f1d06a802dd1b67c9866c19bd4406807.ppt
- Количество слайдов: 183

ABSITE REVIEW Vascular Jessica O’Connell, MD January 25, 2012

Q 0 Question: Most common cranial nerve injured during CEA? Vagus nerve (hoarseness) Question: Other cranial nerves injured during CEA? Hypoglossal nerve – tongue deviation toward side of injury – swallowing/mastication/speech difficulty Question: What happens if you cut the Ansa Cervicalis – no serious deficits – innervates strap muscles
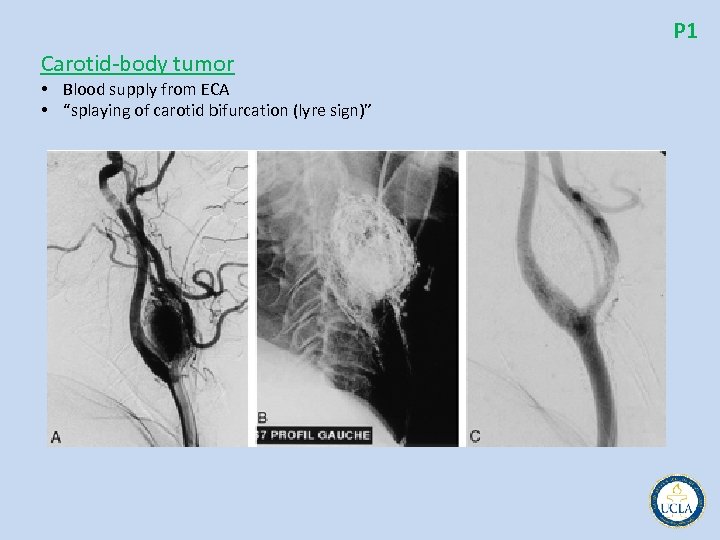
P 1 Carotid body tumor • Blood supply from ECA • “splaying of carotid bifurcation (lyre sign)”
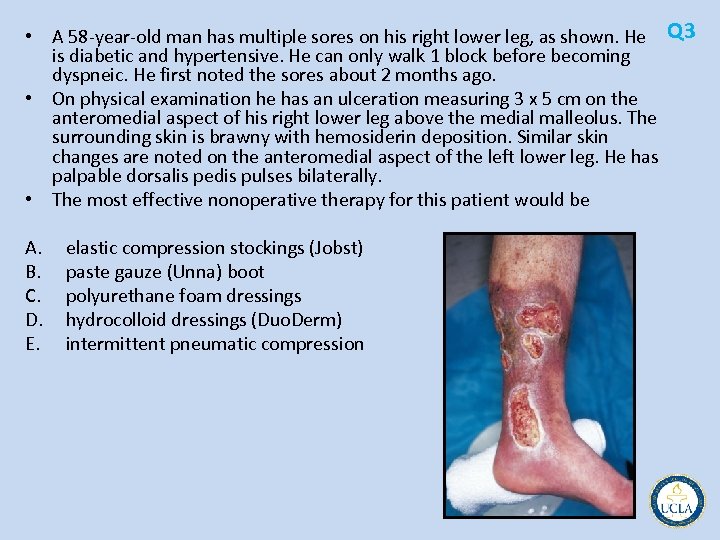
• A 58 year old man has multiple sores on his right lower leg, as shown. He Q 3 is diabetic and hypertensive. He can only walk 1 block before becoming dyspneic. He first noted the sores about 2 months ago. • On physical examination he has an ulceration measuring 3 x 5 cm on the anteromedial aspect of his right lower leg above the medial malleolus. The surrounding skin is brawny with hemosiderin deposition. Similar skin changes are noted on the anteromedial aspect of the left lower leg. He has palpable dorsalis pedis pulses bilaterally. • The most effective nonoperative therapy for this patient would be A. B. C. D. E. elastic compression stockings (Jobst) paste gauze (Unna) boot polyurethane foam dressings hydrocolloid dressings (Duo. Derm) intermittent pneumatic compression
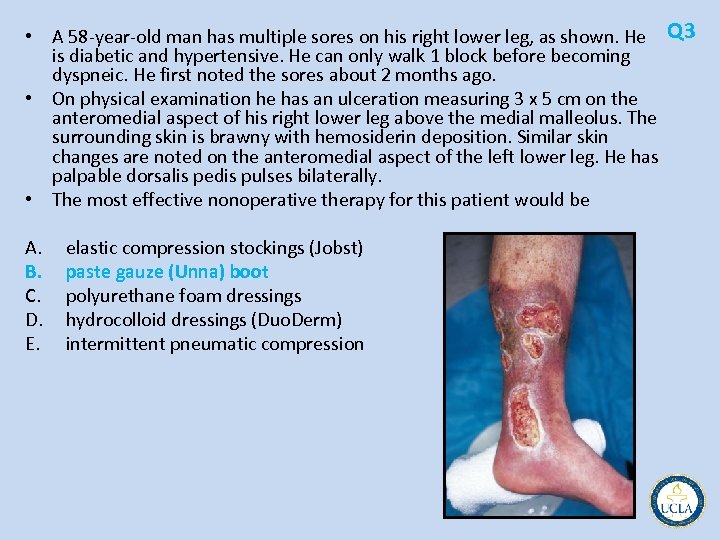
• A 58 year old man has multiple sores on his right lower leg, as shown. He Q 3 is diabetic and hypertensive. He can only walk 1 block before becoming dyspneic. He first noted the sores about 2 months ago. • On physical examination he has an ulceration measuring 3 x 5 cm on the anteromedial aspect of his right lower leg above the medial malleolus. The surrounding skin is brawny with hemosiderin deposition. Similar skin changes are noted on the anteromedial aspect of the left lower leg. He has palpable dorsalis pedis pulses bilaterally. • The most effective nonoperative therapy for this patient would be A. B. C. D. E. elastic compression stockings (Jobst) paste gauze (Unna) boot polyurethane foam dressings hydrocolloid dressings (Duo. Derm) intermittent pneumatic compression

Q 3 • venous stasis ulcers • trial of nonoperative therapy is indicated in this high risk surgical patient • Compressive therapy • paste gauze (Unna) boots are superior to elastic compression stockings (Jobst), polyurethane foam dressings, and elastic compression wraps, hydrocolloid (Duo. Derm) • combination of intermittent pneumatic compression (IPC) stockings and elastic compression wraps superior to elastic compression • However, the IPC patients also had periods of leg elevation, which may have influenced the healing rates • IPC stockings alone have not been compared with Unna boots
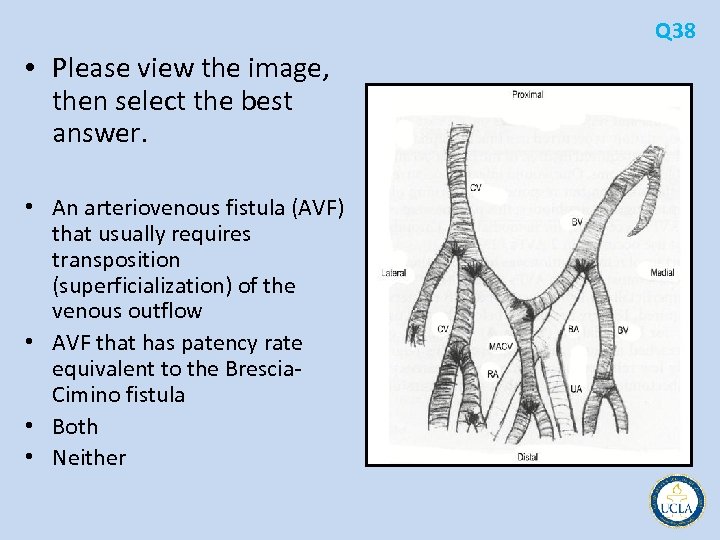
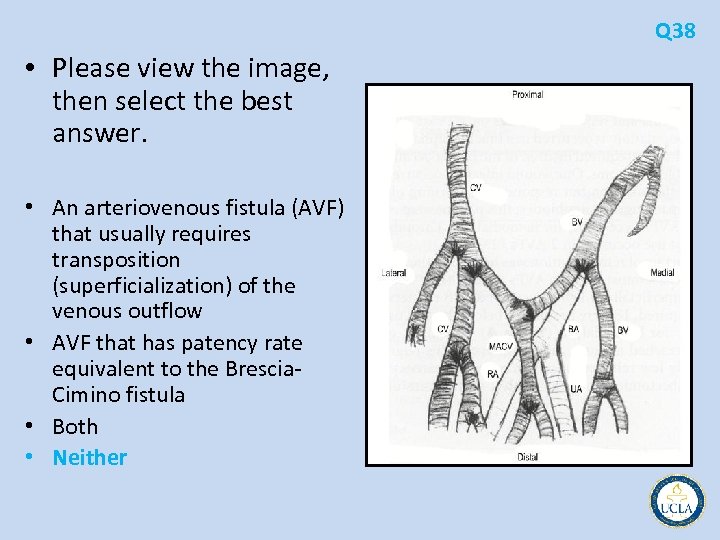
Q 38 • Please view the image, then select the best answer. • An arteriovenous fistula (AVF) that usually requires transposition (superficialization) of the venous outflow • AVF that has patency rate equivalent to the Brescia Cimino fistula • Both • Neither
Q 38 • Please view the image, then select the best answer. • An arteriovenous fistula (AVF) that usually requires transposition (superficialization) of the venous outflow • AVF that has patency rate equivalent to the Brescia Cimino fistula • Both • Neither
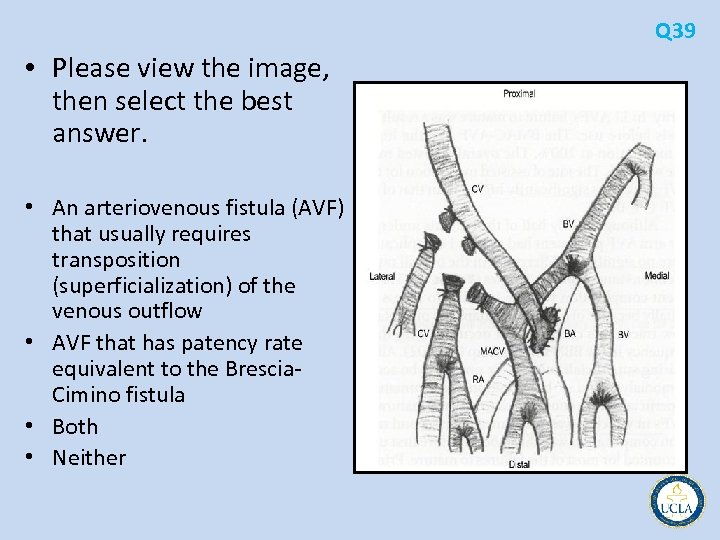
Q 39 • Please view the image, then select the best answer. • An arteriovenous fistula (AVF) that usually requires transposition (superficialization) of the venous outflow • AVF that has patency rate equivalent to the Brescia Cimino fistula • Both • Neither
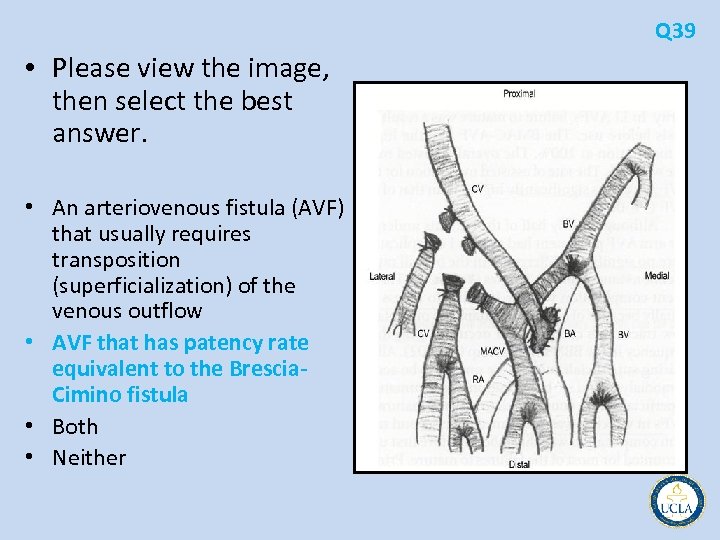
Q 39 • Please view the image, then select the best answer. • An arteriovenous fistula (AVF) that usually requires transposition (superficialization) of the venous outflow • AVF that has patency rate equivalent to the Brescia. Cimino fistula • Both • Neither
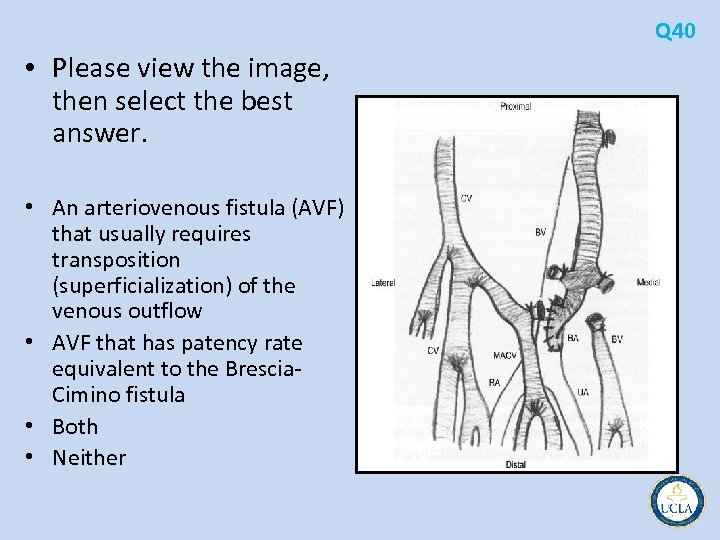
Q 40 • Please view the image, then select the best answer. • An arteriovenous fistula (AVF) that usually requires transposition (superficialization) of the venous outflow • AVF that has patency rate equivalent to the Brescia Cimino fistula • Both • Neither
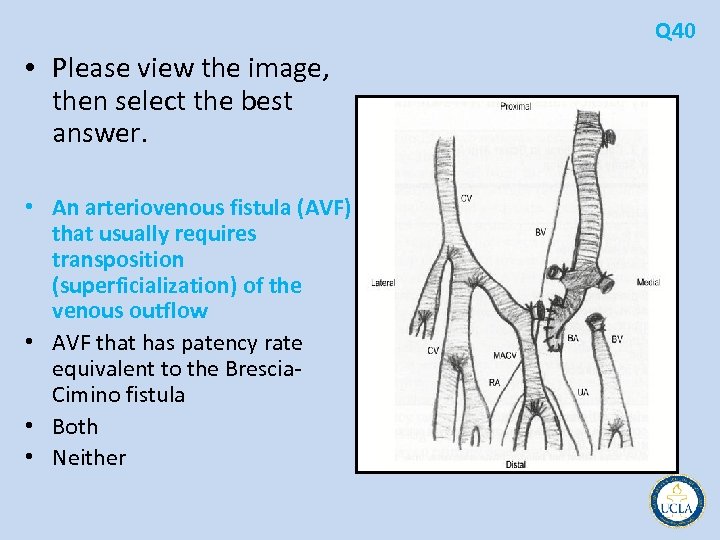
Q 40 • Please view the image, then select the best answer. • An arteriovenous fistula (AVF) that usually requires transposition (superficialization) of the venous outflow • AVF that has patency rate equivalent to the Brescia Cimino fistula • Both • Neither

• 38 is the normal anatomy of the right antecubital fossa • 39 is the brachial artery to cephalic vein fistula, probably the most commonly used • 40 is brachial artery to basilic vein fistula • In a study comparing the three types of fistulas, all had patency rates comparable to the forearm radiocephalic fistula • the brachial artery to basilic vein required transposition of the outflow vein (the brachial vein) into the subcutaneous position Q 38 -40

Q 1

Q 1
Q 1
Q 1

• A 53 year old man has a 1 week history of a painful blue right first Q 4 toe. Before his toe turned blue, he was able to climb 4 flights of stairs without difficulty. On physical examination, his first toe is bluish, and he has palpable pedal pulses bilaterally. He complains of numbness and tingling below the knee. He also has a palpable pulsatile mass in his right popliteal fossa. Ultrasound examination confirms the presence of a 4 cm right popliteal aneurysm. A. B. C. D. E. F. The most appropriate treatment would be systemic anticoagulation ligation of the aneurysm with bypass graft endovascular stent operative resection of the aneurysm with primary repair aneurysmorrhaphy with interposition graft

• A 53 year old man has a 1 week history of a painful blue right first Q 4 toe. Before his toe turned blue, he was able to climb 4 flights of stairs without difficulty. On physical examination, his first toe is bluish, and he has palpable pedal pulses bilaterally. He complains of numbness and tingling below the knee. He also has a palpable pulsatile mass in his right popliteal fossa. Ultrasound examination confirms the presence of a 4 cm right popliteal aneurysm. A. B. C. D. E. F. The most appropriate treatment would be systemic anticoagulation ligation of the aneurysm with bypass graft endovascular stent operative resection of the aneurysm with primary repair aneurysmorrhaphy with interposition graft

• thromboembolic complication from a large popliteal aneurysm • A combined review of 536 asymptomatic patients with popliteal aneurysm, with a mean follow up of approximately 4 years, 35% developed thromboembolic complications. The associated amputation rate was 25%. • Most complications occur in aneurysms with diameters > 2 cm • early operation for asymptomatic aneurysms larger than 2 cm is indicated. • Surgical techniques – exclusion of the aneurysm with a bypass graft. The aneurysm is ligated proximally and distally, then continuity is re established using an extra aneurysmal bypass graft – Aneurysmorhapy with interposition graft, the aneurysm can be incised, followed by ligation of any collateral vessels, and then the bypass graft is placed within the bed of the aneurysm • indicated for larger aneurysms causing any compressive symptoms lower leg pain, numbness, paresthesia, venous congestion, and edema. • eliminates the possibility of recurrence or continued expansion of the aneurysm. – Vascular stent graft stents at the knee in a younger person with a low operative risk ? ? durability and long term patency still under question Q 4

Q 5 • A 28 year old female body builder has the acute onset of a swollen right arm. Which of the following statements about her condition is TRUE? A. B. C. D. E. Higher incidence in females Often accompanied by neurologic symptoms Not successfully treated with anticoagulation therapy Definitively treated with catheter directed thrombolysis Associated with venous gangrene of the upper extremities

Q 5 • A 28 year old female body builder has the acute onset of a swollen right arm. Which of the following statements about her condition is TRUE? A. B. C. D. E. Higher incidence in females Often accompanied by neurologic symptoms Not successfully treated with anticoagulation therapy Definitively treated with catheter directed thrombolysis Associated with venous gangrene of the upper extremities

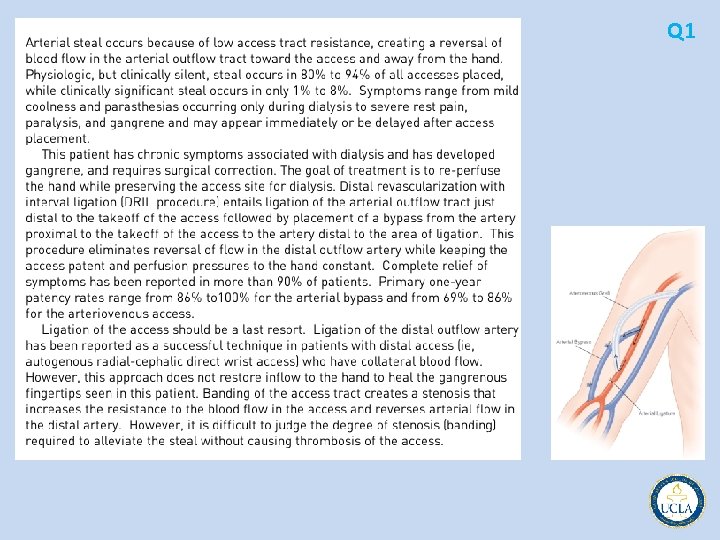
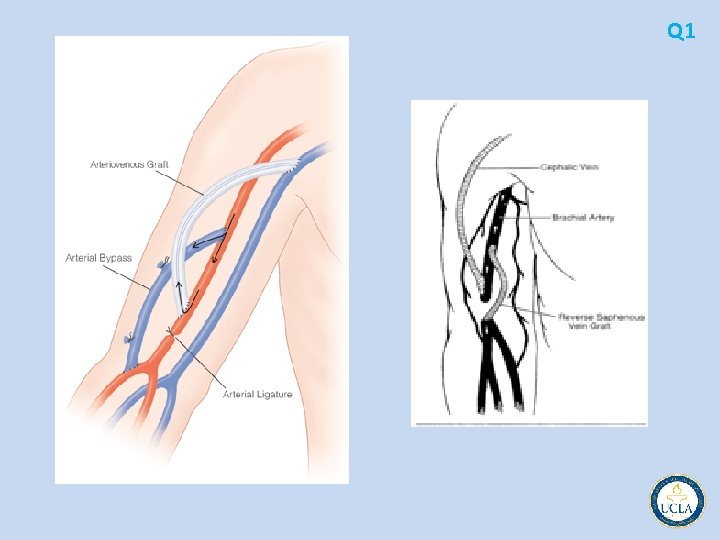
• • • primary axillary subclavian vein thrombosis young patients, 2: 1 male: female ratio strenuous or repetitive upper extremity activity compression of the subclavian vein at the thoracic outlet often becomes chronic, debilitating venous outflow obstruction Neurologic symptoms do not usually accompany primary venous thrombosis, because the vein and nerves are at the opposite ends of the thoracic outlet. traditional treatment elevation of upper extremity/anticoagulation persistent symptoms in up to 80% catheter directed followed by dynamic venography operative thoracic outlet decompression Q 5
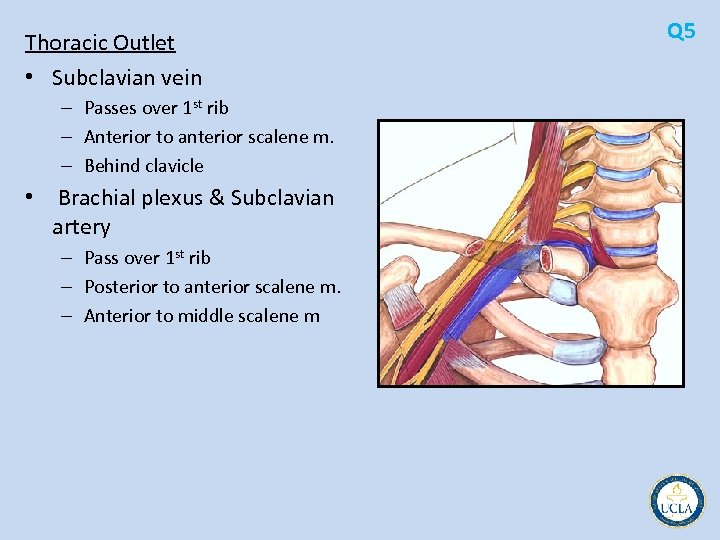
Thoracic Outlet • Subclavian vein – Passes over 1 st rib – Anterior to anterior scalene m. – Behind clavicle • Brachial plexus & Subclavian artery – Pass over 1 st rib – Posterior to anterior scalene m. – Anterior to middle scalene m Q 5

Thoracic Outlet Exam Q 5 Adson maneuvers: While the patient is in a sitting position, ask the patient to inspire deeply, hold his breath, and extend his neck. Then, turn the patient's head passively as far as possible toward one side and then the other. When the head is turned toward the unaffected side, or sometimes the affected side, obliteration of the radial pulse with a drop in blood pressure in the arm is considered a positive result. Roos maneuver: When in the surrender posture, the patient reports paresthesia and numbness in extremities within 1 minute. This maneuver usually provokes symptoms in lateral cord distribution. Elevated-arm stress test: In this test, the patient keeps arms abducted with flexed elbows for 3 minutes while flexing and extending the fingers. Results are considered positive if the patient cannot do this for 3 minutes. Wright maneuver: This maneuver requires the patient to hold the arms next to the ears. Paresthesias usually are noted down the medial scapular border and into lower trunk distribution. Hyperabduction test: The radial pulse is diminished after elevating the involved arm above the head. Military maneuver (ie, costoclavicular bracing): This maneuver provokes symptoms when the patient elevates the chin and pulls the shoulder joint behind in an extreme "attention" position.
Q 1 Question: Which nerve/artery is commonly injured with fracture of the mid shaft humerus? Radial nerve Question: Which nerve/artery is commonly injured with supracondylar fracture of the humerus? Brachial artery Question: Which nerve/artery is commonly injured with distal radius fracture? Median nerve
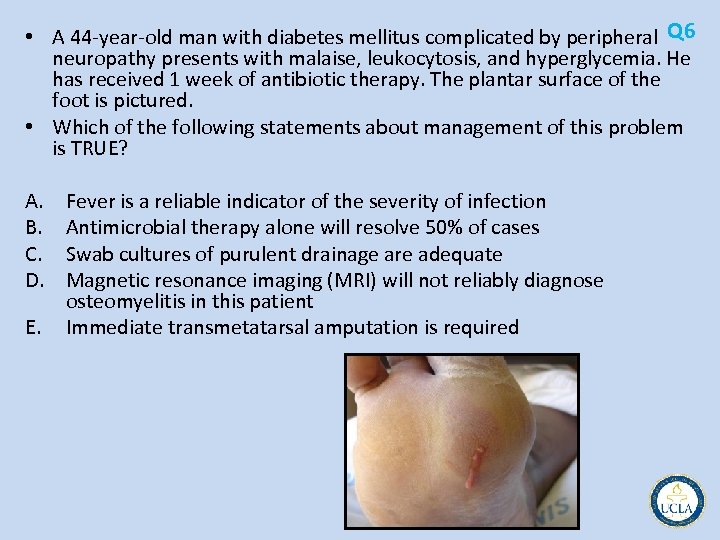
• A 44 year old man with diabetes mellitus complicated by peripheral Q 6 neuropathy presents with malaise, leukocytosis, and hyperglycemia. He has received 1 week of antibiotic therapy. The plantar surface of the foot is pictured. • Which of the following statements about management of this problem is TRUE? A. B. C. D. E. Fever is a reliable indicator of the severity of infection Antimicrobial therapy alone will resolve 50% of cases Swab cultures of purulent drainage are adequate Magnetic resonance imaging (MRI) will not reliably diagnose osteomyelitis in this patient Immediate transmetatarsal amputation is required
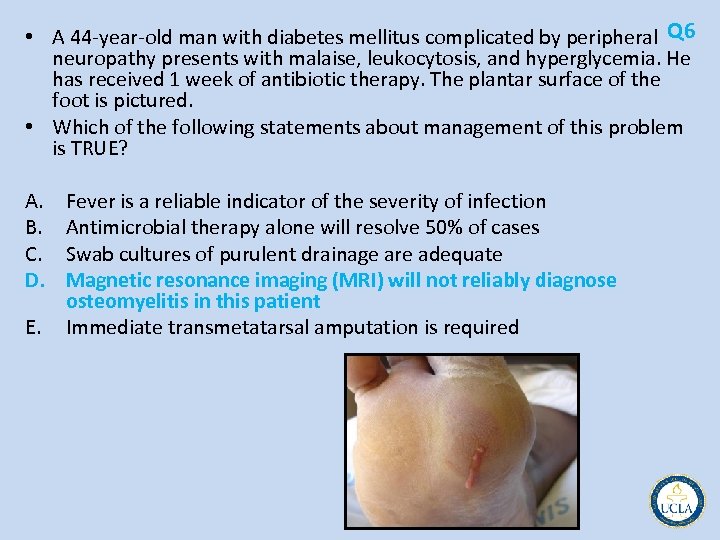
• A 44 year old man with diabetes mellitus complicated by peripheral Q 6 neuropathy presents with malaise, leukocytosis, and hyperglycemia. He has received 1 week of antibiotic therapy. The plantar surface of the foot is pictured. • Which of the following statements about management of this problem is TRUE? A. B. C. D. E. Fever is a reliable indicator of the severity of infection Antimicrobial therapy alone will resolve 50% of cases Swab cultures of purulent drainage are adequate Magnetic resonance imaging (MRI) will not reliably diagnose osteomyelitis in this patient Immediate transmetatarsal amputation is required

Q 6 • Foot ulcers occur in 15% of all patients with diabetes • chronic immunosuppression that accompanies diabetes mellitus, the usual physical signs and symptoms of infection are often not present • Diabetic foot wounds must first be probed – – – underlying sinus tracts or abscesses deep or proximal extension along fascial planes bones and joints involvement Probing to bone PPV 89% for osteomyelitis in diabetic foot infections frequently neuropathic patients. • mixed infections broad spectrum antibiotisc – Staphylococcus aureus, Streptococcus, Enterobacter, and Bacteroides fragilis • MRI sensitive and specific indicator of true bone marrow infection – previous trauma, operation, or Charcot osteoarthropathy reduces the specificity – combining bone scintigraphy with leukocyte scans specificity >80%. • Management – – avoidance of weightbearing immediate drainage and debridement procedures hyperglycemic control management of ischemia
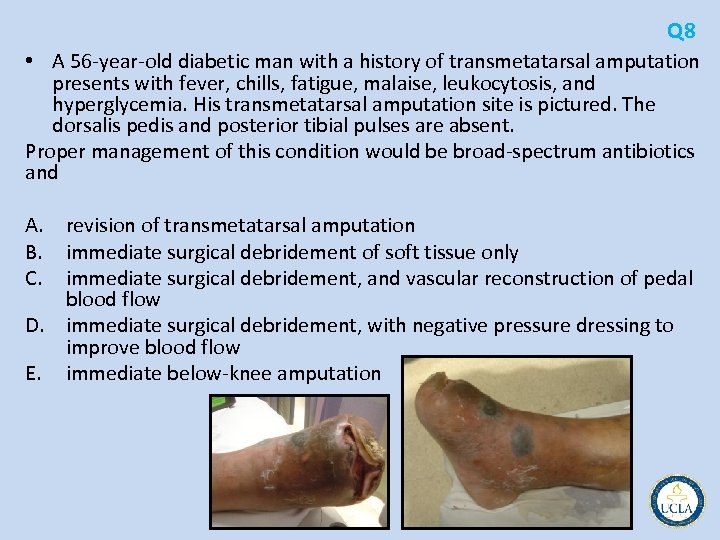
Q 8 • A 56 year old diabetic man with a history of transmetatarsal amputation presents with fever, chills, fatigue, malaise, leukocytosis, and hyperglycemia. His transmetatarsal amputation site is pictured. The dorsalis pedis and posterior tibial pulses are absent. Proper management of this condition would be broad spectrum antibiotics and A. revision of transmetatarsal amputation B. immediate surgical debridement of soft tissue only C. immediate surgical debridement, and vascular reconstruction of pedal blood flow D. immediate surgical debridement, with negative pressure dressing to improve blood flow E. immediate below knee amputation
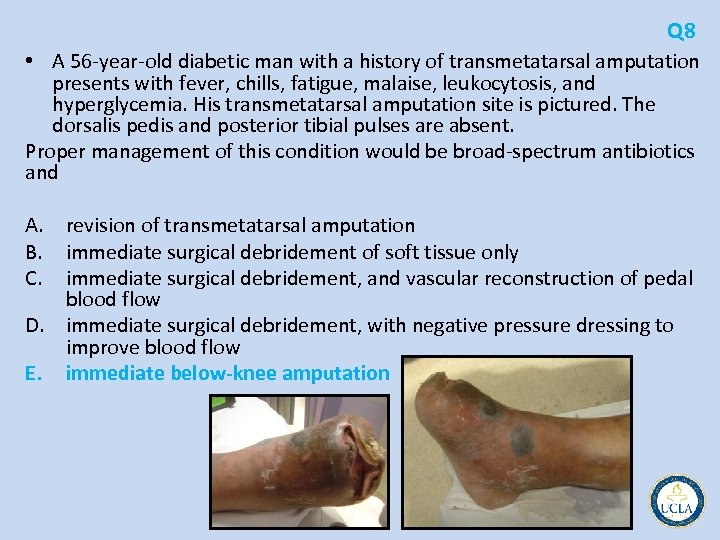
Q 8 • A 56 year old diabetic man with a history of transmetatarsal amputation presents with fever, chills, fatigue, malaise, leukocytosis, and hyperglycemia. His transmetatarsal amputation site is pictured. The dorsalis pedis and posterior tibial pulses are absent. Proper management of this condition would be broad spectrum antibiotics and A. revision of transmetatarsal amputation B. immediate surgical debridement of soft tissue only C. immediate surgical debridement, and vascular reconstruction of pedal blood flow D. immediate surgical debridement, with negative pressure dressing to improve blood flow E. immediate below-knee amputation

Q 8 • clinically infected, gangrenous transmetatarsal amputation • systemic signs and symptoms of sepsis, including leukocytosis and hyperglycemia • absence of dorsalis pedis and posterior tibial pulses • immediate need halt the spread of sepsis before fatal • immediate broad spectrum antibiotic therapy • immediate guillotine amputation • once the sepsis is controlled, revision of the amputation can be undertaken • negative pressure dressings do not improve blood flow to ischemic tissues
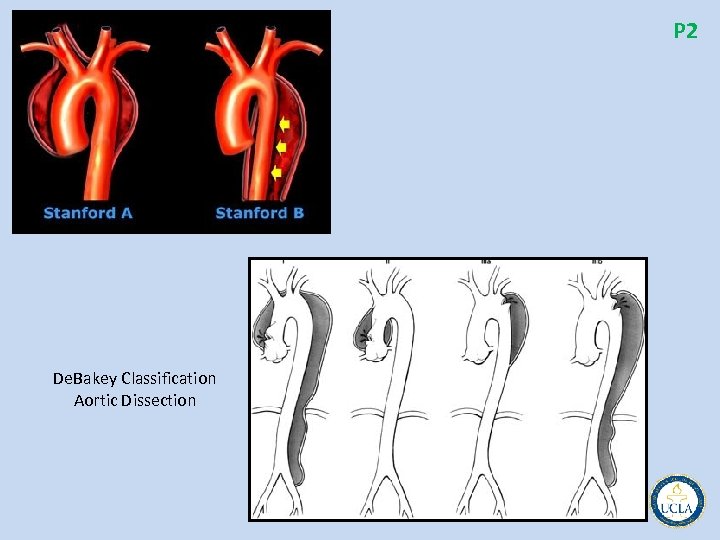
P 2 De. Bakey Classification Aortic Dissection

Q 9 • Which of the following statements about antithrombotic treatments is TRUE? A. In the absence of antithrombin III, unfractionated heparin has no significant anticoagulant effect B. Low molecular weight heparins share the ability to accelerate the activity of factor Xa C. Warfarin inhibits the absorption of vitamin K from the intestinal tract D. Hirudin, a synthetic thrombin inhibitor, is dependent on antithrombin III for anticoagulant activity E. The addition of aspirin to heparin increases the anticoagulant effect without increasing the risk of hemorrhagic side effects

Q 9 • Which of the following statements about antithrombotic treatments is TRUE? A. In the absence of antithrombin III, unfractionated heparin has no significant anticoagulant effect B. Low molecular weight heparins share the ability to accelerate the activity of factor Xa C. Warfarin inhibits the absorption of vitamin K from the intestinal tract D. Hirudin, a synthetic thrombin inhibitor, is dependent on antithrombin III for anticoagulant activity E. The addition of aspirin to heparin increases the anticoagulant effect without increasing the risk of hemorrhagic side effects

• Unfractionated heparin indirect thrombin inhibitor – acceleration of the interaction of antithrombin III with thrombin (factor IIa) – In the absence of antithrombin, unfractionated heparin has no significant antithrombotic effect – Antithrombin III levels can be increased by the infusion of fresh frozen plasma • low molecular weight heparins inhibition of factor Xa – down regulation of thrombin production • Warfarin inhibits vitamin K dependent terminal carboxylation of factors II, VII, IX, and X in the liver – oral anticoagulant, no impact on GI absorption of vitamin K • Hirudin direct thrombin inhibitor – isolated from the saliva of the medical leech, reproduced with recombinant technology – not dependent on the activity of antithrombin III – heparin associated antibodies Q 9

Q 10 • Which of the following statements about management of abdominal aortic aneurysm (AAA) is TRUE? A. Elective operation should be considered for patients with symptomatic AAA in the absence of significant co morbidities B. The risk of rupture is higher in women than men for small aneurysms C. In an otherwise healthy 75 year old man, a 4. 5 cm aneurysm should be repaired D. An unreliable patient who is unlikely to comply with lifelong surveillance should be preferentially offered endograft versus open repair E. Mortality is not related to the hospital's volume of AAA repairs performed

Q 10 • Which of the following statements about management of abdominal aortic aneurysm (AAA) is TRUE? A. Elective operation should be considered for patients with symptomatic AAA in the absence of significant co morbidities B. The risk of rupture is higher in women than men for small aneurysms C. In an otherwise healthy 75 year old man, a 4. 5 cm aneurysm should be repaired D. An unreliable patient who is unlikely to comply with lifelong surveillance should be preferentially offered endograft versus open repair E. Mortality is not related to the hospital's volume of AAA repairs performed

• The mortality of untreated rupture of abdominal aortic aneurysms Q 10 (AAA) approaches 100% • AAA presenting with abdominal and/or back pain (most common) should be repaired urgently in almost all patients regardless of co morbidity • UK Small Aneurysm Trial – significantly higher risk of rupture for small aneurysms in women compared with men • Patients undergoing endograft repair of AAA must be willing to comply with rigorous lifelong surveillance – graft migration, endoleak, and limb obstruction • annual risk of rupture 4. 5 cm AAA in a 75 year old man is ~1% per year VA sponsored Aneurysm Detection and Management (ADAM) trial • No survival advantage for open repair of small (4. 0 to 5. 5 cm) AAA in two large trials in both the United States (ADAM) and Great Britain (UK Small Aneurysm Trial) • The average life expectancy for an 80 year old man after successful repair of AAA is approximately 7 years, or about half the life expectancy for an age matched man without AAA repair • Mortality is lower with higher hospital volume

Q 2 Question: Which nerve/artery is commonly injured with supracondylar fracture of femur? Popliteal artery Question: Which nerve/artery is commonly injured with posterior dislocation of hip? Sciatic nerve Question: Which nerve/artery is commonly injured with posterior dislocation of knee? Popliteal artery

Q 12 • Which of the following statements about the natural history of intermittent claudication is TRUE? A. Five year survival is > 90% B. Most patients eventually require revascularization to avoid amputation C. One in 4 patients will eventually undergo major amputation D. Intermittent claudication is a risk factor for adverse cardiovascular events E. Abstinence from tobacco does not improve the symptoms of intermittent claudication

Q 12 • Which of the following statements about the natural history of intermittent claudication is TRUE? A. Five year survival is > 90% B. Most patients eventually require revascularization to avoid amputation C. One in 4 patients will eventually undergo major amputation D. Intermittent claudication is a risk factor for adverse cardiovascular events E. Abstinence from tobacco does not improve the symptoms of intermittent claudication

• • Q 12 claudication derived from the root word "to limp“ reproducible leg pain relieved with rest ankle: brachial index (ABI) ratio of ankle pressure to arm pressure normal 0. 9 to 1. 2 Peripheral arterial disease, ABI < 0. 9 25% of elderly patients seen in primary care (1/2 asymptomatic) Intermittent claudication is relatively benign – amputation (5% to 7%) – 25% of patients need intervention • marker for patients at risk of future adverse cardiovascular events • modifying the risk factors of systemic atherosclerosis: – smoking, obesity, hypertension, diabetes, and hyperlipidemia • The 5 year mortality 30% to 50%, due to cardiovascular events • Smoking cessation improves the symptoms

Ankle : Brachial index (ABI) – ratio of ankle pressure to arm pressure – Ankle : Arm Index (AAI) normal 0. 9 to 1. 2 Peripheral arterial disease, ABI < 0. 9 Claudication 0. 4– 0. 9 Rest pain 0. 2– 0. 5 Tissue loss < 0. 4 Gangrene < 0. 3 > 0. 50 in 85% of patients with single level of disease • < 0. 50 in 95% with two or more levels of disease • • Q 12

Q 13 • A 30 year old man presents with a brief history of crampy, midabdominal pain. Physical examination is notable for diffuse mild tenderness, but frank signs of peritonitis are absent. Computed tomographic (CT) scan suggests findings consistent with mesenteric venous thrombosis. The initial recommended treatment for symptomatic mesenteric venous thrombosis is A. B. C. D. E. venous thrombectomy anticoagulation with heparin tissue plasminogen activator (t. PA) via the superior mesenteric artery warfarin (Coumadin) anticoagulation systemic t. PA

Q 13 • A 30 year old man presents with a brief history of crampy, midabdominal pain. Physical examination is notable for diffuse mild tenderness, but frank signs of peritonitis are absent. Computed tomographic (CT) scan suggests findings consistent with mesenteric venous thrombosis. The initial recommended treatment for symptomatic mesenteric venous thrombosis is A. B. C. D. E. venous thrombectomy anticoagulation with heparin tissue plasminogen activator (t. PA) via the superior mesenteric artery warfarin (Coumadin) anticoagulation systemic t. PA

Q 13 • diagnosis of mesenteric venous thrombosis increasing frequency – CT imaging • hypercoagulable w/u recommended • Long term anticoagulation in asymptomatic patients NOT generally recommended • symptomatic patient, treatment is clearly indicated • thrombolytic agents has not definitively demonstrated to accelerate the lysis of mesenteric venous thrombosis or improve the clinical outcome • Systemic anticoagulation with intravenous heparin and fluid resuscitation are the mainstays of therapy • Surgical exploration signs of abdominal catastrophe • The apparent lethality of mesenteric venous thrombosis has decreased during the last decade due to earlier detection and treatment • Mesenteric venous thrombosis <10% of clinically significant mesenteric ischemia • A hypercoagulable state > 90% of patients

Q 14 • A 75 year old man with a ruptured abdominal aortic aneurysm, as shown, is taken urgently to the operating room for repair Which of the following has the most important influence on operative mortality? A. B. C. D. E. Distance from patient's home to hospital Number of co morbidities Surgeon experience Annual hospital volume of aneurysm repair Site of aortic rupture

Q 14 • A 75 year old man with a ruptured abdominal aortic aneurysm, as shown, is taken urgently to the operating room for repair Which of the following has the most important influence on operative mortality? A. B. C. D. E. Distance from patient's home to hospital Number of co morbidities Surgeon experience Annual hospital volume of aneurysm repair Site of aortic rupture

• Ruptured abdominal aortic aneurysms (AAA) overall mortality Q 14 rate of 90% • operative mortality arrive at the hospital alive ~50% • but a number of factors influence the 30 day mortality • population studies: advanced patient significantly associated with mortality; however, race, distance from home to hospital, and medical complexity were not significant factors • surgeon experience > 10 ruptured AAA had a significantly lower mortality rate • annual volume of elective AAA repairs did not influence outcome, nor did hospital volume of ruptured or elective AAA repair
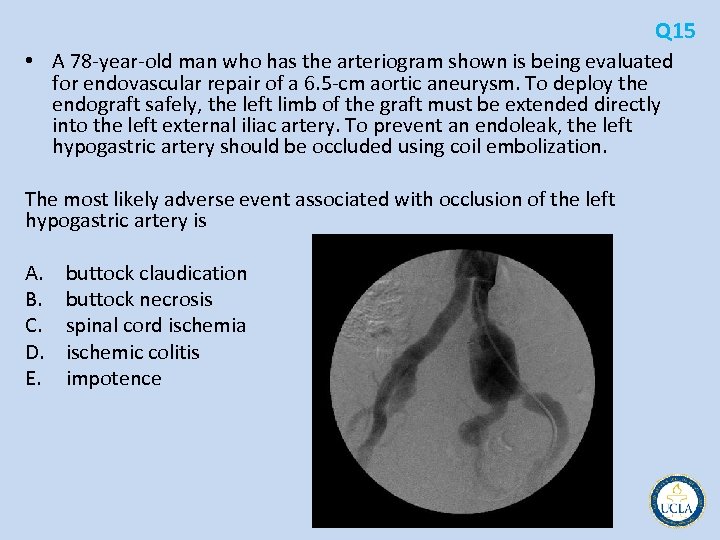
Q 15 • A 78 year old man who has the arteriogram shown is being evaluated for endovascular repair of a 6. 5 cm aortic aneurysm. To deploy the endograft safely, the left limb of the graft must be extended directly into the left external iliac artery. To prevent an endoleak, the left hypogastric artery should be occluded using coil embolization. The most likely adverse event associated with occlusion of the left hypogastric artery is A. B. C. D. E. buttock claudication buttock necrosis spinal cord ischemia ischemic colitis impotence
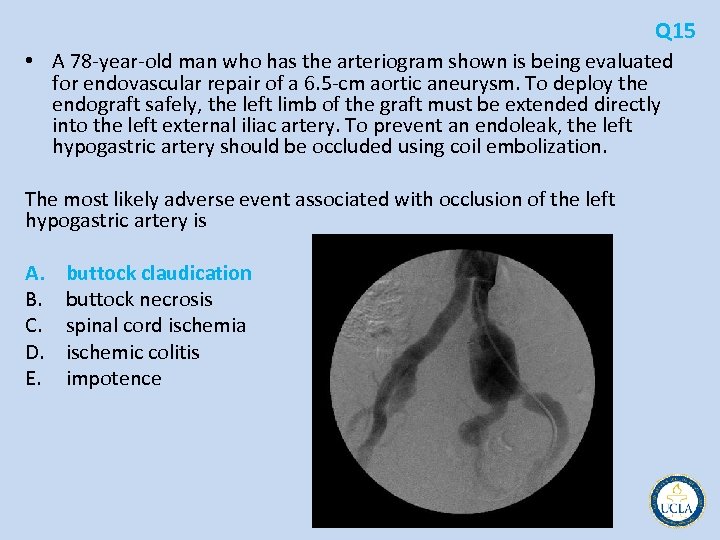
Q 15 • A 78 year old man who has the arteriogram shown is being evaluated for endovascular repair of a 6. 5 cm aortic aneurysm. To deploy the endograft safely, the left limb of the graft must be extended directly into the left external iliac artery. To prevent an endoleak, the left hypogastric artery should be occluded using coil embolization. The most likely adverse event associated with occlusion of the left hypogastric artery is A. B. C. D. E. buttock claudication buttock necrosis spinal cord ischemia ischemic colitis impotence

Q 15 • Endovascular aortic aneurysm repair (EVAR) has become a standard treatment option for aortoiliac aneurysms • As devices have improved, challenging vascular anatomy short aneurysm necks and small iliac arteries • Successful treatment graft device creates a seal proximal and distal ends • distal end (landing zone) problem with common iliac aneurysms that extend to the bifurcation type I endoleak • pelvic ischemia a concern if internal iliac artery occluded • increasing experience interruption of a single internal iliac artery usually well tolerated • coil occlusion or occluding device in internal iliac artery, ipsilateral graft limb into external iliac artery beyond the bifurcation • Most patients completely asymptomatic, but 25% to 30% temporary ipsilateral buttock claudication • Persistent buttock claudication 10% to 15% • Buttock necrosis, ischemic colitis, spinal cord ischemia, and impotence have all been reported, but are rare complications • bilateral internal iliac artery occlusion has been reported to be well tolerated in some patients, most recommend maintaining flow in at least one internal iliac artery – Internal iliac bypass – Snorkel technique? ?
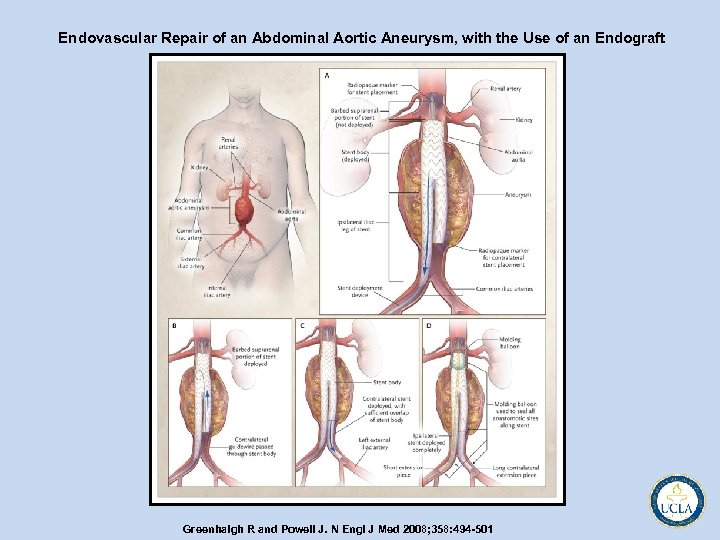
Endovascular Repair of an Abdominal Aortic Aneurysm, with the Use of an Endograft Greenhalgh R and Powell J. N Engl J Med 2008; 358: 494 -501

The 5 Types of Leakage of Blood into the Aneurysm, or Endoleak
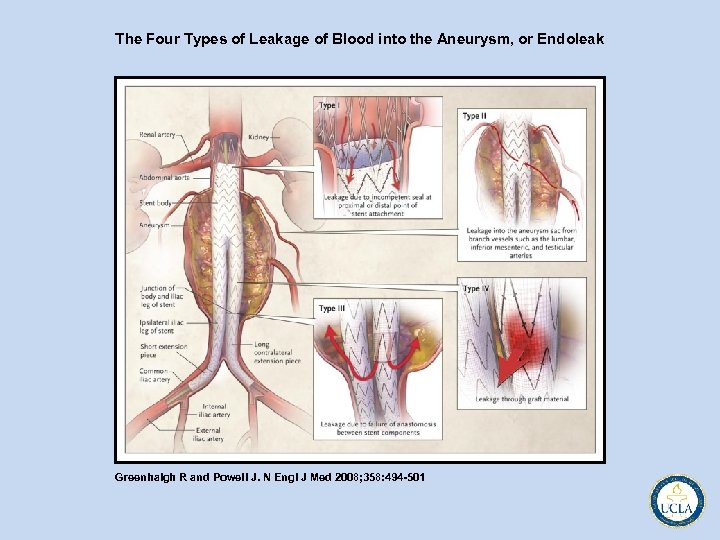
The Four Types of Leakage of Blood into the Aneurysm, or Endoleak Greenhalgh R and Powell J. N Engl J Med 2008; 358: 494 -501

Q 16 • Two days after placement of a brachiocephalic fistula for hemodialysis access, a 53 year old man has extensive edema of the ipsilateral extremity from the hand to the shoulder. Venography confirms a stenosis in the proximal subclavian vein creating an 85% diameter loss. • The best management would be A. B. C. D. E. chronic oral anticoagulation fistula ligation fistula banding near the arterial anastomosis balloon angioplasty of the subclavian vein stenosis subclavian jugular venous bypass

Q 16 • Two days after placement of a brachiocephalic fistula for hemodialysis access, a 53 year old man has extensive edema of the ipsilateral extremity from the hand to the shoulder. Venography confirms a stenosis in the proximal subclavian vein creating an 85% diameter loss. • The best management would be A. B. C. D. E. chronic oral anticoagulation fistula ligation fistula banding near the arterial anastomosis balloon angioplasty of the subclavian vein stenosis subclavian-jugular venous bypass

• Pain and swelling in extremity after placement of an arteriovenous access Q 16 is indicative of venous hypertension • hemodynamically significant stenosis in the central venous system, usually due to previous central venous catheterization • subclavian vein, innominate vein, axillary vein, and superior vena cava • Long term oral anticoagulation will not result in symptomatic improvement • ligating the fistula, but sacrifices a functioning access • External banding will reduce flow in the fistula, but continued venous hypertension is likely • Correction of the venous hypertension requires treatment of the central vein stenosis • endovascular options may be a reasonable alternative, balloon angioplasty of central vein stenoses is associated with early recurrence in most cases – Multiple procedures are often required – long term relief <1/3 patients • Open surgical techniques such as subclavian jugular bypass or jugular turndown (jugular subclavian vein transposition) better option, especially in younger patients with reasonable long term prognosis • Although more invasive, long term patency and symptomatic relief are better than with angioplasty
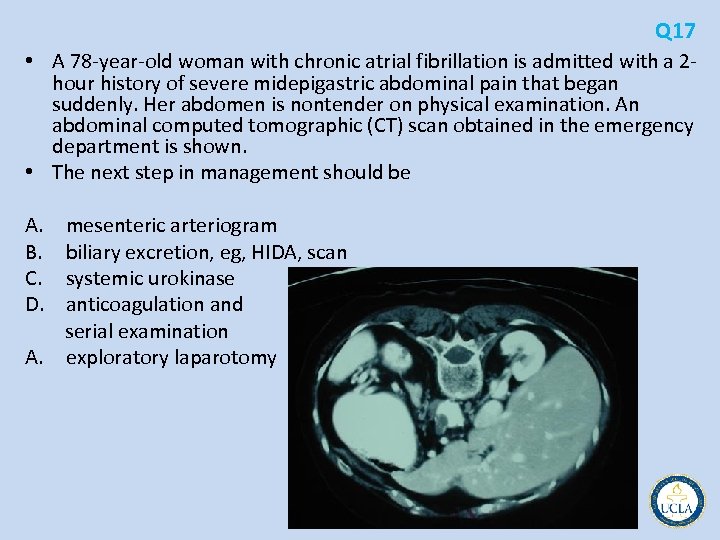
Q 17 • A 78 year old woman with chronic atrial fibrillation is admitted with a 2 hour history of severe midepigastric abdominal pain that began suddenly. Her abdomen is nontender on physical examination. An abdominal computed tomographic (CT) scan obtained in the emergency department is shown. • The next step in management should be A. mesenteric arteriogram B. biliary excretion, eg, HIDA, scan C. systemic urokinase D. anticoagulation and serial examination A. exploratory laparotomy
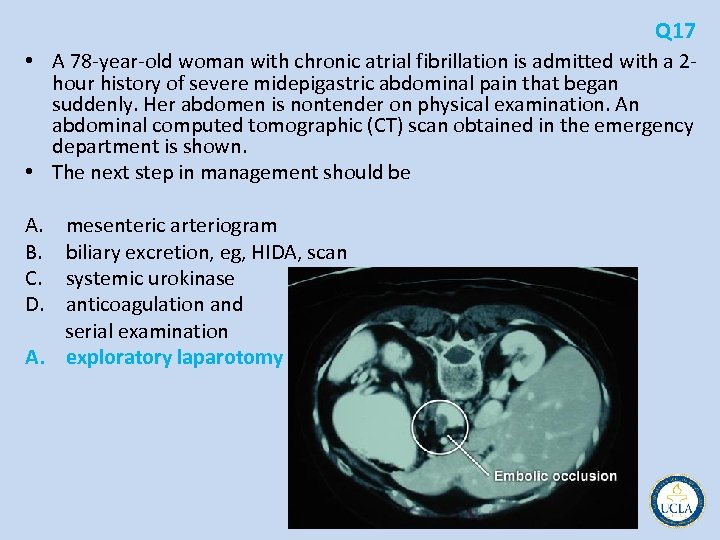
Q 17 • A 78 year old woman with chronic atrial fibrillation is admitted with a 2 hour history of severe midepigastric abdominal pain that began suddenly. Her abdomen is nontender on physical examination. An abdominal computed tomographic (CT) scan obtained in the emergency department is shown. • The next step in management should be A. mesenteric arteriogram B. biliary excretion, eg, HIDA, scan C. systemic urokinase D. anticoagulation and serial examination A. exploratory laparotomy
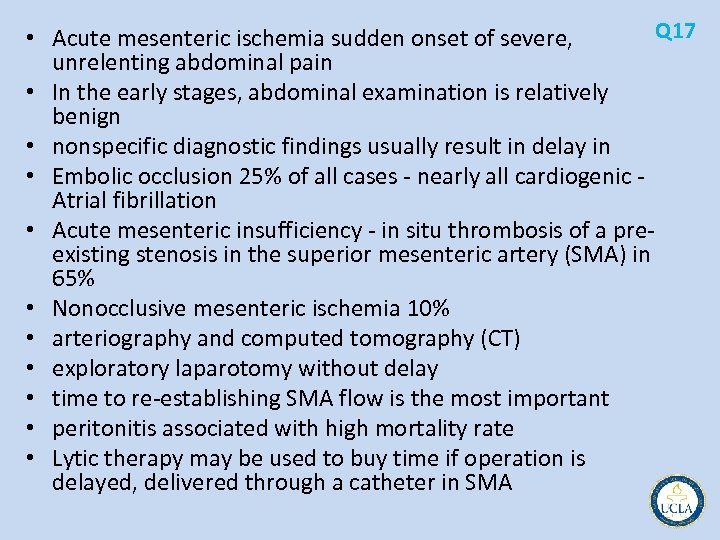
Q 17 • Acute mesenteric ischemia sudden onset of severe, unrelenting abdominal pain • In the early stages, abdominal examination is relatively benign • nonspecific diagnostic findings usually result in delay in • Embolic occlusion 25% of all cases nearly all cardiogenic Atrial fibrillation • Acute mesenteric insufficiency in situ thrombosis of a pre existing stenosis in the superior mesenteric artery (SMA) in 65% • Nonocclusive mesenteric ischemia 10% • arteriography and computed tomography (CT) • exploratory laparotomy without delay • time to re establishing SMA flow is the most important • peritonitis associated with high mortality rate • Lytic therapy may be used to buy time if operation is delayed, delivered through a catheter in SMA

Q 18 • Five days after an uncomplicated right carotid endarterectomy, a 69 year old man arrives in the emergency department after the sudden onset of a severe right sided headache. He is hemodynamically normal and neurologically intact. • The next step in management should be A. B. C. D. E. administration of intravenous heparin carotid duplex ultrasonography cerebral imaging study carotid arteriogram immediate transport to the operating room for carotid re exploration

Q 18 • Five days after an uncomplicated right carotid endarterectomy, a 69 year old man arrives in the emergency department after the sudden onset of a severe right sided headache. He is hemodynamically normal and neurologically intact. • The next step in management should be A. B. C. D. E. administration of intravenous heparin carotid duplex ultrasonography cerebral imaging study carotid arteriogram immediate transport to the operating room for carotid re exploration

• Hyperperfusion syndrome of the brain rare but potentially dangerous Q 18 complication of carotid endarterectomy (CEA) or carotid artery stenting • often heralded by severe ipsilateral headache • progress to seizure activity and cerebral hemorrhage • prevalence after CEA 0. 4% to 7. 7%, depending on the definitions used • Hyperperfusion is believed to represent increased cerebral blood flow in a territory with disturbed autoregulation • Proposed risk factors – correction of a very high grade carotid stenosis (especially when the contralateral carotid artery is occluded) – previous stroke – poor collateral blood supply – uncontrolled hypertension • suspected in any patient with severe ipsilateral headache after CEA/CAS • Imaging to evaluate edema or hemorrhage – CT – hemorrhage – MRI with gadolinium enhancement particularly sensitive for subtle changes associated with hyperperfusion • risk of cerebral hemorrhage, anticoagulants should not be administered, antiplatelet agents should be stopped • Hypertension should be carefully controlled

Q 19 • Compared with open repair, endovascular repair of a 6. 5 cm infrarenal abdominal aortic aneurysm is associated with A. B. C. D. E. reduced 30 day morbidity and mortality longer recovery times due to persistent endoleaks lower incidence of colon ischemia fewer re interventions lower treatment costs

Q 19 • Compared with open repair, endovascular repair of a 6. 5 cm infrarenal abdominal aortic aneurysm is associated with A. B. C. D. E. reduced 30 -day morbidity and mortality longer recovery times due to persistent endoleaks lower incidence of colon ischemia fewer re interventions lower treatment costs

• Three randomized studies, the EVAR, DREAM and OVER trials, compared Q 19 open versus endovascular repair of AAA • EVAR significantly lower morbidity and mortality at 30 days compared with open repair • EVAR (EVAR & DREAM trials) higher number of re interventions to treat graft thromosis or endoleaks – this did not affect the overall recovery rate, faster in the endograft group • OVER same # reinterventions (hernias, bowel obstructions, wound complications) • Ischemic complications 700 endovascular aneurysm repairs, the incidence of colon ischemia was similar to that after open repair. However, small bowel ischemia occurred much more commonly after endografts, and this complication was associated with high mortality • Newer studies show risk of colon ischemia lower with EVAR (4 vs. 1. 4%) • high cost of endografts one of main disadvantages of EVAR • overall higher cost of EVAR compared with open • additional costs of ongoing surveillance to detect graft complications add significantly
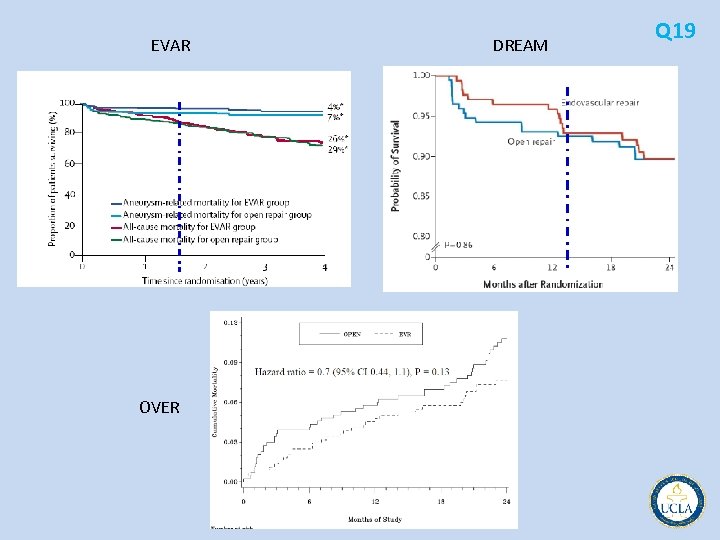
EVAR OVER DREAM Q 19
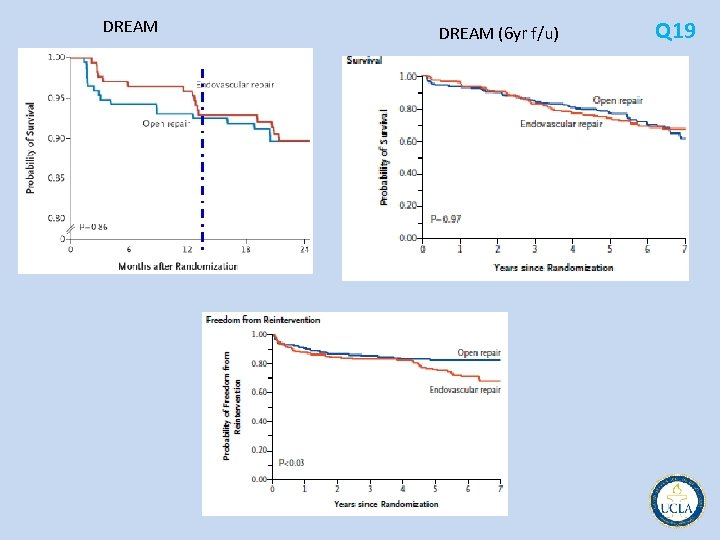
DREAM (6 yr f/u) Q 19

Q 20 • A 42 year old woman presents with a recurrent stasis ulcer on the medial ankle. Venous duplex ultrasonography demonstrates complete valvular incompetence of the ipsilateral saphenous vein. The deep venous system is patent, and the valves are competent at all levels. The ulcer heals after 6 weeks of compression therapy. • The best long term management option is • • • continued compression therapy with a fitted stocking ligation of the saphenofemoral junction and saphenous vein stripping subfascial ligation of perforating veins excision of ulcer scar and split thickness skin graft axillary vein valve transfer

Q 20 • A 42 year old woman presents with a recurrent stasis ulcer on the medial ankle. Venous duplex ultrasonography demonstrates complete valvular incompetence of the ipsilateral saphenous vein. The deep venous system is patent, and the valves are competent at all levels. The ulcer heals after 6 weeks of compression therapy. • The best long term management option is • • • continued compression therapy with a fitted stocking ligation of the saphenofemoral junction and saphenous vein stripping subfascial ligation of perforating veins excision of ulcer scar and split thickness skin graft axillary vein valve transfer

Q 20 • venous stasis ulcers 1% of the adult population, 1/3 unhealed • prolonged venous hypertension from valvular insufficiency in the saphenous venous system, the deep venous system, or both • Subfascial ligation valvular incompetence of the deep or perforating veins • Ligation of the saphenofemoral junction has been associated with ulcer healing, local anesthesia. • saphenous vein stripping is unnecessary to achieve initial ulcer healing, long term recurrence of venous insufficiency is more likely if the saphenofemoral junction is ligated without stripping the vein • Endoluminal saphenous vein ablation using laser or radiofrequency techniques may be an equally good option, but long term results are not yet known • Transfer of an axillary vein segment containing a competent valve deep venous insufficiency

Q 21 • A 53 year old man presents with a 2 day history of pain and swelling in the left leg and thigh. Magnetic resonance venography confirms thrombotic occlusion of the left common and external iliac veins. He is otherwise in good health and has no contraindications to anticoagulation. • This patient should receive A. B. C. D. E. unfractionated heparin only low molecular weight heparin direct thrombin inhibitor catheter directed thrombolysis systemic thrombolysis

Q 21 • A 53 year old man presents with a 2 day history of pain and swelling in the left leg and thigh. Magnetic resonance venography confirms thrombotic occlusion of the left common and external iliac veins. He is otherwise in good health and has no contraindications to anticoagulation. • This patient should receive A. B. C. D. E. unfractionated heparin only low molecular weight heparin direct thrombin inhibitor catheter-directed thrombolysis systemic thrombolysis

• Conventional therapy DVT systemic heparin followed by oral anticoagulation for 3 to 6 months • effective in reducing the risk of pulmonary embolus (PE) and recurrent DVT • iliofemoral DVT at risk for postthrombotic syndrome • incomplete venous recanalization and loss of normal venous valvular function • Surgical thrombectomy often incomplete, and early recurrence of the thrombosis commonplace – rarely performed except in highly symptomatic patients due to phlegmasia Q 21 • Catheter directed lytic therapy introduce the lytic agent directly into the clot (place retrievable IVC filter) • fewer bleeding complications compared with systemic lysis • Multicenter trials overall success rate in over 80% of treated patients, with a major bleeding rate of 11% and a PE rate of 1% • New mechanical endovascular devices have improved the speed and success rate of clot dissolution • Once thrombus has been cleared, oral anticoagulation 6 months • health related quality of life better with lytic therapy better overall physical functioning, less health distress, and fewer postthrombotic symptoms

Q 22 • A 32 year old man presents with chronic left leg pain and edema. Duplex ultrasonography demonstrates continuous flow in the external iliac vein that is suggestive of proximal vein obstruction. Venography demonstrates a stenosis of the left common iliac vein in the area underlying the right common iliac artery. • The most appropriate treatment would be A. immediate administration of heparin, followed by long term anticoagulation B. systemic administration of a lytic agent C. catheter based lytic therapy D. placement of a self expanding stent E. surgical resection of the obstructing lesion

Q 22 • A 32 year old man presents with chronic left leg pain and edema. Duplex ultrasonography demonstrates continuous flow in the external iliac vein that is suggestive of proximal vein obstruction. Venography demonstrates a stenosis of the left common iliac vein in the area underlying the right common iliac artery. • The most appropriate treatment would be A. immediate administration of heparin, followed by long term anticoagulation B. systemic administration of a lytic agent C. catheter based lytic therapy D. placement of a self-expanding stent E. surgical resection of the obstructing lesion

• In humans, the left common iliac vein is crossed anteriorly by the right common iliac artery • chronic compression of the vein by the artery Q 22 – May Thurner syndrome • most cases asymptomatic • risk factor for deep venous thrombosis (DVT) • Patients may present with pain and edema due to venous hypertension before the onset of DVT • Endovascular therapy with metallic stents is effective in relieving the external compression, with 2 year primary patency rates > 90% • catheter directed lysis to treat venous thrombosis before stent placement

Q 23 • Endovascular repair of an abdominal aortic aneurysm has improved outcome over open repair in all of the following EXCEPT A. B. C. D. E. graft complications mortality cardiac complications pulmonary complications length of hospital stay

Q 23 • Endovascular repair of an abdominal aortic aneurysm has improved outcome over open repair in all of the following EXCEPT A. B. C. D. E. graft complications mortality cardiac complications pulmonary complications length of hospital stay

Q 24 • Which of the following statements about arteriovenous fistulas (AVFs) for hemodialysis access in patients with end stage renal disease is TRUE? A. AVFs should be placed immediately after patients have started dialysis B. Over 50% of such patients are being dialyzed through AVFs C. The radiocephalic fistula can be done in over 50% of all patients D. If an AVF fails to mature properly, secondary operations are rarely successful E. For a patient with small vessels, a prosthetic graft will provide a higher patency rate than a radiocephalic fistula

Q 24 • Which of the following statements about arteriovenous fistulas (AVFs) for hemodialysis access in patients with end stage renal disease is TRUE? A. AVFs should be placed immediately after patients have started dialysis B. Over 50% of such patients are being dialyzed through AVFs C. The radiocephalic fistula can be done in over 50% of all patients D. If an AVF fails to mature properly, secondary operations are rarely successful E. For a patient with small vessels, a prosthetic graft will provide a higher patency rate than a radiocephalic fistula

Q 24 • In any given year, some 240, 000 patients with end stage renal disease are being treated with maintenance hemodialysis • Venous catheters last only a few months at most • arteriovenous grafts may last a year or two • arteriovenous fistula (AVF) may last for several years, the best method of access • Center for Medicare and Medicaid Services (CMS) has announced a Fistula First movement, with the objective of placing AVFs in dialysis patients before they begin receiving dialysis. It takes 3 to 4 months for a fistula to mature, and often longer, especially in diabetics, and a revision may be necessary • Achieving a higher rate of first use AVF requires that patients be identified 6 to 12 months prior • The radiocephalic arteriovenous fistula (Brescia Cimino shunt) best • More than half of patients cannot have because vessels too small or because cephalic vein occluded • forearm loop graft with prosthetic material, which has a lower patency rate than a Brescia Cimino shunt, superior in patients with small vessels • In prosthetic grafts, just as with nongraft fistulas, re operation will often salvage a clotted fistula
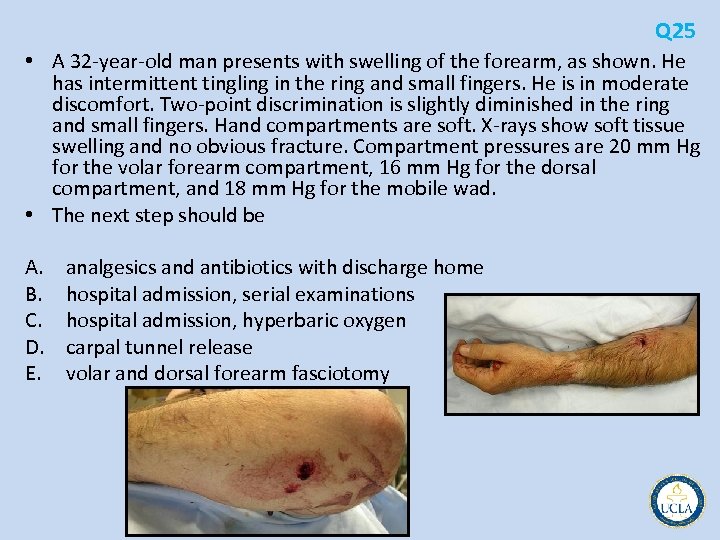
Q 25 • A 32 year old man presents with swelling of the forearm, as shown. He has intermittent tingling in the ring and small fingers. He is in moderate discomfort. Two point discrimination is slightly diminished in the ring and small fingers. Hand compartments are soft. X rays show soft tissue swelling and no obvious fracture. Compartment pressures are 20 mm Hg for the volar forearm compartment, 16 mm Hg for the dorsal compartment, and 18 mm Hg for the mobile wad. • The next step should be A. B. C. D. E. analgesics and antibiotics with discharge home hospital admission, serial examinations hospital admission, hyperbaric oxygen carpal tunnel release volar and dorsal forearm fasciotomy
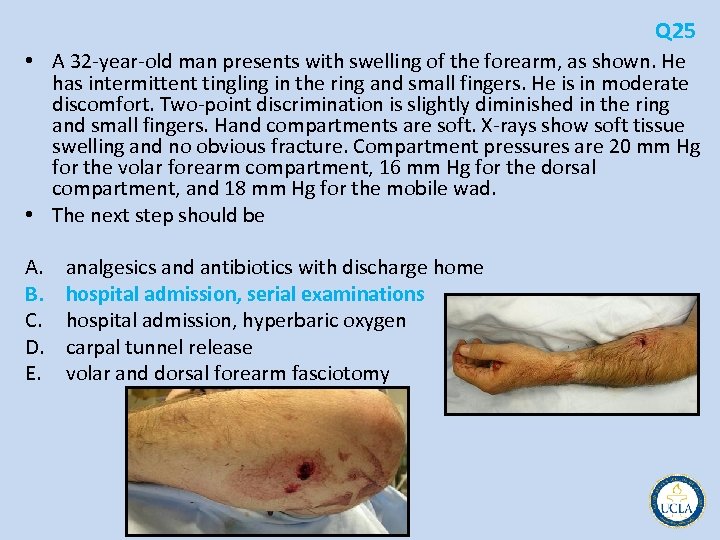
Q 25 • A 32 year old man presents with swelling of the forearm, as shown. He has intermittent tingling in the ring and small fingers. He is in moderate discomfort. Two point discrimination is slightly diminished in the ring and small fingers. Hand compartments are soft. X rays show soft tissue swelling and no obvious fracture. Compartment pressures are 20 mm Hg for the volar forearm compartment, 16 mm Hg for the dorsal compartment, and 18 mm Hg for the mobile wad. • The next step should be A. B. C. D. E. analgesics and antibiotics with discharge home hospital admission, serial examinations hospital admission, hyperbaric oxygen carpal tunnel release volar and dorsal forearm fasciotomy

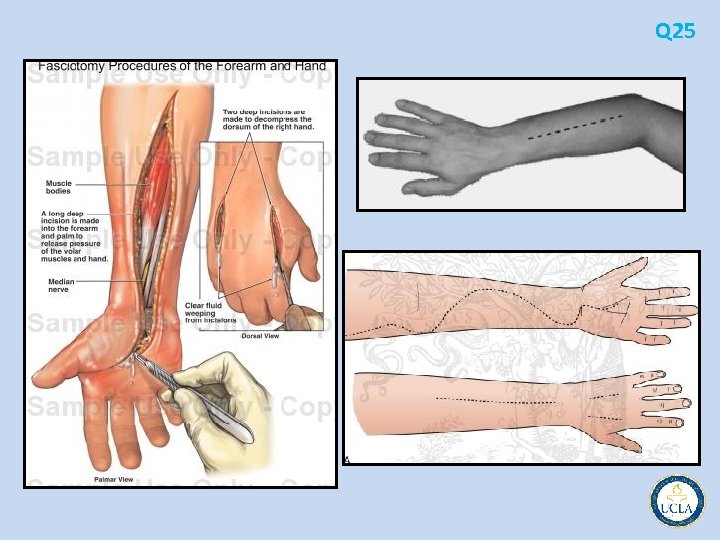
Q 25 • gunshot wound to the forearm • risk for compartment syndrome • may also have injury to the ulnar nerve related to direct injury or compression from local edema or blast injury • documentation of presenting and subsequent neurologic examinations • Sensory deficits (paresthesias or numbness) usually precede motor dysfunction • Muscles and nerves are especially vulnerable to ischemia and incur irreversible damage if increased pressures are maintained • compartment syndrome (pain out of proportion to the injury, pain with passive extension of the compartment muscles, swollen tense compartments) • confirmed by intracompartmental tissue fluid pressures > 30 mm Hg • forearm has three major compartments: – anterior (volar) – posterior (dorsal) – mobile wad (includes brachioradialis, extensor carpi radialis longus, and extensor carpi radialis brevis) – The carpal canal, although open at both ends, is a physiologic compartment and should be released when median nerve compression is identified. • Hyperbaric oxygen is not an acceptable primary treatment for compartment syndrome
Q 25
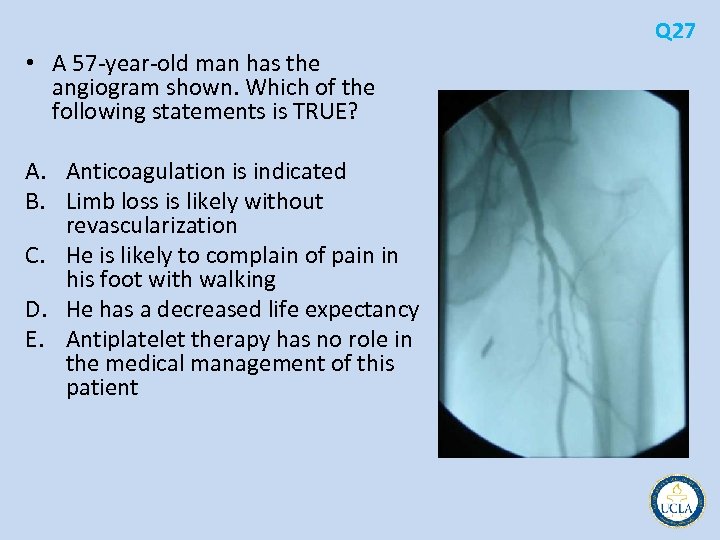
Q 27 • A 57 year old man has the angiogram shown. Which of the following statements is TRUE? A. Anticoagulation is indicated B. Limb loss is likely without revascularization C. He is likely to complain of pain in his foot with walking D. He has a decreased life expectancy E. Antiplatelet therapy has no role in the medical management of this patient
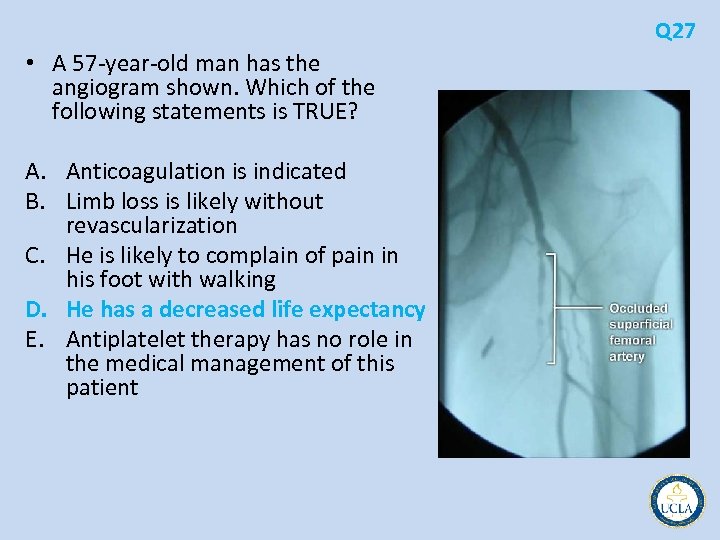
Q 27 • A 57 year old man has the angiogram shown. Which of the following statements is TRUE? A. Anticoagulation is indicated B. Limb loss is likely without revascularization C. He is likely to complain of pain in his foot with walking D. He has a decreased life expectancy E. Antiplatelet therapy has no role in the medical management of this patient

Q 27 • occlusion of the superficial femoral artery • peripheral arterial disease (PAD) • Claudication intermittent nature with occurrence during exercise and abatement with rest • calf, thigh, and buttock • Symptoms occur distal to the stenosis or occlusion as oxygen demand increases with exercise but cannot be supplied • Foot pain with ambulation is not a typical presentation because the amount of muscle in the calf is far greater and usually produces symptoms first • Anticoagulation will not improve walking distance and is not indicated • Revascularization is only required in one third of patients with claudication and limb loss is relatively rare • More ominous, however, is the association of claudication and peripheral arterial disease with stroke and myocardial infarction • Patients with symptomatic peripheral arterial disease have twice the risk of mortality from these atherothrombotic disease processes • Antiplatelet agents are indicated in these patients to reduce cardiovascular mortality and morbidity

Q 28 • Which of the following statements about the findings shown in this computed tomographic (CT) scan is TRUE? A. This is the most common site of aneurysmal disease B. Successful surgical repair eliminates any further enlargement C. Rupture is more likely to occur than thrombosis D. Embolization from the aneurysm is a continuous risk E. There is no role for thrombolytic therapy
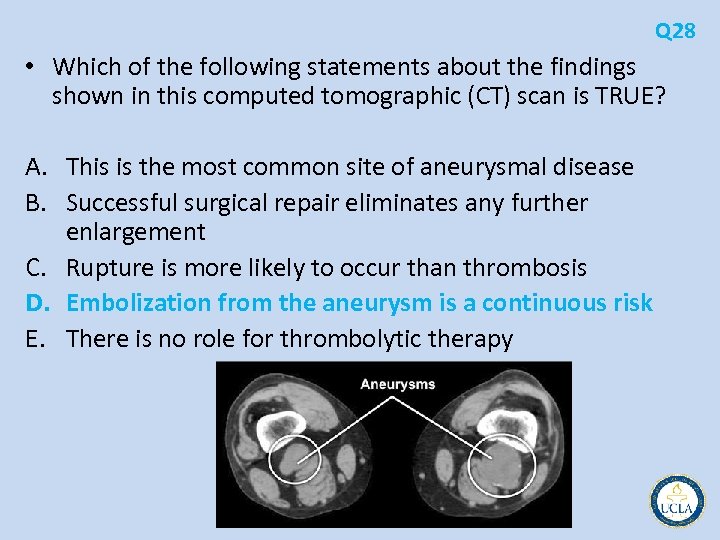
Q 28 • Which of the following statements about the findings shown in this computed tomographic (CT) scan is TRUE? A. This is the most common site of aneurysmal disease B. Successful surgical repair eliminates any further enlargement C. Rupture is more likely to occur than thrombosis D. Embolization from the aneurysm is a continuous risk E. There is no role for thrombolytic therapy

• • • • Q 28 aneurysms of both popliteal arteries (the left is larger than the right) Abdominal aortic aneurysms (AAA) occur more frequently, but aneurysms of the popliteal artery are the most frequently occurring peripheral arterial aneurysms, accounting for more than 70% Unlike AAAs, rupture of an aneurysm in this location is extremely rare Most patients present with symptoms of emoblization (blue toes) or acute limb ischemia Many authors recommend surgical intervention when the aneurysm is diagnosed The risk of developing symptoms is ~14% per year and includes the risk of complete thrombosis. Limb loss in this setting occurs in approximately 30% Planning revascularization is often complicated by the embolization and thrombosis of normal caliber distal vessels that would have been suitable for bypass Thombolytic therapy in this setting to identify patent distal vessels, improve small vessel flow, and improve subsequent bypass patency Surgical intervention requires ligation of the aneurysm and reconstruction with autogenous conduit whenever possible 80% patency at 5 years is commonly reported endovascular exclusion of the aneurysm with in line reconstruction with a covered stent graft Even with ligation of the proximal and distal vessel around the aneurysm, patency of the geniculates resulting in continued aneurysm growth has been reported This complication is best treated with exploration from a posterior incision with ligation of the patent vessels from within the aneurysm sac
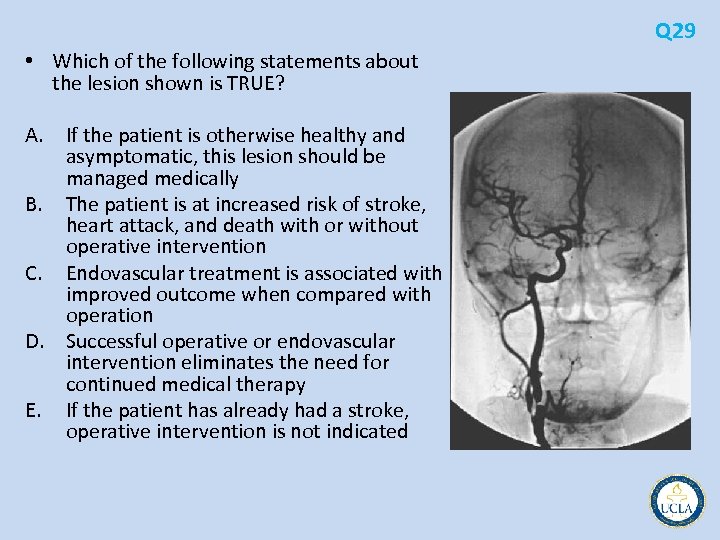
Q 29 • Which of the following statements about the lesion shown is TRUE? A. If the patient is otherwise healthy and asymptomatic, this lesion should be managed medically B. The patient is at increased risk of stroke, heart attack, and death with or without operative intervention C. Endovascular treatment is associated with improved outcome when compared with operation D. Successful operative or endovascular intervention eliminates the need for continued medical therapy E. If the patient has already had a stroke, operative intervention is not indicated
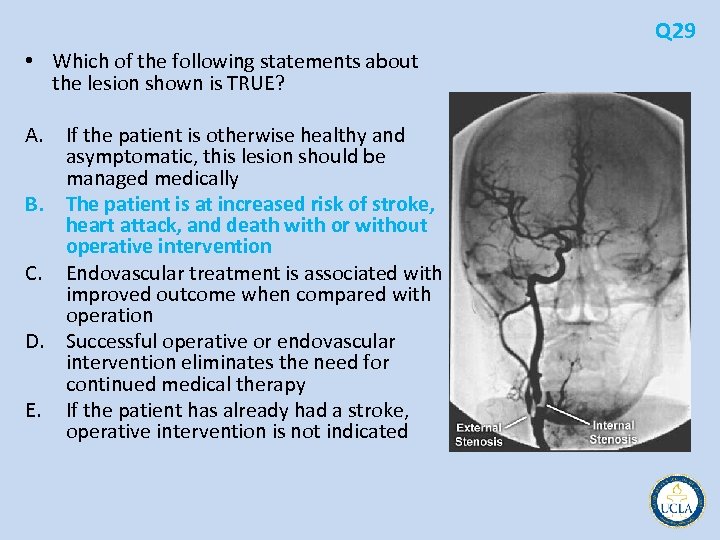
Q 29 • Which of the following statements about the lesion shown is TRUE? A. If the patient is otherwise healthy and asymptomatic, this lesion should be managed medically B. The patient is at increased risk of stroke, heart attack, and death with or without operative intervention C. Endovascular treatment is associated with improved outcome when compared with operation D. Successful operative or endovascular intervention eliminates the need for continued medical therapy E. If the patient has already had a stroke, operative intervention is not indicated

• severe stenosis of the right internal and external carotid artery • patients with atherosclerotic disease of the internal carotid artery are at increased risk of coronary artery disease, heart attack, stroke, and death, regardless of therapy offered Q 29
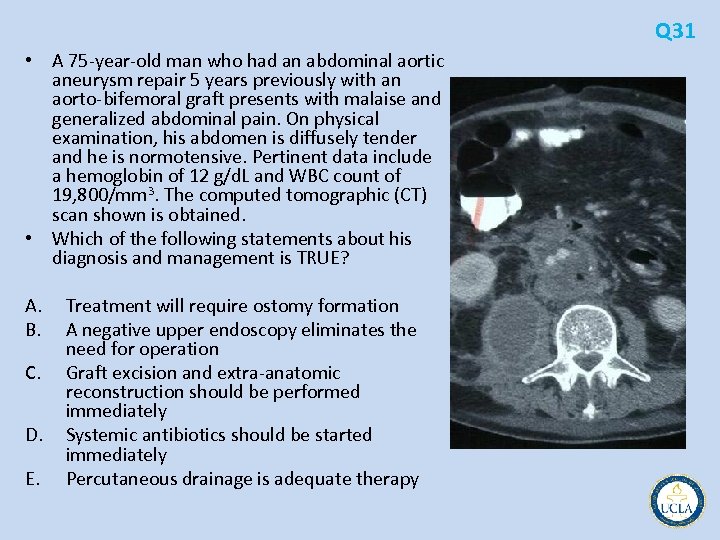
Q 31 • A 75 year old man who had an abdominal aortic aneurysm repair 5 years previously with an aorto bifemoral graft presents with malaise and generalized abdominal pain. On physical examination, his abdomen is diffusely tender and he is normotensive. Pertinent data include a hemoglobin of 12 g/d. L and WBC count of 19, 800/mm 3. The computed tomographic (CT) scan shown is obtained. • Which of the following statements about his diagnosis and management is TRUE? A. B. C. D. E. Treatment will require ostomy formation A negative upper endoscopy eliminates the need for operation Graft excision and extra anatomic reconstruction should be performed immediately Systemic antibiotics should be started immediately Percutaneous drainage is adequate therapy
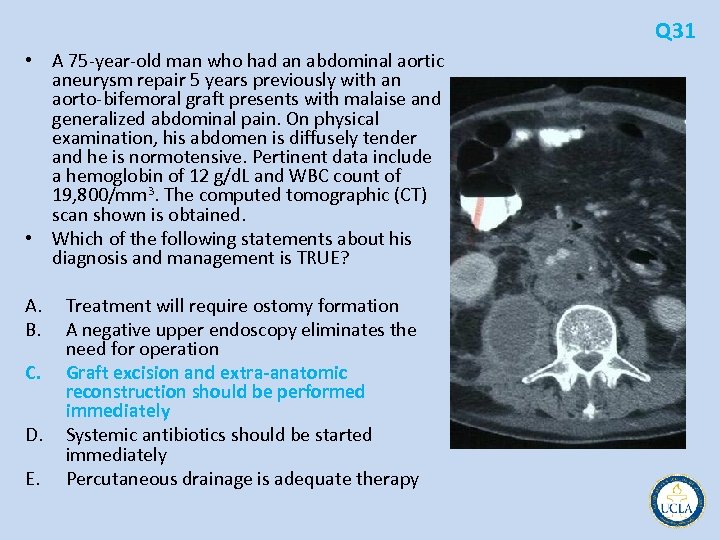
Q 31 • A 75 year old man who had an abdominal aortic aneurysm repair 5 years previously with an aorto bifemoral graft presents with malaise and generalized abdominal pain. On physical examination, his abdomen is diffusely tender and he is normotensive. Pertinent data include a hemoglobin of 12 g/d. L and WBC count of 19, 800/mm 3. The computed tomographic (CT) scan shown is obtained. • Which of the following statements about his diagnosis and management is TRUE? A. B. C. D. E. Treatment will require ostomy formation A negative upper endoscopy eliminates the need for operation Graft excision and extra-anatomic reconstruction should be performed immediately Systemic antibiotics should be started immediately Percutaneous drainage is adequate therapy

• • • • Q 31 Prosthetic graft infections most dreaded complicatios after aortic reconstruction, 1% to 6% of cases generalized malaise, fever, leukocytosis with melena, and hematemesis if the graft has eroded into the adjacent bowe CT findings: perigraft air or fluid, soft tissue attenuation between the graft and the aortic wall after the immediate perioperative period Aortoenteric fistulas most frequently occur at the site of the proximal anastomosis of the graft to the aorta and involve third portion of the duodenum Upper endoscopy may confirm this diagnosis, but might dislodge an already tenuous clot within the lumen of the bowel best performed in the operating room Small bowel fistulas in this setting may be closed primarily and excluded from the site of aortic repair with a wrap of omentum or well vascularized soft tissue complete graft excision with aggressive retroperitoneal debridement and extra anatomic reconstruction has been recommended Mortality rates remain at 30% in the immediate postoperative period For normotensive patients who are not actively bleeding, a radionuclide labeled WBC scan may provide additional useful information, such as whether the graft in the region of the groins is also infected staged procedures Extra anatomic bypass may be performed first after appropriate antibiotics have been administered and the patient's condition has stabilized, followed by laparotomy and excision of all infected graft material improved patient survival survivors remain at risk for aortic stump blowout, thrombosis of the extra anatomoic bypass, and amputation of the extremities Most of these infections develop 5 or more years after initial operation and are from fastidious organisms such as Staphylococcus epidermidis low virulence of these organisms has led many to suggest that long term antibiotics in conjunction with aggressive debridement with in situ reconstruction may be possible antibiotic impregnated grafts, arterial homografts, and autogenous vein grafts harvested from the patient's own deep femoral system of veins
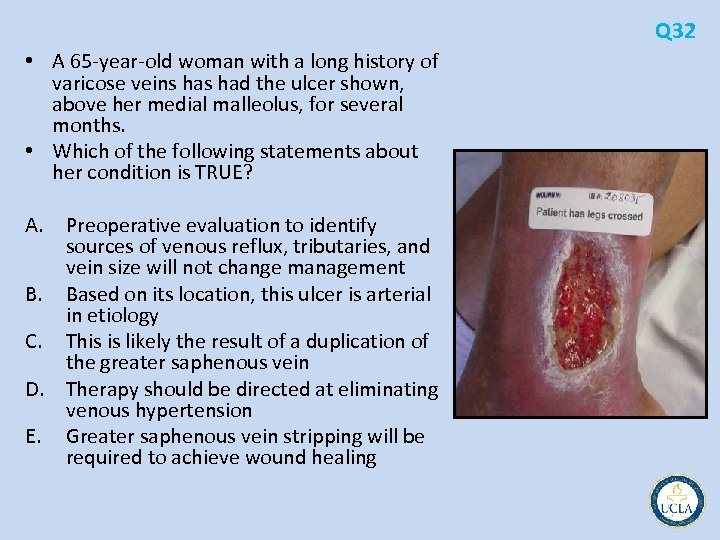
Q 32 • A 65 year old woman with a long history of varicose veins had the ulcer shown, above her medial malleolus, for several months. • Which of the following statements about her condition is TRUE? A. Preoperative evaluation to identify sources of venous reflux, tributaries, and vein size will not change management B. Based on its location, this ulcer is arterial in etiology C. This is likely the result of a duplication of the greater saphenous vein D. Therapy should be directed at eliminating venous hypertension E. Greater saphenous vein stripping will be required to achieve wound healing
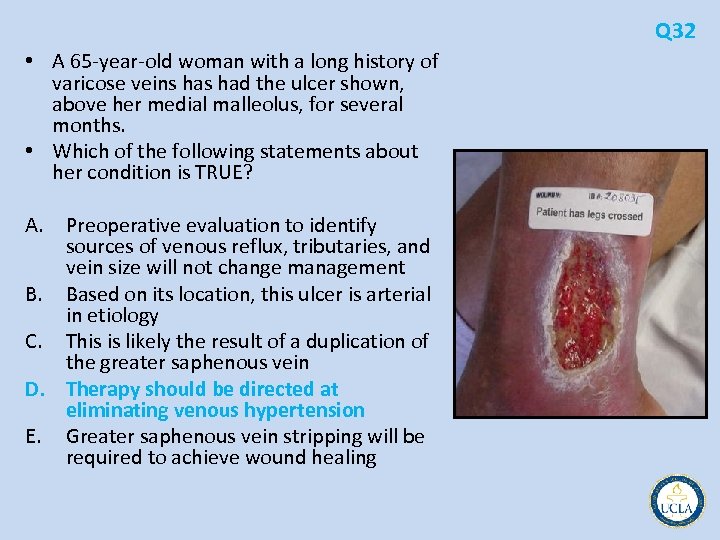
Q 32 • A 65 year old woman with a long history of varicose veins had the ulcer shown, above her medial malleolus, for several months. • Which of the following statements about her condition is TRUE? A. Preoperative evaluation to identify sources of venous reflux, tributaries, and vein size will not change management B. Based on its location, this ulcer is arterial in etiology C. This is likely the result of a duplication of the greater saphenous vein D. Therapy should be directed at eliminating venous hypertension E. Greater saphenous vein stripping will be required to achieve wound healing

Q 32 • Conservative measures to reduce venous hypertension • compression dressings, such as an Unna boot or Profore dressing • rule out deep venous thrombosis • saphenofemoral junction can be evaluated for the presence of reflux • Elimination of the proximal segment and its tributaries may be all that is required to alleviate venous hypertension and promote wound healing • Reflux along the entire length of the greater saphenous vein remains an indication for complete excision or ablation

P 3 Compartments of the Lower Leg Compartment Muscles Neurovascular structures Anterior compartment Tibialis anterior, Extensor hallucis longus, Extensor deep peroneal nerve digitorum longus, Peroneus Anterior Tibial vessels (AT) tertius Lateral compartment Peroneus longus, Peroneus superficial peroneal nerve brevis Deep posterior compartment Tibialis posterior, Flexor tibial nerve hallucis longus, Flexor posterior tibial vessels (PT) digitorum longus, Popliteus peroneal artery (peroneal) Superficial posterior compartment Gastrocnemius, Soleus, Plantaris medial sural cutaneous nerve

Q 33 • Which of the following statements about common iliac artery aneurysms is TRUE? A. B. C. D. E. Surgical repair is not recommended until it is 5 cm Endovascular repair is not recommended They are usually infectious in etiology They frequently rupture when < 3 cm They are most often associated with other aneurysms

Q 33 • Which of the following statements about common iliac artery aneurysms is TRUE? A. B. C. D. E. Surgical repair is not recommended until it is 5 cm Endovascular repair is not recommended They are usually infectious in etiology They frequently rupture when < 3 cm They are most often associated with other aneurysms

• Isolated common iliac artery aneurysms occur in only 0. 1% to 1. 9% Q 33 of all patients with aneurysmal disease • atypical causes such as infection, trauma, medial necrosis, fibrodysplasia, cystic necrosis, Marfan's, or nonspecific inflammatory conditions • liac artery aneurysms are found in 10% to 20% of patients with AAA • difficulty in palpating these aneurysms and their asymptomatic nature, rupture and mortality rates are high • one retrospectively reviewed series, no significant rate of expansion was seen over 4 years in aneurysms < 3 cm, and no deaths were attributable to aneurysmal disease. Currently, repair is not recommended for aneurysms < 3 cm • Endovascular treatment options both in conjunction with AAA repair individually • covered stent and endovascular coiling of an internal iliac artery if a sufficient seal zone of 1. 5 cm cannot be obtained proximal to its origin to decrease flow to the aneurysm sac • Preservation of the contralateral internal iliac flow and collaterals is important to preserve flow to the pelvis

Q 34 • Development of the lower extremity postthrombotic syndrome (stasis, edema, pigmentation, ulceration) A. is most likely in patients with multi segment thrombosis B. is effectively prevented by a 6 month course of low molecular weight heparin C. occurs in 15% to 20% of all patients with deep vein thrombophlebitis D. is uncommon after isolated calf vein thrombophlebitis E. is due entirely to valvular insufficiency

Q 34 • Development of the lower extremity postthrombotic syndrome (stasis, edema, pigmentation, ulceration) A. is most likely in patients with multi-segment thrombosis B. is effectively prevented by a 6 month course of low molecular weight heparin C. occurs in 15% to 20% of all patients with deep vein thrombophlebitis D. is uncommon after isolated calf vein thrombophlebitis E. is due entirely to valvular insufficiency

• The postthrombotic syndrome is a highly morbid late Q 34 complication of deep vein thrombophlebitis (DVT) of the lower extremities • Within 5 years of the sentinel episode, 40% to 60% of patients will develop clinically significant signs and symptoms of the syndrome chronic leg edema and pain, dermatitis, and ulceration • The most common inciting factor is a recurrent episode of DVT after resolution of the initial insult • Obesity and inherited coagulopathies also place patients at greater risk • valvular damage is permanent and venous reflux • Permanent obstruction of one or more venous segments, resulting in outflow obstruction and venous hypertension • ineffective calf muscular pump function
Q 35 • A 77 year old woman presents with a cold left hand. After operative embolectomy, the next step in this patient's evaluation should be A. magnetic resonance angiogram of the subclavian arteries B. duplex examination of the carotid arteries C. echocardiogram D. cardiac catheterization E. Adson's maneuver

Q 35 • A 77 year old woman presents with a cold left hand. After operative embolectomy, the next step in this patient's evaluation should be A. magnetic resonance angiogram of the subclavian arteries B. duplex examination of the carotid arteries C. echocardiogram D. cardiac catheterization E. Adson's maneuver

• Acute extremity ischemia can be caused by either thrombosis or embolism • Distinguishing between the two is often difficult • history of acute onset that can be pinpointed exactly in time is more consistent with an embolic phenomenon • Peripheral emboli most commonly arise from the heart – valvular heart disease or atrial arrhythmia Q 35 • aneurysms of the upper extremity arteries with subsequent mural thrombus and embolism, embolism from an aortic plaque, or embolism associated with arterial instrumentation • Echocardiography search for valvular abnormalities, thrombosis in any of the cardiac chambers, and search for septal defects • Magnetic resonance angiography (MRA) of the subclavian arteries would be indicated if echocardiography is negative, duplex better initial screening test

Q 36 • Three days after knee arthroscopy, a 35 year old man presents with mild dyspnea on exertion. His temperature is 100ºF. His chest is clear to auscultation, except for right lower lobe rales. Minimal knee swelling is noted at the arthroscopy site. His WBC count is 12, 400/mm 3 and D dimer level is normal. The chest x ray shows obscuring of the right hemidiaphragm. • The next diagnostic test should be A. B. C. D. E. bilateral lower extremity duplex examination contrast venography ventilation/perfusion scan computed tomographic (CT) angiography sputum culture

Q 36 • Three days after knee arthroscopy, a 35 year old man presents with mild dyspnea on exertion. His temperature is 100ºF. His chest is clear to auscultation, except for right lower lobe rales. Minimal knee swelling is noted at the arthroscopy site. His WBC count is 12, 400/mm 3 and D dimer level is normal. The chest x ray shows obscuring of the right hemidiaphragm. • The next diagnostic test should be A. B. C. D. E. bilateral lower extremity duplex examination contrast venography ventilation/perfusion scan computed tomographic (CT) angiography sputum culture

Q 36 • Whenever a patient presents with respiratory symptoms after an operation, deep venous thrombosis (DVT) and subsequent pulmonary embolus must be among the differential diagnoses • DVT in only 20% to 35% • diagnostic tests are time consuming, costly, or have a finite complication rate • Serum D dimer is a rapid and simple screening test that may be used to eliminate up to 80% of patients without venous thromboembolism (VTE) • D dimer is a degradation product of cross linked fibrin • Although levels are elevated during any thromboembolic event, many nonthrombotic events, including operation, may cause transient elevations in D dimer • For this reason, documentation of suspected VTE under such circumstances requires additional diagnostic work up • D dimer has a negative predictive value of 96% to 100% • When combined with a low clinical suspicion in a patient with a likely alternative diagnosis, the negative predictive values approach 98% to 99% • For this patient with a presumptive diagnosis of pneumonia and a normal D dimer level, significant VTE is virtually excluded, making any further diagnostic test unnecessary

Q 37 • Following a routine knee arthroscopy, a healthy 33 year old man develops an uncomplicated femoral deep venous thrombosis. A hypercoagulable evaluation is negative. Anticoagulation should be given A. B. C. D. E. for 6 weeks for 3 months for 1 year until symptoms resolve for life

Q 37 • Following a routine knee arthroscopy, a healthy 33 year old man develops an uncomplicated femoral deep venous thrombosis. A hypercoagulable evaluation is negative. Anticoagulation should be given A. B. C. D. E. for 6 weeks for 3 months for 1 year until symptoms resolve for life

• The optimal duration of oral anticoagulation for an uncomplicated Q 37 deep venous thrombosis (DVT) has long been debated • Traditional teaching 3 to 6 month • complication rate with warfarin (Coumadin) • DVT isolated to the calf without proximal extension or pulmonary embolism, 6 weeks of treatment might be sufficient • The American College of Chest Physicians Consensus Statement recommends 3 months of treatment for a first time DVT episode with a known transient, reversible risk factor, as in this patient • Longer periods of treatment (6 months to 1 year) are recommended for patients with permanent risk factors (obesity, varicosity, heart failure, immobile status, malignancy, and known thrombophilia) or idiopathic thrombosis (no known risk factors) • Many patients in the latter group may have an undiagnosed hypercoagulable state with estimates ranging from as little as 1% to as high as 30% of patients presenting with DVT • A number of thrombophilic conditions have been identified: Anticardiolipin antibody syndrome, antithrombin III deficiency, protein C and S levels deficiency, and factor V Leiden are the most common

Q 37

P 4 Embolism vs. Thrombosis

Q 41 • Nonoperative management is MOST appropriate for A. a 6 cm pseudoaneurysm of the common femoral artery after cardiac catheterization B. intimal flap in the popliteal artery after posterior knee dislocation that is not flow limiting C. pulsatile bleeding from a stab wound to the thigh in a hemodynamically stable patient D. large traumatic arteriovenous fistula between the superficial femoral artery and vein from a low velocity gunshot wound E. cool, pulseless foot after external fixation of a femur fracture

Q 41 • Nonoperative management is MOST appropriate for A. a 6 cm pseudoaneurysm of the common femoral artery after cardiac catheterization B. intimal flap in the popliteal artery after posterior knee dislocation that is not flow-limiting C. pulsatile bleeding from a stab wound to the thigh in a hemodynamically stable patient D. large traumatic arteriovenous fistula between the superficial femoral artery and vein from a low velocity gunshot wound E. cool, pulseless foot after external fixation of a femur fracture
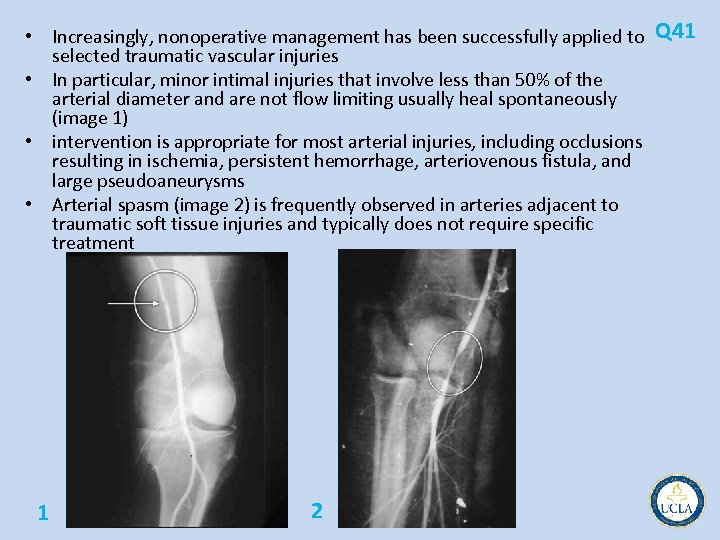
• Increasingly, nonoperative management has been successfully applied to Q 41 selected traumatic vascular injuries • In particular, minor intimal injuries that involve less than 50% of the arterial diameter and are not flow limiting usually heal spontaneously (image 1) • intervention is appropriate for most arterial injuries, including occlusions resulting in ischemia, persistent hemorrhage, arteriovenous fistula, and large pseudoaneurysms • Arterial spasm (image 2) is frequently observed in arteries adjacent to traumatic soft tissue injuries and typically does not require specific treatment 1 2
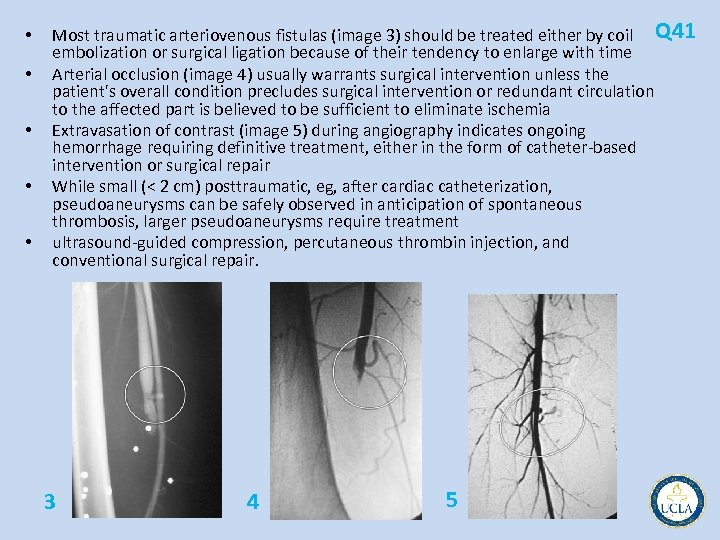
• • • Most traumatic arteriovenous fistulas (image 3) should be treated either by coil Q 41 embolization or surgical ligation because of their tendency to enlarge with time Arterial occlusion (image 4) usually warrants surgical intervention unless the patient's overall condition precludes surgical intervention or redundant circulation to the affected part is believed to be sufficient to eliminate ischemia Extravasation of contrast (image 5) during angiography indicates ongoing hemorrhage requiring definitive treatment, either in the form of catheter based intervention or surgical repair While small (< 2 cm) posttraumatic, eg, after cardiac catheterization, pseudoaneurysms can be safely observed in anticipation of spontaneous thrombosis, larger pseudoaneurysms require treatment ultrasound guided compression, percutaneous thrombin injection, and conventional surgical repair. 3 4 5
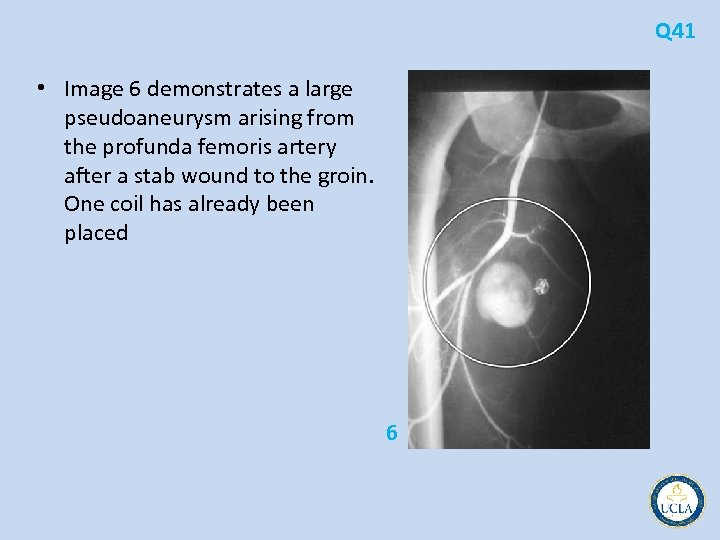
Q 41 • Image 6 demonstrates a large pseudoaneurysm arising from the profunda femoris artery after a stab wound to the groin. One coil has already been placed 6

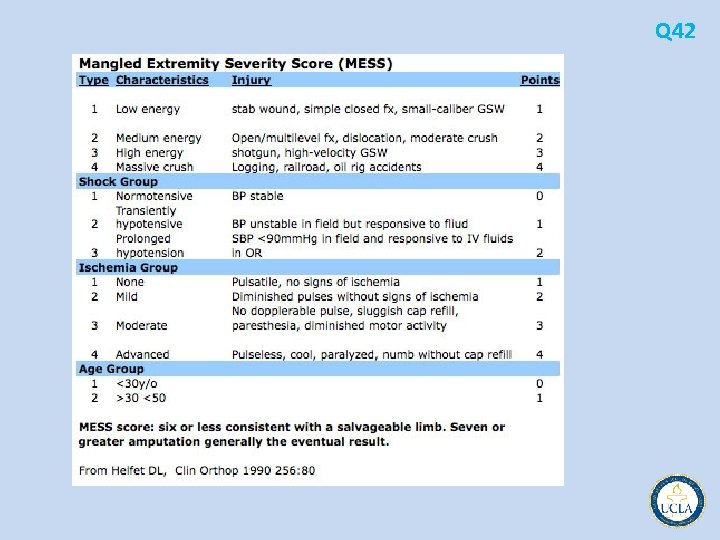
Q 42 • • A. B. C. D. E. A 40 year old male unrestrained driver is brought to the emergency department after being ejected from his car during a motor vehicle crash. . Four hours after injury, he is in class IV hemorrhagic shock with a Glasgow coma scale score of 14. Core temperature is 34°C, and he has a base deficit of 18. After primary and secondary survey, his only injury is an isolated severely comminuted open distal femur fracture Focused assessment with sonography for trauma (FAST) is negative, but he has active bleeding from a crush injury to the mid thigh. The patient is taken to the operating room for ongoing arterial and venous bleeding from his thigh wound. Despite ongoing massive resuscitation, he remains in shock and is hypothermic (temperature < 34°C), acidotic (p. H < 7. 20), and coagulopathic (INR > 1. 5). The most appropriate choice in management now would be above knee amputation of the right lower extremity angiography of the right lower extremity followed by external fixation of the right tibia and femur right below knee amputation with exploration of the femoral vessels and repair followed by external fixation of both femurs immediate ligation of the superficial femoral artery followed by external fixation of the fractures application of a tourniquet to the right thigh and delayed vascular reconstruction

Q 42 • • A. B. C. D. E. A 40 year old male unrestrained driver is brought to the emergency department after being ejected from his car during a motor vehicle crash. . Four hours after injury, he is in class IV hemorrhagic shock with a Glasgow coma scale score of 14. Core temperature is 34°C, and he has a base deficit of 18. After primary and secondary survey, his only injury is an isolated severely comminuted open distal femur fracture Focused assessment with sonography for trauma (FAST) is negative, but he has active bleeding from a crush injury to the mid thigh. The patient is taken to the operating room for ongoing arterial and venous bleeding from his thigh wound. Despite ongoing massive resuscitation, he remains in shock and is hypothermic (temperature < 34°C), acidotic (p. H < 7. 20), and coagulopathic (INR > 1. 5). The most appropriate choice in management now would be above-knee amputation of the right lower extremity angiography of the right lower extremity followed by external fixation of the right tibia and femur right below knee amputation with exploration of the femoral vessels and repair followed by external fixation of both femurs immediate ligation of the superficial femoral artery followed by external fixation of the fractures application of a tourniquet to the right thigh and delayed vascular reconstruction

• likelihood of achieving a functional limb versus the problems Q 42 associated with limb salvage (time involved, duration of disability, medical risks, socioeconomic costs, number of operations and hospitalizations, etc) • The absolute indication for amputation in trauma remains an ischemic limb with unreconstructable vascular injury in a patient with hypothermia, metabolic acidosis, and coagulopathy • Massively crushed muscle and ischemic tissue can release myoglobin and cytokines, leading to a systemic inflammatory response syndrome, resulting in renal failure, adult respiratory distress syndrome, and even death • Prolonged attempts at limb salvage, even though technically possible, may endanger the patient's life and generally should be avoided
Q 42
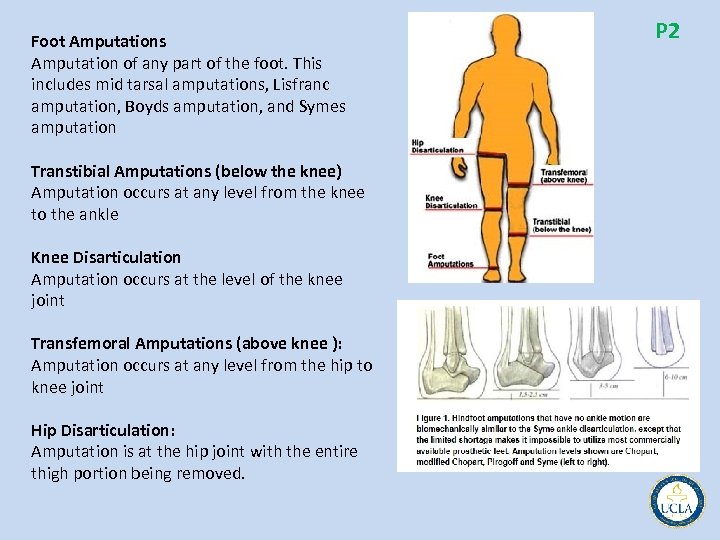
Foot Amputations Amputation of any part of the foot. This includes mid tarsal amputations, Lisfranc amputation, Boyds amputation, and Symes amputation Transtibial Amputations (below the knee) Amputation occurs at any level from the knee to the ankle Knee Disarticulation Amputation occurs at the level of the knee joint Transfemoral Amputations (above knee ): Amputation occurs at any level from the hip to knee joint Hip Disarticulation: Amputation is at the hip joint with the entire thigh portion being removed. P 2

Q 44 • A 27 year old woman sustains a blunt carotid injury. Carotid angiography demonstrates a carotid dissection beginning in the bulb and extending to the petrous portion. A small residual lumen is present. • The optimal treatment would be A. carotid artery stent placement B. systemic anticoagulation with unfractionated heparin C. carotid exploration D. external carotid internal carotid (ECIC) bypass E. low molecular weight heparin (30 mg/kg/day)

Q 44 • A 27 year old woman sustains a blunt carotid injury. Carotid angiography demonstrates a carotid dissection beginning in the bulb and extending to the petrous portion. A small residual lumen is present. • The optimal treatment would be A. carotid artery stent placement B. systemic anticoagulation with unfractionated heparin C. carotid exploration D. external carotid internal carotid (ECIC) bypass E. low molecular weight heparin (30 mg/kg/day)

• • • • Blunt carotid artery injuries are potentially devastating injuries due to neurologic complications Early detection and treatment remain the goals of management hyperextension/rotation injuries sustained in high impact motor vehicle crashes much smaller percentage are caused by a direct blow to the neck Five different mechanisms for the development of traumatic carotid artery: – direct trauma to the artery – hyperextension rotation of the head with stretching of supra aortic vessels – blunt intra oral trauma – basal skull or mandibular fractures – combined chest head injuries with carotid stretching most common mechanism is a direct blow to the head with hyperextension rotation of the neck, which causes stretching of the internal carotid artery over the transverse processes of the first and second cervical vertebrae Carotid artery dissection typically causes headache or neck ache, followed after hours to days by focal motor or sensory deficits carotid four vessel angiography remains the gold standard, CTA now Treatment options: observation, antithrombotic therapy, open surgical repair of the affected carotid artery, and endovascular carotid artery treatment mainstay systemic anticoagulation with intravenous unfractionated heparin, which has been shown to prevent progression of injury to a higher injury grade, to reduce the number of strokes, and to prevent neurologic deterioration Deteriorating or fluctuating neurologic symptoms might be an indication for surgical or endovascular intervention ECIC bypass is a surgical treatment option that is not indicated in this case. Overall mortality resulting from posttraumatic carotid artery dissection varies from 5% to 40% with neurologic morbidity from 12% to 80%, with bilateral lesions being the most severe Q 44

Q 45 • A 53 year old woman undergoes coronary artery bypass grafting and mitral valve replacement with a St. Jude mechanical prosthesis. Warfarin (Coumadin) therapy is initiated postoperatively, but on postoperative day 5 she has the acute onset of right calf pain, swelling, and tenderness. Duplex scanning demonstrates acute deep venous thrombosis of the right femoral popiliteal veins. Intravenous unfractionated heparin therapy is begun. • On postoperative day 9, she has the acute onset of shortness of breath, hypoxemia, and chest pain. Computed tomographic (CT) angiography demonstrates multiple, bilateral pulmonary emboli. In addition, her platelet count has fallen to 50, 000. Definitive management of this problem should be A. B. C. D. E. discontinuing unfractionated heparin and beginning low molecular weight heparin discontinuing unfractionated heparin and beginning argatroban continuing unfractionated heparin and placing an inferior vena cava filter continuing unfractionated heparin and immediate platelet transfusion

Q 45 • A 53 year old woman undergoes coronary artery bypass grafting and mitral valve replacement with a St. Jude mechanical prosthesis. Warfarin (Coumadin) therapy is initiated postoperatively, but on postoperative day 5 she has the acute onset of right calf pain, swelling, and tenderness. Duplex scanning demonstrates acute deep venous thrombosis of the right femoral popiliteal veins. Intravenous unfractionated heparin therapy is begun. • On postoperative day 9, she has the acute onset of shortness of breath, hypoxemia, and chest pain. Computed tomographic (CT) angiography demonstrates multiple, bilateral pulmonary emboli. In addition, her platelet count has fallen to 50, 000. Definitive management of this problem should be A. B. C. D. E. discontinuing unfractionated heparin and beginning low molecular weight heparin discontinuing unfractionated heparin and beginning argatroban continuing unfractionated heparin and placing an inferior vena cava filter continuing unfractionated heparin and immediate platelet transfusion

• • • • Q 45 heparin induced thrombocytopenia (HIT) potentially catastrophic generalized thrombotic disorder triggered by heparin therapy begins 4 to 14 days after initiation of therapy with intravenous unfractionated heparin, although it can be associated with any type of heparin, given at any dose and by any route risk of developing HIT is 2% to 5% diagnosis should be suspected whenever the platelet count < 150, 000, or decreased 50% or more from baseline Thrombotic complications are responsible for the severe morbidity and mortality associated with HIT ½ 2/3 of patients with HIT may have thromboembolic complications HIT has two major subtypes Type 1 is associated with a mild thrombocytopenia, usually occurs within 4 days of starting therapy, is not immune mediated, appears to be caused by a direct agglutinating effect of heparin on platelets, is not associated with thrombosis, and resolves despite the continuation of heparin therapy HIT type 2 is associated with severe thrombocytopenia and/or a significant fall in the baseline platelet count, usually occurring 4 to 14 days after heparin therapy is initiated. It is immune mediated and may be associated with both venous and arterial thrombosis. Type 2 HIT is generally associated with intravenous infusion of unfractionated heparin, but has also been reported with subcutaneous low dose heparin, heparin flushes, heparin coated catheters, and low molecular weight heparins (LMWH) immediate discontinuation of unfractionated Start direct thrombin inhibitor such as argatroban, bivalirudin, or lepirudin inhibit the formation of fibrin bound thrombin, preventing thrombus extension and growth. Platelet transfusion is contraindicated because it can promote thrombosis in the setting of HIT

Q 46 • Blocks glycoprotein IIb/IIIa receptor A. B. C. D. E. Aspirin Clopidogrel (Plavix) Abciximab (Reopro) Cilostazol (Pletal) Ibuprofen

Q 46 • Blocks glycoprotein IIb/IIIa receptor A. B. C. D. E. Aspirin Clopidogrel (Plavix) Abciximab (Reopro) Cilostazol (Pletal) Ibuprofen

Aspirin • relatively weak antiplatelet agent blocks conversion of arachidonic acid to thromboxane by permanently inactivating the cyclo oxygenase activity of the prostaglandin synthase 1 (COX 1) and prostaglandin synthase 2 (COX 2) • effect lasts for the lifetime of the platelet • cessation of aspirin 5 days before operation Clopidogrel (Plavix) and ticlopidine (Ticlid) • thienopyridenes with strong platelet inhibitory properties • selectively inhibit ADP receptor mediated platelet aggregation • ticlopidine can cause thrombocytopenic purpura and neutropenia • clopidogrel should be discontinued at least 5 to 7 days before elective operations • If an emergency operation is required sooner, then platelet transfusions may be required Abciximab (Reopro) • inhibit the platelet glycoprotein IIb/IIIa receptor • These drugs represent the most potent and expensive antiplatelet agents • used in patients at high risk for adverse coronary events • Bleeding complications are significantly increased, and severe thrombocytopenia occurs in 1% to 2% of patient. • The antiplatelet effects usually disappear within 12 hours Cilostazol (Pletal) • reversible phosphodiesterase III inhibitor that allows for increased availability of c. AMP, leading to vasodilation and platelet inhibition • used to improve walking distance in patients with intermittent claudication • relatively weak inhibitor of platelet aggregation, and co administration with aspirin or warfarin does not lead to significant changes in coagulation parameters • bleeding is a reported side effect, so discontinue at least 5 to 7 days before elective operation Nonsteriodal anti inflammatory drugs (NSAIDs) • inhibit thromboxane dependent platelet function by reversibly inhibiting COX 1 • All platelet effects are reversed within 24 hours of drug cessation Q 46
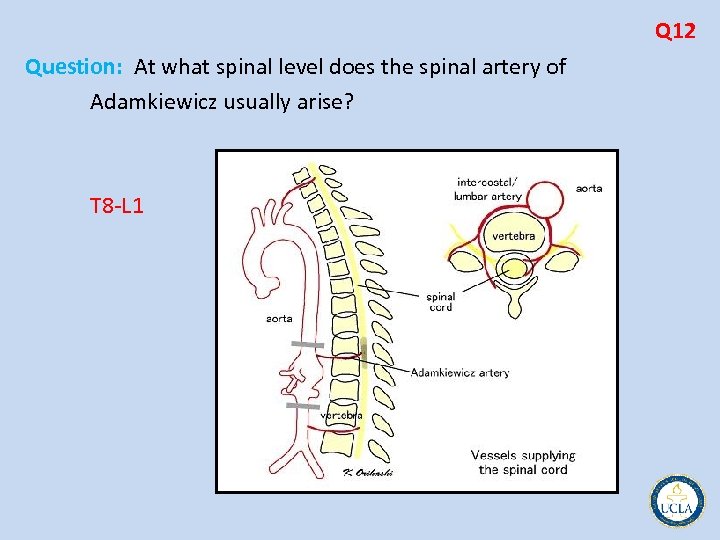
Q 12 Question: At what spinal level does the spinal artery of Adamkiewicz usually arise? T 8 L 1
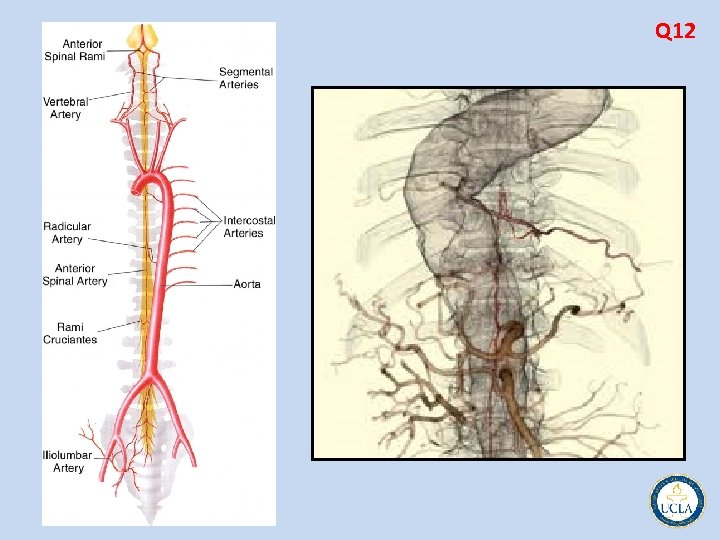
Q 12

Q 11 • Which of the following statements about thromboangiitis obliterans (Buerger's disease) is TRUE? A. Women outnumber men 4: 1 B. It is caused by a primary arterial infection with chlamydia C. In a smoker, tobacco withdrawal should be gradual to avoid rebound arterial vasospasm D. It is characterized by thrombotic occlusions of small and medium sized arteries E. Despite complete abstinence from nicotine, most patients eventually progress to major limb loss

Q 11 • Which of the following statements about thromboangiitis obliterans (Buerger's disease) is TRUE? A. Women outnumber men 4: 1 B. It is caused by a primary arterial infection with chlamydia C. In a smoker, tobacco withdrawal should be gradual to avoid rebound arterial vasospasm D. It is characterized by thrombotic occlusions of smalland medium-sized arteries E. Despite complete abstinence from nicotine, most patients eventually progress to major limb loss

• • • Q 11 Thromboangiitis obliterans (Buerger's disease) chronic arterial inflammatory condition of unknown etiology arterial occlusion in medium and small extremity arteries Major risk factors for atherosclerosis must be absent, proximal sources of emboli must be excluded, as well as underlying autoimmune disease and hypercoagulable states Both men and women can be affected, but most male Many patients develop a form of superficial thrombophlebitis that can be helpful in establishing the diagnosis Complete abstinence from tobacco in all forms (including chewing tobacco and snuff) is the only known effective treatment Most patients are unable to quit smoking If nicotine exposure is not curtailed, amputation rates can approach 80% to 90% Cessation of tobacco use can reduce this rate by 50%

ABSITE REVIEW Vascular Jessica O’Connell, MD January 25, 2012

ABSITE REVIEW Vascular & Orthopedics Jessica O’Connell, MD February 23, 2011
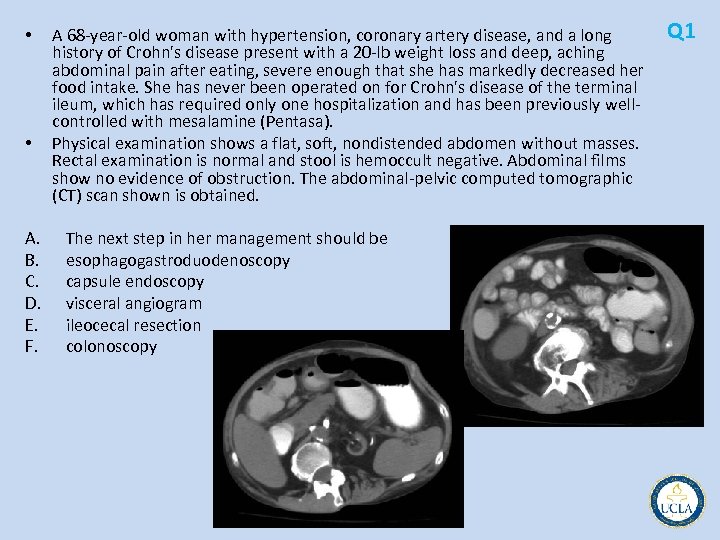
• • A. B. C. D. E. F. A 68 year old woman with hypertension, coronary artery disease, and a long history of Crohn's disease present with a 20 lb weight loss and deep, aching abdominal pain after eating, severe enough that she has markedly decreased her food intake. She has never been operated on for Crohn's disease of the terminal ileum, which has required only one hospitalization and has been previously well controlled with mesalamine (Pentasa). Physical examination shows a flat, soft, nondistended abdomen without masses. Rectal examination is normal and stool is hemoccult negative. Abdominal films show no evidence of obstruction. The abdominal pelvic computed tomographic (CT) scan shown is obtained. The next step in her management should be esophagogastroduodenoscopy capsule endoscopy visceral angiogram ileocecal resection colonoscopy Q 1
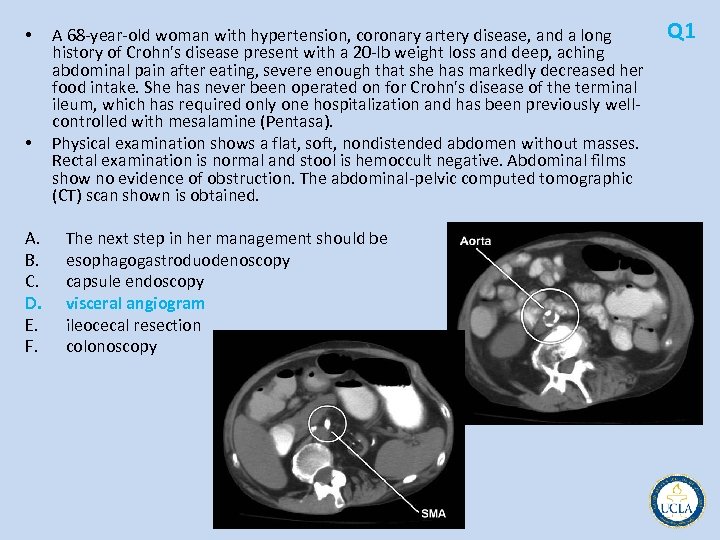
• • A. B. C. D. E. F. A 68 year old woman with hypertension, coronary artery disease, and a long history of Crohn's disease present with a 20 lb weight loss and deep, aching abdominal pain after eating, severe enough that she has markedly decreased her food intake. She has never been operated on for Crohn's disease of the terminal ileum, which has required only one hospitalization and has been previously well controlled with mesalamine (Pentasa). Physical examination shows a flat, soft, nondistended abdomen without masses. Rectal examination is normal and stool is hemoccult negative. Abdominal films show no evidence of obstruction. The abdominal pelvic computed tomographic (CT) scan shown is obtained. The next step in her management should be esophagogastroduodenoscopy capsule endoscopy visceral angiogram ileocecal resection colonoscopy Q 1
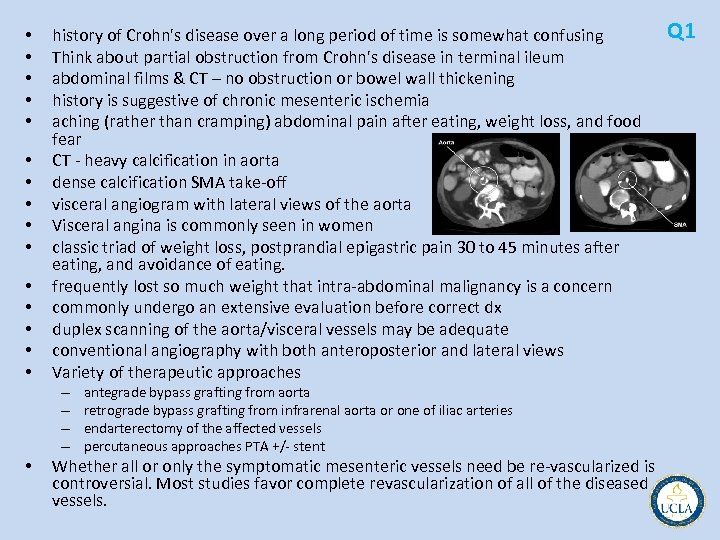
• • • • history of Crohn's disease over a long period of time is somewhat confusing Think about partial obstruction from Crohn's disease in terminal ileum abdominal films & CT – no obstruction or bowel wall thickening history is suggestive of chronic mesenteric ischemia aching (rather than cramping) abdominal pain after eating, weight loss, and food fear CT heavy calcification in aorta dense calcification SMA take off visceral angiogram with lateral views of the aorta Visceral angina is commonly seen in women classic triad of weight loss, postprandial epigastric pain 30 to 45 minutes after eating, and avoidance of eating. frequently lost so much weight that intra abdominal malignancy is a concern commonly undergo an extensive evaluation before correct dx duplex scanning of the aorta/visceral vessels may be adequate conventional angiography with both anteroposterior and lateral views Variety of therapeutic approaches – – • antegrade bypass grafting from aorta retrograde bypass grafting from infrarenal aorta or one of iliac arteries endarterectomy of the affected vessels percutaneous approaches PTA +/ stent Whether all or only the symptomatic mesenteric vessels need be re vascularized is controversial. Most studies favor complete revascularization of all of the diseased vessels. Q 1

Q 2 Which of the following is the most appropriate candidate for protected carotid artery stenting? A. Healthy 60 year old man with amaurosis fugax of the left eye and an 80% stenosis of the left internal carotid artery (ICA) B. Healthy 70 year old woman with a 50% asymptomatic stenosis of the left ICA C. 69 year old man with severe congestive heart failure, left ventricular ejection fraction of 20%, and a 60% asymptomatic stenosis of the left ICA D. 72 year old man with chronic obstructive pulmonary disease (FEV 1 =0. 40), episodes of intermittent right arm weakness, and 90% stenosis of the left ICA E. 60 year old diabetic man with unexplained right eye blindness and 50% stenosis of the left ICA

Q 2 Which of the following is the most appropriate candidate for protected carotid artery stenting? A. Healthy 60 year old man with amaurosis fugax of the left eye and an 80% stenosis of the left internal carotid artery (ICA) B. Healthy 70 year old woman with a 50% asymptomatic stenosis of the left ICA C. 69 year old man with severe congestive heart failure, left ventricular ejection fraction of 20%, and a 60% asymptomatic stenosis of the left ICA D. 72 year old man with chronic obstructive pulmonary disease (FEV 1 =0. 40), episodes of intermittent right arm weakness, and 90% stenosis of the left ICA E. 60 year old diabetic man with unexplained right eye blindness and 50% stenosis of the left ICA

High Risk Medical: • clinically significant cardiac disease “High Risk for CEA” – congestive heart failure, abnormal stress test, EF <30%, need for open heart surgery, MI within 4 weeks, CABG within 6 months • • • severe pulmonary disease Dialysis dependent renal failure age > 80 years High Risk Surgical: • • contralateral carotid occlusion contralateral laryngeal nerve palsy previous radical neck surgery radiation therapy to the neck recurrent stenosis after endarterectomy high lesion (above C 2) Tracheostomy

NASCET Results • North American Symptomatic Carotid Endarterectomy Trial • significant benefit of CEA in patients with 70% to 99% symptomatic stenosis • Two-year ipsilateral stroke risk – 26% in the medically treated patients – 9% in the CEA group (P <. 001; ARR 17. 0%; NNT = 6) Beneficial effect of carotid endarterectomy in symptomatic patients with high grade carotid stenosis. North American Symptomatic Carotid Endarterectomy Trial Collaborators. N Engl J Med. 1991 Aug 15; 325(7): 445 53.
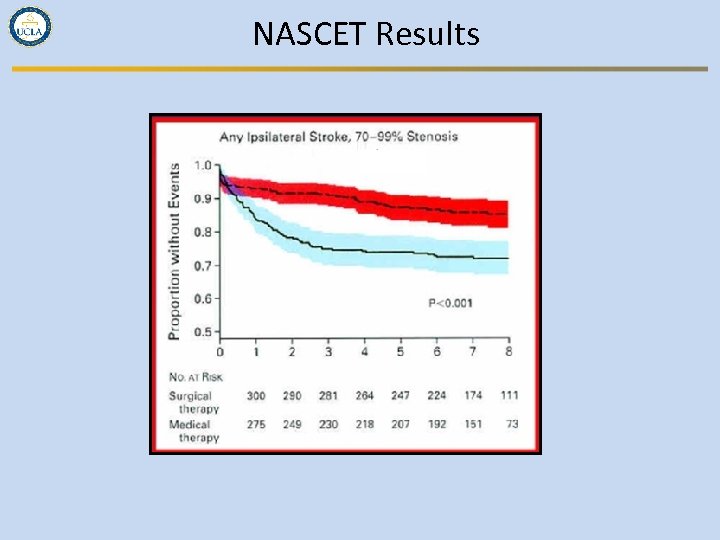
NASCET Results
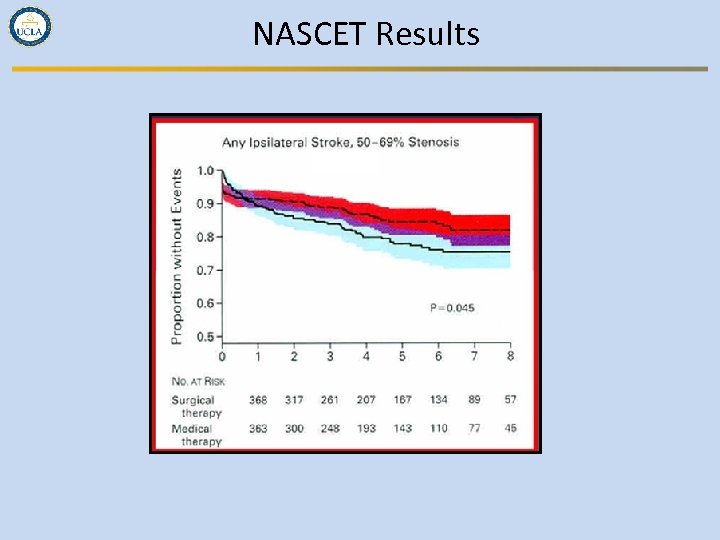
NASCET Results
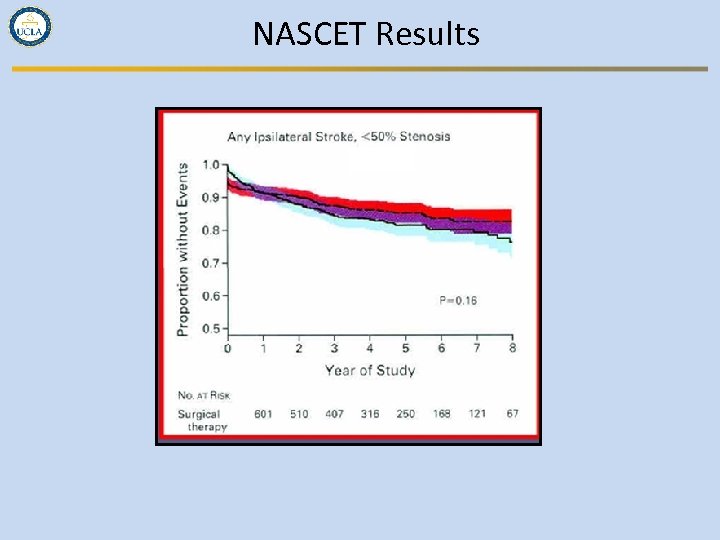
NASCET Results

Asymptomatic Carotid Atherosclerosis Study (ACAS) • Multicenter, randomized, prospective • Medical management vs. medical management & CEA • Asymptomatic patients with ≥ 60% ICA stenosis • Endpoints: stroke or death • Results: stroke / death (at 5 years) • Medical Group: 11% • Surgical Group: 5. 1% (53% RRR; P =. 004) • Surgical Morbidity / Mortality: 1. 5% • Major Angio related Morbidity / Mortality: 1. 2% • Executive Committee for the Asymptomatic Carotid Atherosclerosis Study. Endarterectomy for asymptomatic carotid artery stenosis. JAMA. 1995 May 10; 273(18): 1421 -8.

Carotid Revascularization Endarterectomy vs. Stenting Trial (CREST) • Multicenter, randomized, prospective, 2502 patients • CEA vs. CAS • Symptomatic patients with ICA stenosis • ≥ 50% on angio • ≥ 70% on US • ≥ 70% on CTA or MRA (if US 50 -69% on US) • Asymptomatic patients with ICA stenosis • ≥ 60% on angio • ≥ 70% on US • ≥ 80% on CTA or MRA (if US 50 -69% on US) • Endpoint: periprocedural (randomization to ~1 month postop) stroke, MI, death OR ipsilateral stroke up to 4 years
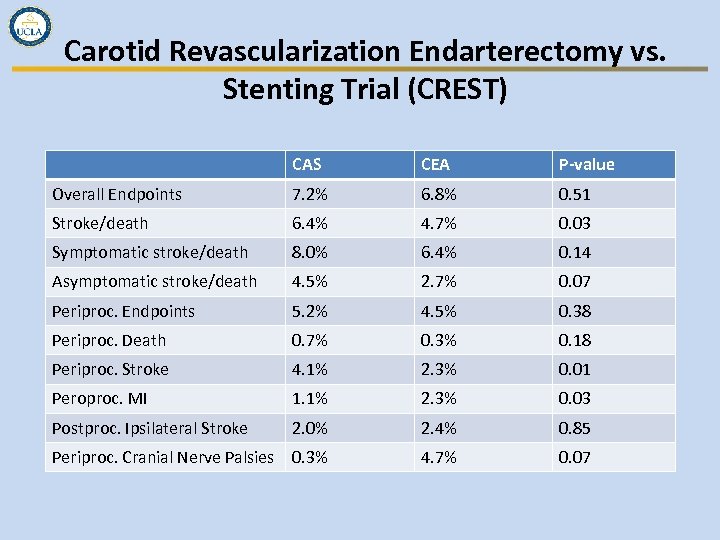
Carotid Revascularization Endarterectomy vs. Stenting Trial (CREST) CAS CEA P-value Overall Endpoints 7. 2% 6. 8% 0. 51 Stroke/death 6. 4% 4. 7% 0. 03 Symptomatic stroke/death 8. 0% 6. 4% 0. 14 Asymptomatic stroke/death 4. 5% 2. 7% 0. 07 Periproc. Endpoints 5. 2% 4. 5% 0. 38 Periproc. Death 0. 7% 0. 3% 0. 18 Periproc. Stroke 4. 1% 2. 3% 0. 01 Peroproc. MI 1. 1% 2. 3% 0. 03 Postproc. Ipsilateral Stroke 2. 0% 2. 4% 0. 85 Periproc. Cranial Nerve Palsies 0. 3% 4. 7% 0. 07
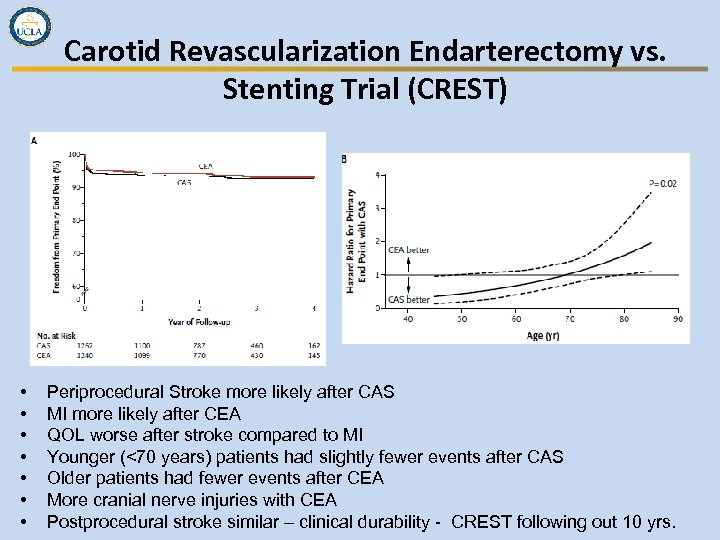
Carotid Revascularization Endarterectomy vs. Stenting Trial (CREST) • • Periprocedural Stroke more likely after CAS MI more likely after CEA QOL worse after stroke compared to MI Younger (<70 years) patients had slightly fewer events after CAS Older patients had fewer events after CEA More cranial nerve injuries with CEA Postprocedural stroke similar – clinical durability - CREST following out 10 yrs.
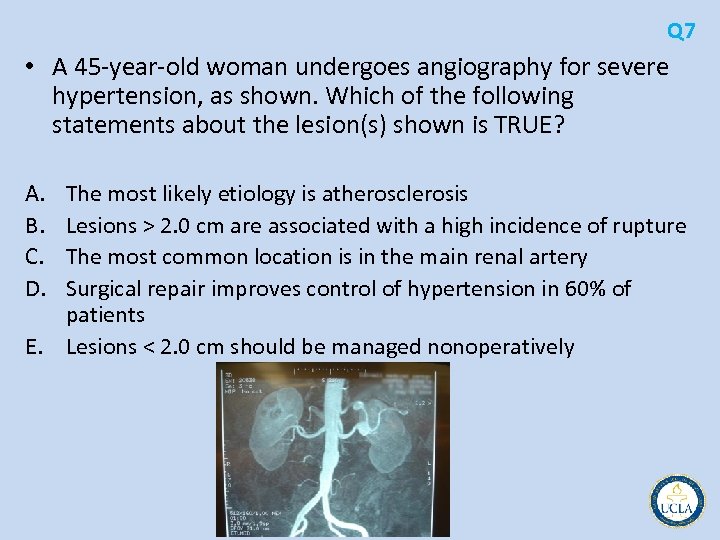
Q 7 • A 45 year old woman undergoes angiography for severe hypertension, as shown. Which of the following statements about the lesion(s) shown is TRUE? A. B. C. D. The most likely etiology is atherosclerosis Lesions > 2. 0 cm are associated with a high incidence of rupture The most common location is in the main renal artery Surgical repair improves control of hypertension in 60% of patients E. Lesions < 2. 0 cm should be managed nonoperatively
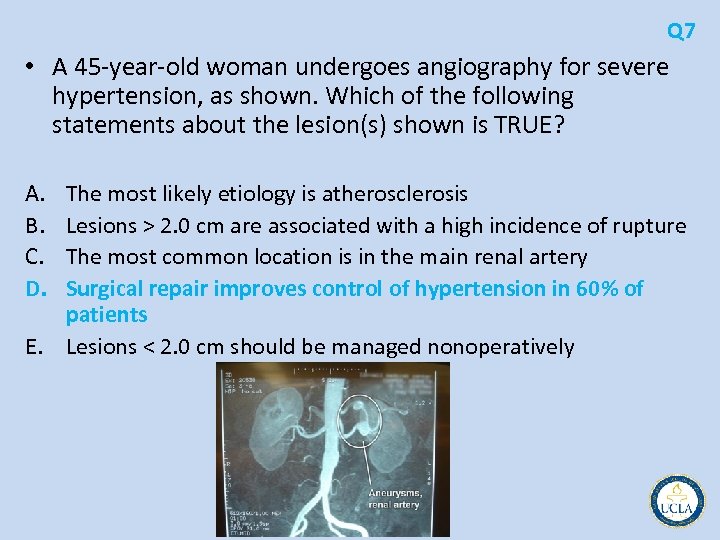
Q 7 • A 45 year old woman undergoes angiography for severe hypertension, as shown. Which of the following statements about the lesion(s) shown is TRUE? A. B. C. D. The most likely etiology is atherosclerosis Lesions > 2. 0 cm are associated with a high incidence of rupture The most common location is in the main renal artery Surgical repair improves control of hypertension in 60% of patients E. Lesions < 2. 0 cm should be managed nonoperatively

• • aneurysm of the renal artery 0. 09% of the general population incidental most common etiology arterial fibrodysplasia – – underlying arterial matrix disruption leads to aneurysm formation, particularly at branch points where discontinuities in the internal elastic lamina are common, even in healthy patients Multiparous women • • • During the latter stages of gestation, an alteration in hormone and enzyme activity contributes to the tissue relaxation necessary for parturition. Sustained release of these matrix altering substances 35 year experience with 252 renal artery aneurysms in 168 patients at the University of Michigan, most asymptomatic, average size 1. 5 cm 60% of patients undergoing repair had a significant decline in blood pressure postoperatively, while taking fewer antihypertensive medications Late renal artery rupture did not occur in the nonoperative patients, but this group saw no change in their hypertension average number of renal artery aneurysms per patient was 1. 5. Most patients had solitary aneurysms, but 53 had multiple renal artery aneurysms. Bilateral aneurysms occurred in 32 patients The most common location bifurcation or the first order renal artery branch not main renal artery itself. Lesions > 2 cm in diameter are not associated with a higher incidence of rupture compared with lesions < 2 cm In fact, patients with aneurysms < 2 cm in diameter can have a significant improvement in their hypertension and should be offered surgical resection Most aneurysms 1. 5 to 2 cm in diameter and all those larger than 2 cm in diameter, regardless of blood pressure status, should be treated surgically if their anatomic characteristics suggest a relatively noncomplex renal artery construction and the procedure is undertaken by an experienced surgeon Q 7
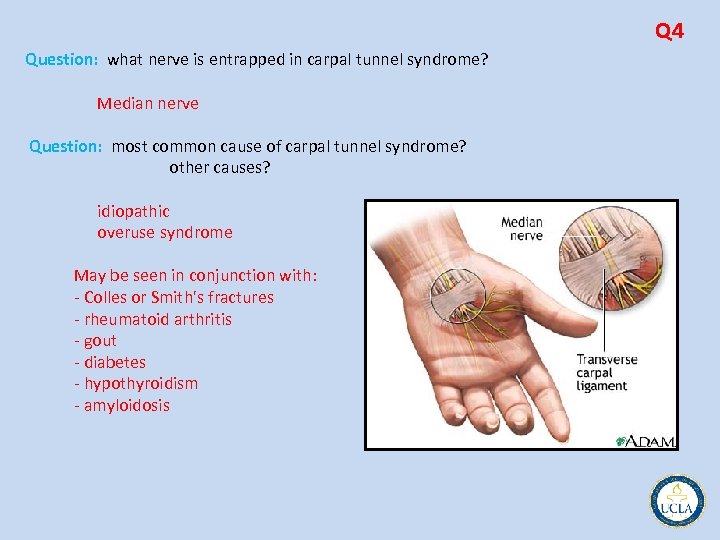
Q 4 Question: what nerve is entrapped in carpal tunnel syndrome? Median nerve Question: most common cause of carpal tunnel syndrome? other causes? idiopathic overuse syndrome May be seen in conjunction with: Colles or Smith's fractures rheumatoid arthritis gout diabetes hypothyroidism amyloidosis
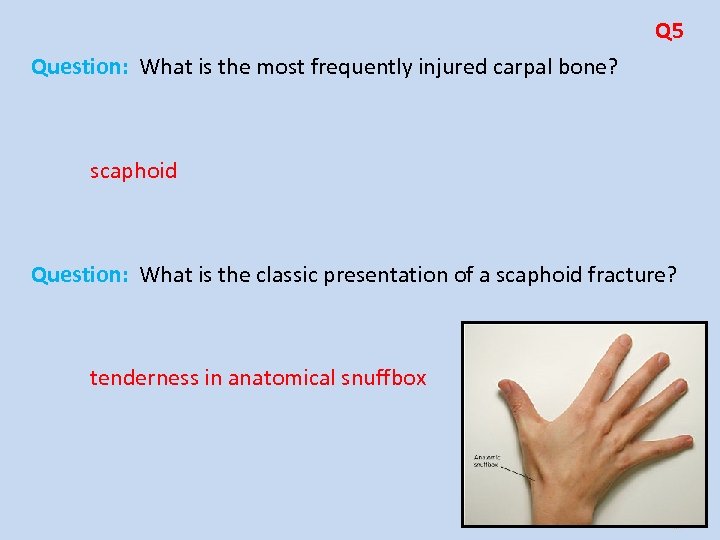
Q 5 Question: What is the most frequently injured carpal bone? scaphoid Question: What is the classic presentation of a scaphoid fracture? tenderness in anatomical snuffbox
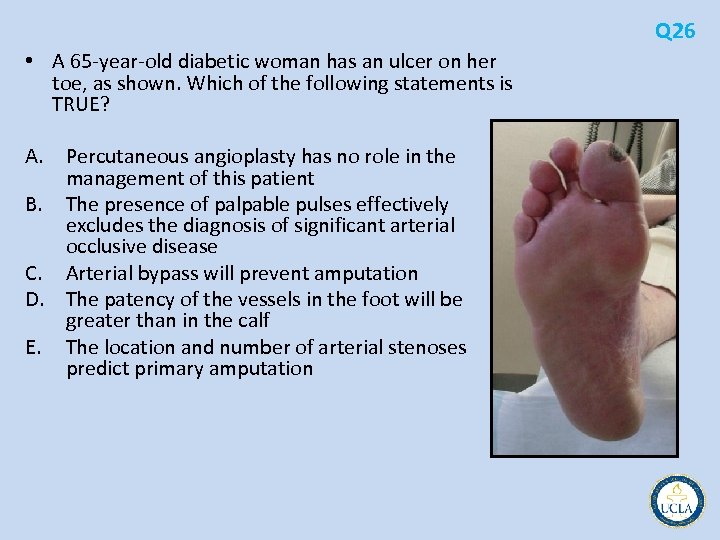
Q 26 • A 65 year old diabetic woman has an ulcer on her toe, as shown. Which of the following statements is TRUE? A. Percutaneous angioplasty has no role in the management of this patient B. The presence of palpable pulses effectively excludes the diagnosis of significant arterial occlusive disease C. Arterial bypass will prevent amputation D. The patency of the vessels in the foot will be greater than in the calf E. The location and number of arterial stenoses predict primary amputation
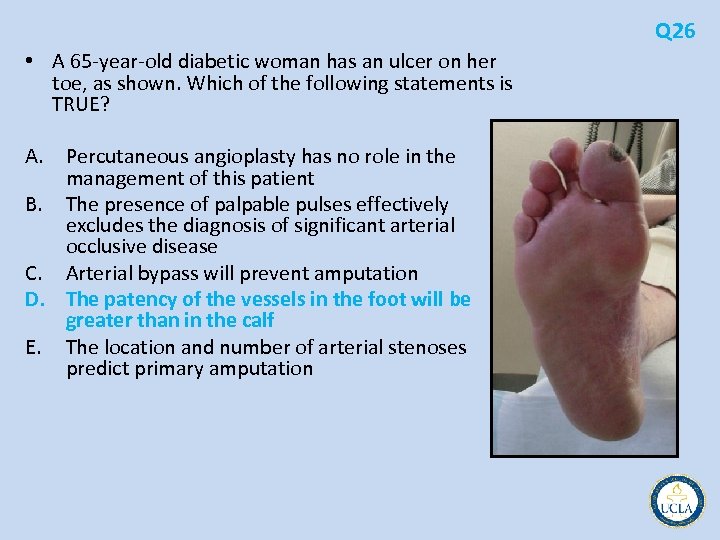
Q 26 • A 65 year old diabetic woman has an ulcer on her toe, as shown. Which of the following statements is TRUE? A. Percutaneous angioplasty has no role in the management of this patient B. The presence of palpable pulses effectively excludes the diagnosis of significant arterial occlusive disease C. Arterial bypass will prevent amputation D. The patency of the vessels in the foot will be greater than in the calf E. The location and number of arterial stenoses predict primary amputation

• A recent study of 104 patients with diabetes mellitus Q 26 and foot ulcers who were evaluated with arteriography • arterial stenosis or occlusion in 103 patients • Significant stenoses were found in patients with palpable foot pulses and normal ankle brachial indices • popliteal and infrapopliteal region • vessels in the foot relatively spared • Nearly 25% of patients could be treated with percutaneous angioplasty to improve wound healing and 10% required arterial bypass procedures • Technical failures occurred in 15% of angioplasty and in 25% of bypass procedures • limb salvage was achieved in 78% of patients with 44% requiring amputation of single or multiple digits.
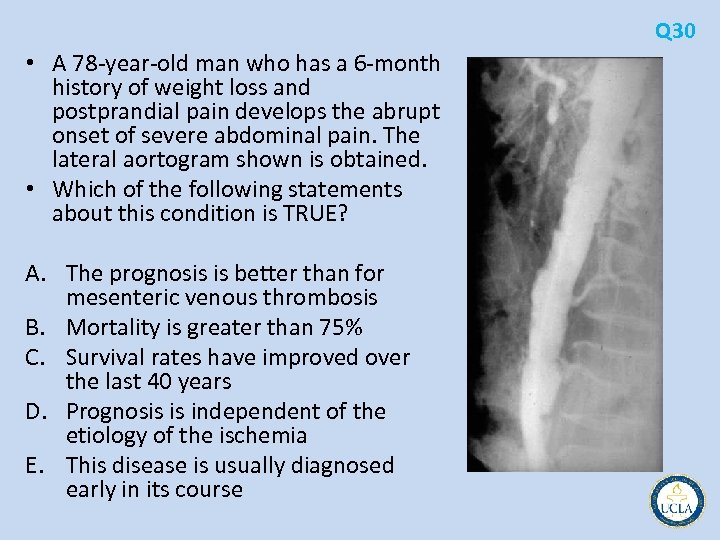
Q 30 • A 78 year old man who has a 6 month history of weight loss and postprandial pain develops the abrupt onset of severe abdominal pain. The lateral aortogram shown is obtained. • Which of the following statements about this condition is TRUE? A. The prognosis is better than for mesenteric venous thrombosis B. Mortality is greater than 75% C. Survival rates have improved over the last 40 years D. Prognosis is independent of the etiology of the ischemia E. This disease is usually diagnosed early in its course
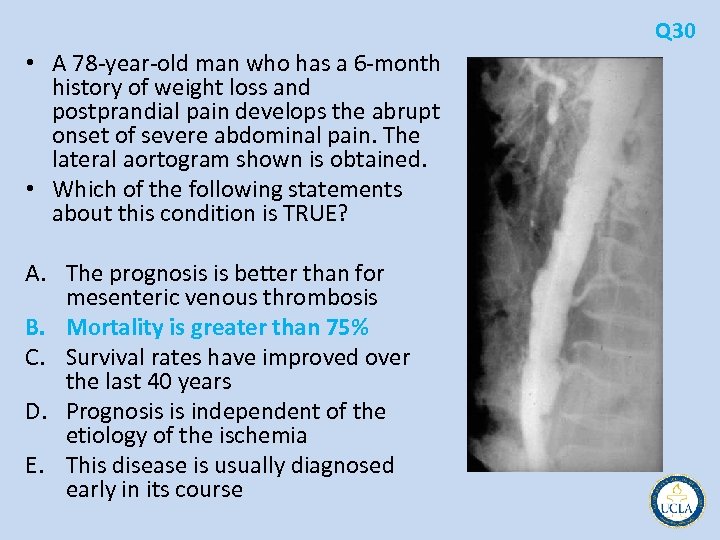
Q 30 • A 78 year old man who has a 6 month history of weight loss and postprandial pain develops the abrupt onset of severe abdominal pain. The lateral aortogram shown is obtained. • Which of the following statements about this condition is TRUE? A. The prognosis is better than for mesenteric venous thrombosis B. Mortality is greater than 75% C. Survival rates have improved over the last 40 years D. Prognosis is independent of the etiology of the ischemia E. This disease is usually diagnosed early in its course
Q 30 • no filling of the superior mesenteric or inferior mesenteric arteries • Late filling of the celiac artery 2 cm distal to the origin • Quantitative analysis of 45 observational studies of 3692 patients – venous thrombosis 32% mortality – arterial emboli 54% – nonocclusive ischemia 72. 7% – acute arterial thrombosis 77. 4%
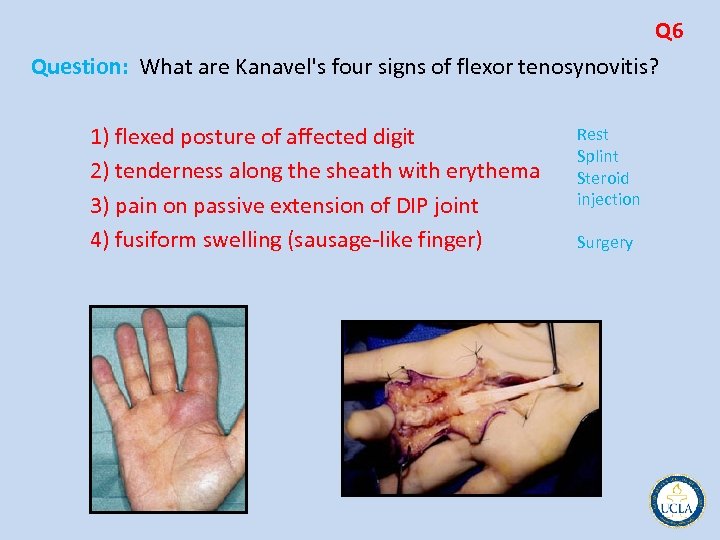
Q 6 Question: What are Kanavel's four signs of flexor tenosynovitis? Rest 1) flexed posture of affected digit Splint 2) tenderness along the sheath with erythema Steroid injection 3) pain on passive extension of DIP joint 4) fusiform swelling (sausage like finger) Surgery
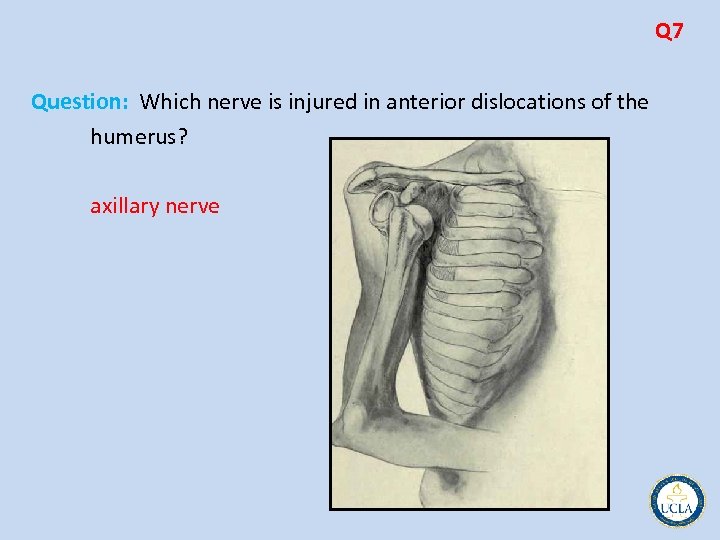
Q 7 Question: Which nerve is injured in anterior dislocations of the humerus? axillary nerve
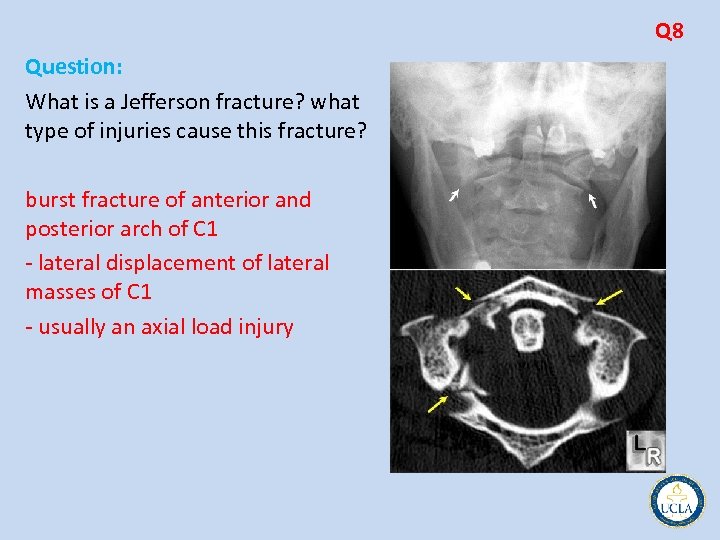
Q 8 Question: What is a Jefferson fracture? what type of injuries cause this fracture? burst fracture of anterior and posterior arch of C 1 lateral displacement of lateral masses of C 1 usually an axial load injury
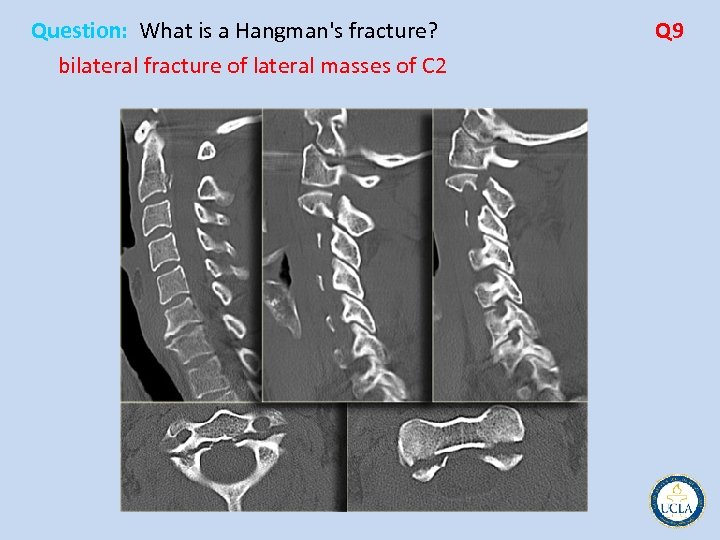
Question: What is a Hangman's fracture? bilateral fracture of lateral masses of C 2 Q 9
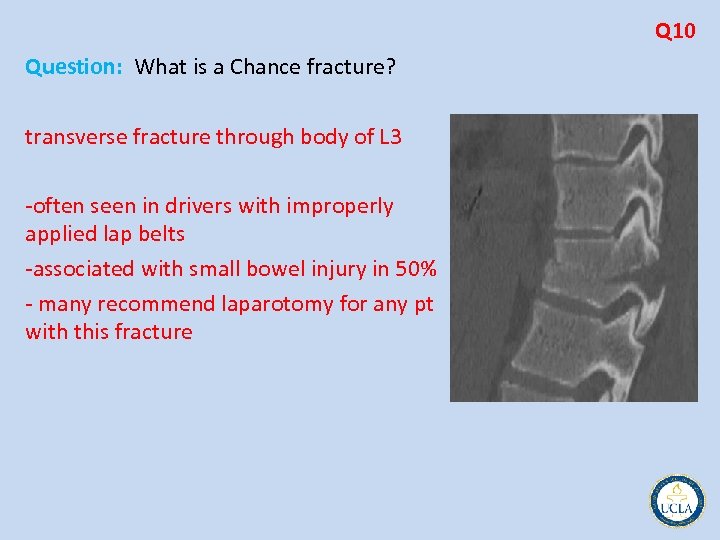
Q 10 Question: What is a Chance fracture? transverse fracture through body of L 3 often seen in drivers with improperly applied lap belts associated with small bowel injury in 50% many recommend laparotomy for any pt with this fracture

Q 43 • The most appropriate initial management for a posterior hip dislocation would be • computed tomography (CT) to evaluate for intra articular fragments prior to reduction A. conscious sedation with closed reduction as soon as possible B. placement of a traction splint C. bed rest and application of skeletal traction to reduce the dislocation D. immediate operative reduction

Q 43 • The most appropriate initial management for a posterior hip dislocation would be • computed tomography (CT) to evaluate for intra articular fragments prior to reduction A. conscious sedation with closed reduction as soon as possible B. placement of a traction splint C. bed rest and application of skeletal traction to reduce the dislocation D. immediate operative reduction E. computed tomography (CT) to evaluate for intra articular fragments prior to reduction

• Hip dislocation is often caused by a force applied to the femur and is most Q 43 commonly associated with fractures of the acetabulum or femoral head • Motor vehicles crashes are a common mechanism • Force applied to an abducted hip can result in anterior dislocation • striking the knee on the dashboard with the hip flexed and adducted results in posterior dislocations • Posterior dislocations often associated with fractures of the posterior wall of the acetabulum • Once the hip has been completely dislocated posteriorly, it may appear shortened and internally rotated • Sometimes femoral head or acetabular fractures are associated with this dislocation • Sciatic nerve injuries are present in up to 15% of posterior hip dislocations • Closed reduction is usually accomplished by longitudinal traction, followed by gentle abduction and external rotation • Stability of the reduction should be determined at the time of closed reduction • Open reduction and internal fixation is indicated only if the reduction is unstable and associated with a posterior wall fracture
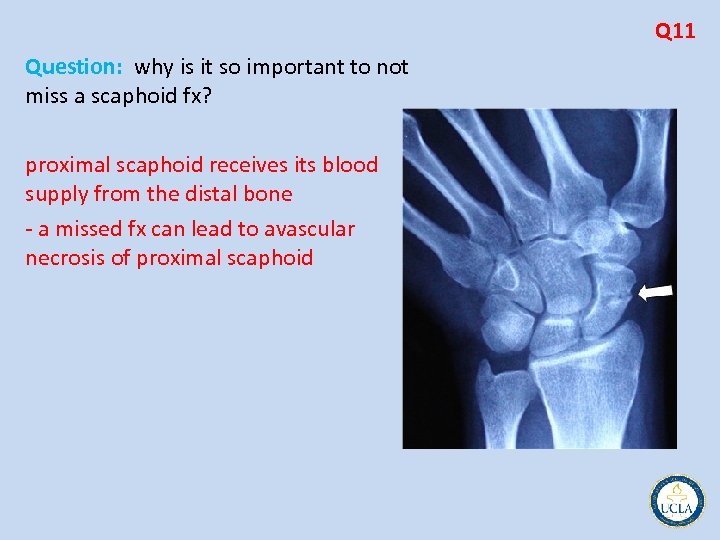
Q 11 Question: why is it so important to not miss a scaphoid fx? proximal scaphoid receives its blood supply from the distal bone a missed fx can lead to avascular necrosis of proximal scaphoid
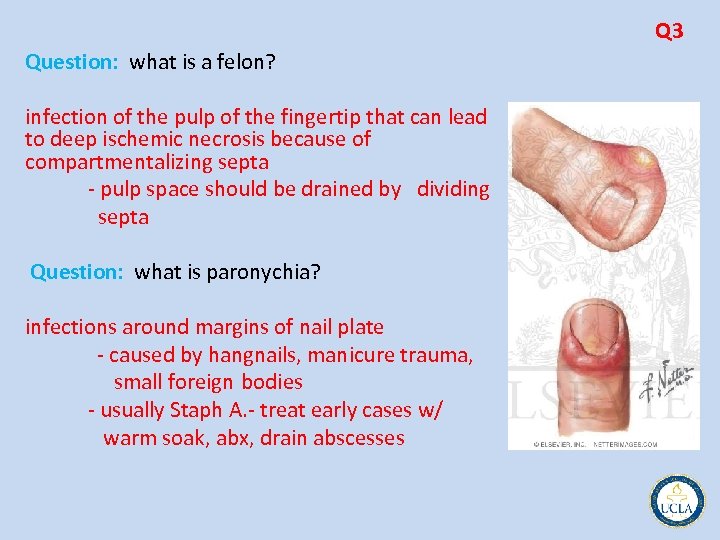
Q 3 Question: what is a felon? infection of the pulp of the fingertip that can lead to deep ischemic necrosis because of compartmentalizing septa pulp space should be drained by dividing septa Question: what is paronychia? infections around margins of nail plate caused by hangnails, manicure trauma, small foreign bodies usually Staph A. treat early cases w/ warm soak, abx, drain abscesses
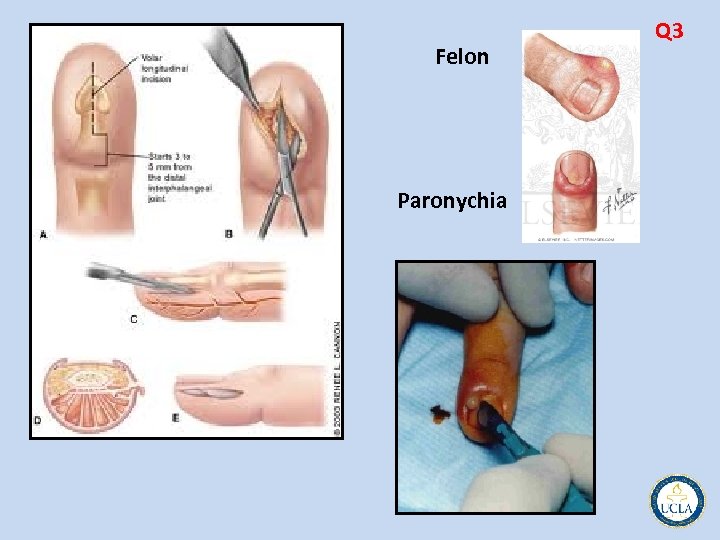
Felon Paronychia Q 3
f1d06a802dd1b67c9866c19bd4406807.ppt