52fd02d4dc7f9df6cebccc88f04f98a0.ppt
- Количество слайдов: 39
 Acute Pneumonia “The most widespread and fatal of all acute diseases, pneumonia is now Captain of the Men of Death. ” The Principals and Practice of Medicine Sir William Oscar, 1901
Acute Pneumonia “The most widespread and fatal of all acute diseases, pneumonia is now Captain of the Men of Death. ” The Principals and Practice of Medicine Sir William Oscar, 1901
 Principles and Practice of Infectious Diseases
Principles and Practice of Infectious Diseases
 Principals and Practice of Infectious Diseases
Principals and Practice of Infectious Diseases
 Diagnosis of CAP • Chest radiograph is the most important diagnostic tool • Clinical presentation is not diagnostic of an etiology • Yield of pathogens from Gram stain of expectorated sputum from patients with CAP is only 30%– 40%.
Diagnosis of CAP • Chest radiograph is the most important diagnostic tool • Clinical presentation is not diagnostic of an etiology • Yield of pathogens from Gram stain of expectorated sputum from patients with CAP is only 30%– 40%.
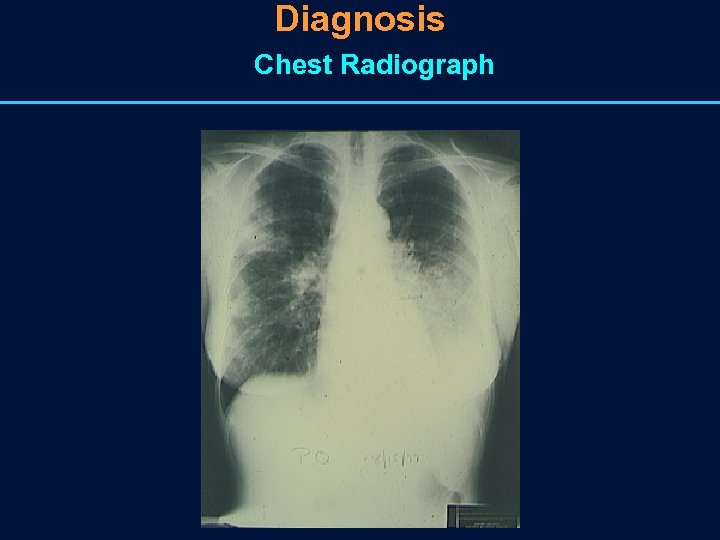 Diagnosis Chest Radiograph
Diagnosis Chest Radiograph
 Gram Stain’s Role in CAP Diagnosis
Gram Stain’s Role in CAP Diagnosis
 CAP Treatment Issues • Causative pathogen frequently not found – Treatment predominantly empiric – Pneumococcal and atypical coverage important • Increasing antibiotic resistance – Clinical significance in question • Use double-coverage for pneumococci? • If outcomes are similar, which agent do we choose?
CAP Treatment Issues • Causative pathogen frequently not found – Treatment predominantly empiric – Pneumococcal and atypical coverage important • Increasing antibiotic resistance – Clinical significance in question • Use double-coverage for pneumococci? • If outcomes are similar, which agent do we choose?
 CAP: Changing Presentation • Aging of the population • Increased number of nursing home beds • Increased number of AIDS cases • Increased number of organs transplanted
CAP: Changing Presentation • Aging of the population • Increased number of nursing home beds • Increased number of AIDS cases • Increased number of organs transplanted
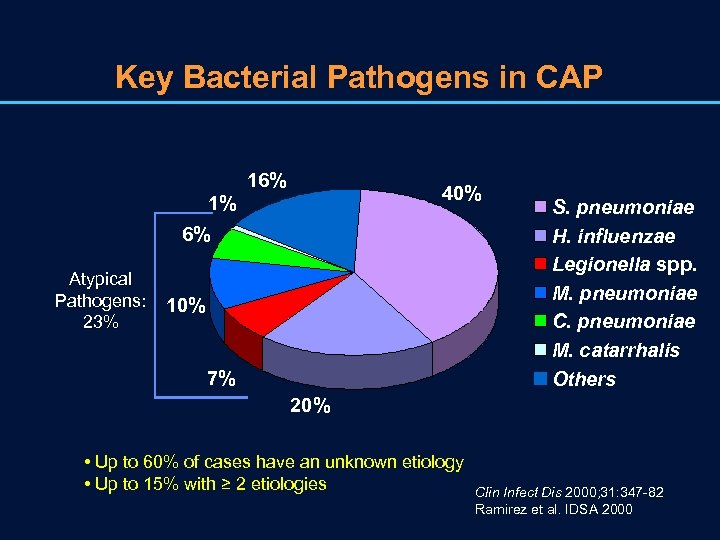 Key Bacterial Pathogens in CAP 16% 40% 1% 6% Atypical Pathogens: 23% 10% 7% S. pneumoniae H. influenzae Legionella spp. M. pneumoniae C. pneumoniae M. catarrhalis Others 20% • Up to 60% of cases have an unknown etiology • Up to 15% with ≥ 2 etiologies Clin Infect Dis 2000; 31: 347 -82 Ramirez et al. IDSA 2000
Key Bacterial Pathogens in CAP 16% 40% 1% 6% Atypical Pathogens: 23% 10% 7% S. pneumoniae H. influenzae Legionella spp. M. pneumoniae C. pneumoniae M. catarrhalis Others 20% • Up to 60% of cases have an unknown etiology • Up to 15% with ≥ 2 etiologies Clin Infect Dis 2000; 31: 347 -82 Ramirez et al. IDSA 2000
 The reported age-related mortality per 100, 000 US population from pneumonia and influenza in individuals >15 yr, 1982 -1990
The reported age-related mortality per 100, 000 US population from pneumonia and influenza in individuals >15 yr, 1982 -1990
 ASCAP Guidelines for Outpatient Treatment of CAP • Otherwise healthy patients (all ages) –First-line • Azithromycin PO –Alternative first-line • Moxifloxacin PO (preferred) or levofloxacin PO or clarithromycin PO or gatifloxacin PO The ASCAP 2002 Consensus Panel. Hosp Med Consensus Rep. 2002: 1 -32; Emerman CL, Bosker G. In: Bosker G, ed. Textbook of Adult and Pediatric Emergency Medicine. 2 nd ed. Atlanta, Ga: American Health Consultants. 2002: 375 -395.
ASCAP Guidelines for Outpatient Treatment of CAP • Otherwise healthy patients (all ages) –First-line • Azithromycin PO –Alternative first-line • Moxifloxacin PO (preferred) or levofloxacin PO or clarithromycin PO or gatifloxacin PO The ASCAP 2002 Consensus Panel. Hosp Med Consensus Rep. 2002: 1 -32; Emerman CL, Bosker G. In: Bosker G, ed. Textbook of Adult and Pediatric Emergency Medicine. 2 nd ed. Atlanta, Ga: American Health Consultants. 2002: 375 -395.
 Indications for Hospitalization • Pulse >140, SBP <90 mm Hg, and/or respiratory rate >30/min • Altered mental status • Hypoxemia (PO <60 mm Hg) • Suppurative complication • Metabolic abnormality
Indications for Hospitalization • Pulse >140, SBP <90 mm Hg, and/or respiratory rate >30/min • Altered mental status • Hypoxemia (PO <60 mm Hg) • Suppurative complication • Metabolic abnormality
 ASCAP Guidelines for Inpatient Treatment of CAP • Hospitalized, non-ICU – First-line • Ceftriaxone PLUS azithromycin IV – Alternative first-line • Moxifloxacin or levofloxacin IV or gatifloxacin • ICU Patients – First-line • Ceftriaxone IV PLUS levofloxacin IV (±) aminoglycoside or ceftriaxone IV PLUS azithromycin IV (±) an antipseudomonal agent – Alternative first-line • Ciprofloxacin IV PLUS an aminoglycoside IV PLUS azithromycin IV The ASCAP 2002 Consensus Panel. Hosp Med Consensus Rep. 2002: 1 -32; Emerman CL, Bosker G. In: Bosker G, ed. Textbook of Adult and Pediatric Emergency Medicine. 2 nd ed. Atlanta, Ga: American Health Consultants. 2002: 375 -395.
ASCAP Guidelines for Inpatient Treatment of CAP • Hospitalized, non-ICU – First-line • Ceftriaxone PLUS azithromycin IV – Alternative first-line • Moxifloxacin or levofloxacin IV or gatifloxacin • ICU Patients – First-line • Ceftriaxone IV PLUS levofloxacin IV (±) aminoglycoside or ceftriaxone IV PLUS azithromycin IV (±) an antipseudomonal agent – Alternative first-line • Ciprofloxacin IV PLUS an aminoglycoside IV PLUS azithromycin IV The ASCAP 2002 Consensus Panel. Hosp Med Consensus Rep. 2002: 1 -32; Emerman CL, Bosker G. In: Bosker G, ed. Textbook of Adult and Pediatric Emergency Medicine. 2 nd ed. Atlanta, Ga: American Health Consultants. 2002: 375 -395.
 ASCAP Guidelines for Inpatient Treatment of CAP – Special Considerations • Nursing home acquired – First-line • Ceftriaxone IV PLUS azithromycin IV – Alternative first-line • Ceftriaxone PLUS doxycycline or moxifloxacin or levofloxacin IV or gatifloxacin • Severe, bacteremic CAP with documented Streptococcus pneumoniae* – First-line • Ceftriaxone PLUS moxifloxacin or ceftriaxone IV PLUS levofloxacin IV – Alternative first-line • Vancomycin† PLUS azithromycin IV * Showing high-level or complete resistence to macrolides, cephalosporins and/or penicillin. † If S. pneumoniae demonstrates complete resistance to extended-spectrum quinolones (very rare), third generation cephalosporins and macrolides, then vancomycin may be required as part of initial therapy, although this would be necessary only in rare circumstances. The ASCAP 2002 Consensus Panel. Hosp Med Consensus Rep. 2002: 1 -32; Emerman CL, Bosker G. In: Bosker G, ed. Textbook of Adult and Pediatric Emergency Medicine. 2 nd ed. Atlanta, Ga: American Health Consultants. 2002: 375 -395.
ASCAP Guidelines for Inpatient Treatment of CAP – Special Considerations • Nursing home acquired – First-line • Ceftriaxone IV PLUS azithromycin IV – Alternative first-line • Ceftriaxone PLUS doxycycline or moxifloxacin or levofloxacin IV or gatifloxacin • Severe, bacteremic CAP with documented Streptococcus pneumoniae* – First-line • Ceftriaxone PLUS moxifloxacin or ceftriaxone IV PLUS levofloxacin IV – Alternative first-line • Vancomycin† PLUS azithromycin IV * Showing high-level or complete resistence to macrolides, cephalosporins and/or penicillin. † If S. pneumoniae demonstrates complete resistance to extended-spectrum quinolones (very rare), third generation cephalosporins and macrolides, then vancomycin may be required as part of initial therapy, although this would be necessary only in rare circumstances. The ASCAP 2002 Consensus Panel. Hosp Med Consensus Rep. 2002: 1 -32; Emerman CL, Bosker G. In: Bosker G, ed. Textbook of Adult and Pediatric Emergency Medicine. 2 nd ed. Atlanta, Ga: American Health Consultants. 2002: 375 -395.
 Infections caused by S. pneumoniae, USA 1997
Infections caused by S. pneumoniae, USA 1997
 Worldwide Prevalence Rates for Penicillin Resistant S. pneumoniae Unknown < 5% 5 -10% 10 -25% > 25% Doern CID 1998; Felmingham JAC 1996 and 2000. Zhanel Low and Hoban AAC 1999.
Worldwide Prevalence Rates for Penicillin Resistant S. pneumoniae Unknown < 5% 5 -10% 10 -25% > 25% Doern CID 1998; Felmingham JAC 1996 and 2000. Zhanel Low and Hoban AAC 1999.
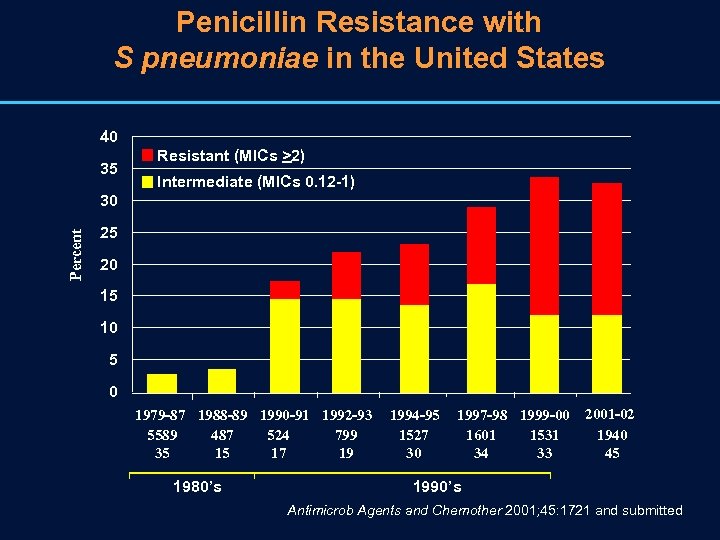 Penicillin Resistance with S pneumoniae in the United States 40 35 Resistant (MICs >2) Intermediate (MICs 0. 12 -1) Percent 30 25 20 15 10 5 0 1979 -87 1988 -89 1990 -91 1992 -93 5589 487 524 799 35 15 17 19 1980’s 1994 -95 1527 30 1997 -98 1999 -00 1601 1531 34 33 2001 -02 1940 45 1990’s Antimicrob Agents and Chemother 2001; 45: 1721 and submitted
Penicillin Resistance with S pneumoniae in the United States 40 35 Resistant (MICs >2) Intermediate (MICs 0. 12 -1) Percent 30 25 20 15 10 5 0 1979 -87 1988 -89 1990 -91 1992 -93 5589 487 524 799 35 15 17 19 1980’s 1994 -95 1527 30 1997 -98 1999 -00 1601 1531 34 33 2001 -02 1940 45 1990’s Antimicrob Agents and Chemother 2001; 45: 1721 and submitted
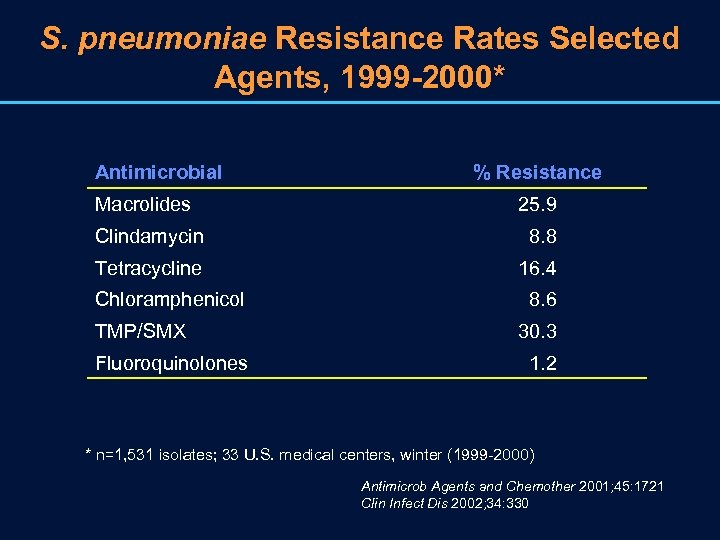 S. pneumoniae Resistance Rates Selected Agents, 1999 -2000* Antimicrobial Macrolides % Resistance 25. 9 Clindamycin 8. 8 Tetracycline 16. 4 Chloramphenicol TMP/SMX Fluoroquinolones 8. 6 30. 3 1. 2 * n=1, 531 isolates; 33 U. S. medical centers, winter (1999 -2000) Antimicrob Agents and Chemother 2001; 45: 1721 Clin Infect Dis 2002; 34: 330
S. pneumoniae Resistance Rates Selected Agents, 1999 -2000* Antimicrobial Macrolides % Resistance 25. 9 Clindamycin 8. 8 Tetracycline 16. 4 Chloramphenicol TMP/SMX Fluoroquinolones 8. 6 30. 3 1. 2 * n=1, 531 isolates; 33 U. S. medical centers, winter (1999 -2000) Antimicrob Agents and Chemother 2001; 45: 1721 Clin Infect Dis 2002; 34: 330
 PRSP-Mechanism • PBP alterations - not -lactamase production - mediate penicillin resistance in pneumococcus thus - lactamase inhibitors do not enhance activity of -lactam agents against penicillinresistant pneumococci
PRSP-Mechanism • PBP alterations - not -lactamase production - mediate penicillin resistance in pneumococcus thus - lactamase inhibitors do not enhance activity of -lactam agents against penicillinresistant pneumococci
 Drug-Resistant S. pneumoniae • Age > 65 years or < 5 years • Exposure to a child in a day care center • Multiple medical comorbidities • Alcoholism • Recent use of antibiotics • Immunosuppression • Recent hospitalization
Drug-Resistant S. pneumoniae • Age > 65 years or < 5 years • Exposure to a child in a day care center • Multiple medical comorbidities • Alcoholism • Recent use of antibiotics • Immunosuppression • Recent hospitalization
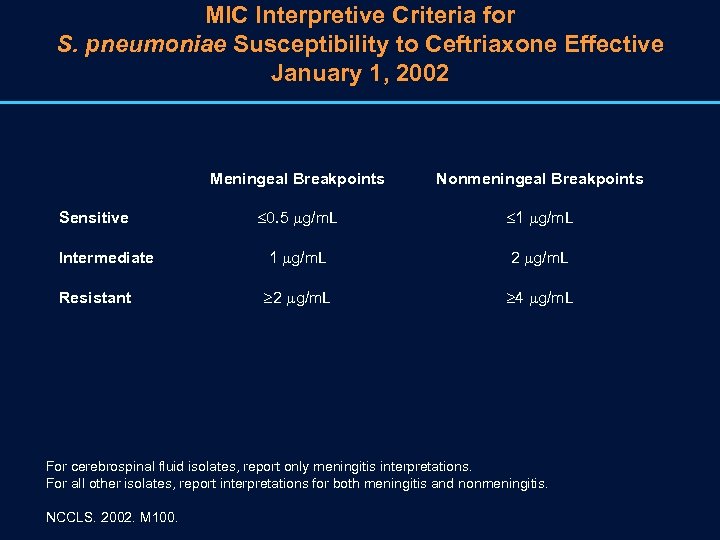 MIC Interpretive Criteria for S. pneumoniae Susceptibility to Ceftriaxone Effective January 1, 2002 Meningeal Breakpoints Nonmeningeal Breakpoints 0. 5 g/m. L 1 g/m. L Intermediate 1 g/m. L 2 g/m. L Resistant 2 g/m. L 4 g/m. L Sensitive For cerebrospinal fluid isolates, report only meningitis interpretations. For all other isolates, report interpretations for both meningitis and nonmeningitis. NCCLS. 2002. M 100.
MIC Interpretive Criteria for S. pneumoniae Susceptibility to Ceftriaxone Effective January 1, 2002 Meningeal Breakpoints Nonmeningeal Breakpoints 0. 5 g/m. L 1 g/m. L Intermediate 1 g/m. L 2 g/m. L Resistant 2 g/m. L 4 g/m. L Sensitive For cerebrospinal fluid isolates, report only meningitis interpretations. For all other isolates, report interpretations for both meningitis and nonmeningitis. NCCLS. 2002. M 100.
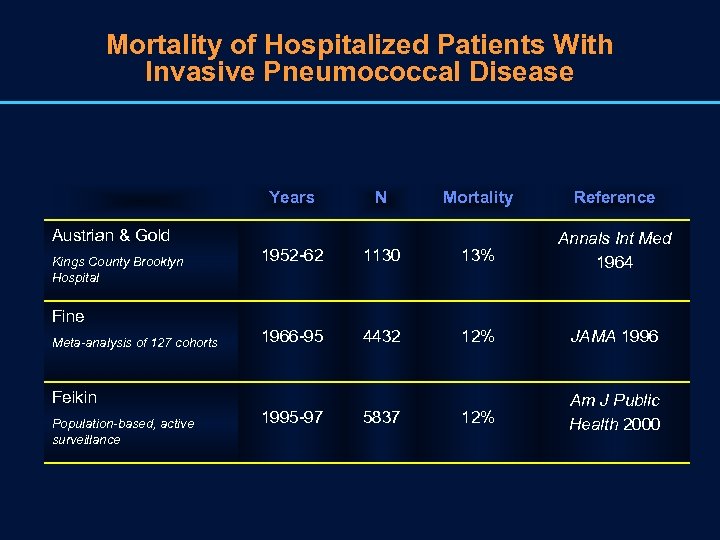 Mortality of Hospitalized Patients With Invasive Pneumococcal Disease Years N Mortality Reference Austrian & Gold Kings County Brooklyn Hospital 1952 -62 1130 13% Annals Int Med 1964 1966 -95 4432 12% JAMA 1996 12% Am J Public Health 2000 Fine Meta-analysis of 127 cohorts Feikin Population-based, active surveillance 1995 -97 5837
Mortality of Hospitalized Patients With Invasive Pneumococcal Disease Years N Mortality Reference Austrian & Gold Kings County Brooklyn Hospital 1952 -62 1130 13% Annals Int Med 1964 1966 -95 4432 12% JAMA 1996 12% Am J Public Health 2000 Fine Meta-analysis of 127 cohorts Feikin Population-based, active surveillance 1995 -97 5837
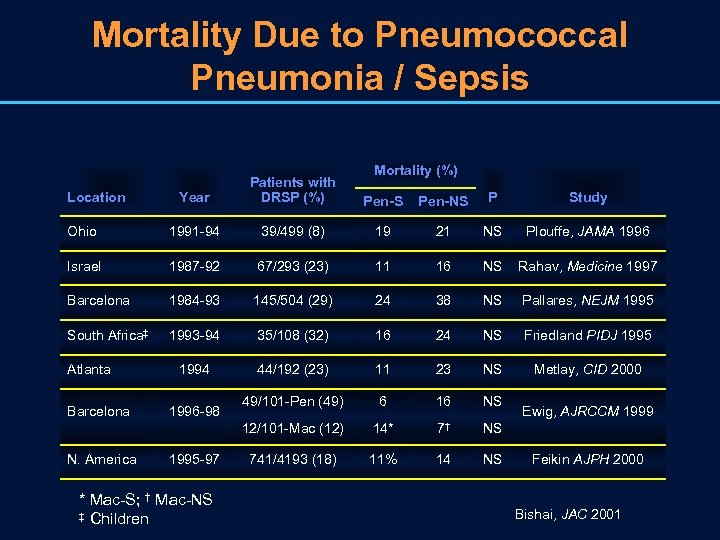 Mortality Due to Pneumococcal Pneumonia / Sepsis Mortality (%) Year Patients with DRSP (%) Pen-S Pen-NS P Study Ohio 1991 -94 39/499 (8) 19 21 NS Plouffe, JAMA 1996 Israel 1987 -92 67/293 (23) 11 16 NS Rahav, Medicine 1997 Barcelona 1984 -93 145/504 (29) 24 38 NS Pallares, NEJM 1995 South Africa‡ 1993 -94 35/108 (32) 16 24 NS Friedland PIDJ 1995 1994 44/192 (23) 11 23 NS Metlay, CID 2000 49/101 -Pen (49) 6 16 NS 12/101 -Mac (12) 14* 7† NS 741/4193 (18) 11% 14 NS Location Atlanta Barcelona N. America 1996 -98 1995 -97 * Mac-S; † Mac-NS ‡ Children Ewig, AJRCCM 1999 Feikin AJPH 2000 Bishai, JAC 2001
Mortality Due to Pneumococcal Pneumonia / Sepsis Mortality (%) Year Patients with DRSP (%) Pen-S Pen-NS P Study Ohio 1991 -94 39/499 (8) 19 21 NS Plouffe, JAMA 1996 Israel 1987 -92 67/293 (23) 11 16 NS Rahav, Medicine 1997 Barcelona 1984 -93 145/504 (29) 24 38 NS Pallares, NEJM 1995 South Africa‡ 1993 -94 35/108 (32) 16 24 NS Friedland PIDJ 1995 1994 44/192 (23) 11 23 NS Metlay, CID 2000 49/101 -Pen (49) 6 16 NS 12/101 -Mac (12) 14* 7† NS 741/4193 (18) 11% 14 NS Location Atlanta Barcelona N. America 1996 -98 1995 -97 * Mac-S; † Mac-NS ‡ Children Ewig, AJRCCM 1999 Feikin AJPH 2000 Bishai, JAC 2001
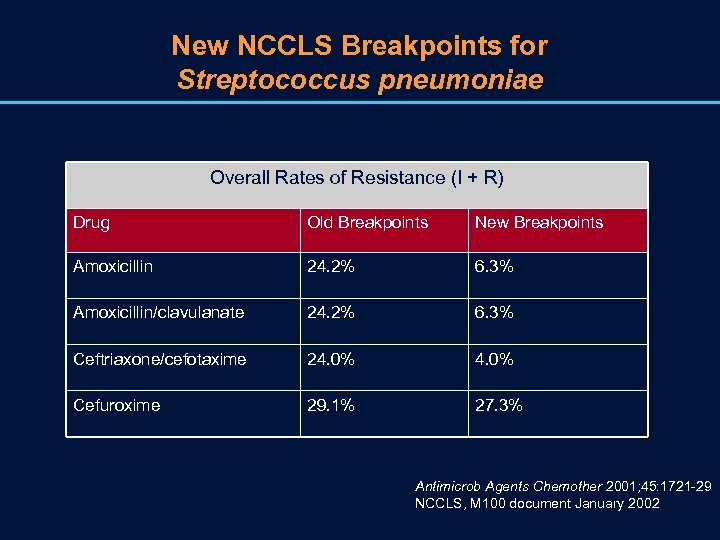 New NCCLS Breakpoints for Streptococcus pneumoniae Overall Rates of Resistance (I + R) Drug Old Breakpoints New Breakpoints Amoxicillin 24. 2% 6. 3% Amoxicillin/clavulanate 24. 2% 6. 3% Ceftriaxone/cefotaxime 24. 0% Cefuroxime 29. 1% 27. 3% Antimicrob Agents Chemother 2001; 45: 1721 -29 NCCLS, M 100 document January 2002
New NCCLS Breakpoints for Streptococcus pneumoniae Overall Rates of Resistance (I + R) Drug Old Breakpoints New Breakpoints Amoxicillin 24. 2% 6. 3% Amoxicillin/clavulanate 24. 2% 6. 3% Ceftriaxone/cefotaxime 24. 0% Cefuroxime 29. 1% 27. 3% Antimicrob Agents Chemother 2001; 45: 1721 -29 NCCLS, M 100 document January 2002
 Antibiotic Activity Against H. influenzae
Antibiotic Activity Against H. influenzae
 H. influenzae Increasing -Lactamase Production
H. influenzae Increasing -Lactamase Production
 Atypical Pneumonia • AP encompasses pneumonias due to Mycoplasma pneumoniae, Chlamydia pneumoniae and Legionella spp* • Prospective studies have failed to identify the cause of 40% to 60% of CAP cases‡ • Today, AP implies • AP often a “mixed” infection* –An often benign course (ambulatory)* –Gradual onset§ –Systemic complaints often greater than respiratory complaints§ *File TM Jr, et al. Infect Dis Clin North Am. 1998; 12: 572, 570, 579. Jr, HO. JAMA. 1938; 111: 2377, 2384. JAMA. ‡Bartlett JG, et al. Clin Infect Dis. 1998; 26: 813. Dis. §Levison ME. Harrison’s Principles of Internal Medicine. Mc. Graw-Hill; 1998: 1439. †Reimann 28
Atypical Pneumonia • AP encompasses pneumonias due to Mycoplasma pneumoniae, Chlamydia pneumoniae and Legionella spp* • Prospective studies have failed to identify the cause of 40% to 60% of CAP cases‡ • Today, AP implies • AP often a “mixed” infection* –An often benign course (ambulatory)* –Gradual onset§ –Systemic complaints often greater than respiratory complaints§ *File TM Jr, et al. Infect Dis Clin North Am. 1998; 12: 572, 570, 579. Jr, HO. JAMA. 1938; 111: 2377, 2384. JAMA. ‡Bartlett JG, et al. Clin Infect Dis. 1998; 26: 813. Dis. §Levison ME. Harrison’s Principles of Internal Medicine. Mc. Graw-Hill; 1998: 1439. †Reimann 28
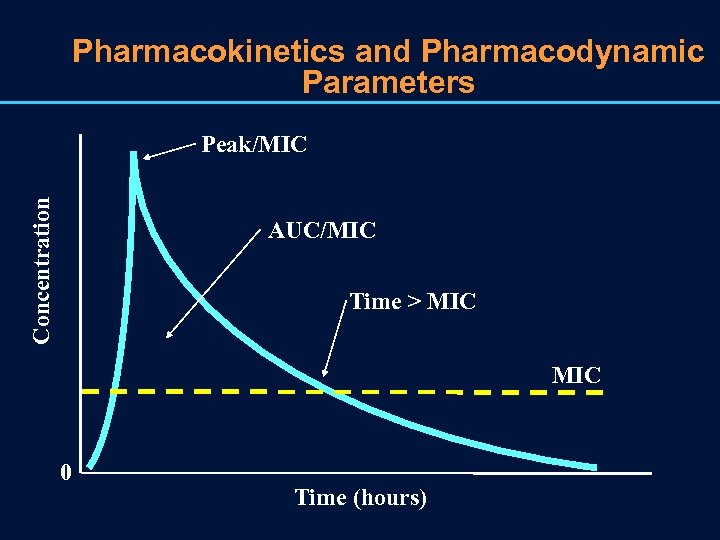 Pharmacokinetics and Pharmacodynamic Parameters Concentration Peak/MIC AUC/MIC Time > MIC 0 Time (hours)
Pharmacokinetics and Pharmacodynamic Parameters Concentration Peak/MIC AUC/MIC Time > MIC 0 Time (hours)
 AUC/MIC 90 Ratio of Major FQ for S. pneumoniae
AUC/MIC 90 Ratio of Major FQ for S. pneumoniae
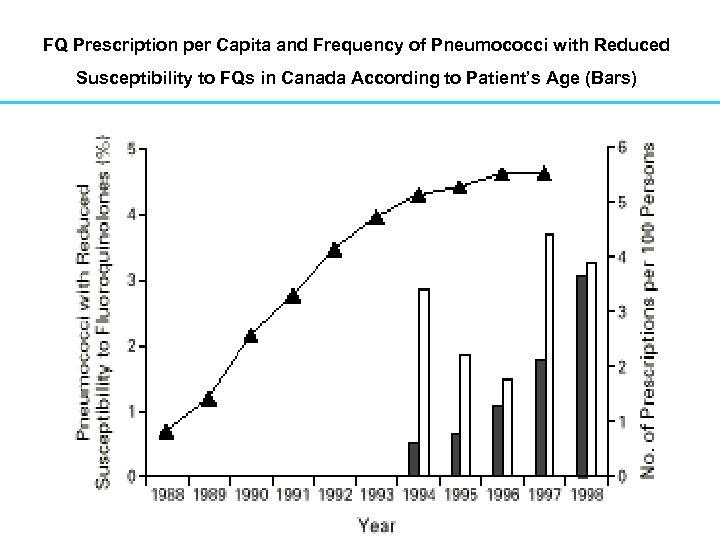 FQ Prescription per Capita and Frequency of Pneumococci with Reduced Susceptibility to FQs in Canada According to Patient’s Age (Bars)
FQ Prescription per Capita and Frequency of Pneumococci with Reduced Susceptibility to FQs in Canada According to Patient’s Age (Bars)
 Gatifloxacin vs Ceftriaxone ± Macrolide in Hospitalized CAP Patients Newly Hospitalized CAP Patients ( 18 years) Gatifloxacin IV 400 mg QD n=141 2 days Gatifloxacin PO 400 mg QD Ceftriaxone IV 1 or 2 g (32%) QD 2 days Clarithromycin PO ± Erythromycin IV 500 mg BID 0. 5 or 1 g (39%) q 6 h n=142 Treatment for 7 to 14 days Fogarty C et al. J Respir Dis. 1999; 20(suppl 11): S 60 -S 69. Please see IMPORTANT SAFETY INFORMATION slides. Please see full Prescribing Information.
Gatifloxacin vs Ceftriaxone ± Macrolide in Hospitalized CAP Patients Newly Hospitalized CAP Patients ( 18 years) Gatifloxacin IV 400 mg QD n=141 2 days Gatifloxacin PO 400 mg QD Ceftriaxone IV 1 or 2 g (32%) QD 2 days Clarithromycin PO ± Erythromycin IV 500 mg BID 0. 5 or 1 g (39%) q 6 h n=142 Treatment for 7 to 14 days Fogarty C et al. J Respir Dis. 1999; 20(suppl 11): S 60 -S 69. Please see IMPORTANT SAFETY INFORMATION slides. Please see full Prescribing Information.
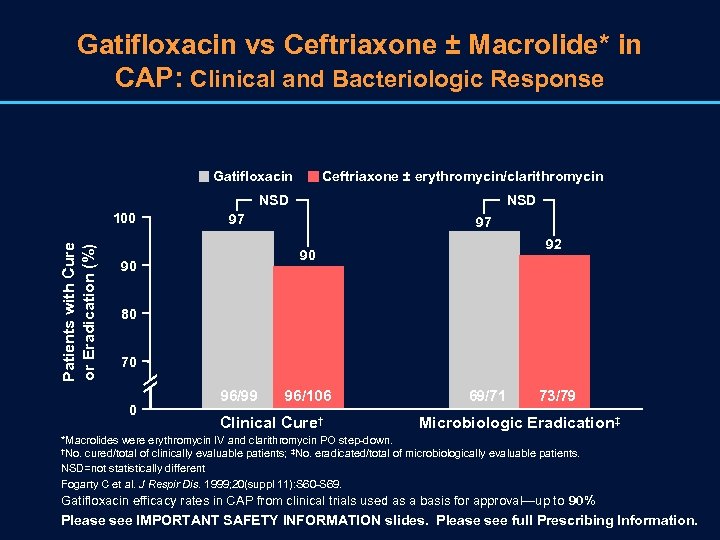 Gatifloxacin vs Ceftriaxone ± Macrolide* in CAP: Clinical and Bacteriologic Response Gatifloxacin Ceftriaxone ± erythromycin/clarithromycin NSD Patients with Cure or Eradication (%) 100 NSD 97 97 92 90 90 80 70 0 96/99 96/106 Clinical Cure† 69/71 73/79 Microbiologic Eradication‡ *Macrolides were erythromycin IV and clarithromycin PO step-down. †No. cured/total of clinically evaluable patients; ‡No. eradicated/total of microbiologically evaluable patients. NSD=not statistically different Fogarty C et al. J Respir Dis. 1999; 20(suppl 11): S 60 -S 69. Gatifloxacin efficacy rates in CAP from clinical trials used as a basis for approval—up to 90% Please see IMPORTANT SAFETY INFORMATION slides. Please see full Prescribing Information.
Gatifloxacin vs Ceftriaxone ± Macrolide* in CAP: Clinical and Bacteriologic Response Gatifloxacin Ceftriaxone ± erythromycin/clarithromycin NSD Patients with Cure or Eradication (%) 100 NSD 97 97 92 90 90 80 70 0 96/99 96/106 Clinical Cure† 69/71 73/79 Microbiologic Eradication‡ *Macrolides were erythromycin IV and clarithromycin PO step-down. †No. cured/total of clinically evaluable patients; ‡No. eradicated/total of microbiologically evaluable patients. NSD=not statistically different Fogarty C et al. J Respir Dis. 1999; 20(suppl 11): S 60 -S 69. Gatifloxacin efficacy rates in CAP from clinical trials used as a basis for approval—up to 90% Please see IMPORTANT SAFETY INFORMATION slides. Please see full Prescribing Information.
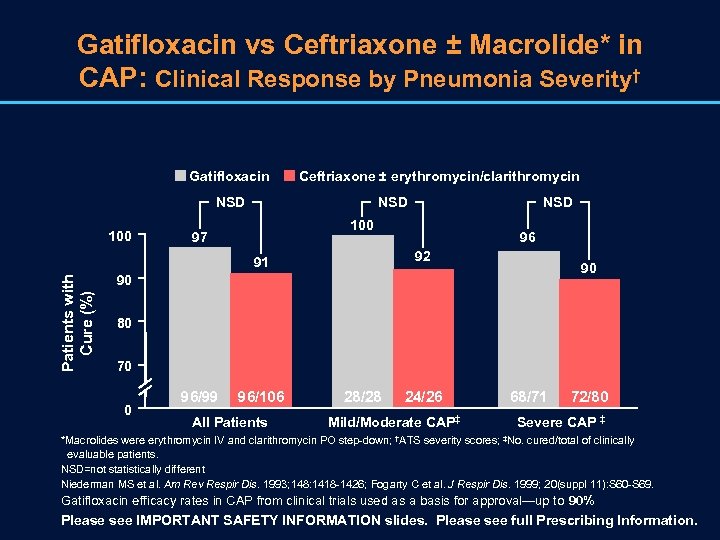 Gatifloxacin vs Ceftriaxone ± Macrolide* in CAP: Clinical Response by Pneumonia Severity† Gatifloxacin Ceftriaxone ± erythromycin/clarithromycin NSD 100 97 96 92 91 Patients with Cure (%) NSD 90 90 80 70 0 96/99 96/106 All Patients 28/28 24/26 Mild/Moderate CAP‡ 68/71 72/80 Severe CAP ‡ *Macrolides were erythromycin IV and clarithromycin PO step-down; †ATS severity scores; ‡No. cured/total of clinically evaluable patients. NSD=not statistically different Niederman MS et al. Am Rev Respir Dis. 1993; 148: 1418 -1426; Fogarty C et al. J Respir Dis. 1999; 20(suppl 11): S 60 -S 69. Gatifloxacin efficacy rates in CAP from clinical trials used as a basis for approval—up to 90% Please see IMPORTANT SAFETY INFORMATION slides. Please see full Prescribing Information.
Gatifloxacin vs Ceftriaxone ± Macrolide* in CAP: Clinical Response by Pneumonia Severity† Gatifloxacin Ceftriaxone ± erythromycin/clarithromycin NSD 100 97 96 92 91 Patients with Cure (%) NSD 90 90 80 70 0 96/99 96/106 All Patients 28/28 24/26 Mild/Moderate CAP‡ 68/71 72/80 Severe CAP ‡ *Macrolides were erythromycin IV and clarithromycin PO step-down; †ATS severity scores; ‡No. cured/total of clinically evaluable patients. NSD=not statistically different Niederman MS et al. Am Rev Respir Dis. 1993; 148: 1418 -1426; Fogarty C et al. J Respir Dis. 1999; 20(suppl 11): S 60 -S 69. Gatifloxacin efficacy rates in CAP from clinical trials used as a basis for approval—up to 90% Please see IMPORTANT SAFETY INFORMATION slides. Please see full Prescribing Information.
 Role of FQ in Treatment of CAP • To limit the emergence of FQ-resistant strains, the new FQ should be limited to adults: • For whom one of the above regimens has already failed, • Who are allergic to alternative agents, OR • Who have documented infection with highly drugresistant pneumococci (MIC ≥ 4 µg/ml)
Role of FQ in Treatment of CAP • To limit the emergence of FQ-resistant strains, the new FQ should be limited to adults: • For whom one of the above regimens has already failed, • Who are allergic to alternative agents, OR • Who have documented infection with highly drugresistant pneumococci (MIC ≥ 4 µg/ml)
 Pneumococcal Vaccine • Older than 2 years with: • functional or anatomic asplenia** • immunocompromise or immunosuppression** • HIV infection** • malignancy** • chronic renal failure, HD, nephrotic syndrome** • chronic cardiovascular or pulmonary illness** • Alaskan natives, American Indians • Revaccination • if >65 years, consider revaccination in 5 yr**
Pneumococcal Vaccine • Older than 2 years with: • functional or anatomic asplenia** • immunocompromise or immunosuppression** • HIV infection** • malignancy** • chronic renal failure, HD, nephrotic syndrome** • chronic cardiovascular or pulmonary illness** • Alaskan natives, American Indians • Revaccination • if >65 years, consider revaccination in 5 yr**
 CDC Recommendations: Who Should Receive Influenza Vaccine? • Persons at increased risk (age 6 mos) • Hospital and outpatient employees • Nursing home employees with patient contact • Home health care providers working with high-risk persons • Household members of high-risk persons • Persons desiring to avoid influenza infection MMWR. 1999; 48: 5 -7.
CDC Recommendations: Who Should Receive Influenza Vaccine? • Persons at increased risk (age 6 mos) • Hospital and outpatient employees • Nursing home employees with patient contact • Home health care providers working with high-risk persons • Household members of high-risk persons • Persons desiring to avoid influenza infection MMWR. 1999; 48: 5 -7.
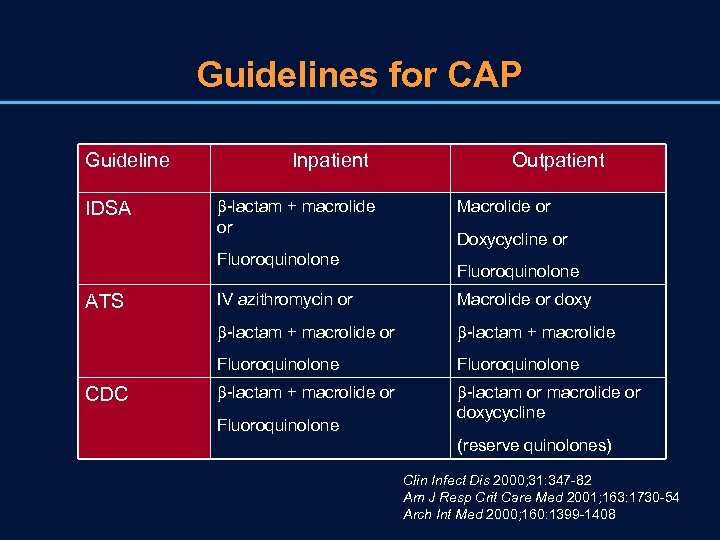 Guidelines for CAP Guideline IDSA Inpatient -lactam + macrolide or Fluoroquinolone Outpatient Macrolide or Doxycycline or Fluoroquinolone Macrolide or doxy -lactam + macrolide Fluoroquinolone CDC IV azithromycin or -lactam + macrolide or ATS Fluoroquinolone -lactam + macrolide or -lactam or macrolide or doxycycline Fluoroquinolone (reserve quinolones) Clin Infect Dis 2000; 31: 347 -82 Am J Resp Crit Care Med 2001; 163: 1730 -54 Arch Int Med 2000; 160: 1399 -1408
Guidelines for CAP Guideline IDSA Inpatient -lactam + macrolide or Fluoroquinolone Outpatient Macrolide or Doxycycline or Fluoroquinolone Macrolide or doxy -lactam + macrolide Fluoroquinolone CDC IV azithromycin or -lactam + macrolide or ATS Fluoroquinolone -lactam + macrolide or -lactam or macrolide or doxycycline Fluoroquinolone (reserve quinolones) Clin Infect Dis 2000; 31: 347 -82 Am J Resp Crit Care Med 2001; 163: 1730 -54 Arch Int Med 2000; 160: 1399 -1408
 I prefer to decide my prescription strategies for CAP on the basis of severity of the patient’s condition, the presence of comorbidities, and the epidemiologic pattern in each geographical area. J. Rello - Chest (May 98)
I prefer to decide my prescription strategies for CAP on the basis of severity of the patient’s condition, the presence of comorbidities, and the epidemiologic pattern in each geographical area. J. Rello - Chest (May 98)
 Acknowledgements • Dr Naiel Nassar MD FACP Assistant professor of Medicine UTSW Dallas
Acknowledgements • Dr Naiel Nassar MD FACP Assistant professor of Medicine UTSW Dallas


