d2b862c82ee019d052cd245b4098847e.ppt
- Количество слайдов: 53
 2008 International Nutrition Survey: Preliminary Results ANZICS/ Au. SPEN Conference Sydney, Australia November 1, 2008
2008 International Nutrition Survey: Preliminary Results ANZICS/ Au. SPEN Conference Sydney, Australia November 1, 2008
 Critical Care Nutrition. Mission Statement To improve practice of nutrition therapies in the critical care setting through knowledge generation, synthesis, and translation that ultimately leads to improved clinical outcomes for critically ill patients and improved efficiencies to our health care systems. Knowledge Generation • RCTs evaluating: - Acidified EN -Small bowel feedings -Cisapride - Immunonutrition - Feeding Algorithms • REDOXS Knowledge Synthesis • Over 40 systematic reviews • Internationally recognized clinical practice guidelines Knowledge Translation • Cluster RCT of guideline implementation strategies • Ongoing international practice audits • International attitudes & beliefs survey
Critical Care Nutrition. Mission Statement To improve practice of nutrition therapies in the critical care setting through knowledge generation, synthesis, and translation that ultimately leads to improved clinical outcomes for critically ill patients and improved efficiencies to our health care systems. Knowledge Generation • RCTs evaluating: - Acidified EN -Small bowel feedings -Cisapride - Immunonutrition - Feeding Algorithms • REDOXS Knowledge Synthesis • Over 40 systematic reviews • Internationally recognized clinical practice guidelines Knowledge Translation • Cluster RCT of guideline implementation strategies • Ongoing international practice audits • International attitudes & beliefs survey
 Critical Care Nutrition Staff
Critical Care Nutrition Staff
 Andrew Day Biostatistician Siouxzy Morrison Project Leader Au. SPEN/ANZICS Nutrition Research Fellow
Andrew Day Biostatistician Siouxzy Morrison Project Leader Au. SPEN/ANZICS Nutrition Research Fellow
 Achieving Best Practice: Quality Improvement What ought to be done? RCTs, Systematic Reviews, and Evidence-based practice guidelines What is done? How to change? Survey results KT Strategies What do we need to do differently? Benchmarking; Best Achievable Practice
Achieving Best Practice: Quality Improvement What ought to be done? RCTs, Systematic Reviews, and Evidence-based practice guidelines What is done? How to change? Survey results KT Strategies What do we need to do differently? Benchmarking; Best Achievable Practice
 Objectives of International Audit • To determine current nutrition practice in the adult critical care setting (overall and subgroups) • Illuminate gaps between best practice and current practice • To identify interventions to target for quality improvement initiatives • To determine factors associated with optimal provision of nutrition • To determine what nutrition practices are associated with best clinical outcomes
Objectives of International Audit • To determine current nutrition practice in the adult critical care setting (overall and subgroups) • Illuminate gaps between best practice and current practice • To identify interventions to target for quality improvement initiatives • To determine factors associated with optimal provision of nutrition • To determine what nutrition practices are associated with best clinical outcomes
 Methods • Prospective observational cohort study • Start date: 14 May 2008 • 20 consecutive critically ill patients • Data included: – Hospital and ICU demographics – Patient baseline information (e. g. age, admission diagnosis, APACHE II) – Baseline Nutrition Assessment – Daily Nutrition data (e. g. type of NS, amount NS received) – 60 day outcomes (e. g. mortality, length of stay)
Methods • Prospective observational cohort study • Start date: 14 May 2008 • 20 consecutive critically ill patients • Data included: – Hospital and ICU demographics – Patient baseline information (e. g. age, admission diagnosis, APACHE II) – Baseline Nutrition Assessment – Daily Nutrition data (e. g. type of NS, amount NS received) – 60 day outcomes (e. g. mortality, length of stay)
 Methods Eligibility Criteria • ICU Site – >5 beds – Availability of individual with knowledge of clinical nutrition to collect data • Patient – In ICU > 72 hours – Mechanically ventilated within 48 hours
Methods Eligibility Criteria • ICU Site – >5 beds – Availability of individual with knowledge of clinical nutrition to collect data • Patient – In ICU > 72 hours – Mechanically ventilated within 48 hours
 Web based Data Capture System
Web based Data Capture System
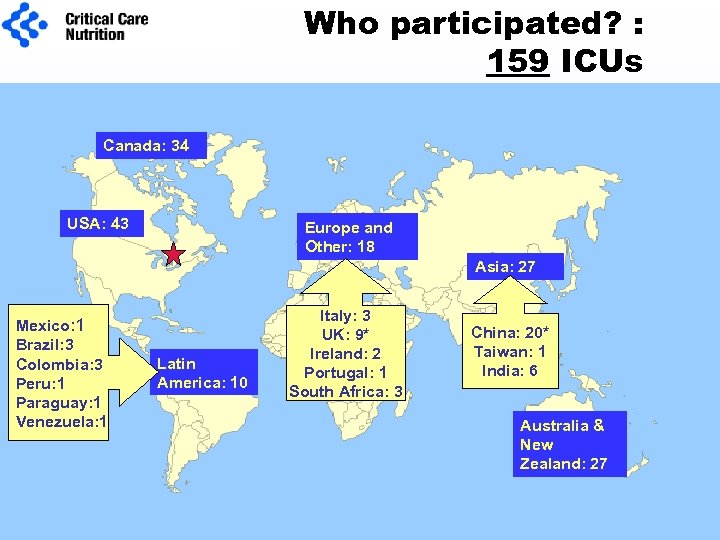 Who participated? : 159 ICUs Canada: 34 USA: 43 Europe and Other: 18 Asia: 27 Mexico: 1 Brazil: 3 Colombia: 3 Peru: 1 Paraguay: 1 Venezuela: 1 Latin America: 10 Italy: 3 UK: 9* Ireland: 2 Portugal: 1 South Africa: 3 China: 20* Taiwan: 1 India: 6 Australia & New Zealand: 27
Who participated? : 159 ICUs Canada: 34 USA: 43 Europe and Other: 18 Asia: 27 Mexico: 1 Brazil: 3 Colombia: 3 Peru: 1 Paraguay: 1 Venezuela: 1 Latin America: 10 Italy: 3 UK: 9* Ireland: 2 Portugal: 1 South Africa: 3 China: 20* Taiwan: 1 India: 6 Australia & New Zealand: 27
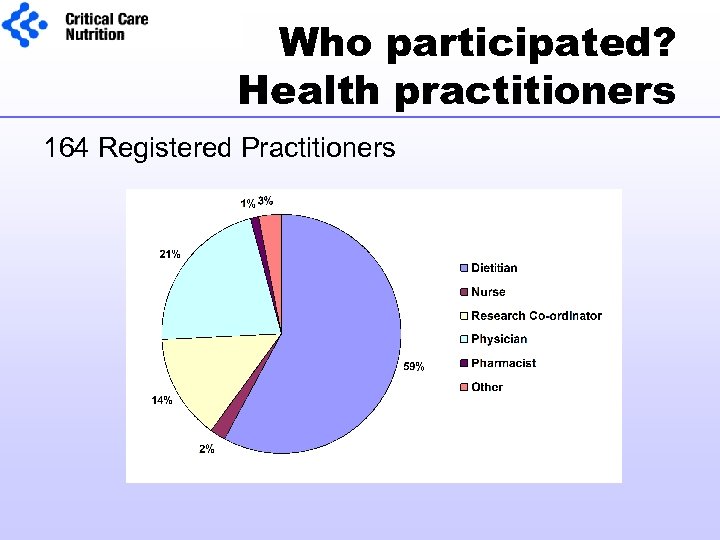 Who participated? Health practitioners 164 Registered Practitioners
Who participated? Health practitioners 164 Registered Practitioners
 Who participated? Patients • Number of finalized patients per site – 18. 0 (1 -26) • Total number of finalized patients – 2486 • Days of observation per patient – 9. 3 (3 -12) • Total number of patient days in ICU – 23199 days • <3% missing data for ALL variables
Who participated? Patients • Number of finalized patients per site – 18. 0 (1 -26) • Total number of finalized patients – 2486 • Days of observation per patient – 9. 3 (3 -12) • Total number of patient days in ICU – 23199 days • <3% missing data for ALL variables
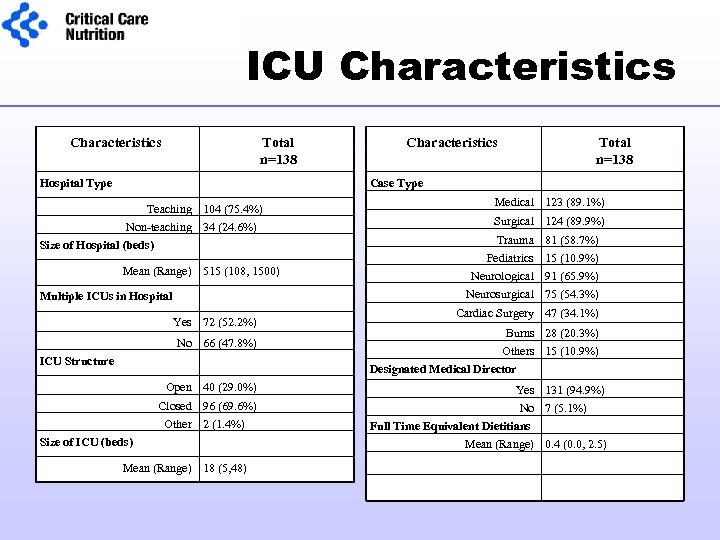 ICU Characteristics Total n=138 Hospital Type Characteristics Total n=138 Case Type Teaching 104 (75. 4%) Non-teaching 34 (24. 6%) Size of Hospital (beds) Mean (Range) 515 (108, 1500) Multiple ICUs in Hospital Yes 72 (52. 2%) No 66 (47. 8%) ICU Structure Open 40 (29. 0%) Closed 96 (69. 6%) Other 2 (1. 4%) Size of ICU (beds) Mean (Range) 18 (5, 48) Medical 123 (89. 1%) Surgical 124 (89. 9%) Trauma 81 (58. 7%) Pediatrics 15 (10. 9%) Neurological 91 (65. 9%) Neurosurgical 75 (54. 3%) Cardiac Surgery 47 (34. 1%) Burns 28 (20. 3%) Others 15 (10. 9%) Designated Medical Director Yes 131 (94. 9%) No 7 (5. 1%) Full Time Equivalent Dietitians Mean (Range) 0. 4 (0. 0, 2. 5)
ICU Characteristics Total n=138 Hospital Type Characteristics Total n=138 Case Type Teaching 104 (75. 4%) Non-teaching 34 (24. 6%) Size of Hospital (beds) Mean (Range) 515 (108, 1500) Multiple ICUs in Hospital Yes 72 (52. 2%) No 66 (47. 8%) ICU Structure Open 40 (29. 0%) Closed 96 (69. 6%) Other 2 (1. 4%) Size of ICU (beds) Mean (Range) 18 (5, 48) Medical 123 (89. 1%) Surgical 124 (89. 9%) Trauma 81 (58. 7%) Pediatrics 15 (10. 9%) Neurological 91 (65. 9%) Neurosurgical 75 (54. 3%) Cardiac Surgery 47 (34. 1%) Burns 28 (20. 3%) Others 15 (10. 9%) Designated Medical Director Yes 131 (94. 9%) No 7 (5. 1%) Full Time Equivalent Dietitians Mean (Range) 0. 4 (0. 0, 2. 5)
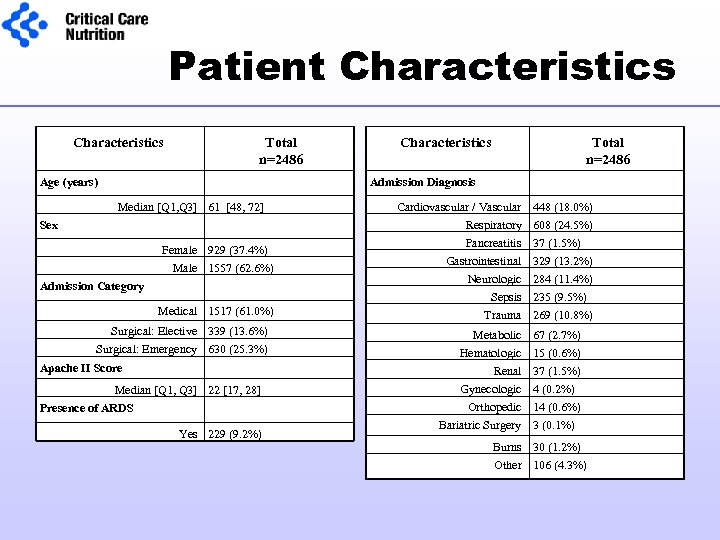 Patient Characteristics Total n=2486 Age (years) Characteristics Total n=2486 Admission Diagnosis Median [Q 1, Q 3] 61 [48, 72] Sex Female 929 (37. 4%) Male 1557 (62. 6%) Admission Category Medical 1517 (61. 0%) Surgical: Elective 339 (13. 6%) Surgical: Emergency 630 (25. 3%) Apache II Score Median [Q 1, Q 3] 22 [17, 28] Presence of ARDS Yes 229 (9. 2%) Cardiovascular / Vascular Respiratory Pancreatitis Gastrointestinal 448 (18. 0%) 608 (24. 5%) 37 (1. 5%) 329 (13. 2%) Neurologic 284 (11. 4%) Sepsis 235 (9. 5%) Trauma 269 (10. 8%) Metabolic 67 (2. 7%) Hematologic 15 (0. 6%) Renal 37 (1. 5%) Gynecologic 4 (0. 2%) Orthopedic 14 (0. 6%) Bariatric Surgery 3 (0. 1%) Burns 30 (1. 2%) Other 106 (4. 3%)
Patient Characteristics Total n=2486 Age (years) Characteristics Total n=2486 Admission Diagnosis Median [Q 1, Q 3] 61 [48, 72] Sex Female 929 (37. 4%) Male 1557 (62. 6%) Admission Category Medical 1517 (61. 0%) Surgical: Elective 339 (13. 6%) Surgical: Emergency 630 (25. 3%) Apache II Score Median [Q 1, Q 3] 22 [17, 28] Presence of ARDS Yes 229 (9. 2%) Cardiovascular / Vascular Respiratory Pancreatitis Gastrointestinal 448 (18. 0%) 608 (24. 5%) 37 (1. 5%) 329 (13. 2%) Neurologic 284 (11. 4%) Sepsis 235 (9. 5%) Trauma 269 (10. 8%) Metabolic 67 (2. 7%) Hematologic 15 (0. 6%) Renal 37 (1. 5%) Gynecologic 4 (0. 2%) Orthopedic 14 (0. 6%) Bariatric Surgery 3 (0. 1%) Burns 30 (1. 2%) Other 106 (4. 3%)
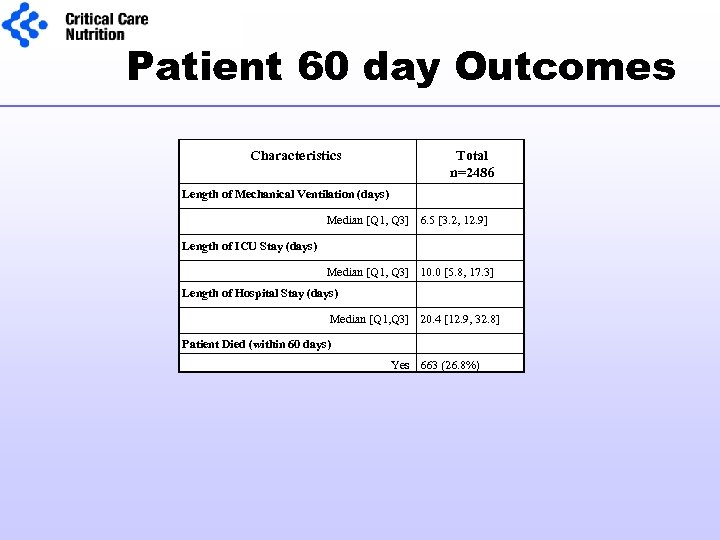 Patient 60 day Outcomes Characteristics Total n=2486 Length of Mechanical Ventilation (days) Median [Q 1, Q 3] 6. 5 [3. 2, 12. 9] Length of ICU Stay (days) Median [Q 1, Q 3] 10. 0 [5. 8, 17. 3] Length of Hospital Stay (days) Median [Q 1, Q 3] 20. 4 [12. 9, 32. 8] Patient Died (within 60 days) Yes 663 (26. 8%)
Patient 60 day Outcomes Characteristics Total n=2486 Length of Mechanical Ventilation (days) Median [Q 1, Q 3] 6. 5 [3. 2, 12. 9] Length of ICU Stay (days) Median [Q 1, Q 3] 10. 0 [5. 8, 17. 3] Length of Hospital Stay (days) Median [Q 1, Q 3] 20. 4 [12. 9, 32. 8] Patient Died (within 60 days) Yes 663 (26. 8%)
![Baseline Nutrition Assessment Characteristics Total n=2486 BMI (kgh|m 2) Median [Q 1, Q 3] Baseline Nutrition Assessment Characteristics Total n=2486 BMI (kgh|m 2) Median [Q 1, Q 3]](https://present5.com/presentation/d2b862c82ee019d052cd245b4098847e/image-16.jpg) Baseline Nutrition Assessment Characteristics Total n=2486 BMI (kgh|m 2) Median [Q 1, Q 3] 26. 1 [22. 9, 30. 5] Prescribed Energy Intake (Kcals) Median (Q 1, Q 3] 1800. 0 [1584. 0, 2040. 0] Prescribed Protein Intake (g) Median [Q 1, Q 3] 85. 0 [71. 5, 100. 0]
Baseline Nutrition Assessment Characteristics Total n=2486 BMI (kgh|m 2) Median [Q 1, Q 3] 26. 1 [22. 9, 30. 5] Prescribed Energy Intake (Kcals) Median (Q 1, Q 3] 1800. 0 [1584. 0, 2040. 0] Prescribed Protein Intake (g) Median [Q 1, Q 3] 85. 0 [71. 5, 100. 0]
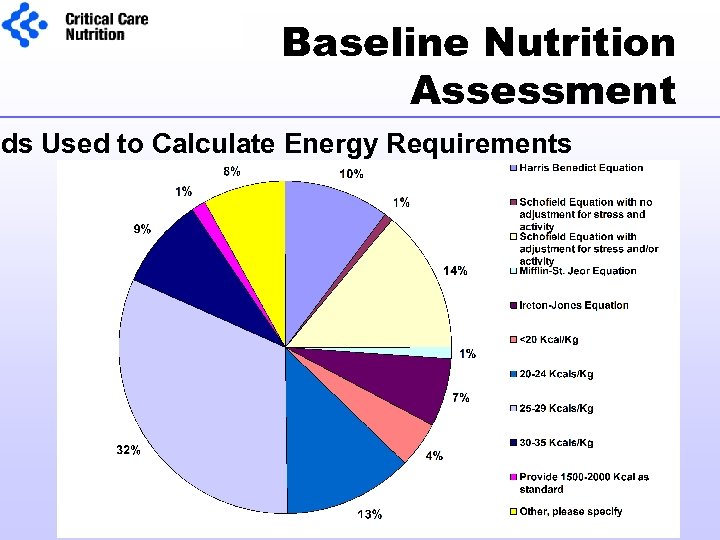 Baseline Nutrition Assessment ods Used to Calculate Energy Requirements
Baseline Nutrition Assessment ods Used to Calculate Energy Requirements
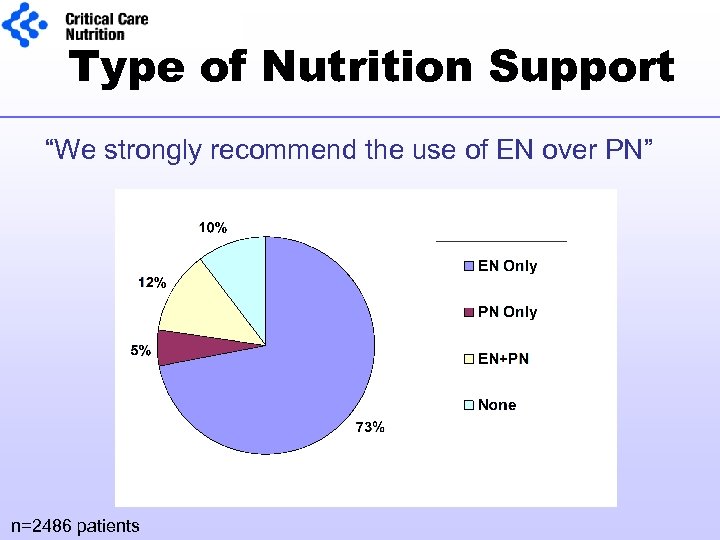 Type of Nutrition Support “We strongly recommend the use of EN over PN” n=2486 patients
Type of Nutrition Support “We strongly recommend the use of EN over PN” n=2486 patients
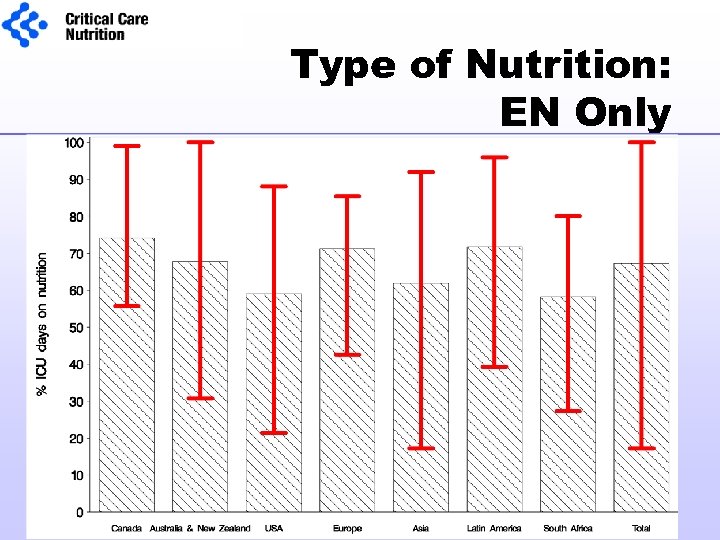 Type of Nutrition: EN Only
Type of Nutrition: EN Only
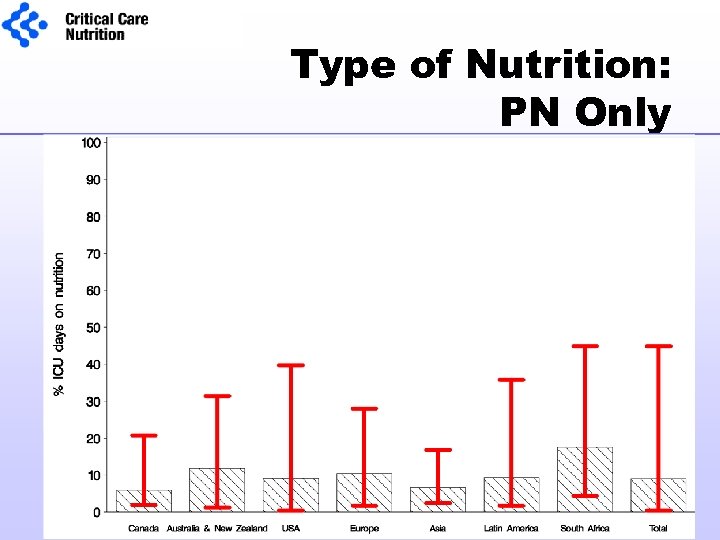 Type of Nutrition: PN Only
Type of Nutrition: PN Only
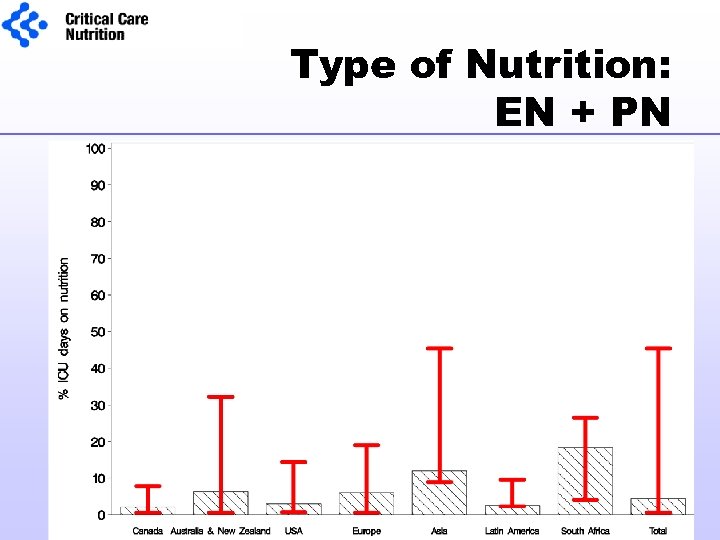 Type of Nutrition: EN + PN
Type of Nutrition: EN + PN
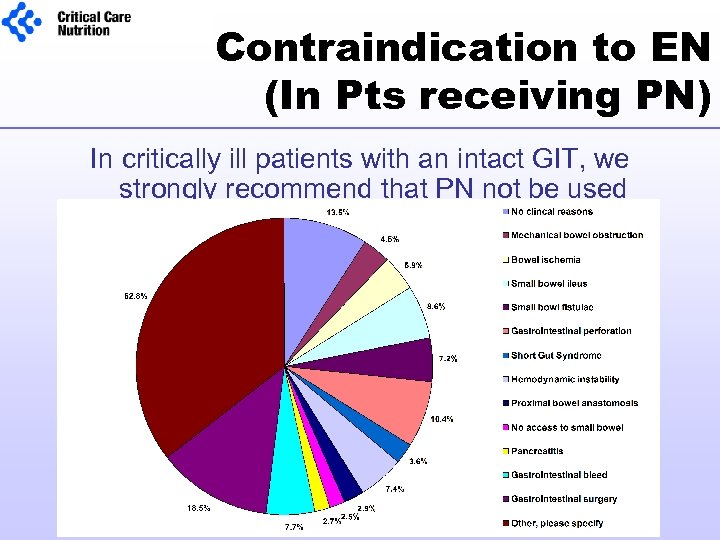 Contraindication to EN (In Pts receiving PN) In critically ill patients with an intact GIT, we strongly recommend that PN not be used routinely
Contraindication to EN (In Pts receiving PN) In critically ill patients with an intact GIT, we strongly recommend that PN not be used routinely
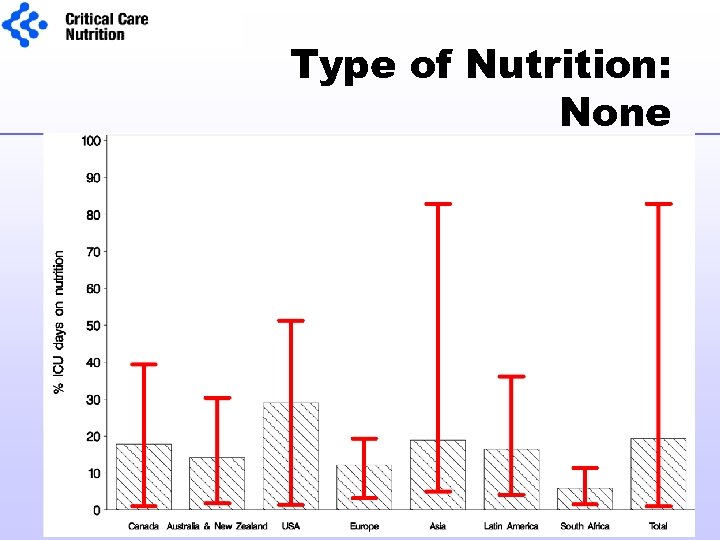 Type of Nutrition: None
Type of Nutrition: None
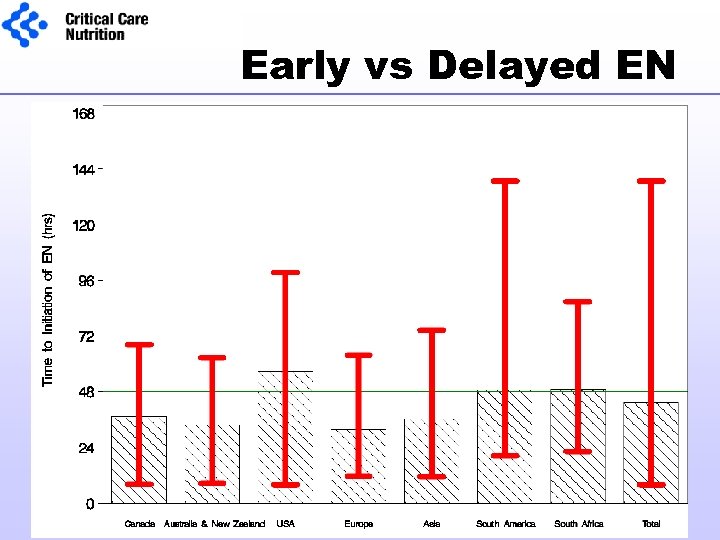 Early vs Delayed EN
Early vs Delayed EN
 Strategies to Optimize EN Delivery: Feeding Protocol Characteristics Total n=138 Feeding Protocol Yes 112 (81. 2%) Gastric Residual Volume Tolerated in Protocol Mean (range) 214 (100, 500) Algorithms included in Protocol Motility agents 72 (70. 6%) Small bowel feeding 52 (51. 0%) Withholding for procedures 47 (46. 1%) HOB Elevation 79 (77. 5%) Other 21 (20. 6%)
Strategies to Optimize EN Delivery: Feeding Protocol Characteristics Total n=138 Feeding Protocol Yes 112 (81. 2%) Gastric Residual Volume Tolerated in Protocol Mean (range) 214 (100, 500) Algorithms included in Protocol Motility agents 72 (70. 6%) Small bowel feeding 52 (51. 0%) Withholding for procedures 47 (46. 1%) HOB Elevation 79 (77. 5%) Other 21 (20. 6%)
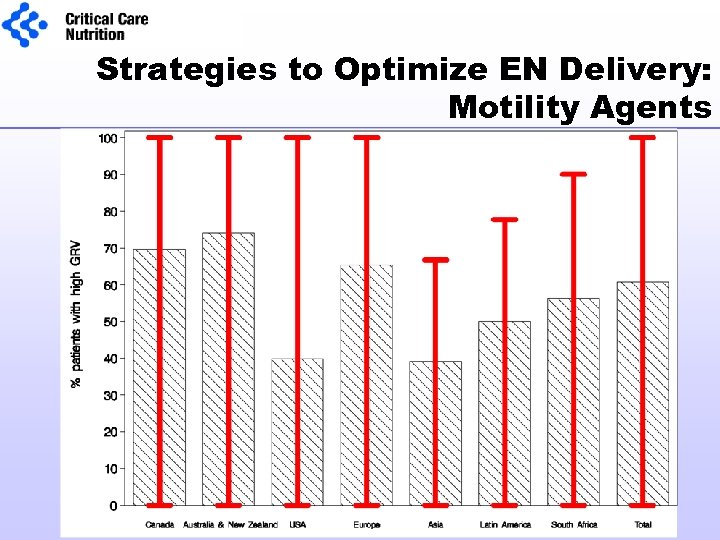 Strategies to Optimize EN Delivery: Motility Agents
Strategies to Optimize EN Delivery: Motility Agents
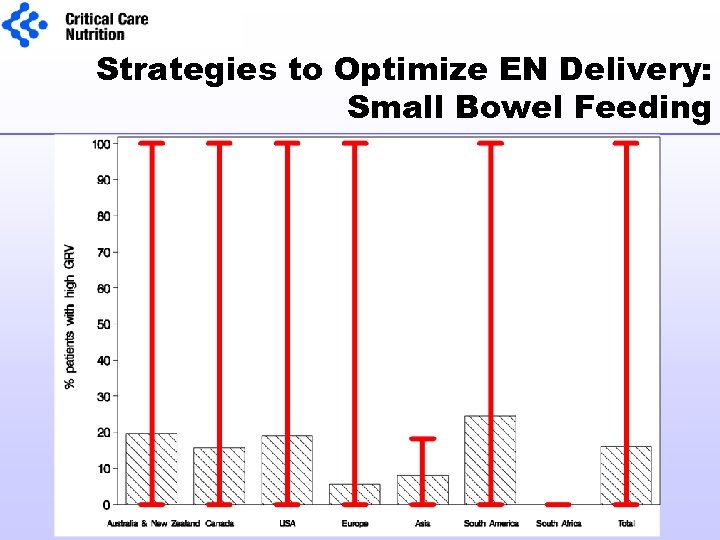 Strategies to Optimize EN Delivery: Small Bowel Feeding
Strategies to Optimize EN Delivery: Small Bowel Feeding
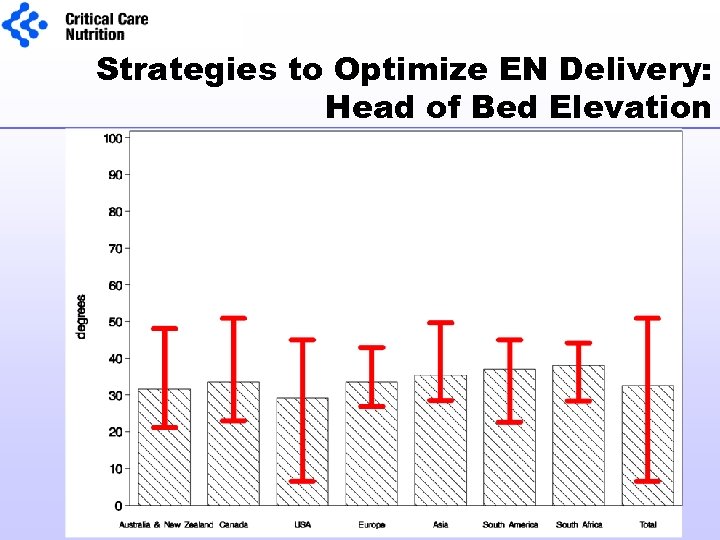 Strategies to Optimize EN Delivery: Head of Bed Elevation
Strategies to Optimize EN Delivery: Head of Bed Elevation
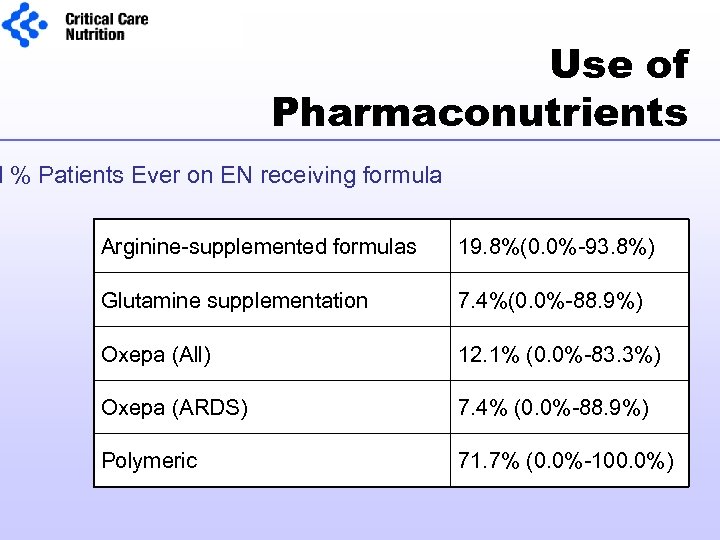 Use of Pharmaconutrients l % Patients Ever on EN receiving formula Arginine-supplemented formulas 19. 8%(0. 0%-93. 8%) Glutamine supplementation 7. 4%(0. 0%-88. 9%) Oxepa (All) 12. 1% (0. 0%-83. 3%) Oxepa (ARDS) 7. 4% (0. 0%-88. 9%) Polymeric 71. 7% (0. 0%-100. 0%)
Use of Pharmaconutrients l % Patients Ever on EN receiving formula Arginine-supplemented formulas 19. 8%(0. 0%-93. 8%) Glutamine supplementation 7. 4%(0. 0%-88. 9%) Oxepa (All) 12. 1% (0. 0%-83. 3%) Oxepa (ARDS) 7. 4% (0. 0%-88. 9%) Polymeric 71. 7% (0. 0%-100. 0%)
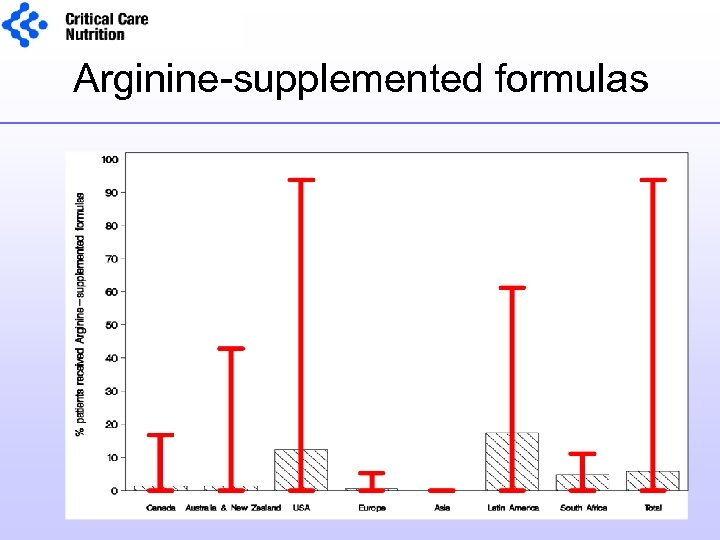 Arginine-supplemented formulas
Arginine-supplemented formulas
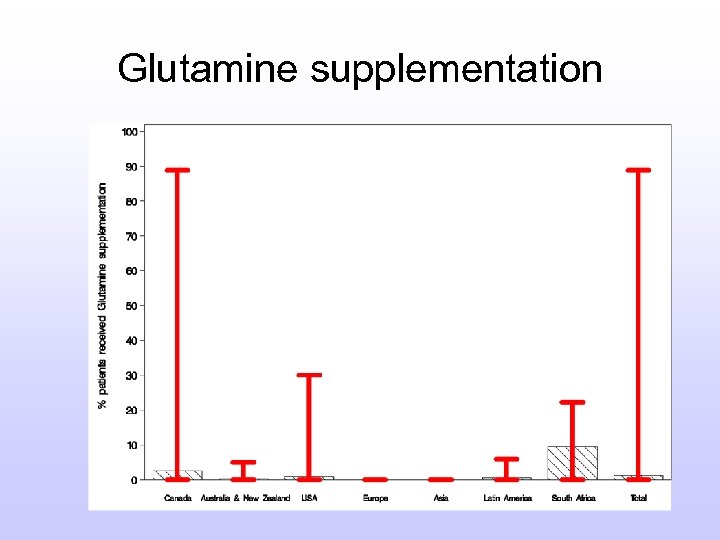 Glutamine supplementation
Glutamine supplementation
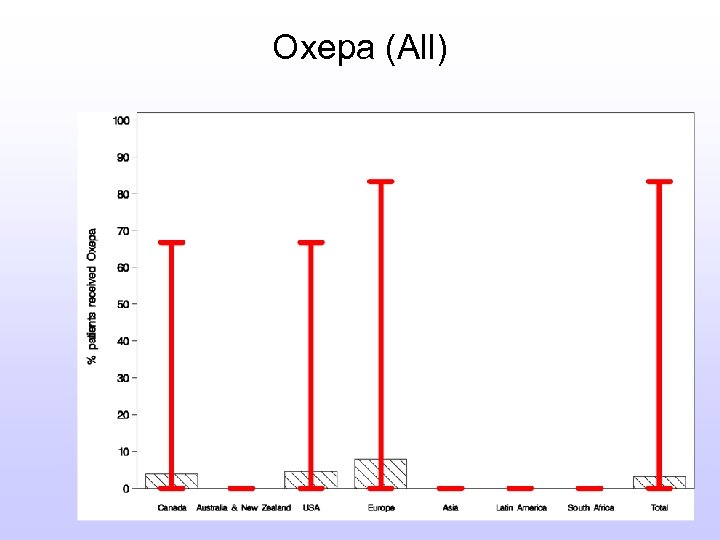 Oxepa (All)
Oxepa (All)
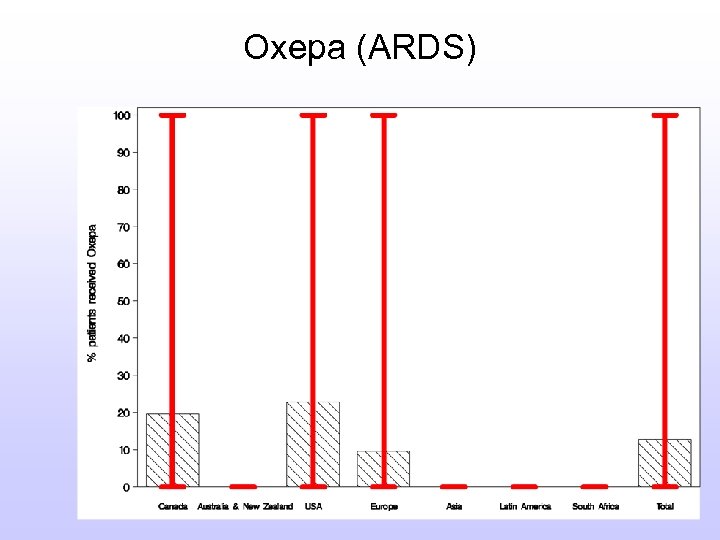 Oxepa (ARDS)
Oxepa (ARDS)
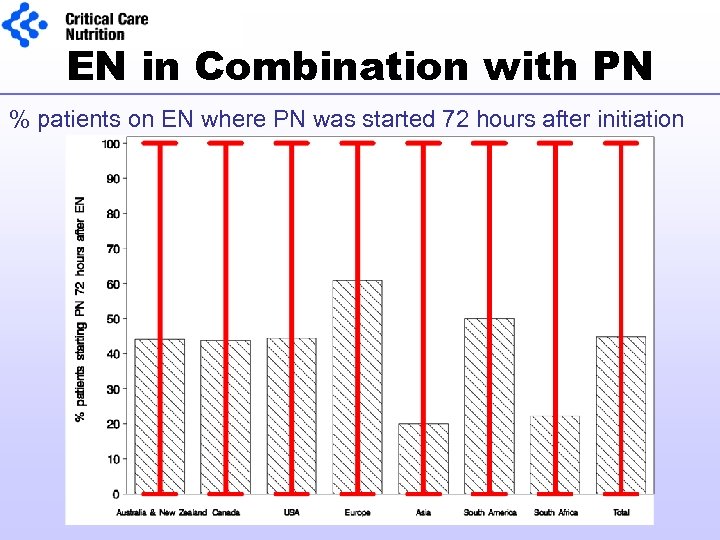 EN in Combination with PN % patients on EN where PN was started 72 hours after initiation of EN
EN in Combination with PN % patients on EN where PN was started 72 hours after initiation of EN
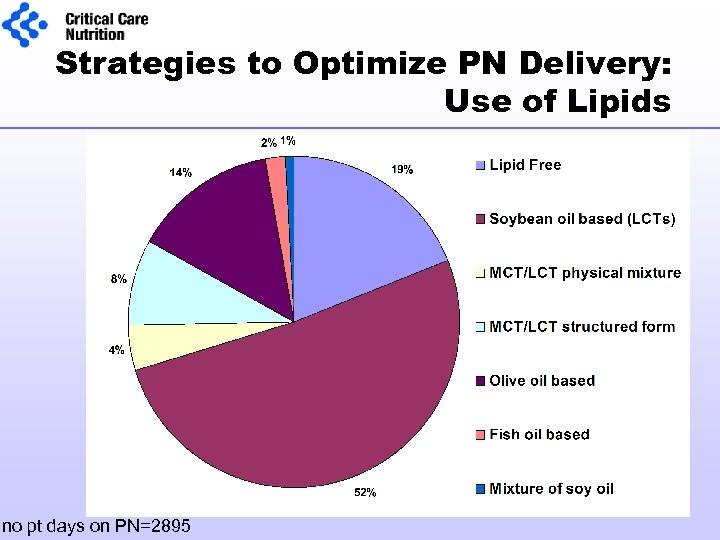 Strategies to Optimize PN Delivery: Use of Lipids no pt days on PN=2895
Strategies to Optimize PN Delivery: Use of Lipids no pt days on PN=2895
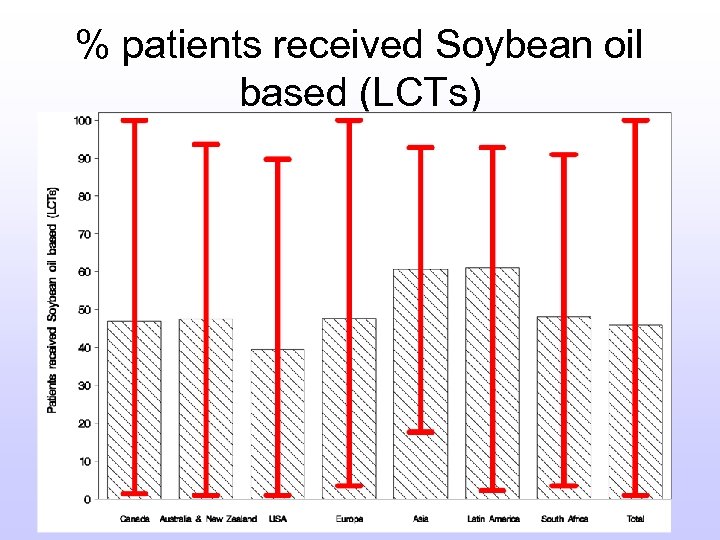 % patients received Soybean oil based (LCTs)
% patients received Soybean oil based (LCTs)
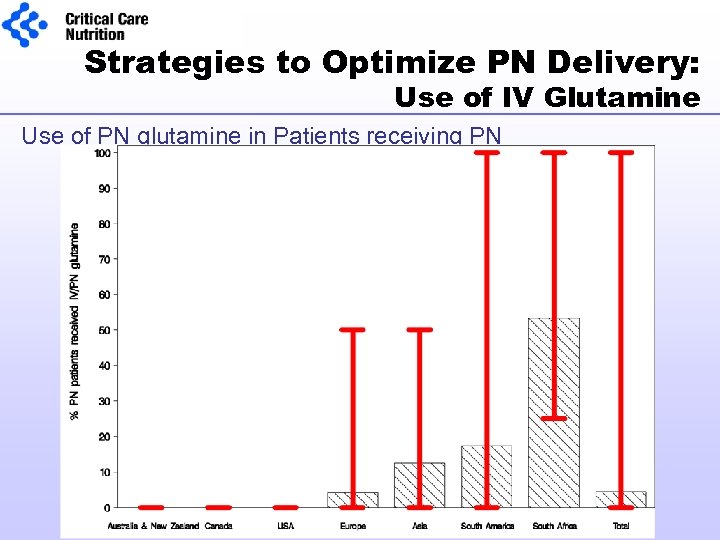 Strategies to Optimize PN Delivery: Use of IV Glutamine Use of PN glutamine in Patients receiving PN
Strategies to Optimize PN Delivery: Use of IV Glutamine Use of PN glutamine in Patients receiving PN
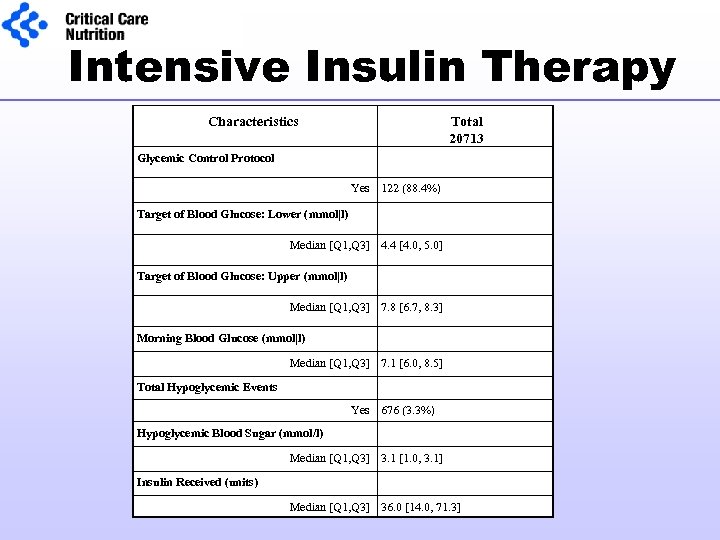 Intensive Insulin Therapy Characteristics Total 20713 Glycemic Control Protocol Yes 122 (88. 4%) Target of Blood Glucose: Lower (mmol|l) Median [Q 1, Q 3] 4. 4 [4. 0, 5. 0] Target of Blood Glucose: Upper (mmol|l) Median [Q 1, Q 3] 7. 8 [6. 7, 8. 3] Morning Blood Glucose (mmol|l) Median [Q 1, Q 3] 7. 1 [6. 0, 8. 5] Total Hypoglycemic Events Yes 676 (3. 3%) Hypoglycemic Blood Sugar (mmol/l) Median [Q 1, Q 3] 3. 1 [1. 0, 3. 1] Insulin Received (units) Median [Q 1, Q 3] 36. 0 [14. 0, 71. 3]
Intensive Insulin Therapy Characteristics Total 20713 Glycemic Control Protocol Yes 122 (88. 4%) Target of Blood Glucose: Lower (mmol|l) Median [Q 1, Q 3] 4. 4 [4. 0, 5. 0] Target of Blood Glucose: Upper (mmol|l) Median [Q 1, Q 3] 7. 8 [6. 7, 8. 3] Morning Blood Glucose (mmol|l) Median [Q 1, Q 3] 7. 1 [6. 0, 8. 5] Total Hypoglycemic Events Yes 676 (3. 3%) Hypoglycemic Blood Sugar (mmol/l) Median [Q 1, Q 3] 3. 1 [1. 0, 3. 1] Insulin Received (units) Median [Q 1, Q 3] 36. 0 [14. 0, 71. 3]
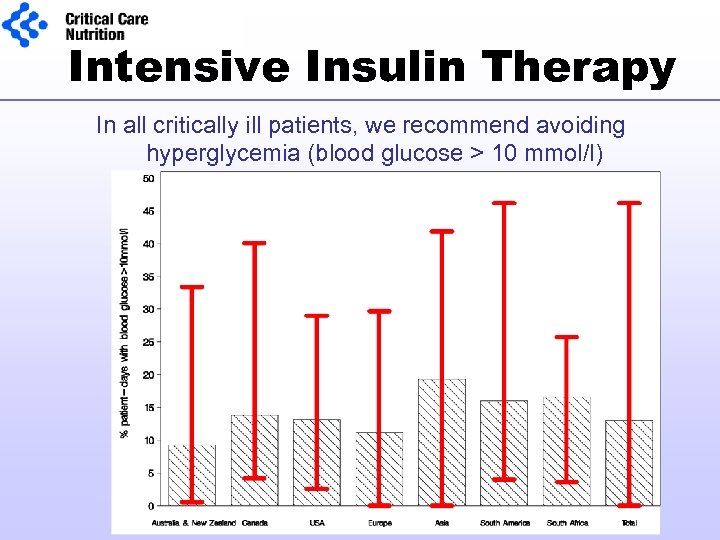 Intensive Insulin Therapy In all critically ill patients, we recommend avoiding hyperglycemia (blood glucose > 10 mmol/l)
Intensive Insulin Therapy In all critically ill patients, we recommend avoiding hyperglycemia (blood glucose > 10 mmol/l)
 Overall Performance Adequacy of Nutrition Support = Calories received from EN + appropriate PN+Propofol Calories prescribed
Overall Performance Adequacy of Nutrition Support = Calories received from EN + appropriate PN+Propofol Calories prescribed
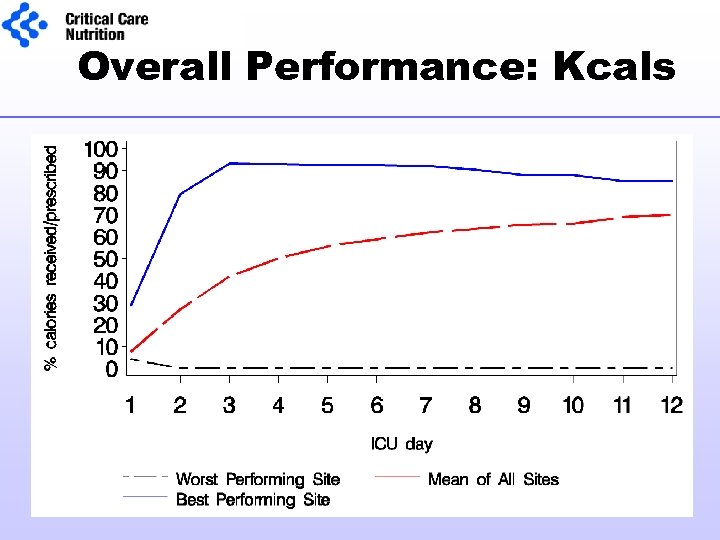 Overall Performance: Kcals
Overall Performance: Kcals
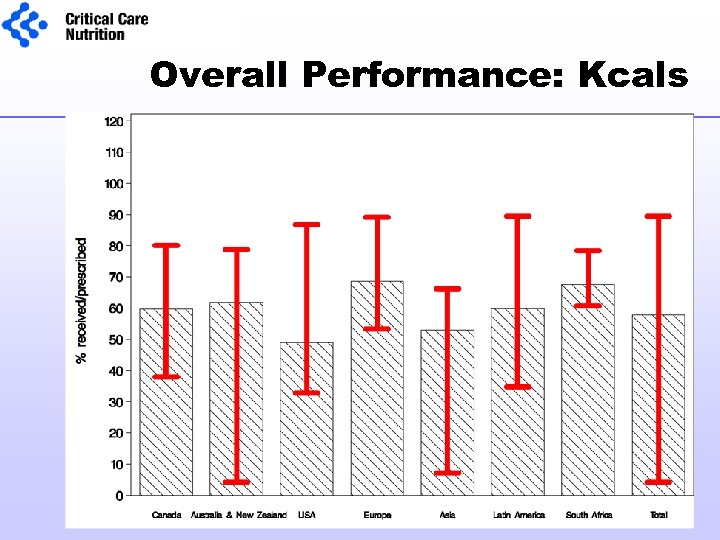 Overall Performance: Kcals
Overall Performance: Kcals
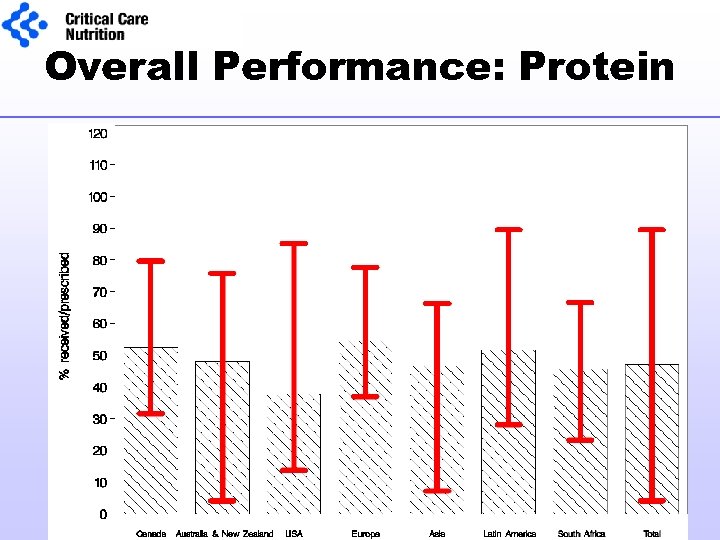 Overall Performance: Protein
Overall Performance: Protein
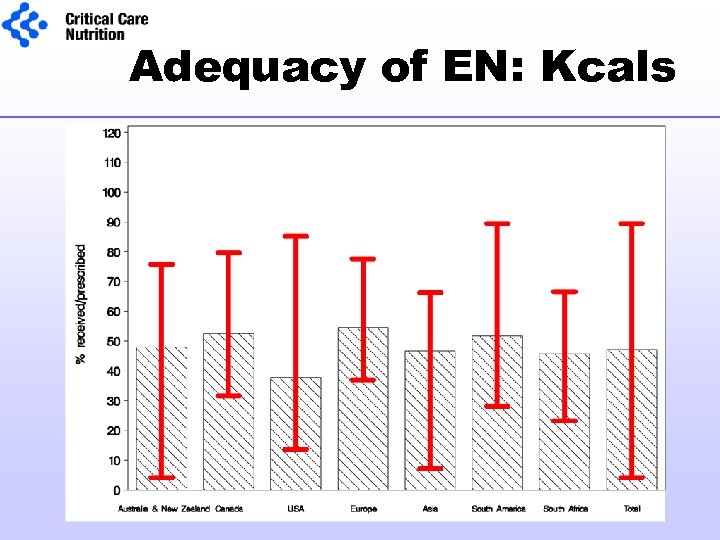 Adequacy of EN: Kcals
Adequacy of EN: Kcals
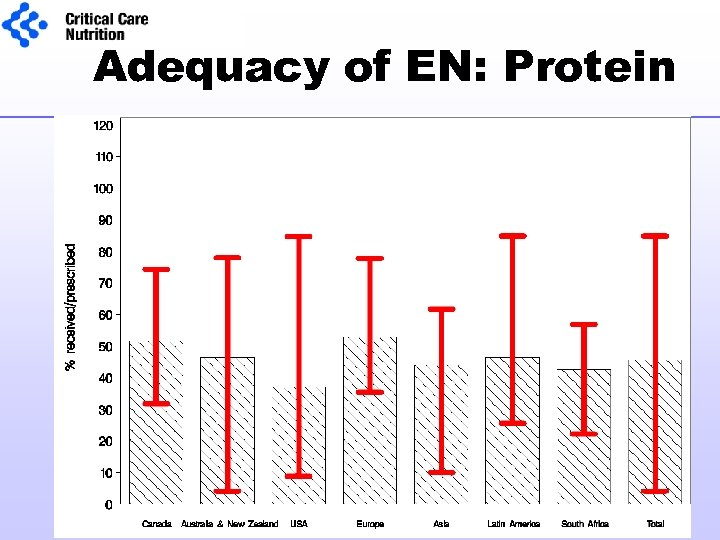 Adequacy of EN: Protein
Adequacy of EN: Protein
 Benchmarking
Benchmarking
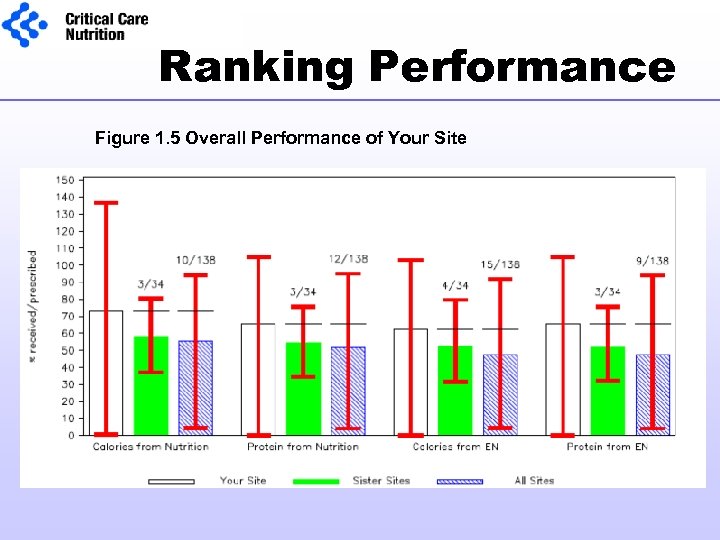 Ranking Performance Figure 1. 5 Overall Performance of Your Site
Ranking Performance Figure 1. 5 Overall Performance of Your Site
 Best of the Best Can you be the best in the International Nutrition Survey 2008 • Eligible sites: § § § Data on 20 critically ill patients Complete baseline nutrition assessment Presence of feeding protocol No missing data or outstanding queries Permit source verification by CCN • Awarded to ICU that demonstrate: § High nutritional adequacy § Adherence to the Canadian guidelines
Best of the Best Can you be the best in the International Nutrition Survey 2008 • Eligible sites: § § § Data on 20 critically ill patients Complete baseline nutrition assessment Presence of feeding protocol No missing data or outstanding queries Permit source verification by CCN • Awarded to ICU that demonstrate: § High nutritional adequacy § Adherence to the Canadian guidelines
 Best of the Best Can you be the best in the International Nutrition Survey 2008 • Eligible sites: § § § Data on 20 critically ill patients Complete baseline nutrition assessment Presence of feeding protocol No missing data or outstanding queries Permit source verification by CCN • Awarded to ICU that demonstrate: § High nutritional adequacy § Adherence to the Canadian guidelines
Best of the Best Can you be the best in the International Nutrition Survey 2008 • Eligible sites: § § § Data on 20 critically ill patients Complete baseline nutrition assessment Presence of feeding protocol No missing data or outstanding queries Permit source verification by CCN • Awarded to ICU that demonstrate: § High nutritional adequacy § Adherence to the Canadian guidelines
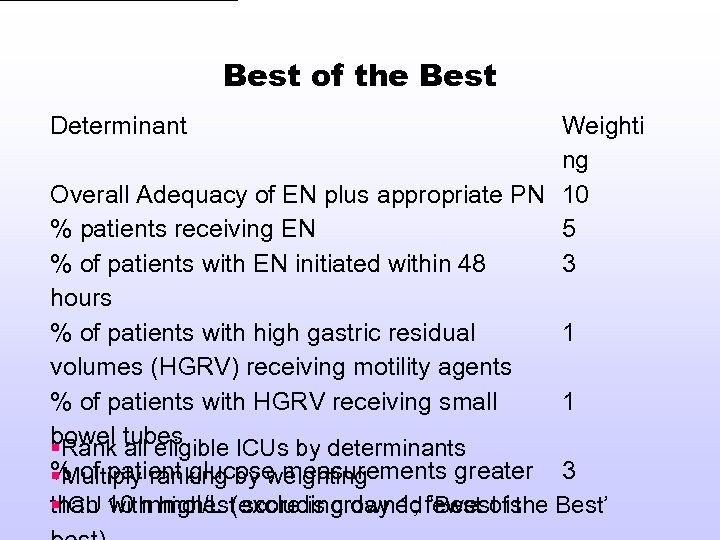 Best of the Best Determinant Weighti ng Overall Adequacy of EN plus appropriate PN 10 % patients receiving EN 5 % of patients with EN initiated within 48 3 hours % of patients with high gastric residual 1 volumes (HGRV) receiving motility agents % of patients with HGRV receiving small 1 bowel all eligible ICUs by determinants §Rank tubes % of patient glucose measurements greater 3 §Multiply ranking by weighting than with highest score is crowned ‘Best of the §ICU 10 mmol/L (excluding day 1; fewest is Best’
Best of the Best Determinant Weighti ng Overall Adequacy of EN plus appropriate PN 10 % patients receiving EN 5 % of patients with EN initiated within 48 3 hours % of patients with high gastric residual 1 volumes (HGRV) receiving motility agents % of patients with HGRV receiving small 1 bowel all eligible ICUs by determinants §Rank tubes % of patient glucose measurements greater 3 §Multiply ranking by weighting than with highest score is crowned ‘Best of the §ICU 10 mmol/L (excluding day 1; fewest is Best’
 Future Directions Quality Improvement Initiatives • Inadequate EN delivery – early EN feeding protocols – small bowel feeding • Optimize Pharmaconutrition – use of glutamine, antioxidants, omega-3 FFA. • Tighten glycemic control • Withhold soy bean emulsion lipids • others?
Future Directions Quality Improvement Initiatives • Inadequate EN delivery – early EN feeding protocols – small bowel feeding • Optimize Pharmaconutrition – use of glutamine, antioxidants, omega-3 FFA. • Tighten glycemic control • Withhold soy bean emulsion lipids • others?
 Future Directions Hypothesis–generating Observations – Protocolized vs Non protocolized – Academic vs Community – Presence of dietitian and how much? – Subgroups • by BMI • by Case Mix (Trauma, Sepsis; Pancreatitis, etc. ) – others?
Future Directions Hypothesis–generating Observations – Protocolized vs Non protocolized – Academic vs Community – Presence of dietitian and how much? – Subgroups • by BMI • by Case Mix (Trauma, Sepsis; Pancreatitis, etc. ) – others?
 Thank you
Thank you


