adbb30d829af8f6f3a459855c2392eb8.ppt
- Количество слайдов: 43
 Alcohol Use Disorders in Primary Care Stephen Maisto, Ph. D. Jennifer S. Funderburk, Ph. D. Center for Integrated Healthcare Syracuse University
Alcohol Use Disorders in Primary Care Stephen Maisto, Ph. D. Jennifer S. Funderburk, Ph. D. Center for Integrated Healthcare Syracuse University
 Alcohol Use and Primary Care Heavy/problem alcohol use is a major public health problem “Cost of illness” estimate: $166. 5 billion in 1995 (Schneider Institute for Health Policy, 2001) Primary care as a major entry point in the healthcare system for individuals with behavioral problems Opportunity for early intervention and identification of harmful alcohol use Harmful alcohol use are priorities within the VA
Alcohol Use and Primary Care Heavy/problem alcohol use is a major public health problem “Cost of illness” estimate: $166. 5 billion in 1995 (Schneider Institute for Health Policy, 2001) Primary care as a major entry point in the healthcare system for individuals with behavioral problems Opportunity for early intervention and identification of harmful alcohol use Harmful alcohol use are priorities within the VA
 Objectives for this Workshop Discuss: – Empirically supported screening measures useful to screen for alcohol misuse in primary care – Brief interventions that can be used in the primary care environment for high risk drinking
Objectives for this Workshop Discuss: – Empirically supported screening measures useful to screen for alcohol misuse in primary care – Brief interventions that can be used in the primary care environment for high risk drinking
 After this workshop, you should feel comfortable Conducting further assessment of alcohol misuse with patients Identifying the specific courses of action to take with a patient reporting either hazardous drinking, alcohol abuse, or alcohol dependence Understanding how to effectively deliver the World Health Organization’s Simple Advice brief alcohol intervention
After this workshop, you should feel comfortable Conducting further assessment of alcohol misuse with patients Identifying the specific courses of action to take with a patient reporting either hazardous drinking, alcohol abuse, or alcohol dependence Understanding how to effectively deliver the World Health Organization’s Simple Advice brief alcohol intervention
 Process Screening Assessment Intervention
Process Screening Assessment Intervention
 Alcohol Screening Definition: The use of empirically-based procedures for identifying individuals with alcohol-related problems or consequences, or those who are at risk for such difficulties.
Alcohol Screening Definition: The use of empirically-based procedures for identifying individuals with alcohol-related problems or consequences, or those who are at risk for such difficulties.
 NIAAA Recommendations Single Question: – How many times in the past year have you had: MEN: 5 or more drinks in a day? WOMEN: 4 or more drinks in a day? AUDIT – 10 -item self-report questionnaire
NIAAA Recommendations Single Question: – How many times in the past year have you had: MEN: 5 or more drinks in a day? WOMEN: 4 or more drinks in a day? AUDIT – 10 -item self-report questionnaire
 WITHIN VA: AUDIT-C 1) How often do you have a drink containing alcohol? Never (0), Monthly or less (1), 2 -4 times a month (2), 2 -3 times a week (3), 4 or more times a week (4) 2) How many drinks containing alcohol do you have on a typical day when you are drinking? 1 or 2 (0), 3 or 4 (1), 5 or 6 (2), 7, 8, or 9 (3), 10 or more (4) 3) How often do you have six or more drinks on one occasion? Never (0), less than monthly (1), Monthly (2), Weekly (3), Daily or almost daily (4)
WITHIN VA: AUDIT-C 1) How often do you have a drink containing alcohol? Never (0), Monthly or less (1), 2 -4 times a month (2), 2 -3 times a week (3), 4 or more times a week (4) 2) How many drinks containing alcohol do you have on a typical day when you are drinking? 1 or 2 (0), 3 or 4 (1), 5 or 6 (2), 7, 8, or 9 (3), 10 or more (4) 3) How often do you have six or more drinks on one occasion? Never (0), less than monthly (1), Monthly (2), Weekly (3), Daily or almost daily (4)
 AUDIT-C Annual Clinical Reminder within VA primary care clinics; a part of the pay for performance for PCPs Developed to effectively screen for excessive drinking or alcohol use disorders in the past year 3 -items Scores range from 0 to 12 Designed to be given in paper format Those individuals that would benefit from reducing or ceasing drinking score: – Men ≥ 4 – Women ≥ 3 Cross-national standardization (see Bradley et al. , 2007)
AUDIT-C Annual Clinical Reminder within VA primary care clinics; a part of the pay for performance for PCPs Developed to effectively screen for excessive drinking or alcohol use disorders in the past year 3 -items Scores range from 0 to 12 Designed to be given in paper format Those individuals that would benefit from reducing or ceasing drinking score: – Men ≥ 4 – Women ≥ 3 Cross-national standardization (see Bradley et al. , 2007)
 Common Concerns About AUDIT-C Cut-offs for the AUDIT-C seem too sensitive – Goal of a screening measure: Maximize sensitivity and specificity Not meant to diagnose, rather identify those individuals needing further assessment – Bradley et al. (2007) conducted a crosssectional validation study— 1, 319 patients Found: Current cut-offs maximized sensitivity (. 86) and specificity (. 89) for detecting alcohol misuse, if you increased the cut-off for males to 5 reduced sensitivity to. 72
Common Concerns About AUDIT-C Cut-offs for the AUDIT-C seem too sensitive – Goal of a screening measure: Maximize sensitivity and specificity Not meant to diagnose, rather identify those individuals needing further assessment – Bradley et al. (2007) conducted a crosssectional validation study— 1, 319 patients Found: Current cut-offs maximized sensitivity (. 86) and specificity (. 89) for detecting alcohol misuse, if you increased the cut-off for males to 5 reduced sensitivity to. 72
 Process Screening Assessment Intervention
Process Screening Assessment Intervention
 FURTHER ASSESSMENT Goals: – Assess for symptoms of: Alcohol Dependence Alcohol Abuse Hazardous Alcohol Use
FURTHER ASSESSMENT Goals: – Assess for symptoms of: Alcohol Dependence Alcohol Abuse Hazardous Alcohol Use
 Definitions Alcohol Dependence: alcohol consumption that may result in a physical dependence on alcohol and results in clinical distress/impairment Harmful Use/Alcohol Abuse: “alcohol consumption that results in consequences to physical and mental health” (World Health Organization, 2001) Hazardous Drinking: “pattern of alcohol consumption that increases the risk of harmful consequences for the user or others” (World Health Organization, 2001)
Definitions Alcohol Dependence: alcohol consumption that may result in a physical dependence on alcohol and results in clinical distress/impairment Harmful Use/Alcohol Abuse: “alcohol consumption that results in consequences to physical and mental health” (World Health Organization, 2001) Hazardous Drinking: “pattern of alcohol consumption that increases the risk of harmful consequences for the user or others” (World Health Organization, 2001)
 Assessment Can use DSM-IV checklist provided You can start by asking: – What are your drinking habits like? – How much have you been drinking? – What have you been drinking? – Has there ever been a time when you had 5 or more drinks on one occasion in the last year?
Assessment Can use DSM-IV checklist provided You can start by asking: – What are your drinking habits like? – How much have you been drinking? – What have you been drinking? – Has there ever been a time when you had 5 or more drinks on one occasion in the last year?
 Further Assessment for Alcohol Dependence Focuses on DSM-IV criteria – Has the patient in the past 12 months: had to drink more to get the same effect experienced withdrawal symptoms when cutting down or trying to quit? (i. e. , sweating, nausea, tremors, insomnia when cutting down or trying to quit drinking) repeatedly drank more than they were planning to? repeatedly failed at cutting down or quitting drinking or persistently wanted to stop drinking? spent the majority of time drinking or recovering from drinking? given up other important activities to go drinking? continued drinking despite physical or psychological problems (e. g. , blackouts, anxiety)?
Further Assessment for Alcohol Dependence Focuses on DSM-IV criteria – Has the patient in the past 12 months: had to drink more to get the same effect experienced withdrawal symptoms when cutting down or trying to quit? (i. e. , sweating, nausea, tremors, insomnia when cutting down or trying to quit drinking) repeatedly drank more than they were planning to? repeatedly failed at cutting down or quitting drinking or persistently wanted to stop drinking? spent the majority of time drinking or recovering from drinking? given up other important activities to go drinking? continued drinking despite physical or psychological problems (e. g. , blackouts, anxiety)?
 Further Assessment for Alcohol Abuse Focuses on DSM-IV criteria: – In the past 12 months, has the patient’s drinking repeatedly (more than once) caused or been associated with: Failures in Responsibility (e. g. , going to work, doing chores around the house)? Bodily Risk? (e. g. driving while intoxicated) Problems with the Law? Problems with Family and / or Friends?
Further Assessment for Alcohol Abuse Focuses on DSM-IV criteria: – In the past 12 months, has the patient’s drinking repeatedly (more than once) caused or been associated with: Failures in Responsibility (e. g. , going to work, doing chores around the house)? Bodily Risk? (e. g. driving while intoxicated) Problems with the Law? Problems with Family and / or Friends?
 What is a Standard Drink? 5 oz. wine 12 oz. beer 1. 5 oz of spirits
What is a Standard Drink? 5 oz. wine 12 oz. beer 1. 5 oz of spirits
 Assessment for Hazardous Use Focuses on clarifying quantity and frequency of drinking: – ON ANY DAY: Drinking more than 4 standard drinks (men ≤ 65) or 3 standard drinks (women and men > 65) – IN ANY TYPICAL WEEK: Drinking more than 14 standard drinks (men ≤ 65) or 7 standard drinks (women and men > 65) – Drinking more than an average of 2 standard drinks per day (men ≤ 65) or drinking more than an average of 1 standard drink per day (women and men > 65) Defined by NIAAA, 2005
Assessment for Hazardous Use Focuses on clarifying quantity and frequency of drinking: – ON ANY DAY: Drinking more than 4 standard drinks (men ≤ 65) or 3 standard drinks (women and men > 65) – IN ANY TYPICAL WEEK: Drinking more than 14 standard drinks (men ≤ 65) or 7 standard drinks (women and men > 65) – Drinking more than an average of 2 standard drinks per day (men ≤ 65) or drinking more than an average of 1 standard drink per day (women and men > 65) Defined by NIAAA, 2005
 Process Screening Assessment Intervention
Process Screening Assessment Intervention
 Institute of Medicine (1990) None Alcohol Consumption Light Moderate Substantial Heavy Severe Substantial Mild None Moderate Alcohol Problems
Institute of Medicine (1990) None Alcohol Consumption Light Moderate Substantial Heavy Severe Substantial Mild None Moderate Alcohol Problems
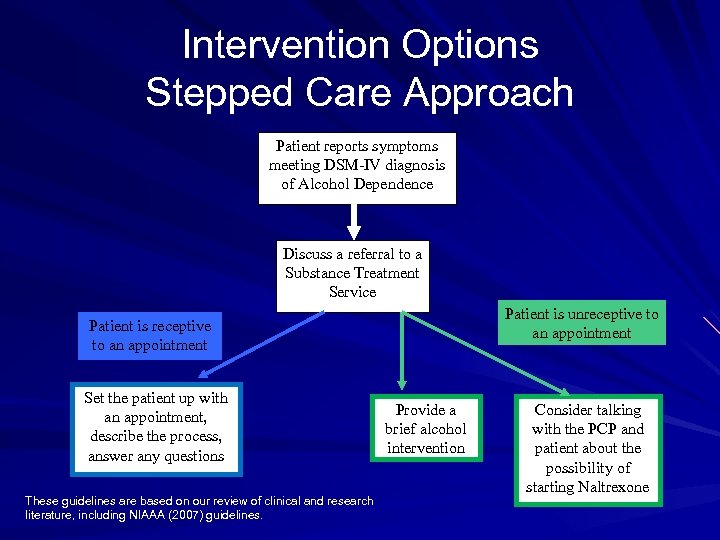 Intervention Options Stepped Care Approach Patient reports symptoms meeting DSM-IV diagnosis of Alcohol Dependence Discuss a referral to a Substance Treatment Service Patient is unreceptive to an appointment Patient is receptive to an appointment Set the patient up with an appointment, describe the process, answer any questions These guidelines are based on our review of clinical and research literature, including NIAAA (2007) guidelines. Provide a brief alcohol intervention Consider talking with the PCP and patient about the possibility of starting Naltrexone
Intervention Options Stepped Care Approach Patient reports symptoms meeting DSM-IV diagnosis of Alcohol Dependence Discuss a referral to a Substance Treatment Service Patient is unreceptive to an appointment Patient is receptive to an appointment Set the patient up with an appointment, describe the process, answer any questions These guidelines are based on our review of clinical and research literature, including NIAAA (2007) guidelines. Provide a brief alcohol intervention Consider talking with the PCP and patient about the possibility of starting Naltrexone
 Basic Information: Naltrexone FDA-approved medication for alcohol dependence Has been associated with fewer drinking days, reduced rates of relapse, briefer relapse, and reduced drinking during relapse periods It is thought to work by reducing an individual’s craving
Basic Information: Naltrexone FDA-approved medication for alcohol dependence Has been associated with fewer drinking days, reduced rates of relapse, briefer relapse, and reduced drinking during relapse periods It is thought to work by reducing an individual’s craving
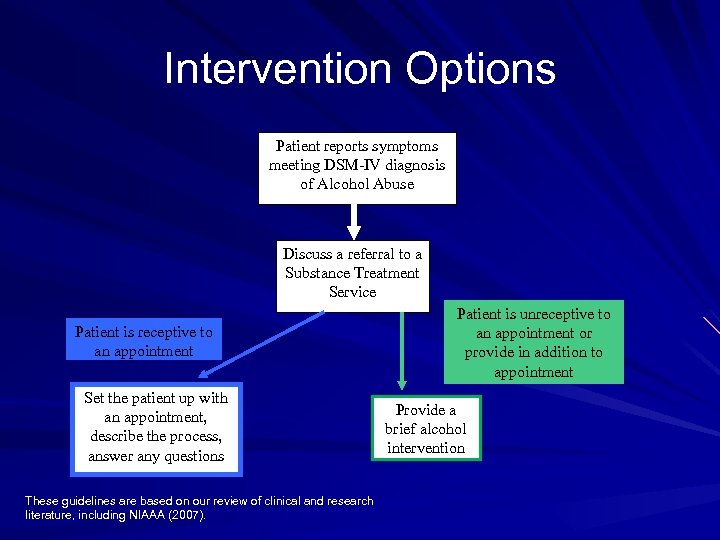 Intervention Options Patient reports symptoms meeting DSM-IV diagnosis of Alcohol Abuse Discuss a referral to a Substance Treatment Service Patient is receptive to an appointment Set the patient up with an appointment, describe the process, answer any questions These guidelines are based on our review of clinical and research literature, including NIAAA (2007). Patient is unreceptive to an appointment or provide in addition to appointment Provide a brief alcohol intervention
Intervention Options Patient reports symptoms meeting DSM-IV diagnosis of Alcohol Abuse Discuss a referral to a Substance Treatment Service Patient is receptive to an appointment Set the patient up with an appointment, describe the process, answer any questions These guidelines are based on our review of clinical and research literature, including NIAAA (2007). Patient is unreceptive to an appointment or provide in addition to appointment Provide a brief alcohol intervention
 Intervention Options Patient reports hazardous/harmful drinking Provide a brief alcohol intervention These guidelines are based on our review of clinical and research literature.
Intervention Options Patient reports hazardous/harmful drinking Provide a brief alcohol intervention These guidelines are based on our review of clinical and research literature.
 STYLE OF COMMUNICATION THROUGHOUT ALL DISCUSSIONS
STYLE OF COMMUNICATION THROUGHOUT ALL DISCUSSIONS
 MOTIVATIONAL INTERVIEWING DANCE RATHER THAN WRESTLE WITH THE PATIENT CLINICAL TOOLS: – LISTEN – ELICIT-PROVIDE-ELICIT – IDENTIFY THE CHANGE TALK – USE REFLECTIVE LISTENING TO RESPOND TO CHANGE TALK
MOTIVATIONAL INTERVIEWING DANCE RATHER THAN WRESTLE WITH THE PATIENT CLINICAL TOOLS: – LISTEN – ELICIT-PROVIDE-ELICIT – IDENTIFY THE CHANGE TALK – USE REFLECTIVE LISTENING TO RESPOND TO CHANGE TALK
 IDENTIFY WHERE THE PATIENT IS ON THE STAGES OF CHANGE “Using the ruler below, indicate how ready you are to make a change in your drinking. ” 1 2 Not Ready to Change 3 4 Unsure 5 6 7 Ready to Change 8 9 Trying to Change 10
IDENTIFY WHERE THE PATIENT IS ON THE STAGES OF CHANGE “Using the ruler below, indicate how ready you are to make a change in your drinking. ” 1 2 Not Ready to Change 3 4 Unsure 5 6 7 Ready to Change 8 9 Trying to Change 10
 Motivational Interviewing PATIENT CENTEREDNESS: – MATCH YOUR COMMUNICATION ABOUT INTERVENTION TO THE PATIENT’S STAGE OF CHANGE Pre-contemplation—focus on education, self-assessment Contemplation—Avoid argument, use reflective listening, roll with resistance, use decisional balance (what are the pros/cons to drinking? ) Preparation/Action—Set S. M. A. R. T. (specific, measurable, attainable, realistic, and timely) goals; be positive about goals set Maintenance—focus on relapse prevention
Motivational Interviewing PATIENT CENTEREDNESS: – MATCH YOUR COMMUNICATION ABOUT INTERVENTION TO THE PATIENT’S STAGE OF CHANGE Pre-contemplation—focus on education, self-assessment Contemplation—Avoid argument, use reflective listening, roll with resistance, use decisional balance (what are the pros/cons to drinking? ) Preparation/Action—Set S. M. A. R. T. (specific, measurable, attainable, realistic, and timely) goals; be positive about goals set Maintenance—focus on relapse prevention
 Brief Interventions for High Risk Drinking “time limited, patient-centered counseling strategy that focuses on changing patient behavior and increasing patient compliance with therapy” (Fleming et al. , 1999) 1, 5 -min. session to 3, 1 -hour sessions Strong evidence for the efficacy of brief interventions (Bertholet et al. , 2005; Bien et al. , 1993; Kahan et al. , 1995; Moyer et al. , 2002; Wilk et al. , 1997; Whitlock et al. , 2004) – Efficacious for substantial reductions of alcohol use compared to no treatment controls Examples: – Based on review by Whitlock et al. , 2004 --10 -19% more of those participants receiving the intervention achieved recommended drinking levels in comparison to no treatment controls – WHO brief alcohol intervention– 21% reduction in alcohol use – These reductions are maintained at 12 month follow-ups
Brief Interventions for High Risk Drinking “time limited, patient-centered counseling strategy that focuses on changing patient behavior and increasing patient compliance with therapy” (Fleming et al. , 1999) 1, 5 -min. session to 3, 1 -hour sessions Strong evidence for the efficacy of brief interventions (Bertholet et al. , 2005; Bien et al. , 1993; Kahan et al. , 1995; Moyer et al. , 2002; Wilk et al. , 1997; Whitlock et al. , 2004) – Efficacious for substantial reductions of alcohol use compared to no treatment controls Examples: – Based on review by Whitlock et al. , 2004 --10 -19% more of those participants receiving the intervention achieved recommended drinking levels in comparison to no treatment controls – WHO brief alcohol intervention– 21% reduction in alcohol use – These reductions are maintained at 12 month follow-ups
 World Health Organization: Simple Advice see handouts Provider reviews with participant: • The Drinker’s Pyramid • Health risks of drinking • Low-risk drinking and standard drink definitions • Consideration of cutting back or abstaining Provider encourages veteran to set a goal of cutting back or abstaining Provider provides veteran with encouragement toward maintaining his/her goal
World Health Organization: Simple Advice see handouts Provider reviews with participant: • The Drinker’s Pyramid • Health risks of drinking • Low-risk drinking and standard drink definitions • Consideration of cutting back or abstaining Provider encourages veteran to set a goal of cutting back or abstaining Provider provides veteran with encouragement toward maintaining his/her goal
 Booster sessions 2 telephone booster sessions – Recommend 2 weeks and 4 weeks after brief alcohol intervention – Inquire about goal – Assess for problems maintaining goal If participant is experiencing problems: – Briefly discuss problem solving – Provide encouragement “I’m just calling today to check in with you regarding our conversation 2 weeks ago. I wanted to see how you have been doing regarding the goals that we set around your alcohol use. ”
Booster sessions 2 telephone booster sessions – Recommend 2 weeks and 4 weeks after brief alcohol intervention – Inquire about goal – Assess for problems maintaining goal If participant is experiencing problems: – Briefly discuss problem solving – Provide encouragement “I’m just calling today to check in with you regarding our conversation 2 weeks ago. I wanted to see how you have been doing regarding the goals that we set around your alcohol use. ”
 NIAAA Recommendations Advise and Assist – State your conclusion and recommendation clearly – Gauge readiness to change Precontemplation-Contemplation---restate concern, encourage reflection, willingness to help Contemplation---Action---set a goal, agree on a plan
NIAAA Recommendations Advise and Assist – State your conclusion and recommendation clearly – Gauge readiness to change Precontemplation-Contemplation---restate concern, encourage reflection, willingness to help Contemplation---Action---set a goal, agree on a plan
 Role-Play
Role-Play
 Common Tricky Areas & Solutions View that different alcoholic beverages are different in their effects (e. g. , I drink beer not alcohol) – Avoid argumentation, just review standard drinks Identifying that the individual is drinking at a high risk level may trigger strong reactions – Avoid creating additional resistance, remember to roll with them – “From what you’ve said I can see that you do not see yourself as a high risk drinker. Let’s just look at what research shows as some of the things that can happen at your current level of alcohol use. ”
Common Tricky Areas & Solutions View that different alcoholic beverages are different in their effects (e. g. , I drink beer not alcohol) – Avoid argumentation, just review standard drinks Identifying that the individual is drinking at a high risk level may trigger strong reactions – Avoid creating additional resistance, remember to roll with them – “From what you’ve said I can see that you do not see yourself as a high risk drinker. Let’s just look at what research shows as some of the things that can happen at your current level of alcohol use. ”
 Common Tricky Areas & Solutions Express your concern as a way to break down resistance – “I’m concerned about your current level of drinking and how it may be increasing…. (e. g, your depressed mood, sleep problems) Support patient’s independence – “Obviously, you need to evaluate the situation yourself and whether or not you should be concerned about the potential consequences of drinking heavily is up to you.
Common Tricky Areas & Solutions Express your concern as a way to break down resistance – “I’m concerned about your current level of drinking and how it may be increasing…. (e. g, your depressed mood, sleep problems) Support patient’s independence – “Obviously, you need to evaluate the situation yourself and whether or not you should be concerned about the potential consequences of drinking heavily is up to you.
 Common Tricky Areas & Solutions When setting the drinking goal at the end, be sensitive to patient’s reaction – Allow patient to take the lead – “It’s up to you to decide what to do about your drinking. Because of your reluctance, what do you think about spending some time thinking about what we’ve discussed today. ” – “Based on what we’ve talked about today, I would suggest that you reduce from 2 beers a night to 1 beer a night. What do you think about that?
Common Tricky Areas & Solutions When setting the drinking goal at the end, be sensitive to patient’s reaction – Allow patient to take the lead – “It’s up to you to decide what to do about your drinking. Because of your reluctance, what do you think about spending some time thinking about what we’ve discussed today. ” – “Based on what we’ve talked about today, I would suggest that you reduce from 2 beers a night to 1 beer a night. What do you think about that?
 Modifying the Simple Advice Intervention for the Telephone Send materials to the patient prior to phone call – Include a cover letter indicating to the patient that you will help them understand these handouts once you talk during the scheduled appointment Be prepared it will be more difficult because you won’t be able to see the patient’s facial reactions Make sure you review the patient’s medical chart (e. g. , look at age of patient, previous treatment, psychiatric diagnoses, and medical issues) If you have never met the patient: – It may be more helpful to conduct the intervention within the arena of talking to the patient about health behaviors in general – Send along some (1 -2) additional handouts on other health behaviors that might be good to include – Begin by assessing health behaviors, including alcohol use – Discuss how the patient wants to improve his/her health; summarize goals
Modifying the Simple Advice Intervention for the Telephone Send materials to the patient prior to phone call – Include a cover letter indicating to the patient that you will help them understand these handouts once you talk during the scheduled appointment Be prepared it will be more difficult because you won’t be able to see the patient’s facial reactions Make sure you review the patient’s medical chart (e. g. , look at age of patient, previous treatment, psychiatric diagnoses, and medical issues) If you have never met the patient: – It may be more helpful to conduct the intervention within the arena of talking to the patient about health behaviors in general – Send along some (1 -2) additional handouts on other health behaviors that might be good to include – Begin by assessing health behaviors, including alcohol use – Discuss how the patient wants to improve his/her health; summarize goals
 Documentation Progress Note – Clearly describe the assessment conducted, symptoms endorsed, and intervention provided Encounter Form— – Diagnosis: Alcohol Abuse (305. 00), Alcohol Dependence (303. 9), Screening for Alcoholism (V 79. 1) – Procedure: use your standard code for treatments (15, 30 or 45 min blocks) OR use preventive medicine counseling and/or risk factor reduction intervention to an individual (15, 30, or 45 minute blocks)
Documentation Progress Note – Clearly describe the assessment conducted, symptoms endorsed, and intervention provided Encounter Form— – Diagnosis: Alcohol Abuse (305. 00), Alcohol Dependence (303. 9), Screening for Alcoholism (V 79. 1) – Procedure: use your standard code for treatments (15, 30 or 45 min blocks) OR use preventive medicine counseling and/or risk factor reduction intervention to an individual (15, 30, or 45 minute blocks)
 Role Plays
Role Plays
 Conclusion
Conclusion
 Competencies Administer and accurately interpret the AUDIT-C Conduct further assessment of alcohol misuse Deliver the WHO Simple Advice intervention Each competency has areas that cover specific content that needs to be covered and the quality of the assessment/ intervention
Competencies Administer and accurately interpret the AUDIT-C Conduct further assessment of alcohol misuse Deliver the WHO Simple Advice intervention Each competency has areas that cover specific content that needs to be covered and the quality of the assessment/ intervention
 Additional Resources in your packets Self-help booklet Brief Counseling script AUDIT
Additional Resources in your packets Self-help booklet Brief Counseling script AUDIT
 Helpful References World Health Organization—Brief Intervention Manual – http: //www. who. int/substance_abuse/publications/alco hol/en/ NIAAA – National Institute of Alcohol Abuse and Alcoholism (NIAAA). (2007). Helping patients who drink too much: A clinician’s guide. NIH Publication No. 07 -3769. http: //pubs. niaaa. nih. gov/publications/Practitioner/Clinicians. Guid e 2005/clinicians_guide. htm Hunter, C. L. , Goodie, J. L. , Oordt, M. S. , & Dobymeyer, A. C. (2009). Integrated Behavioral Health in Primary Care: Step-by-step guidance for assessment and intervention. Washington DC: American Psychological Association.
Helpful References World Health Organization—Brief Intervention Manual – http: //www. who. int/substance_abuse/publications/alco hol/en/ NIAAA – National Institute of Alcohol Abuse and Alcoholism (NIAAA). (2007). Helping patients who drink too much: A clinician’s guide. NIH Publication No. 07 -3769. http: //pubs. niaaa. nih. gov/publications/Practitioner/Clinicians. Guid e 2005/clinicians_guide. htm Hunter, C. L. , Goodie, J. L. , Oordt, M. S. , & Dobymeyer, A. C. (2009). Integrated Behavioral Health in Primary Care: Step-by-step guidance for assessment and intervention. Washington DC: American Psychological Association.


