315bb0fda211d0d48135e2e771d5113b.ppt
- Количество слайдов: 60

1 Rad Protection & Radiobiology review 244 09

2 STAT 8 & 9 Protecting Patients & Personnel • COMMUNICATE • COLLIMATE • SHIELD

3 • • Ch 1 – pg 1 RHB SYLLABUS 5% population have fluoro exams 53% GI tract (1996 ) 120 sec fluoro ~= ese 5 – 15 rads Comp to ABD ~= ese 100 - 500 mrads Fluoro used for dynamic studies USING FLUORO TO POSTION PATIENTS PRIOR TO TAKING FILM IS PROHIBITED • Must have fluoro permit or Supervisor & Operators Certificate from state

4 PATIENT PROTECTION • • LIMIT SIZE OF BEAM ON TIME DISTANCE OF SOURCE TO SKIN PBL FILTRATION (2. 5 mm Al eq) @ 70 SHEILDING SCREEN/FILM COMBO -OVERHEADS

5 more 6 things that will reduce patient exposure: • • • Collimating to the area of interest Using last frame hold Keeping the pt. / detector distance to a minimum Using high kv low m. A Pulsed Fluoro with low frame rates Using the largest II mode
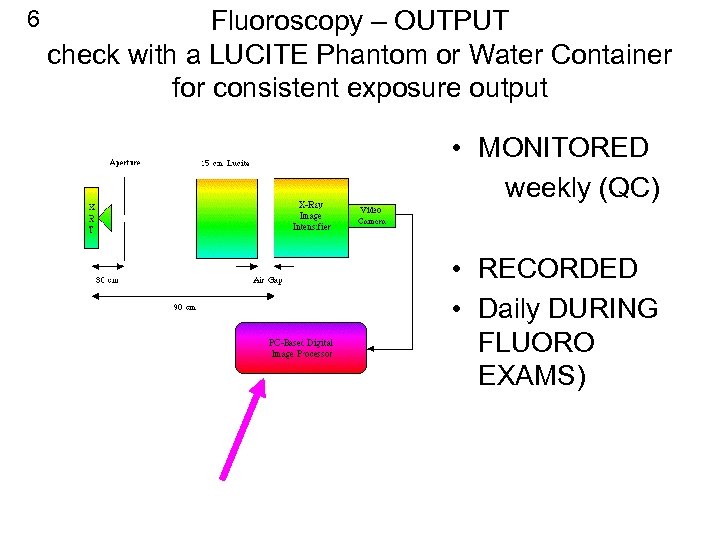
6 Fluoroscopy – OUTPUT check with a LUCITE Phantom or Water Container for consistent exposure output • MONITORED weekly (QC) • RECORDED • Daily DURING FLUORO EXAMS)

7 DOSE REGULATIONS • BEFORE 1974 - AT TABLETOP • 5 R/MIN (WITHOUT AEC) – BOOST MODE • After 1974 with AEC • 10 R/MIN • 20 R/MIN BOOST (Stat p 198)

8 Exposure Bushong – ch 39 DAP • Must not exceed 2. 1 R/ma/min • 2. 2 R/min in RHB • DAP – dose area product • Takes in account the volume of tissue irradiated

9 CINE DOSE • CINE - 2 m. R per frame (30 OR 60 f/sec) • 400 mr per “look” • WHAT WOULD BE THE PATIENT’S DOSE FOR A 5 MIN PROCEDURE • AT 60 F/SEC?

10 Permissible Occupational Dose • Annual dose: • 5 Rem / year 50 m. Sv / year • Cumulative Dose • 1 rem x age 10 m. Sv X age

11 OCCUPATIONAL EXPOSURES • 5 REMS / YEAR BUT NOT TO EXCEED 1. 25 REM/QUARTER • OLD “MPD 5(Age – 18)”

12 Occupational Dose ANNUAL LIMITS • WHOLE BODY = 5 REMS / 5000 m. Rem • LENS OF THE EYE = 15 REMS • EXTREMITIES = 50 REMS
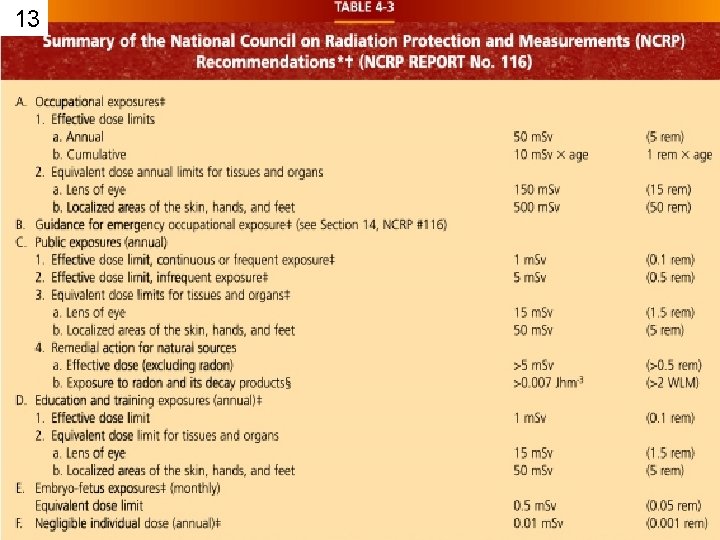
13

14 DOSE LIMIT (DL) • NCRP ? • BEIR ? NCR ? (Stat Book) • DL’S imply that if received annually, risk of death would be less than 1/10, 000 • Based on Linear Non-Threshold • DL – Dose Limits • Occupation Exposure (rems)

15

16 REGULATORY AGENCIES • NCRP – National Council on Radiation Protection and Measurement • Reviews recommendation for radiation protection & safety • NRC – Nuclear Regulatory Committee • Makes LAWS & enforces regulations

17 REGULATORY AGENCIES p 143/5 th BEIR - Biological Effect of Ionizing Radiation UNSCEAR – United Nations Scientific Committee on the Effects of Atomic Radiation

18 ROOM SHIELDING • PRIMARY SHIELD – • PRIMARY BEAM DIRECTED AT WALL • 1/16 LEAD - 7 FEET HIGH

19 ROOM SHIELDING • • • SECONDARY – NO PRIMARY BEAM 1/32 LEAD CONTROL BOOTH (SECONDARY) BEAM SCATTERS 2 X BEFORE HITTING LEAD WINDOW – 1. 5 MM LEAD EQ

20 Room Sheilding Ch. 9 • Workload Factor (W) -ma/sec/week – how much time during the week is the beam on (or ma/min/wk) • Occupancy Factor (T) - # of people in room - beyond the barrier • Use Factor (U) - % of time beam will strike a barrier (table pg 242) Primary vs Secondary • Leakage Radiation

21 SHEILDING • HVL? • TVL? • 1 TVL = 3. 3 HVL

22 SHEILDING PG 72 RHB • HVL – expressed 2 ways • HOW MUCH IT REDUCES THE ORGINAL BEAM INTENSITY • HOW MUCH IS REQUIRED FOR BARRIER THICKNESS (amount needed to attenuated the beam

23 HVL TVL • The amount of material required to reduce the energy of the beam by……. . • HVL ____________ • TVL ___________ • Examples 100 – 50 - 25 – 12. 5 – 6. 25 - 3. 12 • ? How many to reduce to 1/2 ? 1/10 th ?
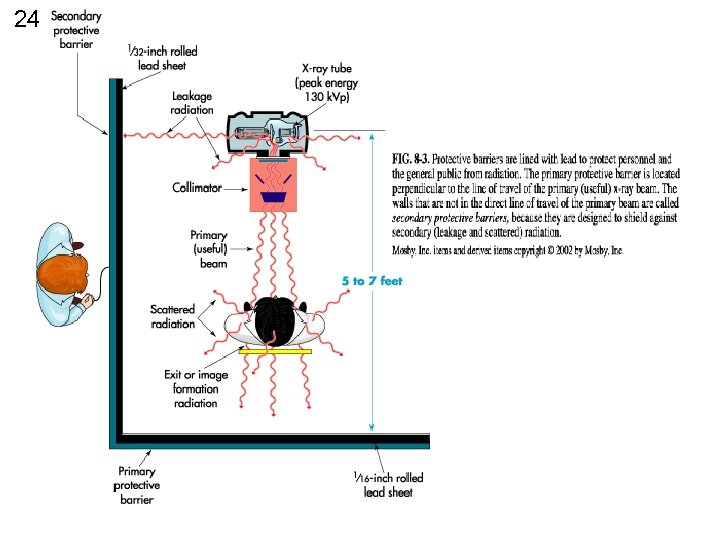
24

25 LEAKAGE RADIATION may not EXCEED • TUBE HOUSING 100 m. R / HR @ 1 meter
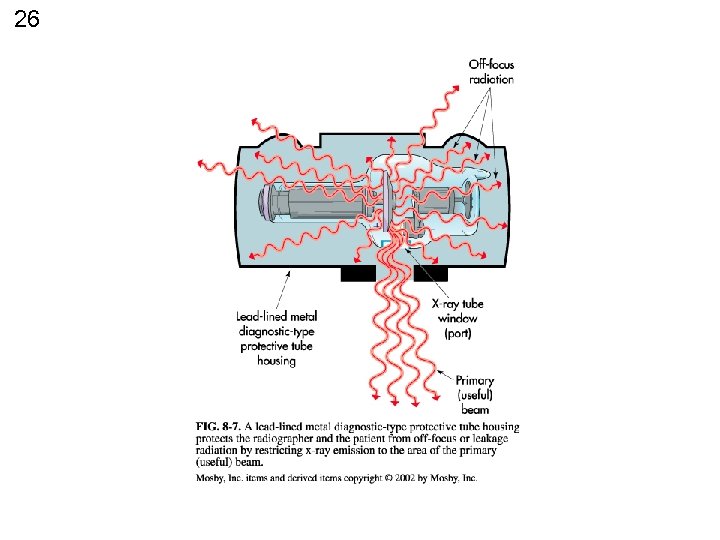
26

27 PERSONNEL PROTECTION • SCATTER FROM THE PATIENT • TABLE TOP, COLLIMATOR, TUBE HOUSING, BUCKY • STRAY RADIATION – LEAKAGE OR SCATTER RADIATION

28 • HIGH RADIATION AREA – • 100 m. Rem ( 0. 1 rem / (1 ms. V) – @ 30 cm from the source of radiaton • RADIATION AREA – • RHB: 5 m. Rem ( 0. 005 rem / (. 05 ms. V) – @ 30 cm from the source of radiation • PUBLIC 2 mrem per week* (STAT)

29 MONITORING • CONTROLLED AREA – Used by occupationaly exposed personnel (monitored) • 100 mrem / WEEK • UNCONTROLLED AREA – PUBLIC • 2 mrem per week*

30 A “controlled area” is defined as one • that is occupied by people trained in radiologic safety • that is occupied by people who wear radiation monitors • whose occupancy factor is 1

31 Personnel Monitoring Devices ACCURACY • • Film Badges TLD POSL Pocket Dosimeter • Ring Badge • • 10 mrem 5 mrem 1 mrem ?

32 Personnel Monitoring Devices $$$$$$ • Film Badges • TLD • POSL • Least cost • $2. 50 • ? most used • $10 • ?

33 Q = t x תּ CUTIE PIE

34 RHB NOTIFICATION (EXP IN 24 HOURS) (RP Syllabus – pg 68) IMMEDIATE reporting – WITHIN 24 HOURS • TOTAL DOSE OF 25 rems • Eye dose – 75 rem • Extremity – 250 RADS OVEREXPOSURE – received w/in 24 hrs Must be Reported WITHIN 30 DAYS • TOTAL DOSE OF 5 rems • Eye dose – 15 rem • Extremity - 50 REMS

35 TYPES OF RADIATON (ALL CAUSE IONIZATION) • • • PARTICULATE (HIGH LET) ALPHA BETA FAST NEUTRONS • More destructive • • • ELECTROMAGNETIC (LOW LET) XRAY GAMMA (damaged caused by indirect action = free radicals – can be repaired)

36 measurement (Rad + QF = REM)

37 Quality Factor “weighting factor for tissue” th ED • See ch 7 - pg 155 5 • Organ tissue weighting factor • “ratio of risk of stochastic effects – rads to type of tissue
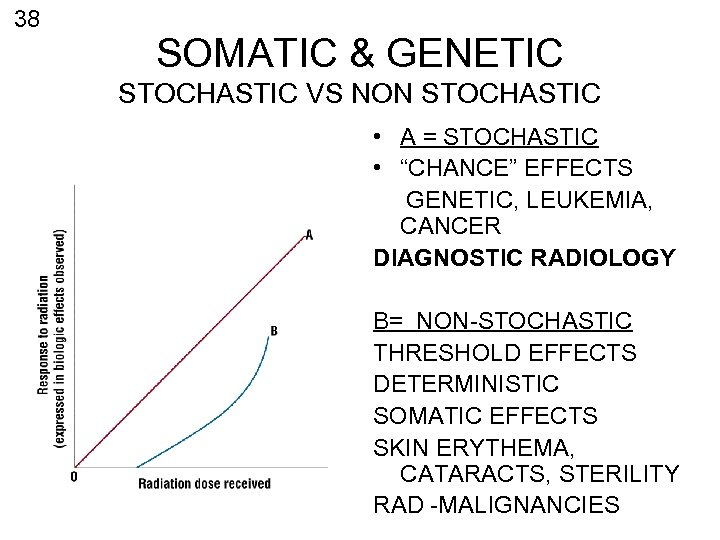
38 SOMATIC & GENETIC STOCHASTIC VS NON STOCHASTIC • A = STOCHASTIC • “CHANCE” EFFECTS GENETIC, LEUKEMIA, CANCER DIAGNOSTIC RADIOLOGY B= NON-STOCHASTIC THRESHOLD EFFECTS DETERMINISTIC SOMATIC EFFECTS SKIN ERYTHEMA, CATARACTS, STERILITY RAD -MALIGNANCIES

39 RHB – Rad Prot – CH. IX p 51 • ALARA (no minimum threshold) • STOCHASTIC EFFECTS – NON TRESHOLD (CA + GENETIC) • NON STHOCAHSTIC (DETERMINISTIC) SEVERITY OF EFFECTS VARIES WITH RADIATION DOSE (THRESHOLD) (CATARACTS, SKIN, BONE MARROW, STERILITY

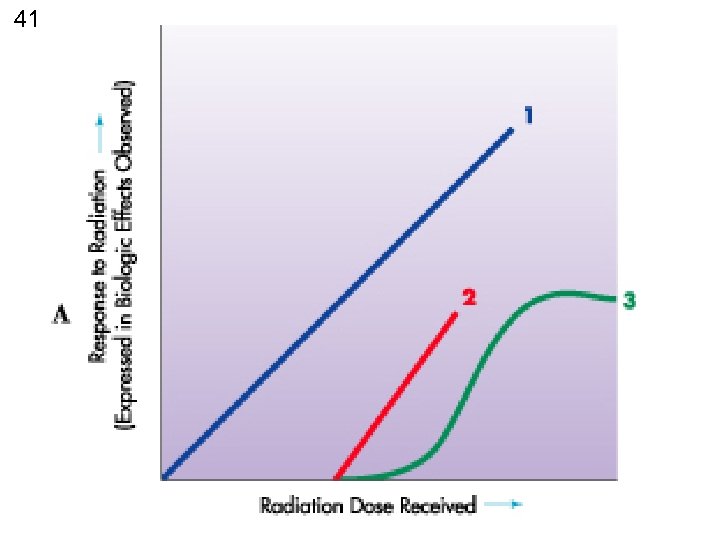
40 Linear vs non linear • Linear – direct response to the dose and the effects seen (proportionally) • Non linear – effects are not proportional to the dose received • S curve – rad therapy & skin erythema
41

42 Direct & In. Direct • Direct - DNA hit or with high LET • In. Direct – most frequently occuring • Does not hit DNA directly – but can effect DNA through radiolysis • 90% of cell damage is repairable

43 • Ch 4 – pg 37 Fluoro Exam ↑ ↑ directly proportional to dose (pt & Rt) • Operator dose & pt dose • Image brightness & rad dose • m. A, kvp, collimation, filtration, time, TPD ↑ ↓indirectly proportional to dose (pt & Rt) • Poor image quality • Room lighting • Tabletop absorption

44 PATIENT DOSE • RAD • MR/MAS PER EXPOSURE - At each k. Vp level – there is a determined output for each radiographic room • EX 70 kvp = 2. 5 mr/mas • ABD done 70 k. Vp, 20 mas • 2. 5 x 20 = 50 m. R for that one exposure. • LOOK AT formula: mr/mas Ch 8 Stat • CH 40 BUSHONG ( for 9/17)

45 Mr/mas • • A room uses 3. 5 m. R @ 80 k. Vp 2. 5 m. R @ 70 k. Vp 4. 5 m. R @ 90 k. Vp 5. 6 m. R @ 100 k. Vp Find the patient’s exposure (ESE) for KUB ( 40 m. As 70 kvp) = ___ m. Rad

46 • A room uses • • 3. 5 m. R @ 80 k. Vp 2. 5 m. R @ 70 k. Vp 4. 5 m. R @ 90 k. Vp 5. 6 m. R @ 100 k. Vp • • 2 views Chest (PA) 5 mas 90 k. Vp (LAT) 10 mas 100 k. Vp _ TOTAL = _____ m. Rad

47 At 1 foot from a source the output intensity is 300 m. R/hr and you were there for 20 minutes. What is your dose?

48 At 1 foot from a source the output intensity is 300 m. R/hr and you were there for 20 minutes. What is your dose? NOW - What is the intensity total if you moved 2 feet away and remained for additional 40 minutes?

49 • During a Fluoroscopy Procedure…. . • Tube output was 1. 5 R/min @ 2. 2 ma • If at 2 feet from the radiation source the intensity of exposure is 240 m. R per hour and the RT remains at this location for 10 minutes, then moved 4 feet away from the radiation source and remained there for 20 minutes? • What is your dose (RT) when you moved? • What is your (RT) total exposure? • What did the patient receive?

50 ESE FOR FLUORO • TLD PLACED AT SKIN ENTRACE POINT • 1 – 5 R/MINUTE AVE IS 4 R/MIN • INTERGRAL DOSE – • 100 ERGS OF TISSUE = 1 RAD EXPOSURE • OR 1 GM RAD = 100 ERGS
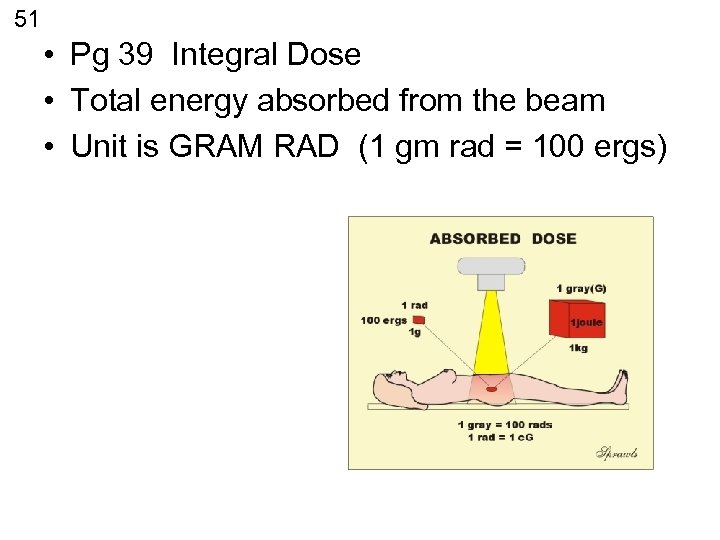
51 • Pg 39 Integral Dose • Total energy absorbed from the beam • Unit is GRAM RAD (1 gm rad = 100 ergs)

52 • The NCRP states that: the risk (to the embryo/fetus) is considered to be negligible at 5 rads or less when compared to the other risks of pregnancy • and the risk of malformation is significantly increased above control levels only at doses above 15 rads

53 10 – 25 RAD Rule and Pregnancy Bush p 545 • Below 10 RAD (100 mgy) ther ab NOT indicated • Above 25 RAD may justify TAB • FETAL doses RARELY reach 5 RAD

54 • As shown in animal experiments, deleterious effects to the embryo may be produced with doses of as little as _____ delivered to the embryo. • a. 5 rads • b. 15 mrads • c. 15 rads • d. 50 mrads • e. 50 rads

55 PERSONNEL PROTECTION • • • PROTECTIVE APRONS – 0. 25 PB = 97% ↓ TO SCATTER 0. 5 PB = 99. 9% ↓ TO SCATTER THYROID SHEILDS (0. 25 & 0. 5) GLOVES (0. 25 & 0. 5)

56 Gonad shielding & dose • ♀ receive 3 x more dose than • ♂ for pelvic x-rays • 1 mm lead will reduce exposure (primary) by about 50% ♀ • by about 90 – 95 % ♂

57 • HIGHLIGHTS RE FLUORO & RAD PROT • PG 43 - lymphocytes most depressed ♀ OVARIES = TEMP STERILITY • 30 rads ♂ TESTIES = TEMP STERILITY • 300 rads • PG 45 – REPEAT INFO

58 GERM CELLS in Females (present at birth) • HIGHLY RADIOSENSITIVE = DEPENDS OF STAGE OF DEVELOPMENT • Mature ovum do not divide frequently • (20 -30 yrs old - least sensitive) • Immature very sensitive • If exposed ova meets sperm – may contain damaged chromosomes – passing genetic damage to offspring = • CONGENTIAL ABNORMALITIES

59 GONAD SHIELDING pg 87 • MUST BE. 5 MM OF LEAD • MUST BE USED WHEN GONADS WILL LIE WITHING 5 CM OF THE COLLIMATED AREA (RHB) • FLAT / CONTACT / SHADOW

60 Doses above 50 gy
315bb0fda211d0d48135e2e771d5113b.ppt