b6979da3a93e3b5a0385091271bcd613.ppt
- Количество слайдов: 142
 126 th Annual AMSUS Meeting Military Health System Consensus Statement on the Prevention, Diagnosis and Treatment of Traumatic Brain Injury 30 November 2017 “Medically Ready Force…Ready Medical Force” 1
126 th Annual AMSUS Meeting Military Health System Consensus Statement on the Prevention, Diagnosis and Treatment of Traumatic Brain Injury 30 November 2017 “Medically Ready Force…Ready Medical Force” 1
 Presenters § Saafan Malik, MD, Defense and Veterans Brain Injury Center § Scott Livingston, Ph. D, PT, ATC, Defense and Veterans Brain Injury Center § Kathy Helmick, MS, CRNP, ANP-BC, CNRN, Defense and Veterans Brain Injury Center § Don Marion, MD, Defense and Veterans Brain Injury Center § Thomas De. Graba, MD, National Intrepid Center of Excellence § Jonathan Wolf, MD, National Intrepid Center of Excellence, Walter Reed National Military Medical Center § Linda Picon, MCD, CCC-SLP, Department of Veterans Affairs § Louis French, Psy. D, National Intrepid Center of Excellence “Medically Ready Force…Ready Medical Force” 2
Presenters § Saafan Malik, MD, Defense and Veterans Brain Injury Center § Scott Livingston, Ph. D, PT, ATC, Defense and Veterans Brain Injury Center § Kathy Helmick, MS, CRNP, ANP-BC, CNRN, Defense and Veterans Brain Injury Center § Don Marion, MD, Defense and Veterans Brain Injury Center § Thomas De. Graba, MD, National Intrepid Center of Excellence § Jonathan Wolf, MD, National Intrepid Center of Excellence, Walter Reed National Military Medical Center § Linda Picon, MCD, CCC-SLP, Department of Veterans Affairs § Louis French, Psy. D, National Intrepid Center of Excellence “Medically Ready Force…Ready Medical Force” 2
 Disclosures § The presenters have no financial relationships to disclose. § This continuing education activity is managed and accredited by Professional Education Services Group in cooperation with AMSUS. § Neither PESG, AMSUS, nor any accrediting organization support or endorse any product or service mentioned in this activity. § PESG and AMSUS staff has no financial interest to disclose. § Commercial support was not received for this activity. “Medically Ready Force…Ready Medical Force” 3
Disclosures § The presenters have no financial relationships to disclose. § This continuing education activity is managed and accredited by Professional Education Services Group in cooperation with AMSUS. § Neither PESG, AMSUS, nor any accrediting organization support or endorse any product or service mentioned in this activity. § PESG and AMSUS staff has no financial interest to disclose. § Commercial support was not received for this activity. “Medically Ready Force…Ready Medical Force” 3
 Session Objectives ∎ Provide state-of-the-science information regarding optimal prevention, diagnosis, treatment and rehabilitation measures for service members who have sustained a TBI ∎ Present the preliminary conclusions and recommendations of consensus working groups regarding the specific TBI-relevant issues of prevention, acute concussion evaluation and management, peri-injury management of severe and penetrating TBI, behavioral health consequences of TBI, rehabilitation, and long term effects. “Medically Ready Force…Ready Medical Force” 4
Session Objectives ∎ Provide state-of-the-science information regarding optimal prevention, diagnosis, treatment and rehabilitation measures for service members who have sustained a TBI ∎ Present the preliminary conclusions and recommendations of consensus working groups regarding the specific TBI-relevant issues of prevention, acute concussion evaluation and management, peri-injury management of severe and penetrating TBI, behavioral health consequences of TBI, rehabilitation, and long term effects. “Medically Ready Force…Ready Medical Force” 4
 Obtaining CME/CE Credit ∎ If you would like to receive continuing education credit for this activity, please visit: http: //amsus. cds. pesgce. com “Medically Ready Force…Ready Medical Force” 5
Obtaining CME/CE Credit ∎ If you would like to receive continuing education credit for this activity, please visit: http: //amsus. cds. pesgce. com “Medically Ready Force…Ready Medical Force” 5
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Introduction & Overview Saafan Malik, MD Defense and Veterans Brain Injury Center “Medically Ready Force…Ready Medical Force” 6
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Introduction & Overview Saafan Malik, MD Defense and Veterans Brain Injury Center “Medically Ready Force…Ready Medical Force” 6
 Project Background ∎ Task direction provided by the Deputy Assistant Secretary of Defense for Health Affairs, December 2016 ∎ Do. D has a longstanding commitment for providing world-class health care for TBI and investing in state-of-the-science research: q 1992 - Establishment of Defense and Veterans Head Injury Program (DVHIP); program later changed to the Defense and Veterans Brain Injury Center (DVBIC) q 2007 - With the Army TBI Task Force Report and the MEDCOM TBI Action Plan, the Do. D has brought clinical standardization, guidelines, and momentum to address TBI q 2012 - Presidential Executive Order directed Do. D, VA, HHS and the Department of Education to develop a National Research Action Plan (NRAP), one of the focus areas being TBI “Medically Ready Force…Ready Medical Force” 7
Project Background ∎ Task direction provided by the Deputy Assistant Secretary of Defense for Health Affairs, December 2016 ∎ Do. D has a longstanding commitment for providing world-class health care for TBI and investing in state-of-the-science research: q 1992 - Establishment of Defense and Veterans Head Injury Program (DVHIP); program later changed to the Defense and Veterans Brain Injury Center (DVBIC) q 2007 - With the Army TBI Task Force Report and the MEDCOM TBI Action Plan, the Do. D has brought clinical standardization, guidelines, and momentum to address TBI q 2012 - Presidential Executive Order directed Do. D, VA, HHS and the Department of Education to develop a National Research Action Plan (NRAP), one of the focus areas being TBI “Medically Ready Force…Ready Medical Force” 7
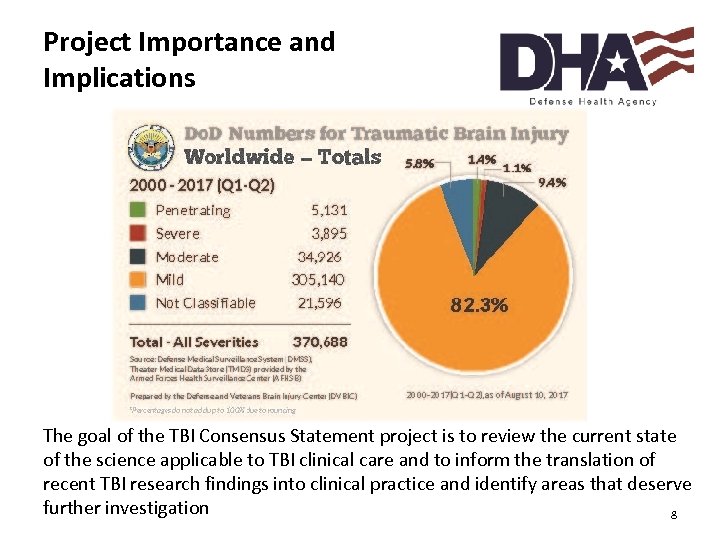 Project Importance and Implications The goal of the TBI Consensus Statement project is to review the current state of the science applicable to TBI clinical care and to inform the translation of recent TBI research findings into clinical practice and identify areas that deserve further investigation “Medically Ready Force…Ready Medical Force” 8
Project Importance and Implications The goal of the TBI Consensus Statement project is to review the current state of the science applicable to TBI clinical care and to inform the translation of recent TBI research findings into clinical practice and identify areas that deserve further investigation “Medically Ready Force…Ready Medical Force” 8
 TBI Topic Areas Consensus Statement Topic Areas 1 2 3 Prevention (Helmets, Education, Sports, & Combatives) Acute Concussion (0 -7 days post injury) Peri-injury Management of Severe and Penetrating TBI (Battlefield/En-Route Care) 4 Biomarkers in TBI – Radiologic and Non-Radiologic 5 Behavioral Health Consequences of TBI – mild TBI Co. Morbidities and Severe Sequelae of TBI 6 7 Rehabilitation (Auditory, Cognitive, Vestibular, & Visual) Long Term Effects “Medically Ready Force…Ready Medical Force” 9
TBI Topic Areas Consensus Statement Topic Areas 1 2 3 Prevention (Helmets, Education, Sports, & Combatives) Acute Concussion (0 -7 days post injury) Peri-injury Management of Severe and Penetrating TBI (Battlefield/En-Route Care) 4 Biomarkers in TBI – Radiologic and Non-Radiologic 5 Behavioral Health Consequences of TBI – mild TBI Co. Morbidities and Severe Sequelae of TBI 6 7 Rehabilitation (Auditory, Cognitive, Vestibular, & Visual) Long Term Effects “Medically Ready Force…Ready Medical Force” 9
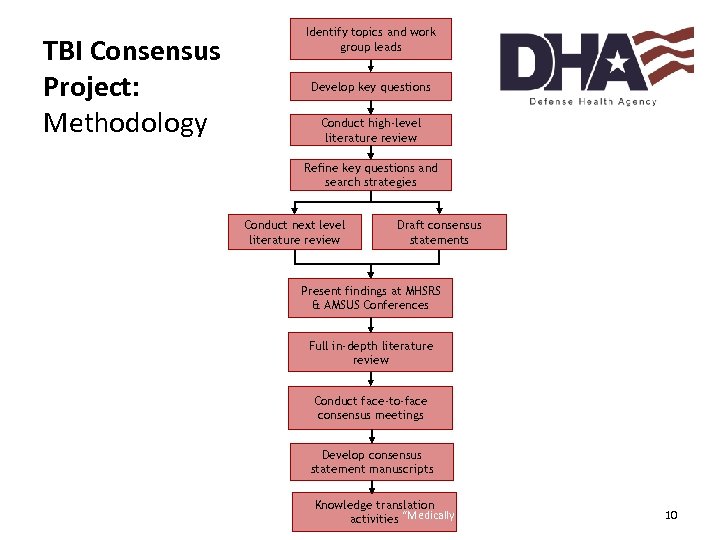 TBI Consensus Project: Methodology Identify topics and work group leads Develop key questions Conduct high-level literature review Refine key questions and search strategies Conduct next level literature review Draft consensus statements Present findings at MHSRS & AMSUS Conferences Full in-depth literature review Conduct face-to-face consensus meetings Develop consensus statement manuscripts Knowledge translation activities “Medically Ready Force…Ready Medical Force” 10
TBI Consensus Project: Methodology Identify topics and work group leads Develop key questions Conduct high-level literature review Refine key questions and search strategies Conduct next level literature review Draft consensus statements Present findings at MHSRS & AMSUS Conferences Full in-depth literature review Conduct face-to-face consensus meetings Develop consensus statement manuscripts Knowledge translation activities “Medically Ready Force…Ready Medical Force” 10
 Progress to Date ∎ Literature reviews have been conducted and research has been synthesized subject to tight timeline q Literature was prioritized based on study type (systematic reviews were prioritized over RCTs and observational studies), comprehensiveness, publication date, population (military vs civilian), and other factors identified by each work group ∎ Work groups conducted weekly/bi-weekly teleconferences to review evidence and draft executive statements ∎ 80 executive statements reported here are draft only; work is ongoing “Medically Ready Force…Ready Medical Force” 11
Progress to Date ∎ Literature reviews have been conducted and research has been synthesized subject to tight timeline q Literature was prioritized based on study type (systematic reviews were prioritized over RCTs and observational studies), comprehensiveness, publication date, population (military vs civilian), and other factors identified by each work group ∎ Work groups conducted weekly/bi-weekly teleconferences to review evidence and draft executive statements ∎ 80 executive statements reported here are draft only; work is ongoing “Medically Ready Force…Ready Medical Force” 11
 Next Steps ∎ Evidence gathering continues, and additional literature will be reviewed in order to fill gaps and ensure that the most relevant and current information is considered ∎ Work groups will continue to meet to refine executive statements; additional subject matter experts will participate as appropriate ∎ Once executive statements are finalized, work groups will produce manuscripts for publication ∎ Project represents a significant step in our ongoing commitment to improve the health and quality of care for Service members and veterans with TBI “Medically Ready Force…Ready Medical Force” 12
Next Steps ∎ Evidence gathering continues, and additional literature will be reviewed in order to fill gaps and ensure that the most relevant and current information is considered ∎ Work groups will continue to meet to refine executive statements; additional subject matter experts will participate as appropriate ∎ Once executive statements are finalized, work groups will produce manuscripts for publication ∎ Project represents a significant step in our ongoing commitment to improve the health and quality of care for Service members and veterans with TBI “Medically Ready Force…Ready Medical Force” 12
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Prevention of Traumatic Brain Injury Scott C. Livingston, Ph. D, PT, ATC Defense and Veterans Brain Injury Center Do. D Photo “Medically Ready Force…Ready Medical Force” 13
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Prevention of Traumatic Brain Injury Scott C. Livingston, Ph. D, PT, ATC Defense and Veterans Brain Injury Center Do. D Photo “Medically Ready Force…Ready Medical Force” 13
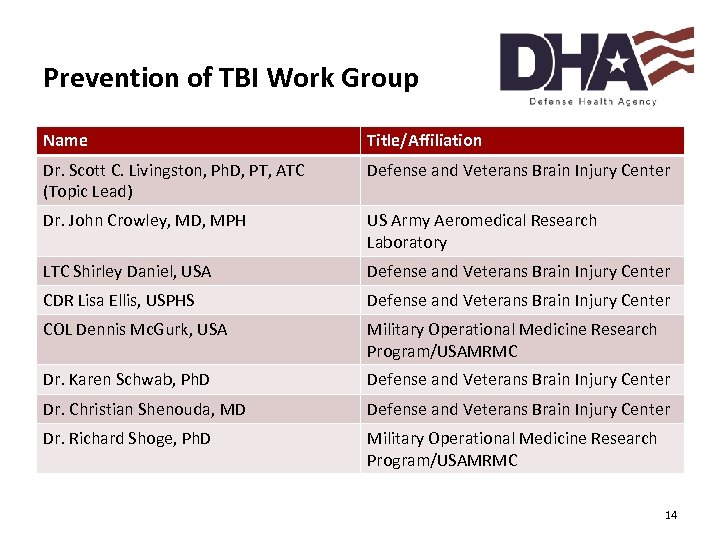 Prevention of TBI Work Group Name Title/Affiliation Dr. Scott C. Livingston, Ph. D, PT, ATC (Topic Lead) Defense and Veterans Brain Injury Center Dr. John Crowley, MD, MPH US Army Aeromedical Research Laboratory LTC Shirley Daniel, USA Defense and Veterans Brain Injury Center CDR Lisa Ellis, USPHS Defense and Veterans Brain Injury Center COL Dennis Mc. Gurk, USA Military Operational Medicine Research Program/USAMRMC Dr. Karen Schwab, Ph. D Defense and Veterans Brain Injury Center Dr. Christian Shenouda, MD Defense and Veterans Brain Injury Center Dr. Richard Shoge, Ph. D Military Operational Medicine Research Program/USAMRMC “Medically Ready Force…Ready Medical Force” 14
Prevention of TBI Work Group Name Title/Affiliation Dr. Scott C. Livingston, Ph. D, PT, ATC (Topic Lead) Defense and Veterans Brain Injury Center Dr. John Crowley, MD, MPH US Army Aeromedical Research Laboratory LTC Shirley Daniel, USA Defense and Veterans Brain Injury Center CDR Lisa Ellis, USPHS Defense and Veterans Brain Injury Center COL Dennis Mc. Gurk, USA Military Operational Medicine Research Program/USAMRMC Dr. Karen Schwab, Ph. D Defense and Veterans Brain Injury Center Dr. Christian Shenouda, MD Defense and Veterans Brain Injury Center Dr. Richard Shoge, Ph. D Military Operational Medicine Research Program/USAMRMC “Medically Ready Force…Ready Medical Force” 14
 Background: Prevention of TBI ∎ Service members at increased risk of TBI compared to civilian counterparts due to dangerous operational and training activities, high participation in sports and other recreational activities, and motorcycle use. ∎ Effective prevention strategies are needed to avoid or minimize short- and long-term detrimental health effects of TBI. “Medically Ready Force…Ready Medical Force” 15
Background: Prevention of TBI ∎ Service members at increased risk of TBI compared to civilian counterparts due to dangerous operational and training activities, high participation in sports and other recreational activities, and motorcycle use. ∎ Effective prevention strategies are needed to avoid or minimize short- and long-term detrimental health effects of TBI. “Medically Ready Force…Ready Medical Force” 15
 Prevention of TBI Properly designed protective helmets, correctly worn during high risk activities, reduces the injury severity and fatalities from TBI. 3 q Wearing military helmets reduces fatalities in training and deployed environments 3 In the military occupational environment, a protective effect of helmets has been convincingly shown for penetrating head trauma. q. Stronger evidence for penetrating head injury and severe blunt injury q. Limited evidence available on non-ballistic head injuries in military personnel; however, existing data suggests that helmets decrease the number and severity of injuries in “Medically Ready Force…Ready Medical Force” 16 combat scenarios
Prevention of TBI Properly designed protective helmets, correctly worn during high risk activities, reduces the injury severity and fatalities from TBI. 3 q Wearing military helmets reduces fatalities in training and deployed environments 3 In the military occupational environment, a protective effect of helmets has been convincingly shown for penetrating head trauma. q. Stronger evidence for penetrating head injury and severe blunt injury q. Limited evidence available on non-ballistic head injuries in military personnel; however, existing data suggests that helmets decrease the number and severity of injuries in “Medically Ready Force…Ready Medical Force” 16 combat scenarios
 Prevention of TBI q Do. D investment in recent combat helmet design and material innovations could significantly improve blunt impact protection provided by modern combat helmets. Helmets have been demonstrated to reduce the dose of primary blast pressure waves in non-human research studies. q There is no clinical data (i. e. human studies) to support the efficacy of helmets in protecting against TBI potentially caused by the less-well-understood primary blast pressure wave. The use of an appropriate helmet also reduces the risk of TBI in many other settings, ranging from sports to motorcycle driving. q Where a beneficial effect of helmets has been established, and such use is operationally feasible, service members’ use “Medically Ready Force…Ready Medical Force” 17 of protective equipment should be compulsory.
Prevention of TBI q Do. D investment in recent combat helmet design and material innovations could significantly improve blunt impact protection provided by modern combat helmets. Helmets have been demonstrated to reduce the dose of primary blast pressure waves in non-human research studies. q There is no clinical data (i. e. human studies) to support the efficacy of helmets in protecting against TBI potentially caused by the less-well-understood primary blast pressure wave. The use of an appropriate helmet also reduces the risk of TBI in many other settings, ranging from sports to motorcycle driving. q Where a beneficial effect of helmets has been established, and such use is operationally feasible, service members’ use “Medically Ready Force…Ready Medical Force” 17 of protective equipment should be compulsory.
 Prevention of TBI Multi-faceted fall prevention strategies are highly applicable to military settings and may reduce the risk and incidence of TBI. 4, 8 q. Certain interventions are highly effective in preventing falls such as workplace fall prevention or educational programs q. Studies in military populations needed to confirm the effectiveness of such interventions and consider other prevention strategies, including assessing association of falls with particular military occupations and locations 12 -13 q. Programs that include general education on fall prevention training and context or environmental-specific factors, such as proper lighting and shoe-wear, anti-skid devices, and fall protection from elevations, show the greatest promise for translation to the military. “Medically Ready Force…Ready Medical Force” 18
Prevention of TBI Multi-faceted fall prevention strategies are highly applicable to military settings and may reduce the risk and incidence of TBI. 4, 8 q. Certain interventions are highly effective in preventing falls such as workplace fall prevention or educational programs q. Studies in military populations needed to confirm the effectiveness of such interventions and consider other prevention strategies, including assessing association of falls with particular military occupations and locations 12 -13 q. Programs that include general education on fall prevention training and context or environmental-specific factors, such as proper lighting and shoe-wear, anti-skid devices, and fall protection from elevations, show the greatest promise for translation to the military. “Medically Ready Force…Ready Medical Force” 18
 Prevention of TBI The workgroup supports the Do. D's continuing aggressive efforts to implement a multifaceted strategy to offer maximum protection against head and brain injury resulting from motor vehicle collisions. 5 q. Military populations have many of the same risk factors as civilians for TBI resulting from motor vehicle collisions: younger age, drunk driving, speeding, distracted driving, and failure to use a seatbelt. 2 q. Several additional factors increasing risk for motor vehicle accidents in the military include: increased motorcycle use, higher sensation-seeking and impulsive behaviors, high levels of fatigue, deployment risk, and driving in combat environments. 5, 14 -17 “Medically Ready Force…Ready Medical Force” 19
Prevention of TBI The workgroup supports the Do. D's continuing aggressive efforts to implement a multifaceted strategy to offer maximum protection against head and brain injury resulting from motor vehicle collisions. 5 q. Military populations have many of the same risk factors as civilians for TBI resulting from motor vehicle collisions: younger age, drunk driving, speeding, distracted driving, and failure to use a seatbelt. 2 q. Several additional factors increasing risk for motor vehicle accidents in the military include: increased motorcycle use, higher sensation-seeking and impulsive behaviors, high levels of fatigue, deployment risk, and driving in combat environments. 5, 14 -17 “Medically Ready Force…Ready Medical Force” 19
 Prevention of TBI q. Programs and strategies that worked well are media campaigns, particularly carefully designed programs which are based in theory, and broadly and strategically disseminated. 2 q. Effective interventions are multipronged, involving two or more complementary approaches to addressing the problem. “Medically Ready Force…Ready Medical Force” 20
Prevention of TBI q. Programs and strategies that worked well are media campaigns, particularly carefully designed programs which are based in theory, and broadly and strategically disseminated. 2 q. Effective interventions are multipronged, involving two or more complementary approaches to addressing the problem. “Medically Ready Force…Ready Medical Force” 20
 Prevention of TBI § There is an inherent risk of injury (including TBI) among military service members engaged in combative sports and training. 6 -8 § Risk of head injury can be mitigated by implementation of screening procedures, safety education on concussion, instruction on general combative techniques, strict enforcement of competition rules, post-injury removal from training or competition, and the use of a graduated return to play protocol following a potentially concussive event. 6. q. Identification of risk factors is paramount to developing risk mitigation strategies “Medically Ready Force…Ready Medical Force” 21
Prevention of TBI § There is an inherent risk of injury (including TBI) among military service members engaged in combative sports and training. 6 -8 § Risk of head injury can be mitigated by implementation of screening procedures, safety education on concussion, instruction on general combative techniques, strict enforcement of competition rules, post-injury removal from training or competition, and the use of a graduated return to play protocol following a potentially concussive event. 6. q. Identification of risk factors is paramount to developing risk mitigation strategies “Medically Ready Force…Ready Medical Force” 21
 Prevention of TBI § Current educational interventions are helpful in improving short-term knowledge about concussions, but may not translate into long-term knowledge or changes in behavior. The work group recommends use of education and training strategies with greatest potential impact for increasing longterm knowledge (i. e. , knowledge retention) and behavior change (i. e. , knowledge application). 11 -12 q General awareness and prevention, knowledge of symptoms & willingness to report a concussive injury; research is limited on education as specific preventative measures. q Best educational practices & adult learning theory with focus on specific prevention approaches (e. g. , helmet use, motorcycle safety, fall reduction) will decrease risk of TBI. q More deliberate methodologically-sound research is needed to support education and knowledge translation efforts. “Medically Ready Force…Ready Medical Force” 22
Prevention of TBI § Current educational interventions are helpful in improving short-term knowledge about concussions, but may not translate into long-term knowledge or changes in behavior. The work group recommends use of education and training strategies with greatest potential impact for increasing longterm knowledge (i. e. , knowledge retention) and behavior change (i. e. , knowledge application). 11 -12 q General awareness and prevention, knowledge of symptoms & willingness to report a concussive injury; research is limited on education as specific preventative measures. q Best educational practices & adult learning theory with focus on specific prevention approaches (e. g. , helmet use, motorcycle safety, fall reduction) will decrease risk of TBI. q More deliberate methodologically-sound research is needed to support education and knowledge translation efforts. “Medically Ready Force…Ready Medical Force” 22
 Research Gaps: TBI Prevention § Evidence-based brain injury criteria scaled to humans for the development of helmets to protect against ballistic, blunt trauma and blast exposures. This will inform research on the use of combat helmets to mitigate risk of TBI associated with blunt head trauma and blast pressure waves. § Well-controlled studies evaluating the effectiveness of fall prevention strategies applied to a military population. § Examination of techniques and approaches to minimize the risk of TBI in motor vehicle crashes in the military. § Epidemiologic research on TBI associated with combative sports and training (acute and repeat TBI, cumulative effects). “Medically Ready Force…Ready Medical Force” 23
Research Gaps: TBI Prevention § Evidence-based brain injury criteria scaled to humans for the development of helmets to protect against ballistic, blunt trauma and blast exposures. This will inform research on the use of combat helmets to mitigate risk of TBI associated with blunt head trauma and blast pressure waves. § Well-controlled studies evaluating the effectiveness of fall prevention strategies applied to a military population. § Examination of techniques and approaches to minimize the risk of TBI in motor vehicle crashes in the military. § Epidemiologic research on TBI associated with combative sports and training (acute and repeat TBI, cumulative effects). “Medically Ready Force…Ready Medical Force” 23
 Research Gaps (cont. ) ∎ Research investigating risk reduction strategies in combative sports/training; secondary and long-term effects of TBI resulting from combative sports/training participation. ∎ Well controlled research studies evaluating the effectiveness of education and training strategies combined with media campaigns and other approaches to reduce the risk and incidence of TBI. “Medically Ready Force…Ready Medical Force” 24
Research Gaps (cont. ) ∎ Research investigating risk reduction strategies in combative sports/training; secondary and long-term effects of TBI resulting from combative sports/training participation. ∎ Well controlled research studies evaluating the effectiveness of education and training strategies combined with media campaigns and other approaches to reduce the risk and incidence of TBI. “Medically Ready Force…Ready Medical Force” 24
 Conclusions: TBI Prevention Ø There is limited evidence for the prevention of TBI, particularly studies focused on military and veteran populations. Ø Wearing of helmets reduces the severity of injury and fatalities from TBI; implementation of fall prevention strategies, and well-planned education and training programs may also reduce the risk for TBI. Ø Identifying and controlling risk factors associated with combative sports and training, and motor vehicle collisions will likely mitigate TBI risk and incidence. “Medically Ready Force…Ready Medical Force” 25
Conclusions: TBI Prevention Ø There is limited evidence for the prevention of TBI, particularly studies focused on military and veteran populations. Ø Wearing of helmets reduces the severity of injury and fatalities from TBI; implementation of fall prevention strategies, and well-planned education and training programs may also reduce the risk for TBI. Ø Identifying and controlling risk factors associated with combative sports and training, and motor vehicle collisions will likely mitigate TBI risk and incidence. “Medically Ready Force…Ready Medical Force” 25
 Conclusions (cont. ) Ø The overall quality and generalizability of evidence on prevention of TBI needs to be carefully considered when translating or extrapolating findings to the military and veteran populations. Ø The military has developed numerous prevention strategies to protect service members against TBI. Ø The military’s advantage in implementing these has been its ability to enforce rules and regulations, such as helmet use, speed limits and zero tolerance for impaired driving. Ø Such approaches can be more widely implemented but effectiveness needs to be studied in order to efficiently guide future efforts towards those that are most protective. “Medically Ready Force…Ready Medical Force” 26
Conclusions (cont. ) Ø The overall quality and generalizability of evidence on prevention of TBI needs to be carefully considered when translating or extrapolating findings to the military and veteran populations. Ø The military has developed numerous prevention strategies to protect service members against TBI. Ø The military’s advantage in implementing these has been its ability to enforce rules and regulations, such as helmet use, speed limits and zero tolerance for impaired driving. Ø Such approaches can be more widely implemented but effectiveness needs to be studied in order to efficiently guide future efforts towards those that are most protective. “Medically Ready Force…Ready Medical Force” 26
 Next Steps: TBI Prevention Ø Determine actual protection provided by modern combat helmets against major causes of TBI in the military. Ø Develop evidence-based design criteria for future combat helmets that will improve protection from blunt head trauma and blast overpressure. Ø Evaluate multifaceted programs to reduce/control risk factors associated with motor vehicle collisions. Ø Determine effectiveness of strategies targeting higher risktaking service members to reduce the incidence of TBI resulting from motorcycle riding and automobile driving. Ø Determine the degree to which return from deployment affects motor vehicle collisions. “Medically Ready Force…Ready Medical Force” 27
Next Steps: TBI Prevention Ø Determine actual protection provided by modern combat helmets against major causes of TBI in the military. Ø Develop evidence-based design criteria for future combat helmets that will improve protection from blunt head trauma and blast overpressure. Ø Evaluate multifaceted programs to reduce/control risk factors associated with motor vehicle collisions. Ø Determine effectiveness of strategies targeting higher risktaking service members to reduce the incidence of TBI resulting from motorcycle riding and automobile driving. Ø Determine the degree to which return from deployment affects motor vehicle collisions. “Medically Ready Force…Ready Medical Force” 27
 Next Steps (cont. ) Ø Determine the efficacy of steps to reduce the risk of TBI in combative sports & training; and the secondary and long-term effects of TBI resulting from combative sports/training participation. Ø Establish the effectiveness of fall prevention strategies proven useful in civilian populations to military populations and settings. Ø Evaluate the effectiveness of education & training approaches to enhance long-term knowledge and effect on behavior change among military personnel. Ø Assess the effectiveness of education & training strategies combined with media campaigns and other approaches in active duty populations, particularly those at most risk for TBI. “Medically Ready Force…Ready Medical Force” 28
Next Steps (cont. ) Ø Determine the efficacy of steps to reduce the risk of TBI in combative sports & training; and the secondary and long-term effects of TBI resulting from combative sports/training participation. Ø Establish the effectiveness of fall prevention strategies proven useful in civilian populations to military populations and settings. Ø Evaluate the effectiveness of education & training approaches to enhance long-term knowledge and effect on behavior change among military personnel. Ø Assess the effectiveness of education & training strategies combined with media campaigns and other approaches in active duty populations, particularly those at most risk for TBI. “Medically Ready Force…Ready Medical Force” 28
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Acute Concussion Kathy Helmick, MS, CRNP, ANP-BC, CNRN Defense and Veterans Brain Injury Center Do. D Photo “Medically Ready Force…Ready Medical Force” 29
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Acute Concussion Kathy Helmick, MS, CRNP, ANP-BC, CNRN Defense and Veterans Brain Injury Center Do. D Photo “Medically Ready Force…Ready Medical Force” 29
 Acute Concussion Work Group Name Title/Affiliation Katherine Helmick, MS, CRNP, ANPBC, CNRN (Topic Lead) Deputy Director, Defense and Veterans Brain Injury Center CDR Scott A. Klimp Director, Ft. Bragg Intrepid Spirit Center Theresa B. Lattimore Chief, Army TBI Program, OTSG Lt. Col Jeffrey C. Mc. Clean II Chief, Air Force TBI Program LCDR Joseph R. Newcomb DVBIC Site Director, Ft. Bragg Intrepid Spirit Center MAJ Thaddeus M. Pajak, DO DVBIC Site director, TBI Clinic, Ft. Drum CDR Randy G. Reese Chief, Navy TBI Program, BUMED “Medically Ready Force…Ready Medical Force” 30
Acute Concussion Work Group Name Title/Affiliation Katherine Helmick, MS, CRNP, ANPBC, CNRN (Topic Lead) Deputy Director, Defense and Veterans Brain Injury Center CDR Scott A. Klimp Director, Ft. Bragg Intrepid Spirit Center Theresa B. Lattimore Chief, Army TBI Program, OTSG Lt. Col Jeffrey C. Mc. Clean II Chief, Air Force TBI Program LCDR Joseph R. Newcomb DVBIC Site Director, Ft. Bragg Intrepid Spirit Center MAJ Thaddeus M. Pajak, DO DVBIC Site director, TBI Clinic, Ft. Drum CDR Randy G. Reese Chief, Navy TBI Program, BUMED “Medically Ready Force…Ready Medical Force” 30
 Background: Acute Concussion ∎ Majority of TBIs in both military and the civilian populations are mild TBI ∎ Effective diagnosis, assessment and management strategies in the acute phase is important for improvement of long-term outcomes after m. TBI ∎ Understanding the risk factors associated with persistent symptoms and poor prognosis will help inform the management of m. TBI ∎ This topic focuses on the diagnosis, assessment and management of m. TBI in the first seven days post-injury “Medically Ready Force…Ready Medical Force” 31
Background: Acute Concussion ∎ Majority of TBIs in both military and the civilian populations are mild TBI ∎ Effective diagnosis, assessment and management strategies in the acute phase is important for improvement of long-term outcomes after m. TBI ∎ Understanding the risk factors associated with persistent symptoms and poor prognosis will help inform the management of m. TBI ∎ This topic focuses on the diagnosis, assessment and management of m. TBI in the first seven days post-injury “Medically Ready Force…Ready Medical Force” 31
 Acute Concussion There are multiple clinical characteristics that may occur after a suspected head injury that can be used to evaluate for the presence of a neurosurgical lesion and therefore precipitate rapid evacuation for further evaluation and definitive care. 1 q. Signs: depressed skull, basal skull fracture, post-traumatic seizures, focal neurological deficits, persistent vomiting, decrease in Glasgow Coma Score (GCS) score, and previous neurosurgery q Evaluation of current Do. D standards and available innovative technologies to aid in the rapid evaluation of a neurosurgical lesion is needed “Medically Ready Force…Ready Medical Force” 32
Acute Concussion There are multiple clinical characteristics that may occur after a suspected head injury that can be used to evaluate for the presence of a neurosurgical lesion and therefore precipitate rapid evacuation for further evaluation and definitive care. 1 q. Signs: depressed skull, basal skull fracture, post-traumatic seizures, focal neurological deficits, persistent vomiting, decrease in Glasgow Coma Score (GCS) score, and previous neurosurgery q Evaluation of current Do. D standards and available innovative technologies to aid in the rapid evaluation of a neurosurgical lesion is needed “Medically Ready Force…Ready Medical Force” 32
 Acute Concussion There is modest evidence of utility of various acute concussion assessment tools. Limitations exist regarding reliability as well as heterogeneity in injuries and assessment. The lack of a diagnostic “gold standard, ” coupled with narrow study participants’ demographics, potentially limits generalizability to other populations. 2 q. Sport screening tests: relatively good sensitivity and specificity q. Technology studies: no clinical significance relationship q. Study populations are primarily athletes, and mostly all male, which limits generalizability to other populations “Medically Ready Force…Ready Medical Force” 33
Acute Concussion There is modest evidence of utility of various acute concussion assessment tools. Limitations exist regarding reliability as well as heterogeneity in injuries and assessment. The lack of a diagnostic “gold standard, ” coupled with narrow study participants’ demographics, potentially limits generalizability to other populations. 2 q. Sport screening tests: relatively good sensitivity and specificity q. Technology studies: no clinical significance relationship q. Study populations are primarily athletes, and mostly all male, which limits generalizability to other populations “Medically Ready Force…Ready Medical Force” 33
 Acute Concussion Emerging evidence demonstrates the benefit of multimodal testing to improve diagnostic and assessment accuracy. Research suggests that domains for further study include cognitive screening, symptom checklists, oculomotor function, and balance testing. 2 q. Importance of multimodal, multi-time based concussion evaluation process q. There was an “absence of valid research confirming the diagnostic accuracy and impact on improving outcomes of currently used sideline screening tests” “Medically Ready Force…Ready Medical Force” 34
Acute Concussion Emerging evidence demonstrates the benefit of multimodal testing to improve diagnostic and assessment accuracy. Research suggests that domains for further study include cognitive screening, symptom checklists, oculomotor function, and balance testing. 2 q. Importance of multimodal, multi-time based concussion evaluation process q. There was an “absence of valid research confirming the diagnostic accuracy and impact on improving outcomes of currently used sideline screening tests” “Medically Ready Force…Ready Medical Force” 34
 Acute Concussion Oculomotor assessment may be useful in detecting changes associated with mild TBI. While there are positive trends in this body of evidence, as yet the strength of evidence is insufficient, and further study with rigorous methodology is warranted. 3 q. Measurements of saccades, smooth pursuit, and convergence are useful in detecting changes associated with mild TBI q. Quality was limited by heterogeneous definitions of mild TBI, small study size, and other methodological issues “Medically Ready Force…Ready Medical Force” 35
Acute Concussion Oculomotor assessment may be useful in detecting changes associated with mild TBI. While there are positive trends in this body of evidence, as yet the strength of evidence is insufficient, and further study with rigorous methodology is warranted. 3 q. Measurements of saccades, smooth pursuit, and convergence are useful in detecting changes associated with mild TBI q. Quality was limited by heterogeneous definitions of mild TBI, small study size, and other methodological issues “Medically Ready Force…Ready Medical Force” 35
 Acute Concussion Evidence suggests that patient education interventions in the early post-injury period confer benefits on anxiety, paranoia, hostility and insomnia. However, patient education interventions are not consistently associated with improved outcomes or a consistent decrease in headache and visual symptoms. 4, 5 q. Mixed results on whether the educational interventions impacted post-concussion symptoms or return to work q. Need for targeted interventions focused on oculomotor dysfunction, and the potential that the unresolved headaches could be due to oculomotor dysfunction “Medically Ready Force…Ready Medical Force” 36
Acute Concussion Evidence suggests that patient education interventions in the early post-injury period confer benefits on anxiety, paranoia, hostility and insomnia. However, patient education interventions are not consistently associated with improved outcomes or a consistent decrease in headache and visual symptoms. 4, 5 q. Mixed results on whether the educational interventions impacted post-concussion symptoms or return to work q. Need for targeted interventions focused on oculomotor dysfunction, and the potential that the unresolved headaches could be due to oculomotor dysfunction “Medically Ready Force…Ready Medical Force” 36
 Acute Concussion Emerging evidence supports that after a brief period of rest, a concussed individual can begin a gradual and progressive return to pre-injury activity. The brief period of rest may assist the acute recovery period by mitigating symptoms and minimizing cerebral energy demands. Finally there is a paucity of data that defines “rest; ” either physical or cognitive rest. 5, 6 q Mixed results: two studies indicated that rest improved outcomes; three studies identified too much activity as detrimental to recovery and resulting in worse outcomes; four studies found no association between rest and outcomes q Clinical practice is trending towards individualized rehabilitation plans; patients are given more targeted interventions when compared to the “empiric rest” approach often utilized in the past decade “Medically Ready Force…Ready Medical Force” 37
Acute Concussion Emerging evidence supports that after a brief period of rest, a concussed individual can begin a gradual and progressive return to pre-injury activity. The brief period of rest may assist the acute recovery period by mitigating symptoms and minimizing cerebral energy demands. Finally there is a paucity of data that defines “rest; ” either physical or cognitive rest. 5, 6 q Mixed results: two studies indicated that rest improved outcomes; three studies identified too much activity as detrimental to recovery and resulting in worse outcomes; four studies found no association between rest and outcomes q Clinical practice is trending towards individualized rehabilitation plans; patients are given more targeted interventions when compared to the “empiric rest” approach often utilized in the past decade “Medically Ready Force…Ready Medical Force” 37
 Acute Concussion There is currently no FDA-approved pharmacotherapy for the indication of mild TBI. Further, there is insufficient evidence to support pharmacotherapy for acute concussion. Current pharmacotherapy for acute concussion is based on management of symptoms; however, further studies are needed to determine effects of pharmacotherapies on acute concussive symptoms. 7 q. One RCT found that sertraline is more effective than placebo in preventing depressive disorder in adults after a TBI “Medically Ready Force…Ready Medical Force” 38
Acute Concussion There is currently no FDA-approved pharmacotherapy for the indication of mild TBI. Further, there is insufficient evidence to support pharmacotherapy for acute concussion. Current pharmacotherapy for acute concussion is based on management of symptoms; however, further studies are needed to determine effects of pharmacotherapies on acute concussive symptoms. 7 q. One RCT found that sertraline is more effective than placebo in preventing depressive disorder in adults after a TBI “Medically Ready Force…Ready Medical Force” 38
 Acute Concussion There may be predictors of mild TBI outcomes (including return to work) that can be used to inform clinical decision-making in the acute management of mild TBI. Demographic factors that have been found to be associated with mild TBI outcomes include sex, age, educational level and occupation. The presence of comorbidities including a past history of brain injury have also been found to be predictors in mild TBI outcomes. 8, 9 q Mixed evidence for predictors of mild TBI outcomes in the acute management of mild TBI q The literature is contradictory in this area and no systematic reviews were found in military or veteran populations “Medically Ready Force…Ready Medical Force” 39
Acute Concussion There may be predictors of mild TBI outcomes (including return to work) that can be used to inform clinical decision-making in the acute management of mild TBI. Demographic factors that have been found to be associated with mild TBI outcomes include sex, age, educational level and occupation. The presence of comorbidities including a past history of brain injury have also been found to be predictors in mild TBI outcomes. 8, 9 q Mixed evidence for predictors of mild TBI outcomes in the acute management of mild TBI q The literature is contradictory in this area and no systematic reviews were found in military or veteran populations “Medically Ready Force…Ready Medical Force” 39
 Research Gaps: Acute Concussion ∎ Studies on military or veteran populations are needed ∎ Studies on assessment using Standardized Assessment of Concussion (SCAT)-5 and pharmacologic therapy for acute mild TBI is lacking ∎ Additional robust studies that can be generalizable to all populations are needed for all interventions “Medically Ready Force…Ready Medical Force” 40
Research Gaps: Acute Concussion ∎ Studies on military or veteran populations are needed ∎ Studies on assessment using Standardized Assessment of Concussion (SCAT)-5 and pharmacologic therapy for acute mild TBI is lacking ∎ Additional robust studies that can be generalizable to all populations are needed for all interventions “Medically Ready Force…Ready Medical Force” 40
 Conclusions and Next Steps Ø Limited high quality evidence addressing both key questions Ø Many authors called for more robust studies Ø Some also included pediatric studies in addition to the studies of adults Ø The overall quality and generalizability of the evidence will need to be carefully considered when translating or extrapolating findings to the military and veteran populations for the acute management of TBI “Medically Ready Force…Ready Medical Force” 41
Conclusions and Next Steps Ø Limited high quality evidence addressing both key questions Ø Many authors called for more robust studies Ø Some also included pediatric studies in addition to the studies of adults Ø The overall quality and generalizability of the evidence will need to be carefully considered when translating or extrapolating findings to the military and veteran populations for the acute management of TBI “Medically Ready Force…Ready Medical Force” 41
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Peri-Injury Management of Severe and Penetrating TBI Don Marion, MD Defense and Veterans Brain Injury Center U. S. Navy photo by PM 2 Marjorie Mc. Namme “Medically Ready Force…Ready Medical Force” 42
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Peri-Injury Management of Severe and Penetrating TBI Don Marion, MD Defense and Veterans Brain Injury Center U. S. Navy photo by PM 2 Marjorie Mc. Namme “Medically Ready Force…Ready Medical Force” 42
 Peri-Injury Management Work Group Name Title/Affiliation Donald Marion, MD (Topic Lead) Senior Consultant, DVBIC Saafan Malik, MD, Director of Research, DVBIC Defense Centers of Excellence for PH & TBI J 3 -Health Care Operations Scott Marshall, MD Critical Care and Vascular Neurology, Intermountain Healthcare COL Randy Mc. Cafferty, MD, FAANS Associate Professor of Surgery, USUHS AF/SG Consultant for Neurosurgery; SAMMC Shelly Timmons, MD, Ph. D, FACS, Professor and Vice Chair for Administration FAANS Director of Neurotrauma, Penn State University Milton S. Hershey Medical Center. Alex Valadka, MD Professor and Chair, Department of Neurosurgery, Virginia Commonwealth University, President of the American Association of Neurological Surgeons “Medically Ready Force…Ready Medical Force” 43
Peri-Injury Management Work Group Name Title/Affiliation Donald Marion, MD (Topic Lead) Senior Consultant, DVBIC Saafan Malik, MD, Director of Research, DVBIC Defense Centers of Excellence for PH & TBI J 3 -Health Care Operations Scott Marshall, MD Critical Care and Vascular Neurology, Intermountain Healthcare COL Randy Mc. Cafferty, MD, FAANS Associate Professor of Surgery, USUHS AF/SG Consultant for Neurosurgery; SAMMC Shelly Timmons, MD, Ph. D, FACS, Professor and Vice Chair for Administration FAANS Director of Neurotrauma, Penn State University Milton S. Hershey Medical Center. Alex Valadka, MD Professor and Chair, Department of Neurosurgery, Virginia Commonwealth University, President of the American Association of Neurological Surgeons “Medically Ready Force…Ready Medical Force” 43
 Background: Peri-Injury Management ∎ The management of severe and penetrating TBI in the field, during transportation, in the emergency room, and in the first 48 hours of critical care can have significant consequences on outcomes, including mortality, complications, and long-term recovery and function ∎ The goal is to enhance cerebral perfusion, and limit cerebral ischemia ∎ Recent studies emphasize the importance of restoring the blood pressure as quickly as possible, and caution that only experienced providers should attempt endotracheal intubation ∎ An emerging area of research is the development of technology for non-invasive detection and monitoring of disturbed cerebral physiology and metabolism, and detection of post-traumatic intracranial mass lesions “Medically Ready Force…Ready Medical Force” 44
Background: Peri-Injury Management ∎ The management of severe and penetrating TBI in the field, during transportation, in the emergency room, and in the first 48 hours of critical care can have significant consequences on outcomes, including mortality, complications, and long-term recovery and function ∎ The goal is to enhance cerebral perfusion, and limit cerebral ischemia ∎ Recent studies emphasize the importance of restoring the blood pressure as quickly as possible, and caution that only experienced providers should attempt endotracheal intubation ∎ An emerging area of research is the development of technology for non-invasive detection and monitoring of disturbed cerebral physiology and metabolism, and detection of post-traumatic intracranial mass lesions “Medically Ready Force…Ready Medical Force” 44
 Peri-Injury Management Pre-hospital assessment and treatment of patients suspected of having a severe brain injury should improve or preserve cerebral perfusion and oxygenation. q. Multiple physiologic and metabolic studies, including positron emission tomography (PET), cerebral blood flow, and microdialysis studies, confirm that severe TBI is associated with reduced cerebral perfusion and oxygenation. q. Optimizing cerebral perfusion and oxygenation is recommended by the Brain Trauma Foundation and Joint Trauma System clinical practice guidelines. “Medically Ready Force…Ready Medical Force” 45
Peri-Injury Management Pre-hospital assessment and treatment of patients suspected of having a severe brain injury should improve or preserve cerebral perfusion and oxygenation. q. Multiple physiologic and metabolic studies, including positron emission tomography (PET), cerebral blood flow, and microdialysis studies, confirm that severe TBI is associated with reduced cerebral perfusion and oxygenation. q. Optimizing cerebral perfusion and oxygenation is recommended by the Brain Trauma Foundation and Joint Trauma System clinical practice guidelines. “Medically Ready Force…Ready Medical Force” 45
 Peri-Injury Management Intubation in the prehospital setting should only be attempted by experienced providers. Otherwise, supplemental oxygen by face mask may be most appropriate. q. One meta-analysis concluded that prehospital intubation by providers with limited experience was associated with a twofold increase in mortality. 1 q. A systematic review did not support any benefit from prehospital intubation and mechanical ventilation after TBI. 2 “Medically Ready Force…Ready Medical Force” 46
Peri-Injury Management Intubation in the prehospital setting should only be attempted by experienced providers. Otherwise, supplemental oxygen by face mask may be most appropriate. q. One meta-analysis concluded that prehospital intubation by providers with limited experience was associated with a twofold increase in mortality. 1 q. A systematic review did not support any benefit from prehospital intubation and mechanical ventilation after TBI. 2 “Medically Ready Force…Ready Medical Force” 46
 Peri-Injury Management Prophylactic hyperventilation is not recommended. q. Hypocarbic patients presenting to the trauma center had an in-hospital mortality of 77%. Those presenting with normal p. CO 2 had a mortality of 15%. 3 q. The clinical practice guidelines by the Brain Trauma Foundation and Joint Trauma System support this statement. “Medically Ready Force…Ready Medical Force” 47
Peri-Injury Management Prophylactic hyperventilation is not recommended. q. Hypocarbic patients presenting to the trauma center had an in-hospital mortality of 77%. Those presenting with normal p. CO 2 had a mortality of 15%. 3 q. The clinical practice guidelines by the Brain Trauma Foundation and Joint Trauma System support this statement. “Medically Ready Force…Ready Medical Force” 47
 Peri-Injury Management Hypotension should be aggressively treated for a target systolic blood pressure above 110 mm. Hg in adults, regardless of possible penetrating torso injuries. q. In one cohort study, there was no threshold and a linear association between the lowest prehospital systolic blood pressure and severity-adjusted probability of death. 4 q. The target level of 110 mm. Hg for systolic blood pressure is supported by the Joint Trauma System clinical practice guideline. “Medically Ready Force…Ready Medical Force” 48
Peri-Injury Management Hypotension should be aggressively treated for a target systolic blood pressure above 110 mm. Hg in adults, regardless of possible penetrating torso injuries. q. In one cohort study, there was no threshold and a linear association between the lowest prehospital systolic blood pressure and severity-adjusted probability of death. 4 q. The target level of 110 mm. Hg for systolic blood pressure is supported by the Joint Trauma System clinical practice guideline. “Medically Ready Force…Ready Medical Force” 48
 Peri-Injury Management The optimal fluid for resuscitation of hemorrhagic shock is blood products or whole blood. If blood products are not available, or as an adjunct to blood products, isotonic or 3% hypertonic saline are recommended for resuscitation of hemorrhagic shock. q. Studies show that the best way to restore perfusion and adequate tissue oxygenation is to restore normal levels of blood products. 5, 6 q. Rapid volume resuscitation is critical to restoring perfusion to the brain. Clinical studies show that 3% hypertonic saline may be as efficacious as isotonic saline solutions. 7, 8 “Medically Ready Force…Ready Medical Force” 49
Peri-Injury Management The optimal fluid for resuscitation of hemorrhagic shock is blood products or whole blood. If blood products are not available, or as an adjunct to blood products, isotonic or 3% hypertonic saline are recommended for resuscitation of hemorrhagic shock. q. Studies show that the best way to restore perfusion and adequate tissue oxygenation is to restore normal levels of blood products. 5, 6 q. Rapid volume resuscitation is critical to restoring perfusion to the brain. Clinical studies show that 3% hypertonic saline may be as efficacious as isotonic saline solutions. 7, 8 “Medically Ready Force…Ready Medical Force” 49
 Peri-Injury Management Mannitol is not recommended for patients at risk for shock because it is a diuretic. 7, 8 q. There were no clinically important differences in mortality, neurological outcomes, and ICP reduction observed between hypertonic saline or mannitol for severe TBI. “Medically Ready Force…Ready Medical Force” 50
Peri-Injury Management Mannitol is not recommended for patients at risk for shock because it is a diuretic. 7, 8 q. There were no clinically important differences in mortality, neurological outcomes, and ICP reduction observed between hypertonic saline or mannitol for severe TBI. “Medically Ready Force…Ready Medical Force” 50
 Peri-Injury Management Temperature resuscitation should target 35 -36 degrees Celsius. Hyperthermia should be aggressively avoided for patients with severe TBI. 9, 10 q. In studies of short-term cooling strategies, there was lower mortality and more common good neurologic outcomes with hypothermia. “Medically Ready Force…Ready Medical Force” 51
Peri-Injury Management Temperature resuscitation should target 35 -36 degrees Celsius. Hyperthermia should be aggressively avoided for patients with severe TBI. 9, 10 q. In studies of short-term cooling strategies, there was lower mortality and more common good neurologic outcomes with hypothermia. “Medically Ready Force…Ready Medical Force” 51
 Peri-Injury Management Ketamine is a safe and effective sedative for agitated TBI patients in the pre-hospital environment. 11 q. The included trials of propofol vs. midazolam and ketamine vs. sufentanil found no difference between agents in ICP and cerebral perfusion pressure (CPP). q. Ketamine is currently widely used by the military and is safe in the appropriate setting. “Medically Ready Force…Ready Medical Force” 52
Peri-Injury Management Ketamine is a safe and effective sedative for agitated TBI patients in the pre-hospital environment. 11 q. The included trials of propofol vs. midazolam and ketamine vs. sufentanil found no difference between agents in ICP and cerebral perfusion pressure (CPP). q. Ketamine is currently widely used by the military and is safe in the appropriate setting. “Medically Ready Force…Ready Medical Force” 52
 Peri-Injury Management All patients suspected of having a severe TBI should be transported to a trauma center with neurosurgical capabilities as quickly and safely as possible, using the mode of transportation most appropriate for the distance to the trauma center, weather conditions, and the operational security environment. Whenever possible, the transport team should include an appropriately trained physician. 12 -15 q There was no significant difference in 24 -hour or six-month outcomes based on ground or air transport. q There was decreased mortality with the addition of a physician during prehospital care. “Medically Ready Force…Ready Medical Force” 53
Peri-Injury Management All patients suspected of having a severe TBI should be transported to a trauma center with neurosurgical capabilities as quickly and safely as possible, using the mode of transportation most appropriate for the distance to the trauma center, weather conditions, and the operational security environment. Whenever possible, the transport team should include an appropriately trained physician. 12 -15 q There was no significant difference in 24 -hour or six-month outcomes based on ground or air transport. q There was decreased mortality with the addition of a physician during prehospital care. “Medically Ready Force…Ready Medical Force” 53
 Peri-Injury Management ICP monitoring is recommended for all patients with a severe TBI who have a GCS less than 9 and an abnormal CT scan. 16 q. ICP monitoring significantly decreased the mortality rate of patients with severe TBI, compared to no ICP monitoring. q. Multiple publications from the past 30 years show that ICP monitoring can provide critical information about who needs treatment for brain swelling. 17 “Medically Ready Force…Ready Medical Force” 54
Peri-Injury Management ICP monitoring is recommended for all patients with a severe TBI who have a GCS less than 9 and an abnormal CT scan. 16 q. ICP monitoring significantly decreased the mortality rate of patients with severe TBI, compared to no ICP monitoring. q. Multiple publications from the past 30 years show that ICP monitoring can provide critical information about who needs treatment for brain swelling. 17 “Medically Ready Force…Ready Medical Force” 54
 Peri-Injury Management Direct brain tissue oxygen monitoring is not necessary in the prehospital setting. ∎ Evidence support for this statement: q. An observational study found no significant benefit of tissue oxygen directed therapy on mortality or functional outcomes. 18 ∎ Other support for this statement: q. No clinical studies have shown that manipulation of brain tissue oxygen alters outcomes, and this is invasive technology that should not be attempted in the pre-hospital setting. “Medically Ready Force…Ready Medical Force” 55
Peri-Injury Management Direct brain tissue oxygen monitoring is not necessary in the prehospital setting. ∎ Evidence support for this statement: q. An observational study found no significant benefit of tissue oxygen directed therapy on mortality or functional outcomes. 18 ∎ Other support for this statement: q. No clinical studies have shown that manipulation of brain tissue oxygen alters outcomes, and this is invasive technology that should not be attempted in the pre-hospital setting. “Medically Ready Force…Ready Medical Force” 55
 Peri-Injury Management Pre-hospital transcranial Doppler performed by an experienced provider can detect abnormal perfusion. 19 q. Transcranial Doppler used in the prehospital setting identified patients whose cerebral perfusion was impaired. q. Only those patients with impaired perfusion required neurosurgery. “Medically Ready Force…Ready Medical Force” 56
Peri-Injury Management Pre-hospital transcranial Doppler performed by an experienced provider can detect abnormal perfusion. 19 q. Transcranial Doppler used in the prehospital setting identified patients whose cerebral perfusion was impaired. q. Only those patients with impaired perfusion required neurosurgery. “Medically Ready Force…Ready Medical Force” 56
 Peri-Injury Management Non-invasive near infrared spectroscopy (NIRS) can detect superficial intracranial hematomas. 20 q. When compared to results of computed tomography (CT) scans, the near-infrared scanner obtained a sensitivity of 93. 3% and a specificity of 78. 6%. “Medically Ready Force…Ready Medical Force” 57
Peri-Injury Management Non-invasive near infrared spectroscopy (NIRS) can detect superficial intracranial hematomas. 20 q. When compared to results of computed tomography (CT) scans, the near-infrared scanner obtained a sensitivity of 93. 3% and a specificity of 78. 6%. “Medically Ready Force…Ready Medical Force” 57
 Research Gaps: Peri-Injury Management ∎ Combat-related and military-specific literature is lacking. ∎ There are gaps in literature for the following interventions: q. Fiber optic ICP monitoring q. Monitoring of neurophysiologic status q. Head positioning or protection of the spine q. Wound care “Medically Ready Force…Ready Medical Force” 58
Research Gaps: Peri-Injury Management ∎ Combat-related and military-specific literature is lacking. ∎ There are gaps in literature for the following interventions: q. Fiber optic ICP monitoring q. Monitoring of neurophysiologic status q. Head positioning or protection of the spine q. Wound care “Medically Ready Force…Ready Medical Force” 58
 Conclusions and Next Steps Ø The most recent and robust SRs investigate the following interventions: Mode of transportation, medication choice for sedation, clinical assessment using the t. GCS, and ICP monitoring. Ø Several SRs and RCTs appeared to be well-designed, but were underpowered to show significant harms or benefits of the interventions of interest. “Medically Ready Force…Ready Medical Force” 59
Conclusions and Next Steps Ø The most recent and robust SRs investigate the following interventions: Mode of transportation, medication choice for sedation, clinical assessment using the t. GCS, and ICP monitoring. Ø Several SRs and RCTs appeared to be well-designed, but were underpowered to show significant harms or benefits of the interventions of interest. “Medically Ready Force…Ready Medical Force” 59
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Biomarkers in TBI: Radiologic and Non. Radiologic Thomas De. Graba, MD National Intrepid Center of Excellence U. S. Air Force photo by SA Freddy Toruno “Medically Ready Force…Ready Medical Force” 60
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Biomarkers in TBI: Radiologic and Non. Radiologic Thomas De. Graba, MD National Intrepid Center of Excellence U. S. Air Force photo by SA Freddy Toruno “Medically Ready Force…Ready Medical Force” 60
 Background: Biomarkers in TBI ∎ TBI subpopulation heterogeneity related to force type, severity, injury location, clinical course, clinical comorbidities, and prognosis represent distinct challenges in determining the extent of injury in a particular individual ∎ Validated radiological or other biomarkers are still needed for diagnosing mild TBI and characterization of neural network injury for managing (including monitoring and response to treatment and prognosis) all severities of TBI ∎ Conventional imaging modalities, such as computed tomography (CT), are useful in diagnosing moderate and severe TBI ∎ Lack of these validated biomarkers confounds the progress of research, including developing new treatments, but the field is quickly evolving “Medically Ready Force…Ready Medical Force” 61
Background: Biomarkers in TBI ∎ TBI subpopulation heterogeneity related to force type, severity, injury location, clinical course, clinical comorbidities, and prognosis represent distinct challenges in determining the extent of injury in a particular individual ∎ Validated radiological or other biomarkers are still needed for diagnosing mild TBI and characterization of neural network injury for managing (including monitoring and response to treatment and prognosis) all severities of TBI ∎ Conventional imaging modalities, such as computed tomography (CT), are useful in diagnosing moderate and severe TBI ∎ Lack of these validated biomarkers confounds the progress of research, including developing new treatments, but the field is quickly evolving “Medically Ready Force…Ready Medical Force” 61
 Radiological Work Group Name Title/Affiliation CDR Grant Bonavia, MD, Ph. D (Topic Lead) Interim Chief, Department of Research, Chief, Imaging & Measurement Devices, National Intrepid Center of Excellence (NICo. E), Walter Reed National Military Medical Center (WRNMMC) John Butman, MD, Ph. D Chief, Neuroradiology Section and Lead Physician, MRI Section, Radiology and Imaging Science, Clinical Center of the National Institutes of Health (NIH), Principal Investigator, Image Processing Core, Center for Neuroscience and Regenerative Medicine Thomas De. Graba, MD Acting National Director, Defense and Veterans Brain Injury Center (DVBIC) John Ollinger, Ph. D Head of Image Processing, NICo. E, WRNMMC Dzung Pham, Ph. D Director, Image Processing Core, Center for Neuroscience and Regenerative Medicine, The Henry M. Jackson Foundation for the Advancement of Military Medicine Gerard Riedy, MD, Ph. D Head of Neuroimaging, NICo. E, WRNMMC “Medically Ready Force…Ready Medical Force” 62
Radiological Work Group Name Title/Affiliation CDR Grant Bonavia, MD, Ph. D (Topic Lead) Interim Chief, Department of Research, Chief, Imaging & Measurement Devices, National Intrepid Center of Excellence (NICo. E), Walter Reed National Military Medical Center (WRNMMC) John Butman, MD, Ph. D Chief, Neuroradiology Section and Lead Physician, MRI Section, Radiology and Imaging Science, Clinical Center of the National Institutes of Health (NIH), Principal Investigator, Image Processing Core, Center for Neuroscience and Regenerative Medicine Thomas De. Graba, MD Acting National Director, Defense and Veterans Brain Injury Center (DVBIC) John Ollinger, Ph. D Head of Image Processing, NICo. E, WRNMMC Dzung Pham, Ph. D Director, Image Processing Core, Center for Neuroscience and Regenerative Medicine, The Henry M. Jackson Foundation for the Advancement of Military Medicine Gerard Riedy, MD, Ph. D Head of Neuroimaging, NICo. E, WRNMMC “Medically Ready Force…Ready Medical Force” 62
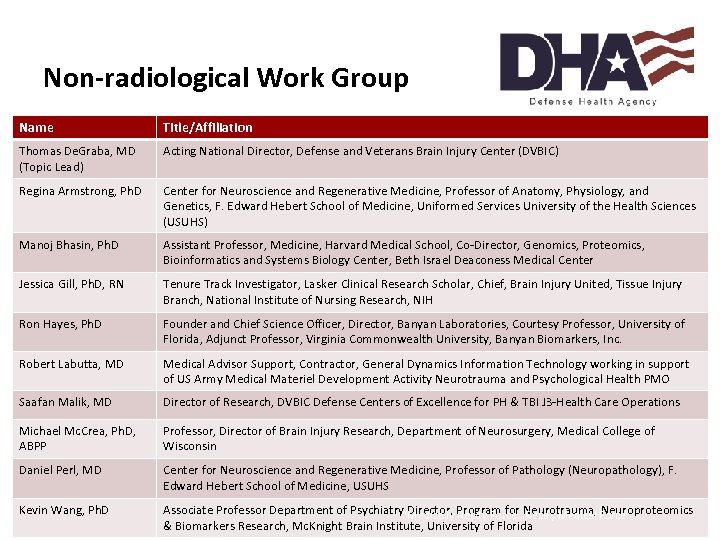 Non-radiological Work Group Name Title/Affiliation Thomas De. Graba, MD (Topic Lead) Acting National Director, Defense and Veterans Brain Injury Center (DVBIC) Regina Armstrong, Ph. D Center for Neuroscience and Regenerative Medicine, Professor of Anatomy, Physiology, and Genetics, F. Edward Hebert School of Medicine, Uniformed Services University of the Health Sciences (USUHS) Manoj Bhasin, Ph. D Assistant Professor, Medicine, Harvard Medical School, Co-Director, Genomics, Proteomics, Bioinformatics and Systems Biology Center, Beth Israel Deaconess Medical Center Jessica Gill, Ph. D, RN Tenure Track Investigator, Lasker Clinical Research Scholar, Chief, Brain Injury United, Tissue Injury Branch, National Institute of Nursing Research, NIH Ron Hayes, Ph. D Founder and Chief Science Officer, Director, Banyan Laboratories, Courtesy Professor, University of Florida, Adjunct Professor, Virginia Commonwealth University, Banyan Biomarkers, Inc. Robert Labutta, MD Medical Advisor Support, Contractor, General Dynamics Information Technology working in support of US Army Medical Materiel Development Activity Neurotrauma and Psychological Health PMO Saafan Malik, MD Director of Research, DVBIC Defense Centers of Excellence for PH & TBI J 3 -Health Care Operations Michael Mc. Crea, Ph. D, ABPP Professor, Director of Brain Injury Research, Department of Neurosurgery, Medical College of Wisconsin Daniel Perl, MD Center for Neuroscience and Regenerative Medicine, Professor of Pathology (Neuropathology), F. Edward Hebert School of Medicine, USUHS Kevin Wang, Ph. D Associate Professor Department of Psychiatry Director, Program for Neurotrauma, Neuroproteomics “Medically Ready Force…Ready Medical Force” 63 & Biomarkers Research, Mc. Knight Brain Institute, University of Florida
Non-radiological Work Group Name Title/Affiliation Thomas De. Graba, MD (Topic Lead) Acting National Director, Defense and Veterans Brain Injury Center (DVBIC) Regina Armstrong, Ph. D Center for Neuroscience and Regenerative Medicine, Professor of Anatomy, Physiology, and Genetics, F. Edward Hebert School of Medicine, Uniformed Services University of the Health Sciences (USUHS) Manoj Bhasin, Ph. D Assistant Professor, Medicine, Harvard Medical School, Co-Director, Genomics, Proteomics, Bioinformatics and Systems Biology Center, Beth Israel Deaconess Medical Center Jessica Gill, Ph. D, RN Tenure Track Investigator, Lasker Clinical Research Scholar, Chief, Brain Injury United, Tissue Injury Branch, National Institute of Nursing Research, NIH Ron Hayes, Ph. D Founder and Chief Science Officer, Director, Banyan Laboratories, Courtesy Professor, University of Florida, Adjunct Professor, Virginia Commonwealth University, Banyan Biomarkers, Inc. Robert Labutta, MD Medical Advisor Support, Contractor, General Dynamics Information Technology working in support of US Army Medical Materiel Development Activity Neurotrauma and Psychological Health PMO Saafan Malik, MD Director of Research, DVBIC Defense Centers of Excellence for PH & TBI J 3 -Health Care Operations Michael Mc. Crea, Ph. D, ABPP Professor, Director of Brain Injury Research, Department of Neurosurgery, Medical College of Wisconsin Daniel Perl, MD Center for Neuroscience and Regenerative Medicine, Professor of Pathology (Neuropathology), F. Edward Hebert School of Medicine, USUHS Kevin Wang, Ph. D Associate Professor Department of Psychiatry Director, Program for Neurotrauma, Neuroproteomics “Medically Ready Force…Ready Medical Force” 63 & Biomarkers Research, Mc. Knight Brain Institute, University of Florida
 Scope of Literature Review Radiological Non-radiological What is the effectiveness of imaging techniques in managing TBI? What is the effectiveness of non-radiological assessment in managing TBI? Patients with TBI of any severity Advanced neuroimaging techniques including: • Structural imaging (magnetic resonance imaging [MR], computed tomography [CT], susceptibility weighted imaging [SWI], contrast) • Diffusion tensor imaging (DTI) • Functional MRI (f. MRI) • Positron emission tomography (PET) • Single photon emission computed tomography (SPECT) • Transcranial Doppler ultrasound (TCD) • Perfusion imaging Non-radiological assessments: • Fluid biomarkers • Genomics • Electroencephalography (EEG) • Magnetoencephalography (MEG) • Biomarkers for chronic traumatic encephalopathy (CTE) • Autonomics Test performance or clinical utility in identifying or managing TBI (or CTE) Studies published within the last seven years “Medically Ready Force…Ready Medical Force” 64
Scope of Literature Review Radiological Non-radiological What is the effectiveness of imaging techniques in managing TBI? What is the effectiveness of non-radiological assessment in managing TBI? Patients with TBI of any severity Advanced neuroimaging techniques including: • Structural imaging (magnetic resonance imaging [MR], computed tomography [CT], susceptibility weighted imaging [SWI], contrast) • Diffusion tensor imaging (DTI) • Functional MRI (f. MRI) • Positron emission tomography (PET) • Single photon emission computed tomography (SPECT) • Transcranial Doppler ultrasound (TCD) • Perfusion imaging Non-radiological assessments: • Fluid biomarkers • Genomics • Electroencephalography (EEG) • Magnetoencephalography (MEG) • Biomarkers for chronic traumatic encephalopathy (CTE) • Autonomics Test performance or clinical utility in identifying or managing TBI (or CTE) Studies published within the last seven years “Medically Ready Force…Ready Medical Force” 64
 Biomarkers – Radiologic Structural CT, MRI, Susceptibility Weighted Imaging (SWI), and Contrast There is a significant body of evidence demonstrating the utility of CT in diagnosis and management of individuals with acute head injury and suspected intracranial pathology based on presentation and clinical evaluation. Evidence supports the use of MRI (including SWI), when available and not contraindicated, in acute and chronic head injury in the setting of new onset, persistent, or worsening symptoms after 72 hours. Contrast-enhanced MRI is rarely used in TBI imaging and has not yet been shown to have a beneficial role. 1 -4, 51 “Medically Ready Force…Ready Medical Force” 65
Biomarkers – Radiologic Structural CT, MRI, Susceptibility Weighted Imaging (SWI), and Contrast There is a significant body of evidence demonstrating the utility of CT in diagnosis and management of individuals with acute head injury and suspected intracranial pathology based on presentation and clinical evaluation. Evidence supports the use of MRI (including SWI), when available and not contraindicated, in acute and chronic head injury in the setting of new onset, persistent, or worsening symptoms after 72 hours. Contrast-enhanced MRI is rarely used in TBI imaging and has not yet been shown to have a beneficial role. 1 -4, 51 “Medically Ready Force…Ready Medical Force” 65
 Biomarkers – Radiologic Diffusion Tensor Imaging (DTI) DTI has low clinical utility for diagnostic, prognostic, and monitoring applications in acute or chronic TBI at this time. Although more advanced diffusion imaging techniques have been proposed, additional studies are needed to evaluate their potential. 5 -8 ∎ Inconsistency in findings in group analyses; specificity likely insufficient at individual patient level ∎ Usefulness is currently limited to detection of lesions “Medically Ready Force…Ready Medical Force” 66
Biomarkers – Radiologic Diffusion Tensor Imaging (DTI) DTI has low clinical utility for diagnostic, prognostic, and monitoring applications in acute or chronic TBI at this time. Although more advanced diffusion imaging techniques have been proposed, additional studies are needed to evaluate their potential. 5 -8 ∎ Inconsistency in findings in group analyses; specificity likely insufficient at individual patient level ∎ Usefulness is currently limited to detection of lesions “Medically Ready Force…Ready Medical Force” 66
 Functional Magnetic Resonance Imaging (f. MRI) There is no significant body of evidence to support the use of either task-based or resting-state f. MRI for the diagnosis or monitoring of TBI patients. Task-based f. MRI has yielded varying and contradictory findings in group studies. Restingstate studies report changes in multiple networks but primarily in the default mode network and thalamus. These studies have been almost exclusively group analyses and have not had sufficient power to be useful at the level of individual subjects. 1, 2, 4, 9 ∎ Some studies found f. MRI useful in differentiating between TBI patients and controls, findings are inconsistent ∎ Emerging literature regarding use of f. MRI in acute stage “Medically Ready Force…Ready Medical Force” 67
Functional Magnetic Resonance Imaging (f. MRI) There is no significant body of evidence to support the use of either task-based or resting-state f. MRI for the diagnosis or monitoring of TBI patients. Task-based f. MRI has yielded varying and contradictory findings in group studies. Restingstate studies report changes in multiple networks but primarily in the default mode network and thalamus. These studies have been almost exclusively group analyses and have not had sufficient power to be useful at the level of individual subjects. 1, 2, 4, 9 ∎ Some studies found f. MRI useful in differentiating between TBI patients and controls, findings are inconsistent ∎ Emerging literature regarding use of f. MRI in acute stage “Medically Ready Force…Ready Medical Force” 67
 Positron Emission Tomography (PET) Fluorodeoxyglucose (FDG) PET has no significant body of evidence to support current clinical utility for diagnosis or monitoring of acute or chronic TBI patients. PET imaging with ligands specific for amyloid or tau have undetermined potential for clinical application to the diagnosis of CTE. 3, 9, 10 ∎ Limited data exists on FDG PET in acute TBI ∎ Some studies suggest regional hypometabolism in mild TBI with persistent post-concussive symptoms, but consistent/repeatable patterns have not been identified ∎ CTE pathology in TBI suggests potential for future clinical utility of specific PET imaging ligands; not yet validated “Medically Ready Force…Ready Medical Force” 68
Positron Emission Tomography (PET) Fluorodeoxyglucose (FDG) PET has no significant body of evidence to support current clinical utility for diagnosis or monitoring of acute or chronic TBI patients. PET imaging with ligands specific for amyloid or tau have undetermined potential for clinical application to the diagnosis of CTE. 3, 9, 10 ∎ Limited data exists on FDG PET in acute TBI ∎ Some studies suggest regional hypometabolism in mild TBI with persistent post-concussive symptoms, but consistent/repeatable patterns have not been identified ∎ CTE pathology in TBI suggests potential for future clinical utility of specific PET imaging ligands; not yet validated “Medically Ready Force…Ready Medical Force” 68
 Single Photon Emission Computed Tomography (SPECT) SPECT imaging has no significant body of evidence to support routine clinical utility for diagnosis or monitoring of acute or chronic TBI patients at this time. A small number of relatively recent reports describe specific areas of potential application which is considered to have low to intermediate likelihood of successful translation into clinical application. ∎ Support for SPECT imaging for diagnosis and monitoring TBI stems primarily from a single systematic review, 11 which lacked consistent/repeatable findings and included a heterogeneous subject population ∎ Areas of potential application include evaluating mild TBI patients with post-concussive headache and investigating cognitive dysfunction following moderate-to-severe TBI “Medically Ready Force…Ready Medical Force” 69
Single Photon Emission Computed Tomography (SPECT) SPECT imaging has no significant body of evidence to support routine clinical utility for diagnosis or monitoring of acute or chronic TBI patients at this time. A small number of relatively recent reports describe specific areas of potential application which is considered to have low to intermediate likelihood of successful translation into clinical application. ∎ Support for SPECT imaging for diagnosis and monitoring TBI stems primarily from a single systematic review, 11 which lacked consistent/repeatable findings and included a heterogeneous subject population ∎ Areas of potential application include evaluating mild TBI patients with post-concussive headache and investigating cognitive dysfunction following moderate-to-severe TBI “Medically Ready Force…Ready Medical Force” 69
 Transcranial Doppler Ultrasound (TCD) ∎ TCD is useful in severe TBI for identifying and monitoring progression of post-traumatic cerebral vasospasm leading to treatment for delayed cerebral ischemia. 12, 13 ∎ TCD measured disruption of cerebrovasomotor reactivity (CVR) in mild TBI is associated with acute concussive events and rate of recovery. CVR is further correlated with severity of persistent post-concussive cognitive deficits. 5, 12, 14, 15, 52 q. Reproducibility and non-invasive testing capabilities of TCD supports studies for its use as a diagnostic tool for mild TBI and marker for recovery. q 2012 Report to Congress: Comparative Effectiveness of Neuroimaging Modalities on the Detection of Traumatic Brain Injury 52 “Medically Ready Force…Ready Medical Force” 70
Transcranial Doppler Ultrasound (TCD) ∎ TCD is useful in severe TBI for identifying and monitoring progression of post-traumatic cerebral vasospasm leading to treatment for delayed cerebral ischemia. 12, 13 ∎ TCD measured disruption of cerebrovasomotor reactivity (CVR) in mild TBI is associated with acute concussive events and rate of recovery. CVR is further correlated with severity of persistent post-concussive cognitive deficits. 5, 12, 14, 15, 52 q. Reproducibility and non-invasive testing capabilities of TCD supports studies for its use as a diagnostic tool for mild TBI and marker for recovery. q 2012 Report to Congress: Comparative Effectiveness of Neuroimaging Modalities on the Detection of Traumatic Brain Injury 52 “Medically Ready Force…Ready Medical Force” 70
 Perfusion and Magnetic Resonance (MR) Spectroscopy ∎ Perfusion imaging (CT or MRI based) has no significant body of evidence to support routine clinical utility for diagnosis or monitoring of acute or chronic TBI patients at this time. q. There are no comprehensive reviews or substantial body of individual papers in the literature that point towards a clinical utility for perfusion imaging in TBI at this time. ∎ The current body of literature does not support the use of MR spectroscopy for clinical care of patients with TBI. “Medically Ready Force…Ready Medical Force” 71
Perfusion and Magnetic Resonance (MR) Spectroscopy ∎ Perfusion imaging (CT or MRI based) has no significant body of evidence to support routine clinical utility for diagnosis or monitoring of acute or chronic TBI patients at this time. q. There are no comprehensive reviews or substantial body of individual papers in the literature that point towards a clinical utility for perfusion imaging in TBI at this time. ∎ The current body of literature does not support the use of MR spectroscopy for clinical care of patients with TBI. “Medically Ready Force…Ready Medical Force” 71
 Genomics ∎ Genetic variants relate to cognitive symptoms following TBI, affecting genes related to cell death, cell proliferation, inflammation and brain development. 16 -23 q. Correlations to outcome include BDNF, APOε 4, and COMT, among others ∎ Gene-expression alterations are associated with recovery following mild TBI, with the inflammatory pathways focusing around NF most often implicated. 24 -26 B are ∎ Recent studies implicate epigenetic modifications and noncoding RNA in recovery from TBI, but there are very few studies published in this area. 27, 28 “Medically Ready Force…Ready Medical Force” 72
Genomics ∎ Genetic variants relate to cognitive symptoms following TBI, affecting genes related to cell death, cell proliferation, inflammation and brain development. 16 -23 q. Correlations to outcome include BDNF, APOε 4, and COMT, among others ∎ Gene-expression alterations are associated with recovery following mild TBI, with the inflammatory pathways focusing around NF most often implicated. 24 -26 B are ∎ Recent studies implicate epigenetic modifications and noncoding RNA in recovery from TBI, but there are very few studies published in this area. 27, 28 “Medically Ready Force…Ready Medical Force” 72
 GFAP and UCH-L 1* Serum/plasma protein biomarkers GFAP and UCH-L 1 are of high sensitivity and specificity as a diagnostics tool in the evaluation and monitoring of mild TBI patients. 29 -32 ∎ Large cohort study found GFAP and UCH-L 1 levels accurately predicted presence of intracranial lesions 36 -144 hours and within first 16 hours post injury, respectively ∎ Two observational studies found GFAP and UCH-L 1 to be effective in differentiating CT positive and CT negative findings in post-injury period “Medically Ready Force…Ready Medical Force” *GFAP: glial fibrillary acidic protein; UCH-L 1: ubiquitin carboxyl-terminal hydrolase isoenzyme L 1 73
GFAP and UCH-L 1* Serum/plasma protein biomarkers GFAP and UCH-L 1 are of high sensitivity and specificity as a diagnostics tool in the evaluation and monitoring of mild TBI patients. 29 -32 ∎ Large cohort study found GFAP and UCH-L 1 levels accurately predicted presence of intracranial lesions 36 -144 hours and within first 16 hours post injury, respectively ∎ Two observational studies found GFAP and UCH-L 1 to be effective in differentiating CT positive and CT negative findings in post-injury period “Medically Ready Force…Ready Medical Force” *GFAP: glial fibrillary acidic protein; UCH-L 1: ubiquitin carboxyl-terminal hydrolase isoenzyme L 1 73
 S 100β and Neuron-specific enolase (NSE) After severe TBI, elevated serum S 100β and NSE protein concentrations are associated with unfavorable prognosis or mortality but optimal thresholds for discrimination have not been determined. 33, 34 ∎ One observational study found increased S 100β and NSE serum levels within three days post-injury in severe TBI patients are associated with outcomes at three months ∎ Another study found overall S 100β levels measured in first five days and NSE levels at 72 hours post-injury were highly predictive of mortality “Medically Ready Force…Ready Medical Force” 74
S 100β and Neuron-specific enolase (NSE) After severe TBI, elevated serum S 100β and NSE protein concentrations are associated with unfavorable prognosis or mortality but optimal thresholds for discrimination have not been determined. 33, 34 ∎ One observational study found increased S 100β and NSE serum levels within three days post-injury in severe TBI patients are associated with outcomes at three months ∎ Another study found overall S 100β levels measured in first five days and NSE levels at 72 hours post-injury were highly predictive of mortality “Medically Ready Force…Ready Medical Force” 74
 Other Fluid Biomarkers Very recent studies indicate biomarker analysis of cerebrospinal fluid can be highly informative as the most proximate biofluid to the site of brain injury, but insufficient data is available to draw conclusive findings. 35 ∎ Seven individual studies were identified with analysis of cerebrospinal fluid samples but only two reported results that could be combined in meta-analysis ∎ Limited data precluded analysis of pooled data “Medically Ready Force…Ready Medical Force” 75
Other Fluid Biomarkers Very recent studies indicate biomarker analysis of cerebrospinal fluid can be highly informative as the most proximate biofluid to the site of brain injury, but insufficient data is available to draw conclusive findings. 35 ∎ Seven individual studies were identified with analysis of cerebrospinal fluid samples but only two reported results that could be combined in meta-analysis ∎ Limited data precluded analysis of pooled data “Medically Ready Force…Ready Medical Force” 75
 Near Infrared Spectroscopy (NIRS), Electroencephalography (EEG) ∎ In adults, near infra-red scanning and q. EEG are useful in assessing need for CT scan after mild TBI. 36 -37 ∎ q. EEG was initially overestimated as a diagnostic test for mild TBI. Recent studies indicate a potential use of q. EEG as a marker of injury and recovery but there is insufficient evidence for recommending clinical use. 1, 10, 38, 39 ∎ EEG is recommended for TBI patients with unexplained and persistent altered consciousness to evaluate for non-convulsive seizures. 40, 41 “Medically Ready Force…Ready Medical Force” 76
Near Infrared Spectroscopy (NIRS), Electroencephalography (EEG) ∎ In adults, near infra-red scanning and q. EEG are useful in assessing need for CT scan after mild TBI. 36 -37 ∎ q. EEG was initially overestimated as a diagnostic test for mild TBI. Recent studies indicate a potential use of q. EEG as a marker of injury and recovery but there is insufficient evidence for recommending clinical use. 1, 10, 38, 39 ∎ EEG is recommended for TBI patients with unexplained and persistent altered consciousness to evaluate for non-convulsive seizures. 40, 41 “Medically Ready Force…Ready Medical Force” 76
 Evoked Potentials (EPs), Magnetoencephalography (MEG) ∎ There is insufficient evidence for recommending the clinical use of evoked potentials (EPs) and event-related potentials (ERPs). 42 -44 ∎ MEG imaging is still in the research phase. Evidence is not sufficient to support clinical use to aid in diagnosis of TBI on an individual basis. 4 “Medically Ready Force…Ready Medical Force” 77
Evoked Potentials (EPs), Magnetoencephalography (MEG) ∎ There is insufficient evidence for recommending the clinical use of evoked potentials (EPs) and event-related potentials (ERPs). 42 -44 ∎ MEG imaging is still in the research phase. Evidence is not sufficient to support clinical use to aid in diagnosis of TBI on an individual basis. 4 “Medically Ready Force…Ready Medical Force” 77
 Oculomotor Assessment Evidence from oculomotor assessments is rapidly accumulating for a possible diagnostic role in acute injury and measure of recovery in m. TBI. However, the evidence is currently insufficient to make a recommendation for the use of eye movement analysis in the diagnosis or recovery of mild TBI. 45 -47 § Digital recordings during different types of eye movements can reveal dysfunction in neuro-anatomical systems § Eye movement analysis provides multi-modal function test of diffuse and diverse pathways known to be dysfunctional in mild TBI and may be useful in diagnosis and monitoring “Medically Ready Force…Ready Medical Force” 78
Oculomotor Assessment Evidence from oculomotor assessments is rapidly accumulating for a possible diagnostic role in acute injury and measure of recovery in m. TBI. However, the evidence is currently insufficient to make a recommendation for the use of eye movement analysis in the diagnosis or recovery of mild TBI. 45 -47 § Digital recordings during different types of eye movements can reveal dysfunction in neuro-anatomical systems § Eye movement analysis provides multi-modal function test of diffuse and diverse pathways known to be dysfunctional in mild TBI and may be useful in diagnosis and monitoring “Medically Ready Force…Ready Medical Force” 78
 Autonomics ∎ Autonomic impairment, as measured by heart rate variability and baroreflex sensitivity, is significantly associated with increased mortality after severe traumatic brain injury. ∎ Autonomic disturbance in mild TBI is associated with persistent cognitive deficits as measured by heart rate variability and cerebral vasomotor reactivity. “Medically Ready Force…Ready Medical Force” 79
Autonomics ∎ Autonomic impairment, as measured by heart rate variability and baroreflex sensitivity, is significantly associated with increased mortality after severe traumatic brain injury. ∎ Autonomic disturbance in mild TBI is associated with persistent cognitive deficits as measured by heart rate variability and cerebral vasomotor reactivity. “Medically Ready Force…Ready Medical Force” 79
 Chronic Traumatic Encephalopathy (CTE) The use of neuroimaging and non-radiologic biomarkers has yet to achieve the goal of contributing to establishing a clinical diagnosis of CTE in at-risk patients. § This statement was based on four systematic reviews 48 -50 § Few studies have reported on use of biomarkers in CTE § A few PET-ligands have recently been reported to bind to pathologic tau; sensitivity and specificity is unclear § Impediments to progress include the lack of validated clinical diagnostic criteria, the current need to establish CTE diagnosis at autopsy, and confounding factors related to other neurodegenerative disorders with overlapping pathologic constituents “Medically Ready Force…Ready Medical Force” 80
Chronic Traumatic Encephalopathy (CTE) The use of neuroimaging and non-radiologic biomarkers has yet to achieve the goal of contributing to establishing a clinical diagnosis of CTE in at-risk patients. § This statement was based on four systematic reviews 48 -50 § Few studies have reported on use of biomarkers in CTE § A few PET-ligands have recently been reported to bind to pathologic tau; sensitivity and specificity is unclear § Impediments to progress include the lack of validated clinical diagnostic criteria, the current need to establish CTE diagnosis at autopsy, and confounding factors related to other neurodegenerative disorders with overlapping pathologic constituents “Medically Ready Force…Ready Medical Force” 80
 Research Gaps: Biomarkers ∎ High-quality research with well-defined methods and populations, including control groups, needs to be conducted with both radiological and non-radiological biomarkers ∎ Combining biomarkers and machine learning techniques should be researched as they relate to managing TBI “Medically Ready Force…Ready Medical Force” 81
Research Gaps: Biomarkers ∎ High-quality research with well-defined methods and populations, including control groups, needs to be conducted with both radiological and non-radiological biomarkers ∎ Combining biomarkers and machine learning techniques should be researched as they relate to managing TBI “Medically Ready Force…Ready Medical Force” 81
 Conclusions and Next Steps Ø Research evolving with mounting evidence on the majority of biomarkers, including radiological and non-radiological biomarkers Ø Few biomarkers currently have sufficient evidence of clinical utility in the management of TBI Ø Additional research is planned for a number of biomarkers, particularly those for which studies have been published recently “Medically Ready Force…Ready Medical Force” 82
Conclusions and Next Steps Ø Research evolving with mounting evidence on the majority of biomarkers, including radiological and non-radiological biomarkers Ø Few biomarkers currently have sufficient evidence of clinical utility in the management of TBI Ø Additional research is planned for a number of biomarkers, particularly those for which studies have been published recently “Medically Ready Force…Ready Medical Force” 82
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Behavioral Health Consequences of TBI: mild TBI Co-morbidities and Severe Sequelae Jonathan Wolf, MD National Intrepid Center of Excellence “Medically Ready Force…Ready Medical Force” 83
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Behavioral Health Consequences of TBI: mild TBI Co-morbidities and Severe Sequelae Jonathan Wolf, MD National Intrepid Center of Excellence “Medically Ready Force…Ready Medical Force” 83
 Work Group Name Title/Affiliation Geoffrey Grammer, MD (Topic Lead) Chief Medical Officer, Greenbrook TMS Neuro. Health Centers Jonathan Wolf, MD (Topic Lead) Attending Psychiatrist, Walter Reed National Military Medicine Center, National Intrepid Center of Excellence David Williamson, MD Neuropsychiatrist, Texas Institute for Rehabilitation and Research “Medically Ready Force…Ready Medical Force” 84
Work Group Name Title/Affiliation Geoffrey Grammer, MD (Topic Lead) Chief Medical Officer, Greenbrook TMS Neuro. Health Centers Jonathan Wolf, MD (Topic Lead) Attending Psychiatrist, Walter Reed National Military Medicine Center, National Intrepid Center of Excellence David Williamson, MD Neuropsychiatrist, Texas Institute for Rehabilitation and Research “Medically Ready Force…Ready Medical Force” 84
 Background: Behavioral Health ∎ Behavioral health conditions have profound effects on the quality of life for military service members and veterans, as well as their families, colleagues, and society ∎ The interaction between TBI and behavioral health conditions remains an active area of investigation, in the behavioral health of veteran and military populations ∎ Greater understanding of the behavioral health impact of TBI can help ameliorate or prevent some adverse outcomes among military service members and veterans “Medically Ready Force…Ready Medical Force” 85
Background: Behavioral Health ∎ Behavioral health conditions have profound effects on the quality of life for military service members and veterans, as well as their families, colleagues, and society ∎ The interaction between TBI and behavioral health conditions remains an active area of investigation, in the behavioral health of veteran and military populations ∎ Greater understanding of the behavioral health impact of TBI can help ameliorate or prevent some adverse outcomes among military service members and veterans “Medically Ready Force…Ready Medical Force” 85
 Scope of Literature Review: Behavioral Health ∎ Key Question 1: In patients with a history of mild TBI, what are the short- and long-term consequences of the TBI exposure on behavioral health outcomes? ∎ Key Question 2: In patients with a history of moderate to severe TBI, what are the short- and long-term consequences of the TBI exposure on behavioral health outcomes? “Medically Ready Force…Ready Medical Force” 86
Scope of Literature Review: Behavioral Health ∎ Key Question 1: In patients with a history of mild TBI, what are the short- and long-term consequences of the TBI exposure on behavioral health outcomes? ∎ Key Question 2: In patients with a history of moderate to severe TBI, what are the short- and long-term consequences of the TBI exposure on behavioral health outcomes? “Medically Ready Force…Ready Medical Force” 86
 Behavioral Health In patients with a history of mild TBI, there is insufficient data to conclude that mild TBI results in an increased risk of mental health or substance use disorders other than an increased rate of PTSD and a possible transient increased risk of depression. 110 q One study showed increased depression following mild TBI compared to controls without TBI 5 “Medically Ready Force…Ready Medical Force” 87
Behavioral Health In patients with a history of mild TBI, there is insufficient data to conclude that mild TBI results in an increased risk of mental health or substance use disorders other than an increased rate of PTSD and a possible transient increased risk of depression. 110 q One study showed increased depression following mild TBI compared to controls without TBI 5 “Medically Ready Force…Ready Medical Force” 87
 Behavioral Health Among patients with a history of mild TBI, behavioral health symptoms correlate with a greater degree of morbidity. ∎ Evidence support for this statement: 4, 8, 11 q. A correlation between mild TBI and depression and anxiety symptoms 4, 11 q. Disability and physical symptoms more strongly associated with PTSD symptoms than with the injury in mild TBI 8 “Medically Ready Force…Ready Medical Force” 88
Behavioral Health Among patients with a history of mild TBI, behavioral health symptoms correlate with a greater degree of morbidity. ∎ Evidence support for this statement: 4, 8, 11 q. A correlation between mild TBI and depression and anxiety symptoms 4, 11 q. Disability and physical symptoms more strongly associated with PTSD symptoms than with the injury in mild TBI 8 “Medically Ready Force…Ready Medical Force” 88
 Behavioral Health There is insufficient data to conclude that in mild TBI there is an increased risk of adverse impact on quality of life or employment. 2 q. While there were a number of studies showing an increase in disability in patients with TBI overall, data looking solely at mild TBI was inconclusive 2 “Medically Ready Force…Ready Medical Force” 89
Behavioral Health There is insufficient data to conclude that in mild TBI there is an increased risk of adverse impact on quality of life or employment. 2 q. While there were a number of studies showing an increase in disability in patients with TBI overall, data looking solely at mild TBI was inconclusive 2 “Medically Ready Force…Ready Medical Force” 89
 Behavioral Health Moderate to severe TBI is associated with increased rates of major depression, suicide, aggression, psychotic illness and apathy syndromes. 1, 12 q. Mean prevalence of depression was reported as 30% in this population, with increased rates of suicide 1, 12 q. Several studies suggest that injuries to the frontal lobes carry higher risk 12 “Medically Ready Force…Ready Medical Force” 90
Behavioral Health Moderate to severe TBI is associated with increased rates of major depression, suicide, aggression, psychotic illness and apathy syndromes. 1, 12 q. Mean prevalence of depression was reported as 30% in this population, with increased rates of suicide 1, 12 q. Several studies suggest that injuries to the frontal lobes carry higher risk 12 “Medically Ready Force…Ready Medical Force” 90
 Behavioral Health Moderate to severe TBI is associated with adverse impacts on self-report quality of life and employment. The impact of moderate to severe TBI on criminal behaviors and rates of incarceration is uncertain. 12 -17 q. Low social support was correlated with low quality of life in patients with moderate to severe TBI 13 q. Participants with severe injuries were more likely to be unemployed one-year post-injury (compared to mild and moderate TBI)14 “Medically Ready Force…Ready Medical Force” 91
Behavioral Health Moderate to severe TBI is associated with adverse impacts on self-report quality of life and employment. The impact of moderate to severe TBI on criminal behaviors and rates of incarceration is uncertain. 12 -17 q. Low social support was correlated with low quality of life in patients with moderate to severe TBI 13 q. Participants with severe injuries were more likely to be unemployed one-year post-injury (compared to mild and moderate TBI)14 “Medically Ready Force…Ready Medical Force” 91
 Behavioral Health While behavioral changes have been described in post-mortem confirmed cases of CTE, the current state of the literature precludes drawing empiric causality between brain injury associated CTE and behavioral symptoms. 18 q. Studies were significantly underpowered to draw any significant conclusions 18 q. Further research on this topic is necessary “Medically Ready Force…Ready Medical Force” 92
Behavioral Health While behavioral changes have been described in post-mortem confirmed cases of CTE, the current state of the literature precludes drawing empiric causality between brain injury associated CTE and behavioral symptoms. 18 q. Studies were significantly underpowered to draw any significant conclusions 18 q. Further research on this topic is necessary “Medically Ready Force…Ready Medical Force” 92
 Research Gaps: Behavioral Health ∎ Further research needed to disentangle behavioral health symptoms from other causes and TBI effects ∎ Most existing literature analyzed mild TBI and moderate to severe TBI together despite their significant differences ∎ Many studies show behavioral health co-occurring conditions increase with TBI severity, but inclusion of mild TBI patients dilutes results for more severely affected ∎ Future research may delineate between TBI severities when reporting and analyzing outcomes of interest “Medically Ready Force…Ready Medical Force” 93
Research Gaps: Behavioral Health ∎ Further research needed to disentangle behavioral health symptoms from other causes and TBI effects ∎ Most existing literature analyzed mild TBI and moderate to severe TBI together despite their significant differences ∎ Many studies show behavioral health co-occurring conditions increase with TBI severity, but inclusion of mild TBI patients dilutes results for more severely affected ∎ Future research may delineate between TBI severities when reporting and analyzing outcomes of interest “Medically Ready Force…Ready Medical Force” 93
 Conclusions and Next Steps Ø Behavioral health and substance use disorders (including PTSD) are associated with TBI at all severities, but a causal relationship is unknown and hard to disentangle Ø For mild TBI, there is insufficient data to conclude that there is any increased risk attributable to brain injury other than a time limited increase in risk of depression Ø For moderate to severe TBI, the majority of the evidence reports increased risk for depression, suicide, aggression, and lower functional status and unemployment Ø The review highlighted need for more research overall but particularly for the causal link between TBI and suicide as well as other behavioral health disorders “Medically Ready Force…Ready Medical Force” 94
Conclusions and Next Steps Ø Behavioral health and substance use disorders (including PTSD) are associated with TBI at all severities, but a causal relationship is unknown and hard to disentangle Ø For mild TBI, there is insufficient data to conclude that there is any increased risk attributable to brain injury other than a time limited increase in risk of depression Ø For moderate to severe TBI, the majority of the evidence reports increased risk for depression, suicide, aggression, and lower functional status and unemployment Ø The review highlighted need for more research overall but particularly for the causal link between TBI and suicide as well as other behavioral health disorders “Medically Ready Force…Ready Medical Force” 94
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Rehabilitation Linda Picon, MCD, CCC-SLP Department of Veterans Affairs “Medically Ready Force…Ready Medical Force” 95
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Rehabilitation Linda Picon, MCD, CCC-SLP Department of Veterans Affairs “Medically Ready Force…Ready Medical Force” 95
 Work Group Name Title/Affiliation Katie Stout, PT, DPT, NCS, MBA (Topic Lead) Director of Clinical Affairs, DVBIC Felix Barker, OD, MS, FAAO Associate Director of Research, Vision Center of Excellence Lynn Henselman, Ph. D Deputy Division Chief, Defense Hearing Center of Excellence Paul Pasquina, MD Chief, Department of Rehabilitation, Walter Reed National Military Medical Center Linda Picon, MCD, CCC-SLP Senior Consultant, Veterans Health Administration Office of Rehabilitation and Prosthetic Services CDR Randy Reese, MSC U. S. Navy, Senior Neuropsychologist, Intrepid Spirit Concussion Recovery Center “Medically Ready Force…Ready Medical Force” 96
Work Group Name Title/Affiliation Katie Stout, PT, DPT, NCS, MBA (Topic Lead) Director of Clinical Affairs, DVBIC Felix Barker, OD, MS, FAAO Associate Director of Research, Vision Center of Excellence Lynn Henselman, Ph. D Deputy Division Chief, Defense Hearing Center of Excellence Paul Pasquina, MD Chief, Department of Rehabilitation, Walter Reed National Military Medical Center Linda Picon, MCD, CCC-SLP Senior Consultant, Veterans Health Administration Office of Rehabilitation and Prosthetic Services CDR Randy Reese, MSC U. S. Navy, Senior Neuropsychologist, Intrepid Spirit Concussion Recovery Center “Medically Ready Force…Ready Medical Force” 96
 Additional Subject Matter Experts Auditory Visual Carlos Esquivel, MD Geeta Girdher, OD Tanisha Hammill, MPH, Ph. D Lynn Greenspan, OD, Ph. D COL Lakeisha Henry, MC, FS Paul Koons, MS, CLVT, CBIS Jeremy Nelson, Ph. D Natasha Merezhinskaya, Ph. D Victoria Tepe, Ph. D Bre Myers, Au. D, Ph. D Marcy Pape, MPT Suzanne Wickum, OD “Medically Ready Force…Ready Medical Force” 97
Additional Subject Matter Experts Auditory Visual Carlos Esquivel, MD Geeta Girdher, OD Tanisha Hammill, MPH, Ph. D Lynn Greenspan, OD, Ph. D COL Lakeisha Henry, MC, FS Paul Koons, MS, CLVT, CBIS Jeremy Nelson, Ph. D Natasha Merezhinskaya, Ph. D Victoria Tepe, Ph. D Bre Myers, Au. D, Ph. D Marcy Pape, MPT Suzanne Wickum, OD “Medically Ready Force…Ready Medical Force” 97
 Background ∎ Rehabilitation is an important aspect of TBI care focused on optimizing patient outcomes, including quality of life and function. ∎ Among active duty service members, unique considerations include: return to duty, fitness for deployment and combat, and future exposures to TBI. ∎ Since rehabilitation of TBI is a broad topic, the focus of this review was auditory, cognitive, vestibular, and visual rehabilitation. “Medically Ready Force…Ready Medical Force” 98
Background ∎ Rehabilitation is an important aspect of TBI care focused on optimizing patient outcomes, including quality of life and function. ∎ Among active duty service members, unique considerations include: return to duty, fitness for deployment and combat, and future exposures to TBI. ∎ Since rehabilitation of TBI is a broad topic, the focus of this review was auditory, cognitive, vestibular, and visual rehabilitation. “Medically Ready Force…Ready Medical Force” 98
 Rehabilitation: Cognitive Rehabilitation ∎ Cognitive rehabilitation may reduce cognitive symptoms and the adverse effects of cognitive impairments, and improve functioning across all levels of TBI severity. There are no reported adverse effects. 1 -13 ∎ The evidence on the effectiveness and comparative effectiveness of various modes, settings and approaches to cognitive rehabilitation for all TBI severities is inconclusive. q. There is limited and inconsistent support for post-acute comprehensive, interdisciplinary services, cognitive skills training, psychotherapeutic interventions and compensatory strategy interventions, including training with assistive technologies. “Medically Ready Force…Ready Medical Force” 99
Rehabilitation: Cognitive Rehabilitation ∎ Cognitive rehabilitation may reduce cognitive symptoms and the adverse effects of cognitive impairments, and improve functioning across all levels of TBI severity. There are no reported adverse effects. 1 -13 ∎ The evidence on the effectiveness and comparative effectiveness of various modes, settings and approaches to cognitive rehabilitation for all TBI severities is inconclusive. q. There is limited and inconsistent support for post-acute comprehensive, interdisciplinary services, cognitive skills training, psychotherapeutic interventions and compensatory strategy interventions, including training with assistive technologies. “Medically Ready Force…Ready Medical Force” 99
 Rehabilitation: Cognitive Rehabilitation (cont. ) ∎ Clinician-directed interventions show benefit over the use of self-directed computer-based programs. 14 -15 q. Computer-based programs may be effective cognitive rehabilitation tools when used in a clinician-directed manner and in support of interventions focused on functional needs. ∎ Common co-occurring conditions such as problems with sleep, headaches and other pain, and substance use; mental health conditions such as anxiety, depression and PTSD; and psychological factors such as negative self-beliefs and limited coping resources impact cognition. 16 -20 q. Integrated treatment models shows promise toward cognitive symptom reduction and improved functioning. “Medically Ready Force…Ready Medical Force” 100
Rehabilitation: Cognitive Rehabilitation (cont. ) ∎ Clinician-directed interventions show benefit over the use of self-directed computer-based programs. 14 -15 q. Computer-based programs may be effective cognitive rehabilitation tools when used in a clinician-directed manner and in support of interventions focused on functional needs. ∎ Common co-occurring conditions such as problems with sleep, headaches and other pain, and substance use; mental health conditions such as anxiety, depression and PTSD; and psychological factors such as negative self-beliefs and limited coping resources impact cognition. 16 -20 q. Integrated treatment models shows promise toward cognitive symptom reduction and improved functioning. “Medically Ready Force…Ready Medical Force” 100
 Rehabilitation: Cognitive Rehabilitation (cont. ) ∎ Further research studies are needed to validate specific cognitive rehabilitation approaches and identify appropriate treatment options. q. Researchers should use a common definition of TBI and attempt to reduce sample heterogeneity. q. Common outcome measures are needed to make comparisons across studies and interventions. Including measures related to community reintegration, such as return to work/school and social roles may shed light on the longterm benefits of cognitive rehabilitation. “Medically Ready Force…Ready Medical Force” 101
Rehabilitation: Cognitive Rehabilitation (cont. ) ∎ Further research studies are needed to validate specific cognitive rehabilitation approaches and identify appropriate treatment options. q. Researchers should use a common definition of TBI and attempt to reduce sample heterogeneity. q. Common outcome measures are needed to make comparisons across studies and interventions. Including measures related to community reintegration, such as return to work/school and social roles may shed light on the longterm benefits of cognitive rehabilitation. “Medically Ready Force…Ready Medical Force” 101
 Rehabilitation: Auditory Rehabilitation ∎ In general, there is insufficient evidence to support specific rehabilitative strategies for auditory injury in TBI. q. The paucity of the current literature on this topic may be due in part to lack of protocols to identify sensory injuries and injury profiles in TBI patients, and to the need for additional studies to develop foundational knowledge with respect to sensory comorbidities in blast and blunt TBI. ∎ Progressive tinnitus management (PTM) is a promising intervention for those with tinnitus. 21 ∎ New research is needed on rehabilitation for TBI-related auditory injury. Also, interventions are needed for auditory injuries in the context of injuries to multiple sensory systems and functions. “Medically Ready Force…Ready Medical Force” 102
Rehabilitation: Auditory Rehabilitation ∎ In general, there is insufficient evidence to support specific rehabilitative strategies for auditory injury in TBI. q. The paucity of the current literature on this topic may be due in part to lack of protocols to identify sensory injuries and injury profiles in TBI patients, and to the need for additional studies to develop foundational knowledge with respect to sensory comorbidities in blast and blunt TBI. ∎ Progressive tinnitus management (PTM) is a promising intervention for those with tinnitus. 21 ∎ New research is needed on rehabilitation for TBI-related auditory injury. Also, interventions are needed for auditory injuries in the context of injuries to multiple sensory systems and functions. “Medically Ready Force…Ready Medical Force” 102
 Rehabilitation: Vestibular Rehabilitation ∎ Vestibular dysfunction after TBI can be peripheral, central or mixed cause. ∎ Evidence supports incorporating vestibular rehabilitation techniques in management of patients vestibular-related symptoms after TBI of any severity (i. e. , vertigo, dizziness and balance dysfunction). 22 q Variability in outcome measurement tools limits standardization of validated clinical treatment models q. Defining standard vestibular rehabilitation prescription is limited due to patient heterogeneity and small sample sizes. ∎ New research is needed to focus on treatment prescription for vestibular rehabilitation to maximize recovery and return to function. “Medically Ready Force…Ready Medical Force” 103
Rehabilitation: Vestibular Rehabilitation ∎ Vestibular dysfunction after TBI can be peripheral, central or mixed cause. ∎ Evidence supports incorporating vestibular rehabilitation techniques in management of patients vestibular-related symptoms after TBI of any severity (i. e. , vertigo, dizziness and balance dysfunction). 22 q Variability in outcome measurement tools limits standardization of validated clinical treatment models q. Defining standard vestibular rehabilitation prescription is limited due to patient heterogeneity and small sample sizes. ∎ New research is needed to focus on treatment prescription for vestibular rehabilitation to maximize recovery and return to function. “Medically Ready Force…Ready Medical Force” 103
 Rehabilitation: Visual Rehabilitation ∎ Mild TBI-associated visual dysfunctions are often subtle and difficult to detect, often persist despite treatment, and interfere with rehabilitation and reintegration. 23 q. TBI-associated visual dysfunctions are often co-morbid with hearing, vestibular and cognitive injuries. q. Prevalence data for TBI-related vision dysfunction support the need for a TBI-specific eye/vision examination by an eye care provider. “Medically Ready Force…Ready Medical Force” 104
Rehabilitation: Visual Rehabilitation ∎ Mild TBI-associated visual dysfunctions are often subtle and difficult to detect, often persist despite treatment, and interfere with rehabilitation and reintegration. 23 q. TBI-associated visual dysfunctions are often co-morbid with hearing, vestibular and cognitive injuries. q. Prevalence data for TBI-related vision dysfunction support the need for a TBI-specific eye/vision examination by an eye care provider. “Medically Ready Force…Ready Medical Force” 104
 Rehabilitation: Visual Rehabilitation (cont. ) ∎ Optical correction of refractive error, especially at near distances, improves reading performance in patients with TBIrelated visual dysfunctions. 24 ∎ Prism spectacles are effective in symptomatic relief of vertical eye misalignment (heterophoria). 25 ∎ Vision therapy is effective for convergence and accommodative dysfunctions. Visual scanning exercises also benefit these and other patients with other forms of binocular dysfunction. Compliance is a limiting factor in the success of these patients. 26 -31 “Medically Ready Force…Ready Medical Force” 105
Rehabilitation: Visual Rehabilitation (cont. ) ∎ Optical correction of refractive error, especially at near distances, improves reading performance in patients with TBIrelated visual dysfunctions. 24 ∎ Prism spectacles are effective in symptomatic relief of vertical eye misalignment (heterophoria). 25 ∎ Vision therapy is effective for convergence and accommodative dysfunctions. Visual scanning exercises also benefit these and other patients with other forms of binocular dysfunction. Compliance is a limiting factor in the success of these patients. 26 -31 “Medically Ready Force…Ready Medical Force” 105
 Rehabilitation Visual Rehabilitation (cont. ) ∎ Visual search training supports visual environment awareness and tasks such as reading; but improvements are task-specific and may not generalize. 32 ∎ Use of specialized field expanding prisms and training in the use of compensatory scanning techniques can provide adaptive improvement for patients with hemianopic field of vision loss. 33 -35 ∎ Chromatically tinted spectacles relieve symptoms of light and glare sensitivity. Lens hues are patient specific. 36 “Medically Ready Force…Ready Medical Force” 106
Rehabilitation Visual Rehabilitation (cont. ) ∎ Visual search training supports visual environment awareness and tasks such as reading; but improvements are task-specific and may not generalize. 32 ∎ Use of specialized field expanding prisms and training in the use of compensatory scanning techniques can provide adaptive improvement for patients with hemianopic field of vision loss. 33 -35 ∎ Chromatically tinted spectacles relieve symptoms of light and glare sensitivity. Lens hues are patient specific. 36 “Medically Ready Force…Ready Medical Force” 106
 Research Gaps: Rehabilitation ∎ Auditory, cognitive, vestibular and visual rehabilitation are all lacking large, well-designed studies due to patient heterogeneity, intervention heterogeneity and varied patient outcomes. Additional well-designed studies are needed: q More research is needed on rehabilitation of ocular motility, visual field loss, and light sensitivity associated with TBI. q Studies regarding prevalence and natural history of TBI vision problems. q Vestibular rehabilitation needs more information on how to individualize treatment to maximize function and Qo. L. q Studies to validate cognitive rehabilitation approaches and identify appropriate treatment options. q More research is needed regarding rehabilitation of TBI patients with multi-sensory problems. “Medically Ready Force…Ready Medical Force” 107
Research Gaps: Rehabilitation ∎ Auditory, cognitive, vestibular and visual rehabilitation are all lacking large, well-designed studies due to patient heterogeneity, intervention heterogeneity and varied patient outcomes. Additional well-designed studies are needed: q More research is needed on rehabilitation of ocular motility, visual field loss, and light sensitivity associated with TBI. q Studies regarding prevalence and natural history of TBI vision problems. q Vestibular rehabilitation needs more information on how to individualize treatment to maximize function and Qo. L. q Studies to validate cognitive rehabilitation approaches and identify appropriate treatment options. q More research is needed regarding rehabilitation of TBI patients with multi-sensory problems. “Medically Ready Force…Ready Medical Force” 107
 Conclusions and Next Steps Ø Auditory rehabilitation is lacking evidence, but progressive tinnitus management is a promising intervention for auditory injury in TBI. Ø Cognitive rehabilitation had the largest evidence base, however further research studies are needed to validate specific cognitive rehabilitation approaches and identify appropriate treatment options. Ø Vestibular rehabilitation has a large volume of evidence available, but further research is needed towards the development of treatment gold standards. Ø Visual rehabilitation has limited high-level evidence and would benefit from additional well designed studies. Clinical expert consensus recommendations are available from the “Medically Ready Force…Ready Medical Force” 108 Do. D Vision Center of Excellence (VCE).
Conclusions and Next Steps Ø Auditory rehabilitation is lacking evidence, but progressive tinnitus management is a promising intervention for auditory injury in TBI. Ø Cognitive rehabilitation had the largest evidence base, however further research studies are needed to validate specific cognitive rehabilitation approaches and identify appropriate treatment options. Ø Vestibular rehabilitation has a large volume of evidence available, but further research is needed towards the development of treatment gold standards. Ø Visual rehabilitation has limited high-level evidence and would benefit from additional well designed studies. Clinical expert consensus recommendations are available from the “Medically Ready Force…Ready Medical Force” 108 Do. D Vision Center of Excellence (VCE).
 MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Long Term Effects of TBI Louis French, Psy. D National Intrepid Center of Excellence U. S. Army photo “Medically Ready Force…Ready Medical Force” 109
MHS Consensus Statement on the Prevention, Diagnosis & Treatment of TBI Long Term Effects of TBI Louis French, Psy. D National Intrepid Center of Excellence U. S. Army photo “Medically Ready Force…Ready Medical Force” 109
 Work Group: Long Term Effects Name Title/Affiliation Louis French, Psy. D (Topic Lead) Deputy Director, Operations, National Intrepid Center of Excellence (NICo. E), Walter Reed National Military Medical Center (WRNMMC) Tracey Brickell, DPsych Senior Scientist/Scientific Director, 15 -Year Longitudinal TBI Study, Defense and Veterans Brain Injury Center (DVBIC), WRNMMC; Research Associate Professor, Uniformed Services University of the Health Sciences (USUHS) David Cifu, MD Associate Dean of Innovation and System Integration, Virginia Commonwealth University School of Medicine; Senior TBI Specialist, Principal Investigator, Chronic Effects of Neurotrauma Consortium, U. S. Department of Veterans Affairs Kristen Dams. O'Connor, Ph. D Associate Professor, Director, Brain Injury Research Center, Research Director, Mount Sinai Injury Control Research Center, Department of Rehabilitation, Department of Neurology, Icahn School of Medicine at Mount Sinai Grant Iverson, Ph. D Professor, Department of Physical Medicine & Rehabilitation (PM&R), Harvard Medical School; Director, Neuropsychology Outcome Assessment Laboratory, Center for Health and Rehabilitation Research, Spaulding Rehabilitation Network; Director, Mass. General Hospital for Children™ Sports Concussion Program Kimbra Kenney, MD Service Chief, Research Operations, NICo. E, WRNMMC; Associate Professor, Department of Neurology, USUHS Rael Lange, Ph. D Research Director & Senior Scientist, DVBIC, WRNMMC; Scientific Director, 15 -Year Longitudinal TBI Study, DVBIC, WRNMMC; Adjunct Professor, University of British Columbia. William Walker, MD Professor, Virginia Commonwealth University Department of PM&R “Medically Ready Force…Ready Medical Force” 110
Work Group: Long Term Effects Name Title/Affiliation Louis French, Psy. D (Topic Lead) Deputy Director, Operations, National Intrepid Center of Excellence (NICo. E), Walter Reed National Military Medical Center (WRNMMC) Tracey Brickell, DPsych Senior Scientist/Scientific Director, 15 -Year Longitudinal TBI Study, Defense and Veterans Brain Injury Center (DVBIC), WRNMMC; Research Associate Professor, Uniformed Services University of the Health Sciences (USUHS) David Cifu, MD Associate Dean of Innovation and System Integration, Virginia Commonwealth University School of Medicine; Senior TBI Specialist, Principal Investigator, Chronic Effects of Neurotrauma Consortium, U. S. Department of Veterans Affairs Kristen Dams. O'Connor, Ph. D Associate Professor, Director, Brain Injury Research Center, Research Director, Mount Sinai Injury Control Research Center, Department of Rehabilitation, Department of Neurology, Icahn School of Medicine at Mount Sinai Grant Iverson, Ph. D Professor, Department of Physical Medicine & Rehabilitation (PM&R), Harvard Medical School; Director, Neuropsychology Outcome Assessment Laboratory, Center for Health and Rehabilitation Research, Spaulding Rehabilitation Network; Director, Mass. General Hospital for Children™ Sports Concussion Program Kimbra Kenney, MD Service Chief, Research Operations, NICo. E, WRNMMC; Associate Professor, Department of Neurology, USUHS Rael Lange, Ph. D Research Director & Senior Scientist, DVBIC, WRNMMC; Scientific Director, 15 -Year Longitudinal TBI Study, DVBIC, WRNMMC; Adjunct Professor, University of British Columbia. William Walker, MD Professor, Virginia Commonwealth University Department of PM&R “Medically Ready Force…Ready Medical Force” 110
 Background: Long Term Effects ∎ For some individuals who sustain a TBI, health consequences of the TBI may persist long after the injury ∎ Long-term consequences depend on a number of factors: injury type, severity, number and timing of injuries, patient characteristics, acute care and rehabilitation interventions received, and environmental factors ∎ Understanding long-term effects of TBI will help to: q. Improve care provided to patients in the acute, subacute and long-term phases of recovery q. Prevent and manage chronic symptoms q. Support patients in achieving maximum recovery and quality of life “Medically Ready Force…Ready Medical Force” 111
Background: Long Term Effects ∎ For some individuals who sustain a TBI, health consequences of the TBI may persist long after the injury ∎ Long-term consequences depend on a number of factors: injury type, severity, number and timing of injuries, patient characteristics, acute care and rehabilitation interventions received, and environmental factors ∎ Understanding long-term effects of TBI will help to: q. Improve care provided to patients in the acute, subacute and long-term phases of recovery q. Prevent and manage chronic symptoms q. Support patients in achieving maximum recovery and quality of life “Medically Ready Force…Ready Medical Force” 111
 Long Term Effects Severe and penetrating TBI are risk factors for development of seizures and posttraumatic epilepsy. 1 -4 q Increased risk of seizures following severe and penetrating TBI q. Evidence was limited on the association between moderate TBI and the development of seizures and posttraumatic epilepsy “Medically Ready Force…Ready Medical Force” 112
Long Term Effects Severe and penetrating TBI are risk factors for development of seizures and posttraumatic epilepsy. 1 -4 q Increased risk of seizures following severe and penetrating TBI q. Evidence was limited on the association between moderate TBI and the development of seizures and posttraumatic epilepsy “Medically Ready Force…Ready Medical Force” 112
 Long Term Effects There is some evidence regarding the association between moderate-to-severe TBI and dementia. There is insufficient evidence to determine the subtype of dementia. 1, 5 q. There is some evidence in the civilian literature of a relationship between moderate-to-severe TBI and dementia; evidence in the military and veteran population is limited “Medically Ready Force…Ready Medical Force” 113
Long Term Effects There is some evidence regarding the association between moderate-to-severe TBI and dementia. There is insufficient evidence to determine the subtype of dementia. 1, 5 q. There is some evidence in the civilian literature of a relationship between moderate-to-severe TBI and dementia; evidence in the military and veteran population is limited “Medically Ready Force…Ready Medical Force” 113
 Long Term Effects Penetrating and severe TBI are associated with a variety of cognitive impairments including difficulties with attention, learning and memory. 6 -11 q. Severity of injury is positively associated with adverse long-term cognitive effects “Medically Ready Force…Ready Medical Force” 114
Long Term Effects Penetrating and severe TBI are associated with a variety of cognitive impairments including difficulties with attention, learning and memory. 6 -11 q. Severity of injury is positively associated with adverse long-term cognitive effects “Medically Ready Force…Ready Medical Force” 114
 Long Term Effects Penetrating and severe TBI are associated with increased mortality and premature death. 12, 13 q. There is limited literature on this topic in the military population “Medically Ready Force…Ready Medical Force” 115
Long Term Effects Penetrating and severe TBI are associated with increased mortality and premature death. 12, 13 q. There is limited literature on this topic in the military population “Medically Ready Force…Ready Medical Force” 115
 Area of Focus ∎ Association between TBI and non-Alzheimer's disease neurodegenerative disorders q. The evidence related to the relationship between the following neurodegenerative disorders and TBI needs to be further explored: Parkinson’s disease, amyotrophic lateral sclerosis (ALS), motor neuron disease (MND), frontotemporal dementia (FTD) and CTE “Medically Ready Force…Ready Medical Force” 116
Area of Focus ∎ Association between TBI and non-Alzheimer's disease neurodegenerative disorders q. The evidence related to the relationship between the following neurodegenerative disorders and TBI needs to be further explored: Parkinson’s disease, amyotrophic lateral sclerosis (ALS), motor neuron disease (MND), frontotemporal dementia (FTD) and CTE “Medically Ready Force…Ready Medical Force” 116
 Research Gaps: Long Term Effects ∎ Longitudinal studies in military populations, across the spectrum of TBI severity, are necessary to understand longterm outcomes (≥ 10 years following injury) of TBI and how aging and military exposure interacts with a history of TBI. ∎ A number of studies in the military are ongoing q. For example: § DVBIC 15 -Year Longitudinal TBI Study § Chronic Effects of Neurotrauma Consortium (CENC) § TBI Model Systems (VA Polytrauma Rehab Centers) § Improved Understanding of Medical and Psychological Needs in Veterans and Service Members with TBI (i. MAP) “Medically Ready Force…Ready Medical Force” 117
Research Gaps: Long Term Effects ∎ Longitudinal studies in military populations, across the spectrum of TBI severity, are necessary to understand longterm outcomes (≥ 10 years following injury) of TBI and how aging and military exposure interacts with a history of TBI. ∎ A number of studies in the military are ongoing q. For example: § DVBIC 15 -Year Longitudinal TBI Study § Chronic Effects of Neurotrauma Consortium (CENC) § TBI Model Systems (VA Polytrauma Rehab Centers) § Improved Understanding of Medical and Psychological Needs in Veterans and Service Members with TBI (i. MAP) “Medically Ready Force…Ready Medical Force” 117
 Conclusions and Next Steps Conclusions: Ø Severe and penetrating TBI are risk factors for development of seizures and posttraumatic epilepsy. Ø There is some evidence regarding the association between moderate-tosevere TBI and dementia. There is insufficient evidence to determine the subtype of dementia. Ø Penetrating and severe TBI are associated with a variety of cognitive impairments including difficulties with attention, learning and memory. Ø Penetrating and severe TBI are associated with increased mortality and premature death. Next steps: Ø Examine the association between TBI and non-Alzheimer's disease neurodegenerative disorders Ø Statement development is ongoing and may change based on review of additional evidence. “Medically Ready Force…Ready Medical Force” 118
Conclusions and Next Steps Conclusions: Ø Severe and penetrating TBI are risk factors for development of seizures and posttraumatic epilepsy. Ø There is some evidence regarding the association between moderate-tosevere TBI and dementia. There is insufficient evidence to determine the subtype of dementia. Ø Penetrating and severe TBI are associated with a variety of cognitive impairments including difficulties with attention, learning and memory. Ø Penetrating and severe TBI are associated with increased mortality and premature death. Next steps: Ø Examine the association between TBI and non-Alzheimer's disease neurodegenerative disorders Ø Statement development is ongoing and may change based on review of additional evidence. “Medically Ready Force…Ready Medical Force” 118
 SUMMARY and CONCLUSIONS Saafan Malik, MD Defense and Veterans Brain Injury Center “Medically Ready Force…Ready Medical Force” 119
SUMMARY and CONCLUSIONS Saafan Malik, MD Defense and Veterans Brain Injury Center “Medically Ready Force…Ready Medical Force” 119
 SUMMARY and CONCLUSIONS v. State of the Science TBI Statements and Outcomes of MHS TBIResearch Investments § Expand the evidence for the current draft executive statements to include recent (last 3 years) published research studies. § Executive statements will be finalized by leveraging the current working groups and will be published in a peer reviewed military relevant journal for wide distribution on the state of the science. These statements will yield actionable knowledge translation opportunities “Medically Ready Force…Ready Medical Force” 120
SUMMARY and CONCLUSIONS v. State of the Science TBI Statements and Outcomes of MHS TBIResearch Investments § Expand the evidence for the current draft executive statements to include recent (last 3 years) published research studies. § Executive statements will be finalized by leveraging the current working groups and will be published in a peer reviewed military relevant journal for wide distribution on the state of the science. These statements will yield actionable knowledge translation opportunities “Medically Ready Force…Ready Medical Force” 120
 Panel Q&A “Medically Ready Force…Ready Medical Force” 121
Panel Q&A “Medically Ready Force…Ready Medical Force” 121
![References [NOTE: All references are listed by subtopic areas] “Medically Ready Force…Ready Medical Force” References [NOTE: All references are listed by subtopic areas] “Medically Ready Force…Ready Medical Force”](https://present5.com/presentation/b6979da3a93e3b5a0385091271bcd613/image-122.jpg) References [NOTE: All references are listed by subtopic areas] “Medically Ready Force…Ready Medical Force” 122
References [NOTE: All references are listed by subtopic areas] “Medically Ready Force…Ready Medical Force” 122
 References: Prevention of TBI 1. 2. 3. 4. 5. 6. 7. 8. Defense and Veterans Brain Injury Center. Do. D worldwide numbers for TBI. 2017; http: //dvbic. dcoe. mil/dod-worldwide-numbers-tbi. Accessed August 17, 2017. Breeze J, Baxter D, Carr D, Midwinter MJ. Defining combat helmet coverage for protection against explosively propelled fragments. J R Army Med Corps. Mar 2015; 161(1): 9 -13. Carr DJ, Lewis E, Horsfall I. A systematic review of military head injuries. J R Army Med Corps. Feb 2017; 163(1): 13 -19. Canham-Chervak M, Cowan DN, Pollack KM, Jackson RR, Jones BH. Identification of fall prevention strategies for the military: A review of the literature. Mil Med. Dec 2015; 180(12): 1225 -1232. RAND Corporation. Understanding and reducing off-duty vehicle crashes among military personnel. Santa Monica, CA: RAND Corporation; 2010. http: //www. rand. org/content/dam/rand/pubs/technical_reports/2010/RAND_TR 820. pdf. Hutchison MG, Lawrence DW, Cusimano MD, Schweizer TA. Head trauma in mixed martial arts. Am J Sports Med. Jun 2014; 42(6): 1352 -1358. Mrazik M, Dennison CR, Brooks BL, Yeates KO, Babul S, Naidu D. A qualitative review of sports concussion education: Prime time for evidence-based knowledge translation. Br J Sports Med. Dec 2015; 49(24): 1548 -1553. Caron JG, Bloom GA, Falcao WR, Sweet SN. An examination of concussion education programmes: A scoping review methodology. Inj Prev. Oct 2015; 21(5): 301 -308. “Medically Ready Force…Ready Medical Force” 123
References: Prevention of TBI 1. 2. 3. 4. 5. 6. 7. 8. Defense and Veterans Brain Injury Center. Do. D worldwide numbers for TBI. 2017; http: //dvbic. dcoe. mil/dod-worldwide-numbers-tbi. Accessed August 17, 2017. Breeze J, Baxter D, Carr D, Midwinter MJ. Defining combat helmet coverage for protection against explosively propelled fragments. J R Army Med Corps. Mar 2015; 161(1): 9 -13. Carr DJ, Lewis E, Horsfall I. A systematic review of military head injuries. J R Army Med Corps. Feb 2017; 163(1): 13 -19. Canham-Chervak M, Cowan DN, Pollack KM, Jackson RR, Jones BH. Identification of fall prevention strategies for the military: A review of the literature. Mil Med. Dec 2015; 180(12): 1225 -1232. RAND Corporation. Understanding and reducing off-duty vehicle crashes among military personnel. Santa Monica, CA: RAND Corporation; 2010. http: //www. rand. org/content/dam/rand/pubs/technical_reports/2010/RAND_TR 820. pdf. Hutchison MG, Lawrence DW, Cusimano MD, Schweizer TA. Head trauma in mixed martial arts. Am J Sports Med. Jun 2014; 42(6): 1352 -1358. Mrazik M, Dennison CR, Brooks BL, Yeates KO, Babul S, Naidu D. A qualitative review of sports concussion education: Prime time for evidence-based knowledge translation. Br J Sports Med. Dec 2015; 49(24): 1548 -1553. Caron JG, Bloom GA, Falcao WR, Sweet SN. An examination of concussion education programmes: A scoping review methodology. Inj Prev. Oct 2015; 21(5): 301 -308. “Medically Ready Force…Ready Medical Force” 123
 References: Acute Concussion 1. 2. 3. 4. 5. 6. 7. 8. 9. Pandor A, Harnan S, Goodacre S, Pickering A, Fitzgerald P, Rees A. Diagnostic accuracy of clinical characteristics for identifying CT abnormality after minor brain injury: A systematic review and metaanalysis. J Neurotrauma. Mar 2012; 29(5): 707 -718. Patricios J, Fuller GW, Ellenbogen R, et al. What are the critical elements of sideline screening that can be used to establish the diagnosis of concussion? A systematic review. Br J Sports Med. Mar 2017. Hunt AW, Mah K, Reed N, Engel L, Keightley M. Oculomotor-based vision assessment in mild traumatic brain injury: A systematic review. J Head Trauma Rehabil. Jul-Aug 2016; 31(4): 252 -261. Eliyahu L, Kirkland S, Campbell S, Rowe BH. The effectiveness of early educational interventions in the emergency department to reduce incidence or severity of postconcussion syndrome following a concussion: A systematic review. Acad Emerg Med. May 2016; 23(5): 531 -542. Gravel J, D'Angelo A, Carriere B, et al. Interventions provided in the acute phase for mild traumatic brain injury: A systematic review. Syst Rev. Aug 2013; 2: 63. Mc. Leod TC, Lewis JH, Whelihan K, Bacon CE. Rest and return to activity after sport-related concussion: A systematic review of the literature. J Athl Train. Mar 2017; 52(3): 262 -287. Jorge RE, Acion L, Burin DI, Robinson RG. Sertraline for preventing mood disorders following traumatic brain injury: A randomized clinical trial. JAMA Psychiatry. Oct 2016; 73(10): 1041 -1047. Silverberg ND, Gardner AJ, Brubacher JR, Panenka WJ, Li JJ, Iverson GL. Systematic review of multivariable prognostic models for mild traumatic brain injury. J Neurotrauma. Apr 2015; 32(8): 517 -526. Cancelliere C, Kristman VL, Cassidy JD, et al. Systematic review of return to work after mild traumatic brain injury: Results of the international collaboration on mild traumatic brain injury prognosis. Arch Phys Med Rehabil. Mar 2014; 95(3 Suppl): S 201 -209. “Medically Ready Force…Ready Medical Force” 124
References: Acute Concussion 1. 2. 3. 4. 5. 6. 7. 8. 9. Pandor A, Harnan S, Goodacre S, Pickering A, Fitzgerald P, Rees A. Diagnostic accuracy of clinical characteristics for identifying CT abnormality after minor brain injury: A systematic review and metaanalysis. J Neurotrauma. Mar 2012; 29(5): 707 -718. Patricios J, Fuller GW, Ellenbogen R, et al. What are the critical elements of sideline screening that can be used to establish the diagnosis of concussion? A systematic review. Br J Sports Med. Mar 2017. Hunt AW, Mah K, Reed N, Engel L, Keightley M. Oculomotor-based vision assessment in mild traumatic brain injury: A systematic review. J Head Trauma Rehabil. Jul-Aug 2016; 31(4): 252 -261. Eliyahu L, Kirkland S, Campbell S, Rowe BH. The effectiveness of early educational interventions in the emergency department to reduce incidence or severity of postconcussion syndrome following a concussion: A systematic review. Acad Emerg Med. May 2016; 23(5): 531 -542. Gravel J, D'Angelo A, Carriere B, et al. Interventions provided in the acute phase for mild traumatic brain injury: A systematic review. Syst Rev. Aug 2013; 2: 63. Mc. Leod TC, Lewis JH, Whelihan K, Bacon CE. Rest and return to activity after sport-related concussion: A systematic review of the literature. J Athl Train. Mar 2017; 52(3): 262 -287. Jorge RE, Acion L, Burin DI, Robinson RG. Sertraline for preventing mood disorders following traumatic brain injury: A randomized clinical trial. JAMA Psychiatry. Oct 2016; 73(10): 1041 -1047. Silverberg ND, Gardner AJ, Brubacher JR, Panenka WJ, Li JJ, Iverson GL. Systematic review of multivariable prognostic models for mild traumatic brain injury. J Neurotrauma. Apr 2015; 32(8): 517 -526. Cancelliere C, Kristman VL, Cassidy JD, et al. Systematic review of return to work after mild traumatic brain injury: Results of the international collaboration on mild traumatic brain injury prognosis. Arch Phys Med Rehabil. Mar 2014; 95(3 Suppl): S 201 -209. “Medically Ready Force…Ready Medical Force” 124
 References: Peri-Injury Management 1. 2. 3. 4. 5. 6. 7. Bossers SM, Schwarte LA, Loer SA, Twisk JW, Boer C, Schober P. Experience in prehospital endotracheal intubation significantly influences mortality of patients with severe traumatic brain injury: A systematic review and meta-analysis. PLo. S One. 2015; 10(10): e 0141034. von Elm E, Schoettker P, Henzi I, Osterwalder J, Walder B. Pre-hospital tracheal intubation in patients with traumatic brain injury: Systematic review of current evidence. Br J Anaesth. Sep 2009; 103(3): 371 -386. Dumont TM, Visioni AJ, Rughani AI, Tranmer BI, Crookes B. Inappropriate prehospital ventilation in severe traumatic brain injury increases in-hospital mortality. J Neurotrauma. Jul 2010; 27(7): 1233 -1241. Spaite DW, Hu C, Bobrow BJ, et al. Mortality and prehospital blood pressure in patients with major traumatic brain injury: Implications for the hypotension threshold. JAMA Surg. Apr 01 2017; 152(4): 360 -368. Elterman J, Brasel K, Brown S, et al. Transfusion of red blood cells in patients with a prehospital glasgow coma scale score of 8 or less and no evidence of shock is associated with worse outcomes. J Trauma Acute Care Surg. Jul 2013; 75(1): 8 -14; discussion 14. Yamal JM, Benoit JS, Doshi P, et al. Association of transfusion red blood cell storage and blood oxygenation, long-term neurologic outcome, and mortality in traumatic brain injury. J Trauma Acute Care Surg. Nov 2015; 79(5): 843 -849. Tan PG, Cincotta M, Clavisi O, et al. Review article: Prehospital fluid management in traumatic brain injury. Emerg Med Australas. Dec 2011; 23(6): 665 -676. “Medically Ready Force…Ready Medical Force” 125
References: Peri-Injury Management 1. 2. 3. 4. 5. 6. 7. Bossers SM, Schwarte LA, Loer SA, Twisk JW, Boer C, Schober P. Experience in prehospital endotracheal intubation significantly influences mortality of patients with severe traumatic brain injury: A systematic review and meta-analysis. PLo. S One. 2015; 10(10): e 0141034. von Elm E, Schoettker P, Henzi I, Osterwalder J, Walder B. Pre-hospital tracheal intubation in patients with traumatic brain injury: Systematic review of current evidence. Br J Anaesth. Sep 2009; 103(3): 371 -386. Dumont TM, Visioni AJ, Rughani AI, Tranmer BI, Crookes B. Inappropriate prehospital ventilation in severe traumatic brain injury increases in-hospital mortality. J Neurotrauma. Jul 2010; 27(7): 1233 -1241. Spaite DW, Hu C, Bobrow BJ, et al. Mortality and prehospital blood pressure in patients with major traumatic brain injury: Implications for the hypotension threshold. JAMA Surg. Apr 01 2017; 152(4): 360 -368. Elterman J, Brasel K, Brown S, et al. Transfusion of red blood cells in patients with a prehospital glasgow coma scale score of 8 or less and no evidence of shock is associated with worse outcomes. J Trauma Acute Care Surg. Jul 2013; 75(1): 8 -14; discussion 14. Yamal JM, Benoit JS, Doshi P, et al. Association of transfusion red blood cell storage and blood oxygenation, long-term neurologic outcome, and mortality in traumatic brain injury. J Trauma Acute Care Surg. Nov 2015; 79(5): 843 -849. Tan PG, Cincotta M, Clavisi O, et al. Review article: Prehospital fluid management in traumatic brain injury. Emerg Med Australas. Dec 2011; 23(6): 665 -676. “Medically Ready Force…Ready Medical Force” 125
 References: Peri-Injury Management 8. 9. 10. 11. 12. 13. Burgess S, Abu-Laban RB, Slavik RS, Vu EN, Zed PJ. A systematic review of randomized controlled trials comparing hypertonic sodium solutions and mannitol for traumatic brain injury: Implications for emergency department management. Ann Pharmacother. Apr 2016; 50(4): 291 -300. Fox JL, Vu EN, Doyle-Waters M, Brubacher JR, Abu-Laban R, Hu Z. Prophylactic hypothermia for traumatic brain injury: A quantitative systematic review. Cjem. Jul 2010; 12(4): 355 -364. Andrews PJD, Rodriguez A, Suter P, et al. Mortality risk stratification after traumatic brain injury and hazard of death with titrated hypothermia in the eurotherm 3235 trial. Crit Care Med. May 2017; 45(5): 883 -890. Roberts DJ, Hall RI, Kramer AH, Robertson HL, Gallagher CN, Zygun DA. Sedation for critically ill adults with severe traumatic brain injury: A systematic review of randomized controlled trials. Crit Care Med. Dec 2011; 39(12): 2743 -2751. Bulger EM, Guffey D, Guyette FX, et al. Impact of prehospital mode of transport after severe injury: A multicenter evaluation from the resuscitation outcomes consortium. J Trauma Acute Care Surg. Mar 2012; 72(3): 567 -573; discussion 573 -565; quiz 803. Garner AA, Mann KP, Fearnside M, Poynter E, Gebski V. The head injury retrieval trial (HIRT): A single-centre randomised controlled trial of physician prehospital management of severe blunt head injury compared with management by paramedics only. Emerg Med J. Nov 2015; 32(11): 869 -875. “Medically Ready Force…Ready Medical Force” 126
References: Peri-Injury Management 8. 9. 10. 11. 12. 13. Burgess S, Abu-Laban RB, Slavik RS, Vu EN, Zed PJ. A systematic review of randomized controlled trials comparing hypertonic sodium solutions and mannitol for traumatic brain injury: Implications for emergency department management. Ann Pharmacother. Apr 2016; 50(4): 291 -300. Fox JL, Vu EN, Doyle-Waters M, Brubacher JR, Abu-Laban R, Hu Z. Prophylactic hypothermia for traumatic brain injury: A quantitative systematic review. Cjem. Jul 2010; 12(4): 355 -364. Andrews PJD, Rodriguez A, Suter P, et al. Mortality risk stratification after traumatic brain injury and hazard of death with titrated hypothermia in the eurotherm 3235 trial. Crit Care Med. May 2017; 45(5): 883 -890. Roberts DJ, Hall RI, Kramer AH, Robertson HL, Gallagher CN, Zygun DA. Sedation for critically ill adults with severe traumatic brain injury: A systematic review of randomized controlled trials. Crit Care Med. Dec 2011; 39(12): 2743 -2751. Bulger EM, Guffey D, Guyette FX, et al. Impact of prehospital mode of transport after severe injury: A multicenter evaluation from the resuscitation outcomes consortium. J Trauma Acute Care Surg. Mar 2012; 72(3): 567 -573; discussion 573 -565; quiz 803. Garner AA, Mann KP, Fearnside M, Poynter E, Gebski V. The head injury retrieval trial (HIRT): A single-centre randomised controlled trial of physician prehospital management of severe blunt head injury compared with management by paramedics only. Emerg Med J. Nov 2015; 32(11): 869 -875. “Medically Ready Force…Ready Medical Force” 126
 References: Peri-Injury Management 14. Pakkanen T, Virkkunen I, Kamarainen A, et al. Pre-hospital severe traumatic brain injury - comparison of outcome in paramedic versus physician staffed emergency medical services. Scand J Trauma Resusc Emerg Med. Apr 29 2016; 24: 62. 15. Wilson S, Gangathimmaiah V. Does prehospital management by doctors affect outcome in major trauma? A systematic review. J Trauma Acute Care Surg. Jun 06 2017. 16. Shen L, Wang Z, Su Z, et al. Effects of intracranial pressure monitoring on mortality in patients with severe traumatic brain injury: A meta-analysis. PLo. S One. 2016; 11(12): e 0168901. 17. Narayan RK, Becker DP. Selection of patients for icp monitoring. J Neurosurg. Apr 1985; 62(4): 624 -625. 18. Green JA, Pellegrini DC, Vanderkolk WE, Figueroa BE, Eriksson EA. Goal directed brain tissue oxygen monitoring versus conventional management in traumatic brain injury: An analysis of in hospital recovery. Neurocrit Care. Feb 2013; 18(1): 20 -25. 19. Tazarourte K, Atchabahian A, Tourtier JP, et al. Pre-hospital transcranial doppler in severe traumatic brain injury: A pilot study. Acta Anaesthesiol Scand. Apr 2011; 55(4): 422 -428. 20. Peters J, Van Wageningen B, Hoogerwerf N, Tan E. Near-infrared spectroscopy: A promising prehospital tool for management of traumatic brain injury. Prehosp Disaster Med. Aug 2017; 32(4): 414 -418. “Medically Ready Force…Ready Medical Force” 127
References: Peri-Injury Management 14. Pakkanen T, Virkkunen I, Kamarainen A, et al. Pre-hospital severe traumatic brain injury - comparison of outcome in paramedic versus physician staffed emergency medical services. Scand J Trauma Resusc Emerg Med. Apr 29 2016; 24: 62. 15. Wilson S, Gangathimmaiah V. Does prehospital management by doctors affect outcome in major trauma? A systematic review. J Trauma Acute Care Surg. Jun 06 2017. 16. Shen L, Wang Z, Su Z, et al. Effects of intracranial pressure monitoring on mortality in patients with severe traumatic brain injury: A meta-analysis. PLo. S One. 2016; 11(12): e 0168901. 17. Narayan RK, Becker DP. Selection of patients for icp monitoring. J Neurosurg. Apr 1985; 62(4): 624 -625. 18. Green JA, Pellegrini DC, Vanderkolk WE, Figueroa BE, Eriksson EA. Goal directed brain tissue oxygen monitoring versus conventional management in traumatic brain injury: An analysis of in hospital recovery. Neurocrit Care. Feb 2013; 18(1): 20 -25. 19. Tazarourte K, Atchabahian A, Tourtier JP, et al. Pre-hospital transcranial doppler in severe traumatic brain injury: A pilot study. Acta Anaesthesiol Scand. Apr 2011; 55(4): 422 -428. 20. Peters J, Van Wageningen B, Hoogerwerf N, Tan E. Near-infrared spectroscopy: A promising prehospital tool for management of traumatic brain injury. Prehosp Disaster Med. Aug 2017; 32(4): 414 -418. “Medically Ready Force…Ready Medical Force” 127
 References: Biomarkers 1. 2. 3. 4. 5. 6. 7. 8. Mc. Crea M, Meier T, Huber D, et al. Role of advanced neuroimaging, fluid biomarkers and genetic testing in the assessment of sport-related concussion: A systematic review. Br J Sports Med. Jun 2017; 51(12): 919929. PMID: 28455364. Studerus-Germann AM, Thiran JP, Daducci A, Gautschi OP. Diagnostic approaches to predict persistent post-traumatic symptoms after mild traumatic brain injury - a literature review. Int J Neurosci. 2016; 126(4): 289 -298. PMID: 26000929. Eierud C, Craddock RC, Fletcher S, et al. Neuroimaging after mild traumatic brain injury: Review and metaanalysis. Neuroimage Clin. 2014; 4: 283 -294. PMID: 25061565. Mu W, Catenaccio E, Lipton ML. Neuroimaging in blast-related mild traumatic brain injury. J Head Trauma Rehabil. Jan/Feb 2017; 32(1): 55 -69. PMID: 27022955. Amyot F, Arciniegas DB, Brazaitis MP, et al. A review of the effectiveness of neuroimaging modalities for the detection of traumatic brain injury. J Neurotrauma. Nov 15 2015; 32(22): 1693 -1721. PMID: 26176603. Asken BM, De. Kosky ST, Clugston JR, Jaffee MS, Bauer RM. Diffusion tensor imaging (DTI) findings in adult civilian, military, and sport-related mild traumatic brain injury (m. TBI): A systematic critical review. Brain Imaging Behav. Mar 24 2017. PMID: 28337734. Douglas DB, Iv M, Douglas PK, et al. Diffusion tensor imaging of TBI: Potentials and challenges. Top Magn Reson Imaging. Oct 2015; 24(5): 241 -251. PMID: 26502306. Wilde EA, Bouix S, Tate DF, et al. Advanced neuroimaging applied to veterans and service personnel with traumatic brain injury: State of the art and potential benefits. Brain Imaging Behav. Sep 2015; 9(3): 367 -402. PMID: 26350144. “Medically Ready Force…Ready Medical Force” 128
References: Biomarkers 1. 2. 3. 4. 5. 6. 7. 8. Mc. Crea M, Meier T, Huber D, et al. Role of advanced neuroimaging, fluid biomarkers and genetic testing in the assessment of sport-related concussion: A systematic review. Br J Sports Med. Jun 2017; 51(12): 919929. PMID: 28455364. Studerus-Germann AM, Thiran JP, Daducci A, Gautschi OP. Diagnostic approaches to predict persistent post-traumatic symptoms after mild traumatic brain injury - a literature review. Int J Neurosci. 2016; 126(4): 289 -298. PMID: 26000929. Eierud C, Craddock RC, Fletcher S, et al. Neuroimaging after mild traumatic brain injury: Review and metaanalysis. Neuroimage Clin. 2014; 4: 283 -294. PMID: 25061565. Mu W, Catenaccio E, Lipton ML. Neuroimaging in blast-related mild traumatic brain injury. J Head Trauma Rehabil. Jan/Feb 2017; 32(1): 55 -69. PMID: 27022955. Amyot F, Arciniegas DB, Brazaitis MP, et al. A review of the effectiveness of neuroimaging modalities for the detection of traumatic brain injury. J Neurotrauma. Nov 15 2015; 32(22): 1693 -1721. PMID: 26176603. Asken BM, De. Kosky ST, Clugston JR, Jaffee MS, Bauer RM. Diffusion tensor imaging (DTI) findings in adult civilian, military, and sport-related mild traumatic brain injury (m. TBI): A systematic critical review. Brain Imaging Behav. Mar 24 2017. PMID: 28337734. Douglas DB, Iv M, Douglas PK, et al. Diffusion tensor imaging of TBI: Potentials and challenges. Top Magn Reson Imaging. Oct 2015; 24(5): 241 -251. PMID: 26502306. Wilde EA, Bouix S, Tate DF, et al. Advanced neuroimaging applied to veterans and service personnel with traumatic brain injury: State of the art and potential benefits. Brain Imaging Behav. Sep 2015; 9(3): 367 -402. PMID: 26350144. “Medically Ready Force…Ready Medical Force” 128
 References: Biomarkers 9. 10. 11. 12. 13. 14. 15. 16. Hannawi Y, Lindquist MA, Caffo BS, Sair HI, Stevens RD. Resting brain activity in disorders of consciousness: A systematic review and meta-analysis. Neurology. Mar 24 2015; 84(12): 1272 -1280. PMID: 25713001. Kutcher JS, Mc. Crory P, Davis G, Ptito A, Meeuwisse WH, Broglio SP. What evidence exists for new strategies or technologies in the diagnosis of sports concussion and assessment of recovery? Br J Sports Med. Apr 2013; 47(5): 299 -303. PMID: 23479488. Raji CA, Tarzwell R, Pavel D, et al. Clinical utility of SPECT neuroimaging in the diagnosis and treatment of traumatic brain injury: A systematic review. PLo. S One. 2014; 9(3): e 91088. PMID: 24646878. Gardner AJ, Tan CO, Ainslie PN, et al. Cerebrovascular reactivity assessed by transcranial Doppler ultrasound in sport-related concussion: A systematic review. Br J Sports Med. Aug 2015; 49(16): 1050 -1055. PMID: 25452613. Armonda RA, Bell RS, Vo AH, et al. Wartime traumatic cerebral vasospasm: Recent review of combat casualties. Neurosurgery. Dec 2006; 59(6): 1215 -1225; discussion 1225. PMID: 17277684. Bouzat P, Almeras L, Manhes P, et al. Transcranial Doppler to predict neurologic outcome after mild to moderate traumatic brain injury. Anesthesiology. Aug 2016; 125(2): 346 -354. PMID: 27224640. Bailey DM, Jones DW, Sinnott A, et al. Impaired cerebral haemodynamic function associated with chronic traumatic brain injury in professional boxers. Clin Sci (Lond). Feb 2013; 124(3): 177 -189. PMID: 22913765. Kurowski BG, Treble-Barna A, Pitzer AJ, et al. Applying systems biology methodology to identify genetic factors possibly associated with recovery after traumatic brain injury. J Neurotrauma. May 03 2017. PMID: 28301983. “Medically Ready Force…Ready Medical Force” 129
References: Biomarkers 9. 10. 11. 12. 13. 14. 15. 16. Hannawi Y, Lindquist MA, Caffo BS, Sair HI, Stevens RD. Resting brain activity in disorders of consciousness: A systematic review and meta-analysis. Neurology. Mar 24 2015; 84(12): 1272 -1280. PMID: 25713001. Kutcher JS, Mc. Crory P, Davis G, Ptito A, Meeuwisse WH, Broglio SP. What evidence exists for new strategies or technologies in the diagnosis of sports concussion and assessment of recovery? Br J Sports Med. Apr 2013; 47(5): 299 -303. PMID: 23479488. Raji CA, Tarzwell R, Pavel D, et al. Clinical utility of SPECT neuroimaging in the diagnosis and treatment of traumatic brain injury: A systematic review. PLo. S One. 2014; 9(3): e 91088. PMID: 24646878. Gardner AJ, Tan CO, Ainslie PN, et al. Cerebrovascular reactivity assessed by transcranial Doppler ultrasound in sport-related concussion: A systematic review. Br J Sports Med. Aug 2015; 49(16): 1050 -1055. PMID: 25452613. Armonda RA, Bell RS, Vo AH, et al. Wartime traumatic cerebral vasospasm: Recent review of combat casualties. Neurosurgery. Dec 2006; 59(6): 1215 -1225; discussion 1225. PMID: 17277684. Bouzat P, Almeras L, Manhes P, et al. Transcranial Doppler to predict neurologic outcome after mild to moderate traumatic brain injury. Anesthesiology. Aug 2016; 125(2): 346 -354. PMID: 27224640. Bailey DM, Jones DW, Sinnott A, et al. Impaired cerebral haemodynamic function associated with chronic traumatic brain injury in professional boxers. Clin Sci (Lond). Feb 2013; 124(3): 177 -189. PMID: 22913765. Kurowski BG, Treble-Barna A, Pitzer AJ, et al. Applying systems biology methodology to identify genetic factors possibly associated with recovery after traumatic brain injury. J Neurotrauma. May 03 2017. PMID: 28301983. “Medically Ready Force…Ready Medical Force” 129
 References: Biomarkers 17. Lawrence DW, Comper P, Hutchison MG, Sharma B. The role of apolipoprotein E episilon (epsilon)-4 allele on outcome following traumatic brain injury: A systematic review. Brain Inj. 2015; 29(9): 1018 -1031. PMID: 25915580. 18. Yue JK, Pronger AM, Ferguson AR, et al. Association of a common genetic variant within ankk 1 with sixmonth cognitive performance after traumatic brain injury. Neurogenetics. Jul 2015; 16(3): 169 -180. PMID: 25633559. 19. Narayanan V, Veeramuthu V, Ahmad-Annuar A, et al. Missense mutation of brain derived neurotrophic factor (bdnf) alters neurocognitive performance in patients with mild traumatic brain injury: A longitudinal study. PLo. S One. 2016; 11(7): e 0158838. PMID: 27438599. 20. Hayes JP, Reagan A, Logue MW, et al. Bdnf genotype is associated with hippocampal volume in mild traumatic brain injury. Genes Brain Behav. Jul 28 2017. PMID: 28755387. 21. Shee K, Lucas A, Flashman LA, et al. Alpha-synuclein (snca) polymorphisms exert protective effects on memory after mild traumatic brain injury. Neurosci Lett. Sep 06 2016; 630: 241 -246. PMID: 27478013. 22. Mc. Allister TW, Tyler AL, Flashman LA, et al. Polymorphisms in the brain-derived neurotrophic factor gene influence memory and processing speed one month after brain injury. J Neurotrauma. Apr 10 2012; 29(6): 1111 -1118. PMID: 22188054. 23. Kurowski BG, Backeljauw B, Zang H, et al. Influence of catechol-o-methyltransferase on executive functioning longitudinally after early childhood traumatic brain injury: Preliminary findings. J Head Trauma Rehabil. May-Jun 2016; 31(3): E 1 -9. PMID: 26394291. 24. Merchant-Borna K, Lee H, Wang D, et al. Genome-wide changes in peripheral gene expression following sports-related concussion. J Neurotrauma. Sep 01 2016; 33(17): 1576 -1585. PMID: 27035221. “Medically Ready Force…Ready Medical Force” 130
References: Biomarkers 17. Lawrence DW, Comper P, Hutchison MG, Sharma B. The role of apolipoprotein E episilon (epsilon)-4 allele on outcome following traumatic brain injury: A systematic review. Brain Inj. 2015; 29(9): 1018 -1031. PMID: 25915580. 18. Yue JK, Pronger AM, Ferguson AR, et al. Association of a common genetic variant within ankk 1 with sixmonth cognitive performance after traumatic brain injury. Neurogenetics. Jul 2015; 16(3): 169 -180. PMID: 25633559. 19. Narayanan V, Veeramuthu V, Ahmad-Annuar A, et al. Missense mutation of brain derived neurotrophic factor (bdnf) alters neurocognitive performance in patients with mild traumatic brain injury: A longitudinal study. PLo. S One. 2016; 11(7): e 0158838. PMID: 27438599. 20. Hayes JP, Reagan A, Logue MW, et al. Bdnf genotype is associated with hippocampal volume in mild traumatic brain injury. Genes Brain Behav. Jul 28 2017. PMID: 28755387. 21. Shee K, Lucas A, Flashman LA, et al. Alpha-synuclein (snca) polymorphisms exert protective effects on memory after mild traumatic brain injury. Neurosci Lett. Sep 06 2016; 630: 241 -246. PMID: 27478013. 22. Mc. Allister TW, Tyler AL, Flashman LA, et al. Polymorphisms in the brain-derived neurotrophic factor gene influence memory and processing speed one month after brain injury. J Neurotrauma. Apr 10 2012; 29(6): 1111 -1118. PMID: 22188054. 23. Kurowski BG, Backeljauw B, Zang H, et al. Influence of catechol-o-methyltransferase on executive functioning longitudinally after early childhood traumatic brain injury: Preliminary findings. J Head Trauma Rehabil. May-Jun 2016; 31(3): E 1 -9. PMID: 26394291. 24. Merchant-Borna K, Lee H, Wang D, et al. Genome-wide changes in peripheral gene expression following sports-related concussion. J Neurotrauma. Sep 01 2016; 33(17): 1576 -1585. PMID: 27035221. “Medically Ready Force…Ready Medical Force” 130
 References: Biomarkers 25. Livingston WS, Gill JM, Cota MR, et al. Differential gene expression associated with meningeal injury in acute mild traumatic brain injury. J Neurotrauma. Feb 15 2017; 34(4): 853 -860. PMID: 27430610. 26. Heinzelmann M, Reddy SY, French LM, et al. Military personnel with chronic symptoms following blast traumatic brain injury have differential expression of neuronal recovery and epidermal growth factor receptor genes. Front Neurol. 2014; 5: 198. PMID: 25346719. 27. Sadeh N, Spielberg JM, Logue MW, et al. Ska 2 methylation is associated with decreased prefrontal cortical thickness and greater PTSD severity among trauma-exposed veterans. Mol Psychiatry. Mar 2016; 21(3): 357 -363. PMID: 26324104. 28. Dash PK, Hergenroeder GW, Jeter CB, Choi HA, Kobori N, Moore AN. Traumatic brain injury alters methionine metabolism: Implications for pathophysiology. Front Syst Neurosci. 2016; 10: 36. PMID: 27199685. 29. Papa L, Brophy GM, Welch RD, et al. Time course and diagnostic accuracy of glial and neuronal blood biomarkers gfap and uch-l 1 in a large cohort of trauma patients with and without mild traumatic brain injury. JAMA Neurol. May 01 2016; 73(5): 551 -560. PMID: 27018834. 30. Welch RD, Ayaz SI, Lewis LM, et al. Ability of serum glial fibrillary acidic protein, ubiquitin c-terminal hydrolase-l 1, and S 100 B to differentiate normal and abnormal head computed tomography findings in patients with suspected mild or moderate traumatic brain injury. J Neurotrauma. Jan 15 2016; 33(2): 203214. PMID: 26467555. 31. Diaz-Arrastia R, Wang KK, Papa L, et al. Acute biomarkers of traumatic brain injury: Relationship between plasma levels of ubiquitin c-terminal hydrolase-l 1 and glial fibrillary acidic protein. J Neurotrauma. Jan 01 2014; 31(1): 19 -25. PMID: 23865516. “Medically Ready Force…Ready Medical Force” 131
References: Biomarkers 25. Livingston WS, Gill JM, Cota MR, et al. Differential gene expression associated with meningeal injury in acute mild traumatic brain injury. J Neurotrauma. Feb 15 2017; 34(4): 853 -860. PMID: 27430610. 26. Heinzelmann M, Reddy SY, French LM, et al. Military personnel with chronic symptoms following blast traumatic brain injury have differential expression of neuronal recovery and epidermal growth factor receptor genes. Front Neurol. 2014; 5: 198. PMID: 25346719. 27. Sadeh N, Spielberg JM, Logue MW, et al. Ska 2 methylation is associated with decreased prefrontal cortical thickness and greater PTSD severity among trauma-exposed veterans. Mol Psychiatry. Mar 2016; 21(3): 357 -363. PMID: 26324104. 28. Dash PK, Hergenroeder GW, Jeter CB, Choi HA, Kobori N, Moore AN. Traumatic brain injury alters methionine metabolism: Implications for pathophysiology. Front Syst Neurosci. 2016; 10: 36. PMID: 27199685. 29. Papa L, Brophy GM, Welch RD, et al. Time course and diagnostic accuracy of glial and neuronal blood biomarkers gfap and uch-l 1 in a large cohort of trauma patients with and without mild traumatic brain injury. JAMA Neurol. May 01 2016; 73(5): 551 -560. PMID: 27018834. 30. Welch RD, Ayaz SI, Lewis LM, et al. Ability of serum glial fibrillary acidic protein, ubiquitin c-terminal hydrolase-l 1, and S 100 B to differentiate normal and abnormal head computed tomography findings in patients with suspected mild or moderate traumatic brain injury. J Neurotrauma. Jan 15 2016; 33(2): 203214. PMID: 26467555. 31. Diaz-Arrastia R, Wang KK, Papa L, et al. Acute biomarkers of traumatic brain injury: Relationship between plasma levels of ubiquitin c-terminal hydrolase-l 1 and glial fibrillary acidic protein. J Neurotrauma. Jan 01 2014; 31(1): 19 -25. PMID: 23865516. “Medically Ready Force…Ready Medical Force” 131
 References: Biomarkers 32. Okonkwo DO, Yue JK, Puccio AM, et al. Gfap-bdp as an acute diagnostic marker in traumatic brain injury: Results from the prospective transforming research and clinical knowledge in traumatic brain injury study. J Neurotrauma. Sep 01 2013; 30(17): 1490 -1497. PMID: 23489259. 33. Chabok SY, Moghadam AD, Saneei Z, Amlashi FG, Leili EK, Amiri ZM. Neuron-specific enolase and S 100 BB as outcome predictors in severe diffuse axonal injury. J Trauma Acute Care Surg. Jun 2012; 72(6): 16541657. PMID: 22695436. 34. Olivecrona Z, Bobinski L, Koskinen LO. Association of ICP, CPP, CT findings and S-100 B and NSE in severe traumatic head injury. Prognostic value of the biomarkers. Brain Inj. 2015; 29(4): 446 -454. PMID: 25518864. 35. Mercier E, Boutin A, Shemilt M, et al. Predictive value of neuron-specific enolase for prognosis in patients with moderate or severe traumatic brain injury: A systematic review and meta-analysis. CMAJ Open. Jul. Sep 2016; 4(3): E 371 -E 382. PMID: 27975043. 36. Robertson CS, Zager EL, Narayan RK, et al. Clinical evaluation of a portable near-infrared device for detection of traumatic intracranial hematomas. J Neurotrauma. Sep 2010; 27(9): 1597 -1604. PMID: 20568959. 37. Hanley D, Prichep LS, Bazarian J, et al. Emergency department triage of traumatic head injury using a brain electrical activity biomarker: A multisite prospective observational validation trial. Acad Emerg Med. May 2017; 24(5): 617 -627. PMID: 28177169. 38. Brooks MA, Bazarian JJ, Prichep LS, Dastidar SG, Talavage TM, Barr W. The use of an electrophysiological brain function index in the evaluation of concussed athletes. J Head Trauma Rehabil. May 17 2017. PMID: 28520677. “Medically Ready Force…Ready Medical Force” 132
References: Biomarkers 32. Okonkwo DO, Yue JK, Puccio AM, et al. Gfap-bdp as an acute diagnostic marker in traumatic brain injury: Results from the prospective transforming research and clinical knowledge in traumatic brain injury study. J Neurotrauma. Sep 01 2013; 30(17): 1490 -1497. PMID: 23489259. 33. Chabok SY, Moghadam AD, Saneei Z, Amlashi FG, Leili EK, Amiri ZM. Neuron-specific enolase and S 100 BB as outcome predictors in severe diffuse axonal injury. J Trauma Acute Care Surg. Jun 2012; 72(6): 16541657. PMID: 22695436. 34. Olivecrona Z, Bobinski L, Koskinen LO. Association of ICP, CPP, CT findings and S-100 B and NSE in severe traumatic head injury. Prognostic value of the biomarkers. Brain Inj. 2015; 29(4): 446 -454. PMID: 25518864. 35. Mercier E, Boutin A, Shemilt M, et al. Predictive value of neuron-specific enolase for prognosis in patients with moderate or severe traumatic brain injury: A systematic review and meta-analysis. CMAJ Open. Jul. Sep 2016; 4(3): E 371 -E 382. PMID: 27975043. 36. Robertson CS, Zager EL, Narayan RK, et al. Clinical evaluation of a portable near-infrared device for detection of traumatic intracranial hematomas. J Neurotrauma. Sep 2010; 27(9): 1597 -1604. PMID: 20568959. 37. Hanley D, Prichep LS, Bazarian J, et al. Emergency department triage of traumatic head injury using a brain electrical activity biomarker: A multisite prospective observational validation trial. Acad Emerg Med. May 2017; 24(5): 617 -627. PMID: 28177169. 38. Brooks MA, Bazarian JJ, Prichep LS, Dastidar SG, Talavage TM, Barr W. The use of an electrophysiological brain function index in the evaluation of concussed athletes. J Head Trauma Rehabil. May 17 2017. PMID: 28520677. “Medically Ready Force…Ready Medical Force” 132
 References: Biomarkers 39. Haneef Z, Levin HS, Frost JD, Jr. , Mizrahi EM. Electroencephalography and quantitative electroencephalography in mild traumatic brain injury. J Neurotrauma. Apr 15 2013; 30(8): 653 -656. PMID: 23249295. 40. Claassen J, Taccone FS, Horn P, Holtkamp M, Stocchetti N, Oddo M. Recommendations on the use of EEG monitoring in critically ill patients: Consensus statement from the neurointensive care section of the ESICM. Intensive Care Med. Aug 2013; 39(8): 1337 -1351. PMID: 23653183. 41. Carney N, Totten AM, O'Reilly C, et al. Guidelines for the management of severe traumatic brain injury, fourth edition. Neurosurgery. Jan 01 2017; 80(1): 6 -15. PMID: 27654000. 42. Duncan CC, Summers AC, Perla EJ, Coburn KL, Mirsky AF. Evaluation of traumatic brain injury: Brain potentials in diagnosis, function, and prognosis. Int J Psychophysiol. Oct 2011; 82(1): 24 -40. PMID: 21356253. 43. Folmer RL, Billings CJ, Diedesch-Rouse AC, Gallun FJ, Lew HL. Electrophysiological assessments of cognition and sensory processing in TBI: Applications for diagnosis, prognosis and rehabilitation. Int J Psychophysiol. Oct 2011; 82(1): 4 -15. PMID: 21419179. 44. Broglio SP, Moore RD, Hillman CH. A history of sport-related concussion on event-related brain potential correlates of cognition. Int J Psychophysiol. Oct 2011; 82(1): 16 -23. PMID: 21338634. 45. Hunt AW, Mah K, Reed N, Engel L, Keightley M. Oculomotor-based vision assessment in mild traumatic brain injury: A systematic review. J Head Trauma Rehabil. Jul-Aug 2016; 31(4): 252 -261. PMID: 26291632. 46. Taghdiri F, Varriano B, Tartaglia MC. Assessment of oculomotor function in patients with postconcussion syndrome: A systematic review. J Head Trauma Rehabil. Feb 10 2017. PMID: 28195951. “Medically Ready Force…Ready Medical Force” 133
References: Biomarkers 39. Haneef Z, Levin HS, Frost JD, Jr. , Mizrahi EM. Electroencephalography and quantitative electroencephalography in mild traumatic brain injury. J Neurotrauma. Apr 15 2013; 30(8): 653 -656. PMID: 23249295. 40. Claassen J, Taccone FS, Horn P, Holtkamp M, Stocchetti N, Oddo M. Recommendations on the use of EEG monitoring in critically ill patients: Consensus statement from the neurointensive care section of the ESICM. Intensive Care Med. Aug 2013; 39(8): 1337 -1351. PMID: 23653183. 41. Carney N, Totten AM, O'Reilly C, et al. Guidelines for the management of severe traumatic brain injury, fourth edition. Neurosurgery. Jan 01 2017; 80(1): 6 -15. PMID: 27654000. 42. Duncan CC, Summers AC, Perla EJ, Coburn KL, Mirsky AF. Evaluation of traumatic brain injury: Brain potentials in diagnosis, function, and prognosis. Int J Psychophysiol. Oct 2011; 82(1): 24 -40. PMID: 21356253. 43. Folmer RL, Billings CJ, Diedesch-Rouse AC, Gallun FJ, Lew HL. Electrophysiological assessments of cognition and sensory processing in TBI: Applications for diagnosis, prognosis and rehabilitation. Int J Psychophysiol. Oct 2011; 82(1): 4 -15. PMID: 21419179. 44. Broglio SP, Moore RD, Hillman CH. A history of sport-related concussion on event-related brain potential correlates of cognition. Int J Psychophysiol. Oct 2011; 82(1): 16 -23. PMID: 21338634. 45. Hunt AW, Mah K, Reed N, Engel L, Keightley M. Oculomotor-based vision assessment in mild traumatic brain injury: A systematic review. J Head Trauma Rehabil. Jul-Aug 2016; 31(4): 252 -261. PMID: 26291632. 46. Taghdiri F, Varriano B, Tartaglia MC. Assessment of oculomotor function in patients with postconcussion syndrome: A systematic review. J Head Trauma Rehabil. Feb 10 2017. PMID: 28195951. “Medically Ready Force…Ready Medical Force” 133
 References: Biomarkers 47. Hoffer ME, Balaban C, Szczupak M, et al. The use of oculomotor, vestibular, and reaction time tests to assess mild traumatic brain injury (m. TBI) over time. Laryngoscope Investigative Otolaryngology. 2017: n/an/a. 48. Levin B, Bhardwaj A. Chronic traumatic encephalopathy: A critical appraisal. Neurocrit Care. Apr 2014; 20(2): 334 -344. PMID: 24190181. 49. Gardner A, Iverson GL, Mc. Crory P. Chronic traumatic encephalopathy in sport: A systematic review. Br J Sports Med. Jan 2014; 48(2): 84 -90. PMID: 23803602. 50. Stern RA, Tripodis Y, Baugh CM, et al. Preliminary study of plasma exosomal tau as a potential biomarker for chronic traumatic encephalopathy. J Alzheimers Dis. 2016; 51(4): 1099 -1109. PMID: 26890775. 51. DCo. E Clinical Recommendation: Neuroimaging following mild traumatic brain injury in the non-deployed setting. Silver Spring, MD: Defense Centers of Excellence; 2013. 52. Report to Congress: Comparative effectiveness of neuroimaging modalities on the detection of traumatic brain injury. Department of Defense; 2012. www. dcoe. mil/Content/navigation/documents/Comparative_Effectiveness_of_Neuroimaging_Modalities _on_the_Detection_of_Traumatic_Brain_Injury_RTC. pdf. “Medically Ready Force…Ready Medical Force” 134
References: Biomarkers 47. Hoffer ME, Balaban C, Szczupak M, et al. The use of oculomotor, vestibular, and reaction time tests to assess mild traumatic brain injury (m. TBI) over time. Laryngoscope Investigative Otolaryngology. 2017: n/an/a. 48. Levin B, Bhardwaj A. Chronic traumatic encephalopathy: A critical appraisal. Neurocrit Care. Apr 2014; 20(2): 334 -344. PMID: 24190181. 49. Gardner A, Iverson GL, Mc. Crory P. Chronic traumatic encephalopathy in sport: A systematic review. Br J Sports Med. Jan 2014; 48(2): 84 -90. PMID: 23803602. 50. Stern RA, Tripodis Y, Baugh CM, et al. Preliminary study of plasma exosomal tau as a potential biomarker for chronic traumatic encephalopathy. J Alzheimers Dis. 2016; 51(4): 1099 -1109. PMID: 26890775. 51. DCo. E Clinical Recommendation: Neuroimaging following mild traumatic brain injury in the non-deployed setting. Silver Spring, MD: Defense Centers of Excellence; 2013. 52. Report to Congress: Comparative effectiveness of neuroimaging modalities on the detection of traumatic brain injury. Department of Defense; 2012. www. dcoe. mil/Content/navigation/documents/Comparative_Effectiveness_of_Neuroimaging_Modalities _on_the_Detection_of_Traumatic_Brain_Injury_RTC. pdf. “Medically Ready Force…Ready Medical Force” 134
 References: Behavioral Health 1. Hesdorffer DC, Rauch SL, Tamminga CA. Long-term psychiatric outcomes following traumatic brain injury: A review of the literature. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 452 -459. 2. O'Neil ME, Carlson KF, Storzbach D, et al. Factors associated with mild traumatic brain injury in veterans and military personnel: A systematic review. J Int Neuropsychol Soc. Mar 2014; 20(3): 249 -261. 3. O'Rourke C, Linden MA, Lohan M, Bates-Gaston J. Traumatic brain injury and co-occurring problems in prison populations: A systematic review. Brain Inj. 2016; 30(7): 839 -854. 4. Meares S, Shores EA, Taylor AJ, et al. The prospective course of postconcussion syndrome: The role of mild traumatic brain injury. Neuropsychology. Jul 2011; 25(4): 454 -465. 5. Fann JR, Burington B, Leonetti A, Jaffe K, Katon WJ, Thompson RS. Psychiatric illness following traumatic brain injury in an adult health maintenance organization population. Arch Gen Psychiatry. Jan 2004; 61(1): 53 -61. 6. Barnes SM, Walter KH, Chard KM. Does a history of mild traumatic brain injury increase suicide risk in veterans with PTSD? Rehabil Psychol. Feb 2012; 57(1): 18 -26. 7. Gaylord KM, Cooper DB, Mercado JM, Kennedy JE, Yoder LH, Holcomb JB. Incidence of posttraumatic stress disorder and mild traumatic brain injury in burned service members: Preliminary report. J Trauma. Feb 2008; 64(2 Suppl): S 200 -205; discussion S 205 -206. 8. Hoge CW, Mc. Gurk D, Thomas JL, Cox AL, Engel CC, Castro CA. Mild traumatic brain injury in U. S. Soldiers returning from Iraq. N Engl J Med. Jan 31 2008; 358(5): 453 -463. 9. Lew HL, Pogoda TK, Hsu PT, et al. Impact of the "polytrauma clinical triad" on sleep disturbance in a department of veterans affairs outpatient rehabilitation setting. Am J Phys Med Rehabil. Jun 2010; 89(6): 437 -445. 10. Theeler BJ, Erickson JC. Mild head trauma and chronic headaches in returning US soldiers. Headache. Apr “Medically Ready Force…Ready Medical Force” 135 2009; 49(4): 529 -534.
References: Behavioral Health 1. Hesdorffer DC, Rauch SL, Tamminga CA. Long-term psychiatric outcomes following traumatic brain injury: A review of the literature. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 452 -459. 2. O'Neil ME, Carlson KF, Storzbach D, et al. Factors associated with mild traumatic brain injury in veterans and military personnel: A systematic review. J Int Neuropsychol Soc. Mar 2014; 20(3): 249 -261. 3. O'Rourke C, Linden MA, Lohan M, Bates-Gaston J. Traumatic brain injury and co-occurring problems in prison populations: A systematic review. Brain Inj. 2016; 30(7): 839 -854. 4. Meares S, Shores EA, Taylor AJ, et al. The prospective course of postconcussion syndrome: The role of mild traumatic brain injury. Neuropsychology. Jul 2011; 25(4): 454 -465. 5. Fann JR, Burington B, Leonetti A, Jaffe K, Katon WJ, Thompson RS. Psychiatric illness following traumatic brain injury in an adult health maintenance organization population. Arch Gen Psychiatry. Jan 2004; 61(1): 53 -61. 6. Barnes SM, Walter KH, Chard KM. Does a history of mild traumatic brain injury increase suicide risk in veterans with PTSD? Rehabil Psychol. Feb 2012; 57(1): 18 -26. 7. Gaylord KM, Cooper DB, Mercado JM, Kennedy JE, Yoder LH, Holcomb JB. Incidence of posttraumatic stress disorder and mild traumatic brain injury in burned service members: Preliminary report. J Trauma. Feb 2008; 64(2 Suppl): S 200 -205; discussion S 205 -206. 8. Hoge CW, Mc. Gurk D, Thomas JL, Cox AL, Engel CC, Castro CA. Mild traumatic brain injury in U. S. Soldiers returning from Iraq. N Engl J Med. Jan 31 2008; 358(5): 453 -463. 9. Lew HL, Pogoda TK, Hsu PT, et al. Impact of the "polytrauma clinical triad" on sleep disturbance in a department of veterans affairs outpatient rehabilitation setting. Am J Phys Med Rehabil. Jun 2010; 89(6): 437 -445. 10. Theeler BJ, Erickson JC. Mild head trauma and chronic headaches in returning US soldiers. Headache. Apr “Medically Ready Force…Ready Medical Force” 135 2009; 49(4): 529 -534.
 References: Behavioral Health 11. Spencer RJ, Drag LL, Walker SJ, Bieliauskas LA. Self-reported cognitive symptoms following mild traumatic brain injury are poorly associated with neuropsychological performance in OIF/OEF veterans. J Rehabil Res Dev. 2010; 47(6): 521 -530. 12. Stefan A, Mathe JF. What are the disruptive symptoms of behavioral disorders after traumatic brain injury? A systematic review leading to recommendations for good practices. Ann Phys Rehabil Med. Feb 2016; 59(1): 5 -17. 13. Daggett V, Bakas T, Habermann B. A review of health-related quality of life in adult traumatic brain injury survivors in the context of combat veterans. J Neurosci Nurs. Apr 2009; 41(2): 59 -71. 14. Scaratti C, Leonardi M, Sattin D, Schiavolin S, Willems M, Raggi A. Work-related difficulties in patients with traumatic brain injury: A systematic review on predictors and associated factors. Disabil Rehabil. May 2017; 39(9): 847 -855. 15. Grauwmeijer E, Heijenbrok-Kal MH, Ribbers GM. Health-related quality of life 3 years after moderate to severe traumatic brain injury: A prospective cohort study. Arch Phys Med Rehabil. Jul 2014; 95(7): 12681276. 16. Ommaya AK, Salazar AM, Dannenberg AL, Ommaya AK, Chervinsky AB, Schwab K. Outcome after traumatic brain injury in the U. S. Military medical system. J Trauma. Dec 1996; 41(6): 972 -975. 17. Pogoda TK, Stolzmann KL, Iverson KM, et al. Associations between traumatic brain injury, suspected psychiatric conditions, and unemployment in Operation Enduring Freedom/Operation Iraqi Freedom Veterans. J Head Trauma Rehabil. May-Jun 2016; 31(3): 191 -203. 18. Antonius D, Mathew N, Picano J, et al. Behavioral health symptoms associated with chronic traumatic encephalopathy: A critical review of the literature and recommendations for treatment and research. J Neuropsychiatry Clin Neurosci. Fall 2014; 26(4): 313 -322. “Medically Ready Force…Ready Medical Force” 136
References: Behavioral Health 11. Spencer RJ, Drag LL, Walker SJ, Bieliauskas LA. Self-reported cognitive symptoms following mild traumatic brain injury are poorly associated with neuropsychological performance in OIF/OEF veterans. J Rehabil Res Dev. 2010; 47(6): 521 -530. 12. Stefan A, Mathe JF. What are the disruptive symptoms of behavioral disorders after traumatic brain injury? A systematic review leading to recommendations for good practices. Ann Phys Rehabil Med. Feb 2016; 59(1): 5 -17. 13. Daggett V, Bakas T, Habermann B. A review of health-related quality of life in adult traumatic brain injury survivors in the context of combat veterans. J Neurosci Nurs. Apr 2009; 41(2): 59 -71. 14. Scaratti C, Leonardi M, Sattin D, Schiavolin S, Willems M, Raggi A. Work-related difficulties in patients with traumatic brain injury: A systematic review on predictors and associated factors. Disabil Rehabil. May 2017; 39(9): 847 -855. 15. Grauwmeijer E, Heijenbrok-Kal MH, Ribbers GM. Health-related quality of life 3 years after moderate to severe traumatic brain injury: A prospective cohort study. Arch Phys Med Rehabil. Jul 2014; 95(7): 12681276. 16. Ommaya AK, Salazar AM, Dannenberg AL, Ommaya AK, Chervinsky AB, Schwab K. Outcome after traumatic brain injury in the U. S. Military medical system. J Trauma. Dec 1996; 41(6): 972 -975. 17. Pogoda TK, Stolzmann KL, Iverson KM, et al. Associations between traumatic brain injury, suspected psychiatric conditions, and unemployment in Operation Enduring Freedom/Operation Iraqi Freedom Veterans. J Head Trauma Rehabil. May-Jun 2016; 31(3): 191 -203. 18. Antonius D, Mathew N, Picano J, et al. Behavioral health symptoms associated with chronic traumatic encephalopathy: A critical review of the literature and recommendations for treatment and research. J Neuropsychiatry Clin Neurosci. Fall 2014; 26(4): 313 -322. “Medically Ready Force…Ready Medical Force” 136
 References: Rehabilitation 1. 2. 3. 4. 5. 6. 7. 8. Brasure M, Lamberty GJ, Sayer NA, et al. AHRQ comparative effectiveness reviews. Multidisciplinary postacute rehabilitation for moderate to severe traumatic brain injury in adults. Rockville (MD): Agency for Healthcare Research and Quality (US); 2012. Trudel TM, Nidiffer FD, Barth JT. Community-integrated brain injury rehabilitation: Treatment models and challenges for civilian, military, and veteran populations. J Rehabil Res Dev. 2007; 44(7): 1007 -1016. Cifu DX, Cohen SI, Lew HL, Jaffee M, Sigford B. The history and evolution of traumatic brain injury rehabilitation in military service members and veterans. Am J Phys Med Rehabil. Aug 2010; 89(8): 688 -694. Malec JF, Basford JS. Postacute brain injury rehabilitation. Arch Phys Med Rehabil. Feb 1996; 77(2): 198207. Salazar AM, Warden DL, Schwab K, et al. Cognitive rehabilitation for traumatic brain injury: A randomized trial. Defense and Veterans head injury program (dvhip) study group. Jama. Jun 21 2000; 283(23): 30753081. Sander AM, Roebuck TM, Struchen MA, Sherer M, High WM, Jr. Long-term maintenance of gains obtained in postacute rehabilitation by persons with traumatic brain injury. J Head Trauma Rehabil. Aug 2001; 16(4): 356 -373. Vanderploeg RD, Schwab K, Walker WC, et al. Rehabilitation of traumatic brain injury in active duty military personnel and veterans: Defense and Veterans brain injury center randomized controlled trial of two rehabilitation approaches. Arch Phys Med Rehabil. Dec 2008; 89(12): 2227 -2238. Tanielian T, Jaycox LH. Invisible wounds of war: Psychological and cognitive injuries, their consequences, and services to assist recovery. RAND Center for Military Health Policy Research. 2008. “Medically Ready Force…Ready Medical Force” 137
References: Rehabilitation 1. 2. 3. 4. 5. 6. 7. 8. Brasure M, Lamberty GJ, Sayer NA, et al. AHRQ comparative effectiveness reviews. Multidisciplinary postacute rehabilitation for moderate to severe traumatic brain injury in adults. Rockville (MD): Agency for Healthcare Research and Quality (US); 2012. Trudel TM, Nidiffer FD, Barth JT. Community-integrated brain injury rehabilitation: Treatment models and challenges for civilian, military, and veteran populations. J Rehabil Res Dev. 2007; 44(7): 1007 -1016. Cifu DX, Cohen SI, Lew HL, Jaffee M, Sigford B. The history and evolution of traumatic brain injury rehabilitation in military service members and veterans. Am J Phys Med Rehabil. Aug 2010; 89(8): 688 -694. Malec JF, Basford JS. Postacute brain injury rehabilitation. Arch Phys Med Rehabil. Feb 1996; 77(2): 198207. Salazar AM, Warden DL, Schwab K, et al. Cognitive rehabilitation for traumatic brain injury: A randomized trial. Defense and Veterans head injury program (dvhip) study group. Jama. Jun 21 2000; 283(23): 30753081. Sander AM, Roebuck TM, Struchen MA, Sherer M, High WM, Jr. Long-term maintenance of gains obtained in postacute rehabilitation by persons with traumatic brain injury. J Head Trauma Rehabil. Aug 2001; 16(4): 356 -373. Vanderploeg RD, Schwab K, Walker WC, et al. Rehabilitation of traumatic brain injury in active duty military personnel and veterans: Defense and Veterans brain injury center randomized controlled trial of two rehabilitation approaches. Arch Phys Med Rehabil. Dec 2008; 89(12): 2227 -2238. Tanielian T, Jaycox LH. Invisible wounds of war: Psychological and cognitive injuries, their consequences, and services to assist recovery. RAND Center for Military Health Policy Research. 2008. “Medically Ready Force…Ready Medical Force” 137
 References: Rehabilitation 9. 10. 11. 12. 13. 14. 15. 16. 17. Duchnick JJ, Ropacki S, Yutsis M, Petska K, Pawlowski C. Polytrauma transitional rehabilitation programs: Comprehensive rehabilitation for community integration after brain injury. Psychol Serv. Aug 2015; 12(3): 313 -321. Cantor J, Ashman T, Dams-O'Connor K, et al. Evaluation of the short-term executive plus intervention for executive dysfunction after traumatic brain injury: A randomized controlled trial with minimization. Arch Phys Med Rehabil. Jan 2014; 95(1): 1 -9. e 3. Twamley EW, Jak AJ, Delis DC, Bondi MW, Lohr JB. Cognitive symptom management and rehabilitation therapy (cogsmart) for veterans with traumatic brain injury: Pilot randomized controlled trial. J Rehabil Res Dev. 2014; 51(1): 59 -70. Twamley EW, Thomas KR, Gregory AM, et al. Cogsmart compensatory cognitive training for traumatic brain injury: Effects over 1 year. J Head Trauma Rehabil. Nov-Dec 2015; 30(6): 391 -401. Cooper DB, Bowles AO, Kennedy JE, et al. Cognitive rehabilitation for military service members with mild traumatic brain injury: A randomized clinical trial. J Head Trauma Rehabil. May/Jun 2017; 32(3): E 1 -e 15. Fetta J, Starkweather A, Gill JM. Computer-based cognitive rehabilitation interventions for traumatic brain injury: A critical review of the literature. J Neurosci Nurs. Aug 2017; 49(4): 235 -240. Leopold A, Lourie A, Petras H, Elias E. The use of assistive technology for cognition to support the performance of daily activities for individuals with cognitive disabilities due to traumatic brain injury: The current state of the research. Neuro. Rehabilitation. 2015; 37(3): 359 -378. Nakase-Richardson R, Sherer M, Barnett SD, et al. Prospective evaluation of the nature, course, and impact of acute sleep abnormality after traumatic brain injury. Arch Phys Med Rehabil. May 2013; 94(5): 875 -882. Nakase-Richardson R. Improving the significance and direction of sleep management in traumatic brain injury. J Head Trauma Rehabil. Mar-Apr 2016; 31(2): 79 -81. “Medically Ready Force…Ready Medical Force” 138
References: Rehabilitation 9. 10. 11. 12. 13. 14. 15. 16. 17. Duchnick JJ, Ropacki S, Yutsis M, Petska K, Pawlowski C. Polytrauma transitional rehabilitation programs: Comprehensive rehabilitation for community integration after brain injury. Psychol Serv. Aug 2015; 12(3): 313 -321. Cantor J, Ashman T, Dams-O'Connor K, et al. Evaluation of the short-term executive plus intervention for executive dysfunction after traumatic brain injury: A randomized controlled trial with minimization. Arch Phys Med Rehabil. Jan 2014; 95(1): 1 -9. e 3. Twamley EW, Jak AJ, Delis DC, Bondi MW, Lohr JB. Cognitive symptom management and rehabilitation therapy (cogsmart) for veterans with traumatic brain injury: Pilot randomized controlled trial. J Rehabil Res Dev. 2014; 51(1): 59 -70. Twamley EW, Thomas KR, Gregory AM, et al. Cogsmart compensatory cognitive training for traumatic brain injury: Effects over 1 year. J Head Trauma Rehabil. Nov-Dec 2015; 30(6): 391 -401. Cooper DB, Bowles AO, Kennedy JE, et al. Cognitive rehabilitation for military service members with mild traumatic brain injury: A randomized clinical trial. J Head Trauma Rehabil. May/Jun 2017; 32(3): E 1 -e 15. Fetta J, Starkweather A, Gill JM. Computer-based cognitive rehabilitation interventions for traumatic brain injury: A critical review of the literature. J Neurosci Nurs. Aug 2017; 49(4): 235 -240. Leopold A, Lourie A, Petras H, Elias E. The use of assistive technology for cognition to support the performance of daily activities for individuals with cognitive disabilities due to traumatic brain injury: The current state of the research. Neuro. Rehabilitation. 2015; 37(3): 359 -378. Nakase-Richardson R, Sherer M, Barnett SD, et al. Prospective evaluation of the nature, course, and impact of acute sleep abnormality after traumatic brain injury. Arch Phys Med Rehabil. May 2013; 94(5): 875 -882. Nakase-Richardson R. Improving the significance and direction of sleep management in traumatic brain injury. J Head Trauma Rehabil. Mar-Apr 2016; 31(2): 79 -81. “Medically Ready Force…Ready Medical Force” 138
 References: Rehabiiltation 18. Farrell-Carnahan L, Barnett S, Lamberty G, et al. Insomnia symptoms and behavioural health symptoms in veterans 1 year after traumatic brain injury. Brain Inj. Aug 14 2015: 1 -9. 19. Holcomb EM, Schwartz DJ, Mc. Carthy M, Thomas B, Barnett SD, Nakase-Richardson R. Incidence, characterization, and predictors of sleep apnea in consecutive brain injury rehabilitation admissions. J Head Trauma Rehabil. Mar-Apr 2016; 31(2): 82 -100. 20. Nakase-Richardson R, Stevens LF, Tang X, et al. Comparison of the VA and nidilrr TBI model system cohorts. J Head Trauma Rehabil. Jul/Aug 2017; 32(4): 221 -233. 21. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehabil Res Dev. 2012; 49(7): 1025 -1042. 22. Murray DA, Meldrum D, Lennon O. Can vestibular rehabilitation exercises help patients with concussion? A systematic review of efficacy, prescription and progression patterns. Br J Sports Med. Mar 2017; 51(5): 442451. 23. Capo-Aponte JE, Jorgensen-Wagers KL, Sosa JA, et al. Visual dysfunctions at different stages after blast and non-blast mild traumatic brain injury. Optom Vis Sci. Jan 2017; 94(1): 7 -15. 24. Johansson J, Nygren de Boussard C, Oqvist Seimyr G, Pansell T. The effect of spectacle treatment in patients with mild traumatic brain injury: A pilot study. Clin Exp Optom. May 2017; 100(3): 234 -242. 25. Rosner MS, Feinberg DL, Doble JE, Rosner AJ. Treatment of vertical heterophoria ameliorates persistent post-concussive symptoms: A retrospective analysis utilizing a multi-faceted assessment battery. Brain Inj. 2016; 30(3): 311 -317. 26. Conrad JS, Mitchell GL, Kulp MT. Vision therapy for binocular dysfunction post brain injury. Optom Vis Sci. Jan 2017; 94(1): 101 -107. 27. Gallaway M, Scheiman M, Mitchell GL. Vision therapy for post-concussion vision disorders. Optom Vis Sci. Jan 2017; 94(1): 68 -73. “Medically Ready Force…Ready Medical Force” 139
References: Rehabiiltation 18. Farrell-Carnahan L, Barnett S, Lamberty G, et al. Insomnia symptoms and behavioural health symptoms in veterans 1 year after traumatic brain injury. Brain Inj. Aug 14 2015: 1 -9. 19. Holcomb EM, Schwartz DJ, Mc. Carthy M, Thomas B, Barnett SD, Nakase-Richardson R. Incidence, characterization, and predictors of sleep apnea in consecutive brain injury rehabilitation admissions. J Head Trauma Rehabil. Mar-Apr 2016; 31(2): 82 -100. 20. Nakase-Richardson R, Stevens LF, Tang X, et al. Comparison of the VA and nidilrr TBI model system cohorts. J Head Trauma Rehabil. Jul/Aug 2017; 32(4): 221 -233. 21. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehabil Res Dev. 2012; 49(7): 1025 -1042. 22. Murray DA, Meldrum D, Lennon O. Can vestibular rehabilitation exercises help patients with concussion? A systematic review of efficacy, prescription and progression patterns. Br J Sports Med. Mar 2017; 51(5): 442451. 23. Capo-Aponte JE, Jorgensen-Wagers KL, Sosa JA, et al. Visual dysfunctions at different stages after blast and non-blast mild traumatic brain injury. Optom Vis Sci. Jan 2017; 94(1): 7 -15. 24. Johansson J, Nygren de Boussard C, Oqvist Seimyr G, Pansell T. The effect of spectacle treatment in patients with mild traumatic brain injury: A pilot study. Clin Exp Optom. May 2017; 100(3): 234 -242. 25. Rosner MS, Feinberg DL, Doble JE, Rosner AJ. Treatment of vertical heterophoria ameliorates persistent post-concussive symptoms: A retrospective analysis utilizing a multi-faceted assessment battery. Brain Inj. 2016; 30(3): 311 -317. 26. Conrad JS, Mitchell GL, Kulp MT. Vision therapy for binocular dysfunction post brain injury. Optom Vis Sci. Jan 2017; 94(1): 101 -107. 27. Gallaway M, Scheiman M, Mitchell GL. Vision therapy for post-concussion vision disorders. Optom Vis Sci. Jan 2017; 94(1): 68 -73. “Medically Ready Force…Ready Medical Force” 139
 References: Rehabilitation 28. Thiagarajan P, Ciuffreda KJ. Effect of oculomotor rehabilitation on vergence responsivity in mild traumatic brain injury. J Rehabil Res Dev. 2013; 50(9): 1223 -1240. 29. Thiagarajan P, Ciuffreda KJ, Capo-Aponte JE, Ludlam DP, Kapoor N. Oculomotor neurorehabilitation for reading in mild traumatic brain injury (m. TBI): An integrative approach. Neuro. Rehabilitation. 2014; 34(1): 129 -146. 30. Thiagarajan P, Ciuffreda KJ. Effect of oculomotor rehabilitation on accommodative responsivity in mild traumatic brain injury. J Rehabil Res Dev. 2014; 51(2): 175 -191. 31. Berger S, Kaldenberg J, Selmane R, Carlo S. Effectiveness of interventions to address visual and visualperceptual impairments to improve occupational performance in adults with traumatic brain injury: A systematic review. Am J Occup Ther. May-Jun 2016; 70(3): 7003180010 p 7003180011 -7003180017. 32. Schmitter-Edgecombe M, Robertson K. Recovery of visual search following moderate to severe traumatic brain injury. J Clin Exp Neuropsychol. 2015; 37(2): 162 -177. 33. O'Neill EC, Connell PP, O'Connor JC, Brady J, Reid I, Logan P. Prism therapy and visual rehabilitation in homonymous visual field loss. Optom Vis Sci. Feb 2011; 88(2): 263 -268. 34. Schuett S, Heywood CA, Kentridge RW, Dauner R, Zihl J. Rehabilitation of reading and visual exploration in visual field disorders: Transfer or specificity? Brain. Mar 2012; 135(Pt 3): 912 -921. 35. de Haan GA, Melis-Dankers BJ, Brouwer WH, Tucha O, Heutink J. The effects of compensatory scanning training on mobility in patients with homonymous visual field defects: A randomized controlled trial. PLo. S One. 2015; 10(8): e 0134459. 36. Clark J, Hasselfeld K, Bigsby K, Divine J. Colored glasses to mitigate photophobia symptoms posttraumatic brain injury. J Athl Train. Jun 26 2017. “Medically Ready Force…Ready Medical Force” 140
References: Rehabilitation 28. Thiagarajan P, Ciuffreda KJ. Effect of oculomotor rehabilitation on vergence responsivity in mild traumatic brain injury. J Rehabil Res Dev. 2013; 50(9): 1223 -1240. 29. Thiagarajan P, Ciuffreda KJ, Capo-Aponte JE, Ludlam DP, Kapoor N. Oculomotor neurorehabilitation for reading in mild traumatic brain injury (m. TBI): An integrative approach. Neuro. Rehabilitation. 2014; 34(1): 129 -146. 30. Thiagarajan P, Ciuffreda KJ. Effect of oculomotor rehabilitation on accommodative responsivity in mild traumatic brain injury. J Rehabil Res Dev. 2014; 51(2): 175 -191. 31. Berger S, Kaldenberg J, Selmane R, Carlo S. Effectiveness of interventions to address visual and visualperceptual impairments to improve occupational performance in adults with traumatic brain injury: A systematic review. Am J Occup Ther. May-Jun 2016; 70(3): 7003180010 p 7003180011 -7003180017. 32. Schmitter-Edgecombe M, Robertson K. Recovery of visual search following moderate to severe traumatic brain injury. J Clin Exp Neuropsychol. 2015; 37(2): 162 -177. 33. O'Neill EC, Connell PP, O'Connor JC, Brady J, Reid I, Logan P. Prism therapy and visual rehabilitation in homonymous visual field loss. Optom Vis Sci. Feb 2011; 88(2): 263 -268. 34. Schuett S, Heywood CA, Kentridge RW, Dauner R, Zihl J. Rehabilitation of reading and visual exploration in visual field disorders: Transfer or specificity? Brain. Mar 2012; 135(Pt 3): 912 -921. 35. de Haan GA, Melis-Dankers BJ, Brouwer WH, Tucha O, Heutink J. The effects of compensatory scanning training on mobility in patients with homonymous visual field defects: A randomized controlled trial. PLo. S One. 2015; 10(8): e 0134459. 36. Clark J, Hasselfeld K, Bigsby K, Divine J. Colored glasses to mitigate photophobia symptoms posttraumatic brain injury. J Athl Train. Jun 26 2017. “Medically Ready Force…Ready Medical Force” 140
 References: Long Term Effects 1. 2. 3. 4. 5. 6. 7. 8. Bazarian JJ, Cernak I, Noble-Haeusslein L, Potolicchio S, Temkin N. Long-term neurologic outcomes after traumatic brain injury. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 439 -451. PMID: 19940677. Pugh MJ, Orman JA, Jaramillo CA, et al. The prevalence of epilepsy and association with traumatic brain injury in veterans of the Afghanistan and Iraq wars. J Head Trauma Rehabil. Jan-Feb 2015; 30(1): 29 -37. PMID: 24695268. Eftekhar B, Sahraian MA, Nouralishahi B, et al. Prognostic factors in the persistence of posttraumatic epilepsy after penetrating head injuries sustained in war. J Neurosurg. Feb 2009; 110(2): 319 -326. PMID: 18976060. Raymont V, Salazar AM, Lipsky R, Goldman D, Tasick G, Grafman J. Correlates of posttraumatic epilepsy 35 years following combat brain injury. Neurology. Jul 20 2010; 75(3): 224 -229. PMID: 20644150. Weiner MW, Harvey D, Hayes J, et al. Effects of traumatic brain injury and posttraumatic stress disorder on development of alzheimer's disease in Vietnam Veterans using the alzheimer's disease neuroimaging initiative: Preliminary report. Alzheimers Dement (N Y). Jun 2017; 3(2): 177 -188. PMID: 28758146. Peltz CB, Gardner RC, Kenney K, Diaz-Arrastia R, Kramer JH, Yaffe K. Neurobehavioral characteristics of older Veterans with remote traumatic brain injury. J Head Trauma Rehabil. Jan/Feb 2017; 32(1): E 8 -E 15. PMID: 27323220. Dunning DL, Westgate B, Adlam AL. A meta-analysis of working memory impairments in survivors of moderate-to-severe traumatic brain injury. Neuropsychology. Oct 2016; 30(7): 811 -819. PMID: 27182710. Dikmen SS, Corrigan JD, Levin HS, Machamer J, Stiers W, Weisskopf MG. Cognitive outcome following traumatic brain injury. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 430 -438. PMID: 19940676. “Medically Ready Force…Ready Medical Force” 141
References: Long Term Effects 1. 2. 3. 4. 5. 6. 7. 8. Bazarian JJ, Cernak I, Noble-Haeusslein L, Potolicchio S, Temkin N. Long-term neurologic outcomes after traumatic brain injury. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 439 -451. PMID: 19940677. Pugh MJ, Orman JA, Jaramillo CA, et al. The prevalence of epilepsy and association with traumatic brain injury in veterans of the Afghanistan and Iraq wars. J Head Trauma Rehabil. Jan-Feb 2015; 30(1): 29 -37. PMID: 24695268. Eftekhar B, Sahraian MA, Nouralishahi B, et al. Prognostic factors in the persistence of posttraumatic epilepsy after penetrating head injuries sustained in war. J Neurosurg. Feb 2009; 110(2): 319 -326. PMID: 18976060. Raymont V, Salazar AM, Lipsky R, Goldman D, Tasick G, Grafman J. Correlates of posttraumatic epilepsy 35 years following combat brain injury. Neurology. Jul 20 2010; 75(3): 224 -229. PMID: 20644150. Weiner MW, Harvey D, Hayes J, et al. Effects of traumatic brain injury and posttraumatic stress disorder on development of alzheimer's disease in Vietnam Veterans using the alzheimer's disease neuroimaging initiative: Preliminary report. Alzheimers Dement (N Y). Jun 2017; 3(2): 177 -188. PMID: 28758146. Peltz CB, Gardner RC, Kenney K, Diaz-Arrastia R, Kramer JH, Yaffe K. Neurobehavioral characteristics of older Veterans with remote traumatic brain injury. J Head Trauma Rehabil. Jan/Feb 2017; 32(1): E 8 -E 15. PMID: 27323220. Dunning DL, Westgate B, Adlam AL. A meta-analysis of working memory impairments in survivors of moderate-to-severe traumatic brain injury. Neuropsychology. Oct 2016; 30(7): 811 -819. PMID: 27182710. Dikmen SS, Corrigan JD, Levin HS, Machamer J, Stiers W, Weisskopf MG. Cognitive outcome following traumatic brain injury. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 430 -438. PMID: 19940676. “Medically Ready Force…Ready Medical Force” 141
 References: Long Term Effects 9. 10. 11. 12. 13. Raymont V, Greathouse A, Reding K, Lipsky R, Salazar A, Grafman J. Demographic, structural and genetic predictors of late cognitive decline after penetrating head injury. Brain. Feb 2008; 131(Pt 2): 543 -558. PMID: 18094019. Glass L, Krueger F, Solomon J, Raymont V, Grafman J. Mental paper folding performance following penetrating traumatic brain injury in combat veterans: A lesion mapping study. Cereb Cortex. Jul 2013; 23(7): 1663 -1672. PMID: 22669970. Zacks JM, Kurby CA, Landazabal CS, Krueger F, Grafman J. Effects of penetrating traumatic brain injury on event segmentation and memory. Cortex. Jan 2016; 74: 233 -246. PMID: 26704077. Mc. Intyre A, Mehta S, Aubut J, Dijkers M, Teasell RW. Mortality among older adults after a traumatic brain injury: A meta-analysis. Brain Inj. 2013; 27(1): 31 -40. PMID: 23163240. Rutherford GW, Wlodarczyk RC. Distant sequelae of traumatic brain injury: Premature mortality and intracranial neoplasms. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 468 -474. PMID: 19940680. “Medically Ready Force…Ready Medical Force” 142
References: Long Term Effects 9. 10. 11. 12. 13. Raymont V, Greathouse A, Reding K, Lipsky R, Salazar A, Grafman J. Demographic, structural and genetic predictors of late cognitive decline after penetrating head injury. Brain. Feb 2008; 131(Pt 2): 543 -558. PMID: 18094019. Glass L, Krueger F, Solomon J, Raymont V, Grafman J. Mental paper folding performance following penetrating traumatic brain injury in combat veterans: A lesion mapping study. Cereb Cortex. Jul 2013; 23(7): 1663 -1672. PMID: 22669970. Zacks JM, Kurby CA, Landazabal CS, Krueger F, Grafman J. Effects of penetrating traumatic brain injury on event segmentation and memory. Cortex. Jan 2016; 74: 233 -246. PMID: 26704077. Mc. Intyre A, Mehta S, Aubut J, Dijkers M, Teasell RW. Mortality among older adults after a traumatic brain injury: A meta-analysis. Brain Inj. 2013; 27(1): 31 -40. PMID: 23163240. Rutherford GW, Wlodarczyk RC. Distant sequelae of traumatic brain injury: Premature mortality and intracranial neoplasms. J Head Trauma Rehabil. Nov-Dec 2009; 24(6): 468 -474. PMID: 19940680. “Medically Ready Force…Ready Medical Force” 142


