7070006e194e8585d0a6eb0871593c74.ppt
- Количество слайдов: 48
 Allergic Disease Dr Garry M. Walsh, School of Medicine, University of Aberdeen
Allergic Disease Dr Garry M. Walsh, School of Medicine, University of Aberdeen
 Atopy • The predisposition to produce high quantities of Immunoglobulin (Ig)-E • Immediate (Type I hypersensitivity) • Mast cells, basophils, eosinophils, Th 2 cells
Atopy • The predisposition to produce high quantities of Immunoglobulin (Ig)-E • Immediate (Type I hypersensitivity) • Mast cells, basophils, eosinophils, Th 2 cells
 Allergy • Allergic Disease is mediated by Ig. E • First described by Prausnitz & Kustner in 1921 • Proposed the existence of “atopic reagin” in serum of allergic subjects • 45 years later Ishizaka described a new class of immunoglobulin - Ig. E
Allergy • Allergic Disease is mediated by Ig. E • First described by Prausnitz & Kustner in 1921 • Proposed the existence of “atopic reagin” in serum of allergic subjects • 45 years later Ishizaka described a new class of immunoglobulin - Ig. E
 Allergic Disease • • • Seen in 30 -35% of the population Perennial & seasonal allergic rhinitis Allergic (extrinsic asthma) Atopic and contact dermatitis Urticaria Food intolerance
Allergic Disease • • • Seen in 30 -35% of the population Perennial & seasonal allergic rhinitis Allergic (extrinsic asthma) Atopic and contact dermatitis Urticaria Food intolerance
 Allergy • Elevated Ig. E levels seen in allergy and parasitic infection • Binds to mast cells and basophils • Often specific for harmless environmental factors - allergens
Allergy • Elevated Ig. E levels seen in allergy and parasitic infection • Binds to mast cells and basophils • Often specific for harmless environmental factors - allergens
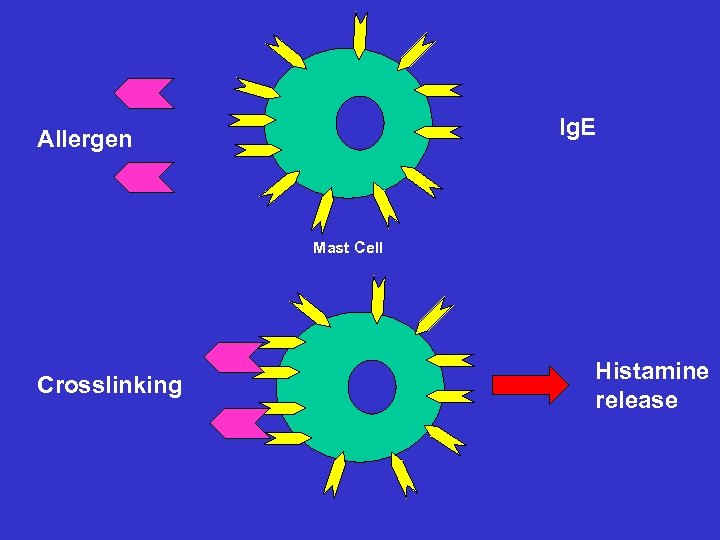 Ig. E Allergen Mast Cell Crosslinking Histamine release
Ig. E Allergen Mast Cell Crosslinking Histamine release
 Allergic rhinitis • Seasonal (pollen, spores) or perennial (house dust mite) • Mucus production (Runny nose, nasal stuffiness • Itching & sneezing • Treat with antihistamines or nasal steroids
Allergic rhinitis • Seasonal (pollen, spores) or perennial (house dust mite) • Mucus production (Runny nose, nasal stuffiness • Itching & sneezing • Treat with antihistamines or nasal steroids
 Urticaria • • • Wheal and flare Itching Allergen-induced Idiopathic – pressure, cold etc. Food – shellfish, strawberries, peanuts Treat with antihistamines
Urticaria • • • Wheal and flare Itching Allergen-induced Idiopathic – pressure, cold etc. Food – shellfish, strawberries, peanuts Treat with antihistamines
 Atopic dermatitis • Allergen –induced particularly milk protein from the gut enters blood stream –deposited in skin – mast cell degranulation • Exfoliating eczema and itching • Treat with antihistamines • May progress to asthma
Atopic dermatitis • Allergen –induced particularly milk protein from the gut enters blood stream –deposited in skin – mast cell degranulation • Exfoliating eczema and itching • Treat with antihistamines • May progress to asthma
 Anaphylaxis • • Very acute and severe reaction to allergen Peanuts, shellfish, penicillin, insect stings Allergen moves from gut to blood stream Massive histamine release from mast cells and basophils • Vasodilatation leads to dramatic drop in blood pressure • Often fatal if not treated with adrenaline
Anaphylaxis • • Very acute and severe reaction to allergen Peanuts, shellfish, penicillin, insect stings Allergen moves from gut to blood stream Massive histamine release from mast cells and basophils • Vasodilatation leads to dramatic drop in blood pressure • Often fatal if not treated with adrenaline
 Allergens • Environmental substances • Usually benign • Sub-group of individuals exhibit a hypersensitivity reaction (type 1)
Allergens • Environmental substances • Usually benign • Sub-group of individuals exhibit a hypersensitivity reaction (type 1)
 Allergens Mite faeces (digestive enzymes) Pollen Animal dander (cats) Insect stings Food
Allergens Mite faeces (digestive enzymes) Pollen Animal dander (cats) Insect stings Food
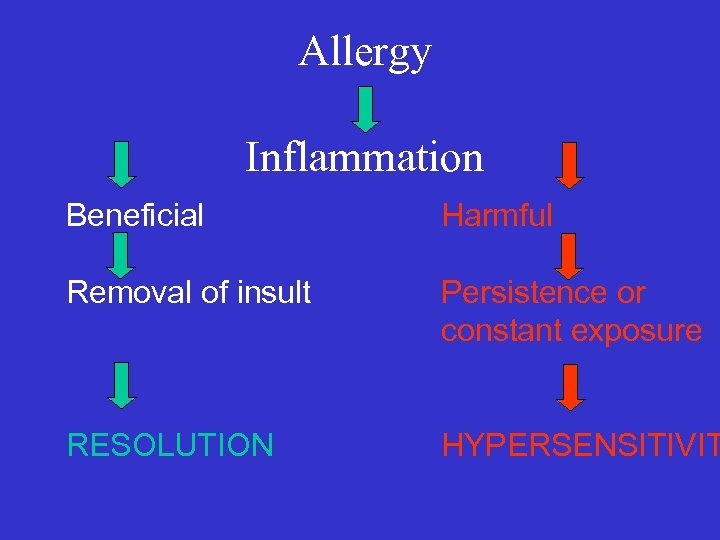 Allergy Inflammation Beneficial Harmful Removal of insult Persistence or constant exposure RESOLUTION HYPERSENSITIVIT
Allergy Inflammation Beneficial Harmful Removal of insult Persistence or constant exposure RESOLUTION HYPERSENSITIVIT
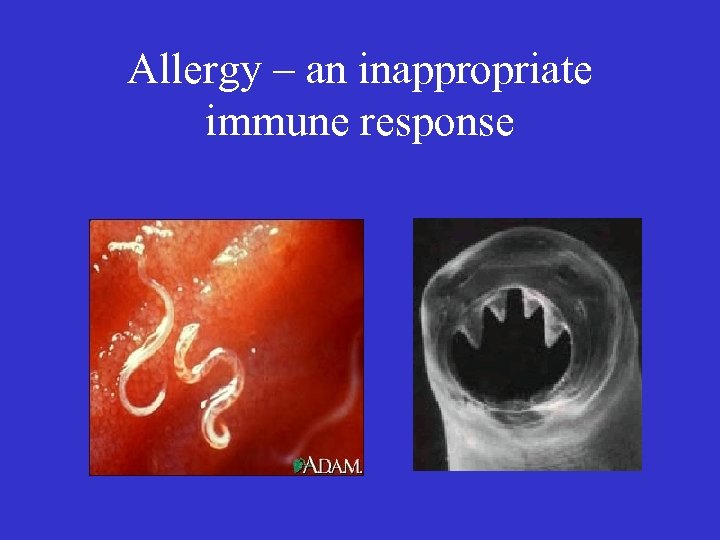 Allergy – an inappropriate immune response
Allergy – an inappropriate immune response
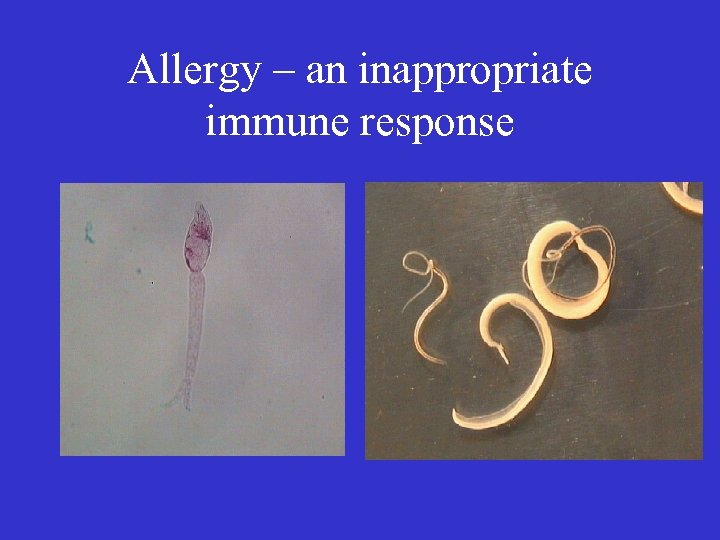 Allergy – an inappropriate immune response
Allergy – an inappropriate immune response
 Allergy – an inappropriate immune response • Parasite larvae – proteases • House dust mite – faeces (skin) – proteases • Pollen – proteases • Cat saliva - proteases
Allergy – an inappropriate immune response • Parasite larvae – proteases • House dust mite – faeces (skin) – proteases • Pollen – proteases • Cat saliva - proteases
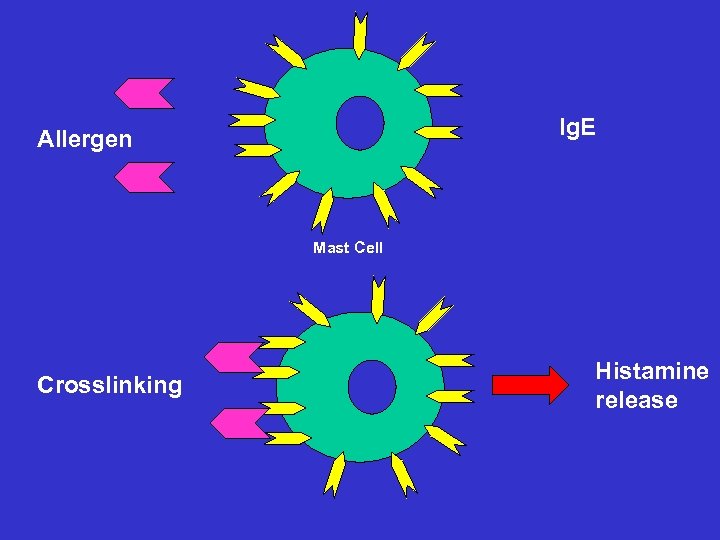 Ig. E Allergen Mast Cell Crosslinking Histamine release
Ig. E Allergen Mast Cell Crosslinking Histamine release
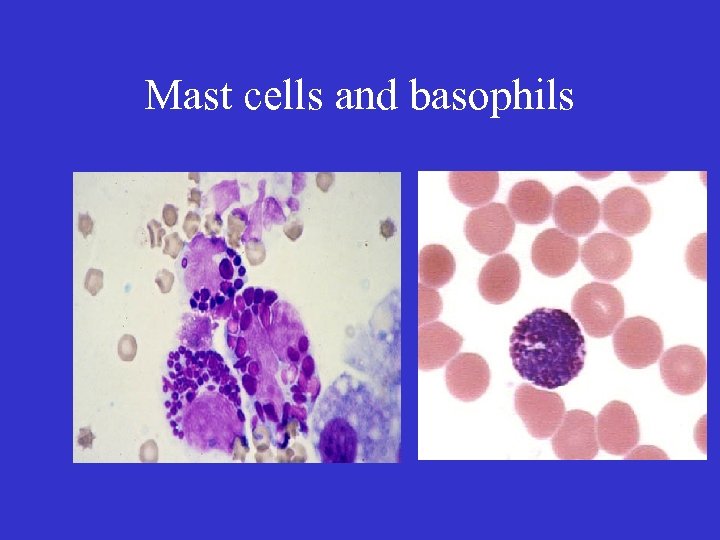 Mast cells and basophils
Mast cells and basophils
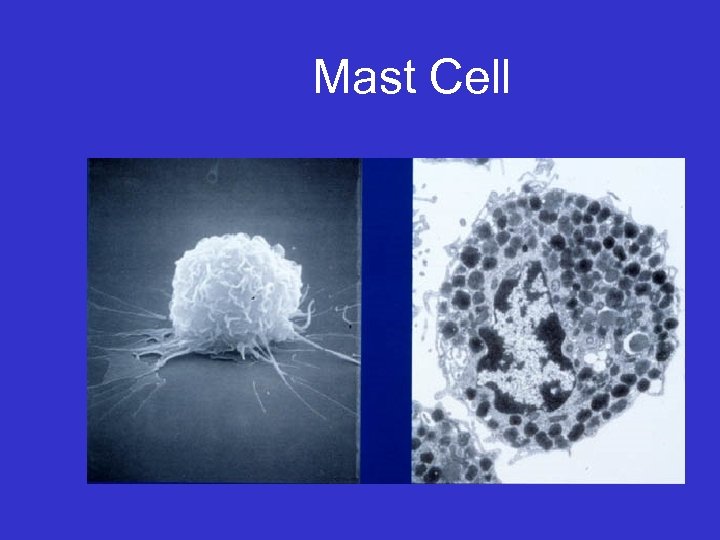 Mast Cell
Mast Cell
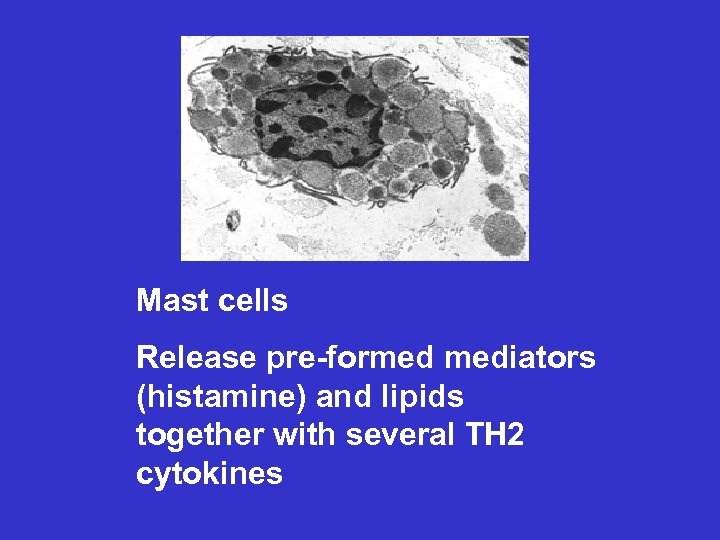 Mast cells Release pre-formed mediators (histamine) and lipids together with several TH 2 cytokines
Mast cells Release pre-formed mediators (histamine) and lipids together with several TH 2 cytokines
 Ig. E • Very low serum concentration – 0. 00005 mg/ml) • Sensitises mast cells and basophils by binding via Fc portion to high affinity receptor – Fce. R 1 • Serum half life of a few days • Binding protects Ig. E from destruction by serum proteases • Sensitisation can last for many months • Detected by skin prick test or radio absorbant test (RAST)
Ig. E • Very low serum concentration – 0. 00005 mg/ml) • Sensitises mast cells and basophils by binding via Fc portion to high affinity receptor – Fce. R 1 • Serum half life of a few days • Binding protects Ig. E from destruction by serum proteases • Sensitisation can last for many months • Detected by skin prick test or radio absorbant test (RAST)
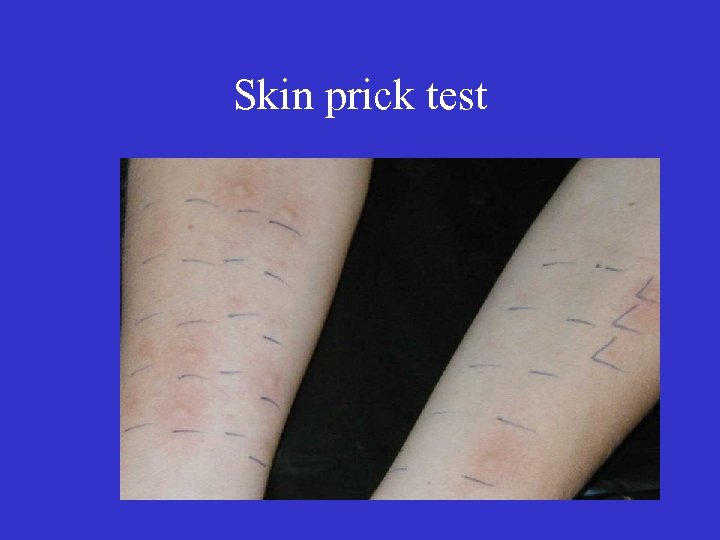 Skin prick test
Skin prick test
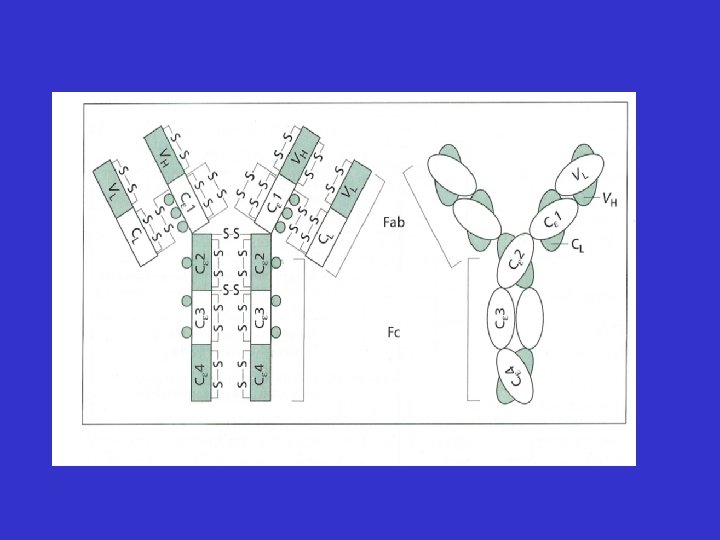
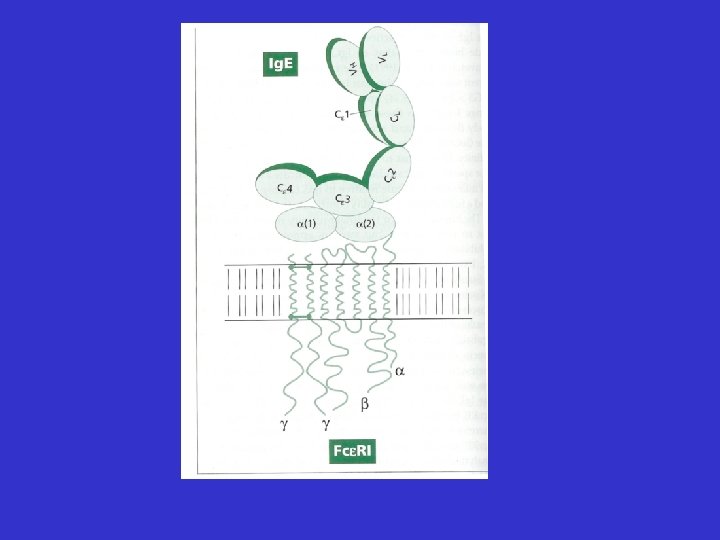
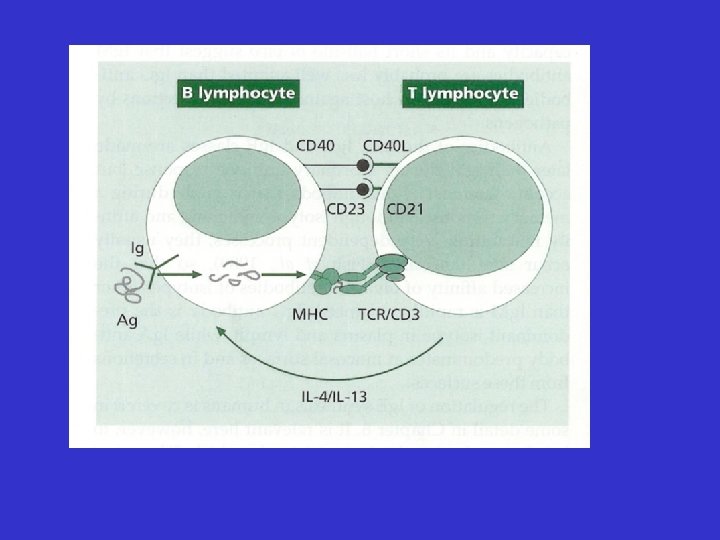

 Allergic Inflammation • Much more complex than histamine release • Involvement of a whole host of cells, cytokines, chemokines and mediators
Allergic Inflammation • Much more complex than histamine release • Involvement of a whole host of cells, cytokines, chemokines and mediators
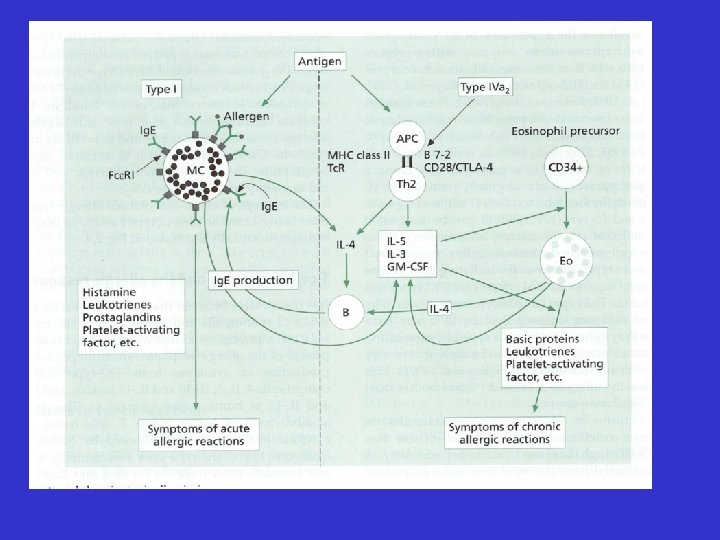
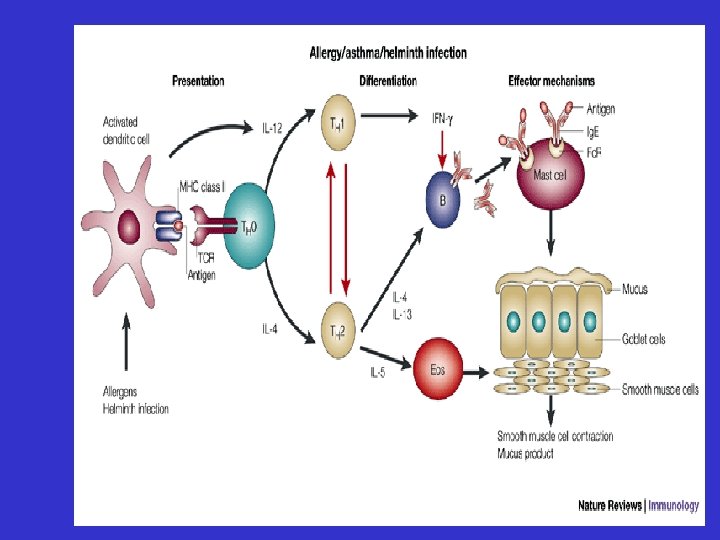
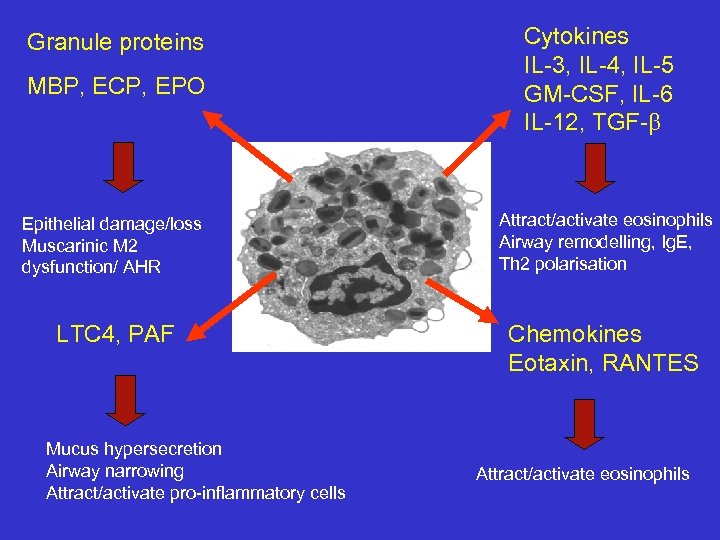 Granule proteins MBP, ECP, EPO Cytokines IL-3, IL-4, IL-5 GM-CSF, IL-6 IL-12, TGF-b Epithelial damage/loss Muscarinic M 2 dysfunction/ AHR Attract/activate eosinophils Airway remodelling, Ig. E, Th 2 polarisation LTC 4, PAF Chemokines Eotaxin, RANTES Mucus hypersecretion Airway narrowing Attract/activate pro-inflammatory cells Attract/activate eosinophils
Granule proteins MBP, ECP, EPO Cytokines IL-3, IL-4, IL-5 GM-CSF, IL-6 IL-12, TGF-b Epithelial damage/loss Muscarinic M 2 dysfunction/ AHR Attract/activate eosinophils Airway remodelling, Ig. E, Th 2 polarisation LTC 4, PAF Chemokines Eotaxin, RANTES Mucus hypersecretion Airway narrowing Attract/activate pro-inflammatory cells Attract/activate eosinophils
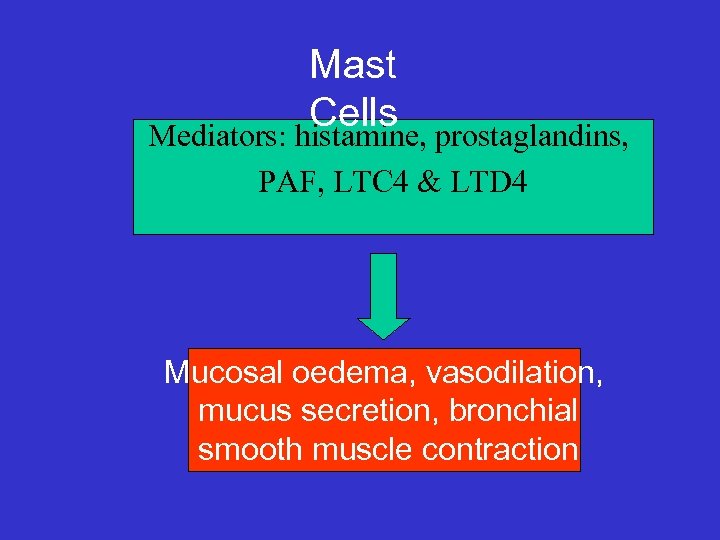 Mast Cells prostaglandins, Mediators: histamine, PAF, LTC 4 & LTD 4 Mucosal oedema, vasodilation, mucus secretion, bronchial smooth muscle contraction
Mast Cells prostaglandins, Mediators: histamine, PAF, LTC 4 & LTD 4 Mucosal oedema, vasodilation, mucus secretion, bronchial smooth muscle contraction
 Mast Cytokines. Cells (e. g. IL-4, IL-5, TNFa, IL-8): LTB 4, PAF Attract and activate neutrophils & eosinophils
Mast Cytokines. Cells (e. g. IL-4, IL-5, TNFa, IL-8): LTB 4, PAF Attract and activate neutrophils & eosinophils
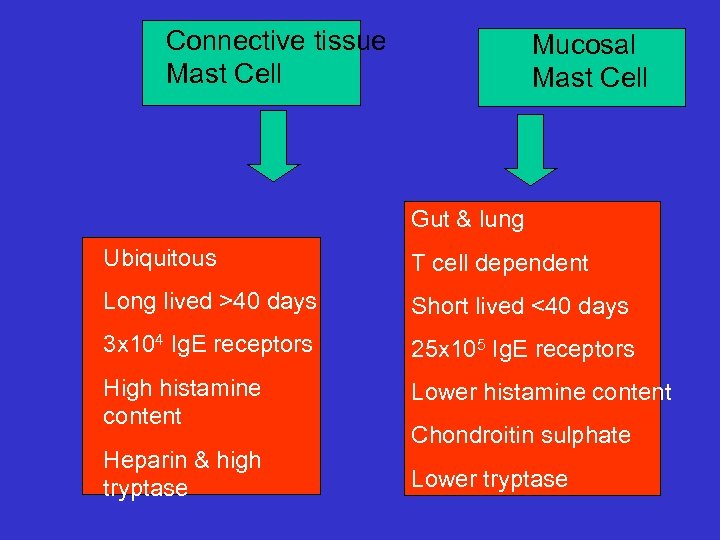 Connective tissue Mast Cell Mucosal Mast Cell Gut & lung Ubiquitous T cell dependent Long lived >40 days Short lived <40 days 3 x 104 Ig. E receptors 25 x 105 Ig. E receptors High histamine content Lower histamine content Heparin & high tryptase Lower tryptase Chondroitin sulphate
Connective tissue Mast Cell Mucosal Mast Cell Gut & lung Ubiquitous T cell dependent Long lived >40 days Short lived <40 days 3 x 104 Ig. E receptors 25 x 105 Ig. E receptors High histamine content Lower histamine content Heparin & high tryptase Lower tryptase Chondroitin sulphate
 Histamine • Skin – wheal, erythema, pruritis • Eye - conjunctivitis, erythema, pruritis • Nose – nasal discharge, sneeze, pruritis • Lung – bronchospasm of smooth muscle
Histamine • Skin – wheal, erythema, pruritis • Eye - conjunctivitis, erythema, pruritis • Nose – nasal discharge, sneeze, pruritis • Lung – bronchospasm of smooth muscle
 Histamine • Therapeutic intervention in allergy often focused on blocking the effects of histamine • Histamine also functions as a neurotransmitter in CNS • Very important in maintaining a state of arousal or awareness
Histamine • Therapeutic intervention in allergy often focused on blocking the effects of histamine • Histamine also functions as a neurotransmitter in CNS • Very important in maintaining a state of arousal or awareness
 First Generation Antihistamines • The first H 1 antagonist synthesised by Bovet & Staub at the Institut Pasteur • Too weak or toxic • Phenbezamine first effective antihistamine • Mepyramine maleate, diphenhydramine & tripelennamine developed in 1940’s • Still in use today
First Generation Antihistamines • The first H 1 antagonist synthesised by Bovet & Staub at the Institut Pasteur • Too weak or toxic • Phenbezamine first effective antihistamine • Mepyramine maleate, diphenhydramine & tripelennamine developed in 1940’s • Still in use today
 First Generation Antihistamines • Easily cross the blood–brain barrier. • Sedative and anticholinergic effects (sedating antihistamines). • Short half-lives. • Limited use in the treatment of allergic symptoms. • Still widely used, mainly as over-thecounter products, often in combination with other drugs.
First Generation Antihistamines • Easily cross the blood–brain barrier. • Sedative and anticholinergic effects (sedating antihistamines). • Short half-lives. • Limited use in the treatment of allergic symptoms. • Still widely used, mainly as over-thecounter products, often in combination with other drugs.
 Second Generation Antihistamines • Highly effective treatments for allergic disease • Do not cross blood-brain barrier • Lack significant CNS & anticholinergic effects • Long half life • Among the most frequently prescribed and safest drugs - expensive
Second Generation Antihistamines • Highly effective treatments for allergic disease • Do not cross blood-brain barrier • Lack significant CNS & anticholinergic effects • Long half life • Among the most frequently prescribed and safest drugs - expensive
 Other treatments • Nasal steroids – must be given before season – relieve nasal blockade • Antihistamines combined with antileukotriene drugs • Avoidance -mattress covers, specialised Hoovers, wood floors,
Other treatments • Nasal steroids – must be given before season – relieve nasal blockade • Antihistamines combined with antileukotriene drugs • Avoidance -mattress covers, specialised Hoovers, wood floors,
 Allergic Disease • Dramatic increase in allergic disease over the past three decades, why is this? • Genetics • Environmental factors - pollution • Changes in Lifestyle • Occupational
Allergic Disease • Dramatic increase in allergic disease over the past three decades, why is this? • Genetics • Environmental factors - pollution • Changes in Lifestyle • Occupational
 Genetics (1) • Family history of allergic disease is a strong risk factor for developing asthma • Danger of developing asthma particularly if one or both parents are atopic • Children with atopic dermatitis at risk of asthma -– “the allergic
Genetics (1) • Family history of allergic disease is a strong risk factor for developing asthma • Danger of developing asthma particularly if one or both parents are atopic • Children with atopic dermatitis at risk of asthma -– “the allergic
 Genetics (2) • No single "allergy or asthma chromosome". Several markers demonstrated in small selected populations - much further work is required • The genetics of allergy and asthma are polygenic - influence many factors such as Ig. E secretion, cytokines and inflammatory cell
Genetics (2) • No single "allergy or asthma chromosome". Several markers demonstrated in small selected populations - much further work is required • The genetics of allergy and asthma are polygenic - influence many factors such as Ig. E secretion, cytokines and inflammatory cell
 Environment (1) • Children & adults 90% spent time indoors • Allergens in dust (dust mite faeces) or pets (particularly cats) - increased risk of allergic sensitization in proportion to exposure. • Most children and adolescents with asthma sensitized to indoor allergens - avoidance often leads to improvement in airway disease. • Modern housing generally poorly ventilated with fitted carpets and central heating - house dust mite infestation
Environment (1) • Children & adults 90% spent time indoors • Allergens in dust (dust mite faeces) or pets (particularly cats) - increased risk of allergic sensitization in proportion to exposure. • Most children and adolescents with asthma sensitized to indoor allergens - avoidance often leads to improvement in airway disease. • Modern housing generally poorly ventilated with fitted carpets and central heating - house dust mite infestation
 Environment (2) • Children exposed to tobacco smoke more likely to develop wheezing and impaired lung function • Outdoor allergens –seasonal variation and weather • Account for 10 -20% of allergic disease in Europe - mainly hay fever. • Increased pollution not responsible for increase in allergic disease - pollutants worsen respiratory symptoms in asthmatics
Environment (2) • Children exposed to tobacco smoke more likely to develop wheezing and impaired lung function • Outdoor allergens –seasonal variation and weather • Account for 10 -20% of allergic disease in Europe - mainly hay fever. • Increased pollution not responsible for increase in allergic disease - pollutants worsen respiratory symptoms in asthmatics
 Changes in Lifestyle (1) • Hygiene hypothesis - Past 30 years - changes in pattern of childhood infection, many no longer experienced • Exposure to certain infections may protect against the development of allergies. • Respiratory viruses may be a risk factor for the development of asthma • Vaccination programmes not thought to have direct effect on the development of allergic disease
Changes in Lifestyle (1) • Hygiene hypothesis - Past 30 years - changes in pattern of childhood infection, many no longer experienced • Exposure to certain infections may protect against the development of allergies. • Respiratory viruses may be a risk factor for the development of asthma • Vaccination programmes not thought to have direct effect on the development of allergic disease
 Changes in Lifestyle (2) • Intake of fresh fruit and vegetables has declined leading to lower anti-oxidant levels. • Certain fatty acids are able to shift the immune system towards allergic susceptibility • Food preservatives may effect gut flora leading to allergic sensitization rather than development of tolerance
Changes in Lifestyle (2) • Intake of fresh fruit and vegetables has declined leading to lower anti-oxidant levels. • Certain fatty acids are able to shift the immune system towards allergic susceptibility • Food preservatives may effect gut flora leading to allergic sensitization rather than development of tolerance
 Changes in Lifestyle (3) • The immune system is severely compromised by poor nutrition • Paradoxically the vast improvement in nutrition in the last fifty years might have led to the immune systems of some individuals "over reacting" to benign substances i. e. allergens
Changes in Lifestyle (3) • The immune system is severely compromised by poor nutrition • Paradoxically the vast improvement in nutrition in the last fifty years might have led to the immune systems of some individuals "over reacting" to benign substances i. e. allergens
 Conclusion • Atopy – propensity to produce high levels of Ig. E from B cells • Allergens mimic parasites – processed and presented by APC (e. g. dendritic cells) • Orchestrated by Th 2 cells – cytokine release • Effector cells – mast cells, basophils • Mediators – cytokines, histamine, leukotrienes, PAF etc.
Conclusion • Atopy – propensity to produce high levels of Ig. E from B cells • Allergens mimic parasites – processed and presented by APC (e. g. dendritic cells) • Orchestrated by Th 2 cells – cytokine release • Effector cells – mast cells, basophils • Mediators – cytokines, histamine, leukotrienes, PAF etc.


