2b19afdeffab6f99ad430cf48c5fad54.ppt
- Количество слайдов: 67

ABCs of Shock Pediatric Critical Care Medicine Emory University Children’s Healthcare of Atlanta

Objectives • Review basic physiology of shock states in pediatrics • Classification and recognition of clinical shock states • Review initial management of shock 2

Definition 3
Shock? 3 month old with lethargy, temp 34 C, HR 180 2 yr old with petechiae and flash cap refill 16 yr old with resp distress, muffled heart sounds, distended neck veins 4
Shock? 3 month old with lethargy, temp 34 C, HR 180 2 yr old with petechiae and flash cap refill 16 yr old with resp distress, muffled heart sounds, distended neck veins SHOCK 5

Definition • Failure of delivery oxygen and substrates to meet the metabolic demands of the tissue beds SUPPLY < DEMAND Oxygen delivery < Oxygen Consumption DO 2 < VO 2 • Failure to remove metabolic end-products • Result of inadequate blood flow and/or oxygen delivery 6

Definition • Common pathway – Failure to deliver substrates conversion to anaerobic metabolism • Reversible if recognized early • Irreversible organ damage at the late stage – Progressive acidosis and eventually cell death • Early recognition is key 7

Epidemiology • Incidence: not clear – Shock is not commonly listed as the diagnosis in ER visits • Estimated that more children die from sepsis than cancer each year • Common causes: hypovolemia, sepsis & trauma – Worldwide: diarrhea – Developed countries: trauma 8

Pathophysiology • Children – – – Higher % body water Higher resting metabolic rate Higher insensible losses Lower renal concentrating ability Subtle signs/symptoms • Higher risk for organ hypo-perfusion 9

Pathophysiology O 2 supply < O 2 demand O 2 delivery < O 2 consumption DO 2 < VO 2 10

Oxygen delivery (DO 2) • DO 2 = CO x Ca. O 2 – DO 2 : oxygen delivery – CO : Cardiac output – Ca. O 2: arterial oxygen content • CO = HR x SV – HR: heart rate – SV: stroke volume • Ca. O 2 = Hg. B x Sa. O 2 x 1. 34 + (0. 003 x Pa. O 2) – Oxygen content = oxygen carried by Hg. B + dissolved oxygen 11

Oxygen delivery (DO 2) DO 2 = CO x Ca. O 2 Critical DO 2: consumption depends on delivery 12
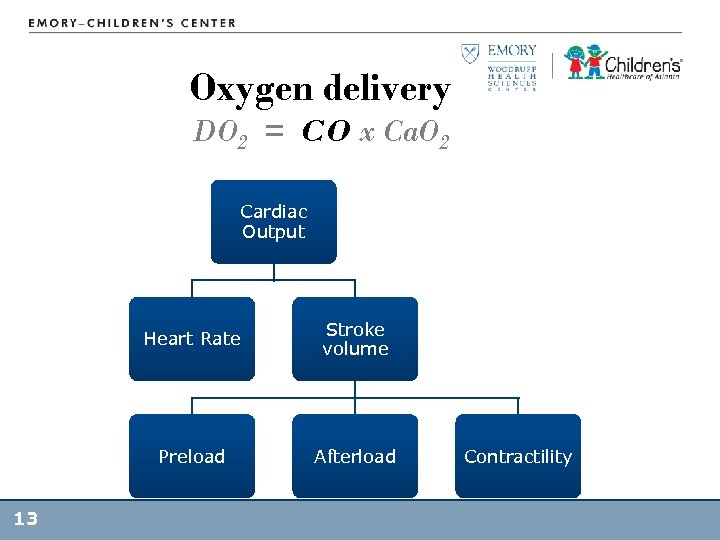
Oxygen delivery DO 2 = CO x Ca. O 2 Cardiac Output Heart Rate Preload 13 Stroke volume Afterload Contractility

Oxygen delivery DO 2 = CO x Ca. O 2 • CO = HR x SV • HR is independent – Neonates depend on HR (can’t increase SV) • SV depends on – Pre-load: volume of blood – After-load: resistance to contraction – Contractility: force 14

Oxygen delivery DO 2 = CO x Ca. O 2 • Ca. O 2 = Hg. B x Sa. O 2 x 1. 34 + (0. 003 x Pa. O 2) • Normal circumstance: Ca. O 2 is closely associated with Sa. O 2 • Severe anemia or in the presence of abnormal Hg. B (i. e. CO poisoning) - Ca. O 2 is strongly affected by Pa. O 2 15

Hypo-perfusion • Poor perfusion of a vital organs leads to organ dysfunction – Decreased urine output – Altered mental status – Elevated LFTs, bilirubin • Switches to anaerobic metabolism Lactate • Activates inflammatory cascade – Activates neutrophils, releases cytokines • Increases adrenergic stress response – Increases lipolysis/glycogenolysis (also increases lactate) – Releases catecholamine and corticosteroid 16

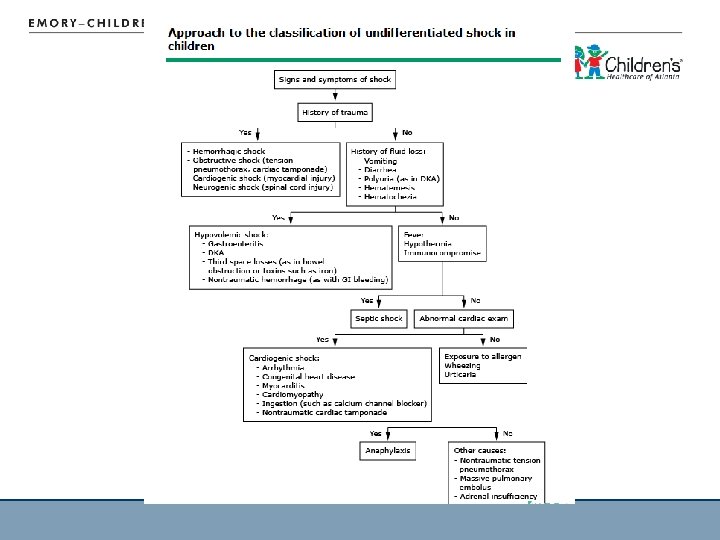
Classification of Shock Stages vs. Types 17

Stages of Shock • Compensated – Maintains end organ perfusion – BP is maintained usually by ↑ HR • Uncompensated – Decreases micro-vascular perfusion – Sign/symptoms of end organ dysfunction – Hypotensive • Irreversible – Progressive end-organ dysfunction – Cellular acidosis results in cell death 18
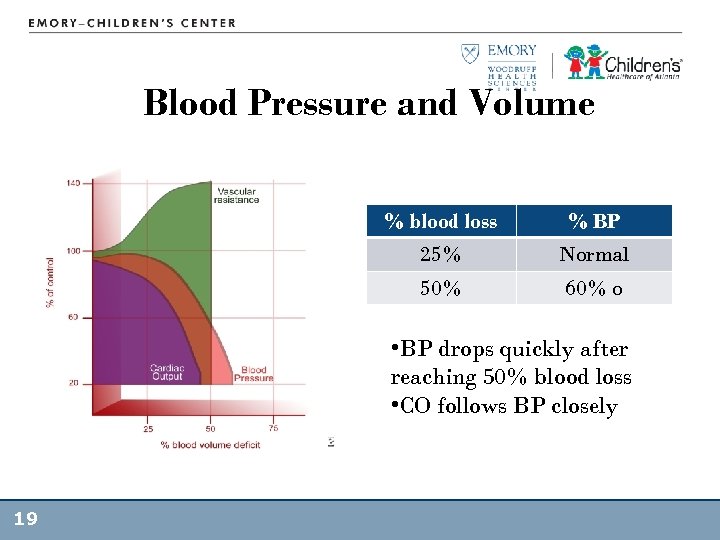
Blood Pressure and Volume % blood loss % BP 25% Normal 50% 60% o • BP drops quickly after reaching 50% blood loss • CO follows BP closely 19

Systemic Inflammatory Response Syndrome (SIRS) • Widespread inflammation due to infection, trauma, burns, etc. • Criteria – requires 2 of the followings – – 20 Core temp >38. 5˚C or <36˚C Tachycardia (or bradycardia in infants) Tachypnea Elevated or depressed WBC or >10% bands

Types of Shock • • 21 Hypovolemic Distributive Cardiogenic Septic
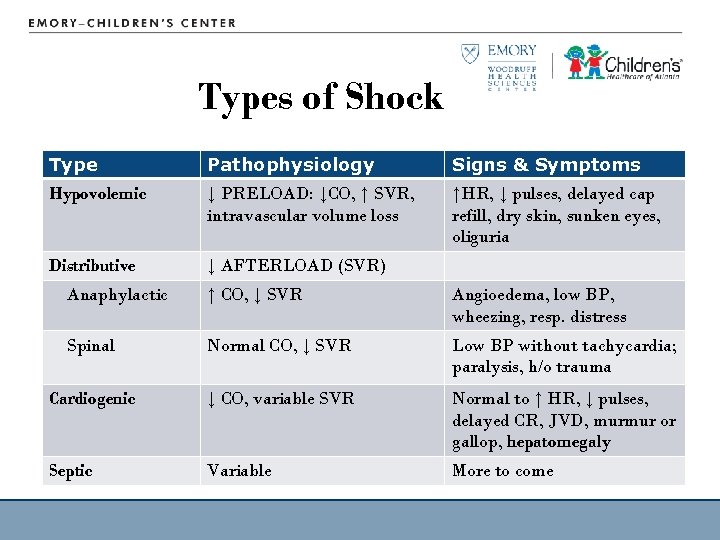
Types of Shock Type Pathophysiology Signs & Symptoms Hypovolemic ↓ PRELOAD: ↓CO, ↑ SVR, intravascular volume loss ↑HR, ↓ pulses, delayed cap refill, dry skin, sunken eyes, oliguria Distributive ↓ AFTERLOAD (SVR) Anaphylactic ↑ CO, ↓ SVR Angioedema, low BP, wheezing, resp. distress Spinal Normal CO, ↓ SVR Low BP without tachycardia; paralysis, h/o trauma Cardiogenic ↓ CO, variable SVR Normal to ↑ HR, ↓ pulses, delayed CR, JVD, murmur or gallop, hepatomegaly Septic Variable More to come

Hypovolemic Shock • Most common type in children • #1 cause of death worldwide – Hemorrhagic: developed countries – GI bleed, trauma (liver/spleen injuries, long bone fractures), intracranial hemorrhage – Non-hemorrhagic: vomiting/diarrhea, heat stroke, burns, DKA • Pathophysiology: – Loss of intravascular volume ↓ PRELOAD 23

Hypovolemic Shock • Clinical symptoms – – – Sunken fontanel/eyes Dry mucous membrane Poor skin turgor Delayed capillary refill Cool extremities • Tachycardia = compensated shock! – Normal BP until volume loss >30 -40% 24

Distributive Shock • Loss of SVR (AFTERLOAD) results in abnormal distribution of blood flow • Increased CO and HR – Often hyper dynamic contractility, bounding pulses, flash CR • Loss of vascular tone eventually leads to loss of PRELOAD – Blood volume pools in the periphery 25

Distributive Shock • Anaphylaxis is Ig. E mediated hypersensitive response – Massive release of cytokines from activated mast cells – Associated with respiratory distress, angioedema, vascular tone collapse • Neurogenic: unusual and mostly transient – Follows acute CNS injury (brain or spinal cord) – Loss of sympathetic and autonomic tone – Unique presentation: hypotension with normal heart rate 26
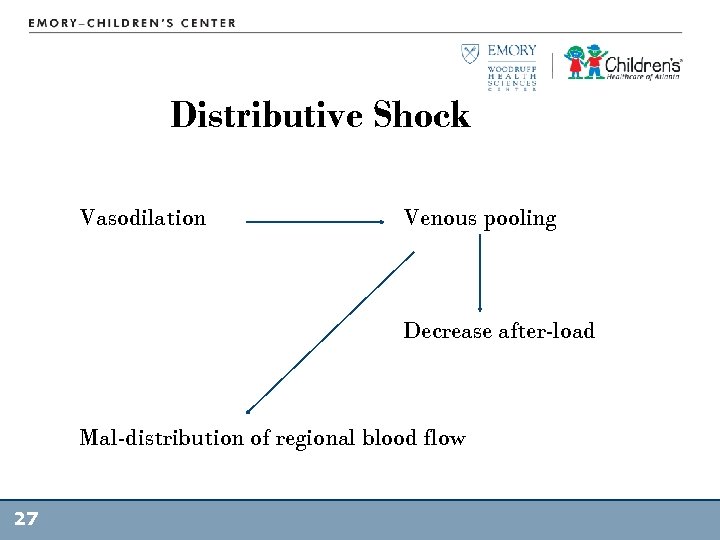
Distributive Shock Vasodilation Venous pooling Decrease after-load Mal-distribution of regional blood flow 27

Cardiogenic Shock • Impaired CONTRACTILITY (pump failure) • 3 categories – Cardiomyopathy – Arrhythmia – Obstruction 28

Cardiogenic Shock • Cardiomyopathy – – 29 Infectious – post viral infection (coxsakie) Infiltrative – storage disease Ischemia – cardiac arrest or bypass Sepsis – late stage

Cardiogenic Shock • Arrhythmia – Ventricular fibrillation & pulseless ventricular tachycardia abolish cardiac output – Prolonged or recurrent SVT – Brady-arrhythmias or heart block seen in neonatal SLE 30

Cardiogenic Shock • Obstructive – Physical obstruction – tension pneumothorax, tamponade, pulmonary embolus – Congenital - coartation of the aorta, hypoplastic left heart, critical aortic stenosis » Usually present in shock with closing of the ductus arteriosus 31
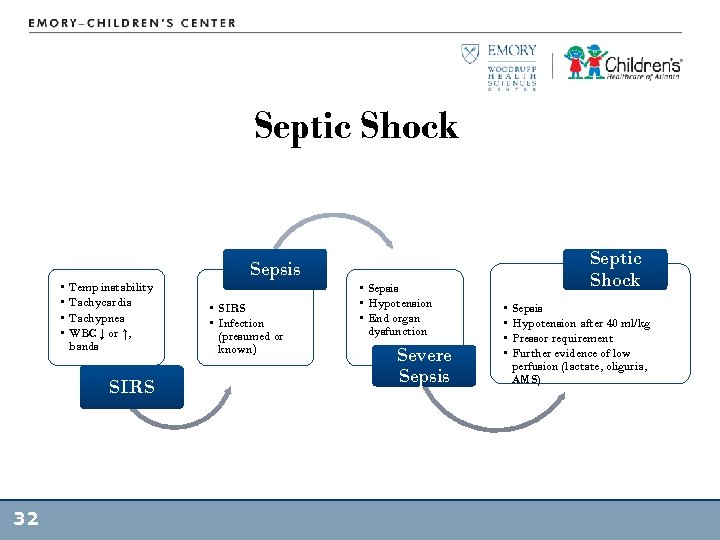
Septic Shock • • Temp instability Tachycardia Tachypnea WBC ↓ or ↑, bands SIRS 32 Sepsis • SIRS • Infection (presumed or known) • Sepsis • Hypotension • End organ dysfunction Severe Sepsis Septic Shock • • Sepsis Hypotension after 40 ml/kg Pressor requirement Further evidence of low perfusion (lactate, oliguria, AMS)

Septic Shock • 20% presentation – classic warm shock – High CO, low SVR • 60% presentation – cold shock – Low CO, high SVR • Small % presentation with mixed pictures 33

Septic Shock • Highest in infants (particularly in newborns) • Risks – – 34 Structural heard disease Neutropenia Neurodevelopmental disorders Invasive devices

Evaluation & Treatment 35

Initial Assessment • Goals – Immediate identification of life-threatening conditions – Rapid recognition of circulatory compromise – Early classification of the type and cause of shock 36

Initial Assessment • Airway – Mental status: can the patient maintain the airway • Breathing – ? impending respiratory failure • Circulation – Heart rate, pulses, blood pressure – Capillary refills - perfusion • Dextrose 37
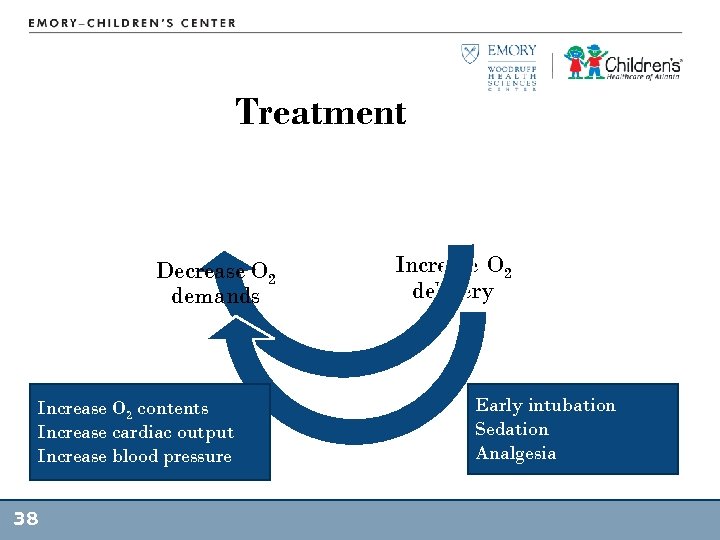
Treatment Decrease O 2 demands Increase O 2 contents Increase cardiac output Increase blood pressure 38 Increase O 2 delivery Early intubation Sedation Analgesia
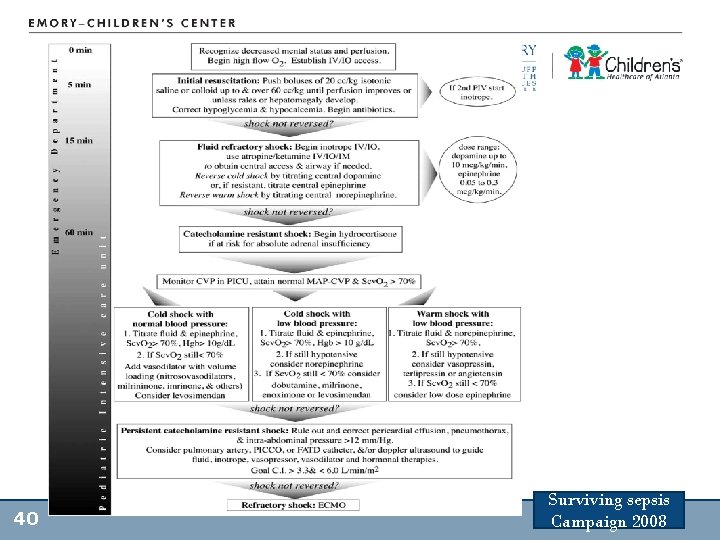
40 Surviving sepsis Campaign 2008

PALS Shock Algorithm

History & Physical Exam • Brief medical history – Preceding events, recent illness or trauma – PMH – Allergies & exposure • Focused physical examination – – 42 Neuro – mental status CV – HR/perfusion/CR, ? gallop/murmur Resp – crackles, wheezing GI - ? HSM

Early Goal-Directed Therapy • Goal – in the first 6 hours of presentation - improvement of indicators of perfusion and vital organ function • Physiologic targets – – – 43 BP >5 th percentile for age Quality of central & peripheral pulses Normal perfusion Mental status UOP > 1 ml/kg/hr

Fluid Resuscitation • Isotonic crystalloids – availability – 20 cc/kg reassess (overload vs. third spacing) • Rapid infusion – 5 - 10 min • NO upper limit – Pressor if > 60 ml/kg – May need up to 100 -200 ml/kg during the first few hours 44
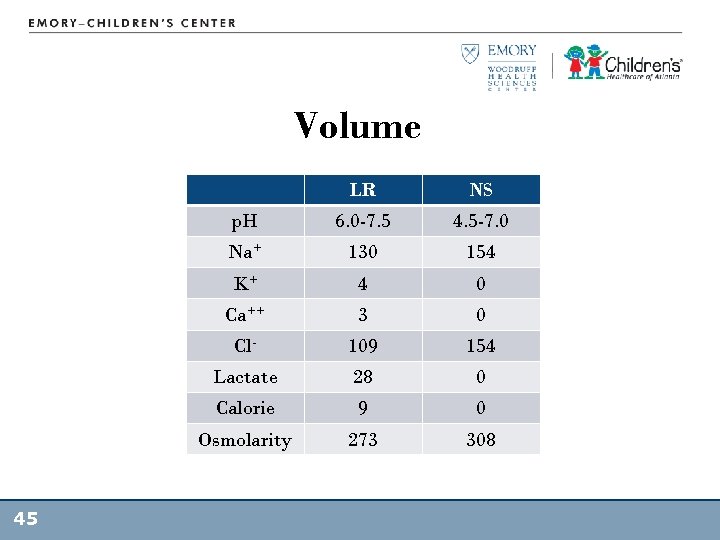
Volume LR p. H 6. 0 -7. 5 4. 5 -7. 0 Na+ 130 154 K+ 4 0 Ca++ 3 0 Cl- 109 154 Lactate 28 0 Calorie 9 0 Osmolarity 45 NS 273 308

Treatment: Volume • Volume resuscitation optimize preload • >60 ml/kg during 1 st hr associated with increase survival • Titrate volume to improve CO, normal HR, BP; improve perfusion/cap refill; improve UOP, MS – Carcillo JA, Fields AI. Clinical practice parameters for hemodynamic support of pediatric and neonatal patients in septic shock. Crit. Care Med. 2002; 30: 1365 -1378 46

Treatment: Volume • Retrospective review of 34 pts with septic shock & hypovolemia with 1 st hr fluid resuscitation – Group 1: – Group 2: – Group 3: up to 20 ml/kg 20 -40 ml/kg >40 mg/kg • No different in rate of ARDS – Carcillo JA, Davis AL, Zaritsky A, Role of early fluid resuscitation in pediatric septic shock. JAMA. 1991; 266: 1242 -1245 47

Treatment: Volume • Colloids – blood products – Trauma or DIC in septic shock – PRBC to help with oxygen carrying and delivery 48

PALS Shock Algorithm

Vasopressors 50

Adrenergic Receptors • α – subtype-1: vascular smooth muscle – Increase SVR, afterload • β – Myocardium, bronchial smooth muscle & vessels – β -1: increase HR & contractility – β -2: bronchodilation, peripheral vasodilation • Dopaminergic – renal, coronary, cerebral beds 51
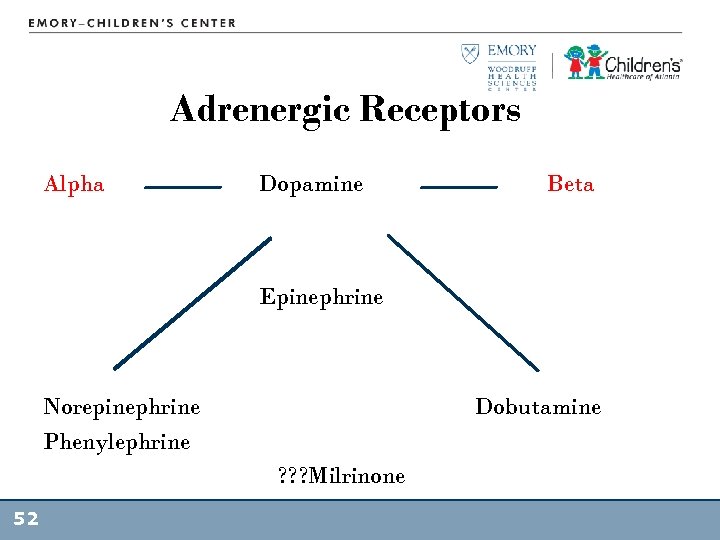
Adrenergic Receptors Alpha Dopamine Beta Epinephrine Norepinephrine Phenylephrine Dobutamine ? ? ? Milrinone 52

Dopamine • • Readily available, pre-mixed PIV up to 10 mcg/kg/min Start at 5 mcg/kg/min, titrate to effects Receptors – 2 -5 mcg/kg/min (renal) – D receptors – 5 -15 mcg/kg/min – β activity – >15 mcg/kg/min – α activity 53

Dopamine • No evidence to support low-dose (“renal” dose) • Evidence that suggests dopamine inhibits secretion of prolactin – Could increase lymphocyte apoptosis – Impairment of immune response to sepsis 54

Norepinephrine • Mostly α, minimum to no β activity increase SVR and after-load • Start at 0. 05 – 0. 1 mcg/kg/min (max 1 mcg/kg/min) • “Warm” septic shock • Avoid in myocardial dysfunction 55

Epinephrine • Mostly β with some α activity • Start at 0. 05 – 0. 1 mcg/kg/min (max 1 mcg/kg/min) • “Cold” septic shock – Improves contractility + vasoconstriction – Best drug for myocardial dysfunction 56

Phenylephrine • Pure α activity • Significantly increases SVR – May have reflex bradycardia • Spinal shock 57

Dobutamine • Mainly β-1; little β-2 and α activity • Increases contractility & HR increases myocardial oxygen consumption • Uses in cardiac patients 58

Milrinone • Phosphodiesterase-3 inhibitor • Increases intracellular Ca++ – Improves contractility – Decreases afterload – No increase in myocardial oxygen demand – Lusotropic: diastolic relaxation improve SV • Start 0. 3 – 0. 5 mcg/kg/min • Side effect: hypotension 59

Vasopressin • V-2 receptor: – Vasoconstriction mainly in the capillaries and small arterioles – Direct stimulation to pituitary gland ACTH production – Restores catecholamine sensitivity • Uses in catecholamine-resistant vasodilatory shock • 0. 01 – 0. 04 U/min 60
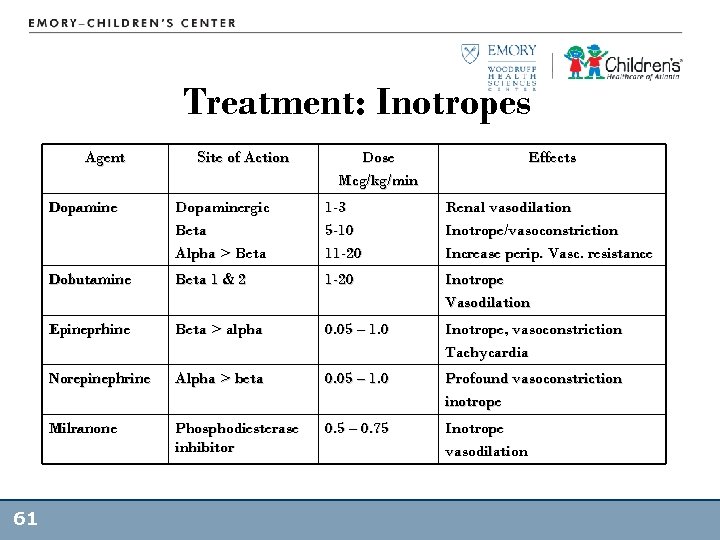

Treatment: Inotropes Agent Site of Action Dose Mcg/kg/min Effects Dopamine 1 -3 5 -10 11 -20 Renal vasodilation Inotrope/vasoconstriction Increase perip. Vasc. resistance Dobutamine Beta 1 & 2 1 -20 Inotrope Vasodilation Epineprhine Beta > alpha 0. 05 – 1. 0 Inotrope, vasoconstriction Tachycardia Norepinephrine Alpha > beta 0. 05 – 1. 0 Profound vasoconstriction inotrope Milranone 61 Dopaminergic Beta Alpha > Beta Phosphodiesterase inhibitor 0. 5 – 0. 75 Inotrope vasodilation
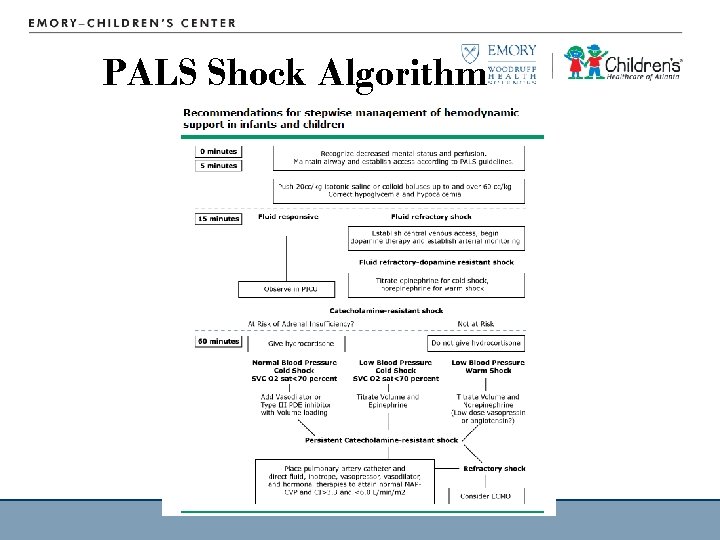
PALS Shock Algorithm

Therapy Monitoring • Central venous pressure – Intravascular volume – Goal 6 mmg. Hg (nl 4 -8 mm. Hg) • Mixed venous saturation (Sv. O 2) – Goal >70% (nl 65 -70%) – Indicate oxygen extraction by the tissues – Best obtained from CVL: SC or IJ • Lactate clearance: indication of anaerobic metabolism – >10% – Follow trends 63

Adrenal Insufficiency • Common occurrence in sepsis – Use of Etomidate for intubation – Chronic steroid use • 2 forms of insufficiency – Absolute: random cortisol <10 – Relative: ∆ <9 • Tx: Hydrocortisone – Load: 100 mg/m 2 – Maintenance: 25 mg/m 2 Q 6 x 7 days 64

Treatment: Steroids • No pediatric study • Adult studies – hydrocortisone controversy over 28 -day mortality • International guidelines for management of severe sepsis & septic shock: Surviving Sepsis Campaign • 65 http: //www. learnicu. org/Site. Collection. Documents/Guideline. Hemodynamic. Supp ort. pdf

Summary • Shock is a dynamic & unstable physiologic state that results in inadequate tissue perfusion – High morbidity and mortality • Tachycardia is the early sign • Hypotension is a very late sign • Early & aggressive treatment during the “golden hour” improves outcomes 66

References 1. 2. 3. 4. 5. 6. 7. Fleegler, E. and M. Kleinman. Guidelines for pediatric advanced life support. Uptodate. com, last updated Oct 14, 2009. Carcillo, JA et al. Goal-directed management of pediatric shock in the emergency department. Clinical Pediatric Emergency Medicine: Vol 8; 3; 165 -175. Dellinger, RP et al. Surviving Sepsis Campaign: international guidelines for management of severe sepsis and septic shock: 2008. Intensive Care Medicine: Vol 34; 1; 17 -60. Han, YY et al. Early reversal of pediatric-neonatal septic shock by community physicians is associated with improved outcome. Pediatrics: Vol 112; 4; 793 -799. Mc. Kiernan, CA and SA Lieberman. Circulatory Shock in Children. Pediatrics in Review 2005; 26; 451 -460. Pomerantz, W. and M. Roback. Physiology and classification of shock in children. Uptodate. com, last updated Aug 21, 2007. Waltzman, M. Initial management of shock in children. Uptodate. com, last updated May 11, 2010.
2b19afdeffab6f99ad430cf48c5fad54.ppt