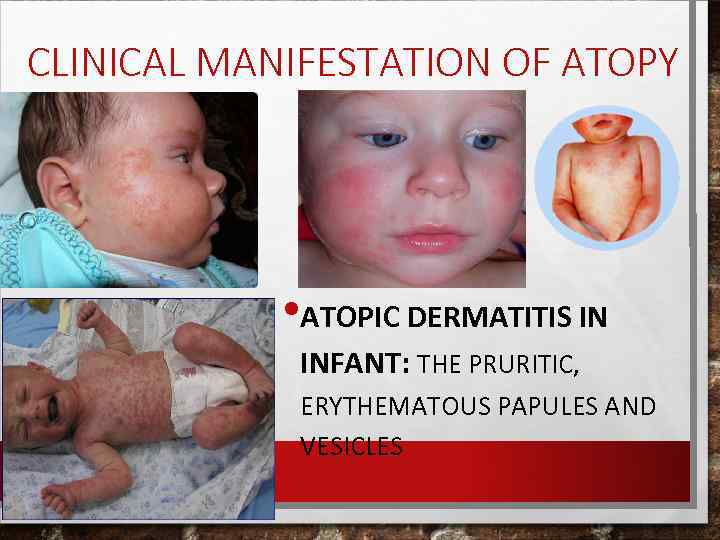 CLINICAL MANIFESTATION OF ATOPY • ATOPIC DERMATITIS IN INFANT: THE PRURITIC, ERYTHEMATOUS PAPULES AND VESICLES
CLINICAL MANIFESTATION OF ATOPY • ATOPIC DERMATITIS IN INFANT: THE PRURITIC, ERYTHEMATOUS PAPULES AND VESICLES
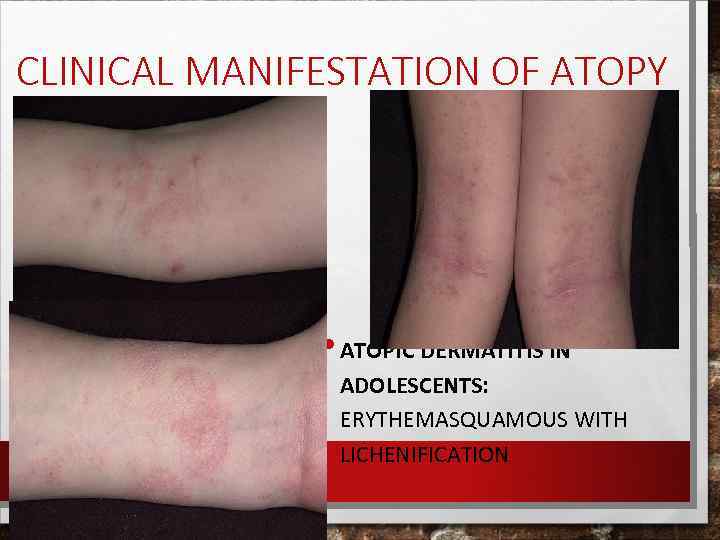 CLINICAL MANIFESTATION OF ATOPY • ATOPIC DERMATITIS IN ADOLESCENTS: ERYTHEMASQUAMOUS WITH LICHENIFICATION
CLINICAL MANIFESTATION OF ATOPY • ATOPIC DERMATITIS IN ADOLESCENTS: ERYTHEMASQUAMOUS WITH LICHENIFICATION
 CLINICAL MANIFESTATION OF ATOPY • DENNIE-MORGAN FOLDS OR DENNIE LINES (PROMINENT CREASES UNDER THE LOWER EYELIDS). • XEROSIS (DRY SKIN)
CLINICAL MANIFESTATION OF ATOPY • DENNIE-MORGAN FOLDS OR DENNIE LINES (PROMINENT CREASES UNDER THE LOWER EYELIDS). • XEROSIS (DRY SKIN)
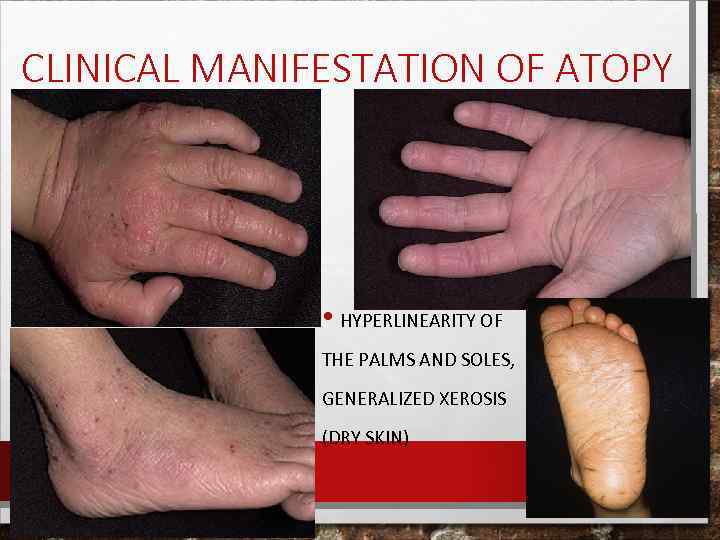 CLINICAL MANIFESTATION OF ATOPY • HYPERLINEARITY OF THE PALMS AND SOLES, GENERALIZED XEROSIS (DRY SKIN)
CLINICAL MANIFESTATION OF ATOPY • HYPERLINEARITY OF THE PALMS AND SOLES, GENERALIZED XEROSIS (DRY SKIN)
 RESPIRATORY ALLERGOSIS (RA) • • • ALLERGIC DISEASES OF URT (SO CALLED MINOR FORMS OF RESPIRATORY ALLERGOSIS): ALLERGIC RHINITIS, SINUSITIS, ADENOIDITIS, PHARYNGITIS, LARYNGITIS, TRACHEITIS BRONCHIAL ASTHMA ALLERGIC ALVEOLITIS, PNEUMONIAS, EOSINOPHILE PULMONARY INFILTRATE.
RESPIRATORY ALLERGOSIS (RA) • • • ALLERGIC DISEASES OF URT (SO CALLED MINOR FORMS OF RESPIRATORY ALLERGOSIS): ALLERGIC RHINITIS, SINUSITIS, ADENOIDITIS, PHARYNGITIS, LARYNGITIS, TRACHEITIS BRONCHIAL ASTHMA ALLERGIC ALVEOLITIS, PNEUMONIAS, EOSINOPHILE PULMONARY INFILTRATE.
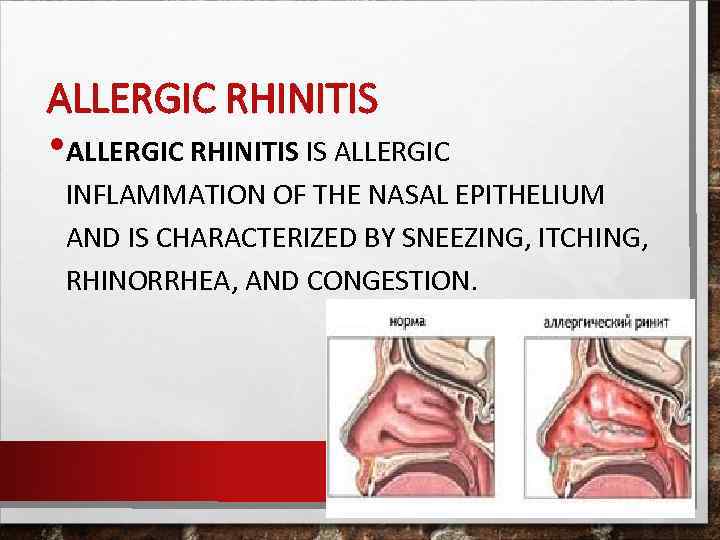 ALLERGIC RHINITIS • ALLERGIC RHINITIS IS ALLERGIC INFLAMMATION OF THE NASAL EPITHELIUM AND IS CHARACTERIZED BY SNEEZING, ITCHING, RHINORRHEA, AND CONGESTION.
ALLERGIC RHINITIS • ALLERGIC RHINITIS IS ALLERGIC INFLAMMATION OF THE NASAL EPITHELIUM AND IS CHARACTERIZED BY SNEEZING, ITCHING, RHINORRHEA, AND CONGESTION.
 EPIDEMIOLOGY • ALLERGIC RHINITIS IS ONE OF THE MOST COMMON DISORDERS IN INFANTS AND CHILDREN. IT IS OBSERVED IN 10% TO 25% OF THE POPULATION, WITH CHILDREN AND ADOLESCENTS MORE COMMONLY AFFECTED THAN ADULTS. • 30% OF PEOPLE WITH ALLERGIC RHINITIS HAVE ASTHMA
EPIDEMIOLOGY • ALLERGIC RHINITIS IS ONE OF THE MOST COMMON DISORDERS IN INFANTS AND CHILDREN. IT IS OBSERVED IN 10% TO 25% OF THE POPULATION, WITH CHILDREN AND ADOLESCENTS MORE COMMONLY AFFECTED THAN ADULTS. • 30% OF PEOPLE WITH ALLERGIC RHINITIS HAVE ASTHMA
 CLASSIFICATIONS OF ALLERGIC RHINITIS • SEASONAL • PERENNIAL • EPISODIC
CLASSIFICATIONS OF ALLERGIC RHINITIS • SEASONAL • PERENNIAL • EPISODIC
 SEASONAL ALLERGIC RHINITIS IS CAUSED BY AIRBORNE POLLEN WITH A SEASONAL PATTERN. INSECT-POLLINATED PLANTS (FLOWERS, FLOWERING TREES) ARE NOT A CAUSE OF ALLERGIC RHINITIS. TYPICALLY, TREES POLLINATE IN THE SPRING, GRASSES IN LATE SPRING TO SUMMER, AND WEEDS IN THE SUMMER AND FALL.
SEASONAL ALLERGIC RHINITIS IS CAUSED BY AIRBORNE POLLEN WITH A SEASONAL PATTERN. INSECT-POLLINATED PLANTS (FLOWERS, FLOWERING TREES) ARE NOT A CAUSE OF ALLERGIC RHINITIS. TYPICALLY, TREES POLLINATE IN THE SPRING, GRASSES IN LATE SPRING TO SUMMER, AND WEEDS IN THE SUMMER AND FALL.
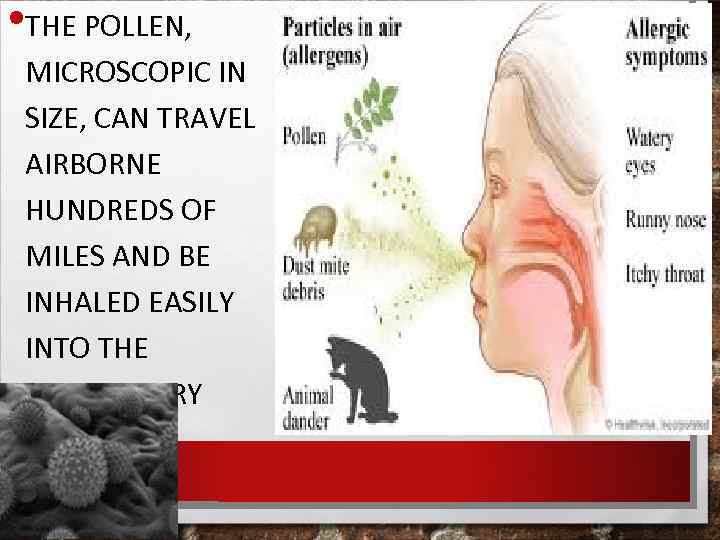 • THE POLLEN, MICROSCOPIC IN SIZE, CAN TRAVEL AIRBORNE HUNDREDS OF MILES AND BE INHALED EASILY INTO THE RESPIRATORY TRACT.
• THE POLLEN, MICROSCOPIC IN SIZE, CAN TRAVEL AIRBORNE HUNDREDS OF MILES AND BE INHALED EASILY INTO THE RESPIRATORY TRACT.
 • PERENNIAL ALLERGIC RHINITIS IS PRIMARILY CAUSED BY INDOOR ALLERGENS, SUCH AS HOUSE DUST MITES, ANIMAL DANDER, MOLD, AND COCKROACHES. • EPISODIC RHINITIS OCCURS WITH INTERMITTENT EXPOSURE TO ALLERGENS, SUCH AS VISITING A FRIEND'S HOME WHERE A PET DWELLS.
• PERENNIAL ALLERGIC RHINITIS IS PRIMARILY CAUSED BY INDOOR ALLERGENS, SUCH AS HOUSE DUST MITES, ANIMAL DANDER, MOLD, AND COCKROACHES. • EPISODIC RHINITIS OCCURS WITH INTERMITTENT EXPOSURE TO ALLERGENS, SUCH AS VISITING A FRIEND'S HOME WHERE A PET DWELLS.
 ALLERGIC RHINITIS IS CAUSED BY A TYPE I, IG EPATOPHYSIOLOGY MEDIATED ALLERGIC RESPONSE. DURING THE EARLY ALLERGIC PHASE, MAST CELLS DEGRANULATE AND RELEASE PREFORMED CHEMICAL MEDIATORS, SUCH AS HISTAMINE AND TRYPTASE, AND NEWLY GENERATED MEDIATORS, SUCH AS LEUKOTRIENES, PROSTAGLANDINS, AND PLATELET-ACTIVATING FACTOR. AFTER A QUIESCENT PHASE IN WHICH OTHER CELLS ARE RECRUITED, A LATE PHASE OCCURS APPROXIMATELY 4 TO 8 HOURS LATER. EOSINOPHILS, BASOPHILS, CD 4 T CELLS, MONOCYTES, AND NEUTROPHILS RELEASE THEIR CHEMICAL MEDIATORS, WHICH LEADS TO THE DEVELOPMENT OF CHRONIC NASAL INFLAMMATION.
ALLERGIC RHINITIS IS CAUSED BY A TYPE I, IG EPATOPHYSIOLOGY MEDIATED ALLERGIC RESPONSE. DURING THE EARLY ALLERGIC PHASE, MAST CELLS DEGRANULATE AND RELEASE PREFORMED CHEMICAL MEDIATORS, SUCH AS HISTAMINE AND TRYPTASE, AND NEWLY GENERATED MEDIATORS, SUCH AS LEUKOTRIENES, PROSTAGLANDINS, AND PLATELET-ACTIVATING FACTOR. AFTER A QUIESCENT PHASE IN WHICH OTHER CELLS ARE RECRUITED, A LATE PHASE OCCURS APPROXIMATELY 4 TO 8 HOURS LATER. EOSINOPHILS, BASOPHILS, CD 4 T CELLS, MONOCYTES, AND NEUTROPHILS RELEASE THEIR CHEMICAL MEDIATORS, WHICH LEADS TO THE DEVELOPMENT OF CHRONIC NASAL INFLAMMATION.
 • ALLERGIC RHINITIS IS RELATIVELY RARE IN CHILDREN YOUNGER THAN 6 MONTHS OLD, AND IF IT IS PRESENT IN INFANCY, IT IS DUE TO FOODS OR HOUSEHOLD INHALANTS RATHER THAN SEASONAL POLLENS. TYPICALLY, SEASONAL ALLERGIC RHINITIS PRESENTS IN CHILDREN OLDER THAN 3 YEARS.
• ALLERGIC RHINITIS IS RELATIVELY RARE IN CHILDREN YOUNGER THAN 6 MONTHS OLD, AND IF IT IS PRESENT IN INFANCY, IT IS DUE TO FOODS OR HOUSEHOLD INHALANTS RATHER THAN SEASONAL POLLENS. TYPICALLY, SEASONAL ALLERGIC RHINITIS PRESENTS IN CHILDREN OLDER THAN 3 YEARS.
 ALLERGIC RHINITIS CLINICAL MANIFESTATIONS • RHINORRHEA; NASAL CONGESTION; • PAROXYSMS OF SNEEZING; • PRURITUS OF THE EYES, NOSE, EARS • POSTNASAL DRIP • NOCTURNAL COUGH
ALLERGIC RHINITIS CLINICAL MANIFESTATIONS • RHINORRHEA; NASAL CONGESTION; • PAROXYSMS OF SNEEZING; • PRURITUS OF THE EYES, NOSE, EARS • POSTNASAL DRIP • NOCTURNAL COUGH
 ALLERGIC RHINITIS CLINICAL MANIFESTATIONS • CHILDREN WITH ALLERGIC RHINITIS MAY EXPERIENCE SLEEP DISTURBANCES, LIMITATIONS OF ACTIVITY, IRRITABILITY, AND MOOD AND COGNITIVE DISORDERS THAT ADVERSELY AFFECT THEIR PERFORMANCE AT SCHOOL AND THEIR SENSE OF WELL-BEING.
ALLERGIC RHINITIS CLINICAL MANIFESTATIONS • CHILDREN WITH ALLERGIC RHINITIS MAY EXPERIENCE SLEEP DISTURBANCES, LIMITATIONS OF ACTIVITY, IRRITABILITY, AND MOOD AND COGNITIVE DISORDERS THAT ADVERSELY AFFECT THEIR PERFORMANCE AT SCHOOL AND THEIR SENSE OF WELL-BEING.
 ALLERGIC RHINITIS PHYSICAL EXAMINATION "ALLERGIC FACE": OPEN MOUTH, MIDFACE HYPOPLASIA
ALLERGIC RHINITIS PHYSICAL EXAMINATION "ALLERGIC FACE": OPEN MOUTH, MIDFACE HYPOPLASIA
 ALLERGIC RHINITIS PHYSICAL EXAMINATION "ALLERGIC SALUTE": NASAL CREASE ON BRIDGE OF NOSE AS A RESULT OF CHRONIC UPWARD RUBBING WITH THE PALM OF THE HAND
ALLERGIC RHINITIS PHYSICAL EXAMINATION "ALLERGIC SALUTE": NASAL CREASE ON BRIDGE OF NOSE AS A RESULT OF CHRONIC UPWARD RUBBING WITH THE PALM OF THE HAND
 ALLERGIC RHINITIS PHYSICAL EXAMINATION ALLERGIC "SHINERS": DARK CIRCLES UNDER THE EYES, CAUSED BY VENOUS CONGESTION
ALLERGIC RHINITIS PHYSICAL EXAMINATION ALLERGIC "SHINERS": DARK CIRCLES UNDER THE EYES, CAUSED BY VENOUS CONGESTION
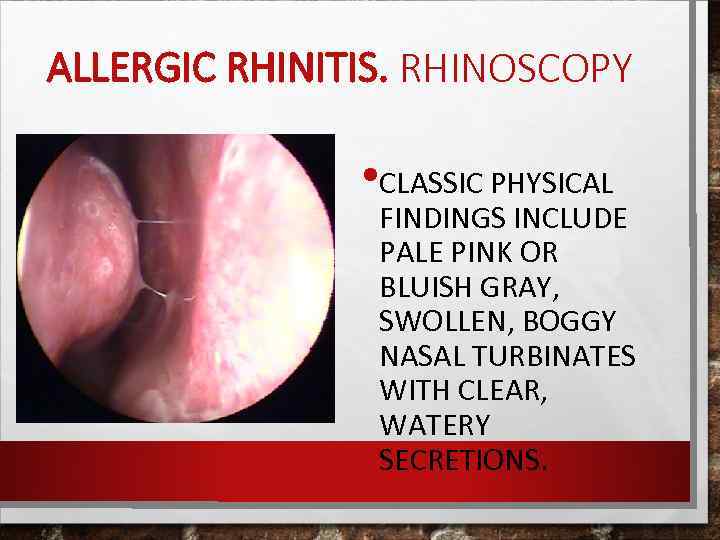 ALLERGIC RHINITIS. RHINOSCOPY • CLASSIC PHYSICAL FINDINGS INCLUDE PALE PINK OR BLUISH GRAY, SWOLLEN, BOGGY NASAL TURBINATES WITH CLEAR, WATERY SECRETIONS.
ALLERGIC RHINITIS. RHINOSCOPY • CLASSIC PHYSICAL FINDINGS INCLUDE PALE PINK OR BLUISH GRAY, SWOLLEN, BOGGY NASAL TURBINATES WITH CLEAR, WATERY SECRETIONS.
 ALLERGIC RHINITIS. LABORATORY AND IMAGING STUDIES • • NASAL SMEAR: >10% EOSINOPHILS. NASAL SMEAR EOSINOPHILIA IS OFTEN PREDICTIVE OF A GOOD CLINICAL RESPONSE TO NASAL CORTICOSTEROID SPRAYS. CBC : EOSINOPHILIA. AN EOSINOPHIL COUNT WITHIN THE NORMAL RANGE DOES NOT EXCLUDE ALLERGIC RHINITIS.
ALLERGIC RHINITIS. LABORATORY AND IMAGING STUDIES • • NASAL SMEAR: >10% EOSINOPHILS. NASAL SMEAR EOSINOPHILIA IS OFTEN PREDICTIVE OF A GOOD CLINICAL RESPONSE TO NASAL CORTICOSTEROID SPRAYS. CBC : EOSINOPHILIA. AN EOSINOPHIL COUNT WITHIN THE NORMAL RANGE DOES NOT EXCLUDE ALLERGIC RHINITIS.
 • SERUM IG E IS ELEVATED, BUT NOT ROUTINELY RECOMMENDED TO EVALUATE ATOPY. AN IG E VALUE WITHIN THE REFERENCE RANGE DOES NOT EXCLUDE ALLERGIC RHINITIS; HOWEVER, AN ELEVATED IGE VALUE IS SUGGESTIVE OF THE DIAGNOSIS.
• SERUM IG E IS ELEVATED, BUT NOT ROUTINELY RECOMMENDED TO EVALUATE ATOPY. AN IG E VALUE WITHIN THE REFERENCE RANGE DOES NOT EXCLUDE ALLERGIC RHINITIS; HOWEVER, AN ELEVATED IGE VALUE IS SUGGESTIVE OF THE DIAGNOSIS.
 • • ALLERGY TESTING SKIN TESTS (PRICK/PUNCTURE) IN VITRO SERUM TESTS (ALLERGEN-SPECIFIC IG E TESTING, ALSO KNOWN AS RADIOALLERGOSORBENT TEST (RAST) CAN BE HELPFUL IF A SPECIFIC ALLERGEN IS SUSPECTED. THOSE ARE USEFUL FOR PATIENTS WITH ABNORMAL SKIN CONDITIONS, PATIENTS WITH A TENDENCY FOR ANAPHYLAXIS, AND PATIENTS TAKING MEDICATIONS THAT INTERFERE WITH SKIN TESTING. SCREENING OF A LARGE NUMBER OF ALLERGENS CAN CAUSE CONFUSION BECAUSE OF THE POSSIBILITY OF FALSE POSITIVES. THIS IS ESPECIALLY TRUE FOR IG E FOOD ALLERGY TESTING.
• • ALLERGY TESTING SKIN TESTS (PRICK/PUNCTURE) IN VITRO SERUM TESTS (ALLERGEN-SPECIFIC IG E TESTING, ALSO KNOWN AS RADIOALLERGOSORBENT TEST (RAST) CAN BE HELPFUL IF A SPECIFIC ALLERGEN IS SUSPECTED. THOSE ARE USEFUL FOR PATIENTS WITH ABNORMAL SKIN CONDITIONS, PATIENTS WITH A TENDENCY FOR ANAPHYLAXIS, AND PATIENTS TAKING MEDICATIONS THAT INTERFERE WITH SKIN TESTING. SCREENING OF A LARGE NUMBER OF ALLERGENS CAN CAUSE CONFUSION BECAUSE OF THE POSSIBILITY OF FALSE POSITIVES. THIS IS ESPECIALLY TRUE FOR IG E FOOD ALLERGY TESTING.
 COMPLICATIONS • ASTHMA. • CHRONIC COUGH • EUSTACHIAN TUBE DYSFUNCTION AND OTITIS MEDIA; • TONSILLAR AND ADENOID HYPERTROPHY, • SLEEP DISTURBANCES, • OBSTRUCTIVE SLEEP APNEA; • SINUSITIS; • NASAL POLYPOSIS, • COGNITIVE DISORDERS
COMPLICATIONS • ASTHMA. • CHRONIC COUGH • EUSTACHIAN TUBE DYSFUNCTION AND OTITIS MEDIA; • TONSILLAR AND ADENOID HYPERTROPHY, • SLEEP DISTURBANCES, • OBSTRUCTIVE SLEEP APNEA; • SINUSITIS; • NASAL POLYPOSIS, • COGNITIVE DISORDERS
 DIFFERENTIAL DIAGNOSIS • INFECTIOUS RHINOSINUSITIS • ADENOIDAL HYPERPLASIA • CONGENITAL ANOMALIES • CHOANAL ATRESIA • GASTROESOPHAGEAL REFLUX • NASAL POLYPS • SINUSITIS • FOREIGN BODY
DIFFERENTIAL DIAGNOSIS • INFECTIOUS RHINOSINUSITIS • ADENOIDAL HYPERPLASIA • CONGENITAL ANOMALIES • CHOANAL ATRESIA • GASTROESOPHAGEAL REFLUX • NASAL POLYPS • SINUSITIS • FOREIGN BODY
 TREATMENT • ENVIRONMENTAL CONTROL MEASURES FOR ALLERGEN AVOIDANCE • EDUCATION OF PATIENT AND FAMILY • PHARMACOTHERAPY: ANTIHISTAMINES, • DECONGESTANTS, LEUKOTRIENE RECEPTOR ANTAGONISTS, INTRANASAL STEROIDS, AND TOPICAL CROMOLYN IMMUNOTHERAPY FOR INDIVIDUALS SUBOPTIMALLY CONTROLLED BY ABOVE MEASURES OR THOSE WITH SEVERE SYMPTOMS
TREATMENT • ENVIRONMENTAL CONTROL MEASURES FOR ALLERGEN AVOIDANCE • EDUCATION OF PATIENT AND FAMILY • PHARMACOTHERAPY: ANTIHISTAMINES, • DECONGESTANTS, LEUKOTRIENE RECEPTOR ANTAGONISTS, INTRANASAL STEROIDS, AND TOPICAL CROMOLYN IMMUNOTHERAPY FOR INDIVIDUALS SUBOPTIMALLY CONTROLLED BY ABOVE MEASURES OR THOSE WITH SEVERE SYMPTOMS
 IMMUNOTHERAPY • THE MECHANISM OF ACTION FOR ALLERGEN IMMUNOTHERAPY IS COMPLEX BUT INCLUDES INCREASED PRODUCTION OF AN IG G-BLOCKING ANTIBODY, DECREASED PRODUCTION OF SPECIFIC IG E, AND ALTERATION OF CYTOKINE EXPRESSION PRODUCED IN RESPONSE TO AN ALLERGEN CHALLENGE. IMMUNOTHERAPY IS EFFECTIVE FOR DESENSITIZATION TO POLLENS, DUST MITES, AND CAT AND DOG PROTEIN.
IMMUNOTHERAPY • THE MECHANISM OF ACTION FOR ALLERGEN IMMUNOTHERAPY IS COMPLEX BUT INCLUDES INCREASED PRODUCTION OF AN IG G-BLOCKING ANTIBODY, DECREASED PRODUCTION OF SPECIFIC IG E, AND ALTERATION OF CYTOKINE EXPRESSION PRODUCED IN RESPONSE TO AN ALLERGEN CHALLENGE. IMMUNOTHERAPY IS EFFECTIVE FOR DESENSITIZATION TO POLLENS, DUST MITES, AND CAT AND DOG PROTEIN.
 • SURGICAL TREATMENTS OF ADENOIDS ONLY FOR STRICT INDICATION AND AFTER INEFFECTIVE CONSERVATIVE TREATMENT IV DEGREE OF ADENOID HYPERPLASIA WITH ALMOST COMPLETE ABSENCE OF NOSE BREATHING, RECURRING OTITIS AND SINUSITIS. ADENOIDECTOMIA FREQUENTLY LEADS TO MANIFESTATION OF ASTHMA IN PATIENTS WITH MINOR FORMS OF RA.
• SURGICAL TREATMENTS OF ADENOIDS ONLY FOR STRICT INDICATION AND AFTER INEFFECTIVE CONSERVATIVE TREATMENT IV DEGREE OF ADENOID HYPERPLASIA WITH ALMOST COMPLETE ABSENCE OF NOSE BREATHING, RECURRING OTITIS AND SINUSITIS. ADENOIDECTOMIA FREQUENTLY LEADS TO MANIFESTATION OF ASTHMA IN PATIENTS WITH MINOR FORMS OF RA.
 BRONCHIAL ASTHMA • CHRONIC INFLAMMATORY AIRWAYS DISEASE CHARACTERIZED BY VARIABLE REVERSIBLE AIRWAY OBSTRUCTION, AIRWAY HYPER-RESPONSIVENESS, AND BRONCHIAL INFLAMMATION. • AN OBSTRUCTION OF AIRFLOW MAY BE COMPLETELY OR PARTIALLY REVERSED WITH OR WITHOUT SPECIFIC THERAPY.
BRONCHIAL ASTHMA • CHRONIC INFLAMMATORY AIRWAYS DISEASE CHARACTERIZED BY VARIABLE REVERSIBLE AIRWAY OBSTRUCTION, AIRWAY HYPER-RESPONSIVENESS, AND BRONCHIAL INFLAMMATION. • AN OBSTRUCTION OF AIRFLOW MAY BE COMPLETELY OR PARTIALLY REVERSED WITH OR WITHOUT SPECIFIC THERAPY.
 EPIDEMIOLOGY • ASTHMA AFFECTS AN ESTIMATED 300 MILLION INDIVIDUALS WORLDWIDE. • THE PREVALENCE IS 8 -10 TIMES HIGHER IN DEVELOPED COUNTRIES (EG, UNITED STATES, GREAT BRITAIN, AUSTRALIA, NEW ZEALAND) THAN IN THE DEVELOPING COUNTRIES.
EPIDEMIOLOGY • ASTHMA AFFECTS AN ESTIMATED 300 MILLION INDIVIDUALS WORLDWIDE. • THE PREVALENCE IS 8 -10 TIMES HIGHER IN DEVELOPED COUNTRIES (EG, UNITED STATES, GREAT BRITAIN, AUSTRALIA, NEW ZEALAND) THAN IN THE DEVELOPING COUNTRIES.
 EPIDEMIOLOGY • ASTHMA IS THE MOST COMMON CHRONIC DISEASE OF CHILDHOOD. ASTHMA AFFECTS 1 IN 13 SCHOOL-AGE CHILDREN AND IS A LEADING CAUSE OF OFFICE AND EMERGENCY DEPARTMENT VISITS, HOSPITALIZATIONS, AND SCHOOL ABSENTEEISM. • APPROXIMATELY 500, 000 ANNUAL HOSPITALIZATIONS (34. 6% IN INDIVIDUALS AGED 18 Y OR YOUNGER) ARE DUE TO ASTHMA.
EPIDEMIOLOGY • ASTHMA IS THE MOST COMMON CHRONIC DISEASE OF CHILDHOOD. ASTHMA AFFECTS 1 IN 13 SCHOOL-AGE CHILDREN AND IS A LEADING CAUSE OF OFFICE AND EMERGENCY DEPARTMENT VISITS, HOSPITALIZATIONS, AND SCHOOL ABSENTEEISM. • APPROXIMATELY 500, 000 ANNUAL HOSPITALIZATIONS (34. 6% IN INDIVIDUALS AGED 18 Y OR YOUNGER) ARE DUE TO ASTHMA.
 EPIDEMIOLOGY • THE PREVALENCE OF ASTHMA IS INCREASING, ESPECIALLY IN CHILDREN. • ASTHMA MORTALITY NEARLY DOUBLED BETWEEN 1980 AND 1993, WITH MORE THAN 5500 FATALITIES ANNUALLY. • DEATH RATE UP 80% IN PEOPLE UNDER 19 YEARS
EPIDEMIOLOGY • THE PREVALENCE OF ASTHMA IS INCREASING, ESPECIALLY IN CHILDREN. • ASTHMA MORTALITY NEARLY DOUBLED BETWEEN 1980 AND 1993, WITH MORE THAN 5500 FATALITIES ANNUALLY. • DEATH RATE UP 80% IN PEOPLE UNDER 19 YEARS
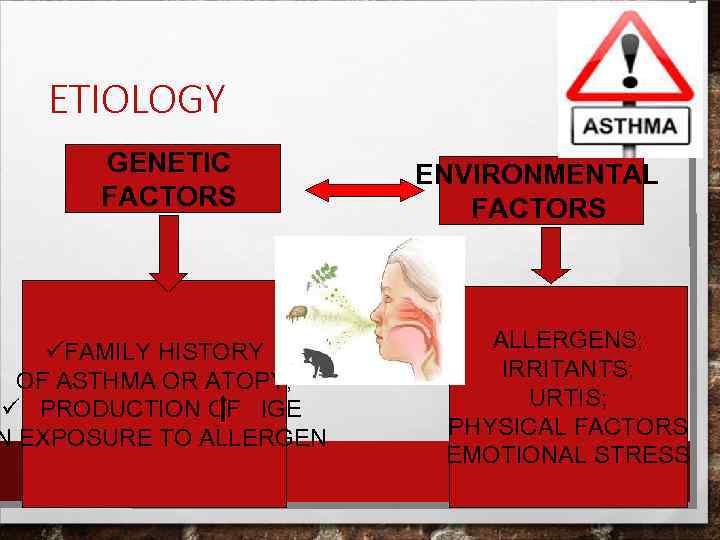 ETIOLOGY GENETIC FACTORS üFAMILY HISTORY OF ASTHMA OR ATOPY; ü PRODUCTION OF IGE N EXPOSURE TO ALLERGEN ENVIRONMENTAL FACTORS ALLERGENS; IRRITANTS; URTIS; PHYSICAL FACTORS EMOTIONAL STRESS
ETIOLOGY GENETIC FACTORS üFAMILY HISTORY OF ASTHMA OR ATOPY; ü PRODUCTION OF IGE N EXPOSURE TO ALLERGEN ENVIRONMENTAL FACTORS ALLERGENS; IRRITANTS; URTIS; PHYSICAL FACTORS EMOTIONAL STRESS
 SOME ALLERGENS WHICH MAY CAUSE ASTHMA HOUSE-DUST MITES WHICH LIVE IN CARPETS, MATTRESSES AND UPHOLSTERED FURNITURE DUST OF BOOK DEPOSITORI ES SALIVA, EXCREMENTS, HAIR AND EPIDERMIS OF DOMESTIC ANIMALS PLANT POLLEN PHARMACOLOGI CAL AGENTS (ENZYMES, ANTIBIOTICS, VACCINES, SERUMS) FOOD COMPONENTS (STABILIZERS, GENETICALLY MODIFIED PRODUCTS)
SOME ALLERGENS WHICH MAY CAUSE ASTHMA HOUSE-DUST MITES WHICH LIVE IN CARPETS, MATTRESSES AND UPHOLSTERED FURNITURE DUST OF BOOK DEPOSITORI ES SALIVA, EXCREMENTS, HAIR AND EPIDERMIS OF DOMESTIC ANIMALS PLANT POLLEN PHARMACOLOGI CAL AGENTS (ENZYMES, ANTIBIOTICS, VACCINES, SERUMS) FOOD COMPONENTS (STABILIZERS, GENETICALLY MODIFIED PRODUCTS)
 IRRITANTS: • PASSIVE OR ACTIVE SMOKING, • PERFUMES, • PAINT ODORS, • FUMES • HAIR SPRAYS, • AIR POLLUTANTS, • OZONE • VARIOUS CHEMICAL SUBSTATIONS
IRRITANTS: • PASSIVE OR ACTIVE SMOKING, • PERFUMES, • PAINT ODORS, • FUMES • HAIR SPRAYS, • AIR POLLUTANTS, • OZONE • VARIOUS CHEMICAL SUBSTATIONS
 PHYSICAL FACTORS: • METEOROLOGICAL FACTORS (COLD AIR, CHANGES IN ATMOSPHERIC TEMPERATURE, BAROMETRIC PRESSURE, AIR HUMIDITY, ETC) • EXERCISE AND HYPERVENTILATION • EMOTIONAL STRESS
PHYSICAL FACTORS: • METEOROLOGICAL FACTORS (COLD AIR, CHANGES IN ATMOSPHERIC TEMPERATURE, BAROMETRIC PRESSURE, AIR HUMIDITY, ETC) • EXERCISE AND HYPERVENTILATION • EMOTIONAL STRESS
 PATHOPHYSIOLOGY THE GENESIS OF ANY ALLERGIC REACTION MAY BE DIVIDED INTO • IMMUNE, • PATHOCHEMICAL, • PATHOPHYSIOLOGIC PHASES.
PATHOPHYSIOLOGY THE GENESIS OF ANY ALLERGIC REACTION MAY BE DIVIDED INTO • IMMUNE, • PATHOCHEMICAL, • PATHOPHYSIOLOGIC PHASES.
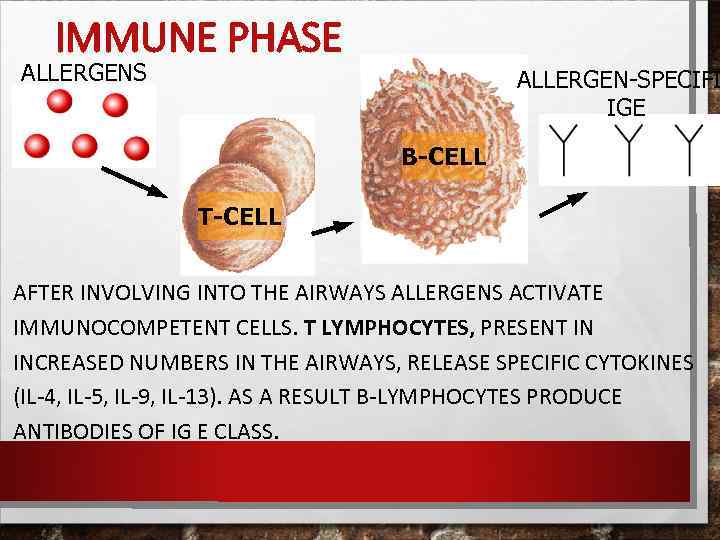 IMMUNE PHASE ALLERGENS ALLERGEN-SPECIFI IGE B-CELL T-CELL AFTER INVOLVING INTO THE AIRWAYS ALLERGENS ACTIVATE IMMUNOCOMPETENT CELLS. T LYMPHOCYTES, PRESENT IN INCREASED NUMBERS IN THE AIRWAYS, RELEASE SPECIFIC CYTOKINES (IL-4, IL-5, IL-9, IL-13). AS A RESULT B-LYMPHOCYTES PRODUCE ANTIBODIES OF IG E CLASS.
IMMUNE PHASE ALLERGENS ALLERGEN-SPECIFI IGE B-CELL T-CELL AFTER INVOLVING INTO THE AIRWAYS ALLERGENS ACTIVATE IMMUNOCOMPETENT CELLS. T LYMPHOCYTES, PRESENT IN INCREASED NUMBERS IN THE AIRWAYS, RELEASE SPECIFIC CYTOKINES (IL-4, IL-5, IL-9, IL-13). AS A RESULT B-LYMPHOCYTES PRODUCE ANTIBODIES OF IG E CLASS.
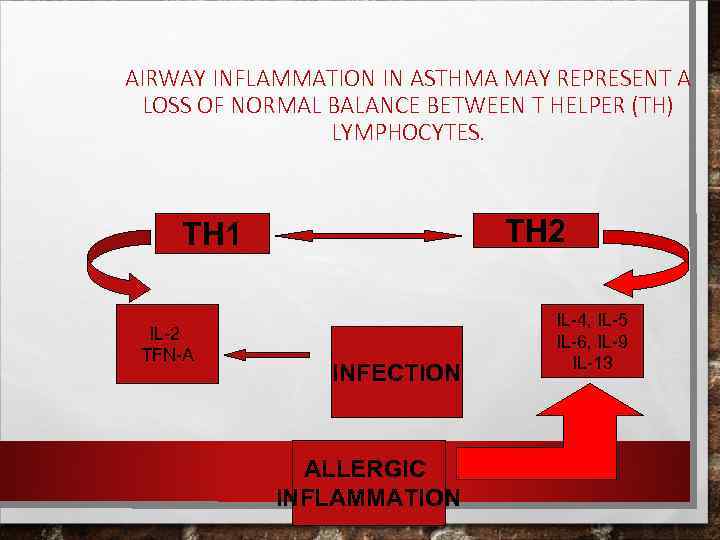 AIRWAY INFLAMMATION IN ASTHMA MAY REPRESENT A LOSS OF NORMAL BALANCE BETWEEN T HELPER (TH) LYMPHOCYTES. TH 2 TH 1 IL-2 TFN-Α INFECTION ALLERGIC INFLAMMATION IL-4, IL-5 IL-6, IL-9 IL-13
AIRWAY INFLAMMATION IN ASTHMA MAY REPRESENT A LOSS OF NORMAL BALANCE BETWEEN T HELPER (TH) LYMPHOCYTES. TH 2 TH 1 IL-2 TFN-Α INFECTION ALLERGIC INFLAMMATION IL-4, IL-5 IL-6, IL-9 IL-13
 • THE CURRENT "HYGIENE HYPOTHESIS" OF ASTHMA • ILLUSTRATES HOW THIS CYTOKINE IMBALANCE MAY EXPLAIN SOME OF THE DRAMATIC INCREASES IN ASTHMA PREVALENCE IN WESTERNIZED COUNTRIES. THIS HYPOTHESIS IS BASED ON THE CONCEPT THAT THE IMMUNE SYSTEM OF THE NEWBORN IS SKEWED TOWARD TH 2 CYTOKINE GENERATION (MEDIATORS OF ALLERGIC INFLAMMATION). OVER TIME, ENVIRONMENTAL STIMULI SUCH AS INFECTIONS ACTIVATE TH 1 RESPONSES AND BRING THE TH 1/TH 2 RELATIONSHIP TO AN APPROPRIATE BALANCE.
• THE CURRENT "HYGIENE HYPOTHESIS" OF ASTHMA • ILLUSTRATES HOW THIS CYTOKINE IMBALANCE MAY EXPLAIN SOME OF THE DRAMATIC INCREASES IN ASTHMA PREVALENCE IN WESTERNIZED COUNTRIES. THIS HYPOTHESIS IS BASED ON THE CONCEPT THAT THE IMMUNE SYSTEM OF THE NEWBORN IS SKEWED TOWARD TH 2 CYTOKINE GENERATION (MEDIATORS OF ALLERGIC INFLAMMATION). OVER TIME, ENVIRONMENTAL STIMULI SUCH AS INFECTIONS ACTIVATE TH 1 RESPONSES AND BRING THE TH 1/TH 2 RELATIONSHIP TO AN APPROPRIATE BALANCE.
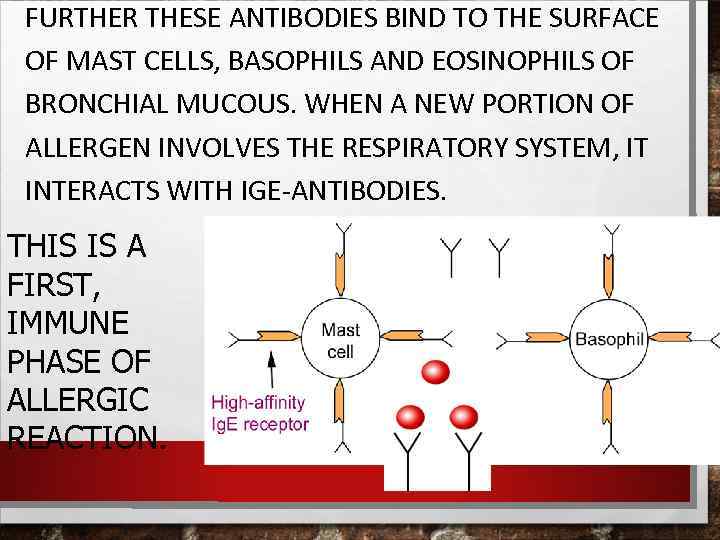 FURTHER THESE ANTIBODIES BIND TO THE SURFACE OF MAST CELLS, BASOPHILS AND EOSINOPHILS OF BRONCHIAL MUCOUS. WHEN A NEW PORTION OF ALLERGEN INVOLVES THE RESPIRATORY SYSTEM, IT INTERACTS WITH IGE-ANTIBODIES. THIS IS A FIRST, IMMUNE PHASE OF ALLERGIC REACTION.
FURTHER THESE ANTIBODIES BIND TO THE SURFACE OF MAST CELLS, BASOPHILS AND EOSINOPHILS OF BRONCHIAL MUCOUS. WHEN A NEW PORTION OF ALLERGEN INVOLVES THE RESPIRATORY SYSTEM, IT INTERACTS WITH IGE-ANTIBODIES. THIS IS A FIRST, IMMUNE PHASE OF ALLERGIC REACTION.
 PATHOCHEMICAL PHASE AS A RESULT OF ANTIGEN-ANTIBODY REACTION THE PECULIAR “EXPLOSION” OCCURS. ACTIVATED MUCOSAL MAST CELLS BASOPHILS AND EOSINOPHILS RELEASE BRONCHOCONSTRICTOR MEDIATORS AND AN OTHER BIOLOGICALLY ACTIVE SUBSTANCES (HISTAMINE, SEROTONIN, CHEMOTAXIS FACTORS, HEPARIN, PROTEASES, THROMBOXANE, LEUKOTRIENES, PROSTAGLANDINS), AIRWAY WHICH INDUCE HYPERERGIC MUSCLES FILL CONTRA WITH INFLAMMATION, MUCOUS MUCUS CT EDEMA, SPASM OF SMOOTH MYOCYTES, GLANDS HYPERSECRETION, VISCOUS EXUDATE FORMATION IN BRONCHIAL LUMEN. AIRWAYS SWELL
PATHOCHEMICAL PHASE AS A RESULT OF ANTIGEN-ANTIBODY REACTION THE PECULIAR “EXPLOSION” OCCURS. ACTIVATED MUCOSAL MAST CELLS BASOPHILS AND EOSINOPHILS RELEASE BRONCHOCONSTRICTOR MEDIATORS AND AN OTHER BIOLOGICALLY ACTIVE SUBSTANCES (HISTAMINE, SEROTONIN, CHEMOTAXIS FACTORS, HEPARIN, PROTEASES, THROMBOXANE, LEUKOTRIENES, PROSTAGLANDINS), AIRWAY WHICH INDUCE HYPERERGIC MUSCLES FILL CONTRA WITH INFLAMMATION, MUCOUS MUCUS CT EDEMA, SPASM OF SMOOTH MYOCYTES, GLANDS HYPERSECRETION, VISCOUS EXUDATE FORMATION IN BRONCHIAL LUMEN. AIRWAYS SWELL
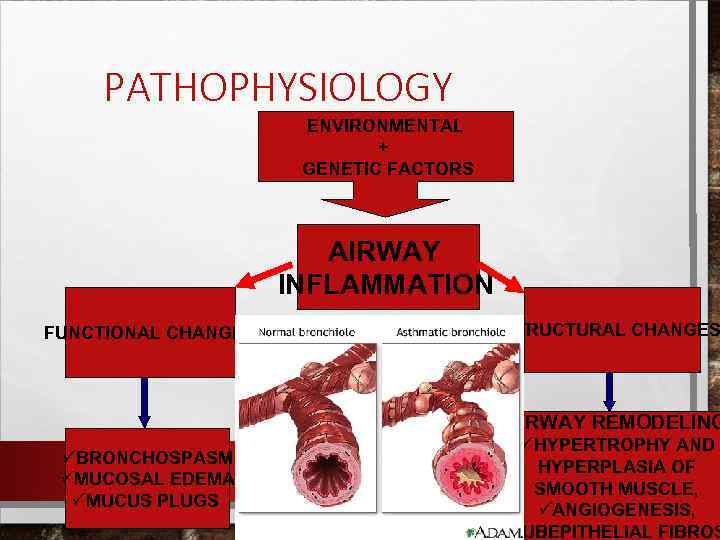 PATHOPHYSIOLOGY ENVIRONMENTAL + GENETIC FACTORS AIRWAY INFLAMMATION FUNCTIONAL CHANGES STRUCTURAL CHANGES AIRWAY REMODELING üBRONCHOSPASM üMUCOSAL EDEMA üMUCUS PLUGS üHYPERTROPHY AND HYPERPLASIA OF SMOOTH MUSCLE, üANGIOGENESIS, ü SUBEPITHELIAL FIBROS
PATHOPHYSIOLOGY ENVIRONMENTAL + GENETIC FACTORS AIRWAY INFLAMMATION FUNCTIONAL CHANGES STRUCTURAL CHANGES AIRWAY REMODELING üBRONCHOSPASM üMUCOSAL EDEMA üMUCUS PLUGS üHYPERTROPHY AND HYPERPLASIA OF SMOOTH MUSCLE, üANGIOGENESIS, ü SUBEPITHELIAL FIBROS
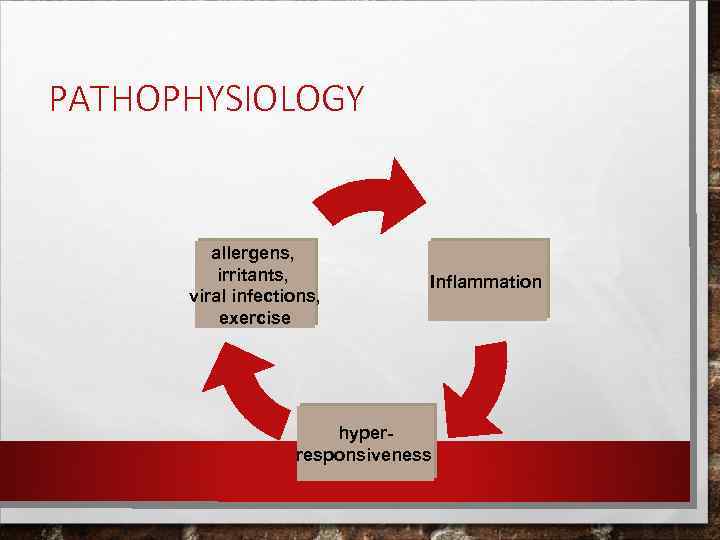 PATHOPHYSIOLOGY allergens, irritants, viral infections, exercise Inflammation hyperresponsiveness
PATHOPHYSIOLOGY allergens, irritants, viral infections, exercise Inflammation hyperresponsiveness
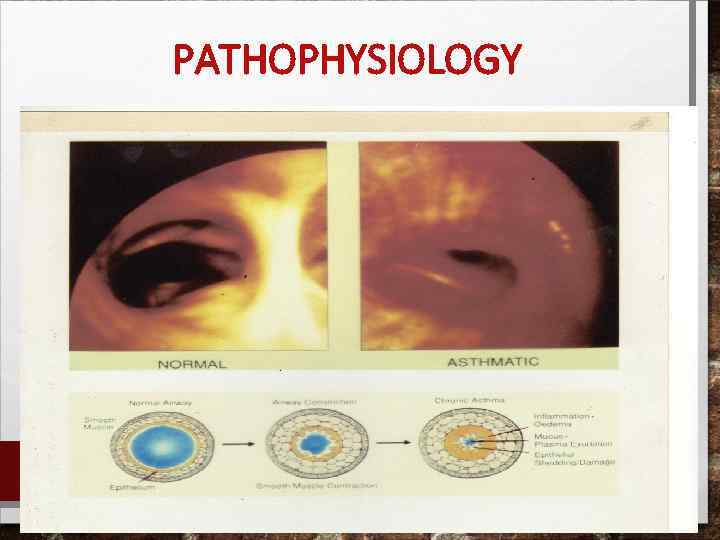 PATHOPHYSIOLOGY
PATHOPHYSIOLOGY
 CLINICAL MANIFESTATIONS ASTHMA IS CHARACTERIZED WITH PERIODICAL APPEARED PAROXYSMS OF EXPIRATORY DYSPNEA. CHILDREN WITH ASTHMA HAVE FOLLOWING SYMPTOMS: WHEEZING COUGHING (ESPECIALLY AT NIGHT OR WITH EXERCISE) SHORTNESS OF BREATH OR RAPID BREATHING CHEST TIGHTNESS • •
CLINICAL MANIFESTATIONS ASTHMA IS CHARACTERIZED WITH PERIODICAL APPEARED PAROXYSMS OF EXPIRATORY DYSPNEA. CHILDREN WITH ASTHMA HAVE FOLLOWING SYMPTOMS: WHEEZING COUGHING (ESPECIALLY AT NIGHT OR WITH EXERCISE) SHORTNESS OF BREATH OR RAPID BREATHING CHEST TIGHTNESS • •
 PHYSICAL EXAMINATION • TACHYPNEA, • TACHYCARDIA, • PROLONGED EXPIRATORY PHASE, • EXPIRATORY WHEEZING, • COARSE CRACKLES. • CYANOSIS, • DIMINISHED AIR MOVEMENT (TIGHT CHEST), • RETRACTIONS, • AGITATION, • INABILITY TO SPEAK, • TRIPOD SITTING POSITION, • SWEATING
PHYSICAL EXAMINATION • TACHYPNEA, • TACHYCARDIA, • PROLONGED EXPIRATORY PHASE, • EXPIRATORY WHEEZING, • COARSE CRACKLES. • CYANOSIS, • DIMINISHED AIR MOVEMENT (TIGHT CHEST), • RETRACTIONS, • AGITATION, • INABILITY TO SPEAK, • TRIPOD SITTING POSITION, • SWEATING
 PHYSICAL EXAMINATION • INFANTS HAVE FEEDING DIFFICULTIES AND A SOFTER, SHORTER CRY. • THE ANTEROPOSTERIOR DIAMETER OF THE CHEST MAY BE INCREASED BECAUSE OF HYPERINFLATION MAY ALSO CAUSE AN ABDOMINAL BREATHING PATTERN.
PHYSICAL EXAMINATION • INFANTS HAVE FEEDING DIFFICULTIES AND A SOFTER, SHORTER CRY. • THE ANTEROPOSTERIOR DIAMETER OF THE CHEST MAY BE INCREASED BECAUSE OF HYPERINFLATION MAY ALSO CAUSE AN ABDOMINAL BREATHING PATTERN.
 INVESTIGATIONS PULMONARY FUNCTION TESTS (IN CHILDRENS OLDER THAN 5 -6 YEARS OF AGE) • SPIROMETRY • PEAK FLOW METER • EXERCISE CHALLENGE • BRONCHIAL PROVOCATION TESTS
INVESTIGATIONS PULMONARY FUNCTION TESTS (IN CHILDRENS OLDER THAN 5 -6 YEARS OF AGE) • SPIROMETRY • PEAK FLOW METER • EXERCISE CHALLENGE • BRONCHIAL PROVOCATION TESTS
 TESTS FOR DIAGNOSIS AND MONITORING SPIROMETRY • IN A TYPICAL CASE, AN OBSTRUCTIVE DEFECT IS PRESENT IN THE FORM OF NORMAL FORCED VITAL CAPACITY (FVC), REDUCED FORCED EXPIRATORY VOLUME IN 1 SECOND (FEV 1), AND REDUCED FORCED EXPIRATORY FLOW MORE THAN 25 -75% OF THE FVC (FEF 25 -75).
TESTS FOR DIAGNOSIS AND MONITORING SPIROMETRY • IN A TYPICAL CASE, AN OBSTRUCTIVE DEFECT IS PRESENT IN THE FORM OF NORMAL FORCED VITAL CAPACITY (FVC), REDUCED FORCED EXPIRATORY VOLUME IN 1 SECOND (FEV 1), AND REDUCED FORCED EXPIRATORY FLOW MORE THAN 25 -75% OF THE FVC (FEF 25 -75).
 TESTS FOR DIAGNOSIS AND MONITORING PEAK EXPIRATORY FLOW METHOD 1. PEF VARIABILITY IS AS THE AMPLITUDE (THE DIFFERENCE BETWEEN THE MAXIMUM AND THE MINIMUM VALUE FOR THE DAY), EXPRESSED AS A PERCENTAGE OF THE MEAN DAILY PEF VALUE, AND AVERAGED OVER 1 -2 WEEKS METHOD 2. PEF VARIABILITY IS THE MINIMUM MORNING PRE-BRONCHODILATOR PEF OVER 1 WEEK, EXPRESSED AS A PERCENT OF THE RECENT BEST (MIN%MAX)
TESTS FOR DIAGNOSIS AND MONITORING PEAK EXPIRATORY FLOW METHOD 1. PEF VARIABILITY IS AS THE AMPLITUDE (THE DIFFERENCE BETWEEN THE MAXIMUM AND THE MINIMUM VALUE FOR THE DAY), EXPRESSED AS A PERCENTAGE OF THE MEAN DAILY PEF VALUE, AND AVERAGED OVER 1 -2 WEEKS METHOD 2. PEF VARIABILITY IS THE MINIMUM MORNING PRE-BRONCHODILATOR PEF OVER 1 WEEK, EXPRESSED AS A PERCENT OF THE RECENT BEST (MIN%MAX)
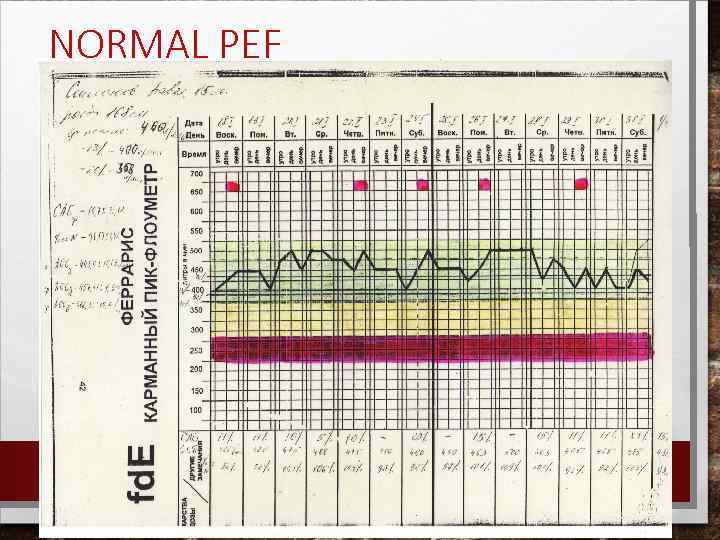 NORMAL PEF
NORMAL PEF
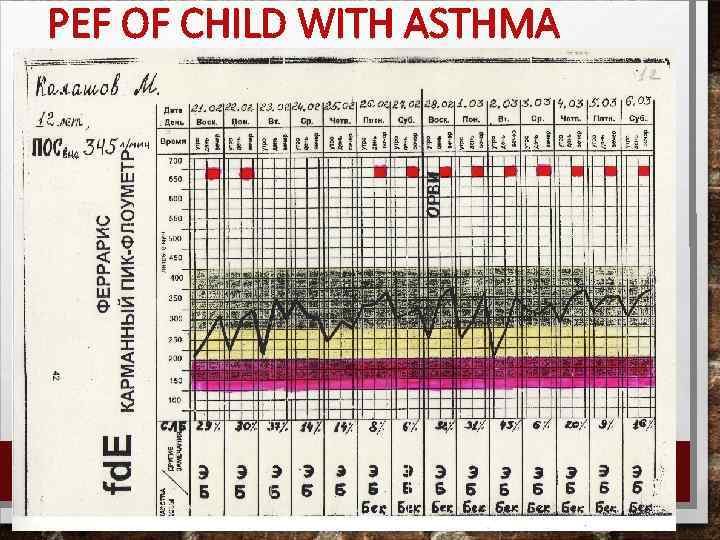 PEF OF CHILD WITH ASTHMA
PEF OF CHILD WITH ASTHMA
 INVESTIGATIONS • ALLERGY TESTING CAN BE USED TO IDENTIFY ALLERGIC • • • FACTORS EOSINOPHIL COUNTS IN BLOOD AND NASAL MUCOSA IGE LEVELS MAY BE USEFUL WHEN ALLERGIC FACTORS ARE SUSPECTED. A CHEST RADIOGRAPH MAY REVEAL EVIDENCE OF PARENCHYMAL DISEASE, ATELECTASIS, PNEUMONIA, CONGENITAL ANOMALY, OR A FOREIGN BODY AND MAY USE FOR DIAGNOSIS OF COMPLICATIONS (PNEUMOTHORAX OR PNEUMOMEDIASTINUM). TYPICAL FINDINGS ARE HYPERINFLATION AND INCREASED BRONCHIAL MARKINGS.
INVESTIGATIONS • ALLERGY TESTING CAN BE USED TO IDENTIFY ALLERGIC • • • FACTORS EOSINOPHIL COUNTS IN BLOOD AND NASAL MUCOSA IGE LEVELS MAY BE USEFUL WHEN ALLERGIC FACTORS ARE SUSPECTED. A CHEST RADIOGRAPH MAY REVEAL EVIDENCE OF PARENCHYMAL DISEASE, ATELECTASIS, PNEUMONIA, CONGENITAL ANOMALY, OR A FOREIGN BODY AND MAY USE FOR DIAGNOSIS OF COMPLICATIONS (PNEUMOTHORAX OR PNEUMOMEDIASTINUM). TYPICAL FINDINGS ARE HYPERINFLATION AND INCREASED BRONCHIAL MARKINGS.
 • ADDITIONAL STUDIES ARE NOT ROUTINELY NECESSARY, BUT THEY MAY BE USEFUL WHEN THE CLINICIAN IS CONSIDERING ALTERNATIVE DIAGNOSES. • FRACTION OF EXHALED NITRIC OXIDE TESTING • MEASURING THE FRACTION OF EXHALED NITRIC OXIDE HAS PROVED USEFUL AS A NONINVASIVE MARKER OF AIRWAY INFLAMMATION, IN ORDER TO GUIDE ADJUSTMENT OF THE DOSE OF INHALED CORTICOSTEROIDS.
• ADDITIONAL STUDIES ARE NOT ROUTINELY NECESSARY, BUT THEY MAY BE USEFUL WHEN THE CLINICIAN IS CONSIDERING ALTERNATIVE DIAGNOSES. • FRACTION OF EXHALED NITRIC OXIDE TESTING • MEASURING THE FRACTION OF EXHALED NITRIC OXIDE HAS PROVED USEFUL AS A NONINVASIVE MARKER OF AIRWAY INFLAMMATION, IN ORDER TO GUIDE ADJUSTMENT OF THE DOSE OF INHALED CORTICOSTEROIDS.
 DIFFERENTIAL DIAGNOSES • INFECTIONS • FOREIGN BODY ASPIRATION • CONGENITAL PROBLEMS: • CYSTIC FIBROSIS • BRONCHOPULMONARY DYSPLASIA • PRIMARY CILIARY DYSKINESIA • HYPERVENTILATION SYNDROME AND PANIC ATTACKS • VOCAL CORD DYSFUNCTION • NON-OBSTRUCTIVE FORMS OF LUNG DISEASE (E. G. , DIFFUSE • PARENCHYMAL LUNG DISEASE) NON-RESPIRATORY CAUSES OF SYMPTOMS (E. G. , LEFT VENTRICULAR FAILURE, GASTROESOPHAGEAL REFLUX )
DIFFERENTIAL DIAGNOSES • INFECTIONS • FOREIGN BODY ASPIRATION • CONGENITAL PROBLEMS: • CYSTIC FIBROSIS • BRONCHOPULMONARY DYSPLASIA • PRIMARY CILIARY DYSKINESIA • HYPERVENTILATION SYNDROME AND PANIC ATTACKS • VOCAL CORD DYSFUNCTION • NON-OBSTRUCTIVE FORMS OF LUNG DISEASE (E. G. , DIFFUSE • PARENCHYMAL LUNG DISEASE) NON-RESPIRATORY CAUSES OF SYMPTOMS (E. G. , LEFT VENTRICULAR FAILURE, GASTROESOPHAGEAL REFLUX )
 DIAGNOSTIC CHALLENGES AND DIFFERENTIAL CHILDREN 5 YEARS AND THREE CATEGORIES OF WHEEZING HAVE BEEN DESCRIBED INDIAGNOSIS YOUNGER: • TRANSIENT EARLY WHEEZING, WHICH IS OFTEN OUTGROWN IN • • THE FIRST 3 YEARS. THIS IS OFTEN ASSOCIATED WITH PREMATURITY AND PARENTAL SMOKING. PERSISTENT EARLY-ONSET WHEEZING (BEFORE AGE 3). RECURRENT EPISODES OF WHEEZING ASSOCIATED WITH ACUTE VIRAL RESPIRATORY INFECTIONS, WITHOUT ATOPY AND FAMILY HISTORY OF ATOPY. THE SYMPTOMS NORMALLY PERSIST THROUGH SCHOOL AGE AND ARE STILL PRESENT AT AGE 12 IN A LARGE PROPORTION OF CHILDREN. THE CAUSE OF THE EPISODE IS USUALLY THE RSV IN CHILDREN YOUNGER THAN AGE 2, WHILE OTHER VIRUSES PREDOMINATE IN OLDER PRESCHOOL CHILDREN. LATE-ONSET WHEEZING/ASTHMA. THESE CHILDREN HAVE ASTHMA WHICH OFTEN PERSISTS THROUGHOUT CHILDHOOD AND INTO ADULT LIFE. THEY TYPICALLY HAVE AN ATOPIC BACKGROUND, OFTEN WITH ECZEMA, AND AIRWAY PATHOLOGY IS CHARACTERISTIC OF ASTHMA.
DIAGNOSTIC CHALLENGES AND DIFFERENTIAL CHILDREN 5 YEARS AND THREE CATEGORIES OF WHEEZING HAVE BEEN DESCRIBED INDIAGNOSIS YOUNGER: • TRANSIENT EARLY WHEEZING, WHICH IS OFTEN OUTGROWN IN • • THE FIRST 3 YEARS. THIS IS OFTEN ASSOCIATED WITH PREMATURITY AND PARENTAL SMOKING. PERSISTENT EARLY-ONSET WHEEZING (BEFORE AGE 3). RECURRENT EPISODES OF WHEEZING ASSOCIATED WITH ACUTE VIRAL RESPIRATORY INFECTIONS, WITHOUT ATOPY AND FAMILY HISTORY OF ATOPY. THE SYMPTOMS NORMALLY PERSIST THROUGH SCHOOL AGE AND ARE STILL PRESENT AT AGE 12 IN A LARGE PROPORTION OF CHILDREN. THE CAUSE OF THE EPISODE IS USUALLY THE RSV IN CHILDREN YOUNGER THAN AGE 2, WHILE OTHER VIRUSES PREDOMINATE IN OLDER PRESCHOOL CHILDREN. LATE-ONSET WHEEZING/ASTHMA. THESE CHILDREN HAVE ASTHMA WHICH OFTEN PERSISTS THROUGHOUT CHILDHOOD AND INTO ADULT LIFE. THEY TYPICALLY HAVE AN ATOPIC BACKGROUND, OFTEN WITH ECZEMA, AND AIRWAY PATHOLOGY IS CHARACTERISTIC OF ASTHMA.
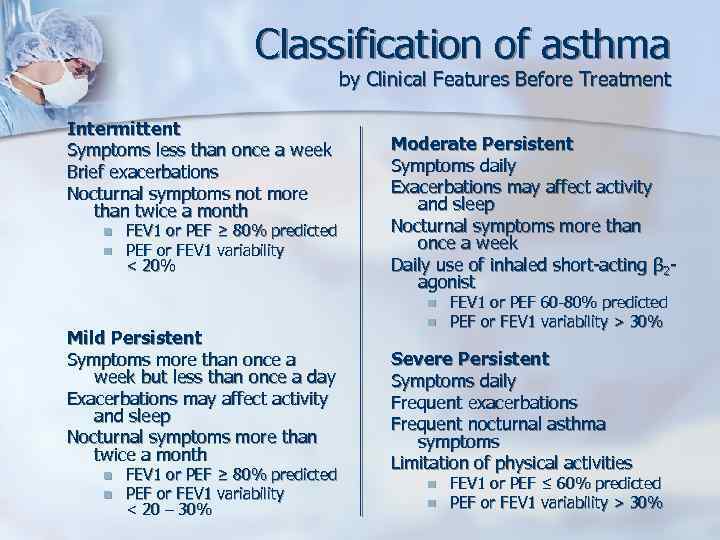 Classification of asthma by Clinical Features Before Treatment Intermittent Symptoms less than once a week Brief exacerbations Nocturnal symptoms not more than twice a month n n FEV 1 or PEF ≥ 80% predicted PEF or FEV 1 variability < 20% Mild Persistent Symptoms more than once a week but less than once a day Exacerbations may affect activity and sleep Nocturnal symptoms more than twice a month n n FEV 1 or PEF ≥ 80% predicted PEF or FEV 1 variability < 20 – 30% Moderate Persistent Symptoms daily Exacerbations may affect activity and sleep Nocturnal symptoms more than once a week Daily use of inhaled short-acting β 2 agonist n n FEV 1 or PEF 60 -80% predicted PEF or FEV 1 variability > 30% Severe Persistent Symptoms daily Frequent exacerbations Frequent nocturnal asthma symptoms Limitation of physical activities n n FEV 1 or PEF ≤ 60% predicted PEF or FEV 1 variability > 30%
Classification of asthma by Clinical Features Before Treatment Intermittent Symptoms less than once a week Brief exacerbations Nocturnal symptoms not more than twice a month n n FEV 1 or PEF ≥ 80% predicted PEF or FEV 1 variability < 20% Mild Persistent Symptoms more than once a week but less than once a day Exacerbations may affect activity and sleep Nocturnal symptoms more than twice a month n n FEV 1 or PEF ≥ 80% predicted PEF or FEV 1 variability < 20 – 30% Moderate Persistent Symptoms daily Exacerbations may affect activity and sleep Nocturnal symptoms more than once a week Daily use of inhaled short-acting β 2 agonist n n FEV 1 or PEF 60 -80% predicted PEF or FEV 1 variability > 30% Severe Persistent Symptoms daily Frequent exacerbations Frequent nocturnal asthma symptoms Limitation of physical activities n n FEV 1 or PEF ≤ 60% predicted PEF or FEV 1 variability > 30%
 CRITERIA OF SEVERITY OF BA ATTACKS. Signs Mild Moderate Severe Status asthmaticus Physical activity Preserved Limited Forced position Absent Speech Preserved Limited. Not fluent speech consists of separate phrases Absent Consciousne es Sometimes excitation Confused consciousnes s hypoxemic, hypoxemichypercapne mic - coma Excitation, fear, “breathing panic”
CRITERIA OF SEVERITY OF BA ATTACKS. Signs Mild Moderate Severe Status asthmaticus Physical activity Preserved Limited Forced position Absent Speech Preserved Limited. Not fluent speech consists of separate phrases Absent Consciousne es Sometimes excitation Confused consciousnes s hypoxemic, hypoxemichypercapne mic - coma Excitation, fear, “breathing panic”
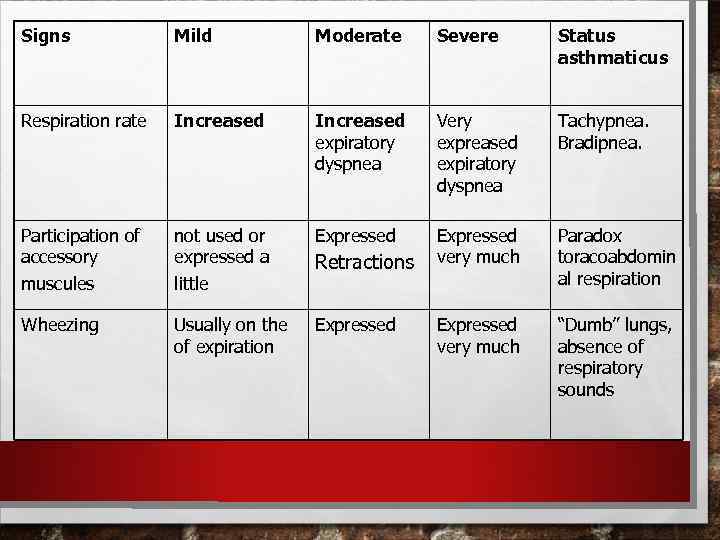 Signs Mild Moderate Severe Status asthmaticus Respiration rate Increased expiratory dyspnea Very expreased expiratory dyspnea Tachypnea. Bradipnea. Participation of accessory not used or expressed a Expressed very much muscules little Paradox toracoabdomin al respiration Wheezing Usually on the of expiration Expressed very much “Dumb” lungs, absence of respiratory sounds Retractions Expressed
Signs Mild Moderate Severe Status asthmaticus Respiration rate Increased expiratory dyspnea Very expreased expiratory dyspnea Tachypnea. Bradipnea. Participation of accessory not used or expressed a Expressed very much muscules little Paradox toracoabdomin al respiration Wheezing Usually on the of expiration Expressed very much “Dumb” lungs, absence of respiratory sounds Retractions Expressed
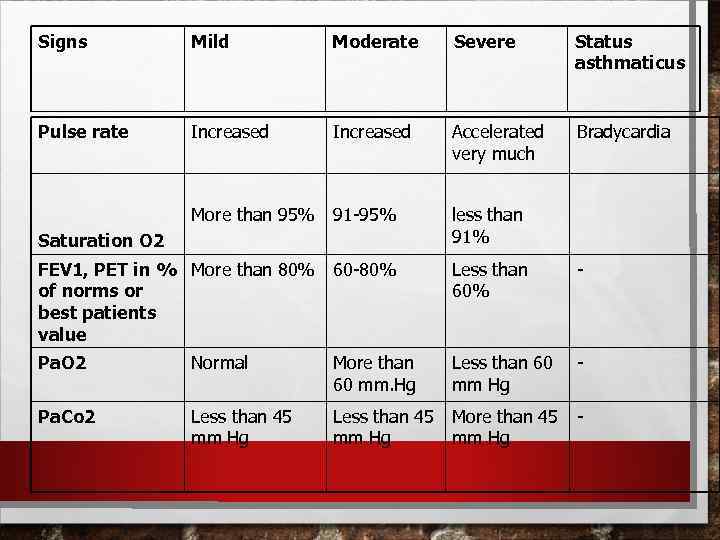 Signs Mild Moderate Severe Status asthmaticus Pulse rate Increased Accelerated very much Bradycardia More than 95% 91 -95% less than 91% FEV 1, PET in % More than 80% of norms or best patients value 60 -80% Less than 60% - Pa. O 2 Normal More than 60 mm. Hg Less than 60 mm Hg - Pa. Co 2 Less than 45 mm Hg More than 45 mm Hg - Saturation O 2
Signs Mild Moderate Severe Status asthmaticus Pulse rate Increased Accelerated very much Bradycardia More than 95% 91 -95% less than 91% FEV 1, PET in % More than 80% of norms or best patients value 60 -80% Less than 60% - Pa. O 2 Normal More than 60 mm. Hg Less than 60 mm Hg - Pa. Co 2 Less than 45 mm Hg More than 45 mm Hg - Saturation O 2
 COMPONENTS OF ASTHMA CARE • • ASSESSMENT AND MONITORING EDUCATION CONTROL OF ENVIRONMENTAL FACTORS AND COMORBID CONDITIONS PHARMACOLOGIC TREATMENT
COMPONENTS OF ASTHMA CARE • • ASSESSMENT AND MONITORING EDUCATION CONTROL OF ENVIRONMENTAL FACTORS AND COMORBID CONDITIONS PHARMACOLOGIC TREATMENT
 ASTHMA MANAGEMENT AND PREVENTION THE GOALS FOR SUCCESSFUL MANAGEMENT OF ASTHMA ARE TO: • ACHIEVE AND MAINTAIN CONTROL OF SYMPTOMS • MAINTAIN NORMAL ACTIVITY LEVELS, INCLUDING EXERCISE • MAINTAIN PULMONARY FUNCTION AS CLOSE TO NORMAL AS POSSIBLE • PREVENT ASTHMA EXACERBATIONS • AVOID ADVERSE EFFECTS FROM ASTHMA MEDICATIONS • PREVENT ASTHMA MORTALITY.
ASTHMA MANAGEMENT AND PREVENTION THE GOALS FOR SUCCESSFUL MANAGEMENT OF ASTHMA ARE TO: • ACHIEVE AND MAINTAIN CONTROL OF SYMPTOMS • MAINTAIN NORMAL ACTIVITY LEVELS, INCLUDING EXERCISE • MAINTAIN PULMONARY FUNCTION AS CLOSE TO NORMAL AS POSSIBLE • PREVENT ASTHMA EXACERBATIONS • AVOID ADVERSE EFFECTS FROM ASTHMA MEDICATIONS • PREVENT ASTHMA MORTALITY.
 ASSESSMENT AND MONITORING • ONCE THE PATIENT'S CONDITION IS CLASSIFIED AND THERAPY HAS BEEN INITIATED, CONTINUAL ASSESSMENT IS IMPORTANT FOR DISEASE CONTROL. ASTHMA CONTROL IS DEFINED AS "THE DEGREE TO WHICH THE MANIFESTATIONS OF ASTHMA ARE MINIMIZED BY THERAPEUTIC INTERVENTION AND THE GOALS OF THERAPY ARE MET. "
ASSESSMENT AND MONITORING • ONCE THE PATIENT'S CONDITION IS CLASSIFIED AND THERAPY HAS BEEN INITIATED, CONTINUAL ASSESSMENT IS IMPORTANT FOR DISEASE CONTROL. ASTHMA CONTROL IS DEFINED AS "THE DEGREE TO WHICH THE MANIFESTATIONS OF ASTHMA ARE MINIMIZED BY THERAPEUTIC INTERVENTION AND THE GOALS OF THERAPY ARE MET. "
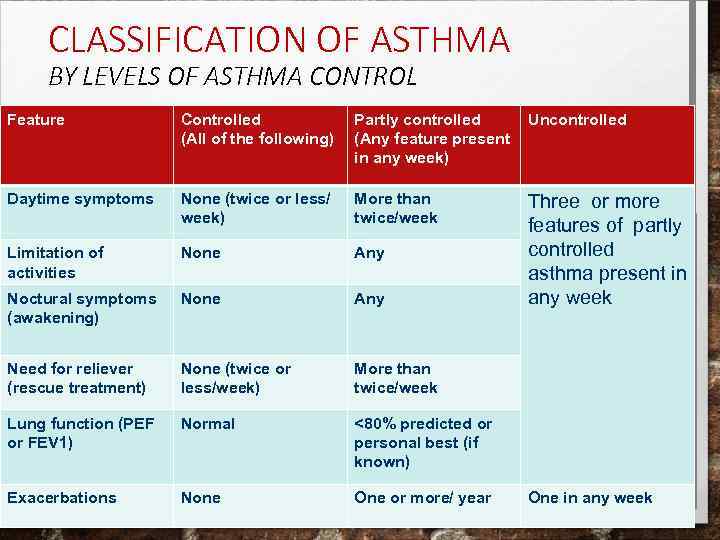 CLASSIFICATION OF ASTHMA BY LEVELS OF ASTHMA CONTROL Feature Controlled (All of the following) Partly controlled (Any feature present in any week) Uncontrolled Daytime symptoms None (twice or less/ week) More than twice/week Limitation of activities None Any Noctural symptoms (awakening) None Any Three or more features of partly controlled asthma present in any week Need for reliever (rescue treatment) None (twice or less/week) More than twice/week Lung function (PEF or FEV 1) Normal <80% predicted or personal best (if known) Exacerbations None One or more/ year One in any week
CLASSIFICATION OF ASTHMA BY LEVELS OF ASTHMA CONTROL Feature Controlled (All of the following) Partly controlled (Any feature present in any week) Uncontrolled Daytime symptoms None (twice or less/ week) More than twice/week Limitation of activities None Any Noctural symptoms (awakening) None Any Three or more features of partly controlled asthma present in any week Need for reliever (rescue treatment) None (twice or less/week) More than twice/week Lung function (PEF or FEV 1) Normal <80% predicted or personal best (if known) Exacerbations None One or more/ year One in any week
 EDUCATION • PATIENT EDUCATION INCLUDING ATTAINMENT OF SELF- • MANAGEMENT SKILLS. SELF-MANAGEMENT EDUCATION SHOULD FOCUS ON TEACHING PATIENTS THE IMPORTANCE OF RECOGNIZING THEIR OWN THEIR LEVEL OF CONTROL AND SIGNS OF PROGRESSIVELY WORSENING ASTHMA SYMPTOMS. PATIENT AND PARENT EDUCATION SHOULD INCLUDE INSTRUCTIONS ON HOW TO USE MEDICATIONS AND DEVICES (EG, SPACERS, NEBULIZERS, METERED-DOSE INHALERS [MDIS]). EDUCATIONAL STRATEGIES SHOULD ALSO FOCUS ON ENVIRONMENTAL CONTROL AND AVOIDANCE STRATEGIES AND MEDICATION USE AND ADHERENCE (EG, CORRECT INHALER TECHNIQUES AND USE OF OTHER DEVICES).
EDUCATION • PATIENT EDUCATION INCLUDING ATTAINMENT OF SELF- • MANAGEMENT SKILLS. SELF-MANAGEMENT EDUCATION SHOULD FOCUS ON TEACHING PATIENTS THE IMPORTANCE OF RECOGNIZING THEIR OWN THEIR LEVEL OF CONTROL AND SIGNS OF PROGRESSIVELY WORSENING ASTHMA SYMPTOMS. PATIENT AND PARENT EDUCATION SHOULD INCLUDE INSTRUCTIONS ON HOW TO USE MEDICATIONS AND DEVICES (EG, SPACERS, NEBULIZERS, METERED-DOSE INHALERS [MDIS]). EDUCATIONAL STRATEGIES SHOULD ALSO FOCUS ON ENVIRONMENTAL CONTROL AND AVOIDANCE STRATEGIES AND MEDICATION USE AND ADHERENCE (EG, CORRECT INHALER TECHNIQUES AND USE OF OTHER DEVICES).
 PHARMACOLOGIC TREATMENT • CONTROL AGENTS INCLUDE INHALED CORTICOSTEROIDS, INHALED CROMOLYN OR NEDOCROMIL, LONG-ACTING BRONCHODILATORS, THEOPHYLLINE, LEUKOTRIENE MODIFIERS, AND MORE RECENT STRATEGIES SUCH AS THE USE OF ANTIIMMUNOGLOBULIN E (IGE) ANTIBODIES (OMALIZUMAB). • RELIEF MEDICATIONS INCLUDE SHORT-ACTING BRONCHODILATORS, SYSTEMIC CORTICOSTEROIDS, AND IPRATROPIUM.
PHARMACOLOGIC TREATMENT • CONTROL AGENTS INCLUDE INHALED CORTICOSTEROIDS, INHALED CROMOLYN OR NEDOCROMIL, LONG-ACTING BRONCHODILATORS, THEOPHYLLINE, LEUKOTRIENE MODIFIERS, AND MORE RECENT STRATEGIES SUCH AS THE USE OF ANTIIMMUNOGLOBULIN E (IGE) ANTIBODIES (OMALIZUMAB). • RELIEF MEDICATIONS INCLUDE SHORT-ACTING BRONCHODILATORS, SYSTEMIC CORTICOSTEROIDS, AND IPRATROPIUM.
 LONG-TERM CONTROL MEDICATIONS • INHALED CORTICOSTEROIDS ARE THE MOST EFFECTIVE ANTI- INFLAMMATORY MEDICATIONS FOR THE TREATMENT OF CHRONIC, PERSISTENT ASTHMA. INHALED FORMS ARE TOPICALLY ACTIVE, POORLY ABSORBED, AND LEAST LIKELY TO CAUSE ADVERSE EFFECTS. INHALED STEROIDS BLOCK LATE ASTHMATIC RESPONSE TO ALLERGENS; REDUCE AIRWAY HYPERRESPONSIVENESS; INHIBIT CYTOKINE PRODUCTION, ADHESION PROTEIN ACTIVATION, AND INFLAMMATORY CELL MIGRATION AND ACTIVATION; AND REVERSE BETA 2 -RECEPTOR DOWNREGULATION AND SUBSENSITIVITY. INHALED CORTICOSTEROIDS INCLUDE BECLOMETHASONE, BUDESONIDE, FLUNISOLIDE, FLUTICASONE, AND TRIAMCINOLONE, WITH MOMETASONE FORTHCOMING.
LONG-TERM CONTROL MEDICATIONS • INHALED CORTICOSTEROIDS ARE THE MOST EFFECTIVE ANTI- INFLAMMATORY MEDICATIONS FOR THE TREATMENT OF CHRONIC, PERSISTENT ASTHMA. INHALED FORMS ARE TOPICALLY ACTIVE, POORLY ABSORBED, AND LEAST LIKELY TO CAUSE ADVERSE EFFECTS. INHALED STEROIDS BLOCK LATE ASTHMATIC RESPONSE TO ALLERGENS; REDUCE AIRWAY HYPERRESPONSIVENESS; INHIBIT CYTOKINE PRODUCTION, ADHESION PROTEIN ACTIVATION, AND INFLAMMATORY CELL MIGRATION AND ACTIVATION; AND REVERSE BETA 2 -RECEPTOR DOWNREGULATION AND SUBSENSITIVITY. INHALED CORTICOSTEROIDS INCLUDE BECLOMETHASONE, BUDESONIDE, FLUNISOLIDE, FLUTICASONE, AND TRIAMCINOLONE, WITH MOMETASONE FORTHCOMING.
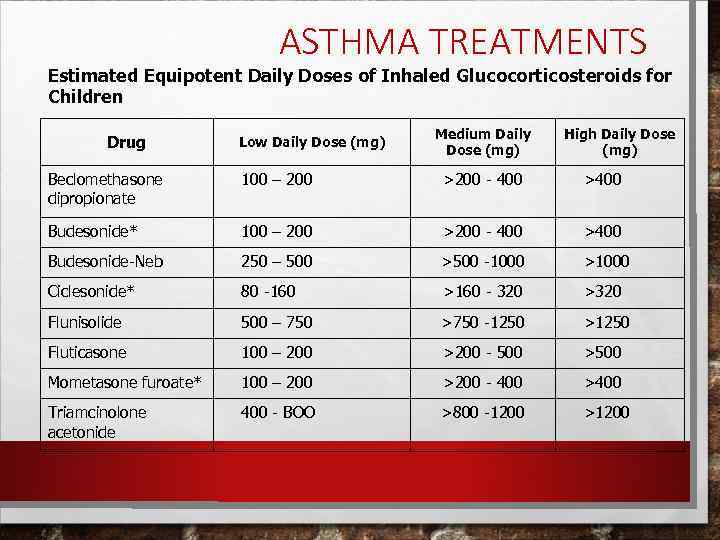 ASTHMA TREATMENTS Estimated Equipotent Daily Doses of Inhaled Glucocorticosteroids for Children Drug Low Daily Dose (mg) Medium Daily Dose (mg) High Daily Dose (mg) Beclomethasone dipropionate 100 – 200 >200 - 400 >400 Budesonide* 100 – 200 >200 - 400 >400 Budesonide-Neb 250 – 500 >500 -1000 >1000 Ciclesonide* 80 -160 >160 - 320 >320 Flunisolide 500 – 750 >750 -1250 >1250 Fluticasone 100 – 200 >200 - 500 >500 Mometasone furoate* 100 – 200 >200 - 400 >400 Triamcinolone acetonide 400 - BOO >800 -1200 >1200
ASTHMA TREATMENTS Estimated Equipotent Daily Doses of Inhaled Glucocorticosteroids for Children Drug Low Daily Dose (mg) Medium Daily Dose (mg) High Daily Dose (mg) Beclomethasone dipropionate 100 – 200 >200 - 400 >400 Budesonide* 100 – 200 >200 - 400 >400 Budesonide-Neb 250 – 500 >500 -1000 >1000 Ciclesonide* 80 -160 >160 - 320 >320 Flunisolide 500 – 750 >750 -1250 >1250 Fluticasone 100 – 200 >200 - 500 >500 Mometasone furoate* 100 – 200 >200 - 400 >400 Triamcinolone acetonide 400 - BOO >800 -1200 >1200
 • INHALER DEVICES CURRENTLY USED TO DELIVER INHALED CORTICOSTEROIDS (ICSS) FALL INTO THE FOLLOWING 4 CATEGORIES: • PRESSURIZED METERED DOSE INHALER (PMDI) - PROPELLANT USED TO DISPENSE STEROID WHEN CANISTER IS PRESSED MANUALLY • BREATH-ACTUATED PMDI - PROPELLANT USED TO DISPENSE STEROID WHEN PATIENT INHALES • DRY POWDER INHALER (DPI) - DOES NOT REQUIRE HAND-BREATH COORDINATION TO OPERATE • NEBULIZED SOLUTION DEVICES
• INHALER DEVICES CURRENTLY USED TO DELIVER INHALED CORTICOSTEROIDS (ICSS) FALL INTO THE FOLLOWING 4 CATEGORIES: • PRESSURIZED METERED DOSE INHALER (PMDI) - PROPELLANT USED TO DISPENSE STEROID WHEN CANISTER IS PRESSED MANUALLY • BREATH-ACTUATED PMDI - PROPELLANT USED TO DISPENSE STEROID WHEN PATIENT INHALES • DRY POWDER INHALER (DPI) - DOES NOT REQUIRE HAND-BREATH COORDINATION TO OPERATE • NEBULIZED SOLUTION DEVICES
 ASTHMA TREATMENTS Choosing an Inhaler Device for Children with Asthma Age Group Preferred Device Alternate Device Younger than 4 years Pressurized metereddose inhaler plus dedicated spacer with face mask Nebulizer with face mask 4 – 6 years Pressurized metereddose inhaler plus dedicated spacer with mouthpiece Nebulizer with mouthpiece Older than 6 years Dry powder inhaler, or breath-actuated ressurized metereddose inhaler, or pressurized metereddose inhaler with spacer and mouthpiece Nebulizer with Mouthpiece
ASTHMA TREATMENTS Choosing an Inhaler Device for Children with Asthma Age Group Preferred Device Alternate Device Younger than 4 years Pressurized metereddose inhaler plus dedicated spacer with face mask Nebulizer with face mask 4 – 6 years Pressurized metereddose inhaler plus dedicated spacer with mouthpiece Nebulizer with mouthpiece Older than 6 years Dry powder inhaler, or breath-actuated ressurized metereddose inhaler, or pressurized metereddose inhaler with spacer and mouthpiece Nebulizer with Mouthpiece
 NEBULIZER TREATMENT
NEBULIZER TREATMENT
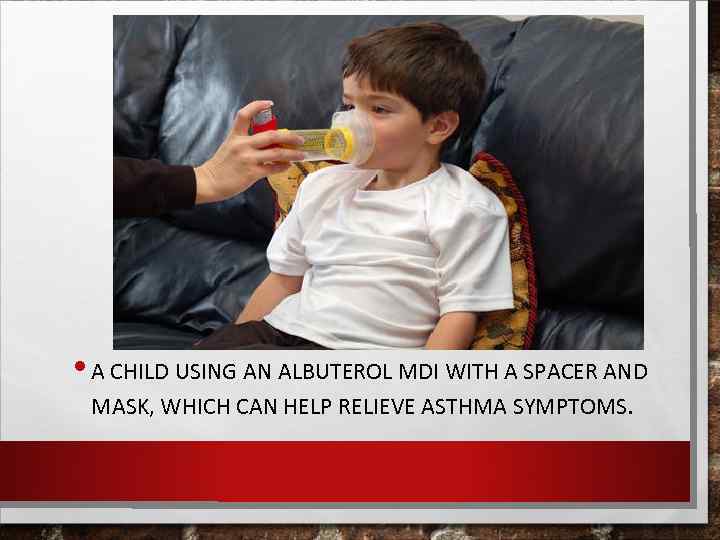 • A CHILD USING AN ALBUTEROL MDI WITH A SPACER AND MASK, WHICH CAN HELP RELIEVE ASTHMA SYMPTOMS.
• A CHILD USING AN ALBUTEROL MDI WITH A SPACER AND MASK, WHICH CAN HELP RELIEVE ASTHMA SYMPTOMS.
 • THIS PRESCHOOL AGE CHILD IS TOO YOUNG TO USE A METERED DOSE INHALER BY ITSELF, AND WOULD BE BETTER OFF USING IT WITH A SPACER AND MASK. • A CHILD USING ADVAIR TO HELP PREVENT HIS ASTHMA SYMPTOMS.
• THIS PRESCHOOL AGE CHILD IS TOO YOUNG TO USE A METERED DOSE INHALER BY ITSELF, AND WOULD BE BETTER OFF USING IT WITH A SPACER AND MASK. • A CHILD USING ADVAIR TO HELP PREVENT HIS ASTHMA SYMPTOMS.
 TREATMENT OF BA BASED ON THE LEVEL DISEASE CONTROL Level of control Terapeutic action Controled BA Choose the minimal basic therapy to achieve the control Partly controlled BA Consider the necessity of increasing of therapy (“step up”) for echievement of control Uncontrolled BA Increasing therapy till control of BA is achieved Exacerbation To treat as exacerbation STEP BY STEP THERAPY
TREATMENT OF BA BASED ON THE LEVEL DISEASE CONTROL Level of control Terapeutic action Controled BA Choose the minimal basic therapy to achieve the control Partly controlled BA Consider the necessity of increasing of therapy (“step up”) for echievement of control Uncontrolled BA Increasing therapy till control of BA is achieved Exacerbation To treat as exacerbation STEP BY STEP THERAPY
 ASTHMA MANAGEMENT APPROACH BASED ON CONTROL FOR CHILDREN 5 YEARS AND YANGER RECOMMENDATIONS OF GINA (2009) BA UNDER CONTROL - CONTROLLED ON AS NEEDED RAPID Β 2 AGONISTS PARTLY CONTROLLED BA – LOWDOSE ICS OR ANTLEUKOTRIENE DRUG UNCONTROLLED BA - DOUBLE LOW-DOSE INHALED GLUCOCORTICOSTEROID ICS + ANTLEUKOTRIENE DRUG
ASTHMA MANAGEMENT APPROACH BASED ON CONTROL FOR CHILDREN 5 YEARS AND YANGER RECOMMENDATIONS OF GINA (2009) BA UNDER CONTROL - CONTROLLED ON AS NEEDED RAPID Β 2 AGONISTS PARTLY CONTROLLED BA – LOWDOSE ICS OR ANTLEUKOTRIENE DRUG UNCONTROLLED BA - DOUBLE LOW-DOSE INHALED GLUCOCORTICOSTEROID ICS + ANTLEUKOTRIENE DRUG
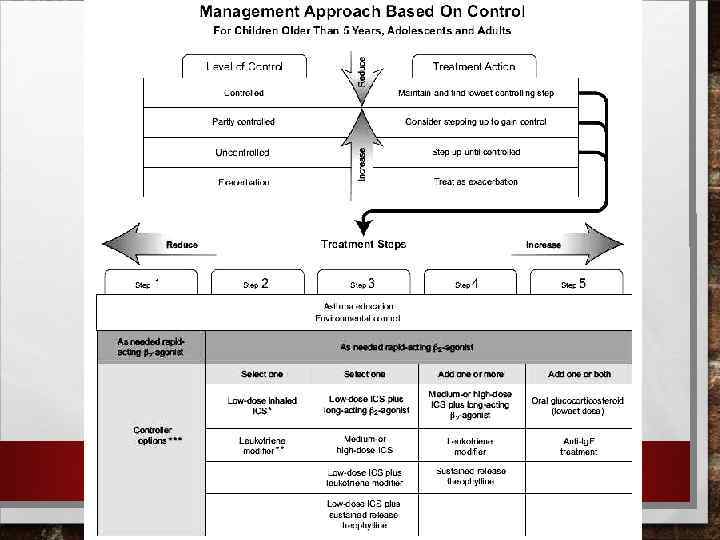
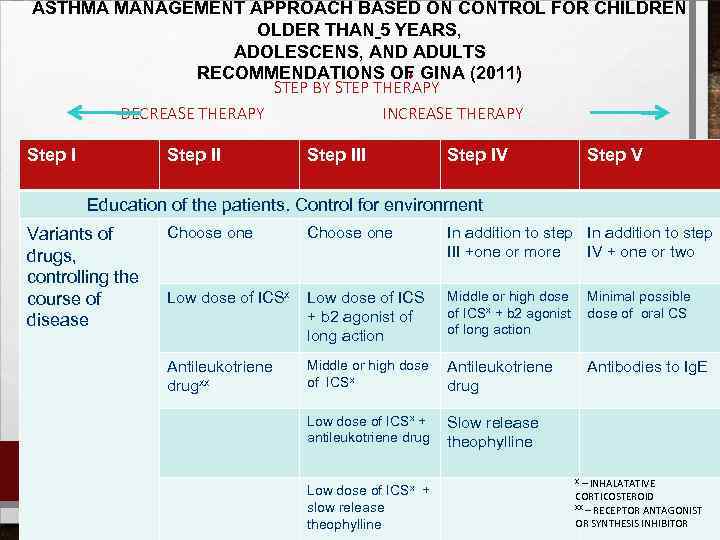 ASTHMA MANAGEMENT APPROACH BASED ON CONTROL FOR CHILDREN OLDER THAN 5 YEARS, ADOLESCENS, AND ADULTS RECOMMENDATIONS OF GINA (2011) STEP BY STEP THERAPY DECREASE THERAPY INCREASE THERAPY Step III Step IV Step V Education of the patients. Control for environment Variants of drugs, controlling the course of disease Choose one In addition to step III +one or more IV + one or two Low dose of ICSx Low dose of ICS + b 2 agonist of long action Middle or high dose of ICSx + b 2 agonist of long action Minimal possible dose of oral CS Antileukotriene drugxx Middle or high dose of ICSx Antileukotriene drug Antibodies to Ig. E Low dose of ICSx + antileukotriene drug Slow release theophylline Low dose of ICSx + slow release theophylline X – INHALATATIVE CORTICOSTEROID XX – RECEPTOR ANTAGONIST OR SYNTHESIS INHIBITOR
ASTHMA MANAGEMENT APPROACH BASED ON CONTROL FOR CHILDREN OLDER THAN 5 YEARS, ADOLESCENS, AND ADULTS RECOMMENDATIONS OF GINA (2011) STEP BY STEP THERAPY DECREASE THERAPY INCREASE THERAPY Step III Step IV Step V Education of the patients. Control for environment Variants of drugs, controlling the course of disease Choose one In addition to step III +one or more IV + one or two Low dose of ICSx Low dose of ICS + b 2 agonist of long action Middle or high dose of ICSx + b 2 agonist of long action Minimal possible dose of oral CS Antileukotriene drugxx Middle or high dose of ICSx Antileukotriene drug Antibodies to Ig. E Low dose of ICSx + antileukotriene drug Slow release theophylline Low dose of ICSx + slow release theophylline X – INHALATATIVE CORTICOSTEROID XX – RECEPTOR ANTAGONIST OR SYNTHESIS INHIBITOR
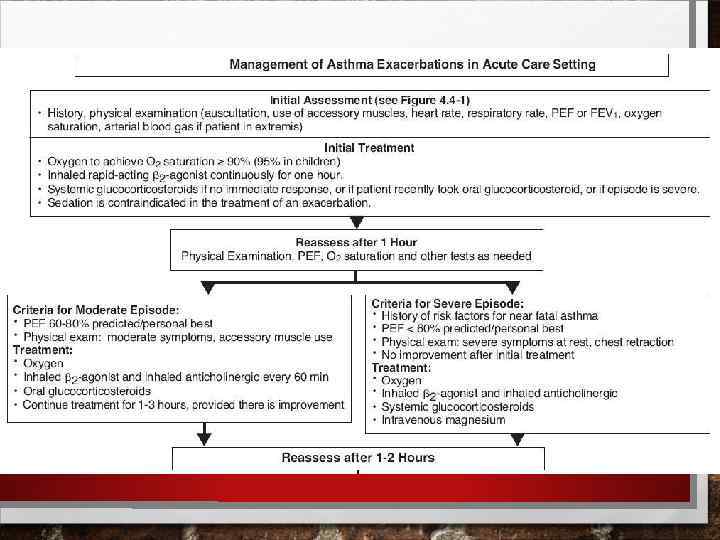
 ASTHMA COMPLICATIONS THE COMPLICATIONS OF ASTHMA EXACERBATIONS ARE: • PNEUMOTHORAX • LUNG ATELECTASIS • PNEUMONIA • ACUTE OR SUBACUTE COR PULMONALE • STATUS ASTHMATICUS PERSISTENT ASTHMA CAUSES: • FIBROSING BRONCHITIS • SMALL BRONCHI DEFORMATION AND OBLITERATION • EMPHYSEMA • PNEUMOSCLEROSIS, • CHRONIC RESPIRATORY FAILURE • CHRONIC COR PULMONALE. STHMA IN CHILDHOOD LEADS TO GROWTH INHIBITION AND THORACIC DEFORMATION.
ASTHMA COMPLICATIONS THE COMPLICATIONS OF ASTHMA EXACERBATIONS ARE: • PNEUMOTHORAX • LUNG ATELECTASIS • PNEUMONIA • ACUTE OR SUBACUTE COR PULMONALE • STATUS ASTHMATICUS PERSISTENT ASTHMA CAUSES: • FIBROSING BRONCHITIS • SMALL BRONCHI DEFORMATION AND OBLITERATION • EMPHYSEMA • PNEUMOSCLEROSIS, • CHRONIC RESPIRATORY FAILURE • CHRONIC COR PULMONALE. STHMA IN CHILDHOOD LEADS TO GROWTH INHIBITION AND THORACIC DEFORMATION.
 LONG-TERM MONITORING • REGULAR FOLLOW-UP VISITS ARE ESSENTIAL TO ENSURE CONTROL AND APPROPRIATE THERAPEUTIC ADJUSTMENTS. IN GENERAL, PATIENTS SHOULD BE ASSESSED EVERY 1 -6 MONTHS. AT EVERY VISIT, ADHERENCE, ENVIRONMENTAL CONTROL, AND COMORBID CONDITIONS SHOULD BE CHECKED. • IF PATIENTS HAVE GOOD CONTROL OF THEIR ASTHMA FOR AT LEAST 3 MONTHS, TREATMENT CAN BE STEPPED DOWN. HOWEVER, THE PATIENT SHOULD BE REASSESSED IN 2 -4 WEEKS TO MAKE SURE THAT CONTROL IS MAINTAINED WITH THE NEW REGIMEN.
LONG-TERM MONITORING • REGULAR FOLLOW-UP VISITS ARE ESSENTIAL TO ENSURE CONTROL AND APPROPRIATE THERAPEUTIC ADJUSTMENTS. IN GENERAL, PATIENTS SHOULD BE ASSESSED EVERY 1 -6 MONTHS. AT EVERY VISIT, ADHERENCE, ENVIRONMENTAL CONTROL, AND COMORBID CONDITIONS SHOULD BE CHECKED. • IF PATIENTS HAVE GOOD CONTROL OF THEIR ASTHMA FOR AT LEAST 3 MONTHS, TREATMENT CAN BE STEPPED DOWN. HOWEVER, THE PATIENT SHOULD BE REASSESSED IN 2 -4 WEEKS TO MAKE SURE THAT CONTROL IS MAINTAINED WITH THE NEW REGIMEN.
 LONG-TERM MONITORING • OUTPATIENT VISITS SHOULD INCLUDE THE FOLLOWING: • INTERVAL HISTORY OF ASTHMATIC COMPLAINTS, INCLUDING • • HISTORY OF ACUTE EPISODES (EG, SEVERITY, MEASURES AND TREATMENT TAKEN, RESPONSE TO THERAPY) HISTORY OF NOCTURNAL SYMPTOMS HISTORY OF SYMPTOMS WITH EXERCISE, AND EXERCISE TOLERANCE REVIEW OF MEDICATIONS, INCLUDING USE OF RESCUE MEDICATIONS REVIEW OF HOME-MONITORING DATA (EG, SYMPTOM DIARY, PEAK FLOW METER READINGS, DAILY TREATMENTS)
LONG-TERM MONITORING • OUTPATIENT VISITS SHOULD INCLUDE THE FOLLOWING: • INTERVAL HISTORY OF ASTHMATIC COMPLAINTS, INCLUDING • • HISTORY OF ACUTE EPISODES (EG, SEVERITY, MEASURES AND TREATMENT TAKEN, RESPONSE TO THERAPY) HISTORY OF NOCTURNAL SYMPTOMS HISTORY OF SYMPTOMS WITH EXERCISE, AND EXERCISE TOLERANCE REVIEW OF MEDICATIONS, INCLUDING USE OF RESCUE MEDICATIONS REVIEW OF HOME-MONITORING DATA (EG, SYMPTOM DIARY, PEAK FLOW METER READINGS, DAILY TREATMENTS)
 LONG-TERM MONITORING • PATIENT EVALUATION SHOULD INCLUDE THE FOLLOWING: • ASSESSMENT FOR SIGNS OF BRONCHOSPASM AND COMPLICATIONS • EVALUATION OF ASSOCIATED CONDITIONS (EG, ALLERGIC RHINITIS) • PULMONARY FUNCTION TESTING (IN APPROPRIATE AGE GROUP) • ADDRESS ISSUES OF TREATMENT ADHERENCE AND AVOIDANCE OF ENVIRONMENTAL TRIGGERS AND IRRITANTS.
LONG-TERM MONITORING • PATIENT EVALUATION SHOULD INCLUDE THE FOLLOWING: • ASSESSMENT FOR SIGNS OF BRONCHOSPASM AND COMPLICATIONS • EVALUATION OF ASSOCIATED CONDITIONS (EG, ALLERGIC RHINITIS) • PULMONARY FUNCTION TESTING (IN APPROPRIATE AGE GROUP) • ADDRESS ISSUES OF TREATMENT ADHERENCE AND AVOIDANCE OF ENVIRONMENTAL TRIGGERS AND IRRITANTS.
 • REMOVAL OR AVOIDANCE OF THE OFFENDING ALLERGEN IS PREVENTION ADVISED. • THE ONLY EFFECTIVE MEASURE FOR MINIMIZING ANIMAL ALLERGENS FROM PETS IS REMOVAL OF THE PET FROM THE • • HOME. AVOIDANCE OF POLLEN AND OUTDOOR MOLDS CAN BE ACCOMPLISHED BY STAYING INDOORS IN A CONTROLLED ENVIRONMENT. AIR CONDITIONING AND KEEPING WINDOWS AND DOORS CLOSED LOWER EXPOSURE TO POLLEN. HEPA FILTERS REDUCE THE COUNTS OF AIRBORNE MOLD SPORES. SEALING THE MATTRESS, PILLOW, AND COVERS IN ALLERGEN-PROOF ENCASINGS IS THE MOST EFFECTIVE STRATEGY FOR REDUCTION OF MITE ALLERGEN. BED LINENS AND BLANKETS SHOULD BE WASHED IN HOT WATER (>60°C) EVERY WEEK.
• REMOVAL OR AVOIDANCE OF THE OFFENDING ALLERGEN IS PREVENTION ADVISED. • THE ONLY EFFECTIVE MEASURE FOR MINIMIZING ANIMAL ALLERGENS FROM PETS IS REMOVAL OF THE PET FROM THE • • HOME. AVOIDANCE OF POLLEN AND OUTDOOR MOLDS CAN BE ACCOMPLISHED BY STAYING INDOORS IN A CONTROLLED ENVIRONMENT. AIR CONDITIONING AND KEEPING WINDOWS AND DOORS CLOSED LOWER EXPOSURE TO POLLEN. HEPA FILTERS REDUCE THE COUNTS OF AIRBORNE MOLD SPORES. SEALING THE MATTRESS, PILLOW, AND COVERS IN ALLERGEN-PROOF ENCASINGS IS THE MOST EFFECTIVE STRATEGY FOR REDUCTION OF MITE ALLERGEN. BED LINENS AND BLANKETS SHOULD BE WASHED IN HOT WATER (>60°C) EVERY WEEK.
 EDUCATIONAL MATERIALS BASED ON THIS GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION ARE AVAILABLE IN SEVERAL FORMS, INCLUDING A POCKET GUIDE FOR HEALTH CARE PROFESSIONALS AND ONE FOR PATIENTS AND FAMILIES. THESE ARE AVAILABLE ON THE GINA WEBSITE (HTTP: //WWW. GINASTHMA. ORG). EACH YEAR, THE GINA SCIENCE COMMITTEE EXAMINES PEERREVIEWED LITERATURE ON ASTHMA MANAGEMENT AND UPDATES VARIOUS GINA DOCUMENTS. A REPORT OF A GINA WORKING GROUP PROVIDES A BLUEPRINT FOR
EDUCATIONAL MATERIALS BASED ON THIS GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION ARE AVAILABLE IN SEVERAL FORMS, INCLUDING A POCKET GUIDE FOR HEALTH CARE PROFESSIONALS AND ONE FOR PATIENTS AND FAMILIES. THESE ARE AVAILABLE ON THE GINA WEBSITE (HTTP: //WWW. GINASTHMA. ORG). EACH YEAR, THE GINA SCIENCE COMMITTEE EXAMINES PEERREVIEWED LITERATURE ON ASTHMA MANAGEMENT AND UPDATES VARIOUS GINA DOCUMENTS. A REPORT OF A GINA WORKING GROUP PROVIDES A BLUEPRINT FOR


