6b39ea42050a5b273ede41d95a3bf0dc.ppt
- Количество слайдов: 34
 Addictive and Co-Occurring Disorders in Late Life David W. Oslin, M. D. University of Pennsylvania, School of Medicine And Philadelphia, VAMC Hazelden Research Co-Chair on Late Life Addictions
Addictive and Co-Occurring Disorders in Late Life David W. Oslin, M. D. University of Pennsylvania, School of Medicine And Philadelphia, VAMC Hazelden Research Co-Chair on Late Life Addictions
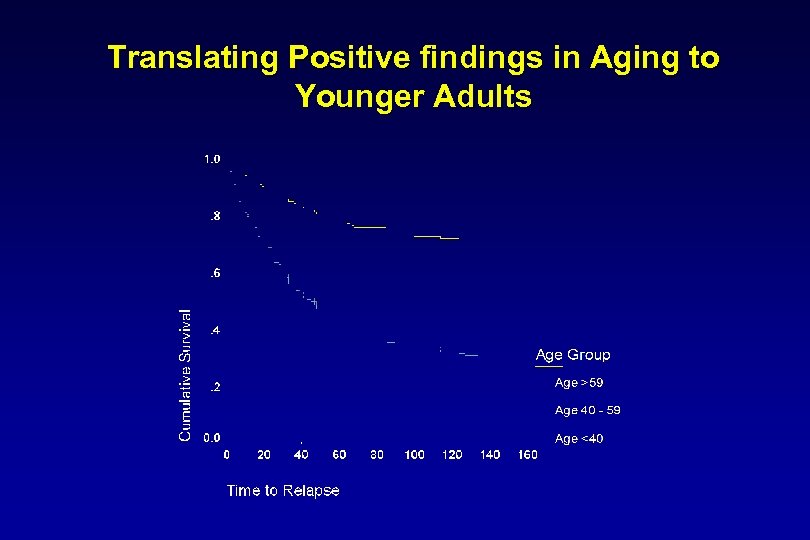 Translating Positive findings in Aging to Younger Adults
Translating Positive findings in Aging to Younger Adults
 Disclosures NIMH § K 08 Award § ACSIR NIDA § Center for Studies on Addiction NIAAA § R 01 VA § Merit Early Entry § MIRECC § HSRD Merit Award Industry Support § § Du. Pont Pharma Forest Labs Hazelden Foundation Pfizer
Disclosures NIMH § K 08 Award § ACSIR NIDA § Center for Studies on Addiction NIAAA § R 01 VA § Merit Early Entry § MIRECC § HSRD Merit Award Industry Support § § Du. Pont Pharma Forest Labs Hazelden Foundation Pfizer
 Relevance of comorbidity to an aging population Cohort changes in exposure – we will see more elderly patients using illicit substances (current and past abuse) Consequences may be greater in older adults § Direct toxicity / withdrawal § Indirect interactions with medications or other illnesses Comorbidity is a significant issue perhaps uniquely so for the elderly § Cognition § Minor depression § Suicide § Anxiety and personality problems Changing environment § Social isolation § Limited resources § Limited access to care
Relevance of comorbidity to an aging population Cohort changes in exposure – we will see more elderly patients using illicit substances (current and past abuse) Consequences may be greater in older adults § Direct toxicity / withdrawal § Indirect interactions with medications or other illnesses Comorbidity is a significant issue perhaps uniquely so for the elderly § Cognition § Minor depression § Suicide § Anxiety and personality problems Changing environment § Social isolation § Limited resources § Limited access to care
 Comorbidity and Drug/Alcohol Dependence Higher than expect rates in representative community samples Markedly higher rates in treatment seeking samples Increased morbidity and mortality particularly suicide Presents diagnostic difficulties Poor prognostic factor Call for integrated care system
Comorbidity and Drug/Alcohol Dependence Higher than expect rates in representative community samples Markedly higher rates in treatment seeking samples Increased morbidity and mortality particularly suicide Presents diagnostic difficulties Poor prognostic factor Call for integrated care system
 Suicide Highest rates of suicide occur in late life among men. Depression causes a 5. 8 fold increase in risk of suicide compared to death from other causes Heavy drinking (3+ drinks/day) causes a 8. 9 fold increase in risk of suicide compared to death from other causes Moderate drinking (1 -2 drinks/day) causes a 10. 6 fold increase in risk of suicide compared to death from other causes Grabble, et al. 1997
Suicide Highest rates of suicide occur in late life among men. Depression causes a 5. 8 fold increase in risk of suicide compared to death from other causes Heavy drinking (3+ drinks/day) causes a 8. 9 fold increase in risk of suicide compared to death from other causes Moderate drinking (1 -2 drinks/day) causes a 10. 6 fold increase in risk of suicide compared to death from other causes Grabble, et al. 1997
 The difficulty Extremely limited research Drug and alcohol dependence are exclusions to most geriatric trials Age >65 is almost always an exclusion for drug and alcohol trials
The difficulty Extremely limited research Drug and alcohol dependence are exclusions to most geriatric trials Age >65 is almost always an exclusion for drug and alcohol trials
 What is the Extent of the Issues? In the Community Current / Last 12 months Alcohol Dependence Medication misuse Nicotine dependence Illicit Substance dependence Pathological Gambling 2 -4% ? Overall Chronic Benzodiazepine use 5 – 20% 10 - 15 % <1% 1– 2%
What is the Extent of the Issues? In the Community Current / Last 12 months Alcohol Dependence Medication misuse Nicotine dependence Illicit Substance dependence Pathological Gambling 2 -4% ? Overall Chronic Benzodiazepine use 5 – 20% 10 - 15 % <1% 1– 2%
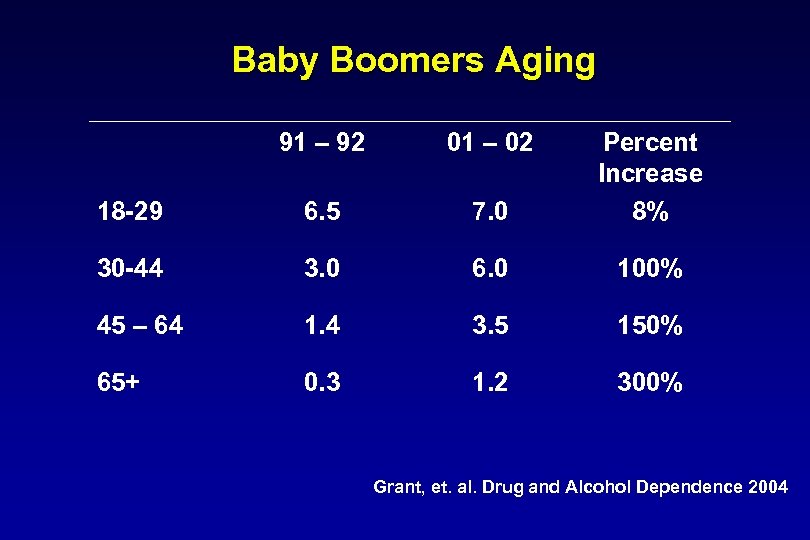 Baby Boomers Aging 91 – 92 01 – 02 18 -29 6. 5 7. 0 Percent Increase 8% 30 -44 3. 0 6. 0 100% 45 – 64 1. 4 3. 5 150% 65+ 0. 3 1. 2 300% Grant, et. al. Drug and Alcohol Dependence 2004
Baby Boomers Aging 91 – 92 01 – 02 18 -29 6. 5 7. 0 Percent Increase 8% 30 -44 3. 0 6. 0 100% 45 – 64 1. 4 3. 5 150% 65+ 0. 3 1. 2 300% Grant, et. al. Drug and Alcohol Dependence 2004
 Veterans (Age 60 and Over) in Addiction Treatment Alcohol Only 51. 8% Street Drugs Only 9. 1% Prescription Medications only 3. 6% Alcohol and Street Drugs 26. 4% Alcohol and Prescription Medications 5. 5% Street Drugs and Prescription Medications 0. 9% All three categories of substances 1. 8% Missing data 0. 9% Sample of 110 subjects in a special geri-addiction program Schonfeld et al. 1990
Veterans (Age 60 and Over) in Addiction Treatment Alcohol Only 51. 8% Street Drugs Only 9. 1% Prescription Medications only 3. 6% Alcohol and Street Drugs 26. 4% Alcohol and Prescription Medications 5. 5% Street Drugs and Prescription Medications 0. 9% All three categories of substances 1. 8% Missing data 0. 9% Sample of 110 subjects in a special geri-addiction program Schonfeld et al. 1990
 Past History of Heavy drinking/alcoholism Many older adults especially those of the “Woodstock” generation will enter late life with a past history of alcohol or drug abuse 5 fold increase in late life mental disorders (depression and dementia) Treatment of late life depression (3 -5 yr outcomes) § 88% of those without an alcohol history significantly improved § 57% of those with an alcohol history significantly improved Saunders et al. 1991, Cook et al. 1991
Past History of Heavy drinking/alcoholism Many older adults especially those of the “Woodstock” generation will enter late life with a past history of alcohol or drug abuse 5 fold increase in late life mental disorders (depression and dementia) Treatment of late life depression (3 -5 yr outcomes) § 88% of those without an alcohol history significantly improved § 57% of those with an alcohol history significantly improved Saunders et al. 1991, Cook et al. 1991
 Behavioral Health Laboratory (BHL): Links To Primary Care
Behavioral Health Laboratory (BHL): Links To Primary Care
 Research to Practice: Behavioral Health Laboratory The BHL is an automated telephone assessment and triage service for patients identified by primary care providers as having depressive symptoms or at-risk drinking. The depression and alcohol clinical reminder system generates a consultation request to the BHL. The BHL conducts a brief telephone (20 -30 minutes) assessment generating a report for the PCP including diagnosis, severity, and general treatment recommendations.
Research to Practice: Behavioral Health Laboratory The BHL is an automated telephone assessment and triage service for patients identified by primary care providers as having depressive symptoms or at-risk drinking. The depression and alcohol clinical reminder system generates a consultation request to the BHL. The BHL conducts a brief telephone (20 -30 minutes) assessment generating a report for the PCP including diagnosis, severity, and general treatment recommendations.
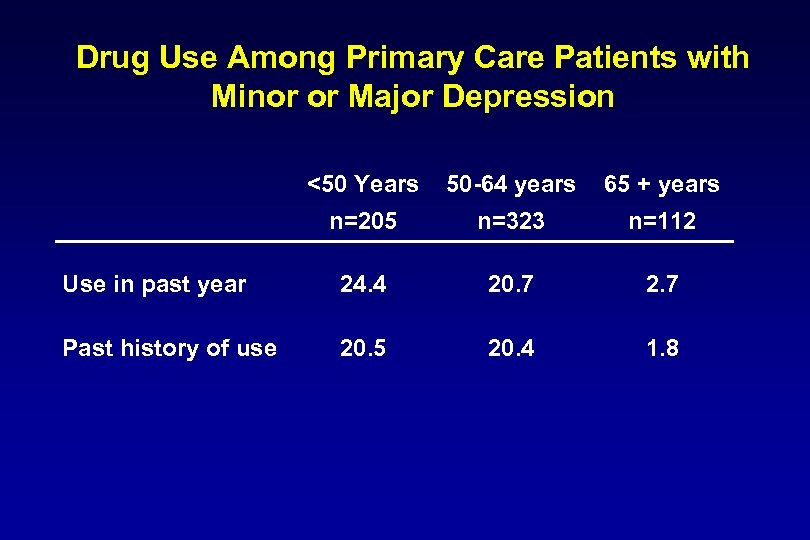 Drug Use Among Primary Care Patients with Minor or Major Depression <50 Years 50 -64 years 65 + years n=205 n=323 n=112 Use in past year 24. 4 20. 7 2. 7 Past history of use 20. 5 20. 4 1. 8
Drug Use Among Primary Care Patients with Minor or Major Depression <50 Years 50 -64 years 65 + years n=205 n=323 n=112 Use in past year 24. 4 20. 7 2. 7 Past history of use 20. 5 20. 4 1. 8
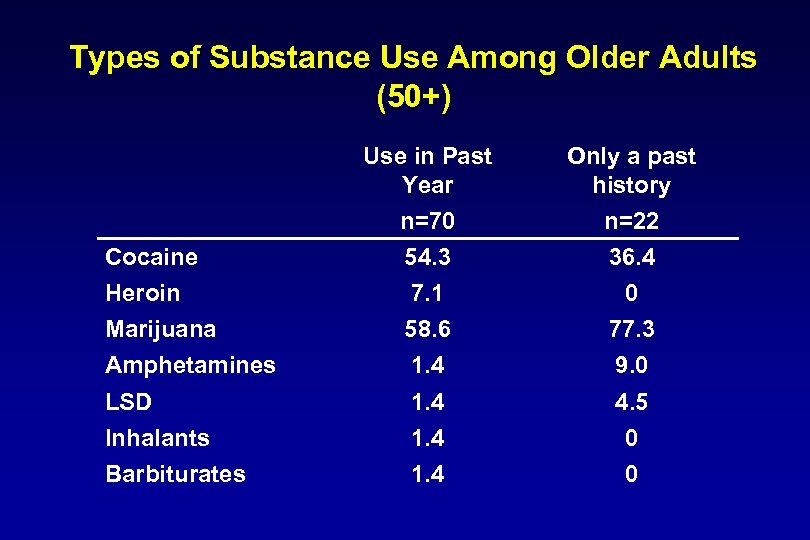 Types of Substance Use Among Older Adults (50+) Use in Past Year Cocaine Heroin Marijuana Amphetamines LSD Inhalants Barbiturates Only a past history n=70 54. 3 7. 1 58. 6 1. 4 n=22 36. 4 0 77. 3 9. 0 1. 4 4. 5 0 0
Types of Substance Use Among Older Adults (50+) Use in Past Year Cocaine Heroin Marijuana Amphetamines LSD Inhalants Barbiturates Only a past history n=70 54. 3 7. 1 58. 6 1. 4 n=22 36. 4 0 77. 3 9. 0 1. 4 4. 5 0 0
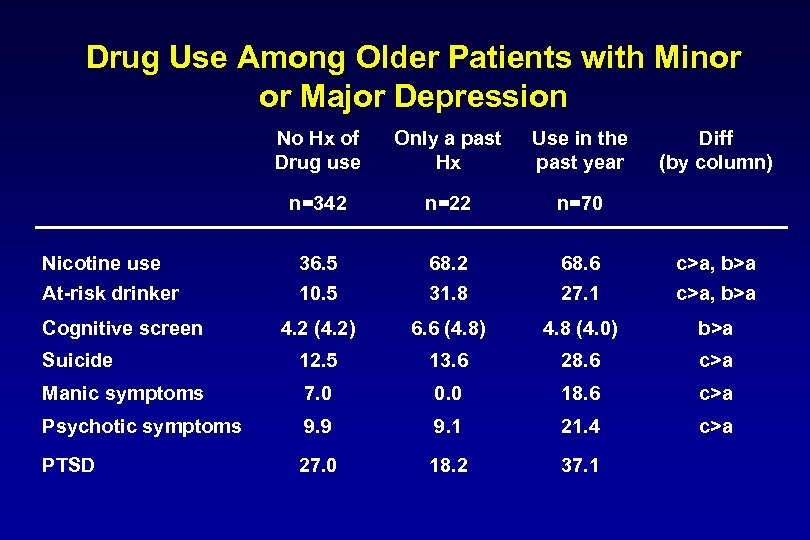 Drug Use Among Older Patients with Minor or Major Depression No Hx of Drug use Only a past Hx Use in the past year n=342 n=22 n=70 Nicotine use 36. 5 68. 2 68. 6 c>a, b>a At-risk drinker 10. 5 31. 8 27. 1 c>a, b>a 4. 2 (4. 2) 6. 6 (4. 8) 4. 8 (4. 0) b>a Suicide 12. 5 13. 6 28. 6 c>a Manic symptoms 7. 0 0. 0 18. 6 c>a Psychotic symptoms 9. 9 9. 1 21. 4 c>a PTSD 27. 0 18. 2 37. 1 Cognitive screen Diff (by column)
Drug Use Among Older Patients with Minor or Major Depression No Hx of Drug use Only a past Hx Use in the past year n=342 n=22 n=70 Nicotine use 36. 5 68. 2 68. 6 c>a, b>a At-risk drinker 10. 5 31. 8 27. 1 c>a, b>a 4. 2 (4. 2) 6. 6 (4. 8) 4. 8 (4. 0) b>a Suicide 12. 5 13. 6 28. 6 c>a Manic symptoms 7. 0 0. 0 18. 6 c>a Psychotic symptoms 9. 9 9. 1 21. 4 c>a PTSD 27. 0 18. 2 37. 1 Cognitive screen Diff (by column)
 Treatment
Treatment
 Depression Alcohol Aging Trial Hypotheses § Among older adults with major depression and comorbid alcoholism, naltrexone combined with sertraline improves the outcomes of both drinking and mood. § Reduction in alcohol consumption will be associated with improved mood regardless of randomization. § Naltrexone will lead to a reduction in alcohol consumption independent of changes in mood.
Depression Alcohol Aging Trial Hypotheses § Among older adults with major depression and comorbid alcoholism, naltrexone combined with sertraline improves the outcomes of both drinking and mood. § Reduction in alcohol consumption will be associated with improved mood regardless of randomization. § Naltrexone will lead to a reduction in alcohol consumption independent of changes in mood.
 Concurrent Treatment of Depression Complicated by Alcohol Dependence Current depressive syndrome Current alcohol dependence Age 55 and over 10 sessions of compliance enhancement therapy 1/2 of subjects are randomly assigned to receive naltrexone 50 mg All subjects receive sertraline 100 mg Outcomes at 3 months (Oslin, 2004)
Concurrent Treatment of Depression Complicated by Alcohol Dependence Current depressive syndrome Current alcohol dependence Age 55 and over 10 sessions of compliance enhancement therapy 1/2 of subjects are randomly assigned to receive naltrexone 50 mg All subjects receive sertraline 100 mg Outcomes at 3 months (Oslin, 2004)
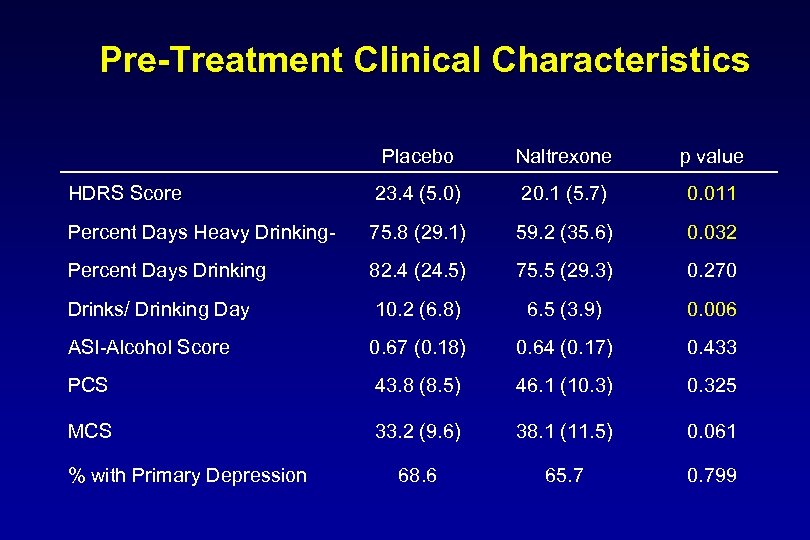 Pre-Treatment Clinical Characteristics Placebo Naltrexone p value HDRS Score 23. 4 (5. 0) 20. 1 (5. 7) 0. 011 Percent Days Heavy Drinking- 75. 8 (29. 1) 59. 2 (35. 6) 0. 032 Percent Days Drinking 82. 4 (24. 5) 75. 5 (29. 3) 0. 270 Drinks/ Drinking Day 10. 2 (6. 8) 6. 5 (3. 9) 0. 006 ASI-Alcohol Score 0. 67 (0. 18) 0. 64 (0. 17) 0. 433 PCS 43. 8 (8. 5) 46. 1 (10. 3) 0. 325 MCS 33. 2 (9. 6) 38. 1 (11. 5) 0. 061 68. 6 65. 7 0. 799 % with Primary Depression
Pre-Treatment Clinical Characteristics Placebo Naltrexone p value HDRS Score 23. 4 (5. 0) 20. 1 (5. 7) 0. 011 Percent Days Heavy Drinking- 75. 8 (29. 1) 59. 2 (35. 6) 0. 032 Percent Days Drinking 82. 4 (24. 5) 75. 5 (29. 3) 0. 270 Drinks/ Drinking Day 10. 2 (6. 8) 6. 5 (3. 9) 0. 006 ASI-Alcohol Score 0. 67 (0. 18) 0. 64 (0. 17) 0. 433 PCS 43. 8 (8. 5) 46. 1 (10. 3) 0. 325 MCS 33. 2 (9. 6) 38. 1 (11. 5) 0. 061 68. 6 65. 7 0. 799 % with Primary Depression
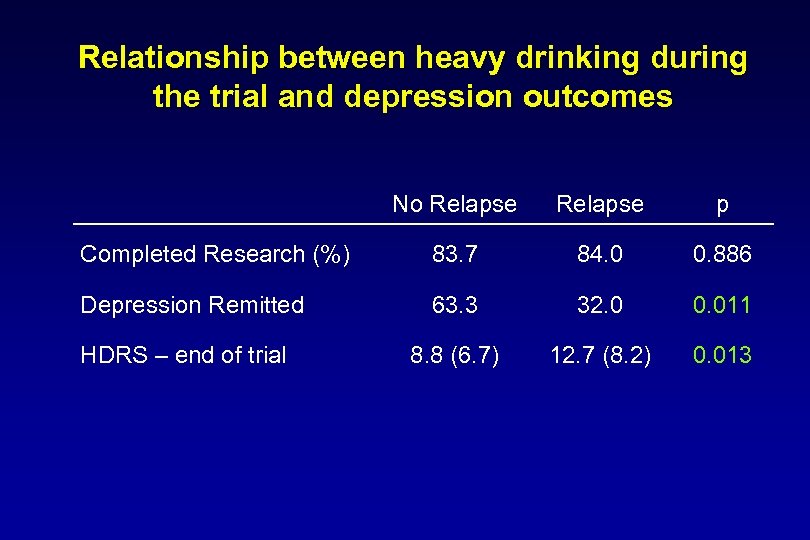 Relationship between heavy drinking during the trial and depression outcomes No Relapse p Completed Research (%) 83. 7 84. 0 0. 886 Depression Remitted 63. 3 32. 0 0. 011 8. 8 (6. 7) 12. 7 (8. 2) 0. 013 HDRS – end of trial
Relationship between heavy drinking during the trial and depression outcomes No Relapse p Completed Research (%) 83. 7 84. 0 0. 886 Depression Remitted 63. 3 32. 0 0. 011 8. 8 (6. 7) 12. 7 (8. 2) 0. 013 HDRS – end of trial
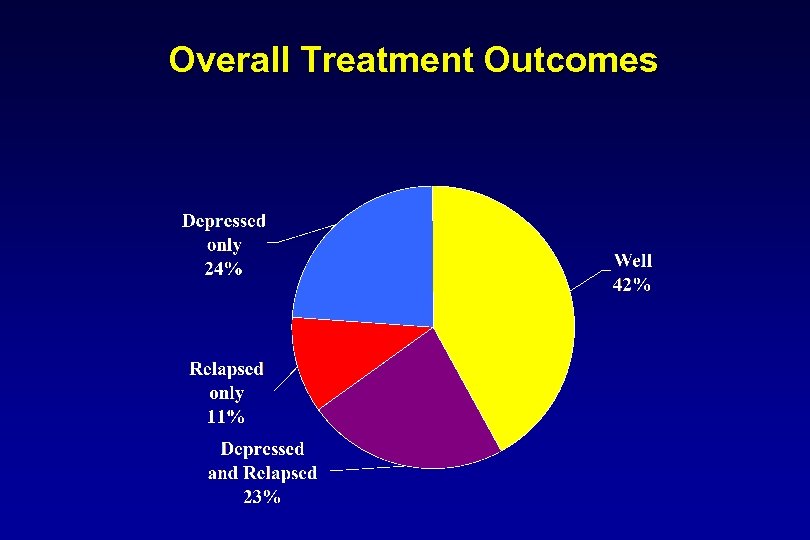 Overall Treatment Outcomes
Overall Treatment Outcomes
 Substance Induced Depression in the elderly? Less than 50% resolution of symptoms early in treatment No relationship between clinical impression of primary vs. secondary depression and early response
Substance Induced Depression in the elderly? Less than 50% resolution of symptoms early in treatment No relationship between clinical impression of primary vs. secondary depression and early response
 Not just Dependence Moving beyond DSM in conceptualizing risk
Not just Dependence Moving beyond DSM in conceptualizing risk
 Disease and Behavior Substance dependence § Follows the biomedical model of an illness At-risk use § Public health model § Recognizes risks (health, economic, etc. ) associated with use in individuals not suffering with the “disease” § Most relevant for alcohol, medications, marijuana and nicotine.
Disease and Behavior Substance dependence § Follows the biomedical model of an illness At-risk use § Public health model § Recognizes risks (health, economic, etc. ) associated with use in individuals not suffering with the “disease” § Most relevant for alcohol, medications, marijuana and nicotine.
 What about moderate or abusive drinking (non-dependent drinking) Most common pattern of drinking among those with depression May be beneficial for heart disease Safety concerns may be less with newer medications (SSRIs) than older meds (TCAs)
What about moderate or abusive drinking (non-dependent drinking) Most common pattern of drinking among those with depression May be beneficial for heart disease Safety concerns may be less with newer medications (SSRIs) than older meds (TCAs)
 Response to Standard Depression Care Among the Elderly PROSPECT study § Remission of depression (men only) § Non-drinkers – 41 % § Moderate drinkers – 18. 2% PRISM-E study (preliminary) § Remission of depression (men only) § Non-drinkers – 33. 8 % § Moderate drinkers – 6. 3 % (Personal Communication, 2002)
Response to Standard Depression Care Among the Elderly PROSPECT study § Remission of depression (men only) § Non-drinkers – 41 % § Moderate drinkers – 18. 2% PRISM-E study (preliminary) § Remission of depression (men only) § Non-drinkers – 33. 8 % § Moderate drinkers – 6. 3 % (Personal Communication, 2002)
 Telephone Disease Management for Depression and At-Risk Drinking §To develop a method for delivering high quality depression and alcoholism treatment in Primary Care, CBOCs, and other clinics in which there are significant transportation, staff resource, or other impediments to the delivery of face-to-face MH/SA care. §To develop methods for translating effects demonstrated in randomized clinical trials to clinic populations.
Telephone Disease Management for Depression and At-Risk Drinking §To develop a method for delivering high quality depression and alcoholism treatment in Primary Care, CBOCs, and other clinics in which there are significant transportation, staff resource, or other impediments to the delivery of face-to-face MH/SA care. §To develop methods for translating effects demonstrated in randomized clinical trials to clinic populations.
 Treatments Telephone Disease Management is algorithm driven care delivered by a Behavioral Health Specialist. Enhanced Usual care. The PCP can monitor, treat, and/or refer. The PCP is provided a diagnosis and references for treatment options.
Treatments Telephone Disease Management is algorithm driven care delivered by a Behavioral Health Specialist. Enhanced Usual care. The PCP can monitor, treat, and/or refer. The PCP is provided a diagnosis and references for treatment options.
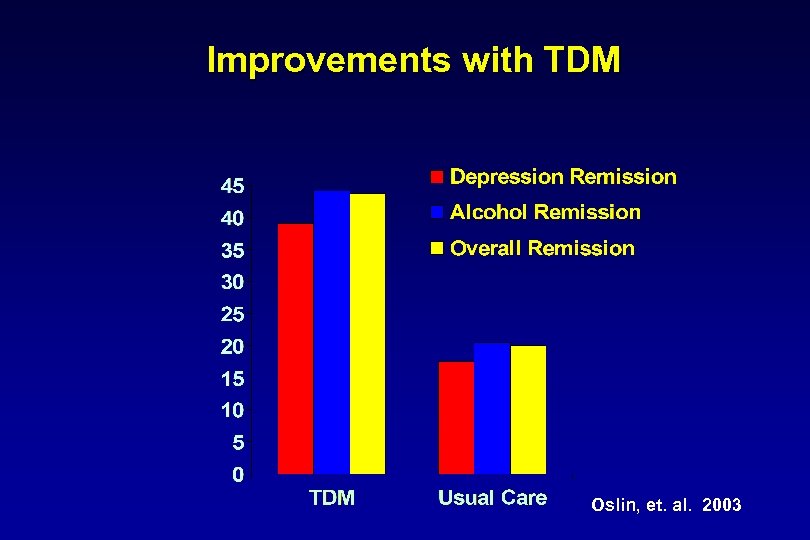 Improvements with TDM Oslin, et. al. 2003
Improvements with TDM Oslin, et. al. 2003
 Is Sedative/Hypnotic Use a Co. Occurring Problem? Association with falls Association with memory impairment ? Association with treatment of depression
Is Sedative/Hypnotic Use a Co. Occurring Problem? Association with falls Association with memory impairment ? Association with treatment of depression
 How to Define Inappropriate Benzodiazepine Use Chronic Use (>3 months) Use of long-acting agents Undocumented response Lowest effective dose (harm reduction)
How to Define Inappropriate Benzodiazepine Use Chronic Use (>3 months) Use of long-acting agents Undocumented response Lowest effective dose (harm reduction)
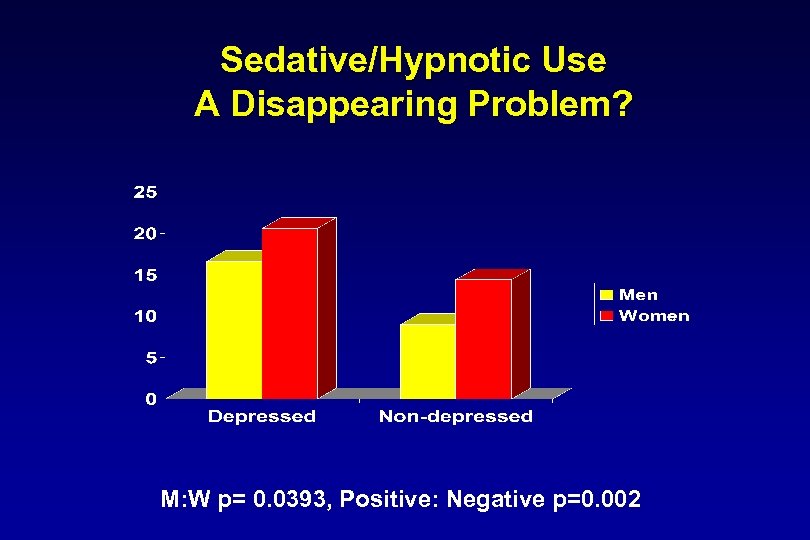 Sedative/Hypnotic Use A Disappearing Problem? M: W p= 0. 0393, Positive: Negative p=0. 002
Sedative/Hypnotic Use A Disappearing Problem? M: W p= 0. 0393, Positive: Negative p=0. 002
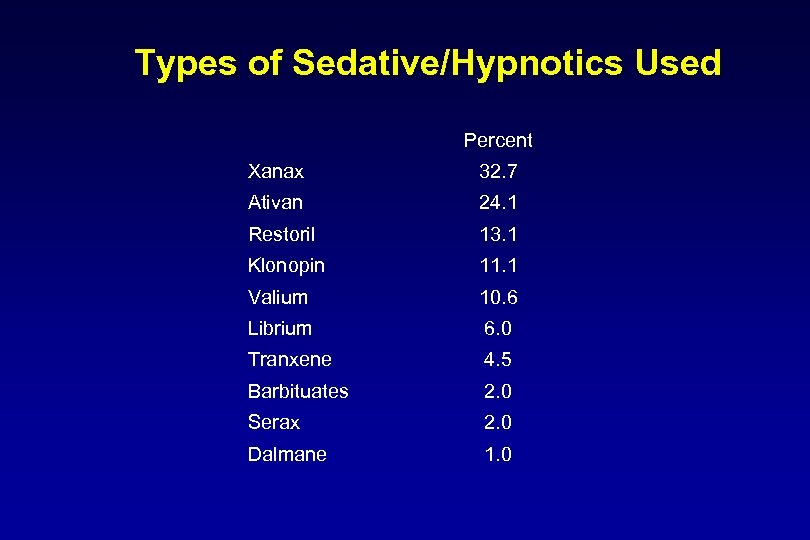 Types of Sedative/Hypnotics Used Percent Xanax 32. 7 Ativan 24. 1 Restoril 13. 1 Klonopin 11. 1 Valium 10. 6 Librium 6. 0 Tranxene 4. 5 Barbituates 2. 0 Serax 2. 0 Dalmane 1. 0
Types of Sedative/Hypnotics Used Percent Xanax 32. 7 Ativan 24. 1 Restoril 13. 1 Klonopin 11. 1 Valium 10. 6 Librium 6. 0 Tranxene 4. 5 Barbituates 2. 0 Serax 2. 0 Dalmane 1. 0


