17e74e2cffd6e5e99462d45abb5ac5b2.ppt
- Количество слайдов: 18

21 th VHPB Meeting on “Prevention of viral hepatitis in Italy: lessons learnt and the way forward” Catania, 7 -8 november 2002 Impact of HBV S-gene mutants on the efficacy of vaccination A. Zanetti Institute of Virology, University of Milan (Italy)
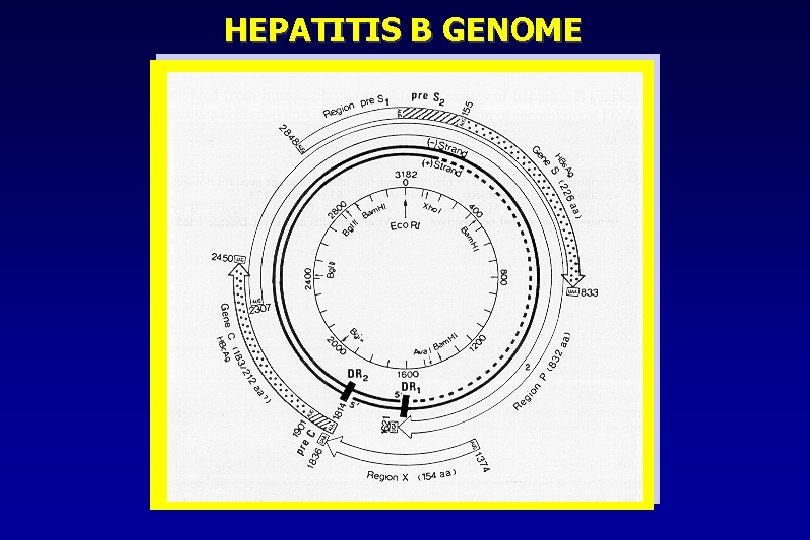
HEPATITIS B GENOME

HBV mutants • Many mutations which occur during replication are highly detrimental or lethal and are not mantained in the virus population. • A proportion of mutants may survive but only if they confer some advantage over pre-existing strains. • The immune responses of the host as well as prophylactic and therapeutic interventions may select variants which arise during the process of replication.
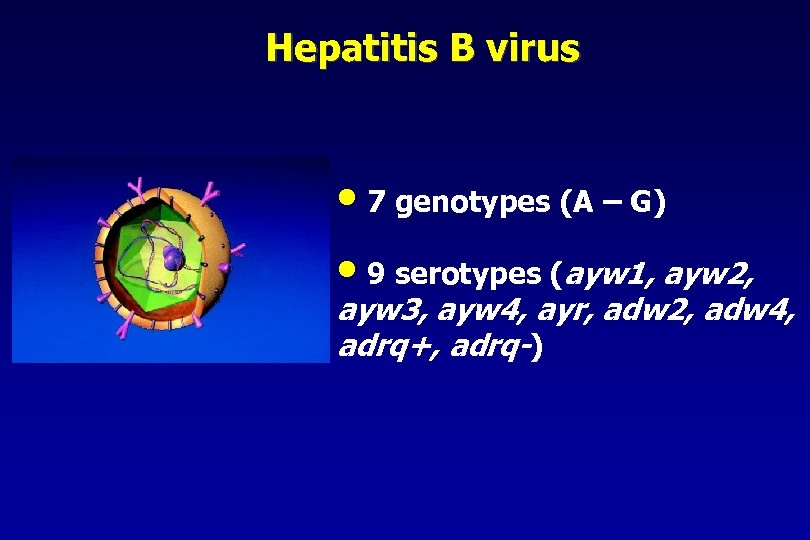
Hepatitis B virus • 7 genotypes (A – G) • 9 serotypes (ayw 1, ayw 2, ayw 3, ayw 4, ayr, adw 2, adw 4, adrq+, adrq-)

HBs. Ag mutants 145 Zuckerman AJ, Lancet 2001; 355: 1382 -4

HBV S-gene mutants (1) • Neutralizing (protective) antibodies induced by vaccines are mainly targeted towards a determinant. • Evidence indicates that aa substitution within this region of HBs. Ag can lead to conformational changes which allows mutated HBV to escape the vaccine-induced antibodies.

HBV S-gene mutants (2) • The emergence of a HBV variant possibly able to escape the vaccine-induced response was first suggested in Italy some 15 years ago (Zanetti et al, Lancet 1988) • 44 of 1590 (2. 8%) vaccinated people, including babies born to HBs. Ag carrier mothers, became HBV infected despite immunisation. All cases showed co-existence of HBs. Ag and anti-HBs.

HBV S-gene mutants (3) • Sequence analysis from one of these cases revealed substitution from Gly to Arg at position 145 of the a determinant (Carman et al, Lancet 1990) • The same mutation (G 145 R) was observed in a patient who underwent transplantation for end-stage HBV induced hepatitis and who was subsequently treated with monoclonal anti-a to prevent reinfection of the homograft (Mc. Mahon et al, 1991)

HBV S-gene mutants (4) • G 145 R mutation as well as other less frequent mutations within the HBs. Ag a determinant were also found in succesfully vaccinated babies in Singapore, Thailand, China, Japan, Brazil, the Gambia and in the USA.

Singapore study (Oon et al, 1995) • 41 breakthrough infections occurred in 345 (11. 9%) infants born to HBs. Ag/HBe. Ag carrier mothers and who were given HBIG + vaccine at birth (the most frequent variant was G 145 R). • No evidence of infection was seen in 670 children born to mothers with HBs. Ag and anti-HBe or in any of 107 immunized babies born to mothers HBs. Ag -ve.

Taiwan study (Hsu et al, 1999) • An increase in the prevalence (7. 8% in 1984, 19. 6% in 1989, 28. 1% in 1994) of HBV mutants (mostly G 145 R) was reported in Taiwan over 10 years after the introduction of universal vaccination. • The rate of mutations was higher among fully immunised children than among those unvaccinated.

Emergence of HBV S-gene mutants secondary to vaccination • Based on the assumption that current vaccines containing S protein do not cross-protect against S-gene mutants, a mathematical model predicted the disappearance of wt HBV and the emergence of G 145 R in approx 100 years.

Ability of licensed vaccines to protect chimpanzees against infection with G 145 R • A study carried out at NIH on 4 chimpanzees vaccinated with licensed recombinant vaccines, showed that immunised animals were protected when challenged with G 145 R (Ogata, 1999)

HBV S-gene mutants in Italy • Studies designed to the detection of HBV S-gene in vaccinees as well in chronic HBs. Ag carriers, are scanty in Italy. • Occasional breakthrough HBV infections due to G 145 R or to the less frequent S gene mutants, have been described both in liver transplant recipients (Cariani et al, 1995) and in children born to HBs. Ag mothers (Mele et al, 2001).

Effectiveness of HB vaccination in babies born to HBs. Ag+ mothers in Italy • 522 babies were given at birth HBIG + vaccine • At 5 -14 years after immunization: ü 97% of children had protective anti-HBs ü 14 children (2. 7%) seroconverted to anti-HBc ü 3 children became HBs. Ag carriers ü 1 child carrier had a double mutation with substitution of proline to serine at codons 120 (P 120 S) and 127 (P 127 S) within the a determinant
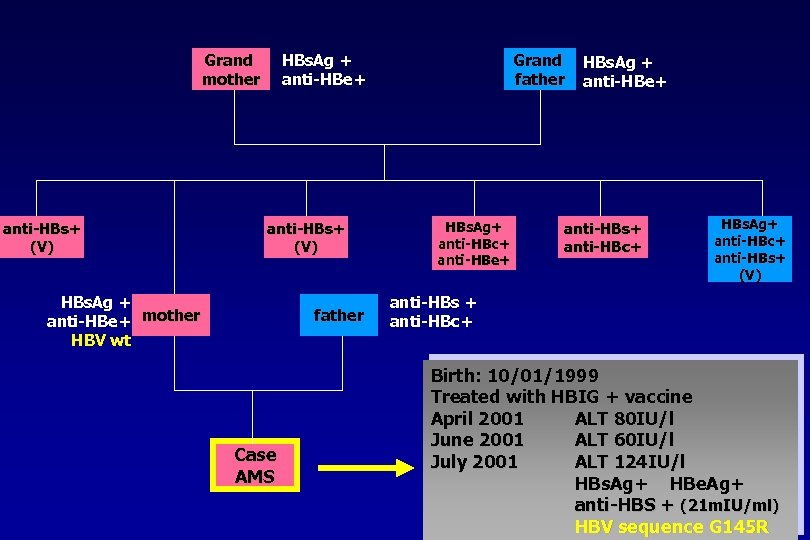
Grand mother anti-HBs+ (V) Grand father HBs. Ag + anti-HBe+ anti-HBs+ (V) HBs. Ag + anti-HBe+ mother HBV wt father Case AMS HBs. Ag+ anti-HBc+ anti-HBe+ HBs. Ag + anti-HBe+ anti-HBs+ anti-HBc+ HBs. Ag+ anti-HBc+ anti-HBs+ (V) anti-HBs + anti-HBc+ Birth: 10/01/1999 Treated with HBIG + vaccine April 2001 ALT 80 IU/l June 2001 ALT 60 IU/l July 2001 ALT 124 IU/l HBs. Ag+ HBe. Ag+ anti-HBS + (21 m. IU/ml) HBV sequence G 145 R

HBV S-gene mutants: a mere curiosity or a potential public health problem? (1) • HBV S-gene mutants have been identified in successfully immunised people worldwide. • There is evidence that such mutants may escape detection by assays based on m. Abs. • G 145 R is replication competent, stable and may persist in the host for years. • S-gene mutants appear to have a greater chance to emerge after post-exposure prophylaxis with HBIG and vaccine.

HBV S-gene mutants: a mere curiosity or a potential public health problem? (2) • At present, in Italy there is no evidence that S-gene mutants may pose a threat to the established program of vaccination. • Epidemiological monitoring of viral mutations, documentation of the natural history and disease progression caused by mutants and their person-to-person trasmissibility in both susceptible and immunised individuals, deserve further studies.
17e74e2cffd6e5e99462d45abb5ac5b2.ppt