18667d0805edfaf1366d7f812a1763e6.ppt
- Количество слайдов: 79

Anesthesia and the Elderly Patient Sheila R Barnett, MD Assistant Professor Anesthesiology Harvard Medical School Beth Israel Deaconess Medical Center
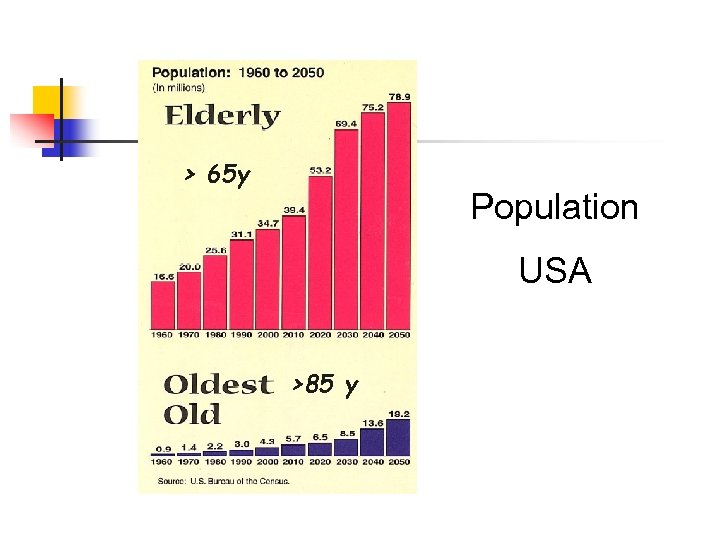
> 65 y Population USA >85 y
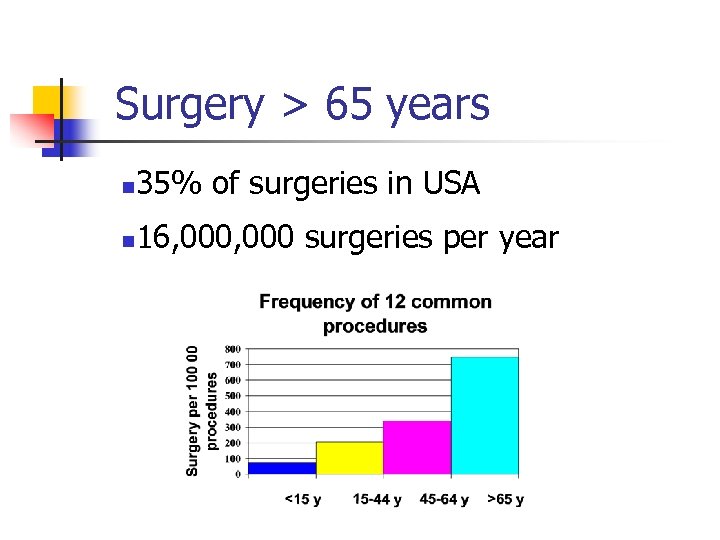
Surgery > 65 years n 35% of surgeries in USA n 16, 000 surgeries per year

RISK & COMORBIDITIES Aging involves physiological changes AND the pathophysiology of superimposed disease
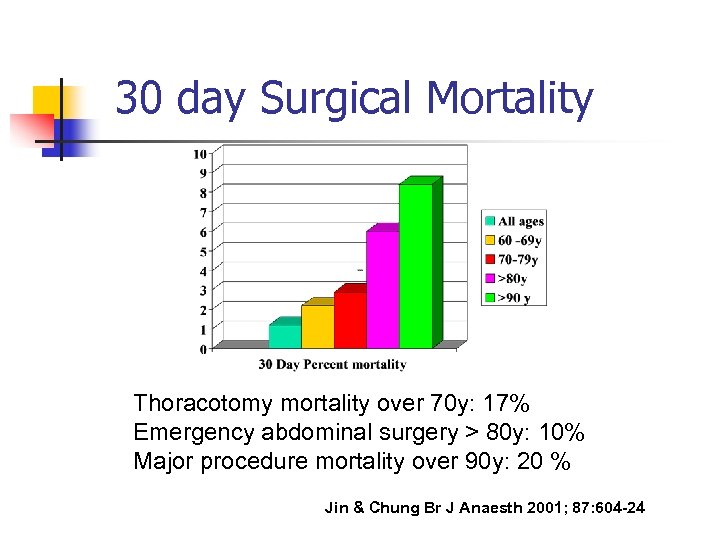
30 day Surgical Mortality Thoracotomy mortality over 70 y: 17% Emergency abdominal surgery > 80 y: 10% Major procedure mortality over 90 y: 20 % Jin & Chung Br J Anaesth 2001; 87: 604 -24

Present later n n Review of colorectal surgery Outcomes 65 -74; 75 -84; >85 years 34 194 patients Oldest patients: n n Presented later More co morbidities Emergency more common Survival lower Lancet 2000; 356: 968
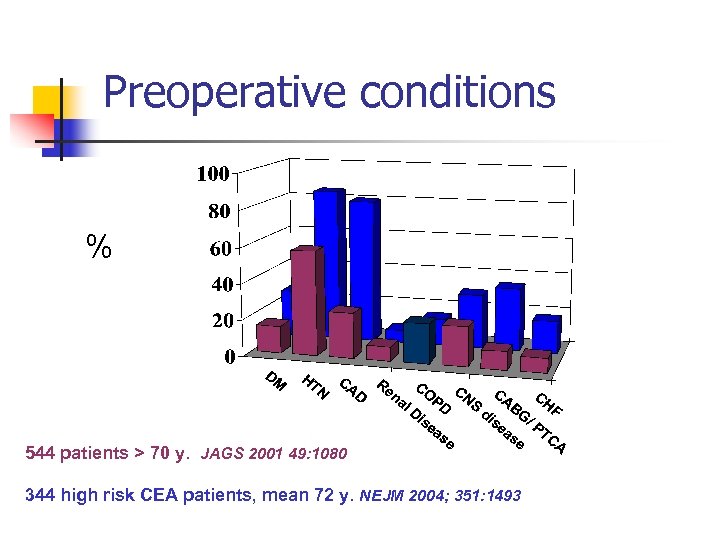
Preoperative conditions % 544 patients > 70 y. JAGS 2001 49: 1080 344 high risk CEA patients, mean 72 y. NEJM 2004; 351: 1493

Surgery Outcomes n > 70 y non cardiac surgery ; prospective 544 patients – age 78 y 21% adverse outcome 3. 7 % died Adverse outcomes: Predictors: Emergency n n n CVS 10% CNS 8% Pulmonary 5. 5% Renal 2. 5% LOS: 9 vs 4 days (p<0. 001) ASA Class Tachycardia Preop : Functional status CHF Leung et al JAGS 2001 49: 1080

Long term impact n Follow up 28 months on 517 patients - 32% deceased With complications: greater 3 month mortality (p 0. 02) Predictors of mortality (p<0. 0001) Cancer, ASA>2, CNS disease, Age, & Postop pulmonary and renal complications n Long term quality of life n n Not impacted by postoperative outcome comorbid conditions, age and new hospitalizations Manku & Leung Anesth Analg 2003; 96: 583 -94 (pts 1&2)

80 year old patients 26 648 > 80 y compared to 568 263 < 80 y n n 30 day mortality all cases 8% vs. 3%, p<0. 001 < 2% > 80 y for simple procedures n n TURP, IH, TKR, CEA > 80 y 20% 1 or more complications 26% mortality in patients > 80 y with complications vs. 4% if no complication Mortality if > 80 y with serious complications > 33% Hamel et al JAGS 2005; 53: 424

General Risk Factors for post operative mortality n n n ASA 3 & 4 Major surgical procedures Disease: Cardiac, pulmonary, DM, Liver and renal impairment Functional status < 1 -4 METS Anemia & Low albumin Bed ridden
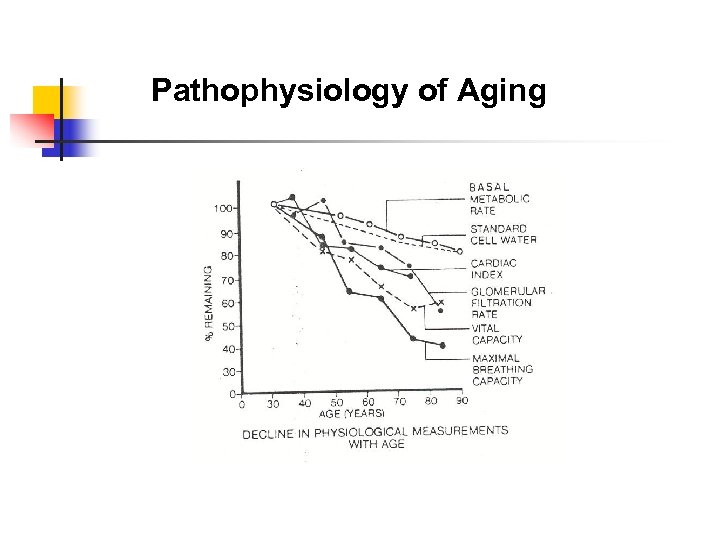
Pathophysiology of Aging
Cardiovascular n Peripheral n n Decrease in arterial elasticity – vascular stiffening Increase in BP Increase peripheral vascular resistance Ventricular n n Increased impedance - wall hypertrophy decreased compliance Resting CO unchanged more atrial dependence

Cardiovascular Rate & Rhythm n Conduction issues: Decline in pacemaker cells, fatty infiltration, fibrosis n Increase in atrial ectopy, sinus and ventricular conduction defects n Reduction in maximal HR – reduced response to catecholamines n Increased ischemic heart disease

Cardiovascular Autonomic Function Dysautonomia of Aging n Decline in beta receptor sensitivity n n HR responses impaired Increased norepinephrine levels Altered sympathovagal balance decreased HRV Decreased baroreflex sensitivity

Heart Failure n n n 6 -10% > 65 heart failure 80% admissions with heart failure are >65 y 40 – 50 % of patients with heart failure have normal LVEF
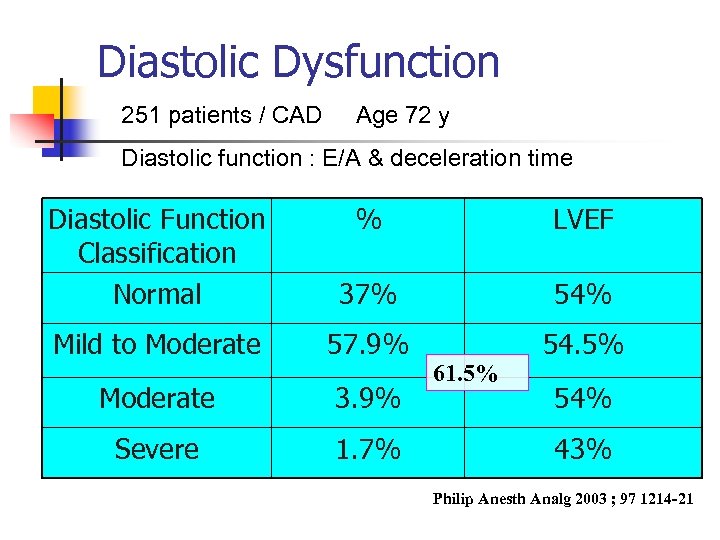
Diastolic Dysfunction 251 patients / CAD Age 72 y Diastolic function : E/A & deceleration time Diastolic Function Classification Normal % LVEF 37% 54% Mild to Moderate 57. 9% 54. 5% Moderate 3. 9% Severe 1. 7% 61. 5% 54% 43% Philip Anesth Analg 2003 ; 97 1214 -21
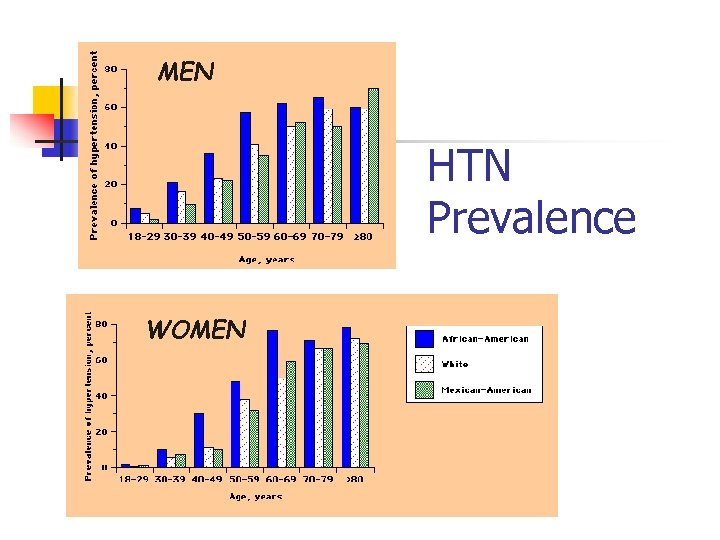
MEN HTN Prevalence WOMEN

Hypertension > 50% elderly n Treatment usually > 140/90 mm. Hg “High normal” 130 -139/85 -89 mm. Hg n VA study – n n n Berlowitz NEJM 1998; 339: 1957 800 males aged 65+/- 9 years 40% BP > 160/90 mm. Hg Despite 6 visits /year NHANES lll only 29% hypertensive population reach target goal

Complications of HTN Risk increases linearly with BP “High normal” BP 130 -139 / 85 -89 mm. Hg also increased risk n Ischemic heart disease & MI n Stroke n LVH n Diastolic dysfunction & pulmonary edema n Renal failure

Increased Pulse Pressure n Pulse pressure = SBP –DBP n ? Possible marker for vascular disease n Low DBP also poor prognosis
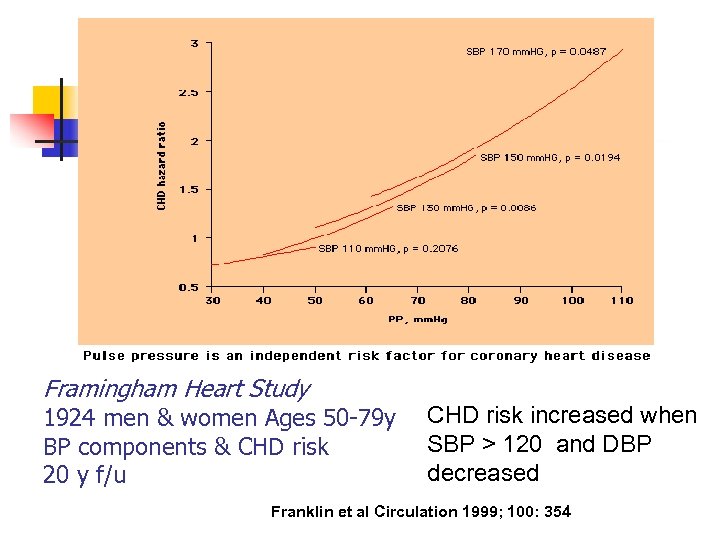
Framingham Heart Study 1924 men & women Ages 50 -79 y BP components & CHD risk 20 y f/u CHD risk increased when SBP > 120 and DBP decreased Franklin et al Circulation 1999; 100: 354

The ll/VI SEM

Aortic Sclerosis - is it really benign? n n >5000 echos 29% (1600) with sclerosis, no obstruction 5 year f/u Almost 50% increase in death from CVS causes and MI in sclerosis Otto et al, NEJM 1999
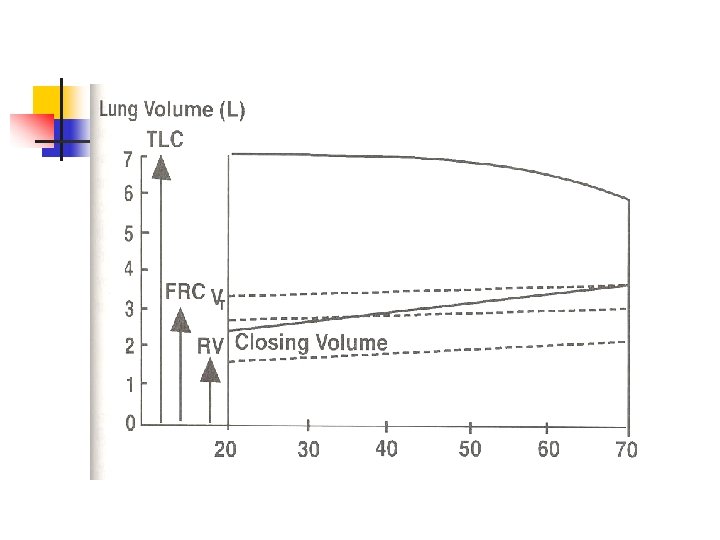
Pulmonary Function and Aging n Thorax stiffens – n n n reduced chest wall compliance & decreased thoracic skeletal muscle mass = Increased work of maximal breathing Lung volumes change – reduced inspiratory and expiratory reserve volume Decrease in elastic lung recoil –closing volume increase

Aspiration Risk n Reduction pharyngeal sensation n Reduction of maximal NIP n Swallowing coordination may be diminished

Central Nervous System n Cortical grey matter attrition – n starts in middle age n Cerebral atrophy – disease vs. aging n Increased intracranial CSF n CBF and auto regulation largely maintained

CNS deficiencies n n n Neurotransmitter deficiencies Integration of neuronal circuits Fluid intelligence Spinal cord demyelination Decreased spinal reflexes
Peripheral nervous system n Fibrosis in peripheral nerves n Less myelinated fibers n Slower nerve conduction n Diminished muscle mass

CNS & Drugs n n n Pharmacodynamic MAC Altered respiratory drive & drugs Spinal drugs Epidural spread sensitivity

Cognitive Dysfunction n Post operative delirium Cognitive dysfunction: non-cardiac surgery Post cardiac surgery

Post-operative delirium n n Incidence 10 -15% in >65 y Increased mortality Longer hospital stay Numerous risk factors: n n n Advanced age Dementia, Depression Anemia n n n Alcohol and drug withdrawal Metabolic derangement Acute MI Infection Emergency surgery

Delirium costs! n n n Per year over 2. 3 million older people have delirium during hospital stay 17. 5 million inpatient days >$ 4 billion (1994 #s) Medicare expenditure Inoye NEJM 1999; 340: 669

Postoperative Cognitive Dysfunction n n Early n n n n 1218 patients >60 years Early 7 days 26% Late 3 months 9. 9% (controls 2. 8%) Increasing Age Duration anesthesia Low education Second operation Infections Respiratory Complications Late n Age only n Moller et al Lancet 1998

Is it the Anesthetic? n n n RCT: 262 patients Knee replacement – epidural vs. general 5% clinical deterioration in cognitive status at 6 months No difference GA vs. regional Early delirium may be marker for ongoing cognitive deterioration Many similar trials and results …(but fractures & joint replacements – apples and oranges? ) Williams Russo et al JAMA 1995; 274: 44

Confusion – what can you do? n n n Quick baseline assessment – date, year etc Days of the week backwards Honest informed consent to patient and family members Careful drug (and ETOH) history Avoid polypharmacy Pain control

Mild Cognitive Impairment n “Transitional state between the cognitive changes of normal aging and the earliest clinical features of Alzheimer's disease” n 10 -15% will develop Alzheimer's in a year 1 -2% normal elderly – Alzheimer’s n Role of genetics and Apolipoprotein E 4 alleles n Petersen et al NEJM 2005; 352: 2379

Vascular patients n n Longitudinal study – 11 years 4141 men & 1681 women Cognitive testing Poor cognitive function Independent of age or SE class n n n Angina p 0. 001 MI p 0. 02 Claudication p. 004 Singh-Manoux JAGS 2003; 51: 1445

Should we do more? n n Informed Consent ? Hospitalization “unmask” marginal cognitive function n Dementia prevalent n Postoperative rehabilitation plans Cognitive Preoperative Assessments?

Renal Function n Progressive decrease in Renal Blood flow n Renal tissue atrophy - primarily cortical n n 30% reduction in nephrons age by middle age Sclerosis reaming nephrons n Glomerular filtration rate declines n Serum creatinine misleading – n ‘occult’ renal insufficiency

Fluid homeostasis n n n Sodium conservation impaired Urine concentrating ability reduced Thirst diminished Post operative Acute Renal Failure >50% mortality in very elderly patients

Body Compartments n Decline in total body water n n intracellular water plasma volume maintained n Less lean tissue & skeletal muscle mass n Increase proportion of fat
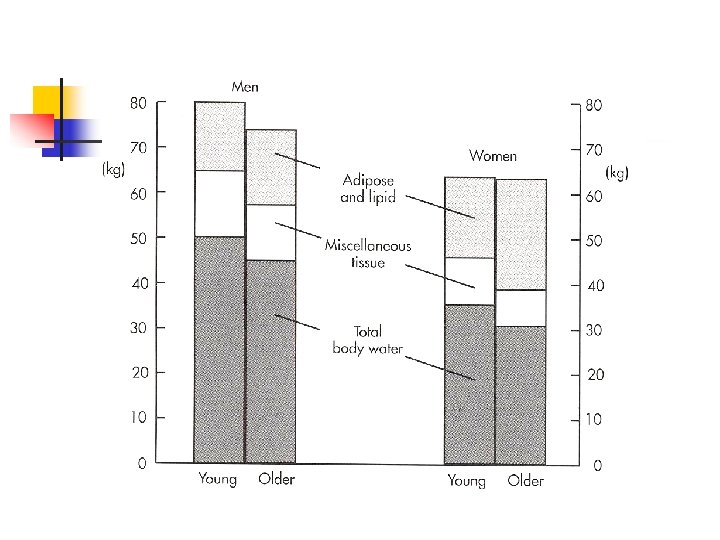

Hepatic n Decrease in hepatic mass n Decrease in hepatic clearance n Less albumin n Qualitative change in protein binding n Alpha-1 -glycoprotein increases

Drug considerations n water soluble drugs n prolonged half life of lipophilic drugs n n decreased hepatic metabolism& renal clearance increased target organ sensitivity
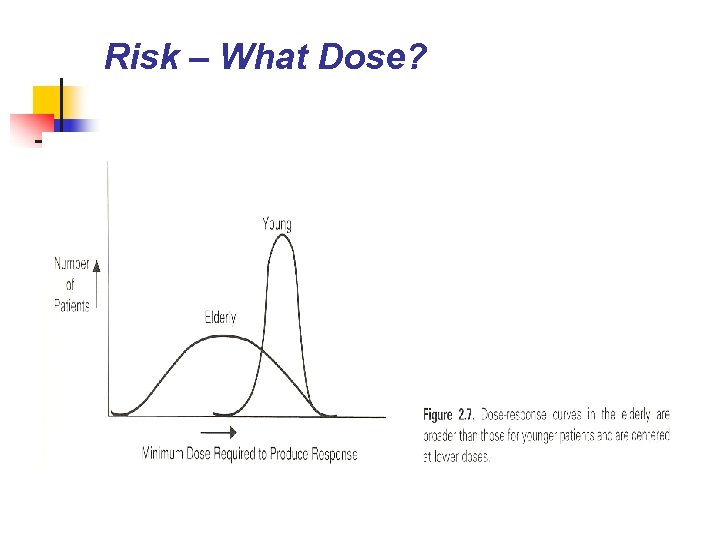
Risk – What Dose?

Summary pathophysiology n n n Steady decline in organ function Unpredictable reserve function Increased comorbidity
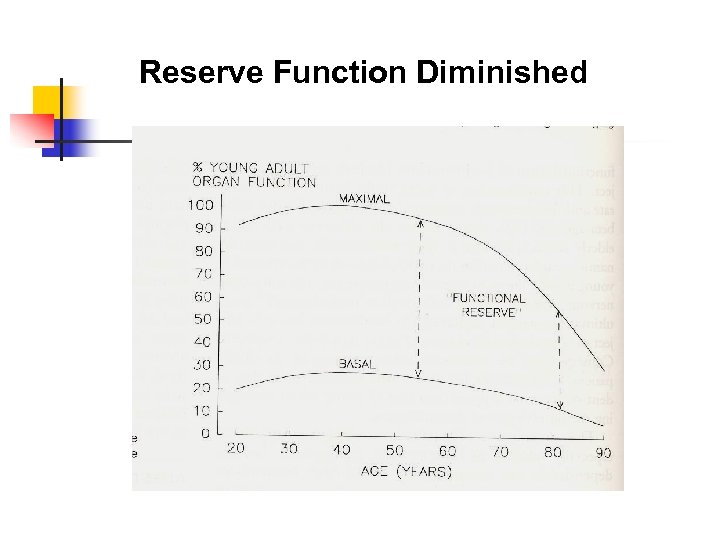
Reserve Function Diminished

Risk Reduction n n Beta Blockade Comprehensive assessments Less invasive surgery ? Regional

Beta Blockade & Risk Reduction Mangano NEJM 1996; 335: 1713 n n 100/200 patients received Atenolol preop and for 7 days Atenolol group improved survival 6 months & up to 2 y. Diabetes major risk Wallace Anesth 1998; 88: 7 n Atenolol reduced postoperative ischemia by 30 - 50%
n High risk vascular patients with positive dobutamine echocardiograhpy. n n Mean age 68 y 173/ 846 positive echos n n 59 bisoprolol 61 excluded on Beta blockers /wma 53 standard care (SC) Bisoprolol vs SC death or non fatal MI: 2 (3. 4%) vs 18 (34%) Poldermans NEJM 1999; 341: 1789

Beta blockers continued … n n > 600 000 patients undergoing non cardiac surgery 18% received perioperative beta blockade Reduction in death for those with a Cardiac Risk Index Score of 2 -4 But possible increased risk of death for those with Cardiac Risk Index of 0 or 1 Lindenauer et al NEJM 2005; 353: 349
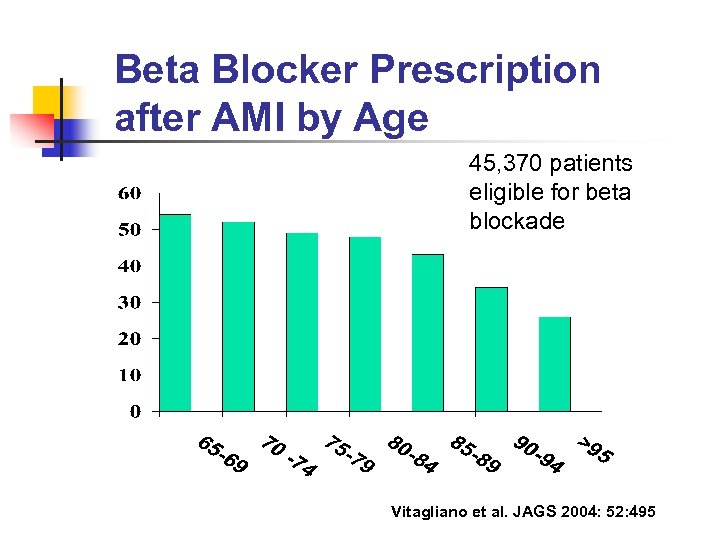
Beta Blocker Prescription after AMI by Age 45, 370 patients eligible for beta blockade Vitagliano et al. JAGS 2004: 52: 495
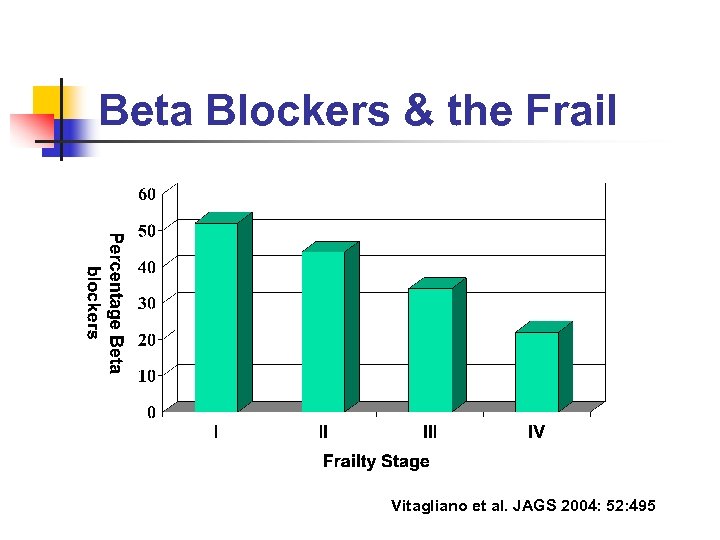
Beta Blockers & the Frail Vitagliano et al. JAGS 2004: 52: 495

Comprehensive Geriatric Assessments (CGA) n n 120 patients >60 y CGA n n ADLs, IADLs (Barhtel Index) , comorbidity, nutrition, MMSE All undergoing thoracic surgery 17% post op complications Predictors – n n n Low Barthel Index Surgery >300 mins Dementia – low MMSE Fukuse Chest 2005; 127: 886

Intervention Program to Reduce Delirium n n 400 patients > 70 y Admitted to Intervention Ward n n n Assessment, prevention treatment education Assessment day 1, 3, 7 Delirious patients in the Intervention ward n n n Shorter duration: by day 7 30% vs 60% (p 0. 001 ) Shorter LOS: 9 vs 13 days (p 0. 001) Reduced mortality: 2 vs. 9 patients died (p 0. 03) Lundstrom et al JAGS 2005: 53: 622

Less invasive surgery ? n CEA n n Yadav et al NEJM 2004; 351: 1493 344 high risk patients average 72 y Stent vs. open Results showed stent as good – possible reduction in death at 1 year and at least as good or less adverse events Endovascular AAA n 1 year perioperative survival advantage vs. open Blankenstein et al NEJM 2005; 352: 2398

Spinal or Epidural vs. General Anesthesia n n n Long a source of controversy Expert opinion suggesting no significant difference in major complications or mortality Meta-analysis of 141 randomized trials Total of 9559 patients Studied neuraxial blockade (either spinal or epidural anesthesia) vs. general anesthesia BMJ 2000; 321: 1 Rodgers et al BMJ 2000; 321: 1 -12

Meta-Analysis of Neuraxial Blockade vs. General Anesthesia Rodgers et al BMJ 2000; 321: 1 -12 Perioperative event Death DVT Pulmonary embolism Pneumonia Respiratory depression Myocardial infarction Odds reduction for neuraxial blockade 30% 44% 55% 39% 59% 33%

Fractures too… n n n Meta analysis 15 randomized trials 2162 patients In Spinal: n n n Reduction in 1 month mortality (6% vs 9%) Reduction in DVT Future – epidural vs LMWH and other anticoagulant strategies Urwin et al Br J Anesth 2000; 84(4) 450 -455

Cataracts n n n Low risk High volume High comorbidity

Do you ever wonder why we are in the room? n 1999 Survey in USA n n Rosenfeld in 1999 n n 1006 patients 33% needed an intervention during surgery No predictive factors International Studies n n n 45% Ophthalmologists using topical 78% anesthesiologist present But low topical rate Reeves survey n ‘net preference’ for anesthesiologists

Routine Testing No Testing Preoperative Medical Assessment EKG; CBC; Lytes, BUN, Creat & Gluc No tests unless new or worsening condition Both groups intra and postoperative medical events 3. 1/ 1000 operations Stein et al; NEJM 2000; 342: 168

“Routine medical testing before cataract surgery does not measurably increase the safety of the surgery” But… n Preoperative evaluation done in ALL patients and ALL patients had opportunity to have testing Conclusion n Testing should directed by history and physical performed prior to surgery

The Hip Fracture A Morbid Event Is the hip fracture the sentinel event marking deterioration ?

Hip fractures n n n 300 000 hospitalizations 1 year mortality 25% - reduction life expectancy Attributable cost of fracture $81 300 Disability significant M & M US in 1997 > $20 Billion n Braithewaite JAGS 2003; 51: 364

Hip fractures, old people and the inevitable …. . Hip fractures have high perioperative mortality 10 -25% Why? n n n 300 unselected hip fractures All received similar multimodal treatment Anesthesia epidural / strict protocol Well defined rehabilitation Foss & Kehlet 2005; Br J Anaesth 94; 24 -9

Why did they die? Foss & Kehlet 2005; Br J Anaesth 94; 24 -9 n 30 day mortality =13% ; >30 days 7 more died Combined mortality=16% n Analysis of 47 deaths n n n 28% (13) unavoidable: terminal cancer, refused care 15% (7) probably unavoidable 34% (16) potentially avoidable; active care curtailed 23% (11) Maximum care; ? avoidable

Miscellaneous

Sensory Changes n Decreased visual acuity & dark adaptation n Attrition of taste buds n Diminished thirst sensation n Compromised joint perception n Diminished fine control of skeletal muscles
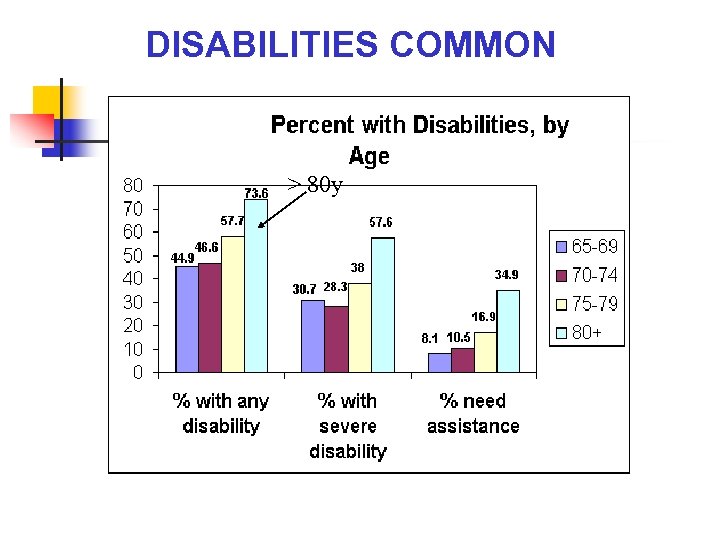
DISABILITIES COMMON > 80 y

Polypharmacy n Adverse drug events 3 -10% admissions common n Elderly on multiple medications 30% prescriptions & 40% of OTC drugs n Drugs and herbs n n n eg Ephedra alkaloids -ma huang Adverse Events : HTN, palpitations, strokes, seizures

ETOH & Elderly Alcohol and Drug prescription problems affect 17% of older Americans n n n Increase sensitivity & decrease in tolerance Decrease lean body mass & TBW = higher concentration Decrease in alcohol dehydrogenase may slow metabolism

Social Issues n Increase in disability n Lack of a spouse n Cognitive and sensory problem n Scheduling - a family commitment

Challenges & Elderly n heterogeneous population n unpredictable organ reserve n disease burden n atypical disease presentation n emergent procedures n minor complications can rapidly escalate
Geriatric Graphs Disease or badness Age years Function Age years

Future ? n Cognitive Preoperative assessment n Functional outcomes n Perioperative interventions
18667d0805edfaf1366d7f812a1763e6.ppt