d1ec63556809174c79b14281b1a8d0d5.ppt
- Количество слайдов: 17
 Anatomia microchirurgica della regione temporo-silviana. Studio anatomico preoperatorio: Tips and Tricks Neurochirurgia - San Giovanni-Addolorata - Roma Massimiliano Neroni
Anatomia microchirurgica della regione temporo-silviana. Studio anatomico preoperatorio: Tips and Tricks Neurochirurgia - San Giovanni-Addolorata - Roma Massimiliano Neroni
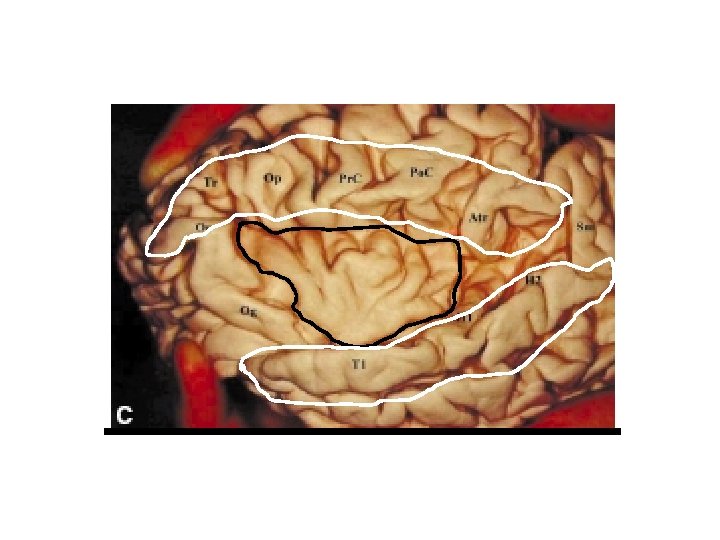 Insular anatomy After opening the temporal and fronto-parietal opercula
Insular anatomy After opening the temporal and fronto-parietal opercula
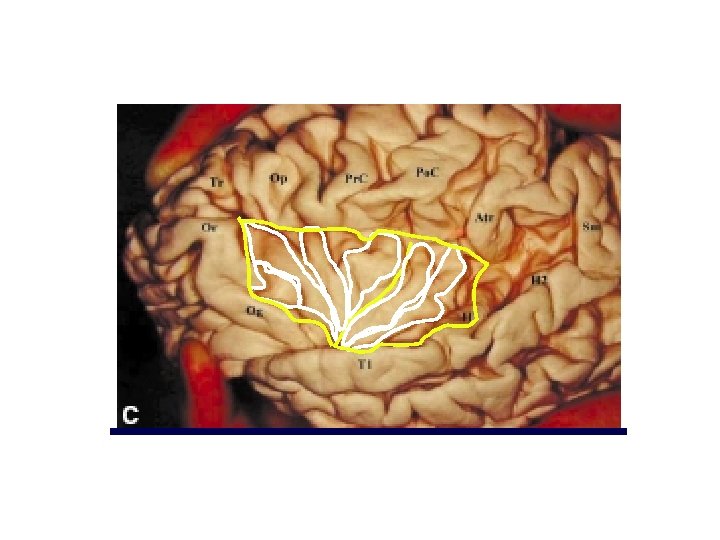 Microsurgical anatomy of the Insular Lobe
Microsurgical anatomy of the Insular Lobe
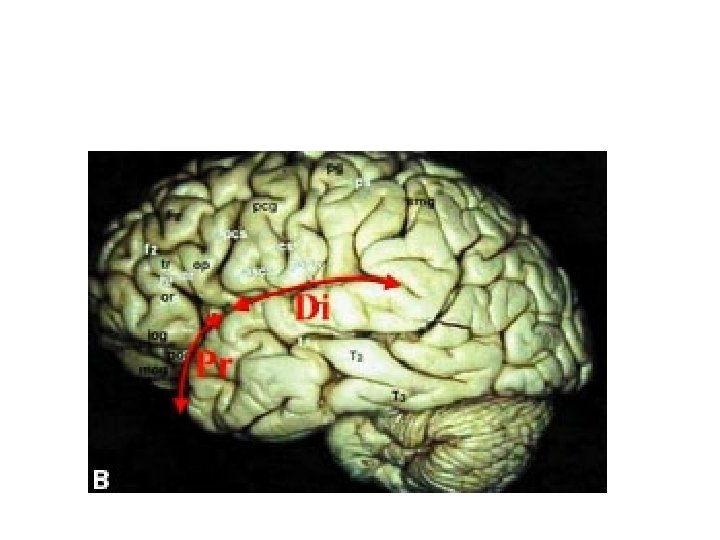 Sylvian fessure distal and prossimal division
Sylvian fessure distal and prossimal division
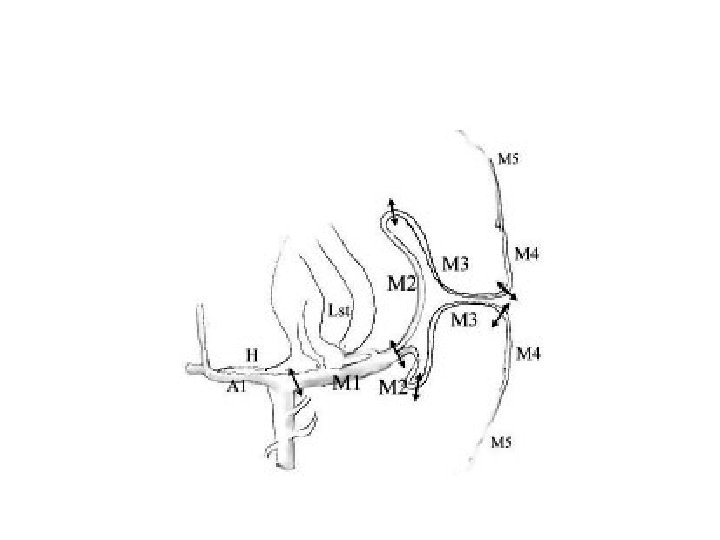 Vascular anatomy of the insula and LSAs
Vascular anatomy of the insula and LSAs
 Knownledge of the phylogenesis of the structures Mesiobasal temporal Temporal pole Limbic Amygdala Hippocampus Parahippocampus 2 layered structures (allocortex) Cingulate Gyrus Paralimbic Fornix Mammillary body Caudal Fronto-Orbital Gyrus (included Pars Orbitalis) INSULA 3 -5 layered structures (mesocortex)
Knownledge of the phylogenesis of the structures Mesiobasal temporal Temporal pole Limbic Amygdala Hippocampus Parahippocampus 2 layered structures (allocortex) Cingulate Gyrus Paralimbic Fornix Mammillary body Caudal Fronto-Orbital Gyrus (included Pars Orbitalis) INSULA 3 -5 layered structures (mesocortex)
 Preferential brain locations of LGG Duffau H. and Capelle L. Cancer, 2004 Jun 15; 100: 2622 -6 66% insular tumor are LGGs show an affinity to phylogenetically more primitive zones. Fillimorf 1947 and then Yakovlev in 1959 LGG are more likely located in “secondary” functional areas immediately near to the so called “eloquent areas”. Insula is a part of the mesocortex with 3 -5 neuronal layers (Paralymbic region: M. G. Yasargil et al: Microsurgery of Insular Gliomas)
Preferential brain locations of LGG Duffau H. and Capelle L. Cancer, 2004 Jun 15; 100: 2622 -6 66% insular tumor are LGGs show an affinity to phylogenetically more primitive zones. Fillimorf 1947 and then Yakovlev in 1959 LGG are more likely located in “secondary” functional areas immediately near to the so called “eloquent areas”. Insula is a part of the mesocortex with 3 -5 neuronal layers (Paralymbic region: M. G. Yasargil et al: Microsurgery of Insular Gliomas)
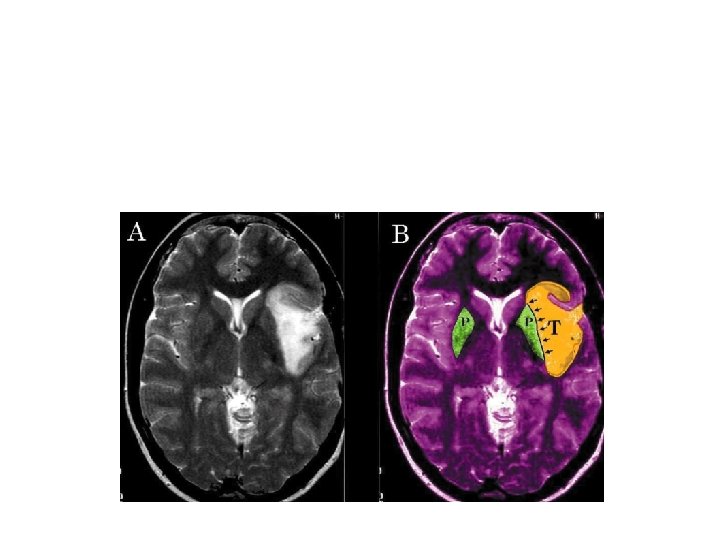 T 2 sharp imaging on benign tumor M. G. Yasargil, Ali F. Krisht, Ugur Ture, Ossama Al-Mefty and D. C. H. Yasargil Microsurgery of insular glioma Part III – Contemporary Neurosurgery 24; 13: 1 -6 Y. A. Moshel, J. D. S. Marcus, E. C. Parker and P. J. Kelly Resection of insular gliomas: the importance of lenticulostriate artery position. Clinical article. JNS November 2008; 109: 5
T 2 sharp imaging on benign tumor M. G. Yasargil, Ali F. Krisht, Ugur Ture, Ossama Al-Mefty and D. C. H. Yasargil Microsurgery of insular glioma Part III – Contemporary Neurosurgery 24; 13: 1 -6 Y. A. Moshel, J. D. S. Marcus, E. C. Parker and P. J. Kelly Resection of insular gliomas: the importance of lenticulostriate artery position. Clinical article. JNS November 2008; 109: 5
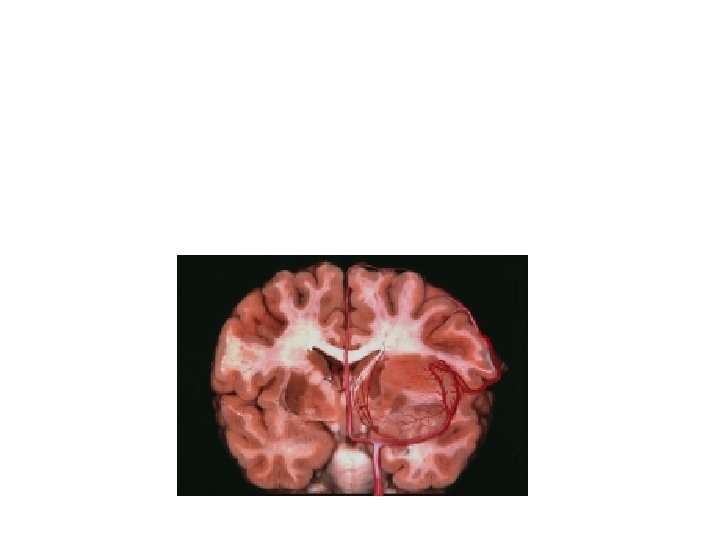 Lesion displacing LSAs medially often represent a sharp-well demarcated T 2 MR images and LGGs histology. On 429 Limbic-Paralimbic tumors 31/191 of the Insular Gliomas demostrated anaplastic grade (MG Yasargil Microsurgery of the insular gliomas on Cont. Neurosurg. VOL. 24, 14: JUL 15. 2002) Tumor with moderate shift of the LSAs and T 2 MR images showing a diffuse boundaries pattern are most likely HGG and aggressive surgery is often associated to permanent deficit.
Lesion displacing LSAs medially often represent a sharp-well demarcated T 2 MR images and LGGs histology. On 429 Limbic-Paralimbic tumors 31/191 of the Insular Gliomas demostrated anaplastic grade (MG Yasargil Microsurgery of the insular gliomas on Cont. Neurosurg. VOL. 24, 14: JUL 15. 2002) Tumor with moderate shift of the LSAs and T 2 MR images showing a diffuse boundaries pattern are most likely HGG and aggressive surgery is often associated to permanent deficit.
 Y. A. Moshel, J. D. S. Marcus, E. C. Parker and P. J. Kelly Resection of insular gliomas: the importance of lenticulostriate artery position. Clinical article. JNS November 2008; 109: 5 - 50% patients underwent previous surgery in other institutions - 70% patients presenting with seizures - 20% with mild hemiparesis - 45% pure insular tumors (55% with opercular extension) - 20% High enhancing lesion with high grade tumor: had postop permanent deficit ((30% TGR) - 80% Low enhancing lesion were LGGs (70% TGR was achieved) - Tumor approach - Opening the sylvian fessure at the sylvian center - Dethetering of M 4 -M 5 vessels - Without metal retractors - Depending on the target: multiple vertical incision dividing the M 2 -M 3 branches - If present opercular extension first approached - MEP and SEEP are strictly necessary only in the dominant hemisphere
Y. A. Moshel, J. D. S. Marcus, E. C. Parker and P. J. Kelly Resection of insular gliomas: the importance of lenticulostriate artery position. Clinical article. JNS November 2008; 109: 5 - 50% patients underwent previous surgery in other institutions - 70% patients presenting with seizures - 20% with mild hemiparesis - 45% pure insular tumors (55% with opercular extension) - 20% High enhancing lesion with high grade tumor: had postop permanent deficit ((30% TGR) - 80% Low enhancing lesion were LGGs (70% TGR was achieved) - Tumor approach - Opening the sylvian fessure at the sylvian center - Dethetering of M 4 -M 5 vessels - Without metal retractors - Depending on the target: multiple vertical incision dividing the M 2 -M 3 branches - If present opercular extension first approached - MEP and SEEP are strictly necessary only in the dominant hemisphere
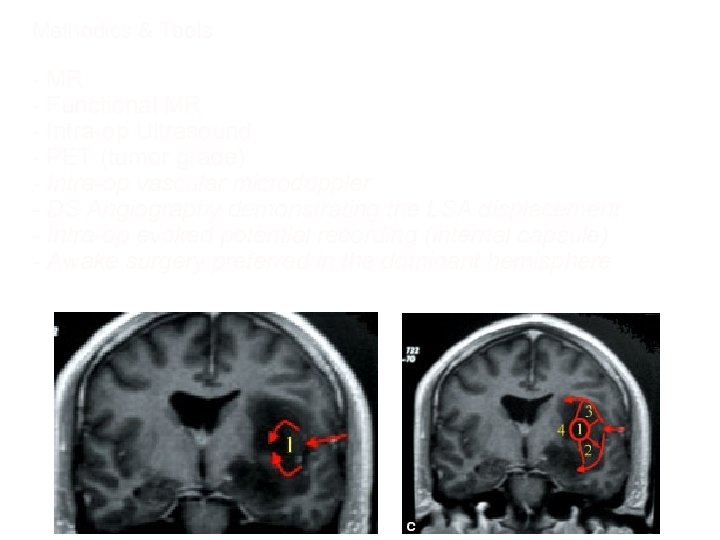 Methodics & Tools - MR - Functional MR - Intra-op Ultrasound - PET (tumor grade) - Intra-op vascular microdoppler - DS Angiography demonstrating the LSA displacement - Intra-op evoked potential recording (internal capsule) - Awake surgery preferred in the dominant hemisphere
Methodics & Tools - MR - Functional MR - Intra-op Ultrasound - PET (tumor grade) - Intra-op vascular microdoppler - DS Angiography demonstrating the LSA displacement - Intra-op evoked potential recording (internal capsule) - Awake surgery preferred in the dominant hemisphere
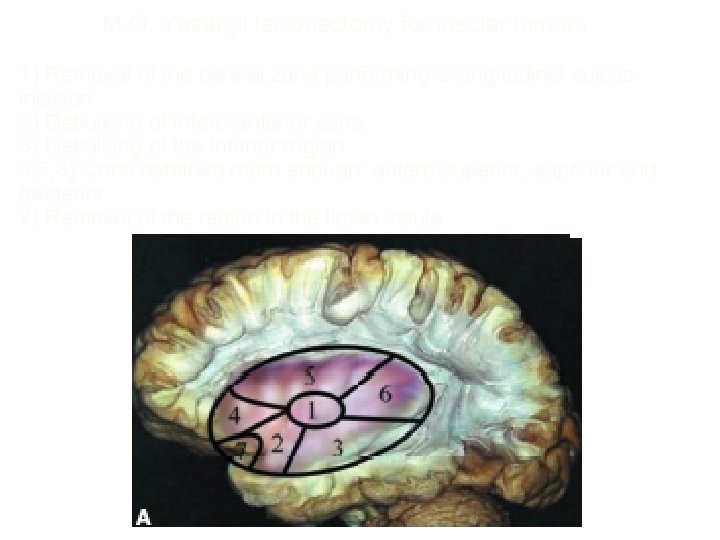 M. G. Yasargil lesionectomy for insular tumors 1) Removal of the central zone performing a longitudinal sulcus incision 2) Debulking of infero-anterior zone 3) Debulking of the inferior region 4, 5, 6) Once obtained room enough: antero-superior, superior and posterior 7) Removal of the region in the limen insula
M. G. Yasargil lesionectomy for insular tumors 1) Removal of the central zone performing a longitudinal sulcus incision 2) Debulking of infero-anterior zone 3) Debulking of the inferior region 4, 5, 6) Once obtained room enough: antero-superior, superior and posterior 7) Removal of the region in the limen insula
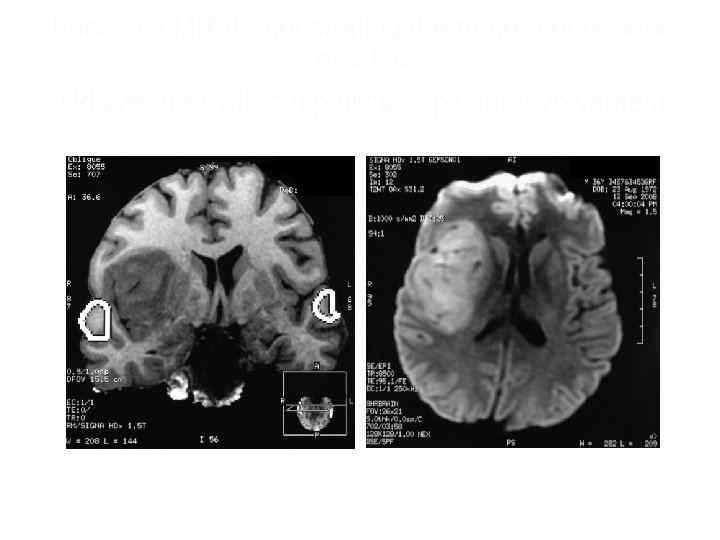 Fuctional MR demonstrating the tumor boundaries and the Uditive area without pallido-capsular involvement
Fuctional MR demonstrating the tumor boundaries and the Uditive area without pallido-capsular involvement
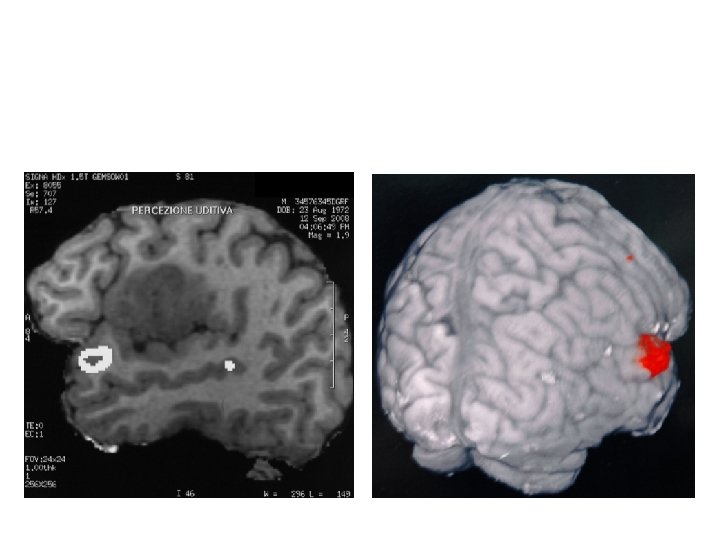 Functional MR demonstating temporal opercular region tumor involvement and uditive area to avoid during the tumor approach (no distraction of the opercula)
Functional MR demonstating temporal opercular region tumor involvement and uditive area to avoid during the tumor approach (no distraction of the opercula)
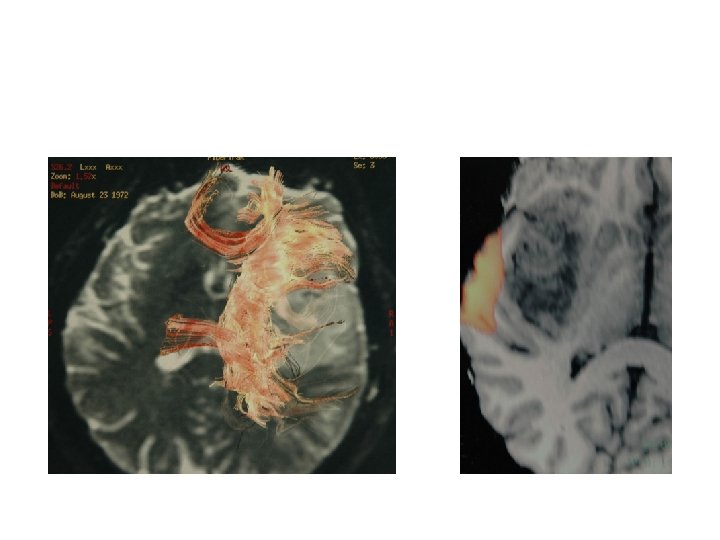 Tractography of capsula interna axial view and temporal opercular uditive area in right hemisphere
Tractography of capsula interna axial view and temporal opercular uditive area in right hemisphere
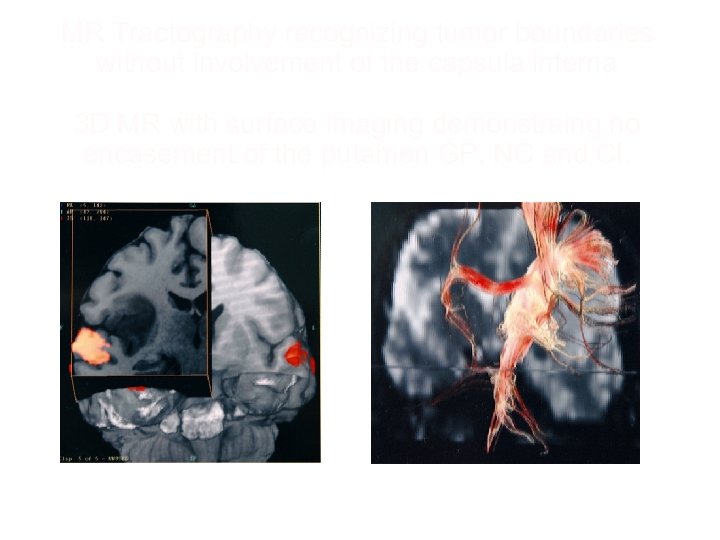 MR Tractography recognizing tumor boundaries without involvement of the capsula interna 3 D MR with surface imaging demonstraing no encasement of the putamen GP, NC and CI.
MR Tractography recognizing tumor boundaries without involvement of the capsula interna 3 D MR with surface imaging demonstraing no encasement of the putamen GP, NC and CI.
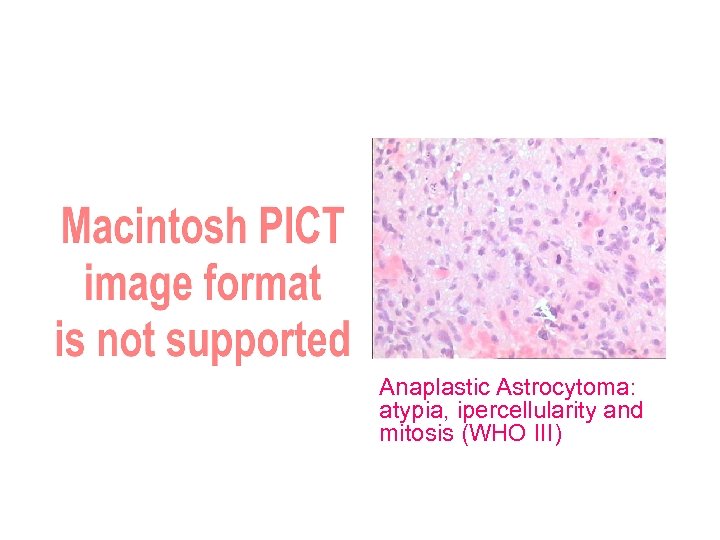 Tumor LSAs medial displacement Open biopsy: anaplastic glioma Anaplastic Astrocytoma: atypia, ipercellularity and mitosis (WHO III)
Tumor LSAs medial displacement Open biopsy: anaplastic glioma Anaplastic Astrocytoma: atypia, ipercellularity and mitosis (WHO III)


