cdebfa2863360f16217aa8d21a05e5a2.ppt
- Количество слайдов: 69

Antibiotic Stewardship Katherine Shea, Pharm. D. , BCPS-AQ-ID Theresa Jaso, Pharm. D. BCPS-AQ-ID Clinical Pharmacy Specialists, Infectious Diseases Seton Healthcare Family

Objectives l Understand the rationale and importance of antibiotic stewardship l Identify key points from the antimicrobial stewardship guidelines l Recognize the necessary components of a stewardship program l Identify key strategies for implementation of an antibiotic stewardship program

Antibiotic Stewardship “Good Antibiotic Stewardship is a practice that ensures the optimal selection, dose, and duration of an antimicrobial therapy that leads to the best clinical outcome for the treatment or prevention of an infection while producing the fewest toxic effects and the lowest risk for subsequent resistance. ” -Dale N. Gerding, MD Gerding DN. Jnt Comm J Qual Improv 2001; 27: 403 -404.

Multi-drug Resistant Organisms (MDROs): “ESCAPE” Enterococcus faecium (VRE) Staphylococcus aureus (MRSA) Clostridium difficile Acinetobacter baumanni Carbapenem resistant Enterobacteriaceae is on the rise! Pseudomonas aeruginosa Enterobacteriaceae (ESBLs) Peterson LR. Clin Inf Dis 2009; 49: 992 -993.

Risk Factors for MDROs l l l l Prior antibiotic exposure History of MDRO or exposure to other colonized patients Recent or prolonged duration of hospital stay Long-term care residence Immunosuppressive disease Dialysis Comorbidity/Dependency (need for contact care) High frequency of antibiotic resistance in the community Drinka P, et al. JAMDA 2011; June editorial: 321 -325. Muto CA, et al. Infect Control Hosp Epidemiol 2002; 23: 429 -435. Muto CA, et al. Infect Control Hosp Epidemiol 2003; 24: 362 -386. Ostrowsky et al. N Engl J Med 2001; 344: 1427 -1433.

Antibiotic Use Linked to MDROs • Collateral Damage: • Use of antimicrobial results in colonization or infection with resistant organisms • 3 rd gen cephalosporins and fluoroquinolones • Linked to multi-drug resistant (MDR) organisms: VRE, MRSA, ESBL-producing organisms, C. difficile, Enterobacteriaceae, CRE (fluoroquinlones) • Clindamycin: C. difficile infection (CDI) Choi et al. Antimicrob Agents Chemother. 2008; 52: 995 -100. Chow et al. Ann Intern Med. 1991; 115: 585 -90. Nauciel et al. Presse Med. 1985; 23: 673 -67. Pai et al. Antimicrob Agents Chemother. 2004; 48: 3720 -28. Paterson. Clin Infect Dis. 2004; 38: S 341 -45.

Impact of Resistant Organisms l Delay in appropriate antibiotic therapy l Up to 30 -44% increase in mortality l Increased length of stay by up to 18 days l Increased attributable hospital cost per case: $9, 000 -$72, 000 Dellit et al. Clin Infect Dis. 2007; 44: 000 -000. Mauldin et al. Antimicrob Agents Chemother 2010; 54: 109 -115. Obritsch et al. Pharmacotherapy 2005; 25(10): 1353 -1364.

Resistance Impact: CDC National Summary Clostridium difficile http: //www. cdc. gov/drugresistance/threat-report-2013/pdf/ar-threats-2013 -508. pdf#page=13

2013 CDC Antibiotic Resistance Threats http: //www. cdc. gov/drugresistance/threat-report-2013/pdf/ar-threats-2013 -508. pdf#page=13

CDI Risk Factors l l l Advanced age (> 64 y/o) Duration of hospitalization Exposure to antimicrobial agents l Including single-dose surgical prophylaxis l Longer duration = higher risk l Highest risk agents: fluoroquinolones, clindamycin, 2 nd & 3 rd generation cephalosporins Chemotherapy GI surgery or tube feeding Acid suppressive agents Cohen SH, et al. Infect Control Hosp Epidemiol 2010; 31. King RN, et al. Pharmacotherapy 2011; 31(7): 642 -648. Loo VG, et al. N Engl J Med 2005; 353: 2442 -9. Owens RC. Pharmacotherapy 2006; 26: 299 -311.

No Antibiotics in Development for Gram-negatives in the Next 10 yrs Infectious Diseases Society of America (IDSA) Campaign in 2004: Bad Bugs, No Drugs. . . 10 New Antibiotics by 2020 http: //www. idsociety. org/uploaded. Files/IDSA/Policy_and_Advocacy/Current_Topics_and_Issues/Advanci ng_Product_Research_and_Development/Bad_Bugs_No_Drugs/Statements/
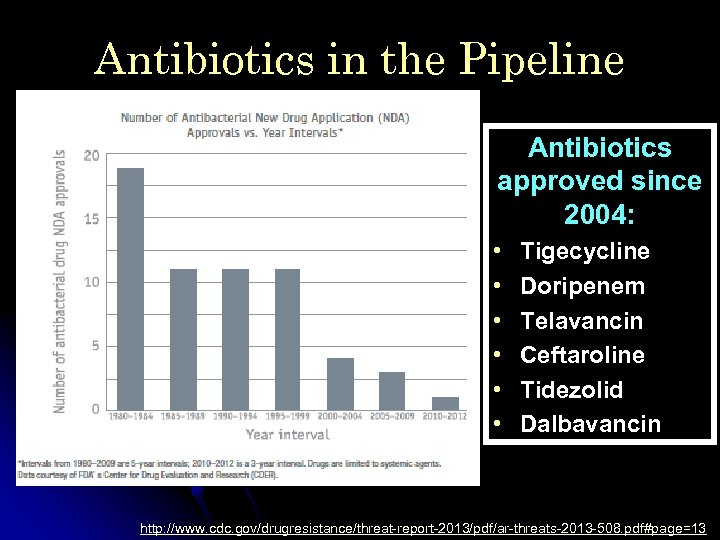
Antibiotics in the Pipeline Antibiotics approved since 2004: • • • Tigecycline Doripenem Telavancin Ceftaroline Tidezolid Dalbavancin http: //www. cdc. gov/drugresistance/threat-report-2013/pdf/ar-threats-2013 -508. pdf#page=13

CDC Core Preventative Actions • Stop inappropriate antibiotic use • Use antibiotics safely & appropriately • Diagnosis • Choice • Dose • Duration http: //www. cdc. gov/drugresistance/threat-report-2013/pdf/ar-threats-2013 -508. pdf#page=13

Antimicrobial Stewardship • Extending the life of antimicrobials requires appropriate use • Maximize therapeutic impact • Minimize unintended consequences • Toxicity • Selection of pathogenic organisms • Emergence of resistance o Prescribe only when appropriate diagnosis o Appropriate treatment: drug, dose and duration o Streamline therapy Dellit et al. Clin Infect Dis. 2007; 44: 000 -000. Shlaes et al. Clin Infect Dis. 1997; 25: 584 -99.

Antibiotic Stewardship l Component of patient safety l Up to 50% antibiotic use = Inappropriate l Inappropriate use = ’d selection of resistance l Programs shown to ↓ antibiotic use by 22 -36% l Annual savings $200 -900, 000 l Successful decrease in multi-drug resistant organisms w/in 3 -5 yrs l Guidelines supported by AAP, ASHP, IDSA, SIDP Delit et al. Clin Infect Dis 2007; 44.

CDC Get Smart Campaign Antibiotics do not fight viral illness like colds. Taking antibiotics for colds can be harmful to your child’s health – In fact, unnecessary antibiotics can make future infections harder to treat http: //www. cdc. gov/getsmart/index. html

Stewardship Core Requirements l Multi-disciplinary team l ID-trained pharmacist l ID physician l Clinical microbiologist l Infection preventionist l Information systems specialist Dellit et al. Clin Infect Dis. 2007; 44: 000 -000.

Core Implementation Strategies l Prospective audit with feedback l l ID physician or pharmacist with ID training Formulary restriction with pre-authorization Dellit et al. Clin Infect Dis. 2007; 44: 000 -000.

Supplemental Strategies l Education l Guidelines & clinical pathways l Antimicrobial order forms l Avoidance of antimicrobial cycling & routine combination therapy l Streamlining or de-escalation of therapy l Dose optimization l IV to PO l Utilization of technology (CPOE, e. MAR) Dellit et al. Clin Infect Dis. 2007; 44: 000 -000.

Barriers to Implementing l l l IDSA guidelines focus on the development of hospital-based programs Lack of resources l Funding l Personnel (physician, ID trained pharmacist) l Data & outcomes management l Creation of antimicrobial stewardship tools Lack of physician participation Drew RH. J Manag Care Pharm 2009; 15: S 18 -23.

Resources: How to implement a program l AHRQ Toolkits l l Abx Stew: http: //www. gnyha. org/resourcecenter/? catid=50 Decreasing CDI through Abx Stew: l l Joint Commission Toolkit l l http: //www. jointcommissioninternational. org/antimicrobial-stewardship-toolkit/ Regional susceptibility info l l http: //www. ahrq. gov/professionals/quality-patient-safety/patient-safetyresources/cdifftoolkit/cdiff-questions 1. html http: //www. cddep. org/resistancemap National Society of Infectious Diseases Guidelines l http: //www. idsociety. org/idsa_practice_guidelines/

Antimicrobial Stewardship Long-term Care Facilities (LTCFs)

Epidemiology ~ 16, 000 nursing homes in the U. S. l ~ 1. 5 million residents l Infection incidence rates: 3. 6 -5. 2/ 1000 resident days l Most commonly reported infections: urinary tract infections (UTIs), pneumonia, skin infections, and gastroenteritis l http: //www. cdc. gov/nchs/fastats/nursing-home-care. htm. Accessed July 11, 2014. Smith PW, et al. SHEA APIC Guideline. Am J Infect Control 2008; 36: 504 -35. Rhee M, et al. Infect Dis Clin N Am 2014; 28: 237 -246.

Epidemiology Infection most common cause for transfer to an acute care hospital l Antibiotics among most frequently prescribed medications in LTCFs and have second highest adverse drug event rate l Estimated inappropriate antibiotic use rates range: 25 - 75% (depends on definition used) l Rhee M, et al. Infect Dis Clin N Am 2014; 28: 237 -246.

Antimicrobial Challenges for LTCFs Distinguishing colonization from infection l Prevalence asymptomatic bacteriuria (ASB): l l Noncatheterized: 25 -50% l Long-term urinary catheters: 100% l Elderly: ASB associated with pyuria 90% cases l Symptomatic UTIs may present atypically Rhee M, et al. Infect Dis Clin N Am 2014; 28: 237 -246.

Antimicrobial Challenges for LTCFs l Lack of resources: l Clinical providers may be offsite l Therapy decisions based on staff clinical assessments l Limited diagnostic testing services Rhee M, et al. Infect Dis Clin N Am 2014; 28: 237 -246.

Implementing Antimicrobial Stewardship in LTCFs SHEA/APIC guidelines encourage infection prevention programs to include a component antimicrobial stewardship l No consensus on specific components l Hampered by limited resources l Smith PW, et al. SHEA APIC Guideline. Am J Infect Control 2008; 36: 504 -35. Nicolle L. Antimicrobial Resistance and Infection Control 2014; 3: 6.

Implementing Antimicrobial Stewardship: LTCFs Consider stepwise approach l Engage key leadership l Medical director l Director of nursing l Infection prevention coordinator l Consultant pharmacist l Representatives from medical & nursing staff l Rhee M, et al. Infect Dis Clin N Am 2014; 28: 237 -246.

Implementing Antimicrobial Stewardship: LTCFs Assess baseline antimicrobial usage if possible (engage pharmacist) l Monitor antibiotic resistance and C. difficile infection rates l Educate providers/ staff regarding appropriate antibiotic use l Educate/ train staff on proper clinical assessments (especially important if clinical providers offsite) l Rhee M, et al. Infect Dis Clin N Am 2014; 28: 237 -246.

Implementing Antimicrobial Stewardship: LTCFs l Develop LTCF diagnostic & treatment guidelines based on currently published national guidelines l Focus on most common LTCF infections; e. g. UTIs, pneumonia l Consider restricting broad spectrum antimicrobials; e. g. fluoroquinolones (levofloxacin, ciprofloxacin), carbapenems (e. g. meropenem) based on usage criteria Rhee M, et al. Infect Dis Clin N Am 2014; 28: 237 -246.

UTI Treatment Guideline: Process Example Collaborate with physician champion, pharmacist, and lead nurse l Review current national UTI treatment guidelines l Develop institution-specific diagnosis & treatment guideline l l Utilize institution pathogen (e. g. E. coli) susceptibility data (if available) l May also use regional (Texas) susceptibility data

National Treatment Guidelines http: //www. idsociety. org/Organ_System/

UTI Treatment Guideline: Process Example Collaborate with physician champion, pharmacist, and lead nurse l Review current national UTI treatment guidelines l Develop institution-specific diagnosis & treatment guideline l l Utilize institution pathogen (e. g. E. coli) susceptibility data (if available) l May also use regional (Texas) susceptibility data
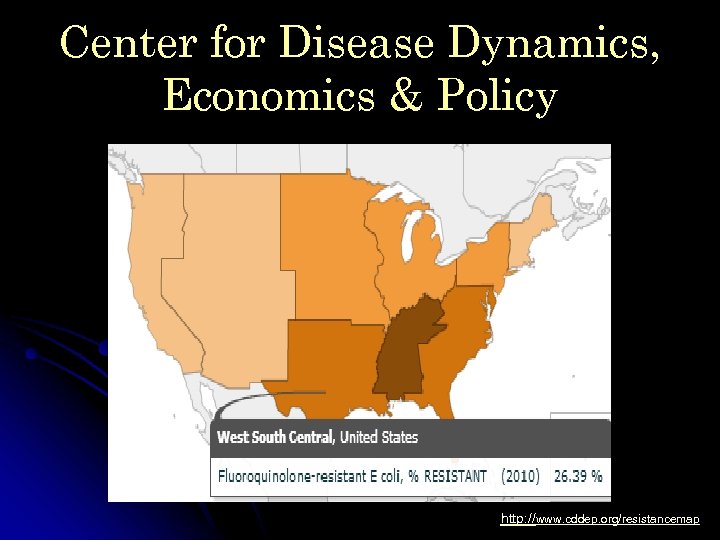
Center for Disease Dynamics, Economics & Policy http: //www. cddep. org/resistancemap

UTI Treatment Guideline: Process Example Educate staff and clinical providers l Ensure guidelines easily accessible l Measure antimicrobial usage improvement l Report post implementation outcomes to clinical providers and staff l Antibiotic usage l C. difficile infection rate l Delit et al. Clin Infect Dis 2007; 44.

Resources: How to implement a program l AHRQ Toolkits l l Abx Stew: http: //www. gnyha. org/resourcecenter/? catid=50 Decreasing CDI through Abx Stew: l l Joint Commission Toolkit l l http: //www. jointcommissioninternational. org/antimicrobial-stewardship-toolkit/ Regional susceptibility info l l http: //www. ahrq. gov/professionals/quality-patient-safety/patient-safetyresources/cdifftoolkit/cdiff-questions 1. html http: //www. cddep. org/resistancemap National Society of Infectious Diseases Guidelines l http: //www. idsociety. org/idsa_practice_guidelines/

Seton Healthcare Family (SHF) Antibiotic Stewardship Program

Seton Healthcare Family l 12 hospital network in Central Texas l Two of the largest medical centers l l l Level I trauma academic hospital (381 bed) Community hospital (473 bed) Limited clinical pharmacy specialists dispersed throughout the network

Implementation l Development of antimicrobial stewardship team (AST) l l Identify key physician groups l l Assessed for implementation of core strategies Infectious diseases (ID), hospitalists, intensivists, emergency medicine Identify key goals for the program l Develop pertinent site-based treatment guidelines or initiatives l Gain support from key physician groups l Develop & disseminate education

Network Multi-disciplinary AST l ID physicians l l Total of 10 throughout the network Network ID pharmacists (3 Co-chairs) l Two adult and one pediatric l Network Director of Infection Prevention l Network Microbiology Clinical Manager

Core Strategies: Formulary Restriction l ID consult/approval required for specific IV antimicrobials l Developed based on antimicrobial spectrum, availability, & cost (additions & modifications as needed) Gram-positive agents: Daptomycin, ceftaroline, linezolid, tigecycline, quinupristin/dalfopristin l l Gram-negative agents: meropenem, amikacin l Antifungals other than fluconazole l Others: acyclovir, trim/sulfa

Core Strategy: Prospective Audit (began FY 2009) l l Two network ID pharmacists dedicated to largest 2 sites ID pharmacists audit daily: IV antibiotic report & microbiology culture report l l Dose-optimization l l Streamlining/de-escalation IV to PO (including non-policy medications) ID pharmacists: microbiology laboratory & infection prevention resource for resistant organisms

SHF Supplemental Strategies l Education (annual presentations): l l Hospitalists, family medicine, emergency medicine Automatic pharmacy policies: l l IV dose optimization IV to PO policy l Review of all order sets containing antibiotics by ID pharmacists l Modification of order sentences within physician order entry & pharmacy system by ID pharmacists

Identification of Key Physician Groups l Identification of all network order sets containing antibiotics (specialty specific) l l Reviewed by ID pharmacist Identification of stakeholder physician groups for treatment guidelines during development l Hospitalists/Internal Medicine l Pulmonologists l Emergency Department

SHF Stewardship Goals l Appropriate antibiotic therapy for core measures l Reduce overall use of fluoroquinolones, ceftriaxone, and clindamycin l Increase cefazolin utilization for communityacquired Gram-negative infections based on antibiogram l Increase usage of SHF treatment guidelines l l l Appropriate empiric & streamlined therapy Appropriate duration of therapy Optimize dosing based on pharmacokinetics & pharmacodynamics

Joint Commission and Antimicrobial Stewardship l Surgical Care Improvement Project (SCIP) l l l Antimicrobial surgical prophylaxis Guideline developed & order set review to ensure correct antibiotic, weight-based dosing, timing of preop dose, and duration Pneumonia Core Measure (CAP) l Patient’s should receive antibiotic regimens based on national guidelines l Guideline & order sets developed consistent with SHF treatment guideline http: //www. jointcommission. org/

SHF Stewardship Goals l Appropriate antibiotic therapy for core measures l Reduce overall use of fluoroquinolones, ceftriaxone, and clindamycin l Increase usage of SHF treatment guidelines l l Appropriate empiric & streamlined therapy Appropriate duration of therapy l Increase cefazolin utilization for communityacquired Gram-negative infections based on antibiogram l Optimize dosing based on pharmacokinetics & pharmacodynamics

Antibiotic Stewardship to Prevent C. difficile Infection (CDI) l Minimize the frequency, duration, and number of antimicrobial agents prescribed l Limit utilization of high risk agents: l Fluoroquinolones (ciprofloxacin, levofloxacin, moxifloxacin) l 2 nd generation cephalosporins (e. g. , cefoxitin, cefotetan) l 3 rd generation cephalosporins (e. g. , ceftriaxone, cefotaxime) Cohen SH, et al. Infect Control Hosp Epidemiol 2010; 431 -455.

Antibiotic Stewardship to Prevent C. difficile Infection (CDI) l Programs implementing restriction criteria or reduced utilization measures l l l Reduction in use of high risk agents Reduction in nosocomial CDI One program reduced high risk agent utilization by 54% corresponding with a 60% reduction in CDI 3 l Also limited duration of therapy (pneumonia, abdominal infection) Aldeyab MA, et al. J Antimicrob Chemother 2012; 67: 2988 -2996. Cohen SH, et al. Infect Control Hosp Epidemiol 2010; 431 -455. (3) Valiquette L, et al. Clin Infect Dis 2007; 45: S 112 -21.

SHF Stewardship Goals l Appropriate antibiotic therapy for core measures l Reduce overall use of fluoroquinolones, ceftriaxone, and clindamycin l Increase usage of SHF treatment guidelines l l Appropriate empiric & streamlined therapy Appropriate duration of therapy l Increase cefazolin utilization for communityacquired Gram-negative infections based on antibiogram l Optimize dosing based on pharmacokinetics & pharmacodynamics

Institution-Based Treatment Guidelines l Assess disease states associated with potential for greatest impact related to program goals l SHF: Urinary tract infections (UTIs) had the largest inpatient utilization of fluoroquinolones (ciprofloxacin) and ceftriaxone l Assess antibiogram susceptibilities of narrowest spectrum agents l Perform literature review l Identify key stakeholders (hospitalists, intensivists, emergency department)
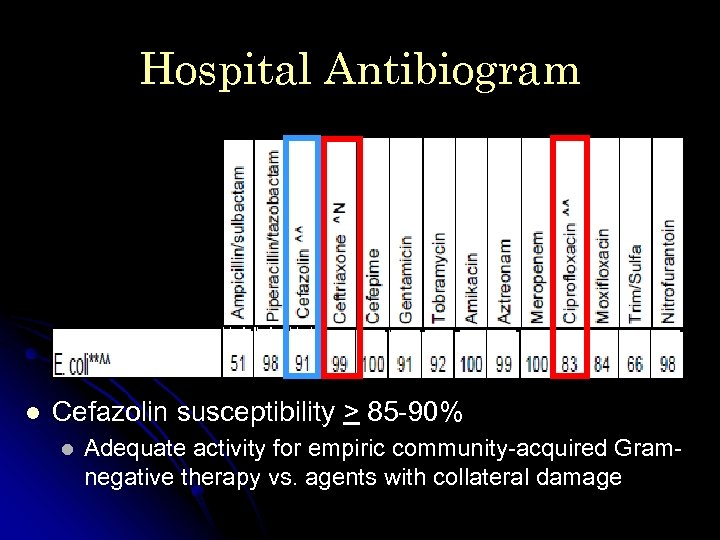
Hospital Antibiogram l Cefazolin susceptibility > 85 -90% l Adequate activity for empiric community-acquired Gramnegative therapy vs. agents with collateral damage

Antibiogram: Clinical Pearls Pros l l Assists in guiding empiric therapy Assess resistance trends Cons l All isolates l Community vs hospital acquired l Not site specific (ie. urine) l Institution specific l “S” may not equal optimal antimicrobial activity l Not able to see incremental increases in resistance

Seton Healthcare Family Antibiotic Stewardship Results

SHF Reduction in Use of Antibiotics Associated with Collateral Damage: Days of Therapy (DOT)/1000 patient days
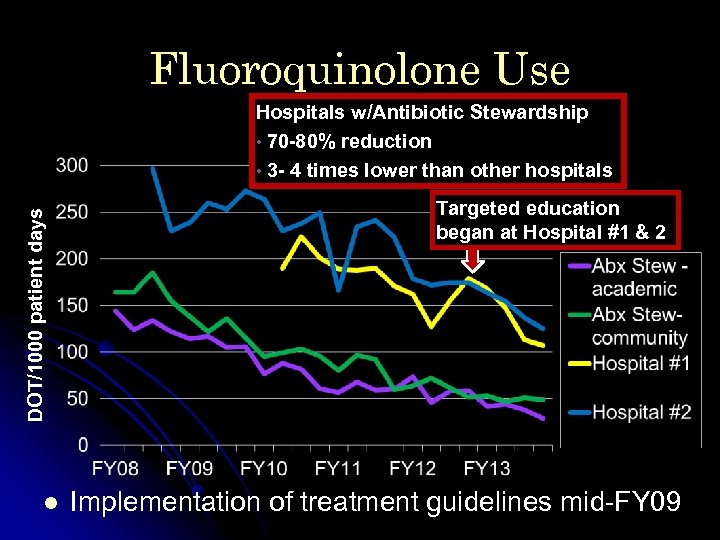
Fluoroquinolone Use DOT/1000 patient days Hospitals w/Antibiotic Stewardship • 70 -80% reduction • 3 - 4 times lower than other hospitals l Targeted education began at Hospital #1 & 2 Implementation of treatment guidelines mid-FY 09
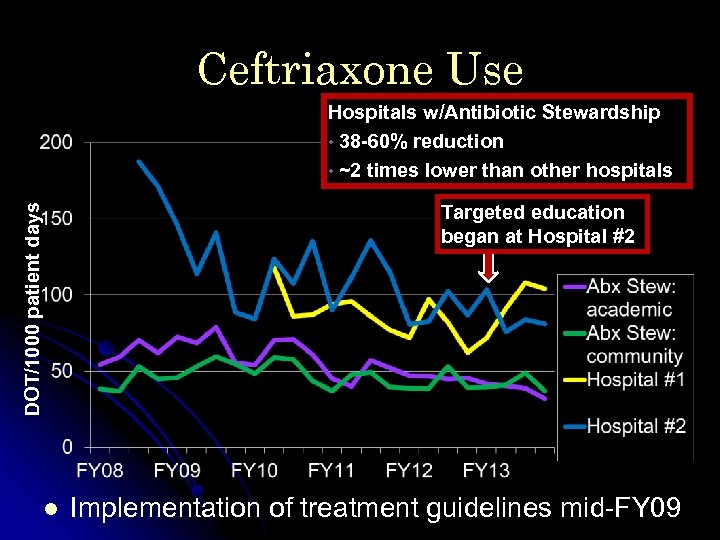
Ceftriaxone Use Hospitals w/Antibiotic Stewardship • 38 -60% reduction • ~2 times lower than other hospitals DOT/1000 patient days Targeted education began at Hospital #2 l Implementation of treatment guidelines mid-FY 09
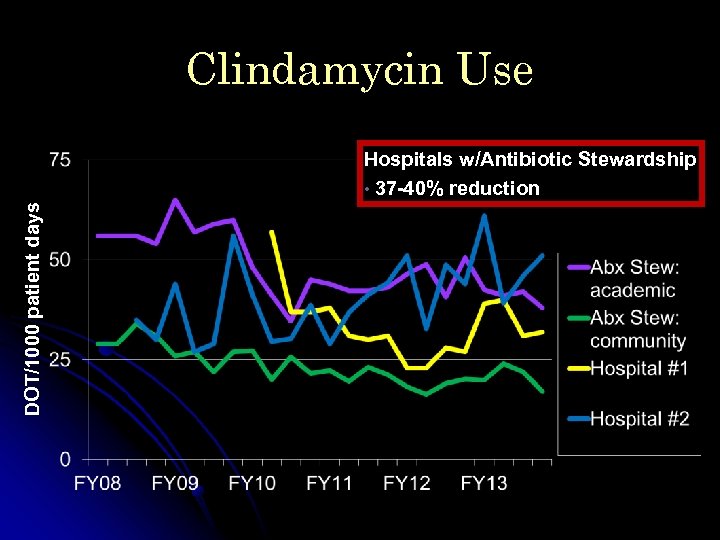
Clindamycin Use DOT/1000 patient days Hospitals w/Antibiotic Stewardship • 37 -40% reduction

Ciprofloxacin Pseudomonas Non-Susceptibility
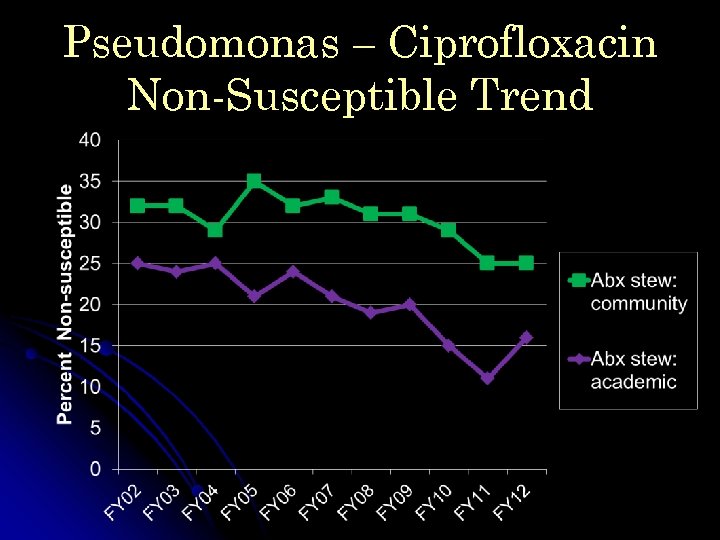
Pseudomonas – Ciprofloxacin Non-Susceptible Trend

C. difficile Infection (CDI)
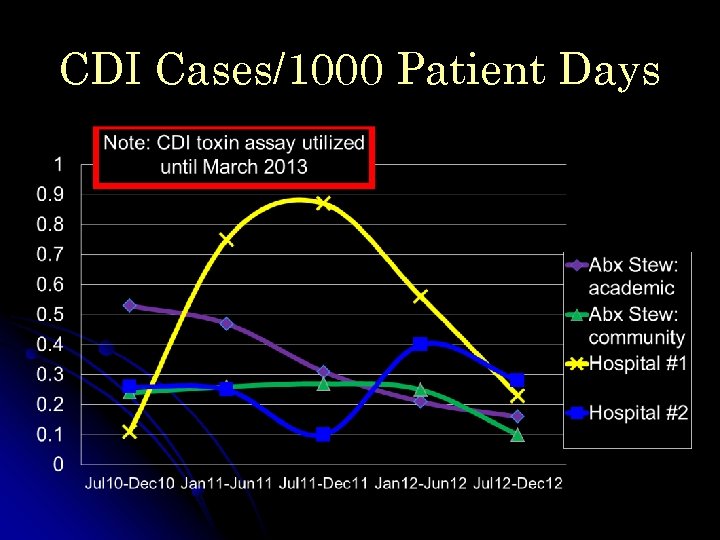
CDI Cases/1000 Patient Days
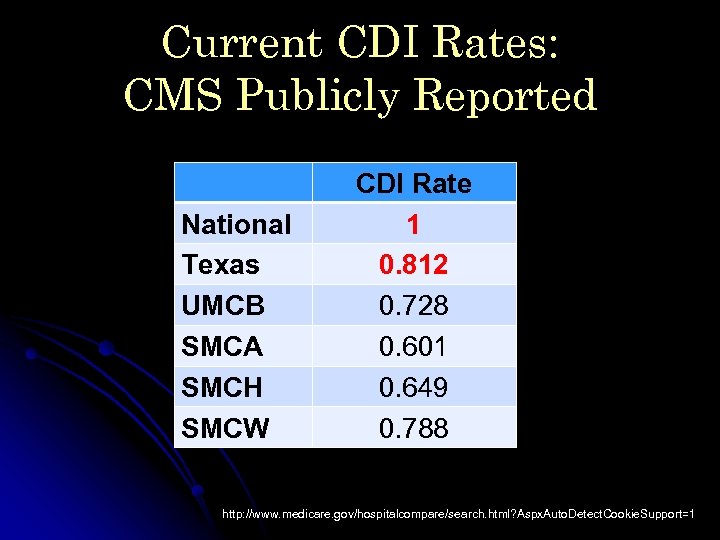
Current CDI Rates: CMS Publicly Reported National Texas UMCB SMCA SMCH SMCW CDI Rate 1 0. 812 0. 728 0. 601 0. 649 0. 788 http: //www. medicare. gov/hospitalcompare/search. html? Aspx. Auto. Detect. Cookie. Support=1

SHF Antibiotic Stewardship Program Cost Savings
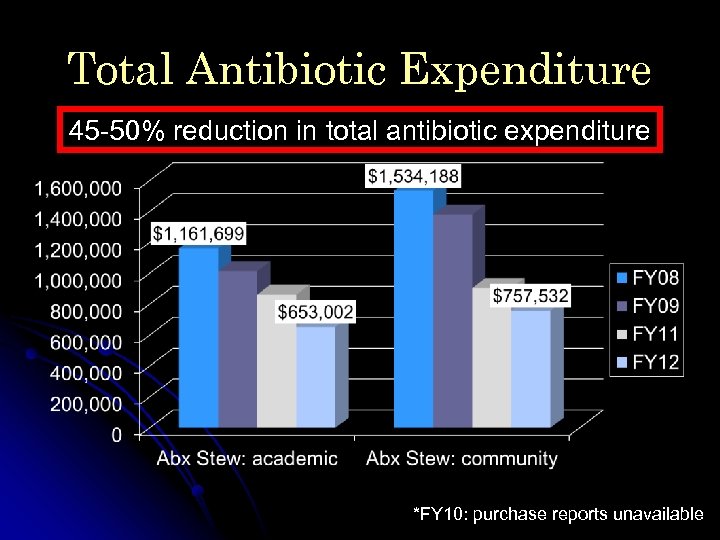
Total Antibiotic Expenditure 45 -50% reduction in total antibiotic expenditure *FY 10: purchase reports unavailable
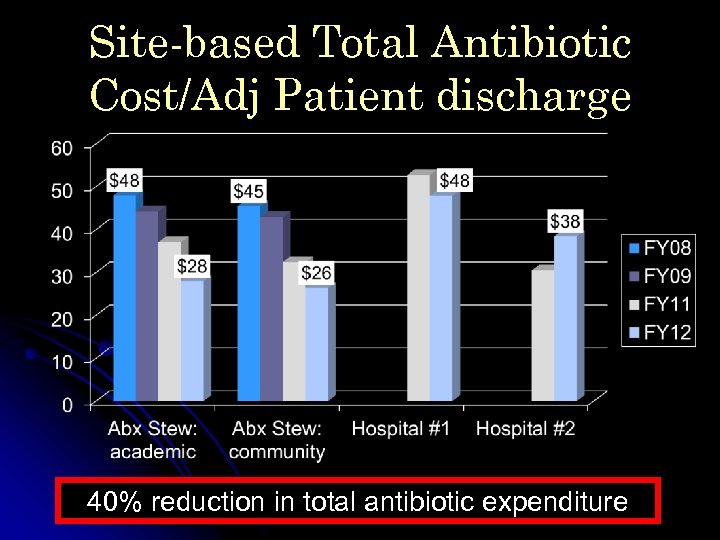
Site-based Total Antibiotic Cost/Adj Patient discharge 40% reduction in total antibiotic expenditure

Conclusion: Antibiotic Stewardship l Important component of patient safety l Associated with a in costly & high mortality resistant organisms l Key implementation strategies l Form antibiotic stewardship team l Identify goals and areas for opportunity l Identify & gain support from key physician groups l Utilization of treatment guidelines can be an instrumental component for implementation l Provide results & feedback l Positive results are motivating to key physician groups!

Antibiotic Stewardship l System-wide implementation of antibiotic stewardship initiatives led to the following: l Decreased antibiotic utilization of agents associated with collateral damage l Formal stewardship programs at both a community & academic setting were associated with: l Lower utilization of broad spectrum agents l Lower CDI rates l 40% lower cost/adjusted patient discharge l Results presented to leadership and resources allotted (additional pharmacy specialists) to further spread to other sites

Antibiotic Stewardship: Katherine Shea, Pharm. D. , BCPS-AQ-ID Theresa Jaso, Pharm. D. BCPS-AQ-ID Clinical Pharmacy Specialists, Infectious Diseases Seton Healthcare Family
cdebfa2863360f16217aa8d21a05e5a2.ppt