86e36b1a4cd20efd98083aa855e75a34.ppt
- Количество слайдов: 96
 A Lady With Confusion Dr Sinn Ting, Maria AC, Department of Medicine Tseung Kwan O Hospital
A Lady With Confusion Dr Sinn Ting, Maria AC, Department of Medicine Tseung Kwan O Hospital
 • F/ 34, F. 6 teacher • Good past health • Presented with fever and flu-like symptoms for 1 week on 17/11/07 • On and off memory loss for 1 week • No headache, no nausea/vomiting • No recent travel/ vaccination
• F/ 34, F. 6 teacher • Good past health • Presented with fever and flu-like symptoms for 1 week on 17/11/07 • On and off memory loss for 1 week • No headache, no nausea/vomiting • No recent travel/ vaccination
 • P/E: Temp 37. 5 C • GCS 15, neck soft, no focal neurological sign • Chest, CV, abdomen: unremarkable • CXR: clear • WBC: 2. 8(N : 56%, L: 30%, M: 1%, atypical lymphocytes: 13%)
• P/E: Temp 37. 5 C • GCS 15, neck soft, no focal neurological sign • Chest, CV, abdomen: unremarkable • CXR: clear • WBC: 2. 8(N : 56%, L: 30%, M: 1%, atypical lymphocytes: 13%)
 Progress • Shortly after admission: developed L sided and then generalized tonic- clonic convulsion, aborted by valium. • Urgent CT brain : NAD • LP: – – clear CSF, opening pressure: 15 cm H 2 O CSF: WBC 6 /mm 3; RBC 3/ mm 3, CSF protein 0. 32 g/L, CSF glucose 3. 3 mmol/L( serum 8. 4) CSF: -ve culture for bacteria/AFB/fungus, viral titre for HSV, VZV <1: 4, PCR for HSV – ve • Blood culture -ve
Progress • Shortly after admission: developed L sided and then generalized tonic- clonic convulsion, aborted by valium. • Urgent CT brain : NAD • LP: – – clear CSF, opening pressure: 15 cm H 2 O CSF: WBC 6 /mm 3; RBC 3/ mm 3, CSF protein 0. 32 g/L, CSF glucose 3. 3 mmol/L( serum 8. 4) CSF: -ve culture for bacteria/AFB/fungus, viral titre for HSV, VZV <1: 4, PCR for HSV – ve • Blood culture -ve
 • Patient was initially given Pen G, cefotaxime, acyclovir, • Dilantin iv was given. • On and off agitation, memory deficit.
• Patient was initially given Pen G, cefotaxime, acyclovir, • Dilantin iv was given. • On and off agitation, memory deficit.
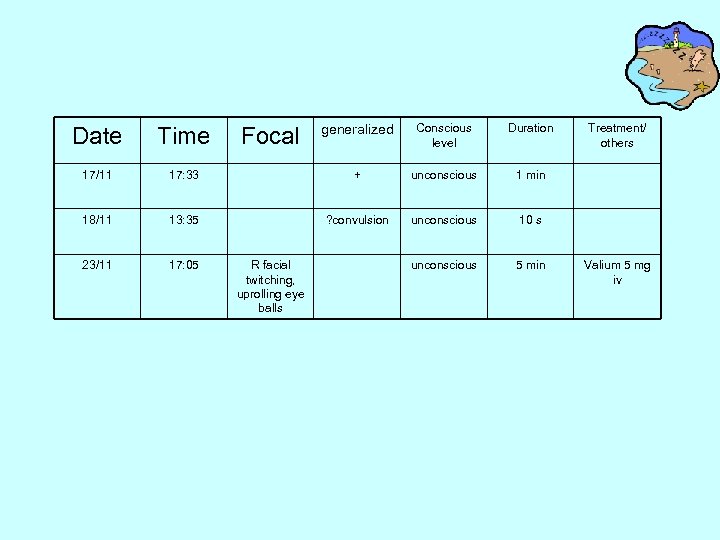 generalized Conscious level Duration 17: 33 + unconscious 1 min 18/11 13: 35 ? convulsion unconscious 10 s 23/11 17: 05 unconscious 5 min Date Time 17/11 Focal R facial twitching, uprolling eye balls Treatment/ others Valium 5 mg iv
generalized Conscious level Duration 17: 33 + unconscious 1 min 18/11 13: 35 ? convulsion unconscious 10 s 23/11 17: 05 unconscious 5 min Date Time 17/11 Focal R facial twitching, uprolling eye balls Treatment/ others Valium 5 mg iv
 • EEG 19/11/07: – 2 episodes of subclinical seizure captured of which there is some subtle bilateral UL motor automatism in the second. The origin is from L temporal region (or both). • Impression: In the context of clinical presentation (fever, headache, viral prodrome), herpes simplex encephalitis complicated with temporal lobe epilepsy is strongly suspected. Suggest book MRI brain.
• EEG 19/11/07: – 2 episodes of subclinical seizure captured of which there is some subtle bilateral UL motor automatism in the second. The origin is from L temporal region (or both). • Impression: In the context of clinical presentation (fever, headache, viral prodrome), herpes simplex encephalitis complicated with temporal lobe epilepsy is strongly suspected. Suggest book MRI brain.
 • MRI 21/11/07: • Bilateral asymmetrical brain edema is noted at the medial temporal lobes, more extensive on left side with abnormal contrast enhancement. The overall features are consistent with encephalitis which could account for the present seizure.
• MRI 21/11/07: • Bilateral asymmetrical brain edema is noted at the medial temporal lobes, more extensive on left side with abnormal contrast enhancement. The overall features are consistent with encephalitis which could account for the present seizure.
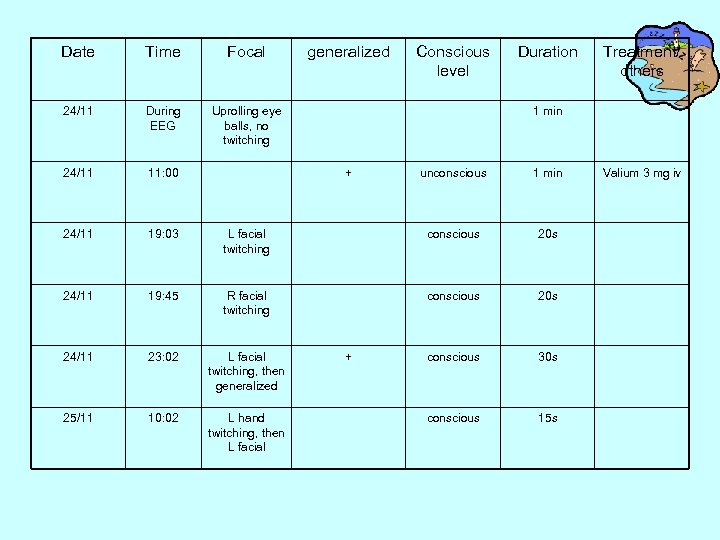 Date Time Focal 24/11 During EEG Uprolling eye balls, no twitching 24/11 11: 00 24/11 19: 03 24/11 generalized Conscious level Duration Treatment/ others 1 min + unconscious 1 min L facial twitching conscious 20 s 19: 45 R facial twitching conscious 20 s 24/11 23: 02 L facial twitching, then generalized conscious 30 s 25/11 10: 02 L hand twitching, then L facial conscious 15 s + Valium 3 mg iv
Date Time Focal 24/11 During EEG Uprolling eye balls, no twitching 24/11 11: 00 24/11 19: 03 24/11 generalized Conscious level Duration Treatment/ others 1 min + unconscious 1 min L facial twitching conscious 20 s 19: 45 R facial twitching conscious 20 s 24/11 23: 02 L facial twitching, then generalized conscious 30 s 25/11 10: 02 L hand twitching, then L facial conscious 15 s + Valium 3 mg iv
 • EEG 24/11/07: – there is an episode of secondarily generalized seizure originated from L hemisphere. The semiology: the patient had initially head intermittent turn to R and R hand automatism(pronate and supinate) and lasted for 2 -3 mins, then going to GTC ( the paroxymal of spike/ fast activity lasts for 1. 5 mins)preceded by forceful head version to R. – Active interictal discharges from R centroparietal region.
• EEG 24/11/07: – there is an episode of secondarily generalized seizure originated from L hemisphere. The semiology: the patient had initially head intermittent turn to R and R hand automatism(pronate and supinate) and lasted for 2 -3 mins, then going to GTC ( the paroxymal of spike/ fast activity lasts for 1. 5 mins)preceded by forceful head version to R. – Active interictal discharges from R centroparietal region.
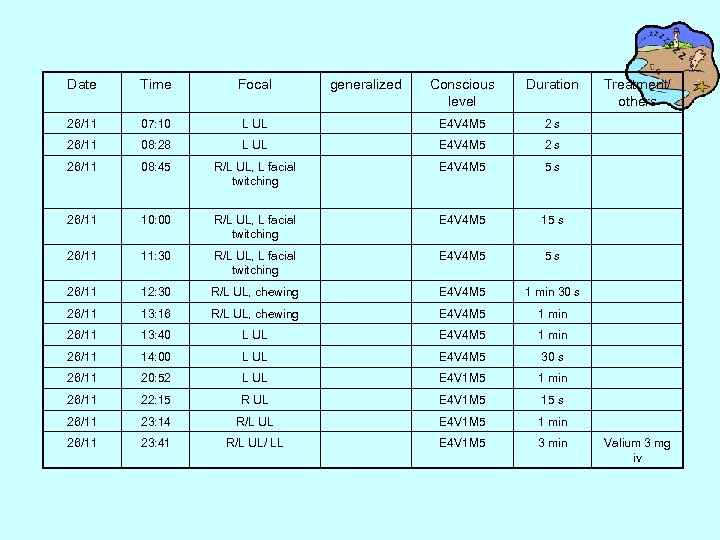 Date Time Focal 26/11 07: 10 26/11 generalized Conscious level Duration L UL E 4 V 4 M 5 2 s 08: 28 L UL E 4 V 4 M 5 2 s 26/11 08: 45 R/L UL, L facial twitching E 4 V 4 M 5 5 s 26/11 10: 00 R/L UL, L facial twitching E 4 V 4 M 5 15 s 26/11 11: 30 R/L UL, L facial twitching E 4 V 4 M 5 5 s 26/11 12: 30 R/L UL, chewing E 4 V 4 M 5 1 min 30 s 26/11 13: 16 R/L UL, chewing E 4 V 4 M 5 1 min 26/11 13: 40 L UL E 4 V 4 M 5 1 min 26/11 14: 00 L UL E 4 V 4 M 5 30 s 26/11 20: 52 L UL E 4 V 1 M 5 1 min 26/11 22: 15 R UL E 4 V 1 M 5 15 s 26/11 23: 14 R/L UL E 4 V 1 M 5 1 min 26/11 23: 41 R/L UL/ LL E 4 V 1 M 5 3 min Treatment/ others Valium 3 mg iv
Date Time Focal 26/11 07: 10 26/11 generalized Conscious level Duration L UL E 4 V 4 M 5 2 s 08: 28 L UL E 4 V 4 M 5 2 s 26/11 08: 45 R/L UL, L facial twitching E 4 V 4 M 5 5 s 26/11 10: 00 R/L UL, L facial twitching E 4 V 4 M 5 15 s 26/11 11: 30 R/L UL, L facial twitching E 4 V 4 M 5 5 s 26/11 12: 30 R/L UL, chewing E 4 V 4 M 5 1 min 30 s 26/11 13: 16 R/L UL, chewing E 4 V 4 M 5 1 min 26/11 13: 40 L UL E 4 V 4 M 5 1 min 26/11 14: 00 L UL E 4 V 4 M 5 30 s 26/11 20: 52 L UL E 4 V 1 M 5 1 min 26/11 22: 15 R UL E 4 V 1 M 5 15 s 26/11 23: 14 R/L UL E 4 V 1 M 5 1 min 26/11 23: 41 R/L UL/ LL E 4 V 1 M 5 3 min Treatment/ others Valium 3 mg iv
 • EEG 26/11/07: – compared with last EEG, the focus of interictal activity shifted to L occipital. One episode of secondarily generalized seizure captured originated from R hemisphere( last for 1. 5 min). • Impression: multi-focal epilepsy(typical finding of post-encephalitic epilepsy)
• EEG 26/11/07: – compared with last EEG, the focus of interictal activity shifted to L occipital. One episode of secondarily generalized seizure captured originated from R hemisphere( last for 1. 5 min). • Impression: multi-focal epilepsy(typical finding of post-encephalitic epilepsy)
 Literature Review : Part A
Literature Review : Part A
 1. Is it a case of status epilepticus?
1. Is it a case of status epilepticus?
 What is SE ? • In 1962, the tenth European Conference on Epileptology and Clinical Neurophysiology defined SE as ‘a condition characterized by an epileptic seizure which is so frequently repeated or so prolonged as to create a fixed and lasting epileptic condition’. • The International Classification of Epileptic Seizures: an seizure lasting more than 30 mins or intermittent seizures from which the patient did not regain consciousness lasting for more than 30 mins.
What is SE ? • In 1962, the tenth European Conference on Epileptology and Clinical Neurophysiology defined SE as ‘a condition characterized by an epileptic seizure which is so frequently repeated or so prolonged as to create a fixed and lasting epileptic condition’. • The International Classification of Epileptic Seizures: an seizure lasting more than 30 mins or intermittent seizures from which the patient did not regain consciousness lasting for more than 30 mins.
 • Treiman and colleagues defined overt convulsive SE as two or more generalized convulsions without full recovery of consciousness between seizures, or continuous convulsive activity for more than 10 mins. • Veterans Affairs Status Epilepticus Coorperative Study Group. NEJM 1998; 339: 792 -8. • Lowenstein, Bleck, and Macdonald : a continuous, generalized seizure lasting greater than 5 mins( in an adult or child older than 5 years), or two or more seizures and the patient did not return to baseline consciousness.
• Treiman and colleagues defined overt convulsive SE as two or more generalized convulsions without full recovery of consciousness between seizures, or continuous convulsive activity for more than 10 mins. • Veterans Affairs Status Epilepticus Coorperative Study Group. NEJM 1998; 339: 792 -8. • Lowenstein, Bleck, and Macdonald : a continuous, generalized seizure lasting greater than 5 mins( in an adult or child older than 5 years), or two or more seizures and the patient did not return to baseline consciousness.
 Nonconvulsive SE (NCSE) • NCSE constitutes 25 -50% of all cases of status epilepticus. • Represents a prolonged state of seizure(s) without marked motor manifestations. • NCSE typically encompasses an ictal impairment of cognition, subtle facial or limb twitches, eyeopen mutism, head or eye deviation, automatisms, and behavioral change.
Nonconvulsive SE (NCSE) • NCSE constitutes 25 -50% of all cases of status epilepticus. • Represents a prolonged state of seizure(s) without marked motor manifestations. • NCSE typically encompasses an ictal impairment of cognition, subtle facial or limb twitches, eyeopen mutism, head or eye deviation, automatisms, and behavioral change.
 NCSE • No current universally accepted definitions of NCSE: – Cannot rely on clinical symptoms alone – Cannot rely simply on EEG criteria because there are no EEG patterns that are pathognomonic of NCSE, which can range from continuous ictal discharges to rhythmic and periodic patterns of undetermined significance. – Cannot based on duration alone either
NCSE • No current universally accepted definitions of NCSE: – Cannot rely on clinical symptoms alone – Cannot rely simply on EEG criteria because there are no EEG patterns that are pathognomonic of NCSE, which can range from continuous ictal discharges to rhythmic and periodic patterns of undetermined significance. – Cannot based on duration alone either
 NCSE • It can be defined as a condition with a prolonged state of impaired consiousness or altered sensorium associated with continuous paroxysmal activity or electrographic discharges on the EEG. • A heterogeneous disorder with varied etiology and several subtypes.
NCSE • It can be defined as a condition with a prolonged state of impaired consiousness or altered sensorium associated with continuous paroxysmal activity or electrographic discharges on the EEG. • A heterogeneous disorder with varied etiology and several subtypes.
 NCSE • Classification: – Age based: neonates, children, adults, elderly – According to etiology: acute brain injury, metabolic disorders, preexisting epilepsy with or without an epileptic encephalopathy. – Clinical classification based on International League Against Epilepsy : • Generalized NCSE: absence status, atypical absence, de novo late absence SE • Focal NCSE: simple partial, complex partial, subtle NCSE
NCSE • Classification: – Age based: neonates, children, adults, elderly – According to etiology: acute brain injury, metabolic disorders, preexisting epilepsy with or without an epileptic encephalopathy. – Clinical classification based on International League Against Epilepsy : • Generalized NCSE: absence status, atypical absence, de novo late absence SE • Focal NCSE: simple partial, complex partial, subtle NCSE
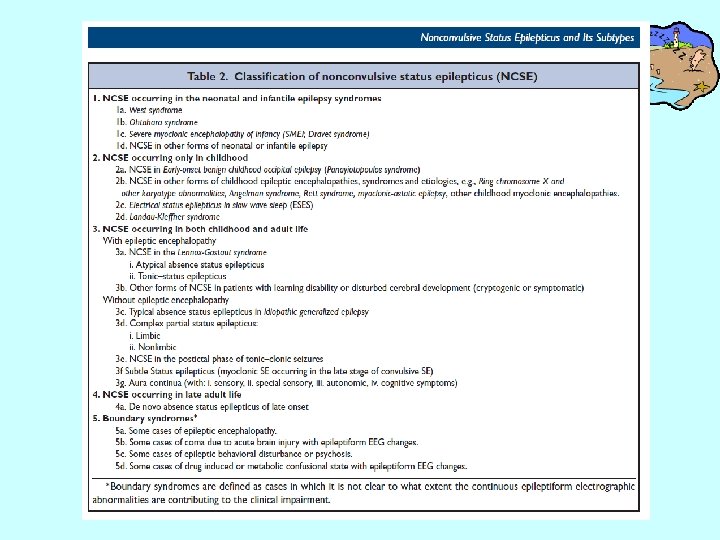

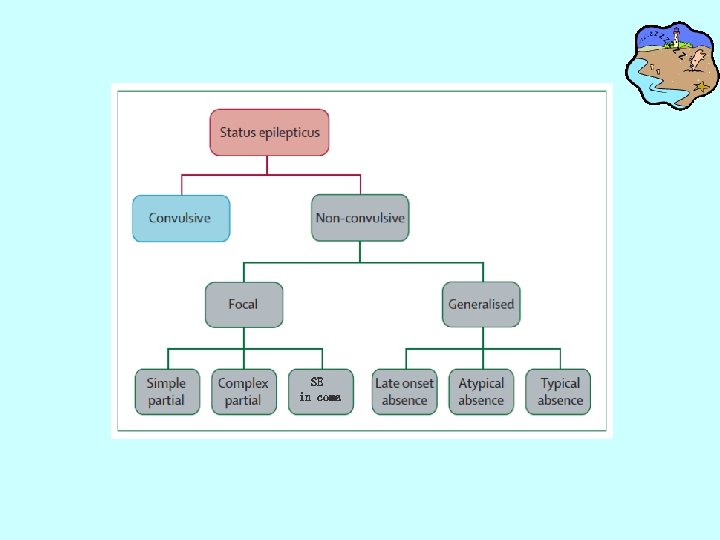 SE in coma
SE in coma
 2. Advances in the pathophysiology of status epilepticus
2. Advances in the pathophysiology of status epilepticus
 Pathophysiology of SE • 1. Excessive activation of excitatory amino acid receptors: – NMDA and AMPA glutamate receptors • 2. Reduction of GABA-mediated inhibition in the hippocampus – Prolonged seizures alter the GABAA receptor function( reduced potency and efficacy of GABA in activating chloride channels) • 3. Decrease in neuropeptides: – Neuropeptide Y – Gelanin
Pathophysiology of SE • 1. Excessive activation of excitatory amino acid receptors: – NMDA and AMPA glutamate receptors • 2. Reduction of GABA-mediated inhibition in the hippocampus – Prolonged seizures alter the GABAA receptor function( reduced potency and efficacy of GABA in activating chloride channels) • 3. Decrease in neuropeptides: – Neuropeptide Y – Gelanin
 Natural course of SE 3 distinct phases in clinical evolution: • 1. pseudo-status or impending SE • 2. convulsive status or established SE • 3. stuporous status or subtle SE • Clark and Prout. Status Epilepticus: a clinical and pathological study in epilepsy. Am J Insanity 1903; 60: 291306.
Natural course of SE 3 distinct phases in clinical evolution: • 1. pseudo-status or impending SE • 2. convulsive status or established SE • 3. stuporous status or subtle SE • Clark and Prout. Status Epilepticus: a clinical and pathological study in epilepsy. Am J Insanity 1903; 60: 291306.
 Basic Mechanisms Self-sustaining SE: • Human data shows that seizures lasting more than 30 min rarely stop spontaneously. • Animal study: after 30 min of intermittent stimulation of an excitatory glutaminergic pathway in the rat, stopping the stimulation no longer stops electrographic or behavioral seizures, which self-perpetuate for many hours and eventually become ‘subtle’
Basic Mechanisms Self-sustaining SE: • Human data shows that seizures lasting more than 30 min rarely stop spontaneously. • Animal study: after 30 min of intermittent stimulation of an excitatory glutaminergic pathway in the rat, stopping the stimulation no longer stops electrographic or behavioral seizures, which self-perpetuate for many hours and eventually become ‘subtle’
 • Time-dependent pharmacoresistance: – Potency of benzodiazepines decrease 20 fold in 30 min of self-sustaining SE (SSSE). – Potency of phenytoin also decrease but at a slower rate. • NMDA blockers are not effective in the first 10 -15 min of seizure, but are effective later in the course of SSSE.
• Time-dependent pharmacoresistance: – Potency of benzodiazepines decrease 20 fold in 30 min of self-sustaining SE (SSSE). – Potency of phenytoin also decrease but at a slower rate. • NMDA blockers are not effective in the first 10 -15 min of seizure, but are effective later in the course of SSSE.
 • The initiation of SSSE can be easily blocked by many pharmacological agents which enhance inhibition or reduce excitation. • Once SSSE is established, it is effectively terminated by only a few agents, most of which inhibit glutaminergic neurotransmission.
• The initiation of SSSE can be easily blocked by many pharmacological agents which enhance inhibition or reduce excitation. • Once SSSE is established, it is effectively terminated by only a few agents, most of which inhibit glutaminergic neurotransmission.
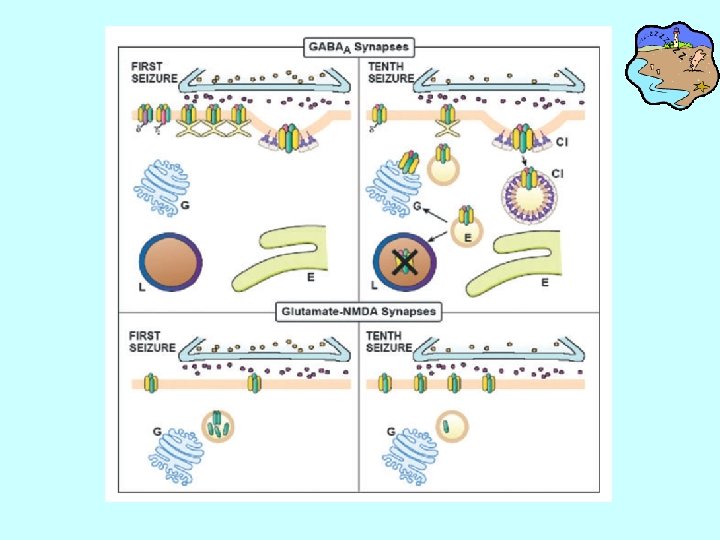
 Biochemical cascades of SSSE • In seconds to mins, GABA receptors move from the synaptic membrane to the cytoplasm, where they are functionally inactive: reducing the no. of GABAA receptors for binding GABA or GABAergic drugs. • At the same time, ‘spare’subunits of AMPA(alpha-amino-3 -hydroxy-5 -methyl-4 -isoxazolepropionic acid) and NMDA(N-methyl-D-aspartic acid) receptors move from subsynaptic sites to the synaptic membrane, causing further hyperexcitability and explaining the preserved sensitivity to NMDA blockers late in the course of SE. • In mins to hours, increase the expression of proconvulsive neuropeptides and decrease the availability of inhibitory neuropeptides: this maintains enhanced excitability.
Biochemical cascades of SSSE • In seconds to mins, GABA receptors move from the synaptic membrane to the cytoplasm, where they are functionally inactive: reducing the no. of GABAA receptors for binding GABA or GABAergic drugs. • At the same time, ‘spare’subunits of AMPA(alpha-amino-3 -hydroxy-5 -methyl-4 -isoxazolepropionic acid) and NMDA(N-methyl-D-aspartic acid) receptors move from subsynaptic sites to the synaptic membrane, causing further hyperexcitability and explaining the preserved sensitivity to NMDA blockers late in the course of SE. • In mins to hours, increase the expression of proconvulsive neuropeptides and decrease the availability of inhibitory neuropeptides: this maintains enhanced excitability.
 3. Use of anticonvulsants in status epilepticus: best current evidences
3. Use of anticonvulsants in status epilepticus: best current evidences
 Anticonvulsants • First- line : benzodiazepines (diazepam, lorazepam) • Second-line: phenytoin/ fosphenytoin, valproic acid, phenobarbital • RSE: iv anaesthetics : midazolam, propofol, barbiturates( thiopental, pentobarbital); inhalational anaesthetics(isoflurane, desflurane); nonanaesthetic: topiramate and levetiracetam.
Anticonvulsants • First- line : benzodiazepines (diazepam, lorazepam) • Second-line: phenytoin/ fosphenytoin, valproic acid, phenobarbital • RSE: iv anaesthetics : midazolam, propofol, barbiturates( thiopental, pentobarbital); inhalational anaesthetics(isoflurane, desflurane); nonanaesthetic: topiramate and levetiracetam.
 Diazepam • Mech: as with other benzodiazepines, it increase chloride conductance in CNS GABA-A receptors and thus decreasing neuronal excitability • 0. 1 -0. 3 mg/kg iv • Onset : 10 -20 s. • Duration : < 20 mins.
Diazepam • Mech: as with other benzodiazepines, it increase chloride conductance in CNS GABA-A receptors and thus decreasing neuronal excitability • 0. 1 -0. 3 mg/kg iv • Onset : 10 -20 s. • Duration : < 20 mins.
 Lorazepam • 0. 02 - 0. 2 mg/kg iv • Peak effect: 2 mins • Duration of anti-seizure effect: 12 -24 hours
Lorazepam • 0. 02 - 0. 2 mg/kg iv • Peak effect: 2 mins • Duration of anti-seizure effect: 12 -24 hours
 Phenytoin • Loading dose of 18 -20 mg/kg • Infused at a rate of up to 50 mg/min • If necessary, an additional 10 mg/kg can be given. • The risk of hypotension and cardiac arrhythmias increase with higher infusion rates, partly due to propylene glycol used to solubilize phenytoin.
Phenytoin • Loading dose of 18 -20 mg/kg • Infused at a rate of up to 50 mg/min • If necessary, an additional 10 mg/kg can be given. • The risk of hypotension and cardiac arrhythmias increase with higher infusion rates, partly due to propylene glycol used to solubilize phenytoin.
 Fosphenytoin • Phosphate ester pro-drug of phenytoin that is hydrolyzed into phenytoin by serum phosphatases within 8 -15 mins. • Water soluble and can be infused at rate up to 150 mg/min • Despite this rapid administration, no clear evidence that fosphenytoin stops SE faster than phenytoin. • Cardiovascular side effects may be less frequent as there is no propylene glycol.
Fosphenytoin • Phosphate ester pro-drug of phenytoin that is hydrolyzed into phenytoin by serum phosphatases within 8 -15 mins. • Water soluble and can be infused at rate up to 150 mg/min • Despite this rapid administration, no clear evidence that fosphenytoin stops SE faster than phenytoin. • Cardiovascular side effects may be less frequent as there is no propylene glycol.
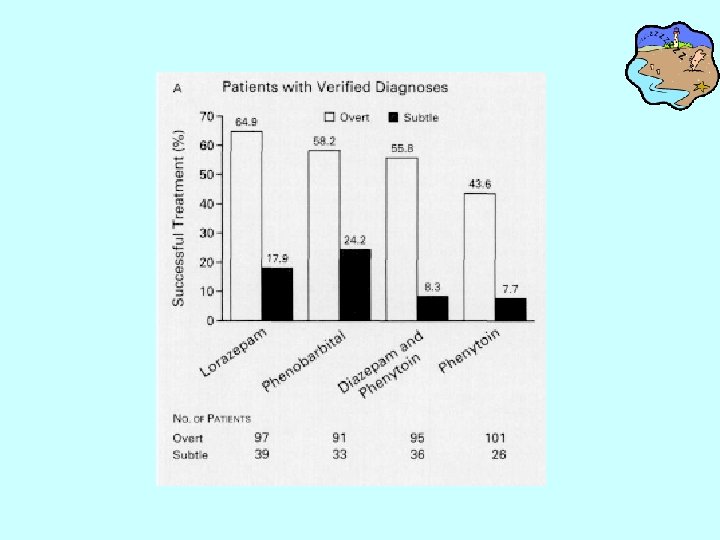
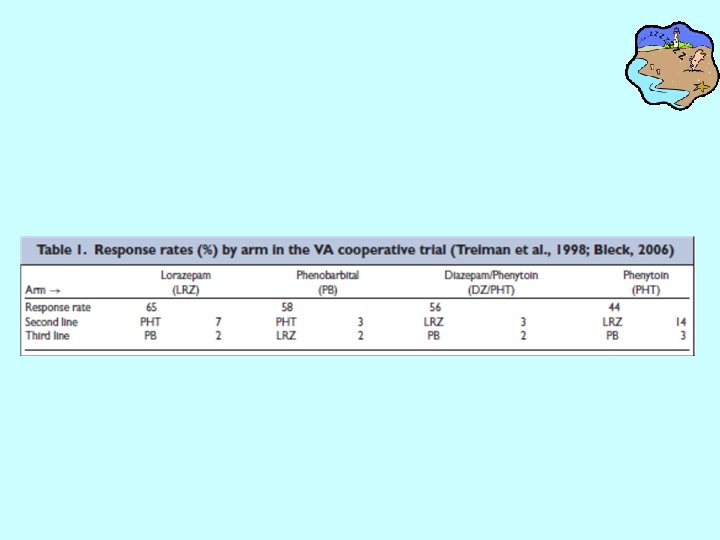
 A Comparison of four treatments for generalized convulsive SE A five-year randomized, double-blind, multicenter trial of four iv regimens in 518 patients with generalized convulsive SE( overt or subtle): • 1. diazepam(0. 15 mg/kg) followed by phenytoin(18 mg/kg), • 2. lorazepam(0. 1 mg/kg) • 3. phenobarbital (15 mg/kg) • 4. phenytoin(18 mg/kg) – Treiman et al. Veterans Affairs Status Epilepticus Cooperative Study. NEJM 1998; 339: 792 -8
A Comparison of four treatments for generalized convulsive SE A five-year randomized, double-blind, multicenter trial of four iv regimens in 518 patients with generalized convulsive SE( overt or subtle): • 1. diazepam(0. 15 mg/kg) followed by phenytoin(18 mg/kg), • 2. lorazepam(0. 1 mg/kg) • 3. phenobarbital (15 mg/kg) • 4. phenytoin(18 mg/kg) – Treiman et al. Veterans Affairs Status Epilepticus Cooperative Study. NEJM 1998; 339: 792 -8
 Lorazepam vs diazepam in SE • RCT, 78 patients • Time of onset was almost the same. • Seizures were controlled in 89 % of the episodes treated with lorazepam and in 76 % treated with diazepam. – Leppik IE. JAMA 1983; 249: 1452 -4.
Lorazepam vs diazepam in SE • RCT, 78 patients • Time of onset was almost the same. • Seizures were controlled in 89 % of the episodes treated with lorazepam and in 76 % treated with diazepam. – Leppik IE. JAMA 1983; 249: 1452 -4.
 Valproic acid • Mech: broad-spectrum, modulate sodium and calcium channels, as well as inhibitory GABA transmission. • iv valporic acid has been advocated as a first-line agent for absence SE and a second-line agent for generalized or partial SE.
Valproic acid • Mech: broad-spectrum, modulate sodium and calcium channels, as well as inhibitory GABA transmission. • iv valporic acid has been advocated as a first-line agent for absence SE and a second-line agent for generalized or partial SE.
 Valproic acid • Currently there are 20 published studies(7 prospective and 13 retrospective)including 533 adults or children. These studies suggest that iv valproate is as effective as phenytoin/frosphenytoin in resolving SE in patients who have previously failed conventional first-line therapies such as benzodiazepines. • The most commonly reported effective doses were between 15 and 45 mg/kg in bolus(6 mg/kg/hr) followed by 5 mg/kg/hr infusion. • The incidence of adverse events(mainly hypotension, dizziness, and thrombocytopenia) was low(< 10%) and independent of infusion rate. Lower risk of respiratory suppression.
Valproic acid • Currently there are 20 published studies(7 prospective and 13 retrospective)including 533 adults or children. These studies suggest that iv valproate is as effective as phenytoin/frosphenytoin in resolving SE in patients who have previously failed conventional first-line therapies such as benzodiazepines. • The most commonly reported effective doses were between 15 and 45 mg/kg in bolus(6 mg/kg/hr) followed by 5 mg/kg/hr infusion. • The incidence of adverse events(mainly hypotension, dizziness, and thrombocytopenia) was low(< 10%) and independent of infusion rate. Lower risk of respiratory suppression.
 Phenobarbital • Mech: depresses neuronal excitability by enhancing the GABA receptor-coupled response • Loading doses of 15 -20 mg/kg infused at a rate of 30 -50 mg/min. An additional 10 mg/kg can be given if needed. • Adverse effects: hypotension via vasodilation and cardiac depression, hypoventilation, risk of prolonged sedation (half-life of 87 -100 hours).
Phenobarbital • Mech: depresses neuronal excitability by enhancing the GABA receptor-coupled response • Loading doses of 15 -20 mg/kg infused at a rate of 30 -50 mg/min. An additional 10 mg/kg can be given if needed. • Adverse effects: hypotension via vasodilation and cardiac depression, hypoventilation, risk of prolonged sedation (half-life of 87 -100 hours).
 Refractory status epileptics • Exact definition is unclear. • Different studies defining RSE with varying durations ( no time criteria, 30 mins, 1 hour, or 2 hours) and a lack of response to different numbers( two or three) and types of medications.
Refractory status epileptics • Exact definition is unclear. • Different studies defining RSE with varying durations ( no time criteria, 30 mins, 1 hour, or 2 hours) and a lack of response to different numbers( two or three) and types of medications.
 Midazolam • Mech: positive allosteric modulation of GABA-A receptors( fast, chloride channels) which suppresses neuronal excitability. • Bolus of 0. 2 mg/kg, followed by a continuous infusion of 0. 05 -0. 5 mg/kg/hr.
Midazolam • Mech: positive allosteric modulation of GABA-A receptors( fast, chloride channels) which suppresses neuronal excitability. • Bolus of 0. 2 mg/kg, followed by a continuous infusion of 0. 05 -0. 5 mg/kg/hr.
 Propofol • Alkyl-phenol GA • Mech: modulate GABA-A receptors. • Initial low-dose bolus of 1 -2 mg/kg, followed by an infusion of 1 -2 mg/kg/hr that is titrated as needed. Infusion rates up to 10 -12 mg/kg/hr may be required. • Hypotension requiring vasopressor administration occurs in 50 -70% of patients.
Propofol • Alkyl-phenol GA • Mech: modulate GABA-A receptors. • Initial low-dose bolus of 1 -2 mg/kg, followed by an infusion of 1 -2 mg/kg/hr that is titrated as needed. Infusion rates up to 10 -12 mg/kg/hr may be required. • Hypotension requiring vasopressor administration occurs in 50 -70% of patients.
 Propofol infusion syndrome: • Characterized by refractory metabolic acidosis, cardiac failure, rhadomyolysis , renal failure and sometimes death. • Occurs most often with prolonged(>48 hours) infusion at doses higher than 5 mg/kg/hr, severe head injury, lean mass, and concurrent use of catecholamines or steroids.
Propofol infusion syndrome: • Characterized by refractory metabolic acidosis, cardiac failure, rhadomyolysis , renal failure and sometimes death. • Occurs most often with prolonged(>48 hours) infusion at doses higher than 5 mg/kg/hr, severe head injury, lean mass, and concurrent use of catecholamines or steroids.
 Pentobarbital • Mech: depresses neuronal excitability by enhancing GABA receptor–coupled responses • First metabolite of thiopental • Compared with phenobarbital, pentobarbital has faster brain penetration (allowing faster control of seizures) a shorter half-life( allowing faster waking from coma) • Loading dose of 10 mg/kg infused at up to 100 mg/min, continuous infusion ranging from 1 -4 mg/kg/hour.
Pentobarbital • Mech: depresses neuronal excitability by enhancing GABA receptor–coupled responses • First metabolite of thiopental • Compared with phenobarbital, pentobarbital has faster brain penetration (allowing faster control of seizures) a shorter half-life( allowing faster waking from coma) • Loading dose of 10 mg/kg infused at up to 100 mg/min, continuous infusion ranging from 1 -4 mg/kg/hour.
 Pentobarbital • Associated with respiratory depression, myocardial depression, hypotension.
Pentobarbital • Associated with respiratory depression, myocardial depression, hypotension.
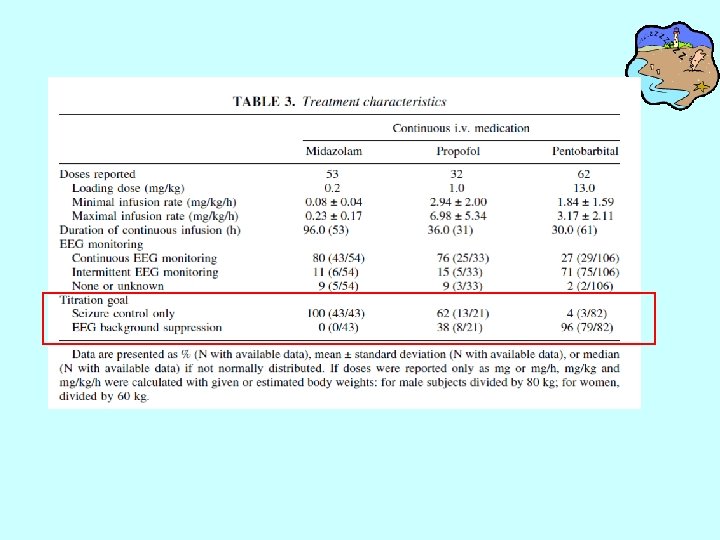
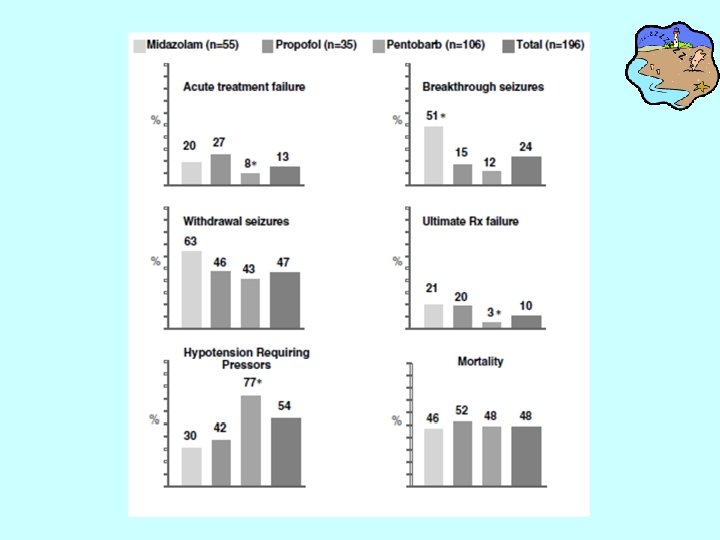
 • A meta-analysis of 28 articles that included 193 adults with RSE compared pentobarbital, midazolem, and propofol. • Pentobarbital was associated with a sig. lower incidence of short-term treatment failure, breakthrough seizures, and the need to change to a different medication, but was also associated with a sig higher f of hypotension. • However, patients treated with pentobarbital tended to be treated to the point of burst suppression, whereas those treated with midazolam or propofol tended to be treated to seizure suppression. – Claasen, Hirsch. Epildepsia 2002; 43: 146 -53.
• A meta-analysis of 28 articles that included 193 adults with RSE compared pentobarbital, midazolem, and propofol. • Pentobarbital was associated with a sig. lower incidence of short-term treatment failure, breakthrough seizures, and the need to change to a different medication, but was also associated with a sig higher f of hypotension. • However, patients treated with pentobarbital tended to be treated to the point of burst suppression, whereas those treated with midazolam or propofol tended to be treated to seizure suppression. – Claasen, Hirsch. Epildepsia 2002; 43: 146 -53.
 Thiopental • Recommended dose is 2 -4 mg /kg bolus, followed by infusion 3 -5 mg/kg/hr. Problems: • 1. higher incidence of adverse cardiovascular effects than pentobarbital. • 2. half-life of thiopental is shorter than that of pentobarbital, but thiopental is degraded to active metabolites(including pentobarbital), which accumulate with long term infusions. • 3. Immunosupressive effects on neutrophil function and mucociliary clearance.
Thiopental • Recommended dose is 2 -4 mg /kg bolus, followed by infusion 3 -5 mg/kg/hr. Problems: • 1. higher incidence of adverse cardiovascular effects than pentobarbital. • 2. half-life of thiopental is shorter than that of pentobarbital, but thiopental is degraded to active metabolites(including pentobarbital), which accumulate with long term infusions. • 3. Immunosupressive effects on neutrophil function and mucociliary clearance.
 Levetiracetam • Mech: multiple sites of action including calcium channels, glutamate receptors and GABA modulation. • iv , oral ( bioequivalent) • Not metabolized by liver, is renally excreted, has lowprotein binding and exhibits limited drug-drug interaction. • Dosage : 500 -3000 mg/day, controlled seizures in 12 -96 hours. • No significant adverse effects.
Levetiracetam • Mech: multiple sites of action including calcium channels, glutamate receptors and GABA modulation. • iv , oral ( bioequivalent) • Not metabolized by liver, is renally excreted, has lowprotein binding and exhibits limited drug-drug interaction. • Dosage : 500 -3000 mg/day, controlled seizures in 12 -96 hours. • No significant adverse effects.
 Topiramate • Mech: blockage of voltage-sensitive sodium and calcium channels, enhancement of GABA activity via modulation of the GABA-A receptor, and modulation of glutamate receptors • Because it exhibits mechanisms independent of GABA receptors, topiramate may be effective later in RSE, after GABA receptors have been targeted by other agent. • Broad spectrum of efficacy • Oral , effective doses range from 300 - 1600 mg/day • Except for lethargy, no adverse effects were reported.
Topiramate • Mech: blockage of voltage-sensitive sodium and calcium channels, enhancement of GABA activity via modulation of the GABA-A receptor, and modulation of glutamate receptors • Because it exhibits mechanisms independent of GABA receptors, topiramate may be effective later in RSE, after GABA receptors have been targeted by other agent. • Broad spectrum of efficacy • Oral , effective doses range from 300 - 1600 mg/day • Except for lethargy, no adverse effects were reported.
 Inhaled anesthetics • Isoflurane, desflurane • Mech: potentiation of inhibitory postsynaptic GABA-A receptor. • In endtidal concentrations of 1. 2 -5 %. • S/E: hypotension, atelectasis, paralytic ileus and DVT • ? As ‘last resort’
Inhaled anesthetics • Isoflurane, desflurane • Mech: potentiation of inhibitory postsynaptic GABA-A receptor. • In endtidal concentrations of 1. 2 -5 %. • S/E: hypotension, atelectasis, paralytic ileus and DVT • ? As ‘last resort’
 Ketamine • Non-competitive N-methyl-D-aspartate glutamate (NMDA)receptor antagonist • Animal models demonstrated a late(at 1 hour) but not early (at 15 mins) efficacy of ketamine, implying that before receptor changes occur, it will be ineffective. • Ketamine may be neuroprotective by reducing NMDA receptor-mediated excitotoxic injury.
Ketamine • Non-competitive N-methyl-D-aspartate glutamate (NMDA)receptor antagonist • Animal models demonstrated a late(at 1 hour) but not early (at 15 mins) efficacy of ketamine, implying that before receptor changes occur, it will be ineffective. • Ketamine may be neuroprotective by reducing NMDA receptor-mediated excitotoxic injury.
 Ketamine • It was associated with improved cerebral perfusion by increasing blood pressure because of its sympathomimetic properties. • It may be as useful adjuvant in the treatment of RSE, esp in late stages when medications that rely on GABA enhancement are ineffective. • Further study is needed to determine the optimal dosing, timing of administration.
Ketamine • It was associated with improved cerebral perfusion by increasing blood pressure because of its sympathomimetic properties. • It may be as useful adjuvant in the treatment of RSE, esp in late stages when medications that rely on GABA enhancement are ineffective. • Further study is needed to determine the optimal dosing, timing of administration.
 4. NCSE: how aggressive is the treatment?
4. NCSE: how aggressive is the treatment?
 NCSE • No systemic prospective trials examining different treatment outcomes : – NCSE is a heterogeneous disease with multiple subtypes – No definition of NCSE that are universally accepted.
NCSE • No systemic prospective trials examining different treatment outcomes : – NCSE is a heterogeneous disease with multiple subtypes – No definition of NCSE that are universally accepted.
 • Treatment has to be based on type and has to be individualized. • As most clinical forms of NCSE, with the exception of subtle SE, are not associated with acute systemic and chronic neurological complications, a less aggressive pharmacological management is suggested.
• Treatment has to be based on type and has to be individualized. • As most clinical forms of NCSE, with the exception of subtle SE, are not associated with acute systemic and chronic neurological complications, a less aggressive pharmacological management is suggested.
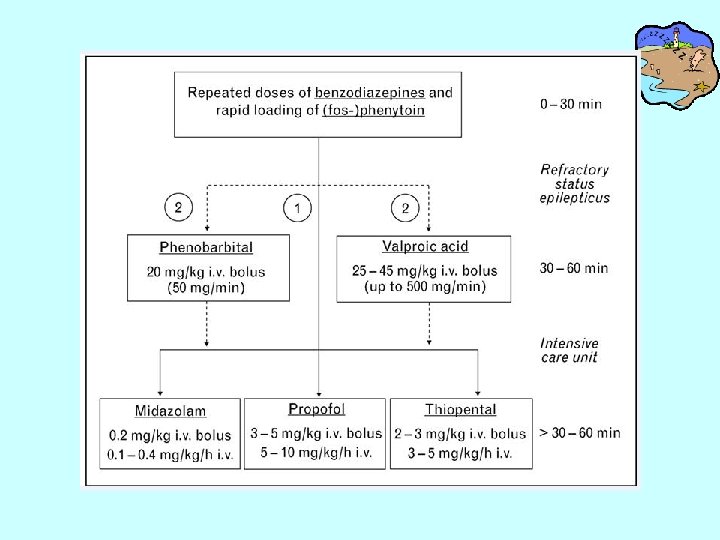
 NCSE subtypes: absence SE • 1. Absence SE : commonly treated successfully by iv diazepam or lorazepam. Eventually bolus iv valproic acid at 25 -45 mg/kg(6 mg/kg/min) or phenobarbital at 20 mg /kg(50 mg/kg/min) is recommended for persistent seizures.
NCSE subtypes: absence SE • 1. Absence SE : commonly treated successfully by iv diazepam or lorazepam. Eventually bolus iv valproic acid at 25 -45 mg/kg(6 mg/kg/min) or phenobarbital at 20 mg /kg(50 mg/kg/min) is recommended for persistent seizures.
 NCSE: SPSE and CPSE • 2. The response to initial drugs in SPSE and CPSE depends on whether the disorder occurs in patients with pre-existing epilepsy or in patients with de novo SE presumably due to acute or progressive systemic or CNS disorders. • In patients with a history of frontal or temporal lobe epilepsy, partial forms of SE responds rapidly to diazepam or lorazepam. If necessary phenytoin/ fosphenytoin is given. • De novo SPSE and CPSE are commonly refractory towards first-line treatment, therefore subsequent iv phenobarbital at 20 mg/kg or valproic acid at 25 -45 mg/kg should be administered.
NCSE: SPSE and CPSE • 2. The response to initial drugs in SPSE and CPSE depends on whether the disorder occurs in patients with pre-existing epilepsy or in patients with de novo SE presumably due to acute or progressive systemic or CNS disorders. • In patients with a history of frontal or temporal lobe epilepsy, partial forms of SE responds rapidly to diazepam or lorazepam. If necessary phenytoin/ fosphenytoin is given. • De novo SPSE and CPSE are commonly refractory towards first-line treatment, therefore subsequent iv phenobarbital at 20 mg/kg or valproic acid at 25 -45 mg/kg should be administered.
 NCSE: SPSE and CPSE • Caution should be taken with further treatment with iv anaesthetics. • Aggressive pharmacological treatment seems to have a greater risk on morbidity and mortality than continuing non-convulsive seizure activity. • Topiramate and levetiracetam may be successful in this disorder. • If complex partial SE cannot be terminated, generalized anaesthesia should be considered in the rare patients who are young and do not have additional medical problems. Treatment should be tailored for each patient.
NCSE: SPSE and CPSE • Caution should be taken with further treatment with iv anaesthetics. • Aggressive pharmacological treatment seems to have a greater risk on morbidity and mortality than continuing non-convulsive seizure activity. • Topiramate and levetiracetam may be successful in this disorder. • If complex partial SE cannot be terminated, generalized anaesthesia should be considered in the rare patients who are young and do not have additional medical problems. Treatment should be tailored for each patient.
 NCSE in coma • Non-convulsive seizures occur in as many as 19% of critically ill patients with altered mental status. • In obtunded or comatose patients, periodic or rhythmic patterns that do not clearly fall into the ‘ictal’ or ‘nonictal’ category predominate. • These patterns include rhythmic delta activity, generalized triphasic waves, periodic lateralizing epileptiform discharges(PLEDs), generalized periodic epileptiform discharges(GPEDs), bilaterally independent periodic lateralizing epileptiform discharges(BIPLEDs), and stimulus-induced, rhythmic, periodic, or ictal discharges (SIRPIDs).
NCSE in coma • Non-convulsive seizures occur in as many as 19% of critically ill patients with altered mental status. • In obtunded or comatose patients, periodic or rhythmic patterns that do not clearly fall into the ‘ictal’ or ‘nonictal’ category predominate. • These patterns include rhythmic delta activity, generalized triphasic waves, periodic lateralizing epileptiform discharges(PLEDs), generalized periodic epileptiform discharges(GPEDs), bilaterally independent periodic lateralizing epileptiform discharges(BIPLEDs), and stimulus-induced, rhythmic, periodic, or ictal discharges (SIRPIDs).
 • The field struggles to determine which patterns should be treated and how aggressively. • Non-coma inducing agents : iv (fos)phenytoin, valproate, intermittent benzodiazepines, levetiracetam and topiramate.
• The field struggles to determine which patterns should be treated and how aggressively. • Non-coma inducing agents : iv (fos)phenytoin, valproate, intermittent benzodiazepines, levetiracetam and topiramate.
 Progress • Patient was transferred to ICU for close monitoring on 24/11/07. • Epilim iv was added. • Repeated episodes of focal twitching involving R/L UL, face, triggered by surrounding people and conversation. • Tegretol was added on 27/11/07 after neurologist’s assessment, also suggested to repeat LP.
Progress • Patient was transferred to ICU for close monitoring on 24/11/07. • Epilim iv was added. • Repeated episodes of focal twitching involving R/L UL, face, triggered by surrounding people and conversation. • Tegretol was added on 27/11/07 after neurologist’s assessment, also suggested to repeat LP.
 • Repeat LP on 27/11/08: – CSF: clear , opening pressure 15 cm. H 2 O, protein 0. 85 g/L, CSF glucose: 3. 8 mmol/L( serum: 6. 7), – CSF WBC 2/mm 3, RBC 3783/mm 3 – CSF: - ve for bacteria/AFB/yeast/viral culture/malig cells. PCR for HSV – ve • Repeat CT brain 27/11/07: NAD
• Repeat LP on 27/11/08: – CSF: clear , opening pressure 15 cm. H 2 O, protein 0. 85 g/L, CSF glucose: 3. 8 mmol/L( serum: 6. 7), – CSF WBC 2/mm 3, RBC 3783/mm 3 – CSF: - ve for bacteria/AFB/yeast/viral culture/malig cells. PCR for HSV – ve • Repeat CT brain 27/11/07: NAD
 • NPA x influenza A and B – ve • Weil-Felix, RPR, monospot, anti-HIV, viral titre (enterovirus, HSV, VZV, influenza A/B, Japanese encephalitis, mycoplasma pneumoniae) - ve , Rickettsial study – ve • Stool x viral study-ve • Blood culture – ve • Autoimmune markers: ANA, anti-ENA, ANCA –ve, C 3: 0. 73, C 4: 0. 2, anti-thyroglobulin Ab – ve • Serum copper, ceruloplasmin : normal • Tumor markers: CA 19 -9, AFP, CEA : N; CA 125 42 U/ml(N<21)
• NPA x influenza A and B – ve • Weil-Felix, RPR, monospot, anti-HIV, viral titre (enterovirus, HSV, VZV, influenza A/B, Japanese encephalitis, mycoplasma pneumoniae) - ve , Rickettsial study – ve • Stool x viral study-ve • Blood culture – ve • Autoimmune markers: ANA, anti-ENA, ANCA –ve, C 3: 0. 73, C 4: 0. 2, anti-thyroglobulin Ab – ve • Serum copper, ceruloplasmin : normal • Tumor markers: CA 19 -9, AFP, CEA : N; CA 125 42 U/ml(N<21)
 • EEG 28/11/07: – 2 episodes of secondarily generalized seizure activities captured. The semiology: initially head version to L side, then to R side, followed by eye staring and uprolling, subsequent oral automatism(lip smacking and chewing). Origin is from L side. Each episode lasted for > 2 mins. – Treated as status epilepticus in view of clinical observations of refractory seizure activity. • Clonazepam was added in view of her intractable condition.
• EEG 28/11/07: – 2 episodes of secondarily generalized seizure activities captured. The semiology: initially head version to L side, then to R side, followed by eye staring and uprolling, subsequent oral automatism(lip smacking and chewing). Origin is from L side. Each episode lasted for > 2 mins. – Treated as status epilepticus in view of clinical observations of refractory seizure activity. • Clonazepam was added in view of her intractable condition.
 • Patient was electively intubated on 29/11/07. • Propofol and midazolam infusion were started. • Continuous EEG: – Neurologist: not useful – Nurses: didn’t know how to read
• Patient was electively intubated on 29/11/07. • Propofol and midazolam infusion were started. • Continuous EEG: – Neurologist: not useful – Nurses: didn’t know how to read
 Literature Review : Part B
Literature Review : Part B
 5. Is continuous EEG really ‘not useful’ in this setting?
5. Is continuous EEG really ‘not useful’ in this setting?
 Continuous EEG monitor in ICU Potential problems: • 1. hardware: – System requirement should conform to parameters stipulated in ACNS guidelines – Drawback of limited no of electrodes
Continuous EEG monitor in ICU Potential problems: • 1. hardware: – System requirement should conform to parameters stipulated in ACNS guidelines – Drawback of limited no of electrodes
 Continuous EEG monitor in ICU • 2. Software: – Staffing: in many hospitals, EDU not provide continuous in-house EEG technologist coverage. – ? More active role by ICU nurse( to be trained in recognition of certain important EEG patterns)
Continuous EEG monitor in ICU • 2. Software: – Staffing: in many hospitals, EDU not provide continuous in-house EEG technologist coverage. – ? More active role by ICU nurse( to be trained in recognition of certain important EEG patterns)
 6. What is the end-point of our treatment?
6. What is the end-point of our treatment?
 Treatment goal? • Targeting EEG seizure suppression? • Treat to burst suppression? • Complete suppression of EEG activity?
Treatment goal? • Targeting EEG seizure suppression? • Treat to burst suppression? • Complete suppression of EEG activity?
 • A meta-analysis of 28 articles that included 193 adults with RSE: titration to EEG background suppression, compared with seizure suppression, resulted in sig fewer breakthrough seizures(4% vs 53%) but a sig higher f of hypotension(29% vs 76%. – Classen, Hirsch. Epilepsia 2002; 43: 146 -53.
• A meta-analysis of 28 articles that included 193 adults with RSE: titration to EEG background suppression, compared with seizure suppression, resulted in sig fewer breakthrough seizures(4% vs 53%) but a sig higher f of hypotension(29% vs 76%. – Classen, Hirsch. Epilepsia 2002; 43: 146 -53.
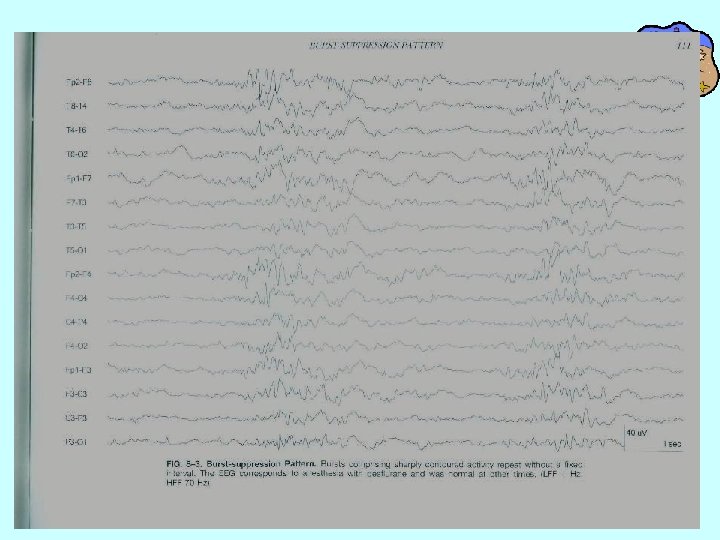
 • If burst suppression is preferred, the optimal degree of burst suppression is also unknown. • Most protocols suggest maintaining a coma for 24 -48 hours. • There are few data regarding the optimal rate of weaning, or the amount of seizure burden or number and types of epileptiform discharges that can be tolerated.
• If burst suppression is preferred, the optimal degree of burst suppression is also unknown. • Most protocols suggest maintaining a coma for 24 -48 hours. • There are few data regarding the optimal rate of weaning, or the amount of seizure burden or number and types of epileptiform discharges that can be tolerated.
 7. Is there other alternative to continuous EEG monitoring?
7. Is there other alternative to continuous EEG monitoring?
 Bispectral index(BIS) monitoring • A continuous processed EEG monitoring. • A sensor placed on the patient’s head transmits EEG signals to the BIS monitor. • Level of hypnosis: • 100= awake • 0= flat line • Could be used to detect non-convulsive seizures • Values >60 in comatose or deep sedate or paralyzed patient should alert the nurse or the physician to order an EEG for confirmation.
Bispectral index(BIS) monitoring • A continuous processed EEG monitoring. • A sensor placed on the patient’s head transmits EEG signals to the BIS monitor. • Level of hypnosis: • 100= awake • 0= flat line • Could be used to detect non-convulsive seizures • Values >60 in comatose or deep sedate or paralyzed patient should alert the nurse or the physician to order an EEG for confirmation.
 BIS monitoring • It is not a complete substitute for comprehensive EEG analysis. • It can be of use when formal EEG is unavailable.
BIS monitoring • It is not a complete substitute for comprehensive EEG analysis. • It can be of use when formal EEG is unavailable.
 Progress • In view of persistently –ve PCR HSV and intractable epilepsy, alternative dx : non-infectious/ autoimmune encephalitis. • Pulse methylprednisolone 1 g daily x 3 days was given 30/11 -2/12/07. • EEG 3/12/07: no epileptic activities. Mild to moderate non-epileptic cerebral dysfunction. • Patient was extubated on 3/12/07. • Discharged on 13/12/07.
Progress • In view of persistently –ve PCR HSV and intractable epilepsy, alternative dx : non-infectious/ autoimmune encephalitis. • Pulse methylprednisolone 1 g daily x 3 days was given 30/11 -2/12/07. • EEG 3/12/07: no epileptic activities. Mild to moderate non-epileptic cerebral dysfunction. • Patient was extubated on 3/12/07. • Discharged on 13/12/07.
 Neurology clinic • DDx : primary cranial angiitis, limbic encephalitis. – MRI and MRA brain: Improvement in signal change at L hippocampi, features might be due to resolving infection, ddx: resolving excitotoxic effect from previous status epilepticus. No evidence to suggest angiitis. – PET scan : no evidence of occult malignancy • Short term memory slightly impaired • Not capable of resuming job • Breakthrough seizures: 1 -2 x/week, major/minor attacks, triggered by noisy environment, usually preceded by auditory aura. • Currently on epilim, phenytoin, oxcarbazepine.
Neurology clinic • DDx : primary cranial angiitis, limbic encephalitis. – MRI and MRA brain: Improvement in signal change at L hippocampi, features might be due to resolving infection, ddx: resolving excitotoxic effect from previous status epilepticus. No evidence to suggest angiitis. – PET scan : no evidence of occult malignancy • Short term memory slightly impaired • Not capable of resuming job • Breakthrough seizures: 1 -2 x/week, major/minor attacks, triggered by noisy environment, usually preceded by auditory aura. • Currently on epilim, phenytoin, oxcarbazepine.
 Literature Review : Part C
Literature Review : Part C
 8. Limbic encephalitis • 1. Characterized by 3 features : – A core amnesic syndrome – Complex-partial and secondary-generalized seizures – Variable affective syndrome • 2. Associated with an isolated high signal in the mesial temporal lobes on MRI scan and histological inflammatory change in these areas.
8. Limbic encephalitis • 1. Characterized by 3 features : – A core amnesic syndrome – Complex-partial and secondary-generalized seizures – Variable affective syndrome • 2. Associated with an isolated high signal in the mesial temporal lobes on MRI scan and histological inflammatory change in these areas.
 Limbic encephalitis • 1 It is initially identified as a paraneoplastic phenomenon: occult small cell-bronchial CA ( ass with autoantibodies to Hu), testicular CA and thymoma ( ass with antibodies to CRMP 5/CV 2). • 2. In recent years, a non-paraneoplastic variant has been characterized( ass with voltage-gated potassium channel antibodies /VGKC-Ab)
Limbic encephalitis • 1 It is initially identified as a paraneoplastic phenomenon: occult small cell-bronchial CA ( ass with autoantibodies to Hu), testicular CA and thymoma ( ass with antibodies to CRMP 5/CV 2). • 2. In recent years, a non-paraneoplastic variant has been characterized( ass with voltage-gated potassium channel antibodies /VGKC-Ab)
 • Consistent with an underlying immunological cause, non-paraneoplastic and paraneoplastic types both respond to immunotherapies including iv steroids, immunoglobulins and plasma exchange.
• Consistent with an underlying immunological cause, non-paraneoplastic and paraneoplastic types both respond to immunotherapies including iv steroids, immunoglobulins and plasma exchange.
 Prognosis of limbic encephalitis • Case reports suggest: – residual cognitive deficits : disorders of memory, performance intelligence and executive function. – Affective and behavioral changes – seizures
Prognosis of limbic encephalitis • Case reports suggest: – residual cognitive deficits : disorders of memory, performance intelligence and executive function. – Affective and behavioral changes – seizures
 9. Prognosis of SE • 1. Underlying etiology is the predominant factor that determines outcome. • 2. Duration of status
9. Prognosis of SE • 1. Underlying etiology is the predominant factor that determines outcome. • 2. Duration of status
 Prognosis of SE • Mortality in patients with SE following brain anoxia is much higher than those due to low AED levels(71% vs 4 %). • In the Veterans Affairs Cooperation Study , outcome of subtle SE was significantly worse than that of overt GCSE, and mortality rates were 65 % and 27 %, respectively. • Absence SE does not appear to cause lasting effects and is not shown to be associated with increased mortality. • Other forms of NCSE, especially CPSE, have been shown to be associated with mortality.
Prognosis of SE • Mortality in patients with SE following brain anoxia is much higher than those due to low AED levels(71% vs 4 %). • In the Veterans Affairs Cooperation Study , outcome of subtle SE was significantly worse than that of overt GCSE, and mortality rates were 65 % and 27 %, respectively. • Absence SE does not appear to cause lasting effects and is not shown to be associated with increased mortality. • Other forms of NCSE, especially CPSE, have been shown to be associated with mortality.
 Majority of patients with CPSE are successfully treated without sequelae, even after several recurrences or a very long duration. Transient disturbances of memory, cognitive function, or personality are common but usually resolves after days to weeks.
Majority of patients with CPSE are successfully treated without sequelae, even after several recurrences or a very long duration. Transient disturbances of memory, cognitive function, or personality are common but usually resolves after days to weeks.
 Further direction for NCSE Non-convulsive status epilepticus (NCSE) is one of the great diagnostic and therapeutic challenges of modern neurology. Future works : 1. To standardize definition(s) for NCSE 2. To determine which EEG patterns clearly represent epileptogenicity which should be treated and how aggressively. 3. Further work should focus on the neuropsychological outcomes of the different subtypes of NCSE. 4. Prospective multicenter studies are needed to further determine the best treatment paradigms for NCSE among different age groups and etiologies.
Further direction for NCSE Non-convulsive status epilepticus (NCSE) is one of the great diagnostic and therapeutic challenges of modern neurology. Future works : 1. To standardize definition(s) for NCSE 2. To determine which EEG patterns clearly represent epileptogenicity which should be treated and how aggressively. 3. Further work should focus on the neuropsychological outcomes of the different subtypes of NCSE. 4. Prospective multicenter studies are needed to further determine the best treatment paradigms for NCSE among different age groups and etiologies.
 Thank You.
Thank You.


