058da2c4f75761cd2e6e243cb6ecca01.ppt
- Количество слайдов: 59

Anesthesia Dr Abdollahi

Anesthesia From Greek anaisthesis means ”not sensation” Ø Listed in Bailey´s English Dictionary 1721. Ø When the effect of ether was discovered”anesthesia” used as a name for the new phenomenon. Ø

Basic Principles of Anesthesia defined as the abolition of sensation Ø Analgesia defined as the abolition of pain Ø “Triad of General Anesthesia” Ø Ø need for unconsciousness Ø need for analgesia Ø need for muscle relaxation

History of Anesthesia

History of Anesthesia Ø Ether synthesized in 1540 by Cordus Ø Ether used as anesthetic in 1842 by Dr. Crawford W. Long Ø Ether publicized as anesthetic in 1846 by Dr. William Morton Ø Chloroform used as anesthetic in 1853 by Dr. John Snow

History of Anesthesia Ø Endotracheal tube discovered in 1878 Ø Local anesthesia with cocaine in 1885 Ø Thiopental first used in 1934 Ø Curare first used in 1942 - opened the “Age of Anesthesia”

Anesthesiologists care for the surgical patient in the preoperative, intraoperative, and postoperative period. Important patient care decisions reflect the preoperative evaluation, creating the anesthesia plan, preparing the operating room, and managing the intraoperative anesthetic.


Preoperative Evaluation The goals of preoperative evaluation include assessing the risk of coexisting diseases, modifying risks, addressing patients' concerns, and discussing options for anesthesia care.

What is the indication for the proposed surgery? It is elective or an emergency? The indication for surgery may have particular anesthetic implications. For example, a patient requiring esophageal fundoplication will likely have severe gastroesophageal reflux disease, which may require modification of the anesthesia plan (e. g. , preoperative non particulate antacid, intraoperative rapid sequence induction of anesthesia).

What are the inherent risk of this surgery? Surgical procedures have different inherent risks. For example, a patient undergoing coronary artery bypass graft has a significant risk of problems such as death, stroke, or myocardial infarction. A patient undergoing cataract extraction has a low risk of major organ damage.

Does the patient have coexisting medical problems? Does the surgery or anesthesia care plan need to be modified because of them?

Has the patient had anesthesia before? Were there Complication such as difficult airway management? Does the patient have risk factor for difficult airway management?

Creating the Anesthesia Plan After the preoperative evaluation, the anesthesia plan can be completed. The plan should list drug choices and doses in detail, as well as anticipated problems. Many variations on a given plan may be acceptable, but the trainee and the supervising anesthesiologist should agree in advance on the details.




Preparing the Operating Room After determining the anesthesia plan, the trainee must prepare the operating room.




Anesthesia Providers Ø Anesthesiologist ( aphysician with 4 or more yearsof speciality training in anesthesiology after medical school) Ø Certified registered nurse anesthetist (CRNA), working under the direction and supervision of an anesthesiologist or a physician Ø CRNA must have 2 years of training in anesthesia

Patient Safety Patient risk and safety are concerns during surgery and anesthesia. Ø Data from a number of studies of death caused by anesthesia indicate a death rate ranging from 1 per 20, 000 -35, 000. Ø A fourfoulded decline over the last 30 years even though surgical procedures are undertaken on increasingly sicker and much higher risk patients than in the past. Ø Awareness of potential problems and constant vigilance (the process of paying close and continuous attention) are crucial to good patient care. Ø

Preoperative preparation patient evaluation Ø Anaesthesiologist: Ø reviews the patient´s chart, Ø evaluate the laboratory data and diagnostic studies such as electrocardiogram and chest x-ray, Ø verify the surgical procedure, Ø examins the patient, Ø discuss the options for anesthesia and the attendant risks and Ø ordered premedication if appropriate

The physical status classification Developed by the American Society of Anesthesiologist (ASA) to provide uniform guidelines for anesthesiologists. Ø It is an evaluation of anesthetic morbidity and mortality related to the extent of systemic diseases, physiological dysfunction, and anatomic abnormalities. Ø Intraoperative difficulties occur more frequently with patients who have a poor physical status classification. Ø


Choice of anesthesia Ø Ø Ø Ø Ø The patient´s understanding and wishes regarding the type of anesthesia that could be used The type and duration of the surgical procedure The patients´s physiologic status and stability The presence and severity of coexisting disease The patient´s mental and psychologic status The postoperative recovery from various kinds of anesthesia Options for management of postoperative pain Any particular requiremets of the surgeon There is major and minor surgery but only major anesthesia

Types of anesthesia care General Anesthesia Ø Reversible, unconscious state is characterised by amnesia (sleep, hypnosis or basal narcosis), analgesia (freedom from pain) depression of reflexes, muscle relaxation Ø Put to sleep

Types of anesthesia care Regional Anesthesia A local anethetic is injected to block or ansthetize a nerve or nerve fibers Ø Implies a major nerve block administered by an anesthesiologist (such as spinal, epidural, caudal, or major peripheral block) Ø

Types of anesthesia care monitered anesthesia care Ø Infiltration of the surgical site with a local anesthesia is performed by the surgeon Ø The anasthesiologist may supplement the local anesthesia with intravenous drugs that provide systemic analgesia and sedation and depress the response of the patient´s autonomic nervous system

Types of anesthesia care local anesthesia Ø Employed for minor procedures in which the surgical site is infiltrated with a local anesthetic such as lidocaine or bupivacaine Ø A perioperative nurse usually monitors the patient´s vital signs Ø May inject intravenous sedatives or analgesic drugs

Premedication Ø Ø Ø Ø Purpose: to sedate the patient and reduce anxiety Classified as sedatives and hypnotics, tranquilizers, analgesic or narcotics and anticholinergics Antiacid or an H 2 receptor-blockingdrug such as cimitidine (tagamet) or ranitidine (Zantac) to decrease gastric acid production and make the gastric contents less acidic If aspiration occur this premedication decreases the resultant pulmonary damage Given 60 -90 minutes before surgery, or may be given i. v. After the pat. arrives in the surgical suite NPO for a minimum of 6 hours before elective surgery Not given to elderly people or ambulatory patients because residual effects of the drugs are present long after the pat. have been discharged and gone home

Perioperative monitoring Undergeneral anesthesia: monitoring Ø Inspired oxygen analyzer(Fi. O 2) which calibrated to room air and 100% oxygen on a daily basis Ø Low pressure disconnect alarm, which senses pressure in the expiratory limb of the patient circuit Ø Inspiratory pressure Ø Respirometer (these four devices are an integral part of most modern anesthesia machine Ø ECG Ø BP-automated unit Ø Heart rate Ø Precordial or esophagel stethoscope Ø Temp

Perioperative monitoring Ø Ø Ø Ø Pulse oximeters End tidal carbon dioxide (ECO 2) Peripheral nerve stimulator if muscle relaxants are used Foly catheter For selected patint with a potential risk of venous air embolism a doppler probe may placed over the right atrium Invasive: arterial pressure mesurements, central venous pressure Pulmonary artery catheter and continous mixed venous oxygen saturation measured

Perioperative monitoring Ø For special conditions other monitors as transesophageal echocardiography Ø Electroencephalogram Ø Cereral or neurological may be used

Inhalational Anesthetic Agents Ø Inhalational anesthesia refers to the delivery of gases or vapors from the respiratory system to produce anesthesia Ø Pharmacokinetics--uptake, distribution, and elimination from the body Ø Pharmacodyamics-- MAC value

Regional Anesthesia Ø Defined as “a reversible loss of sensation in a specific area of the body” Ø Spinal anesthesia Ø Epidural anesthesia Ø IV Regional Blocks Ø Peripheral Nerve Blocks

Spinal Anesthesia ØA local anesthetic agent (lidocaine, tetracaine or bupivacaine) is injected into the subarachnoid space Ø Spinal anesthesia is also known as a subarachnoid block Ø Blocks sensory and motor nerves, producing loss of sensation and temporary paralysis
Possible Complications of Spinal Anesthesia Ø Hypotension Ø Post-dural puncture headache (“Spinal headache”) caused by leakage of spinal fluid through the puncture hole in the duracan be treated by blood patch Ø “High Spinal”- can cause temporary paralysis of respiratory muscles. Patient will need ventilator support until block wears off

Epidural Anesthesia Ø Local anesthetic agent is injected through an intervertebral space into the epidural space. Ø May be administered as a one-time dose, or as a continuous epidural, with a catheter inserted into the epidural space to administer anesthetic drug
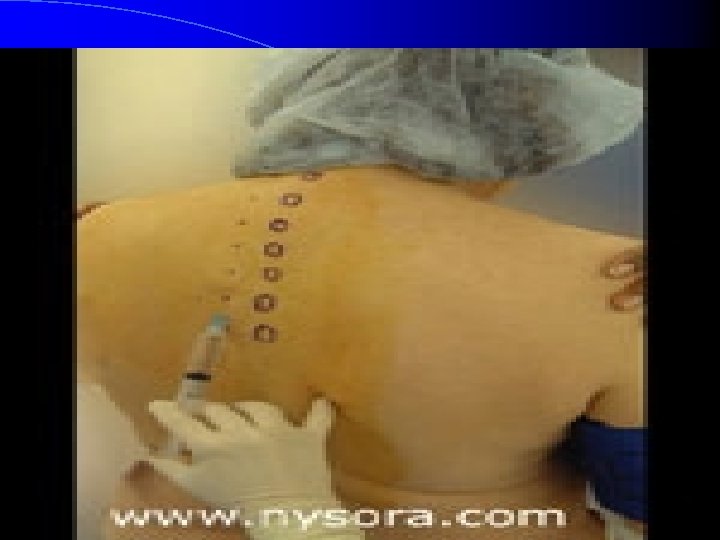
Dr. Aidah Abu Elsoud Alkaissi Division of Intensive Care and Anaesthesiology University of

Complications of Epidural Anesthesia Ø Hypotension Ø Inadvertent dural puncture Ø Inadvertent injection of anesthetic into the subarachnoid space

IV Regional Blocks Ø Also known as a Bier Block Ø Used on surgery of the upper extremities Ø Patient must have an IV inserted in the operative extremity

IV Regional Block Ø After a pneumatic tourniquet is applied to extremity, Lidocaine is injected through the IV. Ø Anesthesia lasts until the tourniquet is deflated at the end of the case.

IV Regional Blocks Ø IMPORTANT- to prevent an overdose of lidocaine it is important not to deflate the tourniquet quickly at the end of the procedure.
Peripheral Nerve Blocks Ø Injection of local anesthetic around a peripheral nerve Ø Can be used for anesthesia during surgery or for post-op pain relief Ø Examples: ankle block for foot surgery, supraclavicular block for post-op pain control after shoulder surgery

Monitored Anesthesia Care (MAC) Ø Generally used for short, minor procedures done under local anesthesia Ø Anesthesia provider monitors the patient and may provide supplemental IV sedation if indicated

Conscious Sedation Ø Used for short, minor procedures Ø Used in the OR and outlying areas Ø (ER, GI Lab, etc) Ø Patient is monitored by a nurse and receives sedation sufficient to cause a depressed level of consciousness, but not enough to interfere with patient’s ability to maintain their airway

Inhalation Anesthetics Ø Nitrous Oxide- can cause expansion of other gases- use of N 20 contraindicated in patients who have had medical gas instilled in their eye(s) during retinal detachment repair surgery
Inhalation Anesthetics Ø Cause cerebrovascular dilation and increased cerebral blood flow Ø Cause systemic vasodilation and decreased blood pressure Ø Post-op N&V Ø All inhalation anesthetics, except N 20, can trigger malignant hyperthermia in susceptible patients

Intravenous Induction/Maintenance Agents Ø Propofol (Diprivan)- pain/burning on injection, can cause bizarre dreams Ø Pentothal (Sodium Thiopental)- can cause laryngospasm

General Anesthesia Ø During induction the room should be as quiet as possible Ø The circulator should be available to assist anesthesia provider during induction & emergence Ø Never move/reposition an intubated patient without coordinating the move with anesthesia first

General Anesthesia Ø Laryngospasm may happen in a patient having a procedure with general anesthesia Ø When laryngospasm occurs, it is usually during intubation or emergency Ø Assist anesthesia provider as needed- call for anesthesia back-up if necessary

Difficult Airway Cart Ø Anesthesia maintains a “Difficult Airway Cart” containing equipment & supplies for difficult intubations Ø This cart is stored in one of the anesthesia supply rooms Ø Page anesthesia tech if the cart is needed for your room

Cricoid Pressure or Sellick Maneuver Ø Used for patients at risk for aspiration during induction, due to a full stomach or other factors such as a history of reflux Ø Pressure on the cricoid cartilage compresses the esophagus against the cervical vertebrae and prevents reflux
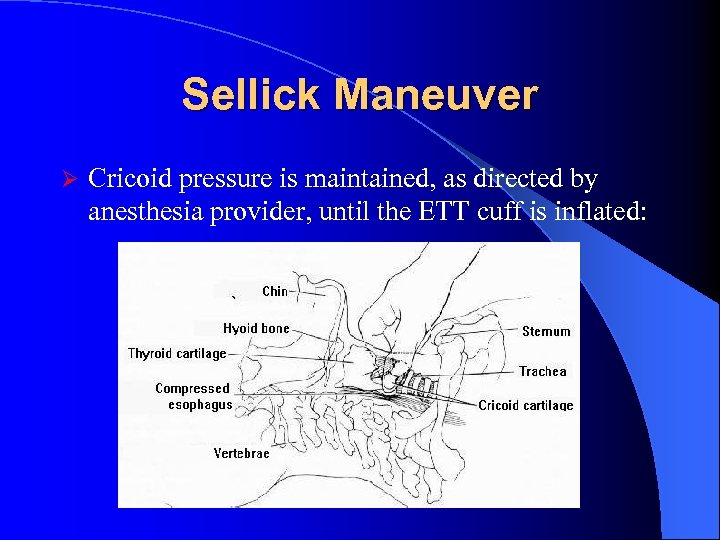
Sellick Maneuver Ø Cricoid pressure is maintained, as directed by anesthesia provider, until the ETT cuff is inflated:

Regional Anesthesia Ø Circulator may need to assist anesthesia provider with positioning for spinal or epidural anesthesia. Ø Patient usually is positioned laterally for placement of regional anesthesia, but may be positioned sitting upright.

The Awake Patient Ø Patients undergoing surgery with regional or local anesthesia, even if sedated, may be aware of conversation and activity in room Ø Post sign on door to OR, “Patient is Awake” so that staff entering room will be aware that patient is conscious

When Patient is Awake Ø Limit any discussion of patient’s medical condition and prognosis Ø Avoid discussion of other patients & limit unnecessary conversation-- a sedated patient can easily misinterpret conversation they overhear
058da2c4f75761cd2e6e243cb6ecca01.ppt