cdfe037a7230676e670b7f916926e4bc.ppt
- Количество слайдов: 142

何謂實證醫學 台大內科 張家勳 MD, MSc in Clinical Epidemiology E-mail address: chiahsuin@yahoo. com

Our Goals… 觀念澄清 n 什麼是“實證醫學” ? n 為什麼要推動實證醫學教學? n 實證醫學教學 和一般教科書上談的知識 有什 麼不一樣?

平常醫師是如何去診斷、治療患者?

醫生, 請問… “我到底有沒有病? ” n “我該不該吃藥? ” n “我一定要開刀嗎 還有沒有更好的方法? ” n “我還能活多久? ” n

n 臨床上面臨的問題有許多不確定性, 這種 不確定性是以機率來表示 n 機率的估計 可以來自個人以往的經驗, 但 免不了有某種程度的偏差 n 沒有任何一位臨床醫師擁有完全足夠的臨 床經驗, 可辨識大部分慢性病之間細微又 長期的互動關係
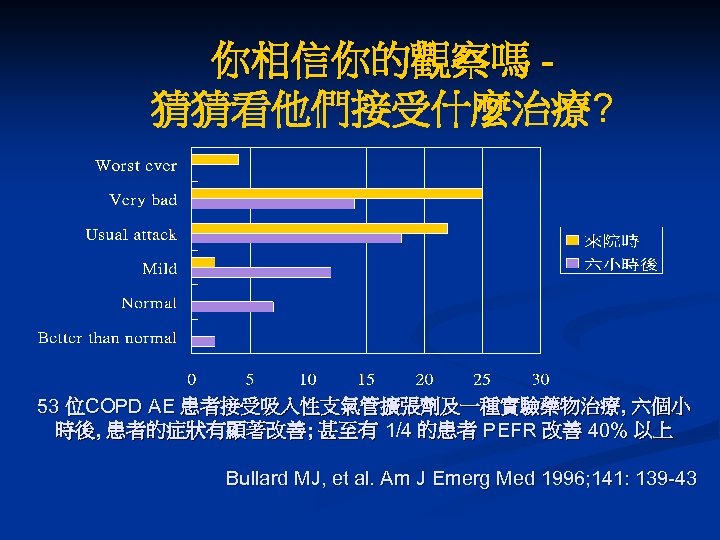
你相信你的觀察嗎 猜猜看他們接受什麼治療? 53 位COPD AE 患者接受吸入性支氣管擴張劑及一種實驗藥物治療, 六個小 時後, 患者的症狀有顯著改善; 甚至有 1/4 的患者 PEFR 改善 40% 以上 Bullard MJ, et al. Am J Emerg Med 1996; 141: 139 -43

Do Something is Better than Do Nothing? “依據我的經驗 : 肝硬化合併門脈高壓的患者, 接受分流手術治療 (Portal-Systemic Shunting)者 比未接受手術治療者, 發生食道靜脈出血的機率要來得少 腹水比較容易控制 因此也活得比較久 …”
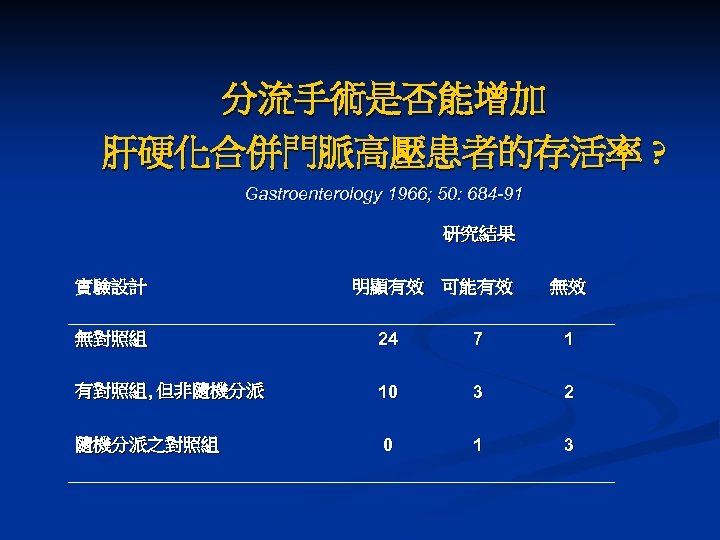
分流手術是否能增加 肝硬化合併門脈高壓患者的存活率 ? Gastroenterology 1966; 50: 684 -91 研究結果 實驗設計 明顯有效 可能有效 無效 無對照組 24 7 1 有對照組, 但非隨機分派 10 3 2 隨機分派之對照組 0 1 3
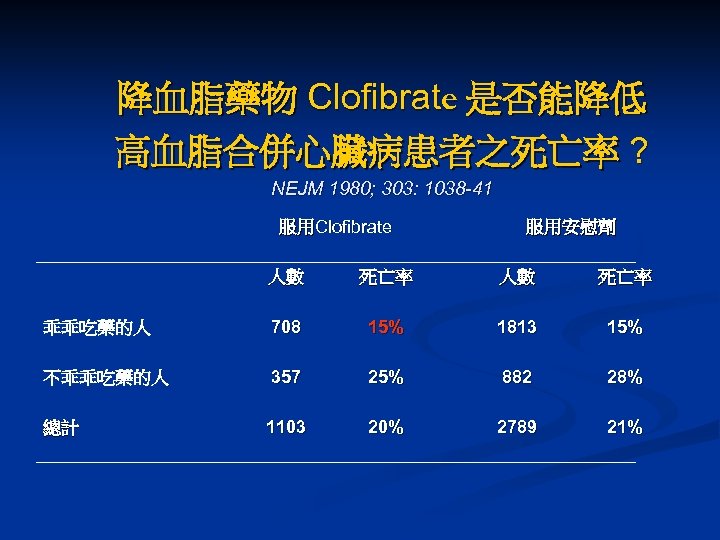
降血脂藥物 Clofibrate 是否能降低 高血脂合併心臟病患者之死亡率 ? NEJM 1980; 303: 1038 -41 服用Clofibrate 服用安慰劑 人數 死亡率 乖乖吃藥的人 708 15% 1813 15% 不乖乖吃藥的人 357 25% 882 28% 總計 1103 20% 2789 21%

Clinical outcomes depend on: Severity of illness n Co-morbidity n Other prognostic factors (known and unknown) n Drug compliance, health awareness, social support… n n Treatment

生理學與病理學是瞭解疾病機轉及治療 患者的基礎,然而… n n 醫學理論往往繁多而不一致 看似合理的治療原則有時對病人反而有害 - 以心肌梗塞後病人的心律不整為例 瞭解疾病的病理生理學是必要的,但是單是如此 對於臨床執業來說仍是不夠的。 所以英國醫師 Archie Cochrane 大力提倡隨機對 照試驗的重要性,並指出醫療資源應運用於經嚴 謹研究證實有效的治療 才能提供合理的服務。

何謂實證醫學 “Conscientious, explicit, and judicious use of current best evidence in making decisions about individual patients” Archie Cochrane 1972 § 設計良好的臨床研究才是讓證據說話的基石 § 不是只有隨機對照試驗才算是證據; 目前的證據未必是 完美的, 絕對正確的 § 將來有可能有新的證據出現

我們為什麼要學(教) “實證醫學”?

我們為什麼要提倡實證醫學 ? ü 提供獨立思考 終生學習的模式及技巧 n 同時提升臨床研究及醫療照護之品質 n 參考以嚴謹科學原則為依據的觀察 作為臨 床決策的指引 n 提供最佳的臨床照護 減少不必要的支出

有多少醫師在醫學院唸書的時候有聽過PET、 EBCT、脈衝光以及各式各樣新的診療方式? 您是如何去學習、評估、應用新的醫療科技?

評讀文獻常犯的錯誤 隨便找一篇文章 n 花很多時間 但找到品質不是很好的文章 n 先看結果, 再看討論, 對於研究背景和方法 卻不詳讀 n 看完文章對照顧病人並沒有幫助 n

有人說 現代醫學本來就是以實證為基礎的; 我們現在要談的實證醫學教學 和一般教科書 上談的知識 有什麼不一樣?

Constantly questioning attitude Lifelong learning Change learners’ behavior (literature searching, reading, practicing) Better patient care and outcomes

有什麼系統性的方式 能讓學生容易養成 終生學習、獨立思考的習慣和技巧?

實證醫學的五大步驟 ü Step 1: 如何明確的分析我們所面臨的臨床問 題? ü Step 2: 證據在哪裡? 如何有效率的搜尋文獻 ü Step 3: 臨床研究的結果可信嗎? ü Step 4: 其臨床意義為何? ü Step 5: 我該如何利用臨床研究的結果照顧我 的病人?

教授實證醫學時 需要特別提醒大家的… 初步的研究報告結果仍需要進一步的驗證 n 目前沒有充分證據支持的治療並非一定無 效 n 參考國外臨床研究的結果 應用於國內病患 的照顧 需要考慮人種、環境、醫療制度等 種種之間的差異 n 除了強調實證外 在診治療病患時 仍應尊重 病患的選擇 (preference) n

如何明確的分析 臨床問題 台大內科 張家勳 MD, MSc in clinical epidemiology

實證醫學的五大步驟 n n n Step 1: 如何明確的分析我們所面臨的臨床問題? Step 2: 證據在哪裡? 如何有效率的搜尋文獻 Step 3: 臨床研究的結果可信嗎? Step 4: 其臨床意義為何? Step 5: 我該如何利用臨床研究的結果照顧個別病人?

Ask Answerable Clinical Questions 請判問題是屬於: 一、治療 的療效、安全性、可行性 二、診斷 具的準確性 三、疾病表現 與鑑別診斷 四、預後 (即自然病史; 如: 這個病真的需要開刀嗎? 不開 刀會怎樣? ) 五、效益 cost-effectiveness問題… 按 Patients Intervention Comparison Outcome 做更明 確的描述 (Answerable clinical questions) *請注意什麼是目前的照護標準 Standard of care

Clinical scenario (I) n 林先生, a 60 y/o cook, visited ER due to increased productive cough and dyspnea for 3 days n n n COPD diagnosed for 3 years; FEV 1 65% predicted; never been hospitalized Smoking: 1 PPD for 30 yrs, quitted for 1+ year Rx: Atrovent 2 puff bid, Mucosolvon 1# tid. PE : 160/90 mm. Hg, 36. 8℃, 110, 24; diffuse wheezing WBC 9800, Cx. R: no definite pneumonic patch Symptoms not responded to Bricanyl IH q 30 min X 2…

How to ask a meaningful question? “學長, 這個病人要不要用類固醇? ” “老師, 我們要不要開類固醇給這個病人? ”

The specific, answerable clinical question: n n Patients Intervention vs. Comparison Outcomes

用什麼治療, 比較什麼治療… In COPD patients with acute exacerbation and… n n n moderate airflow obstruction quit smoking never been treated by steroids no evidence of pneumonia … Systemic steroids, as compared with placebo…

有什麼好處? Be able to: n n Relieve symptoms Improve lung function / air flow obstruction (FEV 1 or PEFR) Reduce treatment failure (death, intubations, readmission, or intensification of drug therapy) Shorten length of hospital stay?

療效是不是大於副作用? Be able to: Relieve symptoms n Improve lung function / air flow obstruction (FEV 1 or PEFR) n Reduce treatment failure (death, intubations, readmission, or intensification of drug therapy) n Shorten length of hospital stay? n Not ↑risk of infection, hyperglycemia, or GI bleeding?

Clinical scenario (II) n 王太太‚ 70歲‚ 有慢性關節炎的病史‚ 長期服用 NSAID。這次因吐咖啡渣、解黑糞前來急診‚ 經內 視鏡檢查為胃潰瘍合併出血‚ 並住院接受治療。 三 天後發生咳嗽、發燒、氣促等症狀… n n WBC: 14000/mm 3 Cx. R: ↑ infiltrate over bilateral lower lung Sputum Gram stain: G(+) cocci with phagocytosis Sputum Acid-fast stain: few acid-fast bacilli ? ?

How to ask a meaningful question? “學長, 我們是不是直接就要開始讓病人接受 抗結合藥物的治療, 還是先安排她做痰液的 TB-PCR檢查? ”

The specific, answerable clinical question: Patients n Intervention vs. n Comparison n Outcomes n

The specific, answerable clinical question: 在懷疑肺結核的患者 n n n 成人 尚未接受治療 HIV 陰性 PPD test 陽性 … 痰液檢體的 Nucleic acid amplification / TB-PCR test n n n Mycobacterium tuberculosis Direct (MTD) test AMPLICOR In-house

The specific, answerable clinical question: 與下列常用的檢查相較 n n n 臨床診斷 (clinical symptoms + risk factors + Cx. R) 痰液 acid-fast bacilli AFB stain 痰液 TB culture 在下列各方面 孰優孰劣? n n 準確度 (accuracy; i. e. , sensitivity and specificity) 安全性 所需時間 花費

國際間常用的實證醫學評估報告資料庫 Cochrane database of systematic review n Guideline clearinghouse: www. guideline. gov n 美國 AHRQ website: www. ahcpr. gov n 英國 NICE website: www. nice. org. uk n 加拿大 CCOHTA website: www. ccohta. ca n 蘇格蘭 SIGN website: www. sign. ac. uk n n 紐西蘭 NZGG website: www. nzgg. org. nz

案例一 71歲女性,有慢性支氣管性炎、心房纖維顫動、慢 性退化性關節炎等疾病,曾分別於民國88至 90 年間接受兩次超音波跟骨骨質密度測定檢查, 檢查結果分別呈示T-score<-3. 6及<-3. 7,經 診斷為骨質疏鬆症第四度,故接受Calcium Citrate 950 mg 1# BID 的治療。 審查專家認為病人接受骨密度檢查之方式和部位並 不適宜

The specific, answerable clinical question: n n Patients: 停經後的婦女 Intervention: 以超音波測量跟骨所得的骨密度 Comparison: 以DXA測量脊椎或髖骨的骨密度 Outcomes: 準確預測未來骨折的發生 花費 方便性 …

案例二 病患為 24歲女性,因頭痛、嘔吐至急診就醫,就診 時意識及理學檢查均正常 但於藥物治療後頭痛、 嘔吐症狀並無緩解,醫師懷疑有蜘蛛膜下腔出血, 安排頭部CT(無顯影劑),其檢查報告為:腦皮質 髓質接合處變不清晰、腦室變小、皮質溝閉塞, 顯示有腦腫脹;疑為不明原因之腦水腫,可能為 假性腦瘤或創傷導致。 健保局認為該醫師未進行詳細神經學檢查,且在此 案例中CT為非必要之檢查。

The specific, answerable clinical question: n n 蜘蛛膜下腔出血的患者中,有多少百分比在一開 始 的理學/神經學檢查 均為正常? 在頭痛急性發作 雖經藥物治療後症狀並未緩解的 患者中,罹患蜘蛛膜下腔出血的可能性有多高?

案例三 50歲女性,因持續有胃酸逆流、心灼熱之症狀, 經診斷為逆流性食道炎,胃鏡檢查結果為糜爛 性食道炎,grade B,醫師依氫離子幫浦阻斷劑 (PPI) 相關藥品給付規定向健保局提出事前審查 申請。 審查醫師認定為「非治療必需」,而應考慮手術 治療,故不予同意使用。

The specific, answerable clinical question: n n Patients: 罹患中等程度逆流性食道炎的患者 在接 受急性期 (6 -8週) PPI 治療後 Intervention: 降低逆流的手術 Comparison: 長期PPI維持療法 Outcomes: 患者症狀、生活品質 食道炎復發率 併發症 (食道狹窄、食道癌) 醫療成本 …

案例四 n n 63歲女性,有糖尿病、高血壓、肝硬化等病史,於住院檢 查時發現肝右葉有一顆肝細胞癌,進而分別接受二次無線 頻率電熱消除療法(radiofrequency ablation, RFA) (目前 支付標準無此項申報項目)。 申請人以「肝腫瘤內酒精注射PEIT」申報費用,初核時以 「與事實不符」為由不予給付,申請人以「病人接受RFA 若以一般PEIT計價才作 2次,比一般PEIT作 4 -6次更便宜. . 」申複,又以「PEIT之治療乃以針穿刺打藥,而與RFA雷 同,在其他各科給付項目亦有健保項目不周全而以類似項 目取代者,且病人追蹤後腫瘤縮小,可見其效果。」為由, 向本會提起爭議審議。

The specific, answerable clinical question: n n Patients: 肝硬化合併小型肝癌 但無法開刀的患者 Intervention: 電燒法 Comparison: 酒精注射 Outcomes: 患者存活率 反應率 併發症, 包括腹痛、發燒等不適 住院天數 經濟效益…

案例五 67歲男性,有定向感及記憶力差等症狀,診 斷為Alzheimer’s disease,以 Aricept 1#QD 治療,使用六個月後評估CDR為 1級, MMSE為 11分,故以 Aricept 繼續治療,因 之後評估CDR降為 2級,故醫師以 Aricept 治 療效果不佳為由,擬改以另一藥物 Exelone 治療。 n 健保局以同類型藥物,非治療所需,不予 同意。 n

案例六 31歲女性,因反復下腹疼痛及經痛就診,經口服藥物治療無 效,近日因症狀加劇,疑似子宮內膜異位症,安排住院而 接受腹腔鏡手術治療。經腹腔鏡檢查,發現子宮有瘤狀突 起 (1 cm)及多囊性卵巢,認為其為引起疼痛及排卵功能不足 之原因,故以腹腔鏡取掉兩處腫瘤。其病理組織切片檢查 報告顯示為 adenomyosis 與 endometriosis。醫師認為前者的 腫瘤較難拿掉,所花的時間比切除肌瘤的時間更多,故以 myomectomy 同等給付應屬合理。 審查醫師認為病患僅有腹部疼痛,且病理報告不符子宮肌瘤 切除術論病例計酬案件之要件,改以子宮肌瘤切除術一般 案件給付(健保尚無腹腔鏡子宮肌瘤切除術之支付標準)。

案例七 林先生, 30歲銀行行員, 這次來門診的主述為三 週來不典型胸痛、心悸、以及有一次近乎暈 厥 急診部醫師臆斷: 過度換氣症候群 n Holter ECG: sinus tachycardia n 心臟超音波檢查: 二尖瓣脫垂合併輕度逆流 n “我會不會有立即的生命危險呢? ”

其它常用的網路資源 n n n Clinical Evidence: www. clinicalevidence. com Bandolier: www. ebandolier. com 專科醫學會網站 n AHA: www. americanheart. org n AASLD: www. aasld. org n ACG: www. acg. gi. org n ACCP: www. chestnet. org n K/DOQI: www. kidney. org n AAN: www. aan. com

How Should I Use Articles about Therapy / Prevention? Examples for evidence-based practice 台大內科 張家勳 / 楊泮池教授

How to ask a meaningful question? “給寶寶喝LGG優酪乳對身體有沒有好處? ”

The specific, answerable clinical question: n n Patients Intervention vs. Comparison Outcomes

什麼樣的人… 小朋友 開發中國家營養不良的小朋友 上托兒所的小朋友 生病住院的小朋友 健康的小朋友 成人 健康人 旅行的人 使用抗生素的人 …

用什麼治療, 比較什麼治療… Intervention: “益生菌” (Probiotics) “乳酸菌” (Lactobacilli) “LGG” (Lactobacillus rhamnosus strain GG) Comparison: 不飲用 Placebo L. acidophillus Bifidobacterium bifidum

有什麼好處? 預防… n n n 感染性腹瀉 (細菌引起的, 病毒引起的…) 使用抗生素引起的腹瀉 (特別是 Clostridium difficile 所引起的) 呼吸道感染, 泌尿道感染, 其它方面的感染… 治療腹瀉: n n n 減輕腹瀉嚴重度 減少腹瀉次數 縮短腹瀉天數…

該如何證明 LGG 的療效呢? 小明五歲前體弱多病, 自從飲用 LGG 牛奶 以後, 就很少感冒了… n 隔壁阿媽給他的孫子喝 LGG 牛奶, 比我家 阿明的抵抗力好得多… n

該如何證明 LGG 的療效呢? 根據某家醫學中心的研究 LGG 可改善腸道 內生態平衡, 使壞菌不容易滋長, 同時並增 加人體腸道製造抗體的能力… n 某觀察性研究顯示: 服用LGG優酪乳越多的 人, 發生腸胃道、泌尿道、以及呼吸道感染 的情況越少… n

Users’ Guides to the Medical Literature Using Electronic Health Information resources n n n Clinical Evidence: www. clinicalevidence. com ACP Journal Club Cochrane Library n Cochrane Database of Systematic Reviews Bandolier: www. ebandolier. com www. guideline. gov National guideline clearinghouse: JAMA 2000; 283: 1875 -9

MEDLINE Search: Hierarchy and Methodological Filter n Meta-analysis / Systematic review: Meta-analysis in publication type (use LIMIT) n Systematic review (search field: Textword) n n Randomized Controlled Trial in publication type n Controlled Clinical Trial in publication type http: //cebm. jr 2. ox. ac. uk/docs/searching. html

健康的小朋友長期飲用LGG牛乳 能將 感染性腹瀉的危險性降低多少? 將問題分解為數個層面 (並不是全部都需要用於搜尋) 病人族群 健康的小朋友 介入方法 LGG 結果 感染性腹瀉 研究設計 系統性文獻回顧 或 隨機對照試驗 找出每個層面的同義字、變異的拼法、及subject headings: 以 LGG 為例, 可考慮下列字彙: LGG, Lactobacillus, Lactobacilli, Probiotics

What we have now… n n Lactobacillus GG reduced diarrhea incidence in children treated with antibiotics - ACP J club 2000; 133(1): 24; J Pediatr. 1999; 135: 564 -8 Lactobacillus therapy for acute infectious diarrhea in children: A metaanalysis - Pediatrics 2002; 109: 678 -84 Probiotics in prevention of antibiotic associated diarrhea: meta-analysis - BMJ 2002; 324: 1 -6 Probiotics in the treatment and prevention of acute infectious diarrhea in infants and children: a systematic review - Cochrane database of systematic reviews, Issue 3, 2002

Effect of Long Term Consumption of Probiotic Milk on Infections in Children n n Design: Randomized, double blind, placebo-controlled trial lasted 7 months over the winter Setting: 18 day care centers in similar socioeconomic areas in Helsinki, Finland Patients: 571 healthy children aged 1 -6 years Excluded children with n n allergy to cow’s milk lactose intolerance severe food allergy, and other severe chronic disease BMJ 2001; 322: 1 -5

Effect of Long Term Consumption of Probiotic Milk on Infections in Children n Intervention: The Lactobacillus milk (1% fat, 5 -10 x 105 cfu /ml of LGG) The control milk (same component but without LGG) The aim was a daily consumption of 200 ml; other products containing probiotic bacteria were forbidden Main outcome: n n # of days with respiratory and GI symptoms (from symptom diary recorded by parents) Absences from day care center due to illness # of children with URI with otitis media, sinusitis, acute bronchitis, pneumonia as diagnosed by a doctor Antibiotic treatments during the seven month intervention

Are the results of the study valid (I)? Was the assignment of patients to treatments randomized? n Was the randomization list concealed? n Were the groups similar at the start of the trial? n JAMA 1993; 270(21): 2598 -2601
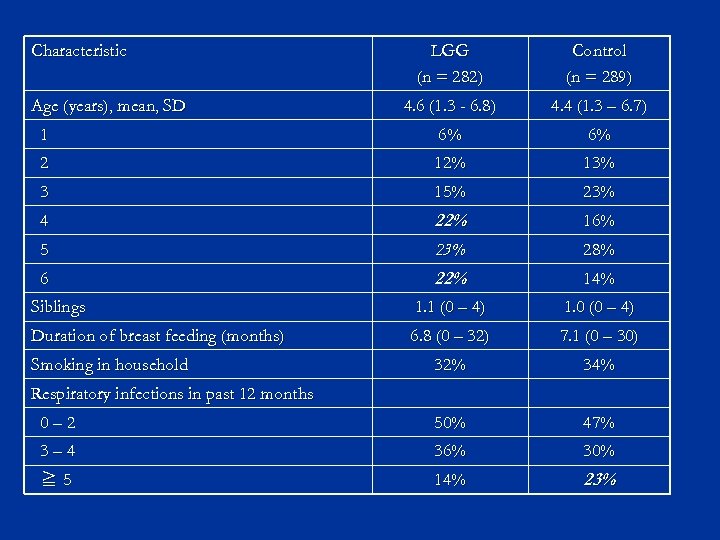
Characteristic LGG (n = 282) Control (n = 289) 4. 6 (1. 3 - 6. 8) 4. 4 (1. 3 – 6. 7) 1 6% 6% 2 12% 13% 3 15% 23% 4 22% 16% 5 23% 28% 6 22% 14% Siblings 1. 1 (0 – 4) 1. 0 (0 – 4) Duration of breast feeding (months) 6. 8 (0 – 32) 7. 1 (0 – 30) 32% 34% 0– 2 50% 47% 3– 4 36% 30% ≧ 5 14% 23% Age (years), mean, SD Smoking in household Respiratory infections in past 12 months

Are the results of the study valid (II)? n n Were patients, health workers, and study personnel “blind” to treatment? Aside from the experimental intervention, were the groups treated equally? Was follow-up complete? Were patients analyzed in the groups to which they were randomized (intention-to-treat analysis)? JAMA 1993; 270(21): 2598 -2601

另一篇主題類似的研究有什麼弱點? n 某家醫院將 100 位年齡 0. 5~5 歲腹瀉小於 5 天的小 朋友, 隨機分配至治療組(AB菌)及對照組(靜脈注 射補充水分), 觀察益生菌的療效, 由護士小姐觀察 小朋友之後腹瀉時間的長短 (定義為至最後一次水 瀉出現的時間), 以 Student’s t test 及 2 test 作分析 統計, 發現治療組的小朋友在入院後第一天及第二 天的腹瀉次數有顯著的減少, 在整個腹瀉時間上也 有明顯的減少 (3. 1 vs. 3. 6 days, p < 0. 01)… Acta Paediatr Tw 2001; 42: 301 -5
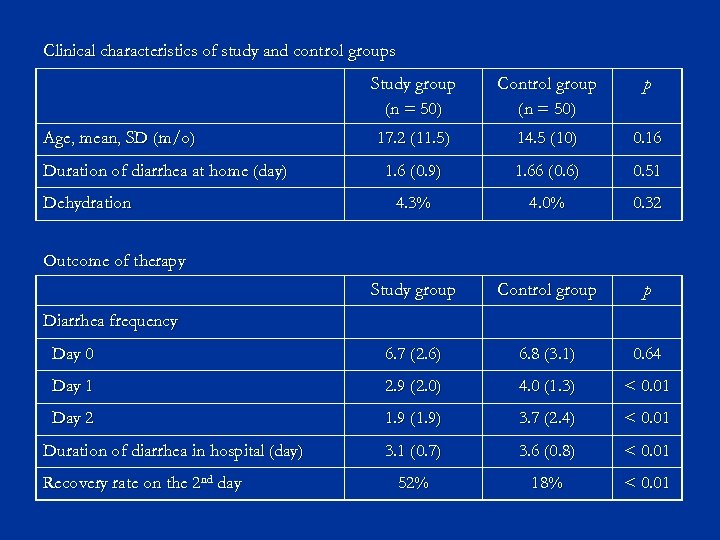
Clinical characteristics of study and control groups Study group (n = 50) Control group (n = 50) p 17. 2 (11. 5) 14. 5 (10) 0. 16 1. 6 (0. 9) 1. 66 (0. 6) 0. 51 4. 3% 4. 0% 0. 32 Study group Control group p Day 0 6. 7 (2. 6) 6. 8 (3. 1) 0. 64 Day 1 2. 9 (2. 0) 4. 0 (1. 3) < 0. 01 Day 2 1. 9 (1. 9) 3. 7 (2. 4) < 0. 01 3. 1 (0. 7) 3. 6 (0. 8) < 0. 01 52% 18% < 0. 01 Age, mean, SD (m/o) Duration of diarrhea at home (day) Dehydration Outcome of therapy Diarrhea frequency Duration of diarrhea in hospital (day) Recovery rate on the 2 nd day
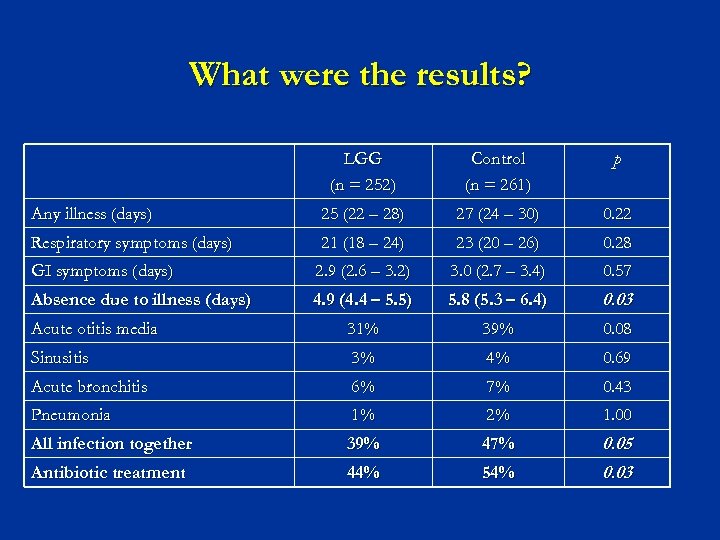
What were the results? LGG (n = 252) Control (n = 261) p Any illness (days) 25 (22 – 28) 27 (24 – 30) 0. 22 Respiratory symptoms (days) 21 (18 – 24) 23 (20 – 26) 0. 28 GI symptoms (days) 2. 9 (2. 6 – 3. 2) 3. 0 (2. 7 – 3. 4) 0. 57 Absence due to illness (days) 4. 9 (4. 4 – 5. 5) 5. 8 (5. 3 – 6. 4) 0. 03 Acute otitis media 31% 39% 0. 08 Sinusitis 3% 4% 0. 69 Acute bronchitis 6% 7% 0. 43 Pneumonia 1% 2% 1. 00 All infection together 39% 47% Antibiotic treatment 44% 54% 0. 05 0. 03
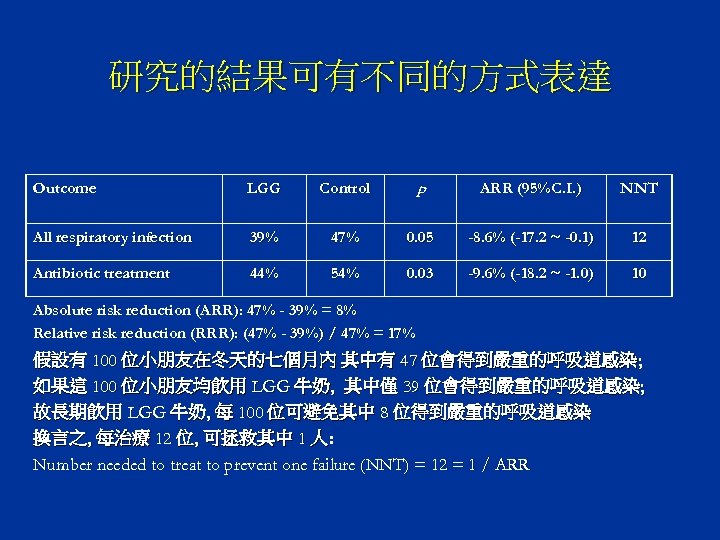
研究的結果可有不同的方式表達 Outcome LGG Control p ARR (95%C. I. ) NNT All respiratory infection 39% 47% 0. 05 -8. 6% (-17. 2 ~ -0. 1) 12 Antibiotic treatment 44% 54% 0. 03 -9. 6% (-18. 2 ~ -1. 0) 10 Absolute risk reduction (ARR): 47% - 39% = 8% Relative risk reduction (RRR): (47% - 39%) / 47% = 17% 假設有 100 位小朋友在冬天的七個月內 其中有 47 位會得到嚴重的呼吸道感染; 如果這 100 位小朋友均飲用 LGG 牛奶, 其中僅 39 位會得到嚴重的呼吸道感染; 故長期飲用 LGG 牛奶, 每 100 位可避免其中 8 位得到嚴重的呼吸道感染 換言之, 每治療 12 位, 可拯救其中 1 人: Number needed to treat to prevent one failure (NNT) = 12 = 1 / ARR
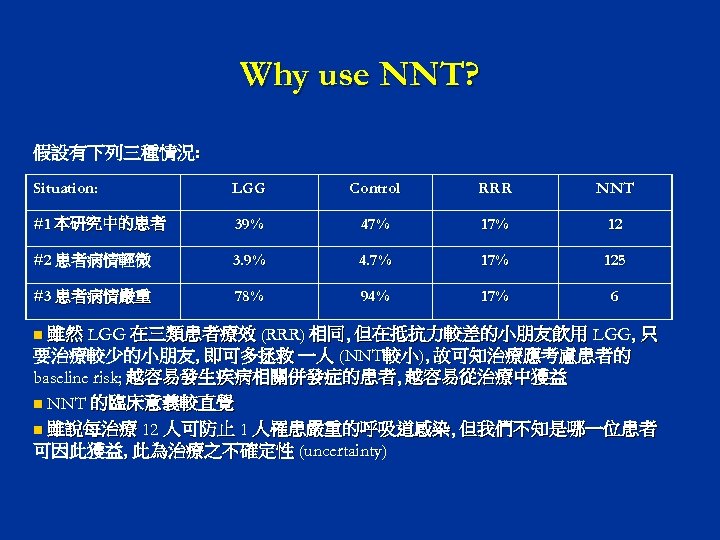
Why use NNT? 假設有下列三種情況: Situation: LGG Control RRR NNT #1 本研究中的患者 39% 47% 12 #2 患者病情輕微 3. 9% 4. 7% 125 #3 患者病情嚴重 78% 94% 17% 6 雖然 LGG 在三類患者療效 (RRR) 相同, 但在抵抗力較差的小朋友飲用 LGG, 只 要治療較少的小朋友, 即可多拯救 一人 (NNT較小), 故可知治療應考慮患者的 baseline risk; 越容易發生疾病相關併發症的患者, 越容易從治療中獲益 n NNT 的臨床意義較直覺 n 雖說每治療 12 人可防止 1 人罹患嚴重的呼吸道感染, 但我們不知是哪一位患者 可因此獲益, 此為治療之不確定性 (uncertainty) n

一篇研究的結果是不是就可以確定治療一定有效? 系統性文獻回顧和傳統的文獻回顧有什麼不同?

其他有關益生菌是否能預防 小兒腹瀉的研究結果如何? Trial Year Saavedra 1994 Szajewska 2001 Oberhelman 1999 Location Age range (month) Probiotic Type of diarrhea IRR USA: longterm care facility 5 – 24 B. Bifidum Nosocomial 0. 23 (0. 02– 1. 18) Poland: pediatric hospital 1 – 36 LGG Nosocomial 0. 17 Peru: urban town 1 – 30 (0. 03 -0. 65) LGG Community acquired 0. 97 (0. 85 -1. 10)
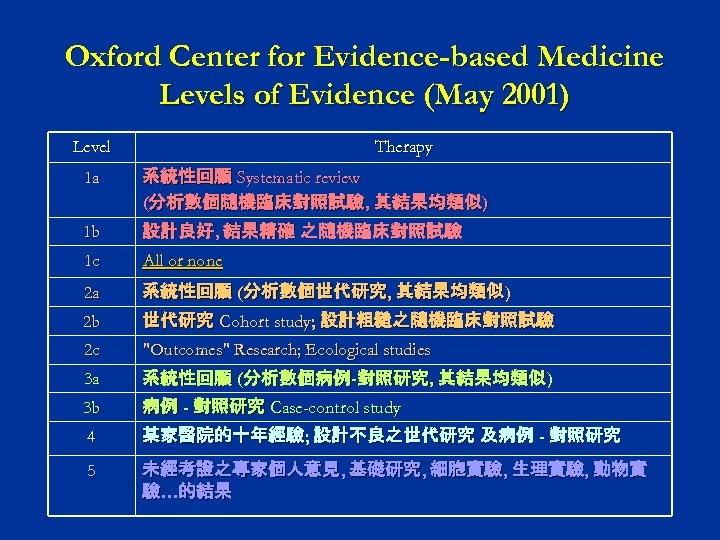

Oxford Center for Evidence-based Medicine Levels of Evidence (May 2001) Level Therapy 1 a 系統性回顧 Systematic review (分析數個隨機臨床對照試驗, 其結果均類似) 1 b 設計良好, 結果精確 之隨機臨床對照試驗 1 c All or none 2 a 系統性回顧 (分析數個世代研究, 其結果均類似) 2 b 世代研究 Cohort study; 設計粗糙之隨機臨床對照試驗 2 c "Outcomes" Research; Ecological studies 3 a 系統性回顧 (分析數個病例-對照研究, 其結果均類似) 3 b 病例 - 對照研究 Case-control study 4 某家醫院的十年經驗; 設計不良之世代研究 及病例 - 對照研究 5 未經考證之專家個人意見, 基礎研究, 細胞實驗, 生理實驗, 動物實 驗…的結果

How Should I Use Articles about Diagnosis? Examples for evidence-based practice 台大內科 張家勳 / 楊泮池教授

Physicians have always had their favorite strategies for the diagnostic management of most problems. But as new tests become available, strategies have changed, are changing, and will continue to change… Paul Cutler MD.

Clinical scenario n 王太太‚ 70歲‚ 有慢性關節炎的病史‚ 長期服用 NSAID。這次因吐咖啡渣、解黑糞前來急診‚ 經內 視鏡檢查為胃潰瘍合併出血‚ 並住院接受治療。 三 天後發生咳嗽、發燒、氣促等症狀… n n WBC: 14000/mm 3 Cx. R: ↑ infiltrate over bilateral lower lung Sputum Gram stain: G(+) cocci with phagocytosis Sputum Acid-fast stain: few acid-fast bacilli ? ?

臨床診斷常犯的錯誤 以為檢查結果為陽性就能 100%的確定患者 有病 n 忽視了患者罹患該疾病的基本可能性 (prior probability) n 不了解診斷 具本身的特性 (敏感度、特異 度) n 重複地選擇不會影響患者處置的檢查 n

What we will learn today… n n n Step 1: 如何明確的分析我們所面臨的臨床問題? Step 2: 證據在哪裡? 如何有效率的搜尋文獻 Step 3: 臨床研究的結果可信嗎? Step 4: 其臨床意義為何? Step 5: 我該如何利用臨床研究的結果照顧我的病人?

How to ask a meaningful question? “學長, 我們是不是直接就要開始讓病人接受 抗結合藥物的治療, 還是先安排她做痰液的 TB-PCR檢查? ”

Step 1: 如何明確的分析我們所面臨的臨床問題?

The specific, answerable clinical question: Patients n Intervention vs. n Comparison n Outcomes n

Step 2: 證據在哪裡? 如何有效率的搜尋文獻

The role of clinical suspicion in evaluating a new diagnostic test for active tuberculosis n n n Design: Prospective cohort study Setting: 6 medical centers and 1 public health TB clinic between Feb and Dec 1996. Participants: n n n 425 patients suspected of having active pulmonary TB based on symptoms, risk factors, PPT test, Cx. R findings. Identified by chest or ID specialist. Not eligible if they received multi-drug treatment for TB for ≧ 7 days during the past 3 months. JAMA 2000; 283: 639 -45

The role of clinical suspicion in evaluating a new diagnostic test for active tuberculosis n n n Description of test: Enhanced MTD. Site physician estimated the probability (0%~100%) that the patient had TB, based on clinical judgment; physicians were blinded to the results of E-MTD. All other lab results (might include AFB smears) were available. Reference standard: n n n Definite active TB: high clinical suspicion (>80%) and ≧ 2 positive cultures Definite absence of active TB: low clinical suspicion (<10%) without any positive culture Otherwise, the cases were reviewed by the independent expert panel: at least 2 of the 3 members had to consider the patient to have or to be free of TB JAMA 2000; 283: 639 -45

Step 3: 這篇臨床研究的結果可信嗎?

Are the results of the study valid? n n Did the patient sample include an appropriate spectrum of patients? Was there an independent, blind comparison with a reference standard? Did the results of the test influence the decision to perform the reference standard? Were the methods for performing the test described in sufficient detail to permit replication? JAMA 1994; 271: 389 -91

試比較不同研究患者納入方式 對研究可信度的影響 Almeda J et al. 收集238位肺結核患者檢體, 與46位健 康醫學院學生及47位未感染肺結核COPD患者所 收集到的檢體相比較, 發現: TB-PCR在診斷肺結核 的敏感度為 62%, 特異度為 100%… Eur J Clin Microbiol Infect Dis 2000; 19: 859 -867

What is “Spectrum of Patients”? The range of features found in patients used to challenge a test’s sensitivity and specificity to distinguish people with or without disease For both diseased and comparative groups, consider… n Pathologic spectrum n Clinical spectrum n Co-morbid spectrum N Engl J Med 1978; 299: 926 -930

試比較不同研究黃金標準的選擇 對研究可信度的影響 在一項前瞻性研究中, Bodmer T et al. 收集了621個懷 疑罹患肺結核患者的呼吸道檢體, 以結合菌培養當 作診斷的黃金標準, 發現TB-PCR的敏感度 74%, 特 異度為 99%… J Clin Microbiol 1994; 32: 1483 -1487

Bias in Associating the Test Results and the Disease n Diagnostic-review bias The test result affects the subjective review of the data that establish the diagnosis n Values of Doppler ultrasound in diagnosis of clinically suspected deep vein thrombosis. BMJ 1975; 4: 552 -4 n Test-review bias A test that is interpreted subjectively can be biased by the knowledge of the diagnosis n Value of infarct-specific isotope (99 m Tc-labeled stannous pyrophosphate) in myocardial scanning. BMJ 1975; 3: 517 -20.

Bias in Associating the Test Results and the Disease n Incorporation bias The test result is actually incorporated into the evidence to diagnose the disease n A test for patency of the cystic duct in acute cholecystitis Ann Intern Med 1975; 82: 13 -17 n Work-up bias The result of the test may affect the subsequent clinical work-up needed to establish the diagnosis…
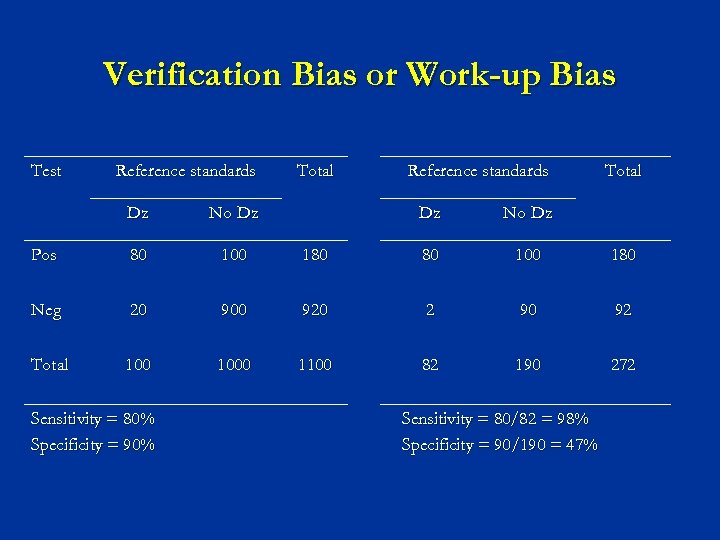
Verification Bias or Work-up Bias Test Reference standards Dz No Dz Pos 80 100 Neg 20 Total 100 Total Sensitivity = 80% Specificity = 90% Reference standards Total Dz No Dz 180 80 100 180 900 920 2 90 92 1000 1100 82 190 272 Sensitivity = 80/82 = 98% Specificity = 90/190 = 47%

Oxford Center for EBM Levels of Evidence Level Diagnosis 1 a SR (with homogeneity) of Level I diagnostic studies 1 b Validating cohort study with good reference standards 1 c Absolute Sp. Pins and Sn. Nouts 2 a SR (with homogeneity) of Level II diagnostic studies 2 b Exploratory cohort study with good reference standards 3 a SR (with homogeneity) of 3 b and better studies 3 b Non-consecutive study; or without consistently applied reference standards 4 Case-control studies, poor or non-independent reference standard 5 Expert opinion without explicit critical appraisal, or based on physiology, bench research or "first principles"

Step 4: 其臨床意義為何?

What are the results? n Are likelihood ratios for the test results presented or data necessary for their calculation provided? JAMA 1994; 271: 703 -707

Predictive values have more explicit clinical meanings… For a test with sensitivity = 80% and specificity = 90% Disease No disease Positive 80 10 90 Negative 20 90 110 Total 100 Positive predictive value = 80/90 = 89% Negative predictive value=90/110 = 82%

But will change while prevalence changes For a test with sensitivity = 80% and specificity = 90% Disease No disease Positive 80 100 180 Negative 20 900 920 Total 1000 Positive predictive value = 80/180 = 44%↓ Negative predict value = 900/920 = 98% ↑

A single cut-off value to indicate abnormality is NOT enough!! Iron deficiency anemia (IDA) No IDA Ferritin < 30 a c Ferritin≧ 30 b d Sensitivity = a / a + b Specificity = d/ c + d

A single cut-off value to indicate abnormality is NOT enough!! Serum ferritin (mg/dl) ≦ 15 Specificity ? Sensitivity ? 15 -24 25 -34 ? ? 35 -44 45 -100 ? ? ≧ 100 ? ?

LR: a richer way to interpret the tests with multiple levels of positive Serum ferritin (mg/dl) ≦ 15 LR 51. 8 15 -24 25 -34 8. 8 2. 5 35 -44 45 -100 1. 8 0. 5 ≧ 100 0. 08

Why use likelihood ratio (LR)? Clinical value Meaning Stability with changing prevalence Can use multiple levels of a test result Sensitivity Specificity No Yes No Predictive value Yes No No Test

Why use likelihood ratio (LR)? Clinical value Meaning Stability with changing prevalence Can use multiple levels of a test result Sensitivity Specificity No Yes No Predictive value Yes No No Likelihood ratio Yes Yes Test

How to calculate and use positive and negative likelihood ratio? LR = probability that finding is present in patients with disease probability that finding is present in patients without disease Post-test odds = pre-test odds x LR Positive LR (LR+) = sensitivity / (1 -specificity) Negative LR (LR-) = (1 -sensitivity) / specificity 註 Odds = p / 1 -p; probability = odds / 1+odds 例如: 和信鯨贏球的機率為 80%, 則鯨隊贏球的勝算為 4: 1=4

診斷的過程是一連串機率的改變… 一位68歲女性, 在最近一週來發生咳嗽有痰的 情形, 您認為她罹患肺結核的可能性有多高?

診斷的過程是一連串機率的改變… 95% 100% 0% 以往有肺結核的病史 咳痰僅一週 午間發燒 夜間盜汗 體重沒有減輕 胸部X光顯示: 右上葉肺炎浸潤 痰液AFB smear顯示 AFB(+) P 5 x LR 5 = P 6
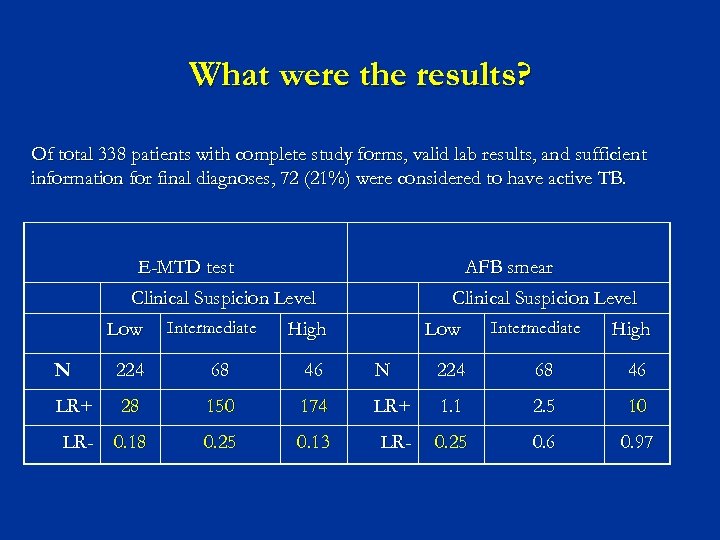
What were the results? Of total 338 patients with complete study forms, valid lab results, and sufficient information for final diagnoses, 72 (21%) were considered to have active TB. E-MTD test AFB smear Clinical Suspicion Level Low Intermediate Clinical Suspicion Level High Low Intermediate High N 224 68 46 LR+ 28 150 174 LR+ 1. 1 2. 5 10 LR- 0. 18 0. 25 0. 13 LR- 0. 25 0. 6 0. 97

How to Interpret a likelihood ratio: Likelihood ratio > 10 5 – 10 2– 5 Interpretation Strong evidence to rule in disease Moderate evidence to rule in disease Weak evidence to rule in disease 0. 5 – 2. 0 0. 2 – 0. 5 No significant change in the likelihood Weak evidence to rule out disease 0. 1 – 0. 2 < 0. 1 Moderate evidence to rule out disease Strong evidence to rule out disease
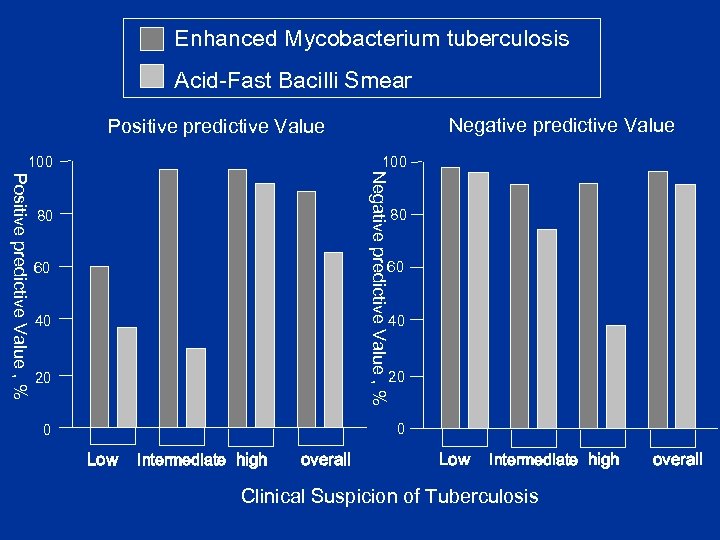
Enhanced Mycobacterium tuberculosis Acid-Fast Bacilli Smear Negative predictive Value Positive predictive Value 100 Positive predictive Value , % Negative predictive Value , % 100 80 80 60 60 40 40 20 20 0 0 Low Intermediate high overall Low Intermediate high Clinical Suspicion of Tuberculosis overall

Other important results in this study n n n For the low clinical suspicion group, both tests were useful for ruling out disease; Neither proved convincing evidence for ruling in disease. For high suspicion group, both tests were useful for ruling in disease; However, the PV- of AFB smear was only 37%, compared with 91% for the E-MTD offers greatest utility in the intermediate suspicion group: n The TB and non-TB cases were equally likely to have a positive AFB smear n The prevalence of the suggestive Cx. R, cough and weight loss were also similar n Mycobacteria other than TB were cultured more commonly

Step 5: 我該如何利用臨床研究的結果照顧我 的病人?

Will the results help me in caring for my patients? n Will the reproducibility of the test result and its interpretation be satisfactory in my setting? Poor reproducibility are due to Problems of the test itself Ex. RIA kits for hormone levels n Expertise is required in performing or interpreting the test Ex. Cardiac echo, abdominal sono, V/Q scan. n

Are the results applicable to my patients? n Test properties may change in different sub-populations n Practice in a similar setting Meet all the inclusion criteria Not violate any of the exclusion criteria n n n Are there compelling reasons that the results should not be applied? n n n Severity of diseases Mix of compelling conditions The issue of generalizability may be resolved if you can find an overview that pools the results of a number of studies

Will patients be better as a result of the test? n The usefulness of a diagnostic test depends on n Whether it adds information beyond that otherwise available Whether this information leads to a change in management that is ultimately beneficial In some situation, tests may be accurate, management may even change, but their impact on patient outcome may be far less certain. Ex. Right heart catheterization for critically ill patients

試著思考下列問題: 參加研究,轉介納入病人的均為對診治肺結 核很有經驗的胸腔科或感染科醫師;將本 研究的結果應用在我們平常臨床照護上有 什麼該注意的呢?

Turning back to our patient… 由以上可知: 在臨床上懷疑罹患肺結核可能性 較低的族群中, 痰液AFB染色陽性者其罹患 肺結核的機率不到 40%; 這時有什麼辦法來 幫助我們提高肺結核的診斷率? ? 多重試驗 (平行試驗或序列試驗) 在此時有幫 助嗎? 若TB-PCR的結果為陰性(或陽性), 對我們的 處理有什麼影響?

Evidence is never enough… n 利用CSF TB-PCR檢查 快速診斷結核性腦膜炎 n n n J Clin Microbiol 1998; 36: 1251 - 1254 J Clin Microbiol 2000; 38: 3150 – 3155 利用TB-PCR檢查 診斷結核性肋膜炎及其他肺外結 核 n n Chest 1998; 113: 1190 - 1194 Chest 2001; 119: 1737 - 1741

How To Use Articles about Clinical Predication Rules Examples for evidence-based practicing 台大內科 張家勳 / 楊泮池教授 E-mail: chiahsuin@yahoo. com

Clinical scenario 林同學, 20歲男性, 這次來急診的主述為三天來持續發 燒, 同時合併咳嗽有黃痰和氣促 n n n 10 天前開始輕微發熱、喉嚨痛、及流鼻水 除過敏性鼻炎外 無其他重大疾病 否認在過去二週內曾出國旅遊 理學檢查: 130/85 mm. Hg, 38℃, 100, 20; no wheezing WBC 18000; Cx. R: pneumonic patch over R’t lower lung 要不要安排林同學住院呢?

實際上常面臨的情況 經驗有限… n 沒有一致地、完整地追蹤病人 n 過於強調特殊的案例 n 不容易了解個別特徵 (即預後因子) 與其他 特徵間的相互關係 n 難以評估個別因子 以及與其他因子相互作 用下 對病人預後的整體影響 n

What we will learn today… n n n Step 1: 如何明確的分析我們所面臨的臨床問題? Step 2: 證據在哪裡? 如何有效率的搜尋文獻 Step 3: 臨床研究的結果可信嗎? Step 4: 其臨床意義為何? Step 5: 我該如何利用臨床研究的結果照顧我的病人?

Step 1: 如何明確的分析我們所面臨的臨床問題?

The Specific, Answerable Clinical Question: n n Patients: 罹患社區性肺炎的病人 Intervention: WBC 高的患者 (eg, >15, 000) Comparison: WBC 不高的患者 Outcomes: 死亡率是否顯著高了許多…

The Specific, Answerable Clinical Question: n n Patients: 罹患社區性肺炎的病人 Intervention: Clinical prediction rule Comparison: 醫師的經驗或直覺 Outcomes: 準確預測住院期間發生 mortality & morbidity 減少不必要的住院 但是不會降低照護的品質 …

What Are Clinical Prediction or Clinical Decision Rules (CPR; CDR) n n n Tools that quantify the individual contributions that various components of history, physical examination, and basic lab results make toward the diagnosis, prognosis, or likely response to treatment in a patient Attempt to formally test, simplify, and increase the accuracy of clinicians’ diagnostic and prognostic assessments Most likely to be useful where decision making is complex, or there are opportunities to achieve cost savings without compromising patient care JAMA, 2000; 284: 79~84

Step 2: 證據在哪裡? 如何有效率的搜尋文獻

Three Steps for Putting CDR into Clinical Practice… Step 1. Derivation Identification of factors with predictive power Step 2. Validation Evidence of reproducible accuracy Broad Validation Narrow Validation Application of rule in Multiple clinical in a similar clinical settings with varying setting and prevalence and population as in Step 1 outcomes of disease Step 3. Impact Analysis Evidence that rule changes physician behavior and improves Patient Outcomes and/or reduces costs Level of Evidence 4 3 2 1

A Prediction Rule to Identify Low-Risk Patients with Community-Acquired pneumonia n Deriving the prediction rule 14, 199 adult inpatients with CAP from 78 hospitals in 23 states in the 1989 Medis. Group hospital database n Age≧ 18 years n Have a principal diagnosis of pneumonia by ICD-9 n Excluded patients with HIV, who had been hospitalized within 7 days before current admission or transferred from another hospital n Patients’ charts are abstracted to collect the mostabnormal key clinical findings on hospital day 1 or 2 n

A Prediction Rule to Identify Low-Risk Patients with Community-Acquired pneumonia n Deriving the prediction rule (Cont. ) n n n Developed the prediction rule with 30 -day hospital mortality as the outcome Step 1: Identify the lowest risk patients solely on history and physical findings Step 2: Quantifying the risk in the remaining patients with the same findings used in step 1 plus lab and Cx. R data N Engl J Med 1997; 336: 243 -50

A Prediction Rule to Identify Low-Risk Patients with Community-Acquired pneumonia n Validation of the prediction rule n n Validated with 1991 Pennsylvania Medis. Groups database on 38, 039 adult patients with CAP, and PORT prospective cohort study of outpatients and inpatients with CAP at 5 medical centers. ≧ 1 symptoms suggestive of pneumonia; have radiographic evidence with 24 hrs of presentation Recording the first values of information on vital signs and lab values Patients were followed prospectively to assess their vital status and a variety of outcomes 30 days after diagnosis, including subsequent hospitalization, admission to ICU, respiratory failure, and length of hospital stay.

Step 3: 這篇臨床研究的結果可信嗎?

Methodological standards for derivation of a clinical prediction rule n n ü ü Were all important predictors included in the derivation process? Were all important predictors present in a significant proportion of the study population? Were all the outcome events and predictors clearly defined? Were those assessing the outcome event blinded to the presence of the predictors and vice versa? Was the sample size adequate (including adequate number of outcome events? Does the rule make clinical sense? JAMA 2000; 284: 79 -84

Methodological standards for validation of a clinical prediction rule ü ü n n Were the patients chosen in an unbiased fashion and do they represent a wide spectrum of severity of disease? Was there 100% follow up of those enrolled? Was there a blinded assessment of the criterion standard for all patients? Was there an explicit and accurate interpretation of the predictor variables and the actual rule without knowledge of the outcome? JAMA 2000; 284: 79 -84

什麼是 “回歸分析” – Regression analysis “羅式回歸分析” – Logistic regression

Logit P = C +α 1(Age) +α 2 (Nursing home resident) +α 3(Neoplastic disease) + … +α 4 (RR≥ 30) +… Logit P = C + (Age) + β 2 (Nursing home resident) +β 3(Neoplastic disease) + … +β 4 (RR≥ 30) +… Score = Age + β 2 + β 3 + β 4 + … 將不具任何危險因子 且為最低死亡風險 (<0. 5%) 的 患者列為Class I;其餘病人按死亡率高低分成四組 (0. 5~0. 1%, 0. 1~4%, 4~10%, >10%) 將上述分數作 區分 (≤ 70, 71~90, 91~130, >130)
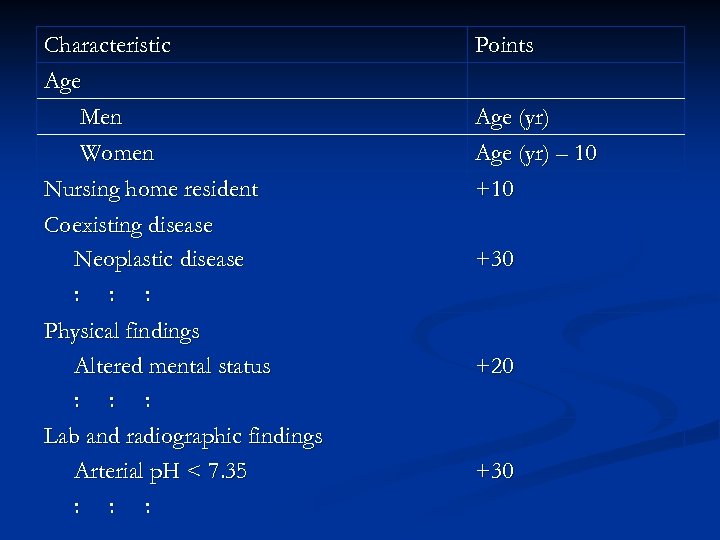
Characteristic Age Men Women Nursing home resident Coexisting disease Neoplastic disease : : : Physical findings Altered mental status : : : Lab and radiographic findings Arterial p. H < 7. 35 : : : Points Age (yr) – 10 +30 +20 +30

Step 4: 其臨床意義為何?

Comparison of Mortality in Derivation and Validation Cohorts Risk Class MEDIS Derivation MEDIS Validation PORT Inpatient PORT Outpatient I 0. 4% 0. 1% 0. 5% 0. 0% II 0. 7% 0. 6% 0. 9% 0. 4% III 2. 8% 1. 2% 0. 0% IV 8. 5% 8. 2% 9. 0% 12. 5% V 10. 2% 10. 6% 8. 0% 0. 6%

Other Important Findings in This Study n n n Of the 1575 PORT patients in the three lowest risk classes, only 7 died. Only 4 of these deaths were pneumonia-related, none of them were preventable. Also a significant relation between risk class and other medical outcomes (subsequent hospitalization, admitted to ICU, length of hospital stay). A strategy of outpatient care for class I and II, brief inpatient observation for class III, and traditional inpatient care for class IV & V, would have reduced the proportion of patients receiving traditional inpatient care by 31%; fewer than 1% died and 4. 3% were admitted to ICU.

A Controlled Trial of a Critical Pathway for Treatment of Community-Acquired Pneumonia n n 一項加拿大的研究將19家醫院隨機分派至傳統處置組及實行 critical pathway組 (包括利用肺炎嚴重指標決定患者是否須住 院、讓病人接受 levofloxacin 單一藥物治療、及有關何時換 成口服藥物和出院的臨床照護指引) 。 自 1998年 1月1日至 7 月31日總共有1743位因社區性肺炎而前往急診的患者參加研 究。 結果發現兩組在患者的死亡率、併發症、再住院率、及六 週後生活品質等品質指標相似, 但後者降低了低風險患者的 住院率, 同時縮短接受靜脈注射抗生素的天數及總住院天數, 減少了醫療資源的不當使用。 JAMA 2000; 283: 749 -55

Hierarchy of Evidence for Clinical Decision Rules Level 1: Rules that can be used in a wide variety of settings with confidence that they can change clinician behavior and improve patient outcomes At least 1 prospective validation in a different population and 1 impact analysis. Demonstrating change in clinician behavior with beneficial consequences Level 2: Rules that can be used in various settings with confidence in their accuracy Demonstrated accuracy in either 1 large prospective study including a broad spectrum of patients and clinicians or validated in several smaller settings that differ from one another Level 3: Rules that clinicians may consider using with caution and only if patients in the study are similar to those in the clinician’s clinical setting Validated in only 1 narrow prospective sample Level 4: Rules that need further evaluation before they can be applied clinically Derived but not validated or validated only in split samples. Large retrospective databases. or by statistical techniques

Step 5: 我該如何利用臨床研究的結果照顧我 的病人?

Evidence is Never Enough!! n Predictive model of diagnosing probable cases of severe acute respirator syndrome in febrile patients with exposure risk n Validation of a novel severe acute respiratory syndrome scoring system Annals of Emergency Medicine Jan 2004: 43(1)
cdfe037a7230676e670b7f916926e4bc.ppt